A case study report : occupational therapy for an older adult with shoulder impingement syndrome
|
|
|
- Sherman Caldwell
- 6 years ago
- Views:
Transcription
1 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects A case study report : occupational therapy for an older adult with shoulder impingement syndrome Lindsey M. Brown The University of Toledo Follow this and additional works at: This Capstone Project is brought to you for free and open access by The University of Toledo Digital Repository. It has been accepted for inclusion in Master s and Doctoral Projects by an authorized administrator of The University of Toledo Digital Repository. For more information, please see the repository's About page.
2 A Case Study Report: Occupational Therapy for an Older Adult with Shoulder Impingement Syndrome Lindsey M. Brown, B.S. Faculty Mentor: Martin Rice, Ph.D., OTR/L Site Mentor: Krista Monroe, OTR/L, CHT Department of Occupational Therapy Occupational Therapy Doctorate Program The University of Toledo Health Science Campus May 2008 Note: This document describes a Capstone Dissemination project reflecting an individually planned experience conducted under faculty and site mentorship. The goal of the Capstone Experience is to provide occupational therapy doctoral students with unique experiences whereby they can demonstrate leadership and autonomous decisionmaking in preparation for enhanced future practice as occupational therapists. As such, the Capstone Dissemination is not formal research.
3 2 Abstract Shoulder impingement syndrome can be very painful and debilitating for persons with this diagnosis. This case study report describes occupational therapy services implemented for a patient diagnosed with shoulder impingement from an injury that occurred more than 30 years prior. The patient demonstrated decreased range of motion and increased pain especially with overhead reaching occupations. The patient described in this case study was a retired surgical nurse who had no previous experience with occupational therapy. During evaluation and initial treatments, the patient was quite skeptical about the benefits of receiving occupational therapy services. As therapy progressed, the patient verbalized the benefits and improvements she had seen from occupational therapy. At discharge, the patient met her pain and instrumental occupations of daily living goals. Treatment approaches were based upon the biomechanical model of practice as well as the Canadian model of occupational performance. Since the Canadian model of occupational performance is client-centered, this model of practice was important to the treatment of this patient due to her expressed goals and concerns.
4 3 Introduction Background Information In December 2007, a 65-year-old female presented to Dr. Davis with a several month history of left shoulder pain. She dated this injury back to almost 30 years ago when she was tubing with her children and hit her shoulder on a chunk of ice. She complained of pain with overhead activities and pain while at rest. X-rays were completed in December 2007 which suggested osteoarthritis (OA) of the acromioclavicular (AC) joint. On this same date, an MRI was ordered to be done in January, The MRI found glenohumeral loose bodies, OA of the AC joint, medial and lateral impingement, as well as interstitial tearing of the rotator cuff. According to Burkart and Post (2002) impingement is the encroachment of the acromion, coracoarcromial ligament, coracoid process, and acromioclavicular joint on the subacromial tissues that pass beneath them as the greater tuberosity passes below during flexion and abduction (p. 1376). At this time, Dr. Davis referred the patient onto Dr. Patel for his recommendations and treatment. During Dr. Patel s examination, the patient was found to be positive for Hawkins sign and had pain at the extremes of internal rotation. The Hawkins sign causes pain when patients have impingement syndrome (Pappas et al., 2006). She did not feel overly disabled and was not ready for surgical intervention. Dr. Patel recommended that she try conservative treatment for six weeks consisting of anti-inflammatory medication and physical/occupational therapy protocol for impingement syndrome. If the six weeks of conservative treatment failed, Dr. Patel offered her a subarcomial corticosteroid injection at her follow-up appointment or athroscopic intervention.
5 4 Model of Practice Trombly s (1995) biomechanical model of practice is used to treat persons who have limited range of motion, decreased strength, decreased endurance, edema, and structural instability. Many evaluation and treatment techniques are utilized with the biomechanical models of practice. Some common assessments include manual muscle testing and range of motion measurements. Treatments can consist of stretching, strengthening, and endurance occupations (Seidel, 2003). The Canadian model of occupational performance focuses on client-centered practice and occupational performance (Department of National Health and Welfare and Canadian Association of Occupational Therapists, 1983). According to Law, Baptiste, and Mills (1995), client-centered practice is an approach that embraces philosophy of respect and partnership with those receiving occupational therapy services. A common assessment used with this model of practice is the Canadian Occupational Performance Measure (Law et al., 1990). This assessment addresses the following areas: self-care, productivity, and leisure. Scientific Evidence for MOP Treatments using the biomechanical model often include rote exercise; therefore many studies have been conducted about purposeful activity versus rote exercise. Many of these studies have found that participation improves with purposeful occupations rather than rote exercise (Riccio, Nelson, & Bush, 1990; Kircher, 1984). The use of physical agents is also commonly done when using the biomechanical model (Kielhofner, 2004). The use of physical agent modalities is supported by the American Occupational
6 5 Therapy Association if modalities are used as an adjunctive method in conjunction with or in preparation for engagement in occupations (American Occupational Therapy Association, 2003). In the Guidelines for Client-Centered Practice of Occupational Therapy (Department of National Health and Welfare and Canadian Association of Occupational Therapists, 1983): The role of the occupational therapist is to facilitate the individual s engagement with his environment. An essential component of the therapeutic relationship is the therapist/client interaction and the exchange which occurs throughout the learning situation created by the occupational therapist. (p. 10) Also, Principle 3 of the Occupational Therapy Code of Ethics states, Occupational therapy personnel shall collaborate with recipients, and if they desire, families, significant others, and/or caregivers in setting goals and priorities throughout the intervention process (American Occupational Therapy Association, 2005, p. 640). Rationale for MOP with this Case The patient described in this case study demonstrated decreased range of motion, decreased strength, and pain in her shoulder therefore warranting use of the biomechanical model. She is also retired and expressed to the occupational therapy student that she wanted to function in daily life without pain and have normal movement patterns. Since these were goals she wanted to achieve by participating in occupational therapy, it warranted the use of the Canadian model of occupational performance because this model has a client-centered component.
