Tibial Tubercle Osteotomy
|
|
|
- Lester Charles
- 5 years ago
- Views:
Transcription
1 Techniques in Knee Surgery 2(1):28 42, 2003 T E C H N I Q U E 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Tibial Tubercle Osteotomy JACK FARR, M.D. Clinical Associate Professor of Orthopaedic Surgery, Indiana University School of Medicine Indianapolis, Indiana, U.S.A. ABSTRACT The patellofemoral joint presents a complex challenge to the surgeon. There are many surgical options for treatment, but none is universally successful in all cases. Tibial tubercle osteotomy has a long history in the distal approach to treating patellar problems. The current approach to the patellofemoral joint continues to evolve. Previous standard measurements and treatments are being re-examined, and with this, the role of moving the tubercle in the treatment of patellar pain and/or instability. Present techniques attempt to optimize joint stability and contact area without increasing articular cartilage stress. Keywords: anteromedialization, patella, patellar dislocation, patellofemoral pain, tubercle osteotomy HISTORICAL PERSPECTIVE Tibial tubercle osteotomy represents one technique for addressing problems with patellofemoral pain and dysfunction. The multifaceted problems of the patellofemoral joint cannot be universally treated by any one surgery, and this equally applies to tibial tubercle surgery. The premise of tubercle surgery is that some patients with patellofemoral problems have, as a basis of these problems, an abnormal (or suboptimal) position of the tubercle. The surgeries may be categorized on how they affect the tubercle in the coronal plane (medial, lateral, proximal, distal) and the sagittal plane (anteriorization). History has demonstrated that the patellofemoral joint is highly sensitive over time to changes in stress. The Hauser procedure called attention to this concern when degeneration was observed in the long term 1,2 (Fig. 1). Tubercle osteotomy requires a comprehensive evaluation of the entire lower extremity, as many of the imbalances of the patellofemoral joint cannot be assigned solely to Address correspondence and reprint requests to Jack Farr, M.D., OrthoIndy, 5255 East Stop 11 Road, Suite 300, Indianapolis, IN, indyknee@hotmail.com Dr. Farr is a Mitek consultant, designed the Tracker AMZ guide, and receives royalties. FIG. 1. Medial patellofemoral arthrosis after Hauser. the position of the tubercle. Two observations are useful when contemplating tubercle surgery: (1) abnormal constraint and increased stress lead to articular cartilage overload with the potential of degeneration, and (2) no single procedure can be applied as a cure-all for patellofemoral problems. The assumption that the original tubercle position is abnormal or suboptimal for distributing force is the reason for moving the tubercle to a new position. Patellofemoral scholars continue to debate the current relevance of tubercle surgery, but review of past clinical outcomes would suggest that with proper indications, tubercle surgery still plays a role in the patellofemoral surgical armamentarium. 3,4 By far the most commonly performed tubercle surgery is medialization, popularized in the United States as the Elmslie-Trillat procedure. 5,6 Reviewing the underlying principles of this surgery may serve as a guide in evaluating the other, less commonly performed tubercle surgeries. In this case, the main premise is that the source of patellofemoral dysfunction (instability or pain) is a result of an abnormal, lateral position of the tubercle. Correcting an abnormal tubercle position suggests that there exists a known normal. Normal infers a median value with standard deviations. With this approach, with a 95% confidence level, 5% of the population by defi- 28 Techniques in Knee Surgery
2 Tibial Tubercle Osteotomy nition would be abnormal. This is not the typical use of these terms in categorizing patellofemoral patients. Instead, the common values often used as normal or abnormal are more related to the values measured in patients with or without patellofemoral problems. When comparing tubercle position to other anatomic landmarks, it is easy to focus at the knee. However, it must be appreciated that tubercle position relative to these other landmarks may be affected by femoral and tibial rotation, and in those cases, addressing the primary site of the abnormality may be more appropriate. The two common clinical measurements of tubercle relative position are the Q angle and the tubercle sulcus angle. The Q angle is measured from the iliac crest to the center of the reduced patella to the center of the tubercle measured either in extension or low levels of flexion. The tubercle sulcus angle is measured at 90 of flexion. This angle is formed by two lines. One line runs from the center of the sulcus distally and is perpendicular to the epicondylar line. The other line runs from the center of the patella to the center of the tibial tubercle. Although normal values are readily available in the literature, it must be noted that ranges are quite large, and there is poor reproducibility of repeated measurements. 7,8 While there may be comfort in using these numbers, their value in determining pathology remains in debate. Post 9 reviewed the literature on the examination of the patellofemoral joint. He found such a high variability in what is considered normal that at present, there is no universally accepted normal or abnormal. This highlights the difficulty of assigning problems of the patellofemoral joint to the position of the tubercle. Thus, at present, the decision to move the tubercle remains somewhat intuitive based on the background of the surgeon, a critical review of the literature, and a broad appreciation of the entire lower extremity. On the other hand, the literature has many reports of positive outcomes with medialization and Fulkerson anteromedialization of the tubercle Therefore, until science catches up with current practice, the surgeon must very carefully evaluate the decision to move the tubercle (and the rationale of the distance and direction of the move). In light of these limitations, an appreciation of the controversy surrounding normals and abnormals remains useful. With the known ill effects of increasing stress, a secondary goal of any tubercle surgery change of patellar tendon force vector is to improve or maintain contact area without increasing force on the joint. Surgery in the sagittal plane is only anterior, as posteriorization has been shown to increase force at the patellofemoral joint leading to degeneration. 2 The concept of anteriorization was popularized by Maquet 15 as a treatment for degeneration of the patellofemoral joint. This was based largely on two-dimensional static biomechanical analysis. Although the theoretical resultant force vector may be reduced, in reality, the calculation is quite complex and will require three-dimensional realtime analysis of both force and contact area as they vary through loaded range of motion. As the anteriorization also rotates the patella in the sagittal plane (rotation of the superior pole of the patella toward the femur) not only the forces but also the contact area change at different ranges of motion. In the normal knee, the force and contact area are uniquely matched so that at high loads, there are also larger contact areas; thus, with flexion, the increased stress is less extreme than without this safeguard. 