N europsychiatric symptoms can induce marked disability
|
|
|
- Laureen Cameron
- 5 years ago
- Views:
Transcription
1 PAPER Neuropsychiatric profiles in patients with Alzheimer s disease and vascular dementia J-L Fuh, S-J Wang, J L Cummings... See end of article for authors affiliations... Correspondence to: Dr J-L Fuh, Neurological Institute, Taipei Veterans General Hospital, Taiwan, Republic of China; jlfuh@ vghtpe.gov.tw Received 14 October 2004 In revised form 16 January 2005 Accepted 26 January J Neurol Neurosurg Psychiatry 2005;76: doi: /jnnp Objective: To explore the neuropsychiatric manifestations in patients with Alzheimer s disease () and cortical and subcortical vascular dementia (VaD). Methods: We investigated consecutive patients with dementia. All the participants received brain computed tomography. The diagnosis of dementia was confirmed by clinical criteria and the imaging findings. Only patients with probable, and subcortical and cortical VaD were included. The Mini Mental State Examination (MMSE) was used to evaluate global cognitive function, and the Neuropsychiatric Inventory (NPI) was used to assess neuropsychiatric symptoms. Results: Of the 536 participants with dementia, 320 (59.7%) had, 161 (30%) had subcortical VaD, 35 (6.4%) had cortical VaD, and 16 (2.9%) had mixed cortical and subcortical VaD. Cortical VaD patients had the highest mean composite NPI scores in all domains and patients had the lowest composite scores in most domains. The mean composite scores of the apathy and sleep disturbance domains in patients with cortical VaD were significantly higher than those in the patients with after controlling for years of education and MMSE score (p,0.01). Conclusions: There were few differences among the patients with, subcortical VaD and cortical VaD. The most consistent differences were the high sleep disturbance scores in those with cortical VaD. N europsychiatric symptoms can induce marked disability in patients with dementia and increase caregiver distress. 1 Several studies have found that neuropsychiatric symptoms are common both in patients with Alzheimer s disease () and those with vascular dementia (VaD). 2 6 Nevertheless, studies of the neuropsychiatric disturbances in patients with VaD are few and the results are controversial. Some studies suggested that neuropsychiatric symptoms were more common in VaD than in, but others report conflicting observations. 2 4 Investigations of affective disorder also revealed controversial findings between the patients with VaD and. 2 5 These discrepancies might be caused by different VaD diagnostic criteria with variable sensitivity and specificity, 7 10 and use of different evaluation tools for neuropsychiatric manifestations. The association between and VaD is complex. It is not uncommon to have vascular changes in patients with, and the vascular lesions can worsen cognitive impairment Nevertheless, the clinical cognitive profiles of and VaD are distinguishable, as frontal executive dysfunction is the most prominent feature of VaD. 14 Could different types of dementia also present different neuropsychiatric profiles? This question is important because these differences could affect treatment approaches and caregiver distress The neuropathology of VaD is heterogeneous. Several vascular pathologies can lead to dementia. 16 The clinical presentation and course of these different subtypes of VaD vary but their neuropsychiatric manifestations have rarely been studied. A syndrome of subcortical VaD incorporating both Binswanger s disease and lacunar state is a more homogenous group. 17 To subgroup VaD into subcortical and cortical types may facilitate comparisons between and VaD. In this study, we assessed neuropsychiatric symptoms using a standard tool, the Neuropsychiatric Inventory (NPI), 18 in a large clinical sample of consecutive patients with and different subtypes of VaD. The aim of this study was to 1337 determine if the neuropsychiatric manifestations in patients with, cortical VaD, and subcortical VaD differ. PATIENTS AND METHODS Patients The study comprised 1376 consecutive outpatients who complained of memory decline and were examined at the outpatient clinic of the Taipei Veterans General Hospital from December 1999 to October The Institutional review board of Taipei Veterans General Hospital approved the study protocol. Assessments and measures All patients were evaluated by clinical interview, and neurological and physical examination. The Mini Mental State Examination (MMSE) 19 and NPI 18 were administered to the patients and caregivers respectively. The MMSE 19 is one of the most widely used screening instruments for dementia, and provides a total score ranging from 0 to 30, with lower scores indicative of greater cognitive impairment. It was administered to the patients to obtain an overall level of current cognitive function. Information on neuropsychiatric symptoms was obtained from caregivers using the NPI. 18 There is a screening question assaying each sub-area, including delusions, hallucinations, agitation, apathy, anxiety, depression, euphoria, irritability, disinhibition, aberrant motor behaviour, change in appetite, and night time behaviour disturbances. If the answer to this screening question was no, then no further questions were asked. If the answer was yes, then sub-questions were asked and ratings of the frequency and severity of the Abbreviations:, Alzheimer s disease; CDR, Clinical Dementia Rating; CT, computed tomography; CVD, cerebrovascular diseases; DSM-IV, Diagnostic and statistical manual of mental disorders, 4th edition; MMSE, Mini Mental State Examination; NINCDS-RDA, National Institute of Neurological and Communicative Disorders and Stroke Alzheimer s Disease and Related Disorders Association; NPI, Neuropsychiatric Inventory; VaD, vascular dementia
2 1338 Fuh, Wang, Cummings behaviour were made by the caregiver based on scales with anchor points (frequency: 1 = occasionally, 2 = often, 3 = frequently, 4 = very frequently; severity: 1 = mild, 2 = moderate, 3 = severe). The frequency rating multiplied by the severity rating produced a composite score for each behaviour. A global score for the NPI was generated by summing the total scores of the individual subscales. Cronbach s a for overall reliability of NPI was 0.88 and the concurrent validity was good, as shown by an acceptable correlation between NPI scores and other validated measurements. 18 The Clinical Dementia Rating (CDR) scale provides a global rating of the severity of dementia, ranging from 0 (no impairment) to 3 (severe impairment). 20 The overall CDR rating was obtained from one primary domain (memory) and five secondary domains (orientation, judgement and problem solving, community affairs, home hobbies, and personal care). We reviewed the relevant medical records and requested laboratory tests for participants with dementia, including complete blood counts, chemistries, serum vitamin B12, folic acid, thyroid function tests, and syphilis serology. Brain computerised tomography (CT) was also obtained on all participants with dementia. Criteria of dementia The diagnosis of dementia was made according to the Diagnostic and statistical manual of mental disorders, 4th edition (DSM-IV) criteria. 21 Patients with delirium were excluded. Subjects who met the dementia criteria were further classified as to their type of dementia at a consensus meeting after the history, laboratory findings, and the results of brain CT were reviewed. The diagnostic physicians were blinded to the results of the NPI. Patients were diagnosed as having if they met the criteria of the National Institute of Neurological and Communicative Disorders and Stroke Alzheimer s Disease and Related Disorders Association (NINCDS-RDA) guidelines. 22 Patients who fulfilled NINCDS-RDA 23 criteria for probable and had a single silent lacune, small cortical infarct, or disproportionately large ventricles found on brain imaging were excluded from analysis in this study. VaD was defined according to modified DSM-IV criteria. 21 DSM-IV criteria 21 for VaD originally allowed focal neurological signs or laboratory evidence indicative of cerebrovascular disease (CVD). However, in this study, we required both the clinical criteria and demonstrate ischaemic abnormalities on CT. We classified VaD based on CT findings as subcortical VaD (small vessel disease, multiple lacunar infarcts, and/or extensive periventricular white matter lesions) and cortical VaD (large vessel disease, infarcts involving the cortical grey matter). We excluded patients with cerebral haemorrhage. Statistical analysis Statistical analysis was performed with SPSS for Windows (version 11.0.; SPSS Inc., Chicago, IL, USA) We used the x 2 test to compare the proportions of participants with different types of dementia who had a score of 1 or higher in any individual NPI domain. We also compared the prevalence of neuropsychiatric disturbances in different dementia stages. We compared the NPI mean scores for participants with, subcortical VaD, cortical VaD, and mixed cortical and subcortical VaD as an indicator of behavioural change in each domain. The differences between the groups were analysed using one way analysis of variance, and the Scheffé test was used to explore the individual group effects. To control for the severity of dementia as a confounding factor, we constructed a series of linear regression models, one for each domain and one for the total NPI score. Individual NPI domain scores or the NPI total score were the dependent variables, and the presence or absence of different types of dementia was the independent variable. We also adjusted for MMSE and educational level in the analysis. A p value,0.01 was regarded as statically significant, balancing the risk of type I and II errors. RESULTS Patients characteristics Fig 1 