Suprapatellar Versus Infrapatellar Tibial Nail Insertion: A Prospective Randomized Control Pilot Study
|
|
|
- Moris Austin
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Suprapatellar Versus Infrapatellar Tibial Nail Insertion: A Prospective Randomized Control Pilot Study Daniel S. Chan, MD, Rafael Serrano-Riera, MD, Rebecca Griffing, BSc, Barbara Steverson, RN, MHA, Anthony Infante, DO, David Watson, MD, H. Claude Sagi, MD, and Roy W. Sanders, MD Purpose: The purpose of this OTA-approved pilot study was to compare the clinical and functional outcomes of the knee joint after infrapatellar (IP) versus suprapatellar (SP) tibial nail insertion. Design: Prospective, randomized. Setting: Level I trauma center. Methods: After institutional review board approval, skeletally mature patients with OTA 42 tibial shaft fractures were randomized into either an IP or SP nail insertion group after informed consent was obtained. The SP also underwent prenail and postnail insertion patella-femoral (PF) joint arthroscopy. Patients underwent follow-up (6 weeks, 3, 6, and 12 months) with standard radiographs, as well as visual analog score and pain diagram documentation. At the 6-month and 12-month visits, knee function questionnaires (Lysholm knee scale and SF-36) were completed. Magnetic resonance imaging/ image (MRI) of the affected knee was obtained at 12 months. Ten patients in each group were required for a power analysis for the anticipated larger randomized control trial, but enrollment in each arm was not limited because of known problems with patient follow-up over a 12-month period. Results: A total of 41 patients/fractures were enrolled in this study. Of those, only 25 patients/fractures (14 IP, 11 SP) fully complied with and completed 12 months of follow-up. Six of 11 SP presented with articular changes (chondromalacia) in the PF joint during the preinsertion arthroscopy. Three patients displayed a change in the articular cartilage based on postnail insertion arthroscopy. At 12 months, all fractures in both groups had proceeded to union. There were no differences between the affected and unaffected knee with Accepted for publication November 16, From the Orthopaedic Trauma Service, Florida Orthopaedic Institute, Tampa, FL. Supported by a grant from the Orthopaedic Trauma Association. Presented in part at the Annual Meeting of the OTA, October 2014, Tampa, FL. D. S. Chan: consultant for Biomet, Synthes, Smith & Nephew. A. Infante: consultant for OmniLife Sciences and Arthrosurface. D. Watson: consultant for Smith & Nephew. H. C. Sagi: consultant for Smith & Nephew, Synthes, and Stryker. R. W. Sanders: Editor-in-Chief Journal of Orthopaedic Trauma, Consultant (Smith and Nephew, Zimmer-Biomet), Royalties (Smith and Nephew, Zimmer-Biomet, Linvatec). The remaining authors report no conflict of interest. This study was approved by the Institutional Review Board at the University of South Florida. Reprints: Daniel S. Chan, MD, Georgia Orthopaedic Trauma Institute, Medical Center of Central Georgia, 840 Pine St, Suite 500, Macon, GA ( chan.daniel@mccg.org). Wolters Kluwer Health, Inc. All rights reserved. respect to range of motion. Functional visual analog score and Lysholm knee scores showed no significant differences between groups (P. 0.05). The SF-36v2 comparison also revealed no significant differences in the overall score, all 4 mental components, and 3/4 physical components (P. 0.05). The bodily pain component score was superior in the SP group (45 vs. 36, P = 0.035). All 11 SP patients obtained MRIs at 1 year. Five of these patients had evidence of chondromalacia on MRI. These findings did not correlate with either the prenail or postnail insertion arthroscopy. Importantly, no patient in the SP group with postnail insertion arthroscopic changes had PF joint pain at 1 year. Conclusions: Overall, there seemed to be no significant differences in pain, disability, or knee range of motion between these 2 tibial intramedullary nail insertion techniques after 12 months of followup. Based on this pilot study data, larger prospective trial with longterm follow-up is warranted. Key Words: suprapatellar, infrapatellar, tibial, tibial nail insertion Level of Evidence: Therapeutic Level II. See Instructions for Authors for a complete description of levels of evidence. (J Orthop Trauma 2016;30: ) INTRODUCTION The insertion of a reamed intramedullary nail (IMN) with interlocking screws is the standard of care for operatively managed tibial shaft fractures. 1 Traditionally, an infrapatellar (IP) approach through or around the patellar tendon, with a flexed or hyperflexed knee, is performed to insert an IMN. 2,3 This insertion site, which requires a flexed knee, becomes more difficult to use correctly in proximal third tibial shaft fractures, because the quadriceps muscle forces the proximal fragment into extension, resulting in a procurvatum deformity postnail insertion. 4,5 The semiextended approach for tibial IMN insertion, to address this risk of malalignment, was first described by Tornetta et al 6 and later modified to a percutaneous suprapatellar (SP) approach by Cole. 7 Through a 2.5-cm incision proximal to the patella, the quadriceps tendon is split to obtain access to the SP pouch and retro-patellar space. A cannula system then allows for the standard insertion of the tibial nail. The full, or near-full, extension position of the leg not only assists in neutralizing the deforming forces of the quadriceps muscle and maintaining proper alignment of the proximal tibia, but the position also helps align comminuted shaft fractures or highly unstable distal third fractures, where maintaining J Orthop Trauma Volume 30, Number 3, March 2016
2 J Orthop Trauma Volume 30, Number 3, March 2016 SP Versus IP Tibial Nail Insertion reduction against gravity in the flexed or hyperflexed position can be extremely challenging. Additionally, the extended position of the lower leg allows for easier fluoroscopic imaging. Although the semiextended procedure requires a formal parapatellar incision, the SP approach is truly percutaneous. The main concern in its use is the potential for damage to the patellafemoral (PF) articulation. This study was a prospective, randomized clinical trial designed to (1) determine whether the SP approach was equivalent to the IP approach with respect to knee pain, (2) determine whether the SP approach was equivalent to the IP approach with respect to healing, alignment, and knee function, and (3) evaluate the safety of the SP approach. STUDY SUPPORT This study was funded as an OTA pilot study and approved by our institutional review board. Preinsertion and postinsertion arthroscopies for the SP patients were not billed because it was considered as part of the procedure. Magnetic resonance imaging/image (MRI) studies were paid for by a grant from the OTA. Furthermore, as a pilot study, formal sample size calculations were not performed, because the information obtained from this investigation would specifically enable a proper power analysis for the future larger prospective study. Although 10 fractures were originally agreed on in each group based on the study budget, 20 patients in each group were planned because of known difficulties with patient follow-up for 12 months. PATIENTS AND METHODS Between April 2011 and December 2012, skeletally mature