Abstract Study Design Retrospective study. Kazunori Hayashi 1 Akira Matsumura 1 Sadahiko Konishi 1 Minori Kato 1 Takashi Namikawa 1 Hiroaki Nakamura 2
|
|
|
- Sharyl Nichols
- 5 years ago
- Views:
Transcription
1 THIEME GLOBAL SPINE JOURNAL Original Article 665 Clinical Outcomes of Posterior Lumbar Interbody Fusion for Patients 80 Years of Age and Older with Lumbar Degenerative Disease: Minimum 2Years Follow-Up Kazunori Hayashi 1 Akira Matsumura 1 Sadahiko Konishi 1 Minori Kato 1 Takashi Namikawa 1 Hiroaki Nakamura 2 1 Department of Orthopedic Surgery, Osaka City General Hospital, Osaka, Japan 2 Department of Orthopedic Surgery, Osaka City Graduate School of Medicine, Osaka, Japan Address for correspondence Akira Matsumura, MD, PhD, Miyakojimahondori, Miyakojima-Ku, , Osaka, Japan ( amatsumura@med.osaka-cu.ac.jp). Global Spine J 2016;6: Abstract Study Design Retrospective study. Objective To compare clinical outcomes, radiographic evaluations including bony union rate and incidence of osteoporotic vertebral fractures (OVFxs), and perioperative complications following posterior lumbar interbody fusion (PLIF) between patients 80 years of age and those <80 years. Methods Ninety-six patients 70 years old who underwent PLIF were reviewed. We divided the patients into the two age groups, 80 group (n ¼ 19) and <80 group (n ¼ 77), and compared the clinical outcomes using Japanese Orthopaedics Association (JOA) scores and the Short-Form Health Survey (SF-36). We also evaluated bony union and the incidence of OVFxs in the both groups. Results The JOA score improved 47.6% in the 80 group and 49.1% in the <80 group. There were no significant differences between the two groups. Only the bodily pain component of the SF-36 improved significantly in the 80 group, and seven of eight Keywords posterior lumbar interbody fusion 80 years of age lumbar degenerative disease clinical outcome osteoporotic vertebral fracture components (exception was general health) improved significantly in the <80 group. Bony union rate was significantly superior in the <80 group (94.8%) compared with that of the 80 group (73.7%, p ¼ 0.013). OVFx prevalence and incidence were not significantly different between the two groups, although postoperative OVFx worsened the JOA score improvement in the 80 group (38.8%, p ¼ 0.02). Conclusions The present study indicated that surgical outcomes of PLIF in patients 80 years were comparable to those < 80 years. However, bony union rate was significantly lower and postoperative OVFx worsened the clinical outcomes in patients 80 years. received September 25, 2015 accepted after revision January 11, 2016 published online February 19, 2016 DOI /s ISSN Georg Thieme Verlag KG Stuttgart New York
2 666 Clinical Outcomes of PLIF for Patients 80 Years Hayashi et al. Introduction Posterior lumbar interbody fusion (PLIF), which was first described by Cloward, 1 has been indicated for the patients who have neurologic claudication and segmental spinal instability. Several authors have already reported that PLIF and other lumbar interbody arthrodesis can provide good surgical outcomes. 2 4 However, to our knowledge, there is little written on these procedures for patients in the eighth and ninth decades of life, despite the fact that the application of lumbar arthrodesis for lumbar degenerative disease in elderly patients has become substantially more widespread over the past decade due to the lengthening life expectancy. 5,6 One of the concerns about surgical interventions in elderly patients is the potential risk associated with their comorbidities and osteoporosis. Severe comorbidities may lead to several perioperative complications, and osteoporosis would impact the bony union and incidence of osteoporotic vertebral fractures (OVFxs) during follow-up. Also, alleviation of their neurologic symptoms with PLIF does not always lead to maintenance or improvement in the patient s quality of life. Spinal surgeons are therefore in a quandary about whether decompression with or without fusion is better for elderly patients. It is important to study the surgical outcomes and complications following PLIF in patients 80 years of age. The purpose of this study was to compare clinical outcomes, radiographic evaluations including bony union rate and incidence of OVFxs, and perioperative complications following PLIF between patients 80 years of age and those <80 years. We hypothesized that clinical outcomes and complications of PLIF would be comparable in patients 80 years of age and those <80 years; on the other hand, the bony union rate might be lower and the incidence of OVFxs higher in the 80 years of age group, and the OVFx incidence could influence the clinical outcomes in both age groups. Materials and Methods Patient Population A total of 105 patients who were >70 years of age and who underwent PLIF for lumbar degenerative disease at our institution from 2008 to 2011 were reviewed. Informed consent was obtained from all participants, and the institutional review board at the Osaka City Graduate School of Medicine approved this study (approval number: 3170). Therefore, this study was performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. Ninety-six of the 105 patients were followed for a minimum of 2 years and were evaluated radiographically and clinically. These 96 patients were enrolled in this study, and the follow-up rate was 91.4%. We divided the patients into two groups according to age: those 80 years of age (80 group: n ¼ 19; mean age 82.2 years, range 80 to 91 years) and those < 80 years of age (<80 