Comparative Study of the Efficacy of Titanium Lag Screw and Titanium Miniplates for Internal Fixation of Anterior Mandibular Fractures
|
|
|
- Natalie Dennis
- 5 years ago
- Views:
Transcription
1 Original Article Print ISSN: Online ISSN: X DOI: /ijss/2017/210 Comparative Study of the Efficacy of Titanium Lag Screw and Titanium Miniplates for Internal Fixation of Anterior Mandibular Fractures Ranvijay 1, Ajoy Kumar Shahi 2, Mandeep Singh 3 1 Consultant Oral and Maxillofacial Surgeon, Patna, Bihar, India, 2 Reader, Department of Oral and Maxillofacial Surgery, Rajendra Institute of Medical Sciences, Ranchi, Jharkhand, India, 3 Professor, Department of Oral and Maxillofacial Surgery, Buddha Institute of Dental Sciences and Hospital, Patna, Bihar, India Abstract Introduction: The maxillofacial skeleton injuries occur due to a variety of causes, such as road traffic accidents, and sports injuries. The mandible is the second most commonly fractured bone of the maxillofacial skeleton because of its position and prominence. Although there is wide variance in the reported percentage of fracture of the anterior mandible (symphysis and parasymphysis), aggregate analysis places this at approximately 17% of all mandibular fractures. Materials and Methods: This study was conducted on 24 patients with clinical and radiological evidence of the anterior mandibular fracture. The patient was treated with two groups; (n - 12) treated with titanium lag screw (2.5 mm lag screw); Group B (n - 12) treated with titanium miniplates (2 mm miniplates). Clinical and radiological evaluations were made at 6 months postoperatively. Intraoperatively, duration of surgery was measured from the time incision was placed till the closure of wound. Results: The results of our study suggest that there were no major differences in stability with lag screw and miniplates. Lag screws have the added advantage of achieving interfragmentary compression and stability with a minimum of implant material. The lag screw principle offers the advantages of fixation using minimal hardware, functional stability, is associated with minimal inflammatory complications and functional restriction, and has a lower incidence of infection when considering the treatment of linear, noncomminuted symphyseal region fractures. The procedure, however, requires more skill and expertise. Conclusion: The choice of suitable osteosynthesis material is an integral part of a treatment plan. Although the sample size is less, the results of our study suggest that there were no major differences in stability with lag screw and miniplates. Lag screws have the added advantage of achieving interfragmentary compression and stability with a minimum of implant material. Key words: Anterior mandibular fractures, Lag screws, Miniplates INTRODUCTION The maxillofacial skeleton injuries occur due to a variety of causes, such as road traffic accidents, and sports injuries. The mandible is the second most commonly fractured bone of the maxillofacial skeleton because of its position and prominence. Although there is wide variance in the reported percentage of fracture of the anterior mandible Access this article online Month of Submission : Month of Peer Review : Month of Acceptance : Month of Publishing : (symphysis and parasymphysis), aggregate analysis places this at approximately 17% of all mandibular fractures. 1,2 This area has been studied extensively and debate continues regarding the ideal treatment method. Although there is a widely accepted consensus about the need for surgical reduction and fixation of a mandibular fracture, a variety of different treatment modalities have been described. Among them are closed or open reduction, extra oral open reduction and internal fixation with a reconstruction plate, intraoral open reduction and internal fixation using different mini-dynamic compression or noncompression plates and an intraoral approach with lag-screw fixation. 3 Miniplate osteosynthesis was introduced to maxillofacial surgery by Michelet et al. in Miniplate osteosynthesis has caused a revolution in mandibular fracture treatment. Corresponding Author: Dr. Ranvijay, C/O Bharat Medical Hall Jandaha, Jandaha, Vaishali, Bihar, India. Phone: drranvijay83@gmail.com 29 International Journal of Scientific Study May 2017 Vol 5 Issue 2
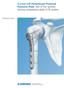
2 Modern plating systems provide better handling, higher stability, and less pressure on the bone. 4 The application of a static compression system has been transformed into a dynamic plating system. 5 Anatomical and biomechanical considerations for placing these miniplates improved this method. Osteosynthesis can be reduced to a tension band plate on the upper border of the mandible. 6,7 One of the most practical methods for open reduction internal fixation of mandibular fractures is the use of lag screw fixation for approximation and stabilization of the fracture segments. The lag screw technique in maxillofacial surgery was first advocated by Brons and Boering in 1970 and was later reintroduced by Niederdellmann et al., 8 who stated that at least two screws were necessary to prevent rotational movement of the fragments in oblique fractures of the mandible. In North America, its use for the management of anterior mandible fractures became popular through the work of Ellis and Ghali. 9 Lag screw fixation is based on the concept of oesteosynthesis by bone compression. A special drilling technique and sequence is followed to establish the desired compression during reduction and stabilization. Compression is achieved because the osteotomy hole in the near cortex (gliding hole) is prepared to a width matching the external diameter of the screw. Therefore, the screw does not engage the near cortex until the screw head is flush with the outer aspect of the cortex. The screw threads on the opposite side of the fracture engage the far cortex, which has been prepared to match the internal diameter of the screw (traction hole). Tightening the screw causes the far cortex to be drawn toward the near cortex, thereby creating compression between the fracture segments. While rigid internal fixation with miniplates is currently considered as the most acceptable technique for stabilization of anterior mandibular fracture, recent studies have reported equally good results with lag screw. Hence, there is need for comparative evaluation of efficacy of miniplate and lag screw in anterior mandibular fracture. The aim of this study is to compare the post-operative results of two different methods for the treatment of mandibular anterior fractures using the miniplate and lag screw for better reproducibility. The objectives included comparative assessments of their ability; 1. To access adequate primary stability, the need for any supplemental maxillomandibular fixation (MMF). 2. To access the time and ease required to complete the procedures. 