7 6 Innovativeness/Creativity The patient s injury occurred more than 30 years ago and following this injury she was able to continue working as an emergency room nurse without problems. It was not until she retired that she began to notice pain in her shoulder and noticed using compensatory movements. This patient was employed in the medical field for numerous years but during the initial evaluation she expressed skepticism about the benefits and role of occupational therapy. Therefore, it was important for the occupational therapy student to be creative with treatments so the patient recognized the usefulness and benefits of occupational therapy. Evaluation The patient was referred to occupational therapy on January 22, 2008 and was evaluated on January 28, The initial occupational therapy evaluation consisted of observation, interview, and standardized testing. Upon entering the outpatient clinic, the patient had slouched posture with slight scapular abduction bilaterally. The only significant diagnosis in her past medical history was hypertension. She is a retired surgical nurse and is right handed. She reported 5/10 pain while completing tasks using her left arm. She reported difficulty with washing across her body and fastening her bra. Both of these occupations required minimal assistance. The patient also stated she had difficulty completing overhead tasks (e.g., removing items from cupboards, hanging laundry, lifting grandchildren) because increased time, minimal to moderate assistance, and/or technique changes were needed. Passive range of motion and active range of measurements were taken bilaterally. Passively she was within normal limits with flexion, abduction, extension, and external
8 7 rotation bilaterally (American Academy of Orthopaedic Surgeons, 1965). Her left shoulder passive internal rotation measurement was 58. In her left shoulder she actively demonstrated 140 of flexion, 120 of abduction, and she could only reach her waistband behind her back. Manual muscle testing was also completed bilaterally (Beasely, 1961). She demonstrated 5/5 for flexion, and 4+/5 for internal and external rotation in her left upper extremity. The patient also tested positive for Hawkins provocative test which indicated impingement syndrome in left shoulder. Goal Setting Goals Identified by the Patient 1. Long Term Goals a. Have less pain b. Do overhead tasks with decreased time and change of technique c. Complete gardening independently. At time of evaluation, the patient required minimal to moderate assistance secondary to the lifting, pushing, and pulling. 2. Short Term Goals a. Be able to thoroughly wash across body independently after 3 weeks b. Be able to fasten bra independently after 3 weeks Occupational Therapy Goals The patient was to attend occupational therapy two times a week for six weeks and during this time the following goals were addressed by occupational therapy.
9 8 Home Exercise Program 1. Justification- Since the patient was only attending therapy two times a week, it was important for her to complete exercises at home for future attainment of goals of decreased pain and improved ability to complete activities of daily living. 2. Goals a. LTG- The patient will be independent with updates and final home exercise program. b. STG- The patient will be independent with home exercise program and will report doing exercises at least two times a day. Pain 1. Justification- The patient expressed decreased ability to complete tasks secondary to intense pain. 2. Goals a. LTG- The patient will report pain 1/10 pain while completing overhead tasks (e.g., retrieving items from kitchen cupboards) that are 1.5 above shoulder height. b. STG- The patient will identify two strategies to reduce pain. c. STG- After six visits, the patient will report pain less then or equal to 2/10 while at rest.
10 9 Range of Motion 1. Justification- The patient reported minimal assistance to fasten bra behind her back and to wash across body. She also needed minimal to moderate assistance to retrieve objects out of cupboards that she was once able to reach. 2. Goals a. LTG- Pt will demonstrate within functional limit active range of motion in left shoulder flexion, internal and external rotation, and abduction so patient can complete leisure tasks (e.g., gardening, playing with grandchildren) independently. b. STG- Pt will increase left shoulder active range of motion (flexion, abduction, extension, internal rotation) by 10 each for improved ability to wash across body and fasten bra. Interventions During occupational therapy sessions, the patient s left shoulder was passively ranged by the occupational therapy student in all planes. Also, the patient completed self-stretches focusing on internal/external rotation as well as flexion. The previous occupations mentioned were completed to improve the patient s active range of motion. While in the outpatient clinic, the patient was educated on the importance of good posture (e.g., shoulders back and back straight) as well as proper body mechanics when completing occupations. Since the patient expressed she had increased pain, difficulty, and using compensatory movements when completing overhead tasks, the occupational therapy student had the patient complete several overhead occupations during therapy sessions.
