Emergency department procedural sedation for primary electrical cardioversion a comparison with procedural sedations for other reasons
|
|
|
- Margery Gaines
- 5 years ago
- Views:
Transcription
1 World J Emerg Med, Vol 8, No 3, 07 Original Article 65 Emergency department procedural sedation for primary electrical cardioversion a comparison with procedural sedations for other reasons Michael Butler,, Patrick Froese, Peter Zed 3,4, George Kovacs, Robert MacKinley, Kirk Magee, Mary-Lynn Watson, Samuel G. Campbell Department of Emergency Medicine, Faculty of Medicine, Dalhousie University, Halifax, Nova Scotia B3H 3A6, Canada Department of Undergraduate Medicine, Faculty of Medicine, Dalhousie University, Halifax, Nova Scotia B3H 3A6, Canada 3 Faculty of Pharmaceutical Sciences, University of British Columbia, Vancouver, British Columbia V6T Z3, Canada 4 Department of Emergency Medicine, Faculty of Medicine, University of British Columbia, Vancouver, British Columbia V6T Z3, Canada Corresponding Author: Samuel G. Campbell, samuel.campbell@cdha.nshealth.ca BACKGROUND: Atrial fibrillation (AF) is the most common arrhythmia treated in the emergency department (ED), with primary electrical cardioversion (PEC) the preferred method of rhythm control. Anecdotally, patients undergoing ED procedural sedation (EDPS) for PEC differ from those requiring EDPS for other procedures: they are at higher risk of adverse events, and require fewer drugs and lower doses. We attempt to verify this using an EDPS registry at a Canadian, tertiary care teaching hospital. METHODS: This is a retrospective review of patients that underwent EDPS for the period of June 006 to September 04. We compared demographics, medication use and intra-procedural adverse events between those receiving EDPS for PEC for AF compared to that for other indications. We report the asssociation between AEs and predictors using logistic regression. RESULTS: A total of patients were included, 74 for PEC for AF and 4 53 for other indications. PEC patients were more likely male (58.5% vs. 47.%), older (59.5 years vs. 48. years), and less likely to be ASA I (46.6% vs. 69.0%). PEC patients received smaller doses of propofol and less likely to receive adjuvant analgesic therapy (.5% vs. 78.%). PEC patients were more likely to experience hypotension (7.6% vs. 6.5%) but respiratory AEs (apnea, hypoxia and airway intervention) were not different. CONCLUSION: EDPS for PEC differs from that conducted for other purposes: patients tend to be less healthy, receive smaller doses of medication and more likely to suffer hypotension without an increase in respiratory AEs. These factors should be considered when performing EDPS. KEY WORDS: Procedural sedation; Atrial fi brillation; Electrical cardioversion World J Emerg Med 07;8(3):65 69 DOI: /wjem.j INTRODUCTION Atrial Fibrillation (AF) is the most common arrhythmia treated in the emergency department (ED). [] Recent years have seen a move toward primary electrical cardioversion (PEC) of the condition in the ED, fuelled by both recognition of the limitations of chemical 07 World Journal of Emergency Medicine cardioversion and increased comfort and expertise in emergency department procedural sedation (EDPS). [] PEC has been found to be both safe and effective, [ 4] and the approach has been supported by the 00 Canadian Cardiovascular Society AF clinical practice guidelines. [5] In June 006, the ED in the Halifax Infirmary developed
2 66 Butler et al World J Emerg Med, Vol 8, No 3, 07 an EDPS registry in which all patients undergoing EDPS are prospectively registered for the purposes of quality improvement. At the Charles V. Keating Emergency and Trauma Centre, approximately 000 EDPS are performed annually. The proportion of all procedural sedations for PEC has increased from 6% in 006 to 9.3% in 04. In a study from the University of Alberta, 30.5% of 77 EDPSs were for PEC. [6] While PEC is the preferred method of treatment for acute AF by emergency physicians in our academic department, this trend is not universal across Canada. One group of investigators found a high degree of variation in management approaches for recent-onset AF in academic hospital EDs. Specifically, they found that the incidence of primary cardioversion in eligible patients varied from 7% to 69% in the hospitals studied, [7] and it does appear that nationally much debate remains regarding the optimal treatment of the condition. [8,9] The primary issues of debate include whether rate or rhythm control is a better strategy, and if so, whether this varies in different subsets of patients, and whether primary cardioversion should be the principle treatment modality in patients with a low risk of stroke. One glaring omission in the debate regarding primary cardioversion is any reference to the optimal way in which sedation to facilitate the PEC should be performed. EDPS requires specific expertise and carries the risk of significant adverse events if not performed with attention to the proper patient selection, medication administration, appropriate monitoring and the skill set to rescue patients from unintended over-sedation. Propofol, a short acting anaesthetic agent, is the most commonly used medication for EDPS. Although it can cause hypotension and respiratory depression, propofol has been extensively studied in the ED setting and has been shown to be both safe and efficacious. [9] However, special care must be used when propofol is administered to patients with underlying cardio-respiratory disease who concurrently have an acute arrhythmia. PEC is an unpleasant, although very brief procedure in the vast majority of cases. It would be expected that EDPS for PEC should require a shorter procedure time and lower doses of sedative or analgesic compared to EDPS for other emergency conditions, which are generally longer in duration and involve more painful stimulation of the patients. In a previous study to evaluate the safety of propofol for EDPS, a majority of patients received solely propofol, with 6.8% of patients receiving fentanyl, with no patient in the study suffering an adverse outcome. [9] Anecdotally, our experienced sedationists have observed that cardioversion for EDPS can be conducted with fewer drugs and lower doses than those for other patients requiring EDPS. This observation, however, needs to be verified objectively. Interestingly a review calling for "guidelines-to-bench approach to research" to "allow for the development of important, clinically relevant new knowledge with impacts on patient management and future AF guidelines" [0] fails to address the issue of how best to manage the sedation required to facilitate the PEC, a point arguably of as much, if not more, importance to emergency physicians who are considering whether to add PEC to their practice. At the Charles V. Keating Emergency and Trauma Centre, EDPS is performed by specially trained Advanced Care Paramedics. [] The EDPS program follows a very stringent protocol [] and the clinical details of every EDPS are recorded on a specific patient care record (Figure ). The physician responsible for the patient determines whether they can tolerate the procedure. The choice of sedative and analgesia is generally left at the discretion of the paramedic, although the attending physician can modify this decision. Anecdotally, such modification is rare at our institution. A registry for the purpose of continuous quality improvement is maintained and regularly reviewed to ensure patient safety and appropriate care. This registry provides an Capital Health Emergency Department Procedural Sedation and Analgesia Patient Care Record Date: / / YYYY MM DD Gender M F Age: ASA classification I Healthy II Mild systemic disease No functional limits III Severe systemic disease-functional limitations IV Severe systemic disease-corstant threat to life V Moribund will not survive without procedure Indication for procedure Orthopedic Incision and drainage Imaging/behavior control Wound care Lumbar puncture Chest tube placement Cardioversion Endoscopy Other Intended depth of sedation Anxiolysis Conscious/moderate sedation Deep sedation General anesthesia MD discipline Emergency Orthopedics Surgery Gastro-enterology Plastics Other: Figure. Data collection tool. Patient history (please circle) Allergies: N Unknown Y Cardio/respiratory co-morbidities N Unknown Y Last PO intake (hrs): Liquid: < 6 >6 Solid: < 6 >6 Pathologic substance use: ETOH Opioid Clinical assessments I Chest exam: Normal Abnormal Specify: Pre Sedation score: (located on reference card) Clinical assessment II airway Malampatti score: I II III IV Hyomntal distance: 3 <3 fingers Mouth opening: 3 <3 fingers Upper lip bite: able unable Neck ROM concern: N Y Neck pathology: N Y Beard N Y Obese N Y Edentulous: N Y Snoring history: N Y Times: Interview: First drug: Procedure start: Procedure end: Monitoring end:
