PERSISTENT PAIN PATHWAY - DATA RETRIEVAL WORKSHEET
|
|
|
- Edward Carter
- 5 years ago
- Views:
Transcription
1 1 PERSISTENT PAIN PATHWAY - DATA RETRIEVAL WORKSHEET Unit: Shift: Date: Time of Data Retrieval: Person Completing Worksheet: III. General Assessment Guidelines for Persistent Pain in the Elderly. Pain assessment entails a multi-layered communication process that often requires the assessor to alter communication to the needs of the person being assessed. It is an incomplete process when there is reliance on single components such as resident record or limited interviews. Regular thorough assessments decrease the reliance on assumptions for the treatment of persistent pain. home/ pain management policies and procedures. Complete this worksheet using resident/family interview, staff interview, direct resident observation, observations of environment and direct care delivery, and record review. Type of Data Retrieval Examination Monitoring Criteria Y/N NA Incomplete Comments 1. Staff member speaks at eye level, face to face with open body language. 2. Staff member introduces self and uses resident s preferred name to establish connection. 3. Consider resident s vision, hearing and comfort. Adjust communication and setting to fit needs. 4. Locations, type, quality, intensity, duration and frequency of pains are assessed. 5. Medications taken to relieve pain is reviewed including frequency and dosage: a. Over the counter b. Prescription c. Adjuvants d. Herbal remedies 6. Non medical strategies or home remedies to relieve pain: a. Examples: sleeping in a recliner, placing a bar of soap in the bed, hot/warm packs, copper jewelry etc.
2 2 7. Pain questions: a. What makes the pain better? Worse? b. What does the pain keep the resident from doing? c. What are the resident s understanding, barriers (cultural, social), expectations and desires of pain relief? d. What is the resident s behavioral response to pain? Examples: sleep, mood change, wandering, perseveration, decreased movement, etc. 8. Pain rating scale is used. a. Use evidence based scale appropriate to resident s cognition and comfort level. b. Examples: 1-10, vertical or thermometer, nominal/ descriptor, PAINAD, etc. c. Any visual scale should be a separate piece of paper with good contrast. d. Same scale is used to record follow up evaluation after treatment is administered. 9. What is the resident s pain number on his/her very worst day - very best day? Daily? 10. Evaluate resident for effects of persistent pain on; a. Sleep b. Appetite c. Energy d. Relationships e. Mood f. Care 11. Many elderly residents may only associate the word pain with excruciating or acute events. a. Ask appropriate questions. Examples: Do your joints ache? Do you feel stiff and sore in the morning? What does that achiness
3 3 keep you from doing? b. Use descriptive words. Examples: Soreness Heaviness Burning Discomfort Tingling, etc. 12. ADLs are observed for changes in comfort or ability. a. Ask resident to put on/take off socks or shirt. b. Ask resident to transfer on/off toilet or in/out of chair. c. Observe ambulation for clues. Example: Holding onto furniture while trying to walk. 13. New or worsening disease processes are evaluated as complicating/contributing factors. 14. Evaluation of efficacy of all treatment for persistent pain including side effects and resident response is part of ongoing assessment.
4 4 PERSISTENT PAIN PATHWAY - DATA RETRIEVAL WORKSHEET Date: Unit: Time of Data Retrieval: Person Completing Worksheet: IV. Assessment of Persistent Pain in the Cognitively Impaired Elderly Person. Persistent pain in the cognitively impaired elderly is often missed or under treated because of changes in communication related to the dementing illness. Behavioral pain symptoms are often attributed to the dementing illness rather than seen as symptoms of discomfort or pain in a person with declining verbal and cognitive abilities. With a few changes in approach thorough assessment is possible for most cognitively impaired elders. Type of Data Retrieval Monitoring Criteria Y/N NA Incomplete Comments 1. Staff member speaks at eye level, face to face with open body language. 2. Staff member introduces self and use the resident s preferred name to establish connection. 3. Consider resident s vision, hearing and comfort. Adjust communication and setting to fit needs. 4. Staff asks appropriate questions for the resident s level of cognition. Example: a. I see you have arthritis - Do your hands hurt? Are your knees sore? b. May need to go joint by joint, area by area 5. Staff may use physical cueing while asking questions. a. Gently touch resident s knees, hands, etc. as you ask about them. b. Touch your own knees, hands, etc as you ask about them. 6. Staff speaks clearly and gives resident plenty of time to answer.
5 5 7. ADLs are observed for changes in comfort or ability. d. Ask resident to put on/take off socks or shirt. e. Ask resident to transfer on/off toilet or in/out of chair. Observe ambulation for clues. Example: Holding onto furniture while trying to walk. 8. Staff asks resident/family about past pain but may have to assess for pain in the moment. a. Resident may not be able to tell you about frequency, character, etc. of past pain. b. Staff may have to monitor resident s pain over several days to get a clear picture. 9. Medications taken to relieve pain are reviewed including frequency and dosage: e. Over the counter f. Prescription g. Adjuvants h. Herbal remedies 10. Non medical strategies or home remedies to relieve pain: b. Examples: sleeping in a recliner, placing a bar of soap in the bed, hot/warm packs, copper jewelry etc. 11. New or worsening disease processes are evaluated as complicating/contributing factors. 12. Staff assesses for behaviors that may indicate pain. a. Examples: guarding, grunting, grimacing, wandering, anxiety, pacing, postural changes, fidgeting, sadness, tense body language, tearfulness, reluctance, withdrawal, resistance, gait changes, aggression, increased or new vocalizations.
6 6 13. Staff asks caregiver/family: a. Changes in resident routine or behavior. b. For help with interpretation of words or behaviors. c. Any increased or new vocalizations, resistance to care. 14. Pain rating scale is used. a. Use evidence based scale appropriate to resident s cognition and comfort level. b. Examples: 1-10, vertical or thermometer, nominal/ descriptor. c. For non-verbal residents with dementia evidence/based scale is used such as PAINAD and/or PACSLAC. d. Same scale is used to record follow up evaluation after treatment is administered. 15. Evaluate resident for effects of persistent pain on: a. Sleep b. Appetite c. Energy d. Relationships e. Mood f. Care 16. Evaluation of efficacy of all treatment for persistent pain including side effects and resident response is part of ongoing assessment. Persistent Pain Pathway - Data Retrieval Worksheet III and IV American Geriatric Society Panel on Pharmacologic Management of Persistent Pain. (2009) Journal of the American Geriatric Society, 57(8), American Medical Directors Association. (2009) Pain Management Clinical Practice Guideline. Columbia,MD: AMDA. Jablonski, A, Ersek, M (2009). Nursing home adherence to evidence-based pain management practices. Journal of Gerontological Nursing, 35(7),
7 7 Minner, D, Marek, K (2005). Evidence based assessment and treatment of persistent pain in the community dwelling elderly receiving home health services: a pathway. Home Health Care Management and Practice, 17(4), Rantz, M, Vinz Miller, T, Popejoy, L, & Zwygart-Stauffacher,M. (2003) Outcome-Based Quality Improvement for Long-Term Care: Using MDS Process and Outcome Measures. [2 nd Ed]Thomson Delmar Learning Center: Clifton Park, NY. Center for Medicare and Medicaid Services. November, Resident Assessment Instrument Manual 3.0.