16 Even if surgery decreases the force in the abnormal knee, if the rotation causes the contact area to diminish, the stress may actually increase (stress force per unit area). Fulkerson 12 combined the theoretical advantages of both the Maquet anteriorization procedure (to decrease patellofemoral forces) and medialization (to improve joint congruity); thus, this procedure is termed anteromedialization (AMZ) (Fig. 2). The AMZ achieved this by an oblique cut between the sagittal and coronal planes. The obliquity can be altered to achieve the same degree of elevation (typically 1.5 cm) with various degrees of medialization (the steeper the cut, the less medialization). In fact, with an offset of local bone graft, the result can be anteriorization without medialization. 17 In addition to addressing two concerns (chondrosis and subluxation), the procedure had fewer complications than the Maquet and did not require iliac bone graft harvest. 18 Using similar logic, with reversal of the oblique cut, it is possible to perform an anterolateralization, which Fulkerson 19 has shown to improve symptoms in patients with iatrogenic medial pain and degeneration such as that which occurs after a Hauser procedure. Proximalization of the tubercle is directed at treating patellar baja (infera), which in most cases occurs after an arthrofibrotic response to trauma typically surgery. 20 This is an alternative to patellar tendon lengthening and may be performed with several variations. On the other hand, distalization is typically for treatment of congenital patella alta associated with patellar instability. As such, it is usually a component of other treatments to address patellar stability and not an isolated procedure, as many patients with patellar alta have a low recurrence rate of dislocation. 21 INDICATIONS/CONTRAINDICATIONS Indications for tibial tubercle surgery may be categorized into seven overlapping groups as outlined in Table 1. Obviously, the total number of patellofemoral diagnoses is much larger, as are the multiple treatment options. In light of the variability of the human perception of pain and the many subsets of pathoanatomy, a thorough physical therapy program precedes any surgical indication. During this period, the surgeon will get to know the Volume 2, Issue 1 29
3 J. Farr FIG. 2. Comparing Maquet, Elmslie- Triatt, and AMZ. patient s postoperative rehabilitation potential and level of pain tolerance, and will be better able to localize the pain so that procedures specific for the patient s pathoanatomy may be applied. In addition, the response to different therapy methods may aid in the decisionmaking process (e.g., the response to a patellar tracking brace). Once again, these options are only in regard to the tibial tubercle after it has been systematically determined that tubercle surgery is necessary in the treatment of a patient s patellofemoral problem. A thorough review of all patellofemoral options should precede planning any of these tubercle surgeries. The total patellofemoral problem is usually complex. It is quite likely that tubercle surgery will not be done in isolation, but rather will often be combined with lateral release and/or repair/reconstruction of the medial patellofemoral ligament. Thorough knowledge of the role of the medial patellofemoral ligament in patella instability should be reviewed before the final decision is made to move the tubercle. 4 Note that the term malalignment has not been applied, as there remains much confusion over the term and its implications, as discussed by Grelsamer. 22 A new category of indications is emerging and evolving. These indications are for tubercle surgery when used in conjunction with articular cartilage restoration (Table 2). Without going into the controversy of cartilage restoration options, the underlying goal when treating any compartment of the knee with cartilage restoration is to unload the treated compartment. This is the basis for correcting subluxation of the patella to improve contact area, and often this is combined with the additional unloading offered by Fulkerson AMZ, as discussed by Peterson et al. 23 and Minas. 24 Highly controversial is the role of anteriorization when cartilage restoration is performed for isolated trochlear lesions. On the surface of the debate, it is intuitive that if anteriorization would be used to unload an isolated patellar chondral lesion, the other half of the joint (trochlea) would be treated in a similar manner. Intuition, however, must be evaluated in the laboratory. These questions may also be considered when transplanting the patellofemoral joint. When bipolar lesions are treated with osteochondral shells, Bugbee and Conver 25 typically do not move the tubercle, while others may combine the allograft transplantation with AMZ (Fig. 3A, B]. Clinical work is awaiting scientific validation; thus, caution should be exercised in these situations. Finally, proximal and distal displacements of the tibial tubercle are for opposite ends of the spectrum (Table 3). Distalization of the tubercle is used typically in patients with increased patellar mobility and delayed entrance into the constraints of the trochlea. This procedure is usually performed in conjunction with concomitant treatment such as repair/reconstruction of the medial patellofemoral ligament or some degree of medialization of the tubercle. On the other hand, proximalization is usually a component of extensive salvage surgery for the patella infera associated with advanced arthrofibrosis. In this case, reviewing the arthrofibrosis literature demonstrates proximalization is only one small part of an approach to modifying a complex and serious problem Techniques in Knee Surgery
4 Tibial Tubercle Osteotomy TABLE 1. Tibial tubercle surgery for specific patellofemoral problem noting these are often combined with various proximal procedures 1. Chronic Patellar Subluxation Medialization Option With recurrent instability (see Arendt (4)) regarding medial patellofemoral ligament) No pain (between instability) Increased T-S angle Chondrosis O-II 2. Chronic Patellar Subluxation Medialization No instability Pain Increased T-S angle Chondrosis O-II 3. Chronic Patellar Subluxation Anteromedialization With or without instability (Evaluated medial patellofemoral ligament) Pain Increased T-S angle Chondrosis III-IV 4. Normal Patellar Position Medialization No instability Pain Increased T-S angle Chondrosis O-II 5. Normal Patellar Position [LH1] Anteromedialization No instability Pain Increased T-S angle Chondrosis III-IV 6. Normal Patellar Position No instability Steep Antermedialization Pain Anteriorization Increased T-S angle Chondrosis III-IV 7. Medial Patella Post-Hauser Anterolateralization No instability Pain Chondrosis Decreased T-S angle The most common contraindication is pain or instability that does not have a rational biomechanical or articular cartilage basis. All rational conservative measures must have failed, or there is documentation of why they would fail. Altering the force and force vector will have no positive result if the pathology cannot be attributed to specific abnormalities. Certainly global anterior knee pain is a contraindication, as is generalized dehabilitation