shows a flow diagram describing the number of participants participating to the study and those meeting inclusion and exclusion criteria. A total 536 subjects participated in this study: 320 (59.7%) with (mean (SD) age 75.2 (7.2) years), 161 (30%) with subcortical VaD (75.1 (7.3) years), 35 (6.4%) with cortical VaD (75.8 (6.9) years), and 16 (2.9%) with mixed cortical and subcortical VaD (74.0 (7.0) years). The proportion of male patients was significantly lower in the compared with the subcortical VaD group (54% v 69%, p,0.01) and the proportion of severe dementia (CDR = 3) was significantly lower in the compared with the cortical VaD group (8% v 29%, p,0.001). The age, educational level, and MMSE score did not differ between the subjects with solely cortical and with mixed cortical and subcortical lesions. The patients with solely cortical VaD had significantly lower mean (SD) MMSE scores compared with or solely subcortical VaD patients (11.6 (7.5) v 17.1 (6.8) and 15.6 (6.8), p,0.001). Neuropsychiatric manifestations among the different types of dementia Fig 2 compares the prevalence of NPI based disturbances in participants with and those with subcortical, cortical, and mixed VaD. The prevalence of NPI disturbances was similar in the four groups. The patients with cortical VaD had marginally greater prevalence of agitation and sleep disturbances (p = 0.03 and 0.04, respectively). Comparing the mean composite subcores of the NPI domains across the four types of dementia, the cortical VaD had the highest composite scores in all domains and the highest total NPI score. The total 12 item NPI score reached significance by one way analysis of variance (p,0.01) but showed only a trend toward a difference between and cortical VaD by the Scheffé test (mean (SD) 13.8 (17.9) v 24.6 (27.3), p = 0.02). Among the subdomains, only the apathy and sleep disturbance domains reached statistical significance by one way analysis of variance (p,0.01). Comparisons using the Scheffé test indicated that the cortical VaD group had significantly higher scores compared with the group in the sleep disturbance domain (3.6 (4.1) v 1.7 (2.8), p,0.01), and there was a trend for patients with cortical VaD and subcortical VaD to have higher scores compared with the group in the apathy domain (3.4 (3.9) and 2.6 (3.8) v 1.6 (2.8), p = 0.03). Relationship of severity of dementia to the neuropsychiatric manifestations Table 1 shows the prevalence of individual NPI domain scores in patients with dementia of different severities as classified by the CDR. We did not include mixed VaD during the analysis because of the small number of patients. The prevalence of delusions, hallucinations, and aberrant motor activities increased significantly with the severity of dementia in patients with and subcortical VaD. The differences were statistically significant for the prevalence of apathy, agitation, and disinhibition in patients with. The prevalence of sleep disturbance was different in the patients with subcortical VaD. There were no differences in the prevalence of any NPI domain except the apathy domain across CDR staging in patients with cortical VaD. In patients with mild dementia (CDR = 1), there were no differences in
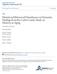
3 BPSD in and VaD 1339 Figure 1 Probable Alzheimer's disease n = screened for diagnosed dementia Screen for dementia (MMSE, history, laboratory tests) 928 had dementia Dementia subtype diagnosis (computed tomographic scan consensus meeting) Subcortical vascular dementia n = 161 Cortical vascular dementia n = 35 Flow diagram of participants meeting inclusion and exclusion criteria. the prevalence of any NPI domain across different types of dementia. Although the prevalence of anxiety differed among different dementia types, the domain scores were not significantly different, owing to the small number of cortical VaD group. As the prevalence of NPI disturbances might be confounded by the severity of dementia, and the cortical VaD patients had the lowest MMSE score and educational level, we conducted a linear regression analysis to compare the apathy score in each of the three groups after controlling for these two factors. The patients with cortical VaD still had higher mean scores than the patients with in the apathy (b = 0.12, t = 2.75, p = 0.006) and sleep disturbance (b = 0.13, t = 2.89, p = 0.004) domains. The total 12 item NPI score did not show significant differences among the different types of dementia after controlling for MMSE and educational level (b = 0.10, t = 2.29, p = 0.02) DISCUSSION The present study demonstrated that behavioural disturbances are very common in patients with dementia, regardless of the dementia type. Consistent with previous reports, our data showed only minor differences in the prevalence of behavioural disturbances in and VaD. It also supported past clinical reports that the differentiation of VaD from is difficult using clinical and neuropsychiatric features only. 5 Nevertheless, specific differences in neuropsychiatric manifestations existed between patients with and VaD, most prominently in the domain of sleep disturbance, which was more severe in cortical VaD. Our study also revealed a trend for the severity of neuropsychiatric manifestations to be Cortical and subcortical vascular dementia n = excluded (no dementia) 391 excluded: No imaging studies (46) Possible Alzheimer's disease (116) Normal pressure hydrocephalus (17) Parkinson's disease (19) Dementia with Lewy bodies (11) Frontotemporal dementia (7) Other or multiple aetiologies (176) greatest in cortical VaD and least in. Our study results emphasise the importance of subgrouping VaD into cortical and subcortical types. Patients with cortical VaD had significantly higher mean composite scores in the sleep disturbance domain. This is consistent with a previous small group studies showing that VaD patients have more disrupted sleep/wake cycles and decreased sleep quality compared with patients. 26 Our study showed that patients with VaD tended to have higher scores on the apathy domain compared with patients, although the differences did not reach statistical significance. Apathy has been attributed to disruption of corticosubcortical circuits involving the basal ganglia, thalamus, and frontal lobes is a cortical dementia, and the subcortical structures are largely preserved, whereas subcortical VaD disturbs corticosubcortical circuits with lacunar lesions and white matter ischaemic injury. Cortical lesions in VaD likewise commonly involve frontal regions and may disrupt corticosubcortical circuits mediating motivational behaviour. Studies investigating the association of neuropsychiatric manifestations with dementia severity have failed to consistently demonstrate differences in compared with VaD. We found that some disturbances such as delusions, hallucinations, and aberrant motor activities were more common in later stages in both patients with and those with subcortical VaD. A large community based study found agitation and aberrant motor behaviour to be more common in participants with advanced dementia. 24 Our findings support this observation; we found agitation to be more common in later stages among patients with but
4 1340 Fuh, Wang, Cummings Percentage Del Hal Dep Anx Apa Irrit Euph Agi Dis Motor Sleep Appet Subcortical VaD Cortical VaD Mixed VaD not VaD. The higher prevalence of neuropsychiatric manifestations in our patients may be attributable to differences in study populations (hospital based versus community based). The strength of this study is that it was a large, prospective study using a standardised assessment tool and concomitant CT. However, there are some limitations. Firstly, because subjects who participated in this study were from a medical centre, caution should be taken in generalising the study Figure 2 The prevalence of 12 Neuropsychiatric Inventory behaviours across the different types of dementia. Del, delusions, Hal, hallucinations, Dep, depression; Anx, anxiety; Apa, apathy; Irrit, irritability; Euph, euphoria; Agi, agitation; Dis, disinhibition; Motor, aberrant motor activity; Sleep, sleep disturbances; Appet, appetite changes;, Alzheimer s disease; VaD, vascular dementia. *Trend of percentage differences among the different types of dementia (p = 0.03 in the apathy domain and p = 0.04 in the sleep disturbance domain, x 2 test). results. Secondly, the rate of diagnostic misclassification was uncertain because of the lack of neuropathological confirmation in our study. In this study, we attempted to identify pure and excluded subjects who fulfilled the NINCDS- RDA 22 but also had vascular lesions on brain CT. For VaD, we used the DSM-IV criteria 21 in addition to brain CT for diagnosis. Imaging may help compensate for the relatively low specificity of DSM-IV criteria for VaD. 21 Mixed cases may Table 1 Percentage frequency of Neuropsychiatric Inventory disturbances in patients with different types dementia classified by dementia severity NPI domain CDR = 1 CDR = 2 CDR = 3 Total (n = 188) (n = 82) (n = 11) (n = 107) (n = 59) (n = 14) (n = 25) (n = 20) (n = 10) (n = 320) (n = 161) Delusions*À Hallucinations*À Depression Anxiety Apathy*` Irritability Euphoria Agitation/aggression* Disinhibition* Aberrant motor activity*à Sleep disturbanceà Appetite change (n = 35) NPI, Neuropsychiatric Inventory, CDR, clinical dementia rating,, Alzheimer s disease,, subcortical vascular dementia,, cortical vascular dementia. *Significant difference in prevalence of different CDR group among patients with Alzheimer disease (p,0.01, x 2 test); Àsignificant difference in prevalence of different CDR group among patients with subcortical vascular dementia (p,0.01, x 2 test); `significant difference in prevalence of different CDR group among patients with cortical vascular dementia (p,0.01, x 2 test).
