HEALTHY AND FULFILLING LIFESTYLE
|
|
|
- Maximilian Russell
- 5 years ago
- Views:
Transcription
1 Reference Guide for Individual Patient Education Keeping a Healthy and Fulfilling Lifestyle Educational topics: 1. Healthy and Fulfilling Lifestyle Health and COPD Healthy Life Habits o No smoking o Medication compliance o Healthy diet o Exercising and physical activity o Good nights sleep o Satisfying sex life o Leisure activities o Planning of trips 2 nd Edition 2006 Authors: D. Nault, R.N., M.Sc. M. Sedeño, M.M. A. Joubert, B.Sc. J. Bourbeau, M.D., M.Sc., F.R.C.P.C. Montreal Chest Institute of the McGill University Health Center (MUHC) 1st edition authors: V. Perreault, R.N. M.Sc. D. Nault, R.N. M.Sc. J. Bourbeau, M.D., M.Sc., F.R.C.P.C. Montreal Chest Institute of the Royal Victoria Hospital
2 General Objective The content of this section aims to help the COPD patient and family to make the appropriate changes in their lifestyle to live better with COPD. Patient / Family Specific Objectives 1. To define what it means to be healthy with COPD 2. To adopt and maintain healthy life habits: To quit smoking (if smokes) To take medications as prescribed and on a regular basis To maintain healthy nutrition habits and a healthy weight To do on a regular basis physical activities and/or follow a formal exercise program To have good night s sleep To have satisfying sex life To practice on a regular basis one or more recreational activities To plan trips (if wants to travel) Living Well with COPD resources Reference guide for individual patient education Keeping a Healthy and Fulfilling Lifestyle, section Healthy and Fulfilling Lifestyle Patient/family learning module: Keeping a healthy and fulfilling lifestyle Summary guide, p. 29 Flipchart: sections: - Healthy lifestyle Health and COPD 1. a. Identify with the patient/family what health means to him*. [1] b. Discuss with the patient/family that it is possible to be healthy when having COPD. [2, 3] Can express clearly his meaning of health by reinforcing the fact that it is possible to be healthy when having COPD What does health mean to you? Do you think it is possible to be healthy when you have COPD? Explain. 2. Review with patient/family healthy behaviours to be adopted and integrated in everyday life to live well with COPD (use the flipchart). [2] Describe the healthy behaviours to be adopted and integrated in everyday life to live well with COPD What do you do to stay healthy? Are there any other changes in your lifestyle you should do to live better with COPD? Which ones? *For simplicity, the pronouns 'he', 'his' and him in this reference guide will refer to both males and females. It is not intended to isolate any one particular gender. Individual Reference Guide: Prevention and Management of COPD Exacerbations. October 22, 2006 Page 2 of 9
3 Healthy Life Habits: Smoking Cessation and Avoiding Second Hand Smoke 1. a. If patient smokes, determine his stage of change (Prochaska). [1] Expresses at what stage he is for quitting smoking Do you still smoke? If you still smoke, do you think of quitting smoking? If you are thinking about it, are you ready to quit? b. If he is ready to quit or has already quit smoking (stage of preparation, action or maintenance), review the goal and benefits and reinforce the plan previously established [5, 7]. quitting smoking and participates in the elaboration of the plan to quit smoking or agrees to continue following the pre-established plan Do you have a date for quitting? Can you tell me what will be the benefits of quitting smoking on your health condition? How can we make a plan to help you to quit smoking? Are you willing to continue following your plan? c. If he is not ready (stages of pre/contemplation) - help him express his feelings, concerns, perceived benefits and risks [1,3]. Expresses his feelings and concerns about his habit of smoking and the need to quit What are your feelings and concerns about quitting smoking? Do you see any benefits for you if you stop smoking? What are the risks if you continue to smoke? - give him pertinent written information to read if it s not done yet. [10] Agrees to read and consult written information Are you planning to read the written information? 2. If a family member smokes stress the importance for the patient/family to live in a smoke-free environment. [3, 7] Agrees with the feedback and reinforcement in regards to the importance of living in a smoke-free environment Can you tell me why it is important for both of you to live in a smoke-free environment Do you see any benefits for you to live in a smoke free environment? What are the risks for your partner or loved one or friend if you continue to smoke? 3. Explore how patient feels about asking people around him not to smoke in his presence. Provide examples of how he could deal with that. [1, 3, 5] States that he feels comfortable in asking people around him not to smoke in his presence How do you feel about asking people around you not to smoke in your presence? Give me examples on how you would ask them not to smoke around you. 4. Evaluate the patient/family s level of self-efficacy with respect to his capacity to live in a smoke-free environment by quitting smoking and/or avoiding second hand smoke [6] Believes that he is able to live in a smoke-free environment by quitting smoking and/or avoiding second hand smoke If he smokes: Do you feel capable of quitting smoking? Do you feel capable of asking people around you not to smoke in your presence? Believes that living in a smoke-free environment will have a positive impact on his health If he smokes: Do you think that quitting smoking will have a positive impact on your health? Do you think that living in a smoke-free environment is good for you? Individual Reference Guide: Prevention and Management of COPD Exacerbations. October 22, 2006 Page 3 of 9
4 5. Refer the patient/family member to a smoking cessation expert if needed [9] Agrees to see an expert in smoking cessation if help is needed Have you met the expert for smoking cessation? Did it help you? Compliance with medications 1. Assess if patient is taking his medications as prescribed and on a regular basis. [1] Describes how he is taking his medications: type, frequency, dosage and timing Are you taking your medications as prescribed? For each medication, What dose and number of pills/puffs you need to take each time? How many times per day you need to take it? What helps you take your medications on a regular basis? What is preventing you from not taking your medications regularly? 2. Review with the patient/family the goal and benefits of taking the medications as prescribed and give reinforcement on the importance of taking them regularly. [2, 7] taking the medications as prescribed and the importance of being compliant with his medications Why should you take your medications as prescribed and on a regular basis? 3. Evaluate patient s level of self-efficacy in regards to taking medications as prescribed and on a regular basis. [6] Believes that he is able to take his COPD medications as prescribed on a regular basis. Believes in the benefits of the medications prescribed for COPD Do you think you are able to take your medications for COPD as prescribed on a regular basis? Do you believe that the medications prescribed for your COPD can stabilize or improve your symptoms? 4. Refer the patient to the physician and/or pharmacist if he needs more detailed information about his medications. [9] Agrees to meet with the physician and/or pharmacist Have you met your physician? Have you met the pharmacist? Healthy diet 1. Assess patient s perceptions related to nutrition (grocery and preparation of meals, feelings / symptoms while eating and after, concerns). [1] Expresses feelings, symptoms and concerns related to his nutrition. How do you organize yourself for doing your grocery? Do you have any problems with the preparation of your meals? Describe. How do you feel while you are eating? After? What can prevent you from eating properly? 2. Ask the patient/family what type of food they are currently eating, their hours of meals and what is the environment at meal times. [1] Describe the types of food they are currently eating, their meal times and the environment while eating. What types of food are you currently eating? What do you like to eat the most and the least? At what times during the day do you eat? Do you like eating? What do you do when you eat? Do you take your time? Explain. Individual Reference Guide: Prevention and Management of COPD Exacerbations. October 22, 2006 Page 4 of 9