patellofemoral pain. A specific pathoanatomic contraindication common to these techniques occurs if the site of the pathology will have an increased load as a result of TABLE 2. Tibial tubercle surgeries for use in conjunction with cartilage restoration 1. Patellar and/or Trochlear Anteromedialization Cartilage Restoration when chronic subluxation is present 2. Isolated trochlear Cartilage Possible Anteriorization Restoration with normal alignment the realignment. A case in point is superior pole or superior medial chondrosis when considering an AMZ. This injury is common with dashboard posttraumatic chondrosis. Likewise, extensive trochlear involvement decreases the positive outcomes with AMZ; thus, in advanced chondrosis situations, preoperative planning should include contemplation of cartilage restoration options. With end-stage bone on bone arthrosis, rather than attempting an isolated anteriorization or AMZ, arthroplasty may be considered using standard metal and plastic arthroplasty or biologic arthroplasty (osteochondral shell allograft). As one underlying premise to the success of some these procedures is a decrease in stress, it should be expected that some body weights are so high that the postoperative stress levels (even with reduction) will still overload the joint and cause symptoms. As previously discussed, abnormal alignment may actually be distant from the knee, such as excessive anteversion of the femur/hip. In that case, the abnormality should be addressed at the source. The remaining (relative) contrain- Volume 2, Issue 1 31
5 J. Farr FIG. 3. (A) Preoperative subluxation and joint space narrowing. (B) After combined patellofemoral bipolar allograft transplantation and AMZ. dications are those shared with other realignment surgery. These would include a systemic or local inflammatory disease or involvement of the other compartments of the knee. PREOPERATIVE PLANNING As is evident in the discussion of indications, the first phase of preoperative planning is a patient-specific rehabilitation program. Optimally rehabilitated extremities will recover from the insult of surgery faster than patients with an atrophic extremity. This will also aid in a more focused diagnosis, which in turn aids in a more rational approach to surgical technique selection. As with any surgery, the history and physical lay the groundwork. In this case, the focus is on whether or not there are patellar subluxation/dislocations as opposed to the common report of giving way. The next goal is to note inciting activities of both instability and pain. On exam, pain must be as well localized as possible by the surgeon. Once the decision is made that the problem is instability, pain, or both, the underlying pathoanatomy is investigated. Patellar subluxation/dislocation patients have increased lateral displacement, and it is often associated with apprehension. With the limitations of the physical examination explained by Post, 26 it remains a goal to identify certain ranges of the patient s anatomy, such as excessive lateral position of the tubercle or J sign so excessive as to be expressed as subluxation during knee extension. These physical findings will allow tempered interpretation of additional studies. While the literature outlines many advanced techniques such as CT, dynamic MRI, and Gadolinium postexercise cartilage enhancement MRI, most decisions can be made combining an axial view such as the Merchant view (Fig. 4) with weight-bearing AP and lateral views (Fig. 5A, B) supplemented with direct arthroscopic inspection of the articular surfaces. 27 These studies are not only important to determine the appropriate patellofemoral surgery but also useful to evaluate the medial and lateral compartments in which pathology may contraindicate isolated patellofemoral surgery. Once it has been determined that TABLE 3. Proximal and distal displacement surgery of the tibial tubercle 1. Patellar instability with patellar alta as one component 2. Patella infra (baja) as a component of arthrofibrosis Distalization in conjunction with a more primary patellofemoral surgery Proximalization 32 Techniques in Knee Surgery
6 Tibial Tubercle Osteotomy FIG. 4. Merchant radiograph. tibial tubercle surgery will play a role in the overall patellofemoral plan, a specific tubercle approach may be applied based on the indications section. TECHNIQUE As the various techniques under consideration have been described numerous times in the literature, only a brief overview will be followed by a summary of technique details. To aid in comparing these surgeries, an axial view is helpful (Fig. 6). Medialization The classic Elmslie-Trillat procedure of medialization as popularized by Cox 5 in the United States is largely unchanged today in concept. The lateral release portion of the procedure may be done arthroscopically, decreasing the length of the incision. The procedure may be performed using local anesthetic infiltration of the skin and periosteum. The longitudinal incision is made immediately lateral to the tibial tubercle beginning at the proximal patellar tendon attachment level and continuing distally approximately 6 to 8 cm. The subcutaneous tissues are elevated from the tubercle, and the anterior compartment musculature is elevated subperiosteally 1 cm posterior to the anterior crest of the tubercle. The proximal attachment of the patellar tendon is protected with an Army-Navy retractor and at 1.5-cm wide osteotome cuts from lateral to medial in the axial plane. Proximally, the flare of the tibia may make it awkward to make the next cut in the coronal plane, so a small portion of the flare may be trimmed, allowing a 2.5-cm osteotome to engage fully the lateral aspect of the tubercle 1.5 cm posterior to the anterior crest. The osteotome is directed lateral to medical with care to create a flat cut or one slightly oblique (resulting in a slight AMZ). The cut is completed medial to lateral while the distal attachment remains intact. With the 2.5-cm osteotome underneath the tubercle, a pair of pliers may aid in grasping and rotating the tubercle anteriorly, which creates an initial osteoclasis of the distal attachment. Then, direct thumb pressure completes the osteoclasis with medial movement of the tubercle. The knee is then placed through range of motion, and the movement of the tubercle is evaluated. At 90 flexion, the bony contour of the trochlea/notch will aid in positioning the tubercle more medially. The goal is to medialize to a more normal position, which is still lateral to the midline of the trochlea. This midline may be estimated by both palpation and inspection. The tubercle is temporarily fixed with a k-wire and then permanently fixed with two screws using the interfragmentary technique (directed medially with knowledge of neurovascular structures) (Fig. 7). Note that when performed in cases involving patellar subluxation, even though the patella may be central statically, it may still dislocate, and therefore, attention must be directed to the medial patellofemoral ligament system. Anteromedialization Fulkerson 12 has published a detailed description of his original techniques, which should be reviewed. Farr 11 modified the technique with the approval of Fulkerson. 