The Allegheny County HealthChoices Program, 2008: The Year in Review
|
|
|
- Gary Craig
- 5 years ago
- Views:
Transcription
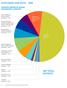
1 The Allegheny County HealthChoices Program, : The Year in Review A publication of Allegheny HealthChoices, Inc. August 2009 Overview and Highlights HealthChoices is Pennsylvania s managed care program for Medical Assistance. This program provides physical and behavioral health care to children and. The Year in Review Report provides an overview of the HealthChoices behavioral health program in Allegheny County during. and alcohol treatment increased 11% from More people accessing needed services is considered a positive change. Paid claims for drug and alcohol services also increased significantly, as payment rates for some services were increased. See page 3. Allegheny HealthChoices, Inc. (AHCI) produces the Year in Review Report as a means of presenting information about the status of the HealthChoices program in Allegheny County. The report describes changes in enrollment and service use in comparison to The highlights of the Year in Review Report include: Enrollment and rates of access to services remained consistent from 2007 to. For both children/adolescent and adult age groups, the average monthly enrollment did not increase from 2007 to. The percentage of enrolled children/ adolescents and who accessed services increased slightly (by 6% and 4% respectively). Race and gender enrollment and service access patterns did not change significantly from 2007 to. See pages 2 and 4. Adolescent access to drug and alcohol services increased. The number of adolescents accessing drug The HealthChoices Program: At a Glance 151,305 people were enrolled, on average, each month in 38,199 people (25%) accessed mental health and/or drug and alcohol treatment $196.8 million was spent on paid claims for treatment services The average cost per service user in was $5,152 Use of residential treatment facility (RTF) services by children and adolescents continued to decrease. Fewer children received RTF services as part of the Integrated Children s Services Initiative (ICSI). See pages 2-3. Access to crisis services increased. In July, Allegheny County s redesigned crisis services became available through the Western Psychiatric Institute and Clinic (WPIC). Publicity efforts for the re:solve Crisis Network have resulted in increased access to these services. Telephone and mobile services began in July, and walk-in and crisis residential services began at the end of December. See pages 3 and 5. Community-based, recoveryoriented services for continued to expand. In order to meet the anticipated community treatment needs with the closure of Mayview State Hospital, capacity to provide Community Treatment Team (CTT), mobile medications, and enhanced clinical case management continued to expand in. See pages 4-5. Inside this issue: Enrollment and Service Use for Children and Adolescents Enrollment and Service Use for Adults Enrollment and Access to Services 2 Enrollment and Access to Services 4 Mental Health Service Use 2 3 Mental Health Service Use 4 5 Common Diagnoses 3 Common Diagnoses 5 Drug and Alcohol Service Use 3 Drug and Alcohol Service Use 6
2 Page 2 Allegheny County HealthChoices Program, Enrollment and Service Use for Children and Adolescents Enrollment and Access to Services Enrollment in the HealthChoices program in remained very similar to 2007 for children and adolescents (0-20 years old). In : 81,107 children and adolescents were enrolled on average per month; 47% of enrollees are African-American, 47% are Caucasian, and 5% are of other races. 14,576 enrollees (18%) used behavioral health services. 14,104 (97%) used mental health services totaling $98.2 million in paid claims, and 1,168 (8%) used drug and alcohol services totaling $3.3 million in paid claims. The average cost per person using services was $7,118. Caucasian males continued to be more likely to access services; African-American females were less likely to access services. This enrollment and service access profile is consistent with 2007 data. Changes in Mental Health Service Use In, over 14,000 children and adolescents used mental health services, a 6% increase from Paid claims for mental health services totaled $98.2 million, a 3% increase from Table 1 summarizes the different mental health services used by children and adolescents in compared to Behavioral health rehabilitation services (BHRS) accounted for the largest portion of paid claims (43%); nearly one third of service users used BHRS services. BHRS service use did not change significantly (defined as an increase or decrease of more than 10%) from Residential treatment facilities accounted for 18% of claims in and were used by 3% of service users. RTF use has varied in the past several years due to the introduction of the Integrated Children s Services Initiative in Use peaked in 2006, and has since decreased due to several factors. First, overall system capacity has decreased. Second, an ongoing initiative of the Office of Children, Youth and Families to decrease the number of children in out-ofhome placement resulted in fewer referrals for RTF services. Inpatient mental health services accounted for 10% of claims, an increase of 13% from The number of children/adolescents using inpatient services did not vary significantly from 2007, and the increase in paid claims is partly due to an increase in the payment rates to providers. Note this category includes a very small number of extended acute care stays, which are not included in the following admission rates. The overall number of admissions decreased 3% from 2007, and the admission rate also decreased slightly from 902 to 8.72 admissions per 1,000 enrollees. Additionally, the rate of readmission occurring within 30 days of discharge decreased from 16% in 2007 to 15% in. The average length of stay increased from 10.4 days to 11.3 days. Family-based mental health services, partial hospitalization, and service coordination services each accounted for less than 10% of claims, and use of these services did not increase or decrease more than 10% from Table 1. Paid Claims and Number of Children and Adolescents (0-20 years) Using Mental Health Services, Paid claims in paid claims decrease in claims? Number of children children Behavioral Health Rehab. Services $ % 4,465 32% Residential Treatment Facilities $ % 433 3% Inpatient Mental Health $9.7 10% 861 6% Family-Based Mental Health Services $7.9 8% 883 6% Partial Hospitalization $6.1 6% 1,138 8% Service Coordination $4.6 5% 1,946 14% Outpatient Mental Health $5.3 5% 9,162 65% Medication Checks $1.1 1% 4,916 35% Family-Focused Solution-Based Services $1.0 1% 205 1% Crisis Services $0.2 0% 1,178 8% Other Mental Health Services $2.9 3% 953 7% All Mental Health Services $ % 14, % KEY: = an increase of more than 10% from 2007 = a decrease of more than 10% from 2007 = a change of less than ± 10% from 2007 decrease in # of children?
3 Allegheny HealthChoices, Inc. Page 3 While outpatient mental health services accounted for only 5% of paid claims in, 65% of consumers accessed outpatient services. Claims increased 10% from Claims for medication checks also increased significantly from 2007 (21%) due to an increase in the average payment rate. A similar number of people (35%) used these services in 2007 and. Family-focused solution based services continued to expand in, with an increase of 22% in paid claims and 18% in the number of service users. While paid claims for crisis services decreased 42% from 2007, 40% more children and adolescents used crisis services in. In July, Allegheny County s redesigned crisis services became available through the Western Psychiatric Institute and Clinic (WPIC). Also in, more claims were submitted for people receiving evaluations at WPIC s diagnostic and evaluation center (DEC). Paid claims for other mental health services increased 22% from 2007, and the number of children/adolescents using these services increased 28%. These increases are due to changes in two services. One service specializes in early identification and brief intervention services for mental health issues in community settings for members of underserved populations. The second service provides intensive services to children and adolescents with a combination of complex mental health, mental retardation, and severe behavioral disorder diagnoses. Also, Multisystemic Therapy (MST) became available as a HealthChoices service in Allegheny County. MST is a research-based therapy model for adolescents years with behavioral issues that put them at risk for out-of-home placement. Common Diagnoses in Diagnosis data in this report comes from claims forms providers submit after they have provided a service. Of the 14,581 people ages 0-20 years who used mental health and/or drug and alcohol services in, many had different diagnoses on different claims. Throughout this report, the diagnosis used most often (on claims forms) is considered that individual s diagnosis. In, the largest amount of claims dollars ($30.2 million, 30%) was spent in the treatment of children with autism spectrum disorders (see Table 2), an 11% increase from The number of children with these diagnoses using services increased 14% from 2007 to. Other common diagnoses included ADHD, adjustment disorder, major depression, and conduct disorder. The number of people with these primary diagnoses and paid claims did not change significantly (increase or decrease more than 10%) from 2007 to. Table 2. Claims Paid by Primary Diagnosis for Children and Adolescents, Claims (millions) # Children Autism Spectrum D/O $30.2 2,098 ADHD $21.6 3,438 Adjustment D/O $8.2 3,062 Major Depression $ Conduct D/O $ Oppositional Defiant D/O $ Bipolar D/O $ Depressive D/O $ Neurotic D/O $ Drug and Alcohol D/O $ Other MH diagnoses $ All Diagnoses $ ,581 Changes in Drug and Alcohol Service Use Table 3 shows commonly used drug and alcohol services for adolescents. Of the children and adolescents using HealthChoices services, 8% (1,168 people) used at least one drug and alcohol treatment service in, an 11% increase from Overall, use of drug and alcohol services accounts for about 3% ($3.3 million) of paid claims for children and adolescents. From 2007 to, paid claims for drug and alcohol services increased 33%. The largest increase occurred in non-hospital rehabilitation services, where payment rates increased in and the average number of units per person also increased. Use of outpatient drug and alcohol services also increased significantly from 2007 to, with more people accessing these services with greater average frequency. Of the adolescents using drug and alcohol services, 37% had a primary diagnosis of a mental health disorder. Common drug and alcohol diagnoses included cannabis (33%), opioid, e.g. heroin and OxyContin (10%) and alcohol (8%) use/abuse disorders. Table 3. Drug and Alcohol Services: Paid Claims and Number of Adolescents Using Services, Paid Claims # Adolescents Non-hospital Rehabilitation $1,938, Outpatient Drug and Alcohol $632, Halfway House $235, Intensive Outpatient Drug and $233, Alcohol Partial Hospitalization Program $79, Methadone Maintenance $75, Non-hospital Detoxification $57, Other Drug and Alcohol Services $15, Total D&A Services $3,266,821 1,168