patients with OTA 42 tibial shaft fractures were randomized into the IP or SP nail insertion groups after informed consent was obtained. Sealed envelopes in a random order were sequentially opened after each patient was enrolled. At that preoperative moment, the technique for nail insertion was revealed to both the surgeon and patient. Patients with intraarticular involvement, peri-prosthetic fractures, nonunions, ipsilateral concomitant injuries, previous knee surgery, or a history of gout, rheumatoid, osteoarthritis, spinal injury, incarceration; patients not likely to follow-up in the estimation of surgeon; or pregnant women were excluded. Patient s age, gender, fracture classification (OTA 42 A, B, C 8 ), and Gustilo Anderson type were recorded. Standard surgical techniques were used (medial parapatellar IP approach; quadriceps tendon split SP approach). All fractures were treated with a statically locked reamed IMN (Trigen Meta Nail; Smith and Nephew, Memphis, TN). SP insertion was performed percutaneously with the use of a commercial available cannula system (Smith and nephew). SP patients also underwent arthroscopy limited to the PF joint, prenail and postnail insertion, to obtain TABLE 1. Patient Demographics Pt Sex Age (y) Side OTA Class Open Fx/ Grade Suprapatellar 1 F 51 L 42B1.2 Closed 12 2 M 30 L 42B2.3 Closed 12 3 F 42 L 42C2.2 Closed 12 4 M 48 L 42A3.3 Closed 13 5 M 21 L 42A2.3 Closed 14 6 M 64 L 43A2.3 Closed 32 7 M 23 R 42A3.1 3A 31 8 F 51 R 42A2.2 Closed 19 9 F 55 R 42A3.2 Closed F 29 R 42A2.2 Closed M 24 R 42B2.1 Closed 15 Infrapatellar 1 M 20 L 42B M 23 L 42A2.3 Closed 12 3 F 47 L 42C1.1 Closed 14 4 M 28 L 42A2.2 Closed 14 5 M 45 R 42C M 62 R 42B2.3 Closed 12 7 F 48 R 42A2.2 Closed 12 8 F 19 R 42B2.3 Closed 13 9 M 69 R 42B2.3 Closed M 43 R 42A2.1 Closed M 18 R 42A2.3 Closed M 59 R 42C3.1 Closed F 35 R 42B3.3 Closed M 82 L 42A1.2 Closed 12 Length of F/U (mos) Wolters Kluwer Health, Inc. All rights reserved
3 Chan et al J Orthop Trauma Volume 30, Number 3, March 2016 a visual evaluation of the PF joint. Images were obtained, saved, and reviewed by an independent fellowship-trained sports medicine orthopaedic surgeon to assess the PF joint for any associated injury. The Outerbridge scale was used to describe the condition of the articular cartilage: grade 0, normal cartilage; grade I, cartilage with softening and swelling; grade II, fragmenting or fissuring,1.5 cm diameter; grade III, fragmenting or fissuring.1.5 cm diameter; grade IV, exposed subchondral bone. Patients underwent routine follow-up (6 weeks, 3, 6, and 12 months) with standard tibia and knee radiographs, as well as a visual analog score (VAS, 0 = excellent, 10 = extreme pain) and pain diagram documentation. At the 6- and 12-month visits, subjective complaints were recorded and a range of motion (ROM) arc was measured. Patient s function was assessed through a completed knee function questionnaire (Lysholm knee scale 9 ) and SF-36v2. All clinical examinations for the purposes of this study were performed by research nurses during a separate clinic visit. Additionally, in the SP group, an MRI of the affected knee was obtained at 12 months and independently reviewed by a board-certified, fellowshiptrained musculoskeletal radiologist. All radiographs were reviewed by the fellowship-trained orthopaedic trauma attending to assess union and alignment. Successful union criteria were the radiographic presence of callus formation bridging at least 3 cortices on orthogonal views of the fracture. Descriptive statistics were reported as mean values and SDs for continuous variables and as frequencies and percentages for categorical variables. RESULTS A total of 41 patients/fractures were enrolled in this study, 23 SP and 18 IP. All fractures were OTA 42. Twelve SP and 4 IP patients either were lost or refused to come back for the follow-up examinations, leaving 25 patients/fractures available at a minimum of 12 months. There were 11 SP and 14 IP patients/fractures. The average time from index procedure to final follow-up was months (range: months) (Table 1). Average age was 42 years (SP = 40, IP = 43), and the predominant sex was male. There were 3 open (SP: 1 3A, IP: 1 type 1, 1 type 2) and 22 closed fractures. All but 1 fracture healed radiographically without deformity. One SP case progressed to a nonunion and required revision IMN insertion, after exchange nailing using the SP portal again. There were no deep infections. Knee ROM was normal and equal to the unaffected contralateral knee in both the SP and IP groups (extension: 0 degree IP, 1 degree SP, P = 0.5;flexion 1 degree IP, 23 degree SP, P = 1.0) (Table 2). The VAS pain scores averaged 1.5 for the IP group. 11/ 14 had a VAS#1. One patient who lacked housing and had an alcohol addiction complained of mild pain (VAS = 3), but this was related to the development of recurrent cellulitis in the leg beginning at the 6-month examination. The remaining 2 IP patients complained of knee pain at the incision site as severe (8 and 10). The VAS score in the SP group averaged 0.36, with 9/11 having a VAS of 0, 1 patient having a VAS = 1, and 1 patient complaining of mild pain (VAS = 3) only when bending the knee. There was no significant statistical difference in VAS scores between the IP and SP groups. The mean Lysholm knee scores were 86 and 98 for the IP and SP groups, respectively, they were not statistically different; as was the case for the Lysholm pain component scores (20 IP vs. 24 SP). Additionally, the SF-36v2 scores were 38/47 for the IP group compared with 46/47 for the SP group. This comparison revealed no significant differences in the overall score, as well as all 4 mental components and 3 of the 4 physical components (P. 0.05). The bodily pain component score was superior in the SP group (46 vs. 36, P = 0.035) suggesting less pain and disability. All 11 SP patients had prenailing and postnailing PF joint arthroscopy performed. Six patients exhibited prenail insertion PF joint chondromalacia patella (Table 3). Three patients had a change in the degree or location of chondromalacia after the nail was inserted. While one of these had preexisting disease, 2 did not. One SP patient seemed to have sustained an iatrogenic scratching of a small portion of the trochlea notch (normal PF examination, grade 0, pre-imn; grade 2 trochlea chondral damage post-imn), whereas 1 patient sustained damage to the undersurface of the patella with changes visible on the MRI (normal PF examination, grade 0, pre-imn, grade 4 chondromalacia patella post- IMN). All SP patients were clinically symptom-free with full return to normal activities at 1 year after index procedure. DISCUSSION There is little information regarding the clinical outcomes in IMN insertion using the SP portal To our knowledge, this is the first report of a randomized clinical TABLE 2. Twelve-Month Outcome Data Analysis Union 100% 100% Malalignment 0% 0% VAS Lysholm-Pain Lysholm SF36-PCS SF36-MCS Physical Functioning Role-physical Bodily Pain 36 46* General Health Vitality Social Functioning Role-emotional Mental Health Affected Extension Unaffected Extension Difference-Extension Affected Flexion Unaffected Flexion Difference-Flexion *P = (Mann Whitney U test). MCS, mental component summary; PCS, physical component summary. IP SP Wolters Kluwer Health, Inc. All rights reserved.
