The Enhanced Recovery Programme (Frederick Salmon Ward)
|
|
|
- Charlotte Franklin
- 6 years ago
- Views:
Transcription
1 Patient Information Leaflet The Enhanced Recovery Programme (Frederick Salmon Ward) CHECKLIST Bowel preparation (day before surgery)... Dalteparin/fragmin injection (the evening before surgery) date/time:... Please go to theatre admissions unit (not Sunday) between 16:00 (4pm) and 18:00 (6pm). On Sunday please go to Frederick Salmon ward between 4pm and 6pm. Pre-operative drinks (morning of the operation) to be taken at 5am and finished by 6am. Fasting/nil by mouth from. (This time may be extended once you arrive at theatre admissions unit) Drugs to be taken on the morning of your operation: Theatre admissions unit is at the back of the hospital, car park 2. The unit opens at 7:15am. The telephone number is Frederick Salmon ward is on level 4 St Marks Hospital. Please use the Northwick Park entrance near the main lifts. There is an entry system to gain access. The telephone number is or SM0721
2 The Enhanced Recovery Programme Explaining the Enhanced Recovery Programme This booklet is to help you understand the St Mark s Hospital Enhanced Recovery Programme and how you will play an active part in your recovery. Aspects of this care can vary from what you might expect. This programme is different to traditional care and can improve your recovery considerably. The booklet describes the steps in your journey of care through St. Mark s until you are ready to go home, which is usually three to five days after your operation. If there is anything you are unsure about, please ask a member of staff or call the relevant number at the end of this booklet. Pre-habilitation Before your operation it is really beneficial for you to try and make yourself as fit as possible. You can do this by eating a mixed healthy diet and if you have lost weight (without meaning to) it