Ulnar nerve stability-based surgery for cubital tunnel syndrome via a small incision: a comparison with classic anterior nerve transposition
|
|
|
- Shannon Carr
- 5 years ago
- Views:
Transcription
1 Kang et al. Journal of Orthopaedic Surgery and Research (2015) 10:121 DOI /s RESEARCH ARTICLE Open Access Ulnar nerve stability-based surgery for cubital tunnel syndrome via a small incision: a comparison with classic anterior nerve transposition Ho-Jung Kang, Il-Hyun Koh, Yong-Min Chun, Won-Taek Oh, Kwang-Ho Chung and Yun-Rak Choi * Abstract Objective: The purpose of this study was to compare the clinical outcomes of ulnar nerve stability-based surgery via a small incision with those of classic anterior transposition of the ulnar nerve for cubital tunnel syndrome. Methods: From March 2008 to December 2013, 107 patients with cubital tunnel syndrome underwent simple decompression or anterior transposition via a small incision, according to an ulnar nerve stability-based decision based on an assessment of intraoperative ulnar nerve stability (group A, n = 51), or anterior transposition via a classic incision (group B, n = 56). Clinical outcome was assessed using grip and pinch strength, two-point discrimination, the mean of the disabilities of arm, shoulder, and hand (DASH) survey, and the modified Bishop scale. Results: At the final follow-up, all outcome measures improved significantly in both groups and there were no significant differences between the two groups. However, there were fewer operation-related complications in group A (one revision surgery) than in group B (one superficial infection, two painful scars, and five cases of numbness at the medial elbow). Conclusions: Outcomes after the ulnar nerve stability-based approach and anterior transposition were similar, although more patients experienced operation-related complications after anterior transposition via a classic incision. Making an ulnar nerve stability-based decision to perform either simple decompression or anterior transposition via a small incision seems to be a better strategy for patients with cubital tunnel syndrome. Background Cubital tunnel syndrome is the second most common upper-extremity compressive neuropathy, after carpal tunnel syndrome. Operative treatment is indicated after failure of conservative management. Studies have investigated the outcomes of operative techniques for treating cubital tunnel syndrome including open [1, 2] or endoscopic [3, 4] simple decompression; subcutaneous [5 7], intramuscular [8], or submuscular [2, 9] anterior transposition; and medial epicondylectomy [6, 10, 11]. However, there is no consensus regarding the best surgical technique for the condition. * Correspondence: yrchoi@yuhs.ac Department of Orthopedic Surgery, Severance Hospital, Yonsei University College of Medicine, Yonseiro 50-1, Seodaemun-gu, Seoul , Republic of Korea The most commonly used procedure for operative treatment of cubital tunnel syndrome is anterior transposition of the ulnar nerve, as this procedure can decrease the tension of the ulnar nerve that occurs with elbow flexion [12 14]. However, extensive dissection is needed to transpose the ulnar nerve, which may compromise its vascularity [15]. In contrast, simple decompression only relieves direct compression of the nerve and does not require extensive dissection; however, it cannot be used to treat dynamic ulnar nerve compression [14]. Another concern of simple decompression is that transposition after a failed simple decompression is likely to be more difficult. A recent meta-analysis of four randomized trials showed no differences in motor nerve conduction velocities or clinical outcome scores for patients with cubital tunnel syndrome treated with either simple decompression or 2015 Kang et al. Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Kang et al. Journal of Orthopaedic Surgery and Research (2015) 10:121 Page 2 of 7 ulnar nerve transposition [15]. However, two out of the four randomized studies specifically excluded patients with nerve subluxation [16, 17], limiting the applicability of these results to patients with nerve instability. Apart from the results of the above meta-analysis, Bimmer and Meyer reported improved outcomes in patients with ulnar nerve instability following anterior transposition [18]. The need for a tailored surgical approach for each patient is on the rise, and a retrospective study by Keith et al. found excellent clinical outcomes for a tailored approach of simple decompression or anterior subcutaneous transposition based on intraoperative ulnar nerve stability assessment [19]. However, data comparing that approach to classic anterior transposition of the nerve is lacking. The purpose of this study was to investigate whether the subjective and objective outcomes after making an ulnar nerve stability-based surgical decision to perform either simple decompression or anterior ulnar nerve transposition depending on intraoperative ulnar nerve stability via a small incision were comparable to those of classic anterior transposition of the ulnar nerve. Materials and methods From March 2008 to December 2013, 163 patients with clinically and electrodiagnostically confirmed cubital tunnel syndrome underwent operative treatment for cubital tunnel syndrome. Electrodiagnostic studies were conducted and interpreted by a professional rehabilitation doctor at our institution. We recommended operative treatment if patients presented with intrinsic atrophy or significant hand weakness and had clinical symptoms of tingling, pain, or weakness after at least 2 months of conservative treatment, such as night splinting and tendon gliding exercises. The inclusion criteria comprised surgically treated cubitaltunnelsyndromeandfollow-updatathatwere available for a minimum of 1 year after surgery. The exclusion criteria were as follows: electrodiagnostically silent cubital tunnel syndrome, cubitus valgus, osseous canal deformity from previous trauma or osteophytes of the elbow joint, previous surgery for cubital tunnel syndrome, associated cervical radiculopathy, carpal tunnel syndrome, ulnar tunnel syndrome, thoracic outlet syndrome, diabetes mellitus, hypothyroidism, worker s compensation issues, and follow-up data unavailability for a minimum of 1 year after surgery. Based on these criteria, four patients with electrodiagnostically silent cubital tunnel syndrome, nine patients with cubitus valgus, 14 patients with elbow osteoarthritis, seven patients requiring revision surgery, 13 patients with one of the associated diseases mentioned above, and five worker s compensation patients were excluded. Four patients were lost to follow-up. Consequently, 56 patients were excluded, and 107 patients were available for the study (Fig. 1). Among our study population, 12 patients had bilateral cubital tunnel syndrome. In these patients, we analyzed only the dominant extremity. We then had 51 patients who underwent an ulnar nerve stability-based approach involving either simple decompression (n = 37) or anterior transposition (n = 14) via a small incision (group A) and 56 patients who underwent anterior subcutaneous transposition of the ulnar nerve via a classic incision (group B). There was a distinct time period for each type of operation. Briefly, we performed anterior transposition of the ulnar nerve via a classic incision earlier in the duration of the study and changed the technique to an ulnar nerve stability-based approach via a small incision in June Group A included 32 men and 19 women with a mean age of 38.3 ± 15.0 years (range, years) at the time of surgery. The duration of symptoms to surgery was 24.1 ± 31.2 months (range, months). The mean Surgically treated cubital tunnel syndrome (n = 163) Excluded (n= 56) Electrodiagnostically silent (n = 4) Cubitus valgus (n=9) Elbow osteoarthritis (n=14) Revisional surgery (n=7) Cervical radiculopathy (n=2) Carpal tunnel syndrome (n=3) Ulnar tunnel syndrome (n=1) Thoracic outlet syndrome (n=3) Diabetes mellitus (n=3) Hypothyroidism (n=1) Worker s compensation issue (n=5) Inadequate follow-up (n=4) Group A: ulnar nerve-stability based surgery (n = 51) Group B: anterior transposition of ulnar nerve (n = 56) Fig. 1 The CONSORT diagram of enrollment and analysis in this study
