Microsurgical dissection of facial nerve in parotidectomy: a discussion of techniques and long-term results
|
|
|
- Joshua Neal
- 6 years ago
- Views:
Transcription
1 Original Article Microsurgical dissection of facial nerve in parotidectomy: a discussion of techniques and long-term results Fabio Nicoli 1,2,3, Christopher D Ambrosia 1,4, Davide Lazzeri 2,3, Georgios Orfaniotis 1, Pedro Ciudad 1, Michele Maruccia 1, Li Tzong Shiun 1,5, Bulent Sacak 1,6, Shih-Heng Chen 5, Hung-Chi Chen 1 1 Department of Plastic and Reconstructive Surgery, China Medical University Hospital, Taichung, Taiwan; 2 Department of Plastic and Reconstructive Surgery, University of Rome Tor Vergata, Rome, Italy; 3 Plastic Reconstructive and Aesthetic Surgery, Villa Salaria Clinic, Rome, Italy; 4 Columbia University School of Medicine, New York, USA; 5 Department of Plastic and Reconstructive Surgery, Chang Gung Memorial Hospital, Linkou, Taiwan; 6 Department of Plastic and Reconstructive Surgery, Marmara University School of Medicine, Istanbul, Turkey Contributions: (I) Conception and design: F Nicoli, C D Ambrosia, D Lazzeri, HC Chen; (II) Administrative support: LT Shiun, B Sacak, SH Chen, HC Chen; (III) Provision of study materials or patients: G Orfaniotis, P Ciudad, M Maruccia, LT Shiun, B Sacak; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: F Nicoli, C D Ambrosia, G Orfaniotis, P Ciudad, M Maruccia, HC Chen; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Prof. Hung-Chi Chen, M.D., Ph.D., F.A.C.S. Department of Plastic and Reconstructive Surgery, China Medical University Hospital, 2 Yuh-Der Road, 40447, Taichung, Taiwan. D19722@mail.cmuh.org.tw. Background: Parotidectomy has well-documented post-operative complications. Dissection of the facial nerve branches can be challenging even under loupe magnification, and partial, or complete injury of the nerve branches can occur during surgery. To reduce this risk and the associated complications, we propose a number of microsurgical best practices, which can be performed during parotidectomy. Methods: A retrospective survey was conducted on 109 patients (45 males and 64 females, average age 46.2 years, range of 6 to 74 years) who underwent parotidectomy in two different institutions. Results: Our data showed no permanent injury to the facial nerve, and 17% of neuroapraxia that had resolved with time. Post-operative complications have occurred in 33 cases (30% rate). In the superficial parotidectomy cohort (78 patients), the number of complications was 17 (21%). In the total parotidectomy cohort (31 patients), the number of complications was 16 (51%). Conclusions: Based on our results, we believe that the use of microsurgical techniques during parotidectomy may represent a useful tool in improving accuracy and minimising local tissue trauma that can affect nerve recovery. This is particularly true in situations such as tumor recurrence, tissue fibrosis or in case of sizeable tumors around the facial nerve branches. We believe that the decreased risk of facial nerve postoperative symptoms outweigh the disadvantage of increased operative time of this procedure. Keywords: Facial nerve; parotid; parotidectomy; parotid tumor; microsurgery Submitted Oct 29, Accepted for publication Feb 06, doi: /gs View this article at: Introduction Parotidectomy, a surgical procedure to treat benign and malignant diseases of the parotid gland, has well-documented post-operative complications (1,2). Major complications include facial nerve paresis or paralysis, and minor complications include salivary fistula, auriculotemporal syndrome (gustatory sweating or Frey syndrome), great auricular nerve anesthesia, and hemorrhage, infection, seroma formation (3,4). The major complications are often a result of damage to the facial nerve which may be accompanied by permanent disfigurement and a significant negative effect on the patient s quality of life (4,5). Surgical technique is one of the primary factors contributing to post-operative complication rates and there is a continuous
2 Gland Surgery, Vol 6, No 4 August 2017 endeavor by surgeons to minimize the risk of complications resulting from parotidectomy (3,6,7). Facial nerve branches are of small size and often difficult to identify even when loupe magnification is used. As a result partial or complete severance of the nerve branches can occur during surgery. Studies have demonstrated that incidences of temporary facial nerve paralysis or paresis following parotidectomy range from 9% to 100%. Permanent paralysis or weakness occurs in 0% to 29% of cases (3,8-10). Moreover, after more extensive operations, including total parotidectomy, temporary paresis and paralysis are even more frequent. To reduce these risks, we propose a number of microsurgical best practices for parotidectomy, and in this study, we will analyze the long-term results we have achieved utilizing these techniques. Methods Patient selection and characteristics This study was a retrospective case analysis of 109 patients who underwent parotidectomy performed by the authors between January 1994 and December 2014 at Chang Gung Memorial Hospital and China Medical University Hospital. The institutional review board of the hospital approved the study (CMUH No: DMR016-IRB-862). The procedures were planned based on clinical findings and the results of fine needle biopsies, with additional imaging in the form of ultrasound scans, CT scans of the head neck with medium contrast and MRIs. Depending on the pathology, size and location of the tumors, superficial or total conservative parotidectomies were performed. The patient-related data collected included age, gender, histological diagnoses, procedure type, facial nerve function preoperatively and postoperatively, and complications with timings. Facial nerve function was graded using the standard House-Brackmann (HB) method. Patients were assessed on the second day, 1 week and 3 months after the treatment. Of the total 109 patients, 45 were males and 64 were females. The average age of the patient cohort was 46.2 years with a range of 6 to 74 years. Surgical procedure The skin incision started at the preauricular region and continued to the internal margin of the tragus. Once the incision reached the ear lobe, it continued 309 posteriorly for 1 to 2 cm on the mastoid, and ran down on the inferior border of the mandible for 4 5 cm. Next, the skin flap was elevated at the level of the superficial plane of the parotid fascia. Following this, the dissection extended to the inferior border of the parotid under the microscope, until the marginal mandibular branch of the facial nerve was identified at a level, where became more superficial and crossed the facial artery and vein. Consequently, the dissection continued in a retrograde fashion under magnification aiming to isolate the nerve branches until their origin from the main trunk. The great auricular nerves as well as the superficial aponeurotic muscle system were always preserved. The entire dissection took place on a plane superficial to the facial nerve trunk and branches, and was carried out using microsurgical scissors and microforceps. Once the main trunks with its branches were isolated, the dissection could proceed on the deep plane removing the whole gland in case a total parotidectomy was required. During the procedure, bipolar diathermy and small hemostatic clips were used for hemostasis. Nerve branches were found without the use of a nerve stimulator. At the conclusion of the surgery, the fascial planes were sutured, a suction drain was inserted, and the skin incision was closed using no resorbable sutures. Results A total of 109 surgical procedures were performed. Seventyeight patients received superficial parotidectomies and 31 patients underwent total conservative parotidectomy. The average operation time in the superficial parotidectomy group was 3 hours, ranging from 2 hours 15 minutes to 4 hours 30 minutes. In the total parotidectomy group, the average operation time was 3 hours 45 minutes, ranging from 2 hours 45 minutes to 7 hours 45 minutes. In the entire patient population, follow-up period ranged from 3 months to 16 years with a median of 32 months. The number of post-operative complication was 33 with a rate of 30%. In the superficial parotidectomy cohort (78 patients), the number of complications was 17 (21%). In the total parotidectomy cohort (31 patients), the number of complications was 16 (51%). In the superficial parotidectomy cohort 7 patients presented temporary facial nerve palsy, 5 had salivary fistula formation and five patients developed Frey s syndrome. Post-operative complications in the total parotidectomy patient cohort included temporary facial nerve palsy in 12 patients, salivary fistula in one patient and development of Frey s syndrome in 4 patients.