4 Page 4 Allegheny County HealthChoices Program, Enrollment and Service Use for Adults Enrollment and Access to Services Enrollment in the HealthChoices program in remained very similar to 2007 for 21 years and older. In : 70,196 were enrolled on average per month; 38% of enrollees are African-American, 58% are Caucasian, and 4% are of other races. 23,831 enrollees (34%) used behavioral health services during, totaling $95.7 in paid claims. The average cost per person using services was $3, ,197 (85%) used mental health services totaling $66.9 million in paid claims, and 7,512 (32%) used drug and alcohol services totaling $28.7 million in paid claims. Caucasian males continued to be more likely to access services; African-American females were less likely. This enrollment and service access profile is consistent with 2007 data. Changes in Mental Health Service Use In, over 20,000 used mental health services, a 6% increase from Paid claims for mental health services totaled $66.9 million, a 13% increase from Table 4 summarizes the different mental health services used by in compared to Inpatient mental health services continued to account for the largest proportion of paid claims ($25.8 million); 15% of adult service users used inpatient mental health services. Use of inpatient services did not change significantly (defined as an increase or decrease of more than 10%) from See page 5. Traditional service coordination services accounted for 15% of paid claims in and were used by 18% of adult service users, consistent with use of this service in A number of services were developed or expanded in in order to meet the anticipated community treatment needs with the closure of Mayview State Hospital. While these services were used by relatively small percentages of people, this expanded capacity helps account for the overall increase in paid claims from 2007 to. The number of Community Treatment Teams expanded from four in 1996 to nine in As a result of this expansion, claims for CTT services increased 47% from 2007 to, and the number of using CTT services increased 29%. CTT services represented 10% of paid claims in, and are accessed by a small percentage (2%) of those using mental health services. Enhanced clinical case management and mobile medication teams continued to grow in their capacity during. Table 4. Paid Claims and Number of Adults (21 Years and Older) Using Mental Health Services, Paid claims in paid claims decrease in claims? Number of Inpatient Mental Health $ % 3,070 15% Service Coordination $9.8 15% 3,573 18% Outpatient Mental Health $7.5 11% 14,470 72% Community Treatment Team (CTT) $6.9 10% 451 2% Inpatient Extended Acute $3.6 5% 59 0% Respite and Diversion/Acute Stabilization $2.4 4% 401 2% Medication Checks $2.4 4% 11,983 59% Residential Treatment Facility for Adults $1.8 3% 64 0% Partial Hospitalization $1.2 2% 622 3% Enhanced Clinical Case Management $0.9 1% 88 0% Mobile Medication Team $0.8 1% 156 1% Psychiatric Rehabilitation $0.7 1% 396 2% Crisis Services $0.2 0% 1,861 9% Other Mental Health Services $2.6 4% 2,882 14% All Mental Health Services $ % 20, % KEY: = an increase of more than 10% from 2007 = a decrease of more than 10% from 2007 = a change of less than ± 10% from 2007 decrease in # of?
5 Allegheny HealthChoices, Inc. Page 5 The Inpatient Extended Acute unit at Western Psychiatric Institute and Clinic (WPIC) expanded its capacity from 15 to 30 beds in early. As a result, claims increased 80% and the number of people using extended acute services increased 28% from 2007 to. Paid claims for the residential treatment facility for (RTF-A) increased 30%, and the number of people using these services increased 10% from 2007 (bed capacity was expanded during 2007). From 2007 to, the average length of stay increased from 58 to 76 days. Outpatient mental health services continued to be used by the largest proportion of ; 72% of adult service users accessed outpatient services during. Because outpatient services are relatively inexpensive, they accounted for 11% of paid claims in, similar to Medication checks were the second most commonly accessed mental health service, with 59% of adult services users accessing these services during. Paid claims increased as a result of a rate increase. Paid claims for crisis services increased 18% and the number of using crisis services doubled from In July, Allegheny County s redesigned crisis services became available through the Western Psychiatric Institute and Clinic (WPIC). Publicity efforts for the re:solve Crisis Network have resulted in increased access to these services. Telephone and mobile services began in July, and walk-in and crisis residential services began at the end of December. In addition to these services, more claims were submitted for people receiving evaluations at WPIC s diagnostic and evaluation center (DEC), contributing to the overall increase. From 2007 to, paid claims for respite services and diversion/acute stabilization services increased 12%, while the number of people using these services remained consistent with The increase is the result of an increase in the average amount of services used per person. Common Diagnoses in In, the largest amount of claims for mental health diagnoses were spent in the treatment of schizophrenia ($28.7 million, 3,557 ). See Table 5. Other common primary diagnoses includer major depression ($11.4 million, 4,777 ), bipolar disorder ($9.2 million, 2,698 ), and depressive disorder ($6.7 million, 1,852). From 2007 to, paid claims for people with primary diagnoses of schizophrenia and unspecified psychoses increased significantly. People in these diagnostic groups used more CTT services. They also used inpatient mental health and extended acute services in larger proportions. Treatment for people with primary drug and alcohol disorders accounts for 31% of paid claims (29.2 million). See page 6. Table 5. Claims Paid by Primary Diagnosis for Adults, Claims (millions) # Adults Schizophrenia $28.7 3,557 Major Depression $11.4 4,777 Bipolar D/O $9.2 2,698 Depressive D/O $6.7 1,852 Neurotic D/O $1.9 1,630 Unspecified Psychosis $ Adjustment D/O $2.0 1,193 Other MH diagnoses $3.7 1,228 Drug and Alcohol D/O $29.2 6,491 All Diagnoses $ ,831 Inpatient Mental Health and Extended Acute Services for Adults, Inpatient mental health services continue to account for the largest portion of claims paid for in the HealthChoices program. Paid claims did not increase or decrease significantly (10% or more) from 2007 to despite the large changes in the adult behavioral health system in (including service expansion and the closure of Mayview State Hospital, both discussed above). The admission rate decreased slightly from 39.5 to 37 admissions per 1,000 enrollees from 2007 to. The average length of stay increased from 10.2 days to 10.8 days (a 6% increase) from 2007 to. The readmission rate remained high, with 20% readmitted within 30 days and an additional 14% readmitted within days. During, inpatient extended acute services expanded capacity. These services are for people who need longer-term stabilization than is available on an inpatient mental health unit. These services are an alternative to state hospital services. In contrast to inpatient mental health services, there were only 53 admissions to extended acute services during, and the average length of stay for extended acute stays remained consistent, at 125 days in 2007 and 128 days in. Table 6. Inpatient Mental Health Services, Key Statistics Number of with at least 3,325 one admission Admission rate (admissions per ,000 enrollees) Average length of stay (days) 10.8 % of discharges resulting in a 20% readmission within 30 days % of discharges resulting in a 14% readmission within days
6 Page 6 Allegheny County HealthChoices Program, Changes in Drug and Alcohol Health Service Use for Adults, In, 7,512 used drug and alcohol services, a 6% increase from Paid claims for drug and alcohol services totaled $28.7 million, a 6% increase from Table 7 summarizes the different drug and alcohol services used by in compared to Overall, use of drug and alcohol treatment by in was similar to Non-hospital rehabilitation accounted for the largest portion of paid claims (40%, $11.4 million); 28% of who accessed drug and alcohol treatment used nonhospital rehab services. Non-hospital rehab use did not change significantly (defined as an increase or decrease of more than 10%) from Methadone maintenance accounted for 25% of paid claims for drug and alcohol treatment ($7.2 million), and was used by 29% of who accessed drug and alcohol treatment. Methadone maintenance use in also did not change significantly from While outpatient drug and alcohol services represented only 8% of paid claims, 56% of using drug and alcohol services accessed outpatient treatment. Paid claims increased 13% from 2007, and the number of using outpatient services increased 10% from Paid claims for partial hospitalization programs increased 13%, as the average number of treatment hours used per person increased. The number of people using partial hospitalization services in was similar to Paid claims for inpatient and non-hospital detoxification services increased. Both types of services had a significant increase (more than 10%) in the average units per service user. The number of people using inpatient detoxification services also increased significantly from The largest amount of drug and alcohol claims dollars were spent in the treatment of opioid (e.g. heroin, OxyContin) addictions ($10.8 million, 2,823 ). Other drug and alcohol diagnoses included dependence on multiple substances ($5.0 million, 1,031 ), cocaine disorders ($4.1 million, 874 ) and alcohol disorders ($3.1 million, 1,059 ). A large number of who used drug and alcohol services had a primary diagnosis of a mental health disorder ($4.1 million, 1,267 people). The most common mental health diagnoses for individuals receiving drug and alcohol services were depressive disorder, major depression, and bipolar disorder. Table 7. Paid Claims and Number of Adults (21 Years and Older) Using Drug and Alcohol Services, Paid claims in (millions) paid claims decrease in claims? Number of Non-hospital Rehabilitation $ % 2,094 28% Methadone Maintenance $7.2 25% 2,213 29% Halfway House $2.6 9% 478 6% Outpatient Drug and Alcohol $2.3 8% 4,186 56% Partial Hospitalization Program $1.7 6% 1,064 14% Intensive Outpatient Program $1.3 5% 1,262 17% Inpatient Detoxification $1.0 5% 362 5% Non-hospital Detoxification $0.7 3% % Inpatient Rehabilitation $0.1 0% 40 1% Medication Checks $0.1 0% % All Drug and Alcohol Services $ % 7, % KEY: = an increase of more than 10% from 2007 = a decrease of more than 10% from 2007 = a change of less than ± 10% from 2007 decrease in # of? 444 Liberty Ave. Suite 240 Pittsburgh, PA Phone: Fax: OUR MISSION IS TO SUPPORT EQUITABLE ACCESS ACROSS ALL POPULATIONS TO QUALITY, HOLISTIC, COST-EFFECTIVE BEHAVIORAL HEALTH CARE. Visit us on the web at to learn more. AHCI is a contract agency for the Allegheny County Department of Human Services HealthChoices Program.
