Osteochondral Allografts for Large Defects in the Knee
|
|
|
- Marianna Louisa Wiggins
- 6 years ago
- Views:
Transcription
1 Techniques in Knee Surgery 5(3): , 2006 Ó 2006 Lippincott Williams & Wilkins, Philadelphia j S P E C I A L F O C U S j Osteochondral Allografts for Large Defects in the Knee Patrick C. McCulloch, MD Department of Orthopedics Baylor College of Medicine Houston, Texas, U.S.A. Richard Kang, BS and Brian J. Cole, MD, MBA Department of Orthopedics & Anatomy Cell Biology Rush University Chicago, Illinois, U.S.A. ABSTRACT Localized osteochondral and chondral lesions of the knee are commonly encountered in orthopaedic practice. They may become symptomatic with patients experiencing pain, swelling, and mechanical symptoms. These lesions have limited ability to heal and may progress to osteoarthritis. This presents an especially difficult clinical problem in young, high-demand individuals. This has led surgeons to pursue biologic solutions for the restoration of damaged cartilage and underlying bone. We have investigated the use of prolonged fresh osteochondral allografts for the treatment of large defects of the knee. The surgical considerations and techniques are presented in this article. Keywords: osteochondral allograft, knee, articular cartilage, transplantation HISTORICAL PERSPECTIVE Address correspondence and reprint requests to Brian J. Cole, MD, MBA, Section Head, Cartilage Restoration Center at Rush, Departments of Orthopedics and Anatomy and Cell Biology, Rush University Medical Center, 1725 W. Harrison St, POB Ste no. 1063, Chicago, IL bcole@rushortho.com. Larger and deeper defects have limited ability to heal and may progress to osteoarthritis. 1Y6 The ability to resurface these defects with mature hyaline articular cartilage and address the underlying bone deficit in a single procedure makes osteochondral allograft (OCA) transplantation an attractive option. The appropriate size and surface contour can be matched when the graft is obtained from an appropriately selected organ donor. The biology of articular cartilage makes it ideal for transplantation. It is both aneural and relatively avascular, receiving its nutrition by diffusion from synovial fluid. Furthermore, it is a relatively immuno-privileged tissue. 7 The chondrocytes are protected from the host immune surveillance by the surrounding matrix. Therefore, this allows mature living chondrocytes to survive for many years after transplantation without the need for tissue matching or immunosuppressive therapy. 8,9 In the 1970s, musculoskeletal tumor surgeons began using frozen OCAs for reconstruction. 3,10 The freezing process decreased immunogenicity and prolonged storage times, but at the expense of chondrocyte viability. These are best considered biologic implants, rather than transplants, because the cells are not alive. Therefore, surgeons seeking to restore focal osteoarticular defects with living chondrocytes have sought to use fresh allografts. Recent advances in allograft processing and storage have made fresh grafts more commercially available. Grafts are harvested and are kept refrigerated in dimethyl sulfoxide at 4-C. This allows for the storage of the grafts for up to 42 days, or so-called Bprolonged fresh^ grafts. 11,12 These grafts have been shown to have minimal immune response, preserved chondrocyte viability, and enhanced revascularization of the bone. 13,14 The ability to prolong fresh grafts up to several weeks has several practical advantages. The safety of the grafts is enhanced by allowing time for complete bacteriologic and DNA polymerase chain reaction screening. This testing period may take up to 14 days, during which the patient and surgeon are able to schedule and plan for the surgery. The longer life of the graft affords more time to find an appropriate match and perform the transplant, thereby minimizing the number of donor grafts wasted due to expiration. This effectively increases the supply of grafts and makes them now more available to the general orthopedic community. These factors have spawned renewed interest in their use for the treatment of osteochondral defects in young, active patients. Volume 5, Issue 3 165
2 McCulloch et al PREOPERATIVE EVALUATION History The diagnosis of a symptomatic osteochondral lesion in the knee may be suspected based on the patient s history. However, the presentation may vary based on the etiology of the lesion. Most commonly, these patients will have a history of an osteochondritis dissecans (OCD) lesion diagnosed in adolescence. Avascular necrosis may have an insidious onset of pain, which can often be linked to a history of known risk factors, such as steroid or alcohol use. Those with traumatic defects will often recall a specific inciting event or injury, whereas those with more degenerative lesions often will not. It is important to note that not all osteochondral lesions require treatment. Incidental lesions are frequently found on radiographs or during knee arthroscopy for the treatment of other pathology. For all incidental lesions, it is preferable to follow patients nonoperatively and delay treatment until they develop signs and symptoms referable to the lesion. This often involves waiting up to 6 months after a meniscectomy, debridement, bone grafting, microfracture, or ligament reconstruction. Typically, patients will complain of mechanical symptoms such as catching, locking, or giving way. They will often give a history of recurrent knee swelling after activity. They may complain of pain specific to the compartment involved, although the level of pain is often quite variable. For those with avascular necrosis, pain may be the presenting complaint. For those with OCD, pain may be relatively