British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy
|
|
|
- Arline Stella Paul
- 5 years ago
- Views:
Transcription
1 British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy Information for Health Care Professionals Caring for Children with Cerebral Palsy 2018
2 SUMMARY British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy was originally established by a group of over 60 multidisciplinary professionals and parents from all regions of the province. Meetings were held in May 2011 and January Attendees established consensus regarding the desire to create a British Columbia (BC) hip surveillance program for children with CP and reached consensus on the commencement, frequency, and discharge criteria for surveillance. In 2017, BC s Consensus was updated to reflect international consensus achieved in the development of the American Academy of Cerebral Palsy and Developmental Medicine (AACPDM) Hip Surveillance Care Pathway. 1 Experts participating in this consensus were from Canada, Australia, Scotland and the United States. This booklet describes the established consensus. AUTHORS OF THIS REPORT: Stacey Miller, Physiotherapist, BC Children s Hospital Kishore Mulpuri, Pediatric Orthopaedic Surgeon, BC Children s Hospital Maureen O Donnell, Developmental Pediatrician & Executive Director, Child Health BC CITING THIS REPORT Miller S, Mulpuri K, O Donnell M. British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy: Information for health care professionals caring for children with cerebral palsy. Child Health BC, Vancouver, BC ACKNOWLEDGEMENTS The original BC Consensus on Hip Surveillance was developed under the direction of the BC Hip Surveillance Planning Committee (in alphabetical order): Janice Duivestein, Program Manager, Sunny Hill Health Centre for Children; Nancy Lanphear, Senior Medical Director, Sunny Hill Health Centre for Children; Mary Lou Matthews, Provincial Lead, Network Operations, Child Health BC; Tanja Mayson, Physiotherapist, Sunny Hill Health Centre for Children; Stacey Miller, Physiotherapist, BC Children s Hospital; Kishore Mulpuri, Orthopaedic Surgeon, BC Children s Hospital; Maureen O Donnell, Executive Director, Child Health BC; Lori Roxborough, Therapy Department Director, Sunny Hill Health Centre for Children; Suzanne Steenburgh, Program Manager, BC Children s Hospital; Esias van Rensburg, Developmental Pediatrician, Sunny Hill Health Centre. The committee s contributions were invaluable to the creation of a provincial surveillance program. The authors would like to thank all of the 2011/2012 meeting participants who contributed to the creation of the first BC Consensus Statement on Hip Surveillance for Children with Cerebral Palsy and an implementation model. Participants are listed in meeting reports that are available on the Child Health BC website ( The authors wish to acknowledge the international experts from Australia, Canada, the United States, and Scotland who were involved in the development of the AACPDM Hip Surveillance Care Pathway. See the AACPDM website ( for a list of those involved. In particular, the authors thank Tanja Mayson from Vancouver, BC who was the project manager for this project.
3 TABLE OF CONTENTS Introduction and Objective... 1 Evidence for Hip Surveillance... 1 Inclusion... 2 Hip Displacement... 2 Level of Risk... 3 Motor Function... 3 Gait Pattern... 4 Assessments... 5 Clinical Examination... 5 Radiological Assessment... 5 Recommended Frequency of Hip Surveillance... 7 Referral to Orthopaedic Surgeon... 7 Recommended Frequency of Hip Surveillance - Quick Guide... 8 Hip Surveillance Discharge Criteria... 9 How To Use This Consensus Statement... 9 References Appendix A Abbreviations... 12
4 British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy INTRODUCTION AND OBJECTIVE Hip surveillance is the process of identifying and monitoring critical early indicators of progressive hip displacement. 2 Hip displacement, or subluxation, is the gradual movement of the femoral head laterally from under the acetabulum. A hip is dislocated when the femoral head is completely displaced from under the acetabulum. Children with cerebral palsy (CP) are at risk for hip displacement. The objective of BC s Consensus is to outline recommendations for hip surveillance to ensure that children with CP receive appropriate screening and are referred to a pediatric orthopaedic surgeon at the appropriate time to minimize or prevent complications associated with hip dislocations. Hip displacement is often silent, with no physical signs or symptoms. Left untreated, displaced or dislocated hips may cause pain, decreased hip range of motion, decreased sitting, standing, or walking tolerance, and difficulty with personal care. Timely orthopaedic management is critical to those children identified through surveillance as having progressive displacement. This document does not address the orthopaedic management of progressive hip displacement. The intervention should be tailored to the needs of the individual child. Surveillance practices in Australia and Sweden 2,3, best available research evidence, and expert opinion were used to establish the 2012 Consensus. In 2017, the BC Consensus was updated to reflect international consensus established during the creation of the American Academy of Cerebral Palsy and Developmental Medicine (AACPDM) Hip Surveillance Care Pathway. 1 Experts participating in this consensus were from Canada, Australia, Scotland and the United States. Differences between BC s Consensus and the AACPDM Care Pathway for children at GMFCS level I and II and those with a Group IV hemiplegic gait pattern are a result of how services are provided to children in British Columbia and the age of school entry. This document was created for health care professionals caring for children at risk for hip displacement. EVIDENCE FOR HIP SURVEILLANCE Early identification of hip displacement through surveillance has been demonstrated to be an effective means of reducing the incidence of hip dislocation in children with CP. A systematic review on the evidence for hip surveillance found surveillance is an effective means of identifying hip displacement. 4 Hip surveillance programs, in combination with timely orthopaedic management, have been shown to decrease or prevent the incidence of hip dislocations in children with CP. 5-8 British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 1
5 INCLUSION All children with CP should be included in a hip surveillance program. CP is defined as: a group of permanent disorders of the development of movement and posture, causing activity limitation, that are attributed to non-progressive disturbances that occurred in the developing fetal or infant brain. The motor disorders of cerebral palsy are often accompanied by disturbances of sensation, perception, cognition, communication, and 9(p. 9) behaviour, by epilepsy, and by secondary musculoskeletal problems. CP is not defined by the underlying cause of the condition. All non-progressive disturbances of the fetal or infant brain occurring in the pre-natal, peri-natal and post-natal period, up to the age of 2 years, can lead to CP. For example, children with a genetic anomaly, a chromosomal abnormality, a metabolic condition, or an acquired brain injury resulting from meningitis, encephalitis, or a stroke in early life can also be diagnosed with CP if they have the motor findings described in the above definition. In these children, we simply understand why they have CP. Children not yet diagnosed with CP, but for whom there is a clinical suspicion of having CP, should receive hip surveillance. Investigations to determine the underlying cause of a child s motor impairment should not prevent or slow the initiation of hip surveillance. Disorders of the spinal nerves (i.e. spina bifida), peripheral nerves (i.e. spinal muscular atrophy), muscles (i.e. muscular dystrophy), or mechanical origins (i.e. arthrogryposis) are not considered CP and, therefore, this Consensus is not applicable. HIP DISPLACEMENT The hip is a ball and socket joint, with the acetabulum making up the socket and the femoral head making up the ball (Figure 1a). In a healthy hip the femoral head rests completely in the acetabulum. Hip displacement, also called subluxation, refers to the gradual movement of the femoral head laterally from under the acetabulum (Figure 1b). A hip is dislocated when the femoral head is completely displaced from under the acetabulum (Figure 1c). Delayed or absent weight bearing, limitations in gross motor function, and abnormal muscle forces around the hip joint may affect the development of the proximal femur and hip joint. Figure 1a: Normal Hip Figure 1b: Displaced Hip Figure 1c: Dislocated Hip British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 2
