Minimally Invasive Plate Osteosynthesis with Locking Compression Plate for Distal Diametaphyseal Tibia Fracture
|
|
|
- Clifford Carpenter
- 5 years ago
- Views:
Transcription
1 Minimally Invasive Plate Osteosynthesis with Locking Compression Plate for Distal Diametaphyseal Tibia Fracture Shrestha D, 1 Acharya BM, 2 Shrestha PM 3 1 Department of Orthopaedics and Traumatology Dhulikhel Hospital-Kathmandu University Hospital Dhulikhel, Nepal 2 Department of Orthopaedics Patan Academy of Health Sciences Patan, Nepal 3 Department of Orthopaedics Norvic International Hospital Kathmandu, Nepal Corresponding Author Dr Dipak Shrestha Department of Orthopaedics and traumatology Dhulikhel Hospital-Kathmandu University Hospital Dhulikhel, Nepal dsmsortho@gmail.com Citation Shrestha D, Acharya BM, Shrestha PM. Minimally invasive plate osteosynthesis with locking compression plate for distal diametaphyseal tibia fracture. Kathmandu Univ Med J 2011;34(2)62-8. ABSTRACT Background Distal diametaphyseal tibia fracture though requires operative treatment is difficult to manage. Conventional osteosynthesis is not suitable because distal tibia is subcutaneous bone with poor vascularity. Closed reduction and minimally invasive plate osteosynthesis (MIPO) with locking compression plate (LCP) has emerged as an alternative treatment option because it respects biology of distal tibia and fracture hematoma and also provides biomechanicaly stable construct. Objectives To find out suitability of MIPO with LCP for distal diametaphyseal tibia fracture including union time and complicatios and compare wih other available management options in literature. Methods Twenty patients with closed distal diametaphyseal tibia fracture with or without intra articular extension (AO classification: 12 type 43A1, 4 type 43A2, 2 type 43A3 and 2 type 43B1) treated with MIPO with LCP were prospectively followed for average duration of months (range 5-30 months). Results Average duration of injury-hospital and injury-surgery interval was 12.8 hrs (range 2-44 hrs) and 4.45 days (range 1-10 days) respectively. All fractures got united with an average duration of 18.5 weeks (range14-28weeks) except one case of delayed union which was managed with percutaneous bone marrow injection. Two patients had union with valgus angulation < 5 degees but no nonunion was found. There were two superficial and one deep post operative wound infection. All infections healed with extended period of intravenous antibiotics besides repeated debridemet for deep infection. Implants were removed in eight patients among whom six (30%) had malleolar skin irritation and pain due to prominent hardware. Conclusion The present case series shows that MIPO with LCP is an effective treatment method in terms of union time and complications rate for distal diametaphyseal tibia fracture. Malleolar skin irritation is common problem because of prominent hardware. Key Words Distal diametaphyseal tibia fracture; LCP, MIPO INTRODUCTION Treatment of distal diametaphyseal tibia fracture with or without articular extension is challenging because of its unique anatomical characteristics of subcutaneous location with precarious blood supply and proximity to the ankle joint. Most of these fractures are managed with an operative intervention such as closed reduction and intramedullary interlocking (IMIL) nailing or open reduction and internal fixation (ORIF) with plating or closed reduction and per cutaneous plating or external fixators. Each of these techniques has their own merits and demerits. IMIL nailing has been reported with higher rate of malunion because it is difficult to achieve two distally locking screws. 1-3 Wound infection, skin breakdown and delayed union or non union requiring secondary procedures like bone grafting are some of the complications associated with conventional osteosynthesis with plates. 4-7 Similarly, pin tract infection, pin loosening, malunion and nonunion leading to osteomyelitis is potential complication of external fixators and hence not preferred as definitive fixation method Recently, techniques of closed reduction and minimally Page 62
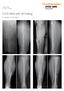
2 Original Article VOL.9 NO. 2 ISSUE 34 APR - JUN 2011 invasive plate osteosynthesis (MIPO) with locking compression plate (LCP) has emerged as an alternative treatment option for distal diametaphyseal tibia fracture. When applied subcutaneously, LCP does not endanger periosteal blood supply, respect fracture heamtoma and also provides biomechanicaly stable construct. 12,13 Numbers of previous clinical studies have established MIPO with LCP as a biologically friendly and technically sound method of fixation for distal diametaphyseal tibia fracture but most of these studies except by Ronga et al. and Ahmad et al. have included both open and closed fractures. 1,14 Since behavior of both of these fracture are different, comparison will be not fair. We therefore prospectively studied only closed distal diametaphyseal tibia fracture with or without articular extension managed with MIPO with LCP and compared with other studies. METHODS Twenty patients with closed distal diametaphyseal tibia fracture with or without intra articular extension treated in three different centers in between June 2007 to July 2010 were prospectively followed. Permission from institutional review committee from all three centers was obtained. Demographic variables, mode of injury, injury-hospital and injury-surgery interval, time required for union, complications and need of secondary procedures were recorded. Fracture was classified according to AO/OTA classification system. Patients with pathological fractures, ipsilateral multiple fractures were excluded. Author DS was involved in all three centers during surgery. Surgical techniques Patient who presented within six hours of injury without gross swelling of leg were operated on the same day or next available day. Limbs with gross swelling were splinted and elevated till swelling subsided and wrinkles appeared over the ankle joint. Fracture blisters if present managed with puncturing with sterile needle and non-adhesive dressing and observed closely for any sign of secondary infection. Under regional or general anesthesia, involved leg was prepared and draped. Tourniquet was routinely applied but inflated only when necessary. A vertical or curvilinear incision was made at the level of medial malleolus with the utmost care not to injure great sephaneous vein and sephaneous nerve. Sub cutaneous plane was made with hemostat without striping periosteum and disturbance to fracture haematoma. Fracture was reduced under C arm control. We did not use calcaneal skeletal traction or other external fixation devices. Instead, where reduction was difficult despite of repeated attempt, we made a small incision and used a Kirschner wire (3mm) as a joystick to aid in fracture reduction and towel clip or reduction clamp to hold reduction. Varus -valgus angulation < 5 and anteriorposterior angulation < 10 and shortening of < 15 mm were considered acceptable criteria for reduction. Pre contoured low metaphyseal LCP was tunneled into subcutaneous plane and its position was reconfirmed with C arm. Before fixing the plates with screws, shagging of distal fragment was prevented by putting towel roll under the fracture site. Provisional non locking screw was applied to bring the plate on the bone. If necessary, interfragmentary compression was achieved by a screw through the plate or outside the plate. Compression osteosynthesis was achieved in simple fracture by using non locking screw on proximal to fracture site as a hybrid fixation. 15 With separate stab incision, at least three locking screws were applied on the either side of fracture. Malleolar fracture if present were reduced and fixed with screws or tension band wiring before tibia fracture reduction and fixation (Figure. 1). Fibula was not routinely fixed unless it was involved at the level of syndesmosis. Skin was closed with non absorbable sutures and limb was splinted with below knee brace or posterior back slab. Figure 1. AO/OTA type 43.B1 fracture. Pre and post operative (a, b) and follow up at 20 weeks (c) and 15 months (d). Note: Posterior malleolus was fixed with anterioposterior compression screw. Post operative protocol Wound was inspected on second post operative day for any sign of wound infection and change of dressing. Patient was discharged on second or third day of surgery if skin condition was satisfactory and wound was dry. Follow up On fourteen postoperative days, stitches were removed and X ray of leg was obtained. Below knee brace or posterior back slab was discontinued. Intermittent ankle mobilization was initiated but weight bearing was not allowed for next four weeks. Patients were subsequently followed up in six weeks interval to asses fracture healing. Partial weight bearing was started once callus was visible in X ray and gradually Page 63