3 310 Nicoli et al. Microsurgical dissection of parotid tumors Table 1 Patients data, operative procedure and complications Disease Sex Age average (range) Pathologic diagnosis Procedure (Sup/Tot) Facial palsy (temp) Complications Salivary fistula Frey s syndrome Benignant (n=106) Malignant (n=3) 62F; 44 M 42.6 ( ) 2 F; 1 M 54.5 ( ) Pleomorphic adenoma [64] 52 Sup Tot Monomorphic adenoma [18] 14 Sup Tot Hemangioma [12] 2 Sup Tot Parotid cyst [6] 5 Sup Tot Basal cell adenoma [4] 3 Sup Tot Fibrolipoma [2] 2 Sup Cystadenocarcinoma [2] 2 Tot Mucoepidermoid carcinoma [1] 1 Tot Total (n=109) 64 F; Sup M ( ) 31 Tot Sup, superficial parotidectomy; Tot, total parotidectomy. Data are summarized in Table 1. In patients who demonstrated temporary facial nerve palsy, seven patients had buccal nerve branch damage and six patients had marginal nerve branch damage. Four patients had symptoms from both the buccal and marginal branches and two patients from the frontal branch. These patients had moderate dysfunction using the HB criteria grossly obvious but no disfiguring difference between the two sides of the face, noticeable but no severe synkinesis, contracture, and/or hemifacial spasm. This was accompanied by loss of sensation or numbness as well as some incontinence of the lower lip. These complications resolved in all 19 patients between 14 days and 3 months post-operative. There were no cases of permanent facial nerve palsy. Clinical pictures are showed in Figures 1-4. The tumor pathology showed pleomorphic adenoma in 64 cases (58%), Warthin tumor in 18 cases (16%), hemangioma in 12 cases (11%), parotid cyst in 6 cases (5%), basal cell adenoma in 4 patients (4%) and fibrolipoma in 2 cases (2%). There were also three cases of malignant disease: two cystadenocarcinoma and one mucoepidermoid carcinoma. Discussion Preservation of the facial nerve remains one of the most important and challenging aspects of parotid gland surgery. Minimizing the incidence and severity of post-operative facial nerve damage is of paramount concern to the surgeon. In prior studies, Henney et al. (3) have described the incidence rates of post-operative temporary facial paralysis after initial parotid surgery to be 42%, of which 78% recovered within 3 months. Marshall et al. (11) have reported that permanent facial paralysis occurred in 1.9% in their series while Mehle et al. (9) 3.9% of cases. In this study, the incidence of temporary facial paralysis was 17% with no reported cases of permanent facial paralysis. In general, complications following parotid gland surgery are grossly dependent on the aggressiveness and
4 Gland Surgery, Vol 6, No 4 August A B C D E F Figure 1 Preoperative and intraoperative microsurgical dissection of facial nerve of 48 years old woman. (A) Preoperative plan of parotidectomy; (B) microsurgical dissection of superficial parotid has been done; (C) specimen of pleomorphic adenoma; (D) view under the microscope of facial nerve branches; (E) the facial nerve is identified and preserved; (F) bipolar diathermy and small hemostatic clips are used for hemostasis. the dimensions of the tumor as well as its relation with the facial nerve. Ward (12), Woods (13), Aljamo (14), Mehle (9), and Valentini (15) have reported that superficial parotidectomy and/or total parotidectomy with preservation of the facial nerve is the gold standard for excision of parotid tumors. However, in their studies, they report a number of post-operative complications related to facial nerve injury. To minimize these complications, we introduce the use of microsurgical techniques for the dissection of the facial nerve. With the assistance of the microscope, we were able to accurately locate all facial nerve branches thus enabling their preservation. Although, even in conventional dissection of facial nerve with naked eye or loupes the nerve branches appear grossly intact, the tiny vessels accompanying the nerve branches may be injured, resulting in temporary functional problems such as weakness in mouth closure and oral incontinence. The benefits of dissection under the microscope are particularly apparent in cases with severe fibrosis around the parotid gland, such as in recurrent parotid tumors, where the absence of distinct tissue planes makes difficult to distinguish the nerve branches from the surrounding tissue. Compression of the nerve branches may also cause nerve atrophy making identification and preservation of the nerve without magnification extremely difficult (16). The microsurgical dissection can also prove beneficial in paediatric patients where the branches are naturally smaller. Additionally, with the use of microsurgical dissection, small nutrient vessels around the branches of facial nerve can also be preserved. This may offer improved recovery time after surgery, especially for cases with resection of both superficial and deep lobes, in which the nutrient vessels around the nerves can be easily damaged. Finally, Ussmueller (7) and Hahn (17) suggested the use of diathermy scissors and bipolar electrosurgical device to minimize the postoperative bleeding following parotidectomy. In our series, we found that the additional use of microsurgical instruments under magnification allows surgeons to achieve an accurate hemostasis avoiding inadvertent cauterization of tissue in the operating field and unnecessary traction on the nerve branches. Although we found a high rate of temporary facial nerve palsy especially after the dissection in hemangiomas, 5 complications in 12 patients (41%), we suggest utilizing the described
5 312 Nicoli et al. Microsurgical dissection of parotid tumors A B C D Figure 2 Intraoperative and postoperative pictures of a case on a 41-year-old female. (A) Facial nerve branches are dissected and isolated; (B) closure of the defect; (C,D) long-term follow-up at 36 months showing no complications after parotidectomy. A B C Figure 3 Preoperative, intraoperative and immediate postoperative pictures of a 52-year-old male. (A) Preoperative plan; (B) all facial nerve branches carefully dissected under microscope; (C) immediate postoperative picture shows full functional recovery of facial nerve. techniques in those circumstances. The hemangiomas excision along the facial nerve results in challenging dissection in most of the cases, and only by adopting fine and distinct surgical methods we were able to avoid major complications and minimize side effects. Another important aspect of our microsurgical technique was the use of retrograde dissection of the facial nerve. As reported by O Regan B (18) and Scarpini (19), retrograde parotidectomy permits a more conservative surgical approach than anterograde parotidectomy, reducing the extent of dissection and the extent of normal parotid gland sacrificed. Recently, Mahmmood (20) reported low morbidity rates
6 Gland Surgery, Vol 6, No 4 August A B C D Figure 4 Preoperative and intraoperative pictures of a 43-year-old male. (A) Preoperative plan; (B) all facial nerve branches are isolated after total parotidectomy; (C) the parotid lesion is removed leaving intact the nerve branches; (D) closure of the defect and suction drainage. with a temporary facial nerve weakness of 26.6%. This study suggested to perform a retrograde approach using the buccal branch as a guide to identify the nerve trunk and the rest of the branches. Lai et al. (21) used the marginal mandibular nerve as the landmark in their 54 superficial parotidectomies and the rate of transient paralysis was 22.2%. Mahmmood (20) and K. Anjum (22) studies utilized the buccal branch as a guide in the retrograde technique parotidectomy and reported respectively 26.6% and 46.0% of temporary facial palsy. Although Lai (21) found in his study lesser complications, he reported also a main major complication as permanent facial nerve paralysis (1.4%). In our 78 cases of superficial parotidectomy only 9% reported temporary facial palsy, and none permanent palsy. The average operation time was 3 hours for superficial parotidectomies and 3 hours 45 minutes, for total. Disadvantages of this method are the longer operative time and the increased cost for the microsurgical equipment. However, in our opinion these are outweighed by the reduced rate of complications and lower risk of temporary or permanent nerve injury. This microsurgical method allows easier identification of nerve branches and trunk, thus can add potential benefits especially in cases impacted by fibrosis, tumor size, age of patient. A limit of this study can be represented by the significant large period and the multicentricity, although some of the surgeons were trained in both hospitals. Furthermore, the HB scale, used for the measurement of facial nerve involvement, can have a significant inter-observer variability during a long period study. Conclusions Our data confirms the low morbidity associated with superficial parotidectomy and total conservative parotidectomy using microsurgical techniques. In a consecutive series of 109 cases and a long-term followup period, no permanent injury to the facial nerve was reported, whilst 7% of cases sustained temporary nerve injury. Further comparative studies with conventional techniques are necessary but, in our opinion, the use of retrograde dissection of the facial nerve branches under microscope during parotidectomy, may represent a useful tool in improving accuracy and minimizing local tissue trauma that can affect nerve recovery. This is particularly true in situations such as tumor recurrence, tissue fibrosis or in case of sizeable tumors around the facial nerve branches. We believe that the decreased risk of facial nerve postoperative symptoms outweigh the disadvantage of increased operative time of this procedure.