3 Kang et al. Journal of Orthopaedic Surgery and Research (2015) 10:121 Page 3 of 7 follow-up period after the operation was 30.2 ± 10.8 months (range, months). Group B included 37 men and 19 women with a mean age of 35.7 ± 16.7 years (range, years) at the time of surgery. The duration of symptoms to surgery was 23.0 ± 26.8 months (range, 5 96 months). The mean follow-up period after the operation was 34.1 ± 13.2 months (range, months; Table 1). Our institutional review board approved the study and waived the requirement for informed consent. Dellon staging was applied in order to grade the preoperative severity of ulnar neuropathy [20]. According to this staging system, patients with intermittent paresthesia and subjective weakness are classified as having mild ulnar nerve compression (grade I). Patients who have moderate compression show intermittent paresthesia and measurable weakness in pinch and grip strength (grade II). Patients with persistent paresthesia, abnormal two-point discrimination, and measurable weakness in pinch and grip strength with intrinsic atrophy are classified as having severe compression (grade III). Accordingly, nine patients were rated as grade I, 27 as grade II, and the remaining 15 as grade III in group A; similarly, 11 patients were rated as grade I, 26 as grade II, and the remaining 19 as grade III in group B (Table 1). An independent observer (BRK) blinded to the method of operation performed the preoperative and postoperative assessments. Each patient was assessed for grip and pinch strength and two-point discrimination (2PD) and completed the disabilities of arm, shoulder, and hand Table 1 Baseline demographic and clinical characteristics Characteristic Group A (n = 51) Group B (n = 56) Mean age (years) 38.3 ± ± Male gender, n (%) 32 (63) 37 (66) Mean duration of symptoms 24.1 ± ± (months) Preoperative stability of ulnar nerve, n (%) Stable 41 (80) 43 (77) Unstable 10 (20) 13 (23) Dellon grade, n (%) I 9 (18) 11 (20) II 27 (53) 26 (46) III 15 (29) 19 (34) MCV at elbow segment (m/s) 39.5 ± ± Surgical procedure, n (%) <0.001 Simple decompression 37 (73) 0 (0) Anterior transposition 14 (27) 56 (100) Mean follow-up after operation (months) 30.2 ± ± MCV motor nerve conduction velocity at the elbow segment p (DASH) survey preoperatively and at each follow-up [21]. Pinch and grip strength were measured using baseline hydraulic pinch and grip dynamometers. The clinical outcome at the final follow-up was based on the Bishop rating system, which assesses subjective and objective parameters [9]. Subjective parameters included severity of residual symptoms (asymptomatic, 3; mild, 2; moderate, 1; severe, 0), subjective improvement compared with the preoperative period (better, 2; unchanged, 1; worse, 0), and preoperative and postoperative work status (working previous job, 2; changed job, 1; not working, 0). Objective parameters were grip strength compared with the normal side (80 % or more, 1; less than 80 %, 0) and sensory measurement of static two-point discrimination (6 mm or less, 1; more than 6 mm, 0). The score was defined as excellent (8 to 9), good (5 to 7), fair (3 to 4), and poor (0 to 2). Surgical technique Under general anesthesia, the patient was placed in a supine position with the affected arm supported by a hand table and sterilely prepped and draped. After exsanguination of the limb with a sterile tourniquet, the shoulder was placed at 90 of abduction and slight external rotation and the medial epicondyle and olecranon were marked. In group A, a 2.5-cm longitudinal skin incision was made between the medial epicondyle and the olecranon. Then, the subcutaneous tissues were gently and carefully separated with dissecting scissors. With the help of mini retractors, the ulnar nerve was located by releasing the brachial fascia just proximal to the cubital tunnel. Blunt dissection was carried out proximally using a curved mosquito hemostat to create a cavity between the subcutaneous tissue and the brachial fascia. A Cobb elevator was then gently introduced into this cavity to extend it at least 8 cm proximal to the medial epicondyle. A long nasal speculum was introduced into the cavity, and the brachial fascia and arcade of Struthers were released under direct visualization (Fig. 2). To allow the operating light to reach the deep operating field, the shoulder of the patient was adducted about 20, and the beam of the light was almost parallel to the upper arm. After removing the nasal speculum, Osborne s ligament was released. Then, a distal cavity was created between the subcutaneous tissue and Osborne s fascia, followed by the release of Osborne s fascia and the deep flexor-pronator aponeurosis. A short nasal speculum was introduced at that moment to assist with clear visualization of the structures (Fig. 3). Only the superficial surface of the nerve was exposed, and neurolysis was not performed to decrease the possibility of nerve subluxation. After complete release of all potential sources of structural nerve compression, the stability of the ulnar nerve was tested by moving the elbow through the full range of motion. If the nerve remained within the cubital tunnel
4 Kang et al. Journal of Orthopaedic Surgery and Research (2015) 10:121 Page 4 of 7 Fig. 2 While introducing and opening a long nasal speculum over the brachial fascia, the proximal nerve compression structures including the arcade of Struthers were completely released throughout elbow flexion, it was considered stable. If the nerve displaced onto the medial epicondyle during flexion or if it did not sit well within the cubital tunnel, it was considered unstable. In such cases where instability was identified intraoperatively, the skin incision was extended 1 cm proximally and distally to transpose the nerve anteriorly. The soft tissue above the flexor-pronator muscle group was elevated, and the ulnar nerve was then carefully lifted from its bed with its accompanying longitudinal vascular supply intact. Segmental feeding vessels were identified and ligated to prevent tethering. Neurolysis of the posterior motor branches from the main ulnar nerve was performed to allow adequate anterior transposition if there was tension. The medial intermuscular septum was also excised as part of the anterior transposition. A fascial sling raised from the underlying muscle fascia was created to prevent slippage of the nerve after transposition (Fig. 4). In group B, a 10-cm incision was placed behind the medial epicondyle. All points of ulnar nerve compression were completely released as described earlier, and care was taken to protect branches of the medial antebrachial cutaneous nerve. The soft tissue above the flexor-pronator muscle origin was elevated, and the ulnar nerve was then lifted from its bed as described earlier. The medial intermuscular septum was also excised, and a fascial sling raised from the underlying muscle fascia was created. After skin closure, a soft dressing and an elastic bandage were applied. Early movement of the fingers, wrist, forearm, elbow, and shoulder was encouraged. Statistical analysis SPSS Statistics version 18.0 (SPSS, Inc, IBM, Chicago, IL, USA) was used for statistical analyses. Group results were compared using Pearson s chi-squared test or Fisher s exact test for categorical variables and Student s t test for continuous variables. The level of significance was set at p < IRB approval This study was approved by Severance Hospital Institutional Review Board: Results Baseline patient characteristics, duration of symptoms, Dellon s grade, initial grip strength, initial pinch strength, initial 2PD, and initial DASH scores did not differ significantly between groups (Table 1). In group A, grip strength increased from a mean of 17.9 ± 8.6 to 31.9 ± 10.9 kg (p<0.001), and pinch strength increased from a mean of 3.3 ± 1.8 to 4.1 ± 2.0 kg Fig. 3 After releasing the proximal nerve compression structures, Osborne s ligament, Osborne s fascia, and the deep flexor-pronator aponeurosis were sequentially released Fig. 4 In patients with an unstable ulnar nerve, the nerve was anteriorly transposed, and a fascial sling (*) was created
5 Kang et al. Journal of Orthopaedic Surgery and Research (2015) 10:121 Page 5 of 7 (p=0.008) at the final follow-up. The mean two-point discrimination improved from 6.4 ± 2.3 to 3.2 ± 1.1 mm (p<0.001). The mean DASH score improved from 35.1 ± 21.3 to 11.0 ± 10.0 (p <0.001;Table2).According to the modified Bishop rating system, excellent results were observed in 29 patients, good in 19, and fair in three. One patient with a fair result, who had undergone in situ decompression as an index procedure, underwent anterior subcutaneous transposition of the nerve at 15 months postoperatively and reported improved symptoms after revision surgery. Based on the modified Bishop rating system, this patient s scorewas 5 at the final follow-up. There were no other complications related to the operation in group A. In group B, grip strength increased from a mean of 20.8 ± 8.8 to 31.8 ± 11.1 kg (p < 0.001) and pinch strength increased from a mean of 3.2 ± 1.6 to 4.0 ± 2.0 kg (p =0.003)atthefinalfollow-up.Themeantwopoint discrimination improved from 6.2 ± 2.7 to 3.1 ± 1.1 mm (p < 0.001). The mean DASH score improved from31±18to11±8(p < 0.001; Table 2). According to the modified Bishop scale, excellent results were observed in 35 patients, good in 16, and fair in five. There were eight complications: superficial infection in one, painful scarring in two, and numbness at the medial elbow in five (Table 3). There were no statistically significant differences between the outcomes of the two groups at the final follow-up. However, the rate of complications was higher in group B than in group A (p = 0.033). Table 2 Clinical outcomes at last follow-up Group A Group