MUSCULOSKELETAL AND NEUROLOGICAL DISORDERS
|
|
|
- Garey Ball
- 5 years ago
- Views:
Transcription
1 MUSCULOSKELETAL AND NEUROLOGICAL DISORDERS There are a wide variety of Neurologic and Musculoskeletal disorders which can impact driving safety. Impairment may be the result of altered muscular, skeletal, neurologic, and/or cognitive function. Motor, sensory, and/or cognitive deficits may adversely affect strength, coordination, reaction time, range of motion, visual perception, processing speed, judgment, problem solving, attention, memory, and/or awareness, in terms of a driver's ability to perform the actions necessary to safely operate a motor vehicle. Disorders affecting cognition such as epilepsy, stroke, traumatic brain injury, Parkinson s disease, dementia, and encephalopathy as well as disorders affecting neuromuscular function such as multiple sclerosis, Parkinson s disease, muscular dystrophy, cerebral palsy, myasthenia gravis, amyotrophic lateral sclerosis, spinocerebellar ataxia, foot drop, neuropathy, and spinal cord disorders all may present their own unique barriers to safe motor vehicle operation. What s more, there is considerable overlap in the clinical manifestations of these disorders. A driver with these conditions may have chronic functional limitations that have the potential to affect safe operation of a motor vehicle and should be evaluated. When functional abilities are in question, a road test may be recommended by the clinician or required by BMV. Many of these conditions may result in symptoms or impairments that fall under more than one Functional Ability Profile (FAP) and will need to be evaluated using more than one FAP. For example, following a stroke a driver may experience a visual field or acuity disturbance and may also need adaptive equipment. This person would need to be evaluated using both the Stroke and the Visual Disorders FAP s. A person with Parkinson s Disease may have cognitive or psychiatric deficits as well as the neurological and motor deficits. They would need to be evaluated using the Parkinson s, as well as the Dementia or Mental Disorders FAP. BMV will use the most restrictive FAP to determine the fitness of a person to drive. Neurological disorders may have an unpredictable, episodic, or progressive course and require periodic evaluation by a qualified medical practitioner. The treating clinician shall determine the timing of evaluation but should have a working knowledge of a driver s current condition when filling out the Driver Medical Evaluation (CR-24) form. When completing the CR-24 the driver must have been seen within the past 12 months or less. Individuals with any number of neurological and musculoskeletal conditions may use adaptive equipment when driving. Person s that use adaptive equipment when driving must take a road test. Although referral to a driving rehabilitation specialist may be indicated in some cases, it is not required by BMV. When BMV requires a road test, it will be administered by a BMV Driver s License Examiner. The road test will determine whether the person is allowed to drive and if there are driving restrictions. Conditions which require review include but are not limited to the following: Amputation or Limb Deficiency Amputation or limb deficiencies may be either congenital or acquired of the upper or lower extremities, with functional implications to safe driving being the decreased ability to operate one or more of the vehicle controls. Adaptive driving equipment will require consideration depending on the specific limb deficiency, use of prosthesis and overall functional abilities of the person. Evaluation by a driving rehabilitation specialist may be appropriate depending on the extent of impairment. However, it is not required and does not take the place of the BMV road test. The Miscellaneous Musculoskeletal and Neurological Functional Ability Profile should be used to assess potential for driving impairment.
2 Arthritis or Joint Disorders This category would include related conditions such as rheumatoid arthritis, osteoarthritis, ankylosing spondylitis, and spinal stenosis, among others. Affected structures include joints of axial and appendicular skeleton, and/or spinal nerves. These conditions can cause pain, decreased strength and range of motion, and impaired functional mobility, potentially altering the ability to safely operate motor vehicle controls. In assessing these persons for potential driving impairment, overall functional performance of the person in terms of ability to perform activities of daily living should be taken into consideration to help determine if adaptive equipment or strategies may be needed. Miscellaneous Musculoskeletal and Neurological Conditions Functional Ability Profile should be used to assess driving impairment. Cerebrovascular Accident (CVA or Stroke) Stroke may have a complicated and variable presentation. Residual impairments may include altered strength, mobility, coordination, motor planning, sensation, spatial planning, body or environmental awareness, vision, communication, judgment, and cognition. Motor deficits or contractures may require upper or lower extremity adaptive equipment for driving. Due to the possibility of multiple potential deficits, a comprehensive evaluation by a driving rehabilitation specialist may be indicated but is not required. Use the TBI/Stroke Functional Ability Profile to assess impairment. Other medical issues following a stroke may include seizures, cognitive impairment, and/or visual disorders which need to be evaluated separately using the proper Functional Ability Profile for those conditions. Please note that a transient ischemic attack (TIA) by definition has no residual deficit and is therefore not subject to the Stroke FAP. Miscellaneous Musculoskeletal and Neurological Conditions Neurologic and musculoskeletal conditions with the potential to impair a person s ability to safely operate a motor vehicle are numerous, and therefore have not all been specifically listed. Even if these conditions have not been adequately identified in any of the other categories, they still should be evaluated. Examples of neuromuscular conditions which would be appropriately evaluated using the Miscellaneous Musculoskeletal and Neurological Conditions FAP include but are not limited to muscular dystrophy, cerebral palsy, amyotrophic lateral sclerosis, peripheral/other neuropathies, syringomyelia, as well as any generalized deconditioning syndrome due to any etiology which reduces functional capacity to drive. These conditions may require personal medical equipment or adaptive accessories to operate a motor vehicle, cause deficits in mobility, sensation, strength, coordination, reaction time, range of motion, and/or other abilities needed to safely operate a motor vehicle. Referral to a driving rehabilitation specialist, although not required, may be indicated in some cases. Also, persons who have an implanted spinal cord/dorsal column stimulator are advised to turn off the device prior to driving due to the potential for unexpected changes in stimulation with activity that could possibly be unsafe. When visual, cognitive, psychiatric or other conditions also exist, they should be evaluated separately using the appropriate profile. Multiple Sclerosis (MS) Multiple Sclerosis is a highly variable disorder. Some people may have few if any perceptible symptoms associated with the disorder, while others may be significantly impaired. MS may cause visual impairment, cognitive impairment, alterations in sensation, muscle weakness, incoordination, spasticity, joint contracture. Upper and/or lower extremity orthotics may be required, and a person may also be operating an adapted vehicle from a mobility device (such as a wheelchair). These deficits may cause difficulties with manipulation of vehicle controls, and driver performance in complex driving environments. Comprehensive evaluation for adaptive equipment and an evaluation by a driving rehabilitation specialist may be beneficial but is not required. The progressive nature of MS warrants periodic reassessment of driving risk using the MS Functional Ability Profile. Psychiatric, cognitive, or visual deficits should be evaluated separately using the appropriate Functional Ability Profile.
