Review Submitted by: Katie Long, PT, DPT
|
|
|
- Samuel Gallagher
- 5 years ago
- Views:
Transcription
1 Added, Marco Aurélio N. et al. "STRENGTHENING THE GLUTEUS MAXIMUS IN SUBJECTS WITH SACROILIAC DYSFUNCTION". International Journal Of Sports Physical Therapy, vol 13, no. 1, 2018, pp The Sports Physical Therapy Session, doi: /ijspt Review Submitted by: Katie Long, PT, DPT Objective: To assess the effect of a gluteus maximus focused exercise program in individuals who demonstrate positive clinical testing for SIJ dysfunction. Methods: Eight subjects were included in the study, 4 males and 4 females. Patient evaluation included trunk and hip ROM, VAS pain assessment, and Oswestry Disability Index scores. Gluteus maximus strength was assessed using dynamometer, Slump test was assessed, Laseque straight leg maneuver, Piriformis test, Grava test, FABER test and Scour test were all performed. SIJ screening included SI compression, SI distraction, Squish, and Gaenslen tests with 3/4 positive testing indicated SIJ Dysfunction. Subjects included in the study had to have unilateral lumbopelvic pain in the SI region for >12 weeks and have received no previous PT intervention. Subjects were excluded if they had clinical and imaging evidence of any spinal or pelvic comorbidity as a potential cause of their symptoms, no signs of lower limb length discrepancy, or if they had a cognitive deficiency. Subjects attended 10 physical therapy treatments at 2x/week. During the first 5 treatment sessions, they performed the following exercises: bilateral bridging, unilateral bridging, prone hip extension with knee bent to 90 degrees. In the following 5 treatment sessions fire hydrant and deadlift exercises were added. Gluteus maximus muscle strength was assessed in prone utilizing hand-held dynamometry Results: Prior to initiating treatment, a significant strength deficit was noted between the asymptomatic side as compared to the symptomatic side. Following treatment intervention, there was a significant increase in gluteus maximus strength on the involved side ranging from 17-29%; however, there was no change noted in strength of the asymptomatic side. A significant decrease in pain as measured by VAS was observed and a significant increase in selfreported function was reported by the Oswestry following 5-week intervention period. Conclusions: The results of this case series suggests that subjects with persistent lumbopelvic pain and positive SIJ testing may benefit from increased gluteus maximus emphasis during a strengthening program. These results show a significant increase in function and strength with decreased reports of pain following a strength training program directed at gluteus maximus strengthening. The authors suggest that by increasing strength of the gluteus maximus muscle, there may be an increased stabilization of the musculature and fascia surrounding the SI joint by aiding in increasing compressive forces at the SI joint in order to aid in load transfer. Commentary: This case series highlights the importance of emphasizing gluteus maximus hip extensor training in patients with persistent lumbopelvic pain and positive SIJ testing. It provides support for the concept of increasing stability of the SIJ during force transfer from the LE to the trunk. Patients with persistent lumbopelvic pain often have decreased hip extensor strength and/or range of motion, and this article provides a nice reminder to address these impairments in this patient population. This article also provides a nice educational framework for utilization with patients to emphasize increased adherence to exercise intervention.
2 Roenz D, Broccolo J, Brust S, et al. The impact of pragmatic vs. prescriptive study designs on the outcomes of low back and neck pain when using mobilization or manipulation techniques: A systematic review and meta-analysis. J Man Manip Ther. 2018;26:3, Review Submitted By: Tyler France, PT, DPT, CSCS Objective: The objective of this study was to examine the impact of pragmatic versus prescriptive study designs on the outcomes of low back and neck pain when using mobilization or manipulation techniques. Methods: This systematic review and meta-analysis was performed according to PRISMA guidelines. MEDLINE and CINAHL were searched to identify studies comparing mobilization and manipulation for neck or back pain that met eligibility criteria. The selected articles needed to meet all the following inclusion criteria: written in English, randomized clinical trial, compared mobilization versus manipulation in isolation, included patients with low back pain or neck pain, and used an outcome measure of pain or disability. Eligible studies were classified as pragmatic or prescriptive based on criteria used by Kent et al. To be classified as pragmatic, clinicians needed to be able to choose the technique and spinal levels to be treated. The validity of studies was examined using the Cochrane Risk of Bias tool. Results: Thirteen studies with a total of 1313 participants were included in the systematic review. 8 studies (61.5%) examined the interventions with a prescriptive approach and 5 studies (38.5%) utilized a pragmatic approach. For most time-points, prescriptive studies found manipulation to be superior to mobilization for both pain and disability. At no time-point did pragmatic designs find a difference between mobilization or manipulation for either pain or disability. When looking at prescriptive studies, manipulation was found to be more effective in the short term (1-4 weeks) and in the long term (3-6 months). There were no significant differences between mobilization and manipulation in pragmatic studies. Conclusions: When a pragmatic design was used, representing actual clinical practice, patients improved with both techniques with no difference between mobilization and manipulation. When clinicians were prescribed techniques, not representing true clinical practice, manipulation showed better outcomes than mobilization for pain and disability. Commentary: The authors suggest that the findings of the systematic review and meta-analysis can be attributed to the differences in pragmatic and prescriptive studies, including inclusion criteria, different level of focus on validity, and the method of treatment delivery. The pragmatic approach more closely resembles actual patient care and demonstrates that when clinicians are allowed to use their clinical reasoning and expertise, mobilization and manipulation have similar effects. After reviewing this study, I will certainly be more aware in the future when looking at studies comparing mobilization and manipulation and determining how closely the design mimics actual clinical practice.
