Inadvertent Perioperative Hypothermia During Orthopedic Surgery
|
|
|
- Wesley Lawrence McCormick
- 5 years ago
- Views:
Transcription
1 Inadvertent Perioperative Hypothermia During Orthopedic Surgery Publish date: July 12, 2018 Authors: Chandrakanth Boddu, MD Joseph Cushner Giles R. Scuderi, MD Author Affiliation Disclosures Authors Disclosure Statement: The authors report no actual or potential conflict of interest in relation to this article. Dr. Boddu is a Clinical Fellow, NSLIJ Adult Reconstruction/Knee, Lenox Hill Hospital, New York, New York. Mr. Cushner is a student, Columbia University, New York, New York. Dr. Scuderi is Program Director, NSLIJ Adult Reconstruction/Knee, Orthopaedic Service Line, North Shore Long Island Jewish Health System, New York, New York. Address correspondence to: Chandrakanth Boddu, MD, Lenox Hill Hospital, 130 East 77th Street, 11th Floor, New York, NY (tel, ; fax, ; , chanduortho@gmail.com). Am J Orthop. 2018;47(7). Copyright Frontline Medical Communications Inc All rights reserved. Take-Home Points Inadvertent perioperative hypothermia, defined as an involuntary drop in core body temperature to <35 C (95 F), is a condition associated with significant morbidity and mortality. Maintenance of core body temperature >36 C is now a measured standard of perioperative care. Overall, in the last 2 decades, the incidence of inadvertent perioperative hypothermia has decreased, mainly due to aggressive intraoperative management. Active patient warming by conduction devices occurs by direct physical contact with the device, which is set at a higher temperature, whereas heat transfer from the convection device to the patient occurs by a physical medium such as forced air or circulating water that moves in between the device and the patient. Active patient warming is superior to passive heat retention methods. Inadvertent perioperative hypothermia, defined as an involuntary drop in core body temperature to <35 C (95 F), is a condition associated with significant morbidity and mortality.1 This phenomenon has been reported in both emergency orthopedic admissions, such as fracture management, as well as in the elective setting such as arthroscopy, arthroplasty, and spine surgery. In a study conducted in the United Kingdom including 781 elderly patients with a mean age of 80 years who presented with hip fractures, the 30-day mortality rate was 15.3% in patients who were admitted with a tympanic temperature of <36.5 C and only 5.1% in patients who maintained a tympanic temperature of 36.5 C to 37.5 C (odds ratio, 2.8; P >.0005).2 For an even better perspective, this analysis can be compared with the UK National Apr 2019 The American Journal of Orthopedics 1
2 Hip Fracture Database of 2013, which reported a 30-day mortality of 8.2% in patients who were admitted to the National Health Service with a diagnosis of hip fracture.3 Inadvertent perioperative hypothermia is also a common phenomenon during elective orthopedic hospital admissions. An Australian audit, which included 5050 postoperative patients, looked into the association between inadvertent perioperative hypothermia and mortality based on diagnostic criteria classifying mild hypothermia as a core temperature of <36 C and severe hypothermia as a core temperature of <35 C.4 The authors found that mild and severe hypothermia was experienced by 36% and 6% of patients, respectively. In-hospital mortality was 5.6% for normothermic patients, 8.9% for all hypothermic patients (P <.001), and 14.7% for severely hypothermic patients (P <.001). For a decrease of 1 C in core body temperature from <36 C to <35 C (but >34 C), there were higher odds of in-hospital mortality (odds ratio, 1.83; 95% confidence interval [CI], ). The physiologic response to hypothermia is to decrease heat loss by cutaneous and peripheral vasoconstriction and increase heat production by increasing the metabolic rate (eg, shivering and shifting to anaerobic metabolism). This response is blunted to a variable extent in perioperative patients for several reasons, including the effect of anesthetic drugs and old age.5 Maintenance of core body temperature >36 C is now a measured standard of perioperative care. A performance measure for perioperative temperature management was developed by the American Medical Association Physician Consortium for Performance Improvement (AMA-PCPI).6 To achieve this performance measure, mandatory documentation of use of active warming intraoperatively or a record of at least 1 body temperature 96.8 F (36 C) within 30 minutes immediately prior to and 15 minutes immediately after anesthesia end time is necessary. This performance measure is also endorsed by the Surgical Care Improvement Project (SCIP-Inf-10) and National Quality Forum (NQF). 6 Overall, in the last 2 decades, the incidence of inadvertent perioperative hypothermia has decreased, mainly due to aggressive intraoperative management.7 In spite of this, studies have shown that perioperative hypothermia remains a significant problem in patients undergoing orthopedic procedures. In a recent community hospital study conducted by the National Association for Healthcare Quality that included 4124 orthopedic patients undergoing elective surgery, it was shown that, in spite of 99% compliance to the AMA-PCPI recommendation, 7.7% of orthopedic patients were found to be hypothermic. 6 Management of hypothermia has long been an integral component of damage control surgery and resuscitation during polytrauma, which aims to aggressively minimize hypovolemic shock and limit the development of the lethal triad of hypothermia, coagulopathy, and acidosis.8 However, critical references to prevention and management of inadvertent perioperative hypothermia are lacking in the orthopedic literature on elective surgical procedures. This review aims to bridge this knowledge gap. Unless otherwise specified, inadvertent perioperative hypothermia in this article refers to the core body temperature. In contrast, peripheral/limb hypothermia refers primarily to the effect of tourniquet application to the involved limb and the effect after deflation of the tourniquet on core body temperature. Risk Factors There are several measurable risk factors that can contribute to inadvertent perioperative hypothermia, which can be subdivided into 3 groups: patient-related risk factors, anesthesia-related risk factors, and procedure-related risk factors (Table 1). 5,9-11 It is important to note that in any given patient a combination of 2 or more risk factors predisposes them to developing inadvertent perioperative hypothermia. Conceptualizing the etiology of Apr 2019 The American Journal of Orthopedics 2
3 inadvertent perioperative hypothermia in this way helps to plan a multipronged strategy to prevent it from occurring in the first place. Some of the important risk factors for inadvertent perioperative hypothermia are discussed below. To identify patient-related risk factors, researchers from the University of Louisville conducted a study including 2138 operative patients who became hypothermic after admission, of whom 27% underwent orthopedic and spine procedures. 9 The patient-related risk factors identified were a high severity of illness on admission (odds ratio, 2.81; 95% CI, ), presence of a neurological disorder such as Alzheimer s disease (odds ratio, 1.71; 95% CI, ), male sex (odds ratio, 1.65; 95% CI, ), age >65 years (odds ratio, 1.61; 95% CI, ), recent weight loss (odds ratio, 1.60; 95% CI, ), anemia (odds ratio, 1.49; 95% CI, ), and chronic renal failure (odds ratio, 1.43; 95% CI, ). Interestingly, diabetes mellitus without end-stage organ failure was not found to be a significant risk factor (odds ratio, 0.58; 95% CI, ). It is also important to note that some of these risk factors identified to contribute to perioperative hypothermia are dependent on each other and others are independent of each other. For example, chronic renal failure and anemia are dependent risk factors. In contrast, age >65 years and low body mass index as risk factors of perioperative hypothermia are independent of each other. The second subgroup of risk factors for perioperative hypothermia is related to anesthesia. The effect of general and regional anesthesia on perioperative core temperature is significantly different, both in terms of intraoperative thermoregulation and postoperative recovery.12 Intraoperatively, the core body temperature during the first 2 hours of general anesthesia decreases at a rate of 1.3 C per hour due to loss of thermoregulatory cutaneous and peripheral vasoconstrictive responses resulting in heat loss exceeding metabolic heat production. However, the core temperature remains virtually constant during the subsequent 3 hours due to the return of the thermoregulatory response, which causes cutaneous and peripheral vasoconstriction and increased metabolic heat production. Postoperative recovery from the hypothermia induced by general anesthesia is significantly faster than from that induced by regional anesthesia.13 The effect of regional hypothermia on core body temperature is more complex because it must be considered in addition to the effect of an associated procedure-related variable (ie, tourniquet application). If a tourniquet is not used during a surgery with regional anesthesia, a linear decrease in core temperature follows until recovery, due to increased blood flow from the loss of sympathetic peripheral vasoconstrictive response with resultant core-toperipheral heat redistribution to the exposed operating limb. If a tourniquet is used during surgery with regional anesthesia, there will be no significant effect of the exposed operating limb on core temperature, as there is no blood flow between them. However, once the tourniquet is deflated, the core body temperature will be affected significantly as a result of core-to-peripheral distribution of heat to the operated limb with the return of blood flow. This fall in core body temperature after tourniquet deflation can be prevented by active forced-air warming initiated from the beginning of surgery. 