11 10 While standing, the patient retrieved items such as cups, plates, and a coffee canister from a 6 shelf and then returned the items. The patient was approximately 5 5 inches tall so she had to reach approximately 1.5 feet above shoulder height. This occupation simulated the patient retrieving items from her cupboards at home. The patient also completed a hanging laundry occupation which is further discussed in the occupational analysis section. Other occupations completed during therapy sessions were simulating fastening a bra, using a hand towel to wash across her body, and strengthening with thera-band. Following each therapy session, the patient was instructed to practice completing the occupations done in the outpatient clinic. For example, at home the patient practiced retrieving items with a variety of weight from cupboards at varying heights. Also, the patient was instructed to use left arm to pull up pants in the back and/or thread belt because this required the same motion as fastening a bra. The patient was also given handouts with all self-stretches as well as strengthening exercises to be completed at home. Occupational Analysis of One Occupational Treatment Session Occupational Form For the occupation of hanging towels, the important occupational forms included green bungee cord approximately 7 feet high which was attached to the wall on one end and occupational therapy student holding up other end, colored clothes pins, 4 hand towels in the hand of occupational therapy student. The simulated clothesline was in the outpatient clinic at the Institute for Orthopaedic Surgery. The occupational therapy student provided encouragement to the patient during the occupation.
12 11 Occupational Performance Prior to the start of the occupation, the patient stated this would be good experience because since attending therapy she had not tried hanging clothes up on her clothesline in her basement. She started the occupation by taking two clothespins into her hand from the occupational therapy student. She then took a white hand towel from the student. She used her left hand to hold one corner of the towel against the line while she used her right hand to clip the clothespin on the corner of the towel. She then released her grasp on the towel and the clothespin. The patient then grasped another corner of the towel with her left hand and brought it up to the clothesline. After this had been completed, she used her right hand to clip another clothespin onto the towel and then released her grasp. After one towel had been hung, the occupational therapy student asked if she was experiencing any pain. The patient stated she was not and would like to try to hang another towel. She retrieved another towel from the arm of the occupational therapy student and two more clothespins. She hung her second towel next to the first towel already hanging on the line. She used the same procedure as described before: holding towel with left hand against clothesline and clipping clothespin with right hand. She continued to hang up a total of four towels. The occupational therapy student asked the client if the task was difficult and what she would do different next time. The patient stated she was surprised with her ability to complete the occupation and next time she would try heavier clothing items.
13 12 Meaning and Purpose Inferred The patient was highly motivated to complete the simulated hanging clothes occupation successfully. She was also motivated to complete overhead tasks without pain and without compensatory shoulder movements so she could achieve her long term goal of successfully completing overhead tasks without pain and with natural shoulder movements. During one therapy session the patient stated, I never really saw a purpose for therapy until it happened to me. Impacts The patient had an impact on the clothesline as she hung towels with clothespins on it. She also had an impact on the towels and clothespins as she removed them from the occupational therapy students hand and put them on the clothesline. Assessment During the occupation, the patient demonstrated normal movement patterns when reaching to hang the towels on the line. A typical movement pattern would consist of shoulder flexion and slight abduction. During prior sessions, the patient would use compensatory movements by abducting, externally rotating, and flexing her shoulder to reach overhead. The patient also did not report an increase or decrease in pain during this occupation. The occupational therapy student recommended that next time the patient should use more items and/or heavier items. Adaptations Adaptations included increase range of motion at her shoulder, decreased pain when moving her shoulder, and increase awareness of the value of participating in an occupational therapy treatment regime. Adaptations occurred by virtue of the fact that
14 13 the patient learned that she was able to hang up items on a clothesline without an increase of pain and time. She was also able to perform the occupation using typical movement patterns. Re-synthesis For a follow-up occupation, the occupational therapy student planned on having the patient hang heavier items on the line such as shirts and/or pants; as well as, have the patient hang up more items. This occupation would require the patient to complete an overhead occupation and compare pain and technique found when hanging lighter and fewer items. Outcomes Goals Achieved 1. Home Exercise Program- The long term and short term goals were met. At every therapy session the patient reported completing her home exercises daily. Three weeks after being discharged, the patient was contacted by the occupational therapy student. At this time, she reported continuing to do her exercises typically once a day. 2. Pain- The long term and short term goals were met. She reported 0/10 pain while at rest and 1/10 while completing overhead tasks. 3. Range of Motion- All goals were met. The patient demonstrated within functional limits active range of motion in all planes. At discharge, the patient s active range of motion measurements were as follows: flexion 167, abduction 171, and she could internally rotate to 2 inches above waistband.