3 Parkinson s or Parkinsonian Syndromes Parkinson s Disease and Parkinsonism physical signs include tremor, bradykinesia, postural instability, and rigidity, along with complex cognitive issues such as dementia and mood disturbance. These deficits may cause slowed reaction times, difficulties with vehicle controls, and impaired performance in complex driving environments. Evaluation by a driving rehabilitation specialist may be indicated. The progressive nature of the disorder warrants periodic reassessment using the Parkinson s Functional Ability Profile. Psychiatric or cognitive issues should be evaluated separately using the appropriate Functional Ability Profile. For the purpose of this FAP, Progressive Supranuclear Palsy, Multisystem Atrophy, Corticobasal Ganglionic Degenerations, Medication Induced Parkinsonism and Lewy Body Dementia are considered Parkinsonian Syndromes. The cognitive implications of Lewy Body Dementia should be reviewed using the Dementia FAP. Spinal Cord Injury (SCI) SCI of the cervical, thoracic, or lumbosacral regions is the result of a medical condition, lesion or trauma to the neural elements within the spinal canal. This causes impairment of motor and sensory function to the upper or lower limbs and trunk which is variable and depends on the level of injury. Although common terms to describe spinal cord injury are paraplegia and tetraplegia (quadriplegia), The American Spinal Injury Association (ASIA) Impairment Scale more precisely grades the degree of impairment according to the spinal level of preserved motor and sensory function. Safe driving after SCI may be impaired due the altered ability to operate vehicle controls; so the use of orthotics, adaptive driving equipment, and an adapted motor vehicle for use with mobility device/wheelchair are often required. Comprehensive evaluation by a driving rehabilitation specialist should be considered. Miscellaneous Musculoskeletal and Neurological Conditions Functional Ability Profile should be used to assess driving impairment. Traumatic Brain Injury (TBI) TBI causes dysfunction of the central nervous system resulting from trauma or forces to the head significant enough to alter brain function. Cognitive changes after TBI can affect mood, memory, executive function, judgment, initiation, attention, and problem-solving. In addition, because selfawareness and judgment may be affected, a person may not be able recognize their impairments. Depending on the extent of the injury, other deficits may include altered gait, balance and sensation, as well as impaired muscle and joint function due to weakness, spasticity, and contracture. These persons may require ankle-foot orthoses or upper extremity orthotics to improve mobility and use of extremities. Factors that impact on ability to drive safely after TBI can be extensive, and a comprehensive driving evaluation by a driving rehabilitation specialist should be considered. Use the Stroke/TBI Functional Ability Profile to assess impairment. Other medical impairments following TBI may include seizures, cognitive, and visual disorders, which need evaluation separately using the proper Functional Ability Profile for those conditions. FOR REFERENCES, SEE BIBLIOGRAPHY AT END OF DOCUMENT.
4 Cerebrovascular Accident (CVA/Stroke) or Traumatic Brain Injury (TBI) 1 Profile Levels Degree of Impairment 2 / Interval for Review and Other Actions 1. No diagnosed condition No known disorder 2. Condition fully recovered History of Stroke or TBI without residual physical or cognitive deficits or impairments. History of Stroke or TBI with residual 3 cognitive and/or physical impairments or deficits. For TIA, see. 4 Please document residual deficits on Driver Medical form. Residual 3 cognitive or physical deficits, but unlikely risk to safely operating a motor vehicle and does not require assistive medical equipment or nonstandard accessory driving devices. 5 Clinician may request if unsure 5 Residual 3 cognitive or physical deficits that could potentially impair ability to safely drive, and/or requires assistive medical equipment or nonstandard accessory driving device(s). 4 years Residual 3 cognitive and/or physical deficits that are significant enough to impair ability to safely drive. Or, a person with physical or cognitive changes when stroke is suspected and condition is being investigated. 1 For further discussion regarding CEREBROVASCULAR ACCIDENT OR TRAUMATIC BRAIN INJURY, please refer to NARRATIVE found at beginning of this section. 3 Stroke and TBI may lead to other cognitive or physical impairments such as seizures, visual deficits such as hemianopsia or diplopia, or cognitive deficits, such as dementia, impairment to reasoning or judgment, these need to be evaluated using the appropriate FAP. The most restrictive Profile will determine the driving privileges. 4 Please note that a transient ischemic attack (TIA) by definition has no residual deficit and is therefore not subject to this FAP. 5 If a provider has concerns regarding an individual s ability to operate a vehicle safely that are not captured in this FAP then a road test may be requested. Include documentation of all pertinent medical concerns, and rationale for requesting road test.
5 Miscellaneous Musculoskeletal and Neurological Disorders 1 Profile Levels Degree of Impairment 2 / Interval for Review and Other Actions 1. No diagnosed condition No known disorder 2. Condition fully recovered History of injury, deficiency, disorder, or other condition recovered, no longer requires treatment and maintains normal function. Chronic condition such as amputation or limitation of limb, arthritis, joint dis-orders, spinal cord injury, or others which may affect neuromuscular function; and currently require treatment or cause impairments, restrictions, or deficits. For spinal cord/dorsal column stimulator see 3. Chronic condition that does not pose risk for safe driving and does not require use of assistive medical equipment or nonstandard accessory driving devices; or Clinician documents stable condition that is unlikely to deteriorate and driver has already passed road test. Chronic condition, which may impair ability to drive safely and/or requires personal assistive medical equipment (such as prosthesis, orthosis, or any type of nonstandard accessory driving device such as hand/foot controls). 4 years 4 Chronic condition, which causes impairments that interfere with the ability to drive safely despite use of personal assistive medical equipment, or any nonstandard accessory driving devices. 1 For further discussion regarding MISCELLANEOUS MUSCULOSKELETAL AND NEUROLOGICAL DISORDERS, please refer to NARRATIVE found at beginning of this section. 3 Persons who have an implanted spinal cord/dorsal column stimulator are advised turn off the device prior to driving due to the potential for unexpected changes in stimulation with activity that could possibly be unsafe. 4 Interval for review may be more frequent if recommended by clinician.
6 Multiple Sclerosis 1 Profile Levels Degree of Impairment 2 / Interval for Review and Other Actions 1. No diagnosed condition No known disorder 2. Condition fully recovered There is no recovery from multiple sclerosis Multiple sclerosis may affect many domains of the nervous system including cognition, vision, motor skills, coordination etc. In addition it may cause fatigue and/or psychiatric symptoms. 3 Symptoms well controlled, or condition is quiescent. No side effects from medications that could potentially impair driving. 4 years Symptoms or medication side effects that may potentially impair safe driving. 2 years Symptoms or side effects of medication severe enough to preclude safe driving. 1 For further discussion regarding MULTIPLE SCLEROSIS, please refer to NARRATIVE found at beginning of this section. 3 Multiple Sclerosis is a highly variable disorder. Some people may have few if any perceptible symptoms associated with the disorder, while others may be significantly physically or cognitively impaired. Symptoms may fall under more than one FAP and all appropriate FAP s should be used. For example, a driver may require adaptive equipment or have a significant visual field or acuity disturbance. The most restrictive FAP will determine driving privileges or restrictions.
7 Parkinson s and Parkinsonian Syndromes 1 Profile Levels Degree of Impairment 2 / Interval for Review and Other Actions 1. No diagnosed condition No known disorder 3 Parkinson s Disease 3 is a lifelong condition and there is no recovery. 2. Condition fully recovered Drug induced Parkinsonism may be considered recovered when symptoms resolve after the causative medication is stopped. Parkinson s Disease 3 may cause tremor, autonomic instability, rigidity, bradykinesia and/or dyskinesia, cognitive or psychiatric symptoms. 4 Mild physical symptoms that do not pose risk for safe operation of a vehicle. No cognitive or psychiatric symptoms. Medications do not cause drowsiness. 2 years 5 Physical symptoms and/or side effects of medication may potentially interfere with the safe operation of a motor vehicle. May have early cognitive or psychiatric symptoms 4. 1 year Physical symptoms or side effects of medications are incompatible with safe operation of a motor vehicle. For cognitive or psychiatric symptoms, see 4. 1 For further discussion regarding PARKINSON S OR PARKINSONIAN SYNDROMES, please refer to NARRATIVE found at beginning of this section. 3 For the purpose of this FAP, Lewy Body Dementia, Multisystem Atrophy, Corticobasal Ganglionic Degenerations, medication induced Parkinsonism, Vascular Parkinsonism, and Progressive Supranuclear Palsy are considered Parkinsonian Syndromes. 4 Cognitive or Psychiatric symptoms should be evaluated using the Dementia or Mental Disorders FAP. 5 When Parkinsonian Syndrome is caused by medications and patient is stable, the clinician may recommend extending the review interval up to 4 years.