10 The extent and rate of development of peripheral/limb hypothermia during surgery (and its subsequent effect on core body temperature) depends on several factors, including the operating room ambient temperature, duration of tourniquet application, and temperature of the irrigation fluid. Postoperative recovery from the hypothermia induced by regional anesthesia takes longer than from that induced by general anesthesia because of the prolonged period of loss of vasoconstrictive response. The third subgroup of risk factors associated with perioperative hypothermia is procedure related. Several procedure-specific risk factors for inadvertent perioperative hypothermia during arthroscopic surgery are identified, including prolonged operating time, low blood pressure during the procedure, and low temperature of the irrigation fluid. 11 It is logical to extrapolate the importance of these risk factors to other orthopedic procedures which also require prolonged operating times, are performed under hypotension, or expose the patient to irrigation fluid that is at a low temperature. Understanding the importance of each of these procedure-related risk Apr 2019 The American Journal of Orthopedics 3
4 factors is the most important from the perspective of the orthopedic surgeon when compared to the rest of the subgroups of risk factors for inadvertent perioperative hypothermia as he/she is directly responsible for them. The ambient operating room temperature has traditionally been considered a risk factor for inadvertent hypothermia in perioperative patients, but evidence is available to the contrary. The recommended ambient room temperature as per the clinical guideline published by the American Society of PeriAnesthesia Nurses (ASPAN) is 20 C to 24 C (68 F-75 F).14 The ambient temperature can have a significant effect on peripheral/limb hypothermia when operating on a limb with a tourniquet inflated, as the limb has no blood supply to distribute heat from the core to the periphery. However, the direct effect of ambient room temperature on the patient s core body temperature is unlikely to be clinically significant if standard active warming interventions are implemented.15 Complications The increased incidence of mortality due to inadvertent hypothermia in the perioperative period has already been discussed. Several other complications of inadvertent perioperative hypothermia include increased incidence of coagulopathy, acidosis, stroke, sepsis, pneumonia, myocardial infarction, surgical site infections, altered drug metabolism, and longer hospital stays. 8,9,16-18 Hypothermia, coagulopathy, and acidosis have long been recognized as a lethal triad more commonly seen in polytrauma patients than in elective orthopedic surgery, as this occurs at extremes of temperature, usually <32 C. When compared with patients who did not develop perioperative hypothermia, patients who developed hypothermia during elective operations were shown to experience an overall doubled complication rate (13.9% vs 26.3%; P <.001) of which the incidence of stroke (1.0% vs 6.5%; P <.001), pneumonia (1.3% vs 5.1%; P <.001), and sepsis (2.6% vs 7.5%; P <.001) were much more likely than myocardial infarction (1.1% vs 3.3%; P =.01) and wound infection (3.3% vs 5.0%; P =.14). 9 Prevention Prevention of perioperative hypothermia is a core measure to improve the outcome after ambulatory and fasttrack orthopedic surgery and rehabilitation. Preventive strategies for perioperative hypothermia can be grouped into passive heat retention methods and active external warming methods (Table 2). Passive methods aim to maintain body temperature by decreasing the heat loss by radiation (eg, reflective blanket), conduction (eg, layered cotton blankets and padding the operating table), or convection (eg, heat and humidity exchanger in the breathing circuits) to the surrounding environment. Active patient heating methods aim to bring in heat from the source to the patient s body using conduction (eg, Hot Dog [Eden Augustine Temperature Management]) or convection (eg, Bair Hugger [Arizant Healthcare]) techniques. Active patient warming is superior to passive heat retention methods. A recent Cochrane study assessed the effects of standard care (ie, use of layered clothing and warm blankets, etc.) and addition of extra thermal insulation by reflective blankets or active forced air warming to standard care on the perioperative core body temperature.19 They concluded that there is no clear benefit of addition of extra thermal insulation by reflective blankets compared with standard care alone. Also, forced-air warming in addition to standard care appeared to maintain core temperature better than standard care alone, by between 0.5 C and 1 C, but the clinical importance of this difference could not be inferred, as none of the included studies in this meta-analysis documented major cardiovascular outcomes. Several clinical guidelines have been developed by not-for-profit, government, and professional organizations Apr 2019 The American Journal of Orthopedics 4
5 aimed at prevention of perioperative hypothermia as primary or secondary outcome. A clinical guideline was published by ASPAN in 2001 for assessment, prevention, and intervention in unplanned perioperative hypothermia.14 Cost and time effectiveness of the ASPAN Hypothermia Guideline was published in The assessment guideline includes identification of risk factors, repeated pre-/intra-/postoperative temperature measurement, and repeated clinical evaluation of the patient s status. The preventive guideline is to maintain an ambient temperature of 20 C to 24 C (68 F-75 F) and use appropriate passive patient warming methods pre-, intra-, and postoperatively. Intervention in the form of active patient heating is advised only if the patient develops hypothermia in spite of the above-mentioned standard preventive measures. But many orthopedic ambulatory surgery centers currently use active patient warming as both a preventive and an intervention strategy. Active patient warming by conduction devices occurs by direct physical contact with the device, which is set at a higher temperature, whereas heat transfer from the convection device to the patient occurs by a physical medium such as forced air or circulating water that moves in between the device and the patient. Any recommendation for use of a specific technique of active patient warming (ie, by the use of a conduction device or a convection device) should only be given after comparing evidence on 3 critical aspects: efficacy, safety, and cost effectiveness. The heating efficacy and core rewarming rates of conduction and convection devices have been compared in the literature. Full-body forced-air heating with the Bair Hugger and full-body resistive polymer heating with the Hot Dog in healthy volunteers were found to be similar.21 Also, in a randomized study conducted on 80 orthopedic patients undergoing surgery, resistive polymer warming performed as efficiently as forced-air warming in patients undergoing orthopedic surgery.22 Secondly, the safety of convection devices such as the Bair Hugger has been under intense scrutiny based on the evidence that it disrupts the laminar airflow in the operating theater This disruption in laminar air flow has been shown to cause emission of significant levels of airborne contaminants of size >0.3 μm (germ size).27 Isolates of Staphylococcus aureus, coagulase-negative Staphylococcus species, and methicillin-resistant Staphylococcus aureus were detected in 13.5%, 3.9%, and 1.9% of forced-air blowers, respectively.28 However, the clinical effect on the rate of deep joint infection due to the disruption of laminar air flow has been examined in only 1 study. McGovern and colleagues 29 reported a significant increase in deep joint infection during a period when forced air warming was used compared to a period when conductive fabric warming was used (odds ratio, 3.8; P =.024) and recommended air-free warming by a conduction device over forced-air warming for orthopedic procedures. Unfortunately, the prophylactic antibiotic regimen was not kept constant during their study period. During an overlapping time frame during which they shifted from the use of a convection device (Bair Hugger ) to a conduction device (Hot Dog ), they also changed their antibiotic regimen from gentamicin 4.5 mg/kg intravenous (IV) to gentamicin 3 mg/kg IV plus teicoplanin 400 mg IV. This change in antibiotic regimen is a major confounding factor that calls into question the validity of the conclusions drawn by the authors. Finally, the cost effectiveness of conduction and convection devices has never been studied. Hence, based on the current evidence, it is not possible to recommend a particular type of active patient-warming device. Conclusion Orthopedic surgeons should be aware that inadvertent perioperative hypothermia is a common phenomenon in perioperative patients. It must be recognized that the maintenance of perioperative normothermia during all major orthopedic surgical procedures is desirable, as inadvertent perioperative hypothermia is shown to be associated with increased mortality and systemic morbidity, such as stroke and sepsis. Compliance with the current clinical guidelines for assessment, prevention, and treatment of inadvertent perioperative hypothermia Apr 2019 The American Journal of Orthopedics 5