LUNCH WITH THE EXPERTS: Palliative Care for Advanced Dementia with Pain and Dementia
 LUNCH WITH THE EXPERTS: Palliative Care for Advanced Dementia with Pain and Dementia Carol Long, PhD, RN, FPCN Principal, Capstone Healthcare & Co-Director, Palliative Care for Advanced Dementia, Beatitudes
LUNCH WITH THE EXPERTS: Palliative Care for Advanced Dementia with Pain and Dementia Carol Long, PhD, RN, FPCN Principal, Capstone Healthcare & Co-Director, Palliative Care for Advanced Dementia, Beatitudes
Geriatric Pain Assessment and Management. Robin Arends, DNP, CNP, FNP-BC
 + Geriatric Pain Assessment and Management Robin Arends, DNP, CNP, FNP-BC + Objectives List three reasons why elderly are less likely to report pain. List three barriers to pain management Describe two
+ Geriatric Pain Assessment and Management Robin Arends, DNP, CNP, FNP-BC + Objectives List three reasons why elderly are less likely to report pain. List three barriers to pain management Describe two
May 2015 Clinical Nurse Educator Arohanui Hospice
 May 2015 Clinical Nurse Educator Arohanui Hospice End of Life Care, what s on top? Feedback from last session (Physiology of Dying) Volunteer to present at August meeting Presentation: Breaking Bad News
May 2015 Clinical Nurse Educator Arohanui Hospice End of Life Care, what s on top? Feedback from last session (Physiology of Dying) Volunteer to present at August meeting Presentation: Breaking Bad News
ELNEC. Module 2 Pain Assessment & Management. Geriatric Curriculum ELNEC- END-OF-LIFE NURSING EDUCATION CONSORTIUM. Geriatric Curriculum
 ELNEC END-OF-LIFE NURSING EDUCATION CONSORTIUM Module 2 Pain Assessment & Management Part I: Module 2 General pain assessment Assessment of pain in nonverbal residents Part II: Pharmacological management
ELNEC END-OF-LIFE NURSING EDUCATION CONSORTIUM Module 2 Pain Assessment & Management Part I: Module 2 General pain assessment Assessment of pain in nonverbal residents Part II: Pharmacological management
pain and dementia Some people with pain give no signs of it.
 Pain& Dementia pain and dementia Pain affects each of us differently. Some people have pain and we would never know. Some people with pain give no signs of it. Others, however, wear facial expressions
Pain& Dementia pain and dementia Pain affects each of us differently. Some people have pain and we would never know. Some people with pain give no signs of it. Others, however, wear facial expressions
PAIN AND DEMENTIA: Recognition, Assessment and Management of Pain in Patients with Late-Life Dementia
 PAIN AND DEMENTIA: Recognition, Assessment and Management of Pain in Patients with Late-Life Dementia TOLU TAIWO PRESENTED AT PHC IGSI WORKSHOP #3 LACOMBE MEMORIAL CENTRE, LACOMBE MAY 25, 2018. Presenter
PAIN AND DEMENTIA: Recognition, Assessment and Management of Pain in Patients with Late-Life Dementia TOLU TAIWO PRESENTED AT PHC IGSI WORKSHOP #3 LACOMBE MEMORIAL CENTRE, LACOMBE MAY 25, 2018. Presenter
HOW WOULD I KNOW? WHAT CAN I DO?
 HOW WOULD I KNOW? WHAT CAN I DO? How to help someone with dementia who is in pain or distress Help! 1 Unusual behaviour may be a sign of pain or distress If you are giving care or support to somebody with
HOW WOULD I KNOW? WHAT CAN I DO? How to help someone with dementia who is in pain or distress Help! 1 Unusual behaviour may be a sign of pain or distress If you are giving care or support to somebody with
Every 67seconds, someone will develop Alzheimer's.
 We all need a purpose and responsibilities to live a healthy life. Dementia Care 101 Corrin Campbell BS, COTA/L & Michael Urban, MS, OTR/L, MBA Every 67seconds, someone will develop Alzheimer's. http://www.alz.org
We all need a purpose and responsibilities to live a healthy life. Dementia Care 101 Corrin Campbell BS, COTA/L & Michael Urban, MS, OTR/L, MBA Every 67seconds, someone will develop Alzheimer's. http://www.alz.org
PAIN MANAGEMENT Help me HELP ME!!
