Hepatitis C, Insulin Resistance, and Steatosis
|
|
|
- Christine Cummings
- 6 years ago
- Views:
Transcription
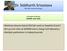
1 Hepatitis C, Insulin Resistance, and Steatosis Dawn M. Torres, MD, and Stephen A. Harrison, MD Corresponding author Stephen A. Harrison, MD Department of Gastroenterology, Brooke Army Medical Center, 3851 Roger Brooke Drive, Fort Sam Houston, TX 78234, USA. Current Hepatitis Reports 2007, 6: Current Medicine Group LLC ISSN Copyright 2007 by Current Medicine Group LLC Chronic hepatitis C (CHC) and nonalcoholic fatty liver disease (NAFLD) are two frequently identified liver diseases worldwide. NAFLD is related to obesity and insulin resistance, which may also be a preexisting condition in patients with CHC. The complex relationship among obesity, steatosis, and insulin resistance as it pertains to the pathogenesis, treatment, and outcomes in CHC is discussed in this article. Introduction The current prevalence of hepatitis C in the United States is estimated to be roughly 1.6%, with 1.3% having chronic hepatitis C (CHC) infection. This equates to 3.2 million people in the United States alone [1]. The worldwide prevalence is somewhat higher, with approximately 2% of the world s population infected with hepatitis C [2]. Recent analysis predicts that death from chronic hepatitis C virus (HCV) complications will continue to rise to about 13,000 people annually in 2030 in the United States, compared with 4200 people predicted to die as a result of HIV [3]. Even more alarming is the growing prevalence of nonalcoholic fatty liver disease (NAFLD), which is estimated to occur in approximately 30% of the US population [4]. A subset of individuals with NAFLD will have nonalcoholic steatohepatitis (NASH), the more aggressive form of NAFLD, which places them at risk for developing cirrhosis, liver failure, and hepatocellular carcinoma. The association of obesity, insulin resistance, and NAFLD is well characterized, and as obesity and diabetes become more prevalent, it is likely that NAFLD will as well. Given the commonality of both these liver diseases, overlap and coexistence of hepatitis C infection and NAFLD are to be expected. Moreover, recent investigation has shown that the hepatitis C virus can promote insulin resistance and hepatic steatosis in a manner unrelated to host metabolic dysregulation. Additionally, the natural history of hepatitis C infection and its response to antiviral therapy have been shown to be affected significantly by coexistence with NAFLD or NASH. Epidemiology The prevalence of hepatic steatosis in CHC has been well described and appears to be around 50%. This is clearly higher than the 20% to 30% seen in the general population and is independently associated with increased body mass index (BMI), insulin resistance, diabetes, older age, alcohol abuse, genotype 3 infection, hepatic inflammation, and fibrosis [5,6]. The degree of fatty infiltration is usually mild and involves less than 33% of the parenchyma. Based on the prevalence of steatosis on liver biopsy in CHC patients along with an estimated prevalence of CHC and NAFLD of 1.8% and 20%, respectively, previous investigators calculated the expected concurrence of HCV infection and steatosis to be 0.36%, or 20% of all cases of CHC [6]. This is much lower than the true 50% prevalence rate and suggests that steatosis occurs 2.5 times more often than would be expected, implying that a direct relationship between steatosis and the virus exists. The coexistence of NASH with CHC has been estimated to occur in 5% to 10% of all cases [7 9]. Pathogenesis of Steatosis in HCV Infection The mechanisms linking hepatic steatosis and hepatitis C are complex and often involve both host and viral factors (Fig. 1). Host-dependent factors include alcohol ingestion and certain medications related to hepatic steatosis, as well as metabolic factors such as obesity, insulin resistance, and diabetes mellitus. The amount of hepatic steatosis in patients with CHC correlates with BMI and insulin resistance [9,10]. The prevalence of being overweight or obese among these patients varies with ethnicity and geographic region, but studies suggest that up to 37% of US veterans are overweight or obese [11]. Hispanics with CHC appear to have even higher rates of obesity (up to 47%) [10]. Central obesity is associated with increased visceral fat, which secretes numerous cytokines involved in regulating
2 130 Hepatitis C: Complex Clinical Issues Host factors 1. Alcohol, medications 2. Metabolic factors Genotype 3 Viral factors *Non genotype 3 Obesity/genetic predisposition Hepati epatic steatosis FAS activity MTP activity (Weak) FFA flux SREBP-1 PA28 FFA oxidation Altered cytokine function TNF-, IL-6, SOCS 3 Adiponectin Insulin/?leptin resistance TNF-, SOCS 3 IRS-1, IRS-2, PI3K, Akt Mitochondrial injury p y g yp patients or genotype 1 derived constructs Figure 1. Pathogenesis of steatosis in hepatitis C virus infection. FAS fatty acid synthase; FFA free fatty acid; IL-6 interleukin-6; IRS insulin resistance substrate; MTP microsomal triglyceride transfer protein; PI3K phosphatidyl inositol 3-kinase; PPAR- peroxisomal proliferator activator receptor- ; SOCS 3 suppressor of cytokine signaling 3; SREBP-1 sterol regulatory binding protein-1; TNF- tumor necrosis factor-. glucose and lipid metabolism, including tumor necrosis factor- (TNF- and adiponectin. The proinflammatory cytokines TNF- and interleukin-6 (IL-6) are elevated in patients with CHC, which may lead to inhibition of insulin signaling in part via up-regulation of the protein SOCS 3 (suppressor of cytokine signaling 3), which is elevated in obese genotype 1 patients [12]. Alternatively, adiponectin has been shown to down-regulate TNF- and is decreased in obese patients with diabetes, CHC, and nonalcoholic steatohepatitis [13]. Data from recent studies show an independent association between low adiponectin levels and hepatic steatosis and insulin resistance [14,15]. Leptin, another protein secreted by adipocytes, may induce insulin resistance via further up-regulation of proinflammatory cytokines, is increased in patients with CHC compared with healthy controls [16], and is associated with steatosis development in genotype 1 CHC patients [17]. Insulin resistance, as a consequence of obesity, leads to enhanced lipolysis within visceral fat, resulting in increased free fatty acid (FFA) flux. This increase in FFA flux alters insulin signaling within skeletal muscle and the liver, leading to inefficient glucose metabolism, enhanced gluconeogenesis, altered FFA metabolism, and impaired triglyceride export, resulting in hepatic steatosis. The hepatitis C virus may also contribute to insulin resistance and subsequent hepatic steatosis. In a recent study by Lecube et al. [18], nondiabetic patients with CHC were found to be significantly more insulin resistant than a group of patients with chronic hepatitis equally matched for age, gender, BMI, waist-to-hip ratio, family history of diabetes, fasting blood glucose, and degree of fibrosis. Indeed, population-based studies provide support for a strong association of hepatitis C with diabetes mellitus. In a large cross-sectional survey of Americans older than 40 years, individuals with HCV were three times more likely to have type 2 diabetes mellitus [19]. Other studies have confirmed the association between type 2 diabetes and HCV, and this has led to attempts to show a cause-andeffect relationship between hepatitis C and diabetes. A prospective case-cohort study followed 1084 adults 44 to 65 years old for 5 years to see if they developed diabetes mellitus [20]. The incidence of hepatitis C in this population was 0.8%. Patients were risk stratified based on BMI and age for their risk of diabetes; high-risk patients with hepatitis C infection were 11 times more likely to develop diabetes compared with uninfected high-risk patients. Regardless of risk factors, HCV-infected patients in this study were two times more likely to develop diabetes. Experimental data support an independent role of HCV in the development of insulin resistance and hepatic steatosis via genotype-specific mechanisms. In a transgenic murine model carrying the core gene of genotype 1b HCV, insulin resistance was noted within the first month, before liver injury, and was associated with a twofold increase in TNF- [21 ]. Administration of anti TNF- antibody reversed the insulin resistance. In earlier studies by the same authors, HCV core protein producing transgenic mice were shown to develop steatosis after the age of 3 months [22], suggesting insulin resistance precedes development of steatosis in this animal model.
