Pattern of recovery following total shoulder arthroplasty and humeral head replacement
|
|
|
- Nelson Perkins
- 5 years ago
- Views:
Transcription
1 Razmjou et al. BMC Musculoskeletal Disorders 2014, 15:306 RESEARCH ARTICLE Pattern of recovery following total shoulder arthroplasty and humeral head replacement Helen Razmjou 1,2,3*, Paul Stratford 4,5, Deborah Kennedy 1,2,4 and Richard Holtby 1,6 Open Access Abstract Background: Understanding the pattern of recovery and expected rate of change after shoulder arthroplasty is helpful to clinicians and patients for setting realistic expectations and goals. The purpose of this study was to describe the pattern of recovery over a 2-year period for patients receiving either a Total Shoulder Arthroplasty (TSA) or Humeral Head Replacement (HHR). Methods: This was a secondary analysis of prospectively collected data of patients who had undergone TSA or HHR and were followed for up to 2 years. Patients were seen prior to surgery and at 6 months, one year and two years after surgery and completed the American Shoulder and Elbow Surgeon s (ASES) questionnaire, Relative Constant Murley score (RCMS) and underwent range of motion and strength assessment. Results: Data of 134 patients who had surgery from April 2001 to July 2011 were used for analysis. One hundred and eight patients underwent TSA (81%) and 26 (19%) had HHR. Both surgeries were associated with a statistically significant improvement in physical symptoms, ASES, RCMS, range of motion and strength (p <0.0001). The greatest change for all outcomes occurred within the first 6-months of surgery. Improvement in ASES, RCMS continued up to 12-months and then plateaued. Improvement in physical symptoms leveled off at 6-months in the HHR group but continued up to 12-months in the TSR group. Strength showed improvement in both groups up to 24-months post-surgery. Conclusion: Both TSA and HHR groups showed a statistically significant improvement in perceived disability, range of motion and strength over two years with the greatest improvement made by 6 months. The recovery profiles for the surgeries showed different patterns. Keywords: Total Shoulder Arthroplasty, Humeral Head Replacement, Disability recovery pattern Background Primary osteoarthritis of the glenohumeral joint is characterized by loss of the articular cartilage producing joint space narrowing, subchondral sclerosis and osteophyte formation. Surgical management is considered when conservative treatment such as rehabilitation, intra-articular corticosteroid injection, anti-inflammatory medication and analgesics fail to provide relief. Traditionally, Total Shoulder Arthroplasty (TSA) is the treatment of choice for primary and posttraumatic osteoarthritis and also some inflammatory conditions of * Correspondence: helen.razmjou@sunnybrook.ca 1 Holland Orthopaedic & Arthritic Centre, Sunnybrook Health Sciences Centre, 43 Wellesley Street East, Toronto, Ontario M1Y 1H1, Canada 2 Department of Physical Therapy, Faculty of Medicine, University of Toronto, Toronto, Canada Full list of author information is available at the end of the article the shoulder as long as the rotator cuff remains intact. Humeral Head Replacement (HHR) has also been utilized for primary osteoarthritis, but is more often indicated for patients with inflammatory arthritis with severe rotator cuff deficiency, cuff tear arthropathy, proximal humeral fractures, osteonecrosis of the humeral head with a preserved glenoid, or in the presence of insufficient glenoid bone stock [1]. The literature shows that the majority of patients improve significantly with respect to pain and range of motion following TSA [2,3]. The outcome of HHR seems to be less predictable [4-6] partly due to rotator cuff or glenoid bone deficiency. To eliminate the impact of cuff pathology or glenoid co-morbidity, a number of randomized clinical trials with homogenized samples (patients with primary osteoarthritis) have been conducted to better examine the difference in outcome of these two 2014 Razmjou et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Razmjou et al. BMC Musculoskeletal Disorders 2014, 15:306 Page 2 of 7 procedures [6,7]. These studies showed that total shoulder arthroplasty provided better functional outcomes than hemiarthroplasty for patients with primary osteoarthritis of the shoulder. Overall, the inferior outcome of HHR is known and partly justified due to more extensive pathology of the shoulder in this population. However, the limitation of the available research is lack of information on important time points which helps to predict when patients reach their maximal recovery as measured by patient reported measures of pain and disability or functional abilities including range of motion and strength. We are not aware of any studies that have determined the specific time point of maximal recovery following shoulder arthroplasty procedures. Understanding the pattern of change would help clinicians to communicate the expected results of surgery and time frame for reaching maximal recovery to their patients. It is also important that studies are controlled for sex and age as aging affects the overall function and females have shown less improvement after shoulder surgery related to rotator cuff pathology [8] and lower extremity arthroplasty [9-11]. The purpose of this study was to describe the pattern of recovery over a 2-year period for patients receiving either a Total Shoulder Arthroplasty (TSA) or Humeral Head Replacement (HHR). Methods This was a secondary analysis of prospectively collected data of patients with advanced osteoarthritis of the glenohumeral joint who had undergone TSA or HHR and had participated in previous formal studies and were followed up for up to 2 years. This study has adhered to the STROBE guidelines for observational studies and has received ethics approval from the Research Ethics Board of the Sunnybrook Health Sciences Centre. Subjects The inclusion criteria included age greater than 18 years, a diagnosis of advanced primary osteoarthritis or inflammatory arthritis with or without rotator cuff pathology that had not responded to conservative treatment. The exclusion criteria included inability to speak or read English, evidence of infection, underlying metabolic disease, avascular necrosis, or capsulorraphy arthropathy. Patients with primary osteoarthritis of the glenohumeral joint and an intact rotator cuff underwent TSA. Those with humeral fractures and a normal glenoid articular surface or with severe glenoid deficiency with or without cuff tear arthropathy received HHR. In addition, younger patients and those with significant medical co-morbidities underwent HHR, rather than reverse arthroplasty, as the reverse prosthesis may not be sufficiently durable in younger age group and may have higher complication rate in the presence of other medical conditions. All patients followed a standardized rehabilitation protocol. A sling was used for two weeks with immediate active assisted mobilization following surgery. Sub-maximal isometric exercises started at four weeks post-operatively. Active exercises started at 6 weeks in lying progressing to upright position at 7 weeks. Resistive exercises involving theraband started at 8-10 weeks. Exercises related to internal rotation followed the other directions of movement with a 4-week delay to avoid strain on subscapularis. Outcome measures Two patient-oriented outcome measures and a record of physical symptoms were obtained 2-3 weeks before surgery and on clinic visits at 6, 12, and 24 months after surgery. The outcome measures were the American Shoulder and Elbow Surgeon s (ASES) assessment form [12] and the Relative Constant Murley score (RCMS) [13]. The ASES is a 100-point scale, 50 points of which