3 Table 1. Patients and injury data. S. No. Age (yrs) Sex AO/ OTA Type Associated injuries 1 17 M 43.A1 Left distal radius fracture Mode of injury Injury- hospital interval (hrs) Injurytreatment interval (days) Union time (wks) Follow up (months) Fall Implant removal (months) Complications 2 38 F 43.A1 Fall Valgus angulation < M 43.A1 RTA M 43.A1 RTA Deep infection 5 35 F 43.A3 RTA F 43.A3 Contralateral diaphyseal tibia fracture, head injury and soft tissue contusion RTA F 43.A1 Fracture blisters RTA Superficial infection, delayed union 8 32 F 43.A1 RTA F 43.A1 Fall M 43.A1 Fall F 43.A2 RTA Ankle stiffness M 43.B1 Left distal radius fracture RTA M 43.A1 Assault M 43.A2 Sports Valgus angulation < F 43.A1 Fall Superficial infection M 43.A1 RTA F 43.A2 Fall M 43.A1 Fall M 43.B1 RTA M 43.A2 Fracture blisters Fall increased according to clinical and radiological signs of fracture healing. Fracture was considered united when visible bridging callus was seen in at least three cortices in anterior-posterior and lateral x rays of leg and absence of pain on weight bearing clinically. If fracture union was not progressing satisfactorily, secondary procedures like bone marrow injection or cortico-cancellous bone grafting were considered. Malunion was defined as varus -valgus angulation 5 and anterior-posterior angulation 10 and shortening of 15 mm. During subsequent follow up once fracture united, if patents wished to remove the hardware or had hardware related complaints like malleolar pain, difficulty of wearing shoes or prominent implants, plate removal was indicated. Statistical analysis was performed by using SPSS (Chicago, Illinois, USA) version 15 software for Window. Mann Whitney U test was used for comparison. A p value <0.05 was regarded as significant. RESULTS There were 12 male (mean age 30.9 yrs, range17-42 yrs) and eight female patients (mean age yrs, range 20-65yrs). According to AO classification, 12 (60%) of fracture were 43A1, 4 (20%) 43A2, 2 (10%) 43A3 and 2 (10%) 43B1. Half of the patients sustained injury in road traffic accident. Other modes of injury were fall injury in 8 (40%) patients and physical assault and sports related injury in 1 (5%) each. One patient had contralateral diaphyseal tibia fracture which was managed with closed reduction and IMIL nailing in same setting. Average duration of injury-hospital and injury-surgery interval was 12.8 hrs (range 2-44 hrs) and 4.45 days (range 1-10 days) respectively. In two patients case no 7 and 19, repeated attempt of closed reduction failed and hence small opening was made at fracture site to apply a towel clip and Kirschner wire as joystick to assist reduction. Patients were followed up for average duration of months (range 5-30 months). No single case of injury to great sephaneous vein and sephaneous nerve was detected. Average duration for fracture union was Page 64
4 Original Article VOL.9 NO. 2 ISSUE 34 APR - JUN weeks (range14-28weeks). Demographic profiles and outcome of each case are tabulated in table 1. Immediate post operative complication of wound infection was found in three patients; two superficial (case no 7, 16) and one (case no 4) deep wound infection. Case no. 7 was brought to hospital after 44 hours of fall injury from remote part of country with swollen leg and fracture blisters. He was operated after 10 days of injury once blisters and swelling settled down. During subsequent follow up to 18 weeks, fracture union was not progressing satisfactorily and hence, was subjected for percutaneous bone marrow injection at fracture site. Finally fracture got united at 28 weeks. In case no 4, wound was dry and non infected at time of discharge on fifth post operative day but came back with wound breakdown and exposed plate. He had a history of application of homemade herbal paste over the wound and fracture site. Both superficial wound infections healed with extended period of intravenous antibiotics but patient with wound breakdown needed repeated debridemet as well. Subsequent follow up was unremarkable in all these three cases. Two patients had union with valgus angulation of less than 5. No malunion was detected. One patient had ankle stiffness requiring extensive physiotherapy to regain range of movement. Implants were removed in eight patients. Six of them had malleolar skin irritation due to prominent hardware and in rest of two patients; implants were removed on request. No problems were encountered during removal of implants. DISCUSSION Distal diametaphyseal tibia fracture with or without intra articular extension is one of the difficult fractures to manage. None of the treatment options available perfectly fulfill requirements of fracture characteristics of distal diametaphyseal tibia. Distal tibia has got circular cross sectional area with thinner cortex as compare to triangular diaphysis with thicker cortex. So, intramedullary nail which is designed for tight interference fit at diaphysis cannot provide same stability at distal fracture. 3,16 Other potential complications of IMIL nailing are malunion (0-29%) and implant failure (5-39%). 1-3 ORIF with conventional plate which needs striping of periosteum is also not an ideal treatment option because tibia is subcutaneous bone and periosteum provides 2/3 rd of blood supply. Non union, delayed union and infection are reported with the range of % and % respectively with ORIF with plating. 4-7,17 Similarly external fixators as a definitive method of treatment for distal diametaphyseal tibia fracture are also reported with higher rate of infection, implant failure and malunion or non union and hence recommended only for temporary method of stabilization in open fracture with severe soft tissue injury. 1,18 With the development of technique of MIPO with LCP which preserve extraosseous blood supply, respect osteogenic fracture haematoma, biologically friendly and stable fixation method is available for distal diametaphyseal tibia fracture. Indirect reduction method and sub-cutaneous tunneling of the plate and application of locking screws with small skin incisions in MIPO technique prevents iatrogenic injury to vascular supply of the bone. 19 Unlike conventional plates, LCP is a friction independent self stable construct which provides both angular and axial stability and minimizes risk of secondary loss of reduction through a threaded interface between the screw heads and the plate body. 12 MIPO with LCP for distal diametaphyseal tibia fracture has been found to be an effective treatment option. 1,14,15,20-25 Table 2 shows comparison of current study with some of the previous studies. But unlike the present study, most of the previous studies have included both open and closed fractures and are retrospective study. Comparative studies with IMIL or conventional open techniques have found conflicting results with MIPO with LCP for distal diametaphyseal tibia fracture. Vallier et al. reported significantly more angular malalignment in distal diametaphyseal tibia fracture, treated with IMIL in comparison to those treated with plating (22 patients vs 2 patients, p=0.003) where as Guo et al. in a comparative study of extra articular distal diametaphyseal tibia fracture reported that patients treated with IMIL nailing had better function, alignment and American Orthopedic Foot Ankle score, though none of them were statistically significant where as operative time (81.33 vs minutes, p< 0.001) and radiation exposure (2.12 vs. 3 minutes, p< 0.001) was significantly more in LCP group and higher mean pain score was found in IMIL group. 