minor compared with their mechanical symptoms. Physical Examination The physical examination begins with inspection. An evaluation of the patient s gait may reveal an antalgic or stiff-knee gait. This also allows for an evaluation of the overall limb alignment. For example, large medial lesions will often result in an obvious varus malalignment. Quadriceps atrophy correlates with the duration and severity of symptoms. The presence of an effusion is of paramount importance in detecting intraarticular pathology. Occasionally, patients referred for treatment of a meniscal tear will present with a tense effusion. This degree of swelling should increase one s suspicion for an TABLE 1. Standard Radiographic Series Standing anterior-posterior view with the knee in full extension Standing posterior-anterior view with the knee flexed 45 degrees (Tunnel or Notch view) Lateral view Patellar (Sunrise) view Bilateral long-leg alignment films osteochondral lesion. Range of motion is usually preserved but may be limited in patients with a large effusion or loose bodies. Ranging the knee also allows for the assessment of the location of the lesion when catching, or crepitus in a specific range is identified. Patients with large condylar lesions will often have tenderness to palpation directly over the condyle with the knee placed in flexion. Up to one half of these patients may present with bilateral knee pathology, and it is therefore important to evaluate both knees. Imaging A standardized series of radiographs is included in Table 1. Weight-bearing views are essential in determining the degree of joint space narrowing and arthrosis. In addition to the standing anterior-posterior view, a standing posterioranterior tunnel view obtained in 45 degrees of flexion is helpful (Fig. 1). Occasionally, a large OCD lesion will only be detected on this view. Standing bilateral long-leg alignment views are also used to measure the mechanical axis through the knee. These will be used to ensure that the knee is corrected to a neutral position with a concomitant osteotomy if needed. These views should be obtained with a radiologic marker alongside the knee, which will be used to correct for magnification when ordering donor tissue of an appropriate size. Magnetic resonance imaging (MRI) remains the gold standard for the evaluation of osteochondral lesions. The sagittal and coronal images can be used to assess the size, depth, and location of the lesion (Fig. 2). Chondral lesions will often have high signal on T2 images in the underlying subchondral bone marrow due to edema. It is important to differentiate this reactive edema from a true osseous defect, so as not to overestimate the extent ofthelesion.thepresenceofhighsignalont2images behind an OCD lesion is highly suggestive of an unstable fragment. In general, a closed high-field magnet (Tesla of 1.5 or greater) with proton density fast-spin echo sequences often provides the greatest resolution of articular cartilage. MR arthrography is not widely used in the knee. Patients often present with the arthroscopic photographs from their previous procedure. These can be very helpful and may obviate the need for a diagnostic arthroscopy. However, most patients will require a diagnostic arthroscopy to adequately assess the lesion and any concomitant pathology. Indications and Contraindications This procedure is indicated for patients with symptomatic, large osteochondral, or full-thickness chondral lesions. Some defects are not amenable to other resurfacing techniques due to their size, location, or depth. Smaller lesions may be amenable to autologous osteochondral 166 Techniques in Knee Surgery
3 Special Focus: Osteochondral Allografts in the Knee FIGURE 1. (A) Anterior-posterior radiograph of OCD lesion on the lateral aspect of the medial femoral condyle. (B) The notch view more clearly demonstrates the size of the lesion. (C) Radiograph demonstrating severe deformity of the condyles in a young patient before undergoing OCA transplantation to both condyles. (D) Standard radiographic notch view shows a large OCD lesion of the lateral femoral condyle. (E) A CT scan demonstrates the extent of bone loss in this LFC defect. plug transfer. However, the amount of available autologous tissue and the associated donor site morbidity may be prohibitive for lesions larger than 2 to 3 cm 2. Microfracture or autologous chondrocyte implantation is useful for superficial defects. When the defect extends through the subchondral bone or involves a structural or uncontained segment, osteochondral allografting may be preferred as a single-stage treatment. In fact, most patients FIGURE 2. (A) MRI of an OCD lesion on the medial femoral condylevcoronal view. (B) MRI of an OCD lesion on the medial femoral condylevsagittal view. Volume 5, Issue 3 167
4 McCulloch et al undergoing OCA transplantation have failed other techniques. In general, OCA transplantation is an excellent option for focal defects larger than 2 to 3 cm 2 with underlying bony deficiency or as salvage for other failed resurfacing technique. There are few contraindications for OCA transplantation. Patients with advanced or diffuse degenerative changes as seen on weight-bearing radiographs may be best served with knee arthroplasty. Bipolar lesions represent a relative contraindication and have less predictable outcomes. If present, both lesions should be addressed. Often the larger, deeper defect is allografted, and the more superficial kissing lesion is amenable to microfracture. Osteochondral allograft transplantation is contraindicated in patients with uncorrectable malalignment, ligamentous instability, or meniscal insufficiency. These comorbidities must be addressed before or during