are derived from patient self-report of pain on a visual analog scale and 50 points of which are computed from a formula using the cumulative score of 10 activities of daily living derived using a four-point ordinal scale. The Constant Murley score is a combined measure, containing a patient reported component (35%) and the clinical assessment of range of motion and strength (65%). The absolute score is then converted to the relative score by accounting for age and sex-related differences. Higher scores on the ASES and RCMS indicate less disability. Both measures have established validity and reliability in patients with glenohumeral osteoarthritis [14,15]. Physical symptoms were measured by the physical symptoms domain of the Western Ontario Osteoarthritis Shoulder (WOOS) Index [16]. Symptoms captured pain with movement, nagging constant pain, weakness, stiffness, grinding and impact of weather changes on pain. The score of the physical symptoms domain varied from 0 as no pain to 600 as the maximal pain and discomfort. Performance measures included active range of motion (ROM) in 3 directions (flexion, abduction, external rotation in neutral, and hand behind back) and strength in scapular plane elevation. Strength was measured with a simple tensiometer with the shoulder at 90 degrees of elevation in the plane of the scapula and the elbow extended while the clinician pulled down on the tensiometer. The maximum painfree force that the patient could resist for 5 seconds as the examiner pulled down on the device was measured. In the case of pain while holding the position, strength was given ascoreofzero. Statistical analyses Descriptive analyses of patients characteristics and outcome measures summary scores were performed. This
3 Razmjou et al. BMC Musculoskeletal Disorders 2014, 15:306 Page 3 of 7 study applied a fixed occasion repeated measures design. We applied Generalized Estimating Equations (GEE) to test for differences in the surgical groups change trajectories for each outcome measure. GEE fit population averaged panel data models. Complete data for a given outcome measure at all time-points is not required for a patient to be included in the analysis. Dependent variables were the outcome measures assessed at multiple timepoints. The independent variables were surgical group (levels were TSA and HHR) and measurement occasion (levels were pre-surgery, 6, 12, 24-months); covariates were gender and age. All analyses were conducted using STATA version 13.0 (STATACorp, College Station, TX). Results Data of 149 patients were reviewed. Three patients died of causes not related to shoulder arthroplasty. Twelve patients (6 in the TSA and 6 in the HHR group) had missed two consecutive assessments, one being the 2 year follow-up, and were not included in the analysis. The baseline characteristics (age, physical symptoms, ASES, RCMS) of these 12 patients were not different than the remaining. Data of 134 patients (73 females (54%), 61 males (46%), mean age = 67 years, SD: 9) who had surgery from April 2001 to July 2011 were used for final analysis. One hundred and eight patients underwent TSA (81%) and 26 (19%) had HHR (Table 1). The diagnoses were primary osteoarthritis (96%) and inflammatory arthritis (4%) with intact rotator cuff in the TSA group. The Neer II prosthesis was used in 18 patients with 49 patients receiving the Bigliani-Flatow (BF) prosthesis and 41 receiving the Total Evolutive Shoulder System (TESS). Seventy percent (18) of the HHR group had primary osteoarthritis with deficient glenoid bone. Four patients had inflammatory arthritis (15%). There were Table 1 Baseline data for the Outcome Measures HHR TSR Variable N Mean SD N Mean SD ASES ACMS Pain* ADL* ROM* Strength* RCMS (%) PS Flex Abd Ext Rot *:Components of the Constant Murley score. : In Pounds. three humeral head fractures (11%) and one cuff tear arthropathy (4%). The patient with cuff tear arthropathy was an 80 year old female who had undergone a rotator cuff repair five year previously and was not a good candidate for reverse arthroplasty due to other medical comorbidities. The majority of the patients in the HHR group received the BF prosthesis (22, 73%) with three TESS prostheses and one Dupuy Global CTA Advantage system. Patients in the TSA group were not different than patients in the HHR group with respect to age, sex, or mechanism of injury (p > 0.05). Table 2 provides a summary of the outcome measure mean values for the TSA and HHR groups for each assessment occasion. All outcome measures reflected large and statistically significant improvements at 2 years. Figure 1 and Figure 2 display the TSA and HHR change profiles for the RCMS and ASES respectively. The greatest change for all outcomes occurred within the first 6-months of surgery. Improvement continued up to 12- months and then plateaued in all measures except physical symptoms, external rotation and strength which showed a different pattern. Figure 3 displays the TSA and HHR change profiles for the physical symptoms. For patients receiving TSA, improvement occurred up to 12- months and then plateaued. For patients receiving HHR, improvement leveled off at 6-months and slightly declined thereafter. Figure 4 shows the change profile for strength which shows improvement in both groups up to 24-months post-surgery. Discussion In the present study, we found that both TSA and HHR groups improved in their physical symptoms, disability level and range of motion over time. However, the HHR group reported overall higher disability as measured by the ASES, RCMS, and symptoms. As apparent in the figures, different patterns of recovery were observed in these measures. Recovery of external rotation was similar between groups. Improvement of external rotation in both groups may be related to change in biomechanics of the replaced joint regardless of type of procedure. It has been shown that an anatomical reconstruction of the humeral head can restore the physiological motions and limited eccentric loading of the glenoid, which may explain more improvement in external rotation than elevation [17]. Although the rate of change was different between HHR and TSA, the most significant recovery of disability, physical symptoms and range of motion was made by 6 months. In terms of the ASES and RCMS outcome measure scores and range of motion, recovery continued to 12 months and then began to plateau. This was also the case for the TSA group with respect to the change profile for the physical symptoms. In contrast, physical
4 Razmjou et al. BMC Musculoskeletal Disorders 2014, 15:306 Page 4 of 7 Table 2 Means of the outcome measures at specific assessment occasions Outcome measure Pre-surgery (95% CI) 6-months (95% CI) 12-months (95% CI) 24-months (95% CI) ASES HHR 27 (21, 34) 63 (56, 70) 62 (55, 69) 63 (55, 70) TSA 34 (31, 38) 73 (70, 77) 80 (77, 83) 80 (77, 84) RCMS HHR 27 (19, 35) 60 (52, 69) 64 (56, 72) 63 (54, 73) TSA 28 (24, 32) 72 (68, 76) 82 (78, 87) 86 (82, 90) Physical Symptoms HHR 458 (413, 503) 175 (129, 221) 180 (135, 226) 253 (199, 306) TSA 410 (388, 432) 128 (106, 150) 100 (77, 122) 98 (76, 121) Strength HHR 3.6 (2.1, 5.0) 5.4 (3.9, 6.9) 6.4 (4.9, 7.8) 6.8 (5.1, 8.5) TSA 4.0 (3.3, 4.7) 6.7 (6.0, 7.4) 8.5 (7.8, 9.2) 9.6 (8.8, 10.3) Flexion HHR 66 (54, 79) 98 (85, 111) 104 (91, 117) 107 (93, 121) TSA 64 (57, 70) 116 (110, 123) 130 (123, 136) 131 (125, 137) Abduction HHR 51 (38, 64) 83 (70, 97) 93 (80, 107) 84 (71, 98) TSA 44 (38, 51) 101 (94, 107) 115 (109, 122) 119 (112, 125) Ext. Rot. HHR 14 (7.9, 20) 40 (33, 46) 40 (34, 46) 42 (35, 49) TSA 13 (10, 16) 42 (39, 45) 47 (44, 50) 47 (44, 50) Change over time (2-year scores - pre-op scores) was significant for TSA and HHR groups for all measures at p < Figure 1 Relative Constant Murley Score change profile.