group: n ¼ 77; mean age 74.6 years, range 70 to 79 years). Of the 96 patients, there were 65 women and 31 men, with no significant difference between the two age groups. The mean follow-up of the two groups was 39.0 months (24 to 62 months) in the 80 group and 41.9 months (24 to 74 months) in the <80 group. The mean numbers of fused levels were 1.42 and 1.29, respectively. In the 80 group, the number of fused cases in L2 L3, L3 L4, L4 L5, L5 L6, L5 S1 was 2, 22, 57, 2, 16 cases, and in the <80 group, 2, 8, 13, 1, 3 cases, respectively. Seven patients in the 80 group (37%) had a history of previous decompression at the fusion levels. This rate was higher than that of the <80 group (12 cases, 16%). There was no significant difference between the two groups in patient demographics, which are summarized in Table 1. The number of lumbar disease diagnoses in the two groups was quite similar ( Table 2). Surgical Indications of PLIF We performed PLIF in patients who complained of leg pain, neurogenic claudication, and low back pain due to the spinal canal stenosis with segmental spinal instability or spondylolisthesis or degenerative lumbar scoliosis. All patients underwent Table 1 Patients demographics of the two groups 80 group (n ¼ 19) <80 group (n ¼ 77) p Value Mean age, 82.2 (80 91) 74.6 (70 79) y(range) Gender 9: 10 22: (male: female) Follow-up period, 39.0 (24 62) 41. (24 74) 0.47 mo (range) Number of fused 1.42 (1 2) 1.29 (1 3) 0.31 levels (range) Fused area 0.39 (cases) L2 L3 2 2 L3 L L4 L L5 L6 2 1 L5 S BMI (kg/m 2 ) Smoking Alcohol a 1 7 >0.99 Diabetics Hemodialysis Abbreviation:BMI,bodymassindex. a Patients who intake alcohol twice as much as the standard drink per day, which is equal to over 180 ml intake of Japanese sake. Table 2 Diagnosis of lumbar degenerative disease in the two groups 80 group (n ¼ 19) <80 group (n ¼ 77) p Value Spinal stenosis 3 13 >0.99 Spondylolisthesis 9 40 >0.99 Degenerative scoliosis
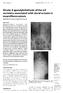
3 Clinical Outcomes of PLIF for Patients 80 Years Hayashi et al. 667 Fig. 1 A 76-year-old man treated with a L4 L5 posterior lumbar interbody fusion for spondylolisthesis. (a) X-ray, anteroposterior view, taken postoperatively. (b) X-ray, lateral view, taken postoperatively. (c) Computed tomography, axial view, at fused level; two box cages were placed with local bone graft. PLIF using pedicle screw and rod system ( Fig. 1). Two open box cages were placed with morselized local bone graft into the disk space. The indications for PLIF were the following: 1. Segmental spinal instability shown in the bending films; segmental kyphosis of more than 5 degrees or anterior translation was more than 3 mm 2. Grade 2 spondylolisthesis in the Meyerding grading system 7 3. Segmental scoliotic disk wedging angle more than 5 degrees or lateral slip more than 3 mm in standing anteroposterior X-ray. 4. Cobb angle more than 20 degrees in standing anteroposterior X-ray Exclusion Criteria We excluded the patients who met the following conditions: 1. Prevalent OVFxs at the fusion levels 2. Previous fusion surgery at the fusion level 3. Any previous OVFx in the thoracic or lumbar spine that met the grade 2 or in semiquantitative (SQ) technique 8 Clinical Outcomes We evaluated clinical outcomes with the Japanese Orthopaedics Association (JOA) score for low back pain and the health-related quality of life (HRQOL) with the Short Form- 36 Health Survey (SF-36) Japanese edition, before surgery and at the latest follow-up. 9 The maximum JOA score is 29 points, based on three subjective symptoms, three clinical signs, activities of daily living, and bladder dysfunction ( Table 3). Improvement of the JOA score was calculated using the formula demonstrated by Hirabayashi et al. 10 The SF-36 has eight health components that were analyzed: physical functioning; role physical; bodily pain (BP); general health (GH); viability; social functioning; role emotional (RE); mental health (MH). 9 Surgical data, including operation time and estimated blood loss, was also evaluated. Radiographic Evaluations Bony union was assessed using the criteria described by Rothman and Glenn on multiplanar reconstruction computed tomography images, and the prevalence of OVFxs were investigated with standing plain X-rays. 11 OVFx was also evaluated with the SQ grading technique proposed by Genant and colleagues, and we defined OVFx as matching SQ grade 2 or 3 in this study. 8 Bony union was evaluated 2 years after surgery, and OVFx was investigated before surgery and 2 years after surgery. Complications The perioperative complications were investigated using the medical charts in each group. The medical complications, including anemia and cardiopulmonary, gastrointestinal, or urinary tract adverse effects during the perioperative period, and reduction of their own comorbidity were evaluated. Additionally, surgery-specific complications were evaluated including dural tear, hematoma, neurologic deficits, infection, implant failure, nonunion, and adjacent segmental degeneration. We classified these events into minor or major complications according to the modified World Health Organization Recommendations for Grading of Acute and Subacute Toxic Effects. 6,12 Blood infusion, additional antibiotics, treatment by another department, revision surgery, and additional surgery associated with any complications were classified as major complications. Statistical Analysis Statistics were analyzed using the paired t test and Fisher exact test. Probability values < 0.05 were considered statistically significant.
