SURGICAL OUTCOME OF SIMULTANEOUS INTRAOCULAR LENS RESCUE AND SUTURELESS INTRASCLERAL TUNNEL FIXATION OF DISLOCATED INTRAOCULAR LENSES
|
|
|
- Claribel Mathews
- 5 years ago
- Views:
Transcription
1 SURGICAL OUTCOME OF SIMULTANEOUS INTRAOCULAR LENS RESCUE AND SUTURELESS INTRASCLERAL TUNNEL FIXATION OF DISLOCATED INTRAOCULAR LENSES MIN KIM, MD,* DONG H. LEE, MD,* HYOUNG J. KOH, MD,* SUNG C. LEE, MD, SUNG S. KIM, MD, PHD Purpose: To report short-term surgical outcomes of single-stage simultaneous rescue and sutureless intrascleral fixation of dislocated intraocular lens (s). Methods: Sixteen eyes of 16 patients who underwent simultaneous rescue and intrascleral fixation of dislocated 3-piece s were retrospectively evaluated. Partial thickness limbal-based scleral flaps ( mm) were created, and a 22-gauge round needle was used to create a sclerotomy at 1.5 mm from the limbus under the previously created scleral flap, and a 23-gauge trans pars plana vitrectomy was performed. Bimanual maneuvers using two 23-gauge end-grasping forceps under chandelier illumination and a wide-angle viewing system enabled 1 step rescue of s from the posterior vitreous cavity with 1 hand and simultaneous haptic externalization through sclerotomy with the other hand. An externalized haptic was placed into the 3-mm intrascleral tunnel created using a bent 26-gauge needle. Fibrin glue was used to fixate haptics and close the scleral flaps. Results: Intraocular lenses were successfully rescued and sclera-fixated through intrascleral tunnels in all 16 eyes (mean age, ± years). The mean preoperative logarithm of the minimum angle of resolution best-corrected visual acuity was 0.92 ± 0.68, and this significantly improved at 6 months to ± 0.36 (P = 0.003). During the follow-up period (10.1 ± 3.21 months), no significant change of endothelial cell count or central foveal thickness was noted postoperatively (P = and P = 0.979, respectively). There were no significant postoperative complications such as dislocation, decentration, retinal detachment, endophthalmitis, or postoperative hypotony. Conclusion: Simultaneous rescue and sutureless intrascleral haptic fixation of dislocated 3-piece s using bimanual maneuvers is an effective, safe, and minimally invasive surgical method to rescue and fixate the dislocated without further explant. RETINA 35: , 2015 Intraocular lens () dislocation is uncommon yet one of the more serious complications of cataract surgerywithseeminglyincreasingfrequencyinrecent years. 1 It can present in the form of either extracapsular out-of-the-bag dislocation or capsular bag complex dislocation in the posterior segment. 2 5 Traditionally, dislocated in the posterior segment requires pars plana vitrectomy, rescue, and removal of the through either a large corneal or scleral incision, followed by implantation of a secondary using various methods for scleral fixation of a new in the absence of capsular support. 1,6,7 This can usually be accomplished by transscleral fixation of posterior chamber s, iris fixation of s, or by implanting anterior chamber s However, the conventional method can be invasive, time consuming, technically challenging, and it may require manipulation of the s in the anterior chamber, potentially causing corneal endothelial damage. As a result, it can be associated with a higher rate of surgical complications such as corneal endothelial damage and risk for redislocation of the after a period because of suture degradation. 1,5,7 Despite these complications, there is no single standard of safe and effective surgical treatment for the management of 1450
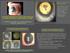
2 SIMULTANEOUS RESCUE AND SUTURELESS FIXATION OF KIM ET AL 1451 dislocated s. Thus, an effective surgical technique for simultaneous rescue and refixation of the dislocated, without a need for explanting the and using sutures, could be less invasive, leading to fewer occurrences of postoperative complications and better postoperative surgical outcomes. As the early work by Maggi and Maggi 14 first described the sutureless scleral fixation technique, intrascleral fixation of s without sutures has become more common, 14,15 and several variations of the technique have been introduced This method enables intrascleral fixation of a three-piece in the absence of capsular support without the use of any sutures. Also, 20-gauge pars plicata vitrectomy for repositioning of dislocated was reported in small case series of 5 eyes, 19 and similar techniques involving small-gauge vitrectomy and bimanual manipulation of the were introduced By modifying these various surgical techniques, using chandelier illumination, a wide-angle visualization system, and small-gauge sutureless vitrectomy, we have performed single-stage simultaneous rescue and fixation in patients with dislocation, thus simultaneously accomplishing two surgical goals. Using chandelier illumination, bimanual manipulation of dislocatedsintheposterior segment allows for simultaneous one-step rescue from the posterior vitreous cavity with one hand and externalization of the dislocated haptic through sclerotomy with the other hand, without further manipulation of the rescued in the anterior chamber. Here, we report the surgical outcome of single-stage simultaneous rescue and sutureless intrascleral tunnel refixation of a dislocated. Methods Patients We retrospectively reviewed all patients who had undergone simultaneous rescue and sutureless fixation of a dislocated between March 2012 and September All surgeries were performed by a single surgeon (M.K.) at Yonsei University Gangnam From the *Department of Ophthalmology, Gangnam Severance Hospital, Yonsei University College of Medicine, Seoul, Korea; and Department of Ophthalmology, Severance Hospital, Institute of Vision Research, Yonsei University College of Medicine, Seoul, Korea. Supported by a faculty research grant of Yonsei University College of Medicine for 2012 ( ). None of the authors have any conflicting interests to disclose. Supplemental digital content is available for this article. Direct URL citations appear in the printed text and are provided in the HTML and PDF versions of this article on the journal s Web site ( Reprint requests: Sung S. Kim, MD, PhD, Department of Ophthalmology, Severance Hospital, Institute of Vision Research, Yonsei University College of Medicine, 134 Sinchon-dong, Seodaemun-gu, Seoul, Korea ; semekim@yuhs.ac Severance Hospital, Seoul, Korea. The study was approved by the Institutional Review Board of Yonsei University Gangnam Severance Hospital and was conducted in accordance with the tenets of the Declaration of Helsinki. Informed consent was obtained from all patients. All patients underwent a standard ophthalmic examination, including measurement of best-corrected visual acuity (BCVA) with autorefraction with a Snellen chart, intraocular pressure measurement with a noncontact tonometer, slit-lamp examination, and dilated fundus examination at all preoperative and postoperative visits. The corneal endothelial cell density was measured by specular microscopy (CellChek CC-7000; Konan Medical Inc, Nishinomiya, Japan) preoperatively and postoperatively at 6 months. Central foveal thickness was measured with spectral domain optical coherence tomography (Cirrus OCT; Carl Zeiss Meditec, Dublin, CA) preoperatively and postoperatively at 3 months. Surgical Technique Conjunctival peritomy was performed first, and a 2.0 mm 2.0 mm partial thickness limbal-based scleral flap was created at either the inferior and superior limbus (if horizontal white-to-white [WTW] was $11 mm) or temporal and nasal limbus (if horizontal WTW was,11 mm) at approximately 180 apart, based on the preoperative measurement of horizontal WTW distance. Threeport 23-gauge trans pars plana vitrectomy was prepared by creating a sclerotomy at 3 mm from the limbus, and a 25-gauge chandelier illumination was placed inferonasally (see Video, Supplemental Digital Content 1, which demonstrates the key steps of the procedure). A 22-gauge round needle was used to create a sclerotomy at 1.5 mm from the limbus through the ciliary sulcus under the previously created scleral flap. A constellation vitrectomy system (Alcon Laboratories, Inc, Fort Worth, TX) was used for vitrectomy, and a wide-angle viewing system with a noncontact lens (BIOM 4; OCULUS Surgical Inc, Port St. Lucie, FL) was used for visualization of the posterior segment throughout the surgery. Posterior vitreous detachment was induced with suction of the 23-gauge vitrectomy probe, if posterior vitreous detachment was not present. While holding the with the forceps, vitrectomy was performed to free the dislocated from the vitreous. In case of in-the-bag dislocation with capsular bag adhesion (Figure 1, top left), a vitrectomy probe was used to free the from the posterior capsular bag complex while holding the with the intraocular forceps (Figure 1, top right). A thorough peripheral vitreous shaving was performed using a scleral indentator. Using two 23-gauge intraocular end-grasping forceps (Grieshaber; Alcon Laboratories, Inc) in both
3 1452 RETINA, THE JOURNAL OF RETINAL AND VITREOUS DISEASES 2015 VOLUME 35 NUMBER 7 hands, 1 hand was used to carefully grasp the haptic to lift up the dislocated to the level of the sclerotomy site and the other forceps was used to gently grasp the haptic and externalize the haptic through the previously created sclerotomy at 1.5 mm from the limbus (Figure 1, middle left). Then, the other haptic was pulled through the other sclerotomy site and externalized in a similar manner (Figure 1, middle right). Bimanual maneuvers using 23-gauge end-grasping forceps under chandelier illumination enabled 1-step rescue of the dislocated from the posterior vitreous cavity with 1 hand and simultaneous haptic externalization through sclerotomy with the other hand. After externalizing the haptics, a 3-mm long intrascleral tunnel was created using a bent 26-gauge needle, and the externalized haptic was tucked into the intrascleral tunnel as described previously 15 (Figure 1, bottom left). Fibrin glue (Tisseel; Baxter, Deerfield, IL) was used to fixate the haptics and close the scleral flaps. The conjunctiva was also closed with the fibrin glue. The 23-gauge sclerotomy sites were sutured with 7-0 Vicryl (Ethicon, Somerville, NJ) if leakage was noted. Topical antibiotics and steroids were used in all patients postoperatively. Statistical Analysis SPSS 18.0 software was used for statistical analysis (SPSS Inc, Chicago, IL). The BCVA was converted to Fig. 1. Patient (Case 14) with in-the-bag dislocation. A. Preoperative wide-angle photograph of in-the-bag dislocation into the vitreous cavity. B. A vitrectomy probe was used to free the from the posterior capsular bag adhesion while holding the with the intraocular forceps. C. Using two 23-gauge intraocular endgrasping forceps in both hands, rescue of under chandelier illumination was performed by carefully grasping the haptic to lift up the dislocated to the level of the sclerotomy site and the other forceps was used to gently grasp the haptic and externalize the haptic through the previously created sclerotomy at 1.5 mm from the limbus. D. Externalization of the other haptic of rescued through the opposite sclerotomy site in a similar manner. E. The externalized haptic was tucked into the 3-mm long intrascleral tunnel created previously with a bent 26-gauge needle.
