Revised 8/4/2007. Trauma
|
|
|
- Britton Simmons
- 5 years ago
- Views:
Transcription
1 Trauma 57
2 General Principles for Trauma Emergencies 1. Do NOT delay transport for treatment. Beyond rapid trauma assessment, establishing an airway (with basic or advanced techniques), spinal immobilization and control of life threatening hemorrhage, the priority in caring for the trauma patient is rapid evacuation of the patient with further care performed en route to the hospital. 2. As a first responder, the priority for Rice EMS is to manage the CABCs and package the patient for transport. Criteria: Any patient suffering from significant trauma, especially when alcohol is involved Scene safety CABC s (Cervical Safety) CPR if necessary V/S Dress open wounds that are bleeding profusely Splinting as appropriate only after life threats are stabilized If hypotensive (systolic BP less than 90 mm/hg), place in Trendelenburg position If open chest or abdominal wound, apply an occlusive dressing EMT-l: Control airway with endotracheal tube or alternative airway device as needed. IV: NS, largest bore possible 58
3 Amputation Criteria: Patient with a part that is pathologically or surgically totally separated (removed) from the rest of the body CABCs Glascow Coma Scale SpO 2 if available V/S Hemorrhage control EMT-I: IV: NS titrated to systolic BP of at least 100 mmhg in adult, largest bore possible. Intubate if necessary C-spine immobilization if needed Oxygen should be at L/min via NRB 100% oxygen IV must be NS titrated to a systolic of at least 100 mmhg in the adult. IV catheters should be the largest bore possible Splint associated fractures Amputated parts SHOULD be: o Rinsed with sterile normal saline o Placed in a plastic bag o Kept cool during transport to the hospital Amputated parts should NOT be: o Soaked or placed in water o Covered with soaked wet gauze or towels o Placed directly on ice or ice packs, as this can result in frostbite Amputations are disabling and sometimes are life-threatening injuries. They have the potential for massive hemorrhage, but most often, the bleeding will control itself with pressure applied to the stump. The stump should be covered with a damp sterile dressing and an elastic wrap that will apply uniform, reasonable pressure across the entire stump. If bleeding absolutely cannot be controlled with pressure and there is a prolonged delay of ambulance transport, a tourniquet may be used. In general, a tourniquet is to be avoided whenever possible. It should be applied as distally as possible. The patient should be transported directly to a facility capable of performing reattachments, if the part appears at all salvageable. 59
4 Bites and Stings Insects Criteria: Known or suspected envenomation by: Hymenoptera Ants Brown recluse spider Black widow spider Remove patient from environment as necessary o Scene safety o If suspect venomous animal bite/sting and animal is dead, place body in sealed container and take to ER for identification ONLY IF IT IS SAFE TO DO SO. CABCs SpO 2 if available V/S If there is an allergic reaction, refer to allergic reaction protocol Remove stinger or venom sacs if present Remove tight clothing and jewelry on affected extremity Apply cool compress for pain control If stinger, wash site with soap and water (if available) EMT-I: IV NS TKO Symptoms and findings of these envenomation include: Ants, Bees, and Wasps Symptoms: Immediate pain Signs: Vary from local reaction to anaphylaxis. Brown Recluse Symptoms: Localized immediate pain, nausea, vomiting, weakness, fever Signs: A blister forms at the bite, which develops into an ulcerative lesion. Cardiac dysrhythmia, hemolysis, renal failure, and shock Black Widow Symptoms: Immediate pain which may subside, muscle cramps and muscle pain which develop in 1/2 to 2 hours after bite, weakness, back pain, abdominal pain Signs: Muscle rigidity (tetany), convulsions, respiratory paralysis 60
5 Bites and Stings (continued) Insects (continued) Oxygen administration is optional in the asymptomatic or very mildly symptomatic patient. It should be by NRB at L/min in the moderately to severely ill patient. IV access is optional in the asymptomatic or very mildly symptomatic patient. It should be NS titrated to an adequate systolic in all other patients. 61