6 LEVEL OF RISK Hip displacement is the second most common deformity in children with CP. 10 The overall incidence of hip displacement in children with CP has been found to be approximately onethird (26-35%). 3,11-13 Motor Function Hip displacement has been shown to be directly related to a child s gross motor function, as described by the child s Gross Motor Function Classification System (GMFCS) level, and is, therefore, used as a basis for this Consensus Statement (Figure 2). 3,11-13 Incidence of Hip Displacement (%) GMFCS Level Figure 2: Incidence of hip displacement (Migration Percentage >30%) by GMFCS Level 11 The GMFCS is a five level classification system for children with CP that is based on self initiated movement. 14,15 It was originally created in 1997 and was expanded and revised in ,15 The GMFCS-Expanded & Revised is available for download, free of charge, at ER_English.pdf. Classifying a child s GMFCS level requires familiarity with the child and their usual performance of motor skills but no formal training is required. It can be completed in only a few minutes. Distinctions between levels are based on functional limitations, the need for hand held mobility devices or wheeled mobility, and, to a lesser extent, quality of movement. Each level has been given a title that reflects the method of mobility typical for children at that level after 6 years of age: GMFCS I: Walks without Limitations GMFCS II: Walks with Limitations GMFCS III: Walks Using a Hand-Held Mobility Device GMFCS IV: Self-Mobility with Limitations; May Use Powered Mobility GMFCS V: Transported in a Manual Wheelchair British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 3
7 Separate age bands exist as classification of motor function is dependent upon age. These age bands include: before 2 nd birthday, between 2 nd and 4 th birthday, between 4th and 6 th birthday, between 6 th and 12 th birthday, and between 12 th and 18 th birthday. Children under the age of 2, if born premature, should be classified based on their corrected age. Expectations for gross motor function differ by age so it is important to consult the User Instructions each time a child s motor function is classified. Gait Pattern Most children with hemiplegia are classified at GMFCS level I or II. As such, they are at low risk for hip displacement and discharged from surveillance prior to skeletal maturity. However, children with a Winters, Gage, and Hicks (WGH) Group IV hemiplegic gait must be followed until skeletal maturity (from now on referred to as Group IV gait). Winters, Gage and Hicks 16 described the classification of hemiplegic gait into four gait patterns (Figure 3). 17 Group IV gait involves more marked proximal involvement of the hip. The WGH classification system is only based on changes in the sagittal plane but many children with hemiplegia also have deviations in the coronal and transverse plane. It is these children who have changes in all three planes of motion that should be included in hip surveillance. For the purposes of hip surveillance, Group IV gait pattern is characterized by: a flexed hip and an anterior pelvic tilt (sagittal plane), an adducted hip (coronal plane), and hip internal rotation (transverse plane). 16,17 Children with this gait pattern are at risk of progressive hip displacement that typically occurs later than children with bilateral CP. 2 Risk of hip displacement in children with bilateral CP is not related to their gait pattern. Their level of risk is determined by GMFCS level only. 16, 17 Figure 3: Group IV Hemiplegic Gait Patterns. Illustration reproduced with permission and copyright Bill Reid, The Royal Children s Hospital, Melbourne, AUS. British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 4
8 ASSESSMENTS Hip surveillance requires both clinical and radiological review. Clinical examination is an important component of hip surveillance but hip displacement cannot be based on clinical assessment alone. 5,18 The frequency of the clinical and radiological examinations is dependent upon a child s risk for hip displacement and is, therefore, determined by the child s GMFCS level and, for children with hemiplegia, the child s gait pattern. The recommended frequency of clinical and radiological examinations is illustrated in the Quick Guide on page 9. Clinical Examination a This Clinical Exam is solely for the purpose of hip surveillance and is to be completed by the child s physiotherapist. If a child does not have a physiotherapist, it is to be completed by a designated health care professional familiar with the assessments. Before completing the clinical exam, please see the Clinical Exam Instructions and e-learning module that are available at for more information on how to complete the measures involved. Step 1: Classify: Determine GMFCS level Identify Group IV hemiplegic gait pattern (in children with hemiplegia) Step 2: Assess: Hip abduction range of motion measured with hips at 0 flexion and knees fully extended Pain during clinical examination Step 3: Ask the Child s Parent or Primary Caregiver: Do [does] you [your child] have hip pain? You may notice this when you move [your child moves] your [their] hip or after prolonged activity, when changing your [your child s] position, when you move your [your child s] leg or when looking after your [your child s] personal care. 1 Who is your family physician/pediatrician? Radiological Assessment The radiological measure used to monitor hip displacement is migration percentage (MP). MP is defined as the percentage of the ossified femoral head outside of the lateral margin of the ossified acetabulum (Figure 4). 19 Reimers reported that the 90th percentile for MP in typically developing children at 4 years of age was 10%. 19 A hip is considered at risk when the MP is greater than 30%. Evidence supports measurement of MP by a single, experienced examiner. 22,23 a The Clinical Exam component of the Consensus Statement does not replace the need for regular, comprehensive musculoskeletal assessment as a component of overall management. British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 5
9 A B Figure 4: Measurement of Migration Percentage 5. Illustration reproduced with permission from Wynter M et al. Australian Hip Surveillance Guidelines for Children with CP An antero-posterior (AP) radiograph of the pelvis taken in a standardized position is required to accurately measure the migration percentage (Figure 5) MP is affected by the amount of abduction or adduction of the leg so the leg should be positioned in neutral. Measurement of the MP requires that the triradiate cartilages be visible and therefore anterior and posterior A pelvic tilt must be corrected. B Figure 5: Standardized positioning for antero-posterior radiograph. Illustration reproduced with permission and copyright Bill Reid, The Royal Children s Hospital, Melbourne, AUS. British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 6
10 RECOMMENDED FREQUENCY OF HIP SURVEILLANCE Surveillance frequency is based on a child s age, GMFCS level, and, for children with hemiplegia, gait type. Surveillance is ideally initiated by 2 years of age, when a CP diagnosis is provided, or when CP is suspected. 1 Enrollment in hip surveillance may occur prior to age 2 years for children who are diagnosed or suspected of having CP at a young age; radiographs may not be recommended until age 2 years. Surveillance frequency increases with increasing GMFCS level. Frequency may be reduced when the migration percentage is less than 30% and has remained stable over a period of 2 years. Stability is defined as < 10% change in MP over a 12 month period. The frequency of clinical exams and radiographs is shown in the Quick Guide on page 8. REFERRAL TO ORTHOPAEDIC SURGEON The intention of BC s Consensus on Hip Surveillance is that review by a pediatric orthopaedic surgeon occurs at the appropriate time. A referral to an orthopaedic surgeon should occur in the following situations: Migration Percentage > 30% End of range hip abduction < 30 when measured with hips at 0 flexion and knees extended Presence of pain on clinical exam Positive answer to the pain question in the Clinical Exam Any other clinical concern that is felt to be related to the hip An aim of hip surveillance is that orthopaedic review occurs at the appropriate time when treatment options are available. Every child referred to orthopaedic services should be managed with an individualized management plan, which may or may not include ongoing hip surveillance. 2 Children who have surgery for hip displacement or dislocation should return to surveillance post operatively until reaching skeletal maturity. British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 7
11 British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy 2018 QUICK GUIDE 1, 2 Classification 3,4 ID or 2 Age in Years For more information, visit Continue Until Bones Stop Growing (on X-ray) GMFCS I * GMFCS II * Every 2 years GMFCS III # Every 2 years Every year GMFCS IV # GMFCS V # Every year Every 2 years Legend: Any GMFCS with Group IV Hemiplegic Gait *5-7 GMFCS: Gross Motor Function Classification System 2 ID: Identification/Diagnosis of cerebral palsy Group IV Hemiplegic Gait: Child walks with one hip turned and pulled inward 5,6 Clinical Exam X-Ray *Altered from AACPDM Care Pathway due to age of school entry #Do not reduce frequency of exam if migration percentage unstable or over 30% References: Every 2 years 1. Miller S, Mulpuri K, O Donnell M. British Columbia s Consensus on Hip Surveillance for Children with Cerebral Palsy. Information for health care professionals caring for children with cerebral palsy. Child Health BC, Vancouver, BC, Canada American Academy of Cerebral Palsy and Developmental Medicine Hip Surveillance Care Pathway. 2017; care-pathways/hip-surveillance. Accessed on: 17 Nov Palisano R et al. Dev Med Child Neurol. 2008;50: Illustrations Version 2. Reid B, Willoughby K, Harvey A, Graham HK. The Royal Children s Hospital, Melbourne, Australia. 5. Winters TF, Gage JR, Hicks R. J Bone Joint Surg (Am). 1987;69: Rodda J & Graham HK. Eur J Child Neurol, 2001; 8 (Suppl. 5): Illustration reproduced with permission and copyright Bill Reid, The Royal Children s Hospital, Melbourne, Australia.