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS. Please check with the LCC bookstore for the required texts for this class.
 LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
Slide 1. Slide 2. Slide 3. Intro to Physical Therapy for Neuromuscular Conditions. PT Evaluation. PT Evaluation
 Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
Clinical Guidelines for Spinal Manipulation in Naturopathic Practice
 QUALITY ASSURANCE REPORT ON NATUROPATHIC MANIPULATION Clinical Guidelines for Spinal Manipulation in Naturopathic Practice Executive Summary April 19, 2005 Clinical guidelines are designed to assist clinicians
QUALITY ASSURANCE REPORT ON NATUROPATHIC MANIPULATION Clinical Guidelines for Spinal Manipulation in Naturopathic Practice Executive Summary April 19, 2005 Clinical guidelines are designed to assist clinicians
Ratified by: Care and Clinical Policies Date: 17 th February 2016
 Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
DISORDERS OF THE NERVOUS SYSTEM
 DISORDERS OF THE NERVOUS SYSTEM Bell Work What s your reaction time? Go to this website and check it out: https://www.justpark.com/creative/reaction-timetest/ Read the following brief article and summarize
DISORDERS OF THE NERVOUS SYSTEM Bell Work What s your reaction time? Go to this website and check it out: https://www.justpark.com/creative/reaction-timetest/ Read the following brief article and summarize
Vibramoov NEUROREHABILITATION OF THE LOCOMOTOR SYSTEM THROUGH FUNCTIONAL PROPRIOCEPTIVE STIMULATION
 Vibramoov NEUROREHABILITATION OF THE LOCOMOTOR SYSTEM THROUGH FUNCTIONAL PROPRIOCEPTIVE STIMULATION Principe of action BRAIN ACTIVATION VIBRAMOOV REVOLUTIONIZES FUNCTIONAL MOVEMENT THERAPY One of the main
Vibramoov NEUROREHABILITATION OF THE LOCOMOTOR SYSTEM THROUGH FUNCTIONAL PROPRIOCEPTIVE STIMULATION Principe of action BRAIN ACTIVATION VIBRAMOOV REVOLUTIONIZES FUNCTIONAL MOVEMENT THERAPY One of the main
CHAPTER 6 NERVOUS SYSTEM G00-G99. Presented by Jan Halloran
 CHAPTER 6 NERVOUS SYSTEM G00-G99 Presented by Jan Halloran 1 LEARNING OUTCOMES After studying this chapter you should be able to: Explain the difference between the central and peripheral nervous systems
CHAPTER 6 NERVOUS SYSTEM G00-G99 Presented by Jan Halloran 1 LEARNING OUTCOMES After studying this chapter you should be able to: Explain the difference between the central and peripheral nervous systems
InterQual Level of Care 2018 Index
 InterQual Level of Care 2018 Index Rehabilitation Criteria Index Words by Subset The Index is an alphabetical listing of conditions and/or diagnoses designed to guide the user to the criteria subset where
InterQual Level of Care 2018 Index Rehabilitation Criteria Index Words by Subset The Index is an alphabetical listing of conditions and/or diagnoses designed to guide the user to the criteria subset where
Physical Therapist Assistant Principles of Neuromuscular Rehabilitation
 Western Technical College 10524144 Physical Therapist Assistant Principles of Neuromuscular Rehabilitation Course Outcome Summary Course Information Description Career Cluster Instructional Level Total
Western Technical College 10524144 Physical Therapist Assistant Principles of Neuromuscular Rehabilitation Course Outcome Summary Course Information Description Career Cluster Instructional Level Total
Physical and Medical Impairments in Elderly Drivers
 Physical and Medical Impairments in Elderly Drivers Kam Hunter, MD PhD AzGS Summer Interdisciplinary Conference August 3 rd, 2011 Physiology Pertinent Systems Affected by Aging Visual Decreased central
Physical and Medical Impairments in Elderly Drivers Kam Hunter, MD PhD AzGS Summer Interdisciplinary Conference August 3 rd, 2011 Physiology Pertinent Systems Affected by Aging Visual Decreased central
United Council for Neurologic Subspecialties Geriatric Neurology Written Examination Content Outline
 United Council for Neurologic Subspecialties Geriatric Neurology Written Examination Content Outline REV 3/24/09 The UCNS Geriatric Neurology examination was established to determine the level of competence
United Council for Neurologic Subspecialties Geriatric Neurology Written Examination Content Outline REV 3/24/09 The UCNS Geriatric Neurology examination was established to determine the level of competence
Certification in Neurological Clinical Practice Program Overview, Course Description and Objectives and Grading Scale
 Certification in Neurological Clinical Practice Program Overview, and Objectives and Grading Scale August 31, 2015 NeuroRTI Grading System (from Policy and Procedure Handbook Section 3.7) Each online course
Certification in Neurological Clinical Practice Program Overview, and Objectives and Grading Scale August 31, 2015 NeuroRTI Grading System (from Policy and Procedure Handbook Section 3.7) Each online course
Clinical Diagnosis. Step 1: Dementia or not? Diagnostic criteria for dementia (DSM-IV)
 Step 1: Dementia or not? Diagnostic criteria for dementia (DSM-IV) A. The development of multiple cognitive deficits manifested by both 1 and 2 1 1. Memory impairment 2. One (or more) of the following
Step 1: Dementia or not? Diagnostic criteria for dementia (DSM-IV) A. The development of multiple cognitive deficits manifested by both 1 and 2 1 1. Memory impairment 2. One (or more) of the following
Table of Contents. Preface... xi. Part I: Introduction to Movement Disorders
 Table of Contents Visit www.healthreferenceseries.com to view A Contents Guide to the Health Reference Series, a listing of more than 14,000 topics and the volumes in which they are covered. Preface...
Table of Contents Visit www.healthreferenceseries.com to view A Contents Guide to the Health Reference Series, a listing of more than 14,000 topics and the volumes in which they are covered. Preface...
DELINEATION OF PRIVILEGES - REHABILITATION MEDICINE
 KALEIDA HEALTH Name ABMS Board DELINEATION OF PRIVILEGES - REHABILITATION MEDICINE Certification: Please circle all that apply: Board Qualified: Inpatient Rehab Care: Admitting Privileges** (**e: Admitting
KALEIDA HEALTH Name ABMS Board DELINEATION OF PRIVILEGES - REHABILITATION MEDICINE Certification: Please circle all that apply: Board Qualified: Inpatient Rehab Care: Admitting Privileges** (**e: Admitting
PHYSICIAN S STATEMENT OF EXAMINATION
 PHYSICIAN S STATEMENT OF EXAMINATION Michigan Department of State Driver Assessment and Appeal Division P.O. Box 30196 Lansing, Michigan 48909-7696 Phone: (517) 335-7051 Fax: (517) 335-2189 INSTRUCTIONS
PHYSICIAN S STATEMENT OF EXAMINATION Michigan Department of State Driver Assessment and Appeal Division P.O. Box 30196 Lansing, Michigan 48909-7696 Phone: (517) 335-7051 Fax: (517) 335-2189 INSTRUCTIONS
A very simplified introduction to neuromuscular illnesses (NMIs) with a particular focus on the muscular dystrophies.
