CIC Edizioni Internazionali. J oints. Assessment of bone defects in anterior shoulder instability
|
|
|
- Quentin Garrison
- 5 years ago
- Views:
Transcription
1 J oints Review article Assessment of bone defects in anterior shoulder instability Paolo Baudi, Gabriele Campochiaro, Manuela Rebuzzi, Giovanni Matino, Fabio Catani Struttura complessa di Ortopedia e Traumatologia, Dipartimento Patologia Apparato Locomotore, Azienda ospedaliero-universitaria, Policlinico di Modena Summary Glenohumeral bone defects are a common finding in shoulder instability and they are strongly correlated with recurrence of dislocation and failure following arthroscopic Bankart repair. Most authors agree that open surgery should be considered in the presence of certain conditions: glenoid bone loss > 25%, a lesion involving > 30% of the humeral head, an engaging Hill- Sachs lesion, bipolar bone lesions even without engagement. A careful imaging evaluation must therefore be performed in order to identify, quantify and characterize the bone defects. Even though magnetic resonance has important additional value in the assessment of the glenoid labrum and rotator cuff, computed tomography scan is the examination of choice for studying bone defects. Several methods have been proposed to quantify the extent of the glenoid bone defect; the most accurate Corresponding author Dr. Paolo Baudi Orthopedics and Traumatology Unit, Department of Locomotor System Disorders, University Hospital of Modena Via del Pozzo, Modena baudi.paolo@policlinico.mo.it ones utilize two-dimensional computed tomography images with multiplanar reconstructions (PICO method) or more sophisticated three-dimensional reconstruction software. Conversely, the literature lacks studies that accurately quantify humeral bone defects and, above all, that demonstrate definitively the clinical and prognostic significance of the lesion location and size. Key Words: bone defect, glenoid, Hill-Sachs, imaging, shoulder instability, PICO. Introduction The glenohumeral joint is the joint most prone to traumatic dislocations (1). Static stabilizers (glenoid labrum, capsule and glenohumeral ligaments) and dynamic stabilizers (rotator cuff and long head of the biceps) work together to ensure the maintenance of the stability of this joint (2, 3). Disruption of this complex balance underlies the onset of recurrent shoulder instability. Glenohumeral bone defects are regarded as one of the main causes of recurrence of instability (4, 5). Numerous clinical (6, 7) and biomechanical (7-10) studies have highlighted the role of these defects in recurrent episodes of dislocation and instability after surgical treatment, showing how they cause changes in the contact forces on the joints and reduce their resistance to dislocation. 40
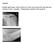
2 Assessment of bone defects in anterior shoulder instability A B C Figure 1. A: Inverted pear glenoid bone defect. B: CT image of a 3 o clock-to-6 o clock defect (corresponding to 20-25% bone loss). C: Arthroscopic view of an inverted pear lesion. Avulsion of the glenoid labrum and inferior glenohumeral ligament complex (Bankart lesion) is the lesion most commonly encountered after a first episode of anterior glenohumeral dislocation (11, 12). In between 5% and 55% of cases it is accompanied by detachment of a bone fragment (bony Bankart lesion) (13, 14). Isolated glenoid defects are found in 22% of patients with first-time anterior dislocation and in up to 73% of subjects with chronic instability (11, 16). Impaction fractures of the humeral head (Hill-Sachs lesions), caused by compressive forces that develop between the proximal humeral epiphysis and the anteroinferior margin of the glenoid in anterior dislocation, are a further factor predisposing to chronic instability. Up to 89% of patients with recurrent shoulder dislocation show glenohumeral bone loss (16, 17) and a clinically relevant correlation has been found between frequency of recurrence and the area of the missing glenoid (18). Sometimes the location of the lesions is more important than their size, as demonstrated in recent biomechanical studies (19). The clinical workup and history, performed in order to identify general risk factors (age, sex, generalized ligamentous laxity, sporting activities, and work), and type of instability, must be followed by a careful imaging assessment. The literature shows that in addition to standard radiographic views, two-dimensional (2D) and three-dimensional (3D) computed tomography (CT) and magnetic resonance imaging (MRI) are fundamental for detecting the site and measuring the size of bone defects, both glenoid and humeral (17, 20). Recognizing and precisely evaluating the degree of bone loss in the pre-operative stage seems to be crucial in order to plan an appropriate treatment and reduce the risk of recurrence. Glenoid bone defects Many authors have highlighted the relationship between glenoid bone loss and recurrence of instability after surgical repair. Rowe (21) reported recurrence rates ranging from 6 to 62% in the presence of an anterior bone defect, while Burkhart and De Beer (4) found recurrence rates of 67% in patients with significant glenoid bone defects ( inverted pear glenoid) versus 4% in those without such bone defects (Fig. 1). Tauber et al. (14) found bone loss in 57% of 41 patients re-operated on for recurrence of instability. It thus seems crucial to be able to identify the presence of glenoid bone loss, establish its location, study its morphology, and quantify its extent. Indeed, this is necessary because patients with glenoid bone loss in the range of 15% to 25% undergoing arthroscopic stabilization surgery show a high rate of recurrence at medium- and long-term follow-up. Given the demonstrated clinical importance of bone defects, all patients who are candidates for stabilization treatments should be carefully assessed for the presence of bone loss, particularly those presenting the most important risk factors, namely: many previous dislocations, a young age at first dislocation, and a long clinical history of instability (22). 41
3 P. Baudi, et al. Glenoid bone defects mainly involve the anterior rim of the glenoid (23, 24), and may be characterized morphologically by erosion (attritional bone loss) or fracture (8, 23, 25-27). Bigliani et al. (28) coined the term bony Bankart lesion to indicate the presence of an anteroinferior bone fragment, and classified anterior rim bone lesions into three types: type 1, displaced bone fragment with inferior glenohumeral ligament clearly recognizable; type 2, poorly consolidated bone fragment and unrecognizable ligamentous connections; type 3, bone defect corresponding to < 25% (type 3- A) or > 25% (type 3-B) of the total glenoid surface (indeed, they established 25% glenoid bone loss as the main risk factor for failure of Bankart repair). Edwards et al. (29), studying 160 unstable shoulders, found osseous lesions in 90% and, after plain radiographs including anteroposterior (AP) and Bernageau views, classified the patterns of glenoid bone defects into three main groups: those in which the bone fragment is still visible (bony Bankart lesion) (Fig. 2); those with loss of the anteroinferior angle and with the bone fragment no longer visible (cliff sign); those characterized by bone loss with compression and rounding of the glenoid rim (blunted angle). Sugaya et al. (27), in a series of 100 unstable shoulders, found a bony Bankart lesion in 50%, bone loss in 40% and normal glenoid morphology in just 10%. There is no unanimous consensus on what method should be used to calculate a glenoid bone defect, or on what to consider the threshold value for defining a lesion as severe, or at risk of recurrence. Bigliani et al. (28) suggested that the Bankart procedure should not be performed in the presence of a glenoid defect width >25%. Itoi et al. (7), in a biomechanical study, A Figure 2. Bony Bankart lesion. A: Axial 2D CT image. B: Coronal 3D CT image. B found 21% to be a critical value, even though limitations of this study are the fact that the defect was artificially created and the authors considered only anteroinferior defects and not exclusively anterior ones. Many authors agree that, in terms of bone loss, the critical limit beyond which there is a clinically significant risk of recurrence after surgical repair (Bankart procedure) without bone grafting is between 20% and 25% of the total glenoid surface (4, 7, 9, 30, 31). However, the real problem is not identifying the glenoid defect (this is now considered a relatively simple procedure, using true AP, Bernageau and West-Point views), but quantifying the bone loss or size of the fragment. The true AP and Bernageau views can show the lesion as a loss of continuity of the anteroinferior profile of the glenoid, with a sensitivity of 66% and a specificity of 100% (18); however, these views have a major limitation, in that they do not provide reliable indications on the real size of the bone defect. The West Point modified axillary view has shown a high correlation with CT in estimating glenoid bone loss (32). Burkhart et al. (33) proposed an arthroscopic measurement based on the glenoid bare spot, i.e. the central area of the glenoid where the cartilage is absent or thinnest. The bare spot is considered to be the central point of the glenoid, from which using an arthroscopic probe, it is possible to measure the anterior or posterior glenoid radius. However, this method can be used only intra-operatively and therefore has no useful role to play in the preoperative planning stage; furthermore, anatomical studies have shown inter-individual variability in the position of the bare spot (34). MRI is the gold standard method for examining the rotator cuff; conversely, it shows less sensitivity and specificity (in the ranges % and 66-95%, respectively) in detecting lesions of the glenoid labrum. MR arthrography, for the capsuloligamentous, labral and cartilaginous structures, showed sensitivity and specificity values of 86%-91% and 86%- 98%, respectively (35). However, in order to quantify the glenoid defect on MR arthrography it is necessary to obtain a perfect sagittal image (en face view) of the glenoid. MR arthrography is, in any case, more sensitive and specific in the presence of attritional bone loss than Bankart bony lesions. Recent studies (20, 26) have demonstrated the validity of MR arthrography in estimating glenoid bone defects in patients with chronic instabil- 42