6 Bites and Stings (continued) Snake Bites Criteria: Known bite by a venomous snake Fang marks, swelling and pain at wound site CABC's V/S If coral snake bite, wash wound immediately with copious amounts of water Keep patient supine and treat symptoms Immobilize limb with splint at the level of the heart DO NOT APPLY ICE, COLD PACK OR ARTERIAL TOURNIQUET If possible, send dead snake to ER If bite is on upper extremity, remove all jewelry Mark edge of swelling and note time EMT-I: IV: NS, titrate to maintain an adequate systolic BP. TRANSPORT IMMEDIATELY Texas has four endogenous venomous snakes: rattlesnakes, water moccasins, copperheads, and coral snakes. Bites by the coral snake are very rare. Only about 50% of snake bites result in envenomation. However, EMS personnel should assume that if the patient has been bitten by a known venomous snake, or by any type of unknown snake, that he/she has been envenomed. The coral snake's venom is essentially a neurotoxin, resulting in altered mental status, seizures, peripheral motor difficulties, paresthesia, respiratory depression and paralysis. Though quite rare, significant envenomation by a coral snake carries a very high mortality rate. The venom of the other three snakes, all pit vipers, is primarily a hemotoxin with some neurotoxin components. With these bites, the patient may present with a wide range of symptoms and signs, varying from little or no local reaction to massive local tissue destruction, generalized hemolysis, shock, kidney failure, and widespread ischemia and infarcts. Factors which influence the patient s clinical status include: Whether or not the snake actually envenomated the victim The size of the snake in relation to the size of the victim: in general, the larger the snake and/or the smaller the victim the more severe the consequences of a bite The type of snake: copperhead bites are generally less toxic than water moccasin bites, which in turn are less toxic than rattlesnake bites. Coral snakes, although 62
7 Bites and Stings (continued) Snake Bites (continued) possessing more toxic venom, rarely inject an adequate volume to result in severe illness. Conversely, pit vipers generally inject a much greater volume. Movement expedites the spread of the venom. Therefore, the patient's physical activity MUST be kept to an absolute minimum. There are many debates concerning the usefulness of constricting bands. At this point, they cannot be clearly supported or eliminated from use. If a constricting band is used, be certain that the constricting band is obstructing venous flow only, and that the patient retains a good pulse distal to the band. 63
8 Burns Criteria: Patient sustaining tissue injury from any of the following types of burns: Thermal Chemical Electrical Lightning Remove patient from burn source CABCs Assess body surface area effected Airway management as necessary V/S with SpO2 if available C-spine immobilization if necessary If chemical, brush off and flush with water If <10% BSA, cool burns with sterile saline Dress with dry sterile burn sheet Remove jewelry and clothing from affected areas EMT-I: IV NS TKO, unless hypotensive (BP < 90 mmhg) then titrate to a SBP > 100 mmhg with 20 ml/kg bolus (Do not initiate in burned extremity if possible) Intubate if necessary The removal of victims from the heat source takes priority over all other treatments. Airway management including intubation should be considered. Oxygen must be via NRB at L/min. Ventilation injuries, if severe, should be treated with endotracheal intubation (the Nasotracheal route is preferred) and mechanical ventilation. Absolute indications for intubation: Rapid, shallow ventilation with tachypnea of breaths/min AND decreased mental status. Respiratory rate of less than 8-10 breaths/min Mechanical airway obstruction from trauma, edema, or laryngospasm Unconsciousness Relative indications for intubation: History of an enclosed space explosion or fire Singed nasal hairs or oral mucosa Erythema of the palate, soot in the mouth, larynx or sputum Edema associated with a burn of the face or neck Signs of respiratory distress such as nasal flaring, respiratory crowing or stridor, anxiety, agitation, or combativeness. 64
9 Burns (continued) Burns are classified by their depth: Superficial (First degree): Limited to the most superficial layers of the skin, producing redness and pain, as in mild or moderate sunburn. There are no blisters and the surface markedly and widely blanches to light pressure. Partial Thickness (Second degree): Penetrates the skin deeper, producing pain and blistering, as well as some subcutaneous edema Blisters may or may not form The base blisters may be erythematous or whitish with fibrinous exudate Full Thickness (Third degree): Involves damage to or destruction of the full thickness of the skin and can involve underlying muscle, bone, and other structures as well. Third degree burns may, but generally do not, present with blisters The surface may be white and pliable when pressure is applied or it may be black, charred, and leathery Third degree burns may be pale in color and mistaken for normal skin, but the subdermal vessels do not blanch to pressure Body temperature should be closely followed because hypothermia occurs frequently in the extensively burned patient. IV s must be NS and should be as large bore as possible. Acute hypotension is rarely found in the early stages of burns. If hypotension is present, consider other possible causes, i.e.; hypovolemia, hypoxia, or undetected underlying injuries. Parkland Burn Formula: (IV fluids for first 8 hours) (% Burn Area) x (Pt. Wt. in Kg) = cc/hr 4 NOTE: This formula does not apply to patients in shock. The patient in shock needs more aggressive IV fluid replacement and should be treated accordingly. Wound Care: The object of wound care in the burn patient is to prevent further damage and infection. Remove all clothing around the burn, but do not pull any clothing that is stuck to the wound. DO NOT apply ointment or solutions to the wound. Cooling, with sterile saline is appropriate for small (<10% BSA burns). Saline should not be used on larger burns; they should be covered with dry, sterile dressings. TIME IS OF THE ESSENCE! 65