B p value Grip strength (kg) <.001 Preoperative 17.9 ± ± Last FU 31.9 ± ± Pinch strength (kg) Preoperative 3.3 ± ± Last FU 4.1 ± ± PD (mm) Preoperative 6.4 ± ± Last FU 3.2 ± ± DASH score Preoperative 35.1 ± ± Last FU 11.0 ± ± Final outcome, n (%) Excellent 29 (57) 35 (63) Good 19 (37) 16 (29) Fair 3 (6) 5 (8) 2PD two-point discrimination, DASH disability of arm, shoulder, and hand, PO postoperation Table 3 Operation-related complications Group A Group B p value Superficial infection 0 1 Revision surgery 1 0 Painful scar 0 2 Numbness at medial elbow 0 5 Total number of complications Discussion Although various surgical techniques have been introduced to treat cubital tunnel syndrome, the optimal surgical treatment is unclear. Anterior transposition of the ulnar nerve is the most commonly performed procedure for operative treatment of cubital tunnel syndrome, as it can address traction on the ulnar nerve during flexion of the elbow [12, 14]. To transpose the ulnar nerve, extensive dissection is necessary, which puts the vascularity of the nerve at risk and increases the risk of injury to the medial antebrachial cutaneous nerve. In contrast, simple decompression is considered to be an effective method for the treatment of cubital tunnel syndrome with advantages over anterior transposition, including cost-effectiveness, preservation of the blood supply to the nerve, and shorter operative and rehabilitation times [1, 15, 22, 23]. When surgeons choose simple decompression or anterior transposition, the presence of ulnar nerve subluxation with elbow flexion is one of the factors that influence the choice [18, 24]. Although making the ulnar nerve stabilitybased surgical decision to perform simple decompression or anterior transposition for patients with cubital tunnel syndrome showed favorable clinical outcomes [19], there have been no investigations comparing this surgical approach to classic anterior transposition of the ulnar nerve. In this study, we asked whether the subjective and objective outcomes after an ulnar nerve stability-based surgical approach via a small incision were comparable to those of anterior transposition of the ulnar nerve via a classic incision. In this study, functional restoration after the ulnar nerve stability-based approach was similar to that after classic anterior transposition of the ulnar nerve, as measured by outcome instruments including grip strength, two-point discrimination, DASH score, and modified Bishop score. Similar to a study conducted by Keith and Wollstein [19], use of the ulnar nerve stability-based approach resulted in 94 % of patients (48 of 51) experiencing improvement in upper limb function based on the modified Bishop score. Previously, no statistically significant differences in clinical outcomes were observed between simple decompression and anterior transposition in patients without ulnar nerve instability [15 17]. This indicates that anterior transposition of the ulnar nerve seems to be
6 Kang et al. Journal of Orthopaedic Surgery and Research (2015) 10:121 Page 6 of 7 necessary only in patients with ulnar nerve instability, so as to eliminate the symptoms of a painful subluxation of the nerve. One of the most common complications following cubital tunnel surgery is injury to the posterior branch of the medial antebrachial cutaneous nerve, which is encountered in all surgical approaches to the ulnar nerve. Injury to the nerve could cause painful neuroma, hyperesthesia, hyperalgesia around the medial elbow, and painful scarring [25, 26]. In this study, 16 % of patients (7 of 56) who underwent anterior transposition of the ulnar nerve via a classic incision experienced painful scarring (two patients) and numbness at the medial elbow (five patients); these complications were likely due to medial antebrachial cutaneous nerve injury during the surgical procedure. However, there were no injuries to the medial antebrachial cutaneous nerve in patients who underwent the ulnar nerve stability-based approach via a small incision. One possible explanation is that the small incision was made proximal to the medial epicondyle and the medial antebrachial cutaneous nerve was elevated without exposure within the elevated skin flap. In contrast, the classic technique for anterior transposition of the ulnar nerve requires a greater amount of tissue dissection than the mini-open technique, which increases the risk of injury to the medial antebrachial nerve. Concerns have been raised regarding the likelihood of ulnar nerve subluxation after simple decompression; however, there were no patients in this study who complained of symptomatic subluxation after simple decompression. This may have been due to there being only superficial release of the ulnar nerve, not neurolysis of the nerve as suggested previously [27]. In this study, one patient who underwent simple decompression and had a fair result was subject to a secondary surgery, anterior transposition of the nerve, at 15 months postoperatively. The secondary surgery may have been more difficult due to the presence of scar tissues; nevertheless, it seems that it would have been much easier after simple decompression than after anterior transposition, as simple decompression requires minimal dissection. There are several limitations to this study. First, we used two outcome measures, the modified Bishop scale and the DASH score, to estimate the clinical outcomes after surgical treatment; however, there is no reliable, reproducible, and valid outcome measure for cubital tunnel syndrome [24]. An instrument reflecting patientreported outcomes and satisfaction in combination with quantitative clinical findings is needed for standardized assessment of patients with cubital tunnel syndrome to accurately assess the clinical outcomes of surgical treatment for this common ulnar neuropathy. Second, this study includes only a limited number of cases with a relatively short-term follow-up period. Third, in our series, the interval between the onset of symptoms and surgeries was relatively longer than other studies, likely because our institution is a tertiary referral hospital and our patients were requested to recall the first time they experienced nerve symptoms even if they had a symptomfree period between each episode of symptoms. Based on the results of our study, we presume that ulnar nerve stability-based surgery for idiopathic cubital tunnel syndrome involving either simple decompression or anterior transposition via a small incision is a safe and effective strategy for surgical treatment following the failure of non-operative management. Competing interests The authors declare that they have no competing interests. Authors contributions All authors made substantive intellectual contributions to this study to qualify as authors. YRC, HJK, and YMC designed the study. KHC, WTO, and IHK collected the subjects data. IHK performed the statistical analysis. An initial draft of the manuscript was written by HJK and YRC. HJK, YMC, and YRC re-drafted parts of the manuscript and provided helpful advice on the final revision. All authors were involved in writing the manuscript. All authors have read and approved the final manuscript. Acknowledgements We thank Bo Ram Kim RN (specializing in orthopedics) for assessing clinical outcomes as an independent observer. Received: 10 June 2015 Accepted: 26 July 2015 References 1. Huang JH, Samadani U, Zager EL. Ulnar nerve entrapment neuropathy at the elbow: simple decompression. Neurosurgery. 2004;55(5): Goldfarb CA, Sutter MM, Martens EJ, Manske PR. Incidence of re-operation and subjective outcome following in situ decompression of the ulnar nerve at the cubital tunnel. J Hand Surg Eur Vol. 2009;34(3): Jiang S, Xu W, Shen Y, Xu JG, Gu YD. Endoscopy-assisted cubital tunnel release under carbon dioxide insufflation and anterior transposition. Ann Plast Surg. 2012;68(1): Yoshida A, Okutsu I, Hamanaka I. Endoscopic anatomical nerve observation and minimally invasive management of cubital tunnel syndrome. J Hand Surg Eur Vol. 2009;34(1): Caputo AE, Watson HK. Subcutaneous anterior transposition of the ulnar nerve for failed decompression of cubital tunnel syndrome. J Hand Surg Am. 2000;25(3): Hahn SB, Choi YR, Kang HJ, Kang ES. Decompression of the ulnar nerve and minimal medial epicondylectomy with a small incision for cubital tunnel syndrome: comparison with anterior subcutaneous transposition of the nerve. J Plast Reconstr Aesthet Surg. 2010;63(7): Lascar T, Laulan J. Cubital tunnel syndrome: a retrospective review of 53 anterior subcutaneous transpositions. J Hand Surg (Br). 2000;25(5): Glowacki KA, Weiss AP. Anterior intramuscular transposition of the ulnar nerve for cubital tunnel syndrome. J Shoulder Elbow Surg. 1997;6(2): Leffert RD. Anterior submuscular transposition of the ulnar nerves by the Learmonth technique. J Hand Surg Am. 1982;7(2): Efstathopoulos DG, Themistocleous GS, Papagelopoulos PJ, Chloros GD, Gerostathopoulos NE, Soucacos PN. Outcome of partial medial epicondylectomy for cubital tunnel syndrome. Clin Orthop Relat Res. 2006;444: Gobel F, Musgrave DS, Vardakas DG, Vogt MT, Sotereanos DG. Minimal medial epicondylectomy and decompression for cubital tunnel syndrome. Clin Orthop Relat Res. 2001;393: Willis BK. Cubital tunnel syndrome. In: Benzel EC, editor. Practical approaches to peripheral nerve surgery. Park Ridge: American Association of Neurosurgical Surgeons; p Bartels RH, Verhagen WI, van der Wilt GJ, Meulstee J, van Rossum LG, Grotenhuis JA. Prospective randomized controlled study comparing simple