12 The modification developed instruments for the surgery without changing the principles or bony cuts (Tracker AMZ instruments; Mitek, Norwood, MA). The procedure is preceded by a lateral release performed open or arthroscopically. The skin incision is from the level of the portals distally 15 to 20 cm. The subcutaneous tissues are elevated, and the lateral release is continued along the patellar tendon. Distal extension continues along the anterior attachment of the anterior compartment musculature. To allow freedom of tibial tubercle movement, an incision is made immediately adjacent to the medial border of the patellar tendon. At this point, a cutting block (in this example, the block does not have a rotating base piece 11 ) is applied to the anterior crest of the tubercle beginning at the medial border of the patellar tendon attachment and angled laterally in its distal course (Fig. 8). The obliquity of the jig will allow the distal cut of the tubercle to exit laterally, fully freeing the tubercle. If placed parallel to the crest, the cut would continue down to tibia. The desired slope of the osteotomy has been determined preoperatively. That is, the steeper the slope, the less medialization, and vice versa. The angle of the slope is visualized as the slope selector outrigger-aiming device is temporarily applied to the block. A custom retractor is placed posterior to the tibia and protects deep neurovascular structures after the anterior compartment musculature has been bluntly elevated from the lateral face of the tibia. The tip of the slope selector is placed posteriorly on the lateral face of the tibia. This predetermines where the osteotomy will exit. After fine-tuning the slope and planned cut exit, the cutting block is temporarily attached to the tibia with fixation pins placed Volume 2, Issue 1 33
7 J. Farr FIG. 5. (A) Patellar height measurement. (B) Lateral view comparisons of patellar position. through holes in the cutting block into drill holes in the tibia. An oscillating saw (irrigated) makes the cut, fully exiting posterior laterally under direct visualization (Fig. 9). The jig is removed. The distal cut is finished using the osteotomy as a saw guide distally. Proximally, an oblique cut is made from the proximal extent of the posterior cut to the lateral proximal attachment of the patellar tendon to the tubercle. The tubercle is fully released after a slightly oblique transverse cut is made from the lateral aspect of the patellar tendon proximal attachment to the medial side. The tubercle is now free (Fig. 10). In open cartilage restoration surgery, the tubercle and patella may 34 Techniques in Knee Surgery
8 Tibial Tubercle Osteotomy FIG. 6. Tubercle osteotomies, axial views compared. be reflected superiorly, fully exposing the trochlea and patellar surfaces. After the desired tubercle position is achieved, it is fixed with the interfragmentary technique. If the elevated medial border of the tubercle is sharp and impinging on soft tissue, it is trimmed with a rongeur (Fig. 11). Figure 12 demonstrates intraoperative elevation measurement. Anteriorization The classic anteriorization is the Maquet, which requires iliac crest bone graft. Multiple variations are available for review in the literature. Today, with documentation of a lower complication rate using the Fulkerson AMZ, the AMZ technique may be modified to effect anteriorization without medialization. The technique begins like a standard AMZ, except the slope is nearly vertical. To avoid cutting through the posterior tibial cortical bone, an additional (near coronal plane) cut is made just anterior to the posterior aspect of the tibia. An osteotome is inserted into this posterior cut so that the saw contacts the osteotome rather than penetrate the posterior cortex. Alternatively, first a standard AMZ cut is made, but it is an extremely steep slope. This is followed by harvesting a local corticocancellous block. This block is the thickness of the measured medialization component. By inserting the block between the tubercle and the tibial cut, the medialization is neutralized; thus, the procedure results in direct anteriorization (Figs. 5, 13). Anterolateralization Fulkerson reversed the slope of the AMZ with anterolateralization (Fig. 4). Care is taken not to injure the MCL or the pes anserine tendon group. Figure 14A demonstrates medial patellofemoral degenerative change after more than 10 years post-hauser in a patient with marked symptoms. Figure 14B shows the same patient s Merchant view 9 years after anterolateralization. The patient remains pain-free to the present. Volume 2, Issue 1 35
9 J. Farr FIG. 7. Tibial tubercle medialization. FIG. 8. Positioning AMZ cutting block. 36 Techniques in Knee Surgery
10 Tibial Tubercle Osteotomy FIG. 11. Fixed AMZ; rongeur trimming tubercle. FIG. 9. AMZ saw cut. Distalization As noted previously, distalization is most commonly used in conjunction with other patellofemoral procedures that are addressing recurrent patellar instability in which there is a component of patellar alta. The tubercle is approached as per the medialization technique above, but before the bony cuts are made, a saw is used to make two distal cuts. The distal cut is made where the tubercle will be transferred with distalization. Just proximal to this cut, a second cut is made. The distance between the cuts delineates the amount of distalization that will occur (Fig. 15). The goal is to normalize the patella height, not to overcorrect it. If medialization is also desired, the more proximal cut is made slightly obliquely such that when reduction occurs, the tubercle cut fits flush with the tibial cut (the obliquity takes into account the rotation of the tubercle and may be modified as the amount of rotation is evaluated intraoperatively). During evaluation of the final position, a tubercle drill hole is made, through which a k-wire is inserted. This can allow rotation of the tubercle even as it is abutted to the tibia with distalization. Final fixation is performed with two interfragmentary screws. Figures 16, 17, 18, and 19 show preoperative and postoperative radiographs in which minor distalization was used in conjunction with medialization of the tubercle performed to centralize the FIG. 10. Measuring tubercle elevation. FIG. 12. Intraoperative AMZ elevation measurement. Volume 2, Issue 1 37
11 J. Farr FIG. 13. Bone block offset of AMZ to effect straight anteriorization. chronic patellar subluxation statically in a patient with recurrent lateral instability. Note that with these two components completed, it was still possible to dislocate the patella laterally; thus, at the same setting, the medial patellofemoral ligament was reconstructed. The thought process was that the medialized quadriceps vector (through medialization) would stress the reconstruction less. Proximalization Proximalization is only one part of a more extensive surgery to address the patella infera of arthrofibrosis. The FIG. 14. (A) Preoperative ALZ (post-hauser medial PF degenerative change). (B) Nine years postoperative ALZ. FIG. 15. Distalization of tibial tubercle. arthrofibrosis surgery and patellofemoral chondrosis will dictate whether the approach is through an AMZ or straight medialization technique (in this situation, the distal attachment would be cut rather than using osteoclasis). Once the tubercle is prepared, two (of many) options are presented for proximalization (Fig. 20). In the first, the channel is cut more proximally in the tibia, paralleling the distal cut. This allows the tubercle to slide proximally. This does alter the patellar tendon angle, and if performed with AMZ, it is limited by potential bony impingement of the tubercle on the roof of the notch/distal trochlea. These limitations may be addressed by skeletonizing the proximal tubercle, as the patellar tendon tubercle attachment is more extensive than just the proximal leading edge (Minas, Personal communication, June 2002). The tendon may be stripped approximately 1 cm, and that portion of stripped bone may be resected. The remaining tubercle is then proximalized to the limit of the original tubercle cut. Extreme caution must be exercised in evaluating the soft tissues and how they might respond to such tampering in light of the underlying disease process. Interfragmentary fixation secures the tubercle. RESULTS As is obvious, the tubercle is only one part of a comprehensive approach to the patient with patellofemoral prob- 38 Techniques in Knee Surgery