3 World J Emerg Med, Vol 8, No 3, ideal opportunity to compare EDPS conducted for PEC to those performed for other reasons. Recognizing that the majority of EDPS is conducted on younger, healthy patients with many for orthopedic manipulations, we hypothesize that that practitioners skilled in EDPS for more traditional reasons may be less well prepared to safely conduct EDPS in patients requiring PEC. Retrospectively examining EDPS records in both groups may allow us to identify features to bear in mind for practitioners expanding their practice into this area. The objective of our study was to determine if there are important differences in patient characteristics and clinical outcomes in patients receiving EDPS using propofol for PEC compared to those receiving EDPS using propofol for other indications. METHODS This retrospective study examined the EDPS records of patients treated at the Charles V. Keating Emergency and Trauma Centre, a tertiary-care, academic teaching center in Halifax, Nova Scotia with an annual ED census of visits. The Halifax EDPS registry has been previously described but in short all EDPS are prospectively captured and for this study the period of review was June 006 to September 04. [ 3] The data are inputted by an administrative assistant, and one of the co-authors regularly runs database queries to detect input errors and missing data for the purpose of reconciliation. All data were abstracted from the registry, a Microsoft Access database created specifically for the purpose of managing the quality of EDPS. We analysed only patients who received exclusively propofol with or without fentanyl. We did this because these drugs are used in the majority of the PSAs at our institution [3] and to reduce pharmacological bias where other medications were used. There is no specific protocol for drug dosing for PEC or any other indication for EDPS at our institution, so these data represent our current practice in ED. Patients were divided into two groups, those that received EDPS for PEC and those that received EDPS for other indications (orthopedic manipulation, incision and drainage [I&D], imaging/behaviour control, wound care, lumbar puncture, chest tube placement). Patient characteristics examined included age, gender and American Society of Anesthesiologists (ASA) physical status. Doses of medication (propofol and fentanyl) were also compared. Adverse outcomes examined included hypotension, hypoxia, apnea and need for airway intervention. Hypotension was defined as any systolic blood pressure (SBP) <00 mmhg, or a 5% decrease from baseline if initial SBP was less than 00 mmhg. Hypoxia was defined as an oxygen saturation as measured by pulse oximetry <90%. Apnea was defined as the cessation of respiration for a period lasting >30 seconds. Airway intervention included the need for an oropharyngeal airway, non-invasive positive pressure ventilation, tracheal intubation or an airway maneuver (e.g., jaw thrust) in the peri-, intra- and post-procedure period. To assess for the association of procedure type (PEC versus all other procedures) with the above outcomes, we utilized a logistic model. We report the crude estimates of the odds ratio (OR), and the estimate of the OR adjusted for patient gender, age, ASA physical status, and propofol and fentanyl dose. We also evaluated patient opinion of the procedure to assess for tolerability of the interventions. To validate the above models, we reported the P value of the Le Cessie-van Houwelingen test, [4,5] and assessed for the effect of collinearity using the variance inflation factors (VIFs). A VIF of greater than five was considered a priori an unacceptable level of dependency between the candidate predictors. All analyses are performed using R (v3..3, "Smooth Sidewalk") in the RStudio GUI (v ). The study was approved by the Capital Health Ethics Review Board. RESULTS A total of patients were included in our study dataset. We excluded 340 patients due to them receiving a sedative that was not propofol. Patient demographics are outlined in Table. Patients in the PEC group Table. Patient demographics Demographics PEC (n=74) Non-PEC (n=4 53) P value Age (mean±sd) 59.5± ±5.9 <0.00 Gender (male), n (%) 48 (58.5) 955 (47.) <0.00 ASA, n (%) <0.00 I 333 (46.6) 865 (69.0) II 39 (44.7) 05 (5.3) III 5 (7.) 6 (3.9) IV 0 (.4) 74 (.8) V (0.) 0 (0.0) Patient opinion, n (%) <0.00 Very satisfied 4 (7.4) 657 (5.8) Satisfied 73 (0.) 676 (6.3) No recollection/neutral 464 (65.0) 448 (58.9) Unpleasant 3 (0.4) 3 (0.5) Very unpleasant 5 (0.7) 46 (.) Unrecorded 45 (6.3) 303 (7.3) Propofol dose (mg) 96.6± ±3.3 <0.00 Fentanyl dose (µg) 80.± ± Without fentanyl, n (%) 558 (78.) 478 (.5) <0.00 : Dosing calculated only for patients that received fentanyl.
4 68 Butler et al World J Emerg Med, Vol 8, No 3, 07 were more likely to be older, male and less likely to be assessed as an ASA I than the comparator group. The PEC group also tended to have received lower doses of both propofol and fentanyl, or received no analgesia. Table outlines the rate of adverse events during EDPS. More patients in the PEC group experienced hypotension (7.6% vs. 6.5%, P<0.00); however, there were no statistically significant differences in hypoxia, apnea and need for airway interventions between the two groups. Logistic regression models assessing the association of the outcomes with PEC showed that patients in the PEC group were more than twice as likely to experience hypotension as the non-pec group (OR=.; 95%CI.78.74), and were 3% more likely to require an airway intervention as the non-pec group (OR=.3; 95%CI.06.64). Although point estimates indicate that hypoxia and apnea were less likely to occur in the PEC group, these differences did not reach statistical significance (Table 3). There were no deaths in the ED associated with EDPS, and no patients received tracheal intubation, or were admitted as a complication of the procedure. No vasopressor agents were used in any patients. All Hosmer- Le Cessie tests were non-significant, indicating an adequate fit of the linear models, and all VIFs were less than.5 for all predictors, indicating no overwhelming problems with variance inflation from collinearity. Table. Adverse events during emergency department procedural sedation, n (%) Adverse events PEC (n=74) Non-PEC (n=4 53) P value Hypotension 97 (7.6) 684 (6.5) <0.00 Hypoxia 0 (.4) 90 (.) 0.33 Apnea 6 (0.8) 36 (0.9) >0.99 Airway intervention 74 (4.4) 903 (.7) 0.30 : <00 mmhg, or 5% decrease from baseline if first SBP is <00 mmhg; : Any one or more of: airway positioning, oropharygneal airway, ETT, BVM. Table 3. Logistic regression results Outcomes Crude OR (95%CI) Adjusted OR (95%CI) P value Hypotension.93 (.6.3). (.78.74) <0.00 Hypoxia 0.64 (0.33.4) 0.60 (0.9.) 