4 SIMULTANEOUS RESCUE AND SUTURELESS FIXATION OF KIM ET AL 1453 the logarithm of the minimum angle of resolution (logmar), and the Wilcoxon signed-rank test was performed to analyze the significance of change in BCVA, endothelial cell count, and central foveal thickness preoperatively versus postoperatively. A P, 0.05 was considered significant. Results The s were successfully rescued and sclerafixated through intrascleral tunnels without sutures in all 16 eyes of 16 patients (11 males, 5 females; mean age, ± years; Table 1). The mean duration of time to dislocation from previous cataract surgery was 5.19 ± 3.1 years, and the mean follow-up period was 10.1 ± 3.21 months. The detailed clinical features and postoperative outcome of patients are presented in Table 2. All patients, except Patient 14, had associated ocular conditions such as complicated cataract surgery, ocular trauma, nystagmus, or pseudoexfoliation syndrome. There were two cases with capsular bag complex dislocation, both of which were successfully rescued, and the s were safely freed from the capsular bag complex by vitrectomy. Table 1. Baseline Characteristics of Patients and Surgical Outcome Characteristics Value Number of eyes (patients) 16 Age (mean ± SD), years ± Gender (male:female) 11:5 Time to dislocation from 5.19 ± 3.1 previous surgery, years Follow-up (mean ± SD), 10.1 ± 3.21 months Preoperative parameters Baseline logmar UCVA 1.16 ± 0.65 (mean ± SD) Baseline logmar BCVA 0.92 ± 0.68 (mean ± SD) Baseline endothelial cell ± count Baseline CFT, mm ± Baseline IOP, mmhg 16 ± 7.03 Postoperative parameters LogMAR BCVA at ± 0.42 (P = 0.001)* months (mean ± SD) LogMAR BCVA at ± 0.36 (P = 0.003)* months (mean ± SD) Endothelial cell count ± (P = 0.203)* at 6 months CFT at 3 months, mm ± (P = 0.979)* IOP at 6 months, mmhg ± 3.99 (P = 0.32)* *Compared with baseline values. CFT, central foveal thickness; IOP, intraocular pressure; logmar, logarithm of the minimum angle of resolution; SD, standard deviation; UCVA, uncorrected visual acuity. The mean preoperative logmar BCVA was 0.92 ± 0.68, and the mean postoperative logmar BCVA at 3 months and at 6 months were 0.38 ± 0.42 and ± 0.36, respectively. All eyes attained statistically significant improvement in BCVA at postoperative 3 and 6 months (P = and P = 0.003, respectively). There was no significant reduction of endothelial cell count postoperatively at 6 months (P = 0.203), and no significant change of central foveal thickness as measured by spectral domain optical coherence tomography or intraocular pressure was noted at postoperative 3 months (P = and P = 0.32, respectively; Table 1). The s remained well fixated and stable postoperatively in all eyes (Figure 2). The mean preoperative cylinder was 2.39 ± 2.08, and the mean postoperative cylinder was 2.42 ± There was no significant change in cylinder, postoperatively (P = 0.755). Transient vitreous hemorrhage developed in 1 patient during the immediate postoperative follow-up period, which resolved within 1 week without further significant complication. Other postoperative complications included iris capture by the in 1 eye (6.3%) and transient ocular hypertension in 1 eye (6.3%). No other significant postoperative complications, such as postoperative hypotony, endophthalmitis, retinal detachment, dislocation, decentration, cystoid macular edema, or choroidal detachment were found during the follow-up period. Discussion The management of dislocation presents two unique challenges to surgeons. One must decide whether to remove the dislocated and perform a new implant or reposition and refixate the dislocated using various surgical techniques. The former procedure necessitates the creation of a large corneal/scleral incision for explant, which may cause unwanted postoperative astigmatism. Even if the dislocated is rescued and used again for refixation to perform either iris fixation or transscleral suture fixation, conventional methods involve manipulation of the in the anterior chamber and placement of additional sutures for fixation of the haptics, which can be technically challenging and time consuming. Moreover, additional risks associated with sutured s include increased risk of bleeding and suture erosion with subsequent malposition or dislocation. Recently, sutureless techniques for the scleral fixation of a posterior chamber and similar techniques using small-gauge vitrectomy and bimanual manipulation of the have been introduced. 15,18 25 With some modification of this technique, using a small-gauge
5 Associated Ocular Conditions From Previous Surgery Table 2. Clinical Features and Postoperative Surgical Outcome of Each Patients Time to Dislocation From Previous Surgery, Years Type of Dislocation at Presentation WTW Distance, mm Postoperative logmar BCVA at 6 Months Cases Sex/ Age Preoperative logmar BCVA Direction of Fixation Postoperative Complications 1 M/52 PCR and sulcus-fixated 14 Out-of-the-bag Vertical Transient ocular hypertension 2 M/72 PCR and sulcus-fixated 5 Out-of-the-bag Vertical None 3 M/44 PCR and sulcus-fixated 3 Out-of-the-bag Vertical None 4 M/38 Nystagmus 6 In-the-bag Vertical iris capture 5 M/70 Pseudoexfoliation 2 Out-of-the-bag Horizontal None syndrome, glaucoma 6 F/76 PCR and sulcus-fixated 3 Out-of-the-bag Vertical None 7 F/67 PCR and sulcus-fixated 2 Out-of-the-bag Vertical None 8 F/47 Trauma 5 Out-of-the-bag Horizontal None 9 M/73 PCR and sulcus-fixated 3 Out-of-the-bag Vertical None 10 M/82 Pseudoexfoliation 4 Out-of-the-bag Vertical None 11 M/50 PCR and sulcus-fixated 7 Out-of-the-bag Vertical Transient vitreous hemorrhage 6 Out-of-the-bag Vertical None 12 F/63 PCR and sulcus-fixated 13 M/49 Trauma 4 Out-of-the-bag Vertical None 14 M/66 None 7 In-the-bag Vertical None 15 M/59 Trauma 9 Out-of-the-bag Vertical None 16 F/44 PCR and sulcus-fixated logmar, logarithm of the minimum angle of resolution; PCR, posterior capsule rupture. 3 Out-of-the-bag Horizontal None 1454 RETINA, THE JOURNAL OF RETINAL AND VITREOUS DISEASES 2015 VOLUME 35 NUMBER 7
6 SIMULTANEOUS RESCUE AND SUTURELESS FIXATION OF KIM ET AL 1455 Fig. 2. Postoperative slit-lamp photograph of a patient with vertical fixation shows a well-centered fixated at postoperative Day 7. vitrectomy system, a wide-angle viewing system, chandelier illumination, and simultaneous use of two intraocular forceps bimanually, we were able to successfully perform a single-stage simultaneous rescue and refixation of dislocated without using any sutures. Use of a wide-angle viewing system under chandelier illumination allowed bimanual surgery by freeing one hand, thereby enabling simultaneous manipulation of both haptics and good visualization of the posterior segment, including the vitreous base, while lifting up the dislocated into the sclerotomy plane. There are several advantages of this technique. First of all, as no explantation was required with this technique, we could avoid the construction of a large corneal or scleral wound for the removal of dislocated and thus prevent creation of visually significant astigmatism. Avoiding the creation of large corneal/ scleral wounds allows surgery to be performed in a closed system, reducing intraocular pressure fluctuations. Utilization of dislocated s without explantation