 1 A very simplified introduction to neuromuscular illnesses (NMIs) with a particular focus on the muscular dystrophies. Available on-line at: Bill Tillier Calgary Alberta September, 2008. Terminology.
1 A very simplified introduction to neuromuscular illnesses (NMIs) with a particular focus on the muscular dystrophies. Available on-line at: Bill Tillier Calgary Alberta September, 2008. Terminology.
Lack of muscle control (Stroke, bladder control, neurological disorders) Mechanical movement therapist assisted
 By Lisa Rosenberg Electrical Current Stimulates muscles and nerves Produces movement Helps Individuals with Disabilities Lack of muscle control (Stroke, bladder control, neurological disorders) Passive
By Lisa Rosenberg Electrical Current Stimulates muscles and nerves Produces movement Helps Individuals with Disabilities Lack of muscle control (Stroke, bladder control, neurological disorders) Passive
Lumbosacral plexus lesion Lumbosacral plexus disorders G54.1 Neuralgic amyotrophy Neuralgic amyotrophy G
 ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES Focal Neuropathy ICD-9-CM ICD-10-CM Mononeuropathy G56.00 Carpal tunnel syndrome 354.00 Other median nerve lesion 354.10 Lesion of ulnar nerve 354.20
ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES Focal Neuropathy ICD-9-CM ICD-10-CM Mononeuropathy G56.00 Carpal tunnel syndrome 354.00 Other median nerve lesion 354.10 Lesion of ulnar nerve 354.20
Notifiable Medical Conditions
 Notifiable Medical Conditions A Acoustic neuroma Addison s disease Agoraphobia AIDS Alcohol problems Alzheimer s disease Amyotrophic Lateral Sclerosis - see Motor Neurone Disease Amputations Aneurysm Angina
Notifiable Medical Conditions A Acoustic neuroma Addison s disease Agoraphobia AIDS Alcohol problems Alzheimer s disease Amyotrophic Lateral Sclerosis - see Motor Neurone Disease Amputations Aneurysm Angina
Covered Critical Illness Conditions Appendix Effective Date: March 1, 2010
 Covered Critical Illness Conditions Appendix Effective Date: March 1, 2010 This Appendix contains definitions for those Conditions that are covered under the Manulife Financial s Group Critical Illness
Covered Critical Illness Conditions Appendix Effective Date: March 1, 2010 This Appendix contains definitions for those Conditions that are covered under the Manulife Financial s Group Critical Illness
Fourth Year BPT Degree Examinations, October Clinical Cardio Respiratory Disorders and Surgery
 QP CODE:403014 Clinical Cardio Respiratory Disorders and Surgery 1. Classify congenital heart disease. What are the clinical features and management of tetrology of fallot. 2. Define respiratory failure.
QP CODE:403014 Clinical Cardio Respiratory Disorders and Surgery 1. Classify congenital heart disease. What are the clinical features and management of tetrology of fallot. 2. Define respiratory failure.
FORM ID. Patient's Personal Details. SECTION A : Medical Record of the Patient. Name. Policy Number. NRIC/Old IC/Passport/Birth Cert/Others
 CRITICAL ILLNESS CLAIM - DOCTOR'S STATEMENT Brain and Nerve Related Conditions Note: This form is to be completed at the Patient s expense by the Attending Physician/ Surgeon who treated the patient. Patient's
CRITICAL ILLNESS CLAIM - DOCTOR'S STATEMENT Brain and Nerve Related Conditions Note: This form is to be completed at the Patient s expense by the Attending Physician/ Surgeon who treated the patient. Patient's
DEPARTMENT OF PHYSICAL MEDICINE AND REHABILITATION P.G. TEACHING SCHEDULE FOR THE MONTH JUNE -2018
 DEPARTMENT OF PHYSICAL MEDICINE AND REHABILITATION P.G. TEACHING SCHEDULE FOR THE MONTH JUNE -2018 THEORY (TIME: 3 PM) DATE TOPIC FACULTY 1/06/2018 NEUROLOGIC LEVEL OF INJURY DR.RAVI 4/06/2018 CERVICAL
DEPARTMENT OF PHYSICAL MEDICINE AND REHABILITATION P.G. TEACHING SCHEDULE FOR THE MONTH JUNE -2018 THEORY (TIME: 3 PM) DATE TOPIC FACULTY 1/06/2018 NEUROLOGIC LEVEL OF INJURY DR.RAVI 4/06/2018 CERVICAL
Contents. copyrighted material by PRO-ED, Inc. Chapter 1. Chapter 2. Chapter 3. Chapter 4. Chapter 5. Conditions in Athletic Injuries
 Acknowledgments xiii Introduction to the First Edition xv Introduction to the Second Edition xvii Chapter 1 Conditions in Athletic Injuries Anterior Cruciate Ligament (ACL) Tear 2 Biceps Tendon Strain
Acknowledgments xiii Introduction to the First Edition xv Introduction to the Second Edition xvii Chapter 1 Conditions in Athletic Injuries Anterior Cruciate Ligament (ACL) Tear 2 Biceps Tendon Strain
Central nervous system
 Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
Neuropsychological Testing (NPT)
 Neuropsychological Testing (NPT) POLICY Psychological testing (96101-03) refers to a series of tests used to evaluate and treat an individual with emotional, psychiatric, neuropsychiatric, personality
Neuropsychological Testing (NPT) POLICY Psychological testing (96101-03) refers to a series of tests used to evaluate and treat an individual with emotional, psychiatric, neuropsychiatric, personality
Initial symptom or syndrome: (1) FOCAL WEAKNESS OR NUMBNESS
 View the referenced DVD patient cases, especially if few hospital or clinic patients are encountered for any one symptom or syndrome. The DVD patient cases are referenced by initial symptom or syndrome
View the referenced DVD patient cases, especially if few hospital or clinic patients are encountered for any one symptom or syndrome. The DVD patient cases are referenced by initial symptom or syndrome
1. The episode should be classified according to the primary reason for the current episode of rehabilitation care
 IMPAIRMENT CODING GUIDELINES The aim of these guidelines is to assist in correctly classifying a rehabilitation episode according to impairment groups. There are 2 over-riding rules that need to be considered
IMPAIRMENT CODING GUIDELINES The aim of these guidelines is to assist in correctly classifying a rehabilitation episode according to impairment groups. There are 2 over-riding rules that need to be considered
IMPAIRMENT OF THE NERVOUS SYSTEM
 IMPAIRMENT OF THE NERVOUS SYSTEM The following information provides criteria for the evaluation of permanent impairment resulting from dysfunction brain, spinal cord and cranial nerves and certain peripheral
IMPAIRMENT OF THE NERVOUS SYSTEM The following information provides criteria for the evaluation of permanent impairment resulting from dysfunction brain, spinal cord and cranial nerves and certain peripheral
Neurostimulators and Neuromuscular
 Neurostimulators and Neuromuscular Stimulators Chapter.1 Enrollment..................................................................... -2.2 Benefits, Limitations, and Authorization Requirements...........................