12 HIP SURVEILLANCE DISCHARGE CRITERIA Hip displacement can occur during the pubertal growth spurt and thus children at risk must be followed until skeletal maturity. 11 The closure of the triradiate cartilage on the AP radiograph is used as the prime indicator of skeletal maturity. 2 Children whose motor function is classified at GMFCS levels I & II, excluding those with a Group IV gait pattern, are at low risk for hip displacement, and are followed until the age of 5 and 10 years, respectively. For children at GMFCS levels III, IV, and V, who have pelvic obliquity associated with clinical or radiographic evidence of increasing scoliosis, hip surveillance should ideally be continued beyond skeletal maturity as their hips continue to be at risk. 1 HOW TO USE THIS CONSENSUS STATEMENT This Consensus is for use by individuals caring for children with CP, within the Child Health BC Hip Surveillance Program. It is intended for education and to assist in clinical decision making. Individual clinicians are to use their own clinical judgment in decision making about individual clients. Should you have questions, contact the child s physician or orthopaedic surgeon. British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 9
13 REFERENCES 1. American Academy of Cerebral Palsy and Developmental Medicine Hip Surveillance Care Pathway. (12 Sep 2017). Accessed 30 Oct Wynter M, Gibson N, Kentish M, Love S, Thomason P, Graham HK. The consensus statement on hip surveillance for children with cerebral palsy: Australian standards of care. J Pediatr Rehabil Med. 2011;4(3): Hagglund G, Lauge-Pedersen H, Wagner P. Characteristics of children with hip displacement in cerebral palsy. BMC Musculoskelet Disord. 2007;8: Gordon GS, Simkiss DE. A systematic review of the evidence for hip surveillance in children with cerebral palsy. J Bone Joint Surg [Br]. 2006;88-B: Dobson F, Boyd RN, Parrott J, Nattrass GR, Graham HK. Hip surveillance in children with cerebral palsy. Impact on the surgical management of spastic disease. J Bone Joint Surg [Br]. 2002;84-B: Elkamil AI, Andersen GL, Hägglund G, Lamvik T, Skranes J, Vik T. Prevalence of hip dislocation among children with cerebral palsy in regions with and without a surveillance programme: a cross sectional study in Sweden and Norway. BMC Musculoskelet Disord. 2011;12: Hagglund G, Andersson S, Duppe H, Lauge-Pedersen H, Nordmark E, & Westbom L. Prevention of dislocation of the hip in children with cerebral palsy. The first ten years of a population-based prevention programme. J Bone Joint Surg [Br]. 2005;87-B: Hagglund G, Alriksson-Schmidt A, Lauge-Pedersen H, Robdy-Bousquet E, Wagner P, Westbom L. Prevention of dislocation of the hip in children with cerebral palsy; 20 year results of a population-based prevention programme. Bone Joint J. 2014; 96-B: Rosenbaum P, Paneth N, Leviton A, Goldstein M, Bax M. A report: The definition and classification of cerebral palsy April Dev Med Child Neurol. 2007;49: Cornell MS. The hip in children with cerebral palsy: Predicting the outcome of soft tissue surgery. Clin Orthop. 1995;340: Soo B, Howard JJ, Boyd RN, Reid SM, Lanigan A, Wolfe R, Reddihough D, Graham HK. Hip displacement in cerebral palsy. J Bone Joint Surg [Am]. 2006;88: Connelly A, Flett P, Graham HK, Oates J. Hip surveillance in Tasmanian children with cerebral palsy. J Pediatr Child Health. 2009;45: Kentish M, Wynter M, Snape N, Boyd R. Five year outcome of state-wide hip surveillance of children and adolescents with cerebral palsy. J Pediatr Rehabil Med. 2011;4: Palisano R, Rosenbaum P, Walter S, Russell D, Wood E, Galuppi B. Development and reliability of a system to classify gross motor function in children with cerebral palsy. Dev Med Child Neurol. 1997:39: Palisano RJ, Rosenbaum P, Bartlett D, Livingston MH. Content validity of the expanded and revised Gross Motor Function Classification System. Dev Med Child Neurol. 2008;50: Winters T, Gage J, Hicks R. Gait patterns in spastic hemiplegia in children and adults. J Bone Joint Surg [Am]. 1987;69: Rodda J & Graham HK. Classification of gait patterns in spastic hemiplegia and spastic diplegia: a basis for a management algorithm. Eur J Neurol. 2001; 8 (Suppl. 5): Scrutton D, Baird G. Surveillance measures of the hips of children with bilateral cerebral palsy. Arch Diseases Child. 1997;76: Reimers J. The stability of the hip in children: a radiological study of results of muscle surgery in cerebral palsy. Acta Orthop Scand. 1980;184: British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 10
14 20. Hagglund G, Lauge-Pedersen H, Persson M. Radiographic threshold values for hip screening in cerebral palsy. J Child Ortho. 2007;1: Scrutton D. The early management of hips in cerebral palsy. Dev Med Child Neurol. 1989;31: Parrott J, Boyd RN, Dobson F, Lancaster A, Love S, Oates J, Wolfe R, Nattrass GR, Graham HK. Hip displacement in spastic cerebral palsy: repeatability of radiological measurement. J Pediatr Orthop. 2002;22: Faraj S, Atherton WG, Stott NS. Inter- and intra-measurer error in the measurement of Reimers hip migration percentage. J Bone Joint Surg [Br]. 2004;86-B: Wynter M, Gibson N, Kentish M, Love SC, Thomason P, Willoughby K, Graham HK. Australian Hip Surveillance Guidelines for Children with CP Accessed 30 Oct British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 11
15 ABBREVIATIONS Appendix A AP BC CP GMFCS MP WGH antero-posterior British Columbia cerebral palsy Gross Motor Function Classification System migration percentage Winter, Gage, and Hicks British Columbia s Consensus On Hip Surveillance for Children with Cerebral Palsy 12
16 For more information on the Child Health BC Hip Surveillance Program, visit To speak with the Hip Surveillance Coordinator, call or , extension 4099, or January 2018
What is Hip Surveillance and Why is It Important for My Child? Information for Parents and Caregivers of Children with Cerebral Palsy
 What is Hip Surveillance and Why is It Important for My Child? Information for Parents and Caregivers of Children with Cerebral Palsy 2018 BC s Consensus on Hip Surveillance for Children with Cerebral
What is Hip Surveillance and Why is It Important for My Child? Information for Parents and Caregivers of Children with Cerebral Palsy 2018 BC s Consensus on Hip Surveillance for Children with Cerebral
HIP SURVEILLANCE. Bottom Line Evidence-Informed Recommendations for the Hip Surveillance in Individuals with Cerebral Palsy
 Bottom Line EvidenceInformed Recommendations for the Hip Surveillance T Mayson (project manager and clinical examination subgroup leader), S Miller (radiology subgroup leader), R Cairns, K Graham, S Love,
Bottom Line EvidenceInformed Recommendations for the Hip Surveillance T Mayson (project manager and clinical examination subgroup leader), S Miller (radiology subgroup leader), R Cairns, K Graham, S Love,
Introduction To The New AACPDM Hip Surveillance Care Pathway For Children With Cerebral Palsy: What's the Consensus? How Can It Be Implemented?