4 668 Clinical Outcomes of PLIF for Patients 80 Years Hayashi et al. Table 3 JOA score for low back pain Domain Item Score Subjective Low back pain (3 points) None 3 symptoms Occasional mild pain 2 Frequent mild or occasional severe pain 1 Continuous severe pain 0 Leg pain and/or tingling (3 points) None 3 Occasional mild symptoms 2 Frequent mild or occasional severe symptoms 1 Continuous severe symptoms 0 Gait (3 points) Normal 3 Able to walk farther than 500m although 2 results in pain, tingling, and/or muscle weakness Unable to walk farther than 500m, results in pain, 1 tingling, and/or muscle weakness Unable to walk farther than 100m, results in pain, 0 tingling, and/or muscle weakness Objective Straight leg raising test (2 points) Normal 2 symptoms degrees 1 Less than 30 degrees 0 Sensory abnormality (2 points) Normal 2 Mild disturbance (not subjective) 1 Marked disturbance 0 Motor disturbance (MMT) (2 points) Normal (grade 5) 2 Slight weakness (grade 4) 1 Marked weakness (grade 3 0) 0 Restriction of ADL (14 points) Turning over while lying Standing Washing No restriction 2 Leaning forward Moderate restriction 1 Sitting (about 1 h) Severe restriction 0 Lifting or holding heavy objects Walking Urinary bladder Normal 0 function ( 6 points) Mild dysuria 3 Severe dysuria 6 Total score 29 Abbreviation: ADL, activities of daily living; JOA, Japanese Orthopaedics Association; MMT, manual muscle testing. Results Operation Data and Clinical Outcomes The mean operative time was 274 minutes in both groups. The mean blood loss was estimated to be 411 g in the 80 group and 409 g in the <80 group. There was no significant difference between the two groups ( Table 4). The mean JOA score for the 80 group was 9.3 before surgery and improved to 18.7 at the latest follow-up. The mean JOA score in the <80 group was 10.4 before surgery and improved to 19.5 at the latest follow-up. The JOA score improvement rates were 47.6 and 49.1%, respectively ( Table 4). There was no significant difference between the two groups (p ¼ 0.98). The SF-36 evaluation revealed no significant differences between the two groups for all components before surgery. Only the BP component improved significantly in the 80 group. In contrast, 7 of the 8 components (the exception was GH) improved significantly at the
5 Clinical Outcomes of PLIF for Patients 80 Years Hayashi et al. 669 Table 4 Operation data and evaluation of the JOA score of the two group Operation data Operation time (min) (range: ) 80 group (n ¼ 19) <80 group (n ¼ 77) p Value EBL (g) (range: 20 1,600) JOA score Preoperative (range: 0 20) FFU (range: 5 28) Improvement rate (%) (range: 5 95) Additional surgery a 1 4 >0.99 Abbreviations: EBL, estimated blood loss; FFU, at final follow-up; JOA, Japanese Orthopaedics Association. Note: Improvement rate is calculated with Hirabayashi s method. a Additional surgery includes both acute and chronic phase reoperation. final follow-up in the <80 group. The RE and MH components of the <80 group were significantly superior to those of the 80 group at the final follow-up ( Fig. 2). Radiographic Evaluation Multiplanar reconstruction computed tomography images 2 years after surgery showed bony union in 14 of the 19 patients in the 80 group and in 73 of the 77 patients in the <80 group. The bony union rate was 73.7% in the 80 group and 94.8% in the <80 group. There was a significant difference between the two groups (p ¼ 0.013). Two cases of spinal stenosis, 2 of spondylolisthesis, and 1 of degenerative scoliosis in the 80 group and 1 case of spinal stenosis, 2 of spondylolisthesis, and 1 of degenerative scoliosis in the <80 group were diagnosed as nonunion. Five patients (26%) in the 80 group and 13 (17%) in the <80 group had newly identified OVFxs postoperatively (PO OVFx), and there were no significant differences (p ¼ 0.52). However, in the 80 group, PO OVFxs significantly impacted the JOA score improvement, and those patients who had PO OVFx did not show substantial JOA score improvement (with PO OVFx versus without OVFx ¼ 38.8 versus 55.0%, respectively; p ¼ 0.02). By contrast, there were no significant differences in the JOA score improvement with or without PO OVFx in the <80 group (44.4 and 50.5%, p ¼ 0.47). The SQ analysis of OVFxs was also evaluated and is summarized in Table 5. No significant differences were noted between the two groups regarding the numbers of OVFx. Complications Perioperative medical complications were identified in 4 patients (21%) in the 80 group and 12 patients (16%) in the <80 group. Likewise, surgery-specific complications occurred in 7 patients (37%) in the 80 group and 15 patients (19%) in the <80 group. Except for nonunion, surgery-related complications occurred in 3 patients (16%) in the 80 group and 11 patients (14%) in the <80 group. In contrast, major complications were noted in 4 patients (16%) in the 80 group and 7 patients (9%) in the <80 group. There were no significant differences between the two groups. Additional spinal surgeries were required in 1 patient in the 80 group and in 4 patients in the <80 group. Two reoperations in the <80 group were needed because of nonunion. This data is summarized in Table 6. There were no life-threatening complications in either group. Discussion Several authors reported that lumbar arthrodesis with PLIF could provide good clinical outcomes for elderly patients with lumbar spinal canal stenosis. 6,13 16 Okuda et al reported that the surgical outcomes of PLIF were comparable in patients 70 years of age and those <70 years of age. 13 Glassman et al evaluated the HRQOL data (SF-36) following lumbar posterolateral fusion in patients 65 years of age, and they showed Fig. 2 The comparison of the two groups with eight components in Short Form-36 Health Survey (left: 80 group, right: <80 group). Abbreviations: BP, bodily pain; GH, general health; MH, mental health; PF, physical functioning; RE, role emotional; RP, role physical; SF, social functioning; VT, viability.
