ORBIS International. Cataracts in Childhood
|
|
|
- Branden Gilmore
- 6 years ago
- Views:
Transcription
1 ORBIS International Cataracts in Childhood
2 Cataracts in Childhood Daniel E. Neely MD, M. Edward Wilson MD, David A. Plager MD and Itay Ben Zion, MD This manual is part of a series of specialized manuals produced by ORBIS Telemedicine, Cyber-Sight. Edited by: Eugene M. Helveston, MD Lynda M. Smallwood Illustrations by: Sharon Teal
3 Dedicated to All the children and their families November 2016
4 TABLE OF CONTENTS Introduction Classification of Pediatric Cataracts by Age of Onset Congenital Infantile Juvenile Morphology of Common Pediatric Cataracts Anterior Polar Cataract Anterior Subcapsular Cataract Lamellar Cataract Nuclear Cataract Posterior Subcapsular Cataract Posterior Lentiglobus (Posterior Lenticonus) Diffuse or Total Cataract Persistent Fetal Vasculature (PFV) Etiology of Pediatric Cataracts Idiopathic Hereditary Ocular Syndromes with Associated Cataracts Systemic Syndromes with Associated Cataracts Metabolic Cataracts Traumatic Cataracts Step-by-Step Approach for Pediatric Cataract Surgery Preoperative Routine Preoperative Laboratory Evaluation Preoperative Drops Examination of Both Eyes Under Anesthesia Intraocular Lens Calculations Cataract Surgery Techniques Cataract Surgery Without IOL in Children 4 Years of Age and Younger: Vitrector Technique.. 15 Cataract Surgery With IOL and Primary Posterior Capsulotomy Via Anterior Approach in Children 4 Years of Age and Younger: Vitrector Technique Cataract Surgery With IOL and Primary Posterior Capsulotomy Via Pars Plana Approach in Children 4 Years of Age and Younger: Vitrector Technique Cataract Surgery With IOL in Children 5 Years of Age and Older: Irrigation/Aspiration Technique (and no posterior capsulotomy or anterior vitrectomy) Postoperative Management of Pediatric Cataract Patients Postoperative Medications Postoperative Follow-Up Refractive Management Amblyopia Management Secondary Opacification of the Visual Axis Secondary IOL Implantation Long-Term Follow-Up Anesthesia for Pediatric Cataract Surgery Summary References
5
6 INTRODUCTION Appropriate management of the pediatric cataract patient presents the ophthalmic surgeon with a unique set of challenges. The entire process, from diagnosis and evaluation to surgical intervention and postoperative care, is significantly different from that of the typical adult cataract patient. This is highlighted by the need for close follow up and support, both by the family and the ophthalmologist, to help the child develop vision and avoid amblyopia by employing appropriate optical correction and regular visual stimulation. Therefore, while an ophthalmologist may be extremely skilled in performing adult cataract surgery, this does not ensure similar success in children. The purpose of this monograph is to describe the unique characteristics of congenital and childhood cataracts emphasizing the differences in treatment techniques compared with the adult cataract patient. The reader is offered a basic, standardized technique for approaching pediatric cataracts in early childhood. The techniques presented are not intended to be the only way to perform pediatric cataract surgery but are generally accepted and considered to be safe, effective, and relatively easy to master. From this basic technique, the reader is free to modify as needed to fit personal preferences and adapt to equipment and supplies available. Considering all of us have something to learn, we welcome your input. If you have a particular surgical tip or tool that you feel would benefit other pediatric cataract surgeons, please feel free to contact us with your suggestion. Also remember that the cataract removal is only the first step in the process. Refraction, amblyopia treatment, and frequent follow up visits monitoring the reaction of the eye, are essential steps leading to successful surgery. CLASSIFICATION OF PEDIATRIC CATARACTS BY AGE OF ONSET 1,2 ❶ Congenital: Present at birth ❷ Infantile: Develop within the first 2 years of life Juvenile: Develop before 10 years of age 1
7 MORPHOLOGY OF COMMON PEDIATRIC CATARACTS ❶ Anterior Polar Cataract Small (usually less than 1-2 mm) white opacity of the central anterior lens capsule i Usually do not increase in size over time Commonly bilateral Can be hereditary and present at birth Favorable visual prognosis i Patients may be found to have significant astigmatic refractive errors monitor refractive error and correct as needed ❷ Anterior Subcapsular Cataract Irregular, refractile or crystalline partial opacities usually seen just beneath the central anterior capsule May be secondary to radiation, uveitis, trauma or atopic skin disease i May require surgery if vision is reduced Lamellar Cataract Partial or complete opacity of the cortical layers surrounding the central lens nucleus 2 i Peripheral lens cortex may be clear i Commonly have an associated posterior capsule plaque opacity
8 Usually acquired and bilateral but may be asymmetric Opacity may initially be mild but tends to progressively worsen over time i Frequently has a more favorable visual prognosis compared to dense fetal nuclear cataracts that are more opaque at birth Lamellar opacities of cortex have a tendency to push forward out of the capsular bag during aspiration and irrigation of lens material Usually normal sized eyes ❹ Nuclear Cataract Central white opacity of the lens nucleus (area within the Y sutures; the Y is anterior and the posterior) i Peripheral cortex is usually clear but may have irregular opacification adjacent to the nucleus and this tends to worsen over time i Commonly have an associated posterior capsule plaque opacity Y Probably the most common type of congenital cataract Usually associated with mild microphthalmia or microcornea Severe impact on visual development unless removed at a very early age i Unilateral cataract ideally treated and optically corrected before 6 weeks of age i Bilateral cataract ideally treated and optically corrected before 8 weeks of age i Later treatment or delayed optical correction may result in irreversible amblyopia and nystagmus Surgery should be performed (if possible) before appearance of nystagmus Note that even in late presentation and with nystagmus, surgery usually has good results with favorable prognosis including attaining functional vision 3
9 ❺ Posterior Subcapsular Cataract Irregular, refractile or crystalline, partial opacities usually seen just beneath the central posterior capsule May be idiopathic but are most commonly seen secondary to radiation, trauma or chronic steroid use i While a less common cause, posterior subcapsular cataracts are frequently found in children with a diagnosis of Neurofibromatosis Type 2. Therefore, evaluation for this diagnosis should be considered if the etiology of a posterior subcapsular cataract is unexplained. May require a posterior capsulotomy (surgical or YAG-laser) to completely clear the visual axis ❻ Posterior Lentiglobus (Posterior Lenticonus) Bulging of the posterior capsule that is progressive over time and results in opacification of the overlying cortical lens material as the posterior capsule weakens i May result in a sudden total cataract if the posterior capsule ruptures Typically unilateral Not associated with microphthalmia or microcornea i Corneal diameter is normal and symmetric Delayed onset usually results in a more favorable visual prognosis Hydrodissection should be avoided during surgery as it may result in a large rupture of the thin and weakened posterior capsule. Even without hydrodissection, the central posterior capsule will frequently rupture during aspiration of lens material. The resulting defect tends to be round and centrally located. Therefore, it typically does not prevent placement of an intraocular lens if desired. During aspiration of the lens material, try to avoid collapse of the anterior chamber as this may push vitreous forward into the bag through the weakened posterior capsule. If this occurs, try to push the vitreous posterior with injection of viscoelastic to avoid engaging vitreous during aspiration of the remaining lens material. 4
10 ❼ Diffuse or Total Cataract Complete opacification of lens substance (nucleus and cortex) Usually the end-stage of partial cataracts (lamellar, nuclear, or posterior lentiglobus) that progress over time May also be secondary to trauma Lens may show resorption (in unilateral cases) i Liquification and dissipation of lens material leaves a thin, white membrane of fused anterior and posterior capsule. If no view of the posterior segment is possible, a B-scan ultrasound of the posterior segment is recommended to rule-out retinal detachment, intraocular mass or foreign body. Peeling of a calcified fibrotic plaque, if present, may result in capsule break but can usually be limited to the size of the plaque. ❽ Persistent Fetal Vasculature (PFV) Formerly called Persistent Hyperplastic Primary Vitreous (PHPV) Dense white vascular membrane at the posterior capsule and anterior vitreous, usually with attachments to the ciliary processes i Ciliary processes may be stretched Presentation is variable but there is usually a persistent hyaloid artery or stalk i This may extend all the way back to the optic nerve or may be a partial remnant See full description of PFV detailed later A minimal expression of persistent fetal vasculature is the Mittendorf dot which can be considered a variation of normal. 5
11 ETIOLOGY OF PEDIATRIC CATARACTS 3 ❶ Idiopathic: The majority (60%) of bilateral congenital/infantile cataracts are of unknown cause. ❷ Hereditary: Familial cataracts that are passed from one generation to the next Approximately 30% of bilateral congenital/infantile cataracts are hereditary Usually autosomal dominant transmission In these cases, cataracts are an isolated ocular finding with no other associated systemic pathology of other organ systems. Ocular Syndromes with Associated Cataracts: Some cataracts presenting primarily as ocular abnormalities may be associated with abnormalities elsewhere in the body. A few important examples include, but are not limited to, the following: 1,3,4,5 Aniridia i Bilateral absence of most or all iris tissue i Associated with cataract, glaucoma, corneal neovascularization, corneal scarring, foveal hypoplasia and nystagmus i Usually hereditary and autosomal dominant (2/3 of cases) The remaining 1/3 of cases are nonhereditary, sporadic, and are frequently associated with a deletion of chromosome 11 (mutation of PAX 6 gene). Because the gene for Wilm s tumor (WTI) is also nearby on chromosome 11, these children have a significant risk for developing Wilm s tumor during the first several years of childhood. If genetic testing is available, sporadic cases of aniridia should undergo this genetic testing to assess their relative risk of developing Wilm s tumor. Otherwise, serial abdominal ultrasounds and a careful evaluation by a pediatrician are recommended. Age 0 5 years, every 3 months Age 6 10 years, every 6 months Age 11 16, once yearly i While cataract formation is common in all cases of aniridia, it should be kept in mind that these patients usually have significant vision impairment from other factors such as the foveal hypoplasia and secondary nystagmus. Therefore, most mild to moderate cataracts in these patients do not require surgical intervention. 6
12 Peter s anomaly i Congenital central corneal opacity with underlying defects of the posterior corneal stroma, Descemet s membrane and endothelium Usually bilateral but asymmetrical Usually associated with secondary glaucoma May have adherent iris with keratolenticular contact and cataract Lens may be in place or it may be displaced anteriorly Microphthalmos i Small, malformed eye that may be unilateral or bilateral, sporadic or hereditary, isolated or sometimes associated with a systemic disorder i May have abnormalities of: Anterior segment (small corneal diameter, iris coloboma) Lens (cataract, coloboma) Posterior segment (persistent fetal vasculature, retinal dysplasia) i Vision may range from normal to no light perception i May be associated with CHARGE syndrome (Charge Association): Colobomatous microphthalmia Heart defects Atresia choanae Retarded growth and development Genital hypoplasia Ear malformation Persistent fetal vasculature (PFV) - formerly called persistent hyperplastic primary vitreous (PHPV) 1,6 i Variable malformation of the eye caused by an abnormal persistence of the fetal vasculature. May include some or all of the following clinical features: Persistent pupillary membrane Stretching of the ciliary processes Iridohyaloid blood vessels Persistence of the posterior fibrovascular sheath of the lens Persistent hyaloid artery Bergmeister papilla Congenital tent-shaped retinal detachment Macular abnormalities Optic nerve abnormalities Microphthalmos Mittendorf dot 7
13 i i Usually a sporadic, isolated abnormality of one eye only Most common cause of unilateral cataract in a smaller than normal eye Less than 10% are bilateral Only rarely associated with other systemic abnormalities Management requires release of traction on the ciliary body and retina Surgery is best performed by use of vitrectomy instrumentation to remove cataract, retrolental mass and the anterior portion of the persistent hyaloid stalk, either by an anterior (limbal) or posterior (pars plana) approach. Because these eyes tend to be significantly smaller and may have extensive capsular involvement, they frequently are not good candidates for placement of an intraocular lens. ❹ Systemic Syndromes with Associated Cataracts: These cataracts are associated with some other primary systemic pathology or abnormality of another organ system. A few important examples include, but are not limited to, the following: 7,8,9 Lowe syndrome (oculocerebralrenal syndrome) i X-linked recessive Patients mothers are typically carriers and may have asymptomatic, punctate or spoke-like lens opacities i Renal tubular dysfunction leads to metabolic acidosis, hyperparathyroidism and hypophosphatemia i Clinical manifestations: Cataract, in almost 100% of patients, frequently found with glaucoma and miotic pupils Mental retardation Bone demineralization and weakening (rickets) i Diagnosis is confirmed by identifying amino acids in the urine. Molecular genetic testing is also available. i Beyond treating the cataracts and glaucoma, management options are limited and patients have a significantly shortened lifespan. Marfan syndrome i Connective tissue disorder that is frequently autosomal dominant i Clinical manifestations: Lens subluxation is very common, approximately 80% Usually displaced superiorly Induces secondary lenticular myopia and astigmatism Cardiovascular problems are frequent and may be severe Aortic root dilation leads to aortic valve regurgitation and ascending aortic aneurysm Cardiology evaluation and echocardiogram are recommended 8