3 Pamukoff D, Montgomery M, Choe K, Moffit T, Gargia S, Vakula M. Bilateral alterations in running mechanics and quadriceps function following unilateral anterior cruciate ligament reconstruction. J Orthop Sports Phys Ther. 2018;1-26. Review submitted by: Jennifer M. Boyle Objective: The primary purpose of this study was to compare sagittal plane knee mechanics and vertical GRF characteristics during running between involved and uninvolved limbs of individuals who have undergone ACLR, and to its limbs of a healthy control group. A secondary purpose of this article was to evaluate the association between quadriceps muscle performance isometric peak torque (PT) and rate of torque (RTD) development and the after mentioned running mechanics in the involved limb of persons who have undergone ACLR. Methods: Thirty- eight participants with primary unilateral ACLR that were matched with thirty eight control participants. This match was based on sex, age and body mass. Quadriceps muscle performance was assessed with isokinetic and isometric knee extension peak torque (PT) and rate of torque (RTD100 and RTD200). Running evaluation consisting of 5- minute jogging warm up followed by a 20-minute run over a force plate where 3-dimensional running biomechanics were analyzed. An assessment of the knee flexion angle (KFA), knee extension moment (KEM), rate of knee extension moment (RKEM), vertical instantaneous loading rate (VILR) and vertical impact peak (VIP) was collected. Results: On average, there was a smaller KFA in the involved limb compared to uninvolved limb in the ACLR group. Compared to control group limbs, involved limbs in the ACLR group had lower RTD100, lower PT at 60 sec, lower PT at 180 sec, smaller KFA, lower KEM, lower RKEM, and higher VILR. Compared to control group limbs, uninvolved limbs in the ACLR group had lower RTD100, lower PT at 60 sec, and smaller KFA. For the involved limbs in the ACLR group, there was a low correlation between isokinetic PT at 180 sec and RKEM, and between RTD100 and RKEM. No differences were found in isometric strength for any comparison. Conclusions: This study found that sagittal plane running mechanics of the involved and uninvolved limbs of individuals after unilateral ACLR are different then control limbs. This study loosely correlates these changes in mechanics to rate of torque development ms and isokinetic strength of the quadriceps. Commentary: After ACLR patients are looking to return to pre -injury levels of physical activities, however, many individuals struggle with return to sport following this surgery. In some cases the impairments that are unresolved post ACLR can lead to decreased ability to perform ADLs, participate in sports and can elevate the risk of re- injury as well as develop post traumatic knee OA. This article has revealed that improving bilateral quadriceps muscle performance and running biomechanics are necessary following unilateral anterior cruciate ligament reconstruction. I feel like at times the unaffected limb is forgotten about and this article reminds therapists to address bilateral deficits to more readily help post-op ACLR back to pre-surgical activities.
4 Wellsandt E, Failla MJ, Axe MJ, Snyder-Mackler L. Does Anterior Cruciate Ligament Reconstruction Improve Functional and Radiographic Outcomes Over Nonoperative Management 5 Years After Injury? Am J Sports Med Jul;46(9): Epub 2018 Jun 21. Review Submitted by: Sarah Bosserman, PT, DPT, CSCS Objective: To determine if differences exist for functional and radiographic outcomes 5 years after patients completed an operative and non-operative treatment of ACL injury, given both complete a progressive criterion-based rehabilitation program. Methods: 144 athletes with acute ACL rupture, aged years old, were used for this cohort study. All subjects participated in level 1 (eg. soccer, basketball) or level 2 (eg. tennis, downhill skiing) cutting and pivoting activities before injury. Patients were excluded if significant meniscal, ligamentous tears, or articular cartilage lesions were present concurrently. Patient were categorized as a potential coper or noncoper as part of the surgical decision-making process. Patients self-selected treatment strategies, leading to 83 patients who underwent ACL reconstruction and 22 who completed the non-operative treatment. For the 5 year follow-up, functional testing included quad strength, single-legged hop, knee effusion testing, and completion of patient-reported outcomes (KOS-ADLS, GRS, IKDC, KOOS, TSK-11, ACL-RSI, VAS). Radiographs were also taken of the knee and graded using the Kellgren-Lawrence system. Results: 105 (72.9%) returned for 5-year testing. A greater proportion of patient treated operatively were participating in level 1 cutting and pivoting activities before injury. After controlling for preactivity level, groups did not differ in quad strength (P=.817) or any of the 4 single-legged hop tests (P= ) at 5 years. 44% of those treated operatively demonstrate knee joint effusion at 5 years vs 10% treated non-operatively. Patients treated operatively reported higher scores on the GRS (P=.001) exceeding the MDC. Patients treated non-operatively reported higher levels of fear on the TSK-11 (P=.035), and higher worst pain levels on the VAS (P=.010), but group differences did not meet the MDC of 2.8. No group differences found for remaining outcome measures. Radiographs were completed for 64 operatively treated patients and 20 non-operatively. Tibiofemoral knee joint OA was present in 23.4% treated operatively and 5% treated non-operatively. Conclusions: The findings of this study demonstrate positive functional outcomes can occur following a progressive criterion-based rehabilitation program for both operative and non-operative management following ACL rupture in athletes. Commentary: The discussion in this article focuses on the fact that athletes can return to high levels of activity with both operative and conservative management. The difficulty comes down to determining who would be appropriate for which treatment without further research into reliable clinical algorithms. Positive results for pain and function were found in both groups. However, there were cons with both treatment options, including increased joint effusion and incidence of OA in the operative group versus increased highest pain level and fear in those treated without surgery. In this current study, the operative group was significantly larger, reflecting the current rate of ACL surgeries in the US. Furthermore, participants had minimal concomitant injuries and the mean age was 34.3 ± 11.4 years, making the results less applicable to those with more involved injuries or to high school and college aged athletes involved in level 1 cutting and pivoting activities. Although more research is needed, this study may aide discussion and education between patient and clinician following ACL injury.