the transplantation to provide an optimal environment for the graft. PREOPERATIVE PLANNING As discussed above, a prior diagnostic arthroscopy can be helpful in determining the size and location of the defect and in identifying any other pathology that may require treatment. The required allograft tissues that are size and side matched can then be ordered. If needed, meniscal or ligament allografts are frozen and therefore can be reserved for the patient while awaiting availability of a fresh osteochondral graft. The tissue bank will provide notification when a potential graft has been harvested. It then takes approximately 7 to 14 days for the completion of all serologic and bacteriologic testing. This provides sufficient time to contact the patient and schedule the surgery. We prefer to implant the graft before 21 days after TABLE 2. Order of Concurrent Procedures 1. Exam under anesthesia 2. Arthroscopy a. Diagnostic arthroscopy b. Debridement/Microfracture of any associated lesions c. Ligament reconstruction and fixation d. Meniscus transplantation 3. Arthrotomy a. Osteochondral allograft transplantation 4. Osteotomy 5. Wound closure donor harvest due to concerns for decreasing cell viability beyond that time point. 15 Measurement of the limb alignment is made on the long-leg films (Fig. 3). If needed, high tibial or distal femoral osteotomies are used to correct malalignment. The degree of correction should be calculated to bring the mechanical axis to neutral, but not overcorrection as in salvage. It is not uncommon for a knee to require multiple procedures at the time of OCA transplantation. Therefore, the surgeon must select the optimal order for the steps involved in these concurrent procedures. An algorithm is presented in Table 2. In general, arthroscopic procedures should be performed before making the arthrotomy. This would include a diagnostic arthroscopy if it has not been previously performed by the treating surgeon. Other arthroscopic procedures such as meniscal transplantation and microfracture are best performed at this stage. If a ligament reconstruction is to be performed, drilling the tunnels, graft passage, and fixation can be performed before allograft transplantation. If an osteotomy is required, it may be best to perform this procedure at the end of the case to avoid undue stress at the osteotomy site. SURGICAL TECHNIQUE FIGURE 3. Long-leg alignment films are used to determine if an osteotomy is required to achieve neutral limb alignment. Positioning This procedure is performed on an outpatient basis and can be done under general or regional anesthesia. Before induction, the surgeon must assess the allograft tissue to ensure that it is of the appropriate size and side matched. The patient is then placed supine on a standard operating room table. A well-padded proximal thigh tourniquet is placed on the patient and is inflated before the arthrotomy. A foot holder device is especially useful to maintain high degrees of flexion needed for accessing more posterior lesions. Exposure An anterior skin incision is made from the proximal pole of the patella to the level of the joint surface. Although a midline incision is used most commonly, it can be moved medially or laterally toward the involved compartment. Once the capsule is exposed, a limited peripatellar arthrotomy is made over the involved compartment. This is 168 Techniques in Knee Surgery
5 Special Focus: Osteochondral Allografts in the Knee FIGURE 4. Exposure of lesion on lateral femoral condyle using a limited arthrotomy. made laterally for lateral defects and medially for medial or bicondylar defects. The incision can be extended proximally using a sub-vastus or mid-vastus approach as needed for greater exposure. The patella is retracted by placing a z- or bent Hohman retractor in the notch. It can be helpful to release the fat pad and dissect the capsule off of the anterior horn of the meniscus to improve exposure. The knee can be flexed, extended, or rotated to place the defect in the center of the incision (Fig. 4). Once the defect has been confirmed, the allograft can be opened and placed on the back table allowing it to gradually rewarm at room temperature. We prefer to place the graft in cool saline with antibiotics (approximately 22-C) before placing in room temperature water because of concerns regarding the effects of rapid rewarming. 15 FIGURE 6. Guide pin driven into defect site to ensure perpendicular placement of the reamer. Defect Preparation Once the defect has been identified, the surrounding damaged cartilage and bone is debrided. This allows for more accurate sizing of the lesion. For most contained defects, a press-fit technique can be performed using a commercial system (Arthrex, Naples, FL). A cannulated, cylindrical sizing guide is positioned such that it completely encompasses the defect (Fig. 5). This determines the optimal plug diameter. It must sit flush with the surrounding normal cartilage to properly restore the geometry of the articular surface. A guide pin is driven into the base of the defect, thereby setting the center and perpendicular axis (Fig. 6). The sizing tube is then removed and taken to the back table where it is positioned on the donor graft to ensure that the size and location can be properly matched. A cannulated counter bore reamer is advanced over the guide pin to a depth of 6 to 8 mm (Fig. 7). Multiple perforations are made in the base of the defect using a k-wire to allow for FIGURE 5. Sizing guide placed over defect. This will be used to determine the size of the allograft as it is harvested. FIGURE 7. Counter-bore reamer advanced down to 6 to 8 mm into the defect site. Volume 5, Issue 3 169