12 Tibial Tubercle Osteotomy Each of the tubercle procedures carries with it unique complications. In general, as with all patellofemoral procedures, a common complication is that of a technically correctly performed surgery, but with an unhappy patient. Patient selection and counseling to assure the patient has realistic expectations cannot be overemphasized. Intraoperative complications may involve neurovascular structures and should be avoided through proper retraction and knowledge of the anatomy. Postoperative complications are similar to those of any knee surgery, including infection, arthrofibrosis, complex regional pain syndrome (previously referred to as RSD), thromboembolism, malunion, nonunion, failure of fixation, and fracture. Arthrofibrosis has many causes, but with the secure fixation of the above surgeries, early motion and patellar mobilization are stressed as an attempt at decreasing this problem. Fracture is avoided by FIG. 16. Preoperative distalization plus medialization (lateral radiograph). lems. Thus, there are no truly isolated tibial tubercle results, and the reader should review specific treatments for specific diagnoses. There remains no uniform consensus on how and when to apply these techniques, and the Hauser late failure should temper enthusiasm for any perceived cures. On the other hand, the literature listed in the historical perspective section shows that with attention to detail, good and excellent results are possible. In the case of the AMZ, Buuck and Fulkerson 14 has found that the initially reported good results are holding with long-term follow-up (Figs. 20,21,22). As further results are reported, it must be remembered that patient selection and surgeon individual technique may be other confounding variables when trying to apply science to this complex subject. COMPLICATIONS FIG. 17. Postoperative distalization plus medialization (lateral radiograph). Volume 2, Issue 1 39
13 J. Farr FIG. 18. Preoperative distalization plus medialization (Merchant radiograph). protected weight bearing up to 6 weeks with the extensive bony cuts of an AMZ. Specific to the patella is that the very musculature (quadriceps) most important in rehabilitation is in line with the surgery. This complicates re-establishment of muscle strength and balance. Profound atrophy may be difficult to reverse. Certainly, the goal is to avoid multiple operations on the knee. Careful planning can help to achieve this goal of accomplishing the desired end result at one setting. A case in point is the lateral release. It is not a small surgery in terms of the effect on the joint. It should not be cavalierly used as a first step to see if it helps. If tubercle surgery is indicated after initial evaluation, then a comprehensive single staged surgery is less traumatic to the knee than two surgeries. In many patients, the surgeon gets only one chance to make them better. Long-term complications may be related the articular surface, which has a limited range of stress acceptance before degeneration occurs. It is important to follow patients, as the articular cartilage deterioration may take several years. This may be done remotely through a web-based outcome study such as available at In addition, any evidence of cartilage abnormality at the time of surgery deserves either close follow-up or possible consideration for cartilage restoration. protected with respect to the extent of bony surgery, and all weight bearing must be done with a normal gait. Home exercise is begun immediately. If quadriceps shutdown occurs, rapid quadriceps re-education is initiated with biofeedback and functional electrical stimulation. In light of the complex nature of the patellofemoral patient, early use of a physical therapist expertly trained in the art and science of the patellofemoral joint is essential. The current advances in therapy techniques address the entire kinetic chain and do not cookbook the rehabilitation program. To monitor this program, the patient is usually evaluated in the office every 1 to 2 weeks for the first month, and bony healing and alignment is checked radiographically at 6 weeks. If gait is normal, pain is resolved, and strength is nearing normal, patients may be released to remote follow-up (e.g., at 8 to 12 weeks. CONCERNS/FUTURE OF TECHNIQUE The major concern for the present techniques is that they are based on clinical observation and the theory of malalignment. Some patellofemoral surgeons even question if there is such a thing as malalignment. These surgeons serve as the conscience of realigning surgeons to first, do no harm. The lesson of the Hauser procedure should never be forgotten. Even subtle changes in stress to a 20-year-old knee may have serious consequences over the next 70 years of life. With these concerns in mind, one of the first steps is to return to basic science and to repeat the force and contact area work previously performed, but using newer technology with an appreciation of the total dynamics. On the clinical front, prospective analysis is needed to allow finally objective quantification of malalignment and how it relates to procedural selection and patient outcome. With this data, ideally there can be some consensus among patellofemoral surgeons as to what malalignment is and how this should direct surgery. This is under ongoing continued POSTOPERATIVE MANAGEMENT Many of the tubercle surgeries may be performed on an outpatient basis, but in the case of more extensive or concomitant surgeries, hospital admission for pain control and initiation of rehabilitation is appropriate. If there is a concern for a marked fibroblastic response, continuous passive motion is added. To facilitate early motion and rehabilitation, salvage and more extensive procedures may be performed using an epidural, which is continued for 2 to 3 days postoperatively while the patient is gradually weaned to oral medication. Weight bearing is FIG. 19. Postoperative distalization plus medialization (Merchant radiograph). 40 Techniques in Knee Surgery