3. To access the incidence of post-operative complications such as occlusal derangement, wound dehiscence, wound discharge, infection, postsurgical swelling, and any functional limitation in lower lip function as evidenced by speech articulation. MATERIALS AND METHODS Patient with traumatic injury to the mandible reporting to the OPD of Department of Oral and Maxillofacial Surgery of Buddha Institute of Dental Sciences and Hospital was selected. This study was conducted on 24 patients with clinical and radiological evidence of the anterior mandibular fracture. The patient was treated with two groups; (n - 12) treated with titanium lag screw (2.5 mm lag screw); (n - 12) treated with titanium miniplates (2 mm miniplates). Inclusion Criteria Symphysis/parasymphysis fracture of mandible with no evidence of pus discharge and infection. Exclusion Criteria Comminuted fracture Uncontrolled systemic disease Mal-union/non-union of fracture segment (due to the previous treatment by other techniques/late treatment) Anterior fracture with dentoalveolar fracture Anterior Fractures with previous associated pathologies (cysts, tumors). Surgical Procedure All cases were treated with aseptic condition under general anesthesia. Access to the fracture site was generally sought through an intraoral approach except where a coexisting laceration is present over the chin region. Exposure of the fracture site was obtained by a standard layered dissection through mucosa, mentalis muscle, and the periosteum. After debridement of the fracture line, MMF is applied using arch bars/ivy eyelet wiring ligated to the dental arches. Fragments were reduced and held in apposition with a reduction forceps (bone clamp) and confirmed visually by verifying the alignment of the buccal cortex and inferior border. For patients, two 2.5 mm diameter cortical screws were placed using the lag screw principle, with care taken to ensure coaxial preparation of the gliding and pilot holes, adequate enlargement of the gliding hole using 3 mm diameter drills to prevent thread engagement proximally, and preparation of the countersink (Figure 1a). For patients, 2.0 mm miniplates were contoured, applied, and fixed using monocortical screws, in accordance with Champy s principles, along the line of osteosynthesis. A minimum of two screws were placed on either side of the fracture line for each of the bone plates applied (Figure 1b). On completion of the procedure, MMF was released and occlusion verified. The incision was then closed in layers and a pressure dressing was applied to the chin. Follow-up The patients were followed up clinically after 24 h, on days 3 and on day 7 postoperatively and then at weekly International Journal of Scientific Study May 2017 Vol 5 Issue 2 30
3 intervals for 6 weeks and at monthly intervals for 6 months. They were followed up radiographically with mandibular anterior occlusal radiographs and orthopantomographs in the immediate post-operative period and after 1 month, 3 months, and 6 months (Figure 2a and b). Method of Collection and Analysis of Data The clinical and radiological findings were recorded in prestructured preformed and was subjected to statistical analysis. RESULTS A total of 24 patients with mandibular fracture requiring open reduction and internal fixation were included in this study. Patients were randomly divided into two equal groups of 12 patients in each group. patients underwent osteosynthesis using Titanium lag screw while a patients underwent osteosynthesis using titanium 2 mm miniplates. In our study, male patient was predominance. Out of 24 patients 75% were male and 25% female. The mean value of age in (31.33 ± ) and (22.33 ± 6.800). The etiological factors of mandibular fractures were noted. Road traffic accident, 66.7% was the leading cause of fracture followed by fall 29.2% and assault 4.2%. The operative delay, i.e., the time interval between trauma and surgery ranged from in (10.08 ± 9.793) and in (6.00 ± 3.790). The majority of patients in, the time needed to complete the procedure ranged from 60 to 90 min (75%), while for the time ranged from 60 to 90 (58.3%) and 90 to 120 min (41.7%). The difference in time required for completion of the procedures between the two groups was found to be statistically significant (Table 1). In, the duration of post-operative swelling varied from a minimum of 5 days in 7 patients (58.3%) and maximum 10 days in 2 patients (16.67%). In, swelling was present for minimum 5 days in 9 patients (75%) and maximum 15 days (16.67%) (Table 2). The mean value preoperative vertical swelling in ( ± ) and ( ± ) and horizontal swelling in ( ± ) and ( ± ) and post-operative vertical swelling in ( ± ) and ( ± ) and b Figure 1: (a) Intraoperative; lag screws fixation. (b) Postoperative; after 6 months radiograph (orthopantomogram) Table 1: Comparison of time required for procedures Time required for completion of procedure (min) χ 2 value P value <30 and<60 2 (16.67) 0 (0) * >60 and<90 9 (75) 7 (58.3) >90 and<120 0 (0) 5 (41.7) >120 and<150 1 (8.3) 0 (0) *Statistically significant differences seen a b Figure 2: (a) Intraoperative; monocotical plate fixation. (b) After 6 month post-operative radiograph (orthopantomogram) Table 2: Comparison of the duration of post operative swelling Presence of post operative swelling (n=12) (n=12) χ 2 value P value Till 24 h 12 (100) 12 (100) # Till 3 days 12 (100) 10 (83.33) Till 5 days 5 (41.67) 9 (75) Till 7 days 3 (25) 6 (50) Till 10 days 2 (16.67) 7 (58.33) Till 15 days 2 (16.67) 2 (16.67) Till 1 month 0 (0) 0 (0) Till 3 months 1 (8.33) 1 (8.33) Till 6 months 0 (0) 0 (0) # Nonsignificant differences 31 International Journal of Scientific Study May 2017 Vol 5 Issue 2
4 horizontal swelling in ( ± ) and ( ± ). The difference in magnitude of swelling as assessed by Student s paired t-test was not statistically significant (Table 3). All patient (n = 24) showed restricted lip mobility that affected articulation of speech. In, restricted lip mobility was present for a minimum of 3 days in 6 patients (50%) and to a maximum of 10 days in 2 patients (16.7%). In, restricted lip mobility was presents for a minimum of 3 days in 3 patients (25%), 5 days in 5 patients (41.7%), and maximum 10 days in 2 patients (16.7%). The χ 2 value was and p value was The difference between the two groups with regard to restriction of lip mobility was statistically significant (Table 4). Wound dehiscence was not seen both groups. Wound discharge and infection was present, 1 patient in and 1 patient in. Only soft tissue swelling was observed in, occurring in one patient (8.3%). The swelling and discharge was resolved after use of antibiotic therapy. One patient was major complication, which initially responded to antibiotics, but recurrent sinus formation Table 3: Swelling in Groups A and B: Descriptive statistics Parameter N Mean SD SEM Pre vertical Post vertical Pre horizontal Post horizontal Pre vertical Post vertical Pre horizontal Post horizontal SD: Standard deviation, SEM: Standard error of mean and discharge prompted removal of plates and screws after 3 months. As there was clinically bony union, no further fixation was required. Stability which was obtained in all patient (100%) (Table 5). Postoperatively, a blinded observer evaluated the patients for stability of fixation by manually manipulating the mandible and checking for interfragment mobility at the fracture site. There was no mobility seen in both groups (Table 6). DISCUSSION This study evaluated the efficacy of miniplates and cortical screws (using the lag screw principle) in open reduction and internal fixation of mandibular symphysis/parasymphysis region fractures. In our study, the incidence of mandibular fracture was more in males (75%) which is similar to the studies done by various authors. 