2017 Year in Review The Allegheny County HealthChoices Behavioral Health Program. A report from Allegheny HealthChoices, Inc.
 2017 Year in Review The Allegheny County HealthChoices Behavioral Health Program A report from Allegheny HealthChoices, Inc. DECEMBER 2018 Introduction Medicaid is a publicly financed health care program
2017 Year in Review The Allegheny County HealthChoices Behavioral Health Program A report from Allegheny HealthChoices, Inc. DECEMBER 2018 Introduction Medicaid is a publicly financed health care program
The Value of Engagement in Substance Use Disorder (SUD) Treatment
 The Value of Engagement in Substance Use Disorder (SUD) Treatment A Report from Allegheny HealthChoices, Inc. June 2016 Introduction When considering substance use disorder (SUD) treatment, the length
The Value of Engagement in Substance Use Disorder (SUD) Treatment A Report from Allegheny HealthChoices, Inc. June 2016 Introduction When considering substance use disorder (SUD) treatment, the length
Youth Using Behavioral Health Services. Making the Transition from the Child to Adult System
 Youth Using Behavioral Health Services Making the Transition from the Child to Adult System Allegheny HealthChoices Inc. January 2013 Youth Using Behavioral Health Services: Making the Transition from
Youth Using Behavioral Health Services Making the Transition from the Child to Adult System Allegheny HealthChoices Inc. January 2013 Youth Using Behavioral Health Services: Making the Transition from
Blair County HealthChoices
 Blair County HealthChoices Annual Report Fiscal Year 2012-2013 County Commissioners Terry Tomassetti, Chair Diane L. Meling, Vice-Chair Ted Beam, Secretary BLAIR COUNTY PENNSYLVANIA Prepared December 2014
Blair County HealthChoices Annual Report Fiscal Year 2012-2013 County Commissioners Terry Tomassetti, Chair Diane L. Meling, Vice-Chair Ted Beam, Secretary BLAIR COUNTY PENNSYLVANIA Prepared December 2014
Blair County HealthChoices
 Blair County HealthChoices Annual Report Fiscal Year 2013-2014 County Commissioners Terry Tomassetti, Chair Diane L. Meling, Vice-Chair Ted Beam, Secretary Prepared January 2015 HEALTHCHOICES HealthChoices
Blair County HealthChoices Annual Report Fiscal Year 2013-2014 County Commissioners Terry Tomassetti, Chair Diane L. Meling, Vice-Chair Ted Beam, Secretary Prepared January 2015 HEALTHCHOICES HealthChoices
Medicaid Long-Term Services and Supports in Maryland:
 Medicaid Long-Term Services and Supports in Maryland: FY 2009 to FY 2012 Volume 2 The Autism Waiver A Chart Book May 29, 2014 Prepared for Maryland Department of Health and Mental Hygiene TABLE OF CONTENTS
Medicaid Long-Term Services and Supports in Maryland: FY 2009 to FY 2012 Volume 2 The Autism Waiver A Chart Book May 29, 2014 Prepared for Maryland Department of Health and Mental Hygiene TABLE OF CONTENTS
Statewide Statistics and Key Findings 1
 % s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
% s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
Blair County HealthChoices
 Blair County HealthChoices Executive Summary Fiscal Year 2016-2017 Ten-Year Edition County Commissioners Bruce Erb, Chair Terry Tomassetti, Vice-Chair Ted Beam, Secretary Prepared October 2017 HEALTHCHOICES
Blair County HealthChoices Executive Summary Fiscal Year 2016-2017 Ten-Year Edition County Commissioners Bruce Erb, Chair Terry Tomassetti, Vice-Chair Ted Beam, Secretary Prepared October 2017 HEALTHCHOICES
Behavioral Health Providers: Facility/Ancillary Application Addendum
 Please complete a separate form for each clinical location. Provider identification Legal business name: Doing business as (if applicable): Address: Anthem Blue Cross and Blue Shield Healthcare Solutions
Please complete a separate form for each clinical location. Provider identification Legal business name: Doing business as (if applicable): Address: Anthem Blue Cross and Blue Shield Healthcare Solutions
New York Medicaid Beneficiaries with Mental Health and Substance Abuse Conditions
 Medicaid institute at united Hospital Fund New York Medicaid Beneficiaries with Mental Health and Substance Abuse Conditions About the Medicaid Institute at United Hospital Fund Established in 2005, the
Medicaid institute at united Hospital Fund New York Medicaid Beneficiaries with Mental Health and Substance Abuse Conditions About the Medicaid Institute at United Hospital Fund Established in 2005, the
PITTSBURGH MERCY: COMPREHENSIVE INTEGRATED CARE JUNE 6, 2018
 PITTSBURGH MERCY: COMPREHENSIVE INTEGRATED CARE JUNE 6, 2018 AN ENHANCED MEDICAL HOME MODEL FOR THE SMI POPULATION Comprehensive Care Patient Centered Care Coordinated Care Accessible Services Quality
PITTSBURGH MERCY: COMPREHENSIVE INTEGRATED CARE JUNE 6, 2018 AN ENHANCED MEDICAL HOME MODEL FOR THE SMI POPULATION Comprehensive Care Patient Centered Care Coordinated Care Accessible Services Quality
Multi-Dimensional Family Therapy. Full Service Partnership Outcomes Report
 MHSA Multi-Dimensional Family Therapy Full Service Partnership Outcomes Report TABLE OF CONTENTS Enrollment 5 Discontinuance 5 Demographics 6-7 Length of Stay 8 Outcomes 9-11 Youth Outcome Questionnaire
MHSA Multi-Dimensional Family Therapy Full Service Partnership Outcomes Report TABLE OF CONTENTS Enrollment 5 Discontinuance 5 Demographics 6-7 Length of Stay 8 Outcomes 9-11 Youth Outcome Questionnaire
ADDING EVEN MORE SUBSTANCE TO MANAGED CARE
 HEALTH WEALTH CAREER ADDING EVEN MORE SUBSTANCE TO MANAGED CARE OPTIMIZING MEDICAID TO RESPOND TO SUBSTANCE USE DISORDERS NATIONAL ACADEMY FOR STATE HEALTH POLICY 30TH ANNUAL STATE HEALTH POLICY CONFERENCE
HEALTH WEALTH CAREER ADDING EVEN MORE SUBSTANCE TO MANAGED CARE OPTIMIZING MEDICAID TO RESPOND TO SUBSTANCE USE DISORDERS NATIONAL ACADEMY FOR STATE HEALTH POLICY 30TH ANNUAL STATE HEALTH POLICY CONFERENCE
Services Provided. Mental Health Outpatient services for individuals and family
 Apple Health Integrated Managed Care and In-Network Agencies and Behavioral Southwest Washington Catholic Services 9300 NE Oak View Dr Suite B Vancouver WA 98662 (360) 567-2211 Crisis Line SW WA: (800)
Apple Health Integrated Managed Care and In-Network Agencies and Behavioral Southwest Washington Catholic Services 9300 NE Oak View Dr Suite B Vancouver WA 98662 (360) 567-2211 Crisis Line SW WA: (800)
Department of Human Services/Oregon Health Authority Addictions and Mental Health Division (AMH) November 25, 2009
 Disclaimer High Level Briefing on Addiction Treatment System Prepared for the Alcohol and Drug Policy Commission This paper reflects only the highest level briefing information about the addiction treatment
Disclaimer High Level Briefing on Addiction Treatment System Prepared for the Alcohol and Drug Policy Commission This paper reflects only the highest level briefing information about the addiction treatment
and Supports in Maryland: The Autism Waiver
 Medicaid Long Term Services and Supports in Maryland: The Autism Waiver FY 2006 to FY 2009 A Chart Book December 3, 2010 Prepared for: Maryland Department of Health and Mental Hygiene Overview of Medicaid
Medicaid Long Term Services and Supports in Maryland: The Autism Waiver FY 2006 to FY 2009 A Chart Book December 3, 2010 Prepared for: Maryland Department of Health and Mental Hygiene Overview of Medicaid