14 Skeletal abnormalities Arachnodactyly Joint laxity i Ocular management: Optical correction through either the phakic or aphakic portions of the pupil Surgical lensectomy if the lens edge bisects the pupil or if anterior displacement of the lens produces pupillary block glaucoma High risk for vitreous loss and retinal detachment Surgical risk is diminished by performing lensectomy with vitrectomy instruments. Patients are usually left aphakic (treated with glasses) but iris or scleral fixated IOLs may be a reasonable option for some patients. Down syndrome (Trisomy 21) i Small lens opacities are very common (50%) but the incidence of visually significant cataract requiring surgery is probably less than 5%. 4,5,6 Cataracts may be present at birth or may develop during the first decade of life. Opacities may be punctate, sutural, zonular or complete. ❺ Metabolic Cataracts: These are typically early onset cataracts (congenital, infantile or juvenile) associated with an underlying metabolic disorder. Early diagnosis and intervention are critical to preventing permanent systemic damage, particularly to the central nervous system. Important examples include, but are not limited to, the following: Galactosemia i Deficiency of galactose metabolism; patients are unable to convert ingested galactose to glucose. i Milk products containing lactose are the main source of the problematic galactose. Management involves a galactose restricted diet Early diagnosis and treatment prevents clinical manifestations of the disease i Autosomal recessive disorder of one of three enzymes: galactose-1-phosphate uridyltransferase (GALT) galactokinase (GALK) uridine diphosphate galactose-4 epimerase (GALE) i Clinical manifestations include: Cataract Typically bilateral oil droplet nuclear changes but may be cortical, lamellar or punctuate opacities. Opacity is secondary to accumulation of galactitol (dulcitol) in the lens 9
15 Liver dysfunction Jaundice Hepatomegally Elevated liver enzymes Renal tubular dysfunction Metabolic acidosis Galactosuria Glycosuria Albuminuria Amino aciduria i Prenatal screening for all three enzyme defects is available. i Preoperative metabolic screening for galactosemia in children with isolated congenital cataracts is not routinely indicated as long as the child appears to be otherwise in good health. Homocystinuria i Deficiency of cystathionine beta-synthase which interferes with methionine metabolism i Autosomal recessive inheritance i Clinical manifestations include: Ectopia lentis Bilateral, progressive lens dislocation Commonly displaced inferiorly or nasally May develop pupillary block glaucoma Osteoporosis Mental retardation in 50% Thromboembolism Patients are at an increased risk of morbidity with cataract surgery. i Early diagnosis and treatment with low methionine, cystine-supplemented diet is important to prevent or diminish clinical manifestations of the disease. Specific precautions should be undertaken to reduce the risk of thromboembolic phenomena at surgery including preoperative aspirin, vitamin B6 maintaining blood volume and compression stockings for the legs. ❻ Traumatic Cataracts: These can occur in children demonstrating a wide range of clinical appearance while having in common a history of trauma. Surgery must be appropriate for the condition of the eye. 10
16 STEP-BY-STEP APPROACH FOR PEDIATRIC CATARACT SURGERY ❶ Preoperative Routine Informed surgical consent stressing the need for postoperative follow-up care including parental (caregiver) involvement, need for appropriate optical correction, and a realistic discussion of any limitations of visual potential specific to each patient and type of cataract ❷ Preoperative Laboratory Evaluation Most pediatric cataract patients do not require an extensive laboratory evaluation. i Unilateral cataracts are most often secondary to an isolated ocular abnormality. i An otherwise apparently normal child with a family history of hereditary cataracts (frequently autosomal dominant) also does not require special laboratory evaluation. Children with bilateral, unexplained cataracts should preferably undergo a few basic laboratory studies: i TORCH titers: Toxoplasmosis Rubella Cytomegalovirus (CMV) Herpes i Syphilis screening More extensive metabolic, genetic or infectious disease workups should be reserved for children with other, usually obvious, systemic abnormalities and should be done in conjunction with a careful evaluation by a pediatrician. Congenital rubella syndrome (CRS) i It is particularly important to identify those children who may have cataract secondary to congenital rubella infection. Cataracts/congenital glaucoma Congenital heart disease Hearing impairment Pigmentary retinopathy Purpura Hepatosplenomegaly Jaundice Microcephaly 11
17 Developmental delay Meningoencephalitis Radiolucent bone disease i The cataractous lens (usually a nuclear type cataract) may serve as an infectious reservoir of live virus. Pregnant health care workers should not be allowed to care for children undergoing surgery for cataract secondary to suspected or confirmed CRS. i Because of the associated systemic disease, children with CRS may be at an increased risk for general anesthesia. i Children with CRS have a high risk of postoperative complications, including: Corneal edema and corneal opacification Secondary glaucoma Intense inflammation, uveitis May require prolonged postoperative steroids Probably best to avoid primary implantation of IOL s Preoperative Drops The pupil must be well-dilated at least one hour prior to surgery using locally available mydriatic or cycloplegic agents. Combinations of cyclopentolate, tropicamide, atropine and phenylephrine in various strengths are all used with success. i Phenylephrine 10% should be avoided in younger/smaller children. Preoperative topical antibiotic drops may be administered if desired. The same bottle may then be given to the patient for postoperative use. ❹ Examination of Both Eyes Under Anesthesia Intraocular pressure should be measured (if possible) during the early induction phase of anesthesia and then again after the airway is secured. This should be done with either the Tono-pen, Shiotz or Perkins applanation devices. Keratometry measurement if not already performed in clinic Retinoscopy if possible Horizontal corneal diameter measurement (mm) using calipers i The average corneal diameter of a full-term infant is 9.9 mm at birth and 11.1 mm at 12 months of postnatal age
18 Evaluation of anterior chamber structure and depth Evaluation of lens and ciliary body: i Document location and characteristics of lens opacity i Inspect anterior and posterior capsules for plaques that may interfere with capsulotomies or abnormally thin areas that may easily rupture during surgery (posterior lentiglobus or other posterior polar opacities) i Look for small lens size or stretching of ciliary processes that would suggest persistent fetal vasculature in smaller eyes (usually unilateral) Evaluation of retina and optic nerve using indirect ophthalmoscopy if possible i Ultrasound B-scan evaluation of posterior segment in clinic or operating room is recommended (if available) when the cataract prevents visualization of the retina. ❺ Intraocular Lens Calculations Performed preoperatively in clinic in older, cooperative children Performed intraoperatively during examination under anesthesia in younger or uncooperative children Keratometry: measurement of corneal curvature i Older, cooperative children should have manual or automated keratometry performed preoperatively in the clinic setting. i Younger, uncooperative children should preferably have measurements performed under anesthesia with a hand-held keratometer at the time of surgery. Several measurements should be taken and averaged as they tend to be quite variable. The examiner should attempt to carefully align the hand-held keratometer with the patient s visual axis. i If it is not possible to obtain keratometry measurements in either the clinic or operating room setting, the operating physician may elect to use previously published normative values as a last resort. 13 Age Group (months) Mean K (D) A-scan biometry: measurement of axial length i Immersion technique (preferred) i Contact technique if immersion technique not available or if eye is too small for immersion bath shell 13
19 Selection of appropriate intraocular lenses for placement within the posterior capsular bag (preferred) or in the ciliary sulcus i Most common intraocular lens calculation formulas seem to be relatively equal for most children, including SRK II, SRK-T, Hoffer-Q and Holladay-I. 10,11 The Hoffer-Q may be slightly more accurate in the shorter eyes of children. 11 i A-scan at this stage serves also as a base line measurement (with IOP) as routine follow up measures are needed to rule out or treat aphakic/pseudophakic glaucoma. ❻ Cataract Surgery Techniques Make sure your operating microscope is functional; preferably have a coaxial light. A superior rectus traction suture can be helpful. i Suggest a 4-0 silk on a noncutting (taper or round point needle) i Large toothed forceps to grasp superior rectus i Superior rectus traction suture is especially important if performing a scleral tunnel A solid blade speculum suitable for the eye size is used. The choice of incision, capsulotomy technique, lens removal technique, management of the posterior capsule, and use of an IOL depend upon the age of the child as well as other factors. For this reason different procedures will be presented - including a technique for children aged 4 years and younger with a posterior capsulotomy (with and without an IOL) and another, more adult-like technique, for children aged 5 years and older where a primary posterior capsulotomy is not done. A technique for inserting a rigid lens with a scleral tunnel will also be shown. 14
20 ❼ Cataract Surgery Without IOL in Children 4 Years of Age and Younger: Vitrector Technique Step 1 A 20-gauge MVR blade is used to create a temporal corneal incision just anterior to the limbus beyond the terminal loops of the limbal blood vessels. (Figure 1) Step 2 Insert a 20-gauge anterior chamber maintainer (Figure 2) or a short, blunt-tipped, infusion cannula that is connected to the saline infusion bottle either via the vitrectomy machine or as a free-hanging infusion bottle. i Suggest a BD Visitec 20- gauge self-retaining anterior chamber maintainer (Lewicky) [BD Ophthalmics product number ] Alternatively, may simply use a 23-gauge butterfly needle as an infusion line first cut the butterfly wings off and insert the needle through clear cornea with minimal or no prior incision. Must ensure that the sharp tip of the needle avoids contact with the anterior capsule of the lens or the endothelium of the cornea. Figure 1 Right eye, surgeon s view Figure 2 15
21 i A bimanual vitrectomy instrument technique is preferred by some and if chosen it proceeds as follows: Using two incisions, 10 and 2 o clock, the vitrectomy handpiece is used in the surgeon s dominant hand and the irrigation handpiece is used for infusion and is held in the non-dominant hand. (Figure 2a) Figure 2a Open the infusion line to deepen the anterior chamber. i We prefer the Alcon Accurus machine with an active fluid pump. It is set at 30 mmhg for infusion pressure and provides constant anterior chamber depth in contrast to gravity infusion systems where anterior chamber depth can be variable. i Or, use the anterior chamber maintainer with a gravity infusion to stabilize the anterior chamber. Step 3 A second, superiorly located incision is created. (Figure 3) i The anterior chamber is entered at the near-clear cornea, just anterior to the arcade of limbal vessels using the 20-gauge MVR blade either as a straight stab incision or as a biplanar incision using a dimpledown technique. Figure 3 16
22 Dimple-down technique: the tip of the 20-gauge MVR blade is initially used to press down perpendicular to the corneal surface; (Figure 3a) before the tip enters the anterior chamber, about half thickness, the MVR blade is flattened downward approximately 45 degrees so that the entry is completed parallel to the plane of the iris, creating a biplanar incision. (Figure 3b) Figure 3a Figure 3b Step 4 The vitrectomy handpiece (Figure 4) is then inserted and placed open port-down, just touching the central anterior capsule to create a vitrectorhexis type anterior capsulotomy. You should become familiar with the behavior of your vitrector as characteristics tend to vary. It is advisable to have prior experience with the vitrector before it is used for infant cataract surgery. i Suggested vitrector settings are*: cut rate 250 cuts/ minute (typical range, 150 to 300); Figure 4 aspiration 250 mmhg maximum. i At this stage the surgeon selects low aspiration to avoid a radial tear. In some vitrectors used commonly in the developing world, the aspiration is done manually using a syringe. In that case, make sure you start with "minimal" aspiration and increase accordingly if needed. *These recommended settings are for the commonly used Alcon Accurus. Surgeons may need to make adjustments for other machines. 17
23 This vitrectorhexis technique makes it possible to create a uniform anterior capsulotomy opening in younger children who tend to have an elastic anterior capsule prone to radial tears, especially in the presence of a greater positive vitreous pressure contributing to anterior chamber collapse during surgery. The vitrectorhexis technique is particularly helpful in children 2 years of age and younger but may be utilized effectively up to 5 years of age. More experienced surgeons, particularly those comfortable with small-incision capsulotomy forceps, may prefer to perform a traditional continuous curvilinear tear capsulorhexis in all children 3 years of age and older. Step 5 Using the minimum amount of aspiration and just enough downward pressure to engage the anterior capsule, use the vitrector in the cutter-on mode and slowly take bites out of the central anterior capsule. Try to avoid engaging the anterior lens cortex. (Figure 5) i Slowly circle the handpiece, gradually enlarging the anterior capsular opening until it is circular and of the intended size. Figure 5 Since the patient is to be left aphakic and will possibly receive a secondary IOL, the anterior capsulotomy should be approximately 5 mm in diameter. Keep in mind that the cutting action occurs slightly behind the tip of the instrument where the port opening is located, not at the very end. 18
24 Step 6 Turn the cutter function off and use the aspiration-only setting to begin aspirating the lens material. (Figure 6) If the vitrector does not have a suction only capacity, remove the vitrector and perform a manual cortex aspiration using a Simcoe cannula or similar instrument. i It may be helpful to begin aspiration at 12-o clock or just below the corneal incision first. (Figure 6) The large amount of lens material present at this stage helps to prevent engagement of the posterior capsule within the vitrector port. (Figure 7) i Gently engage the cortical material adherent to the capsule and strip or pull it into the center of the eye, being careful not to grab the irregular, scalloped edges of the anterior capsulotomy. Figure 6 i If sticky fragments of lens occlude the aspiration port, turn the port so that it is facing up, away from the posterior capsule, and briefly turn the cutter function back on until the port is clear, then go back to aspiration-only. (Figure 8) Figure 7 Figure 8 19