6 will minimize, if not eliminate, such risk. We recommend the following essential clinical guidelines to prevent inadvertent perioperative hypothermia (Table 3). Identification of patient-, anesthesia-, and procedure-related risk factors is an integral component of assessment of the risk of inadvertent perioperative hypothermia. In order to achieve full compliance with implementation of active patient warming during surgery, it is prudent to make active warming information a part of the surgical timeout checklist. Irrespective of the presence of risk factors, passive heat retention methods should be part of perioperative management of patients undergoing elective orthopedic surgery to prevent inadvertent perioperative hypothermia. In addition, there should be a minimum threshold to utilize active patient-warming techniques, especially in patients with inherent risk factors and surgeries that take >30 minutes of operating time, either under regional or general anesthesia. As there are concerns about safety issues with the use of convection devices, we believe a multicenter randomized controlled trial is warranted. Key Info Figures/Tables Figures / Tables: Table 1. Risk Factors for Perioperative Hypothermia Patient-Related Risk Factors High severity of illness Neurological disorder (Alzheimer s etc.) Male Age >65 years Weight loss Anemia Chronic renal failure Low body mass index Anesthesia-Related Risk FactorsProcedure-Specific Risk Factors Type of anesthesia Intravenous fluid temperature Tourniquet application Duration of surgery Irrigation fluid temperature Table 2. Methods to Prevent Inadvertent Perioperative Hypothermia Passive Heat-Retention Methods Active External Warming Methods Apr 2019 The American Journal of Orthopedics 6
7 Isolation (, reflective blanket, layered cotton blankets, padding the operating table) Heat and humidity exchanger in the breathing circuits Conduction techniques: Warm mattress pads/blankets Electrical mattress pads/blankets Convection techniques: Forced-air warming Warm intravenous fluids (to 38C) Low flow anesthesia (fresh gas flow LPM) Warm air flow through the ventilator Table 3. Recommended Essential Clinical Guidelines for Prevention of Inadvertent Perioperative Hypothermia Identify all the patient-related, anesthesia-related, and procedure-related risk factors for perioperative hypothermia. Use passive heat-retention methods in all patients, irrespective of the risk factors. Use active heat-retention methods when any risk factors are identified. Include a statement on methods used to prevent perioperative hypothermia in the surgical timeout checklist. References References References 1. Brown DJ, Brugger H, Boyd J, Paal P. Accidental Hypothermia. N Engl J Med. 2012;367(20): doi: /nejmra Uzoigwe CE, Khan A, Smith RP, et al. Hypothermia and low body temperature are common and associated with high mortality in hip fracture patients. Hip Int. 2014; 24(3): doi: /hipint Johansen A, Wakeman R, Boulton C, Plant F, Roberts J, Williams A. National Hip Fracture Database: National Report London, UK: National Hip Fracture Database, Royal College of Physicians; Karalapillai D, Story DA, Calzavacca, Licari E, Liu YL, Hart GK. Inadvertent hypothermia and mortality in postoperative intensive care patients: retrospective audit of 5050 patients. Anaesthesia. 2009;64(9): doi: /j x. 5. Horosz B, Malec-Milewska M. Inadvertent intraoperative hypothermia. Anaesthesiol Intensive Ther. 2013;45(1): doi: /ait Steelman VM, Perkhounkova YS, Lemke JH. The gap between compliance with the quality performance measure "perioperative temperature management and normothermia. J Healthc Qual. 2014;37(6): doi: /jhq Apr 2019 The American Journal of Orthopedics 7
8 7. National Institute for Health and Clinical Excellence. Inadvertent Perioperative Hypothermia: The Management of Inadvertent Perioperative Hypothermia in Adults. London, UK: National Institute for Health and Clinical Excellence; Carlino W. Damage control resuscitation from major haemorrhage in polytrauma. Eur J Orthop Surg Traumatol. 2014;24(2): doi: /s Billeter AT, Hohmann SF, Druen D, Cannon R, Polk HC Jr. Unintentional perioperative hypothermia is associated with severe complications and high mortality in elective operations. Surgery. 2014;156(5): doi: /j.surg Kim YS, Jeon YS, Lee JA, et al. Intra-operative warming with a forced-air warmer in preventing hypothermia after tourniquet deflation in elderly patients. J Int Med Res. 2009;37(5): doi: / Parodi D, Tobar C, Valderrama J, et al. Hip arthroscopy and hypothermia. Arthroscopy. 2012;28(7): doi: /j.arthro Kurz A, Sessler DI, Christensen R, Dechert M. Heat balance and distribution during the coretemperature plateau in anesthetized humans. Anesthesiology. 1995;83(3): Vaughan MS, Vaughan RW, Cork RC. Postoperative hypothermia in adults: relationship of age, anesthesia, and shivering to rewarming. Anesth Analg. 1981;60(10): American Society of PeriAnesthesia Nurses. Clinical guideline for the prevention of unplanned perioperative hypothermia. J Perianesth Nurs. 2001;16(5): Inaba K, Berg R, Barmparas G, et al. Prospective evaluation of ambient operating room temperature on the core temperature of injured patients undergoing emergent surgery. J Trauma Acute Care Surg. 2012;73(6): doi: /ta.0b013e db Barie PS. Surgical site infections: epidemiology and prevention. Surg Infect (Larchmt). 2002;3 Suppl 1:S9-S21. doi: /sur s Jeran L. Patient temperature: an introduction to the clinical guideline for the prevention of unplanned perioperative hypothermia. J Perianesth Nurs. 2001;16(5): Kurz A, Sessler DI, Lenhardt R. Perioperative normothermia to reduce the incidence of surgical-wound infection and shorten hospitalization. Study of Wound Infection and Temperature Group. N Engl J Med. 1996;334(19): Alderson P, Campbell G, Smith AF, Warttig S, Nicholson A, Lewis SR. Thermal insulation for preventing inadvertent perioperative hypothermia. Cochrane Database Syst Rev. 2014;6:CD doi: / cd pub Berry D, Wick C, Magons P. A clinical evaluation of the cost and time effectiveness of the ASPAN Hypothermia Guideline. J Perianesth Nurs. 2008;23(1): doi: /j.jopan Kimberger O, Held C, Stadelmann K et al. Resistive polymer versus forced-air warming: comparable heat transfer and core rewarming rates in volunteers. Anesth Analg. 2008;107(5): Apr 2019 The American Journal of Orthopedics 8
9 doi: /ane.0b013e Brandt S, Oguz R, Hüttner H, et al. Resistive-polymer versus forced-air warming: comparable efficacy in orthopedic patients. Anesth Analg. 2010;110(3): doi: /ane.0b013e3181cb3f5f. 23. Legg AJ, Hammer AJ. Forced-air patient warming blankets disrupt unidirectional airflow. Bone Joint J. 2013;95-B(3): doi: / x.95b Dasari KB, Albrecht M, Harper M. Effect of forced-air warming on the performance of operating theatre laminar flow ventilation. Anaesthesia. 2012;67(3): doi: /j x. 25. Belani KG, Albrecht M, McGovern PD, Reed M, Nachtsheim C. Patient warming excess heat: the effects on orthopedic operating room ventilation performance. Anesth Analg. 2013;117(2): doi: /ane.0b013e31825f81e Legg AJ, Cannon T, Hammer AJ. Do forced air patient-warming devices disrupt unidirectional downward airflow? J Bone Joint Surg Br. 2012;94(2): doi: / x.94b Albrecht M, Gaithier RL, Belani K, Litchy M, Leaper D. Forced-air warming blowers: An evaluation of filtration adequacy and airborne contamination emissions in the operating room. Am J Infect Control. 2011;39(4): doi: /j.ajic Reed M, Kimberger O, McGovern PD, Albrecht MC. Forced-air warming design: evaluation of intake filtration, internal microbial buildup, and airborne-contamination emissions. AANA J. 2013;81(4): McGovern PD, Albercht M, Belani KG, et al. Forced-air warming and ultra-clean ventilation do not mix: an investigation of theatre ventilation, patient warming and joint replacement infection in orthopaedics. J Bone Joint Surg Br.2011;93(11): doi: / x.93b Multimedia Product Guide Product Guide STRATAFIX Symmetric PDS Plus Knotless Tissue Control Device STRATAFIX Spiral Knotless Tissue Control Device BioComposite SwiveLock Anchor BioComposite SwiveLock C, with White/Black TigerTape Loop Apr 2019 The American Journal of Orthopedics 9
10 Citation Chandrakanth Boddu, MD Joseph Cushner Giles R. Scuderi, MD. Inadvertent Perioperative Hypothermia During Orthopedic Surgery. Am J Orthop. Publish date: July 12, 2018 Chandrakanth Boddu, MD Apr 2019 The American Journal of Orthopedics 10
TEMPERATURE MANAGEMENT
 TEMPERATURE MANAGEMENT Unintentional Hypothermia and the Maintenance of Normothermia Ian Sampson, M.D. SURGICAL CARE IMPROVEMENT PROJECT Temperature Management SCIP INF 7: Colorectal surgery patients with
TEMPERATURE MANAGEMENT Unintentional Hypothermia and the Maintenance of Normothermia Ian Sampson, M.D. SURGICAL CARE IMPROVEMENT PROJECT Temperature Management SCIP INF 7: Colorectal surgery patients with
3M Bair Hugger System is Safe and Effective Patient Warming Therapy - Response to Misstatements in Lawsuits, September 2016
 3M Bair Hugger System is Safe and Effective Patient Warming Therapy - Response to Misstatements in Lawsuits, September 2016 3M is sympathetic to patients who experience surgical site infections. Any surgery
3M Bair Hugger System is Safe and Effective Patient Warming Therapy - Response to Misstatements in Lawsuits, September 2016 3M is sympathetic to patients who experience surgical site infections. Any surgery
Instituting preventive warming measures for patients who are normothermic. A variety of measures may be used, unless contraindicated.
 Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
Postoperative hypothermia in geriatric patients undergoing arthroscopic shoulder surgery
 Anesth Pain Med 2019;14:112-116 https://doi.org/10.17085/apm.2019.14.1.112 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received May 18, 2018 Revised 1st, July 12, 2018 2nd, August 4, 2018 Accepted
Anesth Pain Med 2019;14:112-116 https://doi.org/10.17085/apm.2019.14.1.112 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received May 18, 2018 Revised 1st, July 12, 2018 2nd, August 4, 2018 Accepted
The cold never bother me anymore. R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit
 The cold never bother me anymore R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit Is that really true? Frozen by Walt Disney Animation Studios, 2013 Definition
The cold never bother me anymore R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit Is that really true? Frozen by Walt Disney Animation Studios, 2013 Definition
Temperature Monitoring Locations: For TEMP 01, any temperature measurement coming from a physiologic monitor will suffice (peripheral or core).
 Measure Abbreviation: TEMP 01 Measure Description: Percentage of cases that active warming was administered by the anesthesia provider. NQS Domain: Effective Clinical Care Measure Type: Process Scope:
Measure Abbreviation: TEMP 01 Measure Description: Percentage of cases that active warming was administered by the anesthesia provider. NQS Domain: Effective Clinical Care Measure Type: Process Scope:
03RC1- Greif. Temperature Monitoring. Robert Greif - 1 -
 03RC1- Greif Temperature Monitoring Robert Greif Department of Anaesthesiology and Pain Therapy, University Hospital Bern, Inselspital Bern, Switzerland Small decreases of core body temperature during
03RC1- Greif Temperature Monitoring Robert Greif Department of Anaesthesiology and Pain Therapy, University Hospital Bern, Inselspital Bern, Switzerland Small decreases of core body temperature during
Postoperative hypothermia and patient outcomes after elective cardiac surgery
 doi:10.1111/j.1365-2044.2011.06784.x ORIGINAL ARTICLE Postoperative hypothermia and patient outcomes after elective cardiac surgery D. Karalapillai, 1 D. Story, 2 G. K. Hart, 3,4 M. Bailey, 5 D. Pilcher,
doi:10.1111/j.1365-2044.2011.06784.x ORIGINAL ARTICLE Postoperative hypothermia and patient outcomes after elective cardiac surgery D. Karalapillai, 1 D. Story, 2 G. K. Hart, 3,4 M. Bailey, 5 D. Pilcher,
British Journal of Anaesthesia 101 (5): (2008) doi: /bja/aen272 Advance Access publication September 26, 2008
 British Journal of Anaesthesia 101 (5): 627 31 (2008) doi:10.1093/bja/aen272 Advance Access publication September 26, 2008 CLINICAL PRACTICE Effect of prewarming on post-induction core temperature and
British Journal of Anaesthesia 101 (5): 627 31 (2008) doi:10.1093/bja/aen272 Advance Access publication September 26, 2008 CLINICAL PRACTICE Effect of prewarming on post-induction core temperature and
Infusion of Warm Fluid During Abdominal Surgery Prevents Hypothermia and Postanaesthetic Shivering
 I.J. Engineering and Manufacturing 2011, 5, 26-30 Published Online October 2011 in MECS (http://www.mecs-press.net) DOI: 10.5815/ijem.2011.05.04 Available online at http://www.mecs-press.net/ijem Infusion
I.J. Engineering and Manufacturing 2011, 5, 26-30 Published Online October 2011 in MECS (http://www.mecs-press.net) DOI: 10.5815/ijem.2011.05.04 Available online at http://www.mecs-press.net/ijem Infusion
Underbody Forced-air Warmer Blanket Is Superior to Overbody Blanket in Preventing Hypothermia During Laparoscopic Donor Nephrectomy
 Underbody Forced-air Warmer Blanket Is Superior to Overbody Blanket in Preventing Hypothermia During Laparoscopic Donor Nephrectomy Ryohei Miyazaki 1, Kengo Hayamizu 1 and Sumio Hoka 2** Abstract Background:
Underbody Forced-air Warmer Blanket Is Superior to Overbody Blanket in Preventing Hypothermia During Laparoscopic Donor Nephrectomy Ryohei Miyazaki 1, Kengo Hayamizu 1 and Sumio Hoka 2** Abstract Background:
The Flint Lock: A Novel Technique in Total Knee Arthroplasty Closure
 The Flint Lock: A Novel Technique in Total Knee Arthroplasty Closure Publish date: September 13, 2018 Authors: Jeffrey B. Peck, MD Paul M. Charpentier, MD Sherry K. Bowman, ANP-BC Ajay K. Srivastava, MD
The Flint Lock: A Novel Technique in Total Knee Arthroplasty Closure Publish date: September 13, 2018 Authors: Jeffrey B. Peck, MD Paul M. Charpentier, MD Sherry K. Bowman, ANP-BC Ajay K. Srivastava, MD
2011 Arizant Healthcare Inc. All Rights Reserved A 01/ Arizant Healthcare Inc. All Rights Reserved A 01/11
 Infection Prevention Division Essentials EDU Learning Program UNINTENDED HYPOTHERMIA: THE IMPORTANCE OF MAINTAINING NORMOTHERMIA Disclosure Sponsored by Arizant Healthcare Inc., a 3M company 3M Health
Infection Prevention Division Essentials EDU Learning Program UNINTENDED HYPOTHERMIA: THE IMPORTANCE OF MAINTAINING NORMOTHERMIA Disclosure Sponsored by Arizant Healthcare Inc., a 3M company 3M Health
Hypothermia Presentation
 Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Peri-Operative Management: Guidelines for Inpatient Management of Children with Sickle Cell Disease
 Version 02 Approved by Interprofessional Patient Care Committee: September 16, 2016 1.0 Background Children with Sickle Cell are at risk of developing post-operative Acute Chest Syndrome. With improvements
Version 02 Approved by Interprofessional Patient Care Committee: September 16, 2016 1.0 Background Children with Sickle Cell are at risk of developing post-operative Acute Chest Syndrome. With improvements
Original Article. Postoperative hypothermia and patient outcomes after major elective non-cardiac surgery. Abstract
 Original Article doi:10.1111/anae.12129 Postoperative and patient outcomes after major elective non-cardiac surgery D. Karalapillai, 1 D. Story, 2 G. K. Hart, 3 M. Bailey, 4 D. Pilcher, 5 A. Schneider,
Original Article doi:10.1111/anae.12129 Postoperative and patient outcomes after major elective non-cardiac surgery D. Karalapillai, 1 D. Story, 2 G. K. Hart, 3 M. Bailey, 4 D. Pilcher, 5 A. Schneider,
PERIOPERATIVE HYPOTHERMIA PREVENTION IN BURN PATIENTS
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
Clinical evidence of prewarming patients.
