25-Gauge Vitrectomy versus Intravitreal Bevacizumab for Macular Edema Secondary to Branch Retinal Vein Occlusion: 1 Year Follow-Up
|
|
|
- Rodger Porter
- 5 years ago
- Views:
Transcription
1 294 25G Vitrectomy vs IVB for ME due to BRVO Tatsuhiko Sato et al Original Article 25-Gauge Vitrectomy versus Intravitreal Bevacizumab for Macular Edema Secondary to Branch Retinal Vein Occlusion: 1 Year Follow-Up Tatsuhiko Sato, 1 MD, Kosaku Sawada, 1 MD, Chiharu Iwahashi-Shima, 1 MD, Hajime Bando, 1 MD, Toshihide Ikeda, 1 MD, Kazuyuki Emi, 1 MD Abstract Introduction: This study aims to compare the long-term efficacy of 25-gauge vitrectomy to that of intravitreal bevacizumab (IVB) for the of macular edema (ME) secondary to branch retinal vein occlusion (BRVO). Materials and Methods: The medical records of 46 eyes of 46 consecutive patients were reviewed. Twenty-seven eyes underwent 25-gauge vitrectomy (VIT Group) and 19 eyes received 1.25 mg of IVB (IVB Group). The best-corrected visual acuities (BCVAs) in logarithm of minimum angle resolution units and central macular thicknesses (CMTs) were evaluated before and 3, 6, and 12 months after the initial. Results: There was no significant difference in the pre- BCVA and CMT between the 2 groups. In the VIT Group, the preoperative BCVA was 0.59 and the CMT was μm and the BCVA was 0.35 and the CMT was μm, 12 months after the vitrectomy. Both values were significantly (P <0.05) better at 12 months than the preoperative values. In the IVB Group, the average number of IVB was 2.4 during the 1-year period. The BCVA was 0.69 and the CMT was μm before the IVB, and the BCVA was 0.36 and the CMT was μm, 12 months after the initial IVB. The improvements of these 2 parameters were significant (P <0.05) at 12 months after the initial IVB. The differences in the BCVA and CMT at 12 months between the 2 groups were not significant. Conclusion: These results suggest that the 25-gauge vitrectomy and IVB have similar effects in improving the BCVA and CMT in eyes with ME secondary to BRVO. However, IVB often required several injections to preserve the improvement. Ann Acad Med Singapore 2012;41:294-9 Key words: Eye, Vascular endothelial growth factor Introduction Branch retinal vein occlusion (BRVO) is the second most frequent vascular disorder of the eye, and it can lead to a decrease in vision. One of the main causes for the vision decrease is the development of macular edema (ME), which has been reported to be present in 60% of the cases. 1,2 An earlier study on the natural course of BRVO reported that only 14% of the eyes with chronic ME secondary to BRVO retained a visual acuity of 20/40 or better at the end of the follow-up period. 3 The Branch Vein Occlusion Study Group 4 recommended that grid laser photocoagulation should be used to treat the ME secondary to BRVO. However, grid laser coagulation cannot be used in eyes with intraretinal haemorrhage in the fovea or in the foveal capillary area. In addition, the irreversible destruction of paracentral retinal tissue by the laser photocoagulation can result in parafoveal scotoma. Thus until recently, a number of therapeutic trial studies have been performed retro- or prospectively to determine better ways to treat the ME associated with BRVO. Vitrectomy has been proposed as an alternative, because it is generally believed that vitreous traction on the macula promotes fluid accumulation in the retina. 5-7 Several studies have reported that vitrectomy with or without inner limiting membrane (ILM) peeling can decrease the ME and improve the visual acuity in eyes with BRVO. 8,9 In addition, the 25-gauge vitrectomy system, introduced by Fujii et al, 10 enables surgeons to perform less invasive vitrectomy, which in turn leads to less discomfort and faster postoperative recovery than the conventional 20-gauge vitrectomy. Thus, 25-gauge vitrectomy appears to be an effective way to treat the ME secondary to BRVO. On the other hand, vascular endothelial growth factor (VEGF), also known as vascular permeability factor, has been shown to be a key molecule in the pathogenesis of 1 Osaka Rosai Hospital Clinical Research Center for Occupational Sensory Organ Disability Address for Correspondence: Dr Tatsuhiko Sato, Department of Ophthalmology, Osaka Rosai Hospital, Nagasone-cho, Kita-ku, Sakai, , Japan. t-satou@orh.go.jp Annals Academy of Medicine
2 25G Vitrectomy vs IVB for ME due to BRVO Tatsuhiko Sato et al 295 ME secondary to BRVO. In fact, it has been reported that the intraocular level of VEGF is significantly increased in eyes with BRVO and that its level is correlated with the severity of ME. 11,12 Therefore, pharmacological inhibition of VEGF also seems to be a promising therapy to treat ME secondary to BRVO. Bevacizumab (Avastin ; Genentech, San Francisco, CA, USA) is a full-length humanised monoclonal antibody that is directed against all isoforms of VEGF. Although bevacizumab is approved for intravenous use for the of metastatic colon cancer, 13 it has been widely used as an off-label for ME associated with different ocular disorders including BRVO. Until now, intravitreal injection of bevacizumab has been shown to be effective in resolving the ME secondary to BRVO Furthermore, recent studies have compared the efficacy of intravitreal bevacizumab (IVB) to that of intravitreal triamcinolone 18,19 or of grid laser coagulation 20 for ME secondary to BRVO. However, data for comparison of the efficacy of IVB to 25-gauge vitrectomy in cases with ME secondary to BRVO are not available. Thus, the purpose of this study was to compare the long-term efficacy of 25-gauge vitrectomy to IVB for the of ME secondary to BRVO. Materials and Methods We reviewed the medical records of patients who were initially treated for ME secondary to BRVO at Osaka Rosai Hospital, Sakai, Japan. The procedures used for the s conformed to the tenets of the Declaration of Helsinki and were approved by the Institutional Review Board of Osaka Rosai Hospital. The diagnosis of ME secondary to BRVO was based on clinical examination, fluorescein angiography, and optical coherent tomography (OCT; Stratus OCT-3000; Carl Zeiss Meditec, Dublin, CA, USA). None of the eyes had undergone vitreoretinal surgery, intravitreal injection, and laser before the. Patients with neovascularization before the were excluded. In addition, patients with other ocular diseases, e.g. severe cataract, which could decrease the vision, were excluded. The inclusion criteria were: (i) presence of BRVO of at least 1 month duration, (ii) presence of macular leakage on fluorescein angiography, (iii) best-corrected visual acuity (BCVA) 0.0 in logarithm of minimum angle resolution (logmar) units or central macular thickness (CMT) >250 μm, and (iv) minimum follow-up period of 12 months. The status of the macular perfusion, i.e. ischaemic or nonischaemic vein occlusion, was not evaluated because the grade of ischaemia was often difficult to determine due to retinal haemorrhage. In addition, non-ischaemia vein occlusion can occasionally convert to ischaemic occlusion. After the patients were informed of the potential benefits and risks of 25-gauge vitrectomy and IVB, they chose either 25-gauge vitrectomy (VIT Group) or IVB (IVB Group). Signed informed consents were obtained from all. The BCVA and CMT before and 3, 6, and 12 months after the initial were evaluated. In the VIT Group, standard 3-port pars plana vitrectomy with 25-gauge instruments was performed under local anesthesia. The Accurus (Alcon Laboratories, Inc. Fort Worth, TX, USA) vitrectomy surgical system was used on all eyes. To preserve the conjunctiva, phacoemulsification and aspiration (PEA) and intraocular lens (IOL) implantation were performed through a 2.5-mm clear corneal incision, and a sutureless contact lens ring was used during the vitrectomy. 21 Core vitrectomy was performed with a highspeed vitreous cutter (2500 cycles/minute; MID-Labs, San Leandro, CA, USA) and a conventional halogen light source. The separation of the posterior hyaloid from the retina was performed if it was still attached. To make the ILM more visible, 1.25 mg/ml indocyanine green (ICG) was injected into the vitreal cavity around the ME. 22 After washing out the ICG, the ILM within the major temporal vascular arcades was peeled off with a vitreous forceps. Follow-up examinations were performed within 1 week, 1, 2, 3, 6, and 12 months after the vitrectomy. In the IVB Group, bevacizumab (1.25 mg/0.05 ml) was injected into the vitreous in a surgical room of the outpatient clinic. Prior to the injection, 4% lidocaine hydrochloride and 0.625% povidone-iodine solutions 23,24 were dropped onto the eye. A lid speculum was inserted, and the injection of bevacizumab was performed with a 30-gauge needle inserted through the superior pars plana 3.5 to 4.0 mm from the limbus. The patient s vision was tested after the injection to ensure that the retinal arterial perfusion was intact. After the injection, the patients received topical antibiotic with levofloxacin (Cravit ; Santen Pharmaceutical Co Ltd Osaka, Japan) 4 times per day for a week. Follow-up examinations of BCVA and OCT were performed during the first week, 1 month after the first IVB, and in monthly intervals thereafter. Additional IVB was injected when an increase of the CMT was associated with visual decrease. Statistical analyses were performed with the SPSS program (Sigma Stat; Systat Software, Inc. San Jose, CA, USA). Data are presented as the averages and standard deviations. A significant difference of the ratio between the 2 groups was determined by the chi-square. If the data were normally and equally distributed, one-way repeated measures analysis of variance (ANOVA) was performed to compare 3 or more clinical conditions in July 2012, Vol. 41 No. 7