 Introduction To The New AACPDM Hip Surveillance Care Pathway For Children With Cerebral Palsy: What's the Consensus? How Can It Be Implemented? September 15, 2017 Montreal Quebec Canada 1 CARE PATHWAYS
Introduction To The New AACPDM Hip Surveillance Care Pathway For Children With Cerebral Palsy: What's the Consensus? How Can It Be Implemented? September 15, 2017 Montreal Quebec Canada 1 CARE PATHWAYS
Windswept hip deformity in children with cerebral palsy: a population-based prospective follow-up
 DOI 10.1007/s11832-016-0749-1 ORIGINAL CLINICAL ARTICLE Windswept hip deformity in children with cerebral palsy: a population-based prospective follow-up Gunnar Hägglund 1 Henrik Lauge-Pedersen 1 Måns
DOI 10.1007/s11832-016-0749-1 ORIGINAL CLINICAL ARTICLE Windswept hip deformity in children with cerebral palsy: a population-based prospective follow-up Gunnar Hägglund 1 Henrik Lauge-Pedersen 1 Måns
Risk Factors for Hip Displacement in Children With Cerebral Palsy: Systematic Review
 REVIEW ARTICLE Risk Factors for Hip Displacement in Children With Cerebral Palsy: Systematic Review Blazej Pruszczynski, MD,* Julieanne Sees, DO,w and Freeman Miller, MDw Background: When hip displacement
REVIEW ARTICLE Risk Factors for Hip Displacement in Children With Cerebral Palsy: Systematic Review Blazej Pruszczynski, MD,* Julieanne Sees, DO,w and Freeman Miller, MDw Background: When hip displacement
Guideline for surveillance for hip subluxation and dislocation in children and young people with cerebral palsy. Speciality: General
 Title of Guideline Contact Name and Job Title (author) Directorate & Speciality Guideline for surveillance for hip subluxation and dislocation in children and young people with cerebral palsy Janet Corderoy,
Title of Guideline Contact Name and Job Title (author) Directorate & Speciality Guideline for surveillance for hip subluxation and dislocation in children and young people with cerebral palsy Janet Corderoy,
The natural history of hip development in cerebral palsy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE The natural history of hip development in cerebral palsy TERJE TERJESEN Department of Orthopaedic Surgery, Oslo University Hospital, Rikshospitalet
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE The natural history of hip development in cerebral palsy TERJE TERJESEN Department of Orthopaedic Surgery, Oslo University Hospital, Rikshospitalet
The prognostic value of the head-shaft angle on hip displacement in children with cerebral palsy
 J Child Orthop (2015) 9:129 135 DOI 10.1007/s11832-015-0654-z ORIGINAL CLINICAL ARTICLE The prognostic value of the head-shaft angle on hip displacement in children with cerebral palsy J. P. J. van der
J Child Orthop (2015) 9:129 135 DOI 10.1007/s11832-015-0654-z ORIGINAL CLINICAL ARTICLE The prognostic value of the head-shaft angle on hip displacement in children with cerebral palsy J. P. J. van der
Prevalence and predictive factors of hip displacement in children with cerebral palsy at Paediatric Institute, Kuala Lumpur Hospital
 Neurology Asia 2017; 22(3) : 243 252 Prevalence and predictive factors of hip displacement in children with cerebral palsy at Paediatric Institute, Kuala Lumpur Hospital Bih-Hwa Ching MBBS MRCPCH, Teik-Beng
Neurology Asia 2017; 22(3) : 243 252 Prevalence and predictive factors of hip displacement in children with cerebral palsy at Paediatric Institute, Kuala Lumpur Hospital Bih-Hwa Ching MBBS MRCPCH, Teik-Beng
Is head shaft angle a valuable continuous risk factor for hip migration in cerebral palsy?
 DOI 10.1007/s11832-016-0774-0 ORIGINAL CLINICAL ARTICLE Is head shaft angle a valuable continuous risk factor for hip migration in cerebral palsy? Sanjay Chougule 1 John Dabis 2 Aviva Petrie 3 Karen Daly
DOI 10.1007/s11832-016-0774-0 ORIGINAL CLINICAL ARTICLE Is head shaft angle a valuable continuous risk factor for hip migration in cerebral palsy? Sanjay Chougule 1 John Dabis 2 Aviva Petrie 3 Karen Daly
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip
 Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
Comparison of Botulinum Toxin Type A Injection and Soft- Tissue Surgery to Treat Hip Subluxation in Children With Cerebral Palsy
 2108 ORIGINAL ARTICLE Comparison of Botulinum Toxin Type A Injection and Soft- Tissue Surgery to Treat Hip Subluxation in Children With Cerebral Palsy Eun Joo Yang, MD, Dong-wook Rha, MD, Hyun Woo Kim,
2108 ORIGINAL ARTICLE Comparison of Botulinum Toxin Type A Injection and Soft- Tissue Surgery to Treat Hip Subluxation in Children With Cerebral Palsy Eun Joo Yang, MD, Dong-wook Rha, MD, Hyun Woo Kim,
Postural Therapy Update 12:45-1:30 Thursday Dec 6, Ginny Paleg, PT, DScPT Montgomery County Infants and Toddlers Program
 Postural Therapy Update 12:45-1:30 Thursday Dec 6, 2018 Ginny Paleg, PT, DScPT Montgomery County Infants and Toddlers Program ginny@paleg.com Children with contractures and deformities have pain Let s
Postural Therapy Update 12:45-1:30 Thursday Dec 6, 2018 Ginny Paleg, PT, DScPT Montgomery County Infants and Toddlers Program ginny@paleg.com Children with contractures and deformities have pain Let s
Orthopedic Issues in Children with Special Healthcare Needs
 Orthopedic Issues in Children with Special Healthcare Needs Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department
Orthopedic Issues in Children with Special Healthcare Needs Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department
Author's response to reviews
 Author's response to reviews Title: Prevalence of hip dislocation among children with cerebral palsy in regions with and without a surveillance programme: a cross sectional study in Sweden and Norway Authors:
Author's response to reviews Title: Prevalence of hip dislocation among children with cerebral palsy in regions with and without a surveillance programme: a cross sectional study in Sweden and Norway Authors:
10/26/2017. Comprehensive & Coordinated Orthopaedic Management of Children with CP. Objectives. It s all about function. Robert Bruce, MD Sayan De, MD
 Comprehensive & Coordinated Orthopaedic Management of Children with CP Robert Bruce, MD Sayan De, MD Objectives Understand varying levels of intervention are available to optimize function of children
Comprehensive & Coordinated Orthopaedic Management of Children with CP Robert Bruce, MD Sayan De, MD Objectives Understand varying levels of intervention are available to optimize function of children
A classification system for hip disease in cerebral palsy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE A classification system for hip disease in cerebral palsy JONATHAN ROBIN MBBS 1 HKERRGRAHAMMD FRCS (ED) FRACS 1 RICHARD BAKER PHD CENG CSCI 2 PAULO
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE A classification system for hip disease in cerebral palsy JONATHAN ROBIN MBBS 1 HKERRGRAHAMMD FRCS (ED) FRACS 1 RICHARD BAKER PHD CENG CSCI 2 PAULO
BN M BNeurobiomechanics MBNeurobiomechanics
 Fz (% body weight) N Gait Analysis Gait Analysis The following document explains some the content of the gait report (TMP.122) as well as providing key references for the tests used and sources of normal
Fz (% body weight) N Gait Analysis Gait Analysis The following document explains some the content of the gait report (TMP.122) as well as providing key references for the tests used and sources of normal
Progression of Hip Displacement during Radiographic Surveillance in Patients with Cerebral Palsy
 ORIGINAL ARTICLE Musculoskeletal Disorders http://dx.doi.org/10.3346/jkms.2016.31.7.1143 J Korean Med Sci 2016; 31: 1143-1149 Progression of Hip Displacement during Radiographic Surveillance in Patients
ORIGINAL ARTICLE Musculoskeletal Disorders http://dx.doi.org/10.3346/jkms.2016.31.7.1143 J Korean Med Sci 2016; 31: 1143-1149 Progression of Hip Displacement during Radiographic Surveillance in Patients
Gait analysis and medical treatment strategy
 Gait analysis and medical treatment strategy Sylvain Brochard Olivier Rémy-néris, Mathieu Lempereur CHU and Pediatric Rehabilitation Centre Brest Course for European PRM trainees Mulhouse, October 22,
Gait analysis and medical treatment strategy Sylvain Brochard Olivier Rémy-néris, Mathieu Lempereur CHU and Pediatric Rehabilitation Centre Brest Course for European PRM trainees Mulhouse, October 22,
Elisabet Rodby-Bousquet 1,2, Atli Ágústsson 3, Guðný Jónsdóttir 3, Tomasz Czuba 4, Ann-Christin Johansson 2 and Gunnar Hägglund 1
 465423CRE28110.1177/0269215512465423Clinical RehabilitationRodby-Bousquet et al. 2012 Article CLINICAL REHABILITATION Interrater reliability and construct validity of the Posture and Postural Ability Scale
465423CRE28110.1177/0269215512465423Clinical RehabilitationRodby-Bousquet et al. 2012 Article CLINICAL REHABILITATION Interrater reliability and construct validity of the Posture and Postural Ability Scale
HIP DYSPLASIA AND HYPOTONIA CAN STANDING IN ABDUCTION HELP?