6 McCulloch et al FIGURE 8. Sizing the allograft while it is fixed in the allograft harvester. vascular inflow. A skin marker is used to mark the 12 o clock position for reference. A depth gauge is used to measure and record the socket depth at the 3, 6, 9, and 12 o clock positions. The recipient socket is now complete. For uncontained or large structural lesions, a freehand technique is used. A skin marker is used to outline a geometrical shape that encompasses the defect. A 15- blade knife is used to incise the remaining cartilage, which is then removed using sharp curettes. A highspeed burr is used to remove the underlying bone. Cold irrigation is used during reaming or burring to prevent thermal injury to the surrounding normal tissues. Graft Preparation Graft preparation is performed on the back table. For the press-fit technique, it is helpful to use a graft workstation. The donor graft is positioned in the workstation and a bushing of the chosen diameter is placed in the platform. The sizing tube is again used to confirm that the selected angle will match the contour of the defect (Fig. 8). The 12 o clock position is marked. A donor harvester is passed through the housing and advanced through the entire depth of the donor graft. The plug is then extracted from the harvester. The chosen depths are then marked for each of the 4 quadrants. An allograft forceps is used to hold the plug, whereas a sagittal saw is used to trim the excess bone. For the free-hand technique, the donor graft is fashioned using a sagittal saw. It is advisable to make these cuts slightly wider than measured to allow for trial fittings. Once the graft has been prepared, pulsatile lavage is used to remove any remaining marrow elements, which are felt to be the most immunogenic part of the graft. Insertion and Fixation By aligning the 12 o clock markings, the graft is pressed into place by hand (Fig. 9). If it does not pass easily, the dilator can be used to provide an additional 0.5 mm of dilation. Occasionally, on oversized tamp is used to ensure that the graft is flush with the surrounding articular surface. This step should be minimized to preserve maximal chondrocyte viability. For the press-fit technique, additional fixation is usually not necessary. For the larger structural grafts, fixation can be achieved using compression screws or bioabsorbable polydioxanone pins (Johnson and Johnson Professional, Raynham, MA). POSTOPERATIVE CONSIDERATIONS Analgesia These procedures are performed in an outpatient setting. For cases involving multiple procedures, a postoperative femoral nerve block can be used to assist with immediate postoperative analgesia. A compressive, cryotherapy FIGURE 9. (A) Press-fitting the allograft into the recipient hole by hand. Occasionally, an oversize tamp will be used to ensure that the articular surfaces of the graft and native cartilage are even. (B) Final view of the allograft before closure. The graft has been press-fit into the recipient hole, and no further fixation is necessary. 170 Techniques in Knee Surgery
7 Special Focus: Osteochondral Allografts in the Knee TABLE 3. Postoperative Rehabilitation Protocol Timing Activity 0Y6 wk CPM Quad sets, straight leg raises, patellar mobilization TTWB (alternatively, WBAT) 4Y8 wk CPM Stationary bicycle Discontinue brace Progress to full WB 4Y6 mo Strengthening Return to light recreational sports 12 mo Return to high-impact sports, if desired CPM indicates continuous passive motion; TTWB, toe-touch weightbearing; WBAT, weight-bearing as tolerated; WB, weight-bearing. device (Game Ready, Inc., Berkeley, CA) is helpful to control pain and swelling. Nonsteroidal medications are generally not used during the period of graft integration. Rehabilitation Motion is essential to any chondral resurfacing procedure. Although a brace is used for protection during ambulation, patients are generally allowed unrestricted motion unless a concurrent procedure would dictate otherwise. Continuous passive motion (CPM) is started the day of surgery. Patients are encouraged to use the CPM for 6 to 8 hours per day for the first 6 weeks to prevent adhesions and to accelerate the healing process and to promote graft nutrition. Patients begin supervised physical therapy after the first postoperative visit. A therapy protocol is included in Table 3. Traditionally, these patients have been placed on restricted weight-bearing with the use of crutches. This involves 6 weeks of toe- or heel-touch weight-bearing before they are gradually progressed to full weightbearing. More recently, we have begun studying the use of immediate weight-bearing as tolerated for patients with stable grafts. Once quadriceps function has returned, the brace is discontinued and closed chain strengthening is begun. By 3 months, patients are expected to have full motion and near-normal quadriceps strength. Patients may begin light recreational activities by 4 to 6 months. Higher impact activities are not recommended during the first year. Complications Complications may arise due to the arthrotomy or the donor graft. Stiffness is a concern in the immediate postoperative period. The use of the limited arthrotomy and emphasis one arly motion minimize this risk. Infection and disease transmission are concerns with any allograft tissue. There is only one documented case of HIV transmission from an OCA back in With present tissue banking regulations and the use of DNA polymerase chain reaction testing, there have been no known cases of HIV or Hepatitis C transmission that form an OCA. Occasionally, certain individuals may experience recurrent sterile effusions that are thought to be related to a host immune response. These typically resolve without requiring the removal of the graft. Graft