Thurston Mason Behavioral Health Organization 2017 Budget (Jan-Dec)
 Thurston Mason Behavioral Health Organization (Jan-Dec) Social Services Programs Program: D611 & D699 Chemical Dependency Administration Description: This program is responsible for implementing the program
Thurston Mason Behavioral Health Organization (Jan-Dec) Social Services Programs Program: D611 & D699 Chemical Dependency Administration Description: This program is responsible for implementing the program
County of San Diego, Health and Human Services Agency IN HOME OUTREACH TEAM PROGRAM REPORT (IHOT)
 County of San Diego, Health and Human Services Agency IN HOME OUTREACH TEAM PROGRAM REPORT (IHOT) Annual Report January 1, 2012 to December 31, 2012 County of San Diego, Health and Human Services Agency
County of San Diego, Health and Human Services Agency IN HOME OUTREACH TEAM PROGRAM REPORT (IHOT) Annual Report January 1, 2012 to December 31, 2012 County of San Diego, Health and Human Services Agency
REQUEST FOR PROPOSALS FOR CY 2019 FUNDING. Issue Date: Monday, July 30, Submission Deadline: 5:00 p.m., Friday, August 24, 2018
 REQUEST FOR PROPOSALS FOR CY 2019 FUNDING Issue Date: Monday, July 30, 2018 Submission Deadline: 5:00 p.m., Friday, August 24, 2018 NOTE: RFP proposals received after the deadline will not be considered.
REQUEST FOR PROPOSALS FOR CY 2019 FUNDING Issue Date: Monday, July 30, 2018 Submission Deadline: 5:00 p.m., Friday, August 24, 2018 NOTE: RFP proposals received after the deadline will not be considered.
Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications
 MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MISSION VISION OVERARCHING GOAL. An Overview of Behavioral Health Services. Clients thriving in their natural environments
 San Francisco Health Commission Community and Public Health Committee Presentation: Kavoos Ghane Bassiri, LMFT, LPCC, CGP Director, Behavioral Health Services An Overview of Behavioral Health Services
San Francisco Health Commission Community and Public Health Committee Presentation: Kavoos Ghane Bassiri, LMFT, LPCC, CGP Director, Behavioral Health Services An Overview of Behavioral Health Services
PROCEDURE CODES & UNIT
 PROCEDURE CODES & UNIT CPT Valid and its modifiers, which is billable to SAMH or Medicaid 90801 HW B No Yes Psychiatric Evaluation (Evaluation and management) when funded by the state mental health authority
PROCEDURE CODES & UNIT CPT Valid and its modifiers, which is billable to SAMH or Medicaid 90801 HW B No Yes Psychiatric Evaluation (Evaluation and management) when funded by the state mental health authority
Financial Impact of Emergency Department Visits by Adults for Dental Conditions in Maryland
 Financial Impact of Emergency Department by Adults for Dental Conditions in Maryland Background Access to dental care remains challenging for many children and adults. Lack of preventive care services
Financial Impact of Emergency Department by Adults for Dental Conditions in Maryland Background Access to dental care remains challenging for many children and adults. Lack of preventive care services
Community Services - Eligibility
 Community Services - Eligibility In order for DMH to reimburse care, the individual must meet both financial and clinical eligibility criteria. These criteria are described in detail in the DMH provider
Community Services - Eligibility In order for DMH to reimburse care, the individual must meet both financial and clinical eligibility criteria. These criteria are described in detail in the DMH provider
DELAWARE COUNTY Directory of Child and Adolescent Mental Health and Drug & Alcohol Services
 DELAWARE COUNTY Directory of Mental Health and Drug & Alcohol DELAWARE COUNTY Office of Behavioral Health 20 S. 69 th Street 610-713-2365 December 2012 DELAWARE COUNTY OFFICE OF BEHAVIORAL HEALTH Mission
DELAWARE COUNTY Directory of Mental Health and Drug & Alcohol DELAWARE COUNTY Office of Behavioral Health 20 S. 69 th Street 610-713-2365 December 2012 DELAWARE COUNTY OFFICE OF BEHAVIORAL HEALTH Mission
FACT SHEET Mental Health and Substance Use Disorder Benefits
 FACT SHEET 01-01 Mental Health and Substance Use Disorder Benefits What is CHAMPVA? CHAMPVA is a health benefits program in which the Department of Veterans Affairs (VA) shares the cost of certain health
FACT SHEET 01-01 Mental Health and Substance Use Disorder Benefits What is CHAMPVA? CHAMPVA is a health benefits program in which the Department of Veterans Affairs (VA) shares the cost of certain health
Greenville County Commission on Alcohol and Drug Abuse The Phoenix Center. Public Report. Fiscal Year 2013
 Greenville County Commission on Alcohol and Drug Abuse The Phoenix Center Public Report Fiscal Year 2013 Fiscal Year 2013 Services Report July 2012 June 2013 Introduction The vision of the Greenville County
Greenville County Commission on Alcohol and Drug Abuse The Phoenix Center Public Report Fiscal Year 2013 Fiscal Year 2013 Services Report July 2012 June 2013 Introduction The vision of the Greenville County
(888) pyramidhealthcarepa.com. The Right Choice For Every Stage of Addiction Recovery
 (888) 694-9996 pyramidhealthcarepa.com The Right Choice For Every Stage of Addiction Recovery The Right Choice For Every Stage of Addiction Recovery Our Integrated Recovery Approach Guarantees That the
(888) 694-9996 pyramidhealthcarepa.com The Right Choice For Every Stage of Addiction Recovery The Right Choice For Every Stage of Addiction Recovery Our Integrated Recovery Approach Guarantees That the
Outlook and Outcomes Fiscal Year 2011
 Baltimore Substance Abuse Systems, Inc. Outlook and Outcomes Fiscal Year 2011 Baltimore City Greg Warren, President Compiled July 2012 BSAS Outlook and Outcomes is the first edition of a planned annual
Baltimore Substance Abuse Systems, Inc. Outlook and Outcomes Fiscal Year 2011 Baltimore City Greg Warren, President Compiled July 2012 BSAS Outlook and Outcomes is the first edition of a planned annual
BEHAVIORAL H E A L T H T R E A T M E N T. for a bright future
 BEHAVIORAL H E A L T H T R E A T M E N T Hope for a bright future Providing a comprehensive mental health and addiction treatment continuum for senior adults, adults and adolescents Offering a Comprehensive
BEHAVIORAL H E A L T H T R E A T M E N T Hope for a bright future Providing a comprehensive mental health and addiction treatment continuum for senior adults, adults and adolescents Offering a Comprehensive
DELAWARE COUNTY Directory of Child and Adolescent Mental Health and Drug & Alcohol Services
 DELAWARE COUNTY Directory of Mental Health and Drug & Alcohol DELAWARE COUNTY Office of Behavioral Health 20 S. 69 th Street Upper Darby, PA 19082 610-713-2365 SEPTEMBER 2014 DELAWARE COUNTY OFFICE OF
DELAWARE COUNTY Directory of Mental Health and Drug & Alcohol DELAWARE COUNTY Office of Behavioral Health 20 S. 69 th Street Upper Darby, PA 19082 610-713-2365 SEPTEMBER 2014 DELAWARE COUNTY OFFICE OF
Lancaster County Drug and Alcohol Commission Treatment Needs Assessment Summary
 Lancaster County Drug and Alcohol Commission 2016 Treatment Needs Assessment Summary Rick Kastner, Executive Director Lancaster County Drug and Alcohol Commission 150 N. Queen St. Lancaster, PA 17603 Ph.