5 Modifiable risk factors for patellar tendinopathy in athletes: a systematic review and meta-analysis. Sprague AL, et al. Br J Sports Med 2018;0:1 12. E pub ahead of print. doi: /bjsports Review submitted by: Justin Pretlow, DPT, OCS Objective: To perform a systematic review and meta-analysis identifying (1) potential modifiable risk factors and (2) associated modifiable factors for patellar tendinopathy in athletes. Methods: PubMed, Web of Science, Scopus and Cinahl were searched on Nov. 14, All quantitative original research comparing athletes with patellar tendinopathy with a control group without the injury were considered. Patellar tendinopathy is defined as symptoms isolated to the inferior pole of the patella. The broader definition of jumper s knee, including symptoms in other sites of the patellar tendon were also included. To clarify, prospective studies can identify potential modifiable risk factors, since presence or exposure to the risk factor is determined prior to the development of patellar tendinopathy. At best, items identified in cross-sectional studies can only be considered associated modifiable factors, since a temporal relationship cannot be established. Of the 31 studies considered, 6 were prospective. All six included young athletes, with mean ages under 30. The majority (83%, 5/6) played either volleyball or basketball, and consisted of elite athletes competing at the professional, national or international level (67%, 4/6). Studies were independently assessed for risk of bias and methodological quality by two reviewers using a modified version of the Newcastle-Ottawa Scale (NOS). Results: 862 records were screened and 31 articles were included (6 prospective, 25 cross-sectional). There was a lack of strong evidence for any potential modifiable risk factor or associated factors. There was limited or conflicting evidence that decreased ankle dorsiflexion range of motion, decreased posterior thigh and quadriceps flexibility, greater volume of jump training, more volleyball sets played per week, greater countermovement jump (CMJ) height and greater activity volume are potential modifiable risk factors. Meta-analysis supported greater activity volume (Cohen s d=0.22, 95% CI 0.06 to 0.39, p=0.008), higher body weight (0.36, 0.17 to 0.55, p<0.001) and greater CMJ height (0.31, 0.07 to 0.56, p=0.01) as associated modifiable factors. Conclusions: There is a lack of strong evidence for any potential modifiable risk factors or associated factors. Factors with lower levels of support may be of interest in designing prevention programs but require further research in high-quality, prospective studies. Commentary: The authors point out there were few prospective studies investigating risks factors and none were of high quality. Many of the cross-sectional studies were of low quality, and nearly half failed to control for covariates, which limits the strength of evidence for associated modifiable factors. The authors recognize that the prospective studies included mostly young, male, elite athletes in volleyball and basketball, so the potential modifiable risk factors discussed may not translate well to the general population. The authors highlight that much of the research on risk factors for patellar tendinopathy is weak and/or conflicting. However, the modifiable and associated risk factors listed in the results above do fit the clinical pattern often associated with athletes experiencing patellar tendinopathy. I think we can use these factors as a mental checklist when assessing athletes and when problem-solving with the patient on modifying their routine and prescribing exercise that is more likely to help them return to sport faster, or miss less time due to injury. As with many systematic reviews, the take away is that more high quality evidence looking specifically at modifiable risk factors is needed.
Review Submitted By: Tyler France, PT, DPT, CSCS
 Webster KE, Nagelli CV, Hewett TE, Feller JA. Factors Associated With Psychological Readiness to Return to Sport After Anterior Cruciate Ligament Reconstruction Surgery. Am J Sports Med. 2018;46(7):1545-1550.
Webster KE, Nagelli CV, Hewett TE, Feller JA. Factors Associated With Psychological Readiness to Return to Sport After Anterior Cruciate Ligament Reconstruction Surgery. Am J Sports Med. 2018;46(7):1545-1550.
Theodore Ganley, MD Lawrence Wells, MD J. Todd Lawrence, MD, PhD Anterior Cruciate Ligament Reconstruction Protocol (Revised March 2018)
 Theodore Ganley, MD Lawrence Wells, MD J. Todd Lawrence, MD, PhD Anterior Cruciate Ligament Reconstruction Protocol (Revised March 2018) ***Please refer to written prescription for any special instructions
Theodore Ganley, MD Lawrence Wells, MD J. Todd Lawrence, MD, PhD Anterior Cruciate Ligament Reconstruction Protocol (Revised March 2018) ***Please refer to written prescription for any special instructions
Appendix 2: KNGF Evidence Statement for anterior cruciate ligament reconstruction rehabilitation
 Appendix 2: KNGF Evidence Statement for anterior cruciate ligament reconstruction rehabilitation Inclusion and exclusion criteria for rehabilitation according to the Evidence Statement Inclusion of patients
Appendix 2: KNGF Evidence Statement for anterior cruciate ligament reconstruction rehabilitation Inclusion and exclusion criteria for rehabilitation according to the Evidence Statement Inclusion of patients
ACL Rehabilitation and Return To Play
 ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
Monthly Literature Review
 Monthly Literature Review Perriman A, Leahy E, Semciw AI. The Effect of Open vs Closed Kinetic Chain Exercises on Anterior Tibial Laxity, Strength, and Function Following Anterior Cruciate Ligament Reconstruction:
Monthly Literature Review Perriman A, Leahy E, Semciw AI. The Effect of Open vs Closed Kinetic Chain Exercises on Anterior Tibial Laxity, Strength, and Function Following Anterior Cruciate Ligament Reconstruction:
TREATMENT GUIDELINES FOR GRADE 3 PCL TEAR
 GENERAL CONSIDERATIONS Posterior cruciate ligament (PCL) injuries occur less frequently than anterior cruciate ligament (ACL) injuries, but are much more common than previously thought. The PCL is usually
GENERAL CONSIDERATIONS Posterior cruciate ligament (PCL) injuries occur less frequently than anterior cruciate ligament (ACL) injuries, but are much more common than previously thought. The PCL is usually
OMICS - 3rd Int. Conference & 2
 KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
ACUTE EFFECTS OF DIFFERENT ANTERIOR THIGH SELF-MASSAGE ON HIP RANGE-OF-MOTION IN TRAINED MEN. Monteiro ER. Int J Sports Phys Ther.