nonunion or fragmentation and collapse is uncommon but may occur from months to years after the procedure. Periodic radiographic screening is recommended. RESULTS Several studies have reported the outcome of fresh OCA transplantation in the knee. 17Y23 Since 1972, Allen Gross has been a pioneer in the use of OCA transplantation for traumatic defects of the knee. Although TABLE 4. Results of Osteochondral Allografting Author Patient no. Mean age Location Mean FU Results Meyers et al F, T, P 3.6 y 78% success 22% failure Garrett F 3.5 y 94% success Ghazavi et al F, T, P 7.5 y 85% success Chu et al F, T, P 75 mo 76% good/excellent 16% failure Bugbee F 5 and 10 y 91% success at 5 y 75% success at 10 y 5% failure Aubin et al F 10 y 84% good/excellent 20% failure Sasha et al N/A T 12 y Kaplan-Meier survival rate: 5yV95% 10 yv80% 15 yv65% 20 yv46% F indicates femur; T, tibia; P, patella. Volume 5, Issue 3 171
8 McCulloch et al FIGURE 10. A radiograph taken at a 2-year follow-up visit demonstrates a well-integrated lateral femoral condyle allograft. many of these were larger, uncontained structural grafts, his Toronto group still reported excellent results with 85% survivorship of the grafts at follow-up of 7.5 and 10 years. 17,21,22 These grafts were stored for a maximum of 72 hours. Two studies looked specifically at its use for the treatment of OCD of the femoral condyles. Garrett 20 reported a successful outcome in 16 out of 17 patients who were asymptomatic at 2- to 9-year followup. Bugbee et al 18 reported 79% good or excellent results for a larger series of 69 patients at an average follow-up of 5 years when the grafts were implanted within 5 days of procurement. Meyers et al and Chu et al both reported on the use of fresh OCA for lesions due to multiple different diagnoses. In addition to OCD and traumatic defects, they also included degenerative and osteonecrotic lesions. They reported 77% and 84% good or excellent results, respectively. 19,23 The results are summarized in Table 4. We recently completed a prospective study of 25 consecutive patients who underwent Bprolonged fresh^ OCA transplantation for defects on the femoral condyles with a minimum follow-up of 2 years. All procedures were performed by the senior author (B.J.C.). They included degenerative, traumatic, osteonecrotic, and OCDs lesions. The average size of the primary lesion was 5.24 cm 2. Ninety-six percent had undergone a previous surgery to treat the lesion, and the average number of previous procedures was In contrast to the studies mentioned above, our Bprolonged fresh^ grafts were implanted at an average of 24 days after procurement. The average length of follow-up was 35 months. Statistically significant improvements were seen for Lysholm (39Y67), IKDC (29Y58), all 5 components of the KOOS scores (Pain, 43Y73; Symptom, 46Y64; Activities of Daily Living, 56Y83; Sports, 18Y46; Quality of Life, 22Y50), and the SF-12 physical component score (36Y40). Overall, patients reported an 84% satisfaction with their results and felt that the knee functioned at 79% of their unaffected knee. Radiographically, 88% were incorporated into host bone (Fig. 10), and there was one case of graft fragmentation. It is encouraging that these results of prolonged fresh grafts are similar to the other published reports of OCA transplantation performed within 1 week. FUTURE OF THE TECHNIQUE In summary, fresh OCA transplantation is a safe and effective procedure for the treatment of osteochondral defects of the femoral condyles. It decreases pain and improves function in young, high-demand patients in whom knee arthroplasty is a poor option. The effects of the duration of prolonged storage of these grafts on clinical outcome remain to be determined. Studies are presently underway to further assess the long-term viability of the cartilage, the influence of impaction at insertion, and the role of postoperative protected weight-bearing. REFERENCES 1. Buckwalter JA. Articular cartilage injuries. Clin Orthop. 2002;402:21Y Maletius W, Messner K. The effect of partial meniscectomy on the long-term prognosis of knees with localized, severe chondral damage: a 12Y15 year follow-up. Am J Sports Med. 1996;24:258Y Mankin HJ, Gebhart MC, Tomford WW. The use of frozen cadaveric allograft in the management of patients with bone tumors of the extremities. Orthop Clin North Am. 1987;18:275Y Mankin HJ. The reaction of articular cartilage to injury and osteoarthritis. N Engl J Med. 1974;291:1285Y Mankin HJ. The response of articular cartilage to mechanical injury. J Bone Joint Surg Am. 1982;64:460Y Messner K, Maletius W. The long-term prognosis for severe damage to weight-bearing cartilage in the knee: a 14 year clinical and radiographic follow-up in 28 young athletes. Acta Orthop Scand. 1996;67:165Y Langer F, Gross AE. Immunogenicity of allograft articular cartilage. J Bone Joint Surg Am. 1974;56A:297Y Convery FR, Akeson WH, Meyers MH. The operative technique of fresh osteochondral allografting of the knee. Oper Tech Orthop. 1997;47:340Y Czitrom AA, Keating S, Gross AE. The viability of articular cartilage in fresh osteochondral allografts after clinical transplantation. J Bone Joint Surg Am. 1990;72: 574Y Techniques in Knee Surgery