6 670 Clinical Outcomes of PLIF for Patients 80 Years Hayashi et al. Table 5 Thoracic and lumbar OVFxs of the two groups 80 group (n ¼ 19) <80 group (n ¼ 77) p Value Preoperative OVFx (no. of cases) Postoperative OVFx (no. of cases) Number of vertebrae and their SQ grades 8 Preoperative OVFx (no. of cases) 4 8 Grade Grade PostoperativeOVFx(no.ofcases) 8 16 Grade Grade Abbreviations: OVFx, osteoporotic vertebral fracture; SQ, semiquantitative. Table 6 Complications of the two groups Complications 80 group (n ¼ 19) <80 group (n ¼ 77) p Value Medical complications 4 12 a 0.74 Anemia 0 4 Cardiopulmonary 1 0 Gastrointestinal 1 1 Urinary tract 0 3 Comorbidity deterioration 0 1 Others 2 4 Surgery-specific 7 b Dural tear 1 2 Hematoma 0 1 Neurologic deficit 0 2 Infection 2 2 Implant failure 0 1 Nonunion Adjacent segmental degeneration 0 1 Others 0 2 Major complications c Blood transfusion 0 3 Additional spine surgery 1 4 >0.99 a One patient had postoperative anemia and urinary tract infection. b One patient had infection and nonunion. c The cases needed blood infusion, additional antibiotics, treatment by another department, and additional spine surgery included in major complications. improvement in physical component, which was similar to that of the younger patients. 6 Despite the good clinical outcomes, the authors also indicated that lumbar arthrodesis for elderly patients was associated with a relatively high rate of complications. Most previous studies of lumbar arthrodesis were thought to be inadequate regarding the patients ages, which meant that 65 or 70 years of age was not definitively elderly. In Japan, it is reported that the remaining life expectancy of men at 80 years of age is 8.6 years, and for women it is 11.5 years. 17 Likewise, in the United States, the remaining life expectancy of 75-year-old men is 11.0 years, and for women it is 12.9 years. 14,18 Recently, Rihn and colleague reported operative outcomes in an octogenarian population. 19 They included a large number of the as-treated patients with
7 Clinical Outcomes of PLIF for Patients 80 Years Hayashi et al. 671 lumbar degenerative disease, and they concluded that operative treatment offered a significant benefit over conservative treatment in their population. As noted, they compared the SF-36 BP and physical functioning subdomains in subjects at least 80 years of age and in subjects younger than 80 years. However, they mixed lumbar decompression only and lumbar decompression with fusion as operatively treated patients. Moreover, they did not assess all subdomains in the SF-36. In this study, we evaluated the clinical outcomes and HRQOL data of PLIF for patients older than 80 years old. We found that the JOA score improvement rates were 47.6% in the 80 group and 49.1% in the <80 group. There was no significant difference between the two groups. For the SF-36, only the BP component improved significantly in the 80 group, whereas 7 of the 8 components (GH being the only exception) improved significantly in the <80 group. Comparative analysis indicated that the RE and MH components were significantly superior in the 80 group compared with those in the <80 group. The reason of the gap between JOA score and SF-36 subdomain improvement in the 80 group might be the lack of the assessment for social and mental status in the JOA score. The incidence of complications was not significantly different between the two groups, although patients in the 80 group had a higher tendency of complications. Therefore, our study indicated that PLIF could provide comparable clinical outcomes and adequate pain relief for the patients 80 years of age with acceptable perioperative complications; however, spinal surgeon have to recognize that postoperative HRQOL of the patients 80 years of age cannot improve in comparison with the patients <80 years of age. Bony union is one of the most important outcomes following lumbar arthrodesis. In some previous studies, the bony union rates following PLIF were reported to be 85 to 100%. 13,15,20 In this study, the rate of bony union in the 80 group was 73.7%, which was significantly lower than that of the <80 group (94.8%). Considering both previous reports and our data, aging would be one of the possible risk factors of nonunion. In the future, we should clarify the relationship between age, bone mineral density, and bone union rate in these populations. There was some discrepancy between the clinical outcomes evaluated by JOA score and the bony union rate. However, a previous report noted that the bony union rate was not associated with clinical outcome during the first 2 to 3 postoperative years. 21 Longer followups are necessary to evaluate the impact of nonunion on the clinical outcome. ThepostoperativeincidenceofOVFxinthe80 group (26%) was relatively high, but was not significantly different compared with that in the <80 group (17%). Toyone et al reported that 15% patients over 55 years of age had either adjacent or nonadjacent vertebral fracture after posterior lumbar fusion. 22 Our data is thought to be consistent with their data. On the other hand, postoperatively acquired OVFx significantly worsened the JOA score improvement in the 80 group. OVFx causes severe low back pain and neurologic compromise, and it also worsens the quality of life and increases mortality risk. 23,24 Our results indicate that adequate treatment for osteoporosis could reduce the incidence of postoperative OVFx and prevent the deterioration of the clinical outcomes of PLIF in elderly patients. Recently, Ohtori et al reported that teriparatide improved the bony union rate after spinal arthrodesis. 25 Using teriparatide may be beneficial to improve the clinical outcome of elderly patients following PLIF. There were some limitations to this study. First, the study cohort consisted of small number of patients 80 years of age and a relatively short follow-up. We should continue to investigate the clinical and radiographic outcomes following PLIF in patients 80 years of age. Second, we did not evaluate the sagittal spinal balance in this cohort, and we could not investigate the relationship between clinical outcome or bony union rate and sagittal balance. Third, we did not evaluate bone mineral density for all the patients, and so we could not evaluate the relationship between nonunion and bone mineral density. In conclusion, we demonstrated that clinical outcomes of PLIF evaluated by JOA score in patients 80 years of age were comparable to those of patients < 80 years of age in midterm follow-up. However, a higher rate of nonunion was found in patients 80 years of age, and OVFxs incidence worsened their latest clinical outcomes. Treatment of osteoporosis might be beneficial to prevent the deterioration of the clinical outcomes and to deal with activities of daily living following PLIF. Disclosures Kazunori Hayashi: none Akira Matsumura: none Sadahiko Konishi: none Minori Kato: none Takashi Namikawa: none Hiroaki Nakamura: none References 1 Cloward RB. The treatment of ruptured lumbar intervertebral disc by vertebral body fusion. III. Method of use of banked bone. Ann Surg 1952;136(6): Enker P, Steffee AD. Interbody fusion and instrumentation. Clin Orthop Relat Res 1994;(300): Lowe TG, Tahernia AD, O Brien MF, Smith DA. Unilateral transforaminal posterior lumbar interbody fusion (TLIF): indications, technique, and 2-year results. J Spinal Disord Tech 2002;15(1): Kotwal S, Kawaguchi S, Lebl D, et al. Minimally invasive lateral lumbar interbody fusion: clinical and radiographic outcome at a minimum 2-year follow-up. J Spinal Disord Tech 2015;28(4): DeyoRA,GrayDT,KreuterW,MirzaS,MartinBI.UnitedStates trends in lumbar fusion surgery for degenerative conditions. Spine (Phila Pa 1976) 2005;30(12): , discussion Glassman SD, Polly DW, Bono CM, Burkus K, Dimar JR. Outcome of lumbar arthrodesis in patients sixty-five years of age or older. J Bone Joint Surg Am 2009;91(4): Meyerding HW. Spondylolisthesis. Surg Gynecol Obstet 1932; 54:
8 672 Clinical Outcomes of PLIF for Patients 80 Years Hayashi et al. 8 Genant HK, Wu CY, van Kuijk C, Nevitt MC. Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res 1993;8(9): Fukuhara S, Ware JE Jr, Kosinski M, Wada S, Gandek B. Psychometric and clinical tests of validity of the Japanese SF-36 Health Survey. J Clin Epidemiol 1998;51(11): Hirabayashi K, Miyakawa J, Satomi K, Maruyama T, Wakano K. Operative results and postoperative progression of ossification among patients with ossification of cervical posterior longitudinal ligament. Spine (Phila Pa 1976) 1981;6(4): Rothman SL, Glenn WV Jr. CT evaluation of interbody fusion. Clin Orthop Relat Res 1985;(193): World Health Organization. WHO Handbook for Reporting the Results of Cancer Treatment. Geneva, Switzerland: World Health Organization; 1979: Okuda S, Oda T, Miyauchi A, Haku T, Yamamoto T, Iwasaki M. Surgical outcomes of posterior lumbar interbody fusion in elderly patients. J Bone Joint Surg Am 2006;88(12): Crawford CH III, Smail J, Carreon LY, Glassman SD. Health-related quality of life after posterolateral lumbar arthrodesis in patients seventy-five years of age and older. Spine (Phila Pa 1976) 2011; 36(13): Ino M, Shimizu T, Fueki K, et al. Clinical results of posterior lumbar interbody fusion using titanium intervertebral spacers in elderly patients over 70 years. The Kitakanto Medical Journal 2009; 59: Lian XF, Hou TS, Xu JG, et al. Posterior lumbar interbody fusion for aged patients with degenerative spondylolisthesis: is intentional surgical reduction essential? Spine J 2013;13(10): Ministry of Health, Labour and Welfare, Japan. Simple life table in 2012 (in Japanese). (2012). Available at: toukei/saikin/hw/life/life12/. Accessed September 19, National Center for Health Statistics, United States. Life expectancy at birth, at age 65, and at age 75, by sex, race, and Hispanic origin. (2013). Available at: data/hus/hus13.pdf. Page 99, Table 18. Accessed September 19, Rihn JA, Hilibrand AS, Zhao W, et al. Effectiveness of surgery for lumbar stenosis and degenerative spondylolisthesis in the octogenarian population: analysis of the Spine Patient Outcomes Research Trial (SPORT) data. J Bone Joint Surg Am 2015;97(3): Nakashima H, Yukawa Y, Ito K, et al. Extension CT scan: its suitability for assessing fusion after posterior lumbar interbody fusion. Eur Spine J 2011;20(9): Herkowitz HN, Kurz LT. Degenerative lumbar spondylolisthesis with spinal stenosis. A prospective study comparing decompression with decompression and intertransverse process arthrodesis. J Bone Joint Surg Am 1991;73(6): Toyone T, Ozawa T, Kamikawa K, et al. Subsequent vertebral fractures following spinal fusion surgery for degenerative lumbar disease: a mean ten-year follow-up. Spine (Phila Pa 1976) 2010; 35(21): Johnell O, Kanis JA, Odén A, et al. Mortality after osteoporotic fractures. Osteoporos Int 2004;15(1): Oleksik A, Lips P, Dawson A, et al. Health-related quality of life in postmenopausal women with low BMD with or without prevalent vertebral fractures. J Bone Miner Res 2000;15(7): Ohtori S, Inoue G, Orita S, et al. Comparison of teriparatide and bisphosphonate treatment to reduce pedicle screw loosening after lumbar spinal fusion surgery in postmenopausal women with osteoporosis from a bone quality perspective. Spine (Phila Pa 1976) 2013;38(8):E487 E492
Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with and without Instrumentation
 Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis
 Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis Fujiwara H*, Kaito T**, Makino T**, Ishii T*, Yonenobu K*** Department of Orthopaedic Surgery, *National
Surgical outcome of posterior lumbar interbody fusion for lumbar lesions in rheumatoid arthritis Fujiwara H*, Kaito T**, Makino T**, Ishii T*, Yonenobu K*** Department of Orthopaedic Surgery, *National
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up
 Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Lifestyle-Related Diseases Affect Surgical Outcomes after Posterior Lumbar Interbody Fusion
 2 Original Article GLOBAL SPINE JOURNAL THIEME Lifestyle-Related Diseases Affect Surgical Outcomes after Posterior Lumbar Interbody Fusion Hironobu Sakaura 1 Toshitada Miwa 1 Tomoya Yamashita 2 Yusuke
2 Original Article GLOBAL SPINE JOURNAL THIEME Lifestyle-Related Diseases Affect Surgical Outcomes after Posterior Lumbar Interbody Fusion Hironobu Sakaura 1 Toshitada Miwa 1 Tomoya Yamashita 2 Yusuke
Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report
 Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions:
 Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
ASJ. Radiologic and Clinical Courses of Degenerative Lumbar Scoliosis (10 25 ) after a Short-Segment Fusion. Asian Spine Journal.
 Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases-
 Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis
 Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
Is unilateral pedicle screw fixation superior than bilateral pedicle screw fixation for lumbar degenerative diseases: a meta-analysis
 Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
Lu et al. Journal of Orthopaedic Surgery and Research (2018) 13:296 https://doi.org/10.1186/s13018-018-1004-x SYSTEMATIC REVIEW Open Access Is unilateral pedicle screw fixation superior than bilateral
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
Bare Bones. Use of Systemic Osteoporosis Drugs in Select High Risk Patients Undergoing Spine Surgery
 Use of Systemic Osteoporosis Drugs in Select High Risk Patients Undergoing Spine Surgery 30th Annual Metabolic Bone Disease Society Meeting Denver, CO Oct 11, 2018 Bare Bones 2000 Francesca Pera Kelly
Use of Systemic Osteoporosis Drugs in Select High Risk Patients Undergoing Spine Surgery 30th Annual Metabolic Bone Disease Society Meeting Denver, CO Oct 11, 2018 Bare Bones 2000 Francesca Pera Kelly
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Hiroto Yamaguchi*, Hidetoshi Nojiri**, Kei Miyagawa*, Nozomu Inoue***
 Three-Dimensional High-Resolution Image Analysis of the Segmental Reduction Effect Obtained with Lateral Lumbar Interbody Fusion for Lumbar Intervertebral Deformity Hiroto Yamaguchi*, Hidetoshi Nojiri**,
Three-Dimensional High-Resolution Image Analysis of the Segmental Reduction Effect Obtained with Lateral Lumbar Interbody Fusion for Lumbar Intervertebral Deformity Hiroto Yamaguchi*, Hidetoshi Nojiri**,
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion
 A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis
 Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN Disclosures
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN Disclosures
Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse of a Lumbar Spine Vertebral Body
 Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
Case Reports in Orthopedics Volume 2013, Article ID 682075, 5 pages http://dx.doi.org/10.1155/2013/682075 Case Report Delayed Neurologic Deficit due to Foraminal Stenosis following Osteoporotic Late Collapse
Dept. of Orthopaedic Surgery, Wakayama Medical University, Wakayama, Japan. Brigham and Women s Hospital, Harvard Medical School, Boston, MA, USA.