4 Assessment of bone defects in anterior shoulder instability dius, R, centered on the lower two-thirds of the affected glenoid. A distance, d, is calculated between the center of the circle and the anterior edge of the bone lesion. The percentage of bone loss is identified using a function that takes into account the d/r ratio. Baudi et al. (40) developed a simple CT method for identifying and precisely evaluating the extent of the glenoid bone defects. The advantages of their technique, called PICO, derive from the fact that it combines simple 2D CT examination with subsequent MPR, and thus eliminates the need for 3D processing and dedicated software, yet can still be used to obtain 3D reconstructions. Standard images are processed in MPR in order to obtain an en face view of the glenoid. A circle with a horizontal diameter (from 3 o clock to 9 o clock) is drawn on the inferior part of the healthy glenoid,, and the circle area is measured in mm 2 using commonly available software. The circle is then transferred to the contralateral glenoid and the area of bone loss outlined. The bone defect is quantified in mm 2 and as a percentage (Fig. 4). A study performed using the PICO method on 115 patients with recurrent anterior shoulder dislocation showed glenoid loss in 65% of cases and a Hill-Sachs lesion in 80% (41). The glenoid bone leity of the shoulder, also in comparison with 2D and 3D CT. However, a series of factors limit the applicability of this technique: its high costs, relative invasiveness, general contraindications (presence of pacemakers, cochlear implants, ferromagnetic implants, etc.) and also the various complications that can arise (allergic reactions, infections, pain on injection of the contrast medium). CT scanning is currently the method of choice for studying glenoid bone defects (9, 23-25, 27) (Fig. 3). Recurrent dislocations, a strongly positive apprehension test at minimum degrees of abduction, bone defects shown on plain radiographs, and the need for surgical stabilization are the main indications for performing a CT study (36). A study by De Wilde et al. was the first to confirm the pathological changes on whose basis various methods of measuring glenoid bone loss on CT or MRI studies were developed (37). In a cadaveric study, these authors, examining 98 scapulae, identified 11 reproducible anatomical points that can be used to trace a perfect circle including the inferior part of the glenoid. On this basis, Sugaya et al. (27) developed a method, based on the processing of 3D CT images of the glenoid (with the humeral head eliminated), for identifying and calculating glenoid bone loss, which they expressed as a percentage of the articular surface. CT scans of both the patient s shoulders are acquired; a circle with a horizontal diameter (from 3 o clock to 9 o clock) is drawn on the normal glenoid, following its lower edge; then, using dedicated CT software, the area of the inferior part of the normal glenoid is calculated. The procedure is then repeated on the unstable shoulder, tracing, on the glenoid, the circle of the normal (i.e. contralateral) glenoid and the area of bone loss is outlined. A limitation of this method is the need to have dedicated software (38). Griffith et al. (23) described a method for calculating glenoid defects, based on CT images with multiplanar reconstruction (MPR); they calculated the maximum width of the affected glenoid and compared it with that of the contralateral glenoid. Chuang et al. (9) developed a similar method using 3D CT images; these authors considered a glenoid index defined as the ratio between the diameter of the deficient glenoid and that of the healthy contralateral one. Instead, Barchilon et al. (39) proposed a method based on the tracing, on 3D CT en face images, a circle with a ra- Figure 3. Bony Bankart lesion. 3D CT image (en face view). 43
5 P. Baudi, et al. Figure 4. Quantification of glenoid bone loss using the PICO method on en face 2D CT image of the glenoid with MPR. sions observed could be categorized into three main types. The first is the classic Bankart bony lesion. The second type, called the straight pear (Fig. 5) lesion, is determined by anterior glenoid bone loss, often as a result of compressive injuries, such as those caused by impaction of the humeral head against the anterior edge of the glenoid; lesions of this kind, found in 55%-65% of cases, are characterized by glenoid bone loss of between 5% and 15%, identifiable by drawing a straight line between 2 o clock and 5 o clock (25, 41). The third type of lesion, resulting from more severe injury, is bone loss >20%, identifiable by drawing an oblique line between 3 o clock and 6 o clock; this type of lesion is found in between 5% and 10% of cases (25, 41). Various studies have documented the validity of this method (42). Magarelli et al. (43) applied it to 40 patients and confirmed its excellent reproducibility. In a recent study, the same authors (17) showed high agreement (97%) between 2D and 3D CT measurements for identifying the presence, size and type of glenoid bone defects in anterior glenohumeral instability, and claimed that the two measurements can be considered interchangeable. Finally, Bois et al. (16) studied the accuracy of the Glenoid Index (9), Ratio method (39) and PICO method (40) and concluded that 2D reconstruction is not recommended for these methods; on 3D CT, they found the PICO method to be the one that most accurately quantified bone loss, both anterior and anteroinferior, and thus recommended its wider use. Humeral bone defects The Hill-Sachs lesion, named after the authors who described it in 1940, is a fracture of the posterior-superior aspect of the humeral head, which is caused by impaction of the latter against the glenoid rim during anterior dislocation. In the rare event of posterior dislocation, a similar lesion is formed, in the same way, but on the anterior aspect of the head of the humerus (reverse Hill-Sachs lesion). In the decision-making process in cases of recurrent anterior shoulder instability, humeral bone defects have always tended to be considered less important than glenoid ones, even though the authors who first described the Hill-Sachs lesion found it to be present in 74% of recurrent dislocations (44). The prevalence of this lesion reported in the literature is highly variable, with values ranging from 38 to 93%, depending on the diagnostic instruments used and the sample observed. Bushnell et al. (45) reported a frequency of 70% in first-time dislocations and % in recurrences. Hill-Sachs lesions can be identified using plain radiography, MRI, MR-arthrography and CT. The radiographic views that can highlight a Hill-Sachs lesion are: AP in maximum internal rotation and another more specific view called the Stryker notch view. Plain radiographs often underestimate humeral bone loss and are still considered inadequate for quantifying it (46). MRI is the technique that, thanks to the altered signal intensity of the injured (cancellous) bone compared with the intact humeral bone, detects Hill-Sachs lesions with the greatest reproducibility (47), and it shows high sensitivity (97%). However, MRI can underestimate bone loss (36). Furthermore, MRI can give false-positive results: erosions or small grooves can be mistaken for Hill-Sachs lesions, as can the bare area: this area is in fact visible as a small cartilage-free area on the posterolateral aspect of the humeral head and it is a normal finding; Hill-Sachs lesions, on the other hand, are located, on average, 0-24 mm from the top of the humeral head in a posterosuperior position (48). The gold standard for identifying and quantifying humeral bone defects is CT, especially with 3D reconstructions (46) (Fig. 6). The first method for quantifying Hill-Sachs lesions dates back to 1959: the defect was calculated on plain radiographs as the percentage of lesion involvement in a 180 arc on the surface of the humeral head (49). 44
6 Assessment of bone defects in anterior shoulder instability Even though this method has its limits, given that it calculates the extent of the damage in only one plane and lacks prognostic value, is still widely used and can be quickly and easily applied to CT and MRI studies. It was used in 1984 by Rowe et al. (21), who also took into account the depth of the lesions. They calculated two dimensions (depth and length) of the lesions and correlated these results with clinical severity. This allowed them to grade the lesions as mild (<0.5cm deep and < 2cm long), moderate (0.5-1cm deep and 2-4cm long) and severe (>1cm deep and >4cm long). Flatow et al. (50) suggested quantifying the humeral bone loss as a percentage of involvement of the humeral head, classifying defects in three categories: <20%, 20-40% and >40%. Lesions >40% are clinically significant. Montgomery et al. (51) specified this method further: A the lesion should be calculated on axial and coronal CT images with measurements expressed as a percentage of the total area of the humeral head. Some authors have shown that not only the size, but also the location and orientation of Hill-Sachs lesions can have clinical and prognostic significance and introduced the concept of engagement of the glenoid and humeral head during movements at various degrees of abduction and external rotation (4, 46, 52, 53). Yamamoto et al. (19) used the term glenoid track to describe the zone of contact between the articular surfaces of the glenoid and humeral head during combined abduction and external rotation movements, and showed that there is a risk of engagement if the lesion extends beyond the medial margin of that zone. According to this theory, the depth and extent of the Figure 5. A: Straight pear glenoid bone defect. B: CT image of a 2 o clock-to-5 o clock defect (corresponding to 10-15% bone loss). C: Arthroscopic view of a straight pear lesion. A B B Figure 6. Hill-Sachs lesion on the posterior-superior aspect of the humeral head. A: Axial 2D CT image. B: Coronal 3D CT image. C: Sagittal 3D CT image. C C 45