 ACUTE EFFECTS OF DIFFERENT ANTERIOR THIGH SELF-MASSAGE ON HIP RANGE-OF-MOTION IN TRAINED MEN. Monteiro ER. Int J Sports Phys Ther. 2018 Feb;13(1):104-113. Review submitted by: Justin Pretlow, PT, DPT,
ACUTE EFFECTS OF DIFFERENT ANTERIOR THIGH SELF-MASSAGE ON HIP RANGE-OF-MOTION IN TRAINED MEN. Monteiro ER. Int J Sports Phys Ther. 2018 Feb;13(1):104-113. Review submitted by: Justin Pretlow, PT, DPT,
What s New in ACL Rehabilitation Criteria to Return to Play. ACL Injuries Introduction. ACL Injuries Return to Play. Carey et al: AJSM 06
 Criteria to Return to Play Kevin E. Wilk, PT, DPT, FAPTA ACL INJURIES Introduction ACL injuries common in sports & strenuous work» So frequent that the seriousness is often forgotten Totally disrupted
Criteria to Return to Play Kevin E. Wilk, PT, DPT, FAPTA ACL INJURIES Introduction ACL injuries common in sports & strenuous work» So frequent that the seriousness is often forgotten Totally disrupted
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION REHABILITATION GUIDELINES
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION REHABILITATION GUIDELINES While there is no consensus on the best accelerated rehabilitation program or which specific surgical techniques result in the most favorable
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION REHABILITATION GUIDELINES While there is no consensus on the best accelerated rehabilitation program or which specific surgical techniques result in the most favorable
4/26/2017. Disclosures. Early rehabilitation following ACLR: are we doing enough? Common impairments after ACLR. Objectives
 Disclosures Early rehabilitation following ACLR: are we doing enough? None Laura Schmitt, PT, PhD Associate Professor of Physical Therapy, School of Health and Rehabilitation Sciences Ohio State University
Disclosures Early rehabilitation following ACLR: are we doing enough? None Laura Schmitt, PT, PhD Associate Professor of Physical Therapy, School of Health and Rehabilitation Sciences Ohio State University
Research Theme. Cal PT Fund Research Symposium 2015 Christopher Powers. Patellofemoral Pain to Pathology Continuum. Applied Movement System Research
 Evaluation and Treatment of Movement Dysfunction: A Biomechanical Approach Research Theme Christopher M. Powers, PhD, PT, FAPTA Understanding injury mechanisms will lead to the development of more effective
Evaluation and Treatment of Movement Dysfunction: A Biomechanical Approach Research Theme Christopher M. Powers, PhD, PT, FAPTA Understanding injury mechanisms will lead to the development of more effective
When are athletes ready for return to sports??? Functional Testing for Return to Sports. Important Factors Involved in Return to Sport
 Functional Testing for Return to Sports Meg Jacobs PT Momentum Physical Therapy and Sports Rehab Mjacobs@wegetyouhealthy.com When are athletes ready for return to sports??? Post ACL reconstruction, average
Functional Testing for Return to Sports Meg Jacobs PT Momentum Physical Therapy and Sports Rehab Mjacobs@wegetyouhealthy.com When are athletes ready for return to sports??? Post ACL reconstruction, average
THE FADING ATHLETE WITH AN OLD KNEE: INVESTIGATION OF FACTORS AND OUTCOMES AFTER ANTERIOR CRUCIATE LIGAMENT INJURY
 THE FADING ATHLETE WITH AN OLD KNEE: INVESTIGATION OF FACTORS AND OUTCOMES AFTER ANTERIOR CRUCIATE LIGAMENT INJURY RELATED TO THE DEVELOPMENT OF KNEE OSTEOARTHRITIS by Elizabeth Wellsandt A dissertation
THE FADING ATHLETE WITH AN OLD KNEE: INVESTIGATION OF FACTORS AND OUTCOMES AFTER ANTERIOR CRUCIATE LIGAMENT INJURY RELATED TO THE DEVELOPMENT OF KNEE OSTEOARTHRITIS by Elizabeth Wellsandt A dissertation
ACLR AND MCL REPAIR CLINICAL PRACTICE GUIDELINE
 ACLR AND MCL REPAIR CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics, and clinician evaluation. Contact Ohio State Sports Medicine
ACLR AND MCL REPAIR CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics, and clinician evaluation. Contact Ohio State Sports Medicine
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol
 Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
Sports Rehabilitation & Performance Center Medial Patellofemoral Ligament Reconstruction Guidelines * Follow physician s modifications as prescribed
 The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
Hurry up and wait: Rehab after ACLR: where are we today
 Hurry up and wait: Rehab after ACLR: where are we today Lynn Snyder Mackler ScD, PT University of Delaware Newark, DE Lynn Snyder-Mackler University of Delaware Disclosure: I DO NOT have a financial relationship
Hurry up and wait: Rehab after ACLR: where are we today Lynn Snyder Mackler ScD, PT University of Delaware Newark, DE Lynn Snyder-Mackler University of Delaware Disclosure: I DO NOT have a financial relationship
AETIOLOGY TENDINOPATHY RESEARCH UPDATE - NOVEMBER Contents
 TENDINOPATHY RESEARCH UPDATE - NOVEMBER 2012 Contents AETIOLOGY... 1 A lower limb assessment tool for athletes at risk of developing patellar tendinopathy.... 1 Triceps surae activation is altered in male
TENDINOPATHY RESEARCH UPDATE - NOVEMBER 2012 Contents AETIOLOGY... 1 A lower limb assessment tool for athletes at risk of developing patellar tendinopathy.... 1 Triceps surae activation is altered in male
Anterior Cruciate Ligament Rehabilitation. Rehab Summit Omni Orlando Resort at ChampionsGate Speaker: Terry Trundle, PTA, ATC, LAT
 Anterior Cruciate Ligament Rehabilitation Rehab Summit Omni Orlando Resort at ChampionsGate Speaker: Terry Trundle, PTA, ATC, LAT ACL Graft Selection 1. Autograft Bone-Patella Tendon Bone Hamstrings: Semitendinosus
Anterior Cruciate Ligament Rehabilitation Rehab Summit Omni Orlando Resort at ChampionsGate Speaker: Terry Trundle, PTA, ATC, LAT ACL Graft Selection 1. Autograft Bone-Patella Tendon Bone Hamstrings: Semitendinosus
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