7 Kang et al. Journal of Orthopaedic Surgery and Research (2015) 10:121 Page 7 of 7 decompression versus anterior subcutaneous transposition for idiopathic neuropathy of the ulnar nerve at the elbow: part 1. Neurosurgery. 2005;56(3): Gellberman RH, Yamaguchi K, Hollstien SB, Winn SS, Heidenreich FP Jr, Bindra RR, et al. Changes in interstitial pressure and cross-sectional area of the cubital tunnel and of the ulnar nerve with flexion of the elbow. An experimental study in human cadavera. J Bone Joint Surg Am. 1998;80(4): Zlowodzki M, Chan S, Bhandari M, Kalliainen L, Schubert W. Anterior transposition compared with simple decompression for treatment of cubital tunnel syndrome. A meta-analysis of randomized, controlled trials. J Bone Joint Surg Am. 2007;89(12): Biggs M, Curtis JA. Randomized, prospective study comparing ulnar neurolysis in situ with submuscular transposition. Neurosurgery. 2006;58(2): Gervasio O, Gambardella G, Zaccone C, Branca D. Simple decompression versus anterior submuscular transposition of the ulnar nerve in severe cubital tunnel syndrome: a prospective randomized study. Neurosurgery. 2005;56(1): Bimmler D, Meyer VE. Surgical treatment of the ulnar nerve entrapment neuropathy: submuscular anterior transposition or simple decompression of the ulnar nerve? Long-term results in 79 cases. Ann Chir Main Memb Super. 1996;15(3): Keith J, Wollstein R. A tailored approach to the surgical treatment of cubital tunnel syndrome. Ann Plast Surg. 2011;66(6): Dellon AL. Techniques for successful management of ulnar nerve entrapment at the elbow. Neurosurg Clin N Am. 1991;2(1): Hudak PL, Amadio PC, Bombardier C. Development of an upper extremity outcome measure: the DASH (disabilities of the arm, shoulder and hand) [corrected]. The Upper Extremity Collaborative Group (UECG). Am J Ind Med. 1996;29(3): Bartels RH, Termeer EH, van der Wilt GJ, van Rossum LG, Meulstee J, Verhagen WI, et al. Simple decompression or anterior subcutaneous transposition for ulnar neuropathy at the elbow: a cost-minimization analysis part 2. Neurosurgery. 2005;56(3): Bartels RH, Menovsky T, Van Overbeeke JJ, Verhagen WI. Surgical management of ulnar nerve compression at the elbow: an analysis of the literature. J Neurosurg. 1998;89(5): Macadam SA, Bezuhly M, Lefaivre KA. Outcomes measures used to assess results after surgery for cubital tunnel syndrome: a systematic review of the literature. J Hand Surg Am. 2009;34(8): Dellon AL, MacKinnon SE. Injury to the medial antebrachial cutaneous nerve during cubital tunnel surgery. J Hand Surg (Br). 1985;10: Lowe 3rd JB, Maggi SP, Mackinnon SE. The position of crossing branches of the medial antebrachial cutaneous nerve during cubital tunnel surgery in humans. Plast Reconstr Surg. 2004;114: Adkinson JM, Chung KC. Minimal-incision in situ ulnar nerve decompression at the elbow. Hand Clin. 2014;30: Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Cubital tunnel syndrome: Simple decompression versus decompression and anterior subcutaneous transposition
 CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 2009 / Page 43 C LINICAL A RTICLE Cubital tunnel syndrome: Simple versus and anterior subcutaneous Y Ramguthy BMedSc(UDW), MBChB (Medunsa) Orthopaedic Registrar*
CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 2009 / Page 43 C LINICAL A RTICLE Cubital tunnel syndrome: Simple versus and anterior subcutaneous Y Ramguthy BMedSc(UDW), MBChB (Medunsa) Orthopaedic Registrar*
Michael Ramsis Tawfik 1,*, Wael Mahmoud Khedr 1, Mahmoud Fathy Sakr 2, Ahmed Hafez Farhoud 1 and Waleed Fawzy El Saadany 1
 52 National Journal of Health Sciences, 2017, 2, 52-56 Research Article Comparative Study of Outcome of Simple Decompression Versus Anterior Transposition of Ulnar Nerve in the Treatment of Cubital Tunnel
52 National Journal of Health Sciences, 2017, 2, 52-56 Research Article Comparative Study of Outcome of Simple Decompression Versus Anterior Transposition of Ulnar Nerve in the Treatment of Cubital Tunnel
Ulnar Nerve : What Should I Do? Disclosure. Cubital Tunnel Syndrome 9/9/2018. I have nothing to disclose
 Ulnar Nerve : What Should I Do? John J. Fernandez, MD, FAAOS Assistant Professor Orthopaedic Surgery Hand & Microvascular Surgery Rush-Presbyterian-St. Luke s Medical Center Disclosure I have nothing to
Ulnar Nerve : What Should I Do? John J. Fernandez, MD, FAAOS Assistant Professor Orthopaedic Surgery Hand & Microvascular Surgery Rush-Presbyterian-St. Luke s Medical Center Disclosure I have nothing to
CUBITAL TUNNEL SYNDROME: REVIEW OF 14 ANTERIOR SUBCUTANEOUS TRANSPOSITIONS OF THE VASCULARIZED ULNAR NERVE
 CUBITAL TUNNEL SYNDROME: REVIEW OF 14 ANTERIOR SUBCUTANEOUS TRANSPOSITIONS OF THE VASCULARIZED ULNAR NERVE M. Farzan *, S. M. J. Mortazavi and S. Asadollahi Department of Orthopedic Surgery, Imam Khomeini
CUBITAL TUNNEL SYNDROME: REVIEW OF 14 ANTERIOR SUBCUTANEOUS TRANSPOSITIONS OF THE VASCULARIZED ULNAR NERVE M. Farzan *, S. M. J. Mortazavi and S. Asadollahi Department of Orthopedic Surgery, Imam Khomeini
Endoscopic Cubital Tunnel Recurrence Rates
 HAND (2010) 5:179 183 DOI 10.1007/s11552-009-9227-2 ORIGINAL ARTICLE Endoscopic Cubital Tunnel Recurrence Rates Tyson K. Cobb & Patrick T. Sterbank & Jon H. Lemke Received: 9 February 2009 / Accepted:
HAND (2010) 5:179 183 DOI 10.1007/s11552-009-9227-2 ORIGINAL ARTICLE Endoscopic Cubital Tunnel Recurrence Rates Tyson K. Cobb & Patrick T. Sterbank & Jon H. Lemke Received: 9 February 2009 / Accepted:
Musculofascial lengthening for the treatment of patients with medial epicondylitis and coexistent ulnar neuropathy
 Musculofascial lengthening for the treatment of patients with medial epicondylitis and coexistent ulnar neuropathy H. S. Gong, M. S. Chung, E. S. Kang, J. H. Oh, Y. H. Lee, G. H. Baek From Seoul National
Musculofascial lengthening for the treatment of patients with medial epicondylitis and coexistent ulnar neuropathy H. S. Gong, M. S. Chung, E. S. Kang, J. H. Oh, Y. H. Lee, G. H. Baek From Seoul National
cubital tunnel syndrome: is this method safe and effective?
 Original ARTICLE Subcutaneous anterior transposition for treatment of cubital tunnel syndrome: is this method safe and effective? Sara Lima 1, João Freitas Correia 1, Rui Moura Martins 1, Jorge Miguel
Original ARTICLE Subcutaneous anterior transposition for treatment of cubital tunnel syndrome: is this method safe and effective? Sara Lima 1, João Freitas Correia 1, Rui Moura Martins 1, Jorge Miguel
Clinical Study Our Early Experience in Surgical and Clinical Outcome on Endoscopic Cubital Tunnel Release: A Preliminary Result
 International Scholarly Research Network ISRN Orthopedics Volume 2011, Article ID 427403, 5 pages doi:10.5402/2011/427403 Clinical Study Our Early Experience in Surgical and Clinical Outcome on Endoscopic
International Scholarly Research Network ISRN Orthopedics Volume 2011, Article ID 427403, 5 pages doi:10.5402/2011/427403 Clinical Study Our Early Experience in Surgical and Clinical Outcome on Endoscopic
Disclosure. Carpal Tunnel Syndrome 11/9/15
 Michael S. Bednar, M.D. Chief, Hand Surgery Professor, Dept of Orthopaedic Surgery and Rehab Loyola University - Chicago Disclosure No conflicts for this talk Carpal Tunnel Syndrome AKA Corporal tunnel
Michael S. Bednar, M.D. Chief, Hand Surgery Professor, Dept of Orthopaedic Surgery and Rehab Loyola University - Chicago Disclosure No conflicts for this talk Carpal Tunnel Syndrome AKA Corporal tunnel
Instrument set for endoscopically assisted decompression of the ulnar nerve. Arthroscopy
 Instrument set for endoscopically assisted decompression of the ulnar nerve Arthroscopy Instrument set for endoscopically assisted decompression of the ulnar nerve Introduction The compression of the ulnar
Instrument set for endoscopically assisted decompression of the ulnar nerve Arthroscopy Instrument set for endoscopically assisted decompression of the ulnar nerve Introduction The compression of the ulnar
Long-term sequel of posterolateral rotatory instability of the elbow: a case report
 CASE REPORT Open Access Long-term sequel of posterolateral rotatory instability of the elbow: a case report Chun-Ying Cheng * Abstract The natural course of untreated posterior lateral rotatory instability
CASE REPORT Open Access Long-term sequel of posterolateral rotatory instability of the elbow: a case report Chun-Ying Cheng * Abstract The natural course of untreated posterior lateral rotatory instability
Predicting Revision Following In Situ Ulnar Nerve Decompression for Patients With Idiopathic Cubital Tunnel Syndrome.
 Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 3-1-2016 Predicting Revision Following In Situ Ulnar Nerve Decompression
Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 3-1-2016 Predicting Revision Following In Situ Ulnar Nerve Decompression
Cubital Tunnel Syndrome
 Cubital Tunnel 2 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Numbness or tingling in the little/ring side of the front and back
Cubital Tunnel 2 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Numbness or tingling in the little/ring side of the front and back
Carpal Tunnel Syndrome/ Cubital Tunnel Syndrome. Nerve anatomy. Pathophysiology 6/14/2014. Most common compression neuropathies of the upper extremity
 Carpal Tunnel Syndrome/ Cubital Tunnel Syndrome Justin Arnold MD Family Medicine Update 2014 Most common compression neuropathies of the upper extremity Increasing prevalence CTS 50/1000 subjects Up to
Carpal Tunnel Syndrome/ Cubital Tunnel Syndrome Justin Arnold MD Family Medicine Update 2014 Most common compression neuropathies of the upper extremity Increasing prevalence CTS 50/1000 subjects Up to
Cubital Tunnel Syndrome
 Cubital Tunnel 2 D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y 1122 KENILWORTH DRIVE, SUITE 18, TOWSON, MARYLAND 21204 T410 337 5400 F410 337 5520 dellon.com Right hand
Cubital Tunnel 2 D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y 1122 KENILWORTH DRIVE, SUITE 18, TOWSON, MARYLAND 21204 T410 337 5400 F410 337 5520 dellon.com Right hand
 Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
Inspection. Physical Examination of the Elbow. Anterior Elbow 2/14/2017. Inspection. Carrying angle. Lateral dimple. Physical Exam of the Elbow
 of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
INTRODUCTION Cubital Tunnel Syndrome
 INTRODUCTION Cubital Tunnel Syndrome Diagram of the ulnar nerve supplying the muscles of forearm and hand Cubital Tunnel is a condition that refers to the ulnar nerve being compressed around the elbow.
INTRODUCTION Cubital Tunnel Syndrome Diagram of the ulnar nerve supplying the muscles of forearm and hand Cubital Tunnel is a condition that refers to the ulnar nerve being compressed around the elbow.
What Treatment Works, What Does Not, When Is ENOUGH Enough?
 What Treatment Works, What Does Not, When Is ENOUGH Enough? Hand And Elbow Injuries Dori Cage, M.D. Goals of Talk Provide cases to stimulate discussion Present an approach when considering further surgery
What Treatment Works, What Does Not, When Is ENOUGH Enough? Hand And Elbow Injuries Dori Cage, M.D. Goals of Talk Provide cases to stimulate discussion Present an approach when considering further surgery
Identification of Double Compression Lesion of Ulnar Nerve after Cubital Tunnel Release
 CASE REPORT pissn 1598-3889 eissn 2234-0998 J Korean Soc Surg Hand 2015;20(3):148-152. http://dx.doi.org/10.12790/jkssh.2015.20.3.148 JOURNAL OF THE KOREAN SOCIETY FOR SURGERY OF THE HAND Identification
CASE REPORT pissn 1598-3889 eissn 2234-0998 J Korean Soc Surg Hand 2015;20(3):148-152. http://dx.doi.org/10.12790/jkssh.2015.20.3.148 JOURNAL OF THE KOREAN SOCIETY FOR SURGERY OF THE HAND Identification
Unrecognized dislocation of the medial portion of the triceps: another cause of failed ulnar nerve transposition
 J Neurosurg 92:52 57, 2000 Unrecognized dislocation of the medial portion of the triceps: another cause of failed ulnar nerve transposition ROBERT J. SPINNER, M.D., SHAWN W. O DRISCOLL, M.D., PH.D., JESSE
J Neurosurg 92:52 57, 2000 Unrecognized dislocation of the medial portion of the triceps: another cause of failed ulnar nerve transposition ROBERT J. SPINNER, M.D., SHAWN W. O DRISCOLL, M.D., PH.D., JESSE
Accuracy of Preoperative Ultrasonography for Cubital Tunnel Syndrome: A Comparison with Intraoperative Findings
 Original Article Clinics in Orthopedic Surgery 2018;10:352-357 https://doi.org/10.4055/cios.2018.10.3.352 Accuracy of Preoperative Ultrasonography for Cubital Tunnel Syndrome: A Comparison with Intraoperative
Original Article Clinics in Orthopedic Surgery 2018;10:352-357 https://doi.org/10.4055/cios.2018.10.3.352 Accuracy of Preoperative Ultrasonography for Cubital Tunnel Syndrome: A Comparison with Intraoperative
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome)
 A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
Original Article INTRODUCTION MATERIALS AND METHODS
 Original Article Comparison of anterior subcutaneous and submuscular transposition of ulnar nerve in treatment of cubital tunnel syndrome: A prospective randomized trial Abolghassem Zarezadeh, Hamidreza
Original Article Comparison of anterior subcutaneous and submuscular transposition of ulnar nerve in treatment of cubital tunnel syndrome: A prospective randomized trial Abolghassem Zarezadeh, Hamidreza
Anterior subcutaneous transposition of the ulnar nerve improves neurological function in patients with cubital tunnel syndrome
 NEURAL REGENERATION RESEARCH October 2015,Volume 10,Issue 10 www.nrronline.org Anterior subcutaneous transposition of the ulnar nerve improves neurological function in patients with cubital tunnel syndrome
NEURAL REGENERATION RESEARCH October 2015,Volume 10,Issue 10 www.nrronline.org Anterior subcutaneous transposition of the ulnar nerve improves neurological function in patients with cubital tunnel syndrome
Cubital Tunnel Syndrome
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Outcome and predictors in simple decompression of ulnar nerve entrapment at the elbow
 Original Article Hand Microsurg 2018;7:24-32 doi:10.5455/handmicrosurg.266188 Outcome and predictors in simple decompression of ulnar nerve entrapment at the elbow Ilka Anker 1, Malin Zimmerman 1, Gert
Original Article Hand Microsurg 2018;7:24-32 doi:10.5455/handmicrosurg.266188 Outcome and predictors in simple decompression of ulnar nerve entrapment at the elbow Ilka Anker 1, Malin Zimmerman 1, Gert
Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini
 Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Centerline Carpal Tunnel Release
 Centerline Endoscopic Carpal Tunnel Release Surgical Technique Centerline Carpal Tunnel Release Centerline Endoscopic Carpal Tunnel Release Surgical Set Up The patient is positioned supine on the operating
Centerline Endoscopic Carpal Tunnel Release Surgical Technique Centerline Carpal Tunnel Release Centerline Endoscopic Carpal Tunnel Release Surgical Set Up The patient is positioned supine on the operating
Common Elbow Problems
 Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Other Elbow Concerns in Overhead Athletes
 Other Elbow Concerns in Overhead Athletes John A. Steubs, M.D. Team Physician, Minnesota Twins TRIA Orthopaedic Center Disclosures None relevant to this presentation. Other Elbow Problems Valgus extension
Other Elbow Concerns in Overhead Athletes John A. Steubs, M.D. Team Physician, Minnesota Twins TRIA Orthopaedic Center Disclosures None relevant to this presentation. Other Elbow Problems Valgus extension
region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla.