5 BPSD in and VaD 1341 be present in the sample despite these diagnostic procedures. Thirdly, the relatively small sample size of patients with cortical VaD might cause some differences among behavioural domains to fail to reach statistical significance. It is also possible that a few patients with very severe psychopathology had a large influence on the small number of samples and thus biased the study results. In conclusion, the present study showed a high prevalence of neuropsychiatric symptoms in both and VaD. Symptoms profiles were similar in the, subcortical VaD, and cortical VaD groups. Sleep disturbance was most severe in the patients with cortical VaD. ACKNOWLEDGEMENTS This study was supported in part by grants from National Science Council (NSC B ).... Authors affiliations J-L Fuh, S-J Wang, Neurological Institute, Veterans General Hospital Taipei and National Yang-Ming University Schools of Medicine, Taipei, Taiwan J L Cummings, UCLA Alzheimer s Disease Center, Departments of Neurology and Psychiatry, David Geffen School of Medicine at UCLA, Los Angeles, California, USA Competing interests: none declared. REFERENCES 1 Rabins PV, Mace NL, Lucas MJ. The impact of dementia on the family. JAMA 1982;248: Sultzer DL, Levin HS, Mahler HW, et al. A comparison of psychiatric symptoms in vascular dementia and Alzheimer s disease. Am J Psychiatry 1993;150: Bucht G, Adolfson R. The comprehensive psychopathological rating scale in patients with dementia of Alzheimer s type and multi-infarct dementia. Acta Psychiatr Scand 1983;68: Swearer JM, Drachman DA, O Donnell BF, et al. Troublesome and disruptive behaviors in dementia: relationship to diagnosis and disease severity. JAm Geriatr Soc 1988;36: Groves WC, Brandt J, Steinberg M, et al. Vascular dementia and Alzheimer s disease: is there a difference? A comparison of symptoms by disease duration. J Neuropsychiatry Clin Neurosci 2000;12: Vetter PH, Krauss S, Steiner O, et al. Vascular dementia versus dementia of Alzheimer s type: do they have differential effects on caregivers burden? J Gerontol B Psychol Sci Soc Sci 1999;54:S Wetterling T, Kanitz RD, Borgis KJ. Comparison of different diagnostic criteria for vascular dementia (DTC, DSM-IV, ICD-10, NINDS-AIREN). Stroke 1996;27: Chui HC, Mack W, Jackson JE. Clinical criteria for the diagnostic of vascular dementia: a multi-centre study of comparability and inter-rater reliability. Arch Neurol 2000;57: Pohjasvaara T, Mantyla R, Salonen O. How complex interactions of ischemic brain infarcts, white matter lesions, and atrophy relate to poststroke dementia. Arch Neurol 2000;57: Gold G, Bouras C, Canuto A. Clinicopathological validation study of four sets of clinical criteria for vascular dementia. Am J Psychiatry 2002;159: Goulding JM, Signorini DF, Chatterjee S, et al. Inverse relation between Braak stage and cerebrovascular pathology in Alzheimer predominant dementia. J Neurol Neurosurg Psychiatry 1999;67: Esiri MM, Nagy Z, Smith MZ, Barnetson L, Smith. Cerebrovascular disease and threshold for dementia in the early stages of Alzheimer s disease. Lancet 1999;354: Snowdon DA, Greiner LH, Mortimer JA, et al. Brain infarction and the clinical expression of Alzheimer disease. The Nun study. JAMA 1997;277: Looi JC, Sachdev PS. Differentiation of vascular dementia from on neuropsychological tests. Neurology 1999;53: Kim JM, Lyons D, Shin JS, et al. Differences in behavioral and psychological symptoms between Alzheimer s disease and vascular dementia: Are the different pharmacologic treatment strategies justifiable? Hum Psychopharmacol 2003;18: Brien JT, Erkinjuntti T, Reisberg B, et al. Vascular cognitive impairment. Lancet Neurol 2003;2: Erkinjuntti T, Inzitari D, Pantoni L, et al. Limitations of clinical criteria for the diagnosis of vascular dementia in clinical trials: is a focus on subcortical vascular dementia a solution? Ann N Y Acad Sci 2000;903: Cummings JL, Mega M, Gray K, et al. The Neuropsychiatric Inventory: comprehensive assessment of psychopathology in dementia. Neurology 1994;44: Folstein MF, Folstein SE, McHugh PR. Mini-Mental State. A practical method for grading the cognitive state of patients for clinician. J Psychiat Res 1975;12: Morris JC. The Clinical Dementia Rating (CDR): current version and scoring rules. Neurology 1993;43: American Psychiatric Association. Diagnostic and statistical manual of mental disorders, 4th ed. Washington, DC: American Psychiatric Association, McKhann G, Drachman D, Folstein M, et al. Clinical diagnosis of Alzheimer s disease: report of the NINCDS-RDA work group under the auspices of Department of Health and Human Services Task Force on Alzheimer s Disease. Neurology 1984;34: Kunik ME, Huffman JC, Bharani N, et al. Behavioural disturbances in geropsychiatric inpatients across dementia types. J Geriatr Psychiatry Neurol 2000;13: Lyketsos CG, Steinberg M, Tschanz JT, et al. Mental and behavioural disturbances in dementia: findings from the Cache county study on memory and aging. Am J Psychiatry 2000;157: Cummings JL, Miller B, Hill MA, et al. Neuropsychiatric aspects of multiinfarct dementia and dementia of the Alzheimer type. Arch Neurol 1987;44: Aharon-Peretz J, Masiah A, Pillar T, et al. Sleep-wake cycles in multi-infarct dementia and dementia of the Alzheimer type. Neurology 1991;41: Kuzis G, Sabe L, Tiberti C, et al. Neuropsychological correlates of apathy and depression in patients with dementia. Neurology 1999;52: Starkstein SE, Fedoroff JP, Price TR, et al. Apathy following cerebrovascular lesions. Stroke 1993;24: Cummings JL. Frontal subcortical circuits and human behavior. Arch Neurol 1993;50: Foster NL, Chase TN, Fedio P, et al. Alzheimer s disease: focal cortical changes shown by position emission tomography. Neurology 1983;33: Kertesz A, Clydesdale S. Neuropsychological deficits in vascular dementia vs. Alzheimer s disease. Arch Neurol 1994;51: Mega MS, Cummings JL, Fiorello T, et al. The spectrum of behavioral changes in Alzheimer s disease. Neurology 1996;46: Fuh JL, Liu CK, Mega MS, et al. Behavioral disorders and caregivers reaction in Taiwanese patients with Alzheimer s disease. Int Psychogeriatr 2001;13:121 8.
Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia
 86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
Neuropsychiatric symptoms in patients with vascular
 Research Article DOI: 10.1515/tnsci-2015-0015 Translational Neuroscience 6 2015 157-161 Translational Neuroscience Neuropsychiatric symptoms in patients with vascular dementia in mainland China Abstract
Research Article DOI: 10.1515/tnsci-2015-0015 Translational Neuroscience 6 2015 157-161 Translational Neuroscience Neuropsychiatric symptoms in patients with vascular dementia in mainland China Abstract
Behavioral and psychological symptoms of dementia characteristic of mild Alzheimer patients
 Blackwell Science, LtdOxford, UKPCNPsychiatry and Clinical Neurosciences1323-13162005 Blackwell Publishing Pty Ltd593274279Original ArticleDementia and mild AlzheimersJ. Shimabukuro et al. Psychiatry and
Blackwell Science, LtdOxford, UKPCNPsychiatry and Clinical Neurosciences1323-13162005 Blackwell Publishing Pty Ltd593274279Original ArticleDementia and mild AlzheimersJ. Shimabukuro et al. Psychiatry and
Research Article Behavioural and Psychological Symptoms in Poststroke Vascular Cognitive Impairment
 Behavioural Neurology, Article ID 430128, 5 pages http://dx.doi.org/10.1155/2014/430128 Research Article Behavioural and Psychological Symptoms in Poststroke Vascular Cognitive Impairment Meena Gupta,
Behavioural Neurology, Article ID 430128, 5 pages http://dx.doi.org/10.1155/2014/430128 Research Article Behavioural and Psychological Symptoms in Poststroke Vascular Cognitive Impairment Meena Gupta,
Psychiatric Morbidity in Dementia Patients in a Neurology-Based Memory Clinic
 Original Articles 179 Psychiatric Morbidity in Dementia Patients in a Neurology-Based Memory Clinic Ching-Sen Shih 1, Sui-Hing Yan 2, Ying-Hoo Ho 1, Yuh-Te Lin 1, Jie-Yuan Li 1, and Yuk-Keung Lo 1 Abstract-
Original Articles 179 Psychiatric Morbidity in Dementia Patients in a Neurology-Based Memory Clinic Ching-Sen Shih 1, Sui-Hing Yan 2, Ying-Hoo Ho 1, Yuh-Te Lin 1, Jie-Yuan Li 1, and Yuk-Keung Lo 1 Abstract-
The course of neuropsychiatric symptoms in dementia. Part II: relationships among behavioural sub-syndromes and the influence of clinical variables
 INTERNATIONAL JOURNAL OF GERIATRIC PSYCHIATRY Int J Geriatr Psychiatry 2005; 20: 531 536. Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/gps.1317 The course of neuropsychiatric
INTERNATIONAL JOURNAL OF GERIATRIC PSYCHIATRY Int J Geriatr Psychiatry 2005; 20: 531 536. Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/gps.1317 The course of neuropsychiatric
Estimating the Validity of the Korean Version of Expanded Clinical Dementia Rating (CDR) Scale
 Estimating the Validity of the Korean Version of Expanded Clinical Dementia Rating (CDR) Scale Seong Hye Choi, M.D.*, Duk L. Na, M.D., Byung Hwa Lee, M.A., Dong-Seog Hahm, M.D., Jee Hyang Jeong, M.D.,
Estimating the Validity of the Korean Version of Expanded Clinical Dementia Rating (CDR) Scale Seong Hye Choi, M.D.*, Duk L. Na, M.D., Byung Hwa Lee, M.A., Dong-Seog Hahm, M.D., Jee Hyang Jeong, M.D.,
Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias. Aaron H. Kaufman, MD
 Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, MD Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, M.D. Health Sciences
Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, MD Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, M.D. Health Sciences
Behavioral and Psychologic Symptoms in Different Types of Dementia
 ORIGINAL ARTICLE Behavioral and Psychologic Symptoms in Different Types of Dementia Ming-Jang Chiu,* Ta-Fu Chen, Ping-Keung Yip, Mau-Sun Hua, 1 Li-Yu Tang 2 Background/Purpose: Behavioral and psychologic
ORIGINAL ARTICLE Behavioral and Psychologic Symptoms in Different Types of Dementia Ming-Jang Chiu,* Ta-Fu Chen, Ping-Keung Yip, Mau-Sun Hua, 1 Li-Yu Tang 2 Background/Purpose: Behavioral and psychologic
Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia
 Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia Measure Description Percentage of patients with dementia for whom there was a documented screening* for behavioral
Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia Measure Description Percentage of patients with dementia for whom there was a documented screening* for behavioral
NEUROPSYCHOMETRIC TESTS
 NEUROPSYCHOMETRIC TESTS CAMCOG It is the Cognitive section of Cambridge Examination for Mental Disorders of the Elderly (CAMDEX) The measure assesses orientation, language, memory, praxis, attention, abstract
NEUROPSYCHOMETRIC TESTS CAMCOG It is the Cognitive section of Cambridge Examination for Mental Disorders of the Elderly (CAMDEX) The measure assesses orientation, language, memory, praxis, attention, abstract
Anosognosia, or loss of insight into one s cognitive
 REGULAR ARTICLES Anosognosia Is a Significant Predictor of Apathy in Alzheimer s Disease Sergio E. Starkstein, M.D., Ph.D. Simone Brockman, M.A. David Bruce, M.D. Gustavo Petracca, M.D. Anosognosia and
REGULAR ARTICLES Anosognosia Is a Significant Predictor of Apathy in Alzheimer s Disease Sergio E. Starkstein, M.D., Ph.D. Simone Brockman, M.A. David Bruce, M.D. Gustavo Petracca, M.D. Anosognosia and
Reliability of the Brazilian Portuguese version of the Neuropsychiatric Inventory (NPI) for patients with Alzheimer s disease and their caregivers
 International Psychogeriatrics (2008), 20:2, 383 393 C 2007 International Psychogeriatric Association doi:10.1017/s1041610207006254 Printed in the United Kingdom Reliability of the Brazilian Portuguese
International Psychogeriatrics (2008), 20:2, 383 393 C 2007 International Psychogeriatric Association doi:10.1017/s1041610207006254 Printed in the United Kingdom Reliability of the Brazilian Portuguese
Probable Early-onset Alzheimer s Disease Diagnosed by Comprehensive Evaluation and Neuroimage Studies
 Case Report Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 1 2011 45 Probable Early-onset Alzheimer s Disease Diagnosed by Comprehensive Evaluation and Neuroimage Studies Sin-Yi Chen, M.D. 1, Yuan-Han
Case Report Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 1 2011 45 Probable Early-onset Alzheimer s Disease Diagnosed by Comprehensive Evaluation and Neuroimage Studies Sin-Yi Chen, M.D. 1, Yuan-Han
CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE
 CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE 5.1 GENERAL BACKGROUND Neuropsychological assessment plays a crucial role in the assessment of cognitive decline in older age. In India, there
CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE 5.1 GENERAL BACKGROUND Neuropsychological assessment plays a crucial role in the assessment of cognitive decline in older age. In India, there
Range of neuropsychiatric disturbances in patients with Parkinson s disease
 492 Section of Geriatric Psychiatry, Rogaland Psychiatric Hospital D Aarsland N G Lim C Janvin Department of Neurology, Central Hospital of Rogaland, Stavanger, Norway J P Larsen K Karlsen E Tandberg Departments
492 Section of Geriatric Psychiatry, Rogaland Psychiatric Hospital D Aarsland N G Lim C Janvin Department of Neurology, Central Hospital of Rogaland, Stavanger, Norway J P Larsen K Karlsen E Tandberg Departments
Severity and prevalence of behavioral and psychological symptoms among patients of different dementia stages in Taiwan
 Original article Severity and prevalence of behavioral and psychological symptoms among patients of different dementia stages in Taiwan Si-Sheng Huang 1, Wen-Fu Wang 2, Yi-Cheng Liao 1 1 Department of
Original article Severity and prevalence of behavioral and psychological symptoms among patients of different dementia stages in Taiwan Si-Sheng Huang 1, Wen-Fu Wang 2, Yi-Cheng Liao 1 1 Department of
Clinical Diagnosis. Step 1: Dementia or not? Diagnostic criteria for dementia (DSM-IV)
 Step 1: Dementia or not? Diagnostic criteria for dementia (DSM-IV) A. The development of multiple cognitive deficits manifested by both 1 and 2 1 1. Memory impairment 2. One (or more) of the following
Step 1: Dementia or not? Diagnostic criteria for dementia (DSM-IV) A. The development of multiple cognitive deficits manifested by both 1 and 2 1 1. Memory impairment 2. One (or more) of the following
Effect of neuropsychiatric symptoms of Alzheimer's disease on Chinese and American caregivers
 INTERNATIONAL JOURNAL OF GERIATRIC PSYCHIATRY Int J Geriatr Psychiatry 2002; 17: 29±34. DOI: 10.1002/gps.510 Effect of neuropsychiatric symptoms of Alzheimer's disease on Chinese and American caregivers
INTERNATIONAL JOURNAL OF GERIATRIC PSYCHIATRY Int J Geriatr Psychiatry 2002; 17: 29±34. DOI: 10.1002/gps.510 Effect of neuropsychiatric symptoms of Alzheimer's disease on Chinese and American caregivers
Validation of apathy evaluation scale and assessment of severity of apathy in Alzheimer s diseasepcn_
 Psychiatry and Clinical Neurosciences 2012; 66: 227 234 doi:10.1111/j.1440-1819.2011.02315.x Regular Article Validation of apathy evaluation scale and assessment of severity of apathy in Alzheimer s diseasepcn_2315
Psychiatry and Clinical Neurosciences 2012; 66: 227 234 doi:10.1111/j.1440-1819.2011.02315.x Regular Article Validation of apathy evaluation scale and assessment of severity of apathy in Alzheimer s diseasepcn_2315
DEMENTIA WITH LEWY bodies (DLB) is the
 Psychiatry and Clinical Neurosciences 2017; 71: 409 416 doi:10.1111/pcn.12511 Regular Article Association of premorbid personality with behavioral and psychological symptoms in dementia with Lewy bodies:
Psychiatry and Clinical Neurosciences 2017; 71: 409 416 doi:10.1111/pcn.12511 Regular Article Association of premorbid personality with behavioral and psychological symptoms in dementia with Lewy bodies:
Non Alzheimer Dementias
 Non Alzheimer Dementias Randolph B Schiffer Department of Neuropsychiatry and Behavioral Science Texas Tech University Health Sciences Center 9/11/2007 Statement of Financial Disclosure Randolph B Schiffer,,
Non Alzheimer Dementias Randolph B Schiffer Department of Neuropsychiatry and Behavioral Science Texas Tech University Health Sciences Center 9/11/2007 Statement of Financial Disclosure Randolph B Schiffer,,
Neuropsychiatric Inventory Nursing Home Version (NPI-NH)
 This is a Sample version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) The full version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) comes without sample watermark..
This is a Sample version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) The full version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) comes without sample watermark..
Management of the Acutely Agitated Long Term Care Patient
 Management of the Acutely Agitated Long Term Care Patient 80 60 Graying of the Population US Population Over Age 65 Millions of Persons 40 20 0 1900 1920 1940 1960 1980 1990 2010 2030 Year Defining Dementia
Management of the Acutely Agitated Long Term Care Patient 80 60 Graying of the Population US Population Over Age 65 Millions of Persons 40 20 0 1900 1920 1940 1960 1980 1990 2010 2030 Year Defining Dementia
The place for treatments of associated neuropsychiatric and other symptoms
 The place for treatments of associated neuropsychiatric and other symptoms Luca Pani dg@aifa.gov.it London, 25 th November 2014 Workshop on Alzheimer s Disease European Medicines Agency London, UK Public
The place for treatments of associated neuropsychiatric and other symptoms Luca Pani dg@aifa.gov.it London, 25 th November 2014 Workshop on Alzheimer s Disease European Medicines Agency London, UK Public
Behavioral and Psychological Symptoms of Dementia
 Behavioral and Psychological Symptoms of Dementia Akarachaid Pinidbunjerdkool MD*, Sansanee Saengwanitch MD*, Pasiri Sithinamsuwan MD* * Division of Neurology, Department of Medicine, Phramongkutklao Hospital
Behavioral and Psychological Symptoms of Dementia Akarachaid Pinidbunjerdkool MD*, Sansanee Saengwanitch MD*, Pasiri Sithinamsuwan MD* * Division of Neurology, Department of Medicine, Phramongkutklao Hospital
Cognitive Abilities Screening Instrument, Chinese Version 2.0 (CASI C-2.0): Administration and Clinical Application
 Continuing Medical Education 180 Cognitive Abilities Screening Instrument, Chinese Version 2.0 (CASI C-2.0): Administration and Clinical Application Ker-Neng Lin 1,2, Pei-Ning Wang 1,3, Hsiu-Chih Liu 1,3,
Continuing Medical Education 180 Cognitive Abilities Screening Instrument, Chinese Version 2.0 (CASI C-2.0): Administration and Clinical Application Ker-Neng Lin 1,2, Pei-Ning Wang 1,3, Hsiu-Chih Liu 1,3,
BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA
 BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA Unmet needs What might be your behavioural response to this experience? Content Definition What are BPSD? Prevalence How common are they? Aetiological
BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA Unmet needs What might be your behavioural response to this experience? Content Definition What are BPSD? Prevalence How common are they? Aetiological
ORIGINAL CONTRIBUTION. The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease
 ORIGINAL CONTRIBUTION The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease Michael S. Mega, MD, PhD; Donna M. Masterman, MD; Susan M. O Connor, RNC; Terry R. Barclay,
ORIGINAL CONTRIBUTION The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease Michael S. Mega, MD, PhD; Donna M. Masterman, MD; Susan M. O Connor, RNC; Terry R. Barclay,
Development of a Short Version of the Apathy Evaluation Scale Specifically Adapted for Demented Nursing Home Residents
 Development of a Short Version of the Apathy Evaluation Scale Specifically Adapted for Demented Nursing Home Residents Ulrike Lueken, Ph.D., Ulrich Seidl, M.D., Lena Völker, Cand.Med., Elisabeth Schweiger,
Development of a Short Version of the Apathy Evaluation Scale Specifically Adapted for Demented Nursing Home Residents Ulrike Lueken, Ph.D., Ulrich Seidl, M.D., Lena Völker, Cand.Med., Elisabeth Schweiger,
Mild Cognitive Impairment (MCI)
 October 19, 2018 Mild Cognitive Impairment (MCI) Yonas E. Geda, MD, MSc Professor of Neurology and Psychiatry Consultant, Departments of Psychiatry & Psychology, and Neurology Mayo Clinic College of Medicine
October 19, 2018 Mild Cognitive Impairment (MCI) Yonas E. Geda, MD, MSc Professor of Neurology and Psychiatry Consultant, Departments of Psychiatry & Psychology, and Neurology Mayo Clinic College of Medicine
NEXT-Link DEMENTIA. A network of Danish memory clinics YOUR CLINICAL RESEARCH PARTNER WITHIN ALZHEIMER S DISEASE AND OTHER DEMENTIA DISEASES.