 3M TM Patient Temperature Solutions Clinical evidence of prewarming patients.. Modern perioperative thermal management aims at the prevention of hypothermia during the whole perioperative process to protect
3M TM Patient Temperature Solutions Clinical evidence of prewarming patients.. Modern perioperative thermal management aims at the prevention of hypothermia during the whole perioperative process to protect
Most patients undergoing surgical procedures. Conductive Skin Warming and Hypothermia: An Observational Study
 Conductive Skin Warming and Hypothermia: An Observational Study Victoria M. Steelman, PhD, RN, CNOR, FAAN Ann G. Schaapveld, BSN, RN Yelena Perkhounkova, PhD Jennifer L. Reeve, MSN, RN John P. Herring,
Conductive Skin Warming and Hypothermia: An Observational Study Victoria M. Steelman, PhD, RN, CNOR, FAAN Ann G. Schaapveld, BSN, RN Yelena Perkhounkova, PhD Jennifer L. Reeve, MSN, RN John P. Herring,
Thermal suits as an alternative way to keep patients warm peri-operatively: a randomised trial Eila A. Hirvonen and Minnaliisa Niskanen
 ORIGINAL ARTICLE Thermal suits as an alternative way to keep patients warm peri-operatively: a randomised trial Eila A. Hirvonen and Minnaliisa Niskanen Background and objective Unintentional hypothermia
ORIGINAL ARTICLE Thermal suits as an alternative way to keep patients warm peri-operatively: a randomised trial Eila A. Hirvonen and Minnaliisa Niskanen Background and objective Unintentional hypothermia
Resistive Heating during Off-Pump Coronary Bypass Surgery
 (Acta Anaesth. Belg., 2007, 58, 27-31) Resistive Heating during Off-Pump Coronary Bypass Surgery S. ENGELEN, J.BERGHMANS, S.BORMS, M.SUY-VERBURG and D. HIMPE Summary : Background : Maintaining normothermia
(Acta Anaesth. Belg., 2007, 58, 27-31) Resistive Heating during Off-Pump Coronary Bypass Surgery S. ENGELEN, J.BERGHMANS, S.BORMS, M.SUY-VERBURG and D. HIMPE Summary : Background : Maintaining normothermia
Spinal anesthesia significantly impairs thermoregulation
 MISCELLANEOUS Effect of Preoperative Forced-Air Warming on Hypothermia in Elderly Patients Undergoing Transurethral Resection of the Prostate Youn Yi Jo, Young Jin Chang, Yong Beom Kim, Sehwan Lee, Hyun
MISCELLANEOUS Effect of Preoperative Forced-Air Warming on Hypothermia in Elderly Patients Undergoing Transurethral Resection of the Prostate Youn Yi Jo, Young Jin Chang, Yong Beom Kim, Sehwan Lee, Hyun
8 CONSEQUENCES OF HYPOTHERMIA REVIEW
 1 8 CONSEQUENCES OF HYPOTHERMIA REVIEW Clinical Question: What are the consequences of inadvertent perioperative hypothermia? 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29
1 8 CONSEQUENCES OF HYPOTHERMIA REVIEW Clinical Question: What are the consequences of inadvertent perioperative hypothermia? 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29
Mild hypothermia causes numerous serious
 Insufficiency in a New Temporal-Artery Thermometer for Adult and Pediatric Patients Mohammad-Irfan Suleman, MD*, Anthony G. Doufas, MD, PhD*, Ozan Akça, MD*, Michel Ducharme, PhD, and Daniel I. Sessler,
Insufficiency in a New Temporal-Artery Thermometer for Adult and Pediatric Patients Mohammad-Irfan Suleman, MD*, Anthony G. Doufas, MD, PhD*, Ozan Akça, MD*, Michel Ducharme, PhD, and Daniel I. Sessler,
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Materials and Methods
 1330 Anesthesiology 2000; 92:1330 4 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Predictors of Hypothermia during Spinal Anesthesia Steven M. Frank, M.D.,* Hossam
1330 Anesthesiology 2000; 92:1330 4 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Predictors of Hypothermia during Spinal Anesthesia Steven M. Frank, M.D.,* Hossam
Transfusion & Mortality. Philippe Van der Linden MD, PhD
 Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
PATIENT CARE MANUAL. Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation
 PATIENT CARE MANUAL MANUAL CODE: SUBJECT: Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation DATE ISSUED: DATE REVISED: SUPERSEDES: CROSS REFERENCES:
PATIENT CARE MANUAL MANUAL CODE: SUBJECT: Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation DATE ISSUED: DATE REVISED: SUPERSEDES: CROSS REFERENCES:
Cost-Effective Solutions to Prevent Orthopedic Infections
 Cost-Effective Solutions to Prevent Orthopedic Infections Am J Orthop. 2012 May;41(5):E76-E77 Authors: Hsu AR Author Affiliation Disclosures Andrew R. Hsu, MD Download pdf The unprecedented rising cost
Cost-Effective Solutions to Prevent Orthopedic Infections Am J Orthop. 2012 May;41(5):E76-E77 Authors: Hsu AR Author Affiliation Disclosures Andrew R. Hsu, MD Download pdf The unprecedented rising cost
Dr.A.VASUKINATHAN THERMOREGULATION AND ANAESTHESIA:
 Dr.A.VASUKINATHAN In homeothermic species a thermoregulatory system co-ordinates defenses against cold and heat to maintain internal body temperature within a narrow range, thus optimizing normal physiologic
Dr.A.VASUKINATHAN In homeothermic species a thermoregulatory system co-ordinates defenses against cold and heat to maintain internal body temperature within a narrow range, thus optimizing normal physiologic
Association of Perioperative Hypothermia During Colectomy With Surgical Site Infection
 Research Original Investigation Association of Perioperative Hypothermia During Colectomy With Surgical Site Infection Rebeccah B. Baucom, MD; Sharon E. Phillips, MSPH; Jesse M. Ehrenfeld, MD, MPH; Roberta
Research Original Investigation Association of Perioperative Hypothermia During Colectomy With Surgical Site Infection Rebeccah B. Baucom, MD; Sharon E. Phillips, MSPH; Jesse M. Ehrenfeld, MD, MPH; Roberta
Abstract. Key words: Hypothermia, active warming, forced air warming, general anesthesia
 Assessing the effect of warming up the patient with forced air on the body central temperature during general anesthesia in patients aged 20-70 years under eye surgery in Farabi Hospital Anahide Maleki
Assessing the effect of warming up the patient with forced air on the body central temperature during general anesthesia in patients aged 20-70 years under eye surgery in Farabi Hospital Anahide Maleki
HYPOTHERMIA IN TRAUMA. Kevin Palmer EMT-P, DiMM
 HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
Patient consent for peripheral nerve blocks
 Patient consent for peripheral nerve blocks 1 Membership of Working Party Dr Anand Sardesai Dr James French Dr Amit Pawa Consultant Anaesthetist, Cambridge, UK Consultant Anaesthetist, Nottingham, UK Consultant
Patient consent for peripheral nerve blocks 1 Membership of Working Party Dr Anand Sardesai Dr James French Dr Amit Pawa Consultant Anaesthetist, Cambridge, UK Consultant Anaesthetist, Nottingham, UK Consultant
Key points. S. Perez-Protto 1, D. I. Sessler 2 *, L. F. Reynolds 3, M. H. Bakri 4, E. Mascha 2, J. Cywinski 1, B. Parker 1 and M.
 British Journal of Anaesthesia 105 (4): 466 70 (2010) Advance Access publication 3 August 2010. doi:10.1093/bja/aeq170 Circulating-water garment or the combination of a circulating-water mattress and forced-air
British Journal of Anaesthesia 105 (4): 466 70 (2010) Advance Access publication 3 August 2010. doi:10.1093/bja/aeq170 Circulating-water garment or the combination of a circulating-water mattress and forced-air
Section 3: Shivering. Risks associated with your anaesthetic. What causes it?
 Risks associated with your anaesthetic Section 3: Shivering Summary This leaflet explains the causes of shivering following anaesthesia and surgery, what can be done to prevent it occurring, and treatments
Risks associated with your anaesthetic Section 3: Shivering Summary This leaflet explains the causes of shivering following anaesthesia and surgery, what can be done to prevent it occurring, and treatments
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers
 Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
Multi-Modal Pain Control in Ambulatory Hand Surgery
 Multi-Modal Pain Control in Ambulatory Hand Surgery Publish date: June 8, 2018 Authors: Ryan K. Harrison, MD Teresa DiMeo, RN, MS, CNP, CNOR Ryan D. Klinefelter, MD Michael E. Ruff, MD Hisham M. Awan,
Multi-Modal Pain Control in Ambulatory Hand Surgery Publish date: June 8, 2018 Authors: Ryan K. Harrison, MD Teresa DiMeo, RN, MS, CNP, CNOR Ryan D. Klinefelter, MD Michael E. Ruff, MD Hisham M. Awan,
Neurotrauma: The Place for Cooling
 Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
8/20/12. Discuss the importance of thermoregulation in the neonate.
 Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Comparison of resistive heating and forced-air warming to prevent inadvertent perioperative hypothermia
 British Journal of Anaesthesia, 116 (2): 249 54 (2016) doi: 10.1093/bja/aev412 Clinical Practice Comparison of resistive heating and forced-air warming to prevent inadvertent perioperative hypothermia
British Journal of Anaesthesia, 116 (2): 249 54 (2016) doi: 10.1093/bja/aev412 Clinical Practice Comparison of resistive heating and forced-air warming to prevent inadvertent perioperative hypothermia
Measure Applications Partnership. Hospital Workgroup In-Person Meeting Follow- Up Call
 Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
Surgical Site Infections: the international guidelines for best practices and effective actions
 Surgical Site Infections: the international guidelines for best practices and effective actions SSIs are the second most common type of adverse event occurring in hospitalised patients. SSIs have been
Surgical Site Infections: the international guidelines for best practices and effective actions SSIs are the second most common type of adverse event occurring in hospitalised patients. SSIs have been
Maintenance of normothermia at operation room temperature of 24 C in adult and pediatric patients undergoing liver transplantation
 Transplant International ISSN 0934-0874 ORIGINAL ARTICLE Maintenance of normothermia at operation room temperature of 24 C in adult and pediatric patients undergoing liver transplantation Chia-Jung Huang
Transplant International ISSN 0934-0874 ORIGINAL ARTICLE Maintenance of normothermia at operation room temperature of 24 C in adult and pediatric patients undergoing liver transplantation Chia-Jung Huang
Patient Case. Post cardiac arrest pathophysiology 10/19/2017. Disclosure. Objectives. Patient Case-TM
 Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Prevention of Hypothermia During Interventional Cardiology Procedures in Adults
 ISPUB.COM The Internet Journal of Anesthesiology Volume 23 Number 2 Prevention of Hypothermia During Interventional Cardiology Procedures in Adults K Wagner, C Smith, K Quan Citation K Wagner, C Smith,
ISPUB.COM The Internet Journal of Anesthesiology Volume 23 Number 2 Prevention of Hypothermia During Interventional Cardiology Procedures in Adults K Wagner, C Smith, K Quan Citation K Wagner, C Smith,
If not actively warmed, most surgical patients become
 Technology, Computing, and Simulation Section Editor: Jeffrey M. Feldman New Circulating-Water Devices Warm More Quickly than Forced-Air in Volunteers Anupama Wadhwa, MD* Ryu Komatsu, MD Mukadder Orhan-Sungur,
Technology, Computing, and Simulation Section Editor: Jeffrey M. Feldman New Circulating-Water Devices Warm More Quickly than Forced-Air in Volunteers Anupama Wadhwa, MD* Ryu Komatsu, MD Mukadder Orhan-Sungur,
-Blood Warming- A Hot topic?
 -Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
-Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
Anaesthesia for the Over 75s. Chris Edge
 Anaesthesia for the Over 75s Chris Edge Topics to be Covered Post-operative cognitive management Morbidity and mortality General anaesthesia a good idea or not? Multiple comorbidities and assessment of
Anaesthesia for the Over 75s Chris Edge Topics to be Covered Post-operative cognitive management Morbidity and mortality General anaesthesia a good idea or not? Multiple comorbidities and assessment of
Pain Management Protocol in Adolescent Idiopathic Spinal Fusion Reduces Length of Stay and Complications
 Pain Management Protocol in Adolescent Idiopathic Spinal Fusion Reduces Length of Stay and Complications Abstract Authors: Karen Martin, RHIT, CPHQ - Surgical Clinical Reviewer - Quality Management Analyst,
Pain Management Protocol in Adolescent Idiopathic Spinal Fusion Reduces Length of Stay and Complications Abstract Authors: Karen Martin, RHIT, CPHQ - Surgical Clinical Reviewer - Quality Management Analyst,
Department of Anaesthesiology, Erasmus University Medical Center, Rotterdam, The Netherlands
 Intravenous device feasible for controlled cooling and rewarming of individuals with abnormal body core temperature A. Struijs 1, F. De Ruiter 1, A. Weijerse 1, J. Klein 2, A.J.J.C. Bogers 1 1 Department
Intravenous device feasible for controlled cooling and rewarming of individuals with abnormal body core temperature A. Struijs 1, F. De Ruiter 1, A. Weijerse 1, J. Klein 2, A.J.J.C. Bogers 1 1 Department
Contraindications to time critical surgery; when not to proceed from the perspective of: The Physician A/Prof Peter Morley
 Contraindications to time critical surgery; when not to proceed from the perspective of: The Physician A/Prof Peter Morley British Journal of Surgery 2013; 100: 1045 1049 The risk of 30 day mortality
Contraindications to time critical surgery; when not to proceed from the perspective of: The Physician A/Prof Peter Morley British Journal of Surgery 2013; 100: 1045 1049 The risk of 30 day mortality
UTSW/BioTel EMS TRAINING BULLETIN January EMS TB Accidental Hypothermia
 UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
Anesthesia for Total Hip and Knee Arthroplasty
 Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
Disclosure. Objectives 9/13/2018. NIA/NIH 1R03AG (PI-Bentov) More than Start low go slow. start low go slow
 Sedation and analgesia in geriatric trauma Sept 2018 Itay Bentov MD PhD Disclosure NIA/NIH 1R03AG042353 (PI-Bentov) More than Start low go slow start low go slow Objectives List age-related physiologic
Sedation and analgesia in geriatric trauma Sept 2018 Itay Bentov MD PhD Disclosure NIA/NIH 1R03AG042353 (PI-Bentov) More than Start low go slow start low go slow Objectives List age-related physiologic
SSI. Ren yu Zhang MD
 Ren yu Zhang MD 3 27 2014 1 SSI 16 million operative procedures in 2010. Overall SSI rate 1.9% for 2006 8. Accounts 31% of healthcare associated infection. Leads to further morbidity and mortality. Economic
Ren yu Zhang MD 3 27 2014 1 SSI 16 million operative procedures in 2010. Overall SSI rate 1.9% for 2006 8. Accounts 31% of healthcare associated infection. Leads to further morbidity and mortality. Economic
Investigation performed at the University of Rochester, Department of Orthopaedics and Rehabilitation, Rochester, NY USA
 Intra-articular cocktail offers clinical advantages over femoral nerve block for postoperative analgesia in patients undergoing arthroscopic hip surgery Sean Childs, MD; Sonia Pyne, MD; Kiritpaul Nandra,
Intra-articular cocktail offers clinical advantages over femoral nerve block for postoperative analgesia in patients undergoing arthroscopic hip surgery Sean Childs, MD; Sonia Pyne, MD; Kiritpaul Nandra,
Materials and Methods
 Anesthesiology 2004; 100:1058 64 2004 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Effects of a Circulating-water Garment and Forced-air Warming on Body Heat Content
Anesthesiology 2004; 100:1058 64 2004 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Effects of a Circulating-water Garment and Forced-air Warming on Body Heat Content
Ac#ve, ECMO or locally available alterna#ves. invasive warming. Ini#ally: Ac#ve noninvasive or minimally
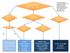 Suspected Hypothermia Temp
Suspected Hypothermia Temp
Anesthesia Impact on Perioperative Outcomes
 Anesthesia Impact on Perioperative Outcomes David L. Reich, M.D. Hospital President and COO Professor of Anesthesiology Icahn School of Medicine at Mount Sinai New York, NY 2000: Institute of Medicine
Anesthesia Impact on Perioperative Outcomes David L. Reich, M.D. Hospital President and COO Professor of Anesthesiology Icahn School of Medicine at Mount Sinai New York, NY 2000: Institute of Medicine
Evidence-Based Recommendations for Intraoperative Prevention of SSI. Intraoperative Antiseptic Skin Preparation of the Patient
 Sven Scheffler, MD PhD Sporthopaedicum Berlin, Germany Symposium: Prevention and Management of Infection in ACL Reconstruction General Considerations for Prevention of Infection Intraoperative Precautions
Sven Scheffler, MD PhD Sporthopaedicum Berlin, Germany Symposium: Prevention and Management of Infection in ACL Reconstruction General Considerations for Prevention of Infection Intraoperative Precautions
Nanette Wells, DNSc., CRNA, APN Regional Director of CRNA Services, MidWest, NorthStar Anesthesia
 Nanette Wells, DNSc., CRNA, APN Regional Director of CRNA Services, MidWest, NorthStar Anesthesia 1 Definition of hypothermia: Body temperature below 95 F / 35 C (ranges 34 36) Normal temperature is 98.6