Lancaster County Drug and Alcohol Commission 2016 Treatment Needs Assessment Summary Rick Kastner, Executive Director Lancaster County Drug and Alcohol Commission 150 N. Queen St. Lancaster, PA 17603 Ph.
Using Evidence to Support Recovery through Comprehensive Community Services (CCS) Presentation Objectives. What is CCS? 10/17/2018
 Using Evidence to Support Recovery through Comprehensive Community Services (CCS) Chris Keenan and Tim Connor October 17, 2018 Presentation Objectives Understand the needs of CCS participants related to
Using Evidence to Support Recovery through Comprehensive Community Services (CCS) Chris Keenan and Tim Connor October 17, 2018 Presentation Objectives Understand the needs of CCS participants related to
Kaiser Telecare Program for Intensive Community Support Intensive Case Management Exclusively for Members within a Managed Care System
 Kaiser Telecare Program for Intensive Community Support Intensive Case Management Exclusively for Members within a Managed Care System 12-Month Customer Report, January to December, 2007 We exist to help
Kaiser Telecare Program for Intensive Community Support Intensive Case Management Exclusively for Members within a Managed Care System 12-Month Customer Report, January to December, 2007 We exist to help
Appendix A AUTIM SPECTRUM DISORDER FEASIBILITY STUDY
 Appendix A AUTIM SPECTRUM DISORDER FEASIBILITY STUDY Description: Representatives from the Departments of Social Services (DSS), Mental Health and Addiction Services (DMHAS), Children and Families (DCF),
Appendix A AUTIM SPECTRUM DISORDER FEASIBILITY STUDY Description: Representatives from the Departments of Social Services (DSS), Mental Health and Addiction Services (DMHAS), Children and Families (DCF),
DMHAS ASAM SERVICE DESCRIPTIONS
 (DMHAS) Fee for Service (FFS) ANNEX A1 DMHAS ASAM SERVICE DESCRIPTIONS Please carefully review the Service Descriptions that are included in the DMHAS FFS Initiatives in this Annex A1 contract section.
(DMHAS) Fee for Service (FFS) ANNEX A1 DMHAS ASAM SERVICE DESCRIPTIONS Please carefully review the Service Descriptions that are included in the DMHAS FFS Initiatives in this Annex A1 contract section.
Hours of Operation. Monday Thursday 9am 9pm Friday 9am 5pm. Call the clinic for evening, Saturday and walk-in hours, where available.
 Lahey Health Behavioral LIST OF SERVICES 1 Ambulatory (Outpatient) Population(s) Served Outpatient Mental Health Counseling Beverly Clinic Lawrence Clinic Accepts most insurances, including. Cigna not
Lahey Health Behavioral LIST OF SERVICES 1 Ambulatory (Outpatient) Population(s) Served Outpatient Mental Health Counseling Beverly Clinic Lawrence Clinic Accepts most insurances, including. Cigna not
DMAS UPDATE ON GAP PROGRAM. Cindi B. Jones, Director, DMAS House Appropriations Committee September 18, 2017
 DMAS UPDATE ON GAP PROGRAM Cindi B. Jones, Director, DMAS House Appropriations Committee September 18, 2017 Bridging the Mental Health Coverage GAP GAP s Inception The Governor s Access Plan 1 of a 10
DMAS UPDATE ON GAP PROGRAM Cindi B. Jones, Director, DMAS House Appropriations Committee September 18, 2017 Bridging the Mental Health Coverage GAP GAP s Inception The Governor s Access Plan 1 of a 10
OPIOID USE DISORDER CENTERS OF EXCELLENCE APPLICATION GENERAL INFORMATION
 OPIOID USE DISORDER CENTERS OF EXCELLENCE APPLICATION GENERAL INFORMATION The Department of Human Services (DHS) is implementing 50 opioid use disorder (OUD) Health Homes or Centers of Excellence (COE)
OPIOID USE DISORDER CENTERS OF EXCELLENCE APPLICATION GENERAL INFORMATION The Department of Human Services (DHS) is implementing 50 opioid use disorder (OUD) Health Homes or Centers of Excellence (COE)
TESTIMONY Of Pam Gehlmann Executive Director/ Assistant Regional Director Pinnacle Treatment Centers Alliance Medical Services-Johnstown
 TESTIMONY Of Pam Gehlmann Executive Director/ Assistant Regional Director Pinnacle Treatment Centers Alliance Medical Services-Johnstown Center for Rural Pennsylvania On Confronting the Heroin Epidemic
TESTIMONY Of Pam Gehlmann Executive Director/ Assistant Regional Director Pinnacle Treatment Centers Alliance Medical Services-Johnstown Center for Rural Pennsylvania On Confronting the Heroin Epidemic
Peer Support Services Improve Clinical Outcomes by Fostering Recovery and Promoting Empowerment
 Peer Support Services Improve Clinical Outcomes by Fostering Recovery and Promoting Empowerment Optum has recognized the role of peer support services as an integral part of state Medicaid plans and has
Peer Support Services Improve Clinical Outcomes by Fostering Recovery and Promoting Empowerment Optum has recognized the role of peer support services as an integral part of state Medicaid plans and has
Learning Objectives. 1. Developing an idea of what High-Fidelity Wraparound (HFW)looks like in Pittsburgh, Pennsylvania
 System Navigators Christine McClellan- Family Resources Steve Freas- Human Services Administration Organization (HSAO) Wednesday, June 8, 2016 1:00 to 2:30 PM Learning Objectives 1. Developing an idea
System Navigators Christine McClellan- Family Resources Steve Freas- Human Services Administration Organization (HSAO) Wednesday, June 8, 2016 1:00 to 2:30 PM Learning Objectives 1. Developing an idea
Mental Disorders Among OEF/OIF Veterans Using VA Health Care: Facts and Figures
 Mental Disorders Among OEF/OIF Veterans Using VA Health Care: Facts and Figures Erin Bagalman Analyst in Health Policy January 11, 2013 CRS Report for Congress Prepared for Members and Committees of Congress
Mental Disorders Among OEF/OIF Veterans Using VA Health Care: Facts and Figures Erin Bagalman Analyst in Health Policy January 11, 2013 CRS Report for Congress Prepared for Members and Committees of Congress
Emergency Department Boarding of Psychiatric Patients in Oregon
 College of Public Health and Human Sciences Emergency Department Boarding of Psychiatric Patients in Oregon Jangho Yoon, PhD, Jeff Luck, PhD April 25, 2017 Scope Quantify the extent of psychiatric emergency
College of Public Health and Human Sciences Emergency Department Boarding of Psychiatric Patients in Oregon Jangho Yoon, PhD, Jeff Luck, PhD April 25, 2017 Scope Quantify the extent of psychiatric emergency
PROVIDER ALERT. The CT BHP WILL NO LONGER create temporary member records for all other levels of care
 PROVIDER ALERT Alert #: PA 2011-22 Issued: September 2011 To: Subject: CT BHP Providers Revised Procedure - Temporary Member Certification Dear Provider, The CT Behavioral Health Partnership issued a Provider
PROVIDER ALERT Alert #: PA 2011-22 Issued: September 2011 To: Subject: CT BHP Providers Revised Procedure - Temporary Member Certification Dear Provider, The CT Behavioral Health Partnership issued a Provider
FIRST STEPS TREATMENT CENTER. David Moran CACD, LCSW, TEP Crozer-Chester Medical Center
 FIRST STEPS TREATMENT CENTER David Moran CACD, LCSW, TEP Crozer-Chester Medical Center SOBERING FACTS 1. 3500 overdose deaths in Pennsylvania in 2015 2. OD rate in PA 26/100,000 OD rate in US 14.7/100,000
FIRST STEPS TREATMENT CENTER David Moran CACD, LCSW, TEP Crozer-Chester Medical Center SOBERING FACTS 1. 3500 overdose deaths in Pennsylvania in 2015 2. OD rate in PA 26/100,000 OD rate in US 14.7/100,000
Mental Health Services Act. Transforming the Santa Barbara County System of Care. Data Report: Santa Barbara County and System of Care
 1 Mental Health Services Act Transforming the Santa Barbara County System of Care Data Report: Santa Barbara County and System of Care Prepared by: April Howard, M.A. Departmental Analyst Santa Barbara
1 Mental Health Services Act Transforming the Santa Barbara County System of Care Data Report: Santa Barbara County and System of Care Prepared by: April Howard, M.A. Departmental Analyst Santa Barbara
In 2008, an estimated 282,000 persons
 National Survey of Substance Abuse Treatment Services The N-SSATS Report January 28, 2010 Similarities and Differences in Opioid Treatment Programs that Provide Methadone Maintenance or Buprenorphine Maintenance
National Survey of Substance Abuse Treatment Services The N-SSATS Report January 28, 2010 Similarities and Differences in Opioid Treatment Programs that Provide Methadone Maintenance or Buprenorphine Maintenance
Carolyn Holder MSN, RN, GCNS-BC Director, Transitional Care and Utilization Management Summa Health System Akron, Ohio
 Carolyn Holder MSN, RN, GCNS-BC Director, Transitional Care and Utilization Management Summa Health System Akron, Ohio Why Involve Hospitals? Where individuals go with acute illness if plan fails or if
Carolyn Holder MSN, RN, GCNS-BC Director, Transitional Care and Utilization Management Summa Health System Akron, Ohio Why Involve Hospitals? Where individuals go with acute illness if plan fails or if
Chester County Drug & Alcohol Services Map
 START Call 911 Chester County Drug & Alcohol Services Map Are you in a lifethreatening situation/ condition (medical or psychiatric)? Do you need ambulance assistance? Go to the nearest hospital/er You
START Call 911 Chester County Drug & Alcohol Services Map Are you in a lifethreatening situation/ condition (medical or psychiatric)? Do you need ambulance assistance? Go to the nearest hospital/er You
Hours of Operation. Monday Thursday 9am 9pm Friday 9am 5pm. Call the clinic for evening, Saturday and walk-in hours, where available.