9 Special Focus: Osteochondral Allografts in the Knee 10. Tomford WW, Springfield DS, Mankin HJ. Fresh and frozen articular cartilage allografts. Orthopedics. 1992;15: 1183Y Egli RJ, Sckell A, Fraitzl CR, et al. Cryopreservation with dimethyl sulfoxide sustains partially the biological function of osteochondral tissue. Bone. 2003;33: 352Y Wingenfeld C, Egli RJ, Hempfing A, et al. Cryopreservation of osteochondral allografts: dimethyl sulfoxide promotes angiogenesis and immune tolerance in mice. J Bone Joint Surg Am. 2002;84:1420Y Pearsall AW, Tucker JA, Hester RB, et al. Chondrocyte viability in refrigerated osteochondral allografts used for transplantation within the knee. Am J Sports Med. 2004; 32:125Y Williams RJ 3rd, Dreese JC, Chen CT. Chondrocyte survival and material properties of hypothermically stored cartilage: an evaluation of tissue used for osteochondral allograft transplantation. Am J Sports Med. 2004;32: 132Y Williams JM, Virdi TK, Pylawka RB, et al. Prolong-fresh preservation of intact whole canine femoral condyles for the potential use as osteochondral allografts. J Orthop Res. 2005;23:831Y McCulloch PC, Kang R, Cole BJ. Transmission of HIV through bone transplantation: case report and public health recommendations. MMWR Morb Mortal Wkly Rep. 1988;37: Aubin PP, Cheah HK, Davis AM, et al. Long-term followup of fresh femoral osteochondral allografts for posttraumatic knee defects. Clin Orthop. 2001;391:S318YS Bugbee WD, Emmerson BC, Jamali A. Fresh osteochondral allografting in the treatment of osteochondritis dissecans of the femoral condyle. Paper no. 054, presented at the AAOS 70th Annual Meeting, February Chu CR, Convery FR, Akeson WA, et al. Articular cartilage transplantation: clinical results in the knee. Clin Orthop. 1999;36:159Y Garrett JC. Fresh osteochondral allografts for treatment of articular defects in osteochondritis dissecans of the lateral femoral condyle in adults. Clin Orthop. 1994;303:33Y Ghazavi MT, Pritzker KP, Davis AM, et al. Fresh osteochondral allografts for post-traumatic defects of the knee. J Bone Joint Surg Br. 1997;79B:1008Y Gross AE, Shasha N, Aubin P. Long-term follow-up of the use of fresh osteochondral allografts for post-traumatic knee defects. Clin Orthop. 2005;435:79Y Meyers MH, Akeson WA, Convery FR. Resurfacing of the knee with fresh osteochondral allograft. J Bone Joint Surg Am. 1989;71A:704Y Bugbee WD. Fresh osteochondral allografting. Oper Tech Sports Med. 2000;8:158Y Shasha N, Krywulak S, Backstein D, et al. Long-term follow-up of fresh tibial osteochondral allografts for failed tibial plateau fractures. JBoneJointSurgAm.2003;85-A Suppl 2:33Y39. Volume 5, Issue 3 173
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
Osteochondritis Dissecans of the Knee. M Lucas Murnaghan MD, MEd, FRCSC
 Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
The management of articular cartilage injuries in the
 1 2 3 4 5 6 7 8 Q1 Osteochondral Allograft Transplantation and Osteochondral Autograft Transfer D12XXAustin V. Stone, D13XXMD, PhD, D14XXDavid R. Christian, D15XXBS, D16XXMichael L. Redondo, D17XXMA, BS,
1 2 3 4 5 6 7 8 Q1 Osteochondral Allograft Transplantation and Osteochondral Autograft Transfer D12XXAustin V. Stone, D13XXMD, PhD, D14XXDavid R. Christian, D15XXBS, D16XXMichael L. Redondo, D17XXMA, BS,
Evaluation & Treatment of the Injured Athlete Autograft OATS versus Osteochondral Allograft Technique: Indications, Problems, Outcomes
 Evaluation & Treatment of the Injured Athlete Autograft OATS versus Osteochondral Allograft Technique: Indications, Problems, Outcomes C H R I S T I A N L AT T E R M A N N C H I E F O F S P O R T S M E
Evaluation & Treatment of the Injured Athlete Autograft OATS versus Osteochondral Allograft Technique: Indications, Problems, Outcomes C H R I S T I A N L AT T E R M A N N C H I E F O F S P O R T S M E
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Chondral Injuries in the Athlete
 Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
Osteochondritis Dissecans
 Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Chondral Disease of the Knee
 Chondral Disease of the Knee Chondral Disease of the Knee A Case-Based Approach Brian J. Cole, MD, MBA Associate Professor, Department of Orthopedics and Department of Anatomy and Cell Biology Director,
Chondral Disease of the Knee Chondral Disease of the Knee A Case-Based Approach Brian J. Cole, MD, MBA Associate Professor, Department of Orthopedics and Department of Anatomy and Cell Biology Director,
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Case Report. Byung Ill Lee, MD and Byoung Min Kim, MD Department of Orthopedic Surgery, Soonchunhyang University Hospital, Seoul, Korea
 Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
A Patient s Guide to Osteochondritis Dissecans of the Knee
 A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
CASE REPORT GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT
 Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
3/21/2011 PCL INJURY WITH OPERATIVE TREATMENT A CASE STUDY PCL PCL MECHANISM OF INJURY PCL PREVALENCE
 PCL PCL INJURY WITH OPERATIVE TREATMENT A CASE STUDY K. Anderson, S. Hjortedal, Y. Jingi, E. Sutcliffe & S. Witschen Washington State University Origin Posterior aspect of tibia Insertion Medial femoral
PCL PCL INJURY WITH OPERATIVE TREATMENT A CASE STUDY K. Anderson, S. Hjortedal, Y. Jingi, E. Sutcliffe & S. Witschen Washington State University Origin Posterior aspect of tibia Insertion Medial femoral
Three-dimensional printing improves osteochondral allograft placement in complex cases
 https://doi.org/10.1007/s00167-018-4849-y KNEE Three-dimensional printing improves osteochondral allograft placement in complex cases Kelechi R. Okoroha 1 Timothy J. Evans 1 Jeffrey P. Stephens 2 Eric
https://doi.org/10.1007/s00167-018-4849-y KNEE Three-dimensional printing improves osteochondral allograft placement in complex cases Kelechi R. Okoroha 1 Timothy J. Evans 1 Jeffrey P. Stephens 2 Eric
8/10/2016. Treatment of Articular Cartilage Injuries: Osteochondral autograft Osteochondral allograft DISCLOSURES CONSIDERATIONS:
 Treatment of Articular Cartilage Injuries: Center for Cartilage Repair and Restoration University of Kentucky Osteochondral autograft Osteochondral allograft Christian Lattermann, MD Professor for Orthopaedics