Nanette Wells, DNSc., CRNA, APN Regional Director of CRNA Services, MidWest, NorthStar Anesthesia 1 Definition of hypothermia: Body temperature below 95 F / 35 C (ranges 34 36) Normal temperature is 98.6
Outcomes of Patients with Preoperative Weight Loss following Colorectal Surgery
 Outcomes of Patients with Preoperative Weight Loss following Colorectal Surgery Zhobin Moghadamyeghaneh MD 1, Michael J. Stamos MD 1 1 Department of Surgery, University of California, Irvine Nothing to
Outcomes of Patients with Preoperative Weight Loss following Colorectal Surgery Zhobin Moghadamyeghaneh MD 1, Michael J. Stamos MD 1 1 Department of Surgery, University of California, Irvine Nothing to
The Impact of Perioperative Warming in an Outpatient Aesthetic Surgery Setting
 Research The Impact of Perioperative Warming in an Outpatient Aesthetic Surgery Setting Frank Lista, MD, FRCSC; Chris D. Doherty, MD; Richard M. Backstein, MD; and Jamil Ahmad, MD, FRCSC Aesthetic Surgery
Research The Impact of Perioperative Warming in an Outpatient Aesthetic Surgery Setting Frank Lista, MD, FRCSC; Chris D. Doherty, MD; Richard M. Backstein, MD; and Jamil Ahmad, MD, FRCSC Aesthetic Surgery
Patient Safety in Postbariatric Body Contouring. Karol A Gutowski, MD, FACS
 Patient Safety in Postbariatric Body Contouring Karol A Gutowski, MD, FACS Disclosures The Doctors Company - Advisory Board Angiotech/Quill - Advisory Board Suneva Medical Instructor Viora - Speaker Will
Patient Safety in Postbariatric Body Contouring Karol A Gutowski, MD, FACS Disclosures The Doctors Company - Advisory Board Angiotech/Quill - Advisory Board Suneva Medical Instructor Viora - Speaker Will
Pre-Operative Protocol
 Pre-Operative Protocol HAVE YOU OPTIMIZED YOUR PRE-OP PROTOCOL TO IMPROVE PATIENT OUTCOMES? 4/28/2017 Disclosure Sponsored by 3M Health Care 3M Health Care is a provider approved by the California Board
Pre-Operative Protocol HAVE YOU OPTIMIZED YOUR PRE-OP PROTOCOL TO IMPROVE PATIENT OUTCOMES? 4/28/2017 Disclosure Sponsored by 3M Health Care 3M Health Care is a provider approved by the California Board
Hemodynamic Optimization HOW TO IMPLEMENT?
 Hemodynamic Optimization HOW TO IMPLEMENT? Why Hemodynamic Optimization? Are post-surgical complications exceptions? Patients undergoing surgery may develop post-surgical complications. The morbidity rate,
Hemodynamic Optimization HOW TO IMPLEMENT? Why Hemodynamic Optimization? Are post-surgical complications exceptions? Patients undergoing surgery may develop post-surgical complications. The morbidity rate,
Cold Water Shock, Hypothermia and Cardiac Arrest
 Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
ENHANCED RECOVERY PROTOCOLS FOR KNEE REPLACEMENT
 ENHANCED RECOVERY PROTOCOLS FOR KNEE REPLACEMENT Jeff Gadsden, MD, FRCPC, FANZCA Associate Professor Duke University Department of Anesthesiology Regional Anesthesia and Acute Pain Medicine DISCLOSURES
ENHANCED RECOVERY PROTOCOLS FOR KNEE REPLACEMENT Jeff Gadsden, MD, FRCPC, FANZCA Associate Professor Duke University Department of Anesthesiology Regional Anesthesia and Acute Pain Medicine DISCLOSURES
TOTAL HIP AND KNEE REPLACEMENTS. FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES
 TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
Malnutrition: An independent Risk Factor for Postoperative Complications
 Malnutrition: An independent Risk Factor for Postoperative Complications Bryan P. Hooks, D.O. University of Pittsburgh-Horizon June 24, 2017 Orthopedic Surgeon-Adult Reconstruction Disclosures: None Objectives:
Malnutrition: An independent Risk Factor for Postoperative Complications Bryan P. Hooks, D.O. University of Pittsburgh-Horizon June 24, 2017 Orthopedic Surgeon-Adult Reconstruction Disclosures: None Objectives:
Anticoagulation for prevention of venous thromboembolism
 Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
Reducing Variation in Perioperative Fluid Utilization Results in Improved Surgical Outcomes
 Reducing Variation in Perioperative Fluid Utilization Results in Improved Surgical Outcomes A Quality Improvement and Cost Savings Initiative for Hospitals, Surgeons and Anesthesiologists Hypoperfusion
Reducing Variation in Perioperative Fluid Utilization Results in Improved Surgical Outcomes A Quality Improvement and Cost Savings Initiative for Hospitals, Surgeons and Anesthesiologists Hypoperfusion
Effects of Warming Therapy on Body Temperature in Spinal Surgery Patients
 Vol.128 (Healthcare and Nursing 2016), pp.18-22 http://dx.doi.org/10.14257/astl.2016. Effects of Warming Therapy on Body Temperature in Spinal Surgery Patients Keun Young Ham 1, Hye Young Ahn 2*, Hye Seon
Vol.128 (Healthcare and Nursing 2016), pp.18-22 http://dx.doi.org/10.14257/astl.2016. Effects of Warming Therapy on Body Temperature in Spinal Surgery Patients Keun Young Ham 1, Hye Young Ahn 2*, Hye Seon
Volumetric Considerations for Valving Long-Arm Casts: The Utility of the Cast Spacer
 Volumetric Considerations for Valving Long-Arm Casts: The Utility of the Cast Spacer Publish date: July 31, 2018 Authors: K. Aaron Shaw, DO, CPT, MC Colleen Moreland, DO, CPT, MC Shawn E. Boomsma, DO,
Volumetric Considerations for Valving Long-Arm Casts: The Utility of the Cast Spacer Publish date: July 31, 2018 Authors: K. Aaron Shaw, DO, CPT, MC Colleen Moreland, DO, CPT, MC Shawn E. Boomsma, DO,
An evaluation of underbody forced-air and resistive heating during hypothermic, on-pump cardiac surgery*
 doi:10.1111/j.1365-2044.2010.06609.x ORIGINAL ARTICLE An evaluation of underbody forced-air and resistive heating during hypothermic, on-pump cardiac surgery* S. Engelen, 1 D. Himpe, 1 S. Borms, 1 J. Berghmans,
doi:10.1111/j.1365-2044.2010.06609.x ORIGINAL ARTICLE An evaluation of underbody forced-air and resistive heating during hypothermic, on-pump cardiac surgery* S. Engelen, 1 D. Himpe, 1 S. Borms, 1 J. Berghmans,
Kenji Hasegawa Chiharu Negishi Fumitoshi Nakagawa Makoto Ozaki
 J Anesth (2012) 26:168 173 DOI 10.1007/s00540-011-1306-1 ORIGINAL ARTICLE Core temperatures during major abdominal surgery in patients warmed with new circulating-water garment, forced-air warming, or
J Anesth (2012) 26:168 173 DOI 10.1007/s00540-011-1306-1 ORIGINAL ARTICLE Core temperatures during major abdominal surgery in patients warmed with new circulating-water garment, forced-air warming, or
Recovery From Postoperative Hypothermia Predicts Survial in Extensively Burned Patients.
 Title Author(s) Recovery From Postoperative Hypothermia Predicts Survial in Extensively Burned Patients Shiozaki, Tadahiko Citation Issue Date Text Version ETD URL https://doi.org/1.1151/37591 DOI 1.1151/37591
Title Author(s) Recovery From Postoperative Hypothermia Predicts Survial in Extensively Burned Patients Shiozaki, Tadahiko Citation Issue Date Text Version ETD URL https://doi.org/1.1151/37591 DOI 1.1151/37591
Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study
 Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study J Quon, K Hynes, P Lapner, A Sheikh The Ottawa Hospital
Percutaneous Fluoroscopic Synovial Biopsy as a New Diagnostic Test for Periprosthetic Infection after Shoulder Arthroplasty: A Feasibility Study J Quon, K Hynes, P Lapner, A Sheikh The Ottawa Hospital
THE NATIONAL QUALITY FORUM
 THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
Damage control resuscitation from major haemorrhage in polytrauma
 Eur J Orthop Surg Traumatol (2014) 24:137 141 DOI 10.1007/s00590-013-1172-7 GENERAL REVIEW Damage control resuscitation from major haemorrhage in polytrauma William Carlino Received: 27 November 2012 /
Eur J Orthop Surg Traumatol (2014) 24:137 141 DOI 10.1007/s00590-013-1172-7 GENERAL REVIEW Damage control resuscitation from major haemorrhage in polytrauma William Carlino Received: 27 November 2012 /
Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review
 Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review Jon P Hedgecock MD, 1 P Christopher Cook MD FRCS(C), 1 John Harrast PhD,2 Judith F
Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review Jon P Hedgecock MD, 1 P Christopher Cook MD FRCS(C), 1 John Harrast PhD,2 Judith F
A review of the literature examining the relationship between temperature and infection in surgical wound healing
 A review of the literature examining the relationship between temperature and infection in surgical wound healing Tweed C Abstract Wound infection following surgery is a relatively common and serious complication.