 HIP DYSPLASIA AND HYPOTONIA CAN STANDING IN ABDUCTION HELP? Written by: MARY MILES, PT, DPT, ATP THIS CASE STUDY IS SPONSORED BY ALTIMATE MEDICAL Standing with hips in abduction has evolved as the new
HIP DYSPLASIA AND HYPOTONIA CAN STANDING IN ABDUCTION HELP? Written by: MARY MILES, PT, DPT, ATP THIS CASE STUDY IS SPONSORED BY ALTIMATE MEDICAL Standing with hips in abduction has evolved as the new
PROGRESSSIVE HIP SUBLUXATION leading to hip dislocation
 431 Hip Migration Percentage in Children With Cerebral Palsy Treated With Botulinum Toxin Type A Frank S. Pidcock, MD, David E. Fish, MD, MPH, Doug Johnson-Greene, PhD, ABPP, Isabel Borras, MD, John McGready,
431 Hip Migration Percentage in Children With Cerebral Palsy Treated With Botulinum Toxin Type A Frank S. Pidcock, MD, David E. Fish, MD, MPH, Doug Johnson-Greene, PhD, ABPP, Isabel Borras, MD, John McGready,
Management of knee flexion contractures in patients with Cerebral Palsy
 Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Severe crouch gait in spastic diplegia can be prevented
 CHILDREN S ORTHOPAEDICS Severe crouch gait in spastic diplegia can be prevented A POPULATION-BASED STUDY C. Vuillermin, J. Rodda, E. Rutz, B. J. Shore, K. Smith, H. K. Graham From Royal Children s Hospital,
CHILDREN S ORTHOPAEDICS Severe crouch gait in spastic diplegia can be prevented A POPULATION-BASED STUDY C. Vuillermin, J. Rodda, E. Rutz, B. J. Shore, K. Smith, H. K. Graham From Royal Children s Hospital,
Hip surveillance at your fingertips!
 Hip surveillance at your fingertips! HipScreen: An App for Community-Based Hip Surveillance Hip Surveillance for children with cerebral palsy can lead to early detection and treatment of hip dysplasia,
Hip surveillance at your fingertips! HipScreen: An App for Community-Based Hip Surveillance Hip Surveillance for children with cerebral palsy can lead to early detection and treatment of hip dysplasia,
Society for Pediatric Radiology 2015 Hands on Session. DDH: Pitfalls and Practical Tips
 Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
Society for Pediatric Radiology 2015 Hands on Session DDH: Pitfalls and Practical Tips Michael A. DiPietro, M.D. John F. Holt Collegiate Professor of Radiology Professor of Pediatrics and Communicable
Changes in lower limb rotation after soft tissue surgery in spastic diplegia
 Acta Orthopaedica 2010; 81 (2): 245 249 245 Changes in lower limb rotation after soft tissue surgery in spastic diplegia 3-dimensional gait analysis in 28 children Bjørn Lofterød 1 and Terje Terjesen 2
Acta Orthopaedica 2010; 81 (2): 245 249 245 Changes in lower limb rotation after soft tissue surgery in spastic diplegia 3-dimensional gait analysis in 28 children Bjørn Lofterød 1 and Terje Terjesen 2
Cerebral Palsy. What is Cerebral Palsy? Clues to Diagnosis of Cerebral Palsy 12/30/2012
 What is Cerebral Palsy? Cerebral Palsy Hamza Alsayouf,MD American Board Of neurology with Special Qualification in Child Neurology American Board of Pediatric Neurology In 2005, a committee of the American
What is Cerebral Palsy? Cerebral Palsy Hamza Alsayouf,MD American Board Of neurology with Special Qualification in Child Neurology American Board of Pediatric Neurology In 2005, a committee of the American
Determinants of Hip Displacement in Children With Cerebral Palsy
 Clin Orthop Relat Res (2015) 473:3675 3681 DOI 10.1007/s11999-015-4515-3 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Determinants
Clin Orthop Relat Res (2015) 473:3675 3681 DOI 10.1007/s11999-015-4515-3 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CLINICAL RESEARCH Determinants
By: Griffin Smith & Eric Foch
 By: Griffin Smith & Eric Foch What is Cerebral Palsy? Non progressive neurodevelopmentalcondition Signs: Spasticity Ataxia Muscle rigidity idit Athetosis Tremor Distribution Among Limbs Why study cerebral
By: Griffin Smith & Eric Foch What is Cerebral Palsy? Non progressive neurodevelopmentalcondition Signs: Spasticity Ataxia Muscle rigidity idit Athetosis Tremor Distribution Among Limbs Why study cerebral
Scoliosis in Patients with Severe Cerebral Palsy: Three Different Courses in Adolescents
 Original Article http ://escholarship.lib.okayama-u.ac.jp/amo/ Scoliosis in Patients with Severe Cerebral Palsy: Three Different Courses in Adolescents Yoshiaki Oda a*, Tomoyuki Takigawa a, Yoshihisa Sugimoto
Original Article http ://escholarship.lib.okayama-u.ac.jp/amo/ Scoliosis in Patients with Severe Cerebral Palsy: Three Different Courses in Adolescents Yoshiaki Oda a*, Tomoyuki Takigawa a, Yoshihisa Sugimoto
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Šmigovec I., Ðapić T., Trkulja V. (2014) Ultrasound screening for decentered hips in children with severe cerebral palsy: a preliminary evaluation. Pediatric Radiology, 44
Središnja medicinska knjižnica Šmigovec I., Ðapić T., Trkulja V. (2014) Ultrasound screening for decentered hips in children with severe cerebral palsy: a preliminary evaluation. Pediatric Radiology, 44
Standing in children with bilateral spastic cerebral palsy: Aspects of muscle strength, vision and motor function
 Standing in children with bilateral spastic cerebral palsy: Aspects of muscle strength, vision and motor function Cecilia Lidbeck, PT, PhD Department of Women s and Children s Health Karolinska Institutet
Standing in children with bilateral spastic cerebral palsy: Aspects of muscle strength, vision and motor function Cecilia Lidbeck, PT, PhD Department of Women s and Children s Health Karolinska Institutet
Keith Bachmann, MD UVA Department of Orthopaedic Surgery
 Keith Bachmann, MD UVA Department of Orthopaedic Surgery Definition Spinal deformity secondary to either neurologic or muscle pathology. Etiology Imbalance of muscle forces Lack of truncal support Similar
Keith Bachmann, MD UVA Department of Orthopaedic Surgery Definition Spinal deformity secondary to either neurologic or muscle pathology. Etiology Imbalance of muscle forces Lack of truncal support Similar
Chapter 1. Overview. General Description. Test Developers. Purpose and Use. Qualifications of Users. Limitations. Communication. General Description
 Chapter 1: Overview Chapter 1 Overview General Description Test Developers Purpose and Use Qualifications of Users Limitations Communication General Description The research version of the Seated Postural
Chapter 1: Overview Chapter 1 Overview General Description Test Developers Purpose and Use Qualifications of Users Limitations Communication General Description The research version of the Seated Postural
Considerations in the selection of patients for Selective Dorsal Rhizotomy
 Considerations in the selection of patients for Selective Dorsal Rhizotomy The best and the worst surgery I have ever been associated with. A therapist's perspective Dean Morgan, PT Disclosure Statement
Considerations in the selection of patients for Selective Dorsal Rhizotomy The best and the worst surgery I have ever been associated with. A therapist's perspective Dean Morgan, PT Disclosure Statement
Surgical release of neurological hip luxation in children H. Klima Ostschweizer Kinderspital St. Gallen Abteilung für Kinderorthopädie
 Surgical release of neurological hip luxation in children H. Klima Ostschweizer Kinderspital St. Gallen Abteilung für Kinderorthopädie Development of hip luxation At birth these hips are normal developed,
Surgical release of neurological hip luxation in children H. Klima Ostschweizer Kinderspital St. Gallen Abteilung für Kinderorthopädie Development of hip luxation At birth these hips are normal developed,
Pain in children and adolescents with cerebral palsy: a population-based registry study
 Acta Pædiatrica ISSN 0803-5253 REGULAR ARTICLE Pain in children and adolescents with cerebral palsy: a population-based registry study Ann Alriksson-Schmidt (ann.alriksson-schmidt@med.lu.se), Gunnar H
Acta Pædiatrica ISSN 0803-5253 REGULAR ARTICLE Pain in children and adolescents with cerebral palsy: a population-based registry study Ann Alriksson-Schmidt (ann.alriksson-schmidt@med.lu.se), Gunnar H
Stability of the Gross Motor Function Classification System after single-event multilevel surgery in children with cerebral palsy
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Stability of the Gross Motor Function Classification System after single-event multilevel surgery in children with cerebral palsy ERICH RUTZ 1,2,3
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Stability of the Gross Motor Function Classification System after single-event multilevel surgery in children with cerebral palsy ERICH RUTZ 1,2,3
Hip joint subluxation after selective dorsal rhizotomy for spastic cerebral palsy
 J Neurosurg (Pediatrics 1) 103:10 16, 2005 Hip joint subluxation after selective dorsal rhizotomy for spastic cerebral palsy TUFAN HICDONMEZ, M.D., PAUL STEINBOK, M.B.B.S., F.R.C.S.(C), RICHARD BEAUCHAMP,
J Neurosurg (Pediatrics 1) 103:10 16, 2005 Hip joint subluxation after selective dorsal rhizotomy for spastic cerebral palsy TUFAN HICDONMEZ, M.D., PAUL STEINBOK, M.B.B.S., F.R.C.S.(C), RICHARD BEAUCHAMP,
NZQA Expiring unit standard 7026 version 4 Page 1 of 7. Apply knowledge of functional anatomy and biomechanics
 Page 1 of 7 Title Apply knowledge of functional anatomy and biomechanics Level 5 Credits 5 Purpose People credited with this unit standard are able to: apply knowledge of human anatomy relevant to exercise
Page 1 of 7 Title Apply knowledge of functional anatomy and biomechanics Level 5 Credits 5 Purpose People credited with this unit standard are able to: apply knowledge of human anatomy relevant to exercise
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway
 Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Hip Dysplasia David S. Feldman, MD
 Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Hip dysplasia
Normal development & reflex
 Normal development & reflex Definition of Development : acquisition & refinement of skills 1 대근육운동발달 2 소근육운동발달 3 대인관계및사회성발달 4 적응능력혹은비언어성발달 5 의사소통및언어발달 6 학습, 청각, 시각의발달 Department of Rehabilitation Medicine,
Normal development & reflex Definition of Development : acquisition & refinement of skills 1 대근육운동발달 2 소근육운동발달 3 대인관계및사회성발달 4 적응능력혹은비언어성발달 5 의사소통및언어발달 6 학습, 청각, 시각의발달 Department of Rehabilitation Medicine,
Why Would Your Child Need to See Me?