10 Burns (continued) Burns requiring a burn facility are as follows: *See Rule of Nines in Reference Section Size: Second degree >30% BSA Third degree >10% BSA Burns with associated significant injuries Burns with associated inhalation injury Involvement of face, hands, or genitalia Circumferential burns Chemical substances requiring special consideration: Dry Lime and soda ash should be brushed off because contact with water will form a corrosive substance. These areas should not be irrigated unless they are already wet. Large quantities of water should be used if the burning process has already begun. Phenol (carbolic acid) is not water-soluble and will not be removed well by water irrigation. It is alcohol-soluble, however, and the affected area should therefore be washed with any alcohol product (e.g. rubbing alcohol, gin, scotch) prior to prolonged flushing with water. Lithium and sodium metal produce considerable heat when mixed with water and may explode. Therefore any large chunks remaining in or around the burn must be placed in oil. After this is done the burn should be washed with copious amounts of water. 66
11 Burns (continued) Remember that chemical injuries are frequently deceiving in that initial skin changes may be minimal even when the injury is severe. Only steam inhalation causes actual thermal damage to the respiratory tract. Inhalation of hot gases can cause immediate upper airway obstruction; airway edema can produce a slower developing upper airway obstruction; and injury to the capillaries of the small airways and alveoli can cause delayed progressive respiratory failure. For all inhalation injuries determine: The nature of the inhalant Duration of exposure Whether the patient was in a closed environment Whether the patient experienced any loss of consciousness For Chemical burns of the eye, refer to the Eye Injury protocol. 67
12 Eye Injury Criteria: Patient who has sustained Injuries to the globe, open or closed, with or without loss of vision and finding of: Corneal abrasion Foreign body in eye Chemical burn Lacerated or avulsed globe Excessive tearing and burning of eyes Arc" burn of globe EMT-B/EMT-I: CABCs o C-spine immobilization if indicated Glascow Coma Scale V/S with SpO2 if available Bandage o If open injury to globe, shield both eyes If chemical burn, flush with sterile saline Chemical burns can cause catastrophic, rapid damage. Therefore, it is imperative to intervene and stop the reaction as soon as possible with by flushing the eye with sterile saline. Flushing of the eye may result in vagal stimulation, with transient hypotension, dizziness, and nausea. These symptoms will usually resolve when flushing is stopped. Flushing a non-intact (disrupted) globe may cause serious injury to the eye. The disrupted globe must be immobilized. The best way to immobilize the eye is to obstruct vision in both eyes by patching. When covering an eye, be sure that no pressure is exerted on the globe. An injury that does not involve or disrupt the globe, such as a simple corneal abrasion, requires the covering of only the affected eye. However, if you are not certain of the extent of the injury, cover both eyes. A foreign body that penetrates the globe should be left in place and supported if necessary, and both eyes should be covered. 68
13 Head Trauma Criteria: Patient sustaining an open or closed head injury with either: Substantial mechanism of injury Altered mental status Loss of consciousness Isolated or in the presence of other injuries, with the exception of patients meeting Multi-System Trauma criteria CABCs o C-spine immobilization Alternative airway device if necessary V/S with SpO2 if available Blood glucose analysis: if less than 80 mg/dl, refer to hypoglycemia protocol EMT-I: IV NS TKO unless hypotensive, BP < 90 mmhg, then titrate to a SBP of 100 mmhg with 20 ml/kg bolus Intubate if necessary Mental status is by far the single most important finding in determining the significance of a head injury. V/S may reflect increasing intracranial pressure or brain injury (Cushing's reflex: increased blood pressure, decreased pulse rate, and irregular respirations), but are far less reliable than mental status. This includes information about a loss