7 314 Nicoli et al. Microsurgical dissection of parotid tumors Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. Ethical Statement: The institutional review board of the hospital approved the study (CMUH No: DMR016- IRB-862) and written informed consent was obtained from all patients. References 1. Mohammed F, Asaria J, Payne RJ, et al. Retrospective review of 242 consecutive patients treated surgically for parotid gland tumours. J Otolaryngol Head Neck Surg 2008;37: Nouraei SA, Ismail Y, Ferguson MS, et al. Analysis of complications following surgical treatment of benign parotid disease. ANZ J Surg 2008;78: Henney SE, Brown R, Phillips D. Parotidectomy: the timing of post-operative complications. Eur Arch Otorhinolaryngol 2010;267: Patel N, Har-El G, Rosenfeld R. Quality of life after great auricular nerve sacrifice during parotidectomy. Arch Otolaryngol Head Neck Surg 2001;127: Nitzan D, Kronenberg J, Horowitz Z, et al. Quality of life following parotidectomy for malignant and benign disease. Plast Reconstr Surg 2004;114: Watanabe Y, Ishikawa M, Shojaku H, et al. Facial nerve palsy as a complication of parotid gland surgery and its prevention. Acta Otolaryngol Suppl 1993;504: Ussmueller JO, Jaehne M, Neumann BG. The use of diathermy scissors in parotid gland surgery. Arch Otolaryngol Head Neck Surg 2004;130: Harney M, Walsh P, Conlon B, et al. Parotid gland surgery: a retrospective review of 108 cases. J Laryngol Otol 2002;116: Mehle ME, Kraus DH, Wood BG, et al. Facial nerve morbidity following parotid surgery for benign disease: the Cleveland Clinic Foundation experience. Laryngoscope 1993;103: Guntinas-Lichius O, Gabriel B, Klussmann JP. Risk of facial palsy and severe Frey's syndrome after conservative parotidectomy for benign disease: analysis of 610 operations. Acta Otolaryngol 2006;126: Marshall AH, Quraishi SM, Bradley PJ. Patients' perspectives on the short- and long-term outcomes following surgery for benign parotid neoplasms. J Laryngol Otol 2003;117: Ward CM. Injury of the facial nerve during surgery of the parotid gland. Br J Surg 1975;62: Woods JE. Parotidectomy versus limited resection for benign parotid masses. Am J Surg 1985;149: Alajmo E, Polli G, De Meester W. Total parotidectomy--a routine treatment for parotid gland swellings? J Laryngol Otol 1989;103: Valentini V, Fabiani F, Perugini M, et al. Surgical techniques in the treatment of pleomorphic adenoma of the parotid gland: our experience and review of literature. J Craniofac Surg 2001;12: Ciudad P, Yeo MS, Sapountzis S, et al. Microsurgical debulking procedure after free lymph node flap transfer. Microsurgery 2014;34: Hahn CH, Sørensen CH. LigaSure small jaws versus cold knife dissection in superficial parotidectomy. Eur Arch Otorhinolaryngol 2013;270: O Regan B, Bharadwaj G, Bhopal S, et al. Facial nerve morbidity after retrograde nerve dissection in parotid surgery for benign disease: a 10-year prospective observational study of 136 cases. Br J Oral Maxillofac Surg 2007;45: Scarpini M, Amore Bonapasta S, Ruperto M, et al. Retrograde parotidectomy for pleomorphic adenoma of the parotid gland: a conservative and effective approach. J Craniofac Surg 2009;20: Mahmmood VH. Buccal branch as a guide for superficial parotidectomy. J Craniofac Surg 2012;23:e Lai YT, Liang Q, Jia XH, et al. Tumor recurrence and complications of parotidectomy using the marginal mandibular branch as a landmark during the retrograde technique. J Craniofac Surg 2015;26:e Anjum K, Revington PJ, Irvine GH. Superficial parotidectomy: antegrade compared with modified retrograde dissections of the facial nerve. Br J Oral Maxillofac Surg 2008;46: Cite this article as: Nicoli F, D'Ambrosia C, Lazzeri D, Orfaniotis G, Ciudad P, Maruccia M, Shiun LT, Sacak B, Chen SH, Chen HC. Microsurgical dissection of facial nerve in parotidectomy: a discussion of techniques and long-term results.. doi: /gs
Partial Parotidectomy Versus Superficial or Total Parotidectomy
 Middle East Journal of Applied Sciences, 3(4): 259-264, 2013 ISSN: 2077-4613 259 Partial Parotidectomy Versus Superficial or Total Parotidectomy 1 Ibrahim Abde-Albare and 2 Mohamed A. Foda 1 Health Director
Middle East Journal of Applied Sciences, 3(4): 259-264, 2013 ISSN: 2077-4613 259 Partial Parotidectomy Versus Superficial or Total Parotidectomy 1 Ibrahim Abde-Albare and 2 Mohamed A. Foda 1 Health Director
DISORDERS OF THE SALIVARY GLANDS Neoplasms Dr.M.Baskaran Selvapathy S IV
 DISORDERS OF THE SALIVARY GLANDS Neoplasms Dr.M.Baskaran Selvapathy S IV NEOPLASMS A) Epithelial I. Benign Pleomorphic adenoma( Mixed tumour) Adenolymphoma (Warthin s tumour) Oxyphil adenoma (Oncocytoma)
DISORDERS OF THE SALIVARY GLANDS Neoplasms Dr.M.Baskaran Selvapathy S IV NEOPLASMS A) Epithelial I. Benign Pleomorphic adenoma( Mixed tumour) Adenolymphoma (Warthin s tumour) Oxyphil adenoma (Oncocytoma)
STEP 1 INCISION AND ELEVATION OF SKIN FLAP STEP 3 SEPARATE PAROTID GLAND FROM SCM STEP 2 IDENTIFICATON OF GREAT AURICULAR NERVE
 STEP 1 INCISION AND ELEVATION OF SKIN FLAP Create a modified Blair Figure 1 or facelift incision. Figure 2 Raise a superficial cervico-fascial flap between the Superficial Musculo Aponeurotic System (SMAS)
STEP 1 INCISION AND ELEVATION OF SKIN FLAP Create a modified Blair Figure 1 or facelift incision. Figure 2 Raise a superficial cervico-fascial flap between the Superficial Musculo Aponeurotic System (SMAS)
A survey of facial nerve dissection techniques in benign parotid surgery among maxillofacial and ear, nose, and throat surgeons in Nigeria
 Original Article A survey of facial nerve dissection techniques in benign parotid surgery among maxillofacial and ear, nose, and throat surgeons in Nigeria WL Adeyemo, OA Taiwo, OA Somefun 1, HO Olasoji
Original Article A survey of facial nerve dissection techniques in benign parotid surgery among maxillofacial and ear, nose, and throat surgeons in Nigeria WL Adeyemo, OA Taiwo, OA Somefun 1, HO Olasoji
Head and neck cancer - patient information guide
 Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
Parotid Disease Case Discussions. Valerie Jefford November 28, 2002
 Parotid Disease Case Discussions Valerie Jefford November 28, 2002 Case 1 44 y.o. man referred with lump anterior to R ear. Q1 What do you want to know? no pain 2 years but bigger now Smoker Q2 What to
Parotid Disease Case Discussions Valerie Jefford November 28, 2002 Case 1 44 y.o. man referred with lump anterior to R ear. Q1 What do you want to know? no pain 2 years but bigger now Smoker Q2 What to
A study of complications of superficial parotidectomy
 A study of complications of superficial parotidectomy *Dr. Probal Chatterji ------------------------------------------------------------------------------------------------------------------------------
A study of complications of superficial parotidectomy *Dr. Probal Chatterji ------------------------------------------------------------------------------------------------------------------------------
Lya Crichlow, MD Lutheran Medical Center November 21, 2008
 Lya Crichlow, MD Lutheran Medical Center November 21, 2008 Case Presentation 64 year old male presented with a painless mass posterior to the right angle of the mandible for 3 months PMHx HTN COPD BPH
Lya Crichlow, MD Lutheran Medical Center November 21, 2008 Case Presentation 64 year old male presented with a painless mass posterior to the right angle of the mandible for 3 months PMHx HTN COPD BPH
Contemporary treatment of salivary gland tumors. A review of the literature
 DOI: 10.18044/Medinform.201742.682 Contemporary treatment of salivary gland tumors. A review of the literature Ioanna Polichroniadou 1, Panagiotis Karakostas 2, Svetoslav Slavkov 3, Assya Krasteva 4 1.