5 3. Identify with the patient recent gains or losses in his weight. [1] Reports weight gains or losses that occurred in the last 3 months. Have you lost or gained weight in the past 3 months? How much weight did you loose or gain? 4. Explain to patient/family the goal and benefits of maintaining a healthy body weight and healthy nutrition habits. [2] maintaining a healthy body weight and healthy nutrition habits. Can you tell me why you should eat properly and maintain a healthy body weight? 5. a. Discuss with the patient/family the Canadian Food Guide recommendations. [2] Ask him to summarize the key elements from the discussion. [8] b. Elaborate with the patient an example of menu appropriate for him. [5,10] Describes the keys elements related to the discussion on the Canadian Food Guide recommendations. According to you, what are the most important recommendations included in the Canadian Food Guide? Participates to the elaboration of a menu appropriate in his case. Can you give me an example of menu appropriate for you? 6. Discuss with patient/family potential problems related to nutrition in COPD. [2] Describes potential problems that can prevent him from eating properly. What are the problems related to nutrition that COPD patients might face? 7. Discuss with patient/family strategies that can help to eat properly and save his energy when preparing meals, while eating and after. [2] Describes the strategies he can use to eat properly and save his energy in preparing meals or while and after eating. What are the strategies that can help you to eat properly and save your energy when preparing meals? When eating? After eating? 8. Evaluate patient s level of self-efficacy with respect to his capacity to keep a healthy diet [6] Believes that he is able to eat properly. Believes in the benefits of keeping a healthy diet. Do you think you are able to eat properly on a regular basis? Do you believe that keeping a healthy diet can have a positive impact in your condition? 9. Refer the patient to a dietician in case of obesity, when there is a risk of malnutrition or in the presence of concomitant health problems. [9] Agrees to see a dietician Have you met a dietician? Did it help you? Exercise and physical activity 1. a. Ask patient/family which activities he considers as exercise. [1] b. Ask patient/family which type of exercise he does presently and the frequency. [1] Describe the activities he considers as exercise and the ones that he does presently. Which activities do you consider to be exercise? Are you exercising presently? What type of exercise or physical activities are you doing? How many times per week are you doing your exercises? 2. If patient/family is ready to start exercising or he is already doing exercise, a. Review with him the goal and benefits of exercising. [2] exercising on a regular basis Are you ready to start exercising? Can you tell me why you should exercise? Why on a regular basis? b. Suggest what he can do to increase his level of physical activity or reinforce what he presently does. [5, 7] Participates in the elaboration of the plan to increase physical activity or agrees to continue doing his exercises. How can we make a plan to help you to exercise? Are you willing to continue to do your exercises? Individual Reference Guide: Prevention and Management of COPD Exacerbations. October 22, 2006 Page 5 of 9
6 3. If he is not ready to exercise, a. Help them to express his feelings and concerns. [3] b. Give them pertinent written information.[10] Expresses his feelings and concerns about exercising. Agrees to read and consult written information What are your feelings and concerns about exercising? Do you like exercising? Do you see any risks for you if you start to exercise? Do you plan to read the written information? c. Stress your belief that he needs to exercise on a regular basis and that this is possible for him. [3,7] Expresses agreement for feedback and reinforcement 4. Evaluate the level of self-efficacy with respect to his capacity to do exercise or physical activity regularly. [6] Believes that he is able to do exercise or physical activities on a regular basis Believes that exercising will have a positive impact on his condition. Do you believe you are capable of exercising or doing physical activities on a regular basis? Do you think that exercising is good for you? 5. Refer patient to a pulmonary rehabilitation program if he is motivated and has no contraindications to do it. [9] Agrees to be referred to a pulmonary rehabilitation program Have you been contacted by (or met) someone from a pulmonary rehabilitation team? Good sleep habits 1. Assess patient s cycle of sleep (bedtime, duration, positions to sleep) and sleep related problems. [1] Describes his cycle of sleep and the problems he is facing. At what time do you go to bed? How many hours do you sleep per night usually? What kind of positions do you sleep in? Do you sleep well usually? Do you have any problems to sleep? Describe. Do you have an idea of the reasons why you cannot sleep well? 2. Discuss with patient/family the goal and benefits of having good sleep habits. [2] having good sleep habits. Can you tell me why it is important to sleep well? 3. Discuss with patient/family strategies that can help to have a good night s sleep. [2,5] Describes the strategies he should use to have a good night s sleep. What do you do when you are not sleeping well or you cannot sleep? What should you do to sleep well? 4. Evaluate patient s level of self-efficacy with respect to his capacity to keep good sleep habits [6] Believes that he is able to keep good sleep habits Believes that having good sleep habits will have a positive impact on his health condition Do you believe you are capable of maintaining good sleep habits? Do you believe that having good sleep habits will help you to sleep better? Individual Reference Guide: Prevention and Management of COPD Exacerbations. October 22, 2006 Page 6 of 9
7 5. Refer patient to his physician if sleep problems persist. [9] Agrees to see his physician Have you met your physician for your sleep problems? Did it help you? Maintain a satisfying sex life 1. Assess patient/partner feelings, concerns, fears and needs in regards to their sex life in an individual basis. Have them share with each other. [1, 3] Expresses individually his feelings, concerns, fears and needs in regards to his sex life and share them with his partner How do you feel about sex? Do you have any concerns or fears related to your sexuality? What would you like to improve in regards to your sexuality? 2. a. Discuss with patient/partner the goal and benefits of having a satisfying sex life. [2] b. Demystify and normalize the fears around sexuality in COPD. [2, 3] having a satisfying sex life. Expresses agreement for normalization Tell me why having a satisfying sex life can be good for you 3. Discuss with patient/partner strategies that can help them to have a satisfying sex life (emphasize on preliminaries, strategies to reduce shortness of breath and facilitate intercourse). [2, 5] Participates in finding strategies to have a satisfying sex life. What strategies are you using or can you use to respond to your sexual needs and those of your partner? What strategies are you using or can you use to reduce your shortness of breath and facilitate intercourse? 4. Evaluate patient s level of self-efficacy with respect to his capacity of maintaining a satisfying sex life [6] Believes that he is able to maintain a satisfying sex life Believes that using the strategies discussed will help him maintain a satisfying sex life Do you believe you are capable of maintaining a satisfying sex life? Do you believe that using the strategies discussed will help you to maintain a satisfying sex life? Leisure activities 5. Refer patient to his physician / sex therapist if sex problems persist. [9] 1. a. Assess patient s/family s leisure activities he is involved in presently. [1] b. Ask patient which leisure activities he had to stop because of COPD and which ones he would like to restart. [1] Agrees to see his physician / sex therapist Lists all the leisure activities he is involved in, the ones he has stopped and the ones he would like to restart. Have you met your physician / sex therapist? Did it help you? What do you do as leisure activity? Are there any leisure activities that you have had to discontinue? Which ones? Why did you have to stop? Would you like to restart any leisure activity(ies)? Which ones? 2. Discuss with patient/family the goal and benefits of doing leisure activities. [2] taking time for leisure activities. Can you tell me why you should take time for leisure activities? 3. Discuss with patient/family possible leisure activities he can get involved in. [2,3] Lists at least three leisure activities that he can get involved in. Name a few leisure activities that are good for you and that you would like to do What are your strengths, the limitations and your abilities to do these leisure activities? Individual Reference Guide: Prevention and Management of COPD Exacerbations. October 22, 2006 Page 7 of 9