Mechanisms of ACL Injury: Implications for Rehabilitation, Injury Prevention & Return to Sport Decisions. Overarching research theme:
 Mechanisms of ACL Injury: Implications for Rehabilitation, Injury Prevention & Return to Sport Decisions Associate Professor Co Director, Musculoskeletal Biomechanics Research Laboratory University of
Mechanisms of ACL Injury: Implications for Rehabilitation, Injury Prevention & Return to Sport Decisions Associate Professor Co Director, Musculoskeletal Biomechanics Research Laboratory University of
Baseline Time to Stabilization Identifies Anterior Cruciate Ligament Rupture Risk in Collegiate Athletes
 Sean Baseline Time to Stabilization Identifies Anterior Cruciate Ligament Rupture Risk in Collegiate Athletes Kevin M. DuPrey,* y DO, Kathy Liu,z PhD, Peter F. Cronholm, MD, Andrew S. Reisman,{ MD, Steven
Sean Baseline Time to Stabilization Identifies Anterior Cruciate Ligament Rupture Risk in Collegiate Athletes Kevin M. DuPrey,* y DO, Kathy Liu,z PhD, Peter F. Cronholm, MD, Andrew S. Reisman,{ MD, Steven
The Effectiveness of Injury-Prevention Programs in Reducing the Incidence of Anterior Cruciate Ligament Sprains in Adolescent Athletes
 Critically Appraised Topics Journal of Sport Rehabilitation, 2012, 21, 371-377 2012 Human Kinetics, Inc. The Effectiveness of Injury-Prevention Programs in Reducing the Incidence of Anterior Cruciate Ligament
Critically Appraised Topics Journal of Sport Rehabilitation, 2012, 21, 371-377 2012 Human Kinetics, Inc. The Effectiveness of Injury-Prevention Programs in Reducing the Incidence of Anterior Cruciate Ligament
Current trends in ACL Rehab. James Kelley, MDS, PT
 Current trends in ACL Rehab James Kelley, MDS, PT Objectives Provide etiological information Discuss the criteria for having an ACL reconstruction Review the basic rehabilitation principles behind ACL
Current trends in ACL Rehab James Kelley, MDS, PT Objectives Provide etiological information Discuss the criteria for having an ACL reconstruction Review the basic rehabilitation principles behind ACL
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
Rehabilitation of Hip Labral Tears and Femoroacetabular Impingement
 Rehabilitation of Hip Labral Tears and Femoroacetabular Impingement Michael Newsome PT, OCS, SCS, CSCS Hip injuries account for 3.1% of all injuries in the NFL from 1997-2006 (Feeley 2008) 59% strains
Rehabilitation of Hip Labral Tears and Femoroacetabular Impingement Michael Newsome PT, OCS, SCS, CSCS Hip injuries account for 3.1% of all injuries in the NFL from 1997-2006 (Feeley 2008) 59% strains
Stephanie Gould Pht, Naudira Stewart P.R.T. i000
 Return to Sport After ACL in the Young Athlete Stephanie Gould Pht, Naudira Stewart P.R.T i000 The ACL epidemic In youth aged 6-18 y.o., ACL injuries occur at a rate of 130/100,000 people per year Rate
Return to Sport After ACL in the Young Athlete Stephanie Gould Pht, Naudira Stewart P.R.T i000 The ACL epidemic In youth aged 6-18 y.o., ACL injuries occur at a rate of 130/100,000 people per year Rate
ACL and Knee Injury Prevention. Presented by: Zach Kirkpatrick, PT, MPT, SCS
 ACL and Knee Injury Prevention Presented by: Zach Kirkpatrick, PT, MPT, SCS ACL Anatomy ACL Mechanism of Injury Contact ACL Tear Noncontact ACL Tear ACL MOI and Pathology Common in young individual who
ACL and Knee Injury Prevention Presented by: Zach Kirkpatrick, PT, MPT, SCS ACL Anatomy ACL Mechanism of Injury Contact ACL Tear Noncontact ACL Tear ACL MOI and Pathology Common in young individual who
ACL Rehabilitation Guidelines
 ACL Rehabilitation Guidelines General Information: These guidelines have been developed to service the spectrum of ACL injured people (non-athlete elite athlete). For this reason, example exercises are
ACL Rehabilitation Guidelines General Information: These guidelines have been developed to service the spectrum of ACL injured people (non-athlete elite athlete). For this reason, example exercises are
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION
 ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol
 REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement. Normalize gait pattern with brace (if indicated) and crutches
 General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
CLINICAL PROTOCOL FOR ACHILLES TENDON ALLOGRAFT PCL RECONSTRUCTION REHABILITATION
 CLINICAL PROTOCOL FOR ACHILLES TENDON ALLOGRAFT PCL RECONSTRUCTION REHABILITATION FREQUENCY: 2-3 times per week. DURATION: Average estimate of formal treatment is 2-3 times per week X 2-3 months based
CLINICAL PROTOCOL FOR ACHILLES TENDON ALLOGRAFT PCL RECONSTRUCTION REHABILITATION FREQUENCY: 2-3 times per week. DURATION: Average estimate of formal treatment is 2-3 times per week X 2-3 months based
Post Injury / Pre Screening Rehabilitation. Implementation of Screening Procedure. Single Leg Hop Series
 Post Injury / Pre Screening Rehabilitation Resolve Joint Effusion -RICE, Massage, possible draining by MD Restore Full Passive Knee Motion -Patellar Mobilizations, Wall Slides, CPM, Bike, Prone hangs Hop
Post Injury / Pre Screening Rehabilitation Resolve Joint Effusion -RICE, Massage, possible draining by MD Restore Full Passive Knee Motion -Patellar Mobilizations, Wall Slides, CPM, Bike, Prone hangs Hop
ACLR Protocol Hamstring Autograft. Name Date. Procedure. Frequency times/week Duration weeks
 Anthony Levenda M.D. Sports Medicine, Shoulder & Knee Reconstruction Direct Line (219) 395-2109 ACLR Protocol Hamstring Autograft Name Date Procedure Procedure Date Frequency 1 2 3 4 5 times/week Duration
Anthony Levenda M.D. Sports Medicine, Shoulder & Knee Reconstruction Direct Line (219) 395-2109 ACLR Protocol Hamstring Autograft Name Date Procedure Procedure Date Frequency 1 2 3 4 5 times/week Duration
Knee Multiligament Rehabilitation