 Lahey Health Behavioral LIST OF SERVICES 1 Ambulatory (Outpatient) Population(s) Served Outpatient Mental Health Counseling Beverly Clinic Lawrence Clinic Accepts most insurances, including. Cigna not
Lahey Health Behavioral LIST OF SERVICES 1 Ambulatory (Outpatient) Population(s) Served Outpatient Mental Health Counseling Beverly Clinic Lawrence Clinic Accepts most insurances, including. Cigna not
PROCEDURE CODES & UNIT
 PROCEDURE CODES & UNIT CPT Procedure Valid Procedure and its modifiers, which is billable to SAMH or Medicaid Modifiers Programs 1 MEDICAID SAMH/DCF Long Description Recommended cost Comments 90801 HW
PROCEDURE CODES & UNIT CPT Procedure Valid Procedure and its modifiers, which is billable to SAMH or Medicaid Modifiers Programs 1 MEDICAID SAMH/DCF Long Description Recommended cost Comments 90801 HW
Medicaid and the Opioid Crisis
 Medicaid and the Opioid Crisis Erica Floyd Thomas Bureau Chief of Medicaid Policy Agency for Health Care Administration Presented to: Medical Care Advisory Committee March 20, 2018 1 Florida Medicaid Covers
Medicaid and the Opioid Crisis Erica Floyd Thomas Bureau Chief of Medicaid Policy Agency for Health Care Administration Presented to: Medical Care Advisory Committee March 20, 2018 1 Florida Medicaid Covers
Making the Business Case for Long-Acting Injectables
 Making the Business Case for Long-Acting Injectables David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Chief Clinical Officer Partners Behavioral Health Management
Making the Business Case for Long-Acting Injectables David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Chief Clinical Officer Partners Behavioral Health Management
Managed Care and the Quality of Substance Abuse Treatment
 The Journal of Mental Health Policy and Economics Managed Care and the Quality of Substance Abuse Treatment Donald S. Shepard, 1 Marilyn Daley, 2 * Grant A. Ritter, 3 Dominic Hodgkin 4 and Richard H. Beinecke
The Journal of Mental Health Policy and Economics Managed Care and the Quality of Substance Abuse Treatment Donald S. Shepard, 1 Marilyn Daley, 2 * Grant A. Ritter, 3 Dominic Hodgkin 4 and Richard H. Beinecke
Appendix A CABHC Reinvestment Project List
 Projects inclusive of ALL Counties Respite Care All YAP 02-03, 04/05 05/06,07/08 08/09,10/11, 13/14 : Respite services offer short-term respite services to children, adolescents, and adults. The services
Projects inclusive of ALL Counties Respite Care All YAP 02-03, 04/05 05/06,07/08 08/09,10/11, 13/14 : Respite services offer short-term respite services to children, adolescents, and adults. The services
Choose an item. Choose an item.
 PROGRAM INFORMATION: Program Title: Support and Overnight Stay (SOS) Provider: Westcare California Program Description: Case Management MHP Work Plan: 4-Behavioral health clinical care 1 Behavioral Health
PROGRAM INFORMATION: Program Title: Support and Overnight Stay (SOS) Provider: Westcare California Program Description: Case Management MHP Work Plan: 4-Behavioral health clinical care 1 Behavioral Health
Request for Proposals
 Request for Proposals Innovative Model for Bringing Autism Expertise and Services to Rural Areas of Pennsylvania The Pennsylvania Department of Public Welfare (DPW) through the Tuscarora Intermediate Unit
Request for Proposals Innovative Model for Bringing Autism Expertise and Services to Rural Areas of Pennsylvania The Pennsylvania Department of Public Welfare (DPW) through the Tuscarora Intermediate Unit
Behavioral Health Hospital and Emergency Department Health Services Utilization
 Behavioral Health Hospital and Emergency Department Health Services Utilization Rhode Island Fee-For-Service Medicaid Recipients Calendar Year 2000 Prepared for: Prepared by: Medicaid Research and Evaluation
Behavioral Health Hospital and Emergency Department Health Services Utilization Rhode Island Fee-For-Service Medicaid Recipients Calendar Year 2000 Prepared for: Prepared by: Medicaid Research and Evaluation
Missouri CCBHC Initiative: Early results show expanded access to care, increased scope of services
 Missouri CCBHC Initiative: Early results show expanded access to care, increased scope of services Section 223 of the Protecting Access to Medicare Act of 2014 established a federal definition and criteria
Missouri CCBHC Initiative: Early results show expanded access to care, increased scope of services Section 223 of the Protecting Access to Medicare Act of 2014 established a federal definition and criteria
Emergency Department Visits for Behavioral Health Conditions in Harris County, Texas,
 Emergency Department Visits for Behavioral Health Conditions in Harris County, Texas, 2007-2008 Prepared by School of Public Health UT Health Patrick Courtney, MA August 2010 1 Table of Contents Executive
Emergency Department Visits for Behavioral Health Conditions in Harris County, Texas, 2007-2008 Prepared by School of Public Health UT Health Patrick Courtney, MA August 2010 1 Table of Contents Executive
Allegheny County Justice Related Services for Individuals with Mental Illness:
 Justice Related Services for Individuals with Mental Illness: From Point of Initial Contact/Diversion to Specialty Courts to Re-Entry from County and State Correctional Institutions Department of Human
Justice Related Services for Individuals with Mental Illness: From Point of Initial Contact/Diversion to Specialty Courts to Re-Entry from County and State Correctional Institutions Department of Human
Exhibit I-1 Performance Measures. Numerator (general description only)
 # Priority Type Performance Measure Core Measures (implement 9/1/09) 1 C OE Hospital readmissions within 7, 30 and 90 days postdischarge 2 C OE Percent of Members prescribed redundant or duplicated antipsychotic
# Priority Type Performance Measure Core Measures (implement 9/1/09) 1 C OE Hospital readmissions within 7, 30 and 90 days postdischarge 2 C OE Percent of Members prescribed redundant or duplicated antipsychotic
Addiction Services in the Central West LHIN
 Addiction Services in the Central West LHIN Helen Danakas Coordinator, Withdrawal Management Hélène (Leela Leela) Tanguay, PhD, RP, ICADC Coordinator, Narcotics Strategy Overview of Presentation Addiction
Addiction Services in the Central West LHIN Helen Danakas Coordinator, Withdrawal Management Hélène (Leela Leela) Tanguay, PhD, RP, ICADC Coordinator, Narcotics Strategy Overview of Presentation Addiction
Report to The Vermont Legislature. Substance Abuse Treatment Services Objectives and Performance Measures Progress: Second Annual Report
 Report to The Vermont Legislature Substance Abuse Treatment Services Objectives and Performance Measures Progress: Second Annual Report In Accordance with Act 179 () Sec. E.306.2 (a)(2) Submitted to: Submitted
Report to The Vermont Legislature Substance Abuse Treatment Services Objectives and Performance Measures Progress: Second Annual Report In Accordance with Act 179 () Sec. E.306.2 (a)(2) Submitted to: Submitted
American Addiction Centers Outcomes Study Long-Term Outcomes Among Residential Addiction Treatment Clients. Centerstone Research Institute
 American Addiction Centers Outcomes Study Long-Term Outcomes Among Residential Addiction Treatment Clients Centerstone Research Institute 2018 1 AAC Outcomes Study: Long-Term Outcomes Executive Summary
American Addiction Centers Outcomes Study Long-Term Outcomes Among Residential Addiction Treatment Clients Centerstone Research Institute 2018 1 AAC Outcomes Study: Long-Term Outcomes Executive Summary
ADVANCED BEHAVIORAL HEALTH, INC. Clinical Level of Care Guidelines