 1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
1 region of the upper limb between the shoulder and the elbow Superiorly communicates with the axilla. Inferiorly, a number of important structures pass between arm & forearm through cubital fossa. 2 medial
Elbow. Chapter 2 LISTEN. Mechanism of Injury (If Applicable) Pain
 Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Title: ANATOMIC CHARACTERISTICS OF A FASCIA AND ITS BANDS OVERLYING THE ULNAR NERVE IN THE PROXIMAL FOREARM: A CADAVER STUDY
 Elsevier Editorial System(tm) for Journal of Hand Surgery (European Volume) Manuscript Draft Manuscript Number: JHSB-D-06-00113R2 Title: ANATOMIC CHARACTERISTICS OF A FASCIA AND ITS BANDS OVERLYING THE
Elsevier Editorial System(tm) for Journal of Hand Surgery (European Volume) Manuscript Draft Manuscript Number: JHSB-D-06-00113R2 Title: ANATOMIC CHARACTERISTICS OF A FASCIA AND ITS BANDS OVERLYING THE
Nerves of Upper limb. Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh
 Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
The optimal surgical technique in the management of idiopathic
 CLINICAL STUDIES RANDOMIZED, PROSPECTIVE STUDY COMPARING ULNAR NEUROLYSIS IN SITU WITH SUBMUSCULAR TRANSPOSITION Michael Biggs, F.R.A.C.S. Department of Neurosurgery, Royal North Shore Hospital, Sydney,
CLINICAL STUDIES RANDOMIZED, PROSPECTIVE STUDY COMPARING ULNAR NEUROLYSIS IN SITU WITH SUBMUSCULAR TRANSPOSITION Michael Biggs, F.R.A.C.S. Department of Neurosurgery, Royal North Shore Hospital, Sydney,
Heterotopic Ossification of the Elbow after Medial Epicondylectomy
 66 neuritis and had undergone medial epicondylectomy and debridement of the common flexor tendon origin of the symptomatic elbow, at another institution seven months prior to visiting to our clinic. Upon
66 neuritis and had undergone medial epicondylectomy and debridement of the common flexor tendon origin of the symptomatic elbow, at another institution seven months prior to visiting to our clinic. Upon
Carpal Tunnel Release
 Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
Ulnar Neuropathy in the Distal Ulnar Tunnel
 Ulnar Neuropathy in the Distal Ulnar Tunnel DAVID W. SHUPE, PT, ATC' Journal of Orthopaedic & Sports Physical Therapy A brief anatomical review of the ulnar nerve and areas of ulnar nerve entrapment is
Ulnar Neuropathy in the Distal Ulnar Tunnel DAVID W. SHUPE, PT, ATC' Journal of Orthopaedic & Sports Physical Therapy A brief anatomical review of the ulnar nerve and areas of ulnar nerve entrapment is
Elbow Pain. Lateral Elbow Pain. Lateral Elbow Pain. tennis elbow lateral epicondylitis extensor tendinopathy
 Elbow Pain Peter Brukner OAM, FACSP Associate Professor in Sports Medicine Centre for Health, Exercise and Sports Medicine University of Melbourne Lateral Elbow Pain tennis elbow lateral epicondylitis
Elbow Pain Peter Brukner OAM, FACSP Associate Professor in Sports Medicine Centre for Health, Exercise and Sports Medicine University of Melbourne Lateral Elbow Pain tennis elbow lateral epicondylitis
1 Upper Extremity Compression Neuropathies Bernard F. Hearon, M.D. Clinical Assistant Professor, Department of Surgery University of Kansas School of
 1 Upper Extremity Compression Neuropathies Bernard F. Hearon, M.D. Clinical Assistant Professor, Department of Surgery University of Kansas School of Medicine - Wichita November 22, 2013 2 www.drhearon.com
1 Upper Extremity Compression Neuropathies Bernard F. Hearon, M.D. Clinical Assistant Professor, Department of Surgery University of Kansas School of Medicine - Wichita November 22, 2013 2 www.drhearon.com
Elbow Elbow Anatomy. Flexion extension. Pronation Supination. Anatomy. Anatomy. Romina Astifidis, MS., PT., CHT
 Elbow Elbow Anatomy Romina Astifidis, MS., PT., CHT Curtis National Hand Center Baltimore, MD October 6-8, 2017 Link between the arm and forearm to position the hand in space Not just a hinge Elbow = 70%
Elbow Elbow Anatomy Romina Astifidis, MS., PT., CHT Curtis National Hand Center Baltimore, MD October 6-8, 2017 Link between the arm and forearm to position the hand in space Not just a hinge Elbow = 70%
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides
 IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure)
 Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
PG Session: Power Ortho: Hand & Wrist/ Kyle Bickel, MD, FACS
 WOHC 2012 Hand & Wrist Kyle D. Bickel, M.D., FACS The Hand Center of San Francisco Disclosure Information Western Occupational Health Conference 2012 Kyle D. Bickel, MD, FACS I have no pertinent financial
WOHC 2012 Hand & Wrist Kyle D. Bickel, M.D., FACS The Hand Center of San Francisco Disclosure Information Western Occupational Health Conference 2012 Kyle D. Bickel, MD, FACS I have no pertinent financial
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Common Upper Extremity Neuropathies (Not Carpal Tunnel Syndrome)
 Common Upper Extremity Neuropathies (Not Carpal Tunnel Syndrome) Nerve Compressions Common in adults, rare in children Frequently cause missed days of work and sleepless nights CDC 2001 26,794 cases of
Common Upper Extremity Neuropathies (Not Carpal Tunnel Syndrome) Nerve Compressions Common in adults, rare in children Frequently cause missed days of work and sleepless nights CDC 2001 26,794 cases of
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
OCCUPATIONAL INJURIES OF THE ELBOW
 PLEASE STAND BY WEBINAR WILL BEGIN AT 12:00 PM PST FOR AUDIO: CALL 866-740-1260 / ACCESS CODE: 764-4915# JAMES VAN DEN BOGAERDE, MD OCCUPATIONAL INJURIES OF THE ELBOW Conflict of Interest Disclosure I,
PLEASE STAND BY WEBINAR WILL BEGIN AT 12:00 PM PST FOR AUDIO: CALL 866-740-1260 / ACCESS CODE: 764-4915# JAMES VAN DEN BOGAERDE, MD OCCUPATIONAL INJURIES OF THE ELBOW Conflict of Interest Disclosure I,
Anatomic Landmarks for the Radial Tunnel
 Anatomic Landmarks for the Radial Tunnel Ron Hazani, MD, Nitin J. Engineer, MD, Arian Mowlavi, MD, Michael Neumeister, MD, W.P. Andrew Lee, MD, and Bradon J. Wilhelmi, MD Division of Plastic and Reconstructive
Anatomic Landmarks for the Radial Tunnel Ron Hazani, MD, Nitin J. Engineer, MD, Arian Mowlavi, MD, Michael Neumeister, MD, W.P. Andrew Lee, MD, and Bradon J. Wilhelmi, MD Division of Plastic and Reconstructive
Recurrent subluxation or dislocation after surgical
 )263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
)263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
Cubital Tunnel Syndrome Caused by Anconeus Epitrochlearis
 Clinical Article J Korean Neurosurg Soc 61 (5) : 618-624, 2018 https://doi.org/10.3340/jkns.2018.0033 pissn 2005-3711 eissn 1598-7876 Cubital Tunnel Syndrome Caused by Anconeus Epitrochlearis Muscle Il-Jung
Clinical Article J Korean Neurosurg Soc 61 (5) : 618-624, 2018 https://doi.org/10.3340/jkns.2018.0033 pissn 2005-3711 eissn 1598-7876 Cubital Tunnel Syndrome Caused by Anconeus Epitrochlearis Muscle Il-Jung
Elbow. Chapter 2 LISTEN. Mechanism of Injury (If Applicable) Pain
 Preface The first decade of the twenty-first century has witnessed the continuation of an explosion in our knowledge and understanding of all aspects of disease. Accompanying this has been the increasing
Preface The first decade of the twenty-first century has witnessed the continuation of an explosion in our knowledge and understanding of all aspects of disease. Accompanying this has been the increasing
INSTRUCTIONAL COURSE 46: Patients and Procedures Those to Avoid and Those to Embrace
 INSTRUCTIONAL COURSE 46: Patients and Procedures Those to Avoid and Those to Embrace Handouts Saturday, September 20 * 6:45-7:45 AM 69TH ANNUAL MEETING OF THE ASSH SEPTEMBER 18-20, 2014 BOSTON, MA Moderator(s):