can reduce surgical time and potential phototoxicity to the retina, which is associated with longer surgical times. Second, this technique enabled direct rescue and subsequent externalization of the haptics without any further manipulation of the in the anterior segment for explantation, thereby minimizing any potential complications associated with the cornea, as manipulations in the anterior chamber may increase the risk for developing intraocular inflammation and corneal endothelial damage. Third, compared with other previously known methods for scleral fixation of s, this technique does not require the use of any sutures for fixation, thereby avoiding suture-related complications such as suture-associated inflammation/infection, suture degradation, and resultant redislocation Furthermore, this could contribute to less postoperative pain and inflammation, as no scleral sutures would be required, and no large corneal/scleral incision for removal would be needed. Fourth, because complete wound healing in scleral tissue can take up to 3 months, 30 placement of the haptic inside the intrascleral tunnel and fixation with fibrin glue can stabilize the immediately in the early postoperative period, thus may lessen the chance of redislocation. Furthermore, the use of fibrin glue helps stabilize the haptic to the sclera and seals the flap, potentially reducing the risk for infection and postoperative hypotony. It may also prevent transverse movement of haptics within the scleral tunnel, and this technique can thus be used successfully even in a patient with recurrent dislocation because of nystagmus (as in Case 4). Because the haptic was placed in its normal configurationintothe intrascleral tunnel without any traction, stabilizing the axial positioning of the, there was no apparent tilt or decentration during the follow-up. Furthermore, the procedure does not require the use of any specifically designed instruments, such as special forceps for handling. In our study, the 23-gauge end-grasping forceps for internal limiting membrane peeling were used for handling of the without any difficulty. Kumar et al 19 previously reported using 20-gauge pars plicata vitrectomy for repositioning of the dislocated s in 5 eyes. Although their technique was successfully performed in five eyes, performing vitrectomy and haptic externalization through pars plicata presents potential risk for intraoperative bleeding. Our technique uses pars plana approach for performing vitrectomy and rescuing dislocated s, thereby providing a better safety profile. There are some caveats in performing this surgical procedure. It is important to maintain the reverse S configuration of the dislocated while lifting it up to the sclerotomy plane, as sudden tilting or movement of the forceps could result in rotation, making it difficult to externalize its haptic. In cases of flipped s, because both hands are available for manipulations, the can be safely rotated upside down before externalizing the haptic, and this also can be safely performed without having to position the in the anterior chamber. It is also important to perform a complete vitrectomy with shaving of the vitreous base to ensure no vitreous traction, as lifting up the dislocated can cause undue vitreoretinal traction, resulting in postoperative retinal break or detachment. Although we were able to successfully remove the thick Soemmering s rings from the in two cases with dislocation of the capsular bag complex, vitrectomy in those cases can be somewhat challenging, as it can fall back into the vitreous cavity. Regarding the optimal location of scleral flap, a limbal-based scleral flap was created at the inferior
7 1456 RETINA, THE JOURNAL OF RETINAL AND VITREOUS DISEASES 2015 VOLUME 35 NUMBER 7 and superior limbus for vertical fixation of s, if WTW was $11 mm, because authors initially believed that there would be less haptics to place within the intrascleral tunnel if placed horizontally. However, contrary to our belief, studies have demonstrated the inaccuracy of WTW measurement at predicting the horizontal diameter of the ciliary sulcus, as there was a poor correlation between external WTW measurements and sulcus-tosulcus measurements using ultrasound biomicroscopy. In fact, vertical sulcus-to-sulcus diameter was found to be longer than the horizontal sulcus-to-sulcus diameter. 31 Thus, one could argue in favor of horizontal placement of haptics for maximum intrascleral haptic length instead of vertical placement, and this is one of the limitations of the study. There are several limitations to our study. Our followup period was limited, but there were no cases of any significant postoperative complications such as retinal detachment or redislocation, except for one case of transient vitreous hemorrhage. Another disadvantage of this technique was that it could only be performed with 3- piece s and could not be used in cases with dislocation of single-piece foldable s, as the haptics were not firm enough to externalize and bury into the scleral tunnels. Also, there is a potential of breakage of haptics due to an undue stress on haptic optic junctions of the while externalizing the haptics through the sclerotomy, but this can be prevented by careful and gentle manipulation of the with forceps. Although no significant tilt or decentration was noted by slitlamp examination during the postoperative follow-up period, the degree of tilt was not exactly quantified using advanced imaging modalities such as anterior segment optical coherence tomography. In conclusion, our technique of single-stage simultaneous rescue and sutureless intrascleral haptic fixation of a dislocated, using bimanual maneuver under chandelier illumination, seems to be an effective, safe, and minimally invasive surgical method to rescue and fixate the dislocated without having to explant it. Further studies with more patients and longer follow-up are warranted in the near future. Key words: dislocated, rescue, scleral fixation, sutureless fixation. Acknowledgments The authors acknowledge Dong Su Jang for his assistance in creating illustrative figures. References 1. Kim SS, Smiddy WE, Feuer W, Shi W. Management of dislocated intraocular lenses. Ophthalmology 2008;115: Gross JG, Kokame GT, Weinberg DV. In-the-bag intraocular lens dislocation. Am J Ophthalmol 2004;137: Gimbel HV, Condon GP, Kohnen T, et al. Late in-the-bag intraocular lens dislocation: incidence, prevention, and management. J Cataract Refract Surg 2005;31: Hayashi K, Hirata A, Hayashi H. Possible predisposing factors for in-the-bag and out-of-the-bag intraocular lens dislocation and outcomes of intraocular lens exchange surgery. Ophthalmology 2007;114: Pueringer SL, Hodge DO, Erie JC. Risk of late intraocular lens dislocation after cataract surgery, : a populationbased study. Am J Ophthalmol 2011;152: Fernandez-Buenaga R, Alio JL, Perez-Ardoy AL, et al. Late inthe-bag intraocular lens dislocation requiring explantation: risk factors and outcomes. Eye (Lond) 2013;27: ; quiz Jakobsson G, Zetterberg M, Sundelin K, Stenevi U. Surgical repositioning of intraocular lenses after late dislocation: complications, effect on intraocular pressure, and visual outcomes. J Cataract Refract Surg 2013;39: Zeh WG, Price