Treatment of Articular Cartilage Injuries: Center for Cartilage Repair and Restoration University of Kentucky Osteochondral autograft Osteochondral allograft Christian Lattermann, MD Professor for Orthopaedics
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS
 ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Figure 3 Figure 4 Figure 5
 Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Knee Preservation and Articular Cartilage Restoration
 Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
Tibial Cartilage Defects
 Tibial Cartilage Defects Kevin C. Wang 1 Rachel M. Frank 2 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Department of Orthopedics, Icahn School of Medicine at Mount Sinai, New York, NY, USA Department
Tibial Cartilage Defects Kevin C. Wang 1 Rachel M. Frank 2 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Department of Orthopedics, Icahn School of Medicine at Mount Sinai, New York, NY, USA Department
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Osteochondritis dissecans (OCD) lesions of the knee
 Extra-articular, Intraepiphyseal Drilling for Osteochondritis Dissecans of the Knee Andrew T. Pennock, M.D., James D. Bomar, M.P.H., and Henry G. Chambers, M.D. Abstract: Symptomatic osteochondritis dissecans
Extra-articular, Intraepiphyseal Drilling for Osteochondritis Dissecans of the Knee Andrew T. Pennock, M.D., James D. Bomar, M.P.H., and Henry G. Chambers, M.D. Abstract: Symptomatic osteochondritis dissecans
Meniscal Tears/Deficiency in Athletes
 Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
INDIVIDUALISED, ANATOMIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 ACL RECONSTRUCTION INDIVIDUALISED, ANATOMIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Written by Thierry Pauyo, Marcio Bottene Villa Albers and Freddie H. Fu, USA Anterior cruciate ligament (ACL) reconstruction
ACL RECONSTRUCTION INDIVIDUALISED, ANATOMIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Written by Thierry Pauyo, Marcio Bottene Villa Albers and Freddie H. Fu, USA Anterior cruciate ligament (ACL) reconstruction
Medical Diagnosis for Michael s Knee
 Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Tibial & Femoral Opening Wedge Osteotomy System. Surgical Technique
 Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Epidemiology. Meniscal Injury & Repair. Meniscus Anatomy. Meniscus Anatomy
 Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Treatment Options for Articular Cartilage Defects of the Knee
 Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
J oints. CIC Edizioni Internazionali. Bipolar fresh osteochondral allograft of the shoulder. Abstract. Methods. Introduction
 Abstract SaNDrO GIaNNINI, elisa SeBaStIaNI, alba SHeHu, MatteO BalDaSSarrI SuSaNNa MaralDI, FraNCeSCa VaNNINI 1 st Clinic of Orthopaedics and traumatology, rizzoli Orthopaedic Institute, Bologna, Italy
Abstract SaNDrO GIaNNINI, elisa SeBaStIaNI, alba SHeHu, MatteO BalDaSSarrI SuSaNNa MaralDI, FraNCeSCa VaNNINI 1 st Clinic of Orthopaedics and traumatology, rizzoli Orthopaedic Institute, Bologna, Italy
Evaluation and Management of Knee Pain. Michael Cassat, MD University of Arkansas for Medical Sciences
 Evaluation and Management of Knee Pain Michael Cassat, MD University of Arkansas for Medical Sciences Disclosure I have no actual or potential conflict of interest in relation to this program/presentation.
Evaluation and Management of Knee Pain Michael Cassat, MD University of Arkansas for Medical Sciences Disclosure I have no actual or potential conflict of interest in relation to this program/presentation.
3/13/2018. Cartilage Cases. Case. Physical exam
 Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Prospective Evaluation of Prolonged Fresh Osteochondral Allograft Transplantation of the Femoral Condyle
 Prospective Evaluation of Prolonged Fresh Osteochondral Allograft Transplantation of the Femoral Condyle Minimum 2-Year Follow-Up Patrick C. McCulloch, MD, Richard W. Kang, BS, Mohamed H. Sobhy, MD, Jennifer
Prospective Evaluation of Prolonged Fresh Osteochondral Allograft Transplantation of the Femoral Condyle Minimum 2-Year Follow-Up Patrick C. McCulloch, MD, Richard W. Kang, BS, Mohamed H. Sobhy, MD, Jennifer
Osteochondritis Dissecans
 P R O C E D U R E 1 4 Ammar Anbari, Adam B. Yanke, and Brian J. Cole ch014-x4397.indd 221 4/11/2008 10:50:21 AM 222 Treatment Options Conservative management Fixation in situ Elevate the OCD lesion, débride
P R O C E D U R E 1 4 Ammar Anbari, Adam B. Yanke, and Brian J. Cole ch014-x4397.indd 221 4/11/2008 10:50:21 AM 222 Treatment Options Conservative management Fixation in situ Elevate the OCD lesion, débride
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
What is Medial Plica Syndrome?
 What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with:
 Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE
 THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Introduction Knee Anatomy and Function Making the Diagnosis
 Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Lateral knee injuries
 Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
Created as a free resource by Clinical Edge Based on Physio Edge podcast episode 051 with Matt Konopinski Get your free trial of online Physio education at Orthopaedic timeframes Traditionally Orthopaedic
Meniscus Reconstruction: Trough Surgical Technique
 Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
OSTEOCHONDRAL GRAFTING OF KNEE
 MEDICAL POLICY OSTEOCHONDRAL GRAFTING OF KNEE Policy Number: 2013T0537D Effective Date: November 1, 2013 Table of Contents COVERAGE RATIONALE... BACKGROUND... CLINICAL EVIDENCE... U.S. FOOD AND DRUG ADMINISTRATION...