8 4. Plan with the patient the start of a new leisure activity that he will do regularly. [5] Chooses at least one new leisure activity that he will start to practice regularly. Which leisure activity are you ready to start and practice regularly? 5. Evaluate patient s level of self-efficacy with respect to his capacity of getting involved in one or more leisure activities [6] Believes that he is able to get involved in one or more leisure activities Believes that getting involved in leisure activities can improve his overall health condition and emotional well-being Do you believe you are capable of practicing one or more leisure activities on a regular basis? Do you believe that getting involved in leisure activities can have a positive impact in your health condition? Planning trips 1. Assess patient s interest in traveling, his concerns and fears. [1] Expresses his desire of travelling or not. Are you interested in traveling? Where would you like to go? What worries you about taking a trip? 2. Discuss with patient/family the goal and benefits of travelling. [2] traveling. What do you think travelling can do for you? 3. Plan with patient the trip he would like to do and discuss with patient/family what needs to be arranged in advance. [2, 5] Does the exercise of planning a trip through one mode of travel. How you would like to get there? (e.g. mode of travel) What are your strengths, limitations and ability to do this trip? Lists the essential elements that should be part of the travelling plan. What are the most important things you need to get and arrange before you can travel? 4. Evaluate patient s level of self-efficacy with respect to his capacity to plan a trip. [6] Believes that he is able to plan and go on a trip Believes that travelling will have a positive impact on his overall health Do you believe you are capable of planning and going on a trip? Do you believe that travelling will have a positive impact on your overall health? 5. Refer patient to his physician to get a summary note of his chart, updated vaccination status, applicable prescriptions and enough medication for the trip. [9] Sees his physician before going on a trip (enough time in advance) Do you have the summary note from your doctor, prescriptions and medications that you need? In case of O 2 and travelling by plane: Have you made arrangements for your in-flight oxygen? Have you been able to book a direct flight? Summary of the session 1. Ask the patient to summarize the key elements of what has been discussed in regards to healthy behaviors that need to be integrated in the daily life to live well with COPD.[8] Summarizes in his own words the key elements in regards to healthy behaviours that need to be integrated in the daily life to live well with COPD Can you tell me what are the most important changes in your lifestyle that you need to do to live well with COPD? Individual Reference Guide: Prevention and Management of COPD Exacerbations. October 22, 2006 Page 8 of 9
9 2. Provide to the patient constructive feedback and reinforcement on the adoption and integration of healthy behaviors needed to live well with COPD. [7] Expresses agreement for feedback and reinforcement Learning contract 1. Ask the patient to continue to integrate in his daily life the healthy behaviors needed to live well with COPD on his daily life. [5] Maintains healthy behaviours to live well with COPD. How are you doing in terms of? (Check for each healthy behaviour) Have you been able to continue with the plan we discussed? What are the problems you have had? **Educational Methods and other actions: 1 Learning needs assessment, 2 Interactive lecturing, 3 Building of ambivalence (motivational interview technique), 4 Demonstration and practice, 5 Learning contract, 6 On a scale of 1 to 10, ask the patient to determine his level of confidence, 1 = not confident at all and 10 = very confident, 7 Constructive feedback and reinforcement, 8 Summarizing information, 9 Reference to other health care professionals, 10 Give pertinent written information, 11 Case scenarios. Suggested Questions: Questions to evaluate patient s needs, comprehension of information, and outcomes. If you find negative results readdress issues in order to reach the specific objectives. Individual Reference Guide: Prevention and Management of COPD Exacerbations. October 22, 2006 Page 9 of 9
Integrating a Plan of Action for Life
 Reference Guide for Individual Patient Education Educational topics: Integrating a Plan of Action for Life 1. Prevention and management of COPD exacerbations Reasons for using an Action Plan and its structure
Reference Guide for Individual Patient Education Educational topics: Integrating a Plan of Action for Life 1. Prevention and management of COPD exacerbations Reasons for using an Action Plan and its structure
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 5 Plan of Action: Part I Overview of the Plan of Action and Management of Respiratory Infections Plan of Action: Objectives
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 5 Plan of Action: Part I Overview of the Plan of Action and Management of Respiratory Infections Plan of Action: Objectives
PROMOTION OF PHYSICAL ACTIVITY
 General objective Resources «Living Well with COPD» Reference guide for individual patient education «Integrating physical activity and/or an exercise program into your life», Section Promotion of physical
General objective Resources «Living Well with COPD» Reference guide for individual patient education «Integrating physical activity and/or an exercise program into your life», Section Promotion of physical
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
Health Professional Manual
 Health Professional Manual Session: Smoking Cessation Smoking and COPD Strategies for quitting smoking Adapted from the Living Well with COPD program (2nd edition), Montreal Chest Institute, Canada SESSION
Health Professional Manual Session: Smoking Cessation Smoking and COPD Strategies for quitting smoking Adapted from the Living Well with COPD program (2nd edition), Montreal Chest Institute, Canada SESSION
Health Professional Manual
 Health Professional Manual Session 6 Continuing Exercise and Self-Management Strategies Maintenance of exercise and physical activity Welfare and Benefits Recap: Integration of Healthy Behaviours and Self-Management
Health Professional Manual Session 6 Continuing Exercise and Self-Management Strategies Maintenance of exercise and physical activity Welfare and Benefits Recap: Integration of Healthy Behaviours and Self-Management
Health Professional Manual
 Health Professional Manual Session 3 Overview of the Action Plan and Management of an Exacerbation Action Plan: Objectives and Structure Signs and Symptoms of an Exacerbation Strategies to Prevent an Exacerbation
Health Professional Manual Session 3 Overview of the Action Plan and Management of an Exacerbation Action Plan: Objectives and Structure Signs and Symptoms of an Exacerbation Strategies to Prevent an Exacerbation
Health Professional Manual
 Health Professional Manual Session: Healthy Eating COPD and healthy eating General healthy eating advice Getting the most out of every meal Adapted from the Living Well with COPD program (2nd edition),
Health Professional Manual Session: Healthy Eating COPD and healthy eating General healthy eating advice Getting the most out of every meal Adapted from the Living Well with COPD program (2nd edition),
Living with Congestive Heart Failure
 Living with Congestive Heart Failure Introduction Congestive heart failure, also known as chronic heart failure, is a common condition that affects millions of people every year. It is possible to control
Living with Congestive Heart Failure Introduction Congestive heart failure, also known as chronic heart failure, is a common condition that affects millions of people every year. It is possible to control
COMPREHENSIVE PAIN REHABILITATION CENTER OUTPATIENT PROGRAMS
 COMPREHENSIVE PAIN REHABILITATION CENTER OUTPATIENT PROGRAMS Our comprehensive whole-person rehabilitative services help patients return to an active lifestyle. THE MAYO CLINIC COMPREHENSIVE PAIN REHABILITATION
COMPREHENSIVE PAIN REHABILITATION CENTER OUTPATIENT PROGRAMS Our comprehensive whole-person rehabilitative services help patients return to an active lifestyle. THE MAYO CLINIC COMPREHENSIVE PAIN REHABILITATION
HEALTH 3--DEPRESSION, SLEEP, AND HEALTH GOALS FOR LEADERS. To educate participants regarding the sleep wake cycle.