10,11 This may be justified by the fact that males are generally more prone to situations such as road traffic accidents and sports activity. This study included patients within the age group of years; commonly affected mean age in our study was years. The foremost cause of mandibular fracture was road traffic accident (66.7%) followed by fall (29.2%), assault (4.2%), which is similar to other studies conducted by Goyal et al. 12 Duration of surgery was measured from the time incision was placed till the closure of wound. The majority of patient in, the time needed to complete the procedure ranged between 60 and 90 min (75%) while for the most time required was min. This difference was found to be statistically significant (P = 0.04). Lag screw fixation is relatively quicker as the time consuming task of plate bending and adaptation is obviated. According to Ellis and Ghali, who reported that Table 4: Comparison of swelling in and by student s paired t test Vertical pre operative Vertical post operative Horizontal pre operative Horizontal post operative Vertical pre operative Vertical post operative Horizontal pre operative Horizontal post operative Paired samples test Paired differences t df Sig. (2 tailed) Mean SD SEM 95% confidence interval of the difference Lower Upper * * * * *Statistically significant differences. SD: Standard deviation, SEM: Standard error of mean International Journal of Scientific Study May 2017 Vol 5 Issue 2 32
5 lag screws could be applied more rapidly as compared to miniplates as the latter require contouring and adaptation, which may be time consuming considering the complexities of the anterior mandible contour. 13 Similar results have been described previously by many authors (Peter and Edward, Leonard, Alanshwimmer, Heidrun Schaaf). In our study, post-operative swelling and lip restriction was shorter with the use of lag screws as compared to miniplate, in spite of similar surgical access. Post-operative edema was evaluated by measuring the distance from the mucocutaneous junction on the lower lip to the upper border of the thyroid cartilage in the vertical axis and the distance between the two gonial angles across the chin in the transverse axis using a 2-0 silk thread, transferring the measurements to a ruler. The average of these two post-operative measurements on post-operative day 3 was subtracted from the average pre-operative values to determine the magnitude of swelling. Duration was determined as the time required for a return to the average pre-operative measurements, as determined on the designated days of follow-up. 14 The similar results were obtained by Agnihotri et al. The swelling and lip restriction was presumed that the greater quantity of implanted hardware and the greater amount of bone drilling required for placement of a large number of screws in the miniplate group contributed to more persistent postsurgical edema and associated functional lip restriction. 14 Table 5: Comparison of post operative restriction of lip movement Presence of post operative restriction of lip movement χ 2 value P value Till 24 h # Till 3 days Till 5 days Till 7 days Till 10 days Till 15 days Till 1 month # Nonsignificant differences In our study, postoperatively, the primary stability was achieved by both groups using lag screw and miniplate in all (100%) cases. According to Agnihotri et al., the primary stabilization achieved by cortical screws was greater than that achieved by miniplate fixation (100% of cases in the former and 97.5% of cases in the latter). Post-operative MMF was not required in patients who received cortical (lag) screw fixation, indicating earlier functional rehabilitation. In cases of lag screw fixation, it appears important to manipulate the jaw segments to check for instability after releasing the MMF, as recommended by Ellis and Ghali. 15 According to Ardary, the ultimate stability of screw fixation is dependent on the number of screws used, the method of screw placement, bicortical placement of screws, and the holding power of the screws; the latter is affected by the cortical bone thickness. 16 Lag screws may also be used to supplement plate fixation so as to augment the rigidity of the fixation. 17,18 Compressing fractured bone fragments against each other when performing osteosynthesis has been shown to result in greater stability of fracture repair. According to Kallela et al., if stability is doubtful, it is better to remove the screw and stabilize the fracture with, for example, a miniplate instead of subjecting the patient to MMF. 8 The most crucial factor in achieving sound compression is screw angulation in the anteroposterior direction, which should be almost sagittal. There is a tendency to drill the screw canal in a lingual direction, which results in the screw bit failing to hold in the thin lingual cortical bone. When drilling is then directed in an almost sagittal plane, it is difficult to find enough bone in the buccal cortex to hold the screw head after countersinking. 19 To achieve a rapid recovery of form and function, internal fixation surgery should meet four basic conditions: (1) Anatomic reduction of the bone fragments; (2) functionally stable fixation of the fragments; (3) preservation of the blood supply to the fragments by atraumatic operating technique; and (4) early, active, pain-free mowbilization. 14 None of the patients had any malocclusion in both groups using lag screw and miniplate which is similar to Tiwana Table 6: Correlation of complications and time interval between injury and treatment Parameter Wound dehiscence Wound discharge Stability Infection Wound dehiscence Wound discharge Stability Infection At 24 h 0 (0) 0 (0) 12 (100) 0 (0) 0 (0) 0 (0) 12 (100) 0 (0) At 3 days 0 (0) 0 (0) 12 (100) 0 (0) 0 (0) 0 (0) 12 (100) 0 (0) At 5 days 0 (0) 0 (0) 12 (100) 0 (0) 0 (0) 0 (0) 12 (100) 0 (0) At 7 days 0 (0) 0 (0) 12 (100) 0 (0) 0 (0) 0 (0) 12 (100) 0 (0) At 10 days 0 (0) 0 (0) 12 (100) 0 (0) 0 (0) 0 (0) 12 (100) 0 (0) At 15 days 0 (0) 0 (0) 12 (100) 0 (0) 0 (0) 0 (0) 12 (100) 0 (0) At 1 month 0 (0) 0 (0) 12 (100) 0 (0) 0 (0) 0 (0) 12 (100) 0 (0) At 3 months 0 (0) 1 (8.3) 12 (100) 1 (8.3) 0 (0) 1 (8.3) 12 (100) 1 (8.3) At 6 months 0 (0) 0 (0) 12 (100) 0 (0) 0 (0) 0 (0) 12 (100) 0 (0) 33 International Journal of Scientific Study May 2017 Vol 5 Issue 2
6 et al. 20 Hany A. Emam et al. 21, observed complication in their study of lag screws was a case of malocclusion in 1 patient. It was managed simply by occlusal adjustment, which was also used by Kuriakose et al and Tuovinen et al. One case of infection (8.3%) was seen in both groups but incidence of major complications (infection requiring hardware removal) seen in miniplate fixation. Plate was removed, curettage was done, and oral antibiotics were advised. In contrast, minor complications occurred in 1 case with use of lag screws which required only antibiotics. The incidence of post-operative infection noted in our study is similar to 6.1% as described by Iizuka et al., 22 and Rosenberg et al. 23 recommended the removal of titanium plates in case of infection at fracture site. The study of Tuovinen et al. 24 who determined the incidence of infection-related plate removal to be 3.6%. However, all the post-operative complications in the lag screw group were minor and resolved without any aggressive management. Possible reasons for infection in the symphyseal region could be pre-existing subclinical infection, loose implant, foreign body reaction, inappropriate sterilization, poor host defense, and poor oral hygiene. Another common complication, wound dehiscence which occurred usually early, 6-10 days after surgery. Dehiscence can be caused by many factors, including poor closure during surgery, smoking, trauma, and