INSTRUCTIONAL COURSE 46: Patients and Procedures Those to Avoid and Those to Embrace Handouts Saturday, September 20 * 6:45-7:45 AM 69TH ANNUAL MEETING OF THE ASSH SEPTEMBER 18-20, 2014 BOSTON, MA Moderator(s):
Proximal radioulnar translocation associated with elbow dislocation and radial neck fracture in child: a case report and review of literature
 DOI 10.1007/s00402-013-1820-8 TRAUMA SURGERY Proximal radioulnar translocation associated with elbow dislocation and radial neck fracture in child: a case report and review of literature Hong Kee Yoon
DOI 10.1007/s00402-013-1820-8 TRAUMA SURGERY Proximal radioulnar translocation associated with elbow dislocation and radial neck fracture in child: a case report and review of literature Hong Kee Yoon
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Diagnosis of Neck & Upper Extremity Pain
 Diagnosis of Neck & Upper Extremity Pain David B. Bumpass, MD Assistant Professor, Spine Surgery UAMS Depts. of Orthopaedic Surgery & Neurosurgery May 12, 2018 Disclosures Medtronic Spine speaking fees
Diagnosis of Neck & Upper Extremity Pain David B. Bumpass, MD Assistant Professor, Spine Surgery UAMS Depts. of Orthopaedic Surgery & Neurosurgery May 12, 2018 Disclosures Medtronic Spine speaking fees
Interesting Case Series. Radial Tunnel Syndrome Complicated by Lateral Epicondylitis in a Middle-Aged Female
 Interesting Case Series Radial Tunnel Syndrome Complicated by Lateral Epicondylitis in a Middle-Aged Female Sumesh Kaswan, MD, a Olivier Deigni, MD, MPH, a Kashyap K. Tadisina, BS, b Michael Totten, BS,
Interesting Case Series Radial Tunnel Syndrome Complicated by Lateral Epicondylitis in a Middle-Aged Female Sumesh Kaswan, MD, a Olivier Deigni, MD, MPH, a Kashyap K. Tadisina, BS, b Michael Totten, BS,
Clinical classification and treatment of cubital tunnel syndrome
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 8: 1365-1370, 2014 Clinical classification and treatment of cubital tunnel syndrome CUI QING, JIANHUA ZHANG, SHIDONG WU, ZHAO LING, SHUANCHI WANG, HAORAN LI and HAIQING
EXPERIMENTAL AND THERAPEUTIC MEDICINE 8: 1365-1370, 2014 Clinical classification and treatment of cubital tunnel syndrome CUI QING, JIANHUA ZHANG, SHIDONG WU, ZHAO LING, SHUANCHI WANG, HAORAN LI and HAIQING
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM
 EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
Lowe Plastic Surgery (LPS)
 Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
Correction of Long Standing Proximal Interphalangeal Flexion Contractures with Cross Finger Flaps and Vigorous Postoperative Exercises
 Original Article DOI 10.3349/ymj.2010.51.4.574 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(4):574-578, 2010 Correction of Long Standing Proximal Interphalangeal Flexion Contractures with Cross Finger
Original Article DOI 10.3349/ymj.2010.51.4.574 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(4):574-578, 2010 Correction of Long Standing Proximal Interphalangeal Flexion Contractures with Cross Finger
Dr. Mahir Alhadidi Anatomy Lecture #9 Feb,28 th 2012
 Quick Revision: Upper arm is divided into two compartments: 1. Anterior Compartment: Contains three muscles (Biceps brachii, Coracobrachialis, Brachialis). Innervated by Musculocutaneous nerve. 2. Posterior
Quick Revision: Upper arm is divided into two compartments: 1. Anterior Compartment: Contains three muscles (Biceps brachii, Coracobrachialis, Brachialis). Innervated by Musculocutaneous nerve. 2. Posterior
Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture Dislocation of the Elbow in an Adult
 Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
Hindawi Case Reports in Orthopedics Volume 2018, Article ID 5401634, 6 pages https://doi.org/10.1155/2018/5401634 Case Report Intra-Articular Entrapment of the Medial Epicondyle following a Traumatic Fracture
Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader. Lab Leaders: STATION I BRACHIAL PLEXUS
 Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader Lab Leaders: STATION I BRACHIAL PLEXUS A. Posterior cervical triangle and axilla B. Formation of plexus 1. Ventral rami C5-T1 2. Trunks
Anatomy Workshop Upper Extremity David Ebaugh, PT, PhD Workshop Leader Lab Leaders: STATION I BRACHIAL PLEXUS A. Posterior cervical triangle and axilla B. Formation of plexus 1. Ventral rami C5-T1 2. Trunks
* WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 84/07
 * WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 84/07 BEFORE: A. Suissa: Vice-Chair HEARING: January 12, 2007 at Toronto Written DATE OF DECISION: January 12, 2007 NEUTRAL CITATION: 2007
* WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 84/07 BEFORE: A. Suissa: Vice-Chair HEARING: January 12, 2007 at Toronto Written DATE OF DECISION: January 12, 2007 NEUTRAL CITATION: 2007
CARPAL TUNNEL SYNDROME
 CARPAL TUNNEL SYNDROME Carpal tunnel syndrome results from the pinching or entrapping of the median nerve in the underside of the wrist. The actual pathology in most cases is due to either a decrease in
CARPAL TUNNEL SYNDROME Carpal tunnel syndrome results from the pinching or entrapping of the median nerve in the underside of the wrist. The actual pathology in most cases is due to either a decrease in
Posteromedial approach to the distal humerus for fracture fixation
 Acta Orthop. Belg., 2006, 72, 395-399 ORIGINAL STUDY Posteromedial approach to the distal humerus for fracture fixation Cédric LAPORTE, Maurice THIONGO, Dominique JEGOU From the General Hospital of Meaux,
Acta Orthop. Belg., 2006, 72, 395-399 ORIGINAL STUDY Posteromedial approach to the distal humerus for fracture fixation Cédric LAPORTE, Maurice THIONGO, Dominique JEGOU From the General Hospital of Meaux,
The Elbow 3/5/2015. The Elbow Scanning Sequence. * Anterior Joint (The anterior Pyramid ) * Lateral Epicondyle * Medial Epicondyle * Posterior Joint
 Scanning Sequence * Anterior Joint (The anterior Pyramid ) * Lateral Epicondyle * Medial Epicondyle * Posterior Joint Anterior Elbow Pyramid Courtesy of Jay Smith, MD. Vice chair PMR Mayo Clinic Rochester,
Scanning Sequence * Anterior Joint (The anterior Pyramid ) * Lateral Epicondyle * Medial Epicondyle * Posterior Joint Anterior Elbow Pyramid Courtesy of Jay Smith, MD. Vice chair PMR Mayo Clinic Rochester,
Clinical examination of the wrist, thumb and hand
 Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
Comparison of the results of open
 1131 Original Article Singapore Med.1 27; 48 (12) : Comparison of the results of open carpal tunnel release and KnifeLight carpal tunnel release Yeo K Q, Yeo E M N Yeo Orthopaedic Centre, Mount Elizabeth
1131 Original Article Singapore Med.1 27; 48 (12) : Comparison of the results of open carpal tunnel release and KnifeLight carpal tunnel release Yeo K Q, Yeo E M N Yeo Orthopaedic Centre, Mount Elizabeth
The arm: *For images refer back to the slides
 The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
The arm: *For images refer back to the slides Muscles of the arm: deltoid, triceps (which is located at the back of the arm), biceps and brachialis (it lies under the biceps), brachioradialis (it lies
Pain Assessment Patient Interview (location/nature of symptoms), Body Diagram. Observation and Examination: Tests and Measures
 Examination of Upper Quarter Neurogenic Pain Jane Fedorczyk, PT, PhD, CHT Thomas Jefferson University, Philadelphia, PA Center of Excellence for Hand and Upper Limb Rehabilitation I. History Mechanism
Examination of Upper Quarter Neurogenic Pain Jane Fedorczyk, PT, PhD, CHT Thomas Jefferson University, Philadelphia, PA Center of Excellence for Hand and Upper Limb Rehabilitation I. History Mechanism
Case Presentation: Comminuted Fractures of the Proximal Ulna 11/28/2017. Disclosures. Surgical Strategy. Implant Choice. Melvin P.