3 Hepatitis C, Insulin Resistance, and Steatosis Torres and Harrison 131 Both in vivo and in vitro data suggest that TNF- and SOCS 3 are increased and expression of insulin resistance substrate-1 (IRS-1) and IRS-2 is diminished in genotype 1 virus, leading to downstream inhibition of phosphatidyl inositol 3-kinase (PI3K) and Akt, and impaired insulin signaling [12,23,24]. This process may be regulated by PA28, a proteasomal activator that may also serve as a cofactor for sterol regulatory binding protein-1 (SREBP- 1) up-regulation via HCV core protein [25,26]. Support for this mechanism of impaired insulin signaling in genotype 1 virus is demonstrated by Kawaguchi et al. [23], who showed that patients achieving a sustained virologic response (SVR) had a threefold increase in IRS-1/2 expression with improved insulin signaling, adding support for a direct viral link to development of insulin resistance. It has also been proposed that the HCV core protein induces mitochondrial injury, leading to oxidative stress and eventual hepatic steatosis [27]. This is consistent with the observation that an increase in lipid peroxidation precedes steatosis in HCV core protein producing transgenic mice [28,29]. Peroxisomal proliferator activator receptor- (PPAR- ) regulates fatty acid import into mitochondria and -oxidation of FFA within mitochondria, microsomes, and peroxisomes. Recently, the expression of PPAR- was shown to be decreased in vitro among genotype 1 derived constructs and in vivo (although genotype-specific responses were not recorded), likely potentiating the development of hepatic steatosis [30,31]. Genotype 3 virus is associated with a greater prevalence and higher severity of steatosis [32] than non genotype 3 virus, and is closely related to levels of viremia. Hourioux et al. [33] compared the amount of lipid in sections of cells producing genotype 1a HCV core protein with genotype 3 specific core protein and found that cumulative lipid droplet area was significantly greater in HCV genotype 3 cells (P < 0.001). Another study comparing HCV-3a and HCV-1b core proteins found that HCV-3a core protein induced significantly higher fatty acid synthase (FAS) promoter activity, which is crucial in de novo lipid synthesis and hepatic steatosis [34]. A recent study by Mirandola et al. [35] also showed significantly reduced liver microsomal triglyceride transfer protein activity when compared with other HCV genotypes (P = 0.004). This protein is essential for hepatic lipoprotein assembly and secretion in the form of very-low-density lipoprotein. Collectively, these studies support the notion of a viral steatosis effect of genotype 3 infection that occurs independently of metabolic risk factors for steatosis, such as obesity. Steatosis and Association With Fibrosis A negative consequence of the presence of steatosis in patients with CHC appears to be fibrosis. Despite some data to suggest otherwise, the preponderance of data demonstrates an association of steatosis with fibrosis. A recent meta-analysis of more than 3000 CHC patients from 10 clinical centers around the world demonstrated that steatosis was independently associated with fibrosis regardless of genotype, although genotype 2 patients had less fibrosis [5 ]. Data from the lead-in phase of the HALT-C (Hepatitis C Antiviral Long-term Treatment Against Cirrhosis) trial showed similar findings in more than 1100 patients, with the caveat that the correlation was lost in cirrhotic or diabetic patients [36]. To further this concept, a correlation of steatosis with fibrosis progression has also been shown. Castera et al. [37] examined paired liver biopsies of untreated patients over an average 48-month period and showed that worsening of steatosis was associated with fibrosis progression (P < ), a finding others have supported. Whereas an association is evident in patients with genotypes 1 through 4, this relationship is particularly evident in genotype 3 infected patients. In the dual liver biopsy analysis by Westin et al. [38] of 98 patients followed over a mean of 5.8 years without treatment, the prevalence and grade of steatosis was strongly associated with genotype 3 infection (P = ) and steatosis was directly related to fibrosis progression, especially in genotype 3 patients. However, others have not been able to show a relationship between hepatic steatosis and fibrosis. Although study design, patient demographics, histopathologic grading criteria, and statistical analysis varied among these studies, which may explain some of the discrepancy, it is probable that the confounding variable of insulin, at least in non genotype 3 patients, may be the reason for this association. Indeed, several recent studies have confirmed an independent association of insulin resistance with hepatic fibrosis on multivariate logistic regression analysis [39 41]. The mechanisms for hepatic stellate activation and subsequent collagen matrix deposition are still under investigation but are thought to mirror those of NASH patients. This pathway may involve the aforementioned satiety hormone, leptin, which has been shown to enhance the secretion of TNF- and other proinflammatory cytokines and to up-regulate the secretion of transforming growth factor-, a cytokine involved in fibrogenesis. In a study comparing 77 patients with CHC to 22 healthy controls, leptin was associated with BMI and glycemia and was the only independent variable associated with severity of fibrosis [42]. This study also speculated that TNF- production triggered by increased leptin was an important pathway in the development of fibrosis. Effect of Steatosis and Insulin Resistance on Treatment Outcomes Several recent studies have supported the observation that patients with significant insulin resistance and steatosis at the beginning of treatment are less likely to obtain an SVR (Table 1). In a large retrospective analysis of 1428 patients, Poynard et al. [43] showed that SVR in all genotypes is
4 132 Hepatitis C: Complex Clinical Issues Table 1. Steatosis, genotype, and sustained virologic response (SVR) rate SVR, % Non genotype 3 Genotype 3 Study Country Patients, n Steatosis No steatosis Steatosis No steatosis Harrison [52] USA Poynard et al. [43] International Patton et al. [44] USA Romero-Gomez et al. [47 ] Spain * * Westin et al. [45] Europe Yaginuma et al. [69] Japan * * Tarantino et al. [70] Italy * 8 Guidi et al. [71] Italy * * *Genotype 3 specific data are not available. decreased in patients with hepatitis C and hepatic steatosis. This complex analysis compared SVR among four grades of steatosis 0%, 1% to 5%, 6% to 32%, and 33% to 100% and found that patients with even small amounts of steatosis had a significantly decreased SVR, from 66% to 52% (P < 0.001). Steatosis remained significant even after adjusting for viral load, genotype, fibrosis, and age. Another retrospective analysis of 574 HCV patients showed that those who achieved SVR had less pretreatment steatosis compared with nonresponders, 4.6% versus 10.1% (P = 0.02) [44]. Additionally, genotype 1 infected patients with an early virologic response (> 2 log reduction in HCV RNA or virus negativity at week 12) were more likely to have grade 0 steatosis compared with those without an early response, 71% versus 42% (P = 0.003). A more recent prospective study of 231 patients confirmed the negative impact of steatosis in obtaining an SVR [45]. Among non genotype 3 patients with and without steatosis, the SVR was 46% and 65%, respectively (P = 0.01). Genotype 3 patients with and without steatosis had an SVR of 88% and 100%, respectively, which was not statistically significant. One notable exception to the relationship between steatosis and decreased SVR was shown in the previously mentioned study by Lok et al. [36]. In this retrospective analysis of CHC patients undergoing retreatment with peginterferon alfa-2a and ribavirin, steatosis was associated with a decreased SVR in nondiabetic patients only. This lack of association between steatosis and decreased SVR in patients with diabetes is unique to this study, and further investigation seems warranted. The effect of significant steatosis and/or NASH on treatment outcome has also been assessed retrospectively. One study enrolling 315 patients compared HCV treatment with either interferon (IFN)/ribavirin or pegylated IFN/ribavirin between two groups: patients who had CHC and steatosis greater than 33% with or without NASH on initial biopsy and patients without NASH and with less than 33% steatosis [46]. The SVR was 28% in patients with steatosis/nash versus 44% in those without steatosis or NASH (P = 0.001). This reduction in response to therapy is even more dramatic when one looks at genotype 2 and 3 patients alone, with SVR of 42% in patients with steatosis/nash versus 78% in those without (P = 0.008). Although these studies implicated steatosis or NASH as the variable responsible for the decreased SVR, others showed that increased BMI, not steatosis, was responsible. Taken together, these studies suggest that a cofactor seen in both steatosis and increased BMI likely plays a role. Insulin resistance is common to both conditions. The results of a recent study by Romero-Gomez et al. [47 ] of 159 patients treated with peginterferon plus ribavirin suggested that insulin resistance, BMI, and fibrosis are associated with decreased SVR. This study showed a large difference between SVR based on a patient s initial degree of insulin resistance as measured by the homeostasis model of assessment insulin resistance index (HOMA-IR), which is calculated by the quotient of the fasting insulin level and fasting glucose divided by Patients with no insulin resistance had an SVR of 60% compared with an SVR of 20% for patients with a significantly altered HOMA-IR greater than 4. Among genotype 1 patients, hepatic steatosis was associated with a decreased SVR, 18.2% versus 53.7% (P = 0.001). Potential Mechanisms for a Decreased Sustained Virologic Clearance The significant negative impact of obesity, insulin resistance, and hepatic steatosis on SVR has led investigators to explore potential pathways for this occurrence (Fig. 2). Obesity seems to be the most unifying clinical variable and has been hypothesized to affect the hepatitis C response to antiviral therapy via several mechanisms. First, obesity is associated with altered cytokine function. White adipose tissue secretes numerous cytokines
5 Hepatitis C, Insulin Resistance, and Steatosis Torres and Harrison 133 Obesity Figure 2. Pathogenetic mechanisms for decreased sustained virologic response. HCV hepatitis C virus; IFN interferon Altered cytokine function* Insulin resistance* Interferon bioavailability Inflammation* Hepatic steatosis* Oxidative stress Fibrogenesis* Impaired IFN signaling pathway Viral r Biologic response to IFN Diminished HCV response to antiviral treatment *Indicates potential for coexistant viral potentiation involved in glucose and lipid metabolism as well as host immune responses. The proinflammatory cytokines leptin, TNF-, and IL-6 are up-regulated and may modulate both development of systemic inflammation and insulin resistance. Chronic systemic inflammation may lead to increased oxidative stress, and this has been shown in patients with CHC [48]. A recent study demonstrated that oxidative stress is associated with altered IFN- signaling via decreased phosphorylation of the JAK/STAT pathway [49]. Furthermore, increased TNF- mediated expression of SOCS 3 has been identified in obese, genotype 1 patients. Overexpression of SOCS 1 and SOCS 3 further inhibits IFN- induced JAK/STAT activation and subsequent transcription of IFN-stimulated genes [50]. Second, obesity-related insulin resistance may lead to development of hepatic steatosis and fibrosis, as previously mentioned [27]. The presence of steatosis impairs the early viral response to pegylated IFN-. Hepatic steatosis likely leads to fibrosis development in a manner similar to that seen in NASH patients, and increased stages of fibrosis are associated with a decreased SVR. Additionally, insulin resistance has been associated with increased viral replication in vitro [51] and in vivo [52]. The mechanisms surrounding this have yet to be well developed. Finally, obesity may result in impaired bioavailability of IFN. Pegylated IFNs are injected subcutaneously and are preferentially taken up by the lymphatic system. Patients with large amounts of subcutaneous fat may have impaired absorption of drug due to decreased lymphatic uptake of interferon [53]. Although the pegylated IFNs are dosed differently (pegylated IFN- -2b is dosed at 1.5 g/kg of body weight, and pegylated IFN- -2a is dosed at a fixed 180 g), the maximum recommended weekly subcutaneous dose is 150 g of pegylated IFN- - 2b and 180 g of pegylated IFN- -2a. Patients weighing more than 100 kg may subsequently receive a suboptimal dose of pegylated IFN- -2b if dosed according to guidelines. Recent data suggest that 180 g of pegylated IFN- -2a may also be suboptimal in heavier patients. Patients weighing more than 85 kg treated with 270 g of pegylated IFN- -2a were found to have higher serum trough concentrations of drug and a better overall SVR [54,55]. Further investigation is under way to assess the efficacy of higher fixed doses of pegylated IFN- -2a in obese patients. Unique Applications to African-American and Hispanic Populations There is emerging evidence that specific demographics are prone to more advanced liver disease, perhaps secondary to greater prevalence of metabolic disturbances. In a recent comparison of 169 Hispanics with 63 non-hispanic whites (NHWs) with hepatitis C, there were profoundly increased rates of obesity, diabetes, and hepatic steatosis among the Hispanic population [10]. These patients also had more histologically advanced disease, with 35% of Hispanics having cirrhosis on their index liver biopsy versus 22% of NHWs. This study is important because it emphasizes the link between increased insulin resistance, increased BMI, hepatic steatosis, and severity of liver disease, particularly in this at-risk population.