A review of the literature examining the relationship between temperature and infection in surgical wound healing Tweed C Abstract Wound infection following surgery is a relatively common and serious complication.
Intrathecal meperidine reduces intraoperative shivering during transurethral prostatectomy in elderly patients
 Clinical Research Article Korean J Anesthesiol 010 December 59(6): 389-393 DOI: 10.4097/kjae.010.59.6.389 Intrathecal meperidine reduces intraoperative shivering during transurethral prostatectomy in elderly
Clinical Research Article Korean J Anesthesiol 010 December 59(6): 389-393 DOI: 10.4097/kjae.010.59.6.389 Intrathecal meperidine reduces intraoperative shivering during transurethral prostatectomy in elderly
Changes in Body Temperature during Anaesthesia
 Changes in Body Temperature during Anaesthesia T. M. Mufti ( Department of Anaesthesiology, A. M. College, Mil Hospital, Rawalpindi. ) Introduction Variable degree of changes occur in body temperature
Changes in Body Temperature during Anaesthesia T. M. Mufti ( Department of Anaesthesiology, A. M. College, Mil Hospital, Rawalpindi. ) Introduction Variable degree of changes occur in body temperature
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
New Strategies in the Management of Patients with Severe Sepsis
 New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
Role of evidence from observational studies in the process of health care decision making
 Role of evidence from observational studies in the process of health care decision making Jan van der Meulen Health Services Research Unit London School of Hygiene and Tropical Medicine Clinical Effectiveness
Role of evidence from observational studies in the process of health care decision making Jan van der Meulen Health Services Research Unit London School of Hygiene and Tropical Medicine Clinical Effectiveness
Geriatric (Orthopaedic) Trauma
 Geriatric (Orthopaedic) Trauma Brian Buck, DO March 3, 2017 31st Annual Geriatric Conference Pearls of Geriatric Care Do not regret growing older. It is a privilege denied to most Overview East Guidelines
Geriatric (Orthopaedic) Trauma Brian Buck, DO March 3, 2017 31st Annual Geriatric Conference Pearls of Geriatric Care Do not regret growing older. It is a privilege denied to most Overview East Guidelines
AMI Talking Points. Provide appropriate treatment to Acute MI patients with these core measures:
 AMI Provide appropriate treatment to Acute MI patients with these core measures: Aspirin received within 24 hours of arrival or contraindication documented Primary PCI Received Within 90 Minutes of Hospital
AMI Provide appropriate treatment to Acute MI patients with these core measures: Aspirin received within 24 hours of arrival or contraindication documented Primary PCI Received Within 90 Minutes of Hospital
The effect of electrically heated humidifier on the body temperature and blood loss in spinal surgery under general anesthesia
 Clinical Research Article Korean J Anesthesiol 2011 August 61(2): 112-116 http://dx.doi.org/10.4097/kjae.2011.61.2.112 The effect of electrically heated humidifier on the body temperature and blood loss
Clinical Research Article Korean J Anesthesiol 2011 August 61(2): 112-116 http://dx.doi.org/10.4097/kjae.2011.61.2.112 The effect of electrically heated humidifier on the body temperature and blood loss
A comparison of peri-operative outcomes between elective and non-elective total hip arthroplasties
 Original Article Page 1 of 8 A comparison of peri-operative outcomes between elective and non-elective total hip arthroplasties Hiba K. Anis 1, Nipun Sodhi 2, Marine Coste 2, Joseph O. Ehiorobo 2, Jared
Original Article Page 1 of 8 A comparison of peri-operative outcomes between elective and non-elective total hip arthroplasties Hiba K. Anis 1, Nipun Sodhi 2, Marine Coste 2, Joseph O. Ehiorobo 2, Jared
Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty
 Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty A Review of ACS-NSQIP 2006-2012 Arjun Sebastian, M.D., Stephanie Polites, M.D., Kristine Thomsen, B.S., Elizabeth Habermann,
Predicting Short Term Morbidity following Revision Hip and Knee Arthroplasty A Review of ACS-NSQIP 2006-2012 Arjun Sebastian, M.D., Stephanie Polites, M.D., Kristine Thomsen, B.S., Elizabeth Habermann,
How to Address an Inappropriately high Mortality Rate? Joe Sharma, MD Associate Professor of Surgery NSQIP Surgical Champion
 How to Address an Inappropriately high Mortality Rate? Joe Sharma, MD Associate Professor of Surgery NSQIP Surgical Champion Disclosure Slide No COI and no disclosures. Hospital Mortality rate : is it
How to Address an Inappropriately high Mortality Rate? Joe Sharma, MD Associate Professor of Surgery NSQIP Surgical Champion Disclosure Slide No COI and no disclosures. Hospital Mortality rate : is it
SCIP-Inf-10. Pediatric Warming Solutions. Complete. Pediatric Warming
 Pediatric Warming Solutions SCIP-Inf-10 goals achieve Complete Pediatric Warming You know the importance of keeping your littlest patients warm, so why trust them to anyone but the leader in patient warming?
Pediatric Warming Solutions SCIP-Inf-10 goals achieve Complete Pediatric Warming You know the importance of keeping your littlest patients warm, so why trust them to anyone but the leader in patient warming?
Show Me the Evidence: Epidurals, PVBs, TAP Blocks Christopher L. Wu, MD Professor of Anesthesiology The Johns Hopkins Hospital
 Show Me the Evidence: Epidurals, PVBs, TAP Blocks Christopher L. Wu, MD Professor of Anesthesiology The Johns Hopkins Hospital Overview Review overall (ERAS and non-eras) data for EA, PVB, TAP Examine
Show Me the Evidence: Epidurals, PVBs, TAP Blocks Christopher L. Wu, MD Professor of Anesthesiology The Johns Hopkins Hospital Overview Review overall (ERAS and non-eras) data for EA, PVB, TAP Examine
Nurse Driven Fluid Optimization Using Dynamic Assessments
 Nurse Driven Fluid Optimization Using Dynamic Assessments 2016 1 WHAT WE BELIEVE We believe that clinicians make vital fluid and drug decisions every day with limited and inconclusive information Cheetah
Nurse Driven Fluid Optimization Using Dynamic Assessments 2016 1 WHAT WE BELIEVE We believe that clinicians make vital fluid and drug decisions every day with limited and inconclusive information Cheetah
Fast Track Surgery and Surgical Carepath in Optimising Colorectal Surgery. R Sim Centre for Advanced Laparoscopic Surgery, TTSH
 Fast Track Surgery and Surgical Carepath in Optimising Colorectal Surgery R Sim Centre for Advanced Laparoscopic Surgery, TTSH Conventional Surgery Postop care Nasogastric tube Enteral feeds when ileus
Fast Track Surgery and Surgical Carepath in Optimising Colorectal Surgery R Sim Centre for Advanced Laparoscopic Surgery, TTSH Conventional Surgery Postop care Nasogastric tube Enteral feeds when ileus
Regulation of Body Temperature. Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY
 Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
Accidental Hypothermia. Peter Paal, MD, Associate Professor DESA, EDIC
 Accidental Hypothermia Peter Paal, MD, Associate Professor DESA, EDIC Conflict of interest Ambu Covidien Genericon Jolife Laerdal Larnygeal Mask Company Ratiopharm VBM 2 Innsbruck 3 Innsbruck 4 Innsbruck
Accidental Hypothermia Peter Paal, MD, Associate Professor DESA, EDIC Conflict of interest Ambu Covidien Genericon Jolife Laerdal Larnygeal Mask Company Ratiopharm VBM 2 Innsbruck 3 Innsbruck 4 Innsbruck