6,8 Cheng et al. in a small sampled paired comparison (15 in each group) of MIPO and open technique with LCP found former is not statistically better in terms of union time (16.8 vs., 19.2 wks, p=0.737), recovery time to return to work (21.1 vs weeks, p=0.35) and functional results. 26 Kao et al. found no statistically significant advantages of LCP over conventional plate group. 27 In spite of use of MIPO with LCP as internal external fixators, anatomical reduction of the fracture by using indirect reduction maneuvers before applying the plate is very important surgical step. Malreduction and suboptimal pre contouring of the plate can result delayed union, non union, prominent hardware, malleolar skin irritation and pain. 23,24,26 In the present study, pain and malleolar skin irritation in six (30%) patients was common indication of implant removal. Other indications were difficulty of wearing shoes and cosmetic concern because of prominent hardware in skinny and thin patient (Fig. 2). Low profile metaphyseal LCP has been designed to reduce hardware prominence related complications but plates specifically designed according to measurement of adult distal tibia of western population may not perfectly match to other communities and often need change in pre contouring to avoid mismatch which in turn, can change the direction Page 65
5 Table 2. Comparison of current study with previous clinical series. Study No of fractures Study Method Fixation Outcomes Complications Ronga M et al. [1] 19 Retrospective MIPO Union: 18 (22.3 wks, range 12-24) Nonunion:1 No malunion ( 7 deformity or 1 cm LLD) Deep infection:3 Ahmad MA et al. [14} 18 Retrospective MIPO Union: 15 (21.2 wks) Delayed union: 3 Superficial wound infarction: 1 Chronic wound infection: 1 Implant failure: 1 Hasenbohehler E et al. [9} 32 (open fracture: 8) Retrospective MIPO Union: 29 ( 27.7 wks, range 24 60) Hazarika S et al. [21] 20 (open fracture: 8) Retrospective MIPO Union: 18 ( 28.5 wks, range, 9 68) Nonunion: 2 No malunion ( 5 deformity or 1 cm LLD) Plate bending (18 ): 1 Pseudoarthrosis: 2 Nonunion: 2 Delayed wound break down: 2 Wound infection: 1 Implant failure: 1 Secondary procedure: 2 Bahari S et al. [25] 42 (open fracture: 8) Prospective MIPO Union: 42 (22.4 wks) No malunion Superficial wound infection: 2 Deep infection: 1 Implant failure: 1 Collinge C et al.[15] 38 (open fracture: 8) Prospective MIPO Union: 38 (21 wks, range 9 48) Mushtaq A et al. [20] 21 (open fracture: 4) Prospective MIPO Union: 21( 5.5 months, range 3 13) Lau TW et al. [30] 48 (open fracture: 9) Retrospective MIPO Union: 47 ( 18.7 wks, range wks) Gupta RK et al.[23] 80 (open fracture:19) Retrospective MIPO : 71, Open: 9 Union: 77 (19 wks, range 16-32) Current study 20 Prospective MIPO Union: 20 (18.5 wks, range 14-28) Malunion ( 5 deformity) : 1 Secondary procedure: 3 Delayed union: 1 Non union :1 Wound infection: 2 Secondary procedure: 2 Delayed union: 5 Wound infection: 8 Secondary procedure:1 Delayed union :7 Non union: 3 Malunion ( 5 deformity or 1 cm LLD): 2 Wound infection:1 Wound breakdown: 2 Secondary procedure: 2 Delayed union :1 No malunion ( 5 deformity or 1 cm LLD) Superficial wound infection: 2 Deep infection: 1 Secondary procedure: 1 of screws in monoaxial type of locking compression plates. 23 Polyaxial locking plates can be an alternative when supramalleolar anatomy mismatch with pre contoured plate because it can provide choice of screw trajectories according to fracture pattern. 24 But there is very little clinical and biomechanical study of polyaxial locking plates for distal tibia. Indirect reduction of fracture under C arm control can be difficult at time. Various reduction maneuvers such as calcaneal pin traction, external fixators or mechanical distractors have been described to achieve reduction. 1,22 We used Kirschner wires (3 mm) as a joystick or a towel clip after making small opening at fracture site whenever reduction could not be achieved by mechanical traction. Concomitant fibula fracture also play the role in success of reduction especially when fracture is at same level of tibia. Some authors recommend fibula fixations before tibia fixation to achieve better tibial alignment and to prevent valgus malalignment but clear indications for fibula fixation are still lacking and controversial. 1,23,24,28 We did not routinely fix fibula unless it has involved syndesmosis. MIPO technique can restore alignment in high velocity distal diametaphyseal tibia fracture and patients can Figure 2. Fracture (AO/OTA type 43.A1) united (a) but clearly visible prominent hardware over skinny and thin patient (b). Page 66
6 Original Article VOL.9 NO. 2 ISSUE 34 APR - JUN 2011 expect predictable return of function. However, Collinge et al. reported increased secondary procedure rate like bone grafting for delayed union. 29 Rate of secondary procedures like iliac crest bone grafting or per cutaneous bone marrow injection for delayed union or non union or change of hardware has been reported 3.8% to as high as up to 35%. 23,29 In the current study, one patient required subcutaneous bone marrow injections as satisfactory callus was not visualized up to 16 weeks follow up. He subsequently had progressive callus formation. Because of sub cutaneous location, distal diametaphyseal tibia are prone to have gross swelling, skin injury and fracture blisters if the leg is left unsplinted for long time and injury-hospital arrival interval is prolonged. In the current series, 13 patients who had injury- surgery interval of > 3 days had average injury- hospital arrival interval hrs as compare to 8.86 hrs in seven patients who were operated within three days of injury. Our protocol for timing of surgery was to fix the fracture as early as possible unless associated with gross swelling or hindered by fracture blisters. But union time in our study was not affected whether patients were operated before or after three days of injury (17.29 ± 2.13 wks vs ± 2.99 wks, p=0.15). The average time for fracture union in the present study is comparable to other studies (Table 2). Hasenboehler et al. found MIPO with LCP though reliable for distal diametaphyseal tibia fracture can prolong union time in simple fracture pattern (43.A1-43.A3) when it was used only as a bridging plate. 9 Hence, percutaneous interfragmentary screw, independent to plate and LCP in a neutralization mode or application of LCP in a compression mode by utilizing non locking screw on one side of the fracture is recommended to avoid delay in fracture union. Though skin and soft tissue injury at the time of conventional osteosynthesis has been found to be significantly associated with higher rate of wound infection as compare to IMIL nailing, effect of same on MIPO with LCP has not been studied yet. 10 Lau et al. did not find fracture union time in MIPO to be affected by presence of late infections occurring after one month of complete wound healing. 30 Reported rate of wound infection varies between 2.6% to 14.6% depending upon whether open fracture are included in the study or not. The present study which included only closed fracture found three (15%) early wound infection. Two patients who had superficial wound infection improved with antibiotics but patient with wound breakdown and exposed implant had protracted post operative rehabilitation period requiring repeated wound debridemet and long hospital stay. Other potential complications like injury to sephaneous nerve and great sephaneous vein has been reported in cadaver studies and can be avoided by careful attention towards selection of skin incision site, dissection of vein, dissection of stab incision up to the plate and atraumatic placement of drill sleeve. 26,31 No case of sephaneous nerve and great sephaneous vein was found in the current study. Removal of LCP can be difficult because usual conical extraction devices may not be useful in locking screws when stripping of hexagonal recess or thread occurs. Cutting and bending of plate around the stripped screw has been suggested to remove the plates and screws but we did not encounter problems during removal of implants in all our eight cases. 23,32 CONCLUSION Distal diametaphyseal tibia fracture with or without intra articular extension is one of the difficult fractures to manage with all currently available treatment options. Fracture pattern, concomitant articular extension, condition of soft tissue are important factors to be considered before selection of fixation method. The present case series though small in number shows that MIPO with LCP is an effective treatment method in terms of union time and complications rate which is comparable to other studies. Implant prominence and its related complications because of mismatching of the implant contouring and supra malleolar anatomy especially in thin built patients or malreduction of fracture still remains a challenge. Prospective randomized controlled trial specially comparing newly available intramedullary nails which has various distal locking options is necessary to establish superiority of the technique. REFERENCES 1. Ronga M, Longo UG, Maffulli N. Minimally invasive locked plating of distal tibia fractures is safe and effective. Clin Orthop Relat Res 2010, 468: Mosheiff R, Safran O, Segal D, Liebergall M. The unreamed tibial nail in the treatment of distal metaphyseal fractures. Injury 1999,30: Kneifel T, Buckley R. A comparison of one versus two distal locking screws in tibial fractures treated with unreamed tibial nails: a prospective randomized clinical trial. Injury 1996, 27: Redfern DJ, Syed SU, Davies SJM. Fractures of the distal tibia: minimally invasive plate osteosynthesis. Injury 2004, 35: Apivatthakakul T, Phornphutkul C, Patumasutra S. Idea and innovation: Simple minimally invasive plate osteosynthesis (MIPO) instruments. Injury Extra 2009,40: Vallier HA, Le TT, Bedi A. Radiographic and clinical comparisons of distal tibia shaffractures (4 to 11 cm proximal to the plafond): plating versus intramedullary nailing. J Orthop Trauma 2008, 22: Yang SW, Tzeng HM, Chou YJ, Teng HP, Liu HH, Wong CY. Treatment of distal tibial metaphyseal fractures: Plating versus shortened intramedullary nailing. Injury 2006, 37: Guo JJ, Tang N, Yang HL, Tang TS. A prospective, randomised trial comparing closed intramedullary nailing with percutaneous plating in the treatment of distal metaphyseal fractures of the tibia. J Bone Joint Surg Br 2010, 92-B: Hasenboehler E, Rikli D, Babst R. Locking compression plate with minimally invasive plate osteosynthesis in diaphyseal and distal tibial fracture: a retrospective study of 32 patients. Injury 2007, 38: Page 67
7 10. Gun-Il Im, Suk-Kee Ta. Distal metaphyseal fractures of tibia: A prospective randomized trial of closed reduction and intramedullary nail versus open reduction and plate and screws fixation. J Trauma 2005,59: Watson JT, Moed BR, Karges DE, Cramer KE. Pilon fractures. Treatment protocol based on severity of soft tissue injury. Clin Orthop Relat Res 2000, 375: Wagner M, Frigg FR. Locked plating: Biomechanics and biology and locked plating: Clinical indications. Techniques in Orthopaedics 2007, 22(4) : Frigg R. Development of the locking compression plate. Injury Suppl 2003, 2:B6 B Ahmad MA, Sivaraman A, Zia A, Rai A, Patel AD. Percutaneous locking plates for fractures of the distal tibia: Our experience and a review of the literature. J Trauma 2010, doi: /TA.0b013e3181f140b3 15. Collinge C, Protzman R. Outcomes of minimally invasive plate osteosynthesis for metaphyseal distal tibia fractures. J Orthop Trauma 2010, 24: Trafton PG.Tibial Shaft Fracturs. In: Skeletal trauma. 4th edn. Edited by Browner DB, Jupiter JB, Levine AN, Trafton PG, Krettek C. Philadelphia: Suanders Elsevier; 2009: Megas P, Zouboulis P, Papadopoulos AX, Karageorgos A, Lambiris E. Distal tibial fractures and non-unions treated with shortened intramedullary nail. Inter Orthop 2003, 27: Joveniaux P, Ohl X, Harisboure A, Berrichi A, Labatut L, Simon P, Mainard D, Vix N, Dehoux E. Distal tibia fractures: management and complications of 101 cases. Inter Orthop 2010, 34: Borrelli J, Prickett W, Song E, Becker D, Ricci W. Extra osseous blood supply of the distal tibia and the effects of different plating techniques: Human cadaveric study. J Orthop Trauma 2002, 16: Mushtaq A, Shahid R, Asif M, Maqsood M. Distal tibial fracture fixation with locking compression plate (LCP) using the minimally invasive percutaneous osteosynthesis (MIPO) technique. Eur J Trauma Emerg Surg 2009, 35: Hazarika S, Chakravarthy J, Cooper J. Minimally invasive locking plate osteosynthesis for fractures of the distal tibia-results in 20 patients. Injury 2006, 37: Shanmugam C, Rahmatalla A, Maffulli N. Percutaneous fixation of distal tibial fractures using locking plates. Techniques in Orthopaedic 2007, 22(3): Gupta RK, Rohilla RK, Sangwan K, Singh V, Walia S. Locking plate fixation in distal metaphyseal tibial fractures: series of 79 patients. Inter Orthop 2010, 34: Gao H, Zhang CQ, Luo CF, Zhou ZB, Zeng BF. Fractures of the distal tibia treated with polyaxial locking plating. Clin Orthop Relat Res 2009, 467: Bahari S, Lenehan B, Khan H, Mcelwain JP. Minimally invasive percutaneous plate fixation of distal tibia fractures. Acta Orthop Belg 2007, 73: Cheng W, Li Y, Manyi W. Comparison study of two surgical options for distal tibia fracture-minimally invasive plate osteosynthesis vs. open reduction and internal fixation. Inter Orthop 2010, doi: / s Kao FC, Tu YK, Hsu KY, Wu CH, Yen Cy, Chou MC. Treatment of distal tibial fractures by minimally invasive percutaneous plate osteosynthesis of three different plates: Results and cost-effectiveness analysis. Formosan Journal of Musculoskeletal Disorders 2010, 1: Bedi A, Le TT, Karunakar MA. Surgical treatment of nonarticular distal tibia fractures. J Am Acad Orthop Surg 2006, 14: Collinge C, Kuper M, Larson K, Protzman R. Minimally invasive plating of high energy metaphyseal distal tibia fractures. J Orthop Trauma 2007, 21: Lau TW, Leung F, Chan CF, Chow SP. Wound complication of minimally invasive plate osteosynthesis in distal tibia fractures. Inter Orthop 2008, 32: Ozsoy MH, Tuccar E, Demiryurek D et al. Minimally invasive plating of the distal tibia: do we really sacrifice saphenous vein and nerve? A cadaver study. J Orthop Trauma 2009, 23(2): Bae JH, Oh JK, Oh CW, Hur CR. Technical difficulties of removal of locking screw after locking compression plating. Arch Orthop Trauma Surg 2009, 129:91-5. Page 68
Minimally Invasive Plate Osteosynthesis with Locking Compression Plate for Distal Diametaphyseal Tibia Fracture
 Minimally Invasive Plate Osteosynthesis with Locking Compression Plate for Distal Diametaphyseal Tibia Fracture Shrestha D, 1 Acharya BM, 2 Shrestha PM 3 1 Department of Orthopaedics and Traumatology Dhulikhel
Minimally Invasive Plate Osteosynthesis with Locking Compression Plate for Distal Diametaphyseal Tibia Fracture Shrestha D, 1 Acharya BM, 2 Shrestha PM 3 1 Department of Orthopaedics and Traumatology Dhulikhel
A study of MIPO by locking compression plate fixation in the management of distal tibial metaphyseal fractures
 International Journal of Research in Medical Sciences Venkateswarlu K et al. Int J Res Med Sci. 2015 Mar;3(3):675-679 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20150328
International Journal of Research in Medical Sciences Venkateswarlu K et al. Int J Res Med Sci. 2015 Mar;3(3):675-679 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20150328
A study of functional outcome of distal tibial extraarticular fracture fixed with locking compression plate using MIPPO technique
 2017; 1(3): 13-18 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2017; 1(3): 13-18 Received: 03-08-2017 Accepted: 04-09-2017 Dr. Somashekar Dr. Girish S Dr.
2017; 1(3): 13-18 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2017; 1(3): 13-18 Received: 03-08-2017 Accepted: 04-09-2017 Dr. Somashekar Dr. Girish S Dr.
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study on Surgical Management of Distal Tibial Fractures by Using Minimally Invasive Technique
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study on Surgical Management of Distal Tibial Fractures by Using Minimally Invasive Technique
Minimally Invasive Plate Osteosynthesis (MIPO) for Proximal and Distal Fractures of The Tibia: A Biological Approach
 http://dx.doi.org/10.5704/moj.1603.006 Minimally Invasive Plate Osteosynthesis (MIPO) for Proximal and Distal Fractures of The Tibia: A Biological Approach Gupta P, MS Orth, Tiwari A, MS Orth, Thora A,
http://dx.doi.org/10.5704/moj.1603.006 Minimally Invasive Plate Osteosynthesis (MIPO) for Proximal and Distal Fractures of The Tibia: A Biological Approach Gupta P, MS Orth, Tiwari A, MS Orth, Thora A,
A comparative study of locking plate by MIPO versus closed interlocking intramedullary nail in extraarticular distal tibia fractures
 2018; 4(3): 145-149 ISSN: 2395-1958 IJOS 2018; 4(3): 145-149 2018 IJOS www.orthopaper.com Received: 26-05-2018 Accepted: 27-06-2018 Kanachur Institute of Medical Sciences Mangalore University Road, Natekal,
2018; 4(3): 145-149 ISSN: 2395-1958 IJOS 2018; 4(3): 145-149 2018 IJOS www.orthopaper.com Received: 26-05-2018 Accepted: 27-06-2018 Kanachur Institute of Medical Sciences Mangalore University Road, Natekal,
Medico Research Chronicles
 Medico Research Chronicles ISSN NO. 2394-3971 DOI No. 10.26838/MEDRECH.2019.6.1.473 Contents available at: www.medrech.com OUTCOMES OF MINIMALLY INVASIVE PLATE OSTEOSYNTHESIS (MIPO) FOR DIAMETAPHYSEAL
Medico Research Chronicles ISSN NO. 2394-3971 DOI No. 10.26838/MEDRECH.2019.6.1.473 Contents available at: www.medrech.com OUTCOMES OF MINIMALLY INVASIVE PLATE OSTEOSYNTHESIS (MIPO) FOR DIAMETAPHYSEAL
Outcome of minimally invasive plate osteosynthesis (MIPO) technique in distal tibial fracture
 2017; 3(3): 10-14 ISSN: 2395-1958 IJOS 2017; 3(3): 10-14 2017 IJOS www.orthopaper.com Received: 03-05-2017 Accepted: 04-06-2017 Yogesh C Patel Professor and Head of Unit, Arvind K Jangid Chirag B Patel
2017; 3(3): 10-14 ISSN: 2395-1958 IJOS 2017; 3(3): 10-14 2017 IJOS www.orthopaper.com Received: 03-05-2017 Accepted: 04-06-2017 Yogesh C Patel Professor and Head of Unit, Arvind K Jangid Chirag B Patel
Minimally Invasive Plating of Fractures:
 Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Minimally invasive plate osteosynthesis for distal tibial fractures
 Journal of Orthopaedic Surgery 2014;22(3):299-303 Minimally invasive plate osteosynthesis for distal tibial fractures Pramod Devkota, 1 Javed A Khan, 2 Suman K Shrestha, 2 Balakrishnan M Acharya, 2 Nabeesman
Journal of Orthopaedic Surgery 2014;22(3):299-303 Minimally invasive plate osteosynthesis for distal tibial fractures Pramod Devkota, 1 Javed A Khan, 2 Suman K Shrestha, 2 Balakrishnan M Acharya, 2 Nabeesman
Plate Fixation Options
 Distal tibia extra-articular fractures can be difficult to treat Tenuous soft tissue Complex fracture patterns Plate Fixation Options Medial plating: Minimally invasive approach Technical ease Anterolateral
Distal tibia extra-articular fractures can be difficult to treat Tenuous soft tissue Complex fracture patterns Plate Fixation Options Medial plating: Minimally invasive approach Technical ease Anterolateral
Outcome of the Treatment of Distal Tibia Fractures by Minimal Invasive Locked Plate A Short Term Study
 ISSN: 2091-2331 (PRINT) 2091-234X (ONLINE) Original Article Journal of Nobel Medical College Available Online: www.nepjol.info, www.nobelmedicalcollege.com.np Volume 6, Number 1, Issue 10, January-June
ISSN: 2091-2331 (PRINT) 2091-234X (ONLINE) Original Article Journal of Nobel Medical College Available Online: www.nepjol.info, www.nobelmedicalcollege.com.np Volume 6, Number 1, Issue 10, January-June
Techique. Results. Discussion. Materials & Methods. Vol. 2 - Year 1 - December 2005
 to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
Minimally Invasive Percutaneous Plate Osteosynthesis Does Not Increase Complication Rates in Extra-Articular Distal Tibial Fractures
 Send Orders for Reprints to reprints@benthamscience.ae The Open Orthopaedics Journal, 2015, 9, 73-77 73 Open Access Minimally Invasive Percutaneous Plate Osteosynthesis Does Not Increase Complication Rates
Send Orders for Reprints to reprints@benthamscience.ae The Open Orthopaedics Journal, 2015, 9, 73-77 73 Open Access Minimally Invasive Percutaneous Plate Osteosynthesis Does Not Increase Complication Rates
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
Percutaneous Screw Fixation of Distal Tibia Fractures Functional Results in Sixteen Patients
 Open Access Macedonian Journal of Medical Sciences. 2014 Jun 15; 2(2):229-233. http://dx.doi.org/10.3889/oamjms.2014.036 Clinical Science Percutaneous Screw Fixation of Distal Tibia Fractures Functional
Open Access Macedonian Journal of Medical Sciences. 2014 Jun 15; 2(2):229-233. http://dx.doi.org/10.3889/oamjms.2014.036 Clinical Science Percutaneous Screw Fixation of Distal Tibia Fractures Functional
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
ROTATIONAL PILON FRACTURES
 CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
Outcome of extra articular distal Shaft of tibia fracture treated by reamed interlock nail
 Original article: Outcome of extra articular distal Shaft of tibia fracture treated by reamed interlock nail 1Dr. Neil Rohra, 2 Dr.RameshPanchal 1Resident, Dept. Of Orthopedics, PS Medical College,Karamsad,Anand,Gujarat.
Original article: Outcome of extra articular distal Shaft of tibia fracture treated by reamed interlock nail 1Dr. Neil Rohra, 2 Dr.RameshPanchal 1Resident, Dept. Of Orthopedics, PS Medical College,Karamsad,Anand,Gujarat.
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3
 OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Plate vs Nail for Distal Tibia Fxs
 Plate vs Nail for Distal Tibia Fxs Frank A. Liporace, MD Associate Professor Dept. of Orthopaedics NYU / HJD Chief Dept. Of Orthopaedics JCMC / RWJBH ??? Controversy??? Nails Minimal invasive Low blood
Plate vs Nail for Distal Tibia Fxs Frank A. Liporace, MD Associate Professor Dept. of Orthopaedics NYU / HJD Chief Dept. Of Orthopaedics JCMC / RWJBH ??? Controversy??? Nails Minimal invasive Low blood
Minimally invasive percutaneous plate fixation of distal tibia fractures
 Acta Orthop. Belg., 2007, 73, 635-640 ORIGINAL STUDY Minimally invasive percutaneous plate fixation of distal tibia fractures Syah BAHARI, Brian LENEHAN, Hamad KHAN, John P. MCELWAIN From Adelaide and
Acta Orthop. Belg., 2007, 73, 635-640 ORIGINAL STUDY Minimally invasive percutaneous plate fixation of distal tibia fractures Syah BAHARI, Brian LENEHAN, Hamad KHAN, John P. MCELWAIN From Adelaide and
Distal Femur Fractures in The Elderly The Ideal Construct
 Distal Femur Fractures in The Elderly The Ideal Construct Tak-Wing Lau Department of Orthopaedics and Traumatology Queen Mary Hospital The University of Hong Kong Singapore Trauma 2015 Trauma Through the
Distal Femur Fractures in The Elderly The Ideal Construct Tak-Wing Lau Department of Orthopaedics and Traumatology Queen Mary Hospital The University of Hong Kong Singapore Trauma 2015 Trauma Through the
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES
 BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
Tibial Shaft Fractures
 Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
LCP Distal Tibia Plate
 Surgical Technique LCP Locking Compression Plate Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF Table of contents Indications 3 Implants/Instruments 5 Surgical
Surgical Technique LCP Locking Compression Plate Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF Table of contents Indications 3 Implants/Instruments 5 Surgical
The study of distal ¼ diaphyseal extra articular fractures of humerus treated with antegrade intramedullary interlocking nailing
 2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
EVOS MINI with IM Nailing
 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Original Research Article
 TREATMENT OF COMPLEX TIBIAL FRACTURES TYPES V AND VI OF SCHATZKER CLASSIFICATION BY DOUBLE PLATE FIXATION WITH SINGLE ANTERIOR INCISION Thoguluva Chandra Sekaran Prem Kumar 1, M. N. Karthi 2 1Senior Assistant
TREATMENT OF COMPLEX TIBIAL FRACTURES TYPES V AND VI OF SCHATZKER CLASSIFICATION BY DOUBLE PLATE FIXATION WITH SINGLE ANTERIOR INCISION Thoguluva Chandra Sekaran Prem Kumar 1, M. N. Karthi 2 1Senior Assistant
AO / Synthes Proximal Posterior Medial Tibia Plate. Tibial Plateau Fx. Osteosynthesis
 Tibial Plateau Fx. Osteosynthesis Articular Fractures Osteosynthesis Characteristics of the LCP system LCP 3.5 system LCP 4.5 system Many different traditional plates (small, large) Lag screws Rafting
Tibial Plateau Fx. Osteosynthesis Articular Fractures Osteosynthesis Characteristics of the LCP system LCP 3.5 system LCP 4.5 system Many different traditional plates (small, large) Lag screws Rafting
VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 Technique Guide VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction VA-LCP Anterior
Technique Guide VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction VA-LCP Anterior
CURRENT TREATMENT OPTIONS
 CURRENT TREATMENT OPTIONS Fix single column or both: Always fix both. A study by Svend-Hansen corroborated the poor results associated with isolated medial malleolar fixation in bimalleolar ankle fractures.
CURRENT TREATMENT OPTIONS Fix single column or both: Always fix both. A study by Svend-Hansen corroborated the poor results associated with isolated medial malleolar fixation in bimalleolar ankle fractures.
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Section: Orthopaedics. Original Article INTRODUCTION
 DOI: 0.2276/aimdr.208.4.3.OR2 Original Article ISSN (O):239-2822; ISSN (P):239-284 A Comparative Study of Operative Management of Internal Fixation of Closed Tibial Plateau Fracture by Plates with Screws
DOI: 0.2276/aimdr.208.4.3.OR2 Original Article ISSN (O):239-2822; ISSN (P):239-284 A Comparative Study of Operative Management of Internal Fixation of Closed Tibial Plateau Fracture by Plates with Screws
3.5 mm LCP Distal Tibia T-Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Distal Tibia T-Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Distal Tibia T-Plates 2 AO Principles 4 Indications
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Distal Tibia T-Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Distal Tibia T-Plates 2 AO Principles 4 Indications
Vasu Pai FRACS, MCh, MS, Nat Board Ortho Surgeon Gisborne
 Vasu Pai FRACS, MCh, MS, Nat Board Ortho Surgeon Gisborne FRACTURE MANAGEMENT I Simple closed fracture : Complete or Incomplete Stable or unstable II Open fracture III Multiple fracture IV Polytrauma Fractures
Vasu Pai FRACS, MCh, MS, Nat Board Ortho Surgeon Gisborne FRACTURE MANAGEMENT I Simple closed fracture : Complete or Incomplete Stable or unstable II Open fracture III Multiple fracture IV Polytrauma Fractures
Segmental tibial fractures treated with unreamed interlocking nail A prospective study
 2017; 3(2): 714-719 ISSN: 2395-1958 IJOS 2017; 3(2): 714-719 2017 IJOS www.orthopaper.com Received: 13-02-2017 Accepted: 14-03-2017 Ashok Singhvi Hemant Jain Siddharth Jauhar Kishore Raichandani Segmental
2017; 3(2): 714-719 ISSN: 2395-1958 IJOS 2017; 3(2): 714-719 2017 IJOS www.orthopaper.com Received: 13-02-2017 Accepted: 14-03-2017 Ashok Singhvi Hemant Jain Siddharth Jauhar Kishore Raichandani Segmental
No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture
 CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
Osteosynthesis involving a joint Thomas P Rüedi
 Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
Osteosynthesis involving a joint Thomas P Rüedi How to use this handout? The left column contains the information given during the lecture. The column at the right gives you space to make personal notes.
management of sports injuries
 Br J Sp Med 1991; 25(4) Internal fixation of closed tibial fractures for the management of sports injuries A. Abdel-Salam FRCS, K. S. Eyres* FRCS and J. Cleary FRCS Department of Orthopaedics, Huddersfield
Br J Sp Med 1991; 25(4) Internal fixation of closed tibial fractures for the management of sports injuries A. Abdel-Salam FRCS, K. S. Eyres* FRCS and J. Cleary FRCS Department of Orthopaedics, Huddersfield
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system.
 LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
Principles of intramedullary nailing. Management for ORP
 Principles of intramedullary nailing Eakachit Sikarinklul,MD Basic Principles of Fracture Management for ORP Bangkok Medical Center Bangkok, 22-24 July 2016 Learning outcomes At the end of this lecture
Principles of intramedullary nailing Eakachit Sikarinklul,MD Basic Principles of Fracture Management for ORP Bangkok Medical Center Bangkok, 22-24 July 2016 Learning outcomes At the end of this lecture
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique
 PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
JMSCR Vol 3 Issue 9 Page September 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x DOI: http://dx.doi.org/10.535/jmscr/v3i9.08 Treatment for Lower One Third Fractures of Tibia by Interlocking Nailing Authors Suresh Reddy.S
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x DOI: http://dx.doi.org/10.535/jmscr/v3i9.08 Treatment for Lower One Third Fractures of Tibia by Interlocking Nailing Authors Suresh Reddy.S
Orthopedics in Motion Tristan Hartzell, MD January 27, 2016
 Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Primary internal fixation of fractures of both bones forearm by intramedullary nailing
 Original article 21 Primary internal fixation of fractures of both bones forearm by intramedullary nailing Nepal Medical College and Teaching Hospital, Kathmandu, Nepal Correspondenc to: Dr R P Singh,
Original article 21 Primary internal fixation of fractures of both bones forearm by intramedullary nailing Nepal Medical College and Teaching Hospital, Kathmandu, Nepal Correspondenc to: Dr R P Singh,
Technique Guide. LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System.
 Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Ankle Fractures in the Elderly: How to Deal with Poor Bone Quality
 : How to Deal with Poor Bone Quality Richard T. Laughlin, MD Professor of Orthopaedic Surgery University of Cincinnati College of Medicine No disclosures relative to this presentation acknowledgement Some
: How to Deal with Poor Bone Quality Richard T. Laughlin, MD Professor of Orthopaedic Surgery University of Cincinnati College of Medicine No disclosures relative to this presentation acknowledgement Some
ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS
 Bahrain Medical Bulletin, Volume 17, Number 2, June 1995 Original ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS Saleh W. Al-Harby, FRCS(Glasg)* This is a prospective study of
Bahrain Medical Bulletin, Volume 17, Number 2, June 1995 Original ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS Saleh W. Al-Harby, FRCS(Glasg)* This is a prospective study of
A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of The Tibia
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 17 Number 2 A Clinical Study For Evaluation Of Results Of Closed Interlocking Nailing Of Fractures Of The Shaft Of R Gupta, T Motten, N Kalsotra,
LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures.
 LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures. Surgical Technique This publication is not intended for distribution in the
LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures. Surgical Technique This publication is not intended for distribution in the
Pilon Fractures Pearls of Treatment Steven Steinlauf, MD The Orthopaedic Foot and Ankle Institute of South Florida CSOT November 2017, Tampa
 Pilon Fractures Pearls of Treatment Steven Steinlauf, MD The Orthopaedic Foot and Ankle Institute of South Florida CSOT November 2017, Tampa Disclosures No relevant disclosures There is more literature
Pilon Fractures Pearls of Treatment Steven Steinlauf, MD The Orthopaedic Foot and Ankle Institute of South Florida CSOT November 2017, Tampa Disclosures No relevant disclosures There is more literature
OBSOLETED. LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Surgical Technique LCP Small Fragment System This publication
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Surgical Technique LCP Small Fragment System This publication
Minimally invasive osteosynthesis of adult tibia fractures by means of rigid fixation with anatomic locked plates
 Strat Traum Limb Recon (2013) 8:103 109 DOI 10.1007/s11751-013-0164-9 ORIGINAL ARTICLE Minimally invasive osteosynthesis of adult tibia fractures by means of rigid fixation with anatomic locked plates
Strat Traum Limb Recon (2013) 8:103 109 DOI 10.1007/s11751-013-0164-9 ORIGINAL ARTICLE Minimally invasive osteosynthesis of adult tibia fractures by means of rigid fixation with anatomic locked plates
Technique Guide. 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
Technique Guide. 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
Minimally Invasive Osteosynthesis of Distal Tibia Fractures using Anterolateral Locking Plate
 doi: http://dx.doi.org/10.5704/moj.1811.008 Minimally Invasive Osteosynthesis of Distal Tibia Fractures using Anterolateral Locking Plate Choudhari P, MS Ortho, Padia D, MBBS Department of Orthopaedics,
doi: http://dx.doi.org/10.5704/moj.1811.008 Minimally Invasive Osteosynthesis of Distal Tibia Fractures using Anterolateral Locking Plate Choudhari P, MS Ortho, Padia D, MBBS Department of Orthopaedics,
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Intramedullary fibular fixation in the operative management of fractures of the distal tibia and fibula
 Royal Liverpool & Broadgreen University Hospitals NHS Foundation Trust Intramedullary fibular fixation in the operative management of fractures of the distal tibia and fibula Michael Smith MBChB, Zuned
Royal Liverpool & Broadgreen University Hospitals NHS Foundation Trust Intramedullary fibular fixation in the operative management of fractures of the distal tibia and fibula Michael Smith MBChB, Zuned
Locked Plating: Clinical Indications
 Techniques in Orthopaedics 22(3):181 185 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Clinical Indications Kyle F. Dickson, M.D., M.B.A., John Munz, M.D. Summary: As shown in the previous article,
Techniques in Orthopaedics 22(3):181 185 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Clinical Indications Kyle F. Dickson, M.D., M.B.A., John Munz, M.D. Summary: As shown in the previous article,
A CASE STUDY OF DISTAL TIBIAL FRACTURES MANAGED WITH LOCKING COMPRESSION PLATE USING MIPO TECHNIQUE DISSERTATION SUBMITTED FOR M.S.
