Rehabilitation Guidelines for Achilles Tendon Repair
|
|
|
- Kenneth Bruce
- 6 years ago
- Views:
Transcription
1 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius) to the heel bone (calcaneus). The tendon transmits force from the contracting calf muscles to the calcaneus to cause the foot action of plantar flexion (foot pointed down) that is important in walking, running, jumping and change of direction activities. Although the Achilles tendon is the strongest tendon in the body, it is also the tendon most commonly torn or ruptured. The most common causes of rupture are: Sudden plantar flexion (foot moving downward) such as taking off to jump. Unplanned or forced dorsiflexion (foot moving upward) such as landing a jump or stepping into a hole. Direct trauma to the tendon. Most Achilles tendon ruptures occur in sports that require running, jumping and change of direction. The typical age for rupture occurs between years of age and is significantly more common in males than females. Older adults can also rupture the Achilles tendon and are more inclined to have degenerative partial tearing of the tendon. Other risk factors for Achilles tendon rupture include use of Fluoroquinolone antibiotics and direct steroid injections into the tendon. Figure 1 The dotted line represents the longitudinal incision used to expose the ruptured Achilles tendon during surgical repair. Figure 2 Torn Achilles tendon. The diagnosis of an Achilles tendon rupture is made from clinical history, physical exam and diagnostic testing. Most patients who sustain an Achilles tendon rupture report a pop and a feeling of being kicked or shot in the back of the leg. On exam, there is a palpable divot or gap in the area of the rupture along with significant swelling. Patients will demonstrate a positive Thompson test, performed by squeezing the calf muscle while the patient lies prone. This test is positive when the calf is squeezed and plantarflexion does not occur. Diagnostic testing such as an Ultrasound or MRI (magnetic resonance imaging) may be used to determine if there is a complete or partial tear. Treatment options for an Achilles tendon rupture include surgical repair and conservative non-surgical rehabilitation. Decision making is based on age, past medical history and desired level of functional return. Conservative non-surgical treatment includes rehabilitation with initial immobilization followed by gentle range of motion and progressive strengthening to regain function. Most surgical procedures to repair a torn Achilles tendon include an open longitudinal incision medial to the Achilles tendon (Figure 1). The incision is made medial to the tendon to improve skin healing and to reduce the risk of scarring to the underlying tendon repair. Once the incision is made and the rupture is identified (Figure 2), clamps are used to match the ends together in an optimal tendon length. A primary repair of the two ends of the tendon is performed by stitching them together. There are many different stitching techniques to repair the tendon. The type used will depend on the surgeon, the type of rupture, and tissue quality. Sometimes the repair is augmented or strengthened using fascia or tendon. A gastrocnemius aponeurosis augmentation is performed when a 1 2 cm wide by 8 cm long flap is made and turned down over the repair and sutured to reinforce the repair. The area that the flap was harvested from is then stitched together. In cases of tendon degeneration, or tendiosis, this may help strengthen the repaired tendon. Historically it has been thought that a surgically repaired Achilles tendon offered a significantly smaller risk of The world class health care team for the UW Badgers and proud sponsor of UW Athletics UWSPORTSMEDICINE.ORG
2 re-rupture rate and increased strength in comparison to non- surgical treatment. The major risks associated with surgery include infection, deep vein thrombosis (DVT) and difficulty with wound closure. Recent studies suggest similar rupture rates, strength and mobility between surgery and non-surgery approaches to the management of Achilles tendon ruptures. The best approach varies for each individual. Your surgeon and you will determine what is best for you by discussing your specific injury and goals. Rehabilitation following Achilles tendon repair is vital in regaining motion, strength and function. Initially a walking boot is used for the first 4 5 