 NEXT-Link DEMENTIA A network of Danish memory clinics YOUR CLINICAL RESEARCH PARTNER WITHIN ALZHEIMER S DISEASE AND OTHER DEMENTIA DISEASES. NEXT-Link DEMENTIA NEXT-Link DEMENTIA is a network of Danish
NEXT-Link DEMENTIA A network of Danish memory clinics YOUR CLINICAL RESEARCH PARTNER WITHIN ALZHEIMER S DISEASE AND OTHER DEMENTIA DISEASES. NEXT-Link DEMENTIA NEXT-Link DEMENTIA is a network of Danish
Comment on administration and scoring of the Neuropsychiatric Inventory in clinical trials
 Alzheimer s & Dementia 4 (2008) 390 394 Comment on administration and scoring of the Neuropsychiatric Inventory in clinical trials Donald J. Connor a, *, Marwan N. Sabbagh a, Jeffery L. Cummings b a Cleo
Alzheimer s & Dementia 4 (2008) 390 394 Comment on administration and scoring of the Neuropsychiatric Inventory in clinical trials Donald J. Connor a, *, Marwan N. Sabbagh a, Jeffery L. Cummings b a Cleo
A wide range of neuropsychiatric disturbances commonly
 36 PAPER Neuropsychiatric symptoms in patients with Parkinson s disease and dementia: frequency, profile and associated care giver stress D Aarsland, K Brønnick, U Ehrt, P P De Deyn, S Tekin, M Emre, J
36 PAPER Neuropsychiatric symptoms in patients with Parkinson s disease and dementia: frequency, profile and associated care giver stress D Aarsland, K Brønnick, U Ehrt, P P De Deyn, S Tekin, M Emre, J
WHAT IS DEMENTIA? An acquired syndrome of decline in memory and other cognitive functions sufficient to affect daily life in an alert patient
 DEMENTIA WHAT IS DEMENTIA? An acquired syndrome of decline in memory and other cognitive functions sufficient to affect daily life in an alert patient Progressive and disabling Not an inherent aspect of
DEMENTIA WHAT IS DEMENTIA? An acquired syndrome of decline in memory and other cognitive functions sufficient to affect daily life in an alert patient Progressive and disabling Not an inherent aspect of
Mental and Behavioral Disturbances in Dementia: Findings from the Cache County Study on Memory in Aging
 Utah State University DigitalCommons@USU Psychology Faculty Publications Psychology 2000 Mental and Behavioral Disturbances in : Findings from the Cache County Study on Memory in Aging Constantine G. Lyketsos
Utah State University DigitalCommons@USU Psychology Faculty Publications Psychology 2000 Mental and Behavioral Disturbances in : Findings from the Cache County Study on Memory in Aging Constantine G. Lyketsos
The Reliability and Validity of the Korean Instrumental Activities of Daily Living (K-IADL)
 The Reliability and Validity of the Korean Instrumental Activities of Daily Living (K-IADL Sue J. Kang, M.S., Seong Hye Choi, M.D.*, Byung H. Lee, M.A., Jay C. Kwon, M.D., Duk L. Na, M.D., Seol-Heui Han
The Reliability and Validity of the Korean Instrumental Activities of Daily Living (K-IADL Sue J. Kang, M.S., Seong Hye Choi, M.D.*, Byung H. Lee, M.A., Jay C. Kwon, M.D., Duk L. Na, M.D., Seol-Heui Han
9/24/2012. Amer M Burhan, MBChB, FRCP(C)
 Depression and Dementia Amer M Burhan MBChB, FRCPC Head of CAMH Memory Clinic, Toronto Geriatric Neuropsychiatrist Assistant Prof Psychiatry at U of T Objectives Discuss the prevalence and impact of depression
Depression and Dementia Amer M Burhan MBChB, FRCPC Head of CAMH Memory Clinic, Toronto Geriatric Neuropsychiatrist Assistant Prof Psychiatry at U of T Objectives Discuss the prevalence and impact of depression
Neuropsychiatric symptoms in 921 elderly subjects with dementia: a comparison between vascular and neurodegenerative types
 Acta Psychiatr Scand 2008: 117: 455 464 All rights reserved DOI: 10.1111/j.1600-0447.2008.01175.x Copyright Ó 2008 The Authors Journal Compilation Ó 2008 Blackwell Munksgaard ACTA PSYCHIATRICA SCANDINAVICA
Acta Psychiatr Scand 2008: 117: 455 464 All rights reserved DOI: 10.1111/j.1600-0447.2008.01175.x Copyright Ó 2008 The Authors Journal Compilation Ó 2008 Blackwell Munksgaard ACTA PSYCHIATRICA SCANDINAVICA
City, University of London Institutional Repository
 City Research Online City, University of London Institutional Repository Citation: Hurt, C. S., Banerjee, S., Tunnard, C., Whitehead, D. L., Tsolaki, M., Mecocci, P., Kloszewska, I., Soininen, H., Vellas,
City Research Online City, University of London Institutional Repository Citation: Hurt, C. S., Banerjee, S., Tunnard, C., Whitehead, D. L., Tsolaki, M., Mecocci, P., Kloszewska, I., Soininen, H., Vellas,
ALZHEIMER DISEASE (AD) AFfects
 ORIGINAL CONTRIBUTION Executive Dysfunction in Alzheimer Disease Margaret M. Swanberg, DO; Rochelle E. Tractenberg, PhD, MPH; Richard Mohs, PhD; Leon J. Thal, MD; Jeffrey L. Cummings, MD Background: Executive
ORIGINAL CONTRIBUTION Executive Dysfunction in Alzheimer Disease Margaret M. Swanberg, DO; Rochelle E. Tractenberg, PhD, MPH; Richard Mohs, PhD; Leon J. Thal, MD; Jeffrey L. Cummings, MD Background: Executive
NeuroPharmac Journal ISSN: Alzheimer s Disease: Pharmacotherapy of noncognitive symptoms Aslam Pathan; Abdulrahman M.
 ISSNISSN ISSN: 2456-3927 NeuroPharmac Journal Alzheimer s Disease: Pharmacotherapy of noncognitive symptoms Aslam Pathan; Abdulrahman M. Alshahrani www. neuropharmac.com Jan-April 2018, Volume 3, Issue
ISSNISSN ISSN: 2456-3927 NeuroPharmac Journal Alzheimer s Disease: Pharmacotherapy of noncognitive symptoms Aslam Pathan; Abdulrahman M. Alshahrani www. neuropharmac.com Jan-April 2018, Volume 3, Issue
White matter hyperintensities correlate with neuropsychiatric manifestations of Alzheimer s disease and frontotemporal lobar degeneration
 White matter hyperintensities correlate with neuropsychiatric manifestations of Alzheimer s disease and frontotemporal lobar degeneration Annual Scientific Meeting Canadian Geriatric Society Philippe Desmarais,
White matter hyperintensities correlate with neuropsychiatric manifestations of Alzheimer s disease and frontotemporal lobar degeneration Annual Scientific Meeting Canadian Geriatric Society Philippe Desmarais,
T he concept of vascular cognitive covers a
 28 PAPER Cognitive profile of subcortical ischaemic vascular disease H Jokinen, H Kalska, R Mäntylä, T Pohjasvaara, R Ylikoski, M Hietanen, O Salonen, M Kaste, T Erkinjuntti... J Neurol Neurosurg Psychiatry
28 PAPER Cognitive profile of subcortical ischaemic vascular disease H Jokinen, H Kalska, R Mäntylä, T Pohjasvaara, R Ylikoski, M Hietanen, O Salonen, M Kaste, T Erkinjuntti... J Neurol Neurosurg Psychiatry
IT IS WELL known that individuals with dementia. Classifying eating-related problems among institutionalized people with dementia.