 A CASE STUDY OF DISTAL TIBIAL FRACTURES MANAGED WITH LOCKING COMPRESSION PLATE USING MIPO TECHNIQUE DISSERTATION SUBMITTED FOR M.S. DEGREE (BRANCH II - ORTHOPAEDIC SURGERY) APRIL 2015 THE TAMILNADU DR.
A CASE STUDY OF DISTAL TIBIAL FRACTURES MANAGED WITH LOCKING COMPRESSION PLATE USING MIPO TECHNIQUE DISSERTATION SUBMITTED FOR M.S. DEGREE (BRANCH II - ORTHOPAEDIC SURGERY) APRIL 2015 THE TAMILNADU DR.
PRONATION-ABDUCTION FRACTURES
 C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
C H A P T E R 1 2 PRONATION-ABDUCTION FRACTURES George S. Gumann, DPM (The opinions of the author should not be considered as reflecting official policy of the US Army Medical Department.) Pronation-abduction
COMPARATIVE STUDY OF MANAGEMENT OF DIAPHYSEAL FEMUR FRACTURE WITH INTRAMEDULLARY INTERLOCKING NAIL AND K. NAIL
 International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 15 No. 3 Apr. 2016, pp. 560-564 2016 Innovative Space of Scientific Research Journals http://www.ijias.issr-journals.org/ COMPARATIVE
International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 15 No. 3 Apr. 2016, pp. 560-564 2016 Innovative Space of Scientific Research Journals http://www.ijias.issr-journals.org/ COMPARATIVE
Original Research Paper
 Original Research Paper Medical Science Evaluation of Functional Outcome Following Minimal Invasive Surgery in Treatment of Distal Tibial Fractures-A Prospective Clinical Study Dr Sanjeev Kansotiya Dr
Original Research Paper Medical Science Evaluation of Functional Outcome Following Minimal Invasive Surgery in Treatment of Distal Tibial Fractures-A Prospective Clinical Study Dr Sanjeev Kansotiya Dr
Clinical. Solutions. Synthes Solutions. Foot and Ankle.
 Clinical Solutions Foot and Ankle. Foot and Ankle. Fractures of the tibial shaft Fractures of the distal fibula Fractures of the distal tibia Fractures and osteotomies of the calcaneus Arthrodesis Fractures,
Clinical Solutions Foot and Ankle. Foot and Ankle. Fractures of the tibial shaft Fractures of the distal fibula Fractures of the distal tibia Fractures and osteotomies of the calcaneus Arthrodesis Fractures,
Diaphyseal Humerus Fractures. OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD
 Diaphyseal Humerus Fractures OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD OBJECTIVES TREATMENT OPTIONS SURGICAL INDICATIONS CONTROVERSIES IN MANAGEMENT Humerus Fractures Treatment Goals: Functional
Diaphyseal Humerus Fractures OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD OBJECTIVES TREATMENT OPTIONS SURGICAL INDICATIONS CONTROVERSIES IN MANAGEMENT Humerus Fractures Treatment Goals: Functional
PediLoc 3.5mm and 4.5mm Bowed Femur Plate Surgical Technique
 PediLoc 3.5mm and 4.5mm Bowed Femur Plate Surgical Technique 2957 Bow Broch_REV_B.indd 1 2/10/11 12:47 PM Surgical Technique Bowed Femur Plate The technique description herein is made available to the
PediLoc 3.5mm and 4.5mm Bowed Femur Plate Surgical Technique 2957 Bow Broch_REV_B.indd 1 2/10/11 12:47 PM Surgical Technique Bowed Femur Plate The technique description herein is made available to the
Outcome of Treatment of Nonunion Tibial Shaft Fracture by Intramedullary Interlocking Nail augmentated with Autogenous Cancellous Bone Graft.
 Original Article Nepal Med Coll J 2014; 16(1): 58-62 Outcome of Treatment of Nonunion Tibial Shaft Fracture by Intramedullary Interlocking Nail augmentated with Autogenous Cancellous Bone Graft. Shah SB,
Original Article Nepal Med Coll J 2014; 16(1): 58-62 Outcome of Treatment of Nonunion Tibial Shaft Fracture by Intramedullary Interlocking Nail augmentated with Autogenous Cancellous Bone Graft. Shah SB,
Tibial plateau fractures: four years review at B&B Hospital
 Kathmandu University Medical Journal (2004) Vol. 2, No. 4, Issue 8, 315-323 Original Article Tibial plateau fractures: four years review at B&B Hospital Shrestha BK 1, Bijukachhe B 2, Rajbhandary T 2,
Kathmandu University Medical Journal (2004) Vol. 2, No. 4, Issue 8, 315-323 Original Article Tibial plateau fractures: four years review at B&B Hospital Shrestha BK 1, Bijukachhe B 2, Rajbhandary T 2,
Study of Evaluation of Lateral Surgical Approach for Diaphyseal Fractures of Distal 2/3rd of Radius at a Tertiary Care Teaching Centre
 Original article : Study of Evaluation of Lateral Surgical Approach for Diaphyseal Fractures of Distal 2/3rd of Radius at a Tertiary Care Teaching Centre Chandra Prakash Singh Associate Professor, Department
Original article : Study of Evaluation of Lateral Surgical Approach for Diaphyseal Fractures of Distal 2/3rd of Radius at a Tertiary Care Teaching Centre Chandra Prakash Singh Associate Professor, Department
Evaluation of the functional outcome in open tibial fractures managed with an Ilizarov fixator as a primary and definitive treatment modality
 2017; 3(2): 436-440 ISSN: 2395-1958 IJOS 2017; 3(2): 436-440 2017 IJOS www.orthopaper.com Received: 05-02-2017 Accepted: 06-03-2017 Dr. SK Irfan Ali Assistant Professor, Dr. Sujai S Associate Professor,
2017; 3(2): 436-440 ISSN: 2395-1958 IJOS 2017; 3(2): 436-440 2017 IJOS www.orthopaper.com Received: 05-02-2017 Accepted: 06-03-2017 Dr. SK Irfan Ali Assistant Professor, Dr. Sujai S Associate Professor,
Technique Guide. LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction LCP Distal Fibula Plates 2 AO Principles 4 Indications 5 Surgical Technique
Technique Guide LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction LCP Distal Fibula Plates 2 AO Principles 4 Indications 5 Surgical Technique
Locking Ankle Plating System. Surgical Technique
 Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Distal third tibia fractures treated with interlocking intramedullary nail
 Original Article Nepal Med Coll J 2015; 17(1-2): 78-82 Distal third tibia fractures treated with interlocking intramedullary nail Sharma S, Pradhan RL, Khanal KR, Rijal KP, Lakhey S, Pandey BK, Manandhar
Original Article Nepal Med Coll J 2015; 17(1-2): 78-82 Distal third tibia fractures treated with interlocking intramedullary nail Sharma S, Pradhan RL, Khanal KR, Rijal KP, Lakhey S, Pandey BK, Manandhar
Surgical Technique. Fibula Rod System
 Surgical Technique Fibula Rod System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve patient
Surgical Technique Fibula Rod System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve patient
Angular Malalignment in Subtrochanteric and Proximal Shaft Femur Fractures after Intramedullary Nailing using SIGN Nails
 Angular Malalignment in Subtrochanteric and Proximal Shaft Femur Fractures after Intramedullary Nailing using SIGN Nails Rolando Junior L. Torres, MD Jeremiah R. Morales, MD, FPOA Subtrochanteric Femur
Angular Malalignment in Subtrochanteric and Proximal Shaft Femur Fractures after Intramedullary Nailing using SIGN Nails Rolando Junior L. Torres, MD Jeremiah R. Morales, MD, FPOA Subtrochanteric Femur
Fibula Rod System. Lateral Malleolus Fracture Indications:
 Fibula Rod System Fibula Rod System Since 1988, Acumed has been designing solutions for the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy has been to know
Fibula Rod System Fibula Rod System Since 1988, Acumed has been designing solutions for the demanding situations facing orthopaedic surgeons, hospitals and their patients. Our strategy has been to know