0.60 Apnea 0.97 (0.4.33) 0.75 (0.9.96) Airway maneuver.6 ( ).3 (.06.64) 0.0 : <00 mmhg, or 5% decrease from baseline if first SBP is <00 mmhg; : Any one or more of: airway positioning, oropharygneal airway, ETT, BVM; Effect of AF, adjusted for age, gender, ASA, propofol dose, fentanyl dose. DISCUSSION The use of PEC for AF in patients at low risk for embolic complications (those with <48 hours of AF, or on therapeutic anticoagulation regimens) is rapidly becoming standard of care in the ED. [] While EDPS has been standard of care for many years, it is a process of care that requires specific skill and knowledge. Experience gained performing EDPS on young patients with orthopedic or infectious indications may not be transferrable to patients with a new cardiac arrhythmia. Our data suggests that, although outcomes in both groups were favorable, patients in the PEC group had a lower baseline level of health (as measure by ASA categories) and were more likely to suffer hypotension and to receive airway manipulation, even though they received lower doses of medication and fewer received opioids in combination with the sedative. Adverse effects of propofol are recognized as being more common with larger doses of the drug, when adjuvant opioids are used, and in patients with a lower baseline level of health. [9] Our findings of lower propofol and fentanyl doses and of more cases done without opioids suggest that the sedationists recognized the increased potential for adverse events in the PEC group and adjusted accordingly, mitigating, although not completely, a large increase in hypotension. Another explanation for the lower doses or non-use of analgesics is that PEC is a rapid and (compared to fracture reduction) less painful procedure, and that the need for opioids is considered less. The increase in airway interventions without an increased incidence of hypoxia or apnea suggests a greater level of vigilance with respect to respiratory monitoring. We were not able to ascertain whether this was because patients in the PEC group were recognized as being potentially at greater risk for EDPS or because they had higher baseline ASA physical status. Limitations This study is a retrospective examination of registry data, and thus carries many of the limitations of retrospective research, especially the fact that the two groups are not randomized and several unmeasured variables may have contributed to differences in practice aside from the indication for EDPS. Although we were not able to find any adverse events that led to sedation related morbidity, the registry does not capture whether the procedure which required EDPS was successfully completed. One limitation of our study is that many patients undergoing EDPS may be under-treated for chronic
5 World J Emerg Med, Vol 8, No 3, hypertension, especially in the PEC group. A higher SBP than our chosen threshold may represent clinically relevant hypoperfusion to the vital organs in these patients. As such, our estimates are likely a minimum estimate of the true proportion of hypotension in both groups. Additionally, our study represents a single centre, that utilizes specially trained paramedics to administer EDPS. This may affect the external validity of the study. Future research should focus on the balance between sedating to successfully complete the procedure and the risk of adverse events during said procedure. CONCLUSION EDPS for PEC is generally safe and well tolerated. It does, however differ from that done for other indications in that patients have a lower baseline level of health, and are more likely to suffer hypotension during the procedure. It appears that PEC patients are given lower doses of medications, are less likely to receive combinations of sedatives and analgesics and are more likely to receive airway interventions, although they do not have a higher rate of hypoxia or apnea. Practitioners should be aware of these differences when considering adding EDPS for PEC to their practice. Funding: None. Ethical approval: The study was approved by the Capital Health Ethics Review Board. Conflicts of interest: The authors declare there is no competing interest related to the study, authors, other individuals or organizations. Contributors: Butler M proposed the study and wrote the first draft. All authors read and approved the final version of the paper. REFERENCES Stiell IG, Clement CM, Perry JJ, Vaillancourt C, Symington C, Dickinson G, et al. Association of the Ottawa Aggressive Protocol with rapid discharge of emergency department patients with recent-onset atrial fibrillation or flutter. CJEM. 00; (3):8 9. Burton JH, Vinson DR, Drummond K, Strout TD, Thode HC, McInturff JJ. Electrical cardioversion of emergency department patients with atrial fibrillation. Ann Emerg Med. 004;44(): Michael JA, Stiell IG, Agarwal S, Mandavia DP. Cardioversion of paroxysmal atrial fibrillation in the emergency department. Ann Emerg Med. 999;33(4): Xavier Scheuermeyer F, Grafstein E, Stenstrom R, Innes G, Poureslami I, Sighary M. Thirty-day outcomes of emergency department patients undergoing electrical cardioversion for atrial fibrillation or flutter. Acad Emerg Med. 00;7(4): Stiell IG, Macle L. Canadian Cardiovascular Society atrial fibrillation guidelines 00: management of recent-onset atrial fibrillation and flutter in the emergency department. Can J Cardiol. 0;7(): Bawden J, Villa-Roel C, Singh M, Fabris G, Bond K, Boyko D, et al. Procedural sedation and analgesia in a Canadian ED: a time-in-motion study. Acad Emerg Med. 00; 9(9): Stiell IG, Clement CM, Brison RJ, Rowe BH, Borgundvaag B, Langhan T, et al. Variation in management of recent-onset atrial fibrillation and flutter among academic hospital emergency departments. Ann Emerg Med. 0;57():3. 8 Murray S, Lazure P, Pullen C, Maltais P, Dorian P. Atrial fibrillation care: challenges in clinical practice and educational needs assessment. Can J Cardiol. 0;7(): Campbell SG, Magee KD, Zed PJ, Froese P, Etsell G, LaPierre A, et al. End-tidal capnometry during emergency department procedural sedation and analgesia: a randomized, controlled study. World J Emerg Med. 06;7(): Stanley N. From guidelines to bench: implications of unresolved clinical issues for basic investigations of atrial fibrillation mechanisms. Can J Cardiol. 0;7():9 6. Campbell SG, Petrie DA, MacKinley P, Froese P, Etsell G, Warren DA, et al. Procedural sedation and analgesia facilitator -expanded scope role for paramedics in the Emergency Department. Journal of Emergency Primary Health Care 6[3]. jephc.com/full_articlecd6f.html?content_id=486 (accessed Mar 05) Campbell SG, Magee KD, Kovacs GJ, Petrie DA, Tallon JM, McKinley R, et al. Procedural sedation and analgesia in a Canadian adult tertiary care emergency department: a case series. CJEM. 006;8(): Campbell SG, Froese P, Butler M, Etsell GR, Lapierre A, MacKinley R, et al. Propofol is officially the sedative of choice' in Halifax! An update from the Halifax ED Procedural Sedation registry. CJEM S5, Le Cessie S, van Houwelingen J. A goodness-of-fit test for binary regression models, based on smoothing methods. Biometrics. 99: Rahman NHNA, Hashim A. The use of propofol for procedural sedation and analgesia in the emergency department: a comparison with midazolam. Emerg Med J. 00;8:86 5. Received September 0, 06 Accepted after revision March 6, 07
PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older)
 Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Effect of post-intubation hypotension on outcomes in major trauma patients
 Effect of post-intubation hypotension on outcomes in major trauma patients Dr. Robert S. Green Professor, Emergency Medicine and Critical Care Dalhousie University Medical Director, Trauma Nova Scotia
Effect of post-intubation hypotension on outcomes in major trauma patients Dr. Robert S. Green Professor, Emergency Medicine and Critical Care Dalhousie University Medical Director, Trauma Nova Scotia
Medical Coverage Policy Monitored Anesthesia care (MAC) EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Monitored Anesthesia care (MAC) EFFECTIVE DATE: 09 01 2004 POLICY LAST UPDATED: 01 08 2013 OVERVIEW Monitored anesthesia care is a specific anesthesia service for a diagnostic or
Medical Coverage Policy Monitored Anesthesia care (MAC) EFFECTIVE DATE: 09 01 2004 POLICY LAST UPDATED: 01 08 2013 OVERVIEW Monitored anesthesia care is a specific anesthesia service for a diagnostic or
Chapter 004 Procedural Sedation and Analgesia
 Chapter 004 Procedural Sedation and Analgesia NOTE: CONTENT CONTAINED IN THIS DOCUMENT IS TAKEN FROM ROSEN S EMERGENCY MEDICINE 9th Ed. Italicized text is quoted directly from Rosen s. Key Concepts: 1.