FW Jr. Iris fixation of posterior chamber intraocular lenses. J Cataract Refract Surg 2000;26: Bloom SM, Wyszynski RE, Brucker AJ. Scleral fixation suture for dislocated posterior chamber intraocular lens. Ophthalmic Surg 1990;21: Schneiderman TE, Johnson MW, Smiddy WE, et al. Surgical management of posteriorly dislocated silicone plate haptic intraocular lenses. Am J Ophthalmol 1997;123: Maguire AM, Blumenkranz MS, Ward TG, Winkelman JZ. Scleral loop fixation for posteriorly dislocated intraocular lenses. Operative technique and long-term results. Arch Ophthalmol 1991;109: Chan CK. An improved technique for management of dislocated posterior chamber implants. Ophthalmology 1992;99: Por YM, Lavin MJ. Techniques of intraocular lens suspension in the absence of capsular/zonular support. Surv Ophthalmol 2005;50: Maggi R, Maggi C. Sutureless scleral fixation of intraocular lenses. J Cataract Refract Surg 1997;23: Agarwal A, Kumar DA, Jacob S, et al. Fibrin glue-assisted sutureless posterior chamber intraocular lens implantation in eyes with deficient posterior capsules. J Cataract Refract Surg 2008;34: Scharioth GB, Prasad S, Georgalas I, et al. Intermediate results of sutureless intrascleral posterior chamber intraocular lens fixation. J Cataract Refract Surg 2010;36: Falavarjani KG, Modarres M, Foroutan A, Bakhtiari P. Fibrin glue-assisted sutureless scleral fixation. J Cataract Refract Surg 2009;35:795; author reply Gabor SG, Pavlidis MM. Sutureless intrascleral posterior chamber intraocular lens fixation. J Cataract Refract Surg 2007;33: Kumar DA, Agarwal A, Jacob S, et al. Repositioning of the dislocated intraocular lens with sutureless 20-gauge vitrectomy. Retina 2010;30: Yamane S, Inoue M, Arakawa A, Kadonosono K. Sutureless 27- gauge needle-guided intrascleral intraocular lens implantation with lamellar scleral dissection. Ophthalmology 2014;121: Ohta T, Toshida H, Murakami A. Simplified and safe method of sutureless intrascleral posterior chamber intraocular lens fixation: Y-fixation technique. J Cataract Refract Surg 2014;40: Prasad S. Transconjunctival sutureless haptic fixation of posterior chamber : a minimally traumatic approach for rescue or secondary implantation. Retina 2013;33:
8 SIMULTANEOUS RESCUE AND SUTURELESS FIXATION OF KIM ET AL Liu S, Cheng S. Modified method of sutureless intrascleral posterior chamber intraocular lens fixation without capsular support. Eur J Ophthalmol 2013;23: Totan Y, Karadag R. Trocar-assisted sutureless intrascleral posterior chamber foldable intra-ocular lens fixation. Eye (Lond) 2012;26: Prenner JL, Feiner L, Wheatley HM, Connors D. A novel approach for posterior chamber intraocular lens placement or rescue via a sutureless scleral fixation technique. Retina 2012;32: Price MO, Price FW Jr, Werner L, et al. Late dislocation of scleral-sutured posterior chamber intraocular lenses. J Cataract Refract Surg 2005;31: McCluskey P, Harrisberg B. Long-term results using scleralfixated posterior chamber intraocular lenses. J Cataract Refract Surg 1994;20: Solomon K, Gussler JR, Gussler C, Van Meter WS. Incidence and management of complications of transsclerally sutured posterior chamber lenses. J Cataract Refract Surg 1993;19: Vote BJ, Tranos P, Bunce C, et al. Long-term outcome of combined pars plana vitrectomy and scleral fixated sutured posterior chamber intraocular lens implantation. Am J Ophthalmol 2006;141: Lee KH, Kim MS, Hahn TW, Kim JH. Comparison of histologic findings in wound healing of rabbit scleral homografts with fibrin glue (Tisseel) and suture material. J Refract Surg 1995;11: Oh J, Shin HH, Kim JH, et al. Direct measurement of the ciliary sulcus diameter by 35-megahertz ultrasound biomicroscopy. Ophthalmology 2007;114:
Visual outcome and early complications of sutureless and glueless scleral fixated intraocular lens
 Original article Visual outcome and early complications of sutureless and glueless scleral fixated intraocular lens Lalit Agarwal, Nisha Agrawal, Rajya Laxmi Gurung, Rahul Chaubey, Bhaskar kumar Jha, Bishwa
Original article Visual outcome and early complications of sutureless and glueless scleral fixated intraocular lens Lalit Agarwal, Nisha Agrawal, Rajya Laxmi Gurung, Rahul Chaubey, Bhaskar kumar Jha, Bishwa
Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular Lens in Previous Vitrectomized Eyes
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
COURSE DESCRIPTION BASIC FUNDAMENTALS
 TACKLING POSTERIOR CAPSULE RUPTURE AND IOL IMPLANTATION: A VIDEO BASED COURSE TUESDAY - 29 th APRIL, 2014: 1.00 PM-2.30 PM, BCEC, ROOM 258 A ; SESSION 29-308 COURSE DESCRIPTION BASIC FUNDAMENTALS Early
TACKLING POSTERIOR CAPSULE RUPTURE AND IOL IMPLANTATION: A VIDEO BASED COURSE TUESDAY - 29 th APRIL, 2014: 1.00 PM-2.30 PM, BCEC, ROOM 258 A ; SESSION 29-308 COURSE DESCRIPTION BASIC FUNDAMENTALS Early
Yong Un Shin, 1,2 Mincheol Seong, 1,2 Hee Yoon Cho, 1,2 and Min Ho Kang 1,2. 1. Introduction
 Hindawi Ophthalmology Volume 2017, Article ID 2683415, 4 pages https://doi.org/10.1155/2017/2683415 Research Article Novel Technique to Overcome the Nonavailability of a Long Needle 9-0 Polypropylene Suture
Hindawi Ophthalmology Volume 2017, Article ID 2683415, 4 pages https://doi.org/10.1155/2017/2683415 Research Article Novel Technique to Overcome the Nonavailability of a Long Needle 9-0 Polypropylene Suture
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: Continuous curvilinear capsulorhexis, phacoemulsification and in-the-bag placement of
 SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM INTRODUCTION
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM INTRODUCTION
2/26/2017. Sameh Galal. M.D, FRCS Glasgow. Lecturer of Ophthalmology Research Institute of Ophthalmology
 Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
 European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
Temporary Haptic Externalization and Four-point Fixation of Intraocular Lens in Scleral Fixation to Enhance Stability
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(1):23-28 https://doi.org/10.3341/kjo.2017.0038 Original Article Temporary Haptic Externalization and Four-point Fixation of Intraocular Lens
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(1):23-28 https://doi.org/10.3341/kjo.2017.0038 Original Article Temporary Haptic Externalization and Four-point Fixation of Intraocular Lens
Navigating the Options for the Treatment of Intraocular Lens Malposition
 Incorporating current trials and technology into clinical practice Howard F. Fine Practical Retina Co-Editor There has been a wave of new and innovative techniques for vitreoretinal surgeons in the management
Incorporating current trials and technology into clinical practice Howard F. Fine Practical Retina Co-Editor There has been a wave of new and innovative techniques for vitreoretinal surgeons in the management
Electronic poster presentations
 Electronic poster presentations Cataract Surgery E-00002 Blue-light exposure in an animal model of uveal melanoma B.F. Fernandes, S. Di Cesare, S. Maloney, J.-C. Marshall, W. Dawson, M.N. Burnier, Jr.
Electronic poster presentations Cataract Surgery E-00002 Blue-light exposure in an animal model of uveal melanoma B.F. Fernandes, S. Di Cesare, S. Maloney, J.-C. Marshall, W. Dawson, M.N. Burnier, Jr.