 The Clinical Level of Care Guidelines contained on the following pages have been developed as a guide to assist care managers, physicians and providers in making medical necessity decisions about the least
The Clinical Level of Care Guidelines contained on the following pages have been developed as a guide to assist care managers, physicians and providers in making medical necessity decisions about the least
Mental Health Services in Georgia
 Mental Health Services in Georgia VISION: A Georgia where all affected by mental illness find Hope, Help, and Acceptance. MISSION: To empower NAMI affiliates to create communities where all effected by
Mental Health Services in Georgia VISION: A Georgia where all affected by mental illness find Hope, Help, and Acceptance. MISSION: To empower NAMI affiliates to create communities where all effected by
Outcomes Monitoring System Iowa Project
 Outcomes Monitoring System Iowa Project Year Six Report Prepared By: Iowa Consortium for Substance Abuse Research and Evaluation University of Iowa, Iowa City, Iowa 52242-5000 With Funds Provided By: Iowa
Outcomes Monitoring System Iowa Project Year Six Report Prepared By: Iowa Consortium for Substance Abuse Research and Evaluation University of Iowa, Iowa City, Iowa 52242-5000 With Funds Provided By: Iowa
Heroin Use in Illinois: A Ten-Year Multiple Indicator Analysis, 1998 to 2008
 Heroin Use in Illinois: A Ten-Year Multiple Indicator Analysis, 1998 to 2008 EXECUTIVE SUMMARY AND FINDINGS Co-authored by: Stephanie Schmitz Kathleen Kane-Willis Research Support: Laura Reichel, Elizabeth
Heroin Use in Illinois: A Ten-Year Multiple Indicator Analysis, 1998 to 2008 EXECUTIVE SUMMARY AND FINDINGS Co-authored by: Stephanie Schmitz Kathleen Kane-Willis Research Support: Laura Reichel, Elizabeth
Treatment Costs Among Adults With Serious Mental Illness: Influences of Criminal Justice Involvement and Psychiatric Diagnoses
 Treatment Costs Among Adults With Serious Mental Illness: Influences of Criminal Justice Involvement and Psychiatric Diagnoses The Promises and Challenges of Administrative Data in Social Policy Research
Treatment Costs Among Adults With Serious Mental Illness: Influences of Criminal Justice Involvement and Psychiatric Diagnoses The Promises and Challenges of Administrative Data in Social Policy Research
Adult Mental Health Services applicable to Members in the State of Connecticut subject to state law SB1160
 Adult Mental Health Services Comparison Create and maintain a document in an easily accessible location on such health carrier's Internet web site that (i) (ii) compares each aspect of such clinical review
Adult Mental Health Services Comparison Create and maintain a document in an easily accessible location on such health carrier's Internet web site that (i) (ii) compares each aspect of such clinical review
Outcomes Monitoring System Iowa Project
 Outcomes Monitoring System Iowa Project Year Seven Report Prepared By: Iowa Consortium for Substance Abuse Research and Evaluation University of Iowa, Iowa City, Iowa 52242-5000 With Funds Provided By:
Outcomes Monitoring System Iowa Project Year Seven Report Prepared By: Iowa Consortium for Substance Abuse Research and Evaluation University of Iowa, Iowa City, Iowa 52242-5000 With Funds Provided By:
New Jersey Department of Human Services Division of Mental Health and Addiction Services
 I. BACKGROUND New Jersey Department of Human Services Division of Mental Health and Addiction Services BIANNUAL REPORT Plan for the Establishment and Funding of Regional Substance Abuse Treatment Facilities
I. BACKGROUND New Jersey Department of Human Services Division of Mental Health and Addiction Services BIANNUAL REPORT Plan for the Establishment and Funding of Regional Substance Abuse Treatment Facilities
Levels of Treatment and 12 Step Self-Help Recovery Programs
 Read the following information. When you come to the questions (which are in italics), enter your answers to them in the space provided. Often a family crisis, such as the intervention of child welfare
Read the following information. When you come to the questions (which are in italics), enter your answers to them in the space provided. Often a family crisis, such as the intervention of child welfare
Patterns of Hospital Admissions and Readmissions Among HIV-Positive Patients in Southwestern Pennsylvania
 Patterns of Hospital Admissions and Readmissions Among HIV-Positive Patients in Southwestern Pennsylvania Keith T. Kanel, MD, MHCM, FACP Colleen Vrbin Susan Elster, PhD Jason Kunzman, MBA Michelle Murawski,
Patterns of Hospital Admissions and Readmissions Among HIV-Positive Patients in Southwestern Pennsylvania Keith T. Kanel, MD, MHCM, FACP Colleen Vrbin Susan Elster, PhD Jason Kunzman, MBA Michelle Murawski,
OUTCOMES AND DATA 2016
 AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
Child & Adolescent Mental Health Services Databook, FY08-09
 Clients Receiving County- Unique clients funded Mental Health Services 17,779 ANASAZI CLIENTS, Q2-4 ONLY 15,179 Age Unique clients % Living Arrangement* Unique clients % Age 0 to 5 1,907 10.7% House or
Clients Receiving County- Unique clients funded Mental Health Services 17,779 ANASAZI CLIENTS, Q2-4 ONLY 15,179 Age Unique clients % Living Arrangement* Unique clients % Age 0 to 5 1,907 10.7% House or
Case Management Policy and Procedures
 Case Management Policy and Procedures Subject: Priority Populations Pregnant Women Interim Services (Form Attached) Policy #: M 5.02.1 Effective Date: 7/1/08 Revision Date:11/09 (Language changes to Referral
Case Management Policy and Procedures Subject: Priority Populations Pregnant Women Interim Services (Form Attached) Policy #: M 5.02.1 Effective Date: 7/1/08 Revision Date:11/09 (Language changes to Referral
Behavioral Health Authorization Requirements*
 100 All inclusive room and board MN 0 MN 0 101 All inclusive room and board MN Use MN Criteria for IP Medically-Supervised detox MN 0 104 Anesthesia, ECT MN 0 MN 0 114 Room and Board- private psychiatric
100 All inclusive room and board MN 0 MN 0 101 All inclusive room and board MN Use MN Criteria for IP Medically-Supervised detox MN 0 104 Anesthesia, ECT MN 0 MN 0 114 Room and Board- private psychiatric
A Model for a Comprehensive Behavioral Health Crisis Service
 National Association of State Mental Health Program Directors (NASMHPD) Annual 2017 Meeting: A Model for a Comprehensive Behavioral Health Crisis Service Edgar K. Wiggins, M.H.S. Executive Director, Baltimore
National Association of State Mental Health Program Directors (NASMHPD) Annual 2017 Meeting: A Model for a Comprehensive Behavioral Health Crisis Service Edgar K. Wiggins, M.H.S. Executive Director, Baltimore
Division of Behavioral Health Services
 Division of Behavioral Health Services Annual Report on Substance Abuse Treatment Programs Fiscal Year 2012 Submitted Pursuant to A.R.S. 36-2023 December 31, 2012 Report Contents Program Names and Locations
Division of Behavioral Health Services Annual Report on Substance Abuse Treatment Programs Fiscal Year 2012 Submitted Pursuant to A.R.S. 36-2023 December 31, 2012 Report Contents Program Names and Locations
Cuyahoga County Council Committee of the Whole
 Cuyahoga County Council Committee of the Whole ADAMHS Board 2016 Budget Presentation William M. Denihan, CEO November 5, 2015 Mission The Alcohol, Drug Addiction and Mental Health Services (ADAMHS) Board
Cuyahoga County Council Committee of the Whole ADAMHS Board 2016 Budget Presentation William M. Denihan, CEO November 5, 2015 Mission The Alcohol, Drug Addiction and Mental Health Services (ADAMHS) Board
HIPAA APPROVED PROCEDURE CODES & ITS DESCRIPTION