6 134 Hepatitis C: Complex Clinical Issues African Americans (AAs) are also of special interest given their known decreased rates of responsiveness to therapy for CHC. Some think these lowered rates are partly the result of the increased rates of genotype 1 infection in AAs, but the role of increased insulin resistance is also under investigation [56]. Conjeevaram et al. [9] looked at the differences in baseline characteristics and response to therapy of Caucasian Americans (CAs) versus AAs infected with genotype 1 virus. This study is particularly interesting because historically AAs have a lower prevalence of NAFLD despite having a higher prevalence of risk factors for fatty liver. Indeed, this was confirmed in the study, as AAs were approximately half as likely to have hepatic steatosis as were CAs when accounting for metabolic factors such as BMI and HOMA-IR. Patients with any degree of steatosis were noted to have a trend toward decreased SVR when compared with those without steatosis (37% vs 46%, P = 0.09). There was a significant stepwise decrease in SVR as the HOMA-IR increased, providing further evidence of the importance of insulin resistance in obtaining an SVR. Further studies are needed to assess why AAs overall have less steatosis than CAs despite their higher rates of obesity, diabetes, and insulin resistance. Future Therapies Improving oxidative stress The growing body of literature that correlates insulin resistance to hepatic steatosis, more severe liver disease, and decreased SVR has led to the question of whether modification of metabolic factors before, or concomitantly with, treatment for hepatitis C infection leads to improved outcomes. Several trials assessing the benefits of antioxidant therapy in addition to pegylated IFN and ribavirin have been performed. Melhem et al. [57] studied the effects of an oral antioxidant cocktail (glycyrrhizin, schisandra, silymarin, ascorbic acid, lipoic acid, l-glutathione, and -tocopherol) given daily for 20 weeks as well as an intravenous preparation of glycyrrhiza, ascorbate, l-glutathione, and B-complex given twice weekly for the first 10 weeks on liver enzymes, HCV viral load, and histopathology in 50 CHC patients (66% genotype 1) [57]. Treatment was well tolerated, and 44% of patients normalized their liver enzymes, HCV viral load decreased by at least 1 log in 25% of patients, and 36% of patients had at least a two-point reduction in their hepatic activity index. Another study using the weak antioxidant ursodeoxycholic acid (UDCA) as part of a treatment regimen for CHC with IFN- showed no difference in SVR, but the UDCA group did have lower relapse rates; however, it is unclear if this was attributable to UDCA [58]. Other studies with vitamin E, in doses ranging from 544 to 1200 IU/day, have shown down-regulation of the fibrogenesis cascade, greater reductions in viral load, and improved end-of-treatment response [59,60]. However, these studies were of limited duration and did not improve relapse rates. Overall, antioxidant therapy, although associated with biochemical and/or histopathologic improvement in small studies, has not been rigorously assessed in large prospective trials with SVR as an end point. Subsequently, its utility as adjuvant therapy is still questioned. Modulating host lipid metabolism It has been proposed that targeting host lipid metabolism may improve response rates to treatment [61]. This proposal is based on an HCV infectivity model using the low-density lipoprotein (LDL) receptor as a means of cell entry [62]. Decreasing the number of LDL receptors, via lifestyle modification or pharmacologic agents, may decrease the ability of HCV to enter hepatocytes. A recent in vitro study identified the HMG-CoA reductase inhibitor atorvastatin as a direct inhibitor of HCV replication [63]. This result was not supported by a subsequent small pilot trial of 10 patients who were given 20 mg of atorvastatin daily for 12 weeks without a statistically significant decrease in HCV RNA levels [64]. It remains to be seen whether combining a cholesterol biosynthesis inhibitor with conventional therapies for CHC, or using increased dosages of these lipid-modifying medications, will provide significant suppression of HCV replication. Weight loss The effect of weight loss on liver histology and biochemistry has also been evaluated in CHC patients. In a study of 19 patients who lost a mean of 5.9 kg, mean fasting insulin was decreased from 16 to 11 mmol/l (P < 0.002) and serum alanine aminotransferase fell progressively with weight loss [65]. Even more intriguing was the improvement in steatosis in nine of 10 patients who underwent paired liver biopsies (P < 0.005); the degree of improvement was associated with percentage of weight lost (P = 0.005). Patients with reduced steatosis also had a trend toward reduced fibrosis (five of nine patients, P = 0.04). This study was limited by its small patient population, but it supports the idea that modifying insulin resistance with weight loss before initiation of therapy for hepatitis C may improve prognosis. Insulin-sensitizing medication Pharmacologic means of reducing insulin resistance provide another intriguing area of study in an effort to improve response rates to therapy. One group of medications, the thiazolidinediones (TZDs), has been shown to improve insulin sensitivity through activation of PPAR- in adipocytes and skeletal muscle [66]. Pioglitazone, one of two currently available PPAR- ligands, decreases insulin resistance and TNF- ; increases adiponectin, thereby increasing PPAR- ligand activity; and decreases hepatic steatosis in NASH patients [67]. Further data suggest pioglitazone also decreases SOCS 3 expression [68]. Ultimately, if insulin resistance mediated increased SOCS
7 Hepatitis C, Insulin Resistance, and Steatosis Torres and Harrison expression and oxidative stress inhibit IFN- mediated JAK/STAT signaling, leading to an inadequate host immune response to virus, then treatment with the TZD class of drugs may improve response to therapy. Prospective trials are needed to assess the effect of combination therapy with a TZD plus pegylated IFN and ribavirin on innate immunity and SVR. Another medication used to reduce insulin resistance that may be of benefit is metformin, a biguanide that decreases the production of glucose in hepatocytes and increases the use of glucose within skeletal muscle. Metformin does not increase adiponectin levels, however, and its effect in NASH patients is less robust than the TZDs. Studies are under way in Europe, however, to assess the efficacy of metformin as adjunctive therapy with pegylated IFN and ribavirin in the treatment of insulin-resistant CHC patients. Conclusions In summary, adjuvant therapy aimed at improving insulin sensitivity (lifestyle modification or insulin-sensitizing medication) may hold the most promise for improving outcomes of antiviral therapy. Studies that are adequately powered and designed to assess both innate immune response and ultimately SVR are urgently needed. The nonresponder population may also benefit from this type of therapeutic approach, and future studies should include this group of patients. If the results of these studies are positive, future treatment regimens may be individually tailored according to the degree of insulin resistance as well as genotype and stage of disease. Disclaimer The opinions or assertions contained herein are the private views of the authors and are not to be construed as official or reflecting the view of the Department of the Army or the Department of Defense. References and Recommended Reading Papers of particular interest, published recently, have been highlighted as: Of importance Of major importance 1. Armstrong GL, Wasley A, Simard EP, et al.: The prevalence of hepatitis C virus infection in the United States, 1992 through Ann Intern Med 2006, 144: Bialek SR, Terrault NA: The changing epidemiology and natural history of hepatitis C virus infection. Clin Liver Dis 2006, 10: Deuffic-Burban S, Poynard T, Sulkowski MS, Wong JB: Estimating the future health burden of chronic hepatitis C and human immunodeficiency virus infections in the United States. J Viral Hepat 2007, 14: Browning JD, Szeczepaniack LS, Dobbins R, et al.: Prevalence of hepatic steatosis in an urban population in the United States: impact of ethnicity. Hepatology 2004, 40: Leandro G, Mangia A, Hui J, et al.: Relationship between steatosis, inflammation, and fibrosis in chronic hepatitis C: A meta-analysis of individual patient data. Gastroenterology 2006, 130: This large meta-analysis of 3068 patients solidifies the link between steatosis and fibrosis in chronic hepatitis C. 6. Lonardo A, Adinolfi L, Loria P, et al.: Steatosis and hepatitis C virus: mechanisms and significance for hepatic and extrahepatic disease. Gastroenterology 2004, 126: Ong JP, Younossi ZM, Speer C, et al.: Chronic hepatitis C and superimposed non-alcoholic fatty liver disease. Liver 2001, 21: Brunt EM, Ramrakhiani S, Cordes BG, et al.: Concurrence of histologic features of steatohepatitis with other forms of chronic liver disease. Mod Pathol 2003, 16: Conjeevaram HS, Kleiner DE, Everhart JE, et al.: Race, insulin resistance and hepatic steatosis in chronic hepatitis C. Hepatology 2007, 45: Verma S, Bonacini M, Govindarajan S, et al.: More advanced hepatic fibrosis in Hispanics with chronic hepatitis C infection: role of patient demographics, hepatic necroinflammation, and steatosis. Am J Gastroenterol 2006, 101: Hu KQ, Currie SL, Shen H, et al.: Clinical implications of hepatic steatosis in patients with chronic hepatitis C: a multicenter study of US veterans. Dig Dis Sci 2007, 52: Walsh MJ, Jonsson JR, Richardson MM, et al.: Nonresponse to antiviral therapy is associated with obesity and increased hepatic expression of suppressor of cytokine signaling 3 (SOCS-3) in patients with chronic hepatitis C, viral genotype 1. Gut 2006, 55: Tsochatzis E, Papatheodoridis GV, Archimandritis AJ: The evolving role of leptin and adiponectin in chronic liver diseases. Am J Gastroenterol 2006, 101: Durante-Mangoni, Zampino R, Marrone A, et al.: Hepatic steatosis and insulin resistance are associated with serum imbalance of adiponectin/tumor necrosis factor-alpha in chronic hepatitis C patients. Aliment Pharmacol Ther 2006, 24: Jonsson JR, Moschen AR, Hickman IJ, et al.: Adiponectin and its receptors in patients with chronic hepatitis C. J Hepatol 2005, 43: Widjaja A, Wedemeyer H, Tillman HL, et al.: Hepatitis C and the leptin system: bound leptin levels are elevated in patients with hepatitis C and decrease during antiviral therapy. Scand J Gastroenterol 2001, 36: Romero-Gomez M, Castellano-Megias VM, Grande L, et al.: Serum leptin levels correlate with hepatic steatosis in chronic hepatitis C. Am J Gastroenterol 2003, 98: Lecube A, Hernandez C, Genesca J, Simo R: Proinflammatory cytokines, insulin resistance, and insulin secretion in chronic hepatitis C patients. Diabetes Care 2006, 29: Metha SH, Brancati FL, Sulkowski MS, et al.: Prevalence of type 2 diabetes mellitus: what is the connection? Ann Intern Med 2000, 133: Mehta SH, Brancati FL, Strathdee SA, et al.: Hepatitis C virus infection and incident type 2 diabetes. Hepatology 2003, 38: Shintani Y, Fujie H, Miyoshi H, et al.: Hepatitis C virus infection and diabetes: direct involvement of the virus in the development of insulin resistance. Gastroenterology 2004, 126: This study clearly demonstrates virally mediated development of insulin resistance. 22. Moriya K, Yotsuyanagi H, Shintani Y, et al.: Hepatitis C virus core protein induces hepatic steatosis in transgenic mice. J Gen Virol 1997, 78:
8 136 Hepatitis C: Complex Clinical Issues 23. Kawaguchi T, Ide T, Taniguchi E, et al.: Clearance of HCV improves insulin resistance, beta-cell function, and hepatic expression of insulin receptor substrate 1 and 2. Am J Gastroenterol 2007, 102: Aytug S, Reich D, Sapiro LE, et al.: Impaired IRS-1/PI3- kinase signaling in patients with HCV: a mechanism for increased prevalence of type 2 diabetes. Hepatology 2003, 38: Miyamoto H, Moriishi K, Moriya K, et al.: Involvement of the PA28gamma-dependent pathway in insulin resistance induced by hepatitis C core protein. J Virol 2006, 81: Moriishi K, Mochizuki, Moriya K et al.: Critical role of PA28gamma in hepatitis C virus associated steatogenesis and carcinogenesis. Proc Natl Acad Sci U S A 2007, 104: Castera L, Chouteau P, Hezode C, et al.: Hepatitis C virus induced hepatocellular steatosis. Am J Gastroenterol 2005, 100: Moriya K, Nakagawa K, Santa T, et al.: Oxidative stress in the absence of inflammation in a mouse model for hepatitis C virus associated hepatocarcinogenesis. Cancer Res 2001, 61: Okuda M, Li K, Beard MR, et al.: Mitochondrial injury, oxidative stress, and antioxidant gene expression are induced by hepatitis C virus core protein. Gastroenterology 2002, 122: Cheng Y, Dharancy S, Malapel M, Desreumaux P: Hepatitis C virus infection down-regulates the expression of peroxisome proliferator-activated receptor alpha and carnitine palmitoyl acyl-coa transferase 1A. World J Gastroenterol 2005, 11: Dharancy S, Malapel M, Perletmuter G, et al.: Impaired expression of the peroxisome proliferator-activated receptor alpha during hepatitis C virus infection. Gastroenterology 2005, 128: Lonardo A, Loria P, Adinolfi LE, et al.: Hepatitis C and steatosis: a reappraisal. J Viral Hepat 2006, 13: Hourioux C, Patient R, Morin A, et al.: The genotype 3- specific hepatitis C virus core protein residue phenylalanine 164 increases steatosis in an in vitro cellular model. Gut 2007, 56(9): Jackel-Cram C, Babiuk L, Liu Q: Up-regulation of fatty acid synthase promoter by hepatitis C virus core protein: genotype-3a core has a stronger effect than genotype 1-b core. J Hepatol 2007, 46: Mirandola S, Realdon S, Iqbal J, et al.: Liver microsomal triglyceride transfer protein is involved in hepatitis C liver steatosis. Gastroenterology 2006, 130: Lok AS, Everhart JE, Chung RT, et al.: Hepatic steatosis in hepatitis C: comparison of diabetic and nondiabetic patients in the hepatitis C antiviral long-term treatment against cirrhosis trial. Clinical Gastroenterol Hepatol 2007, 5: Castera L, Hezode C, Roudot-Thoraval F, et al.: Worsening of steatosis is an independent factor of fibrosis progression in untreated patients with chronic hepatitis C and paired liver biopsies. Gut 2003, 52: Westin J, Nordlinder H, Lagging M, et al.: Steatosis accelerates fibrosis development over time in hepatitis C virus genotype 3 infected patients. J Hepatol 2002, 37: Hui JM, Sud A, Farrell GC, et al.: Insulin resistance is associated with chronic hepatitis C virus infection and fibrosis progression. Gastroenterology 2003, 125: Taura N, Ichikawa T, Hamasaki, et al.: Association between liver fibrosis and insulin sensitivity in chronic hepatitis C patients. Am J Gastroenterol 2006, 101: D Souza R, Sabin CA, Foster GR: Insulin resistance plays a significant role in liver fibrosis in chronic hepatitis C and in the response to antiviral therapy. Am J Gastroenterol 2005, 100: Piche T, Vandenbos F, Abakar-Mahamat A, et al.: The severity of liver fibrosis is associated with high leptin levels in chronic hepatitis C. J Viral Hepatol 2004, 11: Poynard T, Ratziu V, McHutchinson J, et al.: Effect of treatment with peginterferon or interferon alfa-2b and ribavirin on steatosis in patients infected with hepatitis C. Hepatology 2003, 38: Patton HM, Patel K, Behling C, et al.: The impact of steatosis on disease progression and early and sustained treatment response in chronic hepatitis C patients. J Hepatol 2004, 40: Westin J, Lagging M, Dhillon AP, et al.: Impact of hepatic steatosis on viral kinetics and treatment outcome during antiviral treatment of chronic HCV infection. J Viral Hepatol 2007, 14: Harrison SA, Brunt EM, Qazi RA, et al.: Effect of significant histologic steatosis or steatohepatitis on response to antiviral therapy in patients with chronic hepatitis C. Clin Gastroenterol Hepatol 2005, 3: Romero-Gomez M, Del Mar Viloria M, Andrade R, et al.: Insulin resistance impairs sustained response rate to peginterferon plus ribavirin in chronic hepatitis C patients. Gastroenterology 2005, 128: This prospective study showed insulin resistance, fibrosis, and genotype are independent predictors of the response to antiviral therapy in CHC patients treated with pegylated interferon and ribavirin. 48. Choi J, Ou JH: Mechanisms of liver injury. III. Oxidative stress in the pathogenesis of hepatitis C virus. Am J Physiol Gastrointest Liver Physiol 2006, 290: DiBona D, Cippitelli M, Fionda C, et al.: Oxidative stress inhibits IFN-alpha induced antiviral gene expression by blocking the JAK-STAT pathway. J Hepatol 2006, 45: Zimmerer JM, Lesinski GB, Kondadasula SV, et al.: IFNalpha-induced signal transduction, gene expression and antitumor activity. J Immunol 2007, 178: Sanyal AJ, Chand N, Comar K, Mirshahi F: Hyperinsulinemia blocks the inhibition of hepatitis C virus replication by interferon: the potential mechanism for failure of interferon therapy in subjects with HCV and nonalcoholic fatty liver disease. Hepatology 2004, 40:39A. 52. Harrison SA: Correlation between insulin resistance and hepatitis C viral load. Hepatology 2005, 42: Charlton MR, Pockros PJ, Harrison SA: Impact of obesity on treatment of chronic hepatitis C. Hepatology 2006, 43: Bressler B, Wang K, Gries JM, et al.: Pharmacokinetics and response of obese patients with chronic hepatitis C treated with different doses of PEG-IFN Alpha2A(40KD). Hepatology 2005, 42:661A. 55. Fried M, Jensen D, Rodriguez-Torres M, et al.: Improved sustained virological response (SVR) rates with higher, fixed doses of peginterferon Alfa-2A (40KD) plus ribavirin in patients with difficult to cure characteristics. Hepatology 2006, 44:314A. 56. McHutchison JG, Poynard T, Pianko S, et al.: The impact of interferon plus ribavirin on response to therapy in black patients with chronic hepatitis C. Gastroenterology 2000, 199: Melhem A, Stern M, Shibolet O, et al.: Treatment of chronic hepatitis C virus infection via antioxidants. J Clin Gastroenterol 2005, 39: Tanaka K, Kondo M, Sakaguchi T, et al.: Efficacy of ursodeoxycholic acid in combination with interferon-alpha in treating chronic hepatitis C: results of long-term follow-up trial. J Gastroenterol Hepatol 1996, 11: Houglum K, Venkataramani A, Lyche K, et al.: A pilot study of the effects of D-alpha-tocopherol on hepatic stellate cell activation in chronic hepatitis C. Gastroenterology 1997, 113: Look MP, Gerard A, Rao GS, et al.: Interferon/antioxidant combination therapy for chronic hepatitis C-a controlled pilot trial. Antiviral Res 1999, 43: Puri P, Sanyal A: Role of obesity, insulin resistance, and steatosis in hepatitis C virus infection. Clin Liver Dis 2006, 10:
9 Hepatitis C, Insulin Resistance, and Steatosis Torres and Harrison Monazahian M, Bohme I, Bonk S, et al.: Low density lipoprotein receptor as a candidate receptor for hepatitis C virus. J Med Virol 1999, 57: Kim SS, Peng LF, Lin W, et al.: A cell-based, high-throughput screen for small molecule regulators of hepatitis C virus replication. Gastroenterology 2007, 132: O Leary JG, Chan JL, McMahon CM, Chung RT: Atorvastatin does not exhibit antiviral activity against HCV at conventional doses: a pilot clinical trial. Hepatology 2007, 45: Hickman IJ, Clouston AD, Macdonald GA, et al.: Effect of weight reduction on liver histology and biochemistry in patients with chronic hepatitis C. Gut 2002, 51: Harrison SA: Liver disease in patients with diabetes mellitus. J Clin Gastroenterol 2006, 40: Belfort R, Harrison SA, Brown K, et al.: A placebo controlled trial of pioglitazone in subjects with nonalcoholic steatohepatitis. N Eng J Med 2006, 355: Kanatani Y, Usui I, Ishizuka K, et al.: Effects of pioglitazone on suppressor of cytokine signaling 3 expression: potential mechanisms for its effects on insulin sensitivity and adiponectin expression. Diabetes 2007, 56: Yaginuma R, Ikejima K, Okumura K, et al.: Hepatic steatosis is a predictor of poor response to interferon alpha- 2b and ribavirin combination therapy in Japanese patients with chronic hepatitis C. Hepatol Res 2006, 35: Tarantino G, Conca P, Sorrentino P, et al.: Metabolic factors involved in the therapeutic response of patients with hepatitis C virus-related chronic hepatitis. J Gastroenterol Hepatol 2006, 21: Guidi M, Muratori P, Granito A, et al.: Hepatic steatosis in chronic hepatitis C: impact on response to anti-viral treatment with peg-interferon and ribavirin. Aliment Pharmacol Ther 2005, 22:
Steatosi epatica ed HCV
 Steatosi epatica ed HCV Malattie delle vie biliari ed Epatologia Rho, Auditorium Padri Oblati, 11 Novembre 2006 Piero L. Almasio Università di Palermo HISTOPATHOLOGY Steatosis and accelerated fibrogenesis:
Steatosi epatica ed HCV Malattie delle vie biliari ed Epatologia Rho, Auditorium Padri Oblati, 11 Novembre 2006 Piero L. Almasio Università di Palermo HISTOPATHOLOGY Steatosis and accelerated fibrogenesis:
IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA
 UNIGASTRO Il fegato come centrale metabolica e i fattori di danno oltre ai virus epatitici IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA Dr Elisabetta Bugianesi Divisione di Gastro-Epatologia
UNIGASTRO Il fegato come centrale metabolica e i fattori di danno oltre ai virus epatitici IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA Dr Elisabetta Bugianesi Divisione di Gastro-Epatologia
Insulin resistance is extremely common; frequently is associated STATE OF THE ART
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:864 876 STATE OF THE ART Insulin Resistance Among Patients With Chronic Hepatitis C: Etiology and Impact on Treatment STEPHEN A. HARRISON Division of Gastroenterology
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:864 876 STATE OF THE ART Insulin Resistance Among Patients With Chronic Hepatitis C: Etiology and Impact on Treatment STEPHEN A. HARRISON Division of Gastroenterology
METABOLIC SYNDROME AND HCV: FROM HCV
 METABOLIC SYNDROME AND HCV: FROM THEORY TO PRACTICE HCV Steatosis Insulin resistance Arun J Sanyal M.D. Chairman, Div. of Gastroenterology, Hepatology and Nutrition Virginia Commonwealth University Richmond,
METABOLIC SYNDROME AND HCV: FROM THEORY TO PRACTICE HCV Steatosis Insulin resistance Arun J Sanyal M.D. Chairman, Div. of Gastroenterology, Hepatology and Nutrition Virginia Commonwealth University Richmond,
Journal of American Science, 2012;8(4)
 Diabetes Mellitus and peripheral Insulin Resistance in Egyptian Chronic HCV Patients Treated with Standard Antiviral Therapy Amal S. Bakir, Kadry M Elsaeed, Marcel W. Keddeas Faculty of Medicine, Ain Shams
Diabetes Mellitus and peripheral Insulin Resistance in Egyptian Chronic HCV Patients Treated with Standard Antiviral Therapy Amal S. Bakir, Kadry M Elsaeed, Marcel W. Keddeas Faculty of Medicine, Ain Shams
Treatment Options in HCV Relapsers and Nonresponders. Raymond T. Chung, M.D.