25 Step 7 Perform posterior capsulotomy and anterior vitrectomy via anterior approach. i The vitrectomy handpiece is now placed with the port facing down and the machine settings are changed to a higher cut rate and lower aspiration level which is appropriate for working with vitreous rather than lens material. (Figure 9) Suggested settings for the Alcon Accurus vitrector are a minimum cut rate of cuts/minute and low levels of aspiration with a maximum vacuum of 100 mmhg. The infusion/ irrigation pressure is also kept low at 30 mmhg. i The posterior capsule is engaged centrally and the aspiration is increased just enough to engage the capsule in the cutter and create the initial opening. (Figure 9) Continuing to use a minimum amount of aspiration with a high cut rate, the central opening is enlarged until it is round and at least 4 mm in diameter, usually just slightly smaller than the anterior capsulotomy diameter of 5 mm. (Figure 10) Alternatively, after meticulous cortex removal the MVR blade can be used to create a central rent (opening) in the posterior capsule. After this, the vitrector can be used with minimal aspiration and high cutting to perform the anterior vitrectomy. Figure 9 Figure 10 posterior capsulotomy not yet complete 20
26 Step 8 Once the posterior capsulotomy is of the desired size and shape, a limited anterior vitrectomy is performed using the same machine settings. The purpose is to remove the anterior vitreous elements that may serve as a surface allowing retained lens epithelial cells to grow across the visual axis. This may be just as amblyopiogenic as the original cataract. i The vitrectomy handpiece is slowly moved around, just posterior to the posterior capsulotomy, until no movement of vitreous to the port is noted. (Figure 11) The end point of the vitrectomy is difficult to define but there should be no evidence of vitreous strands in the pupillary plane or anterior chamber. The vitrectomy handpiece should not be inserted very far into the vitreous and certainly should never be used where the port is not easily seen. i When the vitrector handpiece is withdrawn, the superior incision is checked to be certain that it is free of vitreous strands that tend to follow the instrument out of the eye. If unsure, the wound should be swept with a cyclodialysis spatula or iris repositor. (Figure 11a) i If desired, nonpreserved or washed Kenalog steroid (triamcinolone) may be injected into the anterior chamber to stain strands of vitreous that may be extending to the wounds. The suspended Kenalog solution is white and binds to the transparent vitreous strands, making them easier to identify. Figure 11 Figure 11a 21
27 Step 9 The superior wound is now sutured closed using 10-0 or 9-0 nylon or absorbable suture such as Vicryl (polyglactin 910, Ethicon, Sommerville, New Jersey, USA) or Biosorb (polyglycolic acid, Alcon Laboratories, Inc., Fort Worth, Texas, USA). (Figure 12) Step 10 The infusion cannula is removed and this incision is also sutured closed. (Figure 13) i The eye is repressurized with saline solution and the suture knots are buried. i The procedure is now finished and the eye is patched. (Figure 14) i Note that it is advisable in children to suture each paracentesis! Their low corneoscleral rigidity and high activity level may contribute to wound leaks. Figure 12 Figure 13 Figure 14 22
28 ❽ Cataract Surgery With IOL and Primary Posterior Capsulotomy Via Anterior Approach in Children 4 Years of Age and Younger: Vitrector Technique Step 1 A 20-gauge MVR blade is used to create a temporal corneal incision just anterior to the limbus beyond the terminal loops of the limbal blood vessels. (Figure 15) Step 2 Insert a 20-gauge anterior chamber maintainer (Figure 16) or a short, blunt-tipped, infusion cannula that is connected to the saline infusion bottle either via the vitrectomy machine or as a freehanging infusion bottle. i Suggest a BD Visitec 20- gauge self-retaining anterior chamber maintainer [Lewicky] BD Ophthalmics product number Alternatively, may use a 23-gauge butterfly needle as an infusion line first cut the butterfly wings off and insert the needle through clear cornea with minimal or no prior incision. Must ensure that the sharp tip of the needle avoids contact with the anterior capsule of the lens or the endothelium of the cornea. Figure 15 Right eye, surgeon s view Figure 16 23
29 i A bimanual vitrectomy instrument technique is preferred by some and if chosen it proceeds as follows: Using two incisions, 10 and 2 o clock, the vitrectomy handpiece is used in the surgeon s dominant hand and the irrigation handpiece is used for infusion and is held in the non-dominant hand. (Figure 16a) Figure 16a Open the infusion line to deepen the anterior chamber. i We prefer the Alcon Accurus machine with an active fluid pump. It is set at 30 mmhg for infusion pressure and provides constant anterior chamber depth in contrast to gravity infusion systems where anterior chamber depth can be variable. Step 3 A second, superiorly located incision is created. (Figure 17) i If a clear corneal incision is to be used, with a small-incision foldable/injectable IOL, the anterior chamber is entered at the near-clear cornea, just anterior to the arcade of limbal vessels using the 20-gauge MVR blade either as a straight stab incision or as a biplanar incision using a dimple-down technique. Figure 17 24
30 Dimple-down technique: the tip of the 20-gauge MVR blade is initially used to press down perpendicular to the corneal surface; (Figure 17a) before the tip enters the anterior chamber, about half thickness, the MVR blade is flattened downward approximately 45 degrees so that the entry is completed parallel to the plane of the iris, creating a biplanar incision. (Figure 17b) Figure 17a Figure 17b i If a scleral tunnel incision is to be used, create this 1 to 2 mm from the superior limbus and tunnel forward at half-thickness into clear cornea. Use the cresent knife to create the tunnel 1mm into clear cornea. Enlarge width to the size necessary for IOL insertion but do not enter anterior chamber. Enter the anterior chamber later through this wound, keeping the entry small, using a small keratome or 20-gauge MVR blade. Create a shelved edge entry into the anterior chamber, making sure your tunnel and entry are on a single surgical plane. Open conjunctiva at or 4 mm from the limbus exposing bare sclera. (Figure 18) 8 mm wide Light cautery, if needed After the conjunctiva is incised, exposing bare sclera, a 5.5 mm wide track for the scleral incision is measured 1 mm behind the limbus and the endpoints of the wound are marked by indenting the sclera using surgical calipers. (Figure 18a) Figure 18 Figure 18a 25
31 Using a #15 or similar blade, a straight, approximately 1/2 thickness scleral groove is made with two backward extensions at each end. (Figure 19) The two backward cuts of mm are made from each end of the wound at a 45 degree angle away from the limbus. A scleral tunnel is then constructed using an angled crescent blade. (Figure 20) The incision extends Figure 19 approximately mm into the cornea. The dissection is carried out towards the limbus on both sides to create a funnelshaped pocket. The crescent blade is then angled to cut backwards to incorporate the backward cuts into the pocket. A frown biplanar incision is constructed but note the anterior chamber is not entered. (Figure 21) Figure 20 Figure 21 26
32 The anterior chamber is then entered with a needle knife, and a chamber maintainer is inserted. (Figure 22) A needle knife is inserted in the middle of the tunnel and enters the anterior chamber making a hole just large enough to admit the vitrector or other aspiration device. (Figure 23) i Once the entry is made into the anterior chamber at the center of the scleral tunnel, management of the anterior lens capsule and lens are carried out in a similar manner to that used with a smaller clear corneal entry. Figure 22 Figure 23 Step 4 The vitrectomy handpiece (Figure 24) is then inserted into the opening made in the anterior chamber either through clear cornea or in the middle of the tunnel and placed open port-down just touching the central anterior capsule to create a vitrectorhexis type anterior capsulotomy. You should become familiar with the behavior of your vitrector as characteristics tend to vary. It is advisable to have prior experience with the vitrector before it is used in infant cataract surgery. i Suggested vitrector settings are*: cut rate 250 cuts/ minute (typical range, 150 to 300); aspiration 250 mmhg maximum. *These recommended settings are for the commonly used Alcon Accurus. Surgeons may need to make adjustments for other machines. Figure 24 27
33 This vitrectorhexis technique makes it possible to create a uniform anterior capsulotomy opening in younger children who tend to have an elastic anterior capsule prone to radial tears, especially in the presence of a greater positive vitreous pressure contributing to anterior chamber collapse during surgery. The vitrectorhexis technique is particularly helpful in children 2 years of age and younger but may be utilized effectively up to 5 years of age. More experienced surgeons, particularly those comfortable with smallincision capsulotomy forceps, may prefer to perform a traditional continuous curvilinear tear capsulorhexis in all children 3 years of age and older. Step 5 Using the minimum amount of aspiration and just enough downward pressure to engage the anterior capsule, use the vitrector in the cutter-on mode and slowly take bites out of the central anterior capsule. Try to avoid engaging the anterior lens cortex. (Figure 25) i Slowly circle the handpiece, gradually enlarging the anterior capsular opening until it is circular and of the intended size. Figure 25 Since the patient is to be left aphakic and will possibly receive a secondary IOL later, the anterior capsulotomy should be approximately 5 mm in diameter. Keep in mind that the cutting action occurs slightly behind the tip of the instrument where the port opening is located, not at the very end. Note: A continuous curvilinear capsulorhexis (a) or a can opener technique using a bent tip small needle (b) can also be used at any age. (Figure 26) a Figure 26 b 28
34 Step 6 Turn the cutter function off and use the aspiration-only setting to begin aspirating all lens material. i It may be helpful to begin aspiration at 12-o clock or just below the corneal incision first. (Figure 27) The large amount of lens material present at this stage helps to prevent engagement of the posterior capsule within the vitrector port. i Gently engage the cortical material adherent to the capsule and strip or pull it into the center of the eye, being careful not to engage the irregular, scalloped edges of the anterior capsulotomy. (Figure 28) Figure 27 Figure 28 i If sticky fragments of lens occlude the aspiration port, turn the port so that it is facing up, away from the posterior capsule and briefly turn the cutter function back on until the port is clear, then go back to aspiration-only. (Figure 29) Figure 29 29
35 Step 7 Perform primary posterior capsulotomy and anterior vitrectomy via anterior approach i The vitrectomy handpiece is now placed with the port facing down and the machine settings are changed to a higher cut rate and lower aspiration level as appropriate for working with vitreous rather than lens material. i Suggested settings for the Alcon Accurus vitrector are a minimum cut rate of cuts/minute and low levels of aspiration with a maximum vacuum of 100 mmhg. The infusion/ irrigation pressure is also kept low at <30 mmhg. Figure 30 The posterior capsule is engaged centrally and the aspiration is increased just enough to engage the capsule in the cutter and create the initial opening. (Figure 30) Continuing to use a minimum amount of aspiration with a high cut rate, the central opening is enlarged until it is round and at least 4 mm in diameter, usually just slightly smaller than the anterior capsulotomy diameter of 5 mm. (Figure 31) Once the posterior capsulotomy is of the desired size and shape, a limited anterior vitrectomy is performed using the same machine settings. The purpose is to remove the anterior vitreous elements that may serve as a surface allowing retained lens epithelial cells to grow across the visual axis. This may be just as amblyopiogenic as the original cataract. i Caution: If placing a primary IOL after the posterior capsulotomy, making the posterior capsulotomy too large may make it more difficult to place the IOL securely within the capsular bag. Figure 31 Posterior capsulotomy not yet complete 30
36 The vitrectomy handpiece is slowly moved around, just posterior to the posterior capsulotomy, until no movement of vitreous to the port is noted. (Figure 32) i The end point of the vitrectomy is difficult to define but there should be no evidence of vitreous strands in the pupillary plane or anterior chamber. i The vitrectomy handpiece should not be inserted very far into the vitreous and certainly should never be used where the port is not easily seen. i If desired, nonpreserved or washed Kenalog steroid (triamcinolone) may be injected into the anterior chamber to stain strands of vitreous that may be extending to the wounds. The suspended Kenalog solution is white and binds to the transparent vitreous strands, making them easier to identify. At this point, the vitrector handpiece is withdrawn (Figure 32a), the superior incision is checked to be certain that it is free of vitreous strands that tend to follow the instrument out of the eye. If unsure, the wound should be swept with a cyclodialysis spatula or iris repositor. (Figure 32b) Figure 32 Figure 32a Figure 32b 31
37 The anterior chamber and the capsular bag are now filled with a high-viscosity, cohesive viscoelastic agent. (Figure 33) i The benefit of a highly cohesive viscoelastic agent is that it is better able to maintain the volume and shape of the pediatric eye which has low scleral rigidity. It is also easier to remove completely at the end of the procedure. However, some viscoelastic agents may be so viscous that they tend to clog the infusion cannula or vitrectomy hand piece. If this occurs, squeezing the infusion line or hitting reflux on the vitrector will usually clear the obstruction. Figure 33 The superior anterior chamber incision is then enlarged to a sufficient width with a keratome to allow placement of the foldable IOL. (Figure 34) Figure 34 32
38 The IOL is inserted or injected and dialed into position with an IOL hook as needed. (Figure 35, 36, 37) Figure 35 Figure 36 Figure 37 If you inject the foldable IOL, remember to inject slowly in the bag and avoid dialing through both openings into the vitreous. To reduce the chance of this, have a cushion of visco-elastic. Some surgeons find it easier to inject the lens into the anterior chamber and then use an IOL hook to dial the IOL into the bag. Alternatively, forceps can be used to place the foldable IOL by aiming the front haptic into the bag then using the hook to dial the near haptic into the bag. 33