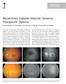
3 296 25G Vitrectomy vs IVB for ME due to BRVO Tatsuhiko Sato et al the subjects, followed by Holm-Sidak or Dunn s method to detect significant differences between each time point and pre-. If the data were not normally or equally distributed, Friedman repeated measures ANOVA on ranks is an alternative to one-way repeated measures ANOVA. The differences between 2 groups was tested by t tests if the data were normally and equally distributed and, if not, by Mann-Whitney rank sum test. The correlation between 2 groups was determined by the Pearson product moment correlation. A P value <0.05 was taken to be statistically significant. Results The demographics of the patients studied are summarised in Table 1. Twenty-seven eyes of 27 patients belonged to the VIT Group, and 19 eyes of 19 patients to the IVB Group. There was no significant difference in the gender ratio, age, pre- BCVA, pre- CMT, and interval from onset to between the 2 groups. Table 1. Patient Demographics and Pre- Ocular Status Parameters VIT Group IVB Group P Value Patients (n) Eyes (n) Sex (female:male) 18:9 11: Age (years, mean ± SDs) 67.1 ± ± * Pre- BCVA (logmar, mean ± SDs) 0.59 ± ± * Pre- CMT (μm, mean ± SDs) ± ± * Duration from onset to (days, mean ± SDs) 86.1 ± ± * Chi-square or *Mann-Whitney Rank Sum test was performed to compare between two groups. VIT: vitrectomy, IVB: intravitreal bevacizumab, SD: standard deviation, BCVA: best-corrected visual acuity, logmar: logarithm of minimum angle resolution, CMT: central macular thickness Fig. 1. Correlation between pre- and post- BCVA. The abscissa represents the BCVA in logmar units before and the ordinate represents the BCVA 12 months after the. (A). Correlation between baseline and post-vitrectomy BCVA in logmar units. Statistical analyses were performed by Pearson product moment correlation (r = 0.769, P = 2.80e -6 ). (B). Correlation between pre- and post-ivb BCVA in logmar units. Statistical analyses were performed by Pearson product moment correlation (r = 0.875, P = 9.47e -7 ). logmar: logarithm of minimum angle resolution, BCVA: best-corrected visual acuity; IVB: intravitreal bevacizumab A A A B In the VIT Group, there were no severe ocular (e.g. infectious endophthalmitis, choroidal haemorrhage, and rhegmatogenous retinal detachment) or systemic complications. Twenty-six phakic eyes underwent vitrectomy with PEA and IOL implantation. The BCVA was 0.59 ± 0.41 logmar units before the vitrectomy and 0.35 ± 0.34 logmar units at 12 months after the vitrectomy (Table 2). There was a positive correlation between the pre- and post-vitrectomy BCVA (r = 0.77, P =2.80 x 10-6 ; Fig. 1A). There was a significant difference in the BCVA among the four time points (P = 7.58 x 10-6 ), and the BCVA at 6 and 12 months after the vitrectomy was significantly (P <0.05) better than the pre-vitrectomy BCVA (Fig. 2). Fig. 2. Time course of best-corrected visual acuity (BCVA) in logarithm of minimum angle resolution (logmar) units. The abscissa represents the time point and the ordinate represents the BCVA in logmar units. Statistical analyses were performed by one way repeated measures analysis of variance (ANOVA) followed by Holm-Sidak in IVB Group and Friedman repeated measure ANOVA on ranks followed by Dunn s method in VIT Group (*P <0.05). : VIT Group, : IVB Group. VIT: vitrectomy, IVB: intravitreal bevacizumab. Annals Academy of Medicine
4 25G Vitrectomy vs IVB for ME due to BRVO Tatsuhiko Sato et al 297 Table 2. Time Course of Visual Acuity and Central Macular Thickness Parameters VIT Group (n = 27) IVB Group (n = 19) P Value BCVA (logmar, mean ± SDs) Pre ± ± * 3 months after initial 0.43 ± ± * 6 months after initial 0.40 ± ± * 12 months after initial 0.35 ± ± * CMT (μm, mean ± SDs) Pre ± ± * 3 months after initial ± ± * 6 months after initial ± ± months after initial ± ± * *Mann-Whitney Rans Sum test or t-test was performed to compare between two groups. VIT: vitrectomy; IVB: intravitreal bevacizumab; BCVA: best-corrected visual acuity; logmar: logarithm of minimum angle resolution; SD: standard deviation; CMT: central macular thickness detachment, and cataract) or systemic (e.g. thrombotic events) complications during the follow-up period. The average number of IVBs was 2.4 ± 1.1 with a range of 1 to 5 during the 1-year follow-up period. Three of 19 eyes (15.8%) had a single IVB. The BCVA was 0.69 ± 0.46 logmar units before the IVB and 0.36 ± 0.47 logmar units at 12 months after the initial IVB (Table 2). There was a positive correlation (r = 0.88, P = 9.47 x 10-7 ) between the 2 time points BCVA (Fig. 1B). There was a significant difference (P = 5.67 x ) in the BCVA among the 4 time points, and the BCVA at 3, 6, and 12 months after the initial IVB was significantly (P <0.05) improved compared to the pre-ivb BCVA (Fig. 2). The CMT was ± μm before the IVB and ± μm at 12 months after the initial IVB (Table 2). There was a significant reduction (P = 4.47 x 10-5 ) in CMT among the 4 time points and the CMT at 3 and 12 months after the initial IVB was significantly (P <0.05) decreased compared to the CMT at pre-ivb (Fig. 3). There was no significant difference in the BCVA and CMT at 12 months after the initial between the IVB and VIT Groups (Table 2). Fig. 3. Time course of central macular thickness (CMT). The abscissa represents the time point and the ordinate represents the CMT. Statistical analyses were performed by Friedman repeated measure analysis of variance on ranks, followed by Dunn s method (*P <0.05). : VIT Group; : IVB Group; VIT: vitrectomy; IVB: intravitreal bevacizumab The CMT was ± μm before the vitrectomy and ± μm at 12 months after the vitrectomy (Table 2). There was a significant reduction (P =7.00 x ) in the CMT for the four time points, and the CMT at 3, 6, and 12 months after the vitrectomy was significantly (P <0.05) decreased compared to the CMT before the vitrectomy (Fig. 3). In the IVB Group, there were no severe ocular (e.g. infectious endophthalmitis, rhegmatogenous retinal Discussion In this study, the long-term efficacy of 25-gauge vitrectomy to IVB for the of ME secondary to BRVO was investigated. The major findings were: the BCVA was significantly improved in both VIT and IVB Groups at 12 months after the initial. In addition, there were positive correlations between the pre- BCVA and the BCVA at 12 months after the in both the VIT and the IVB Groups. Second, the CMT was significantly decreased in both VIT and IVB Groups at 12 months after the initial. Third, at 12 months after the initial, the differences in the BCVA and CMT between the VIT and IVB Groups were not significant. In the VIT Group, 25-gauge instruments were used to minimise the surgically-induced trauma. A recent study has shown that the clearance of VEGF is increased after vitrectomy, 25 suggesting that vitrectomy may lead to the resolution of the ME by reducing the level of the intravitreal VEGF. In addition, ILM peeling was performed in all cases in the VIT Group, and this procedure has been reported to release tangential traction to help resolve the ME. 9 ILM removal has also been reported to facilitate the diffusion of macromolecules from the retina to the vitreous cavity including mediators such as VEGF. 9 Furthermore, removing the ILM at the time of vitrectomy may reduce the risk of postoperative epiretinal membrane proliferation. 26 Through these mechanisms, vitrectomy with ILM peeling could achieve a long-term resolution of the ME associated with July 2012, Vol. 41 No. 7