 Session IV Treatment Options in HCV Relapsers and Nonresponders Raymond T. Chung, M.D. Director of Hepatology, Massachusetts General Hospital, Associate Professor of Medicine, Harvard Medical School, Boston,
Session IV Treatment Options in HCV Relapsers and Nonresponders Raymond T. Chung, M.D. Director of Hepatology, Massachusetts General Hospital, Associate Professor of Medicine, Harvard Medical School, Boston,
Hepatitis C virus (HCV) infection is a major cause of
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:584 589 Clinical Significance of Metabolic Syndrome in the Setting of Chronic Hepatitis C Virus Infection IBRAHIM A. HANOUNEH,* ARIEL E. FELDSTEIN, ROCIO
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:584 589 Clinical Significance of Metabolic Syndrome in the Setting of Chronic Hepatitis C Virus Infection IBRAHIM A. HANOUNEH,* ARIEL E. FELDSTEIN, ROCIO
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and
 Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
The role of Hepatitis C Virus in hepatocarcinogenesis
 The role of Hepatitis C Virus in hepatocarcinogenesis Laura Beretta Fred Hutchinson Cancer Research Center l8 Incidence and mortality of the five most common cancers worldwide, 2000 Incidence Lung Breast
The role of Hepatitis C Virus in hepatocarcinogenesis Laura Beretta Fred Hutchinson Cancer Research Center l8 Incidence and mortality of the five most common cancers worldwide, 2000 Incidence Lung Breast
The Effect of Antiviral Therapy on Liver Fibrosis in CHC. Jidong Jia Beijing Friendship Hospital, Capital Medical University
 The Effect of Antiviral Therapy on Liver Fibrosis in CHC Jidong Jia Beijing Friendship Hospital, Capital Medical University 2016-5-29 1 Disclosure Consultation for Abbvie, BMS, Gilead, MSD, Novartis and
The Effect of Antiviral Therapy on Liver Fibrosis in CHC Jidong Jia Beijing Friendship Hospital, Capital Medical University 2016-5-29 1 Disclosure Consultation for Abbvie, BMS, Gilead, MSD, Novartis and
Hepatitis C wi w t i h Ju J dy y W y W a y t a t t
 Hepatitis C with Judy Wyatt Hepatitis C and the histopathologist Pre-2006 biopsy based treatment of moderate-severe chronic hepatitis Now biopsy for: Watchful waiting, to confirm mild disease? Cirrhosis
Hepatitis C with Judy Wyatt Hepatitis C and the histopathologist Pre-2006 biopsy based treatment of moderate-severe chronic hepatitis Now biopsy for: Watchful waiting, to confirm mild disease? Cirrhosis
NONALCOHOLIC FATTY LIVER DISEASE. Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD. April 13, 2012
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
L iver steatosis is a frequent histological finding in patients
 420 LIVER Effect of antiviral treatment on evolution of liver steatosis in patients with chronic hepatitis C: indirect evidence of a role of hepatitis C virus genotype 3 in steatosis L Castéra, C Hézode,
420 LIVER Effect of antiviral treatment on evolution of liver steatosis in patients with chronic hepatitis C: indirect evidence of a role of hepatitis C virus genotype 3 in steatosis L Castéra, C Hézode,
Anumber of studies have demonstrated a strong association
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:458 462 Reduction of Insulin Resistance With Effective Clearance of Hepatitis C Infection: Results From the HALT-C Trial AYMIN DELGADO BORREGO,* SERGIO H.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:458 462 Reduction of Insulin Resistance With Effective Clearance of Hepatitis C Infection: Results From the HALT-C Trial AYMIN DELGADO BORREGO,* SERGIO H.
29th Viral Hepatitis Prevention Board Meeting
 29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis C José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HEPATITIS C
29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis C José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HEPATITIS C
CHRONIC HCV TREATMENT: In Special Populations.
 CHRONIC HCV TREATMENT: In Special Populations. By Taher EL-ZANATY Prof. of Internal Medicine CAIRO UNIVERSITY Introduction: HCV is the major cause of chronic hepatitis in Egypt. Its end stage is liver
CHRONIC HCV TREATMENT: In Special Populations. By Taher EL-ZANATY Prof. of Internal Medicine CAIRO UNIVERSITY Introduction: HCV is the major cause of chronic hepatitis in Egypt. Its end stage is liver
NASH Bench to Bedside
 NASH Bench to Bedside October 2006 Anna Mae Diehl, M.D. Gastroenterology Division Duke University NonAlcoholic Fatty Liver Disease Common ~1/4-1/3 1/3 US adults Outcome highly variable Course indolent
NASH Bench to Bedside October 2006 Anna Mae Diehl, M.D. Gastroenterology Division Duke University NonAlcoholic Fatty Liver Disease Common ~1/4-1/3 1/3 US adults Outcome highly variable Course indolent
Improving Access to Quality Medical Care Webinar Series
 Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Clearance of HCV by Combination Therapy of Pegylated Interferon α-2a and Ribavirin Improves Insulin Resistance
 Gut and Liver, Vol. 3, No. 2, June 2009, pp. 108-115 original article Clearance of HCV by Combination Therapy of Pegylated Interferon α-2a and Ribavirin Improves Insulin Resistance Hong Joo Kim, Jung Ho
Gut and Liver, Vol. 3, No. 2, June 2009, pp. 108-115 original article Clearance of HCV by Combination Therapy of Pegylated Interferon α-2a and Ribavirin Improves Insulin Resistance Hong Joo Kim, Jung Ho
NONALCOHOLIC FATTY LIVER DISEASE
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
Insulin Resistance in Patients with Chronic Hepatitis C Infection
 Australian Journal of Basic and Applied Sciences, 4(10): 4554-4558, 2010 ISSN 1991-8178 Insulin Resistance in Patients with Chronic Hepatitis C Infection 1 Hoda Abd El-Satar MD. 1 Mahmoud Mahfouz MD. 2
Australian Journal of Basic and Applied Sciences, 4(10): 4554-4558, 2010 ISSN 1991-8178 Insulin Resistance in Patients with Chronic Hepatitis C Infection 1 Hoda Abd El-Satar MD. 1 Mahmoud Mahfouz MD. 2
Hepatitis C Management and Treatment
 Hepatitis C Management and Treatment Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology 1 Discovery of Hepatitis C Key facts Hepatitis C: the virus can cause
Hepatitis C Management and Treatment Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology 1 Discovery of Hepatitis C Key facts Hepatitis C: the virus can cause
NAFLD/NASH. Definitions. Pathology NASH. Vicki Shah PA-C, MMS Rush University Hepatology
 NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
La sindrome metabolica e il suo impatto dopo la guarigione nel paziente HIV/HCV
 WORKSHOP HCV: la guarigione e il parallelismo tra risposta virologica sostenuta e outcome clinico Milano, 25 Ottobre 2018 Ospedale San Raffaele IRCCS - Sede Turro La sindrome metabolica e il suo impatto
WORKSHOP HCV: la guarigione e il parallelismo tra risposta virologica sostenuta e outcome clinico Milano, 25 Ottobre 2018 Ospedale San Raffaele IRCCS - Sede Turro La sindrome metabolica e il suo impatto
Viral Hepatitis The Preventive Potential of Antiviral Therapy. Thomas Berg
 Viral Hepatitis The Preventive Potential of Antiviral Therapy Thomas Berg Therapeutic and preventive strategies in patients with hepatitis virus infection Treatment of acute infection Treatment of chronic
Viral Hepatitis The Preventive Potential of Antiviral Therapy Thomas Berg Therapeutic and preventive strategies in patients with hepatitis virus infection Treatment of acute infection Treatment of chronic
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016.
 Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
Successful Hepatitis C Antiviral Therapy Induces Remission of Type 2 Diabetes: A Case Report
 ISSN 1941-5923 DOI: 10.12659/AJCR.895064 Received: 2015.06.18 Accepted: 2015.06.26 Published: 2015.10.20 Successful Hepatitis C Antiviral Therapy Induces Remission of Type 2 Diabetes: A Case Report Authors
ISSN 1941-5923 DOI: 10.12659/AJCR.895064 Received: 2015.06.18 Accepted: 2015.06.26 Published: 2015.10.20 Successful Hepatitis C Antiviral Therapy Induces Remission of Type 2 Diabetes: A Case Report Authors
Should Elderly CHC Patients (>70 years old) be Treated?
 Should Elderly CHC Patients (>70 years old) be Treated? Deepak Amarapurkar Consultant Gastroenterologist & Hepatologist Bombay Hospital & Medical Research Center, Mumbai & Jagjivanram Western Railway Hospital,
Should Elderly CHC Patients (>70 years old) be Treated? Deepak Amarapurkar Consultant Gastroenterologist & Hepatologist Bombay Hospital & Medical Research Center, Mumbai & Jagjivanram Western Railway Hospital,
T he hepatitis C virus (HCV) is a major cause of chronic
 1638 VIRAL HEPATITIS Liver fibrosis is not associated with steatosis but with necroinflammation in French patients with chronic hepatitis C T Asselah, N Boyer, M-C Guimont, D Cazals-Hatem, F Tubach, K
1638 VIRAL HEPATITIS Liver fibrosis is not associated with steatosis but with necroinflammation in French patients with chronic hepatitis C T Asselah, N Boyer, M-C Guimont, D Cazals-Hatem, F Tubach, K
Non alcoholic fatty liver and Non alcoholic Steatohepatitis. By Dr. Seham Seif
 Non alcoholic fatty liver and Non alcoholic Steatohepatitis By Dr. Seham Seif Definition NAFL describe a common clinicopathological conditions characterized by significant lipid deposition in the hepatocytes
Non alcoholic fatty liver and Non alcoholic Steatohepatitis By Dr. Seham Seif Definition NAFL describe a common clinicopathological conditions characterized by significant lipid deposition in the hepatocytes
Pegylated Interferon Alfa-2b (Peg-Intron) Plus Ribavirin (Rebetol)in the Treatment of Chronic Hepatitis C: A Local Experience
 Pegylated Interferon Alfa-2b (Peg-Intron) Plus Ribavirin (Rebetol)in the Treatment of Chronic Hepatitis C: A Local Experience E L Seow, PH Robert Ding Island Hospital, Penang, Malaysia. Introduction Hepatitis
Pegylated Interferon Alfa-2b (Peg-Intron) Plus Ribavirin (Rebetol)in the Treatment of Chronic Hepatitis C: A Local Experience E L Seow, PH Robert Ding Island Hospital, Penang, Malaysia. Introduction Hepatitis
[Sem Liver Disease 21(1):81-88, Thieme Medical Publishers, Inc.]
![[Sem Liver Disease 21(1):81-88, Thieme Medical Publishers, Inc.] [Sem Liver Disease 21(1):81-88, Thieme Medical Publishers, Inc.]](/thumbs/72/66425194.jpg) Treatment of Nonalcoholic Fatty Liver: Present and Emerging Therapies [Sem Liver Disease 21(1):81-88, 2001. 2001 Thieme Medical Publishers, Inc.] Paul Angulo, M.D., and Keith D. Lindor, M.D., Division
Treatment of Nonalcoholic Fatty Liver: Present and Emerging Therapies [Sem Liver Disease 21(1):81-88, 2001. 2001 Thieme Medical Publishers, Inc.] Paul Angulo, M.D., and Keith D. Lindor, M.D., Division
Original article J Bas Res Med Sci 2014; 1(1):50-55.
 The effect of pioglitazone and metformin on non-alcoholic fatty liver: A double blind clinical trial study Kourosh Sayehmiri 1, 2, Khairollah Asadollahi 1, 2*, Mariam Yaghubi 1, Ghobad Abangah 3, Hassan
The effect of pioglitazone and metformin on non-alcoholic fatty liver: A double blind clinical trial study Kourosh Sayehmiri 1, 2, Khairollah Asadollahi 1, 2*, Mariam Yaghubi 1, Ghobad Abangah 3, Hassan
Current therapy for hepatitis C: pegylated interferon and ribavirin
 Clin Liver Dis 7 (2003) 149 161 Current therapy for hepatitis C: pegylated interferon and ribavirin John G. McHutchison, MD a, Michael W. Fried, MD b, * a Duke Clinical Research Institute, Duke University
Clin Liver Dis 7 (2003) 149 161 Current therapy for hepatitis C: pegylated interferon and ribavirin John G. McHutchison, MD a, Michael W. Fried, MD b, * a Duke Clinical Research Institute, Duke University
ANTIVIRAL THERAPY FOR HCV. Alfredo Alberti
 CLINICAL IMPACT OF SVR AFTER ANTIVIRAL THERAPY FOR HCV Alfredo Alberti Department of Histology,Microbiology and Medical Biotechnologies Molecular Hepatology Unit Venetian Institute of Molecular Medicine
CLINICAL IMPACT OF SVR AFTER ANTIVIRAL THERAPY FOR HCV Alfredo Alberti Department of Histology,Microbiology and Medical Biotechnologies Molecular Hepatology Unit Venetian Institute of Molecular Medicine
Pharmacological management of viruses in obese patients
 Cubist Pharmaceuticals The Shape of Cures to Come Pharmacological management of viruses in obese patients Dr. Dimitar Tonev, Medical Director UKINORD 1 Disclosures } The author is a pharmaceutical physician
Cubist Pharmaceuticals The Shape of Cures to Come Pharmacological management of viruses in obese patients Dr. Dimitar Tonev, Medical Director UKINORD 1 Disclosures } The author is a pharmaceutical physician
Metabolic Syndrome. DOPE amines COGS 163
 Metabolic Syndrome DOPE amines COGS 163 Overview - M etabolic Syndrome - General definition and criteria - Importance of diagnosis - Glucose Homeostasis - Type 2 Diabetes Mellitus - Insulin Resistance
Metabolic Syndrome DOPE amines COGS 163 Overview - M etabolic Syndrome - General definition and criteria - Importance of diagnosis - Glucose Homeostasis - Type 2 Diabetes Mellitus - Insulin Resistance
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES
 NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
Significance of Hepatic Insulin Clearance in Patients with Chronic Hepatitis C and Non-alcoholic Fatty Liver Disease
 ORIGINAL ARTICLE Significance of Hepatic Insulin Clearance in Patients with Chronic Hepatitis C and Non-alcoholic Fatty Liver Disease Hisamitsu Miyaaki 1, Tatsuki Ichikawa 1,NaotaTaura 1, Satoshi Miuma
ORIGINAL ARTICLE Significance of Hepatic Insulin Clearance in Patients with Chronic Hepatitis C and Non-alcoholic Fatty Liver Disease Hisamitsu Miyaaki 1, Tatsuki Ichikawa 1,NaotaTaura 1, Satoshi Miuma
Worldwide Causes of HCC
 Approach to HCV Treatment in Patients with HCC JORGE L. HERRERA, MD, MACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE Worldwide Causes of HCC 60% 50% 40% 54% 30% 20% 10% 31% 15% 0% Hepatitis B Hepatitis
Approach to HCV Treatment in Patients with HCC JORGE L. HERRERA, MD, MACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE Worldwide Causes of HCC 60% 50% 40% 54% 30% 20% 10% 31% 15% 0% Hepatitis B Hepatitis
Non-Alcoholic Fatty Liver Disease
 Non-Alcoholic Fatty Liver Disease None Disclosures Arslan Kahloon M.D Chief, Division of Gastroenterology and Hepatology University of Tennessee College of Medicine Chattanooga Objectives Understand the
Non-Alcoholic Fatty Liver Disease None Disclosures Arslan Kahloon M.D Chief, Division of Gastroenterology and Hepatology University of Tennessee College of Medicine Chattanooga Objectives Understand the
Normal ALT for men 30 IU/L 36% US males abnormal. Abnl ALT. Assess alcohol use/meds. Recheck in 6-8 weeks. still pos
 Fatty liver disease Its not just for big boys anymore Ken Flora, MD, FAASLD, FACG, AGAF No disclosures Common situation Normal ALT for men 30 IU/L 36% US males abnormal Normal ALT for women 20 IU/L 28%
Fatty liver disease Its not just for big boys anymore Ken Flora, MD, FAASLD, FACG, AGAF No disclosures Common situation Normal ALT for men 30 IU/L 36% US males abnormal Normal ALT for women 20 IU/L 28%
Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical
 Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical Disclosure Naim Alkhouri, MD discloses the following relationships with commercial companies: Membership in the Speakers Bureau for Alexion
Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical Disclosure Naim Alkhouri, MD discloses the following relationships with commercial companies: Membership in the Speakers Bureau for Alexion
Fatty liver disease: What do we know?
 Fatty liver disease: What do we know? Prof. Dr. Claus Niederau Katholische Kliniken Oberhausen ggmbh St. Josef-Hospital Academic Teaching Hospital University of Duisburg-Essen NAFLD Non-Alcoholic Fatty
Fatty liver disease: What do we know? Prof. Dr. Claus Niederau Katholische Kliniken Oberhausen ggmbh St. Josef-Hospital Academic Teaching Hospital University of Duisburg-Essen NAFLD Non-Alcoholic Fatty
Worldwide Causes of HCC
 Approach to HCV Treatment in Patients with HCC Mark W. Russo, MD, MPH, FACG Carolinas HealthCare System Charlotte Worldwide Causes of HCC 60% 50% 40% 30% 20% 10% 0% 54% 31% 15% Hepatitis B Hepatitis C
Approach to HCV Treatment in Patients with HCC Mark W. Russo, MD, MPH, FACG Carolinas HealthCare System Charlotte Worldwide Causes of HCC 60% 50% 40% 30% 20% 10% 0% 54% 31% 15% Hepatitis B Hepatitis C
Original Article. Significance of Hepatic Steatosis in Chronic Hepatitis B Infection INTRODUCTION
 Original Article Bhanthumkomol P, et al. THAI J GASTROENTEROL 2013 Vol. 14 No. 1 Jan. - Apr. 2013 29 Bhanthumkomol P 1 Charatcharoenwitthaya P 1 Pongpaiboon A 2 ABSTRACT Background: Significance of liver
Original Article Bhanthumkomol P, et al. THAI J GASTROENTEROL 2013 Vol. 14 No. 1 Jan. - Apr. 2013 29 Bhanthumkomol P 1 Charatcharoenwitthaya P 1 Pongpaiboon A 2 ABSTRACT Background: Significance of liver
Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus
 Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
NIH Public Access Author Manuscript Am J Med Sci. Author manuscript; available in PMC 2015 January 01.
 NIH Public Access Author Manuscript Published in final edited form as: Am J Med Sci. 2014 January ; 347(1):. doi:10.1097/maj.0b013e31828b25a5. Association Between Metabolic Syndrome and Its Individual
NIH Public Access Author Manuscript Published in final edited form as: Am J Med Sci. 2014 January ; 347(1):. doi:10.1097/maj.0b013e31828b25a5. Association Between Metabolic Syndrome and Its Individual
Fatty Liver- how important is it? Jeremy F.L. Cobbold MA PhD MRCP Clinical Lecturer in Hepatology Imperial College London
 Fatty Liver- how important is it? Jeremy F.L. Cobbold MA PhD MRCP Clinical Lecturer in Hepatology Imperial College London Fatty liver- how important is it? Importance in terms of: Prevalence Pathogenesis
Fatty Liver- how important is it? Jeremy F.L. Cobbold MA PhD MRCP Clinical Lecturer in Hepatology Imperial College London Fatty liver- how important is it? Importance in terms of: Prevalence Pathogenesis
C hronic infection with the hepatitis C virus (HCV) is a
 406 LIVER Steatosis affects chronic hepatitis C progression in a genotype specific way L Rubbia-Brandt, P Fabris, S Paganin, G Leandro, P-J Male, E Giostra, A Carlotto, L Bozzola, A Smedile, F Negro...
406 LIVER Steatosis affects chronic hepatitis C progression in a genotype specific way L Rubbia-Brandt, P Fabris, S Paganin, G Leandro, P-J Male, E Giostra, A Carlotto, L Bozzola, A Smedile, F Negro...
Over the past decade, the introduction of
 MANAGEMENT OF CHRONIC HEPATITIS C IN HIV-INFECTED PATIENTS: CLINICAL EXPERIENCE WITH PEGYLATED INTERFERON α PLUS RIBAVIRIN Raymond T. Chung, MD* ABSTRACT Coinfection with hepatitis C virus (HCV) is common
MANAGEMENT OF CHRONIC HEPATITIS C IN HIV-INFECTED PATIENTS: CLINICAL EXPERIENCE WITH PEGYLATED INTERFERON α PLUS RIBAVIRIN Raymond T. Chung, MD* ABSTRACT Coinfection with hepatitis C virus (HCV) is common
Update on Non-Alcoholic Fatty Liver Disease. Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI
 Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Antiviral therapy guidelines for the general population
 Discussion 10 Chapter 10 Hepatitis C a worldwide problem More than 170 million people worldwide suffer from chronic hepatitis C. Its prevalence is 2% in industrialized countries. 1 Approximately 20% of
Discussion 10 Chapter 10 Hepatitis C a worldwide problem More than 170 million people worldwide suffer from chronic hepatitis C. Its prevalence is 2% in industrialized countries. 1 Approximately 20% of
Abstract and Introduction. Patients and Methods. M. Hedenstierna; A. Nangarhari; A. El-Sabini; O. Weiland; S.
 www.medscape.com Cirrhosis, High Age and High Body Mass Index Are Risk Factors for Persisting Advanced Fibrosis After Sustained Virological Response in Chronic Hepatitis C M. Hedenstierna; A. Nangarhari;
www.medscape.com Cirrhosis, High Age and High Body Mass Index Are Risk Factors for Persisting Advanced Fibrosis After Sustained Virological Response in Chronic Hepatitis C M. Hedenstierna; A. Nangarhari;
Hepatitis C: Management of Previous Non-responders with First Line Protease Inhibitors
 Hepatitis C: Management of Previous Non-responders with First Line Protease Inhibitors Fred Poordad, MD The Texas Liver Institute Clinical Professor of Medicine University of Texas Health Science Center
Hepatitis C: Management of Previous Non-responders with First Line Protease Inhibitors Fred Poordad, MD The Texas Liver Institute Clinical Professor of Medicine University of Texas Health Science Center
Management of CHC G1 patients who are relapsers or non-responders to Peg IFN and RBV therapy: Wait or Triple Therapy?