MEDICAL POLICY OSTEOCHONDRAL GRAFTING OF KNEE Policy Number: 2013T0537D Effective Date: November 1, 2013 Table of Contents COVERAGE RATIONALE... BACKGROUND... CLINICAL EVIDENCE... U.S. FOOD AND DRUG ADMINISTRATION...
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE
 KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at if you have any questions.
 OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
Patient Information & Exercise Folder
 MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
Nabeel Salka, MSE & John A. Grant, MD, PhD, FRCSC. MedSport, Department of Orthopedic Surgery University of Michigan, Ann Arbor, MI
 Contralateral Lateral Femoral Condyle Allografts Provide an Acceptable Surface Match for Simulated Osteochondritis Dissecans Lesions of the Medial Femoral Condyle Nabeel Salka, MSE & John A. Grant, MD,
Contralateral Lateral Femoral Condyle Allografts Provide an Acceptable Surface Match for Simulated Osteochondritis Dissecans Lesions of the Medial Femoral Condyle Nabeel Salka, MSE & John A. Grant, MD,
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
Joint Preservation Clinical Case
 Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
I have nothing to disclose
 Management of Common Knee Disorders: What You Knee d to Know UCSF Essentials of Women s Health July 8, 2015 Carlin Senter, M.D. I have nothing to disclose Learning objectives: in 1 hour you will be able
Management of Common Knee Disorders: What You Knee d to Know UCSF Essentials of Women s Health July 8, 2015 Carlin Senter, M.D. I have nothing to disclose Learning objectives: in 1 hour you will be able
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes
 Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
A Patient s Guide. ACL Injury: Ø Frequently asked questions on injury, Ø Preoperative and postoperative. surgery and recovery.
 ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
Lateral Meniscus Transplant
 Lateral Meniscus Transplant Using the CONMED Meniscus Allograft Transplant (MAT) Instruments A complete guide to Lateral Meniscus Transplant using the CONMED meniscus allograft transplant Instruments.
Lateral Meniscus Transplant Using the CONMED Meniscus Allograft Transplant (MAT) Instruments A complete guide to Lateral Meniscus Transplant using the CONMED meniscus allograft transplant Instruments.
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
ACL Reconstruction Cross-Pin Technique
 ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION PATIENT INFORMATION SHEET
 Introduction POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION PATIENT INFORMATION SHEET It has recommended that you undergo an operation to reconstruct your posterior cruciate ligament (PCL). This leaflet aims
Introduction POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION PATIENT INFORMATION SHEET It has recommended that you undergo an operation to reconstruct your posterior cruciate ligament (PCL). This leaflet aims
Physical Examination of the Knee
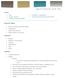 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
ACL Rehabilitation and Return To Play
 ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
KNEE INJURIES IN SPORTS MEDICINE
 KNEE INJURIES IN SPORTS MEDICINE Irving Raphael, MD June 13, 2014 RSM Medical Associates Head Team Physician Syracuse University Outline Meniscal Injuries anatomy Exam Treatment ACL Injuries Etiology Physical
KNEE INJURIES IN SPORTS MEDICINE Irving Raphael, MD June 13, 2014 RSM Medical Associates Head Team Physician Syracuse University Outline Meniscal Injuries anatomy Exam Treatment ACL Injuries Etiology Physical
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3
 AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
*smith&nephew ENDOBUTTON CL. Knee Series Technique Guide. Fixation System
 Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Novel Techniques in Articular Cartilage Restoration
 21 Novel Techniques in Articular Cartilage Restoration Adam B. Yanke, MD and Brian J. Cole, MD, MBA PART ONE: DENOVO NT Introduction DeNovo NT (Zimmer) is minced (1-mm cubes) juvenile allograft cartilage
21 Novel Techniques in Articular Cartilage Restoration Adam B. Yanke, MD and Brian J. Cole, MD, MBA PART ONE: DENOVO NT Introduction DeNovo NT (Zimmer) is minced (1-mm cubes) juvenile allograft cartilage
American College of Physicians 2013 Ohio Chapter Scientific Meeting Columbus, OH October 11, 2013
 American College of Physicians 2013 Ohio Chapter Scientific Meeting Columbus, OH October 11, 2013 Paul J. Gubanich, MD, MPH Assistant Professor of Internal Medicine/Sports Medicine Team Physician, Ohio
American College of Physicians 2013 Ohio Chapter Scientific Meeting Columbus, OH October 11, 2013 Paul J. Gubanich, MD, MPH Assistant Professor of Internal Medicine/Sports Medicine Team Physician, Ohio
TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear Search Terms
 Moksnes eappendix Page 1 of 15 TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear ch Search Terms No. of Studies #1 Anterior cruciate ligament [MeSH] 7768 #2 Child [MeSH] 1,371,559
Moksnes eappendix Page 1 of 15 TABLE E-1 Search Terms and Number of Resulting PubMed Search Results* Sear ch Search Terms No. of Studies #1 Anterior cruciate ligament [MeSH] 7768 #2 Child [MeSH] 1,371,559
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Using the depth probe, determine the appropriate implant size (thickness) for use. The
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Using the depth probe, determine the appropriate implant size (thickness) for use. The
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
October 1999, Supplement 1 Volume 15 Number 7
 October 1999, Supplement 1 Volume 15 Number 7
October 1999, Supplement 1 Volume 15 Number 7
Knee Surgical Technique
 Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