 doi:10.1111/pcn.12375 Regular Article Classifying eating-related problems among institutionalized people with dementia Shunichiro Shinagawa, MD, PhD, 1 * Kazuki Honda, MD, PhD, 2 Tetsuo Kashibayashi, MD,
doi:10.1111/pcn.12375 Regular Article Classifying eating-related problems among institutionalized people with dementia Shunichiro Shinagawa, MD, PhD, 1 * Kazuki Honda, MD, PhD, 2 Tetsuo Kashibayashi, MD,
Acetylcholinesterase inhibitors: donepezil, rivastigmine, tacrine or galantamine for non-alzheimer s dementia
 STEER 2002; Vol 2: No.2 Acetylcholinesterase inhibitors: donepezil, rivastigmine, tacrine or galantamine for non-alzheimer s dementia Bunmi Fajemisin Evidence search date: November 2001 www.signpoststeer.org
STEER 2002; Vol 2: No.2 Acetylcholinesterase inhibitors: donepezil, rivastigmine, tacrine or galantamine for non-alzheimer s dementia Bunmi Fajemisin Evidence search date: November 2001 www.signpoststeer.org
PREVALENCE AND CORRELATES OF ANXIETY IN ALZHEIMER S DISEASE
 166 Chemerinski et al. DEPRESSION AND ANXIETY 7:166 170 (1998) PREVALENCE AND CORRELATES OF ANXIETY IN ALZHEIMER S DISEASE Erán Chemerinski, M.D., 1 * Gustavo Petracca, M.D., 1 Facundo Manes, M.D., 2 Ramón
166 Chemerinski et al. DEPRESSION AND ANXIETY 7:166 170 (1998) PREVALENCE AND CORRELATES OF ANXIETY IN ALZHEIMER S DISEASE Erán Chemerinski, M.D., 1 * Gustavo Petracca, M.D., 1 Facundo Manes, M.D., 2 Ramón
A Neuropsychiatric, Neuroradiological, and Neuropsychological Profile of a Cohort of Patients with Vascular Dementia
 A Neuropsychiatric, Neuroradiological, and Neuropsychological Profile of a Cohort of Patients with Vascular Dementia Moises Gaviria, MD University of Illinois at Chicago Advocate Christ Medical Center
A Neuropsychiatric, Neuroradiological, and Neuropsychological Profile of a Cohort of Patients with Vascular Dementia Moises Gaviria, MD University of Illinois at Chicago Advocate Christ Medical Center
Alzheimer's Disease An update on diagnostic criteria & Neuropsychiatric symptoms. l The diagnosis of AD l Neuropsychiatric symptoms l Place of the ICT
 Alzheimer's Disease An update on diagnostic criteria & Neuropsychiatric symptoms State of the art lecture March 4-2012 Philippe H Robert, Philippe Nice - France Robert The diagnosis of AD Neuropsychiatric
Alzheimer's Disease An update on diagnostic criteria & Neuropsychiatric symptoms State of the art lecture March 4-2012 Philippe H Robert, Philippe Nice - France Robert The diagnosis of AD Neuropsychiatric
Baseline Characteristics of Patients Attending the Memory Clinic Serving the South Shore of Boston
 Article ID: ISSN 2046-1690 Baseline Characteristics of Patients Attending the www.thealzcenter.org Memory Clinic Serving the South Shore of Boston Corresponding Author: Dr. Anil K Nair, Chief of Neurology,
Article ID: ISSN 2046-1690 Baseline Characteristics of Patients Attending the www.thealzcenter.org Memory Clinic Serving the South Shore of Boston Corresponding Author: Dr. Anil K Nair, Chief of Neurology,
Brain imaging for the diagnosis of people with suspected dementia
 Why do we undertake brain imaging in dementia? Brain imaging for the diagnosis of people with suspected dementia Not just because guidelines tell us to! Exclude other causes for dementia Help confirm diagnosis
Why do we undertake brain imaging in dementia? Brain imaging for the diagnosis of people with suspected dementia Not just because guidelines tell us to! Exclude other causes for dementia Help confirm diagnosis
Responsiveness of the QUALID to Improved Neuropsychiatric Symptoms in Patients with Alzheimer s Disease
 ORIGINAL RESEARCH Responsiveness of the QUALID to Improved Neuropsychiatric Symptoms in Patients with Alzheimer s Disease Hadas Benhabib 1, Krista L. Lanctôt, PhD 1,2,4, Goran M. Eryavec, MD, FRCPC 3,4,
ORIGINAL RESEARCH Responsiveness of the QUALID to Improved Neuropsychiatric Symptoms in Patients with Alzheimer s Disease Hadas Benhabib 1, Krista L. Lanctôt, PhD 1,2,4, Goran M. Eryavec, MD, FRCPC 3,4,
Number of Items. Response Categories. Part V: Specific Behavior Scales-Sleep Scales. Based on past month
 Part V: Specific Behavior Scales-Sleep Scales Based on past month First 4 items ask for time or amount of sleep 41. Pittsburgh Sleep Quality Index (PSQI) Sleep quality Sleep latency Sleep duration Habitual
Part V: Specific Behavior Scales-Sleep Scales Based on past month First 4 items ask for time or amount of sleep 41. Pittsburgh Sleep Quality Index (PSQI) Sleep quality Sleep latency Sleep duration Habitual
The Neuropsychiatric Inventory Questionnaire: Background and Administration
 The Neuropsychiatric Inventory Questionnaire: Background and Administration The Neuropsychiatric Inventory Questionnaire (NPI-Q) was developed and crossvalidated with the standard NPI to provide a brief
The Neuropsychiatric Inventory Questionnaire: Background and Administration The Neuropsychiatric Inventory Questionnaire (NPI-Q) was developed and crossvalidated with the standard NPI to provide a brief
Clinical Characteristics of Behavioral and Psychological Symptoms in Patients with Drug-naïve Alzheimer s Disease
 Dementia and Neurocognitive Disorders 2012; 11: 87-94 ORIGINAL ARTICLE Clinical Characteristics of Behavioral and Psychological Symptoms in Patients with Drug-naïve Alzheimer s Disease Yong Tae Kwak, M.D.,
Dementia and Neurocognitive Disorders 2012; 11: 87-94 ORIGINAL ARTICLE Clinical Characteristics of Behavioral and Psychological Symptoms in Patients with Drug-naïve Alzheimer s Disease Yong Tae Kwak, M.D.,
The efficacy of Rivastigmine in the management of the behavioral and psychological symptoms of lewy body dementia- a review of literature
 Review article: The efficacy of Rivastigmine in the management of the behavioral and psychological symptoms of lewy body dementia- a review of literature Dr. Ivan Netto 1, Aditya Iyer 2, Dr. Prathamesh
Review article: The efficacy of Rivastigmine in the management of the behavioral and psychological symptoms of lewy body dementia- a review of literature Dr. Ivan Netto 1, Aditya Iyer 2, Dr. Prathamesh
Clinical Trial Designs for RCTs focussing on the Treatment of Agitation in people with Alzheimer s disease
 Clinical Trial Designs for RCTs focussing on the Treatment of Agitation in people with Alzheimer s disease Professor Clive Ballard Dr Byron Creese University of Exeter, UK Guardian guide for 2018: Top
Clinical Trial Designs for RCTs focussing on the Treatment of Agitation in people with Alzheimer s disease Professor Clive Ballard Dr Byron Creese University of Exeter, UK Guardian guide for 2018: Top
QUESTIONNAIRE: Finland
 QUESTIONNAIRE: Finland To put the assessment and management of behavioural disorders into a broader context of social and health policy and services in Finland, some background information is presented.
QUESTIONNAIRE: Finland To put the assessment and management of behavioural disorders into a broader context of social and health policy and services in Finland, some background information is presented.