Scleral Buckling Using a Non-contact Wide-Angle Viewing System with a 25-Gauge Chandelier Endoilluminator
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(6):533-537 https://doi.org/10.3341/kjo.2017.0044 Original Article Scleral Buckling Using a Non-contact Wide-Angle Viewing System with a 25-Gauge
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(6):533-537 https://doi.org/10.3341/kjo.2017.0044 Original Article Scleral Buckling Using a Non-contact Wide-Angle Viewing System with a 25-Gauge
Late Intraocular Lens Subluxation in Patients with Uveitis
 Late Intraocular Lens Subluxation in Patients with Uveitis LR Steeples, NP Jones Manchester Royal Eye Hospital Introduction Late in-the-bag IOL subluxation is an unusual complication of phacoemulsification
Late Intraocular Lens Subluxation in Patients with Uveitis LR Steeples, NP Jones Manchester Royal Eye Hospital Introduction Late in-the-bag IOL subluxation is an unusual complication of phacoemulsification
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT
 SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM EXCHANGE FOR
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM EXCHANGE FOR
Brijesh Takkar 1, Shorya Vardhan Azad 1, Neelima Aron 1, Ravi Bypareddy 1, Rajvardhan Azad 2. Introduction
 Original Article Page 1 of 7 Combined pars plana vitrectomy and suture less scleral fixation of foldable intraocular lens: single surgery visual rehabilitation of dislocated lens/intraocular lens Brijesh
Original Article Page 1 of 7 Combined pars plana vitrectomy and suture less scleral fixation of foldable intraocular lens: single surgery visual rehabilitation of dislocated lens/intraocular lens Brijesh
Combined 23-gauge transconjunctival vitrectomy and scleral fixation of intraocular lens without conjunctival dissection in managing lens complications
 Yeung et al. BMC Ophthalmology (2018) 18:108 https://doi.org/10.1186/s12886-018-0776-4 RESEARCH ARTICLE Open Access Combined 23-gauge transconjunctival vitrectomy and scleral fixation of intraocular lens
Yeung et al. BMC Ophthalmology (2018) 18:108 https://doi.org/10.1186/s12886-018-0776-4 RESEARCH ARTICLE Open Access Combined 23-gauge transconjunctival vitrectomy and scleral fixation of intraocular lens
Clinical Study The Balanced Two-String Technique for Sulcus Intraocular Lens Implantation in the Absence of Capsular Support
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2015, Article ID 153963, 5 pages http://dx.doi.org/10.1155/2015/153963 Clinical Study The Balanced Two-String Technique for Sulcus Intraocular
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2015, Article ID 153963, 5 pages http://dx.doi.org/10.1155/2015/153963 Clinical Study The Balanced Two-String Technique for Sulcus Intraocular
84 Year Old with Rosacea
 84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
Capsule fixation device for cataract surgery
 European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 143-146 SHORT COMMUNICATIONS & CASE REPORTS Capsule fixation device for cataract surgery N.M. SERGIENKO 1, Y.N. KONDRATENKO 1, A.K. YAKIMOV
European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 143-146 SHORT COMMUNICATIONS & CASE REPORTS Capsule fixation device for cataract surgery N.M. SERGIENKO 1, Y.N. KONDRATENKO 1, A.K. YAKIMOV
In the absence of capsular support, the ophthalmic
 SECTION CO-EDITORS: ROHIT ROSS LAKHANPAL, MD; AND THOMAS ALBINI, MD A print & video series from the Vit-Buckle Society IOL Fixation Techniques BY EFREM D. MANDELCORN, MD, FRCSC; JONATHAN PRENNER, MD; AND
SECTION CO-EDITORS: ROHIT ROSS LAKHANPAL, MD; AND THOMAS ALBINI, MD A print & video series from the Vit-Buckle Society IOL Fixation Techniques BY EFREM D. MANDELCORN, MD, FRCSC; JONATHAN PRENNER, MD; AND
Title. with prior vitrectomy. Author(s) Takashi. Issue Date Wichtig Editore.
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Spontaneous dislocation of in-the-b with prior vitrectomy Matsumoto, Makiko; Yamada, Koki; Ue Azusa; Tsuiki, Eiko; Kumagami, Take Takashi European
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Spontaneous dislocation of in-the-b with prior vitrectomy Matsumoto, Makiko; Yamada, Koki; Ue Azusa; Tsuiki, Eiko; Kumagami, Take Takashi European
Anterior segment imaging
 Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 78/ Sept 28, 2015 Page 13570
 SAFETY AND EFFECTIVENESS OF 20G SUTURELESS PARS PLANA VITRECTOMY: A PROSPECTIVE STUDY AT SAROJINI DEVI HOSPITAL, HYDERABAD Rajalingam Vairagyam 1, Karunakar B 2, Pasyanthi B 3, B. Y. Babu Rao 4, Rita Bahadur
SAFETY AND EFFECTIVENESS OF 20G SUTURELESS PARS PLANA VITRECTOMY: A PROSPECTIVE STUDY AT SAROJINI DEVI HOSPITAL, HYDERABAD Rajalingam Vairagyam 1, Karunakar B 2, Pasyanthi B 3, B. Y. Babu Rao 4, Rita Bahadur
Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients
 Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Capture of intraocular lens optic by residual capsular opening in secondary implantation: long-term follow-up
 Tian et al. BMC Ophthalmology (2018) 18:84 https://doi.org/10.1186/s12886-018-0741-2 RESEARCH ARTICLE Open Access Capture of intraocular lens optic by residual capsular opening in secondary implantation:
Tian et al. BMC Ophthalmology (2018) 18:84 https://doi.org/10.1186/s12886-018-0741-2 RESEARCH ARTICLE Open Access Capture of intraocular lens optic by residual capsular opening in secondary implantation:
Net technique for intraocular lens support in aphakia without capsular support
 DOI 10.1186/s40942-017-0085-8 International Journal of Retina and Vitreous ORIGINAL ARTICLE Open Access Net technique for intraocular lens support in aphakia without capsular support Fernando José De Novelli
DOI 10.1186/s40942-017-0085-8 International Journal of Retina and Vitreous ORIGINAL ARTICLE Open Access Net technique for intraocular lens support in aphakia without capsular support Fernando José De Novelli
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
STAB INCISION GLAUCOMA SURGERY (SIGS)
 STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
Pediatric traumatic cataract Presentation and Management. Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017
 Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Long-term Outcomes of Vitreous Floaters Management with 23-Gauge Transconjunctival Sutureless Vitrectomy
 Long-term Outcomes of Vitreous Floaters Management with 23-Gauge Transconjunctival Sutureless Vitrectomy Malhar 1Consultant 1 Soni, Minas G 2 Georgopoulos, Adriana 2 Kovakova Vitreo-Retinal Surgeon, London,
Long-term Outcomes of Vitreous Floaters Management with 23-Gauge Transconjunctival Sutureless Vitrectomy Malhar 1Consultant 1 Soni, Minas G 2 Georgopoulos, Adriana 2 Kovakova Vitreo-Retinal Surgeon, London,
Clinical Study Passive Removal of Silicone Oil with Temporal Head Position through Two 23-Gauge Cannulas
 Ophthalmology Volume 2016, Article ID 4182693, 4 pages http://dx.doi.org/10.1155/2016/4182693 Clinical Study Passive Removal of Silicone Oil with Temporal Head Position through Two 23-Gauge Cannulas Zhong
Ophthalmology Volume 2016, Article ID 4182693, 4 pages http://dx.doi.org/10.1155/2016/4182693 Clinical Study Passive Removal of Silicone Oil with Temporal Head Position through Two 23-Gauge Cannulas Zhong
Prompt 27-gauge sutureless transconjunctival vitrectomy for bleb-associated endophthalmitis
 Int Ophthalmol (2018) 38:2663 2668 https://doi.org/10.1007/s10792-017-0747-4 (0456789().,-volV) (0456789().,-volV) CASE REPORT Prompt 27-gauge sutureless transconjunctival vitrectomy for bleb-associated
Int Ophthalmol (2018) 38:2663 2668 https://doi.org/10.1007/s10792-017-0747-4 (0456789().,-volV) (0456789().,-volV) CASE REPORT Prompt 27-gauge sutureless transconjunctival vitrectomy for bleb-associated
Closed System and Expanded Instrumentation Improves MIVS Outcomes
 CLOSED SYSTEM AND GRIESHABER EXPANDED DSP INSTRUMENTATION Instrumentation for IMPROVES SurgeryMIVS OUTCOMES Closed System and Expanded Instrumentation Improves MIVS Outcomes By Martin Charles, MD I have
CLOSED SYSTEM AND GRIESHABER EXPANDED DSP INSTRUMENTATION Instrumentation for IMPROVES SurgeryMIVS OUTCOMES Closed System and Expanded Instrumentation Improves MIVS Outcomes By Martin Charles, MD I have