14 Tibial Tubercle Osteotomy FIG. 20. Proximalization of tibial tubercle. review inspection by the International Patellofemoral Study Group ( In addition to radiographic and clinical follow-up, recent advances in cartilage research will allow less invasive monitoring of the status of the articular cartilage. Included in these techniques will be MRIs with improved cartilage specific sequencing and improved sensitivity with enhancing agents (such as the postexercise gadolium studies used today). This may be expanded with position emission biochemical scanning. The byproducts of patellofemoral articular cartilage degradation may be monitored by washout aspiration (blood or urine samples) if only one joint is involved. Certainly, early detection of cartilage injury will ideally avert untoward sequelae from surgery and may suggest earlier intervention in cases where symptoms alone would not suggest intervention. From a technique standpoint, if and when there is agreement as to the quantification of the degree of malalignment, realignment can be directed more objectively. At that point, realignment may be precisely guided aided with three-dimensional computer analysis, which is in limited use for guiding tibiofemoral realignment and for cuts in total joint arthroplasty. This may also allow monitoring of contact areas during range of motion, and when used with intraoperative force transducers, it is possible that stress in the articular cartilage could be calculated through range of motion. The goal would be to keep this stress within the physiologic range in an attempt to optimize cartilage longevity, patient comfort, and function. FIG. 21. Preoperative AMZ (Merchant radiograph). FIG. 22. Nine years after AMZ (Merchant radiograph). Volume 2, Issue 1 41
15 J. Farr REFERENCES 1. Hauser ED. Total tendon transplant for slipping patella: a new operation for recurrent dislocation of the patella. Surg Gyn Obstet 1938;66: Fulkerson JP. Disorders of the Patellofemoral Joint. Baltimore, MA: Williams and Wilkins, Fulkerson JP. Diagnosis and treatment of patients with patellofemoral pain. Am J Sports Med 2002;30: Arendt E. Management of patellofemoral disorders. Orthopedics Special Edition 2001: Cox JS. Evaluation of the Roux-Elmslie-Trillat procedure for knee extensor realignment. Am J Sports Med 1982;10: Shelbourne D, Porter D, Rozzi W. Use of a modified Elmslie-Trillat procedure to improve abnormal patellar congruence angle. Am J Sports Med 1994;2: Sanfridsson J, Arnbjornsson A, Friden T, et al. Femoral rotation and the Q-angle related to the dislocating patella. Acta Radiol 2001;42: Johnson LL, VanDyk GE, Green JR III, et al. Clinical assessment of asymptomatic knees: comparison of men and women. Arthroscopy 1998;14: Post WR. Clinical evaluation of patients with patellofemoral disorders (current concepts). Arthroscopy 1999;15: Bellemans J, Cauwenberghs F, Witvrouw E, et al. Anteromedial tibial tubercle transfer in patients with chronic anterior knee pain and a subluxation-type patellar malalignment. Am J Sports Med 1997;25: Farr J. Anteromedialization of the tibial tubercle for treatment of patellofemoral malpositioning and concomitant isolated patellofemoral arthrosis. Tech Orthop 1997;12: Fulkerson JP. Anteromedialization of the tibial tuberosity for patellofemoral malalignment. Clin Orthop 1983;177: Fulkerson JP, Arendt EA. Anterior knee pain in females. Clin Orthop 2000;372: Buuck DA, Fulkerson JP. Anteromedialization of the tibial tubecle: a 4- to 12-year follow-up. Oper Tech Sports Med 2000;8: Maquet P. Advancement of the tibial tuberosity. Clin Orthop 1976;115: Hehne HJ. Biomechanics of the patellofemoral joint and its clinical relevance. Clin Orthop 1990;258: Fulkerson JP. Patellofemoral pain disorders: evaluation and management. J Am Acad Orthop Surg 1994;2: Radin EL, Pan HQ. Long-term follow-up study on the Maquet procedure with special reference to the causes of failure. Clin Orthop 1993;290: Fulkerson JP. Anterolateralization of the tibial tubercle. Tech Orthop 1997;12: Paulos L, Rosenberg T, Drawbert J, et al. Infrapatellar contracture syndrome: an unrecognized cause of knee stiffness with patellar entrapment and patella infera. Am J Sports Med 1987;15: Atkin DM, Fithian DC, Marangi KS, et al. Characteristics of patients with primary acute lateral patellar dislocation and their recovery within the first 6 months of injury. Am J Sports Med 2000;28: Grelsamer RP. Current concepts review: patellar malalignment. J Bone Joint Surg 2000;82A: Peterson L, Minas T, Brittberg M, et al. Two- to 9-y outcome after autologous chondrocyte transplantation of the knee. Clin Orthop 2000;374: Minas T. Autologous chondrocyte implantation for focal chondral defects of the knee. Clin Orthop 2001;391S: S Bugbee WD, Conver FR. Osteochondral allograft transplantation. Clin Sports Med 1999;1: Merchant AC, Mercer RL, Jacobson RH, et al. Radiographic analysis of patellofemoral congruence. J Bone Join Surg 1974;56A: Malghem J, Maldague B. Le profil du genou: anatomie radiologique differentielle des surfaces articulaires. J Radiol 1986;67: Techniques in Knee Surgery
Which treatment? How I do a Maquet Osteotomy? Maquet: Maquet: Biomechanics. Maquet: /21/10. Philippe Landreau, MD
 Which treatment? How I do a Maquet Osteotomy? Philippe Landreau, MD Paris, France And if the patient is young?! Anterior displacement of the tibial tuberosity design to reduce the joint reactive force
Which treatment? How I do a Maquet Osteotomy? Philippe Landreau, MD Paris, France And if the patient is young?! Anterior displacement of the tibial tuberosity design to reduce the joint reactive force
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Financial Disclosures
 Management of Patellofemoral Compartment Jack Farr, M.D. Cartilage Restoration Center of Indiana OrthoIndy Knee Care Institute Indianapolis, IN Royalties Arthrex DePuy/Synthes Consulting Arthrex Advanced
Management of Patellofemoral Compartment Jack Farr, M.D. Cartilage Restoration Center of Indiana OrthoIndy Knee Care Institute Indianapolis, IN Royalties Arthrex DePuy/Synthes Consulting Arthrex Advanced
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Origins of PF Pain. Genesis of Iatrogenic Patellofemoral Pain
 Origins of PF Pain Genesis of Iatrogenic Patellofemoral Pain ISAKOS: DonJoy Consensus Meeting: Understanding Patellofemoral Pain Saturday, May 26, 2007 8:00-12:30 Talk: 7 minutes Improper Techniques Iatrogenic:
Origins of PF Pain Genesis of Iatrogenic Patellofemoral Pain ISAKOS: DonJoy Consensus Meeting: Understanding Patellofemoral Pain Saturday, May 26, 2007 8:00-12:30 Talk: 7 minutes Improper Techniques Iatrogenic:
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
Tibial Tuberosity Osteotomy
 AJSM PreView, published on November 6, 2013 as doi:10.1177/0363546513507423 Tibial Tuberosity Osteotomy Indications, Techniques, and Outcomes Clinical Sports Medicine Update Seth L. Sherman,* MD, Brandon
AJSM PreView, published on November 6, 2013 as doi:10.1177/0363546513507423 Tibial Tuberosity Osteotomy Indications, Techniques, and Outcomes Clinical Sports Medicine Update Seth L. Sherman,* MD, Brandon
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Malalignment can affect any of the three
 ch05_anbari:layout 1 8/20/2009 2:12 PM Page 47 C H A P T E R 5 Osteotomies: High Tibial, Distal Femoral, and Tibial Tubercle Ammar Anbari, MD Malalignment can affect any of the three compartments of the
ch05_anbari:layout 1 8/20/2009 2:12 PM Page 47 C H A P T E R 5 Osteotomies: High Tibial, Distal Femoral, and Tibial Tubercle Ammar Anbari, MD Malalignment can affect any of the three compartments of the