5 298 25G Vitrectomy vs IVB for ME due to BRVO Tatsuhiko Sato et al BRVO. In concurrence, our findings showed that the reduction of the ME and subsequent improvement of BCVA was sustained for at least 12 months after the vitrectomy. In the IVB Group, a similar effectiveness for improving BCVA and CMT was found during the 12 months follow-up period. Three of 19 eyes (15.8%) had a single IVB while the others needed multiple IVB. The average number of IVB was 2.4 (range, 1 to 5) during the 1-year period. Earlier clinical trials of IVB for cases of ME due to BRVO needed a mean of 2 (Kondo et al 15 ) or 3.4 (Jaissle et al 14 ) injections to preserve the BCVA improvement during a 1-year period. The optimal protocol for IVB for the of ME secondary to BRVO has not been determined. We injected 1.25 mg of IVB while other researchers injected 1.0 mg (Kriechbaum et al 27 ) or 2.5 mg (Hoeh et al 28 ) of IVB. Wu et al 29 reported that IVB at a dose up to 2.5 mg was effective in improving the BCVA and CMT in ME secondary to BRVO, and that there were no significant differences between the 1.25 mg and 2.5 mg dose groups with regard to the number of injections. We selected a single primary injection of bevacizumab with additional injections when needed, while Prager et al 16 used the 3 primary IVB at monthly intervals just as is done to treat age-related macular degeneration. It remains to be determined which of the 2 schedules is better. However, it seems likely that a single primary IVB may be sufficient. One of the reasons is that 3 of our 19 eyes (15.8%) were successfully treated by a single injection during the 1-year follow-up period. Another reason for selecting a single injection of 1.25 mg bevacizumab is that an experimental study on the pharmacokinetics of IVB demonstrated that bevacizumab is retained in the retina for 3 months after the IVB. 30 Although a recurrence of the ME can be treated effectively by re-injection, the number of IVB injections may be important because the benefit of IVB must be carefully weighed against the possible adverse effects of IVB. 31 The results of our study are limited because this was a retrospective, non-randomised, single-center study. Thus, the number of the patients was smaller in the IVB Group than in the VIT Group. In addition, we cannot eliminate the possibility that there may have been a bias in the choice of. A prospective randomised study with a larger number of patients is needed. Conclusion In summary, we compared the efficacy of 25-gauge vitrectomy with that of IVB for the of ME secondary to BRVO and demonstrated that 25-gauge vitrectomy may be as effective as IVB in improving the BCVA and CMT during the 1-year follow-up period. REFERENCES 1. Finkelstein D. Ischemic macular edema. Recognition and favorable natural history in branch vein occlusion. Arch Ophthalmol 1992;110: Greer DV, Constable IJ, Cooper RL. Macular oedema and retinal branch vein occlusion. Aust J Ophthalmol 1980;8: Gutman FA, Zegarra H. The natural course of temporal retinal branch vein occlusion. Trans Am Acad Ophthalmol Otolaryngol 1974;78: The Branch Vein Occlusion Study Group. Argon laser photocoagulation for macular edema in branch vein occlusion. Am J Ophthalmol 1984;98: Avunduk AM, Cetinkaya K, Kapicioglu Z, Kaya C. The effect of posterior vitreous detachment on the prognosis of branch retinal vein occlusion. Acta Ophthalmol Scand 1997;75: Kado M, Trempe CL. Role of the vitreous in branch retinal vein occlusion. Am J Ophthalmol 1988;105: Trempe CL, Takahashi M, Topilow HW. Vitreous changes in retinal branch vein occlusion. Ophthalmology 1981;88: Kumagai K, Furukawa M, Ogino N, Larson E, Uemura A. Long-term visual outcomes after vitrectomy for macular edema with foveal hemorrhage in branch retinal vein occlusion. Retina 2007;27: Ma J, Yao K, Zhang Z, Tang X. 25-gauge vitrectomy and triamcinolone acetonide-assisted internal limiting membrane peeling for chronic cystoid macular edema associated with branch retinal vein occlusion. Retina 2008;28: Fujii GY, De Juan E Jr, Humayun MS, Pieramici DJ, ChangTS, Awh C, et al. A new 25-gauge instrument system for transconjunctival sutureless vitrectomy surgery. Ophthalmology 2002;109: Noma H, Funatsu H, Yamasaki M, Tsukamoto H, Mimura T, Sone T, et al. Pathogenesis of macular edema with branch retinal vein occlusion and intraocular levels of vascular endothelial growth factor and interleukin-6. Am J Ophthalmol 2005;140: Noma H, Minamoto A, Funatsu H, Tsukamoto H, Nakano K, Yamashita H, et al. Intravitreal levels of vascular endothelial growth factor and interleukin-6 are correlated with macular edema in branch retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol 2006;244: Ratner M. Genentech discloses safety concerns over Avastin. Nat Biotechnol 2004;22: Jaissle GB, Leitritz M, Gelisken F, Ziemssen F, Bartz-Schmidt KU, Szurman P. One-year results after intravitreal bevacizumab therapy for macular edema secondary to branch retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol 2009;247: Kondo M, Kondo N, Ito Y, Kachi S, Kikuchi M, Yasuma TR, et al. Intravitreal injection of bevacizumab for macular edema secondary to branch retinal vein occlusion: results after 12 months and multiple regression analysis. Retina 2009;29: Prager F, Michels S, Kriechbaum K, Georgopoulos M, Funk M, Geitzenauer W, et al. Intravitreal bevacizumab (Avastin) for macular oedema secondary to retinal vein occlusion: 12-month results of a prospective clinical trial. Br J Ophthalmol 2009;93: Rabena MD, Pieramici DJ, Castellarin AA, Nasir MA, Avery RL. Intravitreal bevacizumab (Avastin) in the of macular edema secondary to branch retinal vein occlusion. Retina 2007;27: Byun YJ, Roh MI, Lee SC, Koh HJ. Intravitreal triamcinolone acetonide versus bevacizumab therapy for macular edema associated with branch retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol 2010;248: Guthoff R, Meigen T, Hennemann K, Schrader W. Comparison of bevacizumab and triamcinolone for of macular edema secondary to branch retinal vein occlusion in a pair-matched analysis. Ophthalmologica 2010;224: Annals Academy of Medicine
6 25G Vitrectomy vs IVB for ME due to BRVO Tatsuhiko Sato et al Russo V, Barone A, Conte E, Prascina F, Stella A, Noci ND. Bevacizumab compared with macular laser grid photocoagulation for cystoid macular edema in branch retinal vein occlusion. Retina 2009;29: Oshima Y, Ohji M, Tano Y. Surgical outcomes of 25-gauge transconjunctival vitrectomy combined with cataract surgery for vitreoretinal diseases. Ann Acad Med Singapore 2006;35: Kadonosono K, Itoh N, Uchio E, Nakamura S, Ohno S. Staining of internal limiting membrane in macular hole surgery. Arch Ophthalmol 2000;118: Berkelman RL, Holland BW, Anderson RL. Increased bactericidal activity of dilute preparations of povidone-iodine solutions. J Clin Microbiol 1982;15: Inoue Y, Usui M, Ohashi Y, Shiota H, Yamazaki T; Preoperative Disinfection Study Group. Preoperative disinfection of the conjunctival sac with antibiotics and iodine compounds: a prospective randomized multicenter study. Jpn J Ophthalmol 2008;52: Lee SS, Ghosn C, Yu Z, Zacharias LC, Kao H, Lanni C, et al. Vitreous VEGF clearance is increased after vitrectomy. Invest Ophthalmol Vis Sci 2010;51: Gandorfer A, Messmer EM, Ulbig MW, Kampik A. Resolution of diabetic macular edema after surgical removal of the posterior hyaloid and the inner limiting membrane. Retina 2000;20: Kriechbaum K, Michels S, Prager F, Georgopoulos M, Funk M, Geitzenauer W, et al. Intravitreal Avastin for macular oedema secondary to retinal vein occlusion: a prospective study. Br J Ophthalmol 2008;92: Hoeh AE, Ach T, Schaal KB, Scheuerle AF, Dithmar S. Long-term followup of OCT-guided bevacizumab of macular edema due to retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol 2009;247: Wu L, Arevalo JF, Berrocal MH, Maia M, Roca JA, Morales-Canton V, et al. Comparison of two doses of intravitreal bevacizumab as primary for macular edema secondary to branch retinal vein occlusions: results of the Pan American Collaborative Retina Study Group at 24 months. Retina 2009;29: Nomoto H, Shiraga F, Kuno N, Kumura E, Fujii S, Shinomiya K, et al. Pharmacokinetics of bevacizumab after topical, subconjunctival and intravitreal administration in rabbits. Invest Ophthalmol Vis Sci 2009;50: Shima C, Sakaguchi H, Gomi F, Kamei M, Ikuno Y, Oshima Y, et al. Complications in patients after intravitreal injection of bevacizumab. Acta Ophthalmol 2008;86: July 2012, Vol. 41 No. 7
A retrospective nonrandomized study was conducted at 3
 Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Efficacy of intravitreal bevacizumab (Avastin TM ) for shortterm treatment of diabetic macular edema