Clinical Study Air Bubble Technique for Fundus Visualization during Vitrectomy in Aphakia
 Hindawi Ophthalmology Volume 2017, Article ID 4721540, 5 pages https://doi.org/10.1155/2017/4721540 Clinical Study Air Bubble Technique for Fundus Visualization during Vitrectomy in Aphakia Mahmoud Mohamed
Hindawi Ophthalmology Volume 2017, Article ID 4721540, 5 pages https://doi.org/10.1155/2017/4721540 Clinical Study Air Bubble Technique for Fundus Visualization during Vitrectomy in Aphakia Mahmoud Mohamed
Comparison between 23 Gauge and 25 Gauge Pars Plana Vitrectomy for Posterior Segment Disease
 Original Article Comparison between 23 Gauge and 25 Gauge Pars Plana Vitrectomy for Posterior Segment Disease Huma Kayani, Aamir Ahmed, Kashif Jahangir, Hizb-ur-Rehman, Khurram Chauhan Pak J Ophthalmol
Original Article Comparison between 23 Gauge and 25 Gauge Pars Plana Vitrectomy for Posterior Segment Disease Huma Kayani, Aamir Ahmed, Kashif Jahangir, Hizb-ur-Rehman, Khurram Chauhan Pak J Ophthalmol
Original Article Capsular tension ring implantation after lens extraction for management of subluxated cataracts
 Int J Clin Exp Pathol 2014;7(7):3733-3738 www.ijcep.com /ISSN:1936-2625/IJCEP0000754 Original Article Capsular tension ring implantation after lens extraction for management of subluxated cataracts Xiao
Int J Clin Exp Pathol 2014;7(7):3733-3738 www.ijcep.com /ISSN:1936-2625/IJCEP0000754 Original Article Capsular tension ring implantation after lens extraction for management of subluxated cataracts Xiao
Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure Glaucoma
 Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg
 An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases
 Original Article Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases Syed Raza Ali Shah, Nadeem Ahmad, Qasim Lateef Chaudry, Chaudary Nasir Ahmad, Asad
Original Article Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases Syed Raza Ali Shah, Nadeem Ahmad, Qasim Lateef Chaudry, Chaudary Nasir Ahmad, Asad
Evaluation of Wound Morphology of Sclerotomy Sites of Sutureless Vitrectomy Using Spectralis Anterior Segment Optical Coherence Tomography
 ORIGINAL CLINICAL STUDY Evaluation of Wound Morphology of Sclerotomy Sites of Sutureless Vitrectomy Using Spectralis Anterior Segment Optical Coherence Tomography Manish Nagpal, MS, DO, FRCS, Gaurav Paranjpe,
ORIGINAL CLINICAL STUDY Evaluation of Wound Morphology of Sclerotomy Sites of Sutureless Vitrectomy Using Spectralis Anterior Segment Optical Coherence Tomography Manish Nagpal, MS, DO, FRCS, Gaurav Paranjpe,
Anina Abraham, Consultant, Swarup Eye Centre, Hyderabad, India. The author has no financial interests
 Reduced Incidence of Sclerotomy Related Breaks during 23-Gauge Vitrectomy Anina Abraham, Consultant, Swarup Eye Centre, Hyderabad, India The author has no financial interests Introduction Sclerotomy related
Reduced Incidence of Sclerotomy Related Breaks during 23-Gauge Vitrectomy Anina Abraham, Consultant, Swarup Eye Centre, Hyderabad, India The author has no financial interests Introduction Sclerotomy related
Intraocular Lens Power Estimation in Combined Phacoemulsification and Pars Plana Vitrectomy in Eyes with Epiretinal Membranes: A Case-Control Study
 Original Article http://dx.doi.org/10.3349/ymj.2015.56.3.805 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 56(3):805-811, 2015 Intraocular Lens Power Estimation in Combined Phacoemulsification and Pars
Original Article http://dx.doi.org/10.3349/ymj.2015.56.3.805 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 56(3):805-811, 2015 Intraocular Lens Power Estimation in Combined Phacoemulsification and Pars
GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE
 GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE AMAR AGARWAL INTRODUCTION 1-2 Posterior capsular rent (PCR) can occur in early learning curve in phacoemulsification.
GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE AMAR AGARWAL INTRODUCTION 1-2 Posterior capsular rent (PCR) can occur in early learning curve in phacoemulsification.
Venturi versus peristaltic pumps 33 vitrectomy dynamics 34 Fluorescein, vitreous staining 120
 Subject Index Accurus 35, 83 Aflibercept, diabetic macular edema management 167, 168 Air-forced infusion, Stellaris PC 12, 13 Alcon Constellation, see Constellation system Autoclave sterilization lens
Subject Index Accurus 35, 83 Aflibercept, diabetic macular edema management 167, 168 Air-forced infusion, Stellaris PC 12, 13 Alcon Constellation, see Constellation system Autoclave sterilization lens
Structural changes of the anterior chamber following cataract surgery during infancy
 Structural changes of the anterior chamber following cataract surgery during infancy Matthew Nguyen, Emory University Marla Shainberg, Emory University Allen Beck, Emory University Scott Lambert, Emory
Structural changes of the anterior chamber following cataract surgery during infancy Matthew Nguyen, Emory University Marla Shainberg, Emory University Allen Beck, Emory University Scott Lambert, Emory
INTRODUCTION J. DAWCZYNSKI, E. KOENIGSDOERFFER, R. AUGSTEN, J. STROBEL. Department of Ophthalmology, University Hospital Jena, Jena - Germany
 European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
Objectives. Tubes, Ties and Videotape: Financial Disclosure. Five Year TVT Results IOP Similar
 Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Subnormal Vision in Uneventful Cataract Surgery after 6 Weeks Hospital Based Study
 ISSN 2231-4261 ORIGINAL ARTICLE Subnormal Vision in Uneventful Cataract Surgery after 6 Weeks Hospital Based Study 1* 1 1 V. H. Karambelkar, Ankit Sharma, Viraj Pradhan 1 Department of Ophthalmology, Krishna
ISSN 2231-4261 ORIGINAL ARTICLE Subnormal Vision in Uneventful Cataract Surgery after 6 Weeks Hospital Based Study 1* 1 1 V. H. Karambelkar, Ankit Sharma, Viraj Pradhan 1 Department of Ophthalmology, Krishna
Scleral Buckling under a Slit-lamp Illumination System with a Contact Wide-angle Viewing Lens Compared with an Indirect Ophthalmoscope
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(2):126-133 https://doi.org/10.3341/kjo.2017.0092 Original Article Scleral Buckling under a Slit-lamp Illumination System with a Contact Wide-angle
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(2):126-133 https://doi.org/10.3341/kjo.2017.0092 Original Article Scleral Buckling under a Slit-lamp Illumination System with a Contact Wide-angle
Intraoperative biometry for intraocular lens (IOL) power calculation at silicone oil removal
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 622-626 Intraoperative biometry for intraocular lens (IOL) power calculation at silicone oil removal S.M. EL-BAHA, A. EI-SAMADONI, H.F. IDRIS,
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 622-626 Intraoperative biometry for intraocular lens (IOL) power calculation at silicone oil removal S.M. EL-BAHA, A. EI-SAMADONI, H.F. IDRIS,
Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic Syndrome
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE
 GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE AMAR AGARWAL INTRODUCTION 1-2 Posterior capsular rent (PCR) can occur in early learning curve in phacoemulsification.
GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE AMAR AGARWAL INTRODUCTION 1-2 Posterior capsular rent (PCR) can occur in early learning curve in phacoemulsification.
Minimally Invasive Surgery for the Removal of Posterior Intraocular Foreign Bodies
 Surgical Technique Minimally Invasive Surgery for the Removal of Posterior Intraocular Foreign Bodies Jesus Hernan Gonzalez Cortes 1, MD, PhD; Yunuen Bages Rousselon 1, MD; Jesus Emiliano Gonzalez Cantu
Surgical Technique Minimally Invasive Surgery for the Removal of Posterior Intraocular Foreign Bodies Jesus Hernan Gonzalez Cortes 1, MD, PhD; Yunuen Bages Rousselon 1, MD; Jesus Emiliano Gonzalez Cantu
Advanced Eyecare of Orange County/ Kim T. Doan, M.D.
 Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Original Article. Address for Correspondance Dr. Charu Mithal Upgraded Dept. of Ophthalmology, LLRM Medical College Meerut.