 Why Would Your Child Need to See Me? Deborah M Eastwood Great Ormond St Hospital for Children, London The Royal National Orthopaedic Hospital, UK Disclosures I am an orthopaedic surgeon and I do operate
Why Would Your Child Need to See Me? Deborah M Eastwood Great Ormond St Hospital for Children, London The Royal National Orthopaedic Hospital, UK Disclosures I am an orthopaedic surgeon and I do operate
Multiapical Deformities p. 97 Osteotomy Concepts and Frontal Plane Realignment p. 99 Angulation Correction Axis (ACA) p. 99 Bisector Lines p.
 Normal Lower Limb Alignment and Joint Orientation p. 1 Mechanical and Anatomic Bone Axes p. 1 Joint Center Points p. 5 Joint Orientation Lines p. 5 Ankle p. 5 Knee p. 5 Hip p. 8 Joint Orientation Angles
Normal Lower Limb Alignment and Joint Orientation p. 1 Mechanical and Anatomic Bone Axes p. 1 Joint Center Points p. 5 Joint Orientation Lines p. 5 Ankle p. 5 Knee p. 5 Hip p. 8 Joint Orientation Angles
TASC Manual and Scoresheet Printing Suggestions
 TASC Manual and Scoresheet Printing Suggestions The manual (pages 2-21 of this packet) is meant to be printed in booklet form so that the final form is 8.5x5.5 inches in size (achieved by folding the printed
TASC Manual and Scoresheet Printing Suggestions The manual (pages 2-21 of this packet) is meant to be printed in booklet form so that the final form is 8.5x5.5 inches in size (achieved by folding the printed
MOTION DIAGNOSTIC IMAGING (CMDI)/ GAIT ANALYSIS
 Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title COMPUTERIZED MOTION DIAGNOSTIC IMAGING (CMDI)/ GAIT ANALYSIS Policy Number 2.01.13 Category Technology Assessment Effective Date
Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title COMPUTERIZED MOTION DIAGNOSTIC IMAGING (CMDI)/ GAIT ANALYSIS Policy Number 2.01.13 Category Technology Assessment Effective Date
DDH. Abnormal hip development Traditionally CDH (congenital dysplasia of the hip) Today DDH(developmental dysplasia of the hip)
 DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
DDH Update on Screening Kathryn A Keeler, MD Assistant Professor University of Missouri-Kansas City School of Medicine, Department of Orthopaedic Surgery and Department of Pediatrics Children s Mercy Kansas
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease.
 Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Listen Observe Evaluate Test Refer Guide for primary care providers includes: Surveillance Aid: Assessing Weakness
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Listen Observe Evaluate Test Refer Guide for primary care providers includes: Surveillance Aid: Assessing Weakness
Hypotonia Care Pathway Update: Diagnosis Garey Noritz, MD...
 Hypotonia Care Pathway Update: Diagnosis Garey Noritz, MD Disclosure Information- AACPDM 72 nd Annual Meeting October 9-13, 2018 Speaker Name: Garey Noritz, MD Disclosure of Relevant Financial Relationships
Hypotonia Care Pathway Update: Diagnosis Garey Noritz, MD Disclosure Information- AACPDM 72 nd Annual Meeting October 9-13, 2018 Speaker Name: Garey Noritz, MD Disclosure of Relevant Financial Relationships
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Hip surveillance and management of the displaced hip in cerebral palsy
 J Child Orthop (2013) 7:407 413 DOI 10.1007/s11832-013-0515-6 CURRENT CONCEPT REVIEW Hip surveillance and management of the displaced hip in cerebral palsy J. E. Robb G. Hägglund Received: 19 February
J Child Orthop (2013) 7:407 413 DOI 10.1007/s11832-013-0515-6 CURRENT CONCEPT REVIEW Hip surveillance and management of the displaced hip in cerebral palsy J. E. Robb G. Hägglund Received: 19 February
PROBLEMS IN THE EARLY RECOGNITION OF DYSPLASIA
 PROBLEMS IN THE EARLY RECOGNITION OF HIP DYSPLASIA STUART J. M. DAVIES, GEOFFREY WALKER From Queen Mary s Hospitalfor Children, Carshalton Ten children who had clinically stable hips at birth were radiographed
PROBLEMS IN THE EARLY RECOGNITION OF HIP DYSPLASIA STUART J. M. DAVIES, GEOFFREY WALKER From Queen Mary s Hospitalfor Children, Carshalton Ten children who had clinically stable hips at birth were radiographed
Department of Rehabilitation Medicine, CHA Bundang Medical Center, CHA University, Seongnam, Korea
 Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
Effects of lower limb strength training on gross motor functions in children with cerebral palsy
 International Journal of Contemporary Pediatrics Shah VS et al. Int J Contemp Pediatr. 2018 Sep;5(5):1923-1927 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
International Journal of Contemporary Pediatrics Shah VS et al. Int J Contemp Pediatr. 2018 Sep;5(5):1923-1927 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study
 Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
Motor function after selective dorsal rhizotomy: a 10-year practice-based follow-up study
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Motor function after selective dorsal rhizotomy: a 10-year practice-based follow-up study ANNIKA LUNDKVIST JOSENBY 1 PHILIPPE WAGNER 2 GUN-BRITT
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Motor function after selective dorsal rhizotomy: a 10-year practice-based follow-up study ANNIKA LUNDKVIST JOSENBY 1 PHILIPPE WAGNER 2 GUN-BRITT
Adult Hip Dysplasia David S. Feldman, MD
 Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
Adult Hip Dysplasia David S. Feldman, MD Chief of Pediatric Orthopedic Surgery Professor of Orthopedic Surgery & Pediatrics NYU Langone Medical Center & NYU Hospital for Joint Diseases Overview Adult hip
Prevalence and pattern of upper limb involvement in cerebral palsy
 J Child Orthop (2014) 8:215 219 DOI 10.1007/s11832-014-0593-0 ORIGINAL CLINICAL ARTICLE Prevalence and pattern of upper limb involvement in cerebral palsy Daoud Makki J. Duodu Matthew Nixon Received: 14
J Child Orthop (2014) 8:215 219 DOI 10.1007/s11832-014-0593-0 ORIGINAL CLINICAL ARTICLE Prevalence and pattern of upper limb involvement in cerebral palsy Daoud Makki J. Duodu Matthew Nixon Received: 14
Introduction Nutrition & CP ESPGHAN guidelines Flemish situation Conclusion
 // Overview Nutritional status and body composition of Flemish children with cerebral palsy Koen Huysentruyt MD, PhD Onderzoekssymposium Wetenschappelijk onderbouwde zorg voor kinderen met cerebrale parese
// Overview Nutritional status and body composition of Flemish children with cerebral palsy Koen Huysentruyt MD, PhD Onderzoekssymposium Wetenschappelijk onderbouwde zorg voor kinderen met cerebrale parese
Pediatric Orthopedics: ``To Refer or Not to Refer``
 Pediatric Orthopedics: ``To Refer or Not to Refer`` Thierry E. Benaroch, MD, FRCS(C) McGill University Health Centre Intoeing Knock knees Bowlegs Flatfeet Toe walking Knee pain Hip click Intoeing Objectives
Pediatric Orthopedics: ``To Refer or Not to Refer`` Thierry E. Benaroch, MD, FRCS(C) McGill University Health Centre Intoeing Knock knees Bowlegs Flatfeet Toe walking Knee pain Hip click Intoeing Objectives
The influence of age at single-event multilevel surgery on outcome in children with cerebral palsy who walk with flexed knee gait
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE The influence of age at single-event multilevel surgery on outcome in children with cerebral palsy who walk with flexed knee gait MARTIN ƒvehlýk
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE The influence of age at single-event multilevel surgery on outcome in children with cerebral palsy who walk with flexed knee gait MARTIN ƒvehlýk