39 When a rigid IOL is used, the superior anterior chamber scleral tunnel incision is then enlarged to a sufficient width with a keratome to allow placement of the foldable IOL. (Figure 38) The rigid lens is inserted and dialed in the bag with the leading haptic placed first and the trailing haptic placed behind the anterior lens capsule and then the lens is dialed in. (Figure 39, 40) Remember: If operating in a setting with limited resources, it is better to secure solid sulcus placement rather than dealing with complications of having one haptic in the bag and one in the sulcus, IOL dislocation, etc. Figure 38 Figure 39 Figure 40 It is essential to have a good operating microscope providing a good view of both anterior and posterior capsular openings, as this method is more prone to IOL dislocation if visibility is not optimal. The vitrectomy handpiece is used to aspirate residual viscoelastic from the eye which is then re-formed using balanced saline solution. The anterior chamber and superior incision should be checked very carefully to ensure that no vitreous strands have adhered to the lens insertion instruments and followed them back to the wound. Careful sweeping of any vitreous strands with a cyclodialysis spatula, weckcell, or iris repositor is recommended. 34
40 The superior corneal incision used for insertion of a foldable lens is then closed using 9-0 or 10-0 nylon or absorbable suture such as Vicryl (polyglactin 910, Ethicon, Sommerville, New Jersey, USA) or Biosorb (polyglycolic acid, Alcon Laboratories, Inc., Fort Worth, Texas, USA). Remove the anterior chamber infusion cannula (anterior chamber maintainer) and close the corneal incision using 9-0 or 10-0 nylon or absorbable suture such as Vicryl or Biosorb. (Figure 41) The corneal incision used for insertion of a rigid lens is closed first and then the conjunctiva is closed in a separate layer. (Figure 42) Figure 41 clear corneal incision Figure 42 scleral tunnel incision It is optional to administer topical antibiotic and subconjunctival steroid injections. Examples include: i Cefazolin (cefazoline or cephazolin) 50 mg i Dexamethasone 2 mg Cover the operated eye with a patch and protective shield. (Figure 43) NOTE: Another option for anterior vitrectomy is first to place the IOL in the bag, then placing viscoelastic into the capsular bag gently lift up slightly the IOL optic and using a MVR or stiletto blade create a tear in the central posterior capsule followed by anterior vitrectomy through the corneal incision. Figure 43 35
41 ❾ Cataract Surgery With IOL and Primary Posterior Capsulotomy Via Pars Plana Approach in Children 4 Years of Age and Younger: Vitrector Technique Step 1 A 20-gauge MVR blade is used to create a temporal corneal incision just anterior to the limbus beyond the terminal loops of the limbal blood vessels. (Figure 44) Step 2 Insert a 20-gauge anterior chamber maintainer (Figure 45) or a short, blunt-tipped, infusion cannula that is connected to the saline infusion bottle either via the vitrectomy machine or as a free-hanging infusion bottle. i Suggest a BD Visitec 20- gauge self-retaining anterior chamber maintainer [Lewicky]. BD Ophthalmics product number Alternatively, may simply use a 23-gauge butterfly needle as an infusion line first cut the butterfly wings off and insert the needle through clear cornea with minimal or no prior incision. Must ensure that the sharp tip of the needle avoids contact with the anterior capsule of the lens or the endothelium of the cornea. Figure 44 Right eye, surgeon s view Figure 45 36
42 i A bimanual vitrectomy instrument technique is preferred by some and if chosen it proceeds as follows: Using two incisions, 10 and 2 o clock, the vitrectomy handpiece is used in the surgeon s dominant hand and the irrigation handpiece is used for infusion and is held in the non-dominant hand. (Figure 45a) Figure 45a Open the infusion line to deepen the anterior chamber. i We prefer the Alcon Accurus machine with an active fluid pump. It is set at 30 mmhg for infusion pressure and provides constant anterior chamber depth in contrast to gravity infusion systems where anterior chamber depth can be variable. Step 3 A second, superiorly located incision is created. i If a clear corneal incision is to be used, with either no IOL implant or with a small-incision foldable/injectable IOL, the anterior chamber is entered at the near-clear cornea, just anterior to the arcade of limbal vessels using the 20-gauge MVR blade either as a straight stab incision or as a biplanar incision using a dimple-down technique. (Figure 46) Figure 46 37
43 Dimple-down technique: the tip of the 20-gauge MVR blade is initially used to press down perpendicular to the corneal surface; (Figure 46a) before the tip enters the anterior chamber about half thickness, the MVR blade is angled 45 degrees downward so that the entry is completed parallel to the plane of the iris, creating a biplanar incision. (Figure 46b) 45 degrees Figure 46a Figure 46b i If a scleral tunnel incision is to be used, create this 1 to 2 mm from the superior limbus and tunnel forward at half-thickness into clear cornea. Enlarge width to the size necessary for IOL insertion but do not enter anterior chamber. Enter the anterior chamber later through this wound, keeping the entry small, using a small keratome or 20-gauge MVR blade. Open conjunctiva at or 4 mm from the limbus exposing bare sclera. (Figure 47) 8 mm wide Light cautery, if needed After the conjunctiva is incised, exposing bare sclera, a 5.5 mm wide track for the scleral incision is measured 1 mm behind the limbus and the endpoints of the wound are marked by indenting the sclera using surgical calipers. (Figure 47a) Figure 47 Figure 47a 38
44 Using a #15 or similar blade, a straight, approximately 1/2 thickness, scleral groove is made with two backward extensions at each end. (Figure 48) The two backward cuts of mm are made from each end of the wound at a 45 degree angle away from the limbus. Figure 48 A scleral tunnel is then constructed using an angled crescent blade. (Figure 49) The incision extends approximately mm into the cornea. Figure 49 39
45 The dissection is carried out towards the limbus on both sides to create a funnel-shaped pocket. The crescent blade is then angled to cut backwards to incorporate the backward cuts into the pocket. A frown biplanar incision is constructed but note the anterior chamber is not entered. (Figure 50) After the anterior chamber is entered with a needle knife, a chamber maintainer is inserted. (Figure 51) A needle knife is inserted in the middle of the tunnel and enters the anterior chamber making a hole just large enough to admit the vitrector or other aspiration device. (Figure 52) Figure 50 Figure 51 Figure 52 i Once the entry is made into the anterior chamber at the center of the scleral tunnel, management of the anterior capsule and lens material is carried out in a similar manner to that used with a smaller clear corneal entry. 40
46 Step 4 The vitrectomy handpiece (Figure 53) is then inserted into the opening made in the anterior chamber either through clear cornea or in the middle of the scleral tunnel and placed open port-down just touching the central anterior capsule to create a vitrectorhexis type anterior capsulotomy. You should become familiar with the behavior of your vitrector as characteristics tend to vary. It is advisable to have prior experience with the vitrector before it is used in infant cataract surgery. i Suggested vitrector settings are*: cut rate 250 cuts/ minute (typical range, 150 to 300); aspiration 250 mmhg maximum. *These recommended settings are again for the commonly used Alcon Accurus. Surgeons may need to make adjustments for other machines. Figure 53 This vitrectorhexis technique makes it possible to create a uniform anterior capsulotomy opening in younger children who tend to have an elastic anterior capsule prone to radial tears, especially in the presence of a greater positive vitreous pressure contributing to anterior chamber collapse during surgery. The vitrectorhexis technique is particularly helpful in children 2 years of age and younger but may be utilized effectively up to 5 years of age. More experienced surgeons, particularly those comfortable with smallincision capsulotomy forceps, may prefer to perform a traditional continuous curvilinear tear capsulorhexis in all children 3 years of age and older. Step 5 Using the minimum amount of aspiration and just enough downward pressure to engage the anterior capsule, use the vitrector in the cutter-on mode and slowly take bites out of the central anterior capsule. Try to avoid entering the anterior lens cortex. (Figure 54) i Slowly circle the handpiece, gradually engaging the anterior capsular opening until it is circular and of the intended size. Figure 54 41
47 The anterior capsulotomy should be approximately 5 mm, or just slightly smaller than the diameter of the optic of the IOL chosen for implantation. i Keep in mind that the cutting action occurs slightly behind the tip of the instrument where the port opening is located, not at the very end. Step 6 Turn the cutter function off and use the aspiration-only setting to begin aspirating lens material. i It may be helpful to begin aspirating at 12-o clock or just below the corneal incision first. (Figure 55) The large amount of lens material present at this stage helps to prevent engagement of the posterior capsule within the vitrector port. i Gently engage the cortical material adherent to the capsule and strip or pull it into the center of the eye, being careful not to grab the irregular, scalloped edges of the anterior capsulotomy. (Figure 56) Figure 55 Figure 56 i If sticky fragments of lens occlude the aspiration port, turn the port so that it is facing up, away from the posterior capsule and briefly turn the cutter function back on until the port is clear, then go back to aspiration-only. (Figure 57) Figure 57 42
48 Once the capsular bag is completely empty of lens material, the surgeon should now re-form the anterior chamber and fill the capsular bag with a high-viscosity, cohesive viscoelastic agent (examples include Healon and Healon GV from manufacturer AMO, Santa Ana, California, USA). (Figure 58) i The benefit of a highly cohesive viscoelastic agent is that it helps to maintain the volume and shape of pediatric eyes which have low scleral rigidity. It is also easier to remove completely at the end of the procedure. However, some viscoelastic agents may be so Figure 58 viscous that they tend to clog the infusion cannula or vitrectomy hand piece. Squeezing the infusion line or hitting reflux on the vitrector will usually clear the obstruction if this happens. Step 7 The superior, anterior chamber incision is then enlarged sufficiently with a keratome to allow placement of the IOL; smaller and through clear cornea if a foldable IOL is used (Figure 59) or larger through the scleral tunnel if a rigid lens is used (Figure 60) Figure 59 wound enlargement if a clear corneal incision is utilized Figure 60 wound enlargement if a scleral tunnel is utilized 43
49 The foldable IOL is inserted or injected and dialed into position with an IOL hook as needed. (Figure 61, 62, 63) Figure 61 Figure 62 Figure 63 The rigid lens is inserted and dialed in the bag with the leading haptic placed first and the trailing haptic placed behind the anterior lens capsule and then the lens is dialed in. (Figure 64, 65) Figure 64 Figure 65 44
50 The vitrectomy handpiece is used to aspirate residual viscoelastic from the eye which is then re-formed using balanced saline solution. The superior clear corneal incision is then closed using 9-0 or 10-0 nylon or absorbable suture such as Vicryl (polyglactin 910, Ethicon, Sommerville, New Jersey, USA) or Biosorb (polyglycolic acid, Alcon Laboratories, Inc., Fort Worth, TX, USA). (Figure 66) The scleral tunnel is closed in layers, scleral first and then conjunctiva. (Figure 67) Figure 66 Figure 67 Step 8 Perform posterior capsulotomy and anterior vitrectomy using pars plana approach. Conjunctiva and Tenons are incised to access sclera several millimeters behind the limbus in the superiortemporal or superior-nasal quadrant using scissors to expose the bare sclera overlying the pars plana. (Figure 68) i Avoid cutting down directly onto the superior rectus muscle. i Hemostasis is achieved with light cautery if needed. Figure 68 45
51 Calipers are used to measure back an appropriate distance* before entering the eye with the MVR blade. (Figure 69, 70) * < 1 year of age: enter mm from limbus 1 4 years of age: enter 2.5 mm from limbus > 4 years of age: enter 3.0 mm from limbus Figure 69 Figure 70 The MVR blade is directed toward the center of the vitreous cavity while entering the eye and the tip of the blade should be clearly visualized behind the IOL prior to inserting the vitrectomy hand piece. (Figure 71 a and b) Figure 71 a Figure 71 b 46
52 The vitrectomy handpiece is inserted and should be visualized: then make initial cuts but only after visualizing the cutter tip. An initial cut is made in the central posterior capsule with the vitrector port facing upward. This will allow the infusion to more easily circulate from the anterior chamber to the posterior chamber. (Figure 72) i Be certain that the vitrector is behind the posterior capsule and has not inadvertently been passed into the capsular bag. Figure 72 i Suggested settings for the Alcon Accurus vitrector are a minimum cut rate of cuts/minute and low levels of aspiration with a maximum vacuum of 100 mmhg. The infusion/irrigation pressure is also kept low at < 30 mmhg. Gradually enlarge the posterior capsule opening to be at least 4 mm in diameter or just slightly smaller than the 5 mm anterior capsulotomy (and smaller than the IOL optic diameter), ensuring that an adequate rim of support is left in place to support the IOL. (Figure 73, 74) Figure 73 Figure 74 47
53 Perform a limited vitrectomy of the anterior vitreous just posterior to the IOL and capsular bag. (Figure 75) i The vitrectomy handpiece is slowly moved around just posterior to the posterior capsulotomy until no movement of vitreous to the port is noted. i The vitrectomy handpiece should not be inserted very far into the vitreous and certainly should never be used where the port is not easily visualized. Lower the infusion pressure to less than 20 mmhg before removing the vitrector to help reduce the likelihood of vitreous prolapse when the handpiece is removed. Clean up any extruded vitreous at the entry incision using the vitrectomy cutter or scissors. Figure 75 Suture the sclerotomy closed once it is free of vitreous. (Figure 76 a and b) i The suture most commonly used is 9-0 nylon or 8-0 Vicryl. i Some surgeons prefer to pre-place the scleral suture before performing posterior capsulotomy and vitrectomy. Figure 76 a Figure 76 b 48
54 Close the conjunctival incision using an absorbable suture (can use the same 8.0 Vicryl used to close the sclerotomy). (Figure 77) Remove the anterior chamber infusion cannula (anterior chamber maintainer) and close the corneal incision using 9-0 or 10-0 nylon or absorbable suture such as Vicryl or Biosorb. (Figure 78) Administer topical antibiotic and steroid eye drops or a combination antibiotic/steroid ointment. Figure 77 Subconjunctival antibiotic and steroid injections are optional. Examples include: i Cefazolin (cefazoline or cephazolin) 50 mg i Dexamethasone 2 mg Cover the operated eye with a patch and protective shield. (Figure 79) NOTE: This pars plana approach for posterior capsulotomy anterior vitrectomy seems to be the most controlled but is advisable only with the use of an automated high cut rate vitrector. Figure 78 Figure 79 49