 111 ORIGINAL Efficacy of intravitreal bevacizumab (Avastin TM ) for shortterm treatment of diabetic macular edema Toshihiko Nagasawa, Takeshi Naito, Shingo Matsushita, Hiroyuki Sato, Takashi Katome, and
111 ORIGINAL Efficacy of intravitreal bevacizumab (Avastin TM ) for shortterm treatment of diabetic macular edema Toshihiko Nagasawa, Takeshi Naito, Shingo Matsushita, Hiroyuki Sato, Takashi Katome, and
EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA
 Basrah Journal Of Surgery EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA Salah Zuhair Abed Al-Asadi MB,ChB, FICMS, Lecturer, Department of Surgery, College
Basrah Journal Of Surgery EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA Salah Zuhair Abed Al-Asadi MB,ChB, FICMS, Lecturer, Department of Surgery, College
Efficacy of combined intravitreal bevacizumab and triamcinolone for branch retinal vein occlusion
 AOP*** 1 Original Article Efficacy of combined intravitreal bevacizumab and triamcinolone for branch retinal vein occlusion Rasha I Ali1, Kapil G Kapoor 1,2, Adeel N Khan 1, Syed K Gibran 1 Purpose: To
AOP*** 1 Original Article Efficacy of combined intravitreal bevacizumab and triamcinolone for branch retinal vein occlusion Rasha I Ali1, Kapil G Kapoor 1,2, Adeel N Khan 1, Syed K Gibran 1 Purpose: To
Pars Plana Vitrectomy and Internal Limiting Membrane Peeling for Macular Oedema Secondary to Retinal Vein Occlusion: a Pilot Study
 Case Series 293 Pars Plana Vitrectomy and Internal Limiting Membrane Peeling for Macular Oedema Secondary to Retinal Vein Occlusion: a Pilot Study Xiao-Ling Liang, 1* MD, PhD, Hao-Yu Chen, 1* MD, Yong-Sheng
Case Series 293 Pars Plana Vitrectomy and Internal Limiting Membrane Peeling for Macular Oedema Secondary to Retinal Vein Occlusion: a Pilot Study Xiao-Ling Liang, 1* MD, PhD, Hao-Yu Chen, 1* MD, Yong-Sheng
Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
 European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
Vitrectomy for Diabetic Cystoid Macular Edema
 Vitrectomy for Diabetic Cystoid Macular Edema Yukihiro Sato, Zeon Lee and Hiroyuki Shimada Department of Ophthalmology, Nihon University School of Medicine, Tokyo, Japan Purpose: We evaluated visual outcomes
Vitrectomy for Diabetic Cystoid Macular Edema Yukihiro Sato, Zeon Lee and Hiroyuki Shimada Department of Ophthalmology, Nihon University School of Medicine, Tokyo, Japan Purpose: We evaluated visual outcomes
Yoshiro Minami 1*, Taiji Nagaoka 2, Akihiro Ishibazawa 1,2 and Akitoshi Yoshida 2
 Minami et al. BMC Ophthalmology (2017) 17:90 DOI 10.1186/s12886-017-0485-4 RESEARCH ARTICLE Open Access Correlation between short- and long-term effects of intravitreal ranibizumab therapy on macular edema
Minami et al. BMC Ophthalmology (2017) 17:90 DOI 10.1186/s12886-017-0485-4 RESEARCH ARTICLE Open Access Correlation between short- and long-term effects of intravitreal ranibizumab therapy on macular edema
Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients
 Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Natural Short-term Course of Recurrent Macular Edema Following Intravitreal Bevacizumab Therapy in Branch Retinal Vein Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):95-101 https://doi.org/10.3341/kjo.2017.31.2.95 Original Article Natural Short-term Course of Recurrent Macular Edema Following Intravitreal
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):95-101 https://doi.org/10.3341/kjo.2017.31.2.95 Original Article Natural Short-term Course of Recurrent Macular Edema Following Intravitreal
Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
Off-label use of intravitreal bevacizumab in non-ischemic macular edema secondary to retinal vein obstructions
 Romanian Journal of Ophthalmology, Volume 60, Issue 2, April-June 2016. pp:90-95 GENERAL ARTICLE Off-label use of intravitreal bevacizumab in non-ischemic macular edema secondary to retinal vein obstructions
Romanian Journal of Ophthalmology, Volume 60, Issue 2, April-June 2016. pp:90-95 GENERAL ARTICLE Off-label use of intravitreal bevacizumab in non-ischemic macular edema secondary to retinal vein obstructions
Clinical Outcomes After Intravitreal Bevacizumab Injection for Diabetic Macular Edema
 Original Article Clinical Outcomes After Intravitreal Bevacizumab Injection for Diabetic Macular Edema Karen Joyce G. Castro, MD, Marie Joan V. Loy, MD International Eye Institute St. Luke s Medical Center
Original Article Clinical Outcomes After Intravitreal Bevacizumab Injection for Diabetic Macular Edema Karen Joyce G. Castro, MD, Marie Joan V. Loy, MD International Eye Institute St. Luke s Medical Center
황반부부종을동반한분지망막정맥폐쇄의치료에있어서유리체강내베바시주맙의반응을예측하는인자
 Journal of Retina 2018;3(1):20-25 ORIGINAL ARTICLE pissn 2508-1926 eissn 2508-3589 황반부부종을동반한분지망막정맥폐쇄의치료에있어서유리체강내베바시주맙의반응을예측하는인자 Predictive Factors for a Favorable Response to Intravitreal Bevacizumab for
Journal of Retina 2018;3(1):20-25 ORIGINAL ARTICLE pissn 2508-1926 eissn 2508-3589 황반부부종을동반한분지망막정맥폐쇄의치료에있어서유리체강내베바시주맙의반응을예측하는인자 Predictive Factors for a Favorable Response to Intravitreal Bevacizumab for
Kyungmin Lee, Heeyoung Chung, Youngsuk Park, Joonhong Sohn. HanGil Eye Hospital, Incheon, Korea
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):298-305 http://dx.doi.org/10.3341/kjo.2014.28.4.298 Original Article Efficacy of Intravitreal Anti-vascular Endothelial Growth Factor or
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):298-305 http://dx.doi.org/10.3341/kjo.2014.28.4.298 Original Article Efficacy of Intravitreal Anti-vascular Endothelial Growth Factor or
Combined treatment for Coats disease: retinal laser photocoagulation combined with intravitreal bevacizumab injection was effective in two cases
 Kodama et al. BMC Ophthalmology 2014, 14:36 CASE REPORT Open Access Combined treatment for Coats disease: retinal laser photocoagulation combined with intravitreal bevacizumab injection was effective in
Kodama et al. BMC Ophthalmology 2014, 14:36 CASE REPORT Open Access Combined treatment for Coats disease: retinal laser photocoagulation combined with intravitreal bevacizumab injection was effective in
Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization
 Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
Macular edema (ME) is the most common
 MANAGEMENT OF RETINAL VEIN OCCLUSIONS * Peter A. Campochiaro, MD ABSTRACT Macular edema (ME) is the most common cause of reduced vision in patients with retinal vein occlusions (RVOs). The primary cause
MANAGEMENT OF RETINAL VEIN OCCLUSIONS * Peter A. Campochiaro, MD ABSTRACT Macular edema (ME) is the most common cause of reduced vision in patients with retinal vein occlusions (RVOs). The primary cause
Clinical Case Presentation. Branch Retinal Vein Occlusion. Sarita M. Registered Nurse Whangarei Base Hospital
 Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Comparison of Ranibizumab and Bevacizumab for Macular Edema Associated with Branch Retinal Vein Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(3):209-216 https://doi.org/10.3341/kjo.2015.0158 Original Article Comparison of Ranibizumab and Bevacizumab for Macular Edema Associated with
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(3):209-216 https://doi.org/10.3341/kjo.2015.0158 Original Article Comparison of Ranibizumab and Bevacizumab for Macular Edema Associated with
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
Foveal Sensitivity and Morphology in Major and Macular Branch Retinal Vein Occlusion
 Send Orders of Reprints at bspsaif@emirates.net.ae 104 The Open Ophthalmology Journal, 2012, 6, 104-109 Open Access Foveal Sensitivity and Morphology in Major and Macular Branch Retinal Vein Occlusion
Send Orders of Reprints at bspsaif@emirates.net.ae 104 The Open Ophthalmology Journal, 2012, 6, 104-109 Open Access Foveal Sensitivity and Morphology in Major and Macular Branch Retinal Vein Occlusion
Dexamethasone Intravitreal Implant Rescue Treatment for Bevacizumab Refractory Macular Edema Secondary to Branch Retinal Vein Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):108-114 https://doi.org/10.3341/kjo.2017.31.2.108 Original Article Dexamethasone Intravitreal Implant Rescue Treatment for Bevacizumab Refractory
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):108-114 https://doi.org/10.3341/kjo.2017.31.2.108 Original Article Dexamethasone Intravitreal Implant Rescue Treatment for Bevacizumab Refractory
Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution
 Hirota et al. BMC Ophthalmology 2014, 14:39 RESEARCH ARTICLE Open Access Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution Kazunari
Hirota et al. BMC Ophthalmology 2014, 14:39 RESEARCH ARTICLE Open Access Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution Kazunari
Results of bevacizumab as the primary treatment for retinal vein occlusions.
 Results of bevacizumab as the primary treatment for retinal vein occlusions. Marta S Figueroa, Inés Contreras, Susana Noval, Carolina Arruabarrena To cite this version: Marta S Figueroa, Inés Contreras,
Results of bevacizumab as the primary treatment for retinal vein occlusions. Marta S Figueroa, Inés Contreras, Susana Noval, Carolina Arruabarrena To cite this version: Marta S Figueroa, Inés Contreras,
Bevacizumab versus Dexamethasone Implant Followed by Bevacizumab for the Treatment of Macula Edema Associated with Branch Retinal Vein Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(1):29-37 https://doi.org/10.3341/kjo.2016.0134 Original Article Bevacizumab versus Dexamethasone Implant Followed by Bevacizumab for the Treatment
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(1):29-37 https://doi.org/10.3341/kjo.2016.0134 Original Article Bevacizumab versus Dexamethasone Implant Followed by Bevacizumab for the Treatment
Andrew J. Barkmeier, MD; Benjamin P. Nicholson, MA; Levent Akduman, MD
 c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS
 ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
Surgical outcome of pars plana vitrectomy: a retrospective study in a peripheral tertiary eye care centre of Nepal
 Original article : a retrospective study in a peripheral tertiary eye care centre of Nepal Subedi S 1, Sharma MK 2, Sharma BR 2, Kansakar I 2, Dhakwa K 2, Adhikari RK 2 1.Nepal Eye Hospital, National Academy
Original article : a retrospective study in a peripheral tertiary eye care centre of Nepal Subedi S 1, Sharma MK 2, Sharma BR 2, Kansakar I 2, Dhakwa K 2, Adhikari RK 2 1.Nepal Eye Hospital, National Academy
Audit of Macular Hole Surgery, Visual Outcome Prediction on OCT Appearance of Macular Hole
 International Journal of Ophthalmology & Visual Science 2017; 2(4): 93-97 http://www.sciencepublishinggroup.com/j/ijovs doi: 10.11648/j.ijovs.20170204.13 Audit of Macular Hole Surgery, Visual Outcome Prediction
International Journal of Ophthalmology & Visual Science 2017; 2(4): 93-97 http://www.sciencepublishinggroup.com/j/ijovs doi: 10.11648/j.ijovs.20170204.13 Audit of Macular Hole Surgery, Visual Outcome Prediction
Vitrectomy Combined with Intravitreal Triamcinolone Acetonide Injection and Macular Laser Photocoagulation for Nontractional Diabetic Macular Edema
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(3):186-193 http://dx.doi.org/10.3341/kjo.2013.27.3.186 Original Article Vitrectomy Combined with Intravitreal Triamcinolone Acetonide Injection
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(3):186-193 http://dx.doi.org/10.3341/kjo.2013.27.3.186 Original Article Vitrectomy Combined with Intravitreal Triamcinolone Acetonide Injection
Venturi versus peristaltic pumps 33 vitrectomy dynamics 34 Fluorescein, vitreous staining 120
 Subject Index Accurus 35, 83 Aflibercept, diabetic macular edema management 167, 168 Air-forced infusion, Stellaris PC 12, 13 Alcon Constellation, see Constellation system Autoclave sterilization lens
Subject Index Accurus 35, 83 Aflibercept, diabetic macular edema management 167, 168 Air-forced infusion, Stellaris PC 12, 13 Alcon Constellation, see Constellation system Autoclave sterilization lens
Intravitreal versus Posterior Subtenon Injection of Triamcinolone Acetonide for Diabetic Macular Edema
 Intravitreal versus Posterior Subtenon Injection of Triamcinolone Acetonide for Diabetic Macular Edema Young Jae Choi, MD, In Kyung Oh, MD, Jae Ryung Oh, MD, PhD, Kuhl Huh, MD, PhD Department of Ophthalmology,
Intravitreal versus Posterior Subtenon Injection of Triamcinolone Acetonide for Diabetic Macular Edema Young Jae Choi, MD, In Kyung Oh, MD, Jae Ryung Oh, MD, PhD, Kuhl Huh, MD, PhD Department of Ophthalmology,
COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY
 Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Research Article Long-Term Outcome after Vitrectomy for Macular Edema with Retinal Vein Occlusion Dividing into the Occlusion Site
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2014, Article ID 198782, 6 pages http://dx.doi.org/10.1155/2014/198782 Research Article Long-Term Outcome after Vitrectomy for Macular Edema
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2014, Article ID 198782, 6 pages http://dx.doi.org/10.1155/2014/198782 Research Article Long-Term Outcome after Vitrectomy for Macular Edema
Efficacy and safety of Pro Re Nata regimen without loading dose ranibizumab injections in retinal vein occlusion
 Open Access Original Article Efficacy and safety of Pro Re Nata regimen without loading dose ranibizumab injections in retinal vein occlusion Erkan Unsal 1, Kadir Eltutar 2, Pınar Sultan 3, Hulya Gungel
Open Access Original Article Efficacy and safety of Pro Re Nata regimen without loading dose ranibizumab injections in retinal vein occlusion Erkan Unsal 1, Kadir Eltutar 2, Pınar Sultan 3, Hulya Gungel
VMA at the macula resulting in VMT
 Ocriplasmina for pharmacologic treatment in VMT Teresio Avitabile 1 Introduction PVD is a normal, physiologic process that occurs with aging; however, in some cases, PVD is incomplete Incomplete PVD localized
Ocriplasmina for pharmacologic treatment in VMT Teresio Avitabile 1 Introduction PVD is a normal, physiologic process that occurs with aging; however, in some cases, PVD is incomplete Incomplete PVD localized
Quantitative Reduction in Central Foveal Thickness After First Anti-VEGF Injection as a Predictor of Final Outcome in BRVO Patients
 Original clinical study Quantitative Reduction in Central Foveal Thickness After First Anti-VEGF Injection as a Predictor of Final Outcome in BRVO Patients Rupak Roy, MS, Kumar Saurabh, MS, Avirupa Ghose,
Original clinical study Quantitative Reduction in Central Foveal Thickness After First Anti-VEGF Injection as a Predictor of Final Outcome in BRVO Patients Rupak Roy, MS, Kumar Saurabh, MS, Avirupa Ghose,
Bevacizumab for Macular Edema in Branch and Central Retinal Vein Occlusion
 RESEARCH ARTICLE Acta Medica Marisiensis 2012;58(5):329-333 Bevacizumab for Macular Edema in Branch and Central Retinal Vein Occlusion Rusu Monica-Blanka 1, Egyed ZsI 2, Maki Cristina 1 1 Ophthalmology
RESEARCH ARTICLE Acta Medica Marisiensis 2012;58(5):329-333 Bevacizumab for Macular Edema in Branch and Central Retinal Vein Occlusion Rusu Monica-Blanka 1, Egyed ZsI 2, Maki Cristina 1 1 Ophthalmology
Case Report Macular Oedema Related to Idiopathic Macular Telangiectasia Type 1 Treated with Dexamethasone Intravitreal Implant (Ozurdex)
 Case Reports in Ophthalmological Medicine, Article ID 231913, 5 pages http://dx.doi.org/10.1155/2014/231913 Case Report Macular Oedema Related to Idiopathic Macular Telangiectasia Type 1 Treated with Dexamethasone
Case Reports in Ophthalmological Medicine, Article ID 231913, 5 pages http://dx.doi.org/10.1155/2014/231913 Case Report Macular Oedema Related to Idiopathic Macular Telangiectasia Type 1 Treated with Dexamethasone
Efficacy of Anti-VEGF Agents in the Treatment of Age-Related Macular Degeneration
 Efficacy of Anti-VEGF Agents in the Treatment of Age-Related Macular Degeneration Marilita M. Moschos Abstract- Purpose: To evaluate by OCT and mf-erg the macular function in eyes with CNV due to ARMD
Efficacy of Anti-VEGF Agents in the Treatment of Age-Related Macular Degeneration Marilita M. Moschos Abstract- Purpose: To evaluate by OCT and mf-erg the macular function in eyes with CNV due to ARMD
Scott M. Pfahler D.O. Dayton Vitreo-Retinal Associates AOCOO-HNS Palm Springs, CA 2012
 Scott M. Pfahler D.O. Dayton Vitreo-Retinal Associates AOCOO-HNS Palm Springs, CA 2012 Proliferative Diabetic Retinopathy Laser Treatments Medical Treatment Surgical Treatment Diabetic Macular Edema Laser
Scott M. Pfahler D.O. Dayton Vitreo-Retinal Associates AOCOO-HNS Palm Springs, CA 2012 Proliferative Diabetic Retinopathy Laser Treatments Medical Treatment Surgical Treatment Diabetic Macular Edema Laser
CLINICAL SCIENCES. Visual Field Defects After Intravitreous Administration of Indocyanine Green in Macular Hole Surgery
 CLINICAL SCIENCES Visual Field Defects After Intravitreous Administration of Indocyanine Green in Macular Hole Surgery Shigeru Kanda, MD; Akinori Uemura, MD; Takehiro Yamashita, MD; Hazuki Kita, MD; Keita
CLINICAL SCIENCES Visual Field Defects After Intravitreous Administration of Indocyanine Green in Macular Hole Surgery Shigeru Kanda, MD; Akinori Uemura, MD; Takehiro Yamashita, MD; Hazuki Kita, MD; Keita
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
OCT Assessment of the Vitreoretinal Relationship in CSME
 December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
Visual and Anatomical Outcomes of Vitreous Surgery for Large Macular Holes
 March 2009 Raju K.V. et al. - Closed Globe Injuries 31 ORIGINAL ARTICLE Visual and Anatomical Outcomes of Vitreous Surgery for Large Macular Holes Dr. Mahesh G. MS DO DNB FRCSEd, Dr. A. Giridhar MS, Dr.
March 2009 Raju K.V. et al. - Closed Globe Injuries 31 ORIGINAL ARTICLE Visual and Anatomical Outcomes of Vitreous Surgery for Large Macular Holes Dr. Mahesh G. MS DO DNB FRCSEd, Dr. A. Giridhar MS, Dr.