 PAIN MANAGEMENT Help me HELP ME!! RECOGNIZING AND IDENTIFYING PAIN Trust what the resident says Recognize other words to describe pain Implement the appropriate interventions to relieve their pain WHAT
PAIN MANAGEMENT Help me HELP ME!! RECOGNIZING AND IDENTIFYING PAIN Trust what the resident says Recognize other words to describe pain Implement the appropriate interventions to relieve their pain WHAT
UCSF PAIN SUMMIT /8/15
 UCSF PAIN SUMMIT 2015 5/8/15 Case 3 Geriatric Pain Disclosure Statements UCSF PAIN SUMMIT 2015 Wendy Anderson Patrice Villars 5/8/15 Case 3 Geriatric Pain Pain Management in the Geriatric & End-of-Life
UCSF PAIN SUMMIT 2015 5/8/15 Case 3 Geriatric Pain Disclosure Statements UCSF PAIN SUMMIT 2015 Wendy Anderson Patrice Villars 5/8/15 Case 3 Geriatric Pain Pain Management in the Geriatric & End-of-Life
Communication with Cognitively Impaired Clients For CNAs
 Communication with Cognitively Impaired Clients For CNAs This course has been awarded one (1.0) contact hour. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction
Communication with Cognitively Impaired Clients For CNAs This course has been awarded one (1.0) contact hour. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction
Medical History. Instructions. My telephone number is: 1 Tools Medical History
 Medical History Instructions To do the best possible job with your pain, your doctor needs details about your history, including current and past medical problems, medications, health habits, and family
Medical History Instructions To do the best possible job with your pain, your doctor needs details about your history, including current and past medical problems, medications, health habits, and family
THE COMPLEXITY OF PAIN ASSESSMENT IN OLDER PEOPLE
 Art & science The person-centred acute synthesis care of art and care science is lived by the nurse in the nursing act JOSEPHINE G PATERSON THE COMPLEXITY OF PAIN ASSESSMENT IN OLDER PEOPLE Julie Gregory
Art & science The person-centred acute synthesis care of art and care science is lived by the nurse in the nursing act JOSEPHINE G PATERSON THE COMPLEXITY OF PAIN ASSESSMENT IN OLDER PEOPLE Julie Gregory
Promoting Comfort: Management of Pain for all Patient Populations
 Promoting Comfort: Management of Pain for all Patient Populations Objectives Review Wheaton Franciscan Healthcare Interdisciplinary Standard of Care: Sensory Understand assessment process and parameters
Promoting Comfort: Management of Pain for all Patient Populations Objectives Review Wheaton Franciscan Healthcare Interdisciplinary Standard of Care: Sensory Understand assessment process and parameters
Behavioural and Psychological Symptoms and Medications Presentation
 1 2 Vover s research indicated that antipsychotic med are frequently used for individual presenting with disruptive behaviours. This often combined with physical restraints Efficacy of use not justify
1 2 Vover s research indicated that antipsychotic med are frequently used for individual presenting with disruptive behaviours. This often combined with physical restraints Efficacy of use not justify
HealthPartners Inspire Special Needs Basic Care Clinical Care Planning and Resource Guide CHRONIC PAIN
 The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Neurological Disorders and Stroke), Mount Sinai Beth Israel
The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Neurological Disorders and Stroke), Mount Sinai Beth Israel
Effective Date: August 31, 2006
 SUBJECT: PAIN MANAGEMENT 1. PURPOSE: COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Nursing Care POLICY NUMBER: 317 Effective Date: August 31, 2006 This nursing policy will provide
SUBJECT: PAIN MANAGEMENT 1. PURPOSE: COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Nursing Care POLICY NUMBER: 317 Effective Date: August 31, 2006 This nursing policy will provide
Recognizing Pain in People with Dementia
 Recognizing Pain in People with Dementia CAT H Y CIOLEK, D PT, FA PTA B O A R D C E R T I F I E D G E R I AT R I C C L I N I C A L S P E C I A L I S T C E R T I F I E D D E M E N T I A P R A C T I T I
Recognizing Pain in People with Dementia CAT H Y CIOLEK, D PT, FA PTA B O A R D C E R T I F I E D G E R I AT R I C C L I N I C A L S P E C I A L I S T C E R T I F I E D D E M E N T I A P R A C T I T I
Managing Chronic Pain
 Managing Chronic Pain What Is Chronic Pain? Everyone feels pain sometimes the sharp stab of a twisted ankle, the throb of a headache, the muscle soreness that comes from too much activity. This type of
Managing Chronic Pain What Is Chronic Pain? Everyone feels pain sometimes the sharp stab of a twisted ankle, the throb of a headache, the muscle soreness that comes from too much activity. This type of
Dementia and Fall Geriatric Interprofessional Training. Wael Hamade, MD, FAAFP
 Dementia and Fall Geriatric Interprofessional Training Wael Hamade, MD, FAAFP Prevalence of Dementia Age range 65-74 5% % affected 75-84 15-25% 85 and older 36-50% 5.4 Million American have AD Dementia
Dementia and Fall Geriatric Interprofessional Training Wael Hamade, MD, FAAFP Prevalence of Dementia Age range 65-74 5% % affected 75-84 15-25% 85 and older 36-50% 5.4 Million American have AD Dementia
risk factors for falling
 Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
Understanding Dementia &
 Understanding Dementia & Care Options for Those Suffering with the Disease Paige Landry BSN Hospice Care Consultant SouthernCare New Beacon Hospice Objectives Understand Dementia Understand Common Problems
Understanding Dementia & Care Options for Those Suffering with the Disease Paige Landry BSN Hospice Care Consultant SouthernCare New Beacon Hospice Objectives Understand Dementia Understand Common Problems
Pain Assessment and Follow-Up for Patients with Dementia
 Pain Assessment and Follow-Up for Patients with Dementia Measure Description Percentage of patients with dementia who underwent documented screening * for pain symptoms at every visit and if screening
Pain Assessment and Follow-Up for Patients with Dementia Measure Description Percentage of patients with dementia who underwent documented screening * for pain symptoms at every visit and if screening
A Letter From Home February 2016
 More than two thirds of all Americans suffer from multiple, chronic conditions. An estimated 60-70% of people over 65 report at least some persistent pain (Centers for Disease Control and Prevention, 2013).
More than two thirds of all Americans suffer from multiple, chronic conditions. An estimated 60-70% of people over 65 report at least some persistent pain (Centers for Disease Control and Prevention, 2013).
Tools for Assessment of Pain in Nonverbal Older Adults with Dementia: A State-of-the-Science Review
 170 Journal of Pain and Symptom Management Vol. 31 No. 2 February 2006 Review Article Tools for Assessment of Pain in Nonverbal Older Adults with Dementia: A State-of-the-Science Review Keela Herr, PhD,
170 Journal of Pain and Symptom Management Vol. 31 No. 2 February 2006 Review Article Tools for Assessment of Pain in Nonverbal Older Adults with Dementia: A State-of-the-Science Review Keela Herr, PhD,
UNTHSC TCOM Geriatric Competencies Curriculum Mapping Document
 INSTRUCTIONS: Place a "B" (Basic), "I" (Intermediate), or "A" (Advanced) in the box next to the Geriatric Competency to indicate the Geraitaric Competency being taught, the corresponding Method of Subject
INSTRUCTIONS: Place a "B" (Basic), "I" (Intermediate), or "A" (Advanced) in the box next to the Geriatric Competency to indicate the Geraitaric Competency being taught, the corresponding Method of Subject
Table to Demonstrate a method of working through Triggered CAPs.