Neurostimulators and Neuromuscular Stimulators Chapter.1 Enrollment..................................................................... -2.2 Benefits, Limitations, and Authorization Requirements...........................
Differential Diagnosis of Hypokinetic Movement Disorders
 Differential Diagnosis of Hypokinetic Movement Disorders Dr Donald Grosset Consultant Neurologist - Honorary Professor Institute of Neurological Sciences - Glasgow University Hypokinetic Parkinson's Disease
Differential Diagnosis of Hypokinetic Movement Disorders Dr Donald Grosset Consultant Neurologist - Honorary Professor Institute of Neurological Sciences - Glasgow University Hypokinetic Parkinson's Disease
DPT Physical Therapy Curriculum
 PHT 55 Gross Anatomy & Lab PHT 554 Human Physiology PHT 55 Analysis of Human Motion I & Lab PHT 505 Professional Behavior PHT 549 Life Span Development DPT Physical Therapy Curriculum Fall Semster,Year
PHT 55 Gross Anatomy & Lab PHT 554 Human Physiology PHT 55 Analysis of Human Motion I & Lab PHT 505 Professional Behavior PHT 549 Life Span Development DPT Physical Therapy Curriculum Fall Semster,Year
MOTOR NEURONE DISEASE
 MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
Bossier Parish Community College Master Syllabus
 Bossier Parish Community College Master Syllabus Course Prefix and Number: OCTA 213 Credit Hours: 3 Course Title: OT Strategies and Intervention to Physical Challenges Course Prerequisite: Enrollment in
Bossier Parish Community College Master Syllabus Course Prefix and Number: OCTA 213 Credit Hours: 3 Course Title: OT Strategies and Intervention to Physical Challenges Course Prerequisite: Enrollment in
Parkinson Disease. Lorraine Kalia, MD, PhD, FRCPC. Presented by: Ontario s Geriatric Steering Committee
 Parkinson Disease Lorraine Kalia, MD, PhD, FRCPC Key Learnings Parkinson Disease (L. Kalia) Key Learnings Parkinson disease is the most common but not the only cause of parkinsonism Parkinson disease is
Parkinson Disease Lorraine Kalia, MD, PhD, FRCPC Key Learnings Parkinson Disease (L. Kalia) Key Learnings Parkinson disease is the most common but not the only cause of parkinsonism Parkinson disease is
Vague Neurological Disorders
 Vague Neurological Disorders Dr. Philip Smalley MD FRCPC SVP & Global Chief Medical Officer RGA International Rose Conference, September 17, 2015 Agenda Vague neurological symptoms associated with: Alzheimer
Vague Neurological Disorders Dr. Philip Smalley MD FRCPC SVP & Global Chief Medical Officer RGA International Rose Conference, September 17, 2015 Agenda Vague neurological symptoms associated with: Alzheimer
The road to safety starts with us. DRIVING REHABILITATION
 The road to safety starts with us. Stay safe and confident in the driver s seat. As you age, your ability to drive can be a vital key to your independence. Our Driving Rehab Specialists work with you to
The road to safety starts with us. Stay safe and confident in the driver s seat. As you age, your ability to drive can be a vital key to your independence. Our Driving Rehab Specialists work with you to
Possible Precautions or Contraindications. Physical/Sexual/Emotional Abuse. Exacerbations of medical conditions
 Dear Physician, Your patient,, DOB: is interested in participating in one of the following: Physical and/or Occupational Therapy evaluation and treatment using all appropriate treatment methods including
Dear Physician, Your patient,, DOB: is interested in participating in one of the following: Physical and/or Occupational Therapy evaluation and treatment using all appropriate treatment methods including
Neurological Conditions List by Practitioner Type MED-NEURODA~001
 Neurological Conditions List by Practitioner Type MED-NEURODA~001 Date: 26 May 2016 Foreword This guidance has been produced as part of a training programme for Healthcare Professionals approved by the
Neurological Conditions List by Practitioner Type MED-NEURODA~001 Date: 26 May 2016 Foreword This guidance has been produced as part of a training programme for Healthcare Professionals approved by the
Overview. Overview. Parkinson s disease. Secondary Parkinsonism. Parkinsonism: Motor symptoms associated with impairment in basal ganglia circuits
 Overview Overview Parkinsonism: Motor symptoms associated with impairment in basal ganglia circuits The differential diagnosis of Parkinson s disease Primary vs. Secondary Parkinsonism Proteinopathies:
Overview Overview Parkinsonism: Motor symptoms associated with impairment in basal ganglia circuits The differential diagnosis of Parkinson s disease Primary vs. Secondary Parkinsonism Proteinopathies:
Vascular Disorders. Nervous System Disorders (Part B-1) Module 8 -Chapter 14. Cerebrovascular disease S/S 1/9/2013
 Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Course Descriptions for Courses in the Entry-Level Doctorate in Occupational Therapy Curriculum
 Course Descriptions for Courses in the Entry-Level Doctorate in Occupational Therapy Curriculum Course Name Therapeutic Interaction Skills Therapeutic Interaction Skills Lab Anatomy Surface Anatomy Introduction
Course Descriptions for Courses in the Entry-Level Doctorate in Occupational Therapy Curriculum Course Name Therapeutic Interaction Skills Therapeutic Interaction Skills Lab Anatomy Surface Anatomy Introduction
ALTRU HEALTH SYSTEM Grand Forks, ND STANDARD GUIDELINE
 ALTRU HEALTH SYSTEM Grand Forks, ND STANDARD GUIDELINE Title: BACLOFEN PUMP PROGRAM (INTRATHECAL) Issued by: Physical Medicine and Outpatient Therapy Date: 6/99 Reviewed: 2/17 Revision: 2/11 Page: 1 of
ALTRU HEALTH SYSTEM Grand Forks, ND STANDARD GUIDELINE Title: BACLOFEN PUMP PROGRAM (INTRATHECAL) Issued by: Physical Medicine and Outpatient Therapy Date: 6/99 Reviewed: 2/17 Revision: 2/11 Page: 1 of
LOTHIAN LUMBAR SPINE PATHWAYS
 LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
Movement Disorders. Psychology 372 Physiological Psychology. Background. Myasthenia Gravis. Many Types
 Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
SARI Therapeutic Riding GUIDELINES FOR PHYSICIANS / THERAPISTS
 SARI Therapeutic Riding GUIDELINES FOR PHYSICIANS / THERAPISTS CONTRAINDICATIONS AND PRECAUTIONS FOR THERAPEUTIC RIDING The following conditions may represent precautions or contraindications to therapeutic
SARI Therapeutic Riding GUIDELINES FOR PHYSICIANS / THERAPISTS CONTRAINDICATIONS AND PRECAUTIONS FOR THERAPEUTIC RIDING The following conditions may represent precautions or contraindications to therapeutic
Your Orthotics service is changing
 Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
AAPM&R Delineation of Privileges for Physiatrists
 AAPM&R Delineation of Privileges for Physiatrists The purpose of this document is to serve as a guide and facilitate the process of physiatrists (also known as physical medicine and rehabilitation [PM&R]
AAPM&R Delineation of Privileges for Physiatrists The purpose of this document is to serve as a guide and facilitate the process of physiatrists (also known as physical medicine and rehabilitation [PM&R]
Definitions. Peace of mind today and tomorrow. CRITICAL ILLNESS Basic benefit Deluxe benefit. CRITICAL ILLNESS MULTI-PROTECTION (per child)
 Definitions Peace of mind today and tomorrow CRITICAL ILLNESS Basic benefit Deluxe benefit CRITICAL ILLNESS MULTI-PROTECTION (per child) Here are the definitions of the critical and non-critical illnesses
Definitions Peace of mind today and tomorrow CRITICAL ILLNESS Basic benefit Deluxe benefit CRITICAL ILLNESS MULTI-PROTECTION (per child) Here are the definitions of the critical and non-critical illnesses
Nervous System. Unit 6.6 (6 th Edition) Chapter 7.6 (7 th Edition)
 Nervous System Unit 6.6 (6 th Edition) Chapter 7.6 (7 th Edition) 1 Learning Objectives Identify the main parts (anatomy) of a neuron. Identify the 2 divisions of nervous system. Classify the major types
Nervous System Unit 6.6 (6 th Edition) Chapter 7.6 (7 th Edition) 1 Learning Objectives Identify the main parts (anatomy) of a neuron. Identify the 2 divisions of nervous system. Classify the major types
1/28/2019. OSF HealthCare INI Care Center Team. Neuromuscular Disease: Muscular Dystrophy. OSF HealthCare INI Care Center Team: Who are we?