 HEALTH 3--DEPRESSION, SLEEP, AND HEALTH GOALS FOR LEADERS Talk about the relationship between depression, sleep, and health problems. To educate participants regarding the sleep wake cycle. To provide
HEALTH 3--DEPRESSION, SLEEP, AND HEALTH GOALS FOR LEADERS Talk about the relationship between depression, sleep, and health problems. To educate participants regarding the sleep wake cycle. To provide
TOBACCO CESSATION SUPPORT PROGRAMME
 TOBACCO CESSATION SUPPORT PROGRAMME Day MOVING 7ON 2 Day KEEP 6GOING 5 SUPPORT 2 PLAN 3QUIT 4 COPING TOBACCO CESSATION SUPPORT PROGRAMME The Tobacco Cessation Support Programme is a structured behavioural
TOBACCO CESSATION SUPPORT PROGRAMME Day MOVING 7ON 2 Day KEEP 6GOING 5 SUPPORT 2 PLAN 3QUIT 4 COPING TOBACCO CESSATION SUPPORT PROGRAMME The Tobacco Cessation Support Programme is a structured behavioural
Sinclair Community College, Division of Allied Health Technologies
 Sinclair Community College, Division of Allied Health Technologies Health Promotion for Community Health Workers Cardiovascular disease, stroke, and cancer Class #9 Heart Failure (date) Course Objectives:
Sinclair Community College, Division of Allied Health Technologies Health Promotion for Community Health Workers Cardiovascular disease, stroke, and cancer Class #9 Heart Failure (date) Course Objectives:
Life After A Heart Attack
 Life After A Heart Attack A heart attack changes the lives of both seniors and their caregivers. If your loved one has had a heart attack, it's essential to understand the medications and lifestyle changes
Life After A Heart Attack A heart attack changes the lives of both seniors and their caregivers. If your loved one has had a heart attack, it's essential to understand the medications and lifestyle changes
A Guide to Help You Reduce and Stop Using Tobacco
 Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
COPD Program - Group Session # 2 Facilitator documents. May 2013
 COPD Program - Group Session # 2 Facilitator documents May 2013 Introduction to the facilitator documents This document supports the facilitator with respect to the contents of the Group Session 2 of the
COPD Program - Group Session # 2 Facilitator documents May 2013 Introduction to the facilitator documents This document supports the facilitator with respect to the contents of the Group Session 2 of the
get moving breathe easy
 Last update March 2009 BreathWorks toll-free helpline 1-866-717-COPD (2673) www.lung.ca/breathworks www.livingwellwithcopd.com get moving breathe easy Get moving breathe easy Notes: Despite constant breathlessness,
Last update March 2009 BreathWorks toll-free helpline 1-866-717-COPD (2673) www.lung.ca/breathworks www.livingwellwithcopd.com get moving breathe easy Get moving breathe easy Notes: Despite constant breathlessness,
PSYCHOSOCIAL EVALUATION AND TREATMENT IN CHRONIC RESPIRATORY DISEASES
 PSYCHOSOCIAL EVALUATION AND TREATMENT IN CHRONIC RESPIRATORY DISEASES Prof Behcet Coşar M.D. Gazi Uni. School of Med. Psychiatry Dep Consultation Liaison Psychiatry Unit HUMAN Bio Psycho Social 11/6/2009
PSYCHOSOCIAL EVALUATION AND TREATMENT IN CHRONIC RESPIRATORY DISEASES Prof Behcet Coşar M.D. Gazi Uni. School of Med. Psychiatry Dep Consultation Liaison Psychiatry Unit HUMAN Bio Psycho Social 11/6/2009
for the grieving process How to cope as your loved one nears the end stages of IPF
 Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
ORIENTATION SAN FRANCISCO STOP SMOKING PROGRAM
 ORIENTATION SAN FRANCISCO STOP SMOKING PROGRAM PURPOSE To introduce the program, tell the participants what to expect, and set an overall positive tone for the series. AGENDA Item Time 0.1 Acknowledgement
ORIENTATION SAN FRANCISCO STOP SMOKING PROGRAM PURPOSE To introduce the program, tell the participants what to expect, and set an overall positive tone for the series. AGENDA Item Time 0.1 Acknowledgement
Challenge to Change. Appendix A. Part I. Activity 1: Assessing Readiness to Change
 45073_APPA_187_194.qxd 8/24/06 1:22 PM Page 187 Name: Section: Course Number: Date: Challenge to Change You have acquired extensive information about physical activity and health by reading this book.
45073_APPA_187_194.qxd 8/24/06 1:22 PM Page 187 Name: Section: Course Number: Date: Challenge to Change You have acquired extensive information about physical activity and health by reading this book.
Fundamentals of Brief Cessation Counseling Approaches
 Fundamentals of Brief Cessation Counseling Approaches Jamie S. Ostroff Ph.D. Director, Smoking Cessation Program Memorial Sloan Kettering Cancer Center Co-Project Leader Queens Quits! Cessation Center
Fundamentals of Brief Cessation Counseling Approaches Jamie S. Ostroff Ph.D. Director, Smoking Cessation Program Memorial Sloan Kettering Cancer Center Co-Project Leader Queens Quits! Cessation Center
Introduction to Stages of Change and Change Talk in Motivational Interviewing Lisa Kugler, PsyD. March 29, 2018
 Introduction to Stages of Change and Change Talk in Motivational Interviewing Lisa Kugler, PsyD. March 29, 2018 Workshop Objectives Participants will be able to identify 3 key elements of motivational
Introduction to Stages of Change and Change Talk in Motivational Interviewing Lisa Kugler, PsyD. March 29, 2018 Workshop Objectives Participants will be able to identify 3 key elements of motivational
LIVING LONGER, LIVING WELL: YOUR GUIDE TO HEALTHY AGEING
 LIVING LONGER, LIVING WELL: YOUR GUIDE TO HEALTHY AGEING INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS HEALTHY AGEING READ THIS PAMPHLET TO LEARN: What you can do to Enable Healthy Ageing. How
LIVING LONGER, LIVING WELL: YOUR GUIDE TO HEALTHY AGEING INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS HEALTHY AGEING READ THIS PAMPHLET TO LEARN: What you can do to Enable Healthy Ageing. How
FACILITATOR GUIDE: Promoting Adherence and Health Behavior Change DocCom Module 16
 FACILITATOR GUIDE: Promoting Adherence and Health Behavior Change DocCom Module 16 Check-in: (5 min): Ask questions like: What s happening in your lives? ; What do we have to do to clear the air so we
FACILITATOR GUIDE: Promoting Adherence and Health Behavior Change DocCom Module 16 Check-in: (5 min): Ask questions like: What s happening in your lives? ; What do we have to do to clear the air so we
Get moving breathe easy
 get moving breathe easy Get moving breathe easy Despite constant breathlessness, it is very important for people with Chronic Obstructive Pulmonary Disease (COPD) or any chronic respiratory disease to
get moving breathe easy Get moving breathe easy Despite constant breathlessness, it is very important for people with Chronic Obstructive Pulmonary Disease (COPD) or any chronic respiratory disease to
Chronic Obstructive Pulmonary Disease. Information about medication and an Action Plan to use if your condition gets worse due to an infection
 Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
Coaching Patients If I could choose just one thing
 Coaching Patients If I could choose just one thing Patty Fredericks, MS Essentia Health Heart and Vascular Wellness Program Coaching Patients If I could choose just one thing Patty Fredericks, MS Essentia
Coaching Patients If I could choose just one thing Patty Fredericks, MS Essentia Health Heart and Vascular Wellness Program Coaching Patients If I could choose just one thing Patty Fredericks, MS Essentia
HELPING A PERSON WITH SCHIZOPHRENIA
 HELPING A PERSON WITH SCHIZOPHRENIA OVERCOMING CHALLENGES WHILE TAKING CARE OF YOURSELF The love and support of family plays an important role in schizophrenia treatment and recovery. If someone close
HELPING A PERSON WITH SCHIZOPHRENIA OVERCOMING CHALLENGES WHILE TAKING CARE OF YOURSELF The love and support of family plays an important role in schizophrenia treatment and recovery. If someone close
Is there any way you might be better off if you quit? What happens when you think about it? What do you imagine will happen if you don t change?