Tibial & Femoral Opening Wedge Osteotomy System. Surgical Technique
 Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Figure 3 Figure 4 Figure 5
 Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Surgical Technique for. Tracker. Anteromedialization of the Tibial Tubercle with the AMZ Guide System
 Surgical Technique for Tracker Anteromedialization of the Tibial Tubercle with the AZ Guide System Jack Farr, D, Indianapolis, IN Reviewed and approved by John P. Fulkerson, D, Farmington, CT any surgical
Surgical Technique for Tracker Anteromedialization of the Tibial Tubercle with the AZ Guide System Jack Farr, D, Indianapolis, IN Reviewed and approved by John P. Fulkerson, D, Farmington, CT any surgical
RESECTION GUIDE SYSTEM. TRUMATCH Personalized Solutions Surgical Technique with ATTUNE Knee INTUITION Instruments
 RESECTION GUIDE SYSTEM TRUMATCH Personalized Solutions Surgical Technique with ATTUNE Knee INTUITION Instruments RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the ATTUNE Knee
RESECTION GUIDE SYSTEM TRUMATCH Personalized Solutions Surgical Technique with ATTUNE Knee INTUITION Instruments RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the ATTUNE Knee
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with:
 Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
Unicompartmental Knee Replacement
 Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
MD3T -- A New Method
 MD3T -- A New Method for Safe, Secure, Accurate Tibial Tubercle Transfers March 2017, San Diego, CA Alan C. Merchant, MD Clinical Professor, Emeritus, Stanford Staff Surgeon, Emeritus, El Camino Hospital
MD3T -- A New Method for Safe, Secure, Accurate Tibial Tubercle Transfers March 2017, San Diego, CA Alan C. Merchant, MD Clinical Professor, Emeritus, Stanford Staff Surgeon, Emeritus, El Camino Hospital
EXTENDED TROCHANTERIC OSTEOTOMY SURGICAL TECHNIQUE FPO EXTENSIVELY COATED FIXATION
 EXTENDED TROCHANTERIC OSTEOTOMY SURGICAL TECHNIQUE FPO EXTENSIVELY COATED FIXATION SINCE 1983 PREOPERATIVE PLANNING EXPLANTATION OPTIONS the cement from inside the cement canal until the bone/ cement bond
EXTENDED TROCHANTERIC OSTEOTOMY SURGICAL TECHNIQUE FPO EXTENSIVELY COATED FIXATION SINCE 1983 PREOPERATIVE PLANNING EXPLANTATION OPTIONS the cement from inside the cement canal until the bone/ cement bond
ACL Rehabilitation and Return To Play
 ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Pin Guide System SURGICAL TECHNIQUE PIN GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA High Performance
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Pin Guide System SURGICAL TECHNIQUE PIN GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA High Performance
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Minimally Invasive Quad Tendon Harvest System Surgical Technique
 Minimally Invasive Quad Tendon Harvest System Surgical Technique Quad Tendon Harvest System Quadricep tendon grafts offer unique benefits for cruciate ligament reconstruction such as a predictably large
Minimally Invasive Quad Tendon Harvest System Surgical Technique Quad Tendon Harvest System Quadricep tendon grafts offer unique benefits for cruciate ligament reconstruction such as a predictably large
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Patellofemoral Replacement
 Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
Lateral Patellectomy With Anterior Tibial Tubercle Elevation: Surgical Technique and Retrospective Review
 Techniques in Knee Surgery 5(1):47 52, 2006 T E C H N I Q U E Lateral Patellectomy With Anterior Tibial Tubercle Elevation: Surgical Technique and Retrospective Review Shane J. Nho, MD, Christopher C.
Techniques in Knee Surgery 5(1):47 52, 2006 T E C H N I Q U E Lateral Patellectomy With Anterior Tibial Tubercle Elevation: Surgical Technique and Retrospective Review Shane J. Nho, MD, Christopher C.
Disclosures. Why Osteotomy? Osteotomies of the Knee Indications, Techniques and Outcomes
 Osteotomies of the Knee Indications, Techniques and Outcomes Tom Minas MD MS Director, Cartilage Repair Center BWH Associate Professor HMS, Boston Ma www.cartilagerepaircenter.org Disclosures Vericel (
Osteotomies of the Knee Indications, Techniques and Outcomes Tom Minas MD MS Director, Cartilage Repair Center BWH Associate Professor HMS, Boston Ma www.cartilagerepaircenter.org Disclosures Vericel (
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Open reduction; plate fixation 1 Principles
 Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
PRONATION-ABDUCTION FRACTURES
 C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
Surgical Technique. VISIONAIRE FastPak Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
PIN GUIDE SYSTEM SURGICAL TECHNIQUE. with the SIGMA High Performance Instruments System. This publication is not intended for distribution in the USA.
 PIN GUIDE SYSTEM with the SIGMA High Performance Instruments System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Pin Guide Surgical Technique The following steps are
PIN GUIDE SYSTEM with the SIGMA High Performance Instruments System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Pin Guide Surgical Technique The following steps are
ACL Reconstruction for BTB Grafts
 Transtibial ACL Reconstruction System for BTB Grafts Surgical Technique Designed in conjunction with John C. Garrett, M.D., Atlanta, GA ACL Reconstruction for BTB Grafts Reference Anatomical Constants
Transtibial ACL Reconstruction System for BTB Grafts Surgical Technique Designed in conjunction with John C. Garrett, M.D., Atlanta, GA ACL Reconstruction for BTB Grafts Reference Anatomical Constants
AFX. Femoral Implant. System. The AperFix. AM Portal Surgical Technique Guide. with the. The AperFix System with the AFX Femoral Implant
 The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
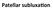 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Pin Guide System. Surgical Technique
 Pin Guide System Surgical Technique Pin Guide Surgical Technique The following steps are an addendum to the SIGMA High Performance (HP) Instruments, Fixed Reference Surgical Technique (Cat. No. 0612-87-510
Pin Guide System Surgical Technique Pin Guide Surgical Technique The following steps are an addendum to the SIGMA High Performance (HP) Instruments, Fixed Reference Surgical Technique (Cat. No. 0612-87-510
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Disclosures. Outline. The Posterior Cruciate Ligament 5/3/2016
 The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Closing Wedge Retrotubercular Tibial Osteotomy and TKA for Posttraumatic Osteoarthritis With Angular Deformity
 ORTHOPEDICS May 2009;32(5):360. Closing Wedge Retrotubercular Tibial Osteotomy and TKA for Posttraumatic Osteoarthritis With Angular Deformity by John P. Meehan, MD; Mohammad A. Khadder, MD; Amir A. Jamali,
ORTHOPEDICS May 2009;32(5):360. Closing Wedge Retrotubercular Tibial Osteotomy and TKA for Posttraumatic Osteoarthritis With Angular Deformity by John P. Meehan, MD; Mohammad A. Khadder, MD; Amir A. Jamali,
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
ANATOMIC. Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0
 ANATOMIC Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0 SCREEN LAYOUT Take screenshot Surgical step Dynamic navigation zone Information area and buttons 2 SCREEN LAYOUT Indicates action when yellow