of consciousness prior to your arrival. If the altered mental status is out of proportion for the apparent injury, consider the altered mental status protocol. Intubation should be utilized to secure the airway and permit hyperventilation (if the patient is exhibiting decerebrate posturing) in the patient whose mental status permits. Generally, any patient who has a Glasgow Coma score of 7 or less should be intubated. Oral intubation is preferred in the deeply comatose patient. Approximately 5-20% of head injury patients have cervical spine injury, so if oral intubation is to be used, extreme caution and modified technique must be employed. An additional person should provide manual cervical spine immobilization during intubation attempts. Seizures will markedly increase ICP. If the head-injured patient is wearing a helmet, such as for motorcycle riding, the prehospital personnel should remove the helmet prior to completing spinal immobilization. Helmets should be removed carefully, using two rescuers, so as not to cause movement of the cervical spine for three primary reasons: 1. The helmet will prevent a complete exam of the patient's head. 2. The helmet will interfere with airway and oxygenation management. 3. The helmet will put the patient's head in flexion, especially if the patient is young. Intravenous access should be large bore, and the fluid of choice is NS. Remember that head injuries rarely result in hypovolemia, so if hypotension is seen, reassess for other injuries. 69
14 Multi-System Trauma Criteria: Injury to the chest, abdomen, pelvis, or extremities with evidence of possibly significant injury Multiple soft-tissue or musculoskeletal injuries with evidence of compensated or uncompensated shock CABCs V/S EMT-I: IV: NS, largest bore possible; titrate systolic blood pressure to >90 mmhg with 20 ml/kg bolus Findings or complaints related to the chest, abdomen, or pelvis must elicit an aggressive response, as these injuries are associated with high morbidity. This is especially true in the elderly patient. Tachycardia in the normotensive trauma patient must be considered to represent compensated shock. Hypotension will not be seen until late in the shock cycle. Airway management and oxygenation must be aggressive. If the patient can be intubated, he should be. Always assist ventilations with the BVM unless the patient's respiratory rate and tidal volume are good, and then use high flow oxygen, via NRB mask. Continual reassessment of the airway and ventilatory status is imperative. TRANSPORT IS TREATMENT in the trauma patient, so REMS personnel should focus on preparing the patient for transport. Spinal precautions influence all aspects of treatment in the trauma patient. Always use airway, ventilation, intubation, assessment, and movement techniques that minimize or eliminate potential aggravation of spinal injury. Hallmark findings of a tension pneumothorax include: EARLY Unilateral decreased or absent breath sounds Continually increasing dyspnea and tachypnea Signs of acute, profound hypoxia LATE JVD Contra lateral tracheal deviation Cardiovascular collapse Tension pneumothorax should also be suspected in the unconscious trauma patient in whom there is unusually high resistance to BVM ventilation. 70
15 Near Drowning/Drowning Criteria: Water submersion WITH or WITHOUT cardiopulmonary arrest WITHOUT evidence of hypothermia Remove from water CABCs If apneic o Initiate and maintain mechanical ventilation with 100% oxygen If pulseless o Initiate CPR o AED C-Spine V/S including SpO 2 if available Blood glucose analysis: if less than 80 mg/dl, refer to hypoglycemia protocol If hypotensive, elevate legs EMT-I: IV: NS TKO (unless hypotensive, BP < 90 mmhg, then titrate to a systolic BP > 100 mmhg with 20 ml/kg bolus) If unconscious, endotracheal intubation or alternative airway device Quickly identify the need for rapid transport. If hypothermic, treat as per "Hypothermia" protocol. Ensure Dispatch advises HFD that an ALS unit is needed. 71
Chapter 29. Objectives. Objectives 01/09/2013. Burns
 Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Pediatric Trauma Care
 2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02
 PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Frontline First Aid 2012 Emergency Care Manual Treatments
 Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Module Summaries: The emergency plan is a crucial part of the total sports program.
 Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Chapter 28. Objectives. Objectives 01/09/2013. Bleeding and Soft-Tissue Trauma
 Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Restore adequate respiratory and circulatory conditions. Reduce pain
 Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Advanced Assessment and Treatment of Trauma
 Advanced Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls
Advanced Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D.