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH)
 Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
Evaluation of three ultrasound techniques used for the diagnosis of developmental dysplasia of the hip (DDH) Poster No.: C-2049 Congress: ECR 2012 Type: Scientific Exhibit Authors: E. M. D. B. Pacheco,
SWASH CERTIFICATION EXAM
 SWASH CERTIFICATION EXAM Sitting Walking And Standing Hip Orthosis Today s Date: Location: Name: License #: Employer: Address: Ste/Apt #: City: State: Zip: Email Address: 1) Which of the following are
SWASH CERTIFICATION EXAM Sitting Walking And Standing Hip Orthosis Today s Date: Location: Name: License #: Employer: Address: Ste/Apt #: City: State: Zip: Email Address: 1) Which of the following are
Effect of acquisition ages of gross motor functions on functional motor impairment in children with cerebral palsy
 Original Article 191 DO I: 10.4274/tpa.896 Effect of acquisition ages of gross motor functions on functional motor impairment in children with cerebral palsy Özgün Kaya Kara, Akmer Mutlu, Mintaze Kerem
Original Article 191 DO I: 10.4274/tpa.896 Effect of acquisition ages of gross motor functions on functional motor impairment in children with cerebral palsy Özgün Kaya Kara, Akmer Mutlu, Mintaze Kerem
Toe walking gives rise to parental concern. Therefore, toe-walkers are often referred at the 3 years of age.
 IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
REX REX Clinical Assessment Guide
 REX Clinical Assessment Guide All product names and brand names in this document are trademarks or registered trademarks of their respective holders. Copyright Rex Bionics Ltd 2016. All rights reserved.
REX Clinical Assessment Guide All product names and brand names in this document are trademarks or registered trademarks of their respective holders. Copyright Rex Bionics Ltd 2016. All rights reserved.
Preserve or improve gait efficiency Early identification and stabilization or correction of lower extremity deformities
 ORTHOPEDICS Primary Outcomes Maintenance of a stable and balanced spine. Optimize pulmonary function. Avoid restrictive pulmonary disease. Optimize spinal growth. Avoid or facilitate healing of sacral/ischial
ORTHOPEDICS Primary Outcomes Maintenance of a stable and balanced spine. Optimize pulmonary function. Avoid restrictive pulmonary disease. Optimize spinal growth. Avoid or facilitate healing of sacral/ischial
Chapter 4B: Reliability Trial 2. Chapter 4B. Reliability. General issues. Inter-rater. Intra - rater. Test - Re-test
 Chapter 4B: Reliability Trial 2 Chapter 4B Reliability General issues Inter-rater Intra - rater Test - Re-test Trial 2 The second clinical trial was conducted in the spring of 1992 using SPCM Draft 6,
Chapter 4B: Reliability Trial 2 Chapter 4B Reliability General issues Inter-rater Intra - rater Test - Re-test Trial 2 The second clinical trial was conducted in the spring of 1992 using SPCM Draft 6,
Circles are Pointless - Angles in the assessment of adult hip dysplasia are not!
 Circles are Pointless - Angles in the assessment of adult hip dysplasia are not! Poster No.: C-1964 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit S. E. West, S. G. Cross, J. Adu,
Circles are Pointless - Angles in the assessment of adult hip dysplasia are not! Poster No.: C-1964 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit S. E. West, S. G. Cross, J. Adu,
Risk factors for emergence and progression of scoliosis in children with severe cerebral palsy: a systematic review
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Risk factors for emergence and progression of scoliosis in children with severe cerebral palsy: a systematic review MARIANNE J B LOETERS 1,2 CAREL G B MAATHUIS
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Risk factors for emergence and progression of scoliosis in children with severe cerebral palsy: a systematic review MARIANNE J B LOETERS 1,2 CAREL G B MAATHUIS
Cerebral Palsy An Update
 Cerebral Palsy An Update Richard D. Stevenson, MD Professor of Pediatrics Disclaimer: Edited a book mentioned in presentation Introduction CP is a common condition presenting in childhood that impacts
Cerebral Palsy An Update Richard D. Stevenson, MD Professor of Pediatrics Disclaimer: Edited a book mentioned in presentation Introduction CP is a common condition presenting in childhood that impacts
MUSCLE STRENGTH EXAMINATION OF HAND AND MOTOR SKILLS OF HAND IN CEREBRAL PALSY
 SCRIPTA MEDICA (BRNO) 81 (4): 205 210, December 2008 MUSCLE STRENGTH EXAMINATION OF HAND AND MOTOR SKILLS OF HAND IN CEREBRAL PALSY Drlíková L. 1, havelková a., MOHSIN A. H. K. 2, MAŠEK M. 2, POHANKA M.
SCRIPTA MEDICA (BRNO) 81 (4): 205 210, December 2008 MUSCLE STRENGTH EXAMINATION OF HAND AND MOTOR SKILLS OF HAND IN CEREBRAL PALSY Drlíková L. 1, havelková a., MOHSIN A. H. K. 2, MAŠEK M. 2, POHANKA M.
GLOSSARY. Active assisted movement: movement where the actions are assisted by an outside force.
 GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
WELCOME. CP Hip Symposium
 WELCOME CP Hip Symposium Freeman Miller Kirk Dabney AI dupont Hospital for Children Wilmington, DE This is a Follow up Meeting First International Meeting for CP Hip Liverpool April 2010 Organized by Dr.
WELCOME CP Hip Symposium Freeman Miller Kirk Dabney AI dupont Hospital for Children Wilmington, DE This is a Follow up Meeting First International Meeting for CP Hip Liverpool April 2010 Organized by Dr.
The aim of this booklet is to provide you with information about your operation and the treatment you will receive.
 Patient Information Physiotherapy after Total Hip Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Patient Information Physiotherapy after Total Hip Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS
 Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS Professor Iona Novak Cerebral Palsy Alliance Australia Neuroplasticity is fundamentally why we believe in
Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS Professor Iona Novak Cerebral Palsy Alliance Australia Neuroplasticity is fundamentally why we believe in
A randomized clinical trial of strength training in young people with cerebral palsy
 A randomized clinical trial of strength training in young people with cerebral palsy Karen J Dodd PhD*; Nicholas F Taylor PhD, Musculoskeletal Research Centre, School of Physiotherapy, Faculty of Health
A randomized clinical trial of strength training in young people with cerebral palsy Karen J Dodd PhD*; Nicholas F Taylor PhD, Musculoskeletal Research Centre, School of Physiotherapy, Faculty of Health
Guidelines, Policies and Statements. Statement on the Use of Ultrasound in the Diagnosis of Developmental Hip Dysplasia and Dislocation
 Guidelines, Policies and Statements Statement on the Use of Ultrasound in the Diagnosis of Developmental Hip Dysplasia and Dislocation Approved by Council June 2018 Disclaimer and Copyright The ASUM Standards
Guidelines, Policies and Statements Statement on the Use of Ultrasound in the Diagnosis of Developmental Hip Dysplasia and Dislocation Approved by Council June 2018 Disclaimer and Copyright The ASUM Standards
Case Study: Christopher
 Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Lifting and Separating
 Lifting and Separating Implementing a 24 - hour Posture Management Program ISS 2018 Lauren Rosen, PT, MPT, MSMS, ATP/SMS and Lee Ann Hoffman, OT, MSc Rehab: Posture Management 1 Learning Objectives 1.