DOI: 10.18044/Medinform.201742.682 Contemporary treatment of salivary gland tumors. A review of the literature Ioanna Polichroniadou 1, Panagiotis Karakostas 2, Svetoslav Slavkov 3, Assya Krasteva 4 1.
Original Article. Section: Surgery INTRODUCTION
 DOI: 10.21276/aimdr.2018.4.3.SG5 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Retrograde Facial Nerve Dissection Using Zygomatic Branch as Landmark in Parotid Gland Surgery for Pleomorphic Adenoma:
DOI: 10.21276/aimdr.2018.4.3.SG5 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Retrograde Facial Nerve Dissection Using Zygomatic Branch as Landmark in Parotid Gland Surgery for Pleomorphic Adenoma:
Small access postaural parotidectomy: an analysis of techniques, feasibility and safety
 Eur Arch Otorhinolaryngol (2016) 273:1879 1883 DOI 10.1007/s00405-015-3691-9 HEAD AND NECK Small access postaural parotidectomy: an analysis of techniques, feasibility and safety Anthony Po-Wing Yuen 1
Eur Arch Otorhinolaryngol (2016) 273:1879 1883 DOI 10.1007/s00405-015-3691-9 HEAD AND NECK Small access postaural parotidectomy: an analysis of techniques, feasibility and safety Anthony Po-Wing Yuen 1
이하선에발생한와르틴종양 : 증례보고. Warthin Tumor of the Parotid Gland: A Case Report. Jungwoo Cho, Seung Hwan Jung, Jin Su Kim, Je Uk Park, Chang Hyen Kim *
 Korean Journal of Oral and Maxillofacial Pathology 2017;41(4):175-179 ISSN:1225-1577(Print); 2384-0900(Online) Available online at http://journal.kaomp.org https://doi.org/10.17779/kaomp.2017.41.4.004
Korean Journal of Oral and Maxillofacial Pathology 2017;41(4):175-179 ISSN:1225-1577(Print); 2384-0900(Online) Available online at http://journal.kaomp.org https://doi.org/10.17779/kaomp.2017.41.4.004
2. Materials and Methods
 e Scientific World Journal, Article ID 564053, 4 pages http://dx.doi.org/10.1155/2014/564053 Research Article Pleomorphic Adenoma of the Parotid: Extracapsular Dissection Compared with Superficial Parotidectomy
e Scientific World Journal, Article ID 564053, 4 pages http://dx.doi.org/10.1155/2014/564053 Research Article Pleomorphic Adenoma of the Parotid: Extracapsular Dissection Compared with Superficial Parotidectomy
THE GREAT auricular nerve
 ORIGINAL ARTICLE Randomized Prospective Study of the Validity of the Great Auricular Nerve Preservation in Parotidectomy Mauro ecker Martins Vieira, MD; Amélio Ferreira Maia, MD; Jaime Carlos Ribeiro,
ORIGINAL ARTICLE Randomized Prospective Study of the Validity of the Great Auricular Nerve Preservation in Parotidectomy Mauro ecker Martins Vieira, MD; Amélio Ferreira Maia, MD; Jaime Carlos Ribeiro,
Thank You Joe Curry, MD David Cognetti, MD Ryan Heffelfinger, MD
 Thank You Joe Curry, MD David Cognetti, MD Ryan Heffelfinger, MD Anatomy Epidemiology Pathology Treatment Controversies Current Research Largest Salivary Gland 80% is superficial lobe Encased in Superficial
Thank You Joe Curry, MD David Cognetti, MD Ryan Heffelfinger, MD Anatomy Epidemiology Pathology Treatment Controversies Current Research Largest Salivary Gland 80% is superficial lobe Encased in Superficial
Partial Superficial Parotidectomy for Pleomorphic Adenoma. Khalid B Alghamdi, MD*
 Bahrain Medical Bulletin, Vol. 35, No. 4, December 2013 Partial Superficial Parotidectomy for Pleomorphic Adenoma Khalid B Alghamdi, MD* Objective: This study aimed to determine the indications of partial
Bahrain Medical Bulletin, Vol. 35, No. 4, December 2013 Partial Superficial Parotidectomy for Pleomorphic Adenoma Khalid B Alghamdi, MD* Objective: This study aimed to determine the indications of partial
Complications after surgery for benign parotid gland neoplasms: A prospective cohort study
 CLINICAL REVIEW David W. Eisele, MD, Section Editor Complications after surgery for benign parotid gland neoplasms: A prospective cohort study Johanna Ruohoalho, MD, 1 * Antti A. M akitie, MD, PhD, 1,2
CLINICAL REVIEW David W. Eisele, MD, Section Editor Complications after surgery for benign parotid gland neoplasms: A prospective cohort study Johanna Ruohoalho, MD, 1 * Antti A. M akitie, MD, PhD, 1,2
This is the largest of the three major glands. It lies partly in the front of the lower half of the ear and partly below the earlobe.
 Parotid Gland Lumps The lining of the mouth contains many small saliva glands. In addition there are three major glands on each side of the face, the parotid, submandibular and sublingual glands. The Parotid
Parotid Gland Lumps The lining of the mouth contains many small saliva glands. In addition there are three major glands on each side of the face, the parotid, submandibular and sublingual glands. The Parotid
Sacrificing the buccal branch of the facial nerve during parotidectomy
 ORIGINAL ARTICLE Sacrificing the buccal branch of the facial nerve during parotidectomy Muthuswamy Dhiwakar, MS, FRCS,* Zubair A. Khan, MS Department of Otolaryngology Head and Neck Surgery, Kovai Medical
ORIGINAL ARTICLE Sacrificing the buccal branch of the facial nerve during parotidectomy Muthuswamy Dhiwakar, MS, FRCS,* Zubair A. Khan, MS Department of Otolaryngology Head and Neck Surgery, Kovai Medical
Mædica - a Journal of Clinical Medicine
 MAEDICA a Journal of Clinical Medicine 2014; 9(1): 39-43 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Study of Preoperative Predictive Signs in Management of Facial Nerve in Parotid Tumors Magdalena
MAEDICA a Journal of Clinical Medicine 2014; 9(1): 39-43 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Study of Preoperative Predictive Signs in Management of Facial Nerve in Parotid Tumors Magdalena
Giant Pleomorphic Adenoma of the Parotid gland- A Case Report
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 14 Number 1 Giant Pleomorphic Adenoma of the Parotid gland- A Case Report O M.E, U A.N, U Akpan, K J, I Bassey Citation O M.E, U A.N, U Akpan,
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 14 Number 1 Giant Pleomorphic Adenoma of the Parotid gland- A Case Report O M.E, U A.N, U Akpan, K J, I Bassey Citation O M.E, U A.N, U Akpan,
Presented by ; Supervised by ; Shahad Samir Khaleel. Dr.Khalaf Rasheed
 Parotid mass Presented by ; Shahad Samir Khaleel Supervised by ; Dr.Khalaf Rasheed Case sheet كامل دمحم عبيد Name: Age: 37 years Sex: male Occupation : manual worker Residence : D.O.A. :31\10\2011 موصل
Parotid mass Presented by ; Shahad Samir Khaleel Supervised by ; Dr.Khalaf Rasheed Case sheet كامل دمحم عبيد Name: Age: 37 years Sex: male Occupation : manual worker Residence : D.O.A. :31\10\2011 موصل
VI. Head and Neck and aesthetics.
 UEMS ENT SECTION SUBSPECIALTY LOG BOOK IN HEAD AND NECK SURGERY VI. Head and Neck and aesthetics. A. Diagnostic Procedures and multidisciplinary approach a) CLINICAL EXAMINATION 1 investigation of the
UEMS ENT SECTION SUBSPECIALTY LOG BOOK IN HEAD AND NECK SURGERY VI. Head and Neck and aesthetics. A. Diagnostic Procedures and multidisciplinary approach a) CLINICAL EXAMINATION 1 investigation of the
Original Article ABSTRACT
 Kasr El-Aini J. Clin. Oncol. Nucl. Med. Vol.4, No.3-4, July-Oct. 28:51-57 NEMROCK Original Article GREAT AURICULAR NERVE PRESERVATION IMPROVES OUTCOME OF SUPERFICIAL PAROTIDECTOMY Hamed Rashad, Emad Abdel
Kasr El-Aini J. Clin. Oncol. Nucl. Med. Vol.4, No.3-4, July-Oct. 28:51-57 NEMROCK Original Article GREAT AURICULAR NERVE PRESERVATION IMPROVES OUTCOME OF SUPERFICIAL PAROTIDECTOMY Hamed Rashad, Emad Abdel
AMSER Rad Path Case of the Month:
 AMSER Rad Path Case of the Month: 62 year old male presents with right-sided facial mass Daniel Morgan, OMS III Lake Erie College of Osteopathic Medicine Dr. Matthew Hartman, M.D. Medical Student Coordinator;
AMSER Rad Path Case of the Month: 62 year old male presents with right-sided facial mass Daniel Morgan, OMS III Lake Erie College of Osteopathic Medicine Dr. Matthew Hartman, M.D. Medical Student Coordinator;
Carcinoma ex Pleomorphic Adenoma on Right Parotid Gland: A Case Report. School of Dentistry, Kyungpook National University
 Korean Journal of Oral and Maxillofacial Pathology 2017;41(4):189-194 ISSN:1225-1577(Print); 2384-0900(Online) Available online at http://journal.kaomp.org https://doi.org/10.17779/kaomp.2017.41.4.006
Korean Journal of Oral and Maxillofacial Pathology 2017;41(4):189-194 ISSN:1225-1577(Print); 2384-0900(Online) Available online at http://journal.kaomp.org https://doi.org/10.17779/kaomp.2017.41.4.006
Management of Salivary Gland Malignancies. No Disclosures or Conflicts of Interest. Anatomy 10/4/2013
 Management of Salivary Gland Malignancies Daniel G. Deschler, MD Director: Division of Head and Neck Surgery Massachusetts Eye & Ear Infirmary Massachusetts General Hospital Professor Harvard Medical School
Management of Salivary Gland Malignancies Daniel G. Deschler, MD Director: Division of Head and Neck Surgery Massachusetts Eye & Ear Infirmary Massachusetts General Hospital Professor Harvard Medical School
Follow-up of parotid pleomorphic adenomas treated by extracapsular dissection
 ORIGINAL ARTICLE Follow-up of parotid pleomorphic adenomas treated by extracapsular dissection Heinrich Iro, MD, PhD*, Johannes Zenk, MD, PhD, Michael Koch, MD, PhD, Nils Klintworth, MD Department of Otorhinolaryngology,
ORIGINAL ARTICLE Follow-up of parotid pleomorphic adenomas treated by extracapsular dissection Heinrich Iro, MD, PhD*, Johannes Zenk, MD, PhD, Michael Koch, MD, PhD, Nils Klintworth, MD Department of Otorhinolaryngology,
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Pleomorphic adenoma of submandibular gland: not so common occurrence
 International Surgery Journal Gajbhiye AS et al. Int Surg J. 2018 Feb;5(2):657-661 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20180371
International Surgery Journal Gajbhiye AS et al. Int Surg J. 2018 Feb;5(2):657-661 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20180371
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
Case Report: Chondroid Syringoma of the Cheek
 Cronicon OPEN ACCESS Dina Amin 1 *, Abdullah Al-Gorashi 2 and Rahaf Y Al-Habbab 2 1 Assistant Consultant Al-Noor Specialist Hospital, Saudi Arabia, Clinical fellow University of Alabama, USA 2 Department
Cronicon OPEN ACCESS Dina Amin 1 *, Abdullah Al-Gorashi 2 and Rahaf Y Al-Habbab 2 1 Assistant Consultant Al-Noor Specialist Hospital, Saudi Arabia, Clinical fellow University of Alabama, USA 2 Department
Outcome of Surgery in different Parotid Neoplasms
 Bangladesh J Otorhinolaryngol 2014; 20(2): 80-86 Original Article Outcome of Surgery in different Parotid Neoplasms Kazi Shameemus Salam 1, Belayat Hossain Siddiquee 2, Md. Mosleh Uddin 3, Syed Farhan
Bangladesh J Otorhinolaryngol 2014; 20(2): 80-86 Original Article Outcome of Surgery in different Parotid Neoplasms Kazi Shameemus Salam 1, Belayat Hossain Siddiquee 2, Md. Mosleh Uddin 3, Syed Farhan
Anatomical Landmarks to Avoid Injury to the Great Auricular Nerve During Rhytidectomy
 Facial Surgery Anatomical Landmarks to Avoid Injury to the Great Auricular Nerve During Rhytidectomy Todd Lefkowitz, MD; Ron Hazani, MD; Saeed Chowdhry, MD; Josh Elston, BS; Michael J. Yaremchuk, MD; and
Facial Surgery Anatomical Landmarks to Avoid Injury to the Great Auricular Nerve During Rhytidectomy Todd Lefkowitz, MD; Ron Hazani, MD; Saeed Chowdhry, MD; Josh Elston, BS; Michael J. Yaremchuk, MD; and
Original Article. Clinical Outcome of Parotidectomy with Reconstruction: Experience of a Regional Head and Neck Cancer Unit
 NJS_24_15R2 [Downloaded free from http://www.nigerianjsurg.com on Tuesday, April 05, 2016, IP: 41.132.79.253] Original Article Clinical Outcome of Parotidectomy with Reconstruction: Experience of a Regional
NJS_24_15R2 [Downloaded free from http://www.nigerianjsurg.com on Tuesday, April 05, 2016, IP: 41.132.79.253] Original Article Clinical Outcome of Parotidectomy with Reconstruction: Experience of a Regional
B I O L I F E R E S E A R C H A R T I C L E
 AN INTERNATIONAL QUARTERLY JOURNAL OF BIOLOGY & LIFE SCIENCES 5(2):170-177 B I O L I F E R E S E A R C H A R T I C L E Partial superficial parotidectomy versus conventional superficial parotidectomy for
AN INTERNATIONAL QUARTERLY JOURNAL OF BIOLOGY & LIFE SCIENCES 5(2):170-177 B I O L I F E R E S E A R C H A R T I C L E Partial superficial parotidectomy versus conventional superficial parotidectomy for
Parotid Swellings: Report of 110 Consecutive Cases
 Parotid Swellings: Report of 110 Consecutive Cases A R Arshad, FRCS, Department of Plastic Surgery, Hospital Kuala Lumpur, Jalan Pahang, 50586 Kuala Lumpur Parotid swellings are uncommon. They usually
Parotid Swellings: Report of 110 Consecutive Cases A R Arshad, FRCS, Department of Plastic Surgery, Hospital Kuala Lumpur, Jalan Pahang, 50586 Kuala Lumpur Parotid swellings are uncommon. They usually