4 J Orthop Trauma Volume 30, Number 3, March 2016 SP Versus IP Tibial Nail Insertion TABLE 3. Patellofemoral Breakdown Pt F/U, mo Arthroscopy MRI: Chondromalacia 1-yr F/U Knee Pain Prenail Postnail Insertion Patellae PFJ Other Suprapatellar P 2P Yes No No P 2P No No No P 2P No No Screw head P 1P Yes No No No No No P Yes No No Yes No Screw head P, 2T 4P, 4T No No No P 2P Yes No No No No No T No No No Infrapatellar 1 12 No No 2 12 No Incision 3 14 No No 4 14 No No 5 13 No Nail insertion 6 12 No No 7 12 No No 8 13 No No 9 13 No No No No No No No Screw head No No No Screw head PFJ, patellofemoral joint. Site of chondromalacia T: trochlea, P: patella. Bold indicates change postnail. trial comparing IP and SP tibial IMN approaches. Although this was only a pilot study, our results show that the SP approach is equivalent to the traditional IP technique with regard to union, alignment, knee pain, and functional outcomes. Based on our data including arthroscopic prenailing and postnailing assessments, 1 year postoperative MRI, and functional outcomes, it seems that the SP method, when using insertional cannulas, does not cause injury to the PF joint. Decreased ROM postoperatively is an undesirable outcome of IMN of the tibia and well documented in the literature. 13 Lefaivre et al 14 reported on long-term follow-up after standard (IP) tibial IMN insertion and found equivalent knee ROM to the unaffected contralateral knee. Our study reproduced these findings in both IP and SP patients alike. Anterior knee pain is frequently associated with IMN insertion of tibia fractures. Its incidence has been reported to be as high as 56%. 15,16 The cause is still unclear. Toivanen found that 69% of patients treated with an IMN using the IP approach continued to have pain even after implant removal. 17 In our small series, 2 IP insertion patients complained of anterior knee symptoms (one incisional, one tibial IMN insertion site). In the SP group, none of the patients complained of anterior knee pain. This was also the finding in a recent report evaluating anterior knee pain in SP IMN insertion patients. 18 The absence of an incision or dissection around the IP area with complete avoidance of the IP branches of the saphenous nerve may be the reason for this finding. In any event, the fact that no SP patient had anterior knee pain was encouraging. Nork et al 19 evaluated patients well-being using the SF-36 after tibial IMN using an IP approach, with a minimum follow-up of 1 year, and noted that physical function, role-physical, and bodily pain were significantly worse than standard normative data. Our SF-36 data indicated that all components but one were equivalent between the 2 groups: bodily pain was worse in the IP group when compared with the SP cohort at 1 year postoperatively. We surmise that again this may be related to anterior knee pain in IP insertion patients. The Lysholm knee scores provide a validated and quantified comparison of patient activities of daily living. Song et al 20 reported a significant correlation between Lysholm scores and anterior knee pain in patients who underwent tibial IM nailing. In our study, the SP score of 98 is considered an excellent outcome, compared with the IP Wolters Kluwer Health, Inc. All rights reserved
5 Chan et al J Orthop Trauma Volume 30, Number 3, March 2016 group score of 86 which is considered good. Similarly, pain measured through the Lysholm pain component showed that the SP group reported less pain while walking compared with their IP counterparts. Although there were no significant differences between groups, both groups did report low incidences of knee pain. Interpreting all of the outcome results, we found overall consistency. The Lysholm knee scores are a functional assessment and are not limited to pain, much like the role-physical subscale of the SF-36; therefore, the equivalence of both scores between SP and IP was expected. The VAS score is more specific to pain and was not statistically significantly different; however, the SP patients did trend to having less pain. The SF-36 bodily pain score also showed that the IP group had worse pain; questionnaire differences likely led to statistical significance. Finally, although MRIs were used to assist in the evaluation of any cartilage changes at the 1-year mark, they did not seem to offer any significant benefit due to lack of sensitivity and/or specificity. There were a few limitations in this study. It was not a blinded study. If the nail insertion technique was blinded to the patient with an additional incision, an added level of objectivity would have been an enhancement, but this was not contemplated for obvious reasons. There did not seem to be any characteristics or anticipated outcomes about those lost to follow-up that would have affected the observed results. The main limitation of this study was that it was a pilot study designed to develop a larger cohort to evaluate. Based on these data, we plan a larger, multicenter randomized control trial, in the hopes of determining both the efficacy of this technique and whether this approach can minimize anterior knee pain. CONCLUSIONS Based on the data of this OTA-approved pilot study, we conclude that the SP approach is equivalent to the IP approach with respect to tibial fracture healing and alignment, knee pain, functional disability, or knee ROM. We were unable to find any PF joint damage clinically and were able to show that anterior knee pain was less prevalent in the SP than the IP approach. A larger prospective trial with long-term follow-up is needed to improve statistical power and establish if any late sequelae exist, when the procedure is properly performed. REFERENCES 1. Bone LB, Johnson KD. Treatment of tibial fractures by reaming and intramedullary nailing. J Bone Joint Surg Am. 1986;68: Weller S, Kuner E, Schweikert CH. Medullary nailing according to Swiss study group principles. Clin Orthop Relat Res. 1979;138: Lottes JO. Medullary nailing of the tibia with the triflanged nail. Clin Orthop. 1974;105: Freedman EL, Johnson EE. Radiographic analysis of tibial fracture malalignment following intramedullary nailing. Clin Orthop Relat Res. 1995;315: Josten C, Marquass B, Schwarz C, et al. Intramedullary nailing of proximal tibial fractures. Complications and risk factors. Unfallchirurg. 2010; 113: Tornetta P III, Riina J, Geller J, et al. Intraarticular anatomic risks of tibial nailing. J Orthop Trauma. 1999;13: Cole JD. Distal tibia fracture: opinion: intramedullary nailing. J Orthop Trauma. 2006;20: Marsh JL, Slongo TF, Agel J, et al. Fracture and dislocation classification compendium 2007: Orthopaedic Trauma Association classification, database and outcomes committee. J Orthop Trauma. 2007;21: S1 S Collins NJ, Misra D, Felson DT, et al. Measures of knee function: international knee documentation committee (IKDC) subjective knee evaluation form, knee injury and osteoarthritis outcome score (KOOS), knee injury and osteoarthritis outcome score physical function short form (KOOS-PS), knee outcome survey activities of daily living scale (KOS-ADL), Lysholm knee scoring scale, oxford knee score (OKS), western ontario and mcmaster universities osteoarthritis index (WOMAC), activity rating scale (ARS), and tegner activity score (TAS). Arthritis Care Res (hoboken). 2011;63 (suppl 11):S208 S Gelbke MK, Coombs D, Powell S, et al. Suprapatellar versus infrapatellar intramedullary nail insertion of the tibia: a cadaveric model for comparison of patellofemoral contact pressures and forces. J Orthop Trauma. 2010;24: Eastman J, Tseng S, Lo E, et al. Retropatellar technique for intramedullary nailing of proximal tibia fractures: a cadaveric assessment. J Orthop Trauma. 2010;24: Eastman JG, Tseng SS, Lee MA, et al. The retropatellar portal as an alternative site for tibial nail insertion: a cadaveric study. J Orthop Trauma. 2010;24: Keating JF, O Brien PI, Blachut PA, et al. Reamed interlocking IMN of open fractures of the tibia. Clin Orthop Relat Res. 1997; 338: Lefaivre KA, Guy P, Chan H, Blachut PA. Long-term follow-up of tibial shaft fractures treated with IMN. J Orthop Trauma. 2008;22: Keating JF, Orfaly R, O Brien PJ. Knee pain after tibial nailing. J Orthop Trauma. 1997;11: Court-Brown CM, Gustilo T, Shaw AD. Knee pain after intramedullary tibial nailing: its incidence, etiology, and outcome. J Orthop Trauma. 1997;11: Toivanen JA, Vaisto O, Kannus P, et al. Anterior knee pain after intramedullary nailing of fractures of the tibial shaft. A prospective, randomized study comparing two different nail-insertion techniques. J Bone Joint Surg Am. 2002;84-A: Sanders RW, DiPasquale TG, Jordan CJ, et al. Semiextended IMN of the tibia using suprapatellar approach: radiographic results and clinical outcomes at a minimum or 12 Months Follow-up. J Orthop Trauma. 2014; 28:S29 S Nork SE, Schwartz AK, Agel J, et al. IMN of distal metaphyseal tibial fractures. J Bone Joint Surg Am. 2005;87-A: Song SY, Chang HG, Byun JC, et al. Anterior knee pain after tibial IMN using a medial paratendinous approach. J Orthop Trauma. 2012; 26: Wolters Kluwer Health, Inc. All rights reserved.