infection. Why there was a difference between the plate and lag screw groups is curious. In our study, there was no wound dehiscence seen in both groups but after 2½ months of surgery wound dehiscence and wound discharge was seen in both groups due to infection. In (lag screw), only antibiotics were required but (miniplate) required plate removal. Agnihotri et al., analyzing wound dehiscence, only four patients in the cortical (lag) screw group developed this problem, and they did not observe this complication in the group treated with miniplates. The probable contributing factors could be inadequate muscle approximation during closure, pre-existing mucosal tear, poor oral hygiene, and delayed treatment. Resolution was obtained by irrigation with normal saline followed by placement of an adhesive elastic bandage over the chin. Unlike Cawood who encountered 12% wound dehiscence with miniplate fixation. Champy et al. 25 reported an incidence of 0.5% for delayed union and nonunion in patients treated with small plate osteosynthesis. In contrast, we did not experience the above problems in our patients. The single patient in the miniplate group who needed supplemental MMF also had a clinically stable union by 6 weeks. Assael 26 concluded that lag screw fixation of symphyseal fractures had a particularly high rate of technique related failures. Improper or inadequate counter-sinking was the chief reason for fractures of the outer cortex or distraction of the fracture when the screw was tightened. Even though the time required for lag screw fixation was high in their series, adherence to a sound clinical technique could be the reason for not having experienced technique-related failures. CONCLUSION The choice of suitable osteosynthesis material is an integral part of a treatment plan. Although the sample size is less, the results of our study suggest that there were no major differences in stability with lag screw and miniplates. Lag screws have the added advantage of achieving interfragmentary compression and stability with a minimum of implant material. The lag screw principle offers the advantages of fixation using minimal hardware, functional stability, is associated with minimal inflammatory complications and functional restriction, and has a lower incidence of infection when considering the treatment of linear, non-comminuted symphyseal region fractures. The procedure, however, requires more skill and expertise. This recommendation is not complete in itself, as the study is limited by the number of patients evaluated. Our observations therefore require validation with a larger sample size. REFERENCES 1. Brown JS, Grew N, Taylor C, Millar BG. Intermaxillary fixation compared to miniplate osteosynthesis in the management of the fractured mandible: An audit. Br J Oral Maxillofac Surg 1991;29: Cawood JI. Small plate osteosynthesis of mandibular fractures. Br J Oral Maxillofac Surg 1985;23: Ellis E 3 rd. Treatment methods for fractures of the mandibular angle. Int J Oral Maxillofac Surg 1999;28: Sauerbier S, Schön R, Otten JE, Schmelzeisen R, Gutwald R. The development of plate osteosynthesis for the treatment of fractures of the mandibular body - A literature review. J Craniomaxillofac Surg 2008;36: Michelet FX, Deymes J, Dessus B. Osteosynthesis with miniaturized screwed plates in maxillo-facial surgery. J Maxillofac Surg 1973;1: Champy M, Lodde JP. Study of stresses in the fractured mandible in man. Theoretical measurement and verification by extensometric gauges in situ. Rev Stomatol Chir Maxillofac 1977;78: Champy M, Lodde JP, Jaeger JH, Wilk A. Mandibular osteo-synthesis according to the Michelet technique. I. Biomechanical bases. Rev Stomatol Chir Maxillofac 1976;77: Brons R, Boering G. Fractures of the mandibular body treated by stable internal fixation: A preliminary report. J Oral Surg 1970;28: Niederdellmann H, Akuamoa-Boateng E, Uhlig G. Lag-screw osteosynthesis: A new procedure for treating fractures of the mandibular angle. J Oral Surg 1981;39: Schön R, Roveda SI, Carter B. Mandibular fractures in Townsville, Australia: Incidence, aetiology and treatment using the 2.0 AO/ASIF miniplate system. Br J Oral Maxillofac Surg 2001;39: Cabrini Gabrielli MA, Real Gabrielli MF, Marcantonio E, Hochuli Vieira E. Fixation of mandibular fractures with 2.0-mm miniplates: Review of International Journal of Scientific Study May 2017 Vol 5 Issue 2 34
7 191 cases. J Oral Maxillofac Surg 2003;61: Goyal M, Jhamb A, Chawla S, Marya K, Dua JS, Yadav S. A comparative evaluation of fixation techniques in anterior mandibular fractures using 2.0 mm monocortical titanium miniplates versus 2.4 mm cortical titanium lag screws. J Maxillofac Oral Surg 2012;11: Ellis E 3 rd, Ghali GE. Lag screw fixation of anterior mandibular fractures. J Oral Maxillofac Surg 1991;49: Agnihotri A, Prabhu S, Thomas S. A comparative analysis of the efficacy of cortical screws as lag screws and miniplates for internal fixation of mandibular symphyseal region fractures: A randomized prospective study. Int J Oral Maxillofac Surg 2014;43: Ellis E 3 rd, Ghali GE. Lag screw fixation of mandibular angle fractures. J Oral Maxillofac Surg 1991;49: Ardary WC. Prospective clinical evaluation of the use of compression plates and screws in the management of mandible fractures. J Oral Maxillofac Surg 1989;47: Spiessl B. Internal Fixation of the Mandible. Berlin: Springer-Verlag; p Niederdellmann H. Rigid internal fixation by means of lag screws. In: Kruger E, Schilli W, editors. Oral and Maxillofacial Traumatology. Chicago: Quintessence; p Kallela I, Ilzuka T, Laine P, Lindqvist C. Lag-screw fixation of mandibular parasymphyseal and angle fractures. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1996;82: Tiwana PS, Kushner GM, Alpert B. Lag screw fixation of anterior mandibular fractures: A retrospective analysis of intra-operative and postoperative complications. J Oral Maxillofac Surg 2007;65: Emam HA, Stevens MR. Can an arch bar replace a second lag screw in management of anterior mandibular fractures? J Oral Maxillofac Surg 2012;70: Iizuka T, Lindqvist C, Hallikainen D, Paukku P. Infection after rigid internal fixation of mandibular fractures: A clinical and radiologic study. J Oral Maxillofac Surg 1991;49: Rosenberg A, Grätz KW, Sailer HF. Should titanium miniplates be removed after bone healing is complete? Int J Oral Maxillofac Surg 1993;22: Tuovinen V, Nørholt SE, Sindet-Pedersen S, Jensen J. A retrospective analysis of 279 patients with isolated mandibular fractures treated with titanium miniplates. J Oral Maxillofac Surg 1994;52: Champy M, Loddé JP, Schmitt R, Jaeger JH, Muster D. Mandibular osteosynthesis by miniature screwed plates via a buccal approach. J Maxillofac Surg 1978;6: Assael LA. Evaluation of rigid internal fixation of mandible fractures performed in the teaching laboratory. J Oral Maxillofac Surg 1993;51: How to cite this article: Ranvijay, Shahi AK, Singh M. Comparative Study of the Efficacy of Titanium Lag Screw and Titanium Miniplates for Internal Fixation of Anterior Mandibular Fractures. Int J Sci Stud 2017;5(2): Source of Support: Nil, Conflict of Interest: None declared. 35 International Journal of Scientific Study May 2017 Vol 5 Issue 2
New innovations in craniomaxillofacial fixation: the 2.0 lock system
 LECTURE New innovations in craniomaxillofacial fixation: the 2.0 lock system Brian Alpert, Rolf Gutwald1 and Rainer Schmelzeisen1 Departments of Oral & Maxillofacial Surgery and Surgical & Hospital Dentistry,