weeks. Gradually more weight bearing and mobility is allowed to prevent stiffness post-operatively. The rehabilitation progresses slowly into strengthening, gait and balancing activities. Rehabilitation guidelines are presented in a criterion based progression. General time frames refer to the usual pace of rehabilitation. Individual patients will progress at different rates depending on their age, associated injuries, pre-injury health status, rehab compliance, tissue quality and injury severity. Specific time frames, restrictions and precautions may also be given to enhance wound healing and to protect the surgical repair/ reconstruction. PHASE I (surgery to 2 weeks after surgery) Rehabilitation appointments begin days after surgery Protection of the surgically repaired tendon Wound healing Precautions Continuous use of the boot in locked plantarflexion (20-30 ) Touchdown weight bearing (TDWB) using the axillary crutches Keep the incision dry Watch for signs of infection Avoid long periods of dependent positioning of the foot during the first week to assist in wound healing Upper Body Ergometer (UBE) circuit training Two weeks after surgery PHASE II (begin after meeting Phase 1 criteria, usually 2-4 weeks after surgery) Rehabilitation appointments are 1-2 times per week Normalize gait with weight bearing as tolerated (WBAT) using the boot and axillary crutches Protection of the post-surgical repair Active dorsiflexion to neutral 2 UWSPORTSMEDICINE.ORG
3 Precautions for Dr. Baer s Patients Precautions for Dr. Scerpella s and Dr. Spiker s Patients Precautions for Dr. Williams Patients Post-operative week 2-3: Continuous use of the boot with 10 of plantar flexion with 1-2 ¼ inch heel lifts, except during rehabilitation Post-operative week 3-4: Continuous use of the boot with 0 of plantar flexion with 1-2 ¼ inch heel lifts, except during rehabilitation WBAT (based on pain, swelling and wound appearance) using the axillary crutches and boot Do not soak the incision (i.e. no pool or bathtub) Watch for signs of poor wound healing Post-operative week 2-3: boot locked at 20 PF, toe touch weight bearing (TTWB) using the axillary crutches and boot, no active dorsiflexion, sleep in boot Post-operative week 3-4: boot locked at 10deg PF, TTWB using the axillary crutches and boot, sleep in boot Post-operative week 4-6: If pt can reach neutral PF/DF comfortably, then neutral boot with 1-2 ¼ inch heel lifts, WBAT (based on pain, swelling and wound appearance) using the axillary crutches and boot, limit active dorsiflexion to neutral sleep in boot Placed into tall walking boot with 2 heel lifts (boot in PF) Instructed to begin active dorsiflexion (to neutral DF only) with passive plantar flexion 10 repetitions 3 times per day (start at 2 weeks) Touchdown weightbearing in boot with crutches Ankle range of motion (ROM) with respect to precautions Pain-free isometric ankle inversion, eversion, dorsiflexion and sub-max plantarflexion Open chain hip and core strengthening Upper extremity circuit training or UBE Six weeks post-operatively Pain-free active dorsiflexion to 0 No wound complications. If wound complications occur, consult with a physician 3 UWSPORTSMEDICINE.ORG
4 PHASE III (begin after meeting Phase II criteria, usually 6 to 8 weeks after surgery) Precautions Rehabilitation appointments are once a week Normalize gait on level surfaces without boot or heel lift Single leg stand with good control for 10 seconds Active ROM between 5 of dorsiflexion and 40 of plantarflexion Slowly wean from use of the boot: Begin by using 1-2 ¼ inch heel lifts in tennis shoes for short distances on level surfaces then gradually remove the heel lifts during the 5th and 8th week depending on the surgeon Avoid over-stressing the repair (avoid large movements in the sagittal plane; any forceful plantarflexion while in a dorsiflexed position; aggressive passive ROM; and impact activities) Frontal and sagittal plane stepping drills (side step, cross-over step, grapevine step) Active ankle ROM Gentle gastroc/soleus stretching Static balance exercises (begin in 2 foot stand, then 2 foot stand on balance board or narrow base of support and gradually progress to single leg stand) 2 foot standing nose touches Ankle strengthening with resistive tubing Low velocity and partial ROM for functional movements (squat, step back, lunge) Hip and core strengthening Pool exercises if the wound is completely healed Upper