Int J Clin Exp Med 2019;12(1): /ISSN: /IJCEM
 Int J Clin Exp Med 2019;12(1):804-811 www.ijcem.com /ISSN:1940-5901/IJCEM0082501 Original Article Comparison of suprapatellar and infrapatellar tibial nailing: more anatomic entry point and fracture reduction
Int J Clin Exp Med 2019;12(1):804-811 www.ijcem.com /ISSN:1940-5901/IJCEM0082501 Original Article Comparison of suprapatellar and infrapatellar tibial nailing: more anatomic entry point and fracture reduction
FIRST DESCRIBED RETROGRADE TECHNIQUE USING MEDIAL EPICONDYLE 6/5/2018. RETROGRADE vs. ANTEGRADE FEMORAL NAILING
 What do I do? ISSUES ANTEGRADE vs. RETROGRADE PIRIFORMIS vs. TROCHANTER FLAT vs. FRACTURE TABLE SWIONTKOWSKI, 1984 FIRST DESCRIBED RETROGRADE TECHNIQUE USING MEDIAL EPICONDYLE 1 RETROGRADE NAILING SANDERS
What do I do? ISSUES ANTEGRADE vs. RETROGRADE PIRIFORMIS vs. TROCHANTER FLAT vs. FRACTURE TABLE SWIONTKOWSKI, 1984 FIRST DESCRIBED RETROGRADE TECHNIQUE USING MEDIAL EPICONDYLE 1 RETROGRADE NAILING SANDERS
Principles Starting Point Trajectory L/A/R Stable Construct. DISCLOSURES Hassan R. Mir, MD, MBA, FACS 5/16/2017
 DISCLOSURES Hassan R. Mir, MD, MBA, FACS Medical/Orthopaedic Publications Editorial/Governing Board OTA Newsletter Editor OsteoSynthesis, The JOT Online Discussion Forum Editor JOT Associate Editor JAAOS
DISCLOSURES Hassan R. Mir, MD, MBA, FACS Medical/Orthopaedic Publications Editorial/Governing Board OTA Newsletter Editor OsteoSynthesis, The JOT Online Discussion Forum Editor JOT Associate Editor JAAOS
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Problems, Tricks, and Pearls in Intramedullary Nailing of Proximal Third Tibial Fractures
 STATE OF THE ART Problems, Tricks, and Pearls in Intramedullary Nailing of Proximal Third Tibial Fractures Frank A. Liporace, MD,* Christopher M. Stadler, BS,* and Richard S. Yoon, MD Summary: Proximal
STATE OF THE ART Problems, Tricks, and Pearls in Intramedullary Nailing of Proximal Third Tibial Fractures Frank A. Liporace, MD,* Christopher M. Stadler, BS,* and Richard S. Yoon, MD Summary: Proximal
EVOS MINI with IM Nailing
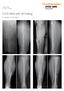 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of The Tibia
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
Techique. Results. Discussion. Materials & Methods. Vol. 2 - Year 1 - December 2005
 to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
Anterior knee pain following the lateral parapatellar approach for tibia nailing
 Original Article Anterior knee pain following the lateral parapatellar approach for tibia nailing Simarjot S Bedi*, R K Arora**, Yogeshwar Saini*** *Junior Resident, ** Professor, *** Professor & Head
Original Article Anterior knee pain following the lateral parapatellar approach for tibia nailing Simarjot S Bedi*, R K Arora**, Yogeshwar Saini*** *Junior Resident, ** Professor, *** Professor & Head
ORIGINAL ARTICLE. Copyright Ó 2017 Wolters Kluwer Health, Inc. Unauthorized reproduction of this article is prohibited.
 ORIGINAL ARTICLE Percutaneous or Open Reduction of Closed Tibial Shaft Fractures During Intramedullary Nailing Does Not Increase Wound Complications, Infection or Nonunion Rates Downloaded from https://journals.lww.com/jorthotrauma
ORIGINAL ARTICLE Percutaneous or Open Reduction of Closed Tibial Shaft Fractures During Intramedullary Nailing Does Not Increase Wound Complications, Infection or Nonunion Rates Downloaded from https://journals.lww.com/jorthotrauma
Safe surgical technique: intramedullary nail fixation of tibial shaft fractures
 Safe surgical technique: intramedullary nail fixation of tibial shaft fractures Zelle and Boni Patient Safety in Surgery (2015) 9:40 DOI 10.1186/s13037-015-0086-1 Zelle and Boni Patient Safety in Surgery
Safe surgical technique: intramedullary nail fixation of tibial shaft fractures Zelle and Boni Patient Safety in Surgery (2015) 9:40 DOI 10.1186/s13037-015-0086-1 Zelle and Boni Patient Safety in Surgery
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Extra-Articular Technique for Semiextended Tibial Nailing
 TECHNICAL TRICK Extra-Articular Technique for Semiextended Tibial Nailing Erik N. Kubiak, MD, Benjamin J. Widmer, MD, and Dan S. Horwitz, MD Downloaded from https://journals.lww.com/jorthotrauma by jychnns+ndjtuoldgsayoccoh2d3hqwbumbvweq6h8ex1ivqeup0w62/kqz3u/duqpzn40ux6scfmfy0qj7ou28ird4z/icxe51mlqzje+dhzfkrfjxv7yr3yigoptr5
TECHNICAL TRICK Extra-Articular Technique for Semiextended Tibial Nailing Erik N. Kubiak, MD, Benjamin J. Widmer, MD, and Dan S. Horwitz, MD Downloaded from https://journals.lww.com/jorthotrauma by jychnns+ndjtuoldgsayoccoh2d3hqwbumbvweq6h8ex1ivqeup0w62/kqz3u/duqpzn40ux6scfmfy0qj7ou28ird4z/icxe51mlqzje+dhzfkrfjxv7yr3yigoptr5
JOURNALOF ORTHOPAEDIC TRAUMA
 JOT Special Case Report Series CASE REPORTS www.jorthotrauma.com JOURNALOF ORTHOPAEDIC TRAUMA OFFICIAL JOURNAL OF Orthopaedic Trauma Association Belgian Orthopaedic Trauma Association Canadian Orthopaedic
JOT Special Case Report Series CASE REPORTS www.jorthotrauma.com JOURNALOF ORTHOPAEDIC TRAUMA OFFICIAL JOURNAL OF Orthopaedic Trauma Association Belgian Orthopaedic Trauma Association Canadian Orthopaedic
Bad Ankle with Soft Tissue Injuries: Fix them all Now! Don t Wait! BOB ZURA, MD OSET 2017 LAS VEGAS
 Bad Ankle with Soft Tissue Injuries: Fix them all Now! Don t Wait! BOB ZURA, MD OSET 2017 LAS VEGAS Disclosures Consultant: Smith-Nephew Bioventus Cardinal Health https://orthointerview.com/news/files/painful-tendon-after-severe-ankle-fracture-21312561.jpg
Bad Ankle with Soft Tissue Injuries: Fix them all Now! Don t Wait! BOB ZURA, MD OSET 2017 LAS VEGAS Disclosures Consultant: Smith-Nephew Bioventus Cardinal Health https://orthointerview.com/news/files/painful-tendon-after-severe-ankle-fracture-21312561.jpg
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
DISCLOSURES Hassan R. Mir, MD, MBA, FACS
 DISCLOSURES Hassan R. Mir, MD, MBA, FACS Medical/Orthopaedic Publications Editorial/Governing Board OTA Newsletter Editor OsteoSynthesis, The JOT Online Discussion Forum Editor JOT Associate Editor JAAOS