LECTURE New innovations in craniomaxillofacial fixation: the 2.0 lock system Brian Alpert, Rolf Gutwald1 and Rainer Schmelzeisen1 Departments of Oral & Maxillofacial Surgery and Surgical & Hospital Dentistry,
Departement of Stomatology, The Second Hospital of Lanzhou University, 82 Cuiyingmwen, Chengguan District, Lanzhou City, Gansu Province, China
 European Review for Medical and Pharmacological Sciences Comparative evaluation of 2.0 mm locking plate system vs 2.0 mm non-locking plate system for mandibular angle fracture fixation: a prospective randomized
European Review for Medical and Pharmacological Sciences Comparative evaluation of 2.0 mm locking plate system vs 2.0 mm non-locking plate system for mandibular angle fracture fixation: a prospective randomized
Three Dimensional Titanium Mini Plates in Management of Mandibular Fractures
 Biomedical & Pharmacology Journal Vol. 7(1), 241-246 (2014) Three Dimensional Titanium Mini Plates in Management of Mandibular Fractures R. BALAKRISHNAN, VIJAY EBENEZER and ABU DAKIR Department of Oral
Biomedical & Pharmacology Journal Vol. 7(1), 241-246 (2014) Three Dimensional Titanium Mini Plates in Management of Mandibular Fractures R. BALAKRISHNAN, VIJAY EBENEZER and ABU DAKIR Department of Oral
Evaluation of Titanium Lag Screw Osteosynthesis in the Management of Mandibular Fractures
 WJD ORIGINAL ARTICLE Evaluation of Titanium Lag Screw Osteosynthesis in the 10.5005/jp-journals-10015-1457 Management of Mandibular Fractures Evaluation of Titanium Lag Screw Osteosynthesis in the Management
WJD ORIGINAL ARTICLE Evaluation of Titanium Lag Screw Osteosynthesis in the 10.5005/jp-journals-10015-1457 Management of Mandibular Fractures Evaluation of Titanium Lag Screw Osteosynthesis in the Management
Technique Guide. Compact 2.0 LOCK Mandible. The locking system for the mandible.
 Technique Guide Compact 2.0 LOCK Mandible. The locking system for the mandible. Table of Contents Introduction Compact 2.0 LOCK Mandible 2 AO Principles 4 Indications and Contraindications 5 Surgical
Technique Guide Compact 2.0 LOCK Mandible. The locking system for the mandible. Table of Contents Introduction Compact 2.0 LOCK Mandible 2 AO Principles 4 Indications and Contraindications 5 Surgical
Scholars Journal of Medical Case Reports
 Scholars Journal of Medical Case Reports Sch J Med Case Rep 2017; 5(11):805-809 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Medical Case Reports Sch J Med Case Rep 2017; 5(11):805-809 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher for Academic and Scientific Resources)
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area.
 Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 Technique Guide VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction VA-LCP Anterior
Technique Guide VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction VA-LCP Anterior
Management of Mandibular Symphysis and Para Symphysis Fractures Using a Single Mini Plate With Erich Arch Bar: Our Experience
 ORIGINAL ARTICLE Management of Mandibular Symphysis and Para Symphysis Fractures Using a Single Mini Plate With Erich Arch Bar: Our Experience Parveen Akhter Lone, Padam Singh*, Kamal Kishore*, Mohit Goel*
ORIGINAL ARTICLE Management of Mandibular Symphysis and Para Symphysis Fractures Using a Single Mini Plate With Erich Arch Bar: Our Experience Parveen Akhter Lone, Padam Singh*, Kamal Kishore*, Mohit Goel*
The treatment of malocclusion after open reduction of maxillofacial fracture: a report of three cases
 CASE REPORT http://dx.doi.org/10.5125/jkaoms..40.2.91 pissn 2234-7550 eissn 2234-5930 The treatment of malocclusion after open reduction of maxillofacial fracture: a report of three cases Sung-Suk Lee,
CASE REPORT http://dx.doi.org/10.5125/jkaoms..40.2.91 pissn 2234-7550 eissn 2234-5930 The treatment of malocclusion after open reduction of maxillofacial fracture: a report of three cases Sung-Suk Lee,
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 Technique Guide LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction LCP Superior Clavicle
Technique Guide LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction LCP Superior Clavicle
Keywords: Maxillofacial plate, mandibular fractures, cat, toy breed dog. Abstract:
 Keywords: Maxillofacial plate, mandibular fractures, cat, toy breed dog Abstract: This study shows the successful application of the titanium maxillofacial miniplate, Compact 1.0, in 12 cats and two toy
Keywords: Maxillofacial plate, mandibular fractures, cat, toy breed dog Abstract: This study shows the successful application of the titanium maxillofacial miniplate, Compact 1.0, in 12 cats and two toy
ORIGINAL ARTICLE. G. K. Vivek 1, Akshay Shetty 2, N. Vaibhav 2, Mohammad Imran 2
 Journal of Advanced Clinical & Research Insights (2016), 3, 194 199 ORIGINAL ARTICLE A comparative study of single 3-D titanium plate versus conventional Champy s 2 miniplate fixation in the management
Journal of Advanced Clinical & Research Insights (2016), 3, 194 199 ORIGINAL ARTICLE A comparative study of single 3-D titanium plate versus conventional Champy s 2 miniplate fixation in the management
Technique Guide. LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System.
 Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Technique Guide. IMF Screw Set. For intermaxillary fixation.
 Technique Guide IMF Screw Set. For intermaxillary fixation. Table of Contents Introduction IMF Screw Set 2 Indications and Contraindications 3 Surgical Technique Preparation 4 Insert IMF Screw 6 Insert
Technique Guide IMF Screw Set. For intermaxillary fixation. Table of Contents Introduction IMF Screw Set 2 Indications and Contraindications 3 Surgical Technique Preparation 4 Insert IMF Screw 6 Insert
Surgical technique. IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults.
 Surgical technique IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Table of contents Features and benefits 2 Indications and contraindications 3 Surgical technique
Surgical technique IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Table of contents Features and benefits 2 Indications and contraindications 3 Surgical technique
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
Current Perspective in the Management of Mandibular Fractures
 ORIGINL RTICLE Current Perspective in the 10.5005/jp-journals-10028-1103 Management of Mandibular Fractures Current Perspective in the Management of Mandibular Fractures 1 Sachin Rai, 2 Vidya Rattan STRCT
ORIGINL RTICLE Current Perspective in the 10.5005/jp-journals-10028-1103 Management of Mandibular Fractures Current Perspective in the Management of Mandibular Fractures 1 Sachin Rai, 2 Vidya Rattan STRCT
Comparitive Study between Proximal Femoral Nailing and Dynamic Hip Screw in Intertrochanteric Fracture of Femur *
 Open Journal of Orthopedics, 2013, 3, 291-295 Published Online November 2013 (http://www.scirp.org/journal/ojo) http://dx.doi.org/10.4236/ojo.2013.37053 291 Comparitive Study between Proximal Femoral Nailing
Open Journal of Orthopedics, 2013, 3, 291-295 Published Online November 2013 (http://www.scirp.org/journal/ojo) http://dx.doi.org/10.4236/ojo.2013.37053 291 Comparitive Study between Proximal Femoral Nailing
Technique Guide. 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
MetaFix Ludloff Plate
 Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor
 Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Technique Guide. 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology.