ANATOMIC Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0 SCREEN LAYOUT Take screenshot Surgical step Dynamic navigation zone Information area and buttons 2 SCREEN LAYOUT Indicates action when yellow
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Extramedullary Tibial Preparation
 Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
DISCLOSURES. Overview 09/24/2015. Patellofemoral Instability and Treatment Options. I do not have anything to disclose
 Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
The AperFix II System
 The AperFix II System A Complete Anatomic Solution Transtibial Surgical Technique 2 AperFix II System Transtibial Surgical Technique Figure 1 A Complete Anatomic Solution The Cayenne Medical AperFix and
The AperFix II System A Complete Anatomic Solution Transtibial Surgical Technique 2 AperFix II System Transtibial Surgical Technique Figure 1 A Complete Anatomic Solution The Cayenne Medical AperFix and
Joint-Preserving Osteotomies for Isolated Patellofemoral Osteoarthritis: Alternatives to Arthroplasty
 Joint-Preserving Osteotomies for Isolated Patellofemoral Osteoarthritis: Alternatives to Arthroplasty Am J Orthop. 2017 May;46(3):139-145 Authors: Vicente Sanchis-Alfonso, MD, PhD Jason L. Koh, MD, MBA
Joint-Preserving Osteotomies for Isolated Patellofemoral Osteoarthritis: Alternatives to Arthroplasty Am J Orthop. 2017 May;46(3):139-145 Authors: Vicente Sanchis-Alfonso, MD, PhD Jason L. Koh, MD, MBA
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
*smith&nephew ENDOBUTTON CL. Knee Series Technique Guide. Fixation System
 Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Opening Wedge Osteotomy
 Tibial Opening Wedge Osteotomy System with Titanium Plates and Screws and OSferion B-TCP Osteotomy Wedge Surgical Technique Opening Wedge Osteotomy Tibial Opening Wedge Osteotomy System w/titanium Plates
Tibial Opening Wedge Osteotomy System with Titanium Plates and Screws and OSferion B-TCP Osteotomy Wedge Surgical Technique Opening Wedge Osteotomy Tibial Opening Wedge Osteotomy System w/titanium Plates
A Guide to Common Ankle Injuries
 A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique
 ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
Zimmer FuZion Instruments. Surgical Technique (Beta Version)
 Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Case Report. Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology
 Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
Transtibial PCL Reconstruction. Surgical Technique. Transtibial PCL Reconstruction
 Transtibial PCL Reconstruction Surgical Technique Transtibial PCL Reconstruction The Arthrex Transtibial PCL Reconstruction System includes unique safety features for protecting posterior neurovascular
Transtibial PCL Reconstruction Surgical Technique Transtibial PCL Reconstruction The Arthrex Transtibial PCL Reconstruction System includes unique safety features for protecting posterior neurovascular
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Patellar Ligament Disease.
 Patellar Ligament Disease. The patellar ligament disease is a condition of the stifle where the cartilage keeping the patella in place over knee joint is weakened or damaged. The patella is held in place
Patellar Ligament Disease. The patellar ligament disease is a condition of the stifle where the cartilage keeping the patella in place over knee joint is weakened or damaged. The patella is held in place
Orthopedics in Motion Tristan Hartzell, MD January 27, 2016
 Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Masterclass. Tips and tricks for a successful outcome. E. Verhaven, M. Thaeter. September 15th, 2012, Brussels
 Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
Exposure EXPOSURE. Exposure - Incision. Extend old incision proximally Expose virgin quadriceps tendon
 Exposure Aaron G Rosenberg MD Professor of Orthopedic Surgery Rush Medical College Chicago, Illinois Exposure - Incision Single incision can be used or modified Multiple longitudinal incisions favor the
Exposure Aaron G Rosenberg MD Professor of Orthopedic Surgery Rush Medical College Chicago, Illinois Exposure - Incision Single incision can be used or modified Multiple longitudinal incisions favor the
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
PediLoc Extension Osteotomy Plate (PLEO)
 PediLoc Extension Osteotomy Plate (PLEO) Left PLEO Plates Sizes: 6, 8 and 10 hole plates Right PLEO Plates Sizes: 6, 8 and 10 hole plates PediLoc Extension Osteotomy Plate The technique description herein
PediLoc Extension Osteotomy Plate (PLEO) Left PLEO Plates Sizes: 6, 8 and 10 hole plates Right PLEO Plates Sizes: 6, 8 and 10 hole plates PediLoc Extension Osteotomy Plate The technique description herein
TOTAL KNEE ARTHROPLASTY (TKA)
 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
Mako Partial Knee Medial bicompartmental
 Mako Partial Knee Medial bicompartmental Surgical reference guide Mako Robotic-Arm Assisted Surgery Table of contents Implant compatibility.... 3 Pre-operative planning.... 4 Intra-operative planning....
Mako Partial Knee Medial bicompartmental Surgical reference guide Mako Robotic-Arm Assisted Surgery Table of contents Implant compatibility.... 3 Pre-operative planning.... 4 Intra-operative planning....
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
LAMINA SPREADER SURGICAL TECHNIQUE
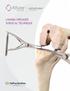 LAMINA SPREADER SURGICAL TECHNIQUE Balanced and appropriate external rotation of the femoral component is important for tibio-femoral stability in flexion and patello-femoral tracking/function. Depending
LAMINA SPREADER SURGICAL TECHNIQUE Balanced and appropriate external rotation of the femoral component is important for tibio-femoral stability in flexion and patello-femoral tracking/function. Depending
STIFFNESS AFTER TKA PRE, PER AND POST OPERATIVE CAUSING FACTORS
 STIFFNESS AFTER TKA PRE, PER AND POST OPERATIVE CAUSING FACTORS Patrick DJIAN INTRODUCTION Stiffness is one of the most common complications following TKR, causing frustration to both the surgeon and the
STIFFNESS AFTER TKA PRE, PER AND POST OPERATIVE CAUSING FACTORS Patrick DJIAN INTRODUCTION Stiffness is one of the most common complications following TKR, causing frustration to both the surgeon and the
Ascension. Silicone MCP surgical technique. surgical technique Ascension Silicone MCP
 Ascension Silicone MCP surgical technique WW 2 Introduction This manual describes the sequence of techniques and instruments used to implant the Ascension Silicone MCP (FIGURE 1A). Successful use of this
Ascension Silicone MCP surgical technique WW 2 Introduction This manual describes the sequence of techniques and instruments used to implant the Ascension Silicone MCP (FIGURE 1A). Successful use of this
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Zimmer NexGen MIS Tibial Component. Cemented Surgical Technique IMAGE TO COME
 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
ACL Reconstruction Cross-Pin Technique
 ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
3/13/2018. Cartilage Cases. Case. Physical exam
 Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Cartilage Cases Aaron J. Krych, MD Professor, Orthopedic Surgery Sports Medicine Fellowship Director Sports Medicine Research Fellowship Director Mayo Clinic 2014 MFMER slide-1 Case 19 yo F division I
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