Chapter 004 Procedural Sedation and Analgesia NOTE: CONTENT CONTAINED IN THIS DOCUMENT IS TAKEN FROM ROSEN S EMERGENCY MEDICINE 9th Ed. Italicized text is quoted directly from Rosen s. Key Concepts: 1.
Addendum D. Procedural Sedation Test MERCY MEDICAL CENTER- SIOUX CITY. Procedural Sedation Questions
 Addendum D. Procedural Sedation Test MERCY MEDICAL CENTER- SIOUX CITY Procedural Sedation Questions Individuals applying for moderate sedation privileges must achieve a score of 80%. PRACTITIONER NAME
Addendum D. Procedural Sedation Test MERCY MEDICAL CENTER- SIOUX CITY Procedural Sedation Questions Individuals applying for moderate sedation privileges must achieve a score of 80%. PRACTITIONER NAME
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Procedural Sedation in the Rural ER
 Procedural Sedation in the Rural ER Hal Irvine MD FCFP Rural FP Anesthetist Sundre, Alberta June 17, 2011 Disclosure I do not have any affiliations (financial or otherwise) with a commercial organization
Procedural Sedation in the Rural ER Hal Irvine MD FCFP Rural FP Anesthetist Sundre, Alberta June 17, 2011 Disclosure I do not have any affiliations (financial or otherwise) with a commercial organization
PHYSICIAN PROCEDURAL SEDATION AND ANALGESIA QUIZ
 PHYSICIAN PROCEDURAL SEDATION AND ANALGESIA QUIZ 1. Which of the following statements are TRUE? (Select ALL that apply) o Sedative/analgesic drugs should be given in small, incremental doses that are titrated
PHYSICIAN PROCEDURAL SEDATION AND ANALGESIA QUIZ 1. Which of the following statements are TRUE? (Select ALL that apply) o Sedative/analgesic drugs should be given in small, incremental doses that are titrated
Mohammad Zubaid, MB, ChB, FRCPC, FACC
 Management and one year outcome of atrial fibrillation in Middle Eastern cohort enrolled in the observational Gulf Survey of Atrial Fibrillation Events (Gulf SAFE) Mohammad Zubaid, MB, ChB, FRCPC, FACC
Management and one year outcome of atrial fibrillation in Middle Eastern cohort enrolled in the observational Gulf Survey of Atrial Fibrillation Events (Gulf SAFE) Mohammad Zubaid, MB, ChB, FRCPC, FACC
I. Subject. Moderate Sedation
 I. Subject II. III. Moderate Sedation Purpose To establish criteria for the monitoring and management of patients receiving moderate throughout the hospital Definitions A. Definitions of three levels of
I. Subject II. III. Moderate Sedation Purpose To establish criteria for the monitoring and management of patients receiving moderate throughout the hospital Definitions A. Definitions of three levels of
Case. You plan to perform an EGD for further evaluation. Footer text is edited under "view/header and footer" menu August 11, 2018 Page 2
 Procedural Sedation Daniela Jodorkovsky M.D. Gastroenterology Fellowship Director Assistant Professor Medicine Columbia University Medical Center-New York Presbyterian NYSGE First Year Fellow Course 2018
Procedural Sedation Daniela Jodorkovsky M.D. Gastroenterology Fellowship Director Assistant Professor Medicine Columbia University Medical Center-New York Presbyterian NYSGE First Year Fellow Course 2018
Sedation-Analgesia Patient Evaluation
 Getting Started A health care provider with current privileges to administer sedation-analgesia must conduct a pre-procedure evaluation, and obtain informed consent for sedation-analgesia Only patients
Getting Started A health care provider with current privileges to administer sedation-analgesia must conduct a pre-procedure evaluation, and obtain informed consent for sedation-analgesia Only patients
Reducing Adverse Drug Events Related to Opioids: An Interview with Thomas W. Frederickson MD, FACP, SFHM, MBA
 Reducing Adverse Drug Events Related to Opioids: An Interview with Thomas W. Frederickson MD, FACP, SFHM, MBA The following is a transcript of part two of an interview with Dr. Thomas Frederickson. For
Reducing Adverse Drug Events Related to Opioids: An Interview with Thomas W. Frederickson MD, FACP, SFHM, MBA The following is a transcript of part two of an interview with Dr. Thomas Frederickson. For
Prospective Study to Revise the Ottawa Heart Failure Risk Scale (OHFRS)
 Prospective Study to Revise the Ottawa Heart Failure Risk Scale (OHFRS) CAEP Edmonton 2015 Ian Stiell MD Shawn Aaron MD Robert Brison MD Alan Forster MD Jeffrey Perry MD George Wells PhD Catherine Clement
Prospective Study to Revise the Ottawa Heart Failure Risk Scale (OHFRS) CAEP Edmonton 2015 Ian Stiell MD Shawn Aaron MD Robert Brison MD Alan Forster MD Jeffrey Perry MD George Wells PhD Catherine Clement
Procedural Sedation. Conscious Sedation AAP Sedation Guidelines: Disclosures. What does it mean for my practice? We have no disclosures
 2016 AAP Sedation Guidelines: What does it mean for my practice? Amber P. Rogers MD FAAP Assistant Professor of Section of Hospital Medicine and Anesthesiology Corrie E. Chumpitazi MD FAAP FACEP Assistant
2016 AAP Sedation Guidelines: What does it mean for my practice? Amber P. Rogers MD FAAP Assistant Professor of Section of Hospital Medicine and Anesthesiology Corrie E. Chumpitazi MD FAAP FACEP Assistant
Attestation for Completion of Procedural Sedation Course for Level I Moderate Procedural Sedation Privileges
 Attestation for Completion of Procedural Sedation Course for Level I Moderate Procedural Sedation Privileges I certify that I have completed the following: I have read the PHSW Procedural Sedation Policy
Attestation for Completion of Procedural Sedation Course for Level I Moderate Procedural Sedation Privileges I certify that I have completed the following: I have read the PHSW Procedural Sedation Policy
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health
 UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Propofol and Etomidate are Safe for Deep Sedation in the Emergency Department Permalink https://escholarship.org/uc/item/9bq8f3ph
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Propofol and Etomidate are Safe for Deep Sedation in the Emergency Department Permalink https://escholarship.org/uc/item/9bq8f3ph
Analgesic-Sedatives Drug Dose Onset
 Table 4. Commonly used medications in procedural sedation and analgesia Analgesic-Sedatives Fentanyl Morphine IV: 1-2 mcg/kg Titrate 1 mcg/kg q3-5 minutes prn IN: 2 mcg/kg Nebulized: 3 mcg/kg IV: 0.05-0.15
Table 4. Commonly used medications in procedural sedation and analgesia Analgesic-Sedatives Fentanyl Morphine IV: 1-2 mcg/kg Titrate 1 mcg/kg q3-5 minutes prn IN: 2 mcg/kg Nebulized: 3 mcg/kg IV: 0.05-0.15
Routine Patient Care Guidelines - Adult
 Routine Patient Care Guidelines - Adult All levels of provider will complete an initial & focused assessment on every patient, and as standing order, use necessary and appropriate skills and procedures
Routine Patient Care Guidelines - Adult All levels of provider will complete an initial & focused assessment on every patient, and as standing order, use necessary and appropriate skills and procedures
DEEP SEDATION TEST QUESTIONS
 Mailing Address: Phone: Fax: The Study Guide is provided for those physicians eligible to apply for Deep Sedation privileges. The Study Guide is approximately 41 pages, so you may consider printing only
Mailing Address: Phone: Fax: The Study Guide is provided for those physicians eligible to apply for Deep Sedation privileges. The Study Guide is approximately 41 pages, so you may consider printing only
Sedation is a dynamic process.