7 P. Baudi, et al. Therefore, in recurrent shoulder instability, careful identification of the site and extent of a Hill-Sachs lesion is crucial in order to plan and to choose the appropriate treatment. Surgical repair of a Hill-Sachs lesion may be indicated in the presence of a defect that is > 25% of the volume of the humeral head, or when there is engagement. It may also be indicated in young people who play collision sports and in cases of recurrence following a previous Bankart repair in patients with humeral bone loss. The following, on the other hand, are contraindications to the procedure: signs of osteoarthritis, avascular necrosis, advanced age (relative), rotator cuff tear associated with functional limitation (46). An isolated Hill-Sachs lesion equal to or less than 25% of the humeral head should never be treated surgically if the Bankart lesion is well repaired. However, the presence of concomitant glenoid bone loss or rotator cuff damage needs to be carefully looked for in order to avoid failures (6, 46, 54). For many years, the Hill-Sachs lesion was considered less important than glenoid bone loss, with the result that surgical repair techniques were performed simply to obtain joint stability, with little attention paid to the achievement of anatomical recovery and the restoration of joint congruity; this approach resulted in early onset of arthritic changes, decreased range of motion and a high number of failures. In 1984, Weber et al. (59) described, for the first time, a technique involving rotational humeral osteotomy of the proximal diaphyseal segment to prevent recurrent instability. In 1972, Connolly (60) introduced the remplissage technique, which was subsequently developed arthroscopically (61), in the form of a technique that involves transferring the infraspinatus and possibly the posterior capsule into the defect in such a way that the Hill-Sachs lesion becomes an extra-articular lesion. This solution guarantees full recovery of stability at the expense of a slight reduction in external rotation (55, 62). Various authors agree that treatment with remplissage is indicated when the defect involves more that 25% of the humeral head, and should be associated with anterior capsulolabral reconstruction (55, 63). For an engaging Hill-Sachs lesion or a lesion involving > 30% of the humeral head associated with > 20% glenoid bone loss, authors recommend surgical autololesion, while contributing to the risk of recurrent shoulder instability, are less important than its location. The authors noted that the medial margin of the glenoid track was located 18.4 ± 2.5 mm medial from the footprint of the rotator cuff, a distance equivalent to 84% ± 14% of the glenoid width (19). Engaging Hill-Sachs lesions are the ones with the worst prognosis, carrying a 100% risk of recurrence of instability (4). In addition to this type of lesion, there are a great amount of Hill-Sachs lesions, of different dimensions and locations, that do not give rise to engagement but are just as severe, in terms of prognosis, as the engaging type, so much so that many authors have sought to establish the existence of a critical lesion size, albeit they failed to document this. However, 25% bone loss has been recognized as a critical threshold beyond which surgery should be recommended, given that biomechanical studies and instrumental-clinical-arthroscopic correlations have shown this volume of humeral bone loss to lead to biomechanical alterations capable of inducing instability (36, 46, 54-56). Other authors have instead linked the risk of recurrent dislocations to the extent of bone loss calculated in relation to the glenoid, claiming that humeral bone loss greater than 21% of the superiorinferior length of the glenoid or 25% of its depth will result in instability (52). It is important to point out that in the presence of a Hill-Sachs lesion it is essential to look for glenoid bone loss, given its remarkably high frequency in these cases (up to 100%). It is fundamentally important to diagnose this association, known as a bipolar injury (36, 57), because in the presence of glenoid bone loss the glenoid track area shrinks and the medial margin draws closer to the footprint, thus increasing the risk of engagement even for apparently innocuous lesions. Other authors have also studied the morphology of humeral bone loss, looking for correlations with clinical history. It has been shown that the volume of bone loss increases with increasing numbers of dislocations, but that its depth reduces, indicating more severe instability; conversely, the defect appears deeper in cases of acute dislocation following a high-energy trauma, repeated attempts at reduction of the dislocation under anesthesia, and in cases of chronic dislocation (53, 58). The mean depth of the lesion in cases of dislocation is 3.9 ± 0.9 mm, as opposed to 2.1 ± 1 mm in subluxation episodes (53). 46
8 Assessment of bone defects in anterior shoulder instability gous graft or allograft reconstruction, fixed with miniscrews (10, 36, 56). In the presence of humeral head defects involving more than 40% of the articular surface, most authors recommend the implantation of shoulder resurfacing prostheses, albeit after very careful patient selection (46, 64). References 1. Kazar B, Relovszky E. Prognosis of primary dislocation of the shoulder. Acta Orthop Scand 1969, 40: Chen AL, Hunt SA, Hawkins RJ, et al. Management of bone loss associated with recurrent anterior glenohumeral instability. Am J Sports Med 2005, 33: Rowe CR, Patel D, Southmayd WW. The Bankart procedure: a long-term end-result study. J Bone Joint Surg 1978, 60: Burkhart SS, De Beer JF. Traumatic glenohumeral bone defect and their relationship to failure of arthroscopic Bankart repairs: significance of the inverted-pear glenoid and the humeral engaging Hill-Sachs lesion. Arthroscopy 2000, 16: Greis PE, Scuderi MG, Mohr A, et al. Glenohumeral articolar contact areas and pressures following labral and osseus injury to the anteroinferior quadrant of the glenoid. J Shoulder Elbow Surg 2002, 11: Boileau P, Villalba M, Hery JY, et al. Risk factors for recurrence of shoulder instability after arthroscopic Bankart repair. J Bone Joint Surg 2006, 88A: Itoi E, Lee SB, Berglund LJ, Berge LL, et al. The effect of a glenoid defect on anteroinferior stability of the shoulder after Bankart repair: a cadaveric study. J Bone Joint Surg 2000, 82A: Burkhart SS, Danaceau SM. Articular arc length mismatch as a cause of failed Bankart repair. Arthroscopy 2000, 16: Chuang TY, Adams CR, Burkhart SS. Use preoperative threedimensional computer tomography to quantify glenoid bone loss in shoulder instability. Arthroscopy 2008, 24: Lynch JR, Clinton JM, Dewing CB, et al. Treatment of osseous defects associated with anterior shoulder instability. J Shoulder Elbow Surg 2009, 18: Taylor DC, Arciero RA. Pathologic changes associated with shoulder dislocations. Arthroscopic and physical examination findings in first-time, traumatic anterior dislocations. Am J Sports Med 1997, 25: Thomas SC, Matsen 3rd FA. An approach to the repair of avulsion of the glenohumeral ligaments in the management of traumatic anterior glenohumeral instability. J Bone Joint Surg 1989, 71A: Fujii Y, Yoneda M, Wakitani S, et al. Histologic analysis of Bony Bankart lesions in recurrent anterior instability of the shoulder. J Shoulder Elbow Surg 2006, 15: Tauber M, Resch H, Forstner R, et al. Reasons for failure after surgical repair of anterior shoulder instability. J Shoulder Elbow Surg 2004, 13: Calandra JJ, Baker CL, Uribe J. The incidence of Hill-Sachs lesions in initial anterior shoulder dislocations. Arthroscopy 1989, 5: Bois AJ, Fening SD, Polster J, et al. Quantifying glenoid bone loss in anterior shoulder instability: reliability and accuracy of 2-dimensional and 3-dimensional computed tomography measurement techniques. Am J Sports Med 2012, 40: Magarelli N, Milano G, Baudi P, et al. Comparison between 2D and 3D computed tomography evaluation of glenoid bone defect in unilateral anterior gleno-humeral instability. Radiol Med 2012, 117: Gerber C, Nyffeler RW. Classification of glenohumeral joint instability. Clin Orthop Relat Res 2002, 400: Yamamoto N, Itoi E, Abe H, et al. Contact between the glenoid and the humeral head in abduction, external rotation, and horizontal extension: a new concept of glenoid track. J Should Elbow Surg 2007, 16: Owens BD, Burns TC, Campbell SE, et al. Simple method of glenoid bone loss calculation using ipsilateral magnetic resonance imaging. Am J Sports Med 2013, 41: Rowe CR, Zarins B, Ciullo JV. Recurrent anterior dislocation of the shoulder after surgical repair. Apparent causes of failure and treatment 1984, 66A: Milano G, Grasso A, Russo A, et al. Analysis of risk factor for glenoid bone defect in anterior shoulder instability. Am J Sports Med 2011, 39: Griffith JF, Antonio GE, Tong CWC, et al. Anterior shoulder dislocation: quantification of glenoid bone loss with CT. AJR Am J Roentgenol 2003, 180: Saito