 Knee Multiligament Rehabilitation Orlando Valle, PT, MSPT, SCS, CSCS Director Ironman Sports Medicine Institute TMC Orlando.Valle@memorialhermann.org 4 Major Ligaments ACL PCL MCL LCL (PLC) Anatomy Function
Knee Multiligament Rehabilitation Orlando Valle, PT, MSPT, SCS, CSCS Director Ironman Sports Medicine Institute TMC Orlando.Valle@memorialhermann.org 4 Major Ligaments ACL PCL MCL LCL (PLC) Anatomy Function
ACL Rehabilitation and Return to Play Guidelines: An Evidence Based Approach
 ACL Rehabilitation and Return to Play Guidelines: An Evidence Based Approach Terry L. Grindstaff, PhD, PT, ATC @GrindstaffTL Summary ACL injury has short and long-term consequences Return to prior level
ACL Rehabilitation and Return to Play Guidelines: An Evidence Based Approach Terry L. Grindstaff, PhD, PT, ATC @GrindstaffTL Summary ACL injury has short and long-term consequences Return to prior level
GOALS. Full knee extension ROM Good quadriceps control (> 20 no lag SLR) Minimize pain Minimize swelling Normal gait pattern
 Hamstring ACL Rehabilitation Guidelines David R. McAllister, MD UCLA Department of Orthoapeadic Surgery Sports Medicine Service (310)206-5250 FAX (310) 825-1311 General Information: The following ACL rehabilitation
Hamstring ACL Rehabilitation Guidelines David R. McAllister, MD UCLA Department of Orthoapeadic Surgery Sports Medicine Service (310)206-5250 FAX (310) 825-1311 General Information: The following ACL rehabilitation
MOON ACL Rehabilitation Guidelines
 MOON ACL Rehabilitation Guidelines M.o.o.n.Team Members General Information: The following ACL rehabilitation guidelines are based on a review of the randomized controlled trials related to ACL rehabilitation.
MOON ACL Rehabilitation Guidelines M.o.o.n.Team Members General Information: The following ACL rehabilitation guidelines are based on a review of the randomized controlled trials related to ACL rehabilitation.
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
6/30/2015. Quadriceps Strength is Associated with Self-Reported Function in Arthroscopic Partial Meniscectomy Patients. Surgical Management
 Quadriceps Strength is Associated with Self-Reported Function in Arthroscopic Partial Meniscectomy Patients Meniscal tears no cause for concern? Among the most common injuries of the knee in sport and
Quadriceps Strength is Associated with Self-Reported Function in Arthroscopic Partial Meniscectomy Patients Meniscal tears no cause for concern? Among the most common injuries of the knee in sport and
MENISCAL REPAIR WITH WEIGHT RESTRICTIONS CLINICAL PRACTICE GUIDELINES
 MENISCAL REPAIR WITH WEIGHT RESTRICTIONS CLINICAL PRACTICE GUIDELINES Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio
MENISCAL REPAIR WITH WEIGHT RESTRICTIONS CLINICAL PRACTICE GUIDELINES Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio
Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer. Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Knee Movement Coordination Deficits. ICD-9-CM: Sprain of cruciate ligament of knee
 1 Knee Movement Coordination Deficits Anterior Cruciate Ligament ACL Tear ICD-9-CM: 844.2 Sprain of cruciate ligament of knee ACL Insufficiency ICD-9-CM: 717.83 Old disruption of anterior cruciate ligament
1 Knee Movement Coordination Deficits Anterior Cruciate Ligament ACL Tear ICD-9-CM: 844.2 Sprain of cruciate ligament of knee ACL Insufficiency ICD-9-CM: 717.83 Old disruption of anterior cruciate ligament
Personalized Blood Flow Restriction Rehabilitation. Knee Arthroscopy. (Debridements, Meniscectomies, Synovectomy, Chondroplasty)
 Personalized Blood Flow Restriction Rehabilitation Knee Arthroscopy (Debridements, Meniscectomies, Synovectomy, Chondroplasty) Knee Arthroscopy 2 The primary goals after knee arthroscopy debridement is
Personalized Blood Flow Restriction Rehabilitation Knee Arthroscopy (Debridements, Meniscectomies, Synovectomy, Chondroplasty) Knee Arthroscopy 2 The primary goals after knee arthroscopy debridement is
Symmetric or Sufficient for Return-to-Sport after ACL Injury? Science Meets Practice Session APTA Combined Sections Meeting 2018
 Symmetric or Sufficient for Return-to-Sport after ACL Injury? Science Meets Practice Session APTA Combined Sections Meeting 2018 Matthew Ithurburn, PT, PhD, DPT, OCS University of Alabama at Birmingham,
Symmetric or Sufficient for Return-to-Sport after ACL Injury? Science Meets Practice Session APTA Combined Sections Meeting 2018 Matthew Ithurburn, PT, PhD, DPT, OCS University of Alabama at Birmingham,
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Algorithm #1 Lumbo-Pelvic Region Examination
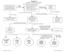 Red Screen for Potentially Serious Conditions (i.e., Red Flags) including Neurologic when indicated Positive Findings Algorithm #1 Lumbo-Pelvic Region Clinical Prediction Rule Screening: Duration of symptoms
Red Screen for Potentially Serious Conditions (i.e., Red Flags) including Neurologic when indicated Positive Findings Algorithm #1 Lumbo-Pelvic Region Clinical Prediction Rule Screening: Duration of symptoms
Anterior Cruciate Ligament (ACL) Reconstruction Protocol. Hamstring Autograft, Allograft, or Revision
 Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft
 Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
REHABILITATION AND RETURN TO SPORTS AFTER ACL RECONSTRUCTION
 REHABILITATION AND RETURN TO SPORTS AFTER ACL RECONSTRUCTION Written by Giovanni Milandri and Willem Mare van der Merwe, South Africa Rehabilitation after anterior cruciate ligament injury remains long
REHABILITATION AND RETURN TO SPORTS AFTER ACL RECONSTRUCTION Written by Giovanni Milandri and Willem Mare van der Merwe, South Africa Rehabilitation after anterior cruciate ligament injury remains long
Preventing Joint Injury & Subsequent Osteoarthritis:
 Preventing Joint Injury & Subsequent Osteoarthritis: A Population Health Prospective Carolyn Emery PT, PhD Public Health Burden of Injury in Alberta The leading cause of death and hospitalization in youth
Preventing Joint Injury & Subsequent Osteoarthritis: A Population Health Prospective Carolyn Emery PT, PhD Public Health Burden of Injury in Alberta The leading cause of death and hospitalization in youth
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
Precautions following Hip Arthroscopy/FAI: (Refixation/Osteochondroplasty)
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION WITH MICROFRACTURE OR CARTIFORM/BIOCARTILAGE (TROCHLEA OR PATELLA)
 Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION PHASE I (0-3 WEEKS) Appointments Begin physical therapy 2-5 days post op
Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION PHASE I (0-3 WEEKS) Appointments Begin physical therapy 2-5 days post op
ACL Reconstruction Rehabilitation Protocol
 ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
Due to differing clinical
 Ingrid Eitzen, PT, PhD1 Håvard Moksnes, PT, MSc2 Lynn Snyder-Mackler, PT, ScD3 May Arna Risberg, PT, PhD 4 A Progressive 5-Week Exercise Therapy Program Leads to Significant Improvement in Knee Function
Ingrid Eitzen, PT, PhD1 Håvard Moksnes, PT, MSc2 Lynn Snyder-Mackler, PT, ScD3 May Arna Risberg, PT, PhD 4 A Progressive 5-Week Exercise Therapy Program Leads to Significant Improvement in Knee Function
Proximal Hamstring Rupture: Physical Therapy Protocol
 Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
ACL RECONSTRUCTION SPORTS REHABILITATION. Written by Bart Sas, Qatar
 ACL RECONSTRUCTION PREDICTORS AND PROGNOSIS OF OUTCOME POST RECONSTRUCTION Written by Bart Sas, Qatar Injury to the anterior cruciate ligament (ACL) is arguably the most devastating injury that an athlete
ACL RECONSTRUCTION PREDICTORS AND PROGNOSIS OF OUTCOME POST RECONSTRUCTION Written by Bart Sas, Qatar Injury to the anterior cruciate ligament (ACL) is arguably the most devastating injury that an athlete
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
Sports Rehabilitation & Performance Center Rehabilitation Guidelines for Non-operative Treatment of Patellofemoral Instability *
 Sports Rehabilitation & Performance Center Rehabilitation Guidelines for Non-operative Treatment of The following guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital
Sports Rehabilitation & Performance Center Rehabilitation Guidelines for Non-operative Treatment of The following guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital
4/21/2017. Outline. Quadriceps inhibition post-acl injury. Stephanie Di Stasi, PT, PhD, OCS
 Stephanie Di Stasi, PT, PhD, OCS Research Scientist, Sports Medicine Research Institute Assistant Professor, Department of Orthopaedics Outline Discuss the evidence for quadriceps activation deficits and
Stephanie Di Stasi, PT, PhD, OCS Research Scientist, Sports Medicine Research Institute Assistant Professor, Department of Orthopaedics Outline Discuss the evidence for quadriceps activation deficits and
Anterior Cruciate Ligament Reconstruction Standard Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Standard Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction
Anterior Cruciate Ligament Reconstruction Standard Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction
During the initial repair and inflammatory phase, focus should be on placing the lower limbs in a position to ensure that:
 The Anatomy Dimensions series of tutorials and workbooks is aimed at improving anatomical and pathological understanding for body movement professionals. It is ideal for teachers in disciplines such as
The Anatomy Dimensions series of tutorials and workbooks is aimed at improving anatomical and pathological understanding for body movement professionals. It is ideal for teachers in disciplines such as
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
ORTHOPEDIC SURGERY, SPORTS MEDICINE, AND ARTHROSCOPY
 WWW.MATTDRISCOLLMD.COM ORTHOPEDIC SURGERY, SPORTS MEDICINE, AND ARTHROSCOPY ACL Reconstruction Rehab Protocol The intent of this protocol is to provide a general framework for ACL rehabilitation. Within
WWW.MATTDRISCOLLMD.COM ORTHOPEDIC SURGERY, SPORTS MEDICINE, AND ARTHROSCOPY ACL Reconstruction Rehab Protocol The intent of this protocol is to provide a general framework for ACL rehabilitation. Within
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION
 REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
Bryan T. Kelly, MD Center for Hip Pain and Preservation Hospital for Special Surgery
 Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Re training Movement Behavior for ACL Injury Prevention and Rehabilitation: A Matter of Strength or Motor Control?
 Re training Movement Behavior for ACL Injury Prevention and Rehabilitation: A Matter of Strength or Motor Control? Christopher M. Powers, PT, PhD, FACSM, FAPTA Beth Fisher, PT, PhD, FAPTA Division of Biokinesiology
Re training Movement Behavior for ACL Injury Prevention and Rehabilitation: A Matter of Strength or Motor Control? Christopher M. Powers, PT, PhD, FACSM, FAPTA Beth Fisher, PT, PhD, FAPTA Division of Biokinesiology
Post Operative Knee Rehab: Return to Play after ACLR
 Post Operative Knee Rehab: Return to Play after ACLR Fall Session 2016 Mary Lloyd Ireland, M.D. Associate Professor University of Kentucky Dept. of Orthopaedic Surgery & Sports Medicine, Lexington, KY
Post Operative Knee Rehab: Return to Play after ACLR Fall Session 2016 Mary Lloyd Ireland, M.D. Associate Professor University of Kentucky Dept. of Orthopaedic Surgery & Sports Medicine, Lexington, KY
Review Submitted by: Scott Resetar, PT, DPT
 Abourezk MN, Ithurburn MP, Mcnally MP, et al. Hamstring Strength Asymmetry at 3 Years After Anterior Cruciate Ligament Reconstruction Alters Knee Mechanics During Gait and Jogging. Am J Sports Med. 2017;45(1):97-105.