55 Cataract Surgery With IOL in Children 5 Years of Age and Older: Irrigation/ Aspiration Technique (and no posterior capsulotomy or anterior vitrectomy) Create a superiorly located incision. i If a scleral tunnel incision is to be used, create this 2-3 mm from the superior limbus and tunnel forward at half-thickness into clear cornea. Enlarge width to the size necessary for IOL insertion but do not enter anterior chamber. Enter the anterior chamber through this wound using a small knife blade (example, 2.5 mm keratome). i If a clear corneal incision is to be used with a foldable or injectable IOL, enter the near-clear cornea, just anterior to the arcade of limbal vessels using a small knife blade (example, 2.5 mm keratome), either as a straight stab incision or as a biplanar incision using a dimple-down technique. Dimple-down technique: the tip of the 20-gauge MVR blade is initially used to press down perpendicular to the corneal surface; before the tip enters the anterior chamber about half thickness, the MVR blade is angled 45 degrees downward so that the entry is completed parallel to the plane of the iris, creating a biplanar incision. Fill the anterior chamber with a viscoelastic agent. i High-viscosity, cohesive viscoelastic agents such as Healon and Healon GV help to better maintain the volume and shape of pediatric eyes with low scleral rigidity and are easier to remove completely at the end of the procedure. Perform an anterior capsulotomy measuring 5 mm or greater in diameter using either a bent-tip needle cystotome or capsulorhexis forceps. i If the patient is to be left aphakic with a possible secondary IOL later, the anterior capsulotomy should be approximately 5 mm in diameter. i If the patient is to have a primary IOL placed at the time of cataract surgery, the anterior capsulotomy should be slightly smaller than the diameter of the optic of the IOL chosen for implantation. i Keep in mind that pediatric anterior capsules tend to be more elastic and tend to extend outward, particularly in younger children. This can be minimized by: Using a high-viscosity, cohesive viscoelastic agent to keep the anterior chamber full and the anterior capsule flat. Reinjecting additional viscoelastic as needed during the performance of the anterior capsulotomy, particularly if the tear begins to extend outward. Regrasping the capsulorhexis edge frequently to maintain control. Staining the anterior capsule with trypan blue under air bubble if the cataract is mature. In young children, the direction of the force should be toward the center of the pupil to keep the capsulorhexis from extending peripherally. 50
56 Perform aspiration of the lens substance. i Use an automated irrigation/aspiration handpiece or manual Simcoe syringe to remove both lens cortex and nucleus. Pediatric cataracts are soft; phacoemulsification power is not needed. It is helpful to have a larger aspiration port size such as a 0.5 mm diameter opening. Multiquadrant hydrodissection may be performed prior to lens aspiration to facilitate the removal of lens material. DO NOT HYDRODISSECT IF THE POSTERIOR CAPSULE IS ABNORMAL OR QUESTIONABLE. traumatic cataract posterior polar cataract posterior lentiglobus cataract After removing a small amount of the anterior, central lens material, engage the peripheral lens cortex and strip it into the center of the pupillary space for aspiration using a technique similar to that of cortical clean-up in an adult cataract patient. It is generally safer to remove the subincisional (12 o'clock) cortex early in the procedure while there is still a large amount of central and posterior lens substance in place to keep the posterior capsule away from the aspiration port. After removal of all lens material, re-form the anterior chamber and posterior capsular bag using viscoelastic. Enlarge the anterior chamber incision with a keratome to allow placement of the IOL. The IOL is inserted or injected and dialed into position with an IOL hook as needed. Use the irrigation/aspiration handpiece to remove the viscoelastic from the anterior chamber and around the IOL. The corneal/scleral incisions are then closed using 9-0 or 10-0 nylon or absorbable suture such as Vicryl or Biosorb. Administer topical antibiotic and steroid eye drops or a combination antibiotic/steroid ointment. i Subconjunctival antibiotic and steroid injections are optional. Examples include: Cefazolin (cefazoline or cephazolin) 50 mg Dexamethasone 2 mg Cover the operated eye with a patch and protective shield. 51
57 POSTOPERATIVE MANAGEMENT OF PEDIATRIC CATARACT PATIENTS ❶ Postoperative Medications Topical steroid i Prednisolone acetate 1% or similar, 4 to 6 times daily for 1 to 2 months i If evidence of significant inflammation persists (anterior chamber flare, cell, fibrin or deposits on the IOL), the topical steroid may be continued longer, up to 3 to 6 months with monitoring of intraocular pressure. Topical antibiotic i Drop or ointment applied 4 times daily for 1 to 2 weeks Atropine i Aphakic and pseudophakic eyes: apply atropine 1% once daily for 2 to 4 weeks If an IOL is implanted, the use of postoperative cycloplegic is optional. Some surgeons use it routinely in all cases while others use it only if inflammatory adhesions begin to develop. If the IOL or anterior capsulotomy are unstable, it may be wise to defer any pupil dilation until the wounds have become watertight and the anterior chamber is stable. i In very small or young infants (less than 1 year of age), consider using more dilute atropine 0.5% if available. ❷ Postoperative Follow-Up Postoperative examination schedule: i 1 day i 1 week i 1 month (3-5 weeks after surgery) i 3 months (every 3 months after surgery for the first year) i At least twice yearly after the first postoperative year for younger children The younger the patient, the more careful and frequent the follow-up should be, particularly in younger children at risk for amblyopia (less than 8 years of age). Consider taking out the corneal sutures (unless absorbable suture material was used) at the 3 month post op visit. Postoperative examination elements: i Assessment of visual acuity with comparison between the two eyes i Ocular motility and alignment i Intraocular pressure (particularly if using topical steroids) Tonometry (preferred) or palpation 52
58 i Anterior segment examination Slit-lamp (preferred) or hand-held light source Penlight, muscle light, flashlight/torch held obliquely at an angle from the side to illuminate the anterior chamber May magnify the view of the anterior segment structures by directly viewing through a 20 to 30 diopter indirect ophthalmoscope lens used without the ophthalmoscope Assess the adequacy of the pupil size and centration of the IOL if one has been implanted i Red reflex Ensure clarity of the visual axis by assessing the quality (brightness) of the red reflex using either: Direct ophthalmoscope set on either a slit-beam or small, bright field of illumination Retinoscope set to a thin beam of light i Refraction Hand-held retinoscope with loose lenses, refraction bar, or phoropter* i Ophthalmoscopy Indirect (preferred) or direct ophthalmoscope Perform at least once or twice yearly and anytime there is change in quality of the vision or red reflex, or if there is a significant refractive shift Refractive Management Refraction should be performed as early as is possible in the postoperative period. Aphakic children and younger pseudophakic children should ideally receive optical correction within the first 1 to 2 weeks following cataract surgery. Older pseudophakic children may have residual refractive error corrected with glasses after the wound and refraction have stabilized 4 to 6 weeks postoperatively. Correction of postoperative refractive error i Bifocals versus single-vision correction Young children, particularly those less than 2-3 years of age, do not generally require a bifocal and do well with single-vision correction using either glasses or contact lens(es) targeted to overcorrect, producing a mild amount of myopia (for better near vision). *See ORBIS Vision and Refraction manual 53
59 The eye is overcorrected by 2.00 to 3.00 diopters so that the far point is 50 to 33 cm. Aphakic eye example: Aphakic refraction** = D Prescription given = D **If an aphakic contact lens is being fitted, the prescription must also be adjusted according to the vertex distance of the loose lens or phoropter being used for the refraction. i Older children (> 2-3 years of age) have greater visual demands and benefit from a traditional bifocal. Upper segment: distance correction for emmetropia Lower segment: near correction with a to add Flat-topped lower segments (D-shaped or executive style) are easier for children to use and have larger optical zones with minimal distortion. ❹ Amblyopia Management Appropriate and effective amblyopia management is vital to the visual result obtained by younger children. Parents or caregivers should have this concept explained to them with sufficient care and detail to ensure successful administration. While occlusion (patch) therapy is most productive in younger children, even children older than 9 years of age may show some benefit to a therapeutic trial of patching. Bilateral cataract patients require occlusion therapy only if there is a measurable visual acuity or fixation difference between the two eyes. It is crucial to develop a team with the parents and child to ensure good patching compliance. Explain to parents the importance of amblyopia treatment even before the operation. In young children even the "perfect" surgery without prompt amblyopia treatment will not yield a favorable outcome. The parents are your partners on the journey to best visual outcome. Unilateral cataract patients almost always require more intensive occlusion therapy than bilateral cataract patients unless the child was older and therefore less sensitive to amblyopia when the cataract developed. i Infants with unilateral cataract should have a patch on the unoperated eye 1 awake hour per day per each month of age, up to 8 months of age (maximum 8 hours/day). Example: a 6-month-old infant would patch 6 hours each day i After 8 months of age, children with unilateral cataracts should have the unoperated eye patched 50% of all awake hours each day. This amount of patching may be adjusted downward as the child becomes older and becomes less sensitive to amblyopia or if accurate visual acuity testing shows no significant difference between the two eyes. 54
60 ❺ Secondary Opacification of the Visual Axis Because secondary opacification of the posterior capsule and anterior vitreous face will occur in virtually all children less than 5 years of age, it is recommended that a primary surgical posterior capsulotomy and anterior vitrectomy be performed at the time of initial cataract surgery. i This step is optional in children 5-8 years of age and a reasonable alternative in this group would be a primary surgical capsulotomy alone, without anterior vitrectomy. i Children older than 8 years of age can generally be managed as adults with the posterior capsule left intact at the time of cataract surgery. If the posterior capsule is left intact in children and a secondary YAG laser capsulotomy is required, surgeons should be cautioned that the opacification of the posterior capsule and anterior vitreous face can be quite dense and difficult to open. i Generally, slightly increased amounts of laser energy and a greater number of laser bursts are required compared to that used for adult capsulotomies. i Reopacification of the visual axis following YAG laser capsulotomy is frequent and repeat treatments may be required. i Some opacifications are so dense that the only method to adequately clear the visual axis is surgery with a pars plana vitrectomy approach. Incising the membrane with an MVR blade may assist in creating an edge that the vitrector can grab and cut. Vertical or horizontal cutting intraocular scissors are also quite helpful for removing dense membranes occluding the visual axis. ❻ Secondary IOL Implantation Children requiring a secondary IOL implantation should have the lens placed either into the ciliary sulcus or within the capsular bag remnants if possible. Implantation within the ciliary sulcus is generally the easiest and most convenient site for secondary IOL implantation. i Posterior synechia should be broken by blunt dissection using an iris spatula. This may be facilitated by visco-dissection using a cannula with a cohesive viscoelastic to expand the ciliary sulcus. i Some Soemmering rings can be so thick and bulky that they need to be debulked before an IOL can be implanted into the ciliary sulcus. After incising the inner portion of the Soemmering ring with an MVR blade, the vitrectomy handpiece can be used to aspirate the bulk of the retained lens material, thereby decompressing the Soemmering ring. This usually requires multiple approaches from several different clear corneal incisions. 55
61 i If the anterior and posterior capsular halves are easily incised and separated, it may be possible to place the IOL entirely within the capsular remnants after the Soemmering ring of retained lens material is aspirated. (Figure 80) E If this is not possible, the IOL should be placed securely within the ciliary sulcus. (Figure 81) P Secondary IOLs placed within the ciliary sulcus should have an optic diameter of 6-7 mm and an overall haptic diameter of mm. P Secondary IOLs placed within the capsular bag may be smaller with an optic diameter of 5-6 mm and an overall haptic diameter of mm. Figure 80 Figure 81 { Long-Term Follow-Up P Even after the first postoperative year is complete, children should be seen at least once or twice yearly to monitor for postoperative complications. This is particularly important in children less than 8 years of age at risk for amblyopia. P Long-term postoperative conditions to monitor include: i Amblyopia i Significant shifts of refractive error E Unpredictable growth patterns E 56 May be secondary to glaucoma