5 Razmjou et al. BMC Musculoskeletal Disorders 2014, 15:306 Page 5 of 7 Figure 2 ASES Score change profile. symptoms for the HHR group improved till 6 months and then began to decline. A different pattern of recovery was noted for strength which showed continued improvement until 24 months post surgery. Our results are consistent with the literature which indicates an overall improvement in pain and disability following shoulder arthroplasty [2-7,18-23]. The contribution of our study is exploring the typical trajectory of recovery after each procedure. This information is useful to clinicians as it enables them to communicate the expected point of maximal recovery or plateau to their patients more accurately. It is also of importance to patients as it helps them to have realistic expectations and set appropriate goals throughout their recovery. More specifically, patients who undergo HHR may benefit from knowing that although elevation may have a slower and less significant improvement, external rotation, and overall disability will show improvement up to one year with strength gains of up to two years. Limitations Despite consistency between our results and the available literature, the present study involved secondary analysis of prospectively collected data of patients operated Figure 3 Physical symptom change profile.
6 Razmjou et al. BMC Musculoskeletal Disorders 2014, 15:306 Page 6 of 7 Figure 4 Strength change profile. by a senior orthopedic surgeon in an academic centre, which may limit generalizability of our findings. In the present study, most of the recovery happened in the first 6 months. Although shoulder joint replacement is a major surgery with a prolonged recovery, future work might include more sampling prior to the 6-month time period. Conclusion Our study showed a statistically significant improvement in all patient reported and performance measures regardless of the type of arthroplasty. The greatest change for all outcomes measured occurred within the first 6- months of surgery. In the HHR group, despite a slight decline in physical symptoms after 6 months, there was a significant overall improvement from the pre-operative level. Strength continued to improve up to 24 months post surgery. The pattern of recovery differed by outcome measure and type of procedure. Knowledge of these recovery patterns will help clinicians direct appropriate rehabilitation and patients set more realistic goals and expectations. Abbreviations Abd: Abduction; ACMS: Absolute Constant Murley Score; ADL: Activities of daily living; ASES: American Shoulder and Elbow Surgeon s form; BF: Bigliani- Flatow; Ext Rot: External Rotation; Flex: Flexion; GEE: Generalized Estimating Equations; HHR: Humeral Head Replacement; PS: Physical Symptoms; ROM: Range of Motion; RCMS: Relative Constant Murley Score; TESS: Total Evolutive Shoulder System; TSA: Total Shoulder Arthroplasty. Competing interests The authors declare that they have no competing interests. Authors contributions HR conceived the idea, supervised data collection and entry and provided input on analysis. PS conducted the analysis. DK provided input on analysis. RH performed the surgical procedures. All authors participated in data analysis interpretation and have contributed to manuscript preparation and have read and approved the final manuscript. Acknowledgement Helen Razmjou was supported by a doctoral fellowship award from the Canadian Institutes of Health Research during three years of one of the original studies. Author details 1 Holland Orthopaedic & Arthritic Centre, Sunnybrook Health Sciences Centre, 43 Wellesley Street East, Toronto, Ontario M1Y 1H1, Canada. 2 Department of Physical Therapy, Faculty of Medicine, University of Toronto, Toronto, Canada. 3 Sunnybrook Research Institute, Sunnybrook Health Sciences Centre, Toronto, Canada. 4 School of Rehabilitation Science, McMaster University, Hamilton, Canada. 5 Department of Clinical Epidemiology & Biostatistics, McMaster University, Hamilton, Canada. 6 Division of Orthopaedic Surgery, Department of Surgery, Faculty of Medicine, University of Toronto, Toronto, Canada. Received: 5 March 2014 Accepted: 18 September 2014 Published: 18 September 2014 References 1. Sanchez-Sotelo J: Total shoulder arthroplasty. Open Orthop J 2011, 5: Carter MJ, Mikuls TR, Nayak S, Fehringer EV, Michaud K: Impact of total shoulder arthroplasty on generic and shoulder-specific health-related quality-of-life measures: a systematic literature review and meta-analysis. J Bone Joint Surg Am 2012, 94(17):e Fevang BT, Lygre SH, Bertelsen G, Skredderstuen A, Havelin LI, Furnes O: Good function after shoulder arthroplasty. Acta Orthop 2012, 83(5): Sperling JW, Cofield RH, Rowland CM: Minimum fifteen-year follow-up of Neer hemiarthroplasty and total shoulder arthroplasty in patients aged fifty years or younger. J Shoulder Elbow Surg 2004, 13(6): Bishop JY, Flatow EL: Humeral head replacement versus total shoulder arthroplasty: clinical outcomes a review. J Shoulder Elbow Surg 2005, 14(1 Suppl S):141S 146S. 6. Sandow MJ, David H, Bentall SJ: Hemiarthroplasty vs total shoulder replacement for rotator cuff intact osteoarthritis: how do they fare after a decade? J Shoulder Elbow Surg 2013, 22(7):
7 Razmjou et al. BMC Musculoskeletal Disorders 2014, 15:306 Page 7 of 7 7. Gartsman GM, Roddey TS, Hammerman SM: Shoulder arthroplasty with or without resurfacing of the glenoid in patients who have osteoarthritis. J Bone Joint Surg Am 2000, 82(1): Razmjou H, Davis AM, Jaglal SB, Holtby R, Richards RR: Disability and satisfaction after rotator cuff decompression or repair: a sex and gender analysis. BMC Musculoskelet Disord 2011, 12: Kennedy D, Stratford PW, Pagura SM, Walsh M, Woodhouse LJ: Comparison of gender and group differences in self-report and physical performance measures in total hip and knee arthroplasty candidates. J Arthroplasty 2002, 17(1): Kennedy DM, Hanna SE, Stratford PW, Wessel J, Gollish JD: Preoperative function and gender predict pattern of functional recovery after hip and knee arthroplasty. J Arthroplasty 2006, 21(4): Kennedy DM, Stratford PW, Riddle DL, Hanna SE, Gollish JD: Assessing recovery and establishing prognosis following total knee arthroplasty. Phys Ther 2008, 88(1): Richards RR, An K, Bigliani LU, Friedman R, Gartsman GM, Gristina AG, Iannotti JP, Mow VC, Sidles JA, Zuckerman JD: A standardized method for the assessment of shoulder