Facelift incision and superficial musculoaponeurotic system advancement in parotidectomy: case reports
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:40 DOI 10.1186/s40902-015-0040-2 CASE REPORT Facelift incision and superficial musculoaponeurotic system advancement in parotidectomy:
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:40 DOI 10.1186/s40902-015-0040-2 CASE REPORT Facelift incision and superficial musculoaponeurotic system advancement in parotidectomy:
Potential Use of Transferred Lymph Nodes as Metastasis Detectors after Tumor Excision
 Potential Use of Transferred Lymph Nodes as Metastasis Detectors after Tumor Excision Fabio Nicoli 1,2,3, Pedro Ciudad 1, Seong Yoon Lim 1, Davide Lazzeri 3, Christopher D Ambrosia 1, Kidakorn Kiranantawat
Potential Use of Transferred Lymph Nodes as Metastasis Detectors after Tumor Excision Fabio Nicoli 1,2,3, Pedro Ciudad 1, Seong Yoon Lim 1, Davide Lazzeri 3, Christopher D Ambrosia 1, Kidakorn Kiranantawat
Extracapsular dissection versus superficial parotidectomy in benign parotid gland tumors: The Vienna Medical School experience
 ORIGINAL ARTICLE Extracapsular dissection versus superficial parotidectomy in benign parotid gland tumors: The Vienna Medical School experience Lorenz Kadletz, MD, 1 Stefan Grasl, MD, 1 Matth aus C. Grasl,
ORIGINAL ARTICLE Extracapsular dissection versus superficial parotidectomy in benign parotid gland tumors: The Vienna Medical School experience Lorenz Kadletz, MD, 1 Stefan Grasl, MD, 1 Matth aus C. Grasl,
Total versus superficial parotidectomy for stage III melanoma
 DOI: 10.1002/hed.24810 ORIGINAL ARTICLE Total versus superficial parotidectomy for stage III melanoma Aileen P. Wertz, MD 1 Alison B. Durham, MD 2 Kelly M. Malloy, MD 1 Timothy M. Johnson, MD 2 Carol R.
DOI: 10.1002/hed.24810 ORIGINAL ARTICLE Total versus superficial parotidectomy for stage III melanoma Aileen P. Wertz, MD 1 Alison B. Durham, MD 2 Kelly M. Malloy, MD 1 Timothy M. Johnson, MD 2 Carol R.
Dr. James B. Lowe Plastic Surgery ORAL SOFT TISSUE SURGERY INFORMATION SHEET AND INFORMED CONSENT
 Dr. James B. Lowe Plastic Surgery ORAL SOFT TISSUE SURGERY INFORMATION SHEET AND INFORMED CONSENT Instructions This is an informed consent document that has been prepared to assist your plastic surgeon
Dr. James B. Lowe Plastic Surgery ORAL SOFT TISSUE SURGERY INFORMATION SHEET AND INFORMED CONSENT Instructions This is an informed consent document that has been prepared to assist your plastic surgeon
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Recurrent Pleomorphic Adenoma of the Parotid Gland: Treatment Outcomes and Risks of Ulterior Recurrence
 Recurrent Pleomorphic Adenoma of the Parotid Gland: Treatment Outcomes and Risks of Ulterior Recurrence Mahendra Maharjan 1, Pranay R. Sakya 2, Zhang Fuyin 3 1,2 Assistant professor, 3 Professor & Head
Recurrent Pleomorphic Adenoma of the Parotid Gland: Treatment Outcomes and Risks of Ulterior Recurrence Mahendra Maharjan 1, Pranay R. Sakya 2, Zhang Fuyin 3 1,2 Assistant professor, 3 Professor & Head
Merkel Cell Carcinoma Case # 2
 DISCHARGE SUMMARY Admitted: 10/11/2010 Discharged: 10/13/2010 Merkel Cell Carcinoma Case # 2 Chief Compliant: A 79 year old lady status post tumor on the scalp excision and left neck likely dissection
DISCHARGE SUMMARY Admitted: 10/11/2010 Discharged: 10/13/2010 Merkel Cell Carcinoma Case # 2 Chief Compliant: A 79 year old lady status post tumor on the scalp excision and left neck likely dissection
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
Risk of Facial Paralysis Following Parotidectomy. Ayad A Hasan FICMS, Ammar Y Khudhir FICMS
 raqi JMS Published by Al-Nahrain College of Medicine SSN 1681-6579 Email: raqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ Risk of Facial Paralysis Following Parotidectomy Ayad A Hasan FCMS,
raqi JMS Published by Al-Nahrain College of Medicine SSN 1681-6579 Email: raqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ Risk of Facial Paralysis Following Parotidectomy Ayad A Hasan FCMS,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Review Article A Review of Our Experience of Surgery for Parotid Gland Neoplasms Nanjundappa 1*, Vasu Reddy Challa 2,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Review Article A Review of Our Experience of Surgery for Parotid Gland Neoplasms Nanjundappa 1*, Vasu Reddy Challa 2,
be very thin and variable. Facial nerve branches that exit the parotid gland are deep to the SMAS.
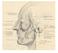 The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
Reoperative central neck surgery
 Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
Grading Facial Nerve Function Following Combined Static and Mimetic Surgical Techniques
 416 Original Article Grading Facial Nerve Function Following Combined Static and Mimetic Surgical Techniques John P. Leonetti 1 Sam J. Marzo 1 Douglas A. Anderson 2 Joshua M. Sappington 1 1 Department
416 Original Article Grading Facial Nerve Function Following Combined Static and Mimetic Surgical Techniques John P. Leonetti 1 Sam J. Marzo 1 Douglas A. Anderson 2 Joshua M. Sappington 1 1 Department
doi: /j.anl
 doi: 10.1016/j.anl.2006.07.001 Synchronous unilateral parotid gland neoplasms of three different histological types Shuho Tanaka 1, Keiji Tabuchi 1, Keiko Oikawa 1, Rika Kohanawa 1, Hideki Okubo 1, Dai
doi: 10.1016/j.anl.2006.07.001 Synchronous unilateral parotid gland neoplasms of three different histological types Shuho Tanaka 1, Keiji Tabuchi 1, Keiko Oikawa 1, Rika Kohanawa 1, Hideki Okubo 1, Dai
A CASE OF A Huge Submandibular Pleomorphic Adenoma
 ISPUB.COM The Internet Journal of Head and Neck Surgery Volume 4 Number 2 S VERMA Citation S VERMA.. The Internet Journal of Head and Neck Surgery. 2009 Volume 4 Number 2. Abstract Pleomorphic adenoma
ISPUB.COM The Internet Journal of Head and Neck Surgery Volume 4 Number 2 S VERMA Citation S VERMA.. The Internet Journal of Head and Neck Surgery. 2009 Volume 4 Number 2. Abstract Pleomorphic adenoma
ORIGINAL ARTICLE. and histological data. An additional confounding factor is infection, which oftendivertsthephysician sattention.