 Current Solutions in Orthopaedic Trauma Case Presentation: Comminuted Fracture of the Proximal Ulna Melvin P. Rosenwasser, MD Robert E. Carroll Professor of Surgery of the Hand Chief, Orthopaedic Hand
Current Solutions in Orthopaedic Trauma Case Presentation: Comminuted Fracture of the Proximal Ulna Melvin P. Rosenwasser, MD Robert E. Carroll Professor of Surgery of the Hand Chief, Orthopaedic Hand
CARPAL TUNNEL RELEASE VIA MINI-OPEN WRIST CREASE INCISION: PROCEDURE AND RESULTS OF FOUR YEARS CLINICAL EXPERIENCE
 CARPAL TUNNEL RELEASE VIA MINI-OPEN WRIST CREASE INCISION: PROCEDURE AND RESULTS OF FOUR YEARS CLINICAL EXPERIENCE Sudqi A. Hamed 1, Falah Z. Harfoushi 2 ABSTRACT Objective: To evaluate prospectively the
CARPAL TUNNEL RELEASE VIA MINI-OPEN WRIST CREASE INCISION: PROCEDURE AND RESULTS OF FOUR YEARS CLINICAL EXPERIENCE Sudqi A. Hamed 1, Falah Z. Harfoushi 2 ABSTRACT Objective: To evaluate prospectively the
Introduction. Anatomy
 Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Endoscopic Carpal Tunnel Release ECTR
 Endoscopic Carpal Tunnel Release ECTR Christophe MATHOULIN Paris, France Historics Paget, 1854 Putnam, 1893 Hunt, 1909 Marie et Foix, 1913 Recommanded surgical release Learmonth, 1933 First reported release
Endoscopic Carpal Tunnel Release ECTR Christophe MATHOULIN Paris, France Historics Paget, 1854 Putnam, 1893 Hunt, 1909 Marie et Foix, 1913 Recommanded surgical release Learmonth, 1933 First reported release
Movement of the Ulnar Nerve at the Elbow
 ORIGINAL RESEARCH Movement of the Ulnar Nerve at the Elbow A Sonographic Study Seung Nam Yang, MD, PhD, Joon Shik Yoon, MD, PhD, Sei Joo Kim, MD, PhD, Hyo Jung Kang, MD, Se Hwa Kim, MD Objectives The aim
ORIGINAL RESEARCH Movement of the Ulnar Nerve at the Elbow A Sonographic Study Seung Nam Yang, MD, PhD, Joon Shik Yoon, MD, PhD, Sei Joo Kim, MD, PhD, Hyo Jung Kang, MD, Se Hwa Kim, MD Objectives The aim
Patient-Related Risk Factors for Infection Following Ulnar Nerve Release at the Cubital Tunnel
 Original Research Patient-Related Risk Factors for Infection Following Ulnar Nerve Release at the Cubital Tunnel An Analysis of 15,188 Cases Christopher L. Camp,* MD, Collin C. Tebo, MA, Ryan M. Degen,
Original Research Patient-Related Risk Factors for Infection Following Ulnar Nerve Release at the Cubital Tunnel An Analysis of 15,188 Cases Christopher L. Camp,* MD, Collin C. Tebo, MA, Ryan M. Degen,
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
CNS & PNS Entrapment. Disclosure - Nothing
 Peripheral Nerve Entrapments That Mimic Spinal Pathology: Evaluation And Treatment Both Medical And Surgical Michel Kliot MD Clinical Professor UCSF Department of NeuroSurgery Director Center For Evaluation
Peripheral Nerve Entrapments That Mimic Spinal Pathology: Evaluation And Treatment Both Medical And Surgical Michel Kliot MD Clinical Professor UCSF Department of NeuroSurgery Director Center For Evaluation
Arm Pain, Numbness, and Tingling: Etiologies and Treatment
 Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
Functional Anatomy of the Elbow
 Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
T HE carpal tunnel syndrome (CTS) is a clinical
 J Neurosurg 62:352-356, 1985 Complications of carpal tunnel surgery DEAN S. LOUIS, M.D., THOMAS L. GREENE, M.D., AND RAYMOND C. NOELLERT, Orthopaedic Hand Service, Department of Surgery, University of
J Neurosurg 62:352-356, 1985 Complications of carpal tunnel surgery DEAN S. LOUIS, M.D., THOMAS L. GREENE, M.D., AND RAYMOND C. NOELLERT, Orthopaedic Hand Service, Department of Surgery, University of
While common peroneal nerve compression is a. Decompression of the superficial peroneal nerve: clinical outcomes and anatomical study
 clinical article J Neurosurg 126:330 335, 2017 Decompression of the superficial peroneal nerve: clinical outcomes and anatomical study Michael J. Franco, MD, Benjamin Z. Phillips, MD, MPH, Gopal R. Lalchandani,
clinical article J Neurosurg 126:330 335, 2017 Decompression of the superficial peroneal nerve: clinical outcomes and anatomical study Michael J. Franco, MD, Benjamin Z. Phillips, MD, MPH, Gopal R. Lalchandani,
1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint
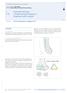 1 Executive Editor: Chris Colton Authors: Mariusz Bonczar, Daniel Rikli, David Ring 1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint Indication All 13-A type fractures, excluding
1 Executive Editor: Chris Colton Authors: Mariusz Bonczar, Daniel Rikli, David Ring 1 Humeral fractures 1.13 l Distal humeral fractures Treatment with a splint Indication All 13-A type fractures, excluding
Co-Innervation of Triceps Brachii Muscle with Variant Branch of Ulnar Nerve
 DOI: 10.5137/1019-5149.JTN.22126-17.2 Received: 23.11.2017 / Accepted: 07.02.2018 Published Online: 26.02.2018 Turk Neurosurg, 2018 Original Investigation Co-Innervation of Triceps Brachii Muscle with
DOI: 10.5137/1019-5149.JTN.22126-17.2 Received: 23.11.2017 / Accepted: 07.02.2018 Published Online: 26.02.2018 Turk Neurosurg, 2018 Original Investigation Co-Innervation of Triceps Brachii Muscle with
Entrapment neuropathies commonly occur as nerves
 Clinical article J Neurosurg 125:1533 1538, 2016 The anconeus epitrochlearis muscle may protect against the development of cubital tunnel syndrome: a preliminary study Thomas J. Wilson, MD, 1 R. Shane
Clinical article J Neurosurg 125:1533 1538, 2016 The anconeus epitrochlearis muscle may protect against the development of cubital tunnel syndrome: a preliminary study Thomas J. Wilson, MD, 1 R. Shane
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM
 TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
ELBOW ARTHROSCOPY WHERE ARE WE NOW?
 ELBOW ARTHROSCOPY WHERE ARE WE NOW? Christian Veillette M.D., M.Sc., FRCSC Assistant Professor, University of Toronto Shoulder & Elbow Reconstructive Surgery Toronto Western Hospital @ University Health
ELBOW ARTHROSCOPY WHERE ARE WE NOW? Christian Veillette M.D., M.Sc., FRCSC Assistant Professor, University of Toronto Shoulder & Elbow Reconstructive Surgery Toronto Western Hospital @ University Health
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL
 Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
Case Report Successful Closed Reduction of a Lateral Elbow Dislocation
 Case Reports in Orthopedics Volume 2016, Article ID 5934281, 5 pages http://dx.doi.org/10.1155/2016/5934281 Case Report Successful Closed Reduction of a Lateral Elbow Dislocation Kenya Watanabe, Takuma
Case Reports in Orthopedics Volume 2016, Article ID 5934281, 5 pages http://dx.doi.org/10.1155/2016/5934281 Case Report Successful Closed Reduction of a Lateral Elbow Dislocation Kenya Watanabe, Takuma
MSK Imaging Conference. 07/22/2016 Eman Alqahtani, MD, MPH R3/PGY4 UCSD Radiology
 MSK Imaging Conference 07/22/2016 Eman Alqahtani, MD, MPH R3/PGY4 UCSD Radiology A 51 years old female with chronic thumb pain, and inability to actively flex the thumb interphalyngeal joint Possible trigger
MSK Imaging Conference 07/22/2016 Eman Alqahtani, MD, MPH R3/PGY4 UCSD Radiology A 51 years old female with chronic thumb pain, and inability to actively flex the thumb interphalyngeal joint Possible trigger
The Elbow Scanning Protocol
 The Elbow Scanning Protocol Diagnostic Imaging of the Elbow: Introduction The elbow maybe considered as consisting of four quadrants, anterior, medial, lateral and posterior. Ultrasound would normally
The Elbow Scanning Protocol Diagnostic Imaging of the Elbow: Introduction The elbow maybe considered as consisting of four quadrants, anterior, medial, lateral and posterior. Ultrasound would normally
Medial Collateral Instability of the Elbow. CSES Residents Course Calgary AB February 1-3, 2017 WD Regan MD
 Medial Collateral Instability of the Elbow CSES Residents Course Calgary AB February 1-3, 2017 WD Regan MD Disclosures I have no disclosures to report Anatomy Medial Collateral Ligament Anterior Oblique
Medial Collateral Instability of the Elbow CSES Residents Course Calgary AB February 1-3, 2017 WD Regan MD Disclosures I have no disclosures to report Anatomy Medial Collateral Ligament Anterior Oblique
Modified anconeus muscle transfer as treatment of failed surgical release of lateral epicondylitis of the elbow
 310 Acta Orthop. Belg., 2017, t. luyckx, 83, 310-314 a. decramer, l. luyckx, j. noyez ORIGINAL STUDY Modified anconeus muscle transfer as treatment of failed surgical release of lateral epicondylitis of
310 Acta Orthop. Belg., 2017, t. luyckx, 83, 310-314 a. decramer, l. luyckx, j. noyez ORIGINAL STUDY Modified anconeus muscle transfer as treatment of failed surgical release of lateral epicondylitis of
Official Definition. Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist.
 Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