DISCLOSURES Hassan R. Mir, MD, MBA, FACS Medical/Orthopaedic Publications Editorial/Governing Board OTA Newsletter Editor OsteoSynthesis, The JOT Online Discussion Forum Editor JOT Associate Editor JAAOS
Intramedullary Nailing of Proximal Quarter Tibial Fractures
 ORIGINAL ARTICLE Intramedullary Nailing of Proximal Quarter Tibial Fractures Downloaded from https://journals.lww.com/jorthotrauma by 8WXeIBH/bhCDXSJhqO4He3zMjDdiDlokyQtApC91PNKG9a/tPy2o9wvYA84dGjHINiBelbocxVu63ADM4AGx5PeXfLYAE9Wwxl/hAO/UvnoQeL/3rrYADLWqdS4+DwtVQeM+OnUtY1I=
ORIGINAL ARTICLE Intramedullary Nailing of Proximal Quarter Tibial Fractures Downloaded from https://journals.lww.com/jorthotrauma by 8WXeIBH/bhCDXSJhqO4He3zMjDdiDlokyQtApC91PNKG9a/tPy2o9wvYA84dGjHINiBelbocxVu63ADM4AGx5PeXfLYAE9Wwxl/hAO/UvnoQeL/3rrYADLWqdS4+DwtVQeM+OnUtY1I=
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
The study of distal ¼ diaphyseal extra articular fractures of humerus treated with antegrade intramedullary interlocking nailing
 2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
Treatment of Diaphysio-Metaphyseal Fracture of Tibia by Intramedullary Nail in Combination with Poller Screw
 Research Article imedpub Journals http://www.imedpub.com DOI: 10.4172/2469-6684.10001 Treatment of Diaphysio-Metaphyseal Fracture of Tibia by Intramedullary Nail in Combination with Poller Screw Ram Kewal
Research Article imedpub Journals http://www.imedpub.com DOI: 10.4172/2469-6684.10001 Treatment of Diaphysio-Metaphyseal Fracture of Tibia by Intramedullary Nail in Combination with Poller Screw Ram Kewal
Treatment Alternatives for Pediatric Femoral Fractures
 Treatment Alternatives for Pediatric Femoral Fractures Gregory A. Schmale, MD Seattle Children's Hospital, USA, gregory.schmale@seattlechildrens.org version 2 I have no conflicts of interest to report
Treatment Alternatives for Pediatric Femoral Fractures Gregory A. Schmale, MD Seattle Children's Hospital, USA, gregory.schmale@seattlechildrens.org version 2 I have no conflicts of interest to report
Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Conflict of Interest 9/24/2015
 Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Cory Collinge, MD Professor of Orthopedic Surgery Vanderbilt University Medical Center Nashville, TN Conflict of Interest Consultant: Smith
Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Cory Collinge, MD Professor of Orthopedic Surgery Vanderbilt University Medical Center Nashville, TN Conflict of Interest Consultant: Smith
Tibial Shaft Fractures
 Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
Plate Fixation Options
 Distal tibia extra-articular fractures can be difficult to treat Tenuous soft tissue Complex fracture patterns Plate Fixation Options Medial plating: Minimally invasive approach Technical ease Anterolateral
Distal tibia extra-articular fractures can be difficult to treat Tenuous soft tissue Complex fracture patterns Plate Fixation Options Medial plating: Minimally invasive approach Technical ease Anterolateral
Minimally Invasive Plating of Fractures:
 Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Principles of intramedullary nailing. Management for ORP
 Principles of intramedullary nailing Eakachit Sikarinklul,MD Basic Principles of Fracture Management for ORP Bangkok Medical Center Bangkok, 22-24 July 2016 Learning outcomes At the end of this lecture
Principles of intramedullary nailing Eakachit Sikarinklul,MD Basic Principles of Fracture Management for ORP Bangkok Medical Center Bangkok, 22-24 July 2016 Learning outcomes At the end of this lecture
Diabetics. Referred for management of complex pilon fracture? 5/10/2017. Pilon Fractures: Exfix as definitive treatment (DM?)
 Pilon Fractures: Exfix as definitive treatment (DM?) Nirmal C Tejwani, MD Professor, NYU Langone Orthopedics Chief of Trauma, Bellevue Hospital, New York, NY 29 th Annual Orthopaedic Trauma Meeting May
Pilon Fractures: Exfix as definitive treatment (DM?) Nirmal C Tejwani, MD Professor, NYU Langone Orthopedics Chief of Trauma, Bellevue Hospital, New York, NY 29 th Annual Orthopaedic Trauma Meeting May
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
The Journal of the Korean Society of Fractures Vol.13, No.3, July, 2000
 The Journal of the Korean Society of Fractures Vol13, No3, July, 2000 2, 3 ) : 40-12, Tel : (02) 966-1616 Fax : (02) 968-2394 E-mail : adkajs@thrunetcom 471 8, 1 2 ) (Table 1) 1 6 14, 2 1 2 1 Ender 29
The Journal of the Korean Society of Fractures Vol13, No3, July, 2000 2, 3 ) : 40-12, Tel : (02) 966-1616 Fax : (02) 968-2394 E-mail : adkajs@thrunetcom 471 8, 1 2 ) (Table 1) 1 6 14, 2 1 2 1 Ender 29
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES
 BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
Angular Malalignment in Subtrochanteric and Proximal Shaft Femur Fractures after Intramedullary Nailing using SIGN Nails
 Angular Malalignment in Subtrochanteric and Proximal Shaft Femur Fractures after Intramedullary Nailing using SIGN Nails Rolando Junior L. Torres, MD Jeremiah R. Morales, MD, FPOA Subtrochanteric Femur
Angular Malalignment in Subtrochanteric and Proximal Shaft Femur Fractures after Intramedullary Nailing using SIGN Nails Rolando Junior L. Torres, MD Jeremiah R. Morales, MD, FPOA Subtrochanteric Femur
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of partial replacement of the meniscus of the knee using a biodegradable scaffold
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of partial replacement of the meniscus of the knee using a biodegradable scaffold
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Diaphyseal Humerus Fractures. OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD
 Diaphyseal Humerus Fractures OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD OBJECTIVES TREATMENT OPTIONS SURGICAL INDICATIONS CONTROVERSIES IN MANAGEMENT Humerus Fractures Treatment Goals: Functional
Diaphyseal Humerus Fractures OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD OBJECTIVES TREATMENT OPTIONS SURGICAL INDICATIONS CONTROVERSIES IN MANAGEMENT Humerus Fractures Treatment Goals: Functional
Neurologic Damage. The most common neurologic injury following intramedullary tibial nailing is injury to the peroneal nerve.