 Technique Guide 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4 mm Variable Angle LCP
Technique Guide 2.4 mm Variable Angle LCP Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4 mm Variable Angle LCP
2.0 mm Mandible Locking Plate System
 Advanced Plating System for Trauma, Microvascular Reconstruction, and Orthognathic Surgery 2.0 mm Mandible Locking Plate System Surgical Technique TABLE OF CONTENTS INTRODUCTION 2.0 mm Mandible Locking
Advanced Plating System for Trauma, Microvascular Reconstruction, and Orthognathic Surgery 2.0 mm Mandible Locking Plate System Surgical Technique TABLE OF CONTENTS INTRODUCTION 2.0 mm Mandible Locking
WINSTA-C. Clavicle Plating System
 Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Clavicle Plating System Clinical Advisor Michael Kurer FRCS FRCS (Orth) Consultant Orthopaedic and Shoulder Surgeon North Middlesex University Hospital NHS Trust Table of Contents Introduction Indication
Humerus shaft - Reduction & Fixation - Compression plate - AO Surgery Reference. Compression plating
 Humerus shaft 12-A3 ORIF 1. Principles Compression plating Authors Compression plate Compression plating provides fixation with absolute stability for two-part fracture patterns, where the bone fragments
Humerus shaft 12-A3 ORIF 1. Principles Compression plating Authors Compression plate Compression plating provides fixation with absolute stability for two-part fracture patterns, where the bone fragments
Merete BLP. Surgical Technique. - Bunion Locking Plate - Low Profile Locking Bone Plate System
 Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Open reduction; plate fixation 1 Principles
 Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
2.4 mm Variable Angle LCP Volar Extra-Articular Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology.
 Technique Guide 2.4 mm Variable Angle LCP Volar Extra-Articular Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4
Technique Guide 2.4 mm Variable Angle LCP Volar Extra-Articular Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Table of Contents Introduction 2.4
LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures.
 LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures. Surgical Technique This publication is not intended for distribution in the
LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures. Surgical Technique This publication is not intended for distribution in the
Small Fragment Plating System. Securing optimal fixation through locked and compression plating technology
 Small Fragment Plating System Securing optimal fixation through locked and compression plating technology Contents Design Rationale Introduction Interfragmentary Fixation Insertion of a 3.5 mm Cortical
Small Fragment Plating System Securing optimal fixation through locked and compression plating technology Contents Design Rationale Introduction Interfragmentary Fixation Insertion of a 3.5 mm Cortical
Conventus CAGE PH Surgical Techniques
 Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Conventus CAGE PH Surgical Techniques Conventus Orthopaedics The Conventus CAGE PH (PH Cage) is a permanent implant comprised of an expandable scaffold, made from nitinol and titanium, which is deployed
Small Fragment Plating System
 Small Fragment Plating System Securing optimal fixation through locked and compression plating technology SURGICAL TECHNIQUE RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to trauma surgery
Small Fragment Plating System Securing optimal fixation through locked and compression plating technology SURGICAL TECHNIQUE RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to trauma surgery
Mandible fracture - Management. Dr Dinesh Kumar Verma OMFS SDCRI, SGNR
 Mandible fracture - Management Dr Dinesh Kumar Verma OMFS SDCRI, SGNR MANAGEMENT OPEN! CLOSE! DIRECT! INDIRECT! IMMEDIATE (PRIMARY) 1. ABC 2. Temporary stabilization 3. Tetanus prophylaxis 4. Antibiotics
Mandible fracture - Management Dr Dinesh Kumar Verma OMFS SDCRI, SGNR MANAGEMENT OPEN! CLOSE! DIRECT! INDIRECT! IMMEDIATE (PRIMARY) 1. ABC 2. Temporary stabilization 3. Tetanus prophylaxis 4. Antibiotics
Surgical Technique. CONQUEST FN Femoral Neck Fracture System
 Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique. Distal Humerus Locking Plate
 Surgical Technique Distal Humerus Locking Plate PERI-LOC Locked Plating System Distal Humerus Locking Plate Surgical Technique Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Surgical Technique Distal Humerus Locking Plate PERI-LOC Locked Plating System Distal Humerus Locking Plate Surgical Technique Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
PROXIMAL TIBIAL PLATE
 SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
SURGICAL NÁSTROJE TECHNIQUE PRO ARTROSKOPII PROXIMAL INSTRUMENTS TIBIAL FOR PLATE ARTHROSCOPY Proximal Tibial Plate Description of medical device The Proximal Tibial Plate is used in epyphyseal and metaphyseal
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
tep Ankle Fracture Plating System
 tep Response Ortho is a global orthopaedic trauma solutions manufacturer offering premium products created under its founding principles of innovation, excellence by design, and functional superiority.
tep Response Ortho is a global orthopaedic trauma solutions manufacturer offering premium products created under its founding principles of innovation, excellence by design, and functional superiority.
Technique Guide. 3.5 mm LCP Proximal Tibia Plate. Part of the Synthes Small Fragment LCP System.
 Technique Guide 3.5 mm LCP Proximal Tibia Plate. Part of the Synthes Small Fragment LCP System. Table of Contents AO ASIF Principles of Internal Fixation 4 Indications/Contraindications 5 Surgical Technique
Technique Guide 3.5 mm LCP Proximal Tibia Plate. Part of the Synthes Small Fragment LCP System. Table of Contents AO ASIF Principles of Internal Fixation 4 Indications/Contraindications 5 Surgical Technique
EVOS MINI with IM Nailing
 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
AcUMEDr. LoCKING CLAVICLE PLATE SYSTEM
 AcUMEDr LoCKING CLAVICLE PLATE SYSTEM LoCKING CLAVICLE PLATE SYSTEM Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients.
AcUMEDr LoCKING CLAVICLE PLATE SYSTEM LoCKING CLAVICLE PLATE SYSTEM Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients.