15 14 She reported being able to wash across her body as well as fasten her bra independently. Changes on Standardized Assessments The patient attended 11 out of 12 sessions of occupational therapy. At discharge, her active range of motion measurements were within functional limits. Her pain had significantly decreased while at rest and when using left arm. Manual muscle testing scores were the same at evaluation and discharge. Lastly, she tested positive for the Hawkins provocative test which indicates subscapularis impingement. Although the impingement continues to exist, the patient is functioning without pain. Inferred Meanings and Purposes The patient initially was skeptical about the role and benefits of occupational therapy. As therapy sessions progressed, the patient reported, I never really saw the purpose of therapy, until now. I am really seeing improvements in my shoulder. She recognized her improved ability to complete occupations that were very difficult and/or painful for her to complete prior to participating in occupational therapy. The patient expressed pleasure about her improved ability to complete overhead tasks without asking for help from her husband. It was very important to this patient to be independent with occupations she was once able to perform without the help of others. This patient expressed concern about being a burden to others due to her need for help with some occupations, especially overhead reaching. Patient s Report on Progress Three weeks after discharge, the patient was contacted via phone by the occupational therapy student. The patient reported hanging clothes on her clothesline in
16 15 her basement without an increase of pain or a change in technique. She also stated that she was able to retrieve items from cupboards easier. The patient stated, I was always compensating when I did things prior and would have to stop and adjust. Now after therapy I can naturally do the things I want to do. The patient also reported that she did her home exercise program daily. She said, I can tell when I need to do them (exercises). The patient was very excited about her ability to perform overhead tasks without pain as well as being able to fasten her bra. At her follow-up visit with Dr. Patel, he offered her rechecks as needed and told her to continue her care as she has been with exercises at home. The patient stated she was satisfied with this plan. Conclusions Discharge Recommendations 1. Home Exercise Program- Recommend that patient continues to do her home exercise program twice daily to maintain strength and flexibility she had gained. 2. Pain- Recommend that patient use heat/ice, good posture, and exercises to keep pain at a minimum. Recommend the patient follow-up with Dr. Patel if sudden increase of pain occurs that does not resolve. 3. Range of Motion- Recommend patient continue to do stretching as well as continue to use left upper extremity to complete activities of daily living and overhead reaching task. Outcomes Related to the Identified Models of Practice
17 16 After participating in occupational therapy, the client improved her active range of motion measurements. This goal was achieved using a variety of methods: passive range of motion and therapeutic occupations. According to Kielhofner (2004), activity may be progressively modified to intensify task demands that will increase musculosketal capacity (p. 86). The first several occupational therapy sessions focused on range of motion then were progressed to completing occupations. The occupations were graded based on the ability of the patient. Fastening a bra and washing across her body were prioritized first because the patient had moderate difficulty completing these occupations. The patient expressed maximal difficulty with overhead tasks so this became the primary focus once the previous occupations had been mastered. Overhead tasks were modified by increasing the height of the task, the weight of the items being retrieved and/or replaced, and the duration of the occupation. All of this was done to intensify the task demands. This case study was also based on the Canadian model of occupational performance therefore the patient s goals were the primary focus of every session. Each therapy session was tailored to the unique difficulties/problems identified by the patient. According to Law, Baptiste, & Mills (1995), several key concepts of client-centered practice are individualized therapy, respect for patients decisions, providing opportunity for patients to succeed, and allowing patients to participate in therapy. After participating in occupational therapy, the patient reported being able to fasten her bra, wash across her body, as well as complete overhead tasks independently. The patient reported she no longer felt she had to rely as much on her husband to help her complete overhead reaching tasks and this made her feel she was less of a burden.
18 17 Implications of the Case for Research Through this case study, it was found that conservative treatment helped to alleviate the pain and loss of range of motion experienced by a patient diagnosed with impingement syndrome. Further research needs to be conducted in this area to compare patient outcomes with conservative treatment versus surgery. Since there are a variety of factors that can contribute to impingement syndrome, treatment options and outcomes need to researched for each type of impingement. This case study was innovative because there has not been a lot of research done with this population especially in occupational therapy. It was found through this case study that occupational therapy services were successful in alleviating this patient s pain and decreased ability to complete occupations of daily living.
19 18 References American Academy of Orthopaedic Surgeons. (1965). Joint motion: Method of measuring and recording. Chicago: Author. American Occupational Therapy Association. (2003). Physical agent modalities: A position paper. American Journal of Occupational Therapy, 57, American Occupational Therapy Association. (2005). Occupational therapy code of ethics (2005). American Journal of Occupational Therapy, 59, Beasley, W.C., (1961). Quantitative muscle testing: Principles and applications to research and clinical services. Archives of Physical Medicine and Rehabilitation, 42, Burkart, S. L., & Post, W. R. (2002). A functionally based neuromechanical approach to shoulder rehabilitation. In E. J. Mackin, A. D. Callahan, T. M. Skirven, L. H. Schneider, & A. L. Osterman (Eds.), Rehabilitation of the hand and upper extremity: Vol. 2. (5th ed., pp ). St. Louis: Mosby. Department of National Health and Welfare and Canadian Association of Occupational Therapists (1983). Guidelines for the Client-Centered Practice of Occupational Therapy. Ottawa, Ontario: Minister of Supply and Services Canada, Cat. No. H39-33/1983E. Kielhofner, G. (2004). Conceptual foundations of occupational therapy (3rd ed.). Philadelphia: F. A. Davis Company. Kircher, M. A. (1984). Motivation as a factor of perceived exertion in purposeful versus non-purposeful activity. American Journal of Occupational Therapy, 38,
20 19 Law, M., Baptist, S., McColl, M.A., et al. (1990). The Canadian Occupational Performance Measure: An outcome measure for occupational therapy. Canadian Journal of Occupational Therapy, 57, Law, M., Baptiste, S., & Mills, J. (1995). Client-centered practice: What does it mean and does it make a difference? Canadian Journal of Occupational Therapy, 62, Pappas, G.P., Blemker, S. S., Beaulieu, C. F., McAdams, T. R., Whalen, S. T., & Gold, G. E. (2006). In vivo anatomy of the Neer and Hawkins sign positions for shoulder impingement. Journal of Shoulder and Elbow Surgery, 15, Riccio, C. M., Nelson, D. L., & Bush, M. A. (1990). Adding purpose to the repetitive exercise of elderly woman. American Journal of Occupational Therapy, 44, Seidel, A. C. (2003). Theories derived from rehabilitation perspectives. In E. B. Crepeau, E. S. Cohn, B. S. Boyt Schell (Eds.), Willard & Spackman s Occupational Therapy (10 ed., ). Philadelphia: Lippincott Williams & Wilkins. Trombly, C.A. (1995). Theoretical foundations for practice. In C. A. Trombly (Ed.), Occupational therapy for physical dysfunction (4th ed., pp ). Baltimore: Lippincott Williams & Wilkins.