 Neuromuscular Disease: Muscular Dystrophy Muscular Dystrophy Association (MDA) and OSF HealthCare Illinois Neurological Institute (INI) Care Center Team The Neuromuscular clinic is a designated MDA Care
Neuromuscular Disease: Muscular Dystrophy Muscular Dystrophy Association (MDA) and OSF HealthCare Illinois Neurological Institute (INI) Care Center Team The Neuromuscular clinic is a designated MDA Care
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
79 HCCs CMS-HCC Risk Adjustment Model. ICD-10-CM to CMS-HCC Crosswalk. Over 9,500 ICD-10-CM codes map to one or more.
 2017 CMS-HCC Risk Adjustment Model Over 9,500 ICD-10-CM codes map to one or more 79 HCCs ICD-10-CM to CMS-HCC Crosswalk CMS-HCC Model On April 4, 2016, the Centers for Medicare & Medicaid Services (CMS)
2017 CMS-HCC Risk Adjustment Model Over 9,500 ICD-10-CM codes map to one or more 79 HCCs ICD-10-CM to CMS-HCC Crosswalk CMS-HCC Model On April 4, 2016, the Centers for Medicare & Medicaid Services (CMS)
Vague Neurological Conditions
 Vague Neurological Conditions Dr. John Lefebre, MD, FRCPC Chief Regional Medical Director Europe, India, South Africa, Middle East and Turkey Canada 2014 2 3 4 Agenda Dr. John Lefebre, M.D., FRCPC 1. TIA
Vague Neurological Conditions Dr. John Lefebre, MD, FRCPC Chief Regional Medical Director Europe, India, South Africa, Middle East and Turkey Canada 2014 2 3 4 Agenda Dr. John Lefebre, M.D., FRCPC 1. TIA
Neurology. Access Center 24/7 access for referring physicians (866) 353-KIDS (5437)
 Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
Neurology The Neurology practice at Valley Children s provides diagnostic services, medical treatment, and followup care to infants, children, and adolescents who have suspected or confirmed neurological
Building Better Balance
 Building Better Balance The Effects of MS on Balance Individuals with MS experience a decline in their balance due to various MS related impairments. Some of these impairments can be improved with exercise
Building Better Balance The Effects of MS on Balance Individuals with MS experience a decline in their balance due to various MS related impairments. Some of these impairments can be improved with exercise
Configure for Diverse
 Configure for Diverse Clinical Needs Foot Drop Lower Cuff Foot Drop & Knee Instability Lower & Thigh Cuffs Pediatric Foot Drop Small Lower Cuff Foot Sensor: required for gait Knee Instability & Thigh Weakness
Configure for Diverse Clinical Needs Foot Drop Lower Cuff Foot Drop & Knee Instability Lower & Thigh Cuffs Pediatric Foot Drop Small Lower Cuff Foot Sensor: required for gait Knee Instability & Thigh Weakness
Disorders of Movement M A R T I N H A R L E Y N E U R O L O G Y
 Disorders of Movement M A R T I N H A R L E Y N E U R O L O G Y Educational Objectives Improved history taking in patients with movement disorders. Develop a systematic approach to observing and describing
Disorders of Movement M A R T I N H A R L E Y N E U R O L O G Y Educational Objectives Improved history taking in patients with movement disorders. Develop a systematic approach to observing and describing
American Osteopathic College of Occupational and Preventive Medicine 2012 Mid-Year Educational Conference St Petersburg, Florida
 Neurological Neurological Liz Clark, D.O., MPH & TM FAOCOPM MY-2012 49 CFR 391.41(b)(7) "A person is physically qualified to drive a commercial motor vehicle if that person Has no established medical history
Neurological Neurological Liz Clark, D.O., MPH & TM FAOCOPM MY-2012 49 CFR 391.41(b)(7) "A person is physically qualified to drive a commercial motor vehicle if that person Has no established medical history
SENSORY (ASCENDING) SPINAL TRACTS
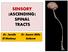 SENSORY (ASCENDING) SPINAL TRACTS Dr. Jamila El-Medany Dr. Essam Eldin Salama OBJECTIVES By the end of the lecture, the student will be able to: Define the meaning of a tract. Distinguish between the different
SENSORY (ASCENDING) SPINAL TRACTS Dr. Jamila El-Medany Dr. Essam Eldin Salama OBJECTIVES By the end of the lecture, the student will be able to: Define the meaning of a tract. Distinguish between the different
Current Clinical Trials for Stroke Survivors in NJ and Philadelphia Areas
 Current Clinical Trials for Survivors in NJ and Philadelphia Areas For more information go to https://clinicaltrials.gov/ and search for the title in search box Condition / Disease 1. Spatial Neglect and
Current Clinical Trials for Survivors in NJ and Philadelphia Areas For more information go to https://clinicaltrials.gov/ and search for the title in search box Condition / Disease 1. Spatial Neglect and
Guidelines for Recognition of Private Hospital-Based Rehabilitation Services March 2016
 Guidelines for Recognition of Private Hospital-Based Rehabilitation Services March 2016 Developed by the Consultative Committee on Private Rehabilitation Guidelines for Recognition of Private Hospital-Based
Guidelines for Recognition of Private Hospital-Based Rehabilitation Services March 2016 Developed by the Consultative Committee on Private Rehabilitation Guidelines for Recognition of Private Hospital-Based
PT/LPTA Skills Checklist
 PT/LPTA Skills Checklist First name: Middle Name: Last Name: Last 4 of SSN# Email Address: Phone # Please indicate your level of experience based on No experience (1) to perform independently (4) 1. No
PT/LPTA Skills Checklist First name: Middle Name: Last Name: Last 4 of SSN# Email Address: Phone # Please indicate your level of experience based on No experience (1) to perform independently (4) 1. No
Parkinson s Disease in the Elderly A Physicians perspective. Dr John Coyle
 Parkinson s Disease in the Elderly A Physicians perspective Dr John Coyle Overview Introduction Epidemiology and aetiology Pathogenesis Diagnosis and clinical features Treatment Psychological issues/ non
Parkinson s Disease in the Elderly A Physicians perspective Dr John Coyle Overview Introduction Epidemiology and aetiology Pathogenesis Diagnosis and clinical features Treatment Psychological issues/ non
AROC Outcome Targets Report Inpatient Pathway 3
 AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
Index SLEEP MEDICINE CLINICS. Note: Page numbers of article titles are in boldface type.