H, Itoi E, Sugaya H, et al. Location of the glenoid defect in shoulders with recurrent anterior dislocation. Am J Sports Med 2005, 33: Griffith JF, Antonio GE, Yung PS, et al. Prevalence, pattern, and spectrum of glenoid bone loss in anterior shoulder dislocation: CT analysis of 218 patients. AJR Am J Roentgenol 2008, 190: Huijsmans PE, Haen PS, Kidd M, et al. Quantification of a glenoid defect with three-dimensional computed tomography and magnetic resonance imaging: a cadaveric study. J Shoulder Elbow Surg 2007, 16: Sugaya H, Moriishi J, Dohi M, et al. Glenoid rim morphology in recurrent anterior glenohumeral instability. J Bone Joint Surg 2003, 85A: Bigliani LU, Newton PM, Steinmann SP, et al. Glenoid rim lesions associated with recurrent anterior dislocation of the shoulder. Am J Sports Med 1998, 26: Edwards TB, Boulahia A, Walch G. Radiographic analysis of bone defects in chronic anterior shoulder instability. Arthroscopy 2003, 19: Lo IK, Parten PM, Burkhart SS. The inverted pear glenoid: an indicator of significant glenoid bone loss. Arthroscopy 2004, 20: Yamamoto N, Muraki T, Sperling JW, et al. Stabilizing mechanism in bone-grafting of a large glenoid defect. J Bone Joint Surg 2010, 92A: Itoi E, Lee SB, Amrami KK, et al. Quantitative assessment of classic anteroinferior bony Bankart lesions by radiography and computed tomography. Am J Sports Med 2003, 31: Burkhart SS, De Beer JF, Tehrany AM, et al. Quantifying glenoid bone loss arthroscopically in shoulder instability. Arthroscopy 2002, 18:
9 P. Baudi, et al. 34. Aigner F, Longato S, Fritsch H, et al. Anatomical considerations regarding the bare spot of the glenoid cavity. Surg Radiol Anat 2004, 26: Steinbach LS. MRI of shoulder instability. Eur J Radiol 2008, 68: Bollier MJ, Arciero R. Management of glenoid and humeral bone loss. Sports Med Arthrosc Rev 2010, 18: De Wilde LF, Berghs BM, Audenaert E, et al. About the variability of the shape of the glenoid cavity. Surg Radiolog Anat 2004, 26: Nofsinger C, Browning B, Burkhart SS, et al. Objective preoperative measurement of anterior glenoid bone loss: a pilot study of a computer-based method using unilateral 3-dimensional computed tomography. Arthroscopy 2011, 27: Barchilon VS, Kotz E, Barchilon Ben-Av M, et al. A simple method for quantitative evaluation of the missing area of the anterior glenoid in anterior instability of the glenohumeral joint. Skeletal Radiol 2008, 37: Baudi P, Righi P, Bolognesi D, et al. How to identify and calculate glenoid bone deficit. Chir Organi Mov 2005, 90: Baudi P. How to manage bone defects in shoulder instability. Instructional Course Lecture, 13th ESSKA Meeting D Elia G, Di Giacomo A. Quantification of traumatic anterior gleno-humeral bone loss by spiral CT. Radiol Med 2008, 113: Magarelli N, Milano G, Sergio P, et al. Intra-observer and interobserver reliability of the Pico computed tomography method for quantification of glenoid bone defect in anterior shoulder instability. Skeletal Radiol 2009, 38: Hill HA, Sachs MD. The grooved defect of the humeral head. A frequently unrecognised complication of dislocation of the shoulder joint. Radiology 1940, 35: Bushnell BD, Creighton RA, Herring MM. Bony instability of the shoulder. Arthroscopy 2008, 24: Sekiya JK, Cutuk A. Humeral head defects - biomechanics, measurements, and treatments. In: Provencher MT, Romeo AA (Eds), Shoulder instability: a comprehensive approach. Elsevier Saunders, Philadelphia 2012, pp Workman TL, Burkhard TK, Resnick D, et al. Hill-Sachs lesion: comparison of detection with MR imaging, radiography, and arthroscopy. Radiology 1992, 185: Saito H, Itoi E, Minagawa H. Location of the Hill-Sachs lesion in shoulders with recurrent anterior dislocation. Arch Orthop Trauma Surg 2009, 129: Hall RH, Isaac F, Booth CR. Dislocations of the shoulder with special reference to accompanying small fractures. J Bone Joint Surg 1959, 41A: Flatow EL, Miniaci A, Evans PJ, et al. Instability of the shoulder: complex problems and failed repairs: Part II. Failed repairs. AAOS Instr Course Lect 1998, 47: Montgomery WH Jr, Wahl M, Hettrich C, et al. Anteroinferior bone-grafting can restore stability in osseous glenoid defects. J Bone Joint Surg 2005, 87A: Bhatia S, McGill K, Ghodarda NS, et al. Radiographic and arthroscopic evaluation of glenoid and humeral head bone loss. In: Provencher MT, Romeo AA (Eds), Shoulder instability: a comprehensive approach. Elsevier Saunders, Philadelphia 2012, pp Ito H, Takayama A, Shirai Y. Radiographic evaluation of the Hill- Sachs lesion in patients with recurrent anterior shoulder instability. J Shoulder Elbow Surg 2000, 9: Burkhart SS, De Beer JF, Barth JR, et al. Results of modified Latarjet reconstruction in patients with anteroinferior instability and significant bone loss. Arthroscopy l 2007, 23: Elkinson I, Giles JW, Faber KJ, et al. The Effect of the Remplissage Procedure on Shoulder Stability and Range of Motion. An in Vitro Biomechanical Assessment. J Bone Joint Surg 2012, 94A: Miniaci A, Berlet G. Recurrent anterior instability following failed surgical repair: Allograft reconstruction of large humeral head defects. J Bone Joint Surg 2001, 83B (Suppl 1): Widjaja AB, Tran A, Bailey M, et al. Correlation between Bankart and Hill-Sachs lesions in anterior shoulder dislocation. ANZ J Surg 2006, 76: Cetik O, Uslu M, Ozsar BK. The relationship between Hill- Sachs lesion and recurrent anterior shoulder dislocation. Acta Orthop Belg 2007, 73: Weber BG, Simpson LA, Hardegger F. Rotational humeral osteotomy for recurrent anterior dislocation of the shoulder associated with a large Hill-Sachs lesion. J Bone Joint Surg 1984, 66A: Connolly J. Humeral head defects associated with shoulder dislocation: their diagnostic and surgical significance. AAOS Instr Course Lect 1972, 21: Purchase RJ, Wolf EM, Hobgood ER, et al. Hill-Sachs remplissage : an arthroscopic solution for the engaging Hill-Sachs lesion. Arthroscopy 2008, 24: Itoi E, Yamamoto N, Kurokawa D, et al. Bone loss in anterior instability. Curr Rev Musculoskelet Med 2013, 6: Boileau P, O Shea K, Vargas P, et al. Anatomical and Functional Results After Arthroscopic Hill-Sachs Remplissage. J Bone Joint Surg 2012, 94A: Pritchett JW, Clark JM. Prosthetic replacement for chronic unreduced dislocations of the shoulder. Clin Orthop Relat Res 1987, 216:
Glenoid Track Concept vs Humeral Head Engagement in Recurrent Anterior Shoulder Instability with Glenoid Bone Loss Less Than 25%
 Med. J. Cairo Univ., Vol. 85, No. 6, September: 2407-2412, 2017 www.medicaljournalofcairouniversity.net Glenoid Track Concept vs Humeral Head Engagement in Recurrent Anterior Shoulder Instability with
Med. J. Cairo Univ., Vol. 85, No. 6, September: 2407-2412, 2017 www.medicaljournalofcairouniversity.net Glenoid Track Concept vs Humeral Head Engagement in Recurrent Anterior Shoulder Instability with
The Bony Bankart Lesion: How to Measure the Glenoid Bone Loss
 Signature: Pol J Radiol, 2017; 82: 58-63 DOI: 10.12659/PJR.898566 REVIEW ARTICLE Received: 2016.03.17 Accepted: 2016.06.16 Published: 2017.02.04 Authors Contribution: A Study Design B Data Collection C
Signature: Pol J Radiol, 2017; 82: 58-63 DOI: 10.12659/PJR.898566 REVIEW ARTICLE Received: 2016.03.17 Accepted: 2016.06.16 Published: 2017.02.04 Authors Contribution: A Study Design B Data Collection C
It is generally accepted that anteroinferior glenoid
 Level V Evidence With Video Illustration Evolving Concept of Bipolar Bone Loss and the Hill-Sachs Lesion: From Engaging/Non-Engaging Lesion to On-Track/Off-Track Lesion Giovanni Di Giacomo, M.D., Eiji
Level V Evidence With Video Illustration Evolving Concept of Bipolar Bone Loss and the Hill-Sachs Lesion: From Engaging/Non-Engaging Lesion to On-Track/Off-Track Lesion Giovanni Di Giacomo, M.D., Eiji
Recurrence after arthroscopic Bankart repair: Is quantitative radiological analysis of bone loss of any predictive value?
 Orthopaedics & Traumatology: Surgery & Research (2012) 98, 514 519 Available online at www.sciencedirect.com ORIGINAL ARTICLE Recurrence after arthroscopic Bankart repair: Is quantitative radiological
Orthopaedics & Traumatology: Surgery & Research (2012) 98, 514 519 Available online at www.sciencedirect.com ORIGINAL ARTICLE Recurrence after arthroscopic Bankart repair: Is quantitative radiological
Patient ID. Case Conference. Physical Examination. Image examination. Treatment 2011/6/16
 Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Three dimensional modeling and parameter analysis of glenohumeral joint: a method to decide the operative treatment of shoulder instability
 Original Article Page 1 of 7 Three dimensional modeling and parameter analysis of glenohumeral joint: a method to decide the operative treatment of shoulder instability Guang-Wen Yu 1, Young Lae Moon 2,
Original Article Page 1 of 7 Three dimensional modeling and parameter analysis of glenohumeral joint: a method to decide the operative treatment of shoulder instability Guang-Wen Yu 1, Young Lae Moon 2,
Assessment of bone loss in anterior shoulder instability
 Review Article Page 1 of 9 Assessment of bone loss in anterior shoulder instability Cory A. Kwong, Eva M. Gusnowski, Kelvin K. W. Tam, Ian K. Y. Lo Section of Orthopedic Surgery, Department of Surgery,
Review Article Page 1 of 9 Assessment of bone loss in anterior shoulder instability Cory A. Kwong, Eva M. Gusnowski, Kelvin K. W. Tam, Ian K. Y. Lo Section of Orthopedic Surgery, Department of Surgery,
3-D CT is the Most Reliable Imaging Modality When Quantifying Glenoid Bone Loss
 Clin Orthop Relat Res (2013) 471:1251 1256 DOI 10.1007/s11999-012-2607-x Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH 3-D CT
Clin Orthop Relat Res (2013) 471:1251 1256 DOI 10.1007/s11999-012-2607-x Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH 3-D CT
Engaging Hill-Sachs Lesion: Is There an Association Between This Lesion and Findings on MRI?
 Musculoskeletal Imaging Original Research Gyftopoulos et al. MRI of Hill-Sachs Lesions Musculoskeletal Imaging Original Research Soterios Gyftopoulos 1 Avner Yemin Luis Beltran James Babb Jenny Bencardino
Musculoskeletal Imaging Original Research Gyftopoulos et al. MRI of Hill-Sachs Lesions Musculoskeletal Imaging Original Research Soterios Gyftopoulos 1 Avner Yemin Luis Beltran James Babb Jenny Bencardino
MRI Evaluation of Bipolar Bone Loss Using the On-Track Off-Track Method: A Feasibility Study
 Musculoskeletal Imaging Original Research Gyftopoulos et al. MRI of Bipolar Bone Loss Musculoskeletal Imaging Original Research Soterios Gyftopoulos 1 Luis S. Beltran 1 Jared Bookman 2 Andrew Rokito 3
Musculoskeletal Imaging Original Research Gyftopoulos et al. MRI of Bipolar Bone Loss Musculoskeletal Imaging Original Research Soterios Gyftopoulos 1 Luis S. Beltran 1 Jared Bookman 2 Andrew Rokito 3
Study of bipolar bone defects in unstable shoulder: From "engaging / non-engaging" to "on-track / off-track".
 Study of bipolar bone defects in unstable shoulder: From "engaging / non-engaging" to "on-track / off-track". Poster No.: C-2219 Congress: ECR 2017 Type: Educational Exhibit Authors: E. Jose Salgado Ribeiro,
Study of bipolar bone defects in unstable shoulder: From "engaging / non-engaging" to "on-track / off-track". Poster No.: C-2219 Congress: ECR 2017 Type: Educational Exhibit Authors: E. Jose Salgado Ribeiro,
Imaging methods for quantifying glenoid and Hill-Sachs bone loss in traumatic instability of the shoulder: a scoping review
 Saliken et al. BMC Musculoskeletal Disorders (2015) 16:164 DOI 10.1186/s12891-015-0607-1 RESEARCH ARTICLE Imaging methods for quantifying glenoid and Hill-Sachs bone loss in traumatic instability of the
Saliken et al. BMC Musculoskeletal Disorders (2015) 16:164 DOI 10.1186/s12891-015-0607-1 RESEARCH ARTICLE Imaging methods for quantifying glenoid and Hill-Sachs bone loss in traumatic instability of the
Measurement of Glenoid Bone Loss
 Measurement of Glenoid Bone Loss A Comparison of Measurement Error Between 45 and 0 Bone Loss Models and With Different Posterior Arthroscopy Portal Locations Matthew T. Provencher,* MD, LCDR, MC, USNR,
Measurement of Glenoid Bone Loss A Comparison of Measurement Error Between 45 and 0 Bone Loss Models and With Different Posterior Arthroscopy Portal Locations Matthew T. Provencher,* MD, LCDR, MC, USNR,
Disclosures. Bipolar Lesions 1/8/16. Technical Pearls for Shoulder Surgery: Tips for the Latarjet Procedure. The Sling Effect of the Conjoined Tendon
 Disclosures Technical Pearls for Shoulder Surgery: Tips for the Latarjet Procedure Stephen S. Burkhart, MD San Antonio, Texas Stephen S. Burkhart, MD The following relationships with commercial interests
Disclosures Technical Pearls for Shoulder Surgery: Tips for the Latarjet Procedure Stephen S. Burkhart, MD San Antonio, Texas Stephen S. Burkhart, MD The following relationships with commercial interests
Case Report Arthroscopic Bony Bankart Repair Using Double-Threaded Headless Screw: A Case Report
 Case Reports in Orthopedics Volume 2012, Article ID 789418, 4 pages doi:10.1155/2012/789418 Case Report Arthroscopic Bony Bankart Repair Using Double-Threaded Headless Screw: A Case Report Takeshi Kokubu,
Case Reports in Orthopedics Volume 2012, Article ID 789418, 4 pages doi:10.1155/2012/789418 Case Report Arthroscopic Bony Bankart Repair Using Double-Threaded Headless Screw: A Case Report Takeshi Kokubu,
HAGL lesion of the shoulder
 HAGL lesion of the shoulder A 24 year old rugby player presented to an orthopaedic surgeon with a history of dislocation of the left shoulder. It reduced spontaneously and again later during the same match.
HAGL lesion of the shoulder A 24 year old rugby player presented to an orthopaedic surgeon with a history of dislocation of the left shoulder. It reduced spontaneously and again later during the same match.
MRI of Shoulder Instabilities
 MRI of Shoulder Instabilities Anna Hirschmann, MD Musculoskeletal Division Clinic of Radiology and Nuclear Medicine University of Basel Hospital Glenohumeral Articulation Centering of the humeral head
MRI of Shoulder Instabilities Anna Hirschmann, MD Musculoskeletal Division Clinic of Radiology and Nuclear Medicine University of Basel Hospital Glenohumeral Articulation Centering of the humeral head
Musculoskeletal Applications for CT. Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine
 Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
My Disclosures. Engaging Hill- Sachs. Engaging Hill- Sachs. Non Engaging Hill-Sachs. Non Engaging Hill-Sachs 5/8/2014
 3-D Modeling of Humeral Head Defects: Jaicharan J. Iyengar, MD May 8, 2014 35 th Annual Inman Lectureship My Disclosures 1. Financial - None 2. Scientific - Peer Reviewer, Journal of Shoulder and Elbow
3-D Modeling of Humeral Head Defects: Jaicharan J. Iyengar, MD May 8, 2014 35 th Annual Inman Lectureship My Disclosures 1. Financial - None 2. Scientific - Peer Reviewer, Journal of Shoulder and Elbow
Repair of an Anteroinferior Glenoid Defect by the Latarjet Procedure: Quantitative Assessment of the Repair by Computed Tomography
 Repair of an Anteroinferior Glenoid Defect by the Latarjet Procedure: Quantitative Assessment of the Repair by Computed Tomography Michael E. Hantes, M.D., Aaron Venouziou, M.D., Konstantinos A. Bargiotas,
Repair of an Anteroinferior Glenoid Defect by the Latarjet Procedure: Quantitative Assessment of the Repair by Computed Tomography Michael E. Hantes, M.D., Aaron Venouziou, M.D., Konstantinos A. Bargiotas,
Glenohumeral Joint Instability. Static Stabilizers of the GHJ. Static Stabilizers of the GHJ. Static Stabilizers of the GHJ
 1 Glenohumeral Joint Instability GHJ Joint Stability: Or Lack Thereof! Christine B. Chung, M.D. Assistant Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Static Stabilizers
1 Glenohumeral Joint Instability GHJ Joint Stability: Or Lack Thereof! Christine B. Chung, M.D. Assistant Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Static Stabilizers
Shoulder Instability and Reconstruction of Bone Defects
 Shoulder Instability and Reconstruction of Bone Defects Anthony Miniaci MD FRCSC Professor of Surgery Cleveland Clinic Foundation Cleveland, Ohio USA Shoulder Instability Surgery Many Questions Open vs.arthroscopic
Shoulder Instability and Reconstruction of Bone Defects Anthony Miniaci MD FRCSC Professor of Surgery Cleveland Clinic Foundation Cleveland, Ohio USA Shoulder Instability Surgery Many Questions Open vs.arthroscopic
Hill-Sachs Lesion on MR Arthrography of the Shoulder: Relationship with Bankart Lesion on Arthroscopy and Frequency of Shoulder Dislocations
 www.ksmrm.org JKSMRM 17(1) : 26-32, 2013 Print ISSN 1226-9751 Original Article Hill-Sachs Lesion on MR Arthrography of the Shoulder: Relationship with Bankart Lesion on Arthroscopy and Frequency of Shoulder
www.ksmrm.org JKSMRM 17(1) : 26-32, 2013 Print ISSN 1226-9751 Original Article Hill-Sachs Lesion on MR Arthrography of the Shoulder: Relationship with Bankart Lesion on Arthroscopy and Frequency of Shoulder
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abduction pillow, ultrasling, 880, 881, 882, 883 Adolescents, shoulder instability in. See Shoulder, instability of, pediatric and adolescent.
Index Note: Page numbers of article titles are in boldface type. A Abduction pillow, ultrasling, 880, 881, 882, 883 Adolescents, shoulder instability in. See Shoulder, instability of, pediatric and adolescent.
Anterior shoulder instability: Evaluation using MR arthrography.
 Anterior shoulder instability: Evaluation using MR arthrography. Poster No.: C-2407 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Lord, I. Katsimilis, N. Purohit, V. T. Skiadas; Southampton/UK
Anterior shoulder instability: Evaluation using MR arthrography. Poster No.: C-2407 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Lord, I. Katsimilis, N. Purohit, V. T. Skiadas; Southampton/UK
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
The suction cup mechanism is enhanced by the slightly negative intra articular pressure within the joint.
 SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
The Reduction in Stability From Combined Humeral Head and Glenoid Bony Defects Is Influenced by Arm Position
 The Reduction in Stability From Combined Humeral Head and Glenoid Bony Defects Is Influenced by Arm Position Piyush Walia,* yz DEng, Ronak M. Patel, MD, Lionel Gottschalk, z MD, Matthew Kuklis, z MS, Morgan
The Reduction in Stability From Combined Humeral Head and Glenoid Bony Defects Is Influenced by Arm Position Piyush Walia,* yz DEng, Ronak M. Patel, MD, Lionel Gottschalk, z MD, Matthew Kuklis, z MS, Morgan
Shoulder Arthroscopy. Dr. J.J.A.M. van Raaij. NOV Jaarvergadering Den Bosch 25 jan 2018
 Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum
 Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum By Matthew T. Provencher, MD, LCDR, MC, USNR; Anthony A. Romeo, MD; Daniel J. Solomon, MD, CDR, MC, USN; Bernard R. Bach, Jr.,
Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum By Matthew T. Provencher, MD, LCDR, MC, USNR; Anthony A. Romeo, MD; Daniel J. Solomon, MD, CDR, MC, USN; Bernard R. Bach, Jr.,
The bony conformity of the glenoid and humeral head articular surfaces
 CONTINUING MEDICAL EDUCATION FORMATION MÉDICALE CONTINUE CASE SERIES Combined large Hill Sachs and bony Bankart lesions treated by Latarjet and partial humeral head resurfacing: a report of 2 cases Philippe
CONTINUING MEDICAL EDUCATION FORMATION MÉDICALE CONTINUE CASE SERIES Combined large Hill Sachs and bony Bankart lesions treated by Latarjet and partial humeral head resurfacing: a report of 2 cases Philippe
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM
 RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
Avulsion fracture of the coracoid process in a patient with chronic anterior shoulder instability treated with the Latarjet procedure: a case report
 Schneider et al. Journal of Medical Case Reports 2014, 8:394 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Avulsion fracture of the coracoid process in a patient with chronic anterior shoulder
Schneider et al. Journal of Medical Case Reports 2014, 8:394 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Avulsion fracture of the coracoid process in a patient with chronic anterior shoulder
Management of Humeral Bone Loss in Anterior Shoulder Instability. Scott D. Mair, MD University of Kentucky Sports Medicine
 Management of Humeral Bone Loss in Anterior Shoulder Instability Scott D. Mair, MD University of Kentucky Sports Medicine Disclosure Smith and Nephew Endoscopy fellowship support Importance Bone loss (glenoid
Management of Humeral Bone Loss in Anterior Shoulder Instability Scott D. Mair, MD University of Kentucky Sports Medicine Disclosure Smith and Nephew Endoscopy fellowship support Importance Bone loss (glenoid
Assessment of Approximate Glenoid Size in Thai People
 Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 January 19, 2012 John W. Hinchey, MD Dept of Orthopaedic Surgery Shoulder & Elbow Service This live activity is designated for a maximum of 1 AMA PRA Category 1 Credit tm. Physicians should claim only
January 19, 2012 John W. Hinchey, MD Dept of Orthopaedic Surgery Shoulder & Elbow Service This live activity is designated for a maximum of 1 AMA PRA Category 1 Credit tm. Physicians should claim only
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai
 POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
Page 1. Shoulder Injuries in Sports.
 www.schulterteam.ch Shoulder Injuries in Sports Matthias A Zumstein Shoulder, Elbow and Orthopaedic Sports Medicine Department of Orthopedic Surgery and Traumatology University of Berne, Switzerland matthias.zumstein@insel.ch
www.schulterteam.ch Shoulder Injuries in Sports Matthias A Zumstein Shoulder, Elbow and Orthopaedic Sports Medicine Department of Orthopedic Surgery and Traumatology University of Berne, Switzerland matthias.zumstein@insel.ch
Shoulder Instability Disclosures
 Bony Deficiency and the Latarjet Procedure Detroit, MI July 13, 2017 Shariff K. Bishai, D.O., M.S., FAOAO Associated Orthopedists of Detroit, PC Sports Medicine, Shoulder Surgery and Hip Arthroscopy Assistant
Bony Deficiency and the Latarjet Procedure Detroit, MI July 13, 2017 Shariff K. Bishai, D.O., M.S., FAOAO Associated Orthopedists of Detroit, PC Sports Medicine, Shoulder Surgery and Hip Arthroscopy Assistant
Glenohumeral Joint Instability: An Athlete s Perspective
 Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
Management of Anterior Shoulder Instability
 Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
The Management of Shoulder Instability. By Debbie Prince Clinical Shoulder Specialist
 The Management of Shoulder Instability By Debbie Prince Clinical Shoulder Specialist Shoulder Dislocation The most common joint dislocation Traumatic Instability, highest incidence in males aged 21 to
The Management of Shoulder Instability By Debbie Prince Clinical Shoulder Specialist Shoulder Dislocation The most common joint dislocation Traumatic Instability, highest incidence in males aged 21 to
Shoulder Instability
 J F de Beer, K van Rooyen, D Bhatia Shoulder Instability INSTABILITY means that the shoulder dislocates completely (dislocation) or partially (subluxation). Anatomy The shoulder consists of a ball (humeral
J F de Beer, K van Rooyen, D Bhatia Shoulder Instability INSTABILITY means that the shoulder dislocates completely (dislocation) or partially (subluxation). Anatomy The shoulder consists of a ball (humeral
MRI SHOULDER WHAT TO SEE
 MRI SHOULDER WHAT TO SEE DR SHEKHAR SRIVASTAV Sr. Consultant- Knee & Shoulder Arthroscopy Sant Parmanand Hospital Normal Anatomy Normal Shoulder MRI Coronal Oblique Sagital Oblique Axial Cuts Normal Coronal
MRI SHOULDER WHAT TO SEE DR SHEKHAR SRIVASTAV Sr. Consultant- Knee & Shoulder Arthroscopy Sant Parmanand Hospital Normal Anatomy Normal Shoulder MRI Coronal Oblique Sagital Oblique Axial Cuts Normal Coronal
Level of Evidence: Therapeutic Level IV. See Instructions to Authors for a complete description of levels of evidence.
 1752 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Arthroscopic Osseous Bankart Repair for Chronic Recurrent Traumatic Anterior Glenohumeral Instability BY HIROYUKI SUGAYA, MD,
1752 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Arthroscopic Osseous Bankart Repair for Chronic Recurrent Traumatic Anterior Glenohumeral Instability BY HIROYUKI SUGAYA, MD,
Types of shoulder Dislocation: Shoulder dislocation. 1. Anterior 2. Posterior 3. Luxatio erecta (inferior dislocation)
 Types of shoulder Dislocation: Shoulder dislocation 1. Anterior 2. Posterior 3. Luxatio erecta (inferior dislocation) Anterior Dislocation: head is dislocated anterior to the glenoid Most common among
Types of shoulder Dislocation: Shoulder dislocation 1. Anterior 2. Posterior 3. Luxatio erecta (inferior dislocation) Anterior Dislocation: head is dislocated anterior to the glenoid Most common among
Arthroscopic Bankart repair has become the standard of care
 TECHNIQUE Bipolar Fixation : A Novel Concept in the Treatment of Recurrent Anterior Shoulder Instability A Prospective Study of 26 Cases With Minimum 2-year Follow-Up Jean Kany, MD, MS,* Biju Pankappilly,
TECHNIQUE Bipolar Fixation : A Novel Concept in the Treatment of Recurrent Anterior Shoulder Instability A Prospective Study of 26 Cases With Minimum 2-year Follow-Up Jean Kany, MD, MS,* Biju Pankappilly,
Strategies for Failed Instability Repair
 Strategies for Failed Instability Repair Robert E Hunter MD Director, Orthopedic Sports Medicine Center HRRMC Salida, Colorado CU Sports Medicine Course Sept 28, 2012 Conflict of Interest Paid Consultant:
Strategies for Failed Instability Repair Robert E Hunter MD Director, Orthopedic Sports Medicine Center HRRMC Salida, Colorado CU Sports Medicine Course Sept 28, 2012 Conflict of Interest Paid Consultant:
Management of bone loss in shoulder instability
 Volume 05 / Issue 01 / March 2017 boa.ac.uk Page 50 JTO Subspecialty Section Management of bone loss in shoulder instability Chu-Hao Chiang Co-Authors: Abhinav Gulihar & Nicholas Little Management Management
Volume 05 / Issue 01 / March 2017 boa.ac.uk Page 50 JTO Subspecialty Section Management of bone loss in shoulder instability Chu-Hao Chiang Co-Authors: Abhinav Gulihar & Nicholas Little Management Management
Glenohumeral instability is a relatively common
 Bulletin of the NYU Hospital for Joint Diseases 2010;68(4):245-50 245 Management of Humeral and Glenoid Bone Loss Associated with Glenohumeral Instability Results with Anatomical Bone Grafting Matthew
Bulletin of the NYU Hospital for Joint Diseases 2010;68(4):245-50 245 Management of Humeral and Glenoid Bone Loss Associated with Glenohumeral Instability Results with Anatomical Bone Grafting Matthew
P V S MEMORIAL HOSPITAL LTD.