extremity circuit training or UBE Normal gait mechanics without the boot Squat to 30 knee flexion without weight shift Single leg stand with good control for 10 seconds Active ROM between 5 of dorsiflexion and 40 of plantarflexion PHASE IV (begin after meeting Phase III criteria, usually 8 weeks after surgery) Precautions Rehabilitation appointments are once every 1-2 weeks Normalize gait on all surfaces without boot or heel lift Single leg stand with good control for 10 seconds Active ROM between 15 of dorsiflexion and 50 of plantarflexion Good control and no pain with functional movements, including step up/down, squat and lunges Avoid forceful impact activities Do not perform exercises that create movement compensations 4 UWSPORTSMEDICINE.ORG
5 Frontal and transverse plane agility drills (progress from low velocity to high, then gradually adding in sagittal plane drills) Active ankle ROM Gastroc/soleus stretching Multi-plane proprioceptive exercises single leg stand 1 foot standing nose touches Ankle strengthening concentric and eccentric gastroc strengthening Functional movements (squat, step back, lunge) Hip and core strengthening Stationary bike, Stair Master, swimming Normal gait mechanics without the boot on all surfaces Squat and lunge to 70 knee flexion without weight shift Single leg stand with good control for 10 seconds Active ROM between 15 of dorsiflexion and 50 of plantarflexion PHASE V (begin after meeting Phase IV criteria usually 4 months after surgery) Precautions Rehabilitation appointments are once every 1-2 weeks Good control and no pain with sport/work specific movements, including impact Post-activity soreness should resolve within 24 hours Avoid post-activity swelling Avoid running with a limp Impact control exercises beginning 2 feet to 2 feet, progressing from 1 foot to other and then 1 foot to same foot Movement control exercise beginning with low velocity, single plane activities and progressing to higher velocity, multi-plane activities Sport/work specific balance and proprioceptive drills Hip and core strengthening Stretching for patient specific muscle imbalances Replicate sport/work specific energy demands Dynamic neuromuscular control with multi-plane activities, without pain or swelling These rehabilitation guidelines were developed collaboratively by UW Health Sports Rehabilitation and the UW Health Sports Medicine Physician group. Updated 2/ UWSPORTSMEDICINE.ORG
6 REFERENCES 1. Paul van der Linden et. Al. Increased Risk of Achilles Tendon Rupture with Quinolone Antibacterial Use Arch Intern Med 2003; 163: Baer GS, Keene JS. Tendon Injuries of the Foot and Ankle: Achilles Tendon Ruptures. In Orthopedic Sports Medicine: Principles and Practice. (Third Edition) Ed. DeLee and Drez, Saunders, Philadelphia, PA, Twaddle, Poon. Early motion for Achilles Tendon Ruptures: Is Surgery Important? AJSM Nilsson-Helander et al. Acute Achilles Tendon Rupture: A Randomized, Controlled Study Comparing Surgical and Nonsurgical Treatments Using Validated Outcome Measures AJSM Bhandari et al. Treatment of acute Achilles tendon ruptures: a systematic overview and metaanalysis Clin orthop Relate Res Willits, et al. Operative versus nonoperative treatment of acute Achilles tendon ruptures: A multicenter randomized trial using accelerated functional rehabilitation. JBJS. 2010:92- A;17( ). At UW Health, patients may have advanced diagnostic and /or treatment options, or may receive educational materials that vary from this information. Please be aware that this information is not intended to replace the care or advice given by your physician or health care provider. It is neither intended nor implied to be a substitute for professional advice. Call your health provider immediately if you think you may have a medical emergency. Always seek the advice of your physician or other qualified health provider prior to starting any new treatment or with any question you may have regarding a medical condition. Copyright 2018 UW Health Sports Medicine 6 UWSPORTSMEDICINE.ORG SM
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair
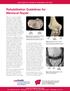 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
Rehabilitation Guidelines for Knee Arthroscopy
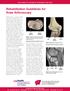 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
Achilles Tendon Rupture
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
NICHOLAS J. AVALLONE, M.D.
 NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
Post Operative ACL Reconstruction Protocol Brian J. White, MD
 Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Post-Operative Meniscus Repair Protocol Brian J.White, MD
 Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
Rehabilitation and Return to Play Following Achilles Tendon Repair
 Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Rehabilitation Program for Achilles Tendon Rupture/Repair
 Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Achilles Tendon Repair and Rehabilitation
 1 Achilles Tendon Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The poorest blood supply to the Achilles tendon is in the central part of the tendon approximately
1 Achilles Tendon Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The poorest blood supply to the Achilles tendon is in the central part of the tendon approximately
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN Tel: Fax:
 Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
Dr Schock Achilles Tendon Repair Protocol
 Dr Schock Achilles Tendon Repair Protocol Phase 1- Maximum Protective Phase (2-4 post-op) Goals for Phase 1 Protect integrity of repair Minimize effusion ROM per guidelines listed Immobilization/Weight
Dr Schock Achilles Tendon Repair Protocol Phase 1- Maximum Protective Phase (2-4 post-op) Goals for Phase 1 Protect integrity of repair Minimize effusion ROM per guidelines listed Immobilization/Weight
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Achilles tendon rupture: management and rehabilitation
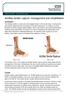 Achilles tendon rupture: management and rehabilitation Introduction The Achilles tendon (or heel cord) is the largest tendon in the human body. It connects the calf muscles (gastrocnemius and soleus) to
Achilles tendon rupture: management and rehabilitation Introduction The Achilles tendon (or heel cord) is the largest tendon in the human body. It connects the calf muscles (gastrocnemius and soleus) to
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015
 PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
Acute Achilles Tendon Repair Protocol
 Acute Achilles Tendon Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that you
Acute Achilles Tendon Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that you
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Patella Tendon Repair
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
Christopher Kim, MD, Minh-Ha Hoang, DO, Scott G. Kaar, MD, William Mitchell, MD and Lauren Smith,PA-C
 Christopher Kim, MD, Minh-Ha Hoang, DO, Scott G. Kaar, MD, William Mitchell, MD and Lauren Smith,PA-C Department of Orthopaedic Surgery Sports Medicine and Shoulder Service Achilles Tendon Rupture Non-Operative
Christopher Kim, MD, Minh-Ha Hoang, DO, Scott G. Kaar, MD, William Mitchell, MD and Lauren Smith,PA-C Department of Orthopaedic Surgery Sports Medicine and Shoulder Service Achilles Tendon Rupture Non-Operative
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
Rehabilitation Guidelines for Large Rotator Cuff Repair
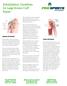 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Sheena Black, MD PHYSICAL THERAPY PRESCRIPTION MCL RECONSTRUCTION. Orthopaedic Surgery, Sports Medicine.
 PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
Hip Arthroscopy Protocol
 The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
Microfracture of Knee Joint
 Microfracture of Knee Joint Post-op Precautions: The patient will ambulate with crutches for 4 weeks or more after surgery. The physician will base weightbearing status upon the location of the lesion.
Microfracture of Knee Joint Post-op Precautions: The patient will ambulate with crutches for 4 weeks or more after surgery. The physician will base weightbearing status upon the location of the lesion.
Femoral Condyle Rehabilitation Guidelines
 Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
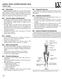 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Following Unilateral Patellar Tendon Repair
 Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
Week 1 Orthotics- 1. Knee brace locked in full extension at all times except for rehab exercises 2. Elastic bandage as needed to control swelling
 General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) Fax: (763)
 Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
ACL Reconstruction Rehabilitation Protocol
 ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
ACHILLES RUPTURE YOUR GUIDE TO. An IPRS Guide to provide you with exercises and advice to ease your condition
 YOUR GUIDE TO ACHILLES RUPTURE Contents What is an Achilles Rupture?..................................... 3 What treatment can I receive?................................... 4 What exercises should I do?......................................
YOUR GUIDE TO ACHILLES RUPTURE Contents What is an Achilles Rupture?..................................... 3 What treatment can I receive?................................... 4 What exercises should I do?......................................