 HIPAA APPROVED PROCEDURE CODES & ITS DESCRIPTION Valid Procedure Codes and its description Below are HIPAA codes and definitions of approved Procedure Codes for Mental Health and Substance Abuse. These
HIPAA APPROVED PROCEDURE CODES & ITS DESCRIPTION Valid Procedure Codes and its description Below are HIPAA codes and definitions of approved Procedure Codes for Mental Health and Substance Abuse. These
Include Substance Use Disorder Services in New Hampshire Medicaid Managed Care
 Include Substance Use Disorder Services in New Hampshire Medicaid Managed Care New Futures mission is to advocate, educate, and collaborate to reduce alcohol and other drug problems in New Hampshire. Expanding
Include Substance Use Disorder Services in New Hampshire Medicaid Managed Care New Futures mission is to advocate, educate, and collaborate to reduce alcohol and other drug problems in New Hampshire. Expanding
Final Evaluation Report
 The Louisiana Access to Recovery Project Final Evaluation Report Access to Recovery II: 2007-2010 Prepared for: Louisiana Department of Health and Hospitals (DHH) Office of Behavioral Health Author: Laurel
The Louisiana Access to Recovery Project Final Evaluation Report Access to Recovery II: 2007-2010 Prepared for: Louisiana Department of Health and Hospitals (DHH) Office of Behavioral Health Author: Laurel
ALCOHOL AND DRUG TREATMENT SERVICES. Provided by the Alcohol and Drug Abuse Division (ADAD) Hawaiʻi Department of Health
 ALCOHOL AND DRUG TREATMENT SERVICES 2015 Provided by the Alcohol and Drug Abuse Division (ADAD) Hawaiʻi Department of Health EXECUTIVE SUMMARY This report focuses on alcohol and drug treatment services
ALCOHOL AND DRUG TREATMENT SERVICES 2015 Provided by the Alcohol and Drug Abuse Division (ADAD) Hawaiʻi Department of Health EXECUTIVE SUMMARY This report focuses on alcohol and drug treatment services
THE IOWA CONSORTIUM FOR SUBSTANCE ABUSE RESEARCH AND EVALUATION. Special Report: Opioid Admissions in Iowa August 2016
 Special Report: State of Iowa Opioid Treatment Admissions 21-215 THE IOWA CONSORTIUM FOR SUBSTANCE ABUSE RESEARCH AND EVALUATION Special Report: Opioid Admissions in Iowa 21-215 August 216 With Funds Provided
Special Report: State of Iowa Opioid Treatment Admissions 21-215 THE IOWA CONSORTIUM FOR SUBSTANCE ABUSE RESEARCH AND EVALUATION Special Report: Opioid Admissions in Iowa 21-215 August 216 With Funds Provided
Optum Behavioral Health Services
 Optum Behavioral Health Services A whole-person approach to improve outcomes for Medicaid agencies and their members Serving the needs of the whole person At Optum, we re keenly aware of the challenges
Optum Behavioral Health Services A whole-person approach to improve outcomes for Medicaid agencies and their members Serving the needs of the whole person At Optum, we re keenly aware of the challenges
Medicaid Expansion: Its Critical Role in Ohio s Response to the Addiction Crisis
 Medicaid Expansion: Its Critical Role in Ohio s Response to the Addiction Crisis 1 Medicaid Expansion: Its Critical Role in Ohio s Response to the Addiction Crisis Ohio expanded Medicaid in 2014 to provide
Medicaid Expansion: Its Critical Role in Ohio s Response to the Addiction Crisis 1 Medicaid Expansion: Its Critical Role in Ohio s Response to the Addiction Crisis Ohio expanded Medicaid in 2014 to provide
Medicaid Treatment and Service Fees for Substance Use Disorder (SUD): CY
 Medicaid Treatment and Service Fees for Substance Use Disorder (SUD): CY 2012 2016 A Chart Book March 22, 2018 Abridged Version Prepared for the Maryland Department of Health TABLE OF CONTENTS Chapter
Medicaid Treatment and Service Fees for Substance Use Disorder (SUD): CY 2012 2016 A Chart Book March 22, 2018 Abridged Version Prepared for the Maryland Department of Health TABLE OF CONTENTS Chapter
State of Iowa Outcomes Monitoring System
 State of Iowa Outcomes Monitoring System THE IOWA CONSORTIUM FOR SUBSTANCE ABUSE RESEARCH AND EVALUATION Year 16 Annual Outcome Evaluation Trend Report November 2014 With Funds Provided By: Iowa Department
State of Iowa Outcomes Monitoring System THE IOWA CONSORTIUM FOR SUBSTANCE ABUSE RESEARCH AND EVALUATION Year 16 Annual Outcome Evaluation Trend Report November 2014 With Funds Provided By: Iowa Department
Strengthening Providers of Substance Use Treatment in Los Angeles County
 Strengthening Providers of Substance Use Treatment in Los Angeles County Summary Presented by July 218 Drug overdose is the thirdranked cause of premature death in L.A. County. 1 Substance use and misuse
Strengthening Providers of Substance Use Treatment in Los Angeles County Summary Presented by July 218 Drug overdose is the thirdranked cause of premature death in L.A. County. 1 Substance use and misuse
Consumers Helping Consumers. Peer Support Helped in my Recovery
 This report is a publication of Allegheny HealthChoices, Inc. Peer Support: S UMMER 2006 Consumers Helping Consumers For many years, people with mental illness have been helping each other in their personal
This report is a publication of Allegheny HealthChoices, Inc. Peer Support: S UMMER 2006 Consumers Helping Consumers For many years, people with mental illness have been helping each other in their personal
ATLAS on substance use 2017:
 WHO Forum on alcohol, drugs and addictive behaviours Enhancing public health actions through partnerships and collaboration ATLAS on substance use 17: resources for the prevention and treatment of substance
WHO Forum on alcohol, drugs and addictive behaviours Enhancing public health actions through partnerships and collaboration ATLAS on substance use 17: resources for the prevention and treatment of substance
Medical Necessity Criteria
 SECTION 3: MEDICAL NECESSITY CRITERIA 3.0 Definition of Medical Necessity Medical necessity is the principal criteria by which the Fresno County Mental Health Plan (FCMHP) decides to accept and approve
SECTION 3: MEDICAL NECESSITY CRITERIA 3.0 Definition of Medical Necessity Medical necessity is the principal criteria by which the Fresno County Mental Health Plan (FCMHP) decides to accept and approve
Using Peer Engagement to Drive Down ED Overutilization. Emergency Department Diversion for Behavioral Health patients at Bon Secours
 Using Peer Engagement to Drive Down ED Overutilization Emergency Department Diversion for Behavioral Health patients at Bon Secours Facilitators Dr. Aliya Jones, M.D. Bon Secours Baltimore Chair of the
Using Peer Engagement to Drive Down ED Overutilization Emergency Department Diversion for Behavioral Health patients at Bon Secours Facilitators Dr. Aliya Jones, M.D. Bon Secours Baltimore Chair of the
2016 Report Card Gwen Neilsen Anderson Rehabilitation Center Inpatient Rehabilitation Unit. stlukesonline.org
 2016 Report Card Gwen Neilsen Anderson Rehabilitation Center Inpatient Rehabilitation Unit stlukesonline.org Why the Gwen Neilsen Anderson Rehabilitation Center? The Gwen Neilsen Anderson Rehabilitation
2016 Report Card Gwen Neilsen Anderson Rehabilitation Center Inpatient Rehabilitation Unit stlukesonline.org Why the Gwen Neilsen Anderson Rehabilitation Center? The Gwen Neilsen Anderson Rehabilitation
RULES OF TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES
 RULES OF TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES CHAPTER 0940-06-04 ALCOHOL AND DRUG ADDICTION TREATMENT FUND SERVICES FOR D.U.I. OFFENDERS AND PEOPLE WITH PROBLEM GAMBLING
RULES OF TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES CHAPTER 0940-06-04 ALCOHOL AND DRUG ADDICTION TREATMENT FUND SERVICES FOR D.U.I. OFFENDERS AND PEOPLE WITH PROBLEM GAMBLING