 19th Annual Mud Season Nursing Symposium Timothy R. Lyons, M.D. 26 March 2011 To allow patients to tolerate unpleasant procedures by relieving anxiety, discomfort or pain To expedite the conduct of a procedure
19th Annual Mud Season Nursing Symposium Timothy R. Lyons, M.D. 26 March 2011 To allow patients to tolerate unpleasant procedures by relieving anxiety, discomfort or pain To expedite the conduct of a procedure
POST TEST: PROCEDURAL SEDATION
 POST TEST: PROCEDURAL SEDATION Name: Date: Instructions: Complete the Post-Test (an 85% is required to pass). If there are areas that you are unsure of, please review the relevant portions of the learning
POST TEST: PROCEDURAL SEDATION Name: Date: Instructions: Complete the Post-Test (an 85% is required to pass). If there are areas that you are unsure of, please review the relevant portions of the learning
Comparison of sedative effectiveness of thiopental versus midazolam in reduction of shoulder dislocation
 Original Article Comparison of sedative effectiveness of thiopental versus midazolam in reduction of shoulder dislocation 125 Elnaz Vahidi, Rezvan Hemati, Mehdi Momeni, Amirhossein Jahanshir, Morteza Saeedi
Original Article Comparison of sedative effectiveness of thiopental versus midazolam in reduction of shoulder dislocation 125 Elnaz Vahidi, Rezvan Hemati, Mehdi Momeni, Amirhossein Jahanshir, Morteza Saeedi
Critical Review Form Therapy
 Critical Review Form Therapy Does End-tidal Carbon Dioxide Monitoring Detect Respiratory Events Prior to Current Sedation Monitoring Practices, Acad Emerg Med 2006; 13:500-504 Objective: To determine the
Critical Review Form Therapy Does End-tidal Carbon Dioxide Monitoring Detect Respiratory Events Prior to Current Sedation Monitoring Practices, Acad Emerg Med 2006; 13:500-504 Objective: To determine the
Thirty-day Outcomes of Emergency Department Patients Undergoing Electrical Cardioversion for Atrial Fibrillation or Flutter
 Thirty-day Outcomes of Emergency Department Patients Undergoing Electrical Cardioversion for Atrial Fibrillation or Flutter Frank Xavier Scheuermeyer, MD, MHSc, Eric Grafstein, MD, Rob Stenstrom, MD, PhD,
Thirty-day Outcomes of Emergency Department Patients Undergoing Electrical Cardioversion for Atrial Fibrillation or Flutter Frank Xavier Scheuermeyer, MD, MHSc, Eric Grafstein, MD, Rob Stenstrom, MD, PhD,
Date 8/95; Rev.12/97; 7/98; 2/99; 5/01, 3/03, 9/03; 5/04; 8/05; 3/07; 10/08; 10/09; 10/10 Manual of Administrative Policy Source Sedation Committee
 Code No. 711 Section Subject Moderate Sedation (formerly termed Conscious Sedation ) Date 8/95; Rev.12/97; 7/98; 2/99; 5/01, 3/03, 9/03; 5/04; 8/05; 3/07; 10/08; Manual of Administrative Policy Source
Code No. 711 Section Subject Moderate Sedation (formerly termed Conscious Sedation ) Date 8/95; Rev.12/97; 7/98; 2/99; 5/01, 3/03, 9/03; 5/04; 8/05; 3/07; 10/08; Manual of Administrative Policy Source
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Pain & Sedation Management in PICU. Marut Chantra, M.D.
 Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS)
 Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
INTUBATION/RSI. PURPOSE: A. To facilitate secure, definitive control of the airway by endotracheal intubation in an expeditious and safe manner
 Manual: LifeLine Patient Care Protocols Section: Adult/Pediatrics Protocol #: AP1-009 Approval Date: 03/01/2018 Effective Date: 03/05/2018 Revision Due Date: 12/01/2018 INTUBATION/RSI PURPOSE: A. To facilitate
Manual: LifeLine Patient Care Protocols Section: Adult/Pediatrics Protocol #: AP1-009 Approval Date: 03/01/2018 Effective Date: 03/05/2018 Revision Due Date: 12/01/2018 INTUBATION/RSI PURPOSE: A. To facilitate
How it Works. CO 2 is the smoke from the flames of metabolism 10/21/18. -Ray Fowler, MD. Metabolism creates ETC0 2 for excretion
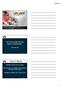 CO 2 is the smoke from the flames of metabolism -Ray Fowler, MD How it Works Metabolism creates ETC0 2 for excretion ETC02 and Oxygen are exchanged at the alveolar level in the lungs with each breath.
CO 2 is the smoke from the flames of metabolism -Ray Fowler, MD How it Works Metabolism creates ETC0 2 for excretion ETC02 and Oxygen are exchanged at the alveolar level in the lungs with each breath.
The following criteria must be met in order to obtain pediatric clinical privileges for pediatric sedation.
 Pediatric Sedation Sedation of children is different from sedation of adults. Sedatives are generally administered to gain the cooperation of the child. The ability of the child to cooperate depends on
Pediatric Sedation Sedation of children is different from sedation of adults. Sedatives are generally administered to gain the cooperation of the child. The ability of the child to cooperate depends on
CalvertHealth Medical Center s Moderate Sedation Competency Examination
 Medical Staff Office Use Only: Congratulations! You passed the Moderate Sedation Competency Examination. Enclosed is the test for your follow-up review. Test Results: % ( of 35 correct) Your test result
Medical Staff Office Use Only: Congratulations! You passed the Moderate Sedation Competency Examination. Enclosed is the test for your follow-up review. Test Results: % ( of 35 correct) Your test result
Case scenarios. We want to do head CT in an middle-aged woman with agitation and confusion. She does not stay still in the CT table.
 Procedural sedation Khrongwong Musikatavorn, M.D. Emergency Medicine Unit, King Chulalongkorn Memorial Hospital and Faculty of Medicine, Chulalongkorn University Case scenarios We need to rule out acute
Procedural sedation Khrongwong Musikatavorn, M.D. Emergency Medicine Unit, King Chulalongkorn Memorial Hospital and Faculty of Medicine, Chulalongkorn University Case scenarios We need to rule out acute
Regulations: Adult Minimal Sedation
 Regulations: Adult Minimal Sedation Jason H. Goodchild, DMD DrGoodchild@yahoo.com April 2017 Regulations Caveats 1. The regulations about to be presented are accurate and current as of today. 2. This could
Regulations: Adult Minimal Sedation Jason H. Goodchild, DMD DrGoodchild@yahoo.com April 2017 Regulations Caveats 1. The regulations about to be presented are accurate and current as of today. 2. This could
Pediatric Sedation Pocket Reference
 Pediatric Sedation Pocket Reference No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form or by any means, electronic, mechanical, photocopy, recording,
Pediatric Sedation Pocket Reference No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form or by any means, electronic, mechanical, photocopy, recording,
Emergency Department Guideline. Procedural Sedation and Analgesia Policy for the Registered Nurse
 Emergency Department Guideline Purpose: To ensure safe, consistent patient monitoring and documentation standards when procedure related sedation and analgesia is indicated. Definitions: Minimal Sedation
Emergency Department Guideline Purpose: To ensure safe, consistent patient monitoring and documentation standards when procedure related sedation and analgesia is indicated. Definitions: Minimal Sedation
Sedation in Children
 CHILDREN S SERVICES Sedation in Children See text for full explanation and drug doses Patient for Sedation Appropriate staffing Resuscitation equipment available Monitoring equipment Patient suitability
CHILDREN S SERVICES Sedation in Children See text for full explanation and drug doses Patient for Sedation Appropriate staffing Resuscitation equipment available Monitoring equipment Patient suitability
GUIDELINES ON CONSCIOUS SEDATION FOR DENTAL PROCEDURES
 AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 ROYAL AUSTRALASIAN COLLEGE OF DENTAL SURGEONS ABN 97 343 369 579 Review PS21 (2003) GUIDELINES ON CONSCIOUS SEDATION FOR DENTAL PROCEDURES
AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 ROYAL AUSTRALASIAN COLLEGE OF DENTAL SURGEONS ABN 97 343 369 579 Review PS21 (2003) GUIDELINES ON CONSCIOUS SEDATION FOR DENTAL PROCEDURES
Conscious Sedation. Edited by D. John Doyle MD PhD FRCPC
 Conscious Sedation Edited by D. John Doyle MD PhD FRCPC In memory of: J. Michael de Ungria, MD 1969-2009 Anesthesia Institute The Cleveland Clinic Goals and Objectives: 1. Define Conscious Sedation. 2.