 This material has been prepared by the Massachusetts Smoker's Quitline, a program of the American Cancer Society. STAGES OF CHANGE Research on addiction and behavior change done by Prochaska and DiClemente,
This material has been prepared by the Massachusetts Smoker's Quitline, a program of the American Cancer Society. STAGES OF CHANGE Research on addiction and behavior change done by Prochaska and DiClemente,
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Fatigue in COPD Session 3 Energy Conservation Daily Activities that Cause Fatigue Energy Conservation Principles 1 st Edition
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Fatigue in COPD Session 3 Energy Conservation Daily Activities that Cause Fatigue Energy Conservation Principles 1 st Edition
Dr Anita Rose Director of Clinical Service: Consultant in Neuropsychology & Rehabilitation
 Dr Anita Rose Director of Clinical Service: Consultant in Neuropsychology & Rehabilitation Hope this finishes soon as I am hungry Did I lock my car when I left it in the car park? Will today finish in
Dr Anita Rose Director of Clinical Service: Consultant in Neuropsychology & Rehabilitation Hope this finishes soon as I am hungry Did I lock my car when I left it in the car park? Will today finish in
Understanding the Stages of Change in the Recovery Process
 Understanding the s of Change in the Recovery Process STAGES OF CHANGE Pre- Contemplation Contemplation PERSON WHO HAS DEVELOPED AN EATING DISORDER The person does not believe they have a problem. Refusal
Understanding the s of Change in the Recovery Process STAGES OF CHANGE Pre- Contemplation Contemplation PERSON WHO HAS DEVELOPED AN EATING DISORDER The person does not believe they have a problem. Refusal
Health Professional Manual
 Health Professional Manual Session 2 Energy Conservation Daily Activities that cause Fatigue Energy Conservation Principles Benefits of Exercise/Physical Activity Adapted from the Living Well with COPD
Health Professional Manual Session 2 Energy Conservation Daily Activities that cause Fatigue Energy Conservation Principles Benefits of Exercise/Physical Activity Adapted from the Living Well with COPD
Problem Situation Form for Parents
 Problem Situation Form for Parents Please complete a form for each situation you notice causes your child social anxiety. 1. WHAT WAS THE SITUATION? Please describe what happened. Provide enough information
Problem Situation Form for Parents Please complete a form for each situation you notice causes your child social anxiety. 1. WHAT WAS THE SITUATION? Please describe what happened. Provide enough information
BASIC VOLUME. Elements of Drug Dependence Treatment
 BASIC VOLUME Elements of Drug Dependence Treatment BASIC VOLUME MODULE 1 Drug dependence concept and principles of drug treatment MODULE 2 Motivating clients for treatment and addressing resistance MODULE
BASIC VOLUME Elements of Drug Dependence Treatment BASIC VOLUME MODULE 1 Drug dependence concept and principles of drug treatment MODULE 2 Motivating clients for treatment and addressing resistance MODULE
Motivational Interviewing in Chronic Diseases. Janelle W. Coughlin, Ph.D. Megan Lavery, Psy.D.. April 21, 2017
 Motivational Interviewing in Chronic Diseases Janelle W. Coughlin, Ph.D. Megan Lavery, Psy.D.. April 21, 2017 Motivational Interviewing in Chronic Diseases Presenter Names: Janelle W. Coughlin, Ph.D. &
Motivational Interviewing in Chronic Diseases Janelle W. Coughlin, Ph.D. Megan Lavery, Psy.D.. April 21, 2017 Motivational Interviewing in Chronic Diseases Presenter Names: Janelle W. Coughlin, Ph.D. &
A new model for prescribing varenicline
 Pharmacist Independent Prescribers in partnership with A new model for prescribing varenicline Dear Stop Smoking Advisor You will be aware of the stop smoking drug varenicline that goes under the brand
Pharmacist Independent Prescribers in partnership with A new model for prescribing varenicline Dear Stop Smoking Advisor You will be aware of the stop smoking drug varenicline that goes under the brand
OPIOID SUMMIT Partners Behavioral Health Management
 OPIOID SUMMIT Partners Behavioral Health Management March 11, 2016 Presented By: David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Integrated Healthcare Consultant MTM Services The National Council for Behavioral
OPIOID SUMMIT Partners Behavioral Health Management March 11, 2016 Presented By: David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Integrated Healthcare Consultant MTM Services The National Council for Behavioral
Living well today...32 Hope for tomorrow...32
 managing diabetes managing managing managing managing managing managing diabetes Scientific research continually increases our knowledge of diabetes and the tools to treat it. This chapter describes what
managing diabetes managing managing managing managing managing managing diabetes Scientific research continually increases our knowledge of diabetes and the tools to treat it. This chapter describes what
Pharmacy Advisor Program. Specialized Health Support
 Pharmacy Advisor Program Specialized Health Support Contents Your Health and Your CVS Caremark Pharmacy Advisor Pharmacist...3 Keys to Your Health....4 Getting the Most from Your Medication...6 Feeling
Pharmacy Advisor Program Specialized Health Support Contents Your Health and Your CVS Caremark Pharmacy Advisor Pharmacist...3 Keys to Your Health....4 Getting the Most from Your Medication...6 Feeling
Coach on Call. Please give me a call if you have more questions about this or other topics.
 Coach on Call It was great to talk with you. Thank you for your interest in. I hope you find this tip sheet helpful. Please give me a call if you have more questions about this or other topics. As your
Coach on Call It was great to talk with you. Thank you for your interest in. I hope you find this tip sheet helpful. Please give me a call if you have more questions about this or other topics. As your
Activity Intolerance (_)Actual (_) Potential
 Activity Intolerance Related To: (_) Chronic illness: (_) Depression (_) Lack of motivation (_) Stressors (_) Other: (_) Client reports intolerance of physical activity (_) Other: : (_) Reduce or eliminate
Activity Intolerance Related To: (_) Chronic illness: (_) Depression (_) Lack of motivation (_) Stressors (_) Other: (_) Client reports intolerance of physical activity (_) Other: : (_) Reduce or eliminate
Stress Management. Presented by: Jennifer Yuen. Campus Wellness Counselling Services. Strategies and Resources
 Stress Management Strategies and Resources Presented by: Jennifer Yuen Campus Wellness Counselling Services Reflection Take a few moments now to reflect on and write down: 1. Which situations do you find
Stress Management Strategies and Resources Presented by: Jennifer Yuen Campus Wellness Counselling Services Reflection Take a few moments now to reflect on and write down: 1. Which situations do you find
Sample blf.org.uk/copd
 Your COPD self-management plan blf.org.uk/copd Thank you to the people with lung conditions and leading health care professionals who helped to develop this plan. This resource has been developed in partnership
Your COPD self-management plan blf.org.uk/copd Thank you to the people with lung conditions and leading health care professionals who helped to develop this plan. This resource has been developed in partnership
Sample Do Not Copy IN GOD S IMAGE: SPIRITUAL PRACTICES FOR YOUTH WELLNESS. Youth Booklet
 IN GOD S IMAGE: SPIRITUAL PRACTICES FOR YOUTH WELLNESS Prevention Plus Wellness, LLC 904-472-5022 http://preventionpluswellness.com/ All Rights Reserved, 2018 Youth Booklet 1 In God s Image: Spiritual
IN GOD S IMAGE: SPIRITUAL PRACTICES FOR YOUTH WELLNESS Prevention Plus Wellness, LLC 904-472-5022 http://preventionpluswellness.com/ All Rights Reserved, 2018 Youth Booklet 1 In God s Image: Spiritual
BASIC VOLUME. Elements of Drug Dependence Treatment
 BASIC VOLUME Elements of Drug Dependence Treatment Module 2 Motivating clients for treatment and addressing resistance Basic counselling skills for drug dependence treatment Special considerations when
BASIC VOLUME Elements of Drug Dependence Treatment Module 2 Motivating clients for treatment and addressing resistance Basic counselling skills for drug dependence treatment Special considerations when
EPHE 575. Exercise Adherence. To Do. 8am Tuesday Presentations
 EPHE 575 Exercise Adherence To Do 8am Tuesday Presentations Quiz Find an article on exercise adherence and do an article summary on it. (If you have already checked it off, I will have one for you to fill
EPHE 575 Exercise Adherence To Do 8am Tuesday Presentations Quiz Find an article on exercise adherence and do an article summary on it. (If you have already checked it off, I will have one for you to fill
PATIENT SURVEY FOR ADMINISTRATIVE USE ONLY. TO BE COMPLETED BY STUDY COORDINATOR.