 1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Pre-hospital Trauma Life Support. Rattiya Banjungam Emergency Physician, Khon Kaen Hospital
 Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
UNIT 4: DISASTER MEDICAL OPERATIONS
 UNIT 4: DISASTER MEDICAL OPERATIONS PART 2 Patient Evaluation: How to perform a head-to-toe assessment to identify and treat injuries. Basic Treatment How to: Treat burns Dress and bandage wounds Treat
UNIT 4: DISASTER MEDICAL OPERATIONS PART 2 Patient Evaluation: How to perform a head-to-toe assessment to identify and treat injuries. Basic Treatment How to: Treat burns Dress and bandage wounds Treat
Head Trauma Protocol
 Injuries to the head may cause underlying brain tissue damage. Increased intracranial pressure from bleeding or swelling tissue is a common threat after head trauma. Common signs and symptoms of increased
Injuries to the head may cause underlying brain tissue damage. Increased intracranial pressure from bleeding or swelling tissue is a common threat after head trauma. Common signs and symptoms of increased
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
First Aid Fact Sheet 2005 Standards
 First Aid Fact Sheet 2005 Standards Five Leading Causes of Unintentional death: 1. Motor vehicle accidents 2. Falls 3. Poisonings 4. Drownings 5. Choking Good Samaritan Laws laws that give legal protection
First Aid Fact Sheet 2005 Standards Five Leading Causes of Unintentional death: 1. Motor vehicle accidents 2. Falls 3. Poisonings 4. Drownings 5. Choking Good Samaritan Laws laws that give legal protection
Face and Throat Injuries. Chapter 26
 Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
FIRST AID & EMERGENCIES
 FIRST AID & EMERGENCIES Kelly Pederson, RN Chris DeLapp, CCH Education Manager Safety & Emergencies What is First Aid? Scene Survey Victim Assessment Bleeding Control Shock Burns Choking Basic First Aid
FIRST AID & EMERGENCIES Kelly Pederson, RN Chris DeLapp, CCH Education Manager Safety & Emergencies What is First Aid? Scene Survey Victim Assessment Bleeding Control Shock Burns Choking Basic First Aid
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
MIAMI-DADE COLLEGE. Common Course Number: HSC Course Title: Basic Emergency Care. Course Catalog Description:
 Common Course Number: HSC 2400 MIAMI-DADE COLLEGE Course Title: Basic Emergency Care Course Catalog Description: Designed to provide opportunities to develop, practice, and display skills concerning emergency
Common Course Number: HSC 2400 MIAMI-DADE COLLEGE Course Title: Basic Emergency Care Course Catalog Description: Designed to provide opportunities to develop, practice, and display skills concerning emergency
FIRST AID WRITTEN EXAM. Team Name: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. a. TRUE b. FALSE
 2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
QI. Read the following questions and choose the most correct answer (20 Marks):
 Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
PEDIATRIC TRAUMA EMERGENCIES
 PEDIATRIC TRAUMA EMERGENCIES Last Revised: January 2015 1 PEDIATRIC COMA SCALE Indicator Eye Opening Spontaneous 4 To verbal stimuli 3 To pain only 2 No response 1 Verbal Response Oriented, appropriate
PEDIATRIC TRAUMA EMERGENCIES Last Revised: January 2015 1 PEDIATRIC COMA SCALE Indicator Eye Opening Spontaneous 4 To verbal stimuli 3 To pain only 2 No response 1 Verbal Response Oriented, appropriate
Disaster Medical Operations Part 2. CERT Basic Training Unit 4
 Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
APPLY FIRST AID ONLINE WORKBOOK
 APPLY FIRST AID ONLINE WORKBOOK STUDENT NAME: ADDRESS: PHONE CONTACT: DATE OF COURSE: Welcome to CYNERGEX GROUP pre-learning package for the APPLY FIRST AID course. This workbook is to be completed in
APPLY FIRST AID ONLINE WORKBOOK STUDENT NAME: ADDRESS: PHONE CONTACT: DATE OF COURSE: Welcome to CYNERGEX GROUP pre-learning package for the APPLY FIRST AID course. This workbook is to be completed in
EmergencyKT: Management of Thermal Injury in Adult Patients
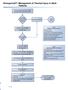 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
Aviation Rescue Swimmer Course
 Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
Environmental Injury and Illnesses. Dc. Anna Toplaghaltsyan
 Environmental Injury and Illnesses Dc. Anna Toplaghaltsyan Yerevan 2018 BITES AND STINGS Insect bites and stings are a common and an annoying occurrence. Most bites are minor but the potential for a serious
Environmental Injury and Illnesses Dc. Anna Toplaghaltsyan Yerevan 2018 BITES AND STINGS Insect bites and stings are a common and an annoying occurrence. Most bites are minor but the potential for a serious
2017 Northern Mine Rescue Contest Written Exam (First Aid Competition)
 2017 Northern Mine Rescue Contest Written Exam (First Aid Competition) 2017 2010 June 5, 2017 Findley Lake, New York 2017 Northern Mine Rescue Contest Written Exam First Aid Competition Directions: Fill
2017 Northern Mine Rescue Contest Written Exam (First Aid Competition) 2017 2010 June 5, 2017 Findley Lake, New York 2017 Northern Mine Rescue Contest Written Exam First Aid Competition Directions: Fill
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
POLICY/PROCEDURE. Issued By: Clinical Services. Policy No.: TX.009. Reference: Code 99 - TX.012. Date Issued: 2/99
 POLICY/PROCEDURE Title: Emergency Medical Care / First Aid Procedures Hanging Bleeding Poison/Overdose Nose Bleeds Drowning Foreign Bodies in the Eye Burns Fractures Fainting Anaphylactic Reactions Hypoglycemic
POLICY/PROCEDURE Title: Emergency Medical Care / First Aid Procedures Hanging Bleeding Poison/Overdose Nose Bleeds Drowning Foreign Bodies in the Eye Burns Fractures Fainting Anaphylactic Reactions Hypoglycemic
BLS ROUTINE MEDICAL CARE
 BLS ROUTINE MEDICAL CARE Scene safety # Assure scene safety prior to patient contact C-spine # Perform manual cervical spine stabilization if indicated (Follow the cervical spine protocol.) ABCs # Assess
BLS ROUTINE MEDICAL CARE Scene safety # Assure scene safety prior to patient contact C-spine # Perform manual cervical spine stabilization if indicated (Follow the cervical spine protocol.) ABCs # Assess
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
ENVIRONMENTAL EMERGENCIES
 SECTION: Environmental Emergencies REVISED: 06/2015 Section 5 1. Environmental Hypothermia Protocol 5-1 2. Environmental Heat Exposure/Heat Protocol 5-2 Exhaustion Environmental Heat Stroke 3. Injury Bites
SECTION: Environmental Emergencies REVISED: 06/2015 Section 5 1. Environmental Hypothermia Protocol 5-1 2. Environmental Heat Exposure/Heat Protocol 5-2 Exhaustion Environmental Heat Stroke 3. Injury Bites
Allergic Reactions and Envenomations. Chapter 16
 Allergic Reactions and Envenomations Chapter 16 Allergic Reactions Allergic reaction Exaggerated immune response to any substance Histamines and leukotrienes Chemicals released by the immune system Anaphylaxis
Allergic Reactions and Envenomations Chapter 16 Allergic Reactions Allergic reaction Exaggerated immune response to any substance Histamines and leukotrienes Chemicals released by the immune system Anaphylaxis
5/2/2018. Notice. Putting Humpty Dumpty Back Together Again
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
ITLS Advanced Pre-Test Annotated Key 8 th Edition
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
BLS, ILS, ALS OTEP BURNS BURN INTRODUCTION TYPES OF BURNS
 BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
oriented evaluation of your patient and establishing priorities of care based on existing and
 1 Chapter 12: Patient Assessment in the Field 2 Patient assessment means conducting a - oriented evaluation of your patient and establishing priorities of care based on existing and potential threats to
1 Chapter 12: Patient Assessment in the Field 2 Patient assessment means conducting a - oriented evaluation of your patient and establishing priorities of care based on existing and potential threats to
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
OUTLINE SHEET 5.4 PRIMARY SURVEY
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
Bites and Envenomations
 Bites and Envenomations Type of bite/sting Description or bring creature with patient (preferably dead) Time, location, size of bite/sting Previous reaction to bite/sting Domestic vs. wild Tetanus and
Bites and Envenomations Type of bite/sting Description or bring creature with patient (preferably dead) Time, location, size of bite/sting Previous reaction to bite/sting Domestic vs. wild Tetanus and
ADMINISTRATIVE REQUIREMENT MANUAL EFFECTIVE DATE
 PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
Chapter 29 - Chest_and_Abdominal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
NOTE If it is necessary to perform abdominal thrusts, expose the abdominal area prior to pressing on the abdomen.