Conscious Sedation Edited by D. John Doyle MD PhD FRCPC In memory of: J. Michael de Ungria, MD 1969-2009 Anesthesia Institute The Cleveland Clinic Goals and Objectives: 1. Define Conscious Sedation. 2.
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Leon H. Charney Division of Cardiology, New York University School of Medicine, New York, NY, USA 5
 https://doi.org/10.15441/ceem.17.286 Effectiveness and safety of electrical cardioversion for acute-onset atrial fibrillation in the emergency department: a real-world 10-year single center experience
https://doi.org/10.15441/ceem.17.286 Effectiveness and safety of electrical cardioversion for acute-onset atrial fibrillation in the emergency department: a real-world 10-year single center experience
Disclosures. Overview. Difficult Airway Mgmt. Airway Evaluation and Management: Recent advances. No financial, consulting, contractual relationships
 Airway Evaluation and Management: Recent advances Disclosures No financial, consulting, contractual relationships Sachin Kheterpal MD MBA Assistant Professor Department of Anesthesiology University of
Airway Evaluation and Management: Recent advances Disclosures No financial, consulting, contractual relationships Sachin Kheterpal MD MBA Assistant Professor Department of Anesthesiology University of
IDENTIFYING SEPSIS IN THE PREHOSPITAL SETTING
 IDENTIFYING SEPSIS IN THE PREHOSPITAL SETTING Christopher Hunter, MD, PhD, FACEP Director, Health Services Department Associate Medical Director, Orange County EMS System Medical Director, Orlando Health
IDENTIFYING SEPSIS IN THE PREHOSPITAL SETTING Christopher Hunter, MD, PhD, FACEP Director, Health Services Department Associate Medical Director, Orange County EMS System Medical Director, Orlando Health
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
POLICY All patients will be assessed for risk factors associated with OSA prior to any surgical procedures.
 Revised Date: Page: 1 of 7 SCOPE All Pre-Admission Testing (PAT) and Same Day Surgery (SDS) nurses at HRMC. PURPOSE The purpose of this policy is to provide guidelines for identifying surgical patients
Revised Date: Page: 1 of 7 SCOPE All Pre-Admission Testing (PAT) and Same Day Surgery (SDS) nurses at HRMC. PURPOSE The purpose of this policy is to provide guidelines for identifying surgical patients
Advanced Cardiac Life Support (ACLS) Science Update 2015
 1 2 3 4 5 6 7 8 9 Advanced Cardiac Life Support (ACLS) Science Update 2015 What s New in ACLS for 2015? Adult CPR CPR remains (Compressions, Airway, Breathing Chest compressions has priority over all other
1 2 3 4 5 6 7 8 9 Advanced Cardiac Life Support (ACLS) Science Update 2015 What s New in ACLS for 2015? Adult CPR CPR remains (Compressions, Airway, Breathing Chest compressions has priority over all other
Emergency Medicine Research: Creating Evidence to Improve Safety and Effectiveness of ED Patient Care
 Emergency Medicine Research: Creating Evidence to Improve Safety and Effectiveness of ED Patient Care Dr Eric Clark MD, FRCPC Department of Emergency Medicine University of Ottawa Canada No Conflicts of
Emergency Medicine Research: Creating Evidence to Improve Safety and Effectiveness of ED Patient Care Dr Eric Clark MD, FRCPC Department of Emergency Medicine University of Ottawa Canada No Conflicts of
Rapid Sequence Induction
 Rapid Sequence Induction Virtual simultaneous administration, after preoxygenation, of a potent sedative agent and a rapidly acting neuromuscular blocking agent to facilitate rapid tracheal intubation
Rapid Sequence Induction Virtual simultaneous administration, after preoxygenation, of a potent sedative agent and a rapidly acting neuromuscular blocking agent to facilitate rapid tracheal intubation
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Anesthesia for Routine Gastrointestinal Endoscopic Procedures (Additional description)
 Anesthesia for Routine Gastrointestinal Endoscopic Procedures (Additional description) Date of Origin: 05/2012 Last Review Date: 12/06/2017 Effective Date: 01/01/2018 Dates Reviewed: 12/2013, 11/2014,
Anesthesia for Routine Gastrointestinal Endoscopic Procedures (Additional description) Date of Origin: 05/2012 Last Review Date: 12/06/2017 Effective Date: 01/01/2018 Dates Reviewed: 12/2013, 11/2014,
Procedural Sedation and Analgesia in the ED
 Overview Procedural Sedation and Analgesia in the ED Susan Lambe, MD Assistant Clinical Professor UCSF Division of Emergency Medicine Terminology Goals Indications Presedation Assessment Consent Issues
Overview Procedural Sedation and Analgesia in the ED Susan Lambe, MD Assistant Clinical Professor UCSF Division of Emergency Medicine Terminology Goals Indications Presedation Assessment Consent Issues
General Pediatric Approach to Sedation in a Community Hospital
 General Pediatric Approach to Sedation in a Community Hospital Guideline developed by Sarah Tariq, MD, in collaboration with the ANGELS team. Last reviewed by Sarah Tariq, MD, September 14, 2016. Preface
General Pediatric Approach to Sedation in a Community Hospital Guideline developed by Sarah Tariq, MD, in collaboration with the ANGELS team. Last reviewed by Sarah Tariq, MD, September 14, 2016. Preface
The Canadian Syncope Risk Score to Identify Patients at Risk for SAE after ED Disposition
 The Canadian Syncope Risk Score to Identify Patients at Risk for SAE after ED Disposition CAEP Edmonton May 2015 Venkatesh Thiruganasambandamoorthy MBBS Kenneth Kwong BSc Marco Sivilotti MD Brian Rowe
The Canadian Syncope Risk Score to Identify Patients at Risk for SAE after ED Disposition CAEP Edmonton May 2015 Venkatesh Thiruganasambandamoorthy MBBS Kenneth Kwong BSc Marco Sivilotti MD Brian Rowe
Results of a one-year, retrospective medication use evaluation. Joseph Ladd, PharmD PGY-1 Pharmacy Resident BHSF Homestead Hospital
 Results of a one-year, retrospective medication use evaluation Joseph Ladd, PharmD PGY-1 Pharmacy Resident BHSF Homestead Hospital Briefly review ketamine s history, mechanism of action, and unique properties
Results of a one-year, retrospective medication use evaluation Joseph Ladd, PharmD PGY-1 Pharmacy Resident BHSF Homestead Hospital Briefly review ketamine s history, mechanism of action, and unique properties
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012
 Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012 Why screen of OSA prior to surgery? What factors increase the risk? When due to anticipate problems?
Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012 Why screen of OSA prior to surgery? What factors increase the risk? When due to anticipate problems?
The goal of deep sedation is to achieve a medically controlled state of depressed consciousness from which the patient is not easily aroused.
 SUBJECT: Deep Sedation POLICY NUMBER: PAMC/MS 951.139 Policy Type: Patient Care New Revised Reviewed EXECUTIVE Approval: Date Signed: 10.29.2014 /s/ Richard D. Mandsager, MD, Chief Executive Providence
SUBJECT: Deep Sedation POLICY NUMBER: PAMC/MS 951.139 Policy Type: Patient Care New Revised Reviewed EXECUTIVE Approval: Date Signed: 10.29.2014 /s/ Richard D. Mandsager, MD, Chief Executive Providence
Biphasic Clinical Summaries
 Biphasic Clinical Summaries Defibrillation of Ventricular Fibrillation and Ventricular Tachycardia Background Physio-Control conducted a multi-centered, prospective, randomized and blinded clinical trial
Biphasic Clinical Summaries Defibrillation of Ventricular Fibrillation and Ventricular Tachycardia Background Physio-Control conducted a multi-centered, prospective, randomized and blinded clinical trial
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
ADVANCED AIRWAY MANAGEMENT
 The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
1/27/2017 RECOGNITION AND MANAGEMENT OF OBSTRUCTIVE SLEEP APNEA: STRATEGIES TO PREVENT POST-OPERATIVE RESPIRATORY FAILURE DEFINITION PATHOPHYSIOLOGY
 RECOGNITION AND MANAGEMENT OF OBSTRUCTIVE SLEEP APNEA: STRATEGIES TO PREVENT POST-OPERATIVE RESPIRATORY FAILURE Peggy Hollis MSN, RN, ACNS-BC March 9, 2017 DEFINITION Obstructive sleep apnea is a disorder
RECOGNITION AND MANAGEMENT OF OBSTRUCTIVE SLEEP APNEA: STRATEGIES TO PREVENT POST-OPERATIVE RESPIRATORY FAILURE Peggy Hollis MSN, RN, ACNS-BC March 9, 2017 DEFINITION Obstructive sleep apnea is a disorder
Competency Indicators Pediatrics Registered Nurse
 Hospital Logo Competency Indicators Pediatrics Registered Nurse mployee Name: Review Key: = ducation Session valuation Key: Able to perform & document A: Airway assessment: mployee Describes unique airway
Hospital Logo Competency Indicators Pediatrics Registered Nurse mployee Name: Review Key: = ducation Session valuation Key: Able to perform & document A: Airway assessment: mployee Describes unique airway
CADTH Therapeutic Review
 Canadian Agency for Drugs and Technologies in Health Agence canadienne des médicaments et des technologies de la santé CADTH Therapeutic Review August 2012 Volume 1, Issue 1A Antithrombotic Therapy for
Canadian Agency for Drugs and Technologies in Health Agence canadienne des médicaments et des technologies de la santé CADTH Therapeutic Review August 2012 Volume 1, Issue 1A Antithrombotic Therapy for
Basic Considerations Of Sedating Children In The Dental Setting
 University of Alabama at Birmingham School of Dentistry Alabama Academy of Pediatric Dentistry Basic Considerations Of Sedating Children In The Dental Setting Stephen Wilson DMD, MA, PhD Professor & Chair
University of Alabama at Birmingham School of Dentistry Alabama Academy of Pediatric Dentistry Basic Considerations Of Sedating Children In The Dental Setting Stephen Wilson DMD, MA, PhD Professor & Chair
Setting The study setting was hospital. The economic analysis appears to have been carried out in the USA.
 Electrical cardioversion of atrial fibrillation or flutter with conscious sedation in the age of cost containment Goldner B G, Baker J, Accordino A, Sabatino L, DiGiulio M, Kalenderian D, Lin D, Zambrotta
Electrical cardioversion of atrial fibrillation or flutter with conscious sedation in the age of cost containment Goldner B G, Baker J, Accordino A, Sabatino L, DiGiulio M, Kalenderian D, Lin D, Zambrotta
ASPIRUS WAUSAU HOSPITAL, INC. Passion for excellence. Compassion for people. SUBJECT: END TIDAL CARBON DIOXIDE MONITORING (CAPNOGRAPHY)
 Passion for excellence. Compassion for people. P&P REF : NEW 7-2011 ONBASE POLICY ID: 13363 REPLACES: POLICY STATUS : FINAL DOCUMENT TYPE: Policy EFFECTIVE DATE: 4/15/2014 PROPOSED BY: Respiratory Therapy
Passion for excellence. Compassion for people. P&P REF : NEW 7-2011 ONBASE POLICY ID: 13363 REPLACES: POLICY STATUS : FINAL DOCUMENT TYPE: Policy EFFECTIVE DATE: 4/15/2014 PROPOSED BY: Respiratory Therapy
yregion I EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic SMO: Airway Management
 yregion I EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic SMO: Airway Management Overview: Managing a patient s airway may be necessitated due to upper or lower airway obstruction, inadequate
yregion I EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic SMO: Airway Management Overview: Managing a patient s airway may be necessitated due to upper or lower airway obstruction, inadequate
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
SURGERY OR ANESTHESIA
 Patient Safety Event Report Hospital SURGERY OR ANESTHESIA Use this form to report an event involving a surgical or other invasive procedure (e.g., colonoscopy), or the administration of anesthesia. Do
Patient Safety Event Report Hospital SURGERY OR ANESTHESIA Use this form to report an event involving a surgical or other invasive procedure (e.g., colonoscopy), or the administration of anesthesia. Do
CLINICAL AUDIT 2017/2018 Procedural Sedation in Adults Clinical Audit Proforma
 CLINICAL AUDIT 2017/2018 Procedural Sedation in Adults Clinical Audit Proforma Data should be submitted between 1 Aug 2017 31 Jan 2018. You can find the link to log into the data entry site at www.rcem.ac.uk/audits
CLINICAL AUDIT 2017/2018 Procedural Sedation in Adults Clinical Audit Proforma Data should be submitted between 1 Aug 2017 31 Jan 2018. You can find the link to log into the data entry site at www.rcem.ac.uk/audits
Administrative Policies and Procedures. Originating Venue: Provision of Care, Treatment and Services Policy No.: PC 2916
 Administrative Policies and Procedures Originating Venue: Provision of Care, Treatment and Services Policy No.: PC 2916 Title: Sedation Cross Reference: Date Issued: 05/09 Date Reviewed: 04/11 Date: Revised:
Administrative Policies and Procedures Originating Venue: Provision of Care, Treatment and Services Policy No.: PC 2916 Title: Sedation Cross Reference: Date Issued: 05/09 Date Reviewed: 04/11 Date: Revised:
Regulations: Minimal Sedation. Jason H. Goodchild, DMD
 Regulations: Minimal Sedation Jason H. Goodchild, DMD August 2016 Caveats 1. The regulations about to be presented are accurate and current as of today. 2. This could change tomorrow. 3. It is up to every
Regulations: Minimal Sedation Jason H. Goodchild, DMD August 2016 Caveats 1. The regulations about to be presented are accurate and current as of today. 2. This could change tomorrow. 3. It is up to every
Cardiothoracic Fellow Expectations Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center
 The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
Pain Module. Opioid-RelatedRespiratory Depression (ORRD)
 Pain Module Opioid-RelatedRespiratory Depression (ORRD) Characteristics of patients who are at higher risk for Opioid- Related Respiratory Depression (ORRD) Sleep apnea or sleep disorder diagnosis : typically
Pain Module Opioid-RelatedRespiratory Depression (ORRD) Characteristics of patients who are at higher risk for Opioid- Related Respiratory Depression (ORRD) Sleep apnea or sleep disorder diagnosis : typically
ACLS Prep. Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep.