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Nonoperative Treatment of Subacromial Impingement Rehabilitation Protocol
 Therapist Nonoperative Treatment of Subacromial Impingement Rehabilitation Protocol Subacromial impingement is a chronic inflammatory process produced as one of the Rotator Cuff Muscle the and the Subdeltoid
Therapist Nonoperative Treatment of Subacromial Impingement Rehabilitation Protocol Subacromial impingement is a chronic inflammatory process produced as one of the Rotator Cuff Muscle the and the Subdeltoid
Labral Tears. Fig 1: Intact labrum and biceps tendon
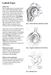 Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY
 Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) REHABILITATION AFTER REVERSE SHOULDER ARTHROPLASTY
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
MOON SHOULDER GROUP NONOPERATIVE TREATMENT OF ROTATOR CUFF TENDONOPATHY PHYSICAL THERAPY GUIDELINES
 MOON SHOULDER GROUP NONOPERATIVE TREATMENT OF ROTATOR CUFF TENDONOPATHY PHYSICAL THERAPY GUIDELINES From: Kuhn JE. Exercise in the treatment of rotator cuff impingement. A systematic review and synthesized
MOON SHOULDER GROUP NONOPERATIVE TREATMENT OF ROTATOR CUFF TENDONOPATHY PHYSICAL THERAPY GUIDELINES From: Kuhn JE. Exercise in the treatment of rotator cuff impingement. A systematic review and synthesized
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
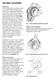 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Christopher K. Jones, MD Colorado Springs Orthopaedic Group
 Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
EVALUATION OF ACUTE SHOULDER INJURIES. Douglas J. Moran, MD Orthopaedic Sports Medicine
 EVALUATION OF ACUTE SHOULDER INJURIES Douglas J. Moran, MD Orthopaedic Sports Medicine DISCLOSURES None of the planners or presenters of this session have disclosed any conflict or commercial interest
EVALUATION OF ACUTE SHOULDER INJURIES Douglas J. Moran, MD Orthopaedic Sports Medicine DISCLOSURES None of the planners or presenters of this session have disclosed any conflict or commercial interest
INFORMATION FOR PATIENTS. Rotator cuff repair operation
 INFORMATION FOR PATIENTS Rotator cuff repair operation This booklet contains information about the shoulder surgery that you have been advised to have, and aims to answer some of the questions you may
INFORMATION FOR PATIENTS Rotator cuff repair operation This booklet contains information about the shoulder surgery that you have been advised to have, and aims to answer some of the questions you may
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection
 The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Rotator Cuff and Shoulder Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Reverse Total Shoulder Replacement
 Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Reverse Total Shoulder Replacement
 Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Looking After Your Shoulders
 A patient s guide to Looking After Your Shoulders Shoulder protection following a Spinal Cord Injury (SCI) This information, for patients with paraplegia, is a guide only and not prescriptive. Your therapist
A patient s guide to Looking After Your Shoulders Shoulder protection following a Spinal Cord Injury (SCI) This information, for patients with paraplegia, is a guide only and not prescriptive. Your therapist
Prater Chiropractic Wellness Center 903 W. South St. Kalamazoo, MI PH: (269)
 Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following a well-structured conditioning
Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following a well-structured conditioning
(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
2778 N. Webb Road Shoulder, Elbow, Wrist, Hand Wichita, KS and Arthroscopic Surgery Phone: Fax:
 Phase I: Protection Phase (Weeks 0-5) FOCUS: Passive range of motion (ROM). Minimize pain and inflammation. Maintain integrity of the repair. Regain full passive foward flexion of operated shoulder. Use
Phase I: Protection Phase (Weeks 0-5) FOCUS: Passive range of motion (ROM). Minimize pain and inflammation. Maintain integrity of the repair. Regain full passive foward flexion of operated shoulder. Use
Frozen Shoulder Syndrome Rehabilitation Using the Resistance Chair
 Frozen Shoulder Syndrome Rehabilitation Using the Resistance Chair General Information Frozen shoulder is a condition where the shoulder joint (glenohumeral joint) gradually becomes stiff, resulting in
Frozen Shoulder Syndrome Rehabilitation Using the Resistance Chair General Information Frozen shoulder is a condition where the shoulder joint (glenohumeral joint) gradually becomes stiff, resulting in
Rehabilitation Guidelines for Large Rotator Cuff Repair
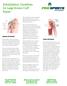 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Shoulder Home Exercise Program Champion Orthopedics
 Shoulder Home Exercise Program Champion Orthopedics Range of Motion Pendulum: Holding the side of a table with your good arm, bend over at the waist, and let your affected arm hang straight down. Swing
Shoulder Home Exercise Program Champion Orthopedics Range of Motion Pendulum: Holding the side of a table with your good arm, bend over at the waist, and let your affected arm hang straight down. Swing