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
REHABILITATION GUIDELINES AFTER ACL RECONSTRUCTION. Shail Vyas, MD Orange County Orthopaedic Group (714)
 REHABILITATION GUIDELINES AFTER ACL RECONSTRUCTION Shail Vyas, MD Orange County Orthopaedic Group (714) 974-0100 The intent of this protocol is to provide the therapist with guidelines of the post-operative
REHABILITATION GUIDELINES AFTER ACL RECONSTRUCTION Shail Vyas, MD Orange County Orthopaedic Group (714) 974-0100 The intent of this protocol is to provide the therapist with guidelines of the post-operative
ACL AUTOGRAFT PATELLAR TENDON RECONSTRUCTION PLUS MENISCUS REPAIR PROTOCOL
 Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
Anterior Cruciate Ligament (ACL) Reconstruction Protocol. Hamstring Autograft, Allograft, or Revision
 Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
Rehabilitation Guidelines for UCL Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for UCL Repair The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the larger bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for UCL Repair The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the larger bone
ACL Patella Tendon Autograft Reconstruction Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Patella Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the clinician
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Patella Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the clinician
Rehabilitation Guidelines for Shoulder Arthroscopy
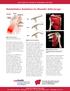 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab Protocol
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab
ANKLE SPRAINS. Explanation. Causes. Symptoms
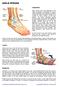 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound
Medial Patellofemoral Ligament Repair/Reconstruction
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
ORTHOPEDIC SURGERY, SPORTS MEDICINE, AND ARTHROSCOPY
 WWW.MATTDRISCOLLMD.COM ORTHOPEDIC SURGERY, SPORTS MEDICINE, AND ARTHROSCOPY ACL Reconstruction Rehab Protocol The intent of this protocol is to provide a general framework for ACL rehabilitation. Within
WWW.MATTDRISCOLLMD.COM ORTHOPEDIC SURGERY, SPORTS MEDICINE, AND ARTHROSCOPY ACL Reconstruction Rehab Protocol The intent of this protocol is to provide a general framework for ACL rehabilitation. Within
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT
 REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
Patellar Tendon Repair Rehabilitation Guideline
 Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol
 REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
ACL PATELLAR TENDON AUTOGRAFT RECONSTRUCTION PROTOCOL
 Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
GALLAND/KIRBY PCL RECONSTRUCTION POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY PCL RECONSTRUCTION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue TED Hose
GALLAND/KIRBY PCL RECONSTRUCTION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue TED Hose
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair
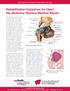 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
REHABILITATION GUIDELINES FOR ACL REPAIR
 Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL REPAIR PHASE I (0-2 WEEKS) Physical therapy 2-3x/week, beginning 2-5 days post-op Rehabilitation
Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL REPAIR PHASE I (0-2 WEEKS) Physical therapy 2-3x/week, beginning 2-5 days post-op Rehabilitation
KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC
 PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC Revised August 2008 Post-op Days 1 14 Dressing POD
PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC Revised August 2008 Post-op Days 1 14 Dressing POD
Achilles Tendonitis and Tears
 Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
ACHILLES TENDON DISORDERS
 MUSCULOSKELETAL YOUR GUIDE TO ACHILLES TENDON DISORDERS An IPRS Guide to provide you with exercises and advice to ease your condition Contents What is the Achilles Tendon?.....................................
MUSCULOSKELETAL YOUR GUIDE TO ACHILLES TENDON DISORDERS An IPRS Guide to provide you with exercises and advice to ease your condition Contents What is the Achilles Tendon?.....................................
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ORIF PATELLA BENJAMIN J. DAVIS, MD
 I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE
 PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE Revised August 2008 Post-op Days 1 14 Dressing POD
PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE Revised August 2008 Post-op Days 1 14 Dressing POD
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL REHABILITATION FOLLOWING UNILATERAL PETELLAR TENDON REPAIR BENJAMIN J.
 I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
Knee OCD Repair/Fixation/Grafting Protocol
 Knee OCD Repair/Fixation/Grafting Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that
Knee OCD Repair/Fixation/Grafting Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are indicators that
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION WITH MICROFRACTURE OR CARTIFORM/BIOCARTILAGE (TROCHLEA OR PATELLA)
 Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION PHASE I (0-3 WEEKS) Appointments Begin physical therapy 2-5 days post op
Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION PHASE I (0-3 WEEKS) Appointments Begin physical therapy 2-5 days post op
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol:
 Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
Hip Arthroscopy with CAM resection/labral Repair Protocol
 Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
Anterior Cruciate Ligament Reconstruction Standard Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Standard Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction
Anterior Cruciate Ligament Reconstruction Standard Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
Rehabilitation Guidelines for ACL Reconstruction in the Older Adolescent Athlete (Hamstrings with No Hardware Across Growth Plates)
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for ACL Reconstruction in the Older Adolescent Athlete (Hamstrings with No Hardware Across Growth Plates) Anterior cruciate ligament (ACL) injuries
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for ACL Reconstruction in the Older Adolescent Athlete (Hamstrings with No Hardware Across Growth Plates) Anterior cruciate ligament (ACL) injuries
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