 Microendoscopic Decompression for Lumbar Spinal Stenosis with Degenerative Spondylolisthesis: the influence of spondylolisthesis stage (disc height and static and dynamic translation) on clinical outcomes
Microendoscopic Decompression for Lumbar Spinal Stenosis with Degenerative Spondylolisthesis: the influence of spondylolisthesis stage (disc height and static and dynamic translation) on clinical outcomes
Case Report Unilateral Pedicle Stress Fracture in a Long-Term Hemodialysis Patient with Isthmic Spondylolisthesis
 Case Reports in Orthopedics Volume 2015, Article ID 426940, 4 pages http://dx.doi.org/10.1155/2015/426940 Case Report Unilateral Pedicle Stress Fracture in a Long-Term Hemodialysis Patient with Isthmic
Case Reports in Orthopedics Volume 2015, Article ID 426940, 4 pages http://dx.doi.org/10.1155/2015/426940 Case Report Unilateral Pedicle Stress Fracture in a Long-Term Hemodialysis Patient with Isthmic
Posterior lumbar interbody fusion versus intertransverse fusion in the treatment of lumbar spondylolisthesis
 Journal of Orthopaedic Surgery 2006;14(1):21-6 Posterior lumbar interbody fusion versus intertransverse fusion in the treatment of lumbar spondylolisthesis DN Inamdar, M Alagappan, L Shyam, S Devadoss,
Journal of Orthopaedic Surgery 2006;14(1):21-6 Posterior lumbar interbody fusion versus intertransverse fusion in the treatment of lumbar spondylolisthesis DN Inamdar, M Alagappan, L Shyam, S Devadoss,
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Dingjun Hao, Baorong He, Liang Yan. Hong Hui Hospital, Xi an Jiaotong University College. of Medicine, Xi an, Shaanxi , China
 Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
DEGENERATIVE SPONDYLOLISTHESIS
 AN INTRODUCTION TO DEGENERATIVE SPONDYLOLISTHESIS This booklet is designed to inform you about lumbar degenerative spondylolisthesis. It is not meant to replace any personal conversations that you might
AN INTRODUCTION TO DEGENERATIVE SPONDYLOLISTHESIS This booklet is designed to inform you about lumbar degenerative spondylolisthesis. It is not meant to replace any personal conversations that you might
Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki 3), Masatsune Yamagata 1), Yoshikazu Ikeda 1), Fumitake Nakajima 1)
 Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Patient Information ACDF. Anterior Cervical Discectomy and Fusion
 Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
Facet orientation in patients with lumbar degenerative spondylolisthesis
 35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
Spine Tango annual report 2012
 DOI 10.1007/s00586-013-2943-x SPINE TANGO REPORT 2012 Spine Tango annual report 2012 M. Neukamp G. Perler T. Pigott E. Munting M. Aebi C. Röder Received: 31 July 2013 / Published online: 30 August 2013
DOI 10.1007/s00586-013-2943-x SPINE TANGO REPORT 2012 Spine Tango annual report 2012 M. Neukamp G. Perler T. Pigott E. Munting M. Aebi C. Röder Received: 31 July 2013 / Published online: 30 August 2013
Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion. Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD
 ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
Spine Center. at Stamford Hospital s Orthopedic Institute
 Spine Center at Stamford Hospital s Orthopedic Institute Back pain related to spinal deformity and injury or congenital conditions is a common health complaint, which can be very debilitating. At Stamford
Spine Center at Stamford Hospital s Orthopedic Institute Back pain related to spinal deformity and injury or congenital conditions is a common health complaint, which can be very debilitating. At Stamford
Disclosures: T. Yoshii: None. T. Yamada: None. T. Taniyama: None. S. Sotome: None. T. Kato: None. S. Kawabata: None. A. Okawa: None.
 Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
Evidence Table. Study Type: Randomized controlled trial. Study Aim: To evaluate the safety and efficacy of the X-Stop interspinous implant.