 ORIGINAL ARTICLE First Branchial Cleft Anomalies A Study of 39 Cases and a Review of the Literature Jean-Michel Triglia, MD; Richard Nicollas, MD; Vincent Ducroz, MD; Peter J. Koltai, MD; Erea-Noël Garabedian,
ORIGINAL ARTICLE First Branchial Cleft Anomalies A Study of 39 Cases and a Review of the Literature Jean-Michel Triglia, MD; Richard Nicollas, MD; Vincent Ducroz, MD; Peter J. Koltai, MD; Erea-Noël Garabedian,
Fine Needle Aspiration Cytology in Parotid Lumps
 Fine Needle Aspiration Cytology in Parotid Lumps Pages with reference to book, From 188 To 190 Abbas Zafar, Mohammad Shafi, Shaukat Malik ( Department of ENT, Karachi Medical and Dental College and Abbasi
Fine Needle Aspiration Cytology in Parotid Lumps Pages with reference to book, From 188 To 190 Abbas Zafar, Mohammad Shafi, Shaukat Malik ( Department of ENT, Karachi Medical and Dental College and Abbasi
ORIGINAL ARTICLE. Masses of the Salivary Gland Region in Children
 ORIGINAL ARTICLE Masses of the Salivary Gland Region in Children Brandon G. Bentz, MD; C. Anthony Hughes, MD; Jeffrey P. Lüdemann, MD; John Maddalozzo, MD Background: Noninflammatory masses of the salivary
ORIGINAL ARTICLE Masses of the Salivary Gland Region in Children Brandon G. Bentz, MD; C. Anthony Hughes, MD; Jeffrey P. Lüdemann, MD; John Maddalozzo, MD Background: Noninflammatory masses of the salivary
Face. Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face
 Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 5 Basic Surgical Procedures Key Points 2 5.1 Wound Management Many important procedures can be performed under local anesthesia and do not require a surgical specialist
Surgical Care at the District Hospital 1 5 Basic Surgical Procedures Key Points 2 5.1 Wound Management Many important procedures can be performed under local anesthesia and do not require a surgical specialist
Accepted 19 May 2008 Published online 2 September 2008 in Wiley InterScience (www.interscience.wiley.com). DOI: /hed.20912
 ORIGINAL ARTICLE OUTCOMES FOLLOWING PAROTIDECTOMY FOR METASTATIC SQUAMOUS CELL CARCINOMA WITH MICROSCOPIC RESIDUAL DISEASE: IMPLICATIONS FOR FACIAL NERVE PRESERVATION N. Gopalakrishna Iyer, MBBS (Hons),
ORIGINAL ARTICLE OUTCOMES FOLLOWING PAROTIDECTOMY FOR METASTATIC SQUAMOUS CELL CARCINOMA WITH MICROSCOPIC RESIDUAL DISEASE: IMPLICATIONS FOR FACIAL NERVE PRESERVATION N. Gopalakrishna Iyer, MBBS (Hons),
Comprehensive Management of Head and Neck Tumors. Stanley E Thawley, William R Panje, John G Batsakis, Robert D Lindberg
 Comprehensive Management of Head and Neck Tumors Stanley E Thawley, William R Panje, John G Batsakis, Robert D Lindberg Chapter 46: Controversies Regarding Therapy of Tumors of the Salivary Glands John
Comprehensive Management of Head and Neck Tumors Stanley E Thawley, William R Panje, John G Batsakis, Robert D Lindberg Chapter 46: Controversies Regarding Therapy of Tumors of the Salivary Glands John
SCOPE OF PRACTICE PGY-6 PGY-7 PGY-8
 PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
Both the major and minor glands have ducts, which are the channels down which the saliva travels on its way to the mouth.
 What and where are salivary glands? make the saliva in your mouth, which is very important for the health of your mouth and teeth (eg it stops your mouth drying out) - and also for the first stages of
What and where are salivary glands? make the saliva in your mouth, which is very important for the health of your mouth and teeth (eg it stops your mouth drying out) - and also for the first stages of
ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 )
 2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
Recurrent thyroglossal duct cysts: a 15-year review of presentation, management and outcomes from a tertiary paediatric institution
 Research Article Page 1 of 6 Recurrent thyroglossal duct cysts: a 15-year review of presentation, management and outcomes from a tertiary paediatric institution Luke M. O Neil 1,2, Alan T. Cheng 1,2,3
Research Article Page 1 of 6 Recurrent thyroglossal duct cysts: a 15-year review of presentation, management and outcomes from a tertiary paediatric institution Luke M. O Neil 1,2, Alan T. Cheng 1,2,3
Case Report Decompression of the inferior alveolar nerve to treat the pain of the mandible caused by fibrous dysplasia-case report
 Int J Clin Exp Med 2015;8(10):19535-19539 www.ijcem.com /ISSN:1940-5901/IJCEM0014642 Case Report Decompression of the inferior alveolar nerve to treat the pain of the mandible caused by fibrous dysplasia-case
Int J Clin Exp Med 2015;8(10):19535-19539 www.ijcem.com /ISSN:1940-5901/IJCEM0014642 Case Report Decompression of the inferior alveolar nerve to treat the pain of the mandible caused by fibrous dysplasia-case
SAJS Trauma General/ENT Surgery
 SAJS Trauma General/ENT Surgery Parotidectomy in Cape Town a review of pathology and management ANTON C. VAN LIEROP, M.B. CH.B., F.C.O.R.L. (S.A.) JOHANNES J. FAGAN, M.B.CH.B., F.C.S. (S.A.), M.MED. (OTOL.)
SAJS Trauma General/ENT Surgery Parotidectomy in Cape Town a review of pathology and management ANTON C. VAN LIEROP, M.B. CH.B., F.C.O.R.L. (S.A.) JOHANNES J. FAGAN, M.B.CH.B., F.C.S. (S.A.), M.MED. (OTOL.)
Fluorescein sodium-guided surgery of parotid gland tumors as a technical advance
 DOI 10.1186/s12901-017-0039-7 TECHNICAL ADVANCE Open Access Fluorescein sodium-guided surgery of parotid gland tumors as a technical advance Frank Haubner 1*, Holger G. Gassner 1, Alexander Brawanski 2
DOI 10.1186/s12901-017-0039-7 TECHNICAL ADVANCE Open Access Fluorescein sodium-guided surgery of parotid gland tumors as a technical advance Frank Haubner 1*, Holger G. Gassner 1, Alexander Brawanski 2
3-Deep fascia: is absent (except over the parotid gland & buccopharngeal fascia covering the buccinator muscle)
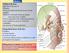 The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
Case Report Joint Use of Skull Base Surgery in a Case of Pediatric Parotid Gland Carcinoma
 Case Reports in Otolaryngology, Article ID 158451, 4 pages http://dx.doi.org/10.1155/2014/158451 Case Report Joint Use of Skull Base Surgery in a Case of Pediatric Parotid Gland Carcinoma Yuri Ueda, 1
Case Reports in Otolaryngology, Article ID 158451, 4 pages http://dx.doi.org/10.1155/2014/158451 Case Report Joint Use of Skull Base Surgery in a Case of Pediatric Parotid Gland Carcinoma Yuri Ueda, 1
Reasons for conversion during VATS lobectomy: what happens with increased experience
 Review Article on Thoracic Surgery Page 1 of 5 Reasons for conversion during VATS lobectomy: what happens with increased experience Dario Amore, Davide Di Natale, Roberto Scaramuzzi, Carlo Curcio Division
Review Article on Thoracic Surgery Page 1 of 5 Reasons for conversion during VATS lobectomy: what happens with increased experience Dario Amore, Davide Di Natale, Roberto Scaramuzzi, Carlo Curcio Division
Salivary Glands. The glands are found in and around your mouth and throat. We call the major
 Salivary Glands Where Are Your Salivary Glands? The glands are found in and around your mouth and throat. We call the major salivary glands the parotid, submandibular, and sublingual glands. They all secrete
Salivary Glands Where Are Your Salivary Glands? The glands are found in and around your mouth and throat. We call the major salivary glands the parotid, submandibular, and sublingual glands. They all secrete
A Clinical Study on Salivary Gland Swellings.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. VIII (July. 2017), PP 53-57 www.iosrjournals.org A Clinical Study on Salivary Gland
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. VIII (July. 2017), PP 53-57 www.iosrjournals.org A Clinical Study on Salivary Gland