Supplementary Online Content
 Supplementary Online Content Atri A, Frölich L, Ballard C, et al. Effect of idalopirdine as adjunct to cholinesterase inhibitors on in cognition in patients with Alzheimer disease: three randomized clinical
Supplementary Online Content Atri A, Frölich L, Ballard C, et al. Effect of idalopirdine as adjunct to cholinesterase inhibitors on in cognition in patients with Alzheimer disease: three randomized clinical
fine age at onset? And, once defined, how consistent is this clinical measure? Despite considerable research
 Clinical Characterization of Alzheimer s Disease: Reliability of Age at Onset and a New Descriptor, Age at Shift Gary W. Small, MD; David E. Kuhl, MD; Denson G. Fujikawa, MD; J. Wesson Ashford, MD, PhD
Clinical Characterization of Alzheimer s Disease: Reliability of Age at Onset and a New Descriptor, Age at Shift Gary W. Small, MD; David E. Kuhl, MD; Denson G. Fujikawa, MD; J. Wesson Ashford, MD, PhD
PRACTICAL NEUROLOGY. Reversible. dementias Blackwell Science Ltd
 138 PRACTICAL NEUROLOGY Reversible dementias JUNE 2002 139 Gunhild Waldemar Memory Disorders Research Unit, Department of Neurology, Rigshospitalet, Copenhagen University Hospital, 9 Blegdamsvej, DK-2100
138 PRACTICAL NEUROLOGY Reversible dementias JUNE 2002 139 Gunhild Waldemar Memory Disorders Research Unit, Department of Neurology, Rigshospitalet, Copenhagen University Hospital, 9 Blegdamsvej, DK-2100
University of Bristol - Explore Bristol Research
 Skrobot, O. A., O'Brien, J., Black, S., Chen, C., DeCarli, C., Erkinjuntti, T.,... Kehoe, P. G. (2016). The vascular impairment of cognition classification consensus study. Alzheimer's and Dementia. DOI:
Skrobot, O. A., O'Brien, J., Black, S., Chen, C., DeCarli, C., Erkinjuntti, T.,... Kehoe, P. G. (2016). The vascular impairment of cognition classification consensus study. Alzheimer's and Dementia. DOI:
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 diagnosis and assessment bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
diagnosis and assessment bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Dementia is a common neuropsychiatric disorder characterized by progressive impairment of
 Focused Issue of This Month Diagnosis and Treatment for Behavioral and Psychological Symptoms of Dementia Byoung Hoon Oh, MD Department of Psychiatry, Yonsei University College of Medicine E - mail : drobh@yuhs.ac
Focused Issue of This Month Diagnosis and Treatment for Behavioral and Psychological Symptoms of Dementia Byoung Hoon Oh, MD Department of Psychiatry, Yonsei University College of Medicine E - mail : drobh@yuhs.ac
A Fresh View of Cognitive Disorders in Older Adults: New Classification and Screening Strategies
 A Fresh View of Cognitive Disorders in Older Adults: New Classification and Screening Strategies Lynda Mackin, PhD, AGPCNP-BC, CNS University of California San Francisco School of Nursing 1 Alzheimer s
A Fresh View of Cognitive Disorders in Older Adults: New Classification and Screening Strategies Lynda Mackin, PhD, AGPCNP-BC, CNS University of California San Francisco School of Nursing 1 Alzheimer s
DEMENTIA MEASURES GROUP OVERVIEW
 DEMENTIA MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN DEMENTIA MEASURES GROUP: #47 Care Plan #280 Dementia: Staging of Dementia #281 Dementia: Cognitive Assessment
DEMENTIA MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN DEMENTIA MEASURES GROUP: #47 Care Plan #280 Dementia: Staging of Dementia #281 Dementia: Cognitive Assessment
ALZHEIMER S DISEASE. Mary-Letitia Timiras M.D. Overlook Hospital Summit, New Jersey
 ALZHEIMER S DISEASE Mary-Letitia Timiras M.D. Overlook Hospital Summit, New Jersey Topics Covered Demography Clinical manifestations Pathophysiology Diagnosis Treatment Future trends Prevalence and Impact
ALZHEIMER S DISEASE Mary-Letitia Timiras M.D. Overlook Hospital Summit, New Jersey Topics Covered Demography Clinical manifestations Pathophysiology Diagnosis Treatment Future trends Prevalence and Impact
T he prevalence of Parkinson s disease (PD) is nearly 1% in
 708 PAPER Donepezil for cognitive impairment in Parkinson s disease: a randomised controlled study D Aarsland, K Laake, J P Larsen, C Janvin... See end of article for authors affiliations... Correspondence
708 PAPER Donepezil for cognitive impairment in Parkinson s disease: a randomised controlled study D Aarsland, K Laake, J P Larsen, C Janvin... See end of article for authors affiliations... Correspondence
Parkinsonian Disorders with Dementia
 Parkinsonian Disorders with Dementia George Tadros Consultant in Old Age Liaison Psychiatry, RAID, Heartlands Hospital Professor of Dementia and Liaison Psychiatry, Aston Medical School Aston University
Parkinsonian Disorders with Dementia George Tadros Consultant in Old Age Liaison Psychiatry, RAID, Heartlands Hospital Professor of Dementia and Liaison Psychiatry, Aston Medical School Aston University
Vascular dementia as a frontal subcortical system dysfunction
 Psychological Medicine, 2000, 30, 997 1003. 2000 Cambridge University Press Printed in the United Kingdom EDITORIAL Vascular dementia as a frontal subcortical system dysfunction Vascular dementia (VaD)
Psychological Medicine, 2000, 30, 997 1003. 2000 Cambridge University Press Printed in the United Kingdom EDITORIAL Vascular dementia as a frontal subcortical system dysfunction Vascular dementia (VaD)
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #283: Dementia Associated Behavioral and Psychiatric Symptoms Screening and Management National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #283: Dementia Associated Behavioral and Psychiatric Symptoms Screening and Management National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Neuropsychiatric Syndromes
 Neuropsychiatric Syndromes Susan Czapiewski,MD VAHCS December 10, 2015 Dr. Czapiewski has indicated no potential conflict of interest to this presentation. She does intend to discuss the off-label use
Neuropsychiatric Syndromes Susan Czapiewski,MD VAHCS December 10, 2015 Dr. Czapiewski has indicated no potential conflict of interest to this presentation. She does intend to discuss the off-label use
Comparison of Different Clinical Criteria (DSM-III, ADDTC, ICD-10, NINDS-AIREN, DSM-IV) for the Diagnosis of Vascular Dementia
 Comparison of Different Clinical Criteria (DSM-III, ADDTC, ICD-10, NINDS-AIREN, DSM-IV) for the Diagnosis of Vascular Dementia T. Pohjasvaara, MD, PhD; R. Mäntylä, MD; R. Ylikoski, MA; M. Kaste, MD, PhD;
Comparison of Different Clinical Criteria (DSM-III, ADDTC, ICD-10, NINDS-AIREN, DSM-IV) for the Diagnosis of Vascular Dementia T. Pohjasvaara, MD, PhD; R. Mäntylä, MD; R. Ylikoski, MA; M. Kaste, MD, PhD;
F rontotemporal dementia (FTD) is the term currently used
 1398 PAPER A study of stereotypic behaviours in Alzheimer s disease and frontal and temporal variant frontotemporal dementia S Nyatsanza, T Shetty, C Gregory, S Lough, K Dawson, J R Hodges... See end of
1398 PAPER A study of stereotypic behaviours in Alzheimer s disease and frontal and temporal variant frontotemporal dementia S Nyatsanza, T Shetty, C Gregory, S Lough, K Dawson, J R Hodges... See end of
Awareness of Deficit in Alzheimer's Disease: Relation to Caregiver Burden 1
 Copyright 1997 by The Cerontological Society of America The Cerontologist Vol.37, No. 1,20-24 Patients with Alzheimer's disease (AD) show varying degrees of awareness of their deficits. To examine the
Copyright 1997 by The Cerontological Society of America The Cerontologist Vol.37, No. 1,20-24 Patients with Alzheimer's disease (AD) show varying degrees of awareness of their deficits. To examine the
Clinical Manifestations of Neuropsychiatric Disorders
 Clinical Manifestations of Neuropsychiatric Disorders Koho Miyoshi and Yasushi Morimura Abstract Cerebral disorders commonly cause psychiatric symptoms. It is recommended to call psychiatric symptoms or
Clinical Manifestations of Neuropsychiatric Disorders Koho Miyoshi and Yasushi Morimura Abstract Cerebral disorders commonly cause psychiatric symptoms. It is recommended to call psychiatric symptoms or
NIH Public Access Author Manuscript Metab Brain Dis. Author manuscript; available in PMC 2011 October 24.
 NIH Public Access Author Manuscript Published in final edited form as: Metab Brain Dis. 2006 September ; 21(2-3): 235 240. doi:10.1007/s11011-006-9017-2. Risk factors for incident Alzheimer s disease in
NIH Public Access Author Manuscript Published in final edited form as: Metab Brain Dis. 2006 September ; 21(2-3): 235 240. doi:10.1007/s11011-006-9017-2. Risk factors for incident Alzheimer s disease in
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a preprint version which may differ from the publisher's version. For additional information about this
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a preprint version which may differ from the publisher's version. For additional information about this
Original Articles. Calne, resting tremor. Mortimer, Pirozzolo, Hansch, & Webster, postural disturbance III
 2004 97-106 Original Articles 1 2 3 1 1 2 3 47 22 III I II muscular rigidity postural disturbance resting tremor bradykinesia Calne, 2001 Mortimer, Pirozzolo, Hansch, & Webster, 1982 Tel: 02-23627076 E-mail:
2004 97-106 Original Articles 1 2 3 1 1 2 3 47 22 III I II muscular rigidity postural disturbance resting tremor bradykinesia Calne, 2001 Mortimer, Pirozzolo, Hansch, & Webster, 1982 Tel: 02-23627076 E-mail:
Missing Data Analysis in Drug-Naïve Alzheimer s Disease with Behavioral and Psychological Symptoms
 Original Article http://dx.doi.org/10.3349/ymj.2013.54.4.825 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(4):825-831, 2013 Missing Data Analysis in Drug-Naïve Alzheimer s Disease with Behavioral
Original Article http://dx.doi.org/10.3349/ymj.2013.54.4.825 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(4):825-831, 2013 Missing Data Analysis in Drug-Naïve Alzheimer s Disease with Behavioral
Introduction, use of imaging and current guidelines. John O Brien Professor of Old Age Psychiatry University of Cambridge
 Introduction, use of imaging and current guidelines John O Brien Professor of Old Age Psychiatry University of Cambridge Why do we undertake brain imaging in AD and other dementias? Exclude other causes
Introduction, use of imaging and current guidelines John O Brien Professor of Old Age Psychiatry University of Cambridge Why do we undertake brain imaging in AD and other dementias? Exclude other causes
DEMENTIA MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: DEMENTIA MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DEMENTIA MEASURES GROUP: #280. Dementia: Staging of Dementia #281. Dementia: Cognitive Assessment #282. Dementia:
2014 PQRS OPTIONS F MEASURES GROUPS: DEMENTIA MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DEMENTIA MEASURES GROUP: #280. Dementia: Staging of Dementia #281. Dementia: Cognitive Assessment #282. Dementia:
CLUSTERING OF BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA (BPSD): A EUROPEAN ALZHEIMER S DISEASE IN CONSORTIUM (EADC) STUDY
 426 Original articles CLUSTERING OF BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA (BPSD): A EUROPEAN ALZHEIMER S DISEASE IN CONSORTIUM (EADC) STUDY M. Petrovic 1,2, C. Hurt 2, D. Collins 2, A. Burns
426 Original articles CLUSTERING OF BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA (BPSD): A EUROPEAN ALZHEIMER S DISEASE IN CONSORTIUM (EADC) STUDY M. Petrovic 1,2, C. Hurt 2, D. Collins 2, A. Burns
Hallucinations, delusions, and cognitive decline in Alzheimer s disease
 172 Department of Neurological Sciences, Rush Alzheimer s Disease Center and Rush Institute for Healthy Aging, 1645 West Jackson Boulevard, Suite 675, Chicago, Illinois 60612, USA R S Wilson D W Gilley
172 Department of Neurological Sciences, Rush Alzheimer s Disease Center and Rush Institute for Healthy Aging, 1645 West Jackson Boulevard, Suite 675, Chicago, Illinois 60612, USA R S Wilson D W Gilley
P20.2. Characteristics of different types of dementia and challenges for the clinician
 P20.2. Characteristics of different types of dementia and challenges for the clinician, professor Danish Dementia Research Center Rigshospitalet, University of Copenhagen (Denmark) This project has received
P20.2. Characteristics of different types of dementia and challenges for the clinician, professor Danish Dementia Research Center Rigshospitalet, University of Copenhagen (Denmark) This project has received
Research Article Sex Differences in Neuropsychiatric Symptoms of Alzheimer s Disease: The Modifying Effect of Apolipoprotein E ε4 Status
 Behavioural Neurology Volume 2015, Article ID 275256, 6 pages http://dx.doi.org/10.1155/2015/275256 Research Article Sex Differences in Neuropsychiatric Symptoms of Alzheimer s Disease: The Modifying Effect
Behavioural Neurology Volume 2015, Article ID 275256, 6 pages http://dx.doi.org/10.1155/2015/275256 Research Article Sex Differences in Neuropsychiatric Symptoms of Alzheimer s Disease: The Modifying Effect
ORIGINAL CONTRIBUTION. Diagnostic Validity of the Dementia Questionnaire for Alzheimer Disease
 ORIGINAL CONTRIBUTION Diagnostic Validity of the Dementia Questionnaire for Alzheimer Disease Ronald J. Ellis, MD, PhD; Kaining Jan, MD; Claudia Kawas, MD; William C. Koller, MD; Kelly E. Lyons, PhD; Dilip
ORIGINAL CONTRIBUTION Diagnostic Validity of the Dementia Questionnaire for Alzheimer Disease Ronald J. Ellis, MD, PhD; Kaining Jan, MD; Claudia Kawas, MD; William C. Koller, MD; Kelly E. Lyons, PhD; Dilip
OLD AGE PSYCHIATRY. Dementia definition TYPES OF DEMENTIA. Other causes. Psychiatric disorders of the elderly. Dementia.