 SHOULDER XRAYS Instability Series o True AP (Grashey s) o Axillary o Stryker Notch view o True AP in Internal rotation o Scapular Y view o West Point view for Bony Bankart ( looks like modif axillary view)
SHOULDER XRAYS Instability Series o True AP (Grashey s) o Axillary o Stryker Notch view o True AP in Internal rotation o Scapular Y view o West Point view for Bony Bankart ( looks like modif axillary view)
A new method to evaluate glenoid erosion in instable shoulder
 Ikemoto et al. International Archives of Medicine 2013, 6:42 ORIGINAL RESEARCH Open Access A new method to evaluate glenoid erosion in instable shoulder Roberto Y Ikemoto 1*, Joel Murachovsky 1, Luis G
Ikemoto et al. International Archives of Medicine 2013, 6:42 ORIGINAL RESEARCH Open Access A new method to evaluate glenoid erosion in instable shoulder Roberto Y Ikemoto 1*, Joel Murachovsky 1, Luis G
 This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
"Stability and Instability of RTSA"
 Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
MRI of the Shoulder What to look for and how to find it? Dr. Eric Handley Musculoskeletal Radiologist Cherry Creek Imaging
 MRI of the Shoulder What to look for and how to find it? Dr. Eric Handley Musculoskeletal Radiologist Cherry Creek Imaging MRI of the Shoulder Benefits of Ultrasound: * Dynamic * Interactive real time
MRI of the Shoulder What to look for and how to find it? Dr. Eric Handley Musculoskeletal Radiologist Cherry Creek Imaging MRI of the Shoulder Benefits of Ultrasound: * Dynamic * Interactive real time
Risk factors for shoulder re-dislocation after arthroscopic Bankart repair
 Shibata et al. Journal of Orthopaedic Surgery and Research 2014, 9:53 RESEARCH ARTICLE Open Access Risk factors for shoulder re-dislocation after arthroscopic Bankart repair Hideaki Shibata 1, Masafumi
Shibata et al. Journal of Orthopaedic Surgery and Research 2014, 9:53 RESEARCH ARTICLE Open Access Risk factors for shoulder re-dislocation after arthroscopic Bankart repair Hideaki Shibata 1, Masafumi
Disclosure. Traumatic Anterior Shoulder Instability 7/23/2018. Orthopaedics for the Primary Care Practitioner & Rehabilitation Therapist
 Orthopaedics for the Primary Care Practitioner & Rehabilitation Therapist Christopher E. Baker M.D. Sports Medicine Shoulder Reconstruction Traumatic Anterior Shoulder Instability Disclosure Speaking/Consulting
Orthopaedics for the Primary Care Practitioner & Rehabilitation Therapist Christopher E. Baker M.D. Sports Medicine Shoulder Reconstruction Traumatic Anterior Shoulder Instability Disclosure Speaking/Consulting
Partial Resurfacing for Humeral Head Defects Associated With Recurrent Shoulder Instability
 Partial Resurfacing for Humeral Head Defects Associated With Recurrent Shoulder Instability MATTHEW C. BESSETTE, MD; NICHOLAS C. FRISCH, MD; PRADEEP KODALI, MD; MORGAN H. JONES, MD; ANTHONY MINIACI, MD,
Partial Resurfacing for Humeral Head Defects Associated With Recurrent Shoulder Instability MATTHEW C. BESSETTE, MD; NICHOLAS C. FRISCH, MD; PRADEEP KODALI, MD; MORGAN H. JONES, MD; ANTHONY MINIACI, MD,
Introduction & Question 1
 Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Case 61. Middle aged farmer with a history of trivial injury and since then pain and stiffness in the L shoulder. Inflammatory markers were negative.
 Case 61 Middle aged farmer with a history of trivial injury and since then pain and stiffness in the L shoulder. Inflammatory markers were negative. Diagnosis GLENOID DYSPLASIA DEFINITION The classic constellation
Case 61 Middle aged farmer with a history of trivial injury and since then pain and stiffness in the L shoulder. Inflammatory markers were negative. Diagnosis GLENOID DYSPLASIA DEFINITION The classic constellation
Sports Medicine: Shoulder Arthrography. Christine B. Chung, M.D. Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System
 Sports Medicine: Shoulder Arthrography Christine B. Chung, M.D. Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Disclosure Off-label use for gadolinium Pediatric Sports Injuries
Sports Medicine: Shoulder Arthrography Christine B. Chung, M.D. Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Disclosure Off-label use for gadolinium Pediatric Sports Injuries
Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?)
 Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?) Thomas J. Gill Chief, MGH Sports Medicine Dept. of Orthopedic Surgery Massachusetts General Hospital Boston, MA Look, just do
Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?) Thomas J. Gill Chief, MGH Sports Medicine Dept. of Orthopedic Surgery Massachusetts General Hospital Boston, MA Look, just do
Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty
 J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
Osteochondral augmentation of glenoid bone loss distal tibia allograft
 Review Article Page 1 of 9 Osteochondral augmentation of glenoid bone loss distal tibia allograft Colin P. Murphy 1, Anthony Sanchez 1, Mitchell I. Kennedy 1, Rachel M. Frank 2, Matthew T. Provencher 1,3
Review Article Page 1 of 9 Osteochondral augmentation of glenoid bone loss distal tibia allograft Colin P. Murphy 1, Anthony Sanchez 1, Mitchell I. Kennedy 1, Rachel M. Frank 2, Matthew T. Provencher 1,3
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
First-Time Anterior Shoulder Dislocation: Is it time to take a stand?
 Evaluation and Treatment of the Injured Athlete Martha s Vineyard July 22nd, 2018 First-Time Anterior Shoulder Dislocation: Is it time to take a stand? Robert A. Arciero, MD Professor, Orthopaedics University
Evaluation and Treatment of the Injured Athlete Martha s Vineyard July 22nd, 2018 First-Time Anterior Shoulder Dislocation: Is it time to take a stand? Robert A. Arciero, MD Professor, Orthopaedics University
International Archives of Medicine 2013, 6:42
 International Archives of Medicine This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. A new method
International Archives of Medicine This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. A new method
CT Findings of Traumatic Posterior Hip Dislocation after Reduction 1
 CT Findings of Traumatic Posterior Hip Dislocation after Reduction 1 Sung Kyoung Moon, M.D., Ji Seon Park, M.D., Wook Jin, M.D. 2, Kyung Nam Ryu, M.D. Purpose: To evaluate the CT images of reduced hips
CT Findings of Traumatic Posterior Hip Dislocation after Reduction 1 Sung Kyoung Moon, M.D., Ji Seon Park, M.D., Wook Jin, M.D. 2, Kyung Nam Ryu, M.D. Purpose: To evaluate the CT images of reduced hips
Acute traumatic posterior shoulder instability is
 Arthroscopic Treatment of a Reverse Hill-Sachs Lesion Richard E. Duey, M.D., and Stephen S. Burkhart, M.D. Abstract: Acute traumatic posterior shoulder instability is a rare injury. Such injuries can result
Arthroscopic Treatment of a Reverse Hill-Sachs Lesion Richard E. Duey, M.D., and Stephen S. Burkhart, M.D. Abstract: Acute traumatic posterior shoulder instability is a rare injury. Such injuries can result
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
APPROPRIATE USE GUIDELINES
 APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Shoulder Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Compiled by Rob Liddell,
APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Shoulder Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Compiled by Rob Liddell,
Learning Curve of Arthroscopic Anatomic Glenoid Reconstruction: Comparison to the Arthroscopic Bristow Latarjet
 Learning Curve of Arthroscopic Anatomic Glenoid Reconstruction: Comparison to the Arthroscopic Bristow Latarjet Iustin Moga MD George Konstantinidis MD, PhD Cathy Coady MD, FRCS(C) Ivan Wong MD, FRCS(C)
Learning Curve of Arthroscopic Anatomic Glenoid Reconstruction: Comparison to the Arthroscopic Bristow Latarjet Iustin Moga MD George Konstantinidis MD, PhD Cathy Coady MD, FRCS(C) Ivan Wong MD, FRCS(C)
Hugo C. van der Veen James P. M. Collins Paul C. Rijk
 DOI 10.1007/s00402-011-1423-1 ARTHROSCOPY AND SPORTS MEDICINE Value of magnetic resonance arthrography in post-traumatic anterior shoulder instability prior to arthroscopy: a prospective evaluation of
DOI 10.1007/s00402-011-1423-1 ARTHROSCOPY AND SPORTS MEDICINE Value of magnetic resonance arthrography in post-traumatic anterior shoulder instability prior to arthroscopy: a prospective evaluation of
Shoulder Arthroscopy Portals
 Shoulder Arthroscopy Portals Alper Deveci and Metin Dogan 7 7.1 Bony Landmarks Before starting shoulder arthroscopy, the patient must be positioned and draping applied. Then the bony landmarks are identified
Shoulder Arthroscopy Portals Alper Deveci and Metin Dogan 7 7.1 Bony Landmarks Before starting shoulder arthroscopy, the patient must be positioned and draping applied. Then the bony landmarks are identified
Glenoid Bone Loss: The Truth
 Sports Medicine & Joint Center Funabashi Orthopaedic Hospital Glenoid Bone Loss: The Truth Hiroyuki Sugaya, MD Disclosure Speakers bureau/paid presentations DepuySynthes; Smith&Nephew Unpaid consultant
Sports Medicine & Joint Center Funabashi Orthopaedic Hospital Glenoid Bone Loss: The Truth Hiroyuki Sugaya, MD Disclosure Speakers bureau/paid presentations DepuySynthes; Smith&Nephew Unpaid consultant
Stability of the glenohumeral joint requires
 Review Article Glenoid Bone Deficiency in Recurrent Anterior Shoulder Instability: Diagnosis and Management Dana P. Piasecki, MD Nikhil N. Verma, MD Anthony A. Romeo, MD William N. Levine, MD Bernard R.