 Evidence Table Clinical Area: Reference: Spinal decompression device for lumbar spinal stenosis Zucherman JF et al. A prospective randomized multi-center study for the treatment of lumbar spinal stenosis
Evidence Table Clinical Area: Reference: Spinal decompression device for lumbar spinal stenosis Zucherman JF et al. A prospective randomized multi-center study for the treatment of lumbar spinal stenosis
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Computed tomography analysis of L5-S1 fusion in Adult spinal deformity
 Eurospine 2018 Barcelona Computed tomography analysis of L5-S1 fusion in Adult spinal deformity Comparison of whether spinopelvic fixation, ALIF vs PLIF, and cage design Jung-Hee Lee MD, Kyung-Chung Kang
Eurospine 2018 Barcelona Computed tomography analysis of L5-S1 fusion in Adult spinal deformity Comparison of whether spinopelvic fixation, ALIF vs PLIF, and cage design Jung-Hee Lee MD, Kyung-Chung Kang
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis
 Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN The following
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN The following
Adult Spinal Deformity: Principles of Surgical Correction
 Adult Spinal Deformity: Principles of Surgical Correction S. Samuel Bederman, MD PhD FRCSC Department of Orthopaedic Surgery California Orthopaedic Association, Indian Wells, CA April 25, 2015 2 3 4 Adult
Adult Spinal Deformity: Principles of Surgical Correction S. Samuel Bederman, MD PhD FRCSC Department of Orthopaedic Surgery California Orthopaedic Association, Indian Wells, CA April 25, 2015 2 3 4 Adult
Range of motion of thoracic spine in sagittal plane
 DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
Lumbar Spinal Fusion Corporate Medical Policy
 Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Patient Selection and Lumbar Operative Interventions
 Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Adult Spinal Deformity Robert Hart. Dept. Orthopaedics and Rehab OHSU
 Adult Spinal Deformity 2010 Robert Hart Dept. Orthopaedics and Rehab OHSU What is Adult Spinal Deformity? Untreated Idiopathic Scoliosis Flat Back Syndrome Adjacent Segment Stenosis Non-Union Degenerative
Adult Spinal Deformity 2010 Robert Hart Dept. Orthopaedics and Rehab OHSU What is Adult Spinal Deformity? Untreated Idiopathic Scoliosis Flat Back Syndrome Adjacent Segment Stenosis Non-Union Degenerative
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis
 Acta Orthop. Belg., 2008, 74, 667-671 ORIGINAL STUDY Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis Mohamed Adel EL MASRY,
Acta Orthop. Belg., 2008, 74, 667-671 ORIGINAL STUDY Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis Mohamed Adel EL MASRY,
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion
 Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 28 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 28 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Yoshinao Koike, Yoshihisa Kotani, Hidemasa Terao, Yoshiaki Hosokawa, Hideyuki Kobayashi, Yusuke Kameda, Hideaki Fukaya
 Comparative Analysis of Physical Function and Quality of Life Parameters in Two Surgical Modalities for Single-level Degenerative Spondylolisthesis: OLIF with Percutaneous Posterior Fixation in Lateral
Comparative Analysis of Physical Function and Quality of Life Parameters in Two Surgical Modalities for Single-level Degenerative Spondylolisthesis: OLIF with Percutaneous Posterior Fixation in Lateral
University of Jordan. Professor Freih Abuhassan -
 Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis
 J Child Orthop (2012) 6:137 143 DOI 10.1007/s11832-012-0400-8 ORIGINAL CLINICAL ARTICLE Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis Bradley P. Jaquith
J Child Orthop (2012) 6:137 143 DOI 10.1007/s11832-012-0400-8 ORIGINAL CLINICAL ARTICLE Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis Bradley P. Jaquith
Current status of managing pediatric kyphosis deformity Papers divided into 3 categories
 Biomechanical and Clinical Evaluation of Rib Anchors Richard H. Gross, MD Research Professor, Clemson University Clemson-MUSC Bioengineering Consortium Charleston, SC Staff surgeon, Shriners Hospital,
Biomechanical and Clinical Evaluation of Rib Anchors Richard H. Gross, MD Research Professor, Clemson University Clemson-MUSC Bioengineering Consortium Charleston, SC Staff surgeon, Shriners Hospital,
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Top spine papers of 2016
 Top spine papers of 2016 Ai Mukai, MD Texas Orthopedics, Sports & Rehabilitation University of Texas-Austin, PM&R Residency October 21, 2016 Top papers in spine? Top papers in Spine How do you define top?
Top spine papers of 2016 Ai Mukai, MD Texas Orthopedics, Sports & Rehabilitation University of Texas-Austin, PM&R Residency October 21, 2016 Top papers in spine? Top papers in Spine How do you define top?
The cortical bone trajectory (CBT) screw technique
 CLINICAL ARTICLE J Neurosurg Spine 28:57 62, 2018 Cortical bone trajectory screw fixation versus traditional pedicle screw fixation for 2-level posterior lumbar interbody fusion: comparison of surgical
CLINICAL ARTICLE J Neurosurg Spine 28:57 62, 2018 Cortical bone trajectory screw fixation versus traditional pedicle screw fixation for 2-level posterior lumbar interbody fusion: comparison of surgical
QF-78. S. Tanaka 1, T.Yokoyama 1, K.Takeuchi 1, K.Wada 2, T. Tanaka 2, S.Abrakawa 2, G.Kumagai 2, T.Asari 2, A.Ono 2, Y.
 QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
vertebra associated with dura) ectasia in
 e287 Case Report Grade 4 spondylolisthesis of the L5 vertebra associated with dura) ectasia in neurofibromatosis Modi H N, Srinivasalu S, Suh S W, Yang J H ABSTRACT Spondylolisthesis associated with neurofibromatosis
e287 Case Report Grade 4 spondylolisthesis of the L5 vertebra associated with dura) ectasia in neurofibromatosis Modi H N, Srinivasalu S, Suh S W, Yang J H ABSTRACT Spondylolisthesis associated with neurofibromatosis
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Abstract Study Design Systematic review. Weerasak Singhatanadgige 1 Worawat Limthongkul 1 Frank Valone III 2 Wicharn Yingsakmongkol 1 K.
 702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
Same Segment Early Recurrence in Surgery of Lumbar Canal Stenosis- Role of Dissectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. II (August. 2016), PP 34-40 www.iosrjournals.org Same Segment Early Recurrence in Surgery
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. II (August. 2016), PP 34-40 www.iosrjournals.org Same Segment Early Recurrence in Surgery
2016 OPAM Mid-Year Educational Conference, sponsored by AOCOPM Thursday, March 10, 2016 C-1
 Long-term Outcomes of Lumbar Fusion Among Workers Compensation Subjects : An Historical Cohort Study Trang Nguyen M.D., Ph.D. David C. Randolph M.D, M.P.H. James Talmage MD Paul Succop PhD Russell Travis
Long-term Outcomes of Lumbar Fusion Among Workers Compensation Subjects : An Historical Cohort Study Trang Nguyen M.D., Ph.D. David C. Randolph M.D, M.P.H. James Talmage MD Paul Succop PhD Russell Travis
Prodisc-L. Retrospective Clinical Study: 7 to 11 Year Follow-up.