 PATIENT SURVEY FOR ADMINISTRATIVE USE ONLY. TO BE COMPLETED BY STUDY COORDINATOR. DATE OF VISIT: / / PATIENT ID: REGULAR PROVIDER: SITE OF VISIT: Cleveland Houston Manhattan Pittsburgh Thank you for agreeing
PATIENT SURVEY FOR ADMINISTRATIVE USE ONLY. TO BE COMPLETED BY STUDY COORDINATOR. DATE OF VISIT: / / PATIENT ID: REGULAR PROVIDER: SITE OF VISIT: Cleveland Houston Manhattan Pittsburgh Thank you for agreeing
Improving the Odds of Success through Motivational Interviewing
 Disclosure Information Western Occupational Health Conference 2011 Robert Scales, Ph.D. I have no financial relationships to disclose I will not discuss off label use and/or investigational use in my presentation
Disclosure Information Western Occupational Health Conference 2011 Robert Scales, Ph.D. I have no financial relationships to disclose I will not discuss off label use and/or investigational use in my presentation
LEARNING OBJECTIVES FOR COPD EDUCATORS
 LEARNING OBJECTIVES FOR COPD EDUCATORS For further Information contact: INTERNATIONAL NETWORK FOR RESPIRATORY CARE 16851 Mount Wolfe Road Caledon, ON Canada L7E 3P6 Phone: 905 880-1092 Fax: 905 880-9733
LEARNING OBJECTIVES FOR COPD EDUCATORS For further Information contact: INTERNATIONAL NETWORK FOR RESPIRATORY CARE 16851 Mount Wolfe Road Caledon, ON Canada L7E 3P6 Phone: 905 880-1092 Fax: 905 880-9733
Managing Inflammatory Arthritis. What to Discuss with Your Health Care Team
 Managing Inflammatory Arthritis What to Discuss with Your Health Care Team Section 1 Introduction What to Discuss with Your Health Care Team This tool has been created with input from patients to provide
Managing Inflammatory Arthritis What to Discuss with Your Health Care Team Section 1 Introduction What to Discuss with Your Health Care Team This tool has been created with input from patients to provide
Modifiable and non-modifiable risk factors
 Checklist Session time: 20 minutes You will need Training card 4 Visual card 4 Session 4 Modifiable and non-modifiable risk factors The aim of the session is to understand: What a risk factor is. What
Checklist Session time: 20 minutes You will need Training card 4 Visual card 4 Session 4 Modifiable and non-modifiable risk factors The aim of the session is to understand: What a risk factor is. What
Chronic Obstructive Pulmonary Disease (COPD)
 James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
Support for Kidney Cancer
 Page 1 Fact sheet Introduction Our series of kidney cancer fact sheets have been developed to help you understand more about kidney cancer. This fact sheet provides support information for people affected
Page 1 Fact sheet Introduction Our series of kidney cancer fact sheets have been developed to help you understand more about kidney cancer. This fact sheet provides support information for people affected
Follow-Up Patient Self-Assessment (Version 2)
 Follow-Up Patient Self-Assessment (Version 2) Demographics: Name: Address: E-mail: Phone Number: Date of Birth: What is your height? What is your current weight? feet inches lbs Have there been any change(s)
Follow-Up Patient Self-Assessment (Version 2) Demographics: Name: Address: E-mail: Phone Number: Date of Birth: What is your height? What is your current weight? feet inches lbs Have there been any change(s)
Executive Summary Report Sample Executive Report Page 1
 Sample Executive Report Page 1 Introduction This report summarizes the primary health findings for those individuals who completed the Personal Wellness Profile (PWP) health assessment. Group health needs
Sample Executive Report Page 1 Introduction This report summarizes the primary health findings for those individuals who completed the Personal Wellness Profile (PWP) health assessment. Group health needs
Smoking and Quitting Assessment
 Smoking and Quitting Assessment A. Which of the following describes you? q I m not interested in trying to quit smoking. q I know I need to quit smoking, but I m not quite ready yet. q I m ready to quit
Smoking and Quitting Assessment A. Which of the following describes you? q I m not interested in trying to quit smoking. q I know I need to quit smoking, but I m not quite ready yet. q I m ready to quit
Assessing Readiness To Change
 Assessing Readiness To Change Transtheoretical Model The Transtheoretical Model describes the stages of behavior prior to change. It focuses on the individual s decision making. This model involves the
Assessing Readiness To Change Transtheoretical Model The Transtheoretical Model describes the stages of behavior prior to change. It focuses on the individual s decision making. This model involves the
Session Eleven - Taking Care of Yourself
 147 Session Eleven - Taking Care of Yourself Materials Needed: Handout U: Taking Care of Yourself I. Challenges of dealing with mental illness in the family Discussion Questions: What is the hardest part
147 Session Eleven - Taking Care of Yourself Materials Needed: Handout U: Taking Care of Yourself I. Challenges of dealing with mental illness in the family Discussion Questions: What is the hardest part
The New York State Cessation Center Collaborative Statewide Conference Call. Jonathan Fader, PhD
 Motivational Interviewing & the Five R s: Helping Clients Who Aren t Ready to Quit The New York State Cessation Center Collaborative Statewide Conference Call Jonathan Fader, PhD September 2, 2009 Disclosure
Motivational Interviewing & the Five R s: Helping Clients Who Aren t Ready to Quit The New York State Cessation Center Collaborative Statewide Conference Call Jonathan Fader, PhD September 2, 2009 Disclosure
Living with COPD: 5 steps to better lung health
 Living with COPD: 5 steps to better lung health Breathe better Feel good Do more Name: Date: COPD or chronic obstructive pulmonary disease mainly affects your lungs and how well you can breathe, but it
Living with COPD: 5 steps to better lung health Breathe better Feel good Do more Name: Date: COPD or chronic obstructive pulmonary disease mainly affects your lungs and how well you can breathe, but it
Anti-tussivestussives
 PULMONARY REHABILITATION IN COPD WHAT DO WE OFFER ROUTINELY? Treatment of exacerbation Treatment of heart failure Treatment of infection Maintainance pharmacotherapy Domicillary oxygen Help for smoking
PULMONARY REHABILITATION IN COPD WHAT DO WE OFFER ROUTINELY? Treatment of exacerbation Treatment of heart failure Treatment of infection Maintainance pharmacotherapy Domicillary oxygen Help for smoking
Let s Sleep On It. Session Overview. Let s Sleep On It. Welcome and Introductions Presenter: Rita Piper, VP of Wellness
 Let s Sleep On It Let s Sleep On It Welcome and Introductions Presenter: Rita Piper, VP of Wellness Session Overview Why Sleep is so Important Types of Sleep Common Sleep Disruptors Sleep Disorders Tips
Let s Sleep On It Let s Sleep On It Welcome and Introductions Presenter: Rita Piper, VP of Wellness Session Overview Why Sleep is so Important Types of Sleep Common Sleep Disruptors Sleep Disorders Tips
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO. Preparing to Quit. About This Kit
 MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Preparing to Quit About This Kit There is no one best way to quit smoking. Your Heart Institute Prevention and Rehabilitation
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Preparing to Quit About This Kit There is no one best way to quit smoking. Your Heart Institute Prevention and Rehabilitation
Living well with COPD
 This factsheet aims to show people with chronic obstructive pulmonary disease (COPD) and their friends and family how they can live a full life with this disease. What is COPD? COPD is a condition that
This factsheet aims to show people with chronic obstructive pulmonary disease (COPD) and their friends and family how they can live a full life with this disease. What is COPD? COPD is a condition that
Beyond Physical Therapy: Incorporating Health Promotion into Your Practice to Help Your Patients Move Better, Feel Better, Live Better
 Saturday, March 25, 2017 10:30 am 11:50 am Auditorium Dr. Janet Bezner, PT, DPT, PhD Beyond Physical Therapy: Incorporating Health Promotion into Your Practice to Help Your Patients Move Better, Feel Better,
Saturday, March 25, 2017 10:30 am 11:50 am Auditorium Dr. Janet Bezner, PT, DPT, PhD Beyond Physical Therapy: Incorporating Health Promotion into Your Practice to Help Your Patients Move Better, Feel Better,
Cannabis. Screening and Action Planning Toolkit. A toolkit for those who are concerned about their cannabis use and those who support them.