 COMPLICATIONS Knee Pain Anterior knee pain was present in 55% Affects younger more than older patients A significant number of the patients with anterior knee pain had pain with kneeling [90%] They also
COMPLICATIONS Knee Pain Anterior knee pain was present in 55% Affects younger more than older patients A significant number of the patients with anterior knee pain had pain with kneeling [90%] They also
Meniscal Injuries with Tibial Plateau Fractures: Role of Arthroscopy
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Meniscal Injuries with Tibial Plateau Fractures: Role of Arthroscopy Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid 3, Munir
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Meniscal Injuries with Tibial Plateau Fractures: Role of Arthroscopy Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid 3, Munir
Locked plating constructs are creating a challenge for surgeons.
 Locked plating constructs are creating a challenge for surgeons. Three recent studies examining supracondylar femur fractures show concern for the high degree of stiffness of locked plating constructs
Locked plating constructs are creating a challenge for surgeons. Three recent studies examining supracondylar femur fractures show concern for the high degree of stiffness of locked plating constructs
To study outcome of surgical management of distal 3rd and proximal 3rd fractures of tibia in adults using expert tibial nails
 International Journal of Research in Orthopaedics Kachhap ND et al. Int J Res Orthop. 2017 Jul;3(4):862-866 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20172887
International Journal of Research in Orthopaedics Kachhap ND et al. Int J Res Orthop. 2017 Jul;3(4):862-866 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20172887
Clinical Results of Genesis-I Total Knee Arthroplasty
 Acta Medica et Biologica Vol. 49, No.2, 47-52, 2001 Clinical Results of Genesis-I Total Knee Arthroplasty for Patients with Knee Osteoarthritis: A Five-year Longitudinal Study H aojiang Kuanyu LIU1, Go
Acta Medica et Biologica Vol. 49, No.2, 47-52, 2001 Clinical Results of Genesis-I Total Knee Arthroplasty for Patients with Knee Osteoarthritis: A Five-year Longitudinal Study H aojiang Kuanyu LIU1, Go
Segmental tibial fractures treated with unreamed interlocking nail A prospective study
 2017; 3(2): 714-719 ISSN: 2395-1958 IJOS 2017; 3(2): 714-719 2017 IJOS www.orthopaper.com Received: 13-02-2017 Accepted: 14-03-2017 Ashok Singhvi Hemant Jain Siddharth Jauhar Kishore Raichandani Segmental
2017; 3(2): 714-719 ISSN: 2395-1958 IJOS 2017; 3(2): 714-719 2017 IJOS www.orthopaper.com Received: 13-02-2017 Accepted: 14-03-2017 Ashok Singhvi Hemant Jain Siddharth Jauhar Kishore Raichandani Segmental
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
Comparison between Intramedullary Nailing and Percutaneous K-Wire Fixation for Fractures in the Distal Third of the Metacarpal Bone
 Comparison between Nailing and K-Wire Fixation for Fractures in the Distal Third of the Metacarpal Bone Original Article Sung Jun Moon 1, Jae-Won Yang 2, Si Young Roh 1, Dong Chul Lee 1, Jin Soo Kim 1
Comparison between Nailing and K-Wire Fixation for Fractures in the Distal Third of the Metacarpal Bone Original Article Sung Jun Moon 1, Jae-Won Yang 2, Si Young Roh 1, Dong Chul Lee 1, Jin Soo Kim 1
Indications TRIGEN META-NAIL Tibial Nail Specifications... 3 Instruments for opening the proximal tibia... 4
 Surgical Technique TRIGEN META-NAIL Semi-extended Instrument Set Surgical Technique Table of Contents Indications... 2... TRIGEN META-NAIL Tibial Nail Specifications... 3 Instruments for opening the proximal
Surgical Technique TRIGEN META-NAIL Semi-extended Instrument Set Surgical Technique Table of Contents Indications... 2... TRIGEN META-NAIL Tibial Nail Specifications... 3 Instruments for opening the proximal
Tibial Nonunions: Should I Tackle and How
 Tibial Nonunions: Should I Tackle and How Frank R. Avilucea, MD Assistant Professor Department of Orthopaedic Surgery University of Cincinnati Medical Center Disclosures Journal Reviewer Journal of Bone
Tibial Nonunions: Should I Tackle and How Frank R. Avilucea, MD Assistant Professor Department of Orthopaedic Surgery University of Cincinnati Medical Center Disclosures Journal Reviewer Journal of Bone
Classification of Acetabular Cartilage Lesions. Claudio Mella, MD
 Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Cost and Time Considerations: Are Minifragment Plates Worth It? Disclosure. More Disclosures. Are minifragment plates worth it? it depends!
 Cost and Time Considerations: Are Minifragment Plates Worth It? Andrew Choo, MD Vumedi Webinar November 15, 2016 Disclosure Paid speaker: Depuy Synthes More Disclosures Price quotes are estimates only!
Cost and Time Considerations: Are Minifragment Plates Worth It? Andrew Choo, MD Vumedi Webinar November 15, 2016 Disclosure Paid speaker: Depuy Synthes More Disclosures Price quotes are estimates only!