Technique Guide. 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
Research report for MSc Dent. University of Witwatersrand. Faculty of health science. Dr J Beukes. Student number: h
 Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Queen Mary's Hospital, Roehampton, Londcn
 A UNIVERSAL KIT IN TITANIUM FOR IMMEDIATE REPLACEMENT OF THE RESECTED MANDIBLE JOHN E. BOWFaMA~, M.B., Ch.B., B.D.S., F.D.S.R.C.S., and BRIAN CONROY, L.I.B.S.T. Queen Mary's Hospital, Roehampton, Londcn
A UNIVERSAL KIT IN TITANIUM FOR IMMEDIATE REPLACEMENT OF THE RESECTED MANDIBLE JOHN E. BOWFaMA~, M.B., Ch.B., B.D.S., F.D.S.R.C.S., and BRIAN CONROY, L.I.B.S.T. Queen Mary's Hospital, Roehampton, Londcn
The Locking Calcaneal Plate Instrument and Implant Sets
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System The Locking Calcaneal Plate Instrument and Implant Sets Surgical Technique Table of Contents Introduction Locking Calcaneal Plate 2 AO
Part of the DePuy Synthes Locking Compression Plate (LCP ) System The Locking Calcaneal Plate Instrument and Implant Sets Surgical Technique Table of Contents Introduction Locking Calcaneal Plate 2 AO
Technique Guide. 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System.
 Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal
Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plate Aiming Instruments. Part of the 3.5 mm LCP Percutaneous Instrument System. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal
The Flower Straight Fibula Plate
 The Flower Straight Fibula Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application STRAIGHT LOCKING FIBULA PLATE ANTERIOR LATERAL DISTAL TIBIAL PLATE MEDIAL DISTAL TIBIAL PLATE ANATOMIC
The Flower Straight Fibula Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application STRAIGHT LOCKING FIBULA PLATE ANTERIOR LATERAL DISTAL TIBIAL PLATE MEDIAL DISTAL TIBIAL PLATE ANATOMIC
Technique Guide. Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones.
 Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Mandible Fractures May 2004
 TITLE: Mandible Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: May 26, 2004 RESIDENT PHYSICIAN: Jacques Peltier, MD FACULTY ADVISOR: Matthew W. Ryan, MD SERIES EDITORS:
TITLE: Mandible Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: May 26, 2004 RESIDENT PHYSICIAN: Jacques Peltier, MD FACULTY ADVISOR: Matthew W. Ryan, MD SERIES EDITORS:
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Surgical Technique. Lower Extremity Plates and Straight Plates
 Surgical Technique Lower Extremity Plates and Straight Plates 2 Table of contents Overview...4 Indications... 4 Contraindications... 4 Screw Options... 5 Straight Plate Options... 6 Proximal Tibia Plate
Surgical Technique Lower Extremity Plates and Straight Plates 2 Table of contents Overview...4 Indications... 4 Contraindications... 4 Screw Options... 5 Straight Plate Options... 6 Proximal Tibia Plate
LOGIC SURGICAL TECHNIQUE GUIDE. In d i c at i o n s. Co n t r a i n d i c at i o n s. Mandibular Distraction System
 TM SURGICAL TECHNIQUE GUIDE In d i c at i o n s The OSTEOMED Mandibular Distractor system is indicated for use as a mandibular bone lengthener for patients diagnosed with conditions where treatment includes
TM SURGICAL TECHNIQUE GUIDE In d i c at i o n s The OSTEOMED Mandibular Distractor system is indicated for use as a mandibular bone lengthener for patients diagnosed with conditions where treatment includes
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
Surgical Technique. Cannulated Angled Blade Plate 3.5 and 4.5, 90
 Surgical Technique Cannulated Angled Blade Plate 3.5 and 4.5, 90 Cannulated Angled Blade Plate 3.5 and 4.5, 90 Table of contents Indications/Contraindications 2 Implants 3 Surgical technique 5 Implant
Surgical Technique Cannulated Angled Blade Plate 3.5 and 4.5, 90 Cannulated Angled Blade Plate 3.5 and 4.5, 90 Table of contents Indications/Contraindications 2 Implants 3 Surgical technique 5 Implant
Technique Guide. 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
Low Bend Distal Tibia Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Low Bend Medial Distal Tibia Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Low Bend Medial Distal Tibia Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia
Technique Guide. LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction LCP Distal Fibula Plates 2 AO Principles 4 Indications 5 Surgical Technique
Technique Guide LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction LCP Distal Fibula Plates 2 AO Principles 4 Indications 5 Surgical Technique
Case Study. Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor.
 Case Study Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor. Micrognathia Secondary to Pierre Robin Sequence Patient profile
Case Study Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor. Micrognathia Secondary to Pierre Robin Sequence Patient profile
Infected Mandibular Fracture; Can the Tooth Buds Be Saved?
 IBIMA Publishing Journal of Research and Practice in Dentistry http://www.ibimapublishing.com/journals/dent/dent.html Vol. 2015(2015), Article ID 727027, 5 pages DOI: 10.5171/2015.727027 Research Article
IBIMA Publishing Journal of Research and Practice in Dentistry http://www.ibimapublishing.com/journals/dent/dent.html Vol. 2015(2015), Article ID 727027, 5 pages DOI: 10.5171/2015.727027 Research Article
Surgical Technique. Clavicle Locking Plate
 Surgical Technique Clavicle Locking Plate PERI-LOC Locked Plating System Clavicle Locking Plate Surgical Technique Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient Positioning...4
Surgical Technique Clavicle Locking Plate PERI-LOC Locked Plating System Clavicle Locking Plate Surgical Technique Table of Contents Introduction...2 Indications...3 Plate Features...3 Patient Positioning...4
Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note
 Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
LCP Distal Humerus Plates
 The anatomic fixation system for the distal humerus with angular stability Surgical technique LCP Locking Compression Plate Contents Indications and contraindications 2 Implants 3 Instruments 5 Preparation
The anatomic fixation system for the distal humerus with angular stability Surgical technique LCP Locking Compression Plate Contents Indications and contraindications 2 Implants 3 Instruments 5 Preparation
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System.
 LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
SMV Scientific Bone Plate and Screw System Surgical Technique
 SMV Scientific Bone Plate and Screw System Surgical Technique Description: The SMV Scientific Bone Plate and Screw System consists of non-locking plates and bone screw fasteners in a variety of lengths,
SMV Scientific Bone Plate and Screw System Surgical Technique Description: The SMV Scientific Bone Plate and Screw System consists of non-locking plates and bone screw fasteners in a variety of lengths,
Lag Screw Device Intended for symphyseal fracture fixation of the mandible
 Lag Screw Device Intended for symphyseal fracture fixation of the mandible SUrgicaL TecHNiqUe Lag Screw Device Intended for symphyseal fracture fixation of the mandible Simplifies the lag screw fixation
Lag Screw Device Intended for symphyseal fracture fixation of the mandible SUrgicaL TecHNiqUe Lag Screw Device Intended for symphyseal fracture fixation of the mandible Simplifies the lag screw fixation
Biodegradable plates and screws in oral and maxillofacial surgery Buijs, Gerrit Jacob
 University of Groningen Biodegradable plates and screws in oral and maxillofacial surgery Buijs, Gerrit Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
University of Groningen Biodegradable plates and screws in oral and maxillofacial surgery Buijs, Gerrit Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
The Flower Medial Column Fusion Plate
 The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Surgical treatment of mandibular condyle fracture with bicortical screws: case report
 ISSN: Electronic version: 1984-5685 RSBO. 2016 Jan-Mar;13(1):50-4 Case Report Article Surgical treatment of mandibular condyle fracture with bicortical screws: case report Guilherme dos Santos Trento 1
ISSN: Electronic version: 1984-5685 RSBO. 2016 Jan-Mar;13(1):50-4 Case Report Article Surgical treatment of mandibular condyle fracture with bicortical screws: case report Guilherme dos Santos Trento 1
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Compact 2.0 LOCK Mandible. The locking system for the mandible.