62 i Opacification of the visual axis Posterior capsule opacification Secondary pupillary membranes Opacification of the anterior vitreous i Decentration of IOL, particularly if implanted in the ciliary sulcus i Retinal complications Retinal detachment Cystoid macular edema (less common in children) i Glaucoma Secondary glaucoma is frequent in both aphakic and pseudophakic children. Children undergoing surgery at a very young age and those with small corneas are at particularly high risk for glaucoma. Abnormalities of the angle structures are more frequent in children with congenital cataracts. Trabeculotomy and goniotomy may be effective surgical treatment options if angle abnormalities exist. In addition to elevated intraocular pressure, signs of glaucoma in younger children include: Myopic refractive shifts Increased corneal diameter Decreased corneal clarity Increased axial length measurements Optic nerve cupping (may be reversible) ANESTHESIA FOR PEDIATRIC CATARACT SURGERY Competent anesthesia care is vital for the conduct of safe and effective cataract surgery in children. While local anesthesia may be possible in older, cooperative children, most young children will require some form of general anesthesia. Infants less than one year of age are particularly challenging to the anesthetist, while at the same time the pediatric patient population are most in need of timely cataract surgery to prevent profound vision loss from amblyopia and nystagmus. General anesthesia for children is best administered by a physician with particular training or experience in pediatric anesthesia care. However, this may be an unrealistic expectation for many areas of the world. If other medical officers or nurse anesthetists are utilized, they should be adequately skilled and comfortable in pediatric anesthesia care to ensure a safe and comfortable procedure. If adequate anesthesia skills and equipment are not available, it is better to not perform surgery at all rather than placing the general health and safety of the child at unacceptable risk. Local physicians and medical teams are best suited to make this decision. 57
63 Recommended Basic Equipment List for Pediatric Anesthesia Airway Management: Facemasks - age range 0-16 yr Oropharyngeal airways - size 0 to 4 LMAs (regular and flexible)- size 1-4 ETT (regular, RAE type) - sizes 3-8 Bougie and stylets Laryngoscopes - range of blades (Mackintosh and Miller) and sizes Suction Tape or ties to secure airway NG tubes (range of sizes - decompress stomachs in small children) Drugs: Premedication - midazolam Induction - propofol, thiopentone Muscle relaxants - suxamethonium, atracurium, rocuronium Reversal agent - glycopyrrolate/neostigmine Anti-emetics - ondansetron, dexamethasone, metoclopramide, cyclizine Analgesics - paracetamol (PO/PR/IV), NSAIDs (PO/PR/IV), opiates (fentanyl, alfentanil, morphine) Emergency - atropine, glycopyrrolate. adrenaline IV fluids - isotonics (saline or Ringers) Breathing: Anesthetic circuits - peds T piece, circle Anesthetic machine - oxygen/air/nitrous oxide + volatile agents isoflurane/ sevoflurane Ventilator - ventilatory modes suitable for children Scavenging of gases from theatre Circulation: Range of cannulas IV Monitoring: Full monitoring - HR, BP, ECG, SpO2, end tidal CO2, gas analysis, temperature 58
64 When available, general anesthesia with inhalational and intravenous agents administered with a secure airway (endotracheal tube or laryngeal mask) provides an adequate depth of anesthesia. This may be supplemented by depolarizing muscle relaxants to ensure akinesia and reduced positive vitreous pressure. These benefits must be measured against potential drawbacks such as the difficulty of obtaining intravenous access in small children, need for adequate oxygen delivery, need for monitoring oxygen saturation (pulse oximetry) as well as the possible side effects of postoperative nausea and vomiting. General anesthesia with ketamine, administered by either intravenous or intramuscular routes, is also possible and requires a less sophisticated health care system for safe use but it may be more difficult to use during long procedures and has the disadvantages of inducing eye movement and increased positive vitreous pressure. These features make it less ideal than inhalation agents and require the use of a supplemental retro- or peribulbar anesthesia. In older, more cooperative children, local or regional anesthesia becomes a more viable alternative to general anesthesia. We have found that children as young as 7 years of age may be safely and adequately operated on using a peribulbar injection technique. 14 One clinical method to identify good potential candidates for such local anesthesia surgery is the lid speculum test. In this assessment, children are given a topical anesthetic and then have an eyelid speculum placed while in the clinic. If the child tolerates this process without significant resistance, they will usually be cooperative enough to tolerate cataract surgery under local anesthesia that can be supplemented with intravenous sedation as needed. SUMMARY We have attempted to present a concise summary of the fundamental techniques and management issues that are specific to pediatric cataracts. The reader will notice that we have given particular emphasis to dealing with younger children, particularly those less than five years of age, as this is the group whose needs differ most from typical adult cataract patients. These younger patients have eyes that are smaller, more elastic and present with a diversity of cataract types that may be accompanied by other ocular abnormalities. Additionally, these younger patients are particularly sensitive to vision loss from amblyopia, large refractive shifts and secondary glaucoma. All of these factors serve to make the pediatric cataract patient more complicated to manage and emphasize the need for specialized surgical techniques and the maintenance of long term follow-up care. We urge the reader to expand their knowledge of these subjects. Online resources and consultation opportunities with other pediatric cataract surgeons are available at 59
Lens Embryology. Lens. Pediatric Cataracts. Cataract 2/15/2017. Lens capsule size is fairly constant. Stable vs. progressive
 Lens Embryology Catherine O. Jordan M.D. Surface ectoderm overlying optic vesicle Day 28 begins to form End of week 5 lens vesicle is formed Embryonic nucleus formed at week 7 Weeks 12-14 anterior Y and
Lens Embryology Catherine O. Jordan M.D. Surface ectoderm overlying optic vesicle Day 28 begins to form End of week 5 lens vesicle is formed Embryonic nucleus formed at week 7 Weeks 12-14 anterior Y and
Paediatric cataract pathogenesis and management
 Paediatric cataract pathogenesis and management Dr. Kavitha Kalaivani. N Paediatric ophthalmology Sankara Nethralaya February 28-2017 Incidence... 1 to 13 per 10 000 live births 1 200,000 children blind
Paediatric cataract pathogenesis and management Dr. Kavitha Kalaivani. N Paediatric ophthalmology Sankara Nethralaya February 28-2017 Incidence... 1 to 13 per 10 000 live births 1 200,000 children blind
Management of Congenital Cataract Surgery. Dr. Vaishali Vasavada, MS. Dr. Abhay R. Vasavada, MS, FRCS (England) Raghudeep Eye Hospital, India
 Management of Congenital Cataract Surgery Dr. Vaishali Vasavada, MS Dr. Abhay R. Vasavada, MS, FRCS (England) Raghudeep Eye Hospital, India Congenital cataract surgery is a complex issue best left to surgeons
Management of Congenital Cataract Surgery Dr. Vaishali Vasavada, MS Dr. Abhay R. Vasavada, MS, FRCS (England) Raghudeep Eye Hospital, India Congenital cataract surgery is a complex issue best left to surgeons
Shedding Light on Pediatric Cataracts. Kimberly G. Yen, MD Associate Professor of Ophthalmology Texas Children s Hospital
 Shedding Light on Pediatric Cataracts Kimberly G. Yen, MD Associate Professor of Ophthalmology Texas Children s Hospital A newborn infant presents with bilateral white cataracts. What is the best age to
Shedding Light on Pediatric Cataracts Kimberly G. Yen, MD Associate Professor of Ophthalmology Texas Children s Hospital A newborn infant presents with bilateral white cataracts. What is the best age to
Pediatric cataract. Nikos Kozeis MD, PhD, FICO, FEBO, MRCOphth. Surgical challenges and postoperative complications
 Pediatric cataract Surgical challenges and postoperative complications Nikos Kozeis MD, PhD, FICO, FEBO, MRCOphth Consultant Paediatric Ophthalmologist Thessaloniki, Greece Pediatric Cataract 2.4 / 10000
Pediatric cataract Surgical challenges and postoperative complications Nikos Kozeis MD, PhD, FICO, FEBO, MRCOphth Consultant Paediatric Ophthalmologist Thessaloniki, Greece Pediatric Cataract 2.4 / 10000
Meet Libby. Corneal Dysgenesis, Degeneration, and Dystrophies Definitions. Dr. Victor Malinovsky
 Meet Libby Corneal Dysgenesis, Degeneration, and Dystrophies 2006 Dr. Victor Malinovsky Definitions Dysgenesis: (congenital anomalies) A development disorder that results in a congenital malformation of
Meet Libby Corneal Dysgenesis, Degeneration, and Dystrophies 2006 Dr. Victor Malinovsky Definitions Dysgenesis: (congenital anomalies) A development disorder that results in a congenital malformation of
Learn Connect Succeed. JCAHPO Regional Meetings 2015
 Learn Connect Succeed JCAHPO Regional Meetings 2015 Pediatric Cataracts: Complicated Cases and Controversies M. Edward Wilson, M.D. N. Edgar Miles Professor of Ophthalmology and Pediatrics Storm Eye Institute
Learn Connect Succeed JCAHPO Regional Meetings 2015 Pediatric Cataracts: Complicated Cases and Controversies M. Edward Wilson, M.D. N. Edgar Miles Professor of Ophthalmology and Pediatrics Storm Eye Institute
STAB INCISION GLAUCOMA SURGERY (SIGS)
 STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
STAB INCISION GLAUCOMA SURGERY (SIGS) AMAR AGARWAL
 STAB INCISION GLAUCOMA SURGERY (SIGS) AMAR AGARWAL SIGS or Stab Incision Glaucoma Surgery is a guarded filtration procedure that was introduced by me and is slowly but surely becoming popular amongst many
STAB INCISION GLAUCOMA SURGERY (SIGS) AMAR AGARWAL SIGS or Stab Incision Glaucoma Surgery is a guarded filtration procedure that was introduced by me and is slowly but surely becoming popular amongst many
STAB INCISION GLAUCOMA SURGERY (SIGS)
 STAB INCISION GLAUCOMA SURGERY (SIGS) DR. SOOSAN JACOB Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Youtube channel*: Dr. Soosan Jacob SIGS or Stab Incision Glaucoma Surgery is a guarded
STAB INCISION GLAUCOMA SURGERY (SIGS) DR. SOOSAN JACOB Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Youtube channel*: Dr. Soosan Jacob SIGS or Stab Incision Glaucoma Surgery is a guarded
Non Phaco Sutureless Cataract Surgery with Small Scleral Tunnel Incision Using Rigid PMMA IOLS
 Original Article Non Phaco Sutureless Cataract Surgery with Small Scleral Tunnel Incision Using Rigid PMMA IOLS Muhammad Hashim Qureshi Pak J Ophthalmol 2007, Vol. 23 No.1.......................................................................................
Original Article Non Phaco Sutureless Cataract Surgery with Small Scleral Tunnel Incision Using Rigid PMMA IOLS Muhammad Hashim Qureshi Pak J Ophthalmol 2007, Vol. 23 No.1.......................................................................................
COURSE DESCRIPTION BASIC FUNDAMENTALS
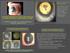 TACKLING POSTERIOR CAPSULE RUPTURE AND IOL IMPLANTATION: A VIDEO BASED COURSE TUESDAY - 29 th APRIL, 2014: 1.00 PM-2.30 PM, BCEC, ROOM 258 A ; SESSION 29-308 COURSE DESCRIPTION BASIC FUNDAMENTALS Early
TACKLING POSTERIOR CAPSULE RUPTURE AND IOL IMPLANTATION: A VIDEO BASED COURSE TUESDAY - 29 th APRIL, 2014: 1.00 PM-2.30 PM, BCEC, ROOM 258 A ; SESSION 29-308 COURSE DESCRIPTION BASIC FUNDAMENTALS Early
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg
 An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR)
 International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR) The International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubrics
International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR) The International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubrics
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
ICO-Ophthalmology Surgical Competence Assessment Rubric Vitrectomy (ICO-OSCAR:VIT)
 ICO-Ophthalmology Surgical Competence Assessment Rubric Vitrectomy (ICO-OSCAR:VIT) Date Resident Evaluator Novice (score = 2) Beginner (score = 3) Advanced Beginner (score = 4) Competent (score = 5) Not
ICO-Ophthalmology Surgical Competence Assessment Rubric Vitrectomy (ICO-OSCAR:VIT) Date Resident Evaluator Novice (score = 2) Beginner (score = 3) Advanced Beginner (score = 4) Competent (score = 5) Not
2/26/2017. Sameh Galal. M.D, FRCS Glasgow. Lecturer of Ophthalmology Research Institute of Ophthalmology
 Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
SECONDARY CAPSULOTOMY USING THE FEMTOSECOND LASER. Surendra Basti, MD Northwestern University Feinberg School of Medicine, Chicago, IL
 SECONDARY CAPSULOTOMY USING THE FEMTOSECOND LASER Surendra Basti, MD Northwestern University Feinberg School of Medicine, Chicago, IL SMALL PUPIL MANAGEMENT DURING FEMTO CATARACT SURGERY Surendra Basti,
SECONDARY CAPSULOTOMY USING THE FEMTOSECOND LASER Surendra Basti, MD Northwestern University Feinberg School of Medicine, Chicago, IL SMALL PUPIL MANAGEMENT DURING FEMTO CATARACT SURGERY Surendra Basti,
Innovative Iris Repair
 UNC Eye Symposium April 2, 2016 Chapel Hill, NC Innovative Iris Repair D Mark A. Terry, MD Director, Corneal Services Devers Eye Institute Scientific Director Lions VisionGift Research Lab Portland, Oregon,
UNC Eye Symposium April 2, 2016 Chapel Hill, NC Innovative Iris Repair D Mark A. Terry, MD Director, Corneal Services Devers Eye Institute Scientific Director Lions VisionGift Research Lab Portland, Oregon,
Interface Vitrectomy Offers an Alternative for Surgery
 Published in the January/February 2012 issue of Retinal Physician Magazine. Interface Vitrectomy Offers an Alternative for Surgery By leaving surface tension management agents in the eye, many vitreoretinal
Published in the January/February 2012 issue of Retinal Physician Magazine. Interface Vitrectomy Offers an Alternative for Surgery By leaving surface tension management agents in the eye, many vitreoretinal
OVERVIEW OF OCULAR MANAGEMENT IN MARFAN SYNDROME
 OVERVIEW OF OCULAR MANAGEMENT IN MARFAN SYNDROME Prepared by: Deborah Alcorn, MD, Dianna Milewicz, MD, and Irene H Maumenee, MD OCULAR FEATURES OF MARFAN SYNDROME Marfan syndrome is a dominantly inherited
OVERVIEW OF OCULAR MANAGEMENT IN MARFAN SYNDROME Prepared by: Deborah Alcorn, MD, Dianna Milewicz, MD, and Irene H Maumenee, MD OCULAR FEATURES OF MARFAN SYNDROME Marfan syndrome is a dominantly inherited
Original article. Amon M Pediatric micro-incision cataract surgery Nepal J Ophthalmol 2011;3(5):3-8
 Original article Surgical management challenges and clinical results of bimanual micro-incision phacoemulsification cataract surgery in children with congenital cataract Department of Ophthalmology and
Original article Surgical management challenges and clinical results of bimanual micro-incision phacoemulsification cataract surgery in children with congenital cataract Department of Ophthalmology and
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Complex cataract cases Managing catarocks : Better surgery on dense lenses, intumescent cataracts
 Complex cataract cases Managing catarocks : Better surgery on dense lenses, intumescent cataracts by Vanessa Caceres EyeWorld Contributing Writer Hypermature white cataract. According to Dr. Donaldson,
Complex cataract cases Managing catarocks : Better surgery on dense lenses, intumescent cataracts by Vanessa Caceres EyeWorld Contributing Writer Hypermature white cataract. According to Dr. Donaldson,
Cataract Surgery: Patient Information
 Cataract Surgery: Patient Information How do the Eyes Work? As light enters the eye, it first passes through the cornea the clear window of the eye. Because the cornea is curved, the light rays bend (refract).
Cataract Surgery: Patient Information How do the Eyes Work? As light enters the eye, it first passes through the cornea the clear window of the eye. Because the cornea is curved, the light rays bend (refract).