Coping with Osteoarthritis in the shoulder
 Coping with Osteoarthritis in the shoulder Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or
Coping with Osteoarthritis in the shoulder Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or
Orthopedic Surgery and Sports Medicine FL License:
 Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Shoulder Labral Tear and Shoulder Dislocation
 Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
Exploring the Rotator Cuff
 Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
POST OPERATIVE ROTATOR CUFF REPAIR PROTOCOL. Home Program MOON SHOULDER GROUP
 MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
Philip Bayliss St Albans Osteopathy
 Philip Bayliss St Albans Osteopathy 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Subacromial (Shoulder) Bursitis 1 Experts estimate that 65% of people
Philip Bayliss St Albans Osteopathy 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Subacromial (Shoulder) Bursitis 1 Experts estimate that 65% of people
Shoulder Arthroscopic Capsular Release Rehabilitation
 Shoulder Arthroscopic Capsular Release Rehabilitation Phase two: 3 to 6 weeks after surgery Goals: 1. Improve range of motion of the shoulder 2. Begin gentle strengthening Activities 1. Sling Your sling
Shoulder Arthroscopic Capsular Release Rehabilitation Phase two: 3 to 6 weeks after surgery Goals: 1. Improve range of motion of the shoulder 2. Begin gentle strengthening Activities 1. Sling Your sling
REMINDER. an exercise program. Senior Fitness Obtain medical clearance and physician s release prior to beginning
 Functional Forever: Exercise for Independent Living REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns. What
Functional Forever: Exercise for Independent Living REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns. What
There are 6 movements you need to train in order to regain strength, flexibility and function in your shoulder. They are:
 Regaining Natural Shoulder Movement There are 6 movements you need to train in order to regain strength, flexibility and function in your shoulder. They are: 1. Lifting forwards (flexion) 2. Pushing arm
Regaining Natural Shoulder Movement There are 6 movements you need to train in order to regain strength, flexibility and function in your shoulder. They are: 1. Lifting forwards (flexion) 2. Pushing arm
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement
 Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement Richard Holtby Assistant professor, Department of Surgery University of Toronto
Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement Richard Holtby Assistant professor, Department of Surgery University of Toronto
OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS
 OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long 614-566-8691 Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS Shoulder Arthroscopy with Labral Repair (SLAP/Bankart/Posterior) Latarjet Procedure
OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long 614-566-8691 Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS Shoulder Arthroscopy with Labral Repair (SLAP/Bankart/Posterior) Latarjet Procedure
1. Occupation; Right or left handed, Age
 SHOULDER HISTORY 1. Occupation; Right or left handed, Age 2. Pain: Site. Any referred pain to the deltoid insertion Any localizing pain at Acromio-clavicular joint How long? Continuous or not Night pain
SHOULDER HISTORY 1. Occupation; Right or left handed, Age 2. Pain: Site. Any referred pain to the deltoid insertion Any localizing pain at Acromio-clavicular joint How long? Continuous or not Night pain
Clinical utility of the Mellville-Nelson Self- Identified Goals Assessment
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Clinical utility of the Mellville-Nelson Self- Identified Goals Assessment Ashley Obarski The University
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Clinical utility of the Mellville-Nelson Self- Identified Goals Assessment Ashley Obarski The University
HOME EXERCISE PROGRAM FOR SHOULDER CONDITIONING
 Exercise Program for: Prepared by: Seasons Family Medicine 37 South 2nd East Rexburg ID, 83440 (208) 356-9231 HOME EXERCISE PROGRAM FOR SHOULDER CONDITIONING For the exercises that use a stick, you may
Exercise Program for: Prepared by: Seasons Family Medicine 37 South 2nd East Rexburg ID, 83440 (208) 356-9231 HOME EXERCISE PROGRAM FOR SHOULDER CONDITIONING For the exercises that use a stick, you may
Rotator Cuff Repair +/- Acromioplasty/Mumford. Phase I: 0 to 2 weeks after surgery
 Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An IPRS Guide to provide you with exercises and advice to ease your condition
 Contents What causes an A/C joint sprain?..................................3 What treatment can I receive?.....................................4 YOUR GUIDE TO ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An
Contents What causes an A/C joint sprain?..................................3 What treatment can I receive?.....................................4 YOUR GUIDE TO ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An
INFORMATION FOR PATIENTS. Arthroscopic subacromial decompression
 INFORMATION FOR PATIENTS Arthroscopic subacromial decompression This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions
INFORMATION FOR PATIENTS Arthroscopic subacromial decompression This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions
Latarjet Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
Rotator Cuff and Shoulder Conditioning Program
 Rotator Cuff and Shoulder Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy
Rotator Cuff and Shoulder Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy
Conservative Massive Rotator Cuff Tear Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Massive Rotator Cuff Tear Protocol 3-4 visits over 4-6 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Emphasize improved
SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Massive Rotator Cuff Tear Protocol 3-4 visits over 4-6 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Emphasize improved
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood
 Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Elbow Replacement Guide
 Elbow Replacement Guide IM-CNOH-12 Rev. 1 Issue Date: March 2011 Review Date: March 2012 Founded 1908 C A P PA G H N AT I O N A L O RT H O PA E D I C H O S P I TA L FINGLAS, DUBLIN 11. TEL: 01 814 0429
Elbow Replacement Guide IM-CNOH-12 Rev. 1 Issue Date: March 2011 Review Date: March 2012 Founded 1908 C A P PA G H N AT I O N A L O RT H O PA E D I C H O S P I TA L FINGLAS, DUBLIN 11. TEL: 01 814 0429
MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No JX
 MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No 202767JX Phone: 9529 3820 Fax: 9573 9693 Email:mevans@mog.com.au www.matthewevans.com.au REHABILITATION
MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No 202767JX Phone: 9529 3820 Fax: 9573 9693 Email:mevans@mog.com.au www.matthewevans.com.au REHABILITATION
Rehabilitation Program for Rotator Cuff & Scapular Muscles
 Kansas City Sports Medicine Sports Medicine & Arthroscopy Olathe, KS Lansing, KS Kansas City, KS/MO Ph: 913-351-3005 Fax: 913-351-3009 Prem Parmar, M.D., F.R.C.S.(C) Sports Medicine and Arthroscopy Fellow
Kansas City Sports Medicine Sports Medicine & Arthroscopy Olathe, KS Lansing, KS Kansas City, KS/MO Ph: 913-351-3005 Fax: 913-351-3009 Prem Parmar, M.D., F.R.C.S.(C) Sports Medicine and Arthroscopy Fellow
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Occupational therapy for adults with secondary lymphedema : a case study
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Occupational therapy for adults with secondary lymphedema : a case study Gina L. D. Kubec The University
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Occupational therapy for adults with secondary lymphedema : a case study Gina L. D. Kubec The University
Suprascapular Nerve Entrapment
 Suprascapular Nerve Entrapment Suprascapular nerve entrapment is an uncommon nerve condition in the shoulder, causing pain and weakness. It involves compression of the suprascapular nerve at the top or
Suprascapular Nerve Entrapment Suprascapular nerve entrapment is an uncommon nerve condition in the shoulder, causing pain and weakness. It involves compression of the suprascapular nerve at the top or
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty
 Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol. Phase 1 Maximum Protection (0-4 weeks)
 Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
POST OPERATIVE ROTATOR CUFF REPAIR PROTOCOL. Home Program
 MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
FOR THE SERVICE MEMBER: Rx3 REHABILITATION PROGRAM
 CREATED BY THE HUMAN PERFORMANCE RESOURCE CENTER / HPRC-ONLINE.ORG / FROM THE CONSORTIUM FOR HEALTH AND MILITARY PERFORMANCE HUMAN PERFORMANCE RESOURCE CENTER Injury/Condition: Injury/Condition: What is
CREATED BY THE HUMAN PERFORMANCE RESOURCE CENTER / HPRC-ONLINE.ORG / FROM THE CONSORTIUM FOR HEALTH AND MILITARY PERFORMANCE HUMAN PERFORMANCE RESOURCE CENTER Injury/Condition: Injury/Condition: What is
REHABILITATION PROTOCOL FOR ROTATOR CUFF SURGERY SMALL TO MEDIUM TEARS PHYSIOTHERAPY GUIDELINES
 MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No 202767JX Phone: 9529 3820 Fax: 9573 9693 Email:mevans@mog.com.au www.matthewevans.com.au REHABILITATION
MATTHEW EVANS MBBS, FRACS (Orth), FAOrthA ORTHOPAEDIC SURGEON Knee and Shoulder Surgery Provider No 202767JX Phone: 9529 3820 Fax: 9573 9693 Email:mevans@mog.com.au www.matthewevans.com.au REHABILITATION
Shoulder Surgery Discharge Instructions
 Note: This information is provided for general educational purposes only. Because every individual is different, these instructions will not apply to every patient. Only your doctor can tell you what is
Note: This information is provided for general educational purposes only. Because every individual is different, these instructions will not apply to every patient. Only your doctor can tell you what is
Protocol S8 Physical Therapy Protocol for Arthroscopic Reverse Bankart Repair or Open Posterior Capsulorrhaphy
 Phase I: Protection Phase (0-5 weeks) Allow time for labral repair to heal. Gradually increase shoulder passive range of motion (ROM) Use pain medications as needed. Wear shoulder immobilizer for 5 weeks.
Phase I: Protection Phase (0-5 weeks) Allow time for labral repair to heal. Gradually increase shoulder passive range of motion (ROM) Use pain medications as needed. Wear shoulder immobilizer for 5 weeks.