Oishi A, Miyamoto K, Yoshimura N. Etiology of carotid cavernous fistula in Japanese. Jpn J Ophthalmol. 2009;53:40-43.
 Kimura T, Takagi H, Miyamoto K, Kita M, Watanabe D, Yoshimura N. Macular hole with epiretinal membrane after triamcinolone-assisted vitrectomy for proliferative diabetic retinopathy. Retinal Cases Brief
Kimura T, Takagi H, Miyamoto K, Kita M, Watanabe D, Yoshimura N. Macular hole with epiretinal membrane after triamcinolone-assisted vitrectomy for proliferative diabetic retinopathy. Retinal Cases Brief
Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases
 Original Article Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases Syed Raza Ali Shah, Nadeem Ahmad, Qasim Lateef Chaudry, Chaudary Nasir Ahmad, Asad
Original Article Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases Syed Raza Ali Shah, Nadeem Ahmad, Qasim Lateef Chaudry, Chaudary Nasir Ahmad, Asad
Vitrectomy Combined with Phacoemulsification and Intraocular Lens Implantation for Diabetic Macular Edema
 Vitrectomy Combined with Phacoemulsification and Intraocular Lens Implantation for Diabetic Macular Edema Kentaro Amino* and Hidenobu Tanihara *Amino Eye Clinic, Shimonoseki, Yamaguchi Prefecture, Japan;
Vitrectomy Combined with Phacoemulsification and Intraocular Lens Implantation for Diabetic Macular Edema Kentaro Amino* and Hidenobu Tanihara *Amino Eye Clinic, Shimonoseki, Yamaguchi Prefecture, Japan;
The Foundation WHAT IS THE RETINA? continued next page. RETINA HEALTH SERIES Facts from the ASRS
 The Foundation American Society of Retina Specialists Committed to improving the quality of life of all people with retinal disease. Intravitreal Injections An intravitreal (pronounced in tra VIT re al)
The Foundation American Society of Retina Specialists Committed to improving the quality of life of all people with retinal disease. Intravitreal Injections An intravitreal (pronounced in tra VIT re al)
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
Recalcitrant Diabetic Macular Oedema: Therapeutic Options
 December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
CSME BCVA. OCT Bevacizumab CMT CMT BCVA. BCVA LogMAR. p CMT NPDR PDR PDR. Bevacizumab PDR FDA. Ranibizumab. Bevacizumab.
 email: rezaj76@yahoo.com Bevacizumab FDA mg Ranibizumab - Bevacizumab NPDR PDR PDR PDR CSME FAZFA BCVA CMT OCT Bevacizumab BCVA CMT BCVA LogMAR p CMT p CSME CRVO CSME BRVO CRVOBRVO (fovea avascular zone)
email: rezaj76@yahoo.com Bevacizumab FDA mg Ranibizumab - Bevacizumab NPDR PDR PDR PDR CSME FAZFA BCVA CMT OCT Bevacizumab BCVA CMT BCVA LogMAR p CMT p CSME CRVO CSME BRVO CRVOBRVO (fovea avascular zone)
Intravitreal bevacizumab for pediatric exudative retinal diseases
 Saudi Journal of Ophthalmology (2011) 25, 193 197 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE Intravitreal bevacizumab
Saudi Journal of Ophthalmology (2011) 25, 193 197 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE Intravitreal bevacizumab
Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema
 Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
Retinal pigment epithelial tears after intravitreal bevacizumab injection for exudative age-related macular degeneration.
 Thomas Jefferson University Jefferson Digital Commons Wills Eye Institute Papers Wills Eye Institute 4-1-2008 Retinal pigment epithelial tears after intravitreal bevacizumab injection for exudative age-related
Thomas Jefferson University Jefferson Digital Commons Wills Eye Institute Papers Wills Eye Institute 4-1-2008 Retinal pigment epithelial tears after intravitreal bevacizumab injection for exudative age-related
Vitrectomy for Diabetic Retinopathy The current role of pars plana vitrectomy for diabetic macular edema and proliferative diabetic retinopathy.
 Vitrectomy for Diabetic Retinopathy The current role of pars plana vitrectomy for diabetic macular edema and proliferative diabetic retinopathy. Y R.V. PUL CHN, MD; ND DONLD J. D MICO, MD The incidence
Vitrectomy for Diabetic Retinopathy The current role of pars plana vitrectomy for diabetic macular edema and proliferative diabetic retinopathy. Y R.V. PUL CHN, MD; ND DONLD J. D MICO, MD The incidence
PREDICTORS OF VISUAL RESPONSE TO INTRAVITREAL BEVACIZUMAB FOR TREATMENT OF DIABETIC MACULAR EDEMA
 ORIGINAL ARTICLE PREDICTORS OF VISUAL RESPONSE TO INTRAVITREAL BEVACIZUMAB FOR TREATMENT OF DIABETIC MACULAR EDEMA Sunny Kumar Gupta 1,*, Ishan Yadav 2, Sujit Deshmukh 3, Rajendra P Maurya 4, V P Singh
ORIGINAL ARTICLE PREDICTORS OF VISUAL RESPONSE TO INTRAVITREAL BEVACIZUMAB FOR TREATMENT OF DIABETIC MACULAR EDEMA Sunny Kumar Gupta 1,*, Ishan Yadav 2, Sujit Deshmukh 3, Rajendra P Maurya 4, V P Singh
Effects of an Intravitreal Bevacizumab Injection Combined With Panretinal Photocoagulation on High-Risk Proliferative Diabetic Retinopathy
 Korean Journal of Ophthalmology 2009;23:266-272 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.4.266 Effects of an Intravitreal Bevacizumab Injection Combined With Panretinal Photocoagulation on High-Risk
Korean Journal of Ophthalmology 2009;23:266-272 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.4.266 Effects of an Intravitreal Bevacizumab Injection Combined With Panretinal Photocoagulation on High-Risk
Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD
 Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
Eccentric Macular Hole after Pars Plana Vitrectomy for Epiretinal Membrane Without Internal Limiting Membrane Peeling: A Case Report
 Ophthalmol Ther (2017) 6:391 395 DOI 10.1007/s40123-017-0113-7 CASE REPORT Eccentric Macular Hole after Pars Plana Vitrectomy for Epiretinal Membrane Without Internal Limiting Membrane Peeling: A Case
Ophthalmol Ther (2017) 6:391 395 DOI 10.1007/s40123-017-0113-7 CASE REPORT Eccentric Macular Hole after Pars Plana Vitrectomy for Epiretinal Membrane Without Internal Limiting Membrane Peeling: A Case
Perioperative Use of Bevacizumab in Vitrectomy for Proliferative Diabetic Retinopathy: A Literature review
 Perioperative Use of Bevacizumab in Vitrectomy for Proliferative Diabetic Retinopathy: A Literature review Khalil Ghasemi Falavarjani, MD 1 Mehdi Modarres, MD 2 Abstract Purpose: To review the effectiveness
Perioperative Use of Bevacizumab in Vitrectomy for Proliferative Diabetic Retinopathy: A Literature review Khalil Ghasemi Falavarjani, MD 1 Mehdi Modarres, MD 2 Abstract Purpose: To review the effectiveness
EPIRETINAL MEMBRANE & VITREOMACULAR TRACTION
 EPIRETINAL MEMBRANE & VITREOMACULAR TRACTION Management of ERM and VMT K.V.Chalam,MD,PhD,MBA,FACS Professor and Director of Retina Loma Linda Eye Institute Los Angeles, USA REVIEW ANATOMY The vitreous
EPIRETINAL MEMBRANE & VITREOMACULAR TRACTION Management of ERM and VMT K.V.Chalam,MD,PhD,MBA,FACS Professor and Director of Retina Loma Linda Eye Institute Los Angeles, USA REVIEW ANATOMY The vitreous
Long-term Outcomes of Vitreous Floaters Management with 23-Gauge Transconjunctival Sutureless Vitrectomy
 Long-term Outcomes of Vitreous Floaters Management with 23-Gauge Transconjunctival Sutureless Vitrectomy Malhar 1Consultant 1 Soni, Minas G 2 Georgopoulos, Adriana 2 Kovakova Vitreo-Retinal Surgeon, London,
Long-term Outcomes of Vitreous Floaters Management with 23-Gauge Transconjunctival Sutureless Vitrectomy Malhar 1Consultant 1 Soni, Minas G 2 Georgopoulos, Adriana 2 Kovakova Vitreo-Retinal Surgeon, London,
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Title. Author(s)Saito, Wataru; Kase, Satoru; Ohgami, Kazuhiro; Mori, CitationActa Ophthalmologica, 88(3): Issue Date Doc URL.