 Management of CHC G1 patients who are relapsers or non-responders to Peg IFN and RBV therapy: Wait or Triple Therapy? Prof. Teerha Piratvisuth NKC Institute of Gastroenterology and Hepatology Prince of
Management of CHC G1 patients who are relapsers or non-responders to Peg IFN and RBV therapy: Wait or Triple Therapy? Prof. Teerha Piratvisuth NKC Institute of Gastroenterology and Hepatology Prince of
Steatosis and hepatitis C
 Gastroenterology Report Advance Access published August 13, 2015 Gastroenterology Report, 2015, 1 6 doi: 10.1093/gastro/gov040 Review Article REVIEW ARTICLE Steatosis and hepatitis C Jamak Modaresi Esfeh
Gastroenterology Report Advance Access published August 13, 2015 Gastroenterology Report, 2015, 1 6 doi: 10.1093/gastro/gov040 Review Article REVIEW ARTICLE Steatosis and hepatitis C Jamak Modaresi Esfeh
Intron A Hepatitis B. Intron A (interferon alfa-2b) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.01 Subject: Intron A Hepatitis B Page: 1 of 7 Last Review Date: November 30, 2018 Intron A Hepatitis
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.01 Subject: Intron A Hepatitis B Page: 1 of 7 Last Review Date: November 30, 2018 Intron A Hepatitis
Dr. Siddharth Srivastava
 Dr. Siddharth Srivastava MD, DM (Gastroenterology) Associate Professor GIPMER, New Delhi Rashtriya Gaurav Award 2013 for work on hepatitis B and C Set up Liver clinic at GIPMER and in charge EUS laboratory.
Dr. Siddharth Srivastava MD, DM (Gastroenterology) Associate Professor GIPMER, New Delhi Rashtriya Gaurav Award 2013 for work on hepatitis B and C Set up Liver clinic at GIPMER and in charge EUS laboratory.
TRANSPARENCY COMMITTEE
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 10 December 2008 REBETOL 200 mg capsules Pack of 84 (CIP code: 351 971.9) Pack of 112 (CIP code: 373 277.8) Pack of
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 10 December 2008 REBETOL 200 mg capsules Pack of 84 (CIP code: 351 971.9) Pack of 112 (CIP code: 373 277.8) Pack of
H epatitis C virus (HCV) is a major cause of chronic liver
 89 LIVER AND BILIARY DISEASE Effect of weight reduction on liver histology and biochemistry in patients with chronic hepatitis C I J Hickman, A D Clouston, G A Macdonald, D M Purdie, J B Prins, S Ash,
89 LIVER AND BILIARY DISEASE Effect of weight reduction on liver histology and biochemistry in patients with chronic hepatitis C I J Hickman, A D Clouston, G A Macdonald, D M Purdie, J B Prins, S Ash,
Liver Pathology in the 0bese
 Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE Impact of ody Weight Reduction via Diet and Exercise on the Anti-Viral Effects of Pegylated Interferon Plus Ribavirin in Chronic Hepatitis C Patients with Insulin Resistance: A Randomized
ORIGINAL ARTICLE Impact of ody Weight Reduction via Diet and Exercise on the Anti-Viral Effects of Pegylated Interferon Plus Ribavirin in Chronic Hepatitis C Patients with Insulin Resistance: A Randomized
HCC Prevention. Jee-Fu Huang. Kaohsiung Municipal Hsiao-Kang Hospital, KMUH Kaohsiung (Takao), Taiwan. TCC, HCC Prevention, 26 Nov, 2011
 HCC Prevention Jee-Fu Huang Kaohsiung Municipal Hsiao-Kang Hospital, KMUH Kaohsiung (Takao), Taiwan TCC, HCC Prevention, 26 Nov, 2011 1 Outline Pathogenic and Risk Factors HBV HCV Primary Secondary Primary
HCC Prevention Jee-Fu Huang Kaohsiung Municipal Hsiao-Kang Hospital, KMUH Kaohsiung (Takao), Taiwan TCC, HCC Prevention, 26 Nov, 2011 1 Outline Pathogenic and Risk Factors HBV HCV Primary Secondary Primary
Waseem Hamoudi MD*, Sami Al-Smadi MD*, Karim Lutfi MD*, Moath Azizi MD*, Yousef Niomat MD* ABSTRACT
 Durability of Sustained Virological Response and Long Term Follow Up To Pegylated Interferon and Ribavirin in Treated Patients with Chronic Hepatitis C Waseem Hamoudi MD*, Sami Al-Smadi MD*, Karim Lutfi
Durability of Sustained Virological Response and Long Term Follow Up To Pegylated Interferon and Ribavirin in Treated Patients with Chronic Hepatitis C Waseem Hamoudi MD*, Sami Al-Smadi MD*, Karim Lutfi
FREQUENCY OF STEATOSIS AND ITS RELATION WITH THE GRADE OF FIBROSIS IN PATIENTS WITH HEPATITIS C
 Original Article FREQUENCY OF STEATOSIS AND ITS RELATION WITH THE GRADE OF FIBROSIS IN PATIENTS WITH HEPATITIS C Samiullah Shaikh 1, Memon Sadik 2, Baloch Ghulam Hussain 3 ABSTRACT Objective: To study
Original Article FREQUENCY OF STEATOSIS AND ITS RELATION WITH THE GRADE OF FIBROSIS IN PATIENTS WITH HEPATITIS C Samiullah Shaikh 1, Memon Sadik 2, Baloch Ghulam Hussain 3 ABSTRACT Objective: To study
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health
 CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
Chronic hepatitis C virus (HCV) infection is a leading
 Metabolic Manifestations and Complications Associated With Chronic Hepatitis C Virus Infection Robert J. Wong, MD, MS, and Robert G. Gish, MD Dr Wong is an assistant clinical professor of medicine at the
Metabolic Manifestations and Complications Associated With Chronic Hepatitis C Virus Infection Robert J. Wong, MD, MS, and Robert G. Gish, MD Dr Wong is an assistant clinical professor of medicine at the
Challenges in the Diagnosis of Steatohepatitis
 The Bugaboos of Fatty Liver Disease: Ballooning and Fibrosis Hans Popper Hepatopathology Society Companion Meeting San Antonio, Tx March, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Challenges
The Bugaboos of Fatty Liver Disease: Ballooning and Fibrosis Hans Popper Hepatopathology Society Companion Meeting San Antonio, Tx March, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Challenges
ةي : لآا ةرقبلا ةروس
 سورة البقرة: اآلية HCV RELAPSERS AND NONRESPONDERS: How to deal with them? BY Prof. Mohamed Sharaf-Eldin Prof. of Hepatology and Gastroenterology Tanta University Achieving SVR The ability to achieve a
سورة البقرة: اآلية HCV RELAPSERS AND NONRESPONDERS: How to deal with them? BY Prof. Mohamed Sharaf-Eldin Prof. of Hepatology and Gastroenterology Tanta University Achieving SVR The ability to achieve a
Safety of Treatment in Cirrhotics in the Era of New Antiviral Therapies for Hepatitis C Virus
 Safety of Treatment in Cirrhotics in the Era of New Antiviral Therapies for Hepatitis C Virus JEFFREY NADELSON MD, ALAN EPSTEIN MD, THOMAS SEPE MD BOSTON UNIVERSITY SCHOOL OF MEDICINE ROGER WILLIAMS MEDICAL
Safety of Treatment in Cirrhotics in the Era of New Antiviral Therapies for Hepatitis C Virus JEFFREY NADELSON MD, ALAN EPSTEIN MD, THOMAS SEPE MD BOSTON UNIVERSITY SCHOOL OF MEDICINE ROGER WILLIAMS MEDICAL
WHAT THE EXPERIMENTAL MODELS CAN TEACH US IN NAFLD/NASH? Claudio Tiribelli, MD PhD Scientific Director FIF
 WHAT THE EXPERIMENTAL MODELS CAN TEACH US IN NAFLD/NASH? Claudio Tiribelli, MD PhD Scientific Director FIF ctliver@fegato.it Worldwide estimated prevalence of NAFLD distribution of PNPLA3 genotypes 2017-Younussi
WHAT THE EXPERIMENTAL MODELS CAN TEACH US IN NAFLD/NASH? Claudio Tiribelli, MD PhD Scientific Director FIF ctliver@fegato.it Worldwide estimated prevalence of NAFLD distribution of PNPLA3 genotypes 2017-Younussi
A COMPARATIVE ANALYSIS OF SERUM LIPIDS IN PATIENTS WITH CHRONIC HEPATITIS C, NONALCOHOLIC FATTY LIVER DISEASE AND HEALTHY CONTROLS
 10.1515/AMB-2017-0001 ORIGINAL ARTICLES A COMPARATIVE ANALYSIS OF SERUM LIPIDS IN PATIENTS WITH CHRONIC HEPATITIS C, NONALCOHOLIC FATTY LIVER DISEASE AND HEALTHY CONTROLS I. Valkov 1,4, R. Ivanova 2,4,
10.1515/AMB-2017-0001 ORIGINAL ARTICLES A COMPARATIVE ANALYSIS OF SERUM LIPIDS IN PATIENTS WITH CHRONIC HEPATITIS C, NONALCOHOLIC FATTY LIVER DISEASE AND HEALTHY CONTROLS I. Valkov 1,4, R. Ivanova 2,4,
How to optimize treatment for HCV Genotype 4
 How to optimize treatment for HCV Genotype 4 Paris Hepatitis Conference Pr Tarik Asselah 14 janvier 2014 MD, PhD Service d Hépatologie & INSERM U773 University Paris Diderot Hôpital Beaujon, Clichy tarik.asselah@bjn.aphp.fr
How to optimize treatment for HCV Genotype 4 Paris Hepatitis Conference Pr Tarik Asselah 14 janvier 2014 MD, PhD Service d Hépatologie & INSERM U773 University Paris Diderot Hôpital Beaujon, Clichy tarik.asselah@bjn.aphp.fr
Targeting Glucose Metabolism to Stop Strokes IRIS: Insulin Resistance In Stroke study
 Targeting Glucose Metabolism to Stop Strokes IRIS: Insulin Resistance In Stroke study Professor Gary Ford Chief Executive Officer, Oxford Academic Health Science Network Consultant Stroke Physician, Oxford
Targeting Glucose Metabolism to Stop Strokes IRIS: Insulin Resistance In Stroke study Professor Gary Ford Chief Executive Officer, Oxford Academic Health Science Network Consultant Stroke Physician, Oxford
Oral combination therapy: future hepatitis C virus treatment? "Lancet Oct 30;376(9751): Oral combination therapy with a nucleoside
 Author manuscript, published in "Journal of Hepatology 2011;55(4):933-5" DOI : 10.1016/j.jhep.2011.04.018 Oral combination therapy: future hepatitis C virus treatment? Commentary article on the following
Author manuscript, published in "Journal of Hepatology 2011;55(4):933-5" DOI : 10.1016/j.jhep.2011.04.018 Oral combination therapy: future hepatitis C virus treatment? Commentary article on the following
Advances in Hepatitis C Virus Therapeutics HBV HIV HCV. Advances in HCV Therapeutics. Greg Dore. Viral Hepatitis Clinical Research Program
 Advances in Hepatitis C Virus Therapeutics Greg Dore Viral Hepatitis Clinical Research Program National Centre in HIV Epidemiology and Clinical Research Hepatitis C notifications: 199-23 Estimates of BBV
Advances in Hepatitis C Virus Therapeutics Greg Dore Viral Hepatitis Clinical Research Program National Centre in HIV Epidemiology and Clinical Research Hepatitis C notifications: 199-23 Estimates of BBV
The impact of the treatment of HCV in developing Hepatocellular Carcinoma
 The impact of the treatment of HCV in developing Hepatocellular Carcinoma Paul Y Kwo, MD Professor of Medicine Medical Director, Liver Transplantation Gastroenterology/Hepatology Division Indiana University
The impact of the treatment of HCV in developing Hepatocellular Carcinoma Paul Y Kwo, MD Professor of Medicine Medical Director, Liver Transplantation Gastroenterology/Hepatology Division Indiana University
The medical management of hepatitis C
 CLINICAL EXPERIENCE WITH PEGYLATED INTERFERON α-2a PLUS RIBAVIRIN FOR CHRONIC HEPATITIS C VIRUS INFECTION IN PATIENTS INFECTED WITH HIV: THE APRICOT STUDY Douglas T. Dieterich, MD* ABSTRACT Currently,
CLINICAL EXPERIENCE WITH PEGYLATED INTERFERON α-2a PLUS RIBAVIRIN FOR CHRONIC HEPATITIS C VIRUS INFECTION IN PATIENTS INFECTED WITH HIV: THE APRICOT STUDY Douglas T. Dieterich, MD* ABSTRACT Currently,
Yun Jung Kim, Byoung Kuk Jang, Eun Soo Kim, Kyung Sik Park, Kwang Bum Cho, Woo Jin Chung, and Jae Seok Hwang
 The Korean Journal of Hepatology 2012;18:41-47 http://dx.doi.org/10.3350/kjhep.2012.18.1.41 pissn: 1738-222X eissn: 2093-8047 Original Article Rapid normalization of alanine aminotransferase predicts viral
The Korean Journal of Hepatology 2012;18:41-47 http://dx.doi.org/10.3350/kjhep.2012.18.1.41 pissn: 1738-222X eissn: 2093-8047 Original Article Rapid normalization of alanine aminotransferase predicts viral
UMHS-PUHSC JOINT INSTITUTE
 Role of Visceral Adiposity in the Pathogenesis of Non-Alcoholic Fatty Liver Disease in Lean versus Obese Patients: A Comparative Study between Patients at UMHS versus PUHSC Lai WEI and Anna LOK W Zhang,
Role of Visceral Adiposity in the Pathogenesis of Non-Alcoholic Fatty Liver Disease in Lean versus Obese Patients: A Comparative Study between Patients at UMHS versus PUHSC Lai WEI and Anna LOK W Zhang,
Viral hepatitis and Hepatocellular Carcinoma
 Viral hepatitis and Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
Viral hepatitis and Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
3/20/2011. Body Mass Index (kg/[m 2 ]) Age at Issue (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Mokdad A.H.