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Bone&JointAppraisal Vol
 Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
3/13/2018. Cartilage Cases. Case. Physical exam
 Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Standard intramedullary (IM) nails are usually used
 67 Effect of Piriformis Versus Trochanteric Starting Point on Fixation Stability of Short Intramedullary Reconstruction Nails Edward T. Su MD Hargovind DeWal MD Roy Sanders MD Frederick J. Kummer PhD Mohammed
67 Effect of Piriformis Versus Trochanteric Starting Point on Fixation Stability of Short Intramedullary Reconstruction Nails Edward T. Su MD Hargovind DeWal MD Roy Sanders MD Frederick J. Kummer PhD Mohammed
Treatment of ipsilateral femoral neck and shaft fractures. Mohamed E. Habib, Yasser S. Hannout, and Ahmed F. Shams
 Treatment of ipsilateral femoral neck and shaft fractures Mohamed E. Habib, Yasser S. Hannout, and Ahmed F. Shams Department of Orthopedic Surgery, Faculty of Medicine, University of El Minoufiya, Egypt
Treatment of ipsilateral femoral neck and shaft fractures Mohamed E. Habib, Yasser S. Hannout, and Ahmed F. Shams Department of Orthopedic Surgery, Faculty of Medicine, University of El Minoufiya, Egypt
Pertrochanteric femur fracture at the proximal end of a retrograde intramedullary nail a case report
 Injury Extra (2005) 36, 271 276 www.elsevier.com/locate/inext CASE REPORT Pertrochanteric femur fracture at the proximal end of a retrograde intramedullary nail a case report Timothy O Mara, David P. Barei*,
Injury Extra (2005) 36, 271 276 www.elsevier.com/locate/inext CASE REPORT Pertrochanteric femur fracture at the proximal end of a retrograde intramedullary nail a case report Timothy O Mara, David P. Barei*,
CASE REPORT. Antegrade tibia lengthening with the PRECICE Limb Lengthening technology
 CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
GREENS SURGICALS. Redefining Excellence INSTRUMENT SYSTEM PREPARED BY: DR. VINAY KUMAR
 GREENS SURGICALS Redefining Excellence TIBIA AND FEMUR INSTRUMENT SYSTEM PREPARED BY: DR. VINAY KUMAR OPERATIVE TECHNIQUES INDEX SR.NO CONTENTS 1 LIST OF INSTRUMENT FOR TIBIA AND FEMUR. 2 RADIO GRAPH OF
GREENS SURGICALS Redefining Excellence TIBIA AND FEMUR INSTRUMENT SYSTEM PREPARED BY: DR. VINAY KUMAR OPERATIVE TECHNIQUES INDEX SR.NO CONTENTS 1 LIST OF INSTRUMENT FOR TIBIA AND FEMUR. 2 RADIO GRAPH OF
Fri., 10/11/13 Knee/Tibia, PAPER #58, 2:30 pm OTA 2013
 Fri., 10/11/13 Knee/Tibia, PAPER #58, 2:30 pm OTA 2013 Are Locked Plates Needed for Fixation of Split Depression Tibial Plateau Fractures (Schatzker Type II)? Michelle Abghari, BS; Alejandro I. Marcano,
Fri., 10/11/13 Knee/Tibia, PAPER #58, 2:30 pm OTA 2013 Are Locked Plates Needed for Fixation of Split Depression Tibial Plateau Fractures (Schatzker Type II)? Michelle Abghari, BS; Alejandro I. Marcano,
Patellofemoral Replacement
 Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
Outcome of surgical implant generation network nail initiative in treatment of long bone shaft fractures in Kenya
 Original Article Outcome of surgical implant generation network nail initiative in treatment of long bone shaft fractures in Kenya O.O. Soren, MBChB (Moi), MMed (Orthopaedics) (Makerere), Consultant Orthopaedic
Original Article Outcome of surgical implant generation network nail initiative in treatment of long bone shaft fractures in Kenya O.O. Soren, MBChB (Moi), MMed (Orthopaedics) (Makerere), Consultant Orthopaedic
Mark VanDer Kaag 1, Ajmal Ikram 2. Hand Unit, Tygerberg Hospital University of Stellenbosch
 A Prospective, Randomized Controlled Study To Determine The Radiological And Functional Outcomes Of IMN Fixation Of Distal Radius Fractures Using A Novel Device The Sonoma Wrx Distal Radius Nail Compared
A Prospective, Randomized Controlled Study To Determine The Radiological And Functional Outcomes Of IMN Fixation Of Distal Radius Fractures Using A Novel Device The Sonoma Wrx Distal Radius Nail Compared
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
5/31/2018. Ipsilateral Femoral Neck And Shaft Fractures. Ipsilateral Neck-Shaft Fractures Introduction. Ipsilateral Neck-Shaft Fractures Introduction
 Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
Ipsilateral Femoral Neck And Shaft Fractures Exchange Nailing For Non- Union Donald Wiss MD Cedars-Sinai Medical Center Los Angeles, California Introduction Uncommon Injury Invariably High Energy Trauma
Musculoskeletal Applications for CT. Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine
 Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
9/24/2015. When Can I Use a SHS? When CAN T I Use a SHS? Sliding Hip Screw. Time proven. Technically simple. Cheap. Quick
 When Can I Use a SHS? Frank A. Liporace, MD Associate Professor Director of Orthopaedic Trauma Research Director of Orthopaedic Trauma Jersey City Medical Center New York University / Hospital for Joint
When Can I Use a SHS? Frank A. Liporace, MD Associate Professor Director of Orthopaedic Trauma Research Director of Orthopaedic Trauma Jersey City Medical Center New York University / Hospital for Joint
Knee Surgical Technique
 Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Percutaneous Humeral Fracture Repair Surgical Technique
 Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
H.P. Teng, Y.J. Chou, L.C. Lin, and C.Y. Wong Under general or spinal anesthesia, the knee was flexed gently. In the cases of limited ROM, gentle and
 THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
3/13/2018. Common Options. ACL Graft Selection in When my Cojones Are On the Line - What I Do in ACL Reconstruction
 ACL Graft Selection in 2018 James P Bradley, MD Clinical Professor UPMC Head Team Physician Pittsburgh Steelers Consultant Miami Marlins Michael S Nickoli, MD University of Pittsburgh Sports Fellow When
ACL Graft Selection in 2018 James P Bradley, MD Clinical Professor UPMC Head Team Physician Pittsburgh Steelers Consultant Miami Marlins Michael S Nickoli, MD University of Pittsburgh Sports Fellow When
Surgical Technique 1
 Surgical Technique 1 TRIGEN META-NAIL Semi-extended Instrument Set Surgical Technique Table of Contents Indications... 2... TRIGEN META-NAIL Tibial Nail Specifications... 3 Instruments for opening the
Surgical Technique 1 TRIGEN META-NAIL Semi-extended Instrument Set Surgical Technique Table of Contents Indications... 2... TRIGEN META-NAIL Tibial Nail Specifications... 3 Instruments for opening the
ROTATIONAL PILON FRACTURES
 CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
THE P.F.C. SIGMA FEMORAL ADAPTER. Surgical Technique
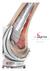 THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
Practical Reduction Techniques: Diaphyseal Reduction. Philip Wolinsky University of California at Davis Medical Center
 OTA Specialty Day 2016 Practical Reduction Techniques: Diaphyseal Reduction Philip Wolinsky University of California at Davis Medical Center 8:55 am 9:55 am Tips and Tricks: Practical Reduction Techniques
OTA Specialty Day 2016 Practical Reduction Techniques: Diaphyseal Reduction Philip Wolinsky University of California at Davis Medical Center 8:55 am 9:55 am Tips and Tricks: Practical Reduction Techniques
KEYWORDS: Tibial fracture, Diaphyseal fracture, closed interlocking intramedullary nailing,
 International Journal of scientific research and management (IJSRM) Volume 3 Issue 4 Pages 2529-2534 2015 \ Website: www.ijsrm.in ISSN (e): 2321-3418 Closed Intra-Medullary Interlocking Nail Improves Surgical
International Journal of scientific research and management (IJSRM) Volume 3 Issue 4 Pages 2529-2534 2015 \ Website: www.ijsrm.in ISSN (e): 2321-3418 Closed Intra-Medullary Interlocking Nail Improves Surgical
Kohei Kawaguchi, Shuji Taketomi, Hiroshi Inui, Ryota Yamagami, Kenichi Kono, Keiu Nakazato, Kentaro Takagi, Manabu Kawata, Sakae Tanaka