 Prodisc-L. Retrospective Clinical Study: 7 to 11 Year Follow-up. Table of Contents 3 Abstract 4 Background 5 Objectives 5 Methodology 5 Verification and validation of all implanted cases 5 Locating patients
Prodisc-L. Retrospective Clinical Study: 7 to 11 Year Follow-up. Table of Contents 3 Abstract 4 Background 5 Objectives 5 Methodology 5 Verification and validation of all implanted cases 5 Locating patients
Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy. Spine January 1, 2009; Volume 34; Issue 1; pp 82-86
 Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy 1 Spine January 1, 2009; Volume 34; Issue 1; pp 82-86 Yukawa, Yasutsugu; Kato, Fumihiko; Ito, Keigo; Horie, Yumiko; Nakashima,
Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy 1 Spine January 1, 2009; Volume 34; Issue 1; pp 82-86 Yukawa, Yasutsugu; Kato, Fumihiko; Ito, Keigo; Horie, Yumiko; Nakashima,
High failure rate of the interspinous distraction device (X-Stop) for the treatment of lumbar spinal stenosis caused by degenerative spondylolisthesis
 Eur Spine J (2008) 17:188 192 DOI 10.1007/s00586-007-0492-x ORIGINAL ARTICLE High failure rate of the interspinous distraction device (X-Stop) for the treatment of lumbar spinal stenosis caused by degenerative
Eur Spine J (2008) 17:188 192 DOI 10.1007/s00586-007-0492-x ORIGINAL ARTICLE High failure rate of the interspinous distraction device (X-Stop) for the treatment of lumbar spinal stenosis caused by degenerative
Patient Information. ADULT SCOLIOSIS Information About Adult Scoliosis, Symptoms, and Treatment Options
 Patient Information ADULT SCOLIOSIS Information About Adult Scoliosis, Symptoms, and Treatment Options Table of Contents Anatomy of the Spine...2 What is Adult Scoliosis...4 What are the Causes of Adult
Patient Information ADULT SCOLIOSIS Information About Adult Scoliosis, Symptoms, and Treatment Options Table of Contents Anatomy of the Spine...2 What is Adult Scoliosis...4 What are the Causes of Adult
Surgical outcomes for lumbar spinal canal stenosis with coexisting cervical stenosis (tandem spinal stenosis): a retrospective analysis of 565 cases
 Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY
 PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
Original Article Clinics in Orthopedic Surgery 2016;8:
 Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
The effect of body mass index on lumbar lordosis on the Mizuho OSI Jackson spinal table
 35 35 40 The effect of body mass index on lumbar lordosis on the Mizuho OSI Jackson spinal table Authors Justin Bundy, Tommy Hernandez, Haitao Zhou, Norman Chutkan Institution Orthopaedic Department, Medical
35 35 40 The effect of body mass index on lumbar lordosis on the Mizuho OSI Jackson spinal table Authors Justin Bundy, Tommy Hernandez, Haitao Zhou, Norman Chutkan Institution Orthopaedic Department, Medical
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI /s
 Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Impact of spino-pelvic and global spinal alignment on the risk of osteoporotic vertebral collapse
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Impact of spino-pelvic and global spinal alignment on the risk of osteoporotic vertebral collapse Takashi Ohnishi 1)2), Akira Iwata 1)2), Masahiro Kanayama
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Impact of spino-pelvic and global spinal alignment on the risk of osteoporotic vertebral collapse Takashi Ohnishi 1)2), Akira Iwata 1)2), Masahiro Kanayama
Effect of Swallowing Function After ROI-C Anterior Cervical Interbody Fusion
 Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Posterior. Lumbar Fusion. Disclaimer. Integrated web marketing. Multimedia Health Education
 Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
INTERSPINOUS STABILIZATION-FUSION IN THE UNSTABLE SPINE.
 INTERSPINOUS STABILIZATION-FUSION IN THE UNSTABLE SPINE. A PRELIMINARY REPORT F. POSTACCHINI, A. PALMESI LUMBAR VERTEBRAL INSTABILITY Still the subject of discussion Variously defined and interpreted Postacchini
INTERSPINOUS STABILIZATION-FUSION IN THE UNSTABLE SPINE. A PRELIMINARY REPORT F. POSTACCHINI, A. PALMESI LUMBAR VERTEBRAL INSTABILITY Still the subject of discussion Variously defined and interpreted Postacchini
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
Degenerative lumbar kyphoscoliosis (DLKS) is
 technical note J Neurosurg Spine 26:150 157, 2017 Posterior corrective surgery with a multilevel transforaminal lumbar interbody fusion and a rod rotation maneuver for patients with degenerative lumbar
technical note J Neurosurg Spine 26:150 157, 2017 Posterior corrective surgery with a multilevel transforaminal lumbar interbody fusion and a rod rotation maneuver for patients with degenerative lumbar
Vertebral body fractures after transpsoas interbody fusion procedures
 The Spine Journal 11 (2011) 1068 1072 Case Report Vertebral body fractures after transpsoas interbody fusion procedures Justin E. Brier-Jones, BS a, Daniel K. Palmer, BS b, Serkan Inceoglu, PhD a, Wayne
The Spine Journal 11 (2011) 1068 1072 Case Report Vertebral body fractures after transpsoas interbody fusion procedures Justin E. Brier-Jones, BS a, Daniel K. Palmer, BS b, Serkan Inceoglu, PhD a, Wayne
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with Thoracolumbar Fractures
 Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Sigita Burneikiene, MD; Alan T. Villavicencio, MD; Alexander Mason, MD; Sharad Rajpal, MD
 The Timing of Surgery and Symptom Resolu6on in Pa6ents Undergoing Transforaminal Lumbar Interbody Fusion for Lumbar Degenera6ve Disc Disease and Radiculopathy Sigita Burneikiene, MD; Alan T. Villavicencio,
The Timing of Surgery and Symptom Resolu6on in Pa6ents Undergoing Transforaminal Lumbar Interbody Fusion for Lumbar Degenera6ve Disc Disease and Radiculopathy Sigita Burneikiene, MD; Alan T. Villavicencio,
ProDisc-L Total Disc Replacement. IDE Clinical Study
 Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