 CAP Problem Goals Triggers Guidelines Physical Activities increase hours of exercises Reports less than 2 hours Personal choice Promotion and physical activity activity in last 3 days Instrumental Activities
CAP Problem Goals Triggers Guidelines Physical Activities increase hours of exercises Reports less than 2 hours Personal choice Promotion and physical activity activity in last 3 days Instrumental Activities
Pain and the MGH Promise
 Pain is an unpleasant sensory & emotional experience associated with actual or potential tissue damage or described in terms of such damage Our promise to patients we will always: Work as a team to evaluate,
Pain is an unpleasant sensory & emotional experience associated with actual or potential tissue damage or described in terms of such damage Our promise to patients we will always: Work as a team to evaluate,
Part IV: Nursing assistant roles in observing and relieving pain. Nursing Assistant Roles in Endof-life. Nursing Assistant Roles in Pain Management
 Part IV: Nursing assistant roles in observing and relieving pain Objectives: Describe the roles of the NA in EOL care and pain management Define pain Describe acute and chronic pain Describe some common
Part IV: Nursing assistant roles in observing and relieving pain Objectives: Describe the roles of the NA in EOL care and pain management Define pain Describe acute and chronic pain Describe some common
Edmonton Symptom Assessment System (ESAS r) Objectives
 Edmonton Symptom Assessment System (ESAS r) Lyn Ceronsky DNP, GNP, FPCN lceronsky@gmail.com December 11, 2018 Objectives Explore the use of Edmonton Symptom Assessment System (ESAS r) tool in clinical
Edmonton Symptom Assessment System (ESAS r) Lyn Ceronsky DNP, GNP, FPCN lceronsky@gmail.com December 11, 2018 Objectives Explore the use of Edmonton Symptom Assessment System (ESAS r) tool in clinical
Considering Your Non-opioid Options for Pain
 YOUR VALUES YOUR PREFERENCES YOUR CHOICE Considering Your Non-opioid Options for Pain Self-Care, Chiropractic, Physical Therapy, Acupuncture and Pain Rehabilitation 2 Managing Your Pain: Options Pain If
YOUR VALUES YOUR PREFERENCES YOUR CHOICE Considering Your Non-opioid Options for Pain Self-Care, Chiropractic, Physical Therapy, Acupuncture and Pain Rehabilitation 2 Managing Your Pain: Options Pain If
Session outline. Introduction to dementia Assessment of dementia Management of dementia Follow-up Review
 Dementia 1 Session outline Introduction to dementia Assessment of dementia Management of dementia Follow-up Review 2 Activity 1: Person s story Present a person s story of what it feels like to live with
Dementia 1 Session outline Introduction to dementia Assessment of dementia Management of dementia Follow-up Review 2 Activity 1: Person s story Present a person s story of what it feels like to live with
Common Chronic diseases An Evidence Base for Yoga Intervention in Advanced Years & at End of Life
 Common Chronic diseases An Evidence Base for Yoga Intervention in Advanced Years & at End of Life Coronary artery disease Arthritis Hypertension Diabetes mellitus Obesity 1 2 Taking it easy Contributes
Common Chronic diseases An Evidence Base for Yoga Intervention in Advanced Years & at End of Life Coronary artery disease Arthritis Hypertension Diabetes mellitus Obesity 1 2 Taking it easy Contributes
DEEP BRAIN STIMULATION SURGICAL CANDIDACY EVALUATION FORM
 Name: MR#: Date: DEEP BRAIN STIMULATION SURGICAL CANDIDACY EVALUATION FORM Referring Physician s Name: Primary Care Provider s Name: 1. What was/were your first movement disorder symptoms? What did you
Name: MR#: Date: DEEP BRAIN STIMULATION SURGICAL CANDIDACY EVALUATION FORM Referring Physician s Name: Primary Care Provider s Name: 1. What was/were your first movement disorder symptoms? What did you
Roy Zagieboylo, MD Assistant Professor University of Connecticut Family Medicine Department
 Roy Zagieboylo, MD Assistant Professor University of Connecticut Family Medicine Department That weight gaining diet I put you on is really working! This won t hurt me a bit. You re in good shape for the
Roy Zagieboylo, MD Assistant Professor University of Connecticut Family Medicine Department That weight gaining diet I put you on is really working! This won t hurt me a bit. You re in good shape for the
Validation Techniques in a Real World By Alisa Tagg, BA ACC/EDU AC-BC CADDCT CDP CDCS NAAP President
 What is Validation? This therapy was developed to attempt understanding what emotions patients with Alzheimer s disease are expressing and respond in a way that allows patients to express their emotions
What is Validation? This therapy was developed to attempt understanding what emotions patients with Alzheimer s disease are expressing and respond in a way that allows patients to express their emotions
Lesson 2: Observation
 Lesson 2: Observation Title Slide Welcome Transcript Hello. My name is Jill Morrow, I am the Medical Director for the Office of Developmental Programs. I will be your narrator for this webcast. Lesson
Lesson 2: Observation Title Slide Welcome Transcript Hello. My name is Jill Morrow, I am the Medical Director for the Office of Developmental Programs. I will be your narrator for this webcast. Lesson
VAO PAIN RELIEF HANDOUT
 HANDOUT AMBULANCE TASMANIA 1 Clinical Field Protocols To complete this module, you will need to become familiar with the following clinical protocols: Clinical Approach to a Patient VAO CFP03 Pain Relief
HANDOUT AMBULANCE TASMANIA 1 Clinical Field Protocols To complete this module, you will need to become familiar with the following clinical protocols: Clinical Approach to a Patient VAO CFP03 Pain Relief
WELCOME to the Florence Chiropractic and Wellness Center.
 WELCOME to the Florence Chiropractic and Wellness Center. Thank you for choosing our practice for your chiropractic and wellness needs. Please complete this form in ink. If you have any questions or concerns,
WELCOME to the Florence Chiropractic and Wellness Center. Thank you for choosing our practice for your chiropractic and wellness needs. Please complete this form in ink. If you have any questions or concerns,
LOW BACK PAIN. what you can do
 LOW BACK PAIN what you can do Back pain Nearly 80 percent of adults will experience back pain at some point in their life. The good news is that back pain will normally go away within four to six weeks
LOW BACK PAIN what you can do Back pain Nearly 80 percent of adults will experience back pain at some point in their life. The good news is that back pain will normally go away within four to six weeks
Resident Assessment Best Practices M E G A N M. G R A E S E R, D N P, G N P - BC P H Y S I C I A N H O U S E C A L L S, L L C
 Resident Assessment Best Practices M E G A N M. G R A E S E R, D N P, G N P - BC P H Y S I C I A N H O U S E C A L L S, L L C Who are you assessing? Elders that needing to make a transition in their care
Resident Assessment Best Practices M E G A N M. G R A E S E R, D N P, G N P - BC P H Y S I C I A N H O U S E C A L L S, L L C Who are you assessing? Elders that needing to make a transition in their care
To help you prepare for your doctor's visit, the Alzheimer Society has developed the following list:
 The Alzheimer Society has a tool kit to help you prepare for a conversation with your doctor or health provider about your concerns and questions about a possible dementia diagnosis. Symptoms of dementia
The Alzheimer Society has a tool kit to help you prepare for a conversation with your doctor or health provider about your concerns and questions about a possible dementia diagnosis. Symptoms of dementia
DISCLAIMER: ECHO Nevada emphasizes patient privacy and asks participants to not share ANY Protected Health Information during ECHO clinics.
 DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
Part IV: Nursing Assistant Roles in Observing and Relieving Pain
 Part IV: Nursing Assistant Roles in Observing and Relieving Pain Objectives: Describe the roles of the NA in EOL care and pain management Define pain Describe acute and chronic pain Describe some common
Part IV: Nursing Assistant Roles in Observing and Relieving Pain Objectives: Describe the roles of the NA in EOL care and pain management Define pain Describe acute and chronic pain Describe some common
Obstacles to appropriate and timely pain relief in the Emergency Department for people with cognitive impairment
 Obstacles to appropriate and timely pain relief in the Emergency Department for people with cognitive impairment Lynn Chenoweth Professor, Centre for Healthy Brain Ageing University of New South Wales,
Obstacles to appropriate and timely pain relief in the Emergency Department for people with cognitive impairment Lynn Chenoweth Professor, Centre for Healthy Brain Ageing University of New South Wales,
SECTION J: HEALTH CONDITIONS. J0100: Pain Management (5-Day Look Back) Item Rationale Health-related Quality of Life.
 SECTION J: HEALTH CONDITIONS Intent: The intent of the items in this section is to document a number of health conditions that impact the resident s functional status and quality of life. The items include
SECTION J: HEALTH CONDITIONS Intent: The intent of the items in this section is to document a number of health conditions that impact the resident s functional status and quality of life. The items include
MOTOR VEHICLE ACCIDENT PAIN CHART
 MOTOR VEHICLE ACCIDENT PAIN CHART Name Today s Date (D/M/Y) Area of Concern What is the WORST pain you have ever experienced? (other than the pain you are experiencing NOW!) What was the date of this painful
MOTOR VEHICLE ACCIDENT PAIN CHART Name Today s Date (D/M/Y) Area of Concern What is the WORST pain you have ever experienced? (other than the pain you are experiencing NOW!) What was the date of this painful
Vanderbilt & Qsource Webinar Series
 Vanderbilt & Qsource Webinar Series Vanderbilt Medical Center Vanderbilt University Center for Quality Aging Qsource Session #1: Introduction to Dementia Care & QAPI Session #2: Dementia & Behavioral Disturbances
Vanderbilt & Qsource Webinar Series Vanderbilt Medical Center Vanderbilt University Center for Quality Aging Qsource Session #1: Introduction to Dementia Care & QAPI Session #2: Dementia & Behavioral Disturbances
Psychosocial Outcome Severity Guide Instructor s Guide
 Centers for Medicare & Medicaid Services (CMS) Instructor s Guide 2006 Prepared by: American Institutes for Research 1000 Thomas Jefferson St, NW Washington, DC 20007 Slide 1 Psychosocial Outcome Severity
Centers for Medicare & Medicaid Services (CMS) Instructor s Guide 2006 Prepared by: American Institutes for Research 1000 Thomas Jefferson St, NW Washington, DC 20007 Slide 1 Psychosocial Outcome Severity
The Palliative Care Journey. By Sandra O Sullivan Clinical Nurse Manager 1 St Luke's home
 The Palliative Care Journey By Sandra O Sullivan Clinical Nurse Manager 1 St Luke's home Aims 1. To provide an overview of what palliative care involves. 2. Identify, at what stage should Dementia be acknowledged
The Palliative Care Journey By Sandra O Sullivan Clinical Nurse Manager 1 St Luke's home Aims 1. To provide an overview of what palliative care involves. 2. Identify, at what stage should Dementia be acknowledged
Parent Pain Questionnaire Understanding your child s pain
 Parent Pain Questionnaire Understanding your child s pain This questionnaire is to help us learn about your child's pain problems. All information obtained from this questionnaire and in interviews will
Parent Pain Questionnaire Understanding your child s pain This questionnaire is to help us learn about your child's pain problems. All information obtained from this questionnaire and in interviews will
(ADULT) Refer to policy MC.E.48 for neonatal to pediatric pain assessment and management.
 Department: Policy/Procedure: PATIENT CARE PAIN ASSESSMENT AND DOCUMENTATION (ADULT) Refer to policy MC.E.48 for neonatal to pediatric pain assessment and management. Definition: Pain can be described
Department: Policy/Procedure: PATIENT CARE PAIN ASSESSMENT AND DOCUMENTATION (ADULT) Refer to policy MC.E.48 for neonatal to pediatric pain assessment and management. Definition: Pain can be described
Guiding Principles for Dementia Care in Assisted Living
 Guiding Principles for Dementia Care in Assisted Living Dementia care is a priority for all long term care providers, including assisted living. According to the 2009 Overview of Assisted Living 1, it
Guiding Principles for Dementia Care in Assisted Living Dementia care is a priority for all long term care providers, including assisted living. According to the 2009 Overview of Assisted Living 1, it
Investigation A: Rib Area Pain 3.3B: Shingles
 Investigation 3.3 3.3A: Rib Area Pain 3.3B: Shingles Investigation 3.3A: Rib Area Pain 1. Introduction: When a patient presents with pain in their chest or ribs, as their physician, must sort out the origin
Investigation 3.3 3.3A: Rib Area Pain 3.3B: Shingles Investigation 3.3A: Rib Area Pain 1. Introduction: When a patient presents with pain in their chest or ribs, as their physician, must sort out the origin
Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego
 Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
Comprehensive Medication History Interview Form
 Comprehensive Medication History Interview Form Introduction Introduce self and profession. Explain purpose of session. PharmD Completing Form: Does the patient wish for a family member to be present during
Comprehensive Medication History Interview Form Introduction Introduce self and profession. Explain purpose of session. PharmD Completing Form: Does the patient wish for a family member to be present during
MODULE III Challenging Behaviors
 Mental Health Ombudsman Training Manual Advocacy and the Adult Home Resident MODULE III Challenging Behaviors S WEHRY 2004 Objectives: Part One Describe principles of communication Describe behavior as
Mental Health Ombudsman Training Manual Advocacy and the Adult Home Resident MODULE III Challenging Behaviors S WEHRY 2004 Objectives: Part One Describe principles of communication Describe behavior as
Pain: Facility Assessment Checklists
 Pain: Facility Assessment Checklists This is a series of self-assessment checklists for nursing home staff to use to assess processes related to pain management in the facility and to identify areas that
Pain: Facility Assessment Checklists This is a series of self-assessment checklists for nursing home staff to use to assess processes related to pain management in the facility and to identify areas that
Fall Risk Assessment and Prevention in the Post-Acute Setting A Road Map
 Fall Risk Assessment and Prevention in the Post-Acute Setting A Road Map Cora M. Butler, JD, RN, CHC HealthCore Value Advisors, Inc. Juli A. James, RN Primaris Holdings, Inc. Objectives Explore the burden
Fall Risk Assessment and Prevention in the Post-Acute Setting A Road Map Cora M. Butler, JD, RN, CHC HealthCore Value Advisors, Inc. Juli A. James, RN Primaris Holdings, Inc. Objectives Explore the burden
The Abuse Intervention Model: A Pragmatic Approach to Detecting & Preventing Elder Mistreatment
 The Abuse Intervention Model: A Pragmatic Approach to Detecting & Preventing Elder Mistreatment Laura Mosqueda, M.D. Professor of Family Medicine and Geriatrics Director, National Center on Elder Abuse
The Abuse Intervention Model: A Pragmatic Approach to Detecting & Preventing Elder Mistreatment Laura Mosqueda, M.D. Professor of Family Medicine and Geriatrics Director, National Center on Elder Abuse
Dementia: What Is It?