 Original Article EVALUATION OF THE VISUAL OUTCOME AND COMPLICATION OF SECONDARY IMPLANTATION OF OPEN-LOOP ANTERIOR CHAMBER, SULCUS FIXATED POSTERIOR CHAMBER AND SCLERAL FIXATED POSTERIOR CHAMBER INTRAOCULAR
Original Article EVALUATION OF THE VISUAL OUTCOME AND COMPLICATION OF SECONDARY IMPLANTATION OF OPEN-LOOP ANTERIOR CHAMBER, SULCUS FIXATED POSTERIOR CHAMBER AND SCLERAL FIXATED POSTERIOR CHAMBER INTRAOCULAR
Nature and Science 2016;14(9)
 Comparison between Implantable Contact Lens (ICL) versus Acry Sof Cachet Phakic Intraocular Lenses in Correction of Moderate to High Myopia Khaled Nada, M. Sc.; Mohammed Attia, M. D and Ashraf El Habbak,
Comparison between Implantable Contact Lens (ICL) versus Acry Sof Cachet Phakic Intraocular Lenses in Correction of Moderate to High Myopia Khaled Nada, M. Sc.; Mohammed Attia, M. D and Ashraf El Habbak,
Full-thickness Sclerotomy for Uveal Effusion Syndrome
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(4):294-298 http://dx.doi.org/10.3341/kjo.2013.27.4.294 Full-thickness Sclerotomy for Uveal Effusion Syndrome Case Report Mingui Kong, Jae Hui
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(4):294-298 http://dx.doi.org/10.3341/kjo.2013.27.4.294 Full-thickness Sclerotomy for Uveal Effusion Syndrome Case Report Mingui Kong, Jae Hui
Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment surgeon can make
 Posterior Segment Complications and Management of Retained Lens Material Jay M. Stewart, MD Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment
Posterior Segment Complications and Management of Retained Lens Material Jay M. Stewart, MD Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment
Posterior Chamber Intraocular Lens Implantation in Pediatric Cataract with Microcornea and/or Microphthalmos
 Posterior Chamber Intraocular Lens Implantation in Pediatric Cataract with Microcornea and/or Microphthalmos Young Suk Yu, MD 1,2, Seong-Joon Kim, MD 1,2, Ho Kyoung Choung, MD 3 Department of Ophthalmology,
Posterior Chamber Intraocular Lens Implantation in Pediatric Cataract with Microcornea and/or Microphthalmos Young Suk Yu, MD 1,2, Seong-Joon Kim, MD 1,2, Ho Kyoung Choung, MD 3 Department of Ophthalmology,
Trauma. steve charles
 Trauma steve charles Pathobiology of Trauma Hypocellular Vitreous Collagen Contraction (formerly called gel contraction) Poor Names: Vitreous Bands & Vitreous Membranes (always along vitreous surface or
Trauma steve charles Pathobiology of Trauma Hypocellular Vitreous Collagen Contraction (formerly called gel contraction) Poor Names: Vitreous Bands & Vitreous Membranes (always along vitreous surface or
Surgical outcome of pars plana vitrectomy: a retrospective study in a peripheral tertiary eye care centre of Nepal
 Original article : a retrospective study in a peripheral tertiary eye care centre of Nepal Subedi S 1, Sharma MK 2, Sharma BR 2, Kansakar I 2, Dhakwa K 2, Adhikari RK 2 1.Nepal Eye Hospital, National Academy
Original article : a retrospective study in a peripheral tertiary eye care centre of Nepal Subedi S 1, Sharma MK 2, Sharma BR 2, Kansakar I 2, Dhakwa K 2, Adhikari RK 2 1.Nepal Eye Hospital, National Academy
Issue 15 The following key clinical peer reviewed journals will be reviewed: MONTHLY RESEARCH UPDATE 151(3) American Journal of Ophthalmology 129(5)
 Welcome to Bausch and Lomb s monthly research update. With our background in clinical ophthalmic research, mainly of the anterior eye, Bausch and Lomb have asked us to produce an independent report of
Welcome to Bausch and Lomb s monthly research update. With our background in clinical ophthalmic research, mainly of the anterior eye, Bausch and Lomb have asked us to produce an independent report of
WGA. The Global Glaucoma Network
 The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
Refractive Dilemma. Challenging Case
 Challenging Case Refractive Dilemma Section Editor: Alireza Baradaran-Rafii, MD Case presentation A 21-year old man was referred to an ophthalmology clinic insisting on getting rid of his glasses which
Challenging Case Refractive Dilemma Section Editor: Alireza Baradaran-Rafii, MD Case presentation A 21-year old man was referred to an ophthalmology clinic insisting on getting rid of his glasses which
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures
 Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Clinical Evaluation of the BunnyLens IOL
 Clinical Evaluation of the BunnyLens IOL Introduction: BunnyLens is a foldable Hydrophlic Acrylic IOL with four ear shaped haptic design. The lens design offers many advantages in terms of: 1. Centration
Clinical Evaluation of the BunnyLens IOL Introduction: BunnyLens is a foldable Hydrophlic Acrylic IOL with four ear shaped haptic design. The lens design offers many advantages in terms of: 1. Centration
Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution
 Hirota et al. BMC Ophthalmology 2014, 14:39 RESEARCH ARTICLE Open Access Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution Kazunari
Hirota et al. BMC Ophthalmology 2014, 14:39 RESEARCH ARTICLE Open Access Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution Kazunari
Intrapapillary hemorrhage with concurrent peripapillary and vitreous hemorrhage in two healthy young patients
 Moon et al. BMC Ophthalmology (2018) 18:172 https://doi.org/10.1186/s12886-018-0833-z CASE REPORT Open Access Intrapapillary hemorrhage with concurrent peripapillary and vitreous hemorrhage in two healthy
Moon et al. BMC Ophthalmology (2018) 18:172 https://doi.org/10.1186/s12886-018-0833-z CASE REPORT Open Access Intrapapillary hemorrhage with concurrent peripapillary and vitreous hemorrhage in two healthy
SECONDARY CAPSULOTOMY USING THE FEMTOSECOND LASER. Surendra Basti, MD Northwestern University Feinberg School of Medicine, Chicago, IL
 SECONDARY CAPSULOTOMY USING THE FEMTOSECOND LASER Surendra Basti, MD Northwestern University Feinberg School of Medicine, Chicago, IL SMALL PUPIL MANAGEMENT DURING FEMTO CATARACT SURGERY Surendra Basti,
SECONDARY CAPSULOTOMY USING THE FEMTOSECOND LASER Surendra Basti, MD Northwestern University Feinberg School of Medicine, Chicago, IL SMALL PUPIL MANAGEMENT DURING FEMTO CATARACT SURGERY Surendra Basti,
Vitrectomy for Diabetic Cystoid Macular Edema
 Vitrectomy for Diabetic Cystoid Macular Edema Yukihiro Sato, Zeon Lee and Hiroyuki Shimada Department of Ophthalmology, Nihon University School of Medicine, Tokyo, Japan Purpose: We evaluated visual outcomes
Vitrectomy for Diabetic Cystoid Macular Edema Yukihiro Sato, Zeon Lee and Hiroyuki Shimada Department of Ophthalmology, Nihon University School of Medicine, Tokyo, Japan Purpose: We evaluated visual outcomes
Inadvertent trypan blue staining of posterior capsule during cataract surgery associated with "Argentinian flag" event
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Inadvertent trypan blue staining of posterior capsule during cataract surgery associated with "Argentinian
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Inadvertent trypan blue staining of posterior capsule during cataract surgery associated with "Argentinian
Anatomical results and complications after silicone oil removal
 Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification
 Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification Mohammad Pakravan, MD; Homayoun Nikkhah, MD; Shahin Yazdani, MD Camelia Shahabi, MD; Massih Sedigh-Rahimabadi, MD Labbafinejad
Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification Mohammad Pakravan, MD; Homayoun Nikkhah, MD; Shahin Yazdani, MD Camelia Shahabi, MD; Massih Sedigh-Rahimabadi, MD Labbafinejad
Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
Andrew J. Barkmeier, MD; Benjamin P. Nicholson, MA; Levent Akduman, MD
 c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
No-Touch Technique and a New Donor Adjuster for Descemet s Stripping Automated Endothelial Keratoplasty
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Surgical Results and Visual Outcomes of Vitreous Surgery for Advanced Stages of Retinopathy of Prematurity
 Surgical Results and Visual Outcomes of Vitreous Surgery for Advanced Stages of Retinopathy of Prematurity Toshihiro Kono, Kenji Oshima and Yuki Fuchino Department of Ophthalmology, School of Medicine,
Surgical Results and Visual Outcomes of Vitreous Surgery for Advanced Stages of Retinopathy of Prematurity Toshihiro Kono, Kenji Oshima and Yuki Fuchino Department of Ophthalmology, School of Medicine,
Informed Consent For Cataract Surgery. And/Or Implantation of an Intraocular Lens INTRODUCTION