 Compact 2.0 LOCK Mandible. The locking system for the mandible. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Compact 2.0 LOCK Mandible. The locking system for the mandible. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
LCP Superior Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 LCP Superior Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for
LCP Superior Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for
Surgical Technique. Targeter Systems Overview
 Surgical Technique Targeter Systems Overview PERI-LOC Locked Plating System Targeter Systems Overview Table of contents Product overview... 2 Introduction... 2 Indications... 2 Design features and benefits...
Surgical Technique Targeter Systems Overview PERI-LOC Locked Plating System Targeter Systems Overview Table of contents Product overview... 2 Introduction... 2 Indications... 2 Design features and benefits...
Original Article Trapezoidal Condylar Plate: Report Of 15 Cases In The Management Of Mandibular Subcondylar Fracture
 Original Article Trapezoidal Condylar Plate: Report Of 15 Cases In The Management Of Mandibular Subcondylar Fracture Geeta Singh, Shadab Mohammad, Somdipto Das, Deepak Passi, Kuldeep Vishwakarma, Nitin
Original Article Trapezoidal Condylar Plate: Report Of 15 Cases In The Management Of Mandibular Subcondylar Fracture Geeta Singh, Shadab Mohammad, Somdipto Das, Deepak Passi, Kuldeep Vishwakarma, Nitin
MatrixRIB. Stable fixation of normal and osteoporotic ribs.
 MatrixRIB. Stable fixation of normal and osteoporotic ribs. Technique Guide CMF Matrix Table of Contents Introduction MatrixRIB 2 AO Principles 4 Indications 5 Surgical Technique Patient Positioning 5
MatrixRIB. Stable fixation of normal and osteoporotic ribs. Technique Guide CMF Matrix Table of Contents Introduction MatrixRIB 2 AO Principles 4 Indications 5 Surgical Technique Patient Positioning 5
DOWNLOAD OR READ : RIGID FIXATION FOR MAXILLOFACIAL SURGERY PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : RIGID FIXATION FOR MAXILLOFACIAL SURGERY PDF EBOOK EPUB MOBI Page 1 Page 2 rigid fixation for maxillofacial surgery rigid fixation for maxillofacial pdf rigid fixation for maxillofacial
DOWNLOAD OR READ : RIGID FIXATION FOR MAXILLOFACIAL SURGERY PDF EBOOK EPUB MOBI Page 1 Page 2 rigid fixation for maxillofacial surgery rigid fixation for maxillofacial pdf rigid fixation for maxillofacial
OBSOLETED. LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Surgical Technique LCP Small Fragment System This publication
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Surgical Technique LCP Small Fragment System This publication
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique
 PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
Variable Angle LCP Volar Rim Distal Radius Plate 2.4. For fragment-specific fracture fixation with variable angle locking technology.
 Technique Guide Variable Angle LCP Volar Rim Distal Radius Plate 2.4. For fragment-specific fracture fixation with variable angle locking technology. Image intensifier control Warning This description
Technique Guide Variable Angle LCP Volar Rim Distal Radius Plate 2.4. For fragment-specific fracture fixation with variable angle locking technology. Image intensifier control Warning This description
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
Surgical Technique. Anterolateral and Medial Distal Tibia Locking Plates
 Surgical Technique Anterolateral and Medial Distal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System Anterolateral and Medial Distal Tibia Locking Plates Surgical Technique Contents Product
Surgical Technique Anterolateral and Medial Distal Tibia Locking Plates PERI-LOC Periarticular Locked Plating System Anterolateral and Medial Distal Tibia Locking Plates Surgical Technique Contents Product
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Technique Guide LCP Small Fragment System Table of Contents Introduction
The study of distal ¼ diaphyseal extra articular fractures of humerus treated with antegrade intramedullary interlocking nailing
 2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system.
 LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
2.4 mm LCP Radial Head Plates. Part of the Synthes LCP Distal Radius Plate System.
 2.4 mm LCP Radial Head Plates. Part of the Synthes LCP Distal Radius Plate System. Technique Guide Instruments and Implants approved by the AO Foundation Table of Contents Introduction 2.4 mm LCP Radial
2.4 mm LCP Radial Head Plates. Part of the Synthes LCP Distal Radius Plate System. Technique Guide Instruments and Implants approved by the AO Foundation Table of Contents Introduction 2.4 mm LCP Radial
Surgical Technique Guide
 Surgical Technique Guide Minimally Invasive, Intramedullary Device For Distal Radius Fragility Fractures The Sonoma WRx Wrist Fracture Repair Device is flexible, inserting easily through a small incision
Surgical Technique Guide Minimally Invasive, Intramedullary Device For Distal Radius Fragility Fractures The Sonoma WRx Wrist Fracture Repair Device is flexible, inserting easily through a small incision
DARCO MFS. Locked plating system for reconstructive forefoot surgery.
 DARCO MFS Locked plating system for reconstructive forefoot surgery. DARCO MFS Locked plating system for reconstructive forefoot surgery System Basics The DARCO MFS plating system for the forefoot has
DARCO MFS Locked plating system for reconstructive forefoot surgery. DARCO MFS Locked plating system for reconstructive forefoot surgery System Basics The DARCO MFS plating system for the forefoot has
Surgical Technique Carpal Fusion
 Carpal Fusion Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Extremity Medical Lag Screw and X-Post System
Carpal Fusion Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Extremity Medical Lag Screw and X-Post System
The Flower Forefoot PROCEDURE GUIDE.
 The Flower Forefoot PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION T-PLATE, OBLIQUE MTP
The Flower Forefoot PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION T-PLATE, OBLIQUE MTP
MATRIX PLATFORM FEATURES DESIGNED TO COMPLEMENT AO FIXATION PRINCIPLES
 MATRIX PLATFORM FEATURES DESIGNED TO COMPLEMENT AO FIXATION PRINCIPLES The aim of surgical fracture treatment is to reconstruct the bony anatomy and restore its function. Internal fixation is distinguished
MATRIX PLATFORM FEATURES DESIGNED TO COMPLEMENT AO FIXATION PRINCIPLES The aim of surgical fracture treatment is to reconstruct the bony anatomy and restore its function. Internal fixation is distinguished
InCoreTM Lapidus System
 InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