Lifting and Separating Implementing a 24 - hour Posture Management Program ISS 2018 Lauren Rosen, PT, MPT, MSMS, ATP/SMS and Lee Ann Hoffman, OT, MSc Rehab: Posture Management 1 Learning Objectives 1.
Case Report Anterior Hip Subluxation due to Lumbar Degenerative Kyphosis and Posterior Pelvic Tilt
 Case Reports in Orthopedics, Article ID 806157, 4 pages http://dx.doi.org/10.1155/2014/806157 Case Report Anterior Hip Subluxation due to Lumbar Degenerative Kyphosis and Posterior Pelvic Tilt Hiroyuki
Case Reports in Orthopedics, Article ID 806157, 4 pages http://dx.doi.org/10.1155/2014/806157 Case Report Anterior Hip Subluxation due to Lumbar Degenerative Kyphosis and Posterior Pelvic Tilt Hiroyuki
Hip ultrasound for developmental dysplasia: the 50% rule
 Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
Pediatr Radiol (2017) 47:817 821 DOI 10.1007/s00247-017-3802-4 COMMENTARY Hip ultrasound for developmental dysplasia: the 50% rule H. Theodore Harcke 1 & B. Pruszczynski 2 Received: 27 October 2016 /Revised:
2016 Report to the Public About. Hip and Knee Replacements
 2016 Report to the Public About Hip and Knee Replacements Using Data to Improve Patient Care Joint replacement surgery has helped relieve pain and restore function for millions of people. Most people who
2016 Report to the Public About Hip and Knee Replacements Using Data to Improve Patient Care Joint replacement surgery has helped relieve pain and restore function for millions of people. Most people who
Use of a patella marker to improve tracking of dynamic hip rotation range of motion
 Gait & Posture 27 (2008) 530 534 www.elsevier.com/locate/gaitpost Use of a patella marker to improve tracking of dynamic hip rotation range of motion Tishya A.L. Wren a,b, *, K. Patrick Do a, Reiko Hara
Gait & Posture 27 (2008) 530 534 www.elsevier.com/locate/gaitpost Use of a patella marker to improve tracking of dynamic hip rotation range of motion Tishya A.L. Wren a,b, *, K. Patrick Do a, Reiko Hara
Lower Extremity Dislocations: Management and Triage on the Field
 Lower Extremity Dislocations: Management and Triage on the Field Scott J Tarantino, MD Towson Orthopaedic Associates, Towson, MD None Disclsures Purpose To provide you with knowledge which may guide you
Lower Extremity Dislocations: Management and Triage on the Field Scott J Tarantino, MD Towson Orthopaedic Associates, Towson, MD None Disclsures Purpose To provide you with knowledge which may guide you
Facts about Scoliosis
 Facts about Scoliosis Have you or someone in your family recently been diagnosed with scoliosis? Or do you suspect somebody you know has the condition? That is when we usually start googling to learn all
Facts about Scoliosis Have you or someone in your family recently been diagnosed with scoliosis? Or do you suspect somebody you know has the condition? That is when we usually start googling to learn all
Algorithm #1 Lumbo-Pelvic Region Examination
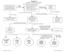 Red Screen for Potentially Serious Conditions (i.e., Red Flags) including Neurologic when indicated Positive Findings Algorithm #1 Lumbo-Pelvic Region Clinical Prediction Rule Screening: Duration of symptoms
Red Screen for Potentially Serious Conditions (i.e., Red Flags) including Neurologic when indicated Positive Findings Algorithm #1 Lumbo-Pelvic Region Clinical Prediction Rule Screening: Duration of symptoms
CLINICAL GUIDELINES ID TAG Developmental Dysplasia of hips Regional Guideline Mr Aidan Cosgrove. Title:
 Title: Author: Designation: Speciality / Division: Directorate: CLINICAL GUIDELINES ID TAG Developmental Dysplasia of hips Regional Guideline Mr Aidan Cosgrove Paediatric Orthopaedics Orthopaedic Orthopaedics
Title: Author: Designation: Speciality / Division: Directorate: CLINICAL GUIDELINES ID TAG Developmental Dysplasia of hips Regional Guideline Mr Aidan Cosgrove Paediatric Orthopaedics Orthopaedic Orthopaedics
Dr Teresa Pountney PhD MA FCSP Chailey Heritage Clinical Services North Chailey, East Sussex, BN8 4JN Tel:
 Dr Teresa Pountney PhD MA FCSP Chailey Heritage Clinical Services North Chailey, East Sussex, BN8 4JN Tel: 01825 720724 Email: terry.pountney@nhs.net CURRENT POSTS: Head of Research, Physiotherapist, Chailey
Dr Teresa Pountney PhD MA FCSP Chailey Heritage Clinical Services North Chailey, East Sussex, BN8 4JN Tel: 01825 720724 Email: terry.pountney@nhs.net CURRENT POSTS: Head of Research, Physiotherapist, Chailey
The McHale procedure in the treatment of the painful chronically dislocated hip in adolescents and adults with cerebral palsy
 Acta Orthop. Belg., 2009, 75, 181-188 ORIGINAL STUDY The McHale procedure in the treatment of the painful chronically dislocated hip in adolescents and adults with cerebral palsy Anne VAN RIET, Pierre
Acta Orthop. Belg., 2009, 75, 181-188 ORIGINAL STUDY The McHale procedure in the treatment of the painful chronically dislocated hip in adolescents and adults with cerebral palsy Anne VAN RIET, Pierre
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK
 ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
Communication and CP: What do CFCS scores tell us?
 CFCS Communication and CP: What do CFCS scores tell us? Mary Jo Cooley Hidecker PhD, MS, MA, CCC-A/SLP Email: MJCHidecker@uca.edu Website: www.cfcs.us 1 Health Condition (Disorder or Disease) Body Functions
CFCS Communication and CP: What do CFCS scores tell us? Mary Jo Cooley Hidecker PhD, MS, MA, CCC-A/SLP Email: MJCHidecker@uca.edu Website: www.cfcs.us 1 Health Condition (Disorder or Disease) Body Functions
OPAS OSTEOARTHRITIS PROGRAMME AT SPORTS SURGERY CLINIC.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries OPAS AT SPORTS SURGERY CLINIC www.sportssurgeryclinic.com INTRODUCTION Osteoarthritis Normal Joint Destruction of Cartilage
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries OPAS AT SPORTS SURGERY CLINIC www.sportssurgeryclinic.com INTRODUCTION Osteoarthritis Normal Joint Destruction of Cartilage
Biomechanics and Its Application to Seating
 Biomechanics and Its Application K E L LY W A U G H, P T, M A P T, AT P S E N I O R I N S T R U C TO R / C L I N I C C O O R D I N ATO R A S S I S T I V E T E C H N O LO G Y PA R T N E R S S C H O O L
Biomechanics and Its Application K E L LY W A U G H, P T, M A P T, AT P S E N I O R I N S T R U C TO R / C L I N I C C O O R D I N ATO R A S S I S T I V E T E C H N O LO G Y PA R T N E R S S C H O O L
A Collection of Brief, Reliable and Valid Instruments to Obtain a Holistic Picture of Children with Cerebral Palsy: Products of the Move & PLAY Study
 A Collection of Brief, Reliable and Valid Instruments to Obtain a Holistic Picture of Children with Cerebral Palsy: Products of the Move & PLAY Study Move & PLAY Study Team Lehmann Day May 2013 Movement
A Collection of Brief, Reliable and Valid Instruments to Obtain a Holistic Picture of Children with Cerebral Palsy: Products of the Move & PLAY Study Move & PLAY Study Team Lehmann Day May 2013 Movement
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ
 Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
Ultrasound Evaluation of Pavlik Harness in Treatment of Infants with Developmental Dysplasia of the Hip: Prone Axial Approach to Harness in Situ C Fernández, MD; M Guasp, MD; J Gómez Fernández-Montes,
Case Studies: Low Back Pain in the Athlete. Jim Messerly DO
 Case Studies: Low Back Pain in the Athlete Jim Messerly DO Nothing to disclose Case #1 History 15 y/o male presents for evaluation of his low back pain. His pain has been present for several months. The
Case Studies: Low Back Pain in the Athlete Jim Messerly DO Nothing to disclose Case #1 History 15 y/o male presents for evaluation of his low back pain. His pain has been present for several months. The