 Chronological changes in anterior knee stability after anatomical anterior cruciate ligament reconstruction using bone-patellar tendon-bone graft and hamstrings graft Kohei Kawaguchi, Shuji Taketomi, Hiroshi
Chronological changes in anterior knee stability after anatomical anterior cruciate ligament reconstruction using bone-patellar tendon-bone graft and hamstrings graft Kohei Kawaguchi, Shuji Taketomi, Hiroshi
K n e e b r a f o r l a t e p a t e l l a r r e t i n a c u
 K n e e b r a f o r l a t e p a t e l l a r r e t i n a c u 20-11-2012 Retinaculum Knee Catherine Blake. Loading. Anatomy Of The Patellar Tendon. Arthroscopic Lateral Release and Medial Imbrication. What
K n e e b r a f o r l a t e p a t e l l a r r e t i n a c u 20-11-2012 Retinaculum Knee Catherine Blake. Loading. Anatomy Of The Patellar Tendon. Arthroscopic Lateral Release and Medial Imbrication. What
CASE NO: 1 PATIENT DETAILS : Occupation : Housewife Date Of Admission :11/06/15 Residence : Nalgonda IP NO :
 CASE NO: 1 PATIENT DETAILS : Name : XXXX Age : 53yr Sex : Female Occupation : Housewife Date Of Admission :11/06/15 Residence : Nalgonda IP NO : 201518441 CHIEF COMPLAINTS : - Pain in the right knee since
CASE NO: 1 PATIENT DETAILS : Name : XXXX Age : 53yr Sex : Female Occupation : Housewife Date Of Admission :11/06/15 Residence : Nalgonda IP NO : 201518441 CHIEF COMPLAINTS : - Pain in the right knee since
Partial Knee Replacement
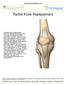 Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Retrograde Locked Intramedullary Nailing For The Stabilisation Of Femoral Fractures With Ipsilateral Tibial Fractures (Floating Knee): A Case Report
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 4 Number 1 Retrograde Locked Intramedullary Nailing For The Stabilisation Of Femoral Fractures With Ipsilateral Tibial Fractures (Floating Knee):
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 4 Number 1 Retrograde Locked Intramedullary Nailing For The Stabilisation Of Femoral Fractures With Ipsilateral Tibial Fractures (Floating Knee):
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Physeal Fractures and Growth Arrest
 Physeal Fractures and Growth Arrest Raymond W. Liu, M.D. Victor M. Goldberg Master Clinician-Scientist in Orthopaedics Rainbow Babies and Children s Hospital Case Western Reserve University Outline General
Physeal Fractures and Growth Arrest Raymond W. Liu, M.D. Victor M. Goldberg Master Clinician-Scientist in Orthopaedics Rainbow Babies and Children s Hospital Case Western Reserve University Outline General
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact)
 STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
Factors affecting fracture healing after intramedullary nailing of the tibial diaphysis for closed and grade I open fractures
 Trauma Factors affecting fracture healing after intramedullary nailing of the tibial diaphysis for closed and grade I open fractures G. I. Drosos, M. Bishay, I. A. Karnezis, A. K. Alegakis From Royal United
Trauma Factors affecting fracture healing after intramedullary nailing of the tibial diaphysis for closed and grade I open fractures G. I. Drosos, M. Bishay, I. A. Karnezis, A. K. Alegakis From Royal United
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Bone transport for the management of severely comminuted fractures without bone loss
 Strat Traum Limb Recon (2016) 11:19 24 DOI 10.1007/s11751-016-0241-y ORIGINAL ARTICLE Bone transport for the management of severely comminuted fractures without bone loss Mootaz F. Thakeb 1 Mahmoud A.
Strat Traum Limb Recon (2016) 11:19 24 DOI 10.1007/s11751-016-0241-y ORIGINAL ARTICLE Bone transport for the management of severely comminuted fractures without bone loss Mootaz F. Thakeb 1 Mahmoud A.
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
1 st Time Patella Dislocation When is it best to intervene? The Dilemma. Patellar Dislocation The Issues 3/9/2018. Is there a difference?
 1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
1 st Time Patella Dislocation When is it best to intervene? Jim Bradley MD Clinical Professor UPMC Head Team Physician, Pittsburgh Steelers Consultant Miami Marlins Michael Nickoli MD Orthopaedic Surgery
Unlocked Nailing vs. Interlocking Nailing for Winquist Type I and II Femoral Isthmus Fractures. Is there a Difference?
 Unlocked Nailing vs. Interlocking Nailing for Winquist Type I and II Femoral Isthmus Fractures. Is there a Difference? CK Yu, MBBS (UM), HY Wong*, MD (UKM), AS Vivek, FRCS (Edin), BC Se To*, FRCS (Edin)
Unlocked Nailing vs. Interlocking Nailing for Winquist Type I and II Femoral Isthmus Fractures. Is there a Difference? CK Yu, MBBS (UM), HY Wong*, MD (UKM), AS Vivek, FRCS (Edin), BC Se To*, FRCS (Edin)
Talus Fractures: When and Why on Screws and Plates
 Talus Fractures: When and Why on Screws and Plates Frank A. Liporace, MD Associate Professor Director of Orthopaedic Research New York University / Hospital for Joint Diseases, NY, NY Director Orthopaedic
Talus Fractures: When and Why on Screws and Plates Frank A. Liporace, MD Associate Professor Director of Orthopaedic Research New York University / Hospital for Joint Diseases, NY, NY Director Orthopaedic
Origins of PF Pain. Genesis of Iatrogenic Patellofemoral Pain
 Origins of PF Pain Genesis of Iatrogenic Patellofemoral Pain ISAKOS: DonJoy Consensus Meeting: Understanding Patellofemoral Pain Saturday, May 26, 2007 8:00-12:30 Talk: 7 minutes Improper Techniques Iatrogenic:
Origins of PF Pain Genesis of Iatrogenic Patellofemoral Pain ISAKOS: DonJoy Consensus Meeting: Understanding Patellofemoral Pain Saturday, May 26, 2007 8:00-12:30 Talk: 7 minutes Improper Techniques Iatrogenic:
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Arthroscopic-Assisted Percutaneous Stabilization of Patellar Fractures
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 389, pp. 57 61 2001 Lippincott Williams & Wilkins, Inc. Arthroscopic-Assisted Percutaneous Stabilization of Patellar Fractures Akin Turgut, MD*; İzge Günal,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 389, pp. 57 61 2001 Lippincott Williams & Wilkins, Inc. Arthroscopic-Assisted Percutaneous Stabilization of Patellar Fractures Akin Turgut, MD*; İzge Günal,
S U R G I C A L T E C H N I Q U E David A. McQueen, MD Return to Menu
 S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture.
 Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Pediatric Tibia Fractures Key Points. Christopher Iobst, MD
 Pediatric Tibia Fractures Key Points Christopher Iobst, MD Goals Bone to heal Return to full weight bearing Acceptable alignment rule of 10s 10 degrees of varus 8 degrees of valgus 12 degrees of procurvatum
Pediatric Tibia Fractures Key Points Christopher Iobst, MD Goals Bone to heal Return to full weight bearing Acceptable alignment rule of 10s 10 degrees of varus 8 degrees of valgus 12 degrees of procurvatum
ORTHOPAEDIC SUMMIT 2016
 Injuries to the Extensor Mechanism Quadriceps & Patellar tendon Pearls and Pitfalls M.Mike Malek, M.D. Washington Orthopaedic and Knee Clinic ORTHOPAEDIC SUMMIT 2016 Las Vegas, Nevada December 8, 2016
Injuries to the Extensor Mechanism Quadriceps & Patellar tendon Pearls and Pitfalls M.Mike Malek, M.D. Washington Orthopaedic and Knee Clinic ORTHOPAEDIC SUMMIT 2016 Las Vegas, Nevada December 8, 2016
Calcaneus Fractures: My Small Incision Tricks
 Calcaneus Fractures: My Small Incision Tricks Steven Steinlauf, MD The Orthopaedic Foot and Ankle Institute of South Florida CSFA Tampa, February 2018 Disclosures Smith & Nephew Design surgeon, Royalties
Calcaneus Fractures: My Small Incision Tricks Steven Steinlauf, MD The Orthopaedic Foot and Ankle Institute of South Florida CSFA Tampa, February 2018 Disclosures Smith & Nephew Design surgeon, Royalties