 Pamela Longmire, RT, BAS Lead Nursing Home Quality Improvement Specialist, Montana No identified conflict of interest for any planner or presenter of this program. 2 RN contact hours have been approved
Pamela Longmire, RT, BAS Lead Nursing Home Quality Improvement Specialist, Montana No identified conflict of interest for any planner or presenter of this program. 2 RN contact hours have been approved
The University of Iowa College of Nursing Alzheimer's Family Involvement in Care Study. Caregiver Stress Inventory (CSI) (4-9) (10-13)
 1 The University of Iowa College of Nursing Alzheimer's Family Involvement in Care Study Caregiver Stress Inventory (CSI) ID# Date: (4-9) (10-13) DIRECTIONS: Each of the statements in this questionnaire
1 The University of Iowa College of Nursing Alzheimer's Family Involvement in Care Study Caregiver Stress Inventory (CSI) ID# Date: (4-9) (10-13) DIRECTIONS: Each of the statements in this questionnaire
Pain: You Can Get Help
 National Institute on Aging AgePage Pain: You Can Get Help Phyllis loves playing with her grandchildren, working in the garden, and going to bingo games twice a week. But, at age 76, the constant knee
National Institute on Aging AgePage Pain: You Can Get Help Phyllis loves playing with her grandchildren, working in the garden, and going to bingo games twice a week. But, at age 76, the constant knee
Medical History Form
 Medical History Form Name: ; Birth date: / / ; Date: / / Person filling out form: ; Relationship: Thank you for taking the time to fill out this valuable information. This allows us to provide the best
Medical History Form Name: ; Birth date: / / ; Date: / / Person filling out form: ; Relationship: Thank you for taking the time to fill out this valuable information. This allows us to provide the best
AMBULATION. Ambulation. Process of moving about. Walking Transferring to and from bed, chair, toilet, car
 AMBULATION AMBULATION Ambulation Process of moving about Walking Transferring to and from bed, chair, toilet, car AMBULATION Levels of ambulation training Independent Setup Supervised Limited Extensive
AMBULATION AMBULATION Ambulation Process of moving about Walking Transferring to and from bed, chair, toilet, car AMBULATION Levels of ambulation training Independent Setup Supervised Limited Extensive
Caring Sheet #17: Safety After Hip Surgery: Tips for Preventing Complications By Ben Atchison, PhD, OTR, FAOTA
 : : Tips for Preventing Complications By Ben Atchison, PhD, OTR, FAOTA Introduction Dementia can increase a person s chances of breaking a hip. After surgery on the hip there is an increased risk of further
: : Tips for Preventing Complications By Ben Atchison, PhD, OTR, FAOTA Introduction Dementia can increase a person s chances of breaking a hip. After surgery on the hip there is an increased risk of further
Catching Some ZZZs Why Sleep Matters. How did YOU sleep last night?
 Catching Some ZZZs Why Sleep Matters. Presenter: Dr. Linda M. Shell MA, RN Linda@Lindashell.com September 2018 How did YOU sleep last night? Centers for Disease Control has declared sleep deprivation to
Catching Some ZZZs Why Sleep Matters. Presenter: Dr. Linda M. Shell MA, RN Linda@Lindashell.com September 2018 How did YOU sleep last night? Centers for Disease Control has declared sleep deprivation to
American Board of Psychiatry and Neurology, Inc. Geriatric Psychiatry Core Competencies Outline
 American Board of Psychiatry and Neurology, Inc. Geriatric Psychiatry Core Competencies Outline I. Geriatric Psychiatry Patient Care and Procedural Skills Core Competencies A. Geriatric psychiatrists shall
American Board of Psychiatry and Neurology, Inc. Geriatric Psychiatry Core Competencies Outline I. Geriatric Psychiatry Patient Care and Procedural Skills Core Competencies A. Geriatric psychiatrists shall
Instructions for Patients Following Vitreoretinal Surgery Who Need to Posture
 Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Instructions for Patients Following Vitreoretinal Surgery Who Need to Posture Patient name: Hospital Number: Consultant: Surgery
Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Instructions for Patients Following Vitreoretinal Surgery Who Need to Posture Patient name: Hospital Number: Consultant: Surgery
Pain and Dementia. How Dementia Impacts Pain Assessment & Intervention. When will DEMENTIA be a factor for you? In Dementia
 Pain and Dementia How Dementia Impacts Pain Assessment & Intervention When will DEMENTIA be a factor for you? End of dementia end of life Mid-dementia - with another terminal disease Early dementia - a
Pain and Dementia How Dementia Impacts Pain Assessment & Intervention When will DEMENTIA be a factor for you? End of dementia end of life Mid-dementia - with another terminal disease Early dementia - a
The role of the caregiver
 The role of the caregiver Presented by Alba Bonetti Neurology training for non-neurologists in West Africa: Focus on Parkinson s Disease and other Neurodegenerative Disorders GHANA SEPTEMBER 15-18 2013
The role of the caregiver Presented by Alba Bonetti Neurology training for non-neurologists in West Africa: Focus on Parkinson s Disease and other Neurodegenerative Disorders GHANA SEPTEMBER 15-18 2013
Managing Challenging Behaviors
 Managing Challenging Behaviors Barbara J. Kocsis, MD Psychiatry Resident, HDSA Center of Excellence UC Davis School of Medicine & Lorin M. Scher, MD Attending Psychiatrist, HDSA Center of Excellence UC
Managing Challenging Behaviors Barbara J. Kocsis, MD Psychiatry Resident, HDSA Center of Excellence UC Davis School of Medicine & Lorin M. Scher, MD Attending Psychiatrist, HDSA Center of Excellence UC
Explaining Epidemiological. Factors of Falls. to Older Adults. After a Fall. Before a Fall. Frequent Falls
 Explaining Epidemiological Factors of Falls to Older Adults Before a Fall After a Fall Frequent Falls Epidemiological Factors of Falls Falls are a serious, epidemic problem. In Canada, it is estimated