 Psychiatric disorders of the elderly OLD AGE PSYCHIATRY Dementia Depression Delusional disorder/late onset schizophrenia Delirium Dementia definition LOCALISATION OF CEREBRAL FUNCTION Impairment of multiple
Psychiatric disorders of the elderly OLD AGE PSYCHIATRY Dementia Depression Delusional disorder/late onset schizophrenia Delirium Dementia definition LOCALISATION OF CEREBRAL FUNCTION Impairment of multiple
Ian McKeith MD, F Med Sci, Professor of Old Age Psychiatry, Newcastle University
 Ian McKeith MD, F Med Sci, Professor of Old Age Psychiatry, Newcastle University Design of trials in DLB and PDD What has been learnt from previous trials in these indications and other dementias? Overview
Ian McKeith MD, F Med Sci, Professor of Old Age Psychiatry, Newcastle University Design of trials in DLB and PDD What has been learnt from previous trials in these indications and other dementias? Overview
Cognitive disorders. Dr S. Mashaphu Department of Psychiatry
 Cognitive disorders Dr S. Mashaphu Department of Psychiatry Delirium Syndrome characterised by: Disturbance of consciousness Impaired attention Change in cognition Develops over hours-days Fluctuates during
Cognitive disorders Dr S. Mashaphu Department of Psychiatry Delirium Syndrome characterised by: Disturbance of consciousness Impaired attention Change in cognition Develops over hours-days Fluctuates during
September 26 28, 2013 Westin Tampa Harbour Island. Co-sponsored by
 September 26 28, 2013 Westin Tampa Harbour Island Co-sponsored by From Brains at Risk to Cognitive Dysfunction: The Role of Vascular Pathology Ralph Sacco, MD, MS, FAHA, FAAN Miller School of Medicine
September 26 28, 2013 Westin Tampa Harbour Island Co-sponsored by From Brains at Risk to Cognitive Dysfunction: The Role of Vascular Pathology Ralph Sacco, MD, MS, FAHA, FAAN Miller School of Medicine
Positron Emission Tomography Metabolic Correlates of Apathy in Alzheimer Disease
 ORIGINAL CONTRIBUTION Positron Emission Tomography Metabolic Correlates of Apathy in Alzheimer Disease Gad A. Marshall, MD; Lorena Monserratt, MA; Dylan Harwood, PhD; Mark Mandelkern, MD, PhD; Jeffrey
ORIGINAL CONTRIBUTION Positron Emission Tomography Metabolic Correlates of Apathy in Alzheimer Disease Gad A. Marshall, MD; Lorena Monserratt, MA; Dylan Harwood, PhD; Mark Mandelkern, MD, PhD; Jeffrey
UDS Progress Report. -Standardization and Training Meeting 11/18/05, Chicago. -Data Managers Meeting 1/20/06, Chicago
 UDS Progress Report -Standardization and Training Meeting 11/18/05, Chicago -Data Managers Meeting 1/20/06, Chicago -Training material available: Gold standard UDS informant and participant interviews
UDS Progress Report -Standardization and Training Meeting 11/18/05, Chicago -Data Managers Meeting 1/20/06, Chicago -Training material available: Gold standard UDS informant and participant interviews
Is PET/CT really helpful in diagnosing Alzheimer s Disease?
 Is PET/CT really helpful in diagnosing Alzheimer s Disease? J. Rudolf MD Ph.D. Consultant in Neurology, Dept. of Neurology, General Hospital Papageorgiou Thessaloniki, Greece Conflict of Interest PET/CT
Is PET/CT really helpful in diagnosing Alzheimer s Disease? J. Rudolf MD Ph.D. Consultant in Neurology, Dept. of Neurology, General Hospital Papageorgiou Thessaloniki, Greece Conflict of Interest PET/CT
Form D1: Clinician Diagnosis
 Initial Visit Packet Form D: Clinician Diagnosis NACC Uniform Data Set (UDS) ADC name: Subject ID: Form date: / / Visit #: Examiner s initials: INSTRUCTIONS: This form is to be completed by the clinician.
Initial Visit Packet Form D: Clinician Diagnosis NACC Uniform Data Set (UDS) ADC name: Subject ID: Form date: / / Visit #: Examiner s initials: INSTRUCTIONS: This form is to be completed by the clinician.
Dementia: How to explain the diagnosis to patients and relatives
 GPHot Topics (April 2017): Dementia: How to explain the diagnosis to patients and relatives mohammad somauroo Consultant Physician with specialist interest in Community Geriatrics Royal Liverpool and Broadgreen
GPHot Topics (April 2017): Dementia: How to explain the diagnosis to patients and relatives mohammad somauroo Consultant Physician with specialist interest in Community Geriatrics Royal Liverpool and Broadgreen
Vascular Dementia. Laura Pedelty, PhD MD The University of Illinois at Chicago and Jesse Brown VA Medical Center
 Vascular Dementia Laura Pedelty, PhD MD The University of Illinois at Chicago and Jesse Brown VA Medical Center none Disclosures Objectives To review the definition of Vascular Cognitive Impairment (VCI);
Vascular Dementia Laura Pedelty, PhD MD The University of Illinois at Chicago and Jesse Brown VA Medical Center none Disclosures Objectives To review the definition of Vascular Cognitive Impairment (VCI);
Behavioural Problems and Patterns of Psychopharmacological Treatment given in Elderly Patients with Dementia
 The International Journal of Indian Psychology ISSN 2348-5396 (e) ISSN: 2349-3429 (p) Volume 6, Issue 4, DIP: 18.01.090/20180604 DOI: 10.25215/0604.090 http://www.ijip.in October-December, 2018 Research
The International Journal of Indian Psychology ISSN 2348-5396 (e) ISSN: 2349-3429 (p) Volume 6, Issue 4, DIP: 18.01.090/20180604 DOI: 10.25215/0604.090 http://www.ijip.in October-December, 2018 Research
Post Stroke Cognitive Decline
 Post Stroke Cognitive Decline Deborah A. Levine, MD, MPH Departments of Medicine & Neurology University of Michigan deblevin@umich.edu Presenter Disclosure Information Deborah A. Levine, MD, MPH Post Stroke
Post Stroke Cognitive Decline Deborah A. Levine, MD, MPH Departments of Medicine & Neurology University of Michigan deblevin@umich.edu Presenter Disclosure Information Deborah A. Levine, MD, MPH Post Stroke
Recent publications using the NACC Database. Lilah Besser
 Recent publications using the NACC Database Lilah Besser Data requests and publications Using NACC data Number of requests by year Type 2009 2010 2011 2012 2013 2014 2015 Data files* 55 85 217 174 204
Recent publications using the NACC Database Lilah Besser Data requests and publications Using NACC data Number of requests by year Type 2009 2010 2011 2012 2013 2014 2015 Data files* 55 85 217 174 204