 Title Intravitreal anti-vascular endothelial growth factor oedema Author(s)Saito, Wataru; Kase, Satoru; Ohgami, Kazuhiro; Mori, CitationActa Ophthalmologica, 88(3): 377-380 Issue Date 2010-05 Doc URL http://hdl.handle.net/2115/45372
Title Intravitreal anti-vascular endothelial growth factor oedema Author(s)Saito, Wataru; Kase, Satoru; Ohgami, Kazuhiro; Mori, CitationActa Ophthalmologica, 88(3): 377-380 Issue Date 2010-05 Doc URL http://hdl.handle.net/2115/45372
Low Illumination 3-D Heads-Up Vitrectomy for Diabetic Macular Edema
 Low Illumination 3-D Heads-Up Vitrectomy for Diabetic Macular Edema Yoshihiro Yonekawa, M.D., Bozho Todorich, M.D., Ph.D., Jeremy D. Wolfe, M.D. Yoshihiro Yonekawa, M.D., is a vitreoretinal surgeon at
Low Illumination 3-D Heads-Up Vitrectomy for Diabetic Macular Edema Yoshihiro Yonekawa, M.D., Bozho Todorich, M.D., Ph.D., Jeremy D. Wolfe, M.D. Yoshihiro Yonekawa, M.D., is a vitreoretinal surgeon at
Vitrectomy in vitreomacular traction syndrome evaluated by ocular coherence tomography (OCT) retinal mapping.
 Vitrectomy in vitreomacular traction syndrome evaluated by ocular coherence tomography (OCT) retinal mapping. Larsson, Jörgen Published in: Acta Ophthalmologica Scandinavica DOI: 10.1111/j.1600-0420.2004.00344.x
Vitrectomy in vitreomacular traction syndrome evaluated by ocular coherence tomography (OCT) retinal mapping. Larsson, Jörgen Published in: Acta Ophthalmologica Scandinavica DOI: 10.1111/j.1600-0420.2004.00344.x
Christina L. Ryu, 1 Adrian Elfersy, 1 Uday Desai, 1 Thomas Hessburg, 1 Paul Edwards, 1 and Hua Gao 1,2. 1. Introduction
 Ophthalmology, Article ID 317694, 6 pages http://dx.doi.org/10.1155/2014/317694 Research Article The Effect of Antivascular Endothelial Growth Factor Therapy on the Development of Neovascular Glaucoma
Ophthalmology, Article ID 317694, 6 pages http://dx.doi.org/10.1155/2014/317694 Research Article The Effect of Antivascular Endothelial Growth Factor Therapy on the Development of Neovascular Glaucoma
Anti VEGF Agents in Retinal Disorders Current Scenario
 Retina Anti VEGF Agents in Retinal Disorders Current Scenario Charu Gupta MS Charu Gupta MS, Cyrus M. Shroff MD Shroff Eye Centre, New Delhi T is a group of proteins involved in the regulation of angiogenesis,
Retina Anti VEGF Agents in Retinal Disorders Current Scenario Charu Gupta MS Charu Gupta MS, Cyrus M. Shroff MD Shroff Eye Centre, New Delhi T is a group of proteins involved in the regulation of angiogenesis,
Five-year Outcomes of Ranibizumab in Neovascular Age-related Macular Degeneration: Real Life Clinical Experience
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(5):424-430 https://doi.org/10.3341/kjo.2016.0125 Original Article Five-year Outcomes of Ranibizumab in Neovascular Age-related Macular Degeneration:
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(5):424-430 https://doi.org/10.3341/kjo.2016.0125 Original Article Five-year Outcomes of Ranibizumab in Neovascular Age-related Macular Degeneration:
Vascular Disease Ocular Manifestations of Systemic Hypertension
 Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
Wataru Kobayashi, MD,* Hiroshi Kunikata, MD, PhD,* Toshiaki Abe, MD, PhD,Þ and Toru Nakazawa, MD, PhD*
 ORIGINAL CLINICAL STUDY Retrospective Comparison of 25- and 23-Gauge Microincision Vitrectomy Surgery and 20-Gauge Vitrectomy for the Repair of Macular Hole Retinal Detachment Wataru Kobayashi, MD,* Hiroshi
ORIGINAL CLINICAL STUDY Retrospective Comparison of 25- and 23-Gauge Microincision Vitrectomy Surgery and 20-Gauge Vitrectomy for the Repair of Macular Hole Retinal Detachment Wataru Kobayashi, MD,* Hiroshi
CLINICAL COURSE OF VITREOMACULAR ADHESION MANAGED BY INITIAL OBSERVATION
 CLINICAL COURSE OF VITREOMACULAR ADHESION MANAGED BY INITIAL OBSERVATION VISHAK J. JOHN, MD,* HARRY W. FLYNN, JR., MD,* WILLIAM E. SMIDDY, MD,* ADAM CARVER, MD, ROBERT LEONARD, MD, HOMAYOUN TABANDEH, MD,
CLINICAL COURSE OF VITREOMACULAR ADHESION MANAGED BY INITIAL OBSERVATION VISHAK J. JOHN, MD,* HARRY W. FLYNN, JR., MD,* WILLIAM E. SMIDDY, MD,* ADAM CARVER, MD, ROBERT LEONARD, MD, HOMAYOUN TABANDEH, MD,
CORRELATION BETWEEN CENTRAL FOVEAL THICKNESS AND VISUAL ACUITY IN PATIENTS WITH IDIOPATHIC VITREOMACULAR TRACTION
 CORRELATION BETWEEN CENTRAL FOVEAL THICKNESS AND VISUAL ACUITY IN PATIENTS WITH IDIOPATHIC VITREOMACULAR TRACTION MEHMET M. UZEL, MD, MEHMET CITIRIK, MD, CAGRI ILHAN, MD, KEMAL TEKIN, MD Purpose: To evaluate
CORRELATION BETWEEN CENTRAL FOVEAL THICKNESS AND VISUAL ACUITY IN PATIENTS WITH IDIOPATHIC VITREOMACULAR TRACTION MEHMET M. UZEL, MD, MEHMET CITIRIK, MD, CAGRI ILHAN, MD, KEMAL TEKIN, MD Purpose: To evaluate
 Research Article http://www.alliedacademies.org/clinical-ophthalmology-and-vision-science/ A 2-year retrospective study of the treatment of retinal vein occlusion with dexamethasone 0.7 mg intravitreal
Research Article http://www.alliedacademies.org/clinical-ophthalmology-and-vision-science/ A 2-year retrospective study of the treatment of retinal vein occlusion with dexamethasone 0.7 mg intravitreal
Early surgery preserves more vision for patients with Epiretinal Membranes
 Early surgery preserves more vision for patients with Epiretinal Membranes Rahman R 1, Stephenson J 2 KEYWORDS: Epiretinal membrane, Combined phakovitrectomy, OCT. Addresses: 1 Ms Rubina Rahman*, CalderdaleRoyalHospital,
Early surgery preserves more vision for patients with Epiretinal Membranes Rahman R 1, Stephenson J 2 KEYWORDS: Epiretinal membrane, Combined phakovitrectomy, OCT. Addresses: 1 Ms Rubina Rahman*, CalderdaleRoyalHospital,
Clinical Study Air Bubble Technique for Fundus Visualization during Vitrectomy in Aphakia
 Hindawi Ophthalmology Volume 2017, Article ID 4721540, 5 pages https://doi.org/10.1155/2017/4721540 Clinical Study Air Bubble Technique for Fundus Visualization during Vitrectomy in Aphakia Mahmoud Mohamed
Hindawi Ophthalmology Volume 2017, Article ID 4721540, 5 pages https://doi.org/10.1155/2017/4721540 Clinical Study Air Bubble Technique for Fundus Visualization during Vitrectomy in Aphakia Mahmoud Mohamed
Y O R K. Health Economics C O N S O R T I U M NOVARTIS. Bevacizumab (Avastin) for Macular Edema Secondary to RVO
 Y O R K Health Economics C O N S O R T I U M NOVARTIS Bevacizumab (Avastin) for Macular Edema Secondary to RVO Review of Evidence on Clinical Effectiveness and Safety from Non-Randomised Controlled Trials
Y O R K Health Economics C O N S O R T I U M NOVARTIS Bevacizumab (Avastin) for Macular Edema Secondary to RVO Review of Evidence on Clinical Effectiveness and Safety from Non-Randomised Controlled Trials
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 78/ Sept 28, 2015 Page 13570
 SAFETY AND EFFECTIVENESS OF 20G SUTURELESS PARS PLANA VITRECTOMY: A PROSPECTIVE STUDY AT SAROJINI DEVI HOSPITAL, HYDERABAD Rajalingam Vairagyam 1, Karunakar B 2, Pasyanthi B 3, B. Y. Babu Rao 4, Rita Bahadur
SAFETY AND EFFECTIVENESS OF 20G SUTURELESS PARS PLANA VITRECTOMY: A PROSPECTIVE STUDY AT SAROJINI DEVI HOSPITAL, HYDERABAD Rajalingam Vairagyam 1, Karunakar B 2, Pasyanthi B 3, B. Y. Babu Rao 4, Rita Bahadur
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Early Avastin management in acute retinal vein occlusion
 Saudi Journal of Ophthalmology (2010) 24, 87 94 King Saud University Saudi Journal of Ophthalmology www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE Early Avastin management in acute retinal vein
Saudi Journal of Ophthalmology (2010) 24, 87 94 King Saud University Saudi Journal of Ophthalmology www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE Early Avastin management in acute retinal vein
Research Article Differentiation between Good and Low-Responders to Intravitreal Ranibizumab for Macular Edema Secondary to Retinal Vein Occlusion
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 9875741, 6 pages http://dx.doi.org/10.1155/2016/9875741 Research Article Differentiation between Good and Low-Responders
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 9875741, 6 pages http://dx.doi.org/10.1155/2016/9875741 Research Article Differentiation between Good and Low-Responders
Bevacizumab for Macular Edema in Central Retinal Vein Occlusion: A Prospective, Randomized, Double-Masked Clinical Study
 Bevacizumab for Macular Edema in Central Retinal Vein Occlusion: A Prospective, Randomized, Double-Masked Clinical Study David L.J. Epstein, MD, Peep V. Algvere, MD, PhD, Gunvor von Wendt, MD, PhD, Stefan
Bevacizumab for Macular Edema in Central Retinal Vein Occlusion: A Prospective, Randomized, Double-Masked Clinical Study David L.J. Epstein, MD, Peep V. Algvere, MD, PhD, Gunvor von Wendt, MD, PhD, Stefan
Anatomical results and complications after silicone oil removal
 Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
Diabetic eye disease. Diabetic retinopathy. Sam S. Dahr, M.D. Retina Center of Oklahoma.