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
Surgical Technique. Ankle Plating System
 Surgical Technique Ankle Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve
Surgical Technique Ankle Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve
Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate
 Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique 1 Zimmer MIS
Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer MIS Periarticular 3.5mm Proximal Tibial Locking Plate Surgical Technique 1 Zimmer MIS
A gross anatomic study of distal tibia and fibula for single-incision approach
 Ma et al. Journal of Orthopaedic Surgery and Research 2014, 9:28 RESEARCH ARTICLE Open Access A gross anatomic study of distal tibia and fibula for single-incision approach Hui Ma 1, Jie Zhao 2, Baoqing
Ma et al. Journal of Orthopaedic Surgery and Research 2014, 9:28 RESEARCH ARTICLE Open Access A gross anatomic study of distal tibia and fibula for single-incision approach Hui Ma 1, Jie Zhao 2, Baoqing
Study of Ender s Nailing in Paediatric Tibial Shaft Fractures
 Study of Ender s Nailing in Paediatric Tibial Shaft Fractures Dr. Himanshu G. Ladani 1* 1 Ex. Assistant Professor of Orthopaedics, M.P.Shah Medical College, Jamnagar, Gujarat. ABSTRACT Background: Closed
Study of Ender s Nailing in Paediatric Tibial Shaft Fractures Dr. Himanshu G. Ladani 1* 1 Ex. Assistant Professor of Orthopaedics, M.P.Shah Medical College, Jamnagar, Gujarat. ABSTRACT Background: Closed
Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Conflict of Interest 9/24/2015
 Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Cory Collinge, MD Professor of Orthopedic Surgery Vanderbilt University Medical Center Nashville, TN Conflict of Interest Consultant: Smith
Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Cory Collinge, MD Professor of Orthopedic Surgery Vanderbilt University Medical Center Nashville, TN Conflict of Interest Consultant: Smith
TIBIAXYS ANKLE FUSION
 TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia.
 LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia. LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia.
LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia. LISS DF and LISS PLT. Less Invasive Stabilization Systems for Distal Femur and Proximal Lateral Tibia.
tep Ankle Fracture Plating System
 tep Response Ortho is a global orthopaedic trauma solutions manufacturer offering premium products created under its founding principles of innovation, excellence by design, and functional superiority.
tep Response Ortho is a global orthopaedic trauma solutions manufacturer offering premium products created under its founding principles of innovation, excellence by design, and functional superiority.
Diabetics. Referred for management of complex pilon fracture? 5/10/2017. Pilon Fractures: Exfix as definitive treatment (DM?)
 Pilon Fractures: Exfix as definitive treatment (DM?) Nirmal C Tejwani, MD Professor, NYU Langone Orthopedics Chief of Trauma, Bellevue Hospital, New York, NY 29 th Annual Orthopaedic Trauma Meeting May
Pilon Fractures: Exfix as definitive treatment (DM?) Nirmal C Tejwani, MD Professor, NYU Langone Orthopedics Chief of Trauma, Bellevue Hospital, New York, NY 29 th Annual Orthopaedic Trauma Meeting May
FUNCTIONAL OUTCOME OF PROXIMAL TIBIA EXTR-ARTICULAR FRACTURES TREATED WITH LOCKING COMPRESSION PLATING
 FUNCTIONAL OUTCOME OF PROXIMAL TIBIA EXTR-ARTICULAR FRACTURES TREATED WITH LOCKING COMPRESSION PLATING Original Article Orthopaedics Pradip B. Patil 1, Dhanish V. Mehendiratta 2, S.A. Lad 3, Rishi K. Doshi
FUNCTIONAL OUTCOME OF PROXIMAL TIBIA EXTR-ARTICULAR FRACTURES TREATED WITH LOCKING COMPRESSION PLATING Original Article Orthopaedics Pradip B. Patil 1, Dhanish V. Mehendiratta 2, S.A. Lad 3, Rishi K. Doshi
Treatment of Diaphysio-Metaphyseal Fracture of Tibia by Intramedullary Nail in Combination with Poller Screw
 Research Article imedpub Journals http://www.imedpub.com DOI: 10.4172/2469-6684.10001 Treatment of Diaphysio-Metaphyseal Fracture of Tibia by Intramedullary Nail in Combination with Poller Screw Ram Kewal
Research Article imedpub Journals http://www.imedpub.com DOI: 10.4172/2469-6684.10001 Treatment of Diaphysio-Metaphyseal Fracture of Tibia by Intramedullary Nail in Combination with Poller Screw Ram Kewal
Cost and Time Considerations: Are Minifragment Plates Worth It? Disclosure. More Disclosures. Are minifragment plates worth it? it depends!
 Cost and Time Considerations: Are Minifragment Plates Worth It? Andrew Choo, MD Vumedi Webinar November 15, 2016 Disclosure Paid speaker: Depuy Synthes More Disclosures Price quotes are estimates only!
Cost and Time Considerations: Are Minifragment Plates Worth It? Andrew Choo, MD Vumedi Webinar November 15, 2016 Disclosure Paid speaker: Depuy Synthes More Disclosures Price quotes are estimates only!
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System.
 LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
Comparing the Techniques for Management of Closed Tibial Fractures
 Comparing the Techniques for Management of Closed Tibial Fractures Dr Bareera Rehman 1 Dr Samee Javed Bhatti 2 Dr Zia Ur Rehman 3 Muhammad Zeeshan 4 1.House officer Nishtar Hospital Multan 2.Medical Officer
Comparing the Techniques for Management of Closed Tibial Fractures Dr Bareera Rehman 1 Dr Samee Javed Bhatti 2 Dr Zia Ur Rehman 3 Muhammad Zeeshan 4 1.House officer Nishtar Hospital Multan 2.Medical Officer
LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system.
 LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 Technique Guide LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction LCP Superior Clavicle
Technique Guide LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction LCP Superior Clavicle
Increasing surgical freedom Restoring patient function
 Increasing surgical freedom Restoring patient function Fracture specific plating solutions for the most common tibia and fibula fractures Frequency of fracture occurrences* 66% 61% 36% 36% 28% 14% 20%
Increasing surgical freedom Restoring patient function Fracture specific plating solutions for the most common tibia and fibula fractures Frequency of fracture occurrences* 66% 61% 36% 36% 28% 14% 20%
Results of distal femur locking plate in communited distal femur fractures
 2018; 4(2): 231-235 ISSN: 2395-1958 IJOS 2018; 4(2): 231-235 2018 IJOS www.orthopaper.com Received: 08-02-2018 Accepted: 11-03-2018 Dr. Hemeshwar Harshwardhan Dr. Arun Kumar Rajpurohit Results of distal
2018; 4(2): 231-235 ISSN: 2395-1958 IJOS 2018; 4(2): 231-235 2018 IJOS www.orthopaper.com Received: 08-02-2018 Accepted: 11-03-2018 Dr. Hemeshwar Harshwardhan Dr. Arun Kumar Rajpurohit Results of distal
Treatment of ipsilateral femoral neck and shaft fractures. Mohamed E. Habib, Yasser S. Hannout, and Ahmed F. Shams
 Treatment of ipsilateral femoral neck and shaft fractures Mohamed E. Habib, Yasser S. Hannout, and Ahmed F. Shams Department of Orthopedic Surgery, Faculty of Medicine, University of El Minoufiya, Egypt
Treatment of ipsilateral femoral neck and shaft fractures Mohamed E. Habib, Yasser S. Hannout, and Ahmed F. Shams Department of Orthopedic Surgery, Faculty of Medicine, University of El Minoufiya, Egypt