Urmston Physio Clinic
 Urmston Physio Clinic Patient Information Shoulder Instability Prepared for Mr B. Roy Consultant Orthopaedic Surgeon 102 Church Road, Urmston, Manchester, M41 9DB Tel: 0161 748 4100 Shoulder Instability
Urmston Physio Clinic Patient Information Shoulder Instability Prepared for Mr B. Roy Consultant Orthopaedic Surgeon 102 Church Road, Urmston, Manchester, M41 9DB Tel: 0161 748 4100 Shoulder Instability
Vol 3, 2008 CEC ARTICLE: Special Medical Conditions Part 2: Shoulder Maintenance and Rehab C. Eggers
 Vol 3, 2008 CEC ARTICLE: Special Medical Conditions Part 2: Shoulder Maintenance and Rehab C. Eggers SHOULDER GIRDLE STABILIZATION Knowledge of the anatomy and biomechanics of the shoulder girdle is essential
Vol 3, 2008 CEC ARTICLE: Special Medical Conditions Part 2: Shoulder Maintenance and Rehab C. Eggers SHOULDER GIRDLE STABILIZATION Knowledge of the anatomy and biomechanics of the shoulder girdle is essential
Phase I: 0 to 3 weeks after surgery
 Dx: Right Left RTC (Massive) Repair Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: 2. Ensure wound healing Phase I:
Dx: Right Left RTC (Massive) Repair Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: 2. Ensure wound healing Phase I:
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C
 WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
RANGE OF MOTION Pendulums. Passive Forward Elevation. Clayton W. Nuelle, MD. Shoulder Home Exercise Program
 Shoulder Home Exercise Program Clayton W. Nuelle, MD RANGE OF MOTION Pendulums Holding the side of a table with the good arm, bend over at the waist, and let your affected arm hang straight down. Swing
Shoulder Home Exercise Program Clayton W. Nuelle, MD RANGE OF MOTION Pendulums Holding the side of a table with the good arm, bend over at the waist, and let your affected arm hang straight down. Swing
Rotator Cuff Injuries
 Rotator Cuff Injuries Introduction Shoulder injuries are fairly common, especially for people who tend to exercise a lot. Some of the most common shoulder injuries are called rotator cuff injuries. This
Rotator Cuff Injuries Introduction Shoulder injuries are fairly common, especially for people who tend to exercise a lot. Some of the most common shoulder injuries are called rotator cuff injuries. This
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT
 REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
On The Road. Training Manual
 On The Road Training Manual ST - 1 Standing External Rotation Strength Training Injury prevention Strengthening the rotator cuff Attach the tubing to a secure location like a fence or the net post. Start
On The Road Training Manual ST - 1 Standing External Rotation Strength Training Injury prevention Strengthening the rotator cuff Attach the tubing to a secure location like a fence or the net post. Start
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
SLAP Repair Therapy Protocol
 PHASE I: PRE-OPERATIVE PHASE (OPTIONAL) SLAP Repair Therapy Protocol Bart Eastwood D.O. 250 South Main St. Suite 224A Blacksburg, VA 24060 540-552-7133 Restore full AROM and PROM Restore full strength
PHASE I: PRE-OPERATIVE PHASE (OPTIONAL) SLAP Repair Therapy Protocol Bart Eastwood D.O. 250 South Main St. Suite 224A Blacksburg, VA 24060 540-552-7133 Restore full AROM and PROM Restore full strength
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
What s Your Game Plan? Sports Injuries
 What s Your Game Plan? Sports Injuries Howard Winston, MD, CCFP, FCFP As presented at the University of Toronto s Primary Care Today conference (October 2003) Sports medicine often involves analyzing the
What s Your Game Plan? Sports Injuries Howard Winston, MD, CCFP, FCFP As presented at the University of Toronto s Primary Care Today conference (October 2003) Sports medicine often involves analyzing the
Jennifer L. Cook, MD Stephen A. Hanff, MD. Rotator Cuff Type I Repair (Small Large Tear)
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Low-Back Strain DESCRIPTION POSSIBLE COMPLICATIONS COMMON SIGNS AND SYMPTOMS GENERAL TREATMENT CONSIDERATIONS CAUSES FACTORS THAT INCREASE RISK
 Page Number: 0 Date:13/6/11 Time:20:10:06 Low-Back Strain DESCRIPTION POSSIBLE COMPLICATIONS Low-back strain is an injury to the muscles and tendons of the lower back. These muscles require great force
Page Number: 0 Date:13/6/11 Time:20:10:06 Low-Back Strain DESCRIPTION POSSIBLE COMPLICATIONS Low-back strain is an injury to the muscles and tendons of the lower back. These muscles require great force
ROTATOR CUFF TEAR, SURGERY FOR
 ROTATOR CUFF TEAR, SURGERY FOR Indications (Who Needs Surgery, When, electricity is used to cauterize small capillaries. Electricity or Why, and Goals) a motorized shaver is used to remove the bursa and
ROTATOR CUFF TEAR, SURGERY FOR Indications (Who Needs Surgery, When, electricity is used to cauterize small capillaries. Electricity or Why, and Goals) a motorized shaver is used to remove the bursa and
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of
 Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
UPPER EXTREMITY INJURIES. Recognizing common injuries to the upper extremity
 UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
Rotator Cuff Repair Therapy Protocol
 Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Rehabilitation Program Following Isolated Biceps Tenodesis
 Rehabilitation Program Following Isolated Biceps Tenodesis Richard Holtby Assistant professor, Department of Surgery University of Toronto Biceps Groove Biceps tendon HOLLAND ORTHOPAEDIC & ARTHRITIC CENTRE
Rehabilitation Program Following Isolated Biceps Tenodesis Richard Holtby Assistant professor, Department of Surgery University of Toronto Biceps Groove Biceps tendon HOLLAND ORTHOPAEDIC & ARTHRITIC CENTRE
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Hemiplegic Shoulder. Incidence & Rationale. Shoulder Pain Assessment & Treatment
 Hemiplegic Shoulder Jeane Davis Fyfe OT, Senior Therapist Incidence & Rationale Up to 72% of stroke survivors will experience shoulder pain Shoulder pain may inhibit patient participation in rehabilitation
Hemiplegic Shoulder Jeane Davis Fyfe OT, Senior Therapist Incidence & Rationale Up to 72% of stroke survivors will experience shoulder pain Shoulder pain may inhibit patient participation in rehabilitation
Theodore B. Shybut, M.D.
 Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Non-operative Shoulder Rehabilitation Protocol Basic shoulder program for: o Scapular Dyskinesis (proximally
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Non-operative Shoulder Rehabilitation Protocol Basic shoulder program for: o Scapular Dyskinesis (proximally
Shoulder Exercises Phase 1 Phase 2
 Shoulder Exercises Phase 1 1. Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion.
Shoulder Exercises Phase 1 1. Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion.
Reverse Total Shoulder
 Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol:
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