 Diabetic eye disease Sam S. Dahr, M.D. Retina Center of Oklahoma www.rcoklahoma.com Downloaded from: The Retina (on 28 May 2007 12:48 AM) 2007 Elsevier Diabetic retinopathy Downloaded from: The Retina
Diabetic eye disease Sam S. Dahr, M.D. Retina Center of Oklahoma www.rcoklahoma.com Downloaded from: The Retina (on 28 May 2007 12:48 AM) 2007 Elsevier Diabetic retinopathy Downloaded from: The Retina
Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation
 Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation Murat Dogru, Makoto Nakamura, Masanori Inoue and Misao Yamamoto Department of Ophthalmology, Kobe
Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation Murat Dogru, Makoto Nakamura, Masanori Inoue and Misao Yamamoto Department of Ophthalmology, Kobe
PREDICTIVE FACTORS OF VISUAL OUTCOME FOR VITREOMACULAR TRACTION SYNDROME AFTER VITRECTOMY
 PREDICTIVE FACTORS OF VISUAL OUTCOME FOR VITREOMACULAR TRACTION SYNDROME AFTER VITRECTOMY Downloaded from https://journals.lww.com/retinajournal by mv7bzw+nz2blpko//cqyhwu2mokppdiwuep6ir1molueskh0dp9rbmb7dum5a2/cp6zifirtq3zbawzt+95f/m61fycawpqbpe8y2wuyzwnns2gw3+gmrxei6x11wu+s
PREDICTIVE FACTORS OF VISUAL OUTCOME FOR VITREOMACULAR TRACTION SYNDROME AFTER VITRECTOMY Downloaded from https://journals.lww.com/retinajournal by mv7bzw+nz2blpko//cqyhwu2mokppdiwuep6ir1molueskh0dp9rbmb7dum5a2/cp6zifirtq3zbawzt+95f/m61fycawpqbpe8y2wuyzwnns2gw3+gmrxei6x11wu+s
Macular Hole Associated with Vogt-Koyanagi-Harada Disease at the Acute Uveitic Stage
 Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Foveal Red Spot, Macular Microhole and Foveal Photoreceptor Defect in the Era of High-Resolution Optical Coherence Tomography
 1:15 PM Foveal Red Spot, Macular Microhole and Foveal Photoreceptor Defect in the Era of High-Resolution Optical Coherence Tomography Edward F. Hall, MD Steven J. Rose, MD Brian P. Connolly, MD Ernest
1:15 PM Foveal Red Spot, Macular Microhole and Foveal Photoreceptor Defect in the Era of High-Resolution Optical Coherence Tomography Edward F. Hall, MD Steven J. Rose, MD Brian P. Connolly, MD Ernest
Scleral Buckling Using a Non-contact Wide-Angle Viewing System with a 25-Gauge Chandelier Endoilluminator
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(6):533-537 https://doi.org/10.3341/kjo.2017.0044 Original Article Scleral Buckling Using a Non-contact Wide-Angle Viewing System with a 25-Gauge
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(6):533-537 https://doi.org/10.3341/kjo.2017.0044 Original Article Scleral Buckling Using a Non-contact Wide-Angle Viewing System with a 25-Gauge
Survey of Surgical Indications and Results of Primary Pars Plana Vitrectomy for Rhegmatogenous Retinal Detachments
 Survey of Surgical Indications and Results of Primary Pars Plana Vitrectomy for Rhegmatogenous Retinal Detachments Yusuke Oshima, Kazuyuki Emi, Masanobu Motokura and Shigeki Yamanishi Department of Ophthalmology,
Survey of Surgical Indications and Results of Primary Pars Plana Vitrectomy for Rhegmatogenous Retinal Detachments Yusuke Oshima, Kazuyuki Emi, Masanobu Motokura and Shigeki Yamanishi Department of Ophthalmology,
LENS CAPSULAR FLAP TRANSPLANTATION IN THE MANAGEMENT OF REFRACTORY MACULAR HOLE FROM MULTIPLE ETIOLOGIES
 LENS CAPSULAR FLAP TRANSPLANTATION IN THE MANAGEMENT OF REFRACTORY MACULAR HOLE FROM MULTIPLE ETIOLOGIES SAN-NI CHEN, MD,* CHUNG-MAY YANG, MD Purpose: To report the clinical results of lens capsular flap
LENS CAPSULAR FLAP TRANSPLANTATION IN THE MANAGEMENT OF REFRACTORY MACULAR HOLE FROM MULTIPLE ETIOLOGIES SAN-NI CHEN, MD,* CHUNG-MAY YANG, MD Purpose: To report the clinical results of lens capsular flap
In the treatment of neovascular and. Original Research
 Original Research Hellenic J Cardiol 2013; 54: 435-440 Influence of Intravitreal Injection of Bevacizumab on Systemic Blood Pressure Changes in Patients with Exudative Form of Age-Related Macular Degeneration
Original Research Hellenic J Cardiol 2013; 54: 435-440 Influence of Intravitreal Injection of Bevacizumab on Systemic Blood Pressure Changes in Patients with Exudative Form of Age-Related Macular Degeneration
Comparison between 23 Gauge and 25 Gauge Pars Plana Vitrectomy for Posterior Segment Disease
 Original Article Comparison between 23 Gauge and 25 Gauge Pars Plana Vitrectomy for Posterior Segment Disease Huma Kayani, Aamir Ahmed, Kashif Jahangir, Hizb-ur-Rehman, Khurram Chauhan Pak J Ophthalmol
Original Article Comparison between 23 Gauge and 25 Gauge Pars Plana Vitrectomy for Posterior Segment Disease Huma Kayani, Aamir Ahmed, Kashif Jahangir, Hizb-ur-Rehman, Khurram Chauhan Pak J Ophthalmol
Early diagnosis and treatment of VMT with single Intravitreal Injection of Pharmacologic Vitreolysis. Stratos Gotzaridis MD Athens
 Early diagnosis and treatment of VMT with single Intravitreal Injection of Pharmacologic Vitreolysis Stratos Gotzaridis MD Athens The Vitreous Body Gel composed of 98-99% water 1% macromolecules Glycoproteins
Early diagnosis and treatment of VMT with single Intravitreal Injection of Pharmacologic Vitreolysis Stratos Gotzaridis MD Athens The Vitreous Body Gel composed of 98-99% water 1% macromolecules Glycoproteins
Original Article. Authors
 Original Article APMC-303 Efficacy of Intra-Vitreal Bevacizumab Combined with Phaco- Emulsification in the Prophylaxis of Macular Edema in Patients with Non-Proliferative Diabetic Retinopathy Muhammad
Original Article APMC-303 Efficacy of Intra-Vitreal Bevacizumab Combined with Phaco- Emulsification in the Prophylaxis of Macular Edema in Patients with Non-Proliferative Diabetic Retinopathy Muhammad
Ophthalmology Macular Pathways
 Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
T.O. Romanova, a Post Graduate student
 Criteria of severity for macular edema associated with retinal vein occlusion: cohort heterogeneity and efficacy evaluation of threshold and subthreshold retinal laser photocoagulation depending on the
Criteria of severity for macular edema associated with retinal vein occlusion: cohort heterogeneity and efficacy evaluation of threshold and subthreshold retinal laser photocoagulation depending on the
Optical Coherence Tomography (OCT) in Uveitis Piergiorgio Neri, BMedSc, MD, PhD Head Ocular Immunology Unit
 The Eye Clinic Polytechnic University of Marche Head: Prof Alfonso Giovannini November, 1991 Optical Coherence Tomography (OCT) in Uveitis Piergiorgio Neri, BMedSc, MD, PhD Head Ocular Immunology Unit
The Eye Clinic Polytechnic University of Marche Head: Prof Alfonso Giovannini November, 1991 Optical Coherence Tomography (OCT) in Uveitis Piergiorgio Neri, BMedSc, MD, PhD Head Ocular Immunology Unit