Review Article Glenoid Bone Deficiency in Recurrent Anterior Shoulder Instability: Diagnosis and Management Dana P. Piasecki, MD Nikhil N. Verma, MD Anthony A. Romeo, MD William N. Levine, MD Bernard R.
Anatomy GH Joint. Glenohumeral Instability. Components of Stability. Components of Stability 7/7/2017. AllinaHealthSystem
 Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX Tel#
 Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D.
 Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
Double bucket handle tears of the superior labrum
 Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Dislocation of the Shoulder Joint Radiographic Analysis of Osseous Abnormalities
 Vande Berg, B and Omoumi, P 2016 Dislocation of the Shoulder Joint Radiographic Analysis of Osseous Abnormalities. Journal of the Belgian Society of Radiology, 100(1): 89, pp. 1 10, DOI: http://dx.doi.org/10.5334/jbr-btr.1210
Vande Berg, B and Omoumi, P 2016 Dislocation of the Shoulder Joint Radiographic Analysis of Osseous Abnormalities. Journal of the Belgian Society of Radiology, 100(1): 89, pp. 1 10, DOI: http://dx.doi.org/10.5334/jbr-btr.1210
MR Imaging for Glenohumeral Instability & Bone Loss
 MR Imaging for Glenohumeral Instability & Bone Loss Russell C. Fritz, M.D. San Francisco, CA I have no conflicts of interest to disclose Russell C. Fritz, M.D. MR imaging is a powerful diagnostic tool
MR Imaging for Glenohumeral Instability & Bone Loss Russell C. Fritz, M.D. San Francisco, CA I have no conflicts of interest to disclose Russell C. Fritz, M.D. MR imaging is a powerful diagnostic tool
The glenohumeral joint s remarkable stability is maintained
 vol. 3 no. 5 SPORTS HEALTH [ Orthopaedic Surgery ] The Importance of the Recognition and Treatment of Glenoid Bone Loss in an Athletic Population Sanjeev Bhatia, MD, Neil S. Ghodadra, MD, Anthony A. Romeo,
vol. 3 no. 5 SPORTS HEALTH [ Orthopaedic Surgery ] The Importance of the Recognition and Treatment of Glenoid Bone Loss in an Athletic Population Sanjeev Bhatia, MD, Neil S. Ghodadra, MD, Anthony A. Romeo,
Arthroscopic Findings After Traumatic Shoulder Instability in Patients Older Than 35 Years
 Arthroscopic Findings After Traumatic Shoulder Instability in Patients Older Than 35 Years Elisabeth C. Robinson,* MD, Vijay B. Thangamani, MD, Michael A. Kuhn, MD, and Glen Ross, MD Investigation performed
Arthroscopic Findings After Traumatic Shoulder Instability in Patients Older Than 35 Years Elisabeth C. Robinson,* MD, Vijay B. Thangamani, MD, Michael A. Kuhn, MD, and Glen Ross, MD Investigation performed
Outcome analysis of management of recurrent shoulder dislocation by latarjet procedure
 2018; 4(3): 82-86 ISSN: 2395-1958 IJOS 2018; 4(3): 82-86 2018 IJOS www.orthopaper.com Received: 17-05-2018 Accepted: 18-06-2018 Dr. AN Sarath Babu Senior Assistant Professor, Institute of Orthopaedics
2018; 4(3): 82-86 ISSN: 2395-1958 IJOS 2018; 4(3): 82-86 2018 IJOS www.orthopaper.com Received: 17-05-2018 Accepted: 18-06-2018 Dr. AN Sarath Babu Senior Assistant Professor, Institute of Orthopaedics
OBJECTIVES. Therapists Management of Shoulder Instability SHOULDER STABILITY SHOULDER STABILITY WHAT IS SHOULDER INSTABILITY? SHOULDER INSTABILITY
 Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Coordinated interaction between static, dynamic, and
 REVIEW ARTICLE Matthew J. Bollier, MD* and Robert Arciero, MDw Abstract: Glenoid and humeral head bone deficiency is a common reason for recurrent anterior shoulder instability and failure of capsulolabral
REVIEW ARTICLE Matthew J. Bollier, MD* and Robert Arciero, MDw Abstract: Glenoid and humeral head bone deficiency is a common reason for recurrent anterior shoulder instability and failure of capsulolabral
Impact of Sagittal Rotation on Axial Glenoid Width Measurement in the Setting of Glenoid Bone Loss
 Impact of Sagittal Rotation on Axial Glenoid Width Measurement in the Setting of Glenoid Bone Loss Publish date: June 5, 2018 Authors: Rachel M. Frank, MD Petar Golijanin, BS Bryan G. Vopat, MD Daniel
Impact of Sagittal Rotation on Axial Glenoid Width Measurement in the Setting of Glenoid Bone Loss Publish date: June 5, 2018 Authors: Rachel M. Frank, MD Petar Golijanin, BS Bryan G. Vopat, MD Daniel
Shoulder Instability in the Contact Athlete - I do it arthroscopically Brian J. Cole, MD, MBA
 Shoulder Instability in the Contact Athlete - I do it arthroscopically Brian J. Cole, MD, MBA bcole@rushortho.com Key points: o Greater incidence of anterior shoulder instability in contact and collision
Shoulder Instability in the Contact Athlete - I do it arthroscopically Brian J. Cole, MD, MBA bcole@rushortho.com Key points: o Greater incidence of anterior shoulder instability in contact and collision
Treatment of Primary Anterior Shoulder Dislocation: Conflicting Study Outcomes. Prof. C. Milgrom Hadassah University Hospital Jerusalem, Israel
 Treatment of Primary Anterior Shoulder Dislocation: Conflicting Study Outcomes Prof. C. Milgrom Hadassah University Hospital Jerusalem, Israel I. Natural history of shoulder dislocation and traditional
Treatment of Primary Anterior Shoulder Dislocation: Conflicting Study Outcomes Prof. C. Milgrom Hadassah University Hospital Jerusalem, Israel I. Natural history of shoulder dislocation and traditional
Common Surgical Shoulder Injury Repairs
 Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Acute Versus Delayed Magnetic Resonance Imaging and Associated Abnormalities in Traumatic Anterior Shoulder Dislocations
 Original Research Acute Versus Delayed Magnetic Resonance Imaging and Associated Abnormalities in Traumatic Anterior Shoulder Dislocations Nathan D. Orvets,* MD, Robert L. Parisien,* MD, Emily J. Curry,*
Original Research Acute Versus Delayed Magnetic Resonance Imaging and Associated Abnormalities in Traumatic Anterior Shoulder Dislocations Nathan D. Orvets,* MD, Robert L. Parisien,* MD, Emily J. Curry,*
By Dr. Girish V.Patil, Dr. Sanjeev I. Kolagi & Dr. Umesh Ramdurg DM-Wayanad Institute of Medical Sciences, India
 : H Orthopedic and Musculoskeletal System Volume 14 Issue 2 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online ISSN: 2249-4618
: H Orthopedic and Musculoskeletal System Volume 14 Issue 2 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online ISSN: 2249-4618
Diagnostic Accuracy of MRI in the Measurement of Glenoid Bone Loss
 Musculoskeletal Imaging Original Research Gyftopoulos et al. MRI of Glenoid one Loss Musculoskeletal Imaging Original Research Soterios Gyftopoulos 1 Saqib Hasan 2 Jenny encardino 1 Jason Mayo 1 Samir
Musculoskeletal Imaging Original Research Gyftopoulos et al. MRI of Glenoid one Loss Musculoskeletal Imaging Original Research Soterios Gyftopoulos 1 Saqib Hasan 2 Jenny encardino 1 Jason Mayo 1 Samir
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Biomechanical Comparison of the Latarjet Procedure with and without Capsular Repair
 Original Article Clinics in Orthopedic Surgery 2016;8:84-91 http://dx.doi.org/10.4055/cios.2016.8.1.84 Biomechanical Comparison of the Procedure with and without Capsular Repair Matthew T. Kleiner, MD,
Original Article Clinics in Orthopedic Surgery 2016;8:84-91 http://dx.doi.org/10.4055/cios.2016.8.1.84 Biomechanical Comparison of the Procedure with and without Capsular Repair Matthew T. Kleiner, MD,
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Atypical traumatic anterior shoulder instability with excessive joint laxity: recurrent shoulder subluxation without a history of dislocation
 Kim et al. Journal of Orthopaedic Surgery and Research (2018) 13:80 https://doi.org/10.1186/s13018-018-0791-4 RESEARCH ARTICLE Open Access Atypical traumatic anterior shoulder instability with excessive
Kim et al. Journal of Orthopaedic Surgery and Research (2018) 13:80 https://doi.org/10.1186/s13018-018-0791-4 RESEARCH ARTICLE Open Access Atypical traumatic anterior shoulder instability with excessive
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT
 SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
Diagnosis of Hill-Sachs Lesion of the Shoulder
 Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Diagnosis of Hill-Sachs Lesion of the Shoulder Luigi Pancione, G. Gatti & B. Mecozzi
Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Diagnosis of Hill-Sachs Lesion of the Shoulder Luigi Pancione, G. Gatti & B. Mecozzi