 299 SLEEP MEDICINE CLINICS Sleep Med Clin 1 (2006) 299 303 Note: Page numbers of article titles are in boldface type. A Acid reflux, sleep disturbances in older adults related to, 238 Aging, alterations
299 SLEEP MEDICINE CLINICS Sleep Med Clin 1 (2006) 299 303 Note: Page numbers of article titles are in boldface type. A Acid reflux, sleep disturbances in older adults related to, 238 Aging, alterations
Plan for Today. Brain Injury: 8/4/2017. Effective Services for People Living with Brain Injury. What is it & what causes it?
 Effective Services for People Living with Brain Injury Jean Capler, MSW, LSW Local Support Network Leader The Rehabilitation Hospital of Indiana Department of Resource Facilitation Plan for Today Brain
Effective Services for People Living with Brain Injury Jean Capler, MSW, LSW Local Support Network Leader The Rehabilitation Hospital of Indiana Department of Resource Facilitation Plan for Today Brain
III./3.1. Movement disorders with akinetic rigid symptoms
 III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
ICD-9 to ICD-10 Crosswalk Adult Codes
 ICD- to ICD- Crosswalk Adult Codes On October 1, 2015, the Centers for Medicare & Medicaid Services (CMS) transitioned to the new International Classification of Diseases, th Revision System (ICD-), which
ICD- to ICD- Crosswalk Adult Codes On October 1, 2015, the Centers for Medicare & Medicaid Services (CMS) transitioned to the new International Classification of Diseases, th Revision System (ICD-), which
Approach to a Neurologic Diagnosis
 Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Information contained in this curriculum guide is subject to change.
 Curriculum Overview The curriculum plan includes up to 55 required courses. During the first year students build on their prerequisite coursework through courses in the basic sciences and begin clinical
Curriculum Overview The curriculum plan includes up to 55 required courses. During the first year students build on their prerequisite coursework through courses in the basic sciences and begin clinical
Health History Questionnaire
 LTC Health History Questionnaire The first step in long-term care expense planning is determining insurability. Long-term care insurance is medically underwritten. Health history will determine carrier,
LTC Health History Questionnaire The first step in long-term care expense planning is determining insurability. Long-term care insurance is medically underwritten. Health history will determine carrier,
Case Study 2: Neurological Degenerative Disease FDA Regulatory and Clinical Background
 Case Study 2: Neurological Degenerative Disease FDA Regulatory and Clinical Background Heather Benz, Ph.D. FDA Center for Devices and Radiological Health Neurological Degenerative Diseases Neurodegenerative
Case Study 2: Neurological Degenerative Disease FDA Regulatory and Clinical Background Heather Benz, Ph.D. FDA Center for Devices and Radiological Health Neurological Degenerative Diseases Neurodegenerative
Joint Disorders. Musculoskeletal Disorders (Part B-2) Module 7 -Chapter 10. Overview Disorders of the Muscular System Disorders of the Skeletal System
 Musculoskeletal Disorders (Part B-2) Module 7 -Chapter 10 Overview Disorders of the Muscular System Disorders of the Skeletal System Susie Turner, MD 1/9/13 Joint Disorders Arthritis Inflammation of Joint
Musculoskeletal Disorders (Part B-2) Module 7 -Chapter 10 Overview Disorders of the Muscular System Disorders of the Skeletal System Susie Turner, MD 1/9/13 Joint Disorders Arthritis Inflammation of Joint
PD AND FALLS J U MALLYA FALLS AWARENESS MEETING
 PD AND FALLS J U MALLYA FALLS AWARENESS MEETING 23-09-2016 PD Chronic Progressive neurodegenerative disease Motor system disorder Degeneration of Dopaminergic neurons in Substantia nigra in the midbrain.
PD AND FALLS J U MALLYA FALLS AWARENESS MEETING 23-09-2016 PD Chronic Progressive neurodegenerative disease Motor system disorder Degeneration of Dopaminergic neurons in Substantia nigra in the midbrain.
Neurology Goals: Knowledge:
 Neurology Goals: A solid understanding of normal neurological development, anatomy and neurophysiology is imperative to the treatment of neurological pathology. The goal is to sensitize the family medicine
Neurology Goals: A solid understanding of normal neurological development, anatomy and neurophysiology is imperative to the treatment of neurological pathology. The goal is to sensitize the family medicine
Paraplegia: Exercise and Health Considerations. By: Juli and Trina
 Paraplegia: Exercise and Health Considerations By: Juli and Trina What is paraplegia? Paraplegia is impairment of motor and/or sensory function to the lower extremities, and sometimes the lower trunk Complete
Paraplegia: Exercise and Health Considerations By: Juli and Trina What is paraplegia? Paraplegia is impairment of motor and/or sensory function to the lower extremities, and sometimes the lower trunk Complete
ICD-9 to ICD-10 Conversion Sample for Physical, Occupational and Speech Therapy - SNF Setting
 1 ICD-9 to ICD-10 Conversion Sample for Physical, Occupational and Speech Therapy - SNF Setting ICD-9 Code ICD-9 Description New ICD-10 New ICD-10 Description DM with Neuropathy E11.21 Type 2 diabetes
1 ICD-9 to ICD-10 Conversion Sample for Physical, Occupational and Speech Therapy - SNF Setting ICD-9 Code ICD-9 Description New ICD-10 New ICD-10 Description DM with Neuropathy E11.21 Type 2 diabetes
Course Focus This course introduces neurological principles, pathology and specialized rehabilitation techniques for pediatric and adult care.
 Technical College of the Lowcountry JCulbreth 921 Ribaut Rd. 4/125 Beaufort, SC 29901 843-470-5956 jculbreth@tcl.edu PTH246 Neuromuscular Rehabilitation Fall 2013 Course Description PTH 246 Neuromuscular
Technical College of the Lowcountry JCulbreth 921 Ribaut Rd. 4/125 Beaufort, SC 29901 843-470-5956 jculbreth@tcl.edu PTH246 Neuromuscular Rehabilitation Fall 2013 Course Description PTH 246 Neuromuscular
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Allied and Therapeutic Extender Benefit
 Allied and Therapeutic Extender Benefit 2012 Allied and Therapeutic Extender Benefit The Allied and Therapeutic Extender Benefit is available on the Executive and Comprehensive Plans only. Overview This
Allied and Therapeutic Extender Benefit 2012 Allied and Therapeutic Extender Benefit The Allied and Therapeutic Extender Benefit is available on the Executive and Comprehensive Plans only. Overview This
Medicare Regulations for Chiropractors. Presented by Clinic Pro Software Inc. Marilyn K. Gard. CEO, MBA
 Medicare Regulations for Chiropractors Presented by Clinic Pro Software Inc. Marilyn K. Gard. CEO, MBA Use AT modifier which means active treatment. Claims submitted for Chiropractic manipulative treatment
Medicare Regulations for Chiropractors Presented by Clinic Pro Software Inc. Marilyn K. Gard. CEO, MBA Use AT modifier which means active treatment. Claims submitted for Chiropractic manipulative treatment
JEFFERSON COLLEGE COURSE SYLLABUS OTA105 HEALTH CONDITIONS. 2 Credit Hours
 JEFFERSON COLLEGE COURSE SYLLABUS OTA105 HEALTH CONDITIONS 2 Credit Hours Prepared by: Lisa Martin MS, OTR/L Occupational Therapy Assistant Program Director Revised Date: June 2014 By: Lisa Martin Dena
JEFFERSON COLLEGE COURSE SYLLABUS OTA105 HEALTH CONDITIONS 2 Credit Hours Prepared by: Lisa Martin MS, OTR/L Occupational Therapy Assistant Program Director Revised Date: June 2014 By: Lisa Martin Dena
Aflac Plus Rider. We ve been dedicated to helping provide peace of mind and financial security for nearly 60 years.