function. J Shoulder Elbow Surg 1994, 3: Constant CR: An evaluation of the Constant-Murley shoulder assessment. J Bone Joint Surg (Br) 1997, 79(4): Razmjou H, Richards RR, Denis S, Axelrod T, Holtby R: Disability outcome measures in patients with advanced osteoarthritis of shoulder [abstract]. J Bone Joint Surg Br 2012, 94-B:(SUPP XXI) Michener LA, McClure PW, Sennett BJ: American Shoulder and Elbow Surgeons Standardized Shoulder Assessment Form, patient self-report section: reliability, validity, and responsiveness. J Shoulder Elbow Surg 2002, 11(6): Lo IK, Litchfield RB, Griffin S, Faber K, Patterson SD, Kirkley A: Quality-of-life outcome following hemiarthroplasty or total shoulder arthroplasty in patients with osteoarthritis. A prospective, randomized trial. J Bone Joint Surg Am 2005, 87(10): Buchler P, Farron A: Benefits of an anatomical reconstruction of the humeral head during shoulder arthroplasty: a finite element analysis. Clin Biomech (Bristol, Avon) 2004, 19(1): Iannotti JP, Norris TR: Influence of preoperative factors on outcome of shoulder arthroplasty for glenohumeral osteoarthritis. J Bone Joint Surg Am 2003, 85-A(2): Radnay CS, Setter KJ, Chambers L, Levine WN, Bigliani LU, Ahmad CS: Total shoulder replacement compared with humeral head replacement for the treatment of primary glenohumeral osteoarthritis: a systematic review. J Shoulder Elbow Surg 2007, 16(4): Deshmukh AV, Koris M, Zurakowski D, Thornhill TS: Total shoulder arthroplasty: long-term survivorship, functional outcome, and quality of life. J Shoulder Elbow Surg 2005, 14(5): Edwards TB, Kadakia NR, Boulahia A, Kempf JF, Boileau P, Nemoz C, Walch G: A comparison of hemiarthroplasty and total shoulder arthroplasty in the treatment of primary glenohumeral osteoarthritis: results of a multicenter study. J Shoulder Elbow Surg 2003, 12(3): Sajadi KR, Kwon YW, Zuckerman JD: Revision shoulder arthroplasty: an analysis of indications and outcomes. J Shoulder Elbow Surg 2010, 19(2): Torchia ME, Cofield RH, Settergren CR: Total shoulder arthroplasty with the Neer prosthesis: long-term results. J Shoulder Elbow Surg 1997, 6(6): doi: / Cite this article as: Razmjou et al.: Pattern of recovery following total shoulder arthroplasty and humeral head replacement. BMC Musculoskeletal Disorders :306. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Shoulder Replacement Commonly Asked Questions
 Shoulder Replacement Commonly Asked Questions Patrick J Denard, MD Shoulder Specialist 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Background Information What is the anatomy of the shoulder? The
Shoulder Replacement Commonly Asked Questions Patrick J Denard, MD Shoulder Specialist 2780 E. Barnett Rd Medford, OR 97530 541-779-6250 Background Information What is the anatomy of the shoulder? The
Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty
 Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty Vaqar Latif, MD; Patrick J. Denard, MD; Allan A. Young, MD; Jean-Pierre Liotard, MD; Gilles Walch, MD abstract Full article
Bilateral Anatomic Total Shoulder Arthroplasty Versus Reverse Shoulder Arthroplasty Vaqar Latif, MD; Patrick J. Denard, MD; Allan A. Young, MD; Jean-Pierre Liotard, MD; Gilles Walch, MD abstract Full article
Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease
 Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease Geoffrey S. Van Thiel, M.D., M.B.A., Steven Sheehan, B.S., Rachel M. Frank, B.S., Mark Slabaugh, M.D., Brian J. Cole,
Retrospective Analysis of Arthroscopic Management of Glenohumeral Degenerative Disease Geoffrey S. Van Thiel, M.D., M.B.A., Steven Sheehan, B.S., Rachel M. Frank, B.S., Mark Slabaugh, M.D., Brian J. Cole,
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Total Shoulder Arthroplasty
 1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY
 Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Both anatomic (atsa) and reverse (rtsa) total
 S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
S101 Comparison of Outcomes Using Anatomic and Reverse Total Shoulder Arthroplasty Pierre-Henri Flurin, M.D., Yann Marczuk, M.D., Martin Janout, M.D., Thomas W. Wright, M.D., Joseph Zuckerman, M.D., and
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol. Phase 1 Maximum Protection (0-4 weeks)
 Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Biomechanical concepts of total shoulder replacement. «Shoulder Course» Day 1. Richard W. Nyffeler Orthopädie Sonnenhof Bern. 11. Sept.
 Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Biomechanical concepts of total shoulder replacement Richard W. Nyffeler Orthopädie Sonnenhof Bern First total shoulder prosthesis Jules Emile Péan, 1830-1898 Monobloc prostheses Charles Neer, 1917-2011
Early To Medium Term Results of the Anatomical Total Shoulder Replacement
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 13 Number 2 Early To Medium Term Results of the Anatomical Total Shoulder Replacement R Sloan, J Young, N Parker, I Nwachukwu Citation R Sloan,
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 13 Number 2 Early To Medium Term Results of the Anatomical Total Shoulder Replacement R Sloan, J Young, N Parker, I Nwachukwu Citation R Sloan,
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 366, pp. 39-45 0 1999 Lippincott Williams & Wilkins, Inc. Late Results of Total Shoulder Replacement in Patients With Rheumatoid Arthritis Jens 0. S@jbjerg,
Name of Policy: Shoulder Resurfacing
 Name of Policy: Shoulder Resurfacing Policy #: 366 Latest Review Date: November 2010 Category: Surgery Policy Grade: Active policy but no longer scheduled for regular literature reviews and update. Background/Definitions:
Name of Policy: Shoulder Resurfacing Policy #: 366 Latest Review Date: November 2010 Category: Surgery Policy Grade: Active policy but no longer scheduled for regular literature reviews and update. Background/Definitions:
Two Rotator Cuff Disease Specific Outcome Measures, The RC-QOL And the WORC Exhibit Similar Construct Validity And Responsiveness
 Two Rotator Cuff Disease Specific Outcome Measures, The RC-QOL And the WORC Exhibit Similar Construct Validity And Responsiveness Helen Razmjou 1,2, Andrea Bean 1,2, Varda van Osnabrugge 1,2, Joy C Mac
Two Rotator Cuff Disease Specific Outcome Measures, The RC-QOL And the WORC Exhibit Similar Construct Validity And Responsiveness Helen Razmjou 1,2, Andrea Bean 1,2, Varda van Osnabrugge 1,2, Joy C Mac
Not relevant to this presentation.
 Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Nolan R. May, MD Kearney, NE Heartland Surgery Center, Kearney NE Not relevant to this presentation. 1 What are the indications for total shoulder arthroplasty? What are the differences between total shoulder
Shoulder Joint Replacement
 Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Shoulder Joint Replacement Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was first performed
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT. Page: 1 of 6
 Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title SHOULDER ARTHROPLASTY (TOTAL, PARTIAL AND REVERSE) Policy Number 7.01.95 Category Technology Assessment Effective Date 6/21/18 Revised
Shoulder Arthroplasty. Valentin Lance 3/24/16
 Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Shoulder Arthroplasty Valentin Lance 3/24/16 Outline Background Pre-operative imaging assessment Total Shoulder Arthroplasty: Standard and Reverse Complications Other shoulder hardware Hemiarthroplasty
Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review
 Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
Review Article Comparison of Pegged and Keeled Glenoid Components for Total Shoulder Arthroplasty: A Systematic Review Journal of Shoulder and Elbow Arthroplasty Volume 1: 1 7! The Author(s) 2017 Reprints
Relationship between clinical and surgical findings and reparability of large and massive rotator cuff tears: a longitudinal study
 Holtby and Razmjou BMC Musculoskeletal Disorders 2014, 15:180 RESEARCH ARTICLE Open Access Relationship between clinical and surgical findings and reparability of large and massive rotator cuff tears:
Holtby and Razmjou BMC Musculoskeletal Disorders 2014, 15:180 RESEARCH ARTICLE Open Access Relationship between clinical and surgical findings and reparability of large and massive rotator cuff tears:
Sidus Stem-Free Shoulder. Secure fixation through a bone-sparing design
 Sidus Stem-Free Shoulder Secure fixation through a bone-sparing design An efficient, bone-sparing solution, should revision become necessary Humeral shaft is untouched, minimal bone is removed from the
Sidus Stem-Free Shoulder Secure fixation through a bone-sparing design An efficient, bone-sparing solution, should revision become necessary Humeral shaft is untouched, minimal bone is removed from the
Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication?
 CASE REPORT Open Access Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication? A case report Timothy R Judkins, Michael R Dayton * Abstract
CASE REPORT Open Access Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication? A case report Timothy R Judkins, Michael R Dayton * Abstract
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Shoulder Arthroplasty: Pioneers, Choices and Controversy
 Article ID: 2046-1690 Shoulder Arthroplasty: Pioneers, Choices and Controversy Corresponding Author: Dr. William Kent, Foundation doctor, Eastbourne District General Hospital - United Kingdom Submitting
Article ID: 2046-1690 Shoulder Arthroplasty: Pioneers, Choices and Controversy Corresponding Author: Dr. William Kent, Foundation doctor, Eastbourne District General Hospital - United Kingdom Submitting
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
The Role of Concomitant Biceps Tenodesis in Shoulder Arthroplasty for Primary Osteoarthritis: Results of a Multicentric Study
 4edwards.qxd 4/6/04 3:53 PM Page 401 The Role of Concomitant Biceps Tenodesis in Shoulder Arthroplasty for Primary Osteoarthritis: Results of a Multicentric Study GIUSEPPE FAMA, MD*; T. BRADLEY EDWARDS,
4edwards.qxd 4/6/04 3:53 PM Page 401 The Role of Concomitant Biceps Tenodesis in Shoulder Arthroplasty for Primary Osteoarthritis: Results of a Multicentric Study GIUSEPPE FAMA, MD*; T. BRADLEY EDWARDS,
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Results of a new stemless shoulder prosthesis: Radiologic proof of maintained fixation and stability after a minimum of three years follow-up
 J Shoulder Elbow Surg (2010) 19, 847-852 www.elsevier.com/locate/ymse Results of a new stemless shoulder prosthesis: Radiologic proof of maintained fixation and stability after a minimum of three years
J Shoulder Elbow Surg (2010) 19, 847-852 www.elsevier.com/locate/ymse Results of a new stemless shoulder prosthesis: Radiologic proof of maintained fixation and stability after a minimum of three years
A 42-year-old patient presenting with femoral
 Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Disclosure. General. Total Shoulder Arthroplasty : Results, Outcomes and Expectations 2/8/2016. Consultant for Tornier/Wright, DJO, and Conventus
 Total Shoulder Arthroplasty : Results, Outcomes and Expectations Edwin E Spencer Jr MD Knoxville Orthopaedic Clinic Disclosure Consultant for Tornier/Wright, DJO, and Conventus General The literature is
Total Shoulder Arthroplasty : Results, Outcomes and Expectations Edwin E Spencer Jr MD Knoxville Orthopaedic Clinic Disclosure Consultant for Tornier/Wright, DJO, and Conventus General The literature is
Patient-Specific Implants in Severe Glenoid Bone Loss
 Patient-Specific Implants in Severe Glenoid Bone Loss Publish date: February 8, 2018 Authors: Ivan De Martino, MD David M. Dines, MD Russell F. Warren, MD Edward V. Craig, MD, MPH Lawrence V. Gulotta,
Patient-Specific Implants in Severe Glenoid Bone Loss Publish date: February 8, 2018 Authors: Ivan De Martino, MD David M. Dines, MD Russell F. Warren, MD Edward V. Craig, MD, MPH Lawrence V. Gulotta,
ISSUES FROM AN ORTHOPEDIC PERSPECTIVE
 ISSUES FROM AN ORTHOPEDIC PERSPECTIVE John Brown, MD The Core Institute Objectives: Understand the common orthopedic problems of the geriatric population. Describe the standard treatment algorithms for
ISSUES FROM AN ORTHOPEDIC PERSPECTIVE John Brown, MD The Core Institute Objectives: Understand the common orthopedic problems of the geriatric population. Describe the standard treatment algorithms for
SHOULDER ARTHROPLASTY (TOTAL, HEMI, REVERSE)/ARTHRODESIS
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Risks of loosening of a prosthetic glenoid implanted in retroversion
 Risks of loosening of a prosthetic glenoid implanted in retroversion Alain Farron, MD, a Alexandre Terrier, PhD, b and Philippe Büchler, PhD, b Lausanne, Switzerland Osteoarthritis of the shoulder is frequently
Risks of loosening of a prosthetic glenoid implanted in retroversion Alain Farron, MD, a Alexandre Terrier, PhD, b and Philippe Büchler, PhD, b Lausanne, Switzerland Osteoarthritis of the shoulder is frequently
Materials and methods. Table I. 2 J.W. Uribe, A.B.-van Bemden
 2 J.W. Uribe, A.B.-van Bemden Table I Stage I Stage II Stage III Stage IV Stage V Cruess classification for osteonecrosis of humeral head Preradiographic, requires magnetic resonance imaging, bone scan,
2 J.W. Uribe, A.B.-van Bemden Table I Stage I Stage II Stage III Stage IV Stage V Cruess classification for osteonecrosis of humeral head Preradiographic, requires magnetic resonance imaging, bone scan,
Shoulder hemiarthroplasty in the management of humeral head fractures
 Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
Acta Orthop. Belg., 2004, 70, 214-218 ORIGINAL STUDY Shoulder hemiarthroplasty in the management of humeral head fractures Joseph J. CHRISTOFORAKIS, George M. KONTAKIS, Pavlos G. KATONIS, Konstantinos
Degenerative joint disease of the shoulder, while
 Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis
 Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
Cigna Medical Coverage Policies Musculoskeletal Shoulder Arthroplasty (Total, Hemi, Reverse)/Arthrodesis Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit
L. Favard a,, D. Katz b, M. Colmar c, T. Benkalfate d, H. Thomazeau e, S. Emily c WORKSHOPS OF THE SOO (2011, LA BAULE).
 Orthopaedics & Traumatology: Surgery & Research (2012) 98, S41 S47 Available online at www.sciencedirect.com WORKSHOPS OF THE SOO (2011, LA BAULE). ORIGINAL ARTICLE Total shoulder arthroplasty Arthroplasty
Orthopaedics & Traumatology: Surgery & Research (2012) 98, S41 S47 Available online at www.sciencedirect.com WORKSHOPS OF THE SOO (2011, LA BAULE). ORIGINAL ARTICLE Total shoulder arthroplasty Arthroplasty
Surface Replacement for the Active Patient with GH DJD. Disclosures. Popularized by Copeland 3/1/2018
 Surface Replacement for the Active Patient with GH DJD E. Rhett Hobgood, M.D. MS Sports Medicine Jackson, MS Disclosures Consultant for Exactech No royalties from any company Fellowship support from Mitek,
Surface Replacement for the Active Patient with GH DJD E. Rhett Hobgood, M.D. MS Sports Medicine Jackson, MS Disclosures Consultant for Exactech No royalties from any company Fellowship support from Mitek,
YEAR EXPERIENCE WITH STEMLESS ARTHROPLASTY. Disclosures INDICATIONS FOR STEMMLES TSA
 5-10 YEAR EXPERIENCE WITH STEMLESS ARTHROPLASTY PETER HABERMEYER DEUTSCHES SCHULTERZENTRUM MUNICH Germany Disclosures Consultant for Arthrex Inc. Royalties Arthrex Inc. INDICATIONS FOR STEMMLES TSA 1.
5-10 YEAR EXPERIENCE WITH STEMLESS ARTHROPLASTY PETER HABERMEYER DEUTSCHES SCHULTERZENTRUM MUNICH Germany Disclosures Consultant for Arthrex Inc. Royalties Arthrex Inc. INDICATIONS FOR STEMMLES TSA 1.
WHAT YOU IS BACK WITHIN ARM S REACH
 YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
YOUR TOTAL SHOULDER REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE WHAT YOU IS BACK WITHIN ARM S REACH Nathan Richardson, MD Orthopedics, Shoulder & Elbow Surgeon Board Certified in
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty
 Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
)19( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )19( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Failure of Anatomic Total Shoulder Arthroplasty with Revision to Another Anatomic Total Shoulder Arthroplasty Mihir Sheth,
)19( COPYRIGHT 2019 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Failure of Anatomic Total Shoulder Arthroplasty with Revision to Another Anatomic Total Shoulder Arthroplasty Mihir Sheth,
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
)532( COPYRIGHT 2018 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE The Midterm Results of the Delta Xtend Reverse Shoulder System: A Five-Year Outcome Study John G. Horneff, MD; Thema A. Nicholson,
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Reverse Total Shoulder
 Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Shoulder Arthroplasty
 Shoulder Arthroplasty Nathan G. Everding, MD Specializing in Hand, Wrist, Elbow & Shoulder Surgery Syracuse Orthopedic Specialists SJH Family Practice Refresher course 3/8/19 Shoulder Arthroplasty Rate
Shoulder Arthroplasty Nathan G. Everding, MD Specializing in Hand, Wrist, Elbow & Shoulder Surgery Syracuse Orthopedic Specialists SJH Family Practice Refresher course 3/8/19 Shoulder Arthroplasty Rate
The complex characteristics of 282 unsatisfactory shoulder arthroplasties
 The complex characteristics of 282 unsatisfactory shoulder arthroplasties Amy K. Franta, MD, a Tim R. Lenters, MD, a Doug Mounce, MSc, a Blazej Neradilek, MSc, b and Frederick A. Matsen, III, MD, a Seattle,
The complex characteristics of 282 unsatisfactory shoulder arthroplasties Amy K. Franta, MD, a Tim R. Lenters, MD, a Doug Mounce, MSc, a Blazej Neradilek, MSc, b and Frederick A. Matsen, III, MD, a Seattle,
IJSPT CASE REPORT ABSTRACT
 IJSPT CASE REPORT COMPREHENSIVE POST-ARTHROSCOPIC MANAGEMENT OF A MIDDLE-AGED ADULT WITH GLENOHUMERAL OSTEOARTHRITIS: A CASE REPORT Nicholas D. Hagen, PT, DPT, SCS, CSCS 1 Thomas Olson, PT, DPT, SCS 1
IJSPT CASE REPORT COMPREHENSIVE POST-ARTHROSCOPIC MANAGEMENT OF A MIDDLE-AGED ADULT WITH GLENOHUMERAL OSTEOARTHRITIS: A CASE REPORT Nicholas D. Hagen, PT, DPT, SCS, CSCS 1 Thomas Olson, PT, DPT, SCS 1
Assessment of Approximate Glenoid Size in Thai People
 Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
Assessment of Approximate Glenoid Size in Thai People J Med Assoc Thai 2014; 97 (Suppl. 2): S14-S18 Full text. e-journal: http://www.jmatonline.com Pason Phonphok MD*, Nattha Kulkamthorn MD* * Division
DK7215-Levine-ch12_R2_211106
 12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
Arthroplasty Of The Shoulder
 Arthroplasty Of The Shoulder 1 / 7 2 / 7 3 / 7 Arthroplasty Of The Shoulder About Your Shoulder. Ligaments and tendons hold it together. Ligaments connect the bones, while tendons connect muscles to the
Arthroplasty Of The Shoulder 1 / 7 2 / 7 3 / 7 Arthroplasty Of The Shoulder About Your Shoulder. Ligaments and tendons hold it together. Ligaments connect the bones, while tendons connect muscles to the
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Physical Therapy Intervention Strategies Post Ream and Run Hemiarthroplasty
 Physical Therapy Intervention Strategies Post Ream and Run Hemiarthroplasty Jessica Ottow, Student Physical Therapist Suzanne Ryer, MPT Faculty Mentor Abstract Background: Treatment of glenohumeral arthritis
Physical Therapy Intervention Strategies Post Ream and Run Hemiarthroplasty Jessica Ottow, Student Physical Therapist Suzanne Ryer, MPT Faculty Mentor Abstract Background: Treatment of glenohumeral arthritis
Integra. Titan Modular Shoulder System, 2.5
 Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
Titan Modular Shoulder System, 2.5 Limit uncertainty with a shoulder implant system that redefines modularity, addresses multiple indications, and allows for reproducible results. Titan Modular Shoulder
CLINICAL GUIDELINES. CMM-318: Shoulder Arthroplasty/ Replacement/Resurfacing/ Revision/Arthrodesis. Version Effective October 22, 2018
 CLINICAL GUIDELINES CMM-318: / Replacement/Resurfacing/ Revision/Arthrodesis Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-318:
CLINICAL GUIDELINES CMM-318: / Replacement/Resurfacing/ Revision/Arthrodesis Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-318:
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
RCR or rtsa? Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair?
 Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair? JESSE W. ALLERT, MD THOMAS SELLERS, MD PETER SIMON, PHD RACHEL CLARK,
Massive Rotator Cuff Tears without Arthritis in Patients Older than 65 Reverse Total Shoulder Arthroplasty or Rotator Cuff Repair? JESSE W. ALLERT, MD THOMAS SELLERS, MD PETER SIMON, PHD RACHEL CLARK,
Addressing Glenoid Erosion in Anatomic Total Shoulder Arthroplasty
 S46 Addressing Glenoid Erosion in Anatomic Total Shoulder Arthroplasty Richard B. Jones, M.D. Abstract Glenoid wear is common in the setting of shoulder arthritis. Severe glenoid erosion presents a serious
S46 Addressing Glenoid Erosion in Anatomic Total Shoulder Arthroplasty Richard B. Jones, M.D. Abstract Glenoid wear is common in the setting of shoulder arthritis. Severe glenoid erosion presents a serious
Lateral meniscus allograft biologic glenoid arthroplasty in total shoulder arthroplasty for young shoulders with degenerative joint disease
 Lateral meniscus allograft biologic glenoid arthroplasty in total shoulder arthroplasty for young shoulders with degenerative joint disease Gregory P. Nicholson, MD, Jordan L. Goldstein, MD, Anthony A.
Lateral meniscus allograft biologic glenoid arthroplasty in total shoulder arthroplasty for young shoulders with degenerative joint disease Gregory P. Nicholson, MD, Jordan L. Goldstein, MD, Anthony A.
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder
 Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
Revision of the humeral component for aseptic loosening in arthroplasty of the shoulder A. Cil, C. J. H. Veillette, J. Sanchez-Sotelo, J. W. Sperling, C. Schleck, R. H. Cofield From the Mayo Clinic, Rochester,
ANATOMIC TOTAL SHOULDER REPLACEMENT:
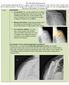 The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
The Shoulder Replacement A total shoulder arthroplasty (TSA) is a surgery to replace the damaged parts of the ball and socket shoulder joint with an artificial prosthesis. The damage to the shoulder can
Nationwide Trends in Total Shoulder Arthroplasty and Hemiarthroplasty for Osteoarthritis
 An Original Study Nationwide Trends in Total Shoulder Arthroplasty and Hemiarthroplasty for Osteoarthritis David Trofa, MD, Sean S. Rajaee, MD, and Eric L. Smith, MD Abstract Recent literature reports
An Original Study Nationwide Trends in Total Shoulder Arthroplasty and Hemiarthroplasty for Osteoarthritis David Trofa, MD, Sean S. Rajaee, MD, and Eric L. Smith, MD Abstract Recent literature reports
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE
 ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty
 J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
J Shoulder Elbow Surg (2009) -, 1-6 www.elsevier.com/locate/ymse Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty Heinz R. Hoenecke Jr., MD*, Juan C. Hermida, MD, Cesar
Developments in Shoulder Arthroplasty
 Developments in Shoulder Arthroplasty Andrew L. Wallace PhD MFSEM FRCS FRACS Consultant Shoulder Surgeon Glenohumeral Joint Arthritis Relatively uncommon Not as common as hip/knee/hand UK National Joint
Developments in Shoulder Arthroplasty Andrew L. Wallace PhD MFSEM FRCS FRACS Consultant Shoulder Surgeon Glenohumeral Joint Arthritis Relatively uncommon Not as common as hip/knee/hand UK National Joint
Surgeons agree more on treatment recommendations than on classification of proximal humeral fractures
 Brorson et al. BMC Musculoskeletal Disorders 2012, 13:114 RESEARCH ARTICLE Open Access Surgeons agree more on treatment recommendations than on classification of proximal humeral fractures Stig Brorson
Brorson et al. BMC Musculoskeletal Disorders 2012, 13:114 RESEARCH ARTICLE Open Access Surgeons agree more on treatment recommendations than on classification of proximal humeral fractures Stig Brorson
Excision arthroplasty following shoulder replacement
 Acta Orthop. Belg., 2011, 77, 448-452 ASPECT OF CURRENT MANAGEMENT Excision arthroplasty following shoulder replacement Charalambos P. CHARALAMBOUS, Shivappa SAIDAPUR, Farhan ALVI, John HAINES, Ian TRAIL
Acta Orthop. Belg., 2011, 77, 448-452 ASPECT OF CURRENT MANAGEMENT Excision arthroplasty following shoulder replacement Charalambos P. CHARALAMBOUS, Shivappa SAIDAPUR, Farhan ALVI, John HAINES, Ian TRAIL
No Financial Disclosures
 Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
No relationship between critical shoulder angle and glenoid erosion after shoulder hemiarthroplasty: a comparative radiographic study
 DOI 10.1007/s00402-017-2708-9 ORTHOPAEDIC SURGERY No relationship between critical shoulder angle and glenoid erosion after shoulder hemiarthroplasty: a comparative radiographic study S. Cerciello 1,2,10
DOI 10.1007/s00402-017-2708-9 ORTHOPAEDIC SURGERY No relationship between critical shoulder angle and glenoid erosion after shoulder hemiarthroplasty: a comparative radiographic study S. Cerciello 1,2,10
(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
Common Shoulder Problems and Treatment Options. Benjamin W. Szerlip D.O. Austin Shoulder Institute
 Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
Common Shoulder Problems and Treatment Options Benjamin W. Szerlip D.O. Austin Shoulder Institute Speaker Disclosure Dr. Szerlip has disclosed that he has no actual or potential conflict of interest in
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty
 Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
Disclosures A prospective comparison between reverse and anatomic total shoulder arthroplasty Tuyen Kiet Micah Naimark, MD Brian T. Feeley, MD Teddy T. Chung Tatiana Gajiu Sarah L. Hall, MA C. Benjamin
REVERSE SHOULDER REPLACEMENT
 REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is designed specifically for the use in shoulders with a deficient rotator cuff and arthritis, as well as other difficult shoulder reconstructive
REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is designed specifically for the use in shoulders with a deficient rotator cuff and arthritis, as well as other difficult shoulder reconstructive
Shoulder DJD in Athletic patient. What is Athletic? McCarty University of Colorado Fall Sports Medicine Symposium. Oct. 3, 2008
 Indications for Shoulder Arthroplasty in Athletic Patients Eric C. McCarty, M.D. Associate Professor, Dept. of Orthopaedics Chief, Sports Medicine and Shoulder Surgery Head Team Physician, University of
Indications for Shoulder Arthroplasty in Athletic Patients Eric C. McCarty, M.D. Associate Professor, Dept. of Orthopaedics Chief, Sports Medicine and Shoulder Surgery Head Team Physician, University of
Humeral surface replacement for the sequelae of fractures of the proximal humerus
 Humeral surface replacement for the sequelae of fractures of the proximal humerus G. Pape, F. Zeifang, T. Bruckner, P. Raiss, M. Rickert, M. Loew From University of Heidelberg, Heidelberg, Germany G. Pape,
Humeral surface replacement for the sequelae of fractures of the proximal humerus G. Pape, F. Zeifang, T. Bruckner, P. Raiss, M. Rickert, M. Loew From University of Heidelberg, Heidelberg, Germany G. Pape,
Relationship of the Penn Shoulder Score with Measures of Range of Motion and Strength in Patients with Shoulder Disorders: A Preliminary Report
 The University of Pennsylvania Orthopaedic Journal 16: 39 44, 2003 2003 The University of Pennsylvania Orthopaedic Journal Relationship of the Penn Shoulder Score with Measures of Range of Motion and Strength
The University of Pennsylvania Orthopaedic Journal 16: 39 44, 2003 2003 The University of Pennsylvania Orthopaedic Journal Relationship of the Penn Shoulder Score with Measures of Range of Motion and Strength
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
Characteristics of unsatisfactory shoulder arthroplasties
 Characteristics of unsatisfactory shoulder arthroplasties Samer S. Hasan, MD, PhD, a Jordan M. Leith, MD, FRCSC, b Barry Campbell, MS, c Ranjit Kapil, c Kevin L. Smith, MD, c and Frederick A. Matsen III,
Characteristics of unsatisfactory shoulder arthroplasties Samer S. Hasan, MD, PhD, a Jordan M. Leith, MD, FRCSC, b Barry Campbell, MS, c Ranjit Kapil, c Kevin L. Smith, MD, c and Frederick A. Matsen III,
A GUIDE TO TOTAL SHOULDER REPLACEMENT
 A GUIDE TO TOTAL SHOULDER REPLACEMENT Making the decision to have a total shoulder replacement should be a topic discussed between the individual considering the surgery as well as the individual s family,
A GUIDE TO TOTAL SHOULDER REPLACEMENT Making the decision to have a total shoulder replacement should be a topic discussed between the individual considering the surgery as well as the individual s family,
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair
 Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Proximal humeral fractures are
 Clin Orthop Relat Res (2015) 473:2750 2756 / DOI 10.1007/s11999-015-4430-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 27 June
Clin Orthop Relat Res (2015) 473:2750 2756 / DOI 10.1007/s11999-015-4430-7 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 27 June
The anteromedial approach for shoulder arthroplasty: The importance of the anterior deltoid
 The anteromedial approach for shoulder arthroplasty: The importance of the anterior deltoid David R. J. Gill, MB, ChB, FRACS, a Robert H. Cofield, MD, b and Charles Rowland, MS, c Joondalup, Australia,
The anteromedial approach for shoulder arthroplasty: The importance of the anterior deltoid David R. J. Gill, MB, ChB, FRACS, a Robert H. Cofield, MD, b and Charles Rowland, MS, c Joondalup, Australia,
S h o u l d e r Solutions by Tornier C o n v e r T i b l e S h o u l d e r S y S T e m
 S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
The Irreparable Rotator Cuff Tear:
 The Irreparable Rotator Cuff Tear: Trauma 101: Shoulder Session #2 Brian Grawe, MD Assistant Professor Orthopaedics & Sports Medicine 5/10/2018 Brian Grawe, MD Assistant Professor Phone Number: 513-558-4516
The Irreparable Rotator Cuff Tear: Trauma 101: Shoulder Session #2 Brian Grawe, MD Assistant Professor Orthopaedics & Sports Medicine 5/10/2018 Brian Grawe, MD Assistant Professor Phone Number: 513-558-4516
The Patient-Rated Elbow Evaluation (PREE) User Manual. June 2010
 The Patient-Rated Elbow Evaluation (PREE) User Manual June 2010 Joy C. MacDermid, BScPT, MSc, PhD School of Rehabilitation Science, McMaster University, Hamilton, Ontario, Canada Clinical Research Lab,
The Patient-Rated Elbow Evaluation (PREE) User Manual June 2010 Joy C. MacDermid, BScPT, MSc, PhD School of Rehabilitation Science, McMaster University, Hamilton, Ontario, Canada Clinical Research Lab,
"Stability and Instability of RTSA"
 Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Orthopedics Update «Reverse Total Shoulder Arthroplasty» Stability and Instability of RTSA A. LÄDERMANN Orthopaedics and Traumatology, La Tour Hospital, Meyrin, Switzerland Orthopaedics and Traumatology,
Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol:
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Resurfacing Arthroplasty of the Humerus: Indications, Surgical Technique, and Clinical Results
 8(3):152 160, 2007 Ó 2007 Lippincott Williams & Wilkins, Philadelphia R E V I E W Resurfacing Arthroplasty of the Humerus: Indications, Surgical Technique, and Clinical Results Jason J. Scalise, MD, Anthony
8(3):152 160, 2007 Ó 2007 Lippincott Williams & Wilkins, Philadelphia R E V I E W Resurfacing Arthroplasty of the Humerus: Indications, Surgical Technique, and Clinical Results Jason J. Scalise, MD, Anthony