 Cannabis Screening and Action Planning Toolkit A toolkit for those who are concerned about their cannabis use and those who support them. V1.: 015 About this tool: Cannabis dependency hasn t always been
Cannabis Screening and Action Planning Toolkit A toolkit for those who are concerned about their cannabis use and those who support them. V1.: 015 About this tool: Cannabis dependency hasn t always been
Health Behaviour Change: Applying Prochaska and DiClemente s Stages of Change Model
 Health Behaviour Change: Applying Prochaska and DiClemente s Stages of Change Model Image Sources http://www.clevelandseniors.com/forever/100 smoker.htm http://bacontoday.com/bacon flavored diet coke/
Health Behaviour Change: Applying Prochaska and DiClemente s Stages of Change Model Image Sources http://www.clevelandseniors.com/forever/100 smoker.htm http://bacontoday.com/bacon flavored diet coke/
CREATING YOUR DAILY ROADMAP Creating Your Daily Roadmap
 CREATING YOUR DAILY ROADMAP Creating Your Daily Roadmap If you've been diagnosed with idiopathic pulmonary fibrosis (IPF), then you're sure to have a lot of questions. People with IPF can experience a
CREATING YOUR DAILY ROADMAP Creating Your Daily Roadmap If you've been diagnosed with idiopathic pulmonary fibrosis (IPF), then you're sure to have a lot of questions. People with IPF can experience a
Not sure if a talking therapy is for you?
 South Tyneside NHS Foundation Trust Primary Care Mental Health Service Not sure if a talking therapy is for you? Take a look at the different types of therapy we have available to find out more about them.
South Tyneside NHS Foundation Trust Primary Care Mental Health Service Not sure if a talking therapy is for you? Take a look at the different types of therapy we have available to find out more about them.
handouts for women 1. Self-test for depression symptoms in pregnancy and postpartum Edinburgh postnatal depression scale (epds) 2
 handouts for women 1. Self-test for depression symptoms in pregnancy and postpartum Edinburgh postnatal depression scale (epds) 2 2. The Cognitive-Behaviour Therapy model of depression 4 3. Goal setting
handouts for women 1. Self-test for depression symptoms in pregnancy and postpartum Edinburgh postnatal depression scale (epds) 2 2. The Cognitive-Behaviour Therapy model of depression 4 3. Goal setting
Chronic Fatigue Syndrome (CFS) / Myalgic Encephalomyelitis/Encephalopathy (ME)
 Chronic Fatigue Syndrome (CFS) / Myalgic Encephalomyelitis/Encephalopathy (ME) This intervention (and hence this listing of competences) assumes that practitioners are familiar with, and able to deploy,
Chronic Fatigue Syndrome (CFS) / Myalgic Encephalomyelitis/Encephalopathy (ME) This intervention (and hence this listing of competences) assumes that practitioners are familiar with, and able to deploy,
Chronic Obstructive Pulmonary Disease (COPD) Self-management plan
 Chronic Obstructive Pulmonary Disease (COPD) Self-management plan Respiratory Respiratory Nurses Royal Lancaster Infirmary & Westmorland General Hospital 01524 583608 Furness General Hospital 01229 403584
Chronic Obstructive Pulmonary Disease (COPD) Self-management plan Respiratory Respiratory Nurses Royal Lancaster Infirmary & Westmorland General Hospital 01524 583608 Furness General Hospital 01229 403584
Worries and Anxiety F O R K I D S. C o u n s e l l i n g D i r e c t o r y H a p p i f u l K i d s
 Worries and Anxiety F O R K I D S C o u n s e l l i n g D i r e c t o r y H a p p i f u l K i d s Contents What is anxiety? Types of anxiety What does anxiety look like? Top tips for tackling worries Asking
Worries and Anxiety F O R K I D S C o u n s e l l i n g D i r e c t o r y H a p p i f u l K i d s Contents What is anxiety? Types of anxiety What does anxiety look like? Top tips for tackling worries Asking
Your Guide to a Smoke Free Future
 Your Guide to a Smoke Free Future If you smoke, or if you have quit within the past 2 months, then ask for our detailed handout which provides information on how to begin and maintain a smoke-free lifestyle.
Your Guide to a Smoke Free Future If you smoke, or if you have quit within the past 2 months, then ask for our detailed handout which provides information on how to begin and maintain a smoke-free lifestyle.
Tobacco Cessation For Providers. Betty Murphy Health Promotion Program Naval Hospital Rota
 Tobacco Cessation For Providers Betty Murphy Health Promotion Program Naval Hospital Rota Tobacco Statistics Strategies for Implementation Stages of Change Pharmacotherapy Tobacco Use Statistics 70% of
Tobacco Cessation For Providers Betty Murphy Health Promotion Program Naval Hospital Rota Tobacco Statistics Strategies for Implementation Stages of Change Pharmacotherapy Tobacco Use Statistics 70% of
DISCLAIMER: ECHO Nevada emphasizes patient privacy and asks participants to not share ANY Protected Health Information during ECHO clinics.
 DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
COPD. Living With Long-Term Lung Disease. COPD is a lung disease that. makes it harder to breathe. Doctors can help people
 Living With Long-Term Lung Disease COPD is a lung disease that makes it harder to breathe. Doctors can help people with COPD feel better, live more active lives, and slow the damage to their lungs. The
Living With Long-Term Lung Disease COPD is a lung disease that makes it harder to breathe. Doctors can help people with COPD feel better, live more active lives, and slow the damage to their lungs. The
Motivational Interviewing Maureen P. Scahill, NP, MS Center for Health & Behavioral Training
 Motivational Interviewing Maureen P. Scahill, NP, MS Center for Health & Behavioral Training Infectious Disease Division, Department of Medicine, University of Rochester Medical Center STD/HIV Program,
Motivational Interviewing Maureen P. Scahill, NP, MS Center for Health & Behavioral Training Infectious Disease Division, Department of Medicine, University of Rochester Medical Center STD/HIV Program,
WORTH A CLOSER LOOK.