Abourezk MN, Ithurburn MP, Mcnally MP, et al. Hamstring Strength Asymmetry at 3 Years After Anterior Cruciate Ligament Reconstruction Alters Knee Mechanics During Gait and Jogging. Am J Sports Med. 2017;45(1):97-105.
ACL Rehabilitation Guidelines
 ACL Rehabilitation Guidelines Phase 0: Pre-operative Recommendations Normal gait AROM 0 to 120 degrees of flexion Strength: 20 SLR with no lag Minimal effusion Patient education on post-operative exercises
ACL Rehabilitation Guidelines Phase 0: Pre-operative Recommendations Normal gait AROM 0 to 120 degrees of flexion Strength: 20 SLR with no lag Minimal effusion Patient education on post-operative exercises
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
REHABILITATION GUIDELINES AFTER ACL RECONSTRUCTION. Shail Vyas, MD Orange County Orthopaedic Group (714)
 REHABILITATION GUIDELINES AFTER ACL RECONSTRUCTION Shail Vyas, MD Orange County Orthopaedic Group (714) 974-0100 The intent of this protocol is to provide the therapist with guidelines of the post-operative
REHABILITATION GUIDELINES AFTER ACL RECONSTRUCTION Shail Vyas, MD Orange County Orthopaedic Group (714) 974-0100 The intent of this protocol is to provide the therapist with guidelines of the post-operative
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
AAP Boot Camp KNEE AND ANKLE EXAM
 AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
Does the use of an Isokinetic Strengthening Programme improve outcomes in adults following unilateral ACL Reconstruction versus usual rehabilitation?
 Specific Question: Does the use of an Strengthening Programme improve outcomes in adults following unilateral ACL Reconstruction versus usual? Clinical bottom line There is no high quality evidence to
Specific Question: Does the use of an Strengthening Programme improve outcomes in adults following unilateral ACL Reconstruction versus usual? Clinical bottom line There is no high quality evidence to
The Female Athlete: Train Like a Girl. Sarah DoBroka Wilson, PT, SCS Ron Weathers, PT, DPT, ATC, LAT
 The Female Athlete: Train Like a Girl Sarah DoBroka Wilson, PT, SCS Ron Weathers, PT, DPT, ATC, LAT Page 1 of 6 The Female Athlete: Train Like a Girl Sarah DoBroka Wilson PT, SCS Ron Weathers PT, DPT,
The Female Athlete: Train Like a Girl Sarah DoBroka Wilson, PT, SCS Ron Weathers, PT, DPT, ATC, LAT Page 1 of 6 The Female Athlete: Train Like a Girl Sarah DoBroka Wilson PT, SCS Ron Weathers PT, DPT,
l. Initiate early proprioceptive activity and progress by means of distraction techniques: i. eyes open to eyes closed ii. stable to unstable m.
 Meniscus Repair 1. Defined a. Sutures or bioabsorbable fixation devices (arrows, darts, screws, etc.) bring together and fixate the edges of a tear in the meniscus in order to maintain the shock absorption
Meniscus Repair 1. Defined a. Sutures or bioabsorbable fixation devices (arrows, darts, screws, etc.) bring together and fixate the edges of a tear in the meniscus in order to maintain the shock absorption
Personalized Blood Flow Restriction Rehabilitation. Anterior Cruciate Reconstruction with Meniscal Repair
 Personalized Blood Flow Restriction Rehabilitation Anterior Cruciate Reconstruction with Meniscal Repair ACL with Meniscus Repair 2 PHASE 1 (PROTECTED PHASE) Typically, after an anterior cruciate reconstruction
Personalized Blood Flow Restriction Rehabilitation Anterior Cruciate Reconstruction with Meniscal Repair ACL with Meniscus Repair 2 PHASE 1 (PROTECTED PHASE) Typically, after an anterior cruciate reconstruction
7/23/2018. Disclosures. Outline. No disclosures
 Disclosures No disclosures Outline Epidemiology Anatomy Skeletal Maturity Alignment Growth Arrest Basic Science Non-operative Treatment Operative Treatment Techniques New Technology on the Horizon 1 Reasons
Disclosures No disclosures Outline Epidemiology Anatomy Skeletal Maturity Alignment Growth Arrest Basic Science Non-operative Treatment Operative Treatment Techniques New Technology on the Horizon 1 Reasons
REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION WITH MICROFRACTURE OR CARTIFORM/BIOCARTILAGE (FEMORAL CONDYLE OR TIBIAL PLATEAU)
 Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION WITH MICROFRACTURE OR CARTIFORM/BIOCARTILAGE (FEMORAL CONDYLE OR TIBIAL
Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION WITH MICROFRACTURE OR CARTIFORM/BIOCARTILAGE (FEMORAL CONDYLE OR TIBIAL
Patellar Tendon Repair Rehabilitation Guideline
 Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Anterior Cruciate Ligament (ACL) Reconstruction Protocol
 Christopher M. Larson, MD Anterior Cruciate Ligament (ACL) Reconstruction Protocol **Please see the IMPORTANT NOTE for STRETCHING / KNEE EXTENSION on page 5** The intent of this protocol is to provide
Christopher M. Larson, MD Anterior Cruciate Ligament (ACL) Reconstruction Protocol **Please see the IMPORTANT NOTE for STRETCHING / KNEE EXTENSION on page 5** The intent of this protocol is to provide
OBJECTIVES HARNESSING TECHNOLOGY IN THE CLINICAL SETTING OBJECTIVES OBJECTIVES
 OBJECTIVES HARNESSING TECHNOLOGY IN THE CLINICAL SETTING WPTA CONFERENCE OCTOBER 4-5, 2018 The purpose of this course is to show the benefits of utilizing technology in the clinical setting and also demonstrate
OBJECTIVES HARNESSING TECHNOLOGY IN THE CLINICAL SETTING WPTA CONFERENCE OCTOBER 4-5, 2018 The purpose of this course is to show the benefits of utilizing technology in the clinical setting and also demonstrate
Meniscus Repair Rehabilitation Protocol
 Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
Alejandro Verdugo m.d.
 Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