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
IOL Power Calculation for Children
 1 IOL Power Calculation for Children Rupal H. Trivedi, MD MSCR M. Edward Wilson, MD The authors have no financial interest in the subject matter of this presentation. Intraocular lens (IOL) implantation
1 IOL Power Calculation for Children Rupal H. Trivedi, MD MSCR M. Edward Wilson, MD The authors have no financial interest in the subject matter of this presentation. Intraocular lens (IOL) implantation
The crystalline lens, the cataract and its surgical treatment
 The crystalline lens, the cataract and its surgical treatment The crystalline lens position: behind the iris suspended by the zonular fibers structure: capsule cortex epinucleus nucleus function: to focus
The crystalline lens, the cataract and its surgical treatment The crystalline lens position: behind the iris suspended by the zonular fibers structure: capsule cortex epinucleus nucleus function: to focus
Pediatric traumatic cataract Presentation and Management. Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017
 Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Humanity s Vision Is Our Focus. The Ahmed Glaucoma Valve
 Humanity s Vision Is Our Focus The Ahmed Glaucoma Valve Dr. A. Mateen Ahmed President - New World Medical New World Medical is a high tech medical device company whose goal is to help humanity lead a better
Humanity s Vision Is Our Focus The Ahmed Glaucoma Valve Dr. A. Mateen Ahmed President - New World Medical New World Medical is a high tech medical device company whose goal is to help humanity lead a better
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Cataract Surgery in 2017 DARBY D. MILLER, MD MPH CORNEA, CATARACT AND REFRACTIVE SURGERY ASSISTANT PROFESSOR OF OPHTHALMOLOGY MAYO CLINIC FLORIDA Natural
Learn Connect Succeed JCAHPO Regional Meetings 2017 Cataract Surgery in 2017 DARBY D. MILLER, MD MPH CORNEA, CATARACT AND REFRACTIVE SURGERY ASSISTANT PROFESSOR OF OPHTHALMOLOGY MAYO CLINIC FLORIDA Natural
Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
Plate/Valve Specifications: Thickness: 0.9mm Width: 13.00mm Length: 16.00mm Surface Area: mm 2
 Distribué en France par FCI S.A.S. France Chirurgie Instrumentation SAS 20/22 rue Louis Armand 75015 PARIS Tél. 01.53.98.98.98 / Fax. 01.53.98.98.99 fci@fci.fr / www.fci.fr CATALOGUE DE VENTE Features:
Distribué en France par FCI S.A.S. France Chirurgie Instrumentation SAS 20/22 rue Louis Armand 75015 PARIS Tél. 01.53.98.98.98 / Fax. 01.53.98.98.99 fci@fci.fr / www.fci.fr CATALOGUE DE VENTE Features:
Clinical study of traumatic cataract and its management
 Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
Advanced Examination of the Retina: Scleral Indentation & Retinal 3-Mirror
 Advanced Examination of the Retina: Scleral Indentation & Retinal 3-Mirror Meredith Whiteside, OD, FAAO Nimesh Patel, OD, FAAO John Shan, OD, FAAO Please silence all mobile devices. Unauthorized recording
Advanced Examination of the Retina: Scleral Indentation & Retinal 3-Mirror Meredith Whiteside, OD, FAAO Nimesh Patel, OD, FAAO John Shan, OD, FAAO Please silence all mobile devices. Unauthorized recording
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique
 Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
Correlate the structure of the lens with its functions. Define cataract and describe its epidemiology Classify cataract on the basis of morphology,
 LENS Correlate the structure of the lens with its functions. Define cataract and describe its epidemiology Classify cataract on the basis of morphology, aetiology and maturity of cataract. Diagnose a case
LENS Correlate the structure of the lens with its functions. Define cataract and describe its epidemiology Classify cataract on the basis of morphology, aetiology and maturity of cataract. Diagnose a case
Venturi versus peristaltic pumps 33 vitrectomy dynamics 34 Fluorescein, vitreous staining 120
 Subject Index Accurus 35, 83 Aflibercept, diabetic macular edema management 167, 168 Air-forced infusion, Stellaris PC 12, 13 Alcon Constellation, see Constellation system Autoclave sterilization lens
Subject Index Accurus 35, 83 Aflibercept, diabetic macular edema management 167, 168 Air-forced infusion, Stellaris PC 12, 13 Alcon Constellation, see Constellation system Autoclave sterilization lens
EX-PRESS Glaucoma Filtration Device Surgical Procedure
 EX-PRESS Glaucoma Filtration Device Surgical Procedure Surgical Recommendations EX-PRESS Glaucoma Filtration Device preloaded device (plus 1 back-up) Sterile caliper Lid speculum Corneal forceps 0.12 forceps
EX-PRESS Glaucoma Filtration Device Surgical Procedure Surgical Recommendations EX-PRESS Glaucoma Filtration Device preloaded device (plus 1 back-up) Sterile caliper Lid speculum Corneal forceps 0.12 forceps
FROM CATARACTS TO CLARITY
 Cathy Cataracts FROM CATARACTS TO CLARITY If you re 55 or older, you may have cataracts and not even know it. What You Need to Know Seeing Beyond the Symptoms Cataracts are one of the leading causes of
Cathy Cataracts FROM CATARACTS TO CLARITY If you re 55 or older, you may have cataracts and not even know it. What You Need to Know Seeing Beyond the Symptoms Cataracts are one of the leading causes of
Complication and Visual Outcome after Peadiatric Cataract Surgery with or Without Intra Ocular Lens Implantation
 Original Article Complication and Visual Outcome after Peadiatric with or Without Intra Ocular Lens Implantation Mazhar-ul-Hasan, Umair A. Qidwai, Aziz-ur-Rehman, Nasir Bhatti, Rashid H. Alvi Pak J Ophthalmol
Original Article Complication and Visual Outcome after Peadiatric with or Without Intra Ocular Lens Implantation Mazhar-ul-Hasan, Umair A. Qidwai, Aziz-ur-Rehman, Nasir Bhatti, Rashid H. Alvi Pak J Ophthalmol
Mechanics of the Ahmed Glaucoma Valve
 Dr. A. Mateen Ahmed President & CEO - New World Medical, Inc. New World Medical, Inc. (NWMI) is a high tech medical device company whose goal is to help humanity lead a better life through improved technology
Dr. A. Mateen Ahmed President & CEO - New World Medical, Inc. New World Medical, Inc. (NWMI) is a high tech medical device company whose goal is to help humanity lead a better life through improved technology
Capsule fixation device for cataract surgery
 European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 143-146 SHORT COMMUNICATIONS & CASE REPORTS Capsule fixation device for cataract surgery N.M. SERGIENKO 1, Y.N. KONDRATENKO 1, A.K. YAKIMOV
European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 143-146 SHORT COMMUNICATIONS & CASE REPORTS Capsule fixation device for cataract surgery N.M. SERGIENKO 1, Y.N. KONDRATENKO 1, A.K. YAKIMOV
BAG-TO-THE-WALL TECHNIQUE FOR A SUBLUXATED LENS
 AG-TO-THE-WALL TECHNIQUE FOR A SULUXATED LENS A one-piece foldable lens is implanted in an eye after blunt trauma created a large zonular tear. Y CYRES KEIKI MEHTA, MS(Ophth), MCH(Ophth) This article describes
AG-TO-THE-WALL TECHNIQUE FOR A SULUXATED LENS A one-piece foldable lens is implanted in an eye after blunt trauma created a large zonular tear. Y CYRES KEIKI MEHTA, MS(Ophth), MCH(Ophth) This article describes
Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular Lens in Previous Vitrectomized Eyes
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
 European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Childhood Glaucoma. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Childhood Glaucoma. These podcasts are designed to give medical students an overview of key topics in pediatrics.
CATARACT SURGERY IN UVEITIS. Professor Harminder Singh Dua
 Research Institute of Ophthalmology, Cairo 11 th International Conference, 3-4 February, 2017 CATARACT SURGERY IN UVEITIS Professor Harminder Singh Dua MBBS, DO, DO(Lond), MS, MNAMS, FRCS, FRCOphth., FEBO,
Research Institute of Ophthalmology, Cairo 11 th International Conference, 3-4 February, 2017 CATARACT SURGERY IN UVEITIS Professor Harminder Singh Dua MBBS, DO, DO(Lond), MS, MNAMS, FRCS, FRCOphth., FEBO,
TITLE: Femtosecond Laser Cataract Surgery : How to Avoid and Manage Complications
 ASCRS 2016 Course Handouts TITLE: Femtosecond Laser Cataract Surgery : How to Avoid and Manage Complications Course Director: Dr Seng-Ei TI Faculty: Prof Soon-Phaik CHEE, Dr Ron YEOH This course discusses
ASCRS 2016 Course Handouts TITLE: Femtosecond Laser Cataract Surgery : How to Avoid and Manage Complications Course Director: Dr Seng-Ei TI Faculty: Prof Soon-Phaik CHEE, Dr Ron YEOH This course discusses
Clinical Study Dual Approach Using Vitrectorhexis Combined with Anterior Vitrectomy in Pediatric Cataract Surgery
 ISRN Ophthalmology Volume 2013, Article ID 124754, 5 pages http://dx.doi.org/10.1155/2013/124754 Clinical Study Dual Approach Using Vitrectorhexis Combined with Anterior Vitrectomy in Pediatric Cataract
ISRN Ophthalmology Volume 2013, Article ID 124754, 5 pages http://dx.doi.org/10.1155/2013/124754 Clinical Study Dual Approach Using Vitrectorhexis Combined with Anterior Vitrectomy in Pediatric Cataract
Slide 1. Slide 2. Slide 3. An EK For All Reasons: When and How to Perform DSAEK and DMEK. Financial Disclosure
 Slide 1 An EK For All Reasons: When and How to Perform DSAEK and DMEK M I C H A E L T A R A V E L L A, M D R I C H A R D D A V I D S O N, M D V I P U L S H A H, M D A A R O N W A I T E, M D Slide 2 Financial
Slide 1 An EK For All Reasons: When and How to Perform DSAEK and DMEK M I C H A E L T A R A V E L L A, M D R I C H A R D D A V I D S O N, M D V I P U L S H A H, M D A A R O N W A I T E, M D Slide 2 Financial
Anterior segment imaging
 Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
(PSEUDOPHAKOI)*t PERSONAL TECHNIQUES OF PSEUDOPHAKIA
 Brit. J. Ophthal. (1967) 51, 767 IRIS-CLIP AND IRIIDO-CAPSULAR LENS IMPLANTS (PSEUDOPHAKOI)*t PERSONAL TECHNIQUES OF PSEUDOPHAKIA BY C. D. BINKHORST Terneuzen, Netherlands THE iris-clip lens implant or
Brit. J. Ophthal. (1967) 51, 767 IRIS-CLIP AND IRIIDO-CAPSULAR LENS IMPLANTS (PSEUDOPHAKOI)*t PERSONAL TECHNIQUES OF PSEUDOPHAKIA BY C. D. BINKHORST Terneuzen, Netherlands THE iris-clip lens implant or
Original Article Capsular tension ring implantation after lens extraction for management of subluxated cataracts
 Int J Clin Exp Pathol 2014;7(7):3733-3738 www.ijcep.com /ISSN:1936-2625/IJCEP0000754 Original Article Capsular tension ring implantation after lens extraction for management of subluxated cataracts Xiao
Int J Clin Exp Pathol 2014;7(7):3733-3738 www.ijcep.com /ISSN:1936-2625/IJCEP0000754 Original Article Capsular tension ring implantation after lens extraction for management of subluxated cataracts Xiao
TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY
 TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY Traumatic cataract :Traumatic lens damage caused by mechanical injury and by physical forces (Ionising radiation,ir radiation, electrical
TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY Traumatic cataract :Traumatic lens damage caused by mechanical injury and by physical forces (Ionising radiation,ir radiation, electrical
FROM PRE-OP TO POST-OP, OPTIMIZE YOUR WORKFLOW WITH THE CATALYS SYSTEM MOBILE PATIENT BED.
 FROM PRE-OP TO POST-OP, OPTIMIZE YOUR WORKFLOW WITH THE CATALYS SYSTEM MOBILE PATIENT BED. PUSH THE LIMITS Imagine if your CATALYS System patient bed could: Optimize your productivity throughout the full
FROM PRE-OP TO POST-OP, OPTIMIZE YOUR WORKFLOW WITH THE CATALYS SYSTEM MOBILE PATIENT BED. PUSH THE LIMITS Imagine if your CATALYS System patient bed could: Optimize your productivity throughout the full
Hooks & Rings In The Management Of Subluxated Cataracts. Introduction. Introduction- Capsular Support 3/31/2015
 Hooks & Rings In The Management Of Subluxated Cataracts Financial Disclosure Ashu Agarwal Perfect Sight Centre New Delhi India I have no financial interests or relationships to disclose. 1 Introduction
Hooks & Rings In The Management Of Subluxated Cataracts Financial Disclosure Ashu Agarwal Perfect Sight Centre New Delhi India I have no financial interests or relationships to disclose. 1 Introduction
PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL
 PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL Endothelial keratoplasty (EK) has evolved at a brisk pace and the volume of data accumulated over the past 10 years has demonstrated that
PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL Endothelial keratoplasty (EK) has evolved at a brisk pace and the volume of data accumulated over the past 10 years has demonstrated that
DIABETIC VITRECTOMY INDICATIONS AND TECHNIQUES. steve charles
 DIABETIC VITRECTOMY INDICATIONS AND TECHNIQUES steve charles Traction Retinal Detachment Macula involved TRD TRD with rhegmatogenous component even if extra-macular TTRD Extra-Macular TRD should be observed
DIABETIC VITRECTOMY INDICATIONS AND TECHNIQUES steve charles Traction Retinal Detachment Macula involved TRD TRD with rhegmatogenous component even if extra-macular TTRD Extra-Macular TRD should be observed
You can see vivid colours again after cataract management at Sankar Foundation Eye Hospital
 The Department of Cataract in our Sankar Foundation is equipped with state-of-the-art operation theatres, surgical microscope phacoemulsification machine and microsurgical instruments. And also the department
The Department of Cataract in our Sankar Foundation is equipped with state-of-the-art operation theatres, surgical microscope phacoemulsification machine and microsurgical instruments. And also the department
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
FROM PRE-OP TO POST-OP, HELP OPTIMIZE YOUR WORKFLOW WITH THE CATALYS SYSTEM MOBILE PATIENT BED.
 FROM PRE-OP TO POST-OP, HELP OPTIMIZE YOUR WORKFLOW WITH THE CATALYS SYSTEM MOBILE PATIENT BED. PUSH THE LIMITS Imagine if your CATALYS System patient bed could: Optimize patient workflow throughout the
FROM PRE-OP TO POST-OP, HELP OPTIMIZE YOUR WORKFLOW WITH THE CATALYS SYSTEM MOBILE PATIENT BED. PUSH THE LIMITS Imagine if your CATALYS System patient bed could: Optimize patient workflow throughout the
2/6/2018. Andrew Siedlecki, M.D.