Temple and Postauricular Dissection in Face and Neck Lift Surgery
 Temple and Postauricular Dissection in Face and Neck Lift Surgery Topic Joo Heon Lee 1, Tae Suk Oh 2, Sung Wan Park 3, Jae Hoon Kim 3, Tanvaa Tansatit 4 1 Area88 Plastic Surgery Clinic, Seoul; 2 Department
Temple and Postauricular Dissection in Face and Neck Lift Surgery Topic Joo Heon Lee 1, Tae Suk Oh 2, Sung Wan Park 3, Jae Hoon Kim 3, Tanvaa Tansatit 4 1 Area88 Plastic Surgery Clinic, Seoul; 2 Department
Facelift approach for mandibular resection and reconstruction
 ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
Sentinel lymph node biopsy for early oral cancer
 Sentinel lymph node biopsy for early oral cancer Information for patients from the Oral and Maxillofacial Department When cancer cells start to spread from the main cancer this represents an important
Sentinel lymph node biopsy for early oral cancer Information for patients from the Oral and Maxillofacial Department When cancer cells start to spread from the main cancer this represents an important
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD
 STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
ORIGINAL ARTICLE. Fine-Needle Aspiration Biopsy of Salivary Gland Lesions in a Selected Patient Population
 ORIGINAL ARTICLE Fine-Needle Aspiration Biopsy of Salivary Gland Lesions in a Selected Patient Population Erik G. Cohen, MD; Snehal G. Patel, MD; Oscar Lin, MD; Jay O. Boyle, MD; Dennis H. Kraus, MD; Bhuvanesh
ORIGINAL ARTICLE Fine-Needle Aspiration Biopsy of Salivary Gland Lesions in a Selected Patient Population Erik G. Cohen, MD; Snehal G. Patel, MD; Oscar Lin, MD; Jay O. Boyle, MD; Dennis H. Kraus, MD; Bhuvanesh
Departmental Segregated Total Form for Plastic and Reconstructive Surgery
 Departmental Segregated Total Form for Plastic and Reconstructive Surgery American Osteopathic Association and the American College of Osteopathic Surgeons Revised, COPT 11/2001 Revised, BOT 2/2006, Effective,
Departmental Segregated Total Form for Plastic and Reconstructive Surgery American Osteopathic Association and the American College of Osteopathic Surgeons Revised, COPT 11/2001 Revised, BOT 2/2006, Effective,
Surgical Correction of Crow s Feet Deformity With Radiofrequency Current
 INTERNATIONAL CONTRIBUTION Oculoplastic Surgery Surgical Correction of Crow s Feet Deformity With Radiofrequency Current Min-Hee Ryu, MD; David Kahng, MD; and Yongho Shin, MD, PhD Aesthetic Surgery Journal
INTERNATIONAL CONTRIBUTION Oculoplastic Surgery Surgical Correction of Crow s Feet Deformity With Radiofrequency Current Min-Hee Ryu, MD; David Kahng, MD; and Yongho Shin, MD, PhD Aesthetic Surgery Journal
Learning Outcomes. The Carotid 20/02/2013. Scalp, Face, Parotid. Layers of the Scalp. The Parotid Gland. The Scalp. The Carotid The Facial Artery
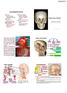 Learning Outcomes The Scalp Layers of the Scalp Bleeding from the Scalp The Carotid The Facial Artery Major Muscles of the Face and Jaw(s) Muscles of Mastication Muscles of Facial Expression The Parotid
Learning Outcomes The Scalp Layers of the Scalp Bleeding from the Scalp The Carotid The Facial Artery Major Muscles of the Face and Jaw(s) Muscles of Mastication Muscles of Facial Expression The Parotid
Salivary ultrasound. Dr T J Beale Royal National Throat Nose & Ear and UCLH Hospitals London UK
 Salivary ultrasound Dr T J Beale Royal National Throat Nose & Ear and UCLH Hospitals London UK Two main groups of patients with presenting symptoms of: Obstructive or chronic inflammatory symptoms (salivary
Salivary ultrasound Dr T J Beale Royal National Throat Nose & Ear and UCLH Hospitals London UK Two main groups of patients with presenting symptoms of: Obstructive or chronic inflammatory symptoms (salivary
Outcome, General, and Symptom-Specific Quality of Life After Various Types of Parotid Resection
 The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. Outcome, General, and Symptom-Specific Quality of Life After Various Types of Parotid Resection Raphael Richard
The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. Outcome, General, and Symptom-Specific Quality of Life After Various Types of Parotid Resection Raphael Richard
Facial Nerve Monitoring During Parotidectomy: A Two-Center Retrospective Study
 Original Article Iranian Journal of Otorhinolaryngology, Vol.28(4), Serial No.87, Jul 2016 Facial Nerve Monitoring During Parotidectomy: A Two-Center Retrospective Study * Stanislas Ballivet de Régloix
Original Article Iranian Journal of Otorhinolaryngology, Vol.28(4), Serial No.87, Jul 2016 Facial Nerve Monitoring During Parotidectomy: A Two-Center Retrospective Study * Stanislas Ballivet de Régloix
Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor
 Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Cancer of the Oral Cavity
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Continuing Education Independent Study Series
 Continuing Education Independent Study Series Association of Surgical Technologists Publication made possible by an educational grant provided by Kimberly-Clark Corporation OF SURGICAL ECHNOLOGISTS AEGER
Continuing Education Independent Study Series Association of Surgical Technologists Publication made possible by an educational grant provided by Kimberly-Clark Corporation OF SURGICAL ECHNOLOGISTS AEGER
SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY
 MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note
 Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
An Algorithm to Guide Recipient Vessel Selection in Cases of Free Functional Muscle Transfer for Facial Reanimation
 An Algorithm to Guide Recipient Vessel Selection in Cases of Free Functional Muscle Transfer for Facial Reanimation Original Article Francis P Henry, Jonathan I Leckenby, Daniel P Butler, Adriaan O Grobbelaar
An Algorithm to Guide Recipient Vessel Selection in Cases of Free Functional Muscle Transfer for Facial Reanimation Original Article Francis P Henry, Jonathan I Leckenby, Daniel P Butler, Adriaan O Grobbelaar
SURGICAL TECHNIQUE. Radical treatment for left upper-lobe cancer via complete VATS. Jun Liu, Fei Cui, Shu-Ben Li. Introduction
 SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW
 MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Original Article Analysis of neurologic complications after modified temporomandibular joint disc anchorage surgery
 Int J Clin Exp Med 2017;10(3):5440-5444 www.ijcem.com /ISSN:1940-5901/IJCEM0041511 Original Article Analysis of neurologic complications after modified temporomandibular joint disc anchorage surgery Jin-Ze
Int J Clin Exp Med 2017;10(3):5440-5444 www.ijcem.com /ISSN:1940-5901/IJCEM0041511 Original Article Analysis of neurologic complications after modified temporomandibular joint disc anchorage surgery Jin-Ze
Chapter 11 Worksheet Code It
 Class: Date: Chapter 11 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. Surgical destruction is considered part of the surgical procedure description. 2. Prepping
Class: Date: Chapter 11 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. Surgical destruction is considered part of the surgical procedure description. 2. Prepping
Risk factors for postoperative haemorrhage after total thyroidectomy: clinical results based on 2,678 patients
 www.nature.com/scientificreports OPEN Received: 2 February 2017 Accepted: 28 June 2017 Published online: 1 August 2017 Risk factors for postoperative haemorrhage after total thyroidectomy: clinical results
www.nature.com/scientificreports OPEN Received: 2 February 2017 Accepted: 28 June 2017 Published online: 1 August 2017 Risk factors for postoperative haemorrhage after total thyroidectomy: clinical results