 A birth control pill... WORTH A CLOSER LOOK. Ask your healthcare provider about. Please see Important Safety Information including Boxed Warning throughout this brochure and on pages 4 and 5. offers a
A birth control pill... WORTH A CLOSER LOOK. Ask your healthcare provider about. Please see Important Safety Information including Boxed Warning throughout this brochure and on pages 4 and 5. offers a
For groups of young people aged 15 to 21
 Drug Awareness Week ACTIVITY GUIDE 2010 10-001-13WA Gouvernement du Québec, 2010 For groups of young people aged 15 to 21 Drug Awareness Week ACTIVITY GUIDE 2010 For groups of young people aged 15 to 21
Drug Awareness Week ACTIVITY GUIDE 2010 10-001-13WA Gouvernement du Québec, 2010 For groups of young people aged 15 to 21 Drug Awareness Week ACTIVITY GUIDE 2010 For groups of young people aged 15 to 21
Become a Partner with Your Clinician to Improve Your Health
 What is health? You may think this is a simple question or even a silly one. Everyone knows that being healthy means not feeling sick or having a disease. Right? But health is more than this. The World
What is health? You may think this is a simple question or even a silly one. Everyone knows that being healthy means not feeling sick or having a disease. Right? But health is more than this. The World
Chapter 5. Group & Social Influences on Exercise
 Chapter 5 Group & Social Influences on Exercise Social Influence Real or imagined pressure to change one s behavior, attitudes, or beliefs Can come from doctors, fitness leaders, family members, and so
Chapter 5 Group & Social Influences on Exercise Social Influence Real or imagined pressure to change one s behavior, attitudes, or beliefs Can come from doctors, fitness leaders, family members, and so
Smoking Cessation Medbelle Information Brochure
 Smoking Cessation Medbelle Information Brochure Why we prepared this brochure for you Hi, my name is Sarah. I m a cosmetic treatment adviser with Medbelle. Every day, I speak with men and women in the
Smoking Cessation Medbelle Information Brochure Why we prepared this brochure for you Hi, my name is Sarah. I m a cosmetic treatment adviser with Medbelle. Every day, I speak with men and women in the
Motivational Interviewing
 Motivational Interviewing April Wiechmann, PhD Assistant Professor Associate Director of the Memory Disorders Clinic Department of Geriatrics Adapted with permission from Dr. Susan Franks and Dr. James
Motivational Interviewing April Wiechmann, PhD Assistant Professor Associate Director of the Memory Disorders Clinic Department of Geriatrics Adapted with permission from Dr. Susan Franks and Dr. James
All About Smoking Cessation Going for the 3 Increases: Increase in Health, Increase in Happiness & Increase in Energy
 All About Smoking Cessation Going for the 3 Increases: Increase in Health, Increase in Happiness & Increase in Energy Strategies for Success in Health Management By: James J. Messina, Ph.D. Negative Impact
All About Smoking Cessation Going for the 3 Increases: Increase in Health, Increase in Happiness & Increase in Energy Strategies for Success in Health Management By: James J. Messina, Ph.D. Negative Impact
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
Pain Rehabilitation Executive Program
 Pain Rehabilitation Executive Program The Mayo Clinic Pain Rehabilitation Executive Program (PREP) is an intensive 2-day rehabilitation program for patients with chronic pain. The PREP provides an overview
Pain Rehabilitation Executive Program The Mayo Clinic Pain Rehabilitation Executive Program (PREP) is an intensive 2-day rehabilitation program for patients with chronic pain. The PREP provides an overview
Questions to ask your healthcare professional
 Prepare to quit Get ready! Talk to your healthcare professional about how to quit Set a date for quitting. Choose a date that is within the next 2 weeks and make a strong commitment to quit on that day
Prepare to quit Get ready! Talk to your healthcare professional about how to quit Set a date for quitting. Choose a date that is within the next 2 weeks and make a strong commitment to quit on that day
physical Many of us know that having a healthy body weight is important for our health.
 Healthy weight and physical activity Many of us know that having a healthy body weight is important for our health. However, we also know that managing our body weight is not easy. The good news is that
Healthy weight and physical activity Many of us know that having a healthy body weight is important for our health. However, we also know that managing our body weight is not easy. The good news is that
Participation - Demographics. Age Ranges*
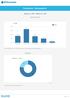 Participation - Demographics January 1, 2017 - March 31, 2017 Age Ranges* 50% n = 139 42.4% Total 38% 25% 20.9% 20.1% 13% 12.9% 3.6% 0% 18-29 years 30-39 years 40-49 years 50-59 years 60+ * Age ranges
Participation - Demographics January 1, 2017 - March 31, 2017 Age Ranges* 50% n = 139 42.4% Total 38% 25% 20.9% 20.1% 13% 12.9% 3.6% 0% 18-29 years 30-39 years 40-49 years 50-59 years 60+ * Age ranges
Concussion & You. A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL
 Concussion & You A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL Trusted experts in youth concussion www.hollandbloorview.ca/concussion
Concussion & You A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL Trusted experts in youth concussion www.hollandbloorview.ca/concussion
Kelly J. Lundberg, Ph.D. Associate Professor, Department of Psychiatry Executive Director, ARS Director of Psychotherapy Training, Adult Psychiatry
 Kelly J. Lundberg, Ph.D. Associate Professor, Department of Psychiatry Executive Director, ARS Director of Psychotherapy Training, Adult Psychiatry Residency Program University of Utah kelly.lundberg@hsc.utah.edu
Kelly J. Lundberg, Ph.D. Associate Professor, Department of Psychiatry Executive Director, ARS Director of Psychotherapy Training, Adult Psychiatry Residency Program University of Utah kelly.lundberg@hsc.utah.edu
Motivation and Emotion. Unit 2: Biopsychology
 Motivation and Emotion Unit 2: Biopsychology Theories of Motivation Motivation: an internal state that activates behaviour and directs it towards a goal. Motivation cannot be observed directly so psychologists
Motivation and Emotion Unit 2: Biopsychology Theories of Motivation Motivation: an internal state that activates behaviour and directs it towards a goal. Motivation cannot be observed directly so psychologists
The Eating Disorders Service
 Contact us Clinical Team Leader Eating Disorders Service Steps Unit Southmead Hospital Bristol BS10 5NB 0117 3236113 www.awp.nhs.uk The Eating Disorders Service PALS To make a comment, raise a concern
Contact us Clinical Team Leader Eating Disorders Service Steps Unit Southmead Hospital Bristol BS10 5NB 0117 3236113 www.awp.nhs.uk The Eating Disorders Service PALS To make a comment, raise a concern
SRP Component 1. PART II: Session-by-Session Guide
 SRP Component 1 PART II: Session-by-Session Guide Phase 2: Motivational Interviewing Therapists use Motivational Interviewing to provide feedback on the assessment results and to help a client reach a
SRP Component 1 PART II: Session-by-Session Guide Phase 2: Motivational Interviewing Therapists use Motivational Interviewing to provide feedback on the assessment results and to help a client reach a
Choosing Life: Empowerment, Action, Results! CLEAR Menu Sessions. Health Care 3: Partnering In My Care and Treatment
 Choosing Life: Empowerment, Action, Results! CLEAR Menu Sessions Health Care 3: Partnering In My Care and Treatment This page intentionally left blank. Session Aims: Partnering In My Care and Treatment
Choosing Life: Empowerment, Action, Results! CLEAR Menu Sessions Health Care 3: Partnering In My Care and Treatment This page intentionally left blank. Session Aims: Partnering In My Care and Treatment
COPD. The goals of COPD. about. you quit. If you. efforts to quit. Heart
 How Is COPD Treated? COPD has no cure yet. However, lifestyle changes and treatments can help you feel better, stay more active, and slow the progress of the disease. The goals of COPD treatment include:
How Is COPD Treated? COPD has no cure yet. However, lifestyle changes and treatments can help you feel better, stay more active, and slow the progress of the disease. The goals of COPD treatment include:
Planning for Your Surgery and Recovery at Home A guide and checklist to help you plan ahead for your total knee replacement surgery
 Patient Education Planning for Your Surgery and Recovery at Home A guide and checklist to help you plan ahead for your total knee replacement surgery Total knee replacement surgery is a choice you have
Patient Education Planning for Your Surgery and Recovery at Home A guide and checklist to help you plan ahead for your total knee replacement surgery Total knee replacement surgery is a choice you have