Explaining Epidemiological Factors of Falls to Older Adults Before a Fall After a Fall Frequent Falls Epidemiological Factors of Falls Falls are a serious, epidemic problem. In Canada, it is estimated
Exercise, Physical Therapy and Fall Prevention
 Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
Managing Challenging Behaviors
 Managing Challenging Behaviors Barbara J. Kocsis, MD Psychiatry Resident, HDSA Center of Excellence UC Davis School of Medicine In partnership with Drs. Lorin Scher, MD and Vicki Wheelock, MD 1 Our Goal
Managing Challenging Behaviors Barbara J. Kocsis, MD Psychiatry Resident, HDSA Center of Excellence UC Davis School of Medicine In partnership with Drs. Lorin Scher, MD and Vicki Wheelock, MD 1 Our Goal
Module 1 Worksheet: INTRODUCTION TO END-OF-LIFE DEMENTIA CARE
 Your Name: Date: Module 1 Worksheet: INTRODUCTION TO END-OF-LIFE DEMENTIA CARE 1. Circle all of the following that are examples of a reflex: Sucking Talking c) Grasping d) Waving 2. Define mottled. (Hint:
Your Name: Date: Module 1 Worksheet: INTRODUCTION TO END-OF-LIFE DEMENTIA CARE 1. Circle all of the following that are examples of a reflex: Sucking Talking c) Grasping d) Waving 2. Define mottled. (Hint:
CHS 446 Communication Skills for the Healthcare Professional Mohammed S. Alnaif, Ph.D.
 CHS 446 Communication Skills for the Healthcare Professional Mohammed S. Alnaif, Ph.D. alnaif@ksu.edu.sa 1 As discussed in previous chapters, pain, fear, and anxiety may negatively impact communication
CHS 446 Communication Skills for the Healthcare Professional Mohammed S. Alnaif, Ph.D. alnaif@ksu.edu.sa 1 As discussed in previous chapters, pain, fear, and anxiety may negatively impact communication
BODY SYSTEMS, DRUGS, AND OBSERVATIONS SCOPE OF UNIT: This unit includes guidelines for observing and reporting.
 LESSON PLAN: 10 COURSE TITLE: UNIT: III MEDICATION TECHNICIAN BODY SYSTEMS, DRUGS, AND OBSERVATIONS SCOPE OF UNIT: This unit includes guidelines for observing and reporting. INFORMATION TOPIC: III-10 OR
LESSON PLAN: 10 COURSE TITLE: UNIT: III MEDICATION TECHNICIAN BODY SYSTEMS, DRUGS, AND OBSERVATIONS SCOPE OF UNIT: This unit includes guidelines for observing and reporting. INFORMATION TOPIC: III-10 OR
Understanding the impact of pain and dementia
 Understanding the impact of pain and dementia Knowing how to identify and manage the symptoms of pain in people living with dementia is an important part of a carer s role. This guide provides an overview
Understanding the impact of pain and dementia Knowing how to identify and manage the symptoms of pain in people living with dementia is an important part of a carer s role. This guide provides an overview
CNA Training Advisor
 CNA Training Advisor Volume 12 Issue No. 1 January 2014 Pain management Pain affects many nursing home residents. It often results from injury or sensory stimulation. A variety of factors affect recognition,
CNA Training Advisor Volume 12 Issue No. 1 January 2014 Pain management Pain affects many nursing home residents. It often results from injury or sensory stimulation. A variety of factors affect recognition,
Please describe, in detail, when the symptoms began:
 161 East Mallard Drive, Suite 130, Boise, ID 83706 (208) 947-0100 New Patient Intake Patient Name: Primary Care Physician: Date: Email address: How did you hear about AVT (mark all that apply) Online On
161 East Mallard Drive, Suite 130, Boise, ID 83706 (208) 947-0100 New Patient Intake Patient Name: Primary Care Physician: Date: Email address: How did you hear about AVT (mark all that apply) Online On
LSU Health Sciences Center
 LSU Health Sciences Center Speech-Language-Hearing Clinic, Department of Communication Disorders, School of Allied Health Professions, 1900 Gravier Street, 9 th Floor, New Orleans, La 70112 Date: Identification
LSU Health Sciences Center Speech-Language-Hearing Clinic, Department of Communication Disorders, School of Allied Health Professions, 1900 Gravier Street, 9 th Floor, New Orleans, La 70112 Date: Identification
Pain Assessment. Cathy Murray MSN RN OCNS-C Clinical Nurse Specialist December /21/2014 1
 Pain Assessment Cathy Murray MSN RN OCNS-C Clinical Nurse Specialist December 2013 3/21/2014 1 Objectives Articulate pain assessment strategies. Identify appropriate assessment tools for patients. Describe
Pain Assessment Cathy Murray MSN RN OCNS-C Clinical Nurse Specialist December 2013 3/21/2014 1 Objectives Articulate pain assessment strategies. Identify appropriate assessment tools for patients. Describe
The Psychometric Qualities of Four Observational Pain Tools (OPTs) for the Assessment of Pain in Elderly People with Osteoarthritic Pain
 582 Journal of Pain and Symptom Management Vol. 40 No. 4 October 2010 Original Article The Psychometric Qualities of Four Observational Pain Tools (OPTs) for the Assessment of Pain in Elderly People with
582 Journal of Pain and Symptom Management Vol. 40 No. 4 October 2010 Original Article The Psychometric Qualities of Four Observational Pain Tools (OPTs) for the Assessment of Pain in Elderly People with
OBJECTIVES 5NW GERIATRICS UNIT. nicheprogram.org 2016 Annual NICHE Conference Care Across the Continuum 1
 Family Education for Nonverbal Patient Pain Control Jeannette (Jeannie) Meyer, MSN, RN, CCRN CCNS, PCCN, ACHPN Clinical Nurse Specialist Palliative Care Santa Monica UCLA Medical Center Anila Ladak, RN,
Family Education for Nonverbal Patient Pain Control Jeannette (Jeannie) Meyer, MSN, RN, CCRN CCNS, PCCN, ACHPN Clinical Nurse Specialist Palliative Care Santa Monica UCLA Medical Center Anila Ladak, RN,
Recognizing and Managing the Emotional Aspects of Parkinson s. Pamela R. Palmentera, LCSW Coordinator & Clinical Social Worker
 Recognizing and Managing the Emotional Aspects of Parkinson s Pamela R. Palmentera, LCSW Coordinator & Clinical Social Worker Sensory information from the one hemisphere crosses over to the other side
Recognizing and Managing the Emotional Aspects of Parkinson s Pamela R. Palmentera, LCSW Coordinator & Clinical Social Worker Sensory information from the one hemisphere crosses over to the other side