 November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
61.10 Dental anesthesia certification.
 61.10 Dental anesthesia certification. a. *Definitions. For purposes of this section, the following definitions shall apply: 1. Acceptable accrediting body means an accrediting body which is accepted by
61.10 Dental anesthesia certification. a. *Definitions. For purposes of this section, the following definitions shall apply: 1. Acceptable accrediting body means an accrediting body which is accepted by
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Capnography for Monitoring End-Tidal CO 2 in Hospital and Pre-hospital Settings: A Health Technology Assessment
 CADTH HEALTH TECHNOLOGY ASSESSMENT Capnography for Monitoring End-Tidal CO 2 in Hospital and Pre-hospital Settings: A Health Technology Assessment Product Line: Health Technology Assessment Issue Number:
CADTH HEALTH TECHNOLOGY ASSESSMENT Capnography for Monitoring End-Tidal CO 2 in Hospital and Pre-hospital Settings: A Health Technology Assessment Product Line: Health Technology Assessment Issue Number:
Optimize vent weaning and SBT outcomes. Identify underlying causes for SBT failures. Role SBT and weaning protocol have in respiratory care
 Optimize vent weaning and SBT outcomes Identify underlying causes for SBT failures Role SBT and weaning protocol have in respiratory care Lower risk of developing complications Lower risk of VAP, other
Optimize vent weaning and SBT outcomes Identify underlying causes for SBT failures Role SBT and weaning protocol have in respiratory care Lower risk of developing complications Lower risk of VAP, other
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
May 2013 Anesthetics SLOs Page 1 of 5
 May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
CURRICULUM FOR FELLOWSHIP IN CRITICAL CARE MEDICINE
 CURRICULUM FOR FELLOWSHIP IN CRITICAL CARE MEDICINE AIM: The course has been designed to train candidates by the anesthesiologists in the principles and practice of intensive care & artificial ventilation
CURRICULUM FOR FELLOWSHIP IN CRITICAL CARE MEDICINE AIM: The course has been designed to train candidates by the anesthesiologists in the principles and practice of intensive care & artificial ventilation
Guidelines on the Safe Practice of Acute Pain Management
 Page 1 of 7 Guidelines on the Safe Practice of Acute Pain Version Effective Date 1 1 MAY 1994 (Reviewed Feb 2002) 2 1 DEC 2014 Document No. HKCA P11 v2 Prepared by College Guidelines Committee Endorsed
Page 1 of 7 Guidelines on the Safe Practice of Acute Pain Version Effective Date 1 1 MAY 1994 (Reviewed Feb 2002) 2 1 DEC 2014 Document No. HKCA P11 v2 Prepared by College Guidelines Committee Endorsed
PAAQS Reference Guide
 Q. 1 Patient's Date of Birth (DOB) *Required Enter patient's date of birth PAAQS Reference Guide Q. 2 Starting Anesthesiologist *Required Record the anesthesiologist that started the case Q. 3 Reporting
Q. 1 Patient's Date of Birth (DOB) *Required Enter patient's date of birth PAAQS Reference Guide Q. 2 Starting Anesthesiologist *Required Record the anesthesiologist that started the case Q. 3 Reporting
Where Emergency Medicine Meets Critical Care: Next Level Resuscitation
 Where Emergency Medicine Meets Critical Care: Next Level Resuscitation Rob Green, BSc, MD, DABEM, FRCPC, FRCP(Edin) Professor, Dalhousie University Departments of Emergency Medicine,Critical Care Medicine
Where Emergency Medicine Meets Critical Care: Next Level Resuscitation Rob Green, BSc, MD, DABEM, FRCPC, FRCP(Edin) Professor, Dalhousie University Departments of Emergency Medicine,Critical Care Medicine
Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients.
 Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
Moderate and Deep Sedation Pathway
 A Quick Reference to the Advocate System Sedation Policy *This information is meant as a guideline only and not a substitute for physician order or clinical judgment Introduction: This Pediatric Emergency
A Quick Reference to the Advocate System Sedation Policy *This information is meant as a guideline only and not a substitute for physician order or clinical judgment Introduction: This Pediatric Emergency
Comparison of Procedural Sedation for the Reduction of Dislocated Total Hip Arthroplasty
 ORIGINAL RESEARCH for the Reduction of Dislocated Total Hip Arthroplasty Jonathan E. dela Cruz, MD* Donald N. Sullivan, MD Eric Varboncouer, MD Joseph C. Milbrandt, PhD* Myto Duong, MD * Scott Burdette,
ORIGINAL RESEARCH for the Reduction of Dislocated Total Hip Arthroplasty Jonathan E. dela Cruz, MD* Donald N. Sullivan, MD Eric Varboncouer, MD Joseph C. Milbrandt, PhD* Myto Duong, MD * Scott Burdette,
Joint Theater Trauma System Clinical Practice Guideline
 Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Adult Intubation Skill Sheet
 Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Direct Current Cardioversion (DCCV)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is a This is a procedure carried out under a brief anaesthetic, which uses a
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is a This is a procedure carried out under a brief anaesthetic, which uses a
Conscious Sedation Permit Evaluation. General Comments Emergency Algorithms
 General Comments Emergency Algorithms These algorithms delineate appropriate responses to the simulated emergencies listed in Article 5, Section 1043.4c of the California Code of Regulations. Each algorithm
General Comments Emergency Algorithms These algorithms delineate appropriate responses to the simulated emergencies listed in Article 5, Section 1043.4c of the California Code of Regulations. Each algorithm
FOAM A New Style of Learning for a New Generation. Eric Einstein, M.D. Henry Ford Hospital Department of Emergency Medicine November 13, 2014
 FOAM A New Style of Learning for a New Generation Eric Einstein, M.D. Henry Ford Hospital Department of Emergency Medicine November 13, 2014 Objectives Define and discuss the basics Peer review a podcast
FOAM A New Style of Learning for a New Generation Eric Einstein, M.D. Henry Ford Hospital Department of Emergency Medicine November 13, 2014 Objectives Define and discuss the basics Peer review a podcast
Guidelines for the Use of Sedation and General Anesthesia by Dentists
 Guidelines for the Use of Sedation and General Anesthesia by Dentists I. INTRODUCTION The administration of local anesthesia, sedation and general anesthesia is an integral part of dental practice. The
Guidelines for the Use of Sedation and General Anesthesia by Dentists I. INTRODUCTION The administration of local anesthesia, sedation and general anesthesia is an integral part of dental practice. The
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adverse drug events, polypharmacy and perioperative considerations in elderly patients, 377 389 Age, and risk of postoperative urinary retention,
Note: Page numbers of article titles are in boldface type. A Adverse drug events, polypharmacy and perioperative considerations in elderly patients, 377 389 Age, and risk of postoperative urinary retention,