 Informed Consent For Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is given to you so that you can make an informed decision about having eye surgery. Take as
Informed Consent For Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is given to you so that you can make an informed decision about having eye surgery. Take as
Incidence and Risk Factors of Cystoid Macular Edema after Vitrectomy with Silicone Oil Tamponade for Retinal Detachment
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(3):204-210 https://doi.org/10.3341/kjo.2017.0050 Original Article Incidence and Risk Factors of Cystoid Macular Edema after Vitrectomy with
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(3):204-210 https://doi.org/10.3341/kjo.2017.0050 Original Article Incidence and Risk Factors of Cystoid Macular Edema after Vitrectomy with
ICO-Ophthalmology Surgical Competence Assessment Rubric Vitrectomy (ICO-OSCAR:VIT)
 ICO-Ophthalmology Surgical Competence Assessment Rubric Vitrectomy (ICO-OSCAR:VIT) Date Resident Evaluator Novice (score = 2) Beginner (score = 3) Advanced Beginner (score = 4) Competent (score = 5) Not
ICO-Ophthalmology Surgical Competence Assessment Rubric Vitrectomy (ICO-OSCAR:VIT) Date Resident Evaluator Novice (score = 2) Beginner (score = 3) Advanced Beginner (score = 4) Competent (score = 5) Not
Modified Technique of Four Point Scleral Sutured Posterior Chamber Intraocular Lens Without Scleral Flaps
 Original Article Modified Technique of Four Point Scleral Sutured Posterior Chamber Intraocular Lens Without Scleral Flaps Haroon Tayyab, Muhammad Ali Haider, Tehmina Jahangir Sana Jahangir, Samina Jahangir,
Original Article Modified Technique of Four Point Scleral Sutured Posterior Chamber Intraocular Lens Without Scleral Flaps Haroon Tayyab, Muhammad Ali Haider, Tehmina Jahangir Sana Jahangir, Samina Jahangir,
Cronicon EC OPHTHALMOLOGY. Research Article Trephine Assisted Trabeculectomy Technique. Idrees* Introduction
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Idrees* Al Dara Hospital and Medical Center at Riyadh, Saudi Arabia *Corresponding Author: Dr Idrees, Al Dara Hospital and Medical Center at Riyadh,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Idrees* Al Dara Hospital and Medical Center at Riyadh, Saudi Arabia *Corresponding Author: Dr Idrees, Al Dara Hospital and Medical Center at Riyadh,
DIABETIC VITRECTOMY INDICATIONS AND TECHNIQUES. steve charles
 DIABETIC VITRECTOMY INDICATIONS AND TECHNIQUES steve charles Traction Retinal Detachment Macula involved TRD TRD with rhegmatogenous component even if extra-macular TTRD Extra-Macular TRD should be observed
DIABETIC VITRECTOMY INDICATIONS AND TECHNIQUES steve charles Traction Retinal Detachment Macula involved TRD TRD with rhegmatogenous component even if extra-macular TTRD Extra-Macular TRD should be observed
Original article. Amon M Pediatric micro-incision cataract surgery Nepal J Ophthalmol 2011;3(5):3-8
 Original article Surgical management challenges and clinical results of bimanual micro-incision phacoemulsification cataract surgery in children with congenital cataract Department of Ophthalmology and
Original article Surgical management challenges and clinical results of bimanual micro-incision phacoemulsification cataract surgery in children with congenital cataract Department of Ophthalmology and
IOL Subluxation Top 5 Pearls for Management. Disclosure. David G. Hwang, MD, FACS. Shire Consultant. Not relevant to this talk.
 IOL Subluxation Top 5 Pearls for Management David G. Hwang, MD, FACS Professor and Vice Chair Kimura Endowed Chair in Ophthalmology Director, Cornea Service and Refractive Surgery Services University of
IOL Subluxation Top 5 Pearls for Management David G. Hwang, MD, FACS Professor and Vice Chair Kimura Endowed Chair in Ophthalmology Director, Cornea Service and Refractive Surgery Services University of
A patient with dropped nucleus and intraocular lens
 OPHTHALMIC FORUM A patient with dropped nucleus and intraocular lens by: Ricky W. K. Law, FRCS, FCOphthHK, Ronald Yeoh, M Med (Singapore), FRCS, Tarun Sharma, MD FRCS (Ed) Case history A 75-year-old female
OPHTHALMIC FORUM A patient with dropped nucleus and intraocular lens by: Ricky W. K. Law, FRCS, FCOphthHK, Ronald Yeoh, M Med (Singapore), FRCS, Tarun Sharma, MD FRCS (Ed) Case history A 75-year-old female
Intravitreal versus Posterior Subtenon Injection of Triamcinolone Acetonide for Diabetic Macular Edema
 Intravitreal versus Posterior Subtenon Injection of Triamcinolone Acetonide for Diabetic Macular Edema Young Jae Choi, MD, In Kyung Oh, MD, Jae Ryung Oh, MD, PhD, Kuhl Huh, MD, PhD Department of Ophthalmology,
Intravitreal versus Posterior Subtenon Injection of Triamcinolone Acetonide for Diabetic Macular Edema Young Jae Choi, MD, In Kyung Oh, MD, Jae Ryung Oh, MD, PhD, Kuhl Huh, MD, PhD Department of Ophthalmology,
Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD
 Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
Changes in corneal topography following 25-gauge transconjunctival. sutureless vitrectomy versus 20-gauge standard vitrectomy
 Changes in corneal topography following 25-gauge transconjunctival sutureless vitrectomy versus 20-gauge standard vitrectomy F. Okamoto 1, C. Okamoto 1, N. Sakata 1, K. Hiratsuka 1, N. Yamane 1, T. Hiraoka
Changes in corneal topography following 25-gauge transconjunctival sutureless vitrectomy versus 20-gauge standard vitrectomy F. Okamoto 1, C. Okamoto 1, N. Sakata 1, K. Hiratsuka 1, N. Yamane 1, T. Hiraoka
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Insertion of an epiretinal prosthesis for retinitis pigmentosa
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Insertion of an epiretinal prosthesis for retinitis pigmentosa Retinitis pigmentosa is a disease that affects
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Insertion of an epiretinal prosthesis for retinitis pigmentosa Retinitis pigmentosa is a disease that affects
Challenging complications of valve implantation. Salah M Al-Mosallamy MD Assistant professor of ophthalmology 2014
 Challenging complications of valve implantation by Salah M Al-Mosallamy MD Assistant professor of ophthalmology 2014 PREDISPOSING FACTORS It is important to consider the case mix for these devices on dealing
Challenging complications of valve implantation by Salah M Al-Mosallamy MD Assistant professor of ophthalmology 2014 PREDISPOSING FACTORS It is important to consider the case mix for these devices on dealing
Surgery for COEXISTING CATARACT AND GLAUCOMA:
 Surgery for COEXISTING CATARACT AND GLAUCOMA: UNEASY RELATIONSHIP Session: 20-107 Monday, April 20, 2015 Time: 8:00 AM-9:30 AM Room 7B (San Diego Convention Center) Course Instructors Ahmad K Khalil Alan
Surgery for COEXISTING CATARACT AND GLAUCOMA: UNEASY RELATIONSHIP Session: 20-107 Monday, April 20, 2015 Time: 8:00 AM-9:30 AM Room 7B (San Diego Convention Center) Course Instructors Ahmad K Khalil Alan
Silicone oil pupillary block after laser retinopexy in aphakic eyes with presumed closed peripheral iridectomy: report of three cases
 Int Ophthalmol (2014) 34:913 917 DOI 10.1007/s10792-013-9862-z CASE REPORT Silicone oil pupillary block after laser retinopexy in aphakic eyes with presumed closed peripheral iridectomy: report of three
Int Ophthalmol (2014) 34:913 917 DOI 10.1007/s10792-013-9862-z CASE REPORT Silicone oil pupillary block after laser retinopexy in aphakic eyes with presumed closed peripheral iridectomy: report of three
Original article. Preliminar treatment of astigmatism during phacoemulsification. Sharma BR 1, Kumar A 2 1
 Original article Preliminar eliminary experiences with limbal relaxing incision for treatment of astigmatism during phacoemulsification Sharma BR 1, Kumar A 2 1 Associate Professor, 2 Ophthalmologist,
Original article Preliminar eliminary experiences with limbal relaxing incision for treatment of astigmatism during phacoemulsification Sharma BR 1, Kumar A 2 1 Associate Professor, 2 Ophthalmologist,
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC
 CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
INTRODUCTION. Trans Am Ophthalmol Soc 2007:105:
 HANGING BY A THREAD: THE LONG-TERM EFFICACY AND SAFETY OF TRANSSCLERAL SUTURED INTRAOCULAR LENSES IN CHILDREN (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY Edward G. Buckley MD ABSTRACT Purpose: To
HANGING BY A THREAD: THE LONG-TERM EFFICACY AND SAFETY OF TRANSSCLERAL SUTURED INTRAOCULAR LENSES IN CHILDREN (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY Edward G. Buckley MD ABSTRACT Purpose: To