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
PROTOCOL 1 Endotracheal Intubation (Adult and Pediatric) REQUEST EMT-P RESPONSE DO NOT DELAY TRANSPORT
 PROTOCOL 1 Endotracheal Intubation (Adult and Pediatric) 1. Basic Life Support airway management procedures are initiated. 2. Endotracheal Intubation is indicated under any of the following conditions:
PROTOCOL 1 Endotracheal Intubation (Adult and Pediatric) 1. Basic Life Support airway management procedures are initiated. 2. Endotracheal Intubation is indicated under any of the following conditions:
68W COMBAT MEDIC POCKET GUIDE
 GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Stinging Insects, Spiders and Snakes
 Stinging Insects, Spiders and Snakes Stinging Insects Bites and stings happen. The stings and bites from most insects are more often a nuisance than a serious problem. A person s response to a bite or
Stinging Insects, Spiders and Snakes Stinging Insects Bites and stings happen. The stings and bites from most insects are more often a nuisance than a serious problem. A person s response to a bite or
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Providing for Players Safety 31. Emergency Plan
 Providing for Players Safety 31 Emergency Plan An emergency plan is the final step in preparing to take appropriate action for severe or serious injuries. The plan calls for three steps: 1. Survey the
Providing for Players Safety 31 Emergency Plan An emergency plan is the final step in preparing to take appropriate action for severe or serious injuries. The plan calls for three steps: 1. Survey the
EL DORADO COUNTY EMS AGENCY PREHOSPITAL PROTOCOLS
 EL DORADO COUNTY EMS AGENCY PREHOSPITAL PROTOCOLS Effective: July 1, 2017 Reviewed: November 9, 2016 Revised: November 9, 2016 EMS Agency Medical Director ALLERGIC REACTION/ANAPHYLAXIS ADULT BLS TREATMENT
EL DORADO COUNTY EMS AGENCY PREHOSPITAL PROTOCOLS Effective: July 1, 2017 Reviewed: November 9, 2016 Revised: November 9, 2016 EMS Agency Medical Director ALLERGIC REACTION/ANAPHYLAXIS ADULT BLS TREATMENT
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES. Accidental Hypothermia/Cold Exposure
 Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Chapter Goal. Learning Objectives. Chapter 17. Hemorrhage & Shock
 Chapter 17 Hemorrhage & Shock Chapter Goal Use assessment findings to formulate field impression and implement treatment plan for patient with hemorrhage or shock Learning Objectives Describe epidemiology,
Chapter 17 Hemorrhage & Shock Chapter Goal Use assessment findings to formulate field impression and implement treatment plan for patient with hemorrhage or shock Learning Objectives Describe epidemiology,
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Yaniv Berliner EMS STABILIZATION
 Yaniv Berliner EMS STABILIZATION Scene survey EMS must first evaluate the safety of the scene. Downed power lines, fire, traffic Is there a need for specialized equipment for extrication. Is there a need
Yaniv Berliner EMS STABILIZATION Scene survey EMS must first evaluate the safety of the scene. Downed power lines, fire, traffic Is there a need for specialized equipment for extrication. Is there a need
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
9/10/2012. Chapter 44. Learning Objectives. Learning Objectives (Cont d) Bleeding
 Chapter 44 Bleeding 1 Learning Objectives Describe the etiology, history, and physical findings of external bleeding Predict hemorrhage on the basis of the patient s mechanism of injury Distinguish between
Chapter 44 Bleeding 1 Learning Objectives Describe the etiology, history, and physical findings of external bleeding Predict hemorrhage on the basis of the patient s mechanism of injury Distinguish between
EMT. Chapter 10 Review
 EMT Chapter 10 Review 1. The term shock is MOST accurately defined as: A. a decreased supply of oxygen to the brain. B. cardiovascular collapse leading to inadequate perfusion. C. decreased circulation
EMT Chapter 10 Review 1. The term shock is MOST accurately defined as: A. a decreased supply of oxygen to the brain. B. cardiovascular collapse leading to inadequate perfusion. C. decreased circulation
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Northwest Community EMS System Feb 2018 CE: Multiple Patient Incidents/ChemPack Intro Credit Questions
 Northwest Community EMS System Feb 2018 CE: Multiple Patient Incidents/ChemPack Intro Credit Questions Name: EMS Agency/hospital: EMSC/Educator reviewer: Date submitted: Credit awarded (date): Returned
Northwest Community EMS System Feb 2018 CE: Multiple Patient Incidents/ChemPack Intro Credit Questions Name: EMS Agency/hospital: EMSC/Educator reviewer: Date submitted: Credit awarded (date): Returned