Working together to prevent falls
 Quality Care - for you, with you Working together to prevent falls Introduction Falling is a common problem throughout our lifetime but as we get older the risk of injury from falls unfortunately gets
Quality Care - for you, with you Working together to prevent falls Introduction Falling is a common problem throughout our lifetime but as we get older the risk of injury from falls unfortunately gets
CARPAL TUNNEL RELEASE
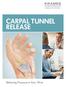 CARPAL TUNNEL RELEASE Relieving Pressure in Your Wrist What Is Carpal Tunnel Syndrome? Carpal tunnel syndrome (CTS) is a condition that affects nerves in the wrist and hand. CTS causes tingling and numbness
CARPAL TUNNEL RELEASE Relieving Pressure in Your Wrist What Is Carpal Tunnel Syndrome? Carpal tunnel syndrome (CTS) is a condition that affects nerves in the wrist and hand. CTS causes tingling and numbness
Redefining Fall Risk for Persons with Dementia Tena Alonzo LeadingAge Arizona May 30, 2018
 Redefining Fall Risk for Persons with Dementia Tena Alonzo LeadingAge Arizona May 30, 2018 Learning Objectives 1. Describe the progression of dementia as it applies to falls and persons who have trouble
Redefining Fall Risk for Persons with Dementia Tena Alonzo LeadingAge Arizona May 30, 2018 Learning Objectives 1. Describe the progression of dementia as it applies to falls and persons who have trouble
Psychosocial Problems In Reproductive Health Of Elders
 Psychosocial Problems In Reproductive Health Of Elders Dr. Sonia Oveisi Maternity and Child Health Assistant Professor of Qazvin University of Medical Science 6/2/2014 1 Goals 1. Definition 2. Epidemiology
Psychosocial Problems In Reproductive Health Of Elders Dr. Sonia Oveisi Maternity and Child Health Assistant Professor of Qazvin University of Medical Science 6/2/2014 1 Goals 1. Definition 2. Epidemiology
POSTNATAL EXERCISES & ADVICE. Physiotherapy Department
 POSTNATAL EXERCISES & ADVICE Physiotherapy Department This booklet provides advice and exercises to help you to get back to normal after the birth or your baby. Rest: After having your baby it is important
POSTNATAL EXERCISES & ADVICE Physiotherapy Department This booklet provides advice and exercises to help you to get back to normal after the birth or your baby. Rest: After having your baby it is important
Winter health advice for older people
 Winter health advice for older people Here are some simple things you can do to stay well this winter Common winter illnesses Keep warm to help prevent colds, flu or more serious health conditions such
Winter health advice for older people Here are some simple things you can do to stay well this winter Common winter illnesses Keep warm to help prevent colds, flu or more serious health conditions such
9/11/2012. Clare I. Hays, MD, CMD
 Clare I. Hays, MD, CMD Review regulatory background for current CMS emphasis on antipsychotics Understand the risks and (limited) benefits of antipsychotic medications Review non-pharmacologic management
Clare I. Hays, MD, CMD Review regulatory background for current CMS emphasis on antipsychotics Understand the risks and (limited) benefits of antipsychotic medications Review non-pharmacologic management
NTG-EDSD v.1/ Instructions: For each question block, check the item that best applies to the individual or situation. Name of person: (3) First
 NTG-EDSD v.1/2013.2 The NTG-Early Detection Screen for Dementia, adapted from the DSQIID*, can be used for the early detection screening of those adults with an intellectual disability who are suspected
NTG-EDSD v.1/2013.2 The NTG-Early Detection Screen for Dementia, adapted from the DSQIID*, can be used for the early detection screening of those adults with an intellectual disability who are suspected
EXERCISE and ADVICE. after pregnancy
 EXERCISE and ADVICE after pregnancy Contents Introduction...1 Comfort...2 Activity in the early days...3 Caesarean section operation...3 Exercises...4 Regaining your physical well-being...7 Contact information...ibc
EXERCISE and ADVICE after pregnancy Contents Introduction...1 Comfort...2 Activity in the early days...3 Caesarean section operation...3 Exercises...4 Regaining your physical well-being...7 Contact information...ibc
Delirium Information for relatives, carers and patients
 Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Communication and Dementia Listening with your Heart. Presented by: Kelly Tye Vallis Speech-Language Pathologist WRHA LTC SLP service
 Communication and Dementia Listening with your Heart Presented by: Kelly Tye Vallis Speech-Language Pathologist WRHA LTC SLP service Learning Objectives To understand the communication process To recognize
Communication and Dementia Listening with your Heart Presented by: Kelly Tye Vallis Speech-Language Pathologist WRHA LTC SLP service Learning Objectives To understand the communication process To recognize
Tuberculosis Facts. TB is not spread by: Sharing food and drink Shaking someone s hand Touching bed lines or toilet seats
 Tuberculosis Facts Below are frequently asked questions about TB, and their answers. If you have additional questions you may contact the City of Ennis Department of Health Services at 972-875-1234 or
Tuberculosis Facts Below are frequently asked questions about TB, and their answers. If you have additional questions you may contact the City of Ennis Department of Health Services at 972-875-1234 or
Redefining Fall Risk for Persons with Dementia Tena Alonzo 2016 NASRM Conference October 6, 2016
 Redefining Fall Risk for Persons with Dementia Tena Alonzo 2016 NASRM Conference October 6, 2016 Learning Objectives 1. Describe the progression of dementia as it applies to falls and persons who have
Redefining Fall Risk for Persons with Dementia Tena Alonzo 2016 NASRM Conference October 6, 2016 Learning Objectives 1. Describe the progression of dementia as it applies to falls and persons who have