![3/20/2011. Body Mass Index (kg/[m 2 ]) Age at Issue (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Mokdad A.H. 3/20/2011. Body Mass Index (kg/[m 2 ]) Age at Issue (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Mokdad A.H.](/thumbs/82/84935173.jpg) U.S. Adults: 1988 Nineteen states with 10-14% 14% Prevalence of Obesity (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Metabolic John P. Cello, MD Professor of Medicine and Surgery, University of California,
U.S. Adults: 1988 Nineteen states with 10-14% 14% Prevalence of Obesity (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Metabolic John P. Cello, MD Professor of Medicine and Surgery, University of California,
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE
 PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
Eighty percent of hepatocellular carcinoma cases are caused by infection with hepatitis B virus
 Chapter 1 Prevention Introduction Eighty percent of hepatocellular carcinoma cases are caused by infection with hepatitis B virus (HBV) or hepatitis C virus (HCV). Cases of fatty liver and nonalcoholic
Chapter 1 Prevention Introduction Eighty percent of hepatocellular carcinoma cases are caused by infection with hepatitis B virus (HBV) or hepatitis C virus (HCV). Cases of fatty liver and nonalcoholic
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
Liver transplantation and hepatitis C virus
 Liver transplantation and hepatitis C virus Where do we come from? Where are we? Where are we going? François Durand Hépatologie & Réanimation Hépato-Digestive INSERM U1149 Hôpital Beaujon, Clichy HCV:
Liver transplantation and hepatitis C virus Where do we come from? Where are we? Where are we going? François Durand Hépatologie & Réanimation Hépato-Digestive INSERM U1149 Hôpital Beaujon, Clichy HCV:
Interaction of Adipokines and Hepatitis B Virus on Histological Liver Injury in the Chinese
 132 ORIGINAL CONTRIBUTIONS nature publishing group Interaction of Adipokines and Hepatitis B Virus on Histological Liver Injury in the Chinese Vincent Wai-Sun Wong, MD1, 2, Grace Lai-Hung Wong, MD 1, 2,
132 ORIGINAL CONTRIBUTIONS nature publishing group Interaction of Adipokines and Hepatitis B Virus on Histological Liver Injury in the Chinese Vincent Wai-Sun Wong, MD1, 2, Grace Lai-Hung Wong, MD 1, 2,
Hepatocellular Carcinoma: Can We Slow the Rising Incidence?
 Hepatocellular Carcinoma: Can We Slow the Rising Incidence? K.Rajender Reddy M.D. Professor of Medicine Director of Hepatology Medical Director of Liver Transplantation University of Pennsylvania Outline
Hepatocellular Carcinoma: Can We Slow the Rising Incidence? K.Rajender Reddy M.D. Professor of Medicine Director of Hepatology Medical Director of Liver Transplantation University of Pennsylvania Outline
At Least 1 in 5 Patients in Your Practice Have Fatty Liver
 At Least 1 in 5 Patients in Your Practice Have Fatty Liver What Can You Tell Your Patients Magnus McLeod MD FRCPC Assistant Professor Dalhousie University 30-NOV-2017 NAFLD Non-Alcoholic Fatty Liver Disease
At Least 1 in 5 Patients in Your Practice Have Fatty Liver What Can You Tell Your Patients Magnus McLeod MD FRCPC Assistant Professor Dalhousie University 30-NOV-2017 NAFLD Non-Alcoholic Fatty Liver Disease
An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications
 REVIEW An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications Naim Alkhouri, M.D.,*, and Andrea Scott, B.S.* Nonalcoholic fatty liver disease (NAFLD)
REVIEW An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications Naim Alkhouri, M.D.,*, and Andrea Scott, B.S.* Nonalcoholic fatty liver disease (NAFLD)
Antiviral agents in HCV
 Antiviral agents in HCV : Upcoming Therapeutic Options Su Jong Yu, M.D., Ph.D. Department of Internal Medicine, Liver Research Institute, Seoul National University College of Medicine Estimated 170 Million
Antiviral agents in HCV : Upcoming Therapeutic Options Su Jong Yu, M.D., Ph.D. Department of Internal Medicine, Liver Research Institute, Seoul National University College of Medicine Estimated 170 Million
Non-Alcoholic Fatty Liver Disease (NAFLD)
 HEPATO-PANCREATO-BILIARY STOMACH CANCER PROGRAM Non-Alcoholic Fatty Liver Disease (NAFLD) Steatosis and Non-Alcoholic Steatohepatitis (NASH) Management Recommendations UCSF Fresno Department of Surgery
HEPATO-PANCREATO-BILIARY STOMACH CANCER PROGRAM Non-Alcoholic Fatty Liver Disease (NAFLD) Steatosis and Non-Alcoholic Steatohepatitis (NASH) Management Recommendations UCSF Fresno Department of Surgery
tage Percent Total & over Total & over Men Women Men Women
 Paul Angulo, MD, FACG, AGAF Professor of Medicine, Section Chief of Hepatology Division i i of Digestive i Diseases and Nutrition i University of Kentucky Medical Center Lexington, KY Paul Angulo, MD University
Paul Angulo, MD, FACG, AGAF Professor of Medicine, Section Chief of Hepatology Division i i of Digestive i Diseases and Nutrition i University of Kentucky Medical Center Lexington, KY Paul Angulo, MD University
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
5/12/2016. Learning Objectives. Management of Hepatitis C Virus Genotype 2 or 3 Infected Treatment-Naive or Experienced Patients
 5/12/216 Management of Hepatitis C Virus Genotype 2 or 3 Infected Treatment-Naive or Experienced Patients Alexander Monto, MD Professor of Clinical Medicine University of California San Francisco San Francisco,
5/12/216 Management of Hepatitis C Virus Genotype 2 or 3 Infected Treatment-Naive or Experienced Patients Alexander Monto, MD Professor of Clinical Medicine University of California San Francisco San Francisco,
Prise en charge actuelle de l'hépatite C et nouvelles approches thérapeutiques
 Prise en charge actuelle de l'hépatite C et nouvelles approches thérapeutiques Future Complications of Darius Moradpour Service de Gastro-entérologie et d'hépatologie Centre Hospitalier Universitaire Vaudois
Prise en charge actuelle de l'hépatite C et nouvelles approches thérapeutiques Future Complications of Darius Moradpour Service de Gastro-entérologie et d'hépatologie Centre Hospitalier Universitaire Vaudois
HCV: Racial Disparities. Charles D. Howell, M.D., A.G.A.F Professor of Medicine University of Maryland School of Medicine Baltimore, MD
 HCV: Racial Disparities Charles D. Howell, M.D., A.G.A.F Professor of Medicine University of Maryland School of Medicine Baltimore, MD Charles Howell Disclosures Research Grants Boehringer Ingelheim, Inc.
HCV: Racial Disparities Charles D. Howell, M.D., A.G.A.F Professor of Medicine University of Maryland School of Medicine Baltimore, MD Charles Howell Disclosures Research Grants Boehringer Ingelheim, Inc.
Consensus AASLD-EASL HBV Treatment Endpoint and HBV Cure Definition
 Consensus AASLD-EASL HBV Treatment Endpoint and HBV Cure Definition Anna S. Lok, MD, DSc Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research
Consensus AASLD-EASL HBV Treatment Endpoint and HBV Cure Definition Anna S. Lok, MD, DSc Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research
NAFLD: evidence-based management. Curso de residentes AEEH Salvador Augustin, MD Liver Unit Vall d Hebron Hospital Barcelona, Spain
 NAFLD: evidence-based management Curso de residentes AEEH 2017 Salvador Augustin, MD Liver Unit Vall d Hebron Hospital Barcelona, Spain Clinical case - 55 yo female - Sent for incidental steatosis at abdominal
NAFLD: evidence-based management Curso de residentes AEEH 2017 Salvador Augustin, MD Liver Unit Vall d Hebron Hospital Barcelona, Spain Clinical case - 55 yo female - Sent for incidental steatosis at abdominal