 Andrew Siedlecki, M.D. Siedlecki Cataract and Vision Care Optimization- Improved Uncorrected VA Reduced Spectacle Dependency Minimize Complications Fast Rehabilitation Provide Options for Patients Optometrists
Andrew Siedlecki, M.D. Siedlecki Cataract and Vision Care Optimization- Improved Uncorrected VA Reduced Spectacle Dependency Minimize Complications Fast Rehabilitation Provide Options for Patients Optometrists
Integrating the LenSx Laser Laser into your Clinic: Our advice for those considering it
 Integrating the LenSx Laser Laser into your Clinic: Our advice for those considering it (DAY) Facilitator: (Name) LenSx Laser Important Safety Information Caution United States Federal Law restricts this
Integrating the LenSx Laser Laser into your Clinic: Our advice for those considering it (DAY) Facilitator: (Name) LenSx Laser Important Safety Information Caution United States Federal Law restricts this
A Guide to Administering
 A Guide to Administering INDICATIONS AND USAGE YUTIQ (fluocinolone acetonide intravitreal implant) 0.18 mg is indicated for the treatment of chronic non-infectious uveitis affecting the posterior segment
A Guide to Administering INDICATIONS AND USAGE YUTIQ (fluocinolone acetonide intravitreal implant) 0.18 mg is indicated for the treatment of chronic non-infectious uveitis affecting the posterior segment
Megalocornea is a non-progressive, uniformly
 Case Report 191 Anterior Megalophthalmos Chien-Kuang Tsai, MD; Ing-Chou Lai, MD; Hsi-Kung Kuo, MD; Mei-Chung Teng, MD; Po-Chiung Fang, MD We describe a 36-year-old female who suffered from presenile cataract
Case Report 191 Anterior Megalophthalmos Chien-Kuang Tsai, MD; Ing-Chou Lai, MD; Hsi-Kung Kuo, MD; Mei-Chung Teng, MD; Po-Chiung Fang, MD We describe a 36-year-old female who suffered from presenile cataract
Nature and Science 2016;14(9)
 Comparison between Implantable Contact Lens (ICL) versus Acry Sof Cachet Phakic Intraocular Lenses in Correction of Moderate to High Myopia Khaled Nada, M. Sc.; Mohammed Attia, M. D and Ashraf El Habbak,
Comparison between Implantable Contact Lens (ICL) versus Acry Sof Cachet Phakic Intraocular Lenses in Correction of Moderate to High Myopia Khaled Nada, M. Sc.; Mohammed Attia, M. D and Ashraf El Habbak,
LASIK. Lens. Cornea. Iris. Vitreous. Macula. Retina
 LASIK Introduction LASIK surgery is a procedure that improves vision and can decrease or eliminate the need for eyeglasses or contact lenses. If you and your doctor decide that LASIK surgery is right for
LASIK Introduction LASIK surgery is a procedure that improves vision and can decrease or eliminate the need for eyeglasses or contact lenses. If you and your doctor decide that LASIK surgery is right for
Advanced Eyecare of Orange County/ Kim T. Doan, M.D.
 Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures
 Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age
 Original Article Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age Suma Ganesh 1, Reena Gupta 2, Sumita Sethi 3, Chandra Gurung 4, Raman Mehta 5 1,5 Dr. Shroff s Charitable
Original Article Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age Suma Ganesh 1, Reena Gupta 2, Sumita Sethi 3, Chandra Gurung 4, Raman Mehta 5 1,5 Dr. Shroff s Charitable
Minimally Invasive Surgery for the Removal of Posterior Intraocular Foreign Bodies
 Surgical Technique Minimally Invasive Surgery for the Removal of Posterior Intraocular Foreign Bodies Jesus Hernan Gonzalez Cortes 1, MD, PhD; Yunuen Bages Rousselon 1, MD; Jesus Emiliano Gonzalez Cantu
Surgical Technique Minimally Invasive Surgery for the Removal of Posterior Intraocular Foreign Bodies Jesus Hernan Gonzalez Cortes 1, MD, PhD; Yunuen Bages Rousselon 1, MD; Jesus Emiliano Gonzalez Cantu
KASHIKA ENTERPRISE PRODUCT LIST
 KASHIKA ENTERPRISE PRODUCT LIST S.No. PRODUCT QUANTITY KERATOPLASTY & CORNEA 1. ENDOTHELIAL PUNCH (PRECENTERED) 2. DISPOSABLE TREPHINES (6 TO 11MM) 3. ARTIFICIAL ANTERIOR CHAMBER (TITANIUM BODY) 4. SUCTION
KASHIKA ENTERPRISE PRODUCT LIST S.No. PRODUCT QUANTITY KERATOPLASTY & CORNEA 1. ENDOTHELIAL PUNCH (PRECENTERED) 2. DISPOSABLE TREPHINES (6 TO 11MM) 3. ARTIFICIAL ANTERIOR CHAMBER (TITANIUM BODY) 4. SUCTION
Retinal Tear and Detachment
 Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Frequently Asked Questions about General Ophthalmology:
 1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
Complex Cataract Surgery: Audit Considerations, Coding & Compliance
 Complex Cataract Surgery: Audit Considerations, Coding & Compliance Riva Lee Asbell Fort Lauderdale, FL INTRODUCTION The following is the CPT (Current Procedural Terminology) description of CPT code 66982:
Complex Cataract Surgery: Audit Considerations, Coding & Compliance Riva Lee Asbell Fort Lauderdale, FL INTRODUCTION The following is the CPT (Current Procedural Terminology) description of CPT code 66982:
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White
 Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Refractive Dilemma. Challenging Case
 Challenging Case Refractive Dilemma Section Editor: Alireza Baradaran-Rafii, MD Case presentation A 21-year old man was referred to an ophthalmology clinic insisting on getting rid of his glasses which
Challenging Case Refractive Dilemma Section Editor: Alireza Baradaran-Rafii, MD Case presentation A 21-year old man was referred to an ophthalmology clinic insisting on getting rid of his glasses which
SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP*
 Brit. J. Ophthal. (1959) 43, 361. SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP* BY V. CAVKA Belgrade, Yugoslavia AMONG the various operative procedures carried out for detachment of the retina,
Brit. J. Ophthal. (1959) 43, 361. SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP* BY V. CAVKA Belgrade, Yugoslavia AMONG the various operative procedures carried out for detachment of the retina,
Basic microsurgical suturing techniques for beginners
 ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
Trauma. steve charles
 Trauma steve charles Pathobiology of Trauma Hypocellular Vitreous Collagen Contraction (formerly called gel contraction) Poor Names: Vitreous Bands & Vitreous Membranes (always along vitreous surface or
Trauma steve charles Pathobiology of Trauma Hypocellular Vitreous Collagen Contraction (formerly called gel contraction) Poor Names: Vitreous Bands & Vitreous Membranes (always along vitreous surface or
Injury. Contusion Lamellar Laceration Laceration Rupture. Penetrating IOFB. Perforating
 Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
POSTTRAUMATIC WHITE CATARACT
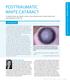 POSTTRAUMATIC WHITE CATARACT BY MARJAN FARID, MD; JEREMY Z. KIEVAL, MD; D. BRIAN KIM, MD; JASON R. MAYER, MD; AND BRANDON D. AYRES, MD CASE PRESENTATION A 34-year-old man sustains blunt trauma from a wrench
POSTTRAUMATIC WHITE CATARACT BY MARJAN FARID, MD; JEREMY Z. KIEVAL, MD; D. BRIAN KIM, MD; JASON R. MAYER, MD; AND BRANDON D. AYRES, MD CASE PRESENTATION A 34-year-old man sustains blunt trauma from a wrench
Clinical Evaluation of the BunnyLens IOL
 Clinical Evaluation of the BunnyLens IOL Introduction: BunnyLens is a foldable Hydrophlic Acrylic IOL with four ear shaped haptic design. The lens design offers many advantages in terms of: 1. Centration
Clinical Evaluation of the BunnyLens IOL Introduction: BunnyLens is a foldable Hydrophlic Acrylic IOL with four ear shaped haptic design. The lens design offers many advantages in terms of: 1. Centration
Written by Administrator Wednesday, 13 January :27 - Last Updated Thursday, 21 January :34
 angle closure glaucoma A type of glaucoma caused by a sudden and severe rise in eye pressure. Occurs when the pupil enlarges too much or too quickly, and the outer edge of the iris blocks the eye s drainage
angle closure glaucoma A type of glaucoma caused by a sudden and severe rise in eye pressure. Occurs when the pupil enlarges too much or too quickly, and the outer edge of the iris blocks the eye s drainage
Third Generation. Glaucoma Drainage Device
 MOLTENO 3 Third Generation Glaucoma Drainage Device A Step by Step Guide to Inserting the Molteno3 Glaucoma Drainage Device for Delayed or Immediate Drainage and either translimal or pars plana insertion
MOLTENO 3 Third Generation Glaucoma Drainage Device A Step by Step Guide to Inserting the Molteno3 Glaucoma Drainage Device for Delayed or Immediate Drainage and either translimal or pars plana insertion
Fate of anterior capsule tears during cataract surgery
 J CATARACT REFRACT SURG - VOL 32, OCTOBER 2006 Fate of anterior capsule tears during cataract surgery Frederico F. Marques, MD, Daniela M.V. Marques, MD, Robert H. Osher, MD, James M. Osher, MS PURPOSE:
J CATARACT REFRACT SURG - VOL 32, OCTOBER 2006 Fate of anterior capsule tears during cataract surgery Frederico F. Marques, MD, Daniela M.V. Marques, MD, Robert H. Osher, MD, James M. Osher, MS PURPOSE:
ALTERNATIVES TO PHAKIC IMPLANT SURGERY
 Visian ICL Consent INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness. Only you and your
Visian ICL Consent INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness. Only you and your
Prediction Error After Lens Implantation in Children With Axial Length Less than 22 mm Below 2 Yrs
 E-ISSN 2454-2784 Original Article Prediction Error After Lens Implantation in Children With Axial Length Less than 22 mm Below 2 Yrs Reena Gupta 1, Suma Ganesh 2, Chekitaan Singh 3, A.K Khurana 1 1 Regional
E-ISSN 2454-2784 Original Article Prediction Error After Lens Implantation in Children With Axial Length Less than 22 mm Below 2 Yrs Reena Gupta 1, Suma Ganesh 2, Chekitaan Singh 3, A.K Khurana 1 1 Regional
Specialist Referral Service Willows Information Sheets. Cataract surgery
 Specialist Referral Service Willows Information Sheets Cataract surgery An operating microscope in use A total cataract - the normally black pupil is bluish white Cataract surgery These notes do not cover
Specialist Referral Service Willows Information Sheets Cataract surgery An operating microscope in use A total cataract - the normally black pupil is bluish white Cataract surgery These notes do not cover
Clinical Study Continuous Curvilinear Capsulorhexis in Cataract Surgery Using a Modified 3-Bend Cystotome
 Ophthalmology Volume 2015, Article ID 412810, 5 pages http://dx.doi.org/10.1155/2015/412810 Clinical Study Continuous Curvilinear Capsulorhexis in Cataract Surgery Using a Modified 3-Bend Cystotome Yuan
Ophthalmology Volume 2015, Article ID 412810, 5 pages http://dx.doi.org/10.1155/2015/412810 Clinical Study Continuous Curvilinear Capsulorhexis in Cataract Surgery Using a Modified 3-Bend Cystotome Yuan
Clinical Study The Balanced Two-String Technique for Sulcus Intraocular Lens Implantation in the Absence of Capsular Support
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2015, Article ID 153963, 5 pages http://dx.doi.org/10.1155/2015/153963 Clinical Study The Balanced Two-String Technique for Sulcus Intraocular
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2015, Article ID 153963, 5 pages http://dx.doi.org/10.1155/2015/153963 Clinical Study The Balanced Two-String Technique for Sulcus Intraocular
Practical Care of the Cataract Patient with Retinal Disease
 Practical Care of the Cataract Patient with Retinal Disease Brooks R. Alldredge, OD, FAAO Kelly L. Cyr, OD, FAAO The Retina Center Eye Associates of New Mexico 4411 The 25 Way NE, Suite 325 Albuquerque,
Practical Care of the Cataract Patient with Retinal Disease Brooks R. Alldredge, OD, FAAO Kelly L. Cyr, OD, FAAO The Retina Center Eye Associates of New Mexico 4411 The 25 Way NE, Suite 325 Albuquerque,
Glaucoma. Cornea. Iris
 Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Cataract. A cataract is a clouding of the lens in your eye. It
 Cataract A cataract is a clouding of the lens in your eye. It affects your vision. Cataracts are very common in older people. By age 80, more than half of all Americans either have a cataract or have had
Cataract A cataract is a clouding of the lens in your eye. It affects your vision. Cataracts are very common in older people. By age 80, more than half of all Americans either have a cataract or have had
Start with ME. LEAVE A LEGACY OF EXCELLENT OUTCOMES FOR PATIENTS WITH ASTIGMATISM. TECNIS TORIC 1-PIECE IOL
 LEAVE A LEGACY OF EXCELLENT OUTCOMES FOR PATIENTS WITH ASTIGMATISM. Start with ME. TECNIS TORIC 1-PIECE IOL INDICATIONS: The TECNIS Toric 1-Piece Posterior Chamber Lens is indicated for the visual correction
LEAVE A LEGACY OF EXCELLENT OUTCOMES FOR PATIENTS WITH ASTIGMATISM. Start with ME. TECNIS TORIC 1-PIECE IOL INDICATIONS: The TECNIS Toric 1-Piece Posterior Chamber Lens is indicated for the visual correction
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Relationship between limbal incisions. angle. and the structures of the anterior chamber
 Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