 Aflac Plus Rider OPTIONAL LUMP SUM CRITICAL ILLNESS BENEFIT RIDER We ve been dedicated to helping provide peace of mind and financial security for nearly 60 years. CIR076N IC(4/14) AP AFLAC PLUS RIDER
Aflac Plus Rider OPTIONAL LUMP SUM CRITICAL ILLNESS BENEFIT RIDER We ve been dedicated to helping provide peace of mind and financial security for nearly 60 years. CIR076N IC(4/14) AP AFLAC PLUS RIDER
Identification number: TÁMOP /1/A
 Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
International Brain Bee Syllabus 2012 Department of Neurosciences, Universiti Sains Malaysia
 BRAIN DEVELOPMENT The cells of the nervous system connect with one another in trillions of remarkably specific patterns that form and change over the course of an organism s life. These connections develop
BRAIN DEVELOPMENT The cells of the nervous system connect with one another in trillions of remarkably specific patterns that form and change over the course of an organism s life. These connections develop
NEUROLOGY CLERKSHIP CORE CURRICULUM GUIDELINES
 NEUROLOGY CLERKSHIP CORE CURRICULUM GUIDELINES Endorsed by the following organizations - October 2000: American Academy of Neurology Association of University Professors of Neurology American Neurological
NEUROLOGY CLERKSHIP CORE CURRICULUM GUIDELINES Endorsed by the following organizations - October 2000: American Academy of Neurology Association of University Professors of Neurology American Neurological
UDS version 3 Summary of major changes to UDS form packets
 UDS version 3 Summary of major changes to UDS form packets from version 2 to VERSION 3 february 18 final Form A1: Subject demographics Updated question on principal referral source to add additional options
UDS version 3 Summary of major changes to UDS form packets from version 2 to VERSION 3 february 18 final Form A1: Subject demographics Updated question on principal referral source to add additional options
Table of Contents Treatment Guides Basic Activities of Daily Living Basic and Instrumental Activities of Daily Living 11 Bathing and Showering 13 Dres
 Treatment Guides Basic Activities of Daily Living Basic and Instrumental Activities of Daily Living 11 Bathing and Showering 13 Dressing 15 Feeding 18 Functional Communication 20 Functional Mobility 22
Treatment Guides Basic Activities of Daily Living Basic and Instrumental Activities of Daily Living 11 Bathing and Showering 13 Dressing 15 Feeding 18 Functional Communication 20 Functional Mobility 22
This page is for information. Do not submit.
 This page is for information. Do not submit. AISH Application - Part B Medical Report Information for Physicians Your patient (the applicant) is applying for the Assured Income for the Severely Handicapped
This page is for information. Do not submit. AISH Application - Part B Medical Report Information for Physicians Your patient (the applicant) is applying for the Assured Income for the Severely Handicapped
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
CHRONIC CONDITIONS FYI
 CHRONIC CONDITIONS FYI AIDS More than 2,500 cases of HIV/AIDS have been identified in Nebraska. ALS (Amyotrophic Lateral Sclerosis) Approximately 95 people in Nebraska have ALS. As many as 800 Nebraskans
CHRONIC CONDITIONS FYI AIDS More than 2,500 cases of HIV/AIDS have been identified in Nebraska. ALS (Amyotrophic Lateral Sclerosis) Approximately 95 people in Nebraska have ALS. As many as 800 Nebraskans
Using 3-Digit ICD-9-CM Codes with the Elixhauser Comorbidity Index
 Congestive Heart Failure 398.91 Rheumatic heart failure (congestive) 398 Other rheumatic heart disease 402.01, 402.11, 402.91 402 Hypertensive heart disease 404.01, 404.03, 404.11, 404.13, 404.91, 404.93
Congestive Heart Failure 398.91 Rheumatic heart failure (congestive) 398 Other rheumatic heart disease 402.01, 402.11, 402.91 402 Hypertensive heart disease 404.01, 404.03, 404.11, 404.13, 404.91, 404.93
Parkinson s Disease Initial Clinical and Diagnostic Evaluation. J. Timothy Greenamyre, MD, PhD
 Parkinson s Disease Initial Clinical and Diagnostic Evaluation J. Timothy Greenamyre, MD, PhD Involuntary tremulous motion, with lessened muscular power, in parts not in action and even when supported
Parkinson s Disease Initial Clinical and Diagnostic Evaluation J. Timothy Greenamyre, MD, PhD Involuntary tremulous motion, with lessened muscular power, in parts not in action and even when supported
PTA 20. Pathology SYLLABUS AND COURSE INFORMATION PACKET. Spring 2018
 PTA 20 Pathology SYLLABUS AND COURSE INFORMATION PACKET Spring 2018 3 credits Prof. Michael Mattia, PT DPT MS MHA 3 hour lecture Office: S-128 Phone: (718) 368-4818 Email: Michael.mattia@kbcc.cuny.edu
PTA 20 Pathology SYLLABUS AND COURSE INFORMATION PACKET Spring 2018 3 credits Prof. Michael Mattia, PT DPT MS MHA 3 hour lecture Office: S-128 Phone: (718) 368-4818 Email: Michael.mattia@kbcc.cuny.edu
Alberta Transportation. Driver Fitness and Monitoring
 Alberta Transportation Driver Fitness and Monitoring Mature Driver Medical Examinations Driver Fitness and Monitoring Section Alberta Transportation Traffic Safety Services Driver Programs DFM Roles Driver
Alberta Transportation Driver Fitness and Monitoring Mature Driver Medical Examinations Driver Fitness and Monitoring Section Alberta Transportation Traffic Safety Services Driver Programs DFM Roles Driver
Acoustic neuroma s/p removal BPPV (Crystals)- 50% of people over 65 y/ o with dizziness will have this as main reason for dizziness
 Dizziness and the Heart Mended Hearts Inservice Karen Hansen, PT, DPT, Cert Vestibular Rehab, CEAS Tennessee Therapy & Balance Center, LLC July 21, 2016 Balance We maintain balance with input from our
Dizziness and the Heart Mended Hearts Inservice Karen Hansen, PT, DPT, Cert Vestibular Rehab, CEAS Tennessee Therapy & Balance Center, LLC July 21, 2016 Balance We maintain balance with input from our
Enhanced Primary Care Pathway: Parkinson s Disease
 Enhanced Primary Care Pathway: Parkinson s Disease 1. Focused summary of PD relevant to primary care Parkinson s Disease (PD) and Essential tremor (ET) are two of the most common movement disorders encountered
Enhanced Primary Care Pathway: Parkinson s Disease 1. Focused summary of PD relevant to primary care Parkinson s Disease (PD) and Essential tremor (ET) are two of the most common movement disorders encountered