EMT OPTIONAL SKILL. Cell Phones and Pagers. Epinephrine Auto-injector. Course Outline 9/2017
 EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Assessment and Scoring Tools
 Assessment and Scoring Tools 2013 APGAR Scale 0 points 1 point 2 points Heart Rate Absent 100 Respiratory Rate Absent Slow, irregular Good, drying Irritability Flaccid Some flexion Active motion
Assessment and Scoring Tools 2013 APGAR Scale 0 points 1 point 2 points Heart Rate Absent 100 Respiratory Rate Absent Slow, irregular Good, drying Irritability Flaccid Some flexion Active motion
Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System
 1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
Bites, Stings and Venomous Things Amanda Wickman, MBA Southwest Center for Agricultural Health, Injury Prevention and Education
 Bites, Stings and Venomous Things Amanda Wickman, MBA Southwest Center for Agricultural Health, Injury Prevention and Education Midwest Migrant Stream Forum November 2015 Background Objectives 1. Dispel
Bites, Stings and Venomous Things Amanda Wickman, MBA Southwest Center for Agricultural Health, Injury Prevention and Education Midwest Migrant Stream Forum November 2015 Background Objectives 1. Dispel
OV United Soccer Club
 Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
Disaster Medical Operations-Part 2
 Disaster Medical Operations-Part 2 Community Emergency Response Team Disaster Medical Operations Part 1 Review The killers Airway obstruction Excessive bleeding Shock All immediate receive airway control,
Disaster Medical Operations-Part 2 Community Emergency Response Team Disaster Medical Operations Part 1 Review The killers Airway obstruction Excessive bleeding Shock All immediate receive airway control,
 TRAUMA LIFE SUPPORT PRE-HOSPITAL EXAMINATION (TLS P) 1. A high-risk bodily fluid for spreading infection is. a. sweat b. saliva c. blood d. urine 2. Items that can be used to reduce the spread of infection
TRAUMA LIFE SUPPORT PRE-HOSPITAL EXAMINATION (TLS P) 1. A high-risk bodily fluid for spreading infection is. a. sweat b. saliva c. blood d. urine 2. Items that can be used to reduce the spread of infection
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2
 CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
( PLUM BOROUGH SCHOOL DISTRICT
 No. 209.1 ( PLUM BOROUGH SCHOOL DISTRICT SECTION: PUPILS TITLE: FIRST AID STANDING ORDERS ADOPTED: March 27,1990 REVISED: February 27, 2001 209.1. FIRST AID STANDING ORDERS 1. Guidelines When a student
No. 209.1 ( PLUM BOROUGH SCHOOL DISTRICT SECTION: PUPILS TITLE: FIRST AID STANDING ORDERS ADOPTED: March 27,1990 REVISED: February 27, 2001 209.1. FIRST AID STANDING ORDERS 1. Guidelines When a student
FIRST AID TEST Practice Test
 FIRST AID TEST Practice Test www.schoolbusing.com West County Transportation Agency This test was developed to help school bus driver s study and prepare for the California Special Drivers Certificate
FIRST AID TEST Practice Test www.schoolbusing.com West County Transportation Agency This test was developed to help school bus driver s study and prepare for the California Special Drivers Certificate
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT NC ITLS Rev. 2/18 STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT What to wear ITLS is a practical course that stresses hands-on teaching. You should wear comfortable
INTERNATIONAL TRAUMA LIFE SUPPORT NC ITLS Rev. 2/18 STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT What to wear ITLS is a practical course that stresses hands-on teaching. You should wear comfortable
Review. 1. Which of the following is NOT a component of the cardiovascular system? A. Heart B. Lungs C. Venules D. Plasma
 Chapter 23 Review 1. Which of the following is NOT a component of the cardiovascular system? A. Heart B. Lungs C. Venules D. Plasma Answer: B Rationale: Components of the cardiovascular system include
Chapter 23 Review 1. Which of the following is NOT a component of the cardiovascular system? A. Heart B. Lungs C. Venules D. Plasma Answer: B Rationale: Components of the cardiovascular system include
Unit 7 INJURY MANAGEMENT Review Game
 Unit 7 INJURY MANAGEMENT Review Game Print and cut out the playing cards. Divide the class into groups of 3 or 4. Each group will need a set of playing cards. Directions for the Review game 1. Stack all
Unit 7 INJURY MANAGEMENT Review Game Print and cut out the playing cards. Divide the class into groups of 3 or 4. Each group will need a set of playing cards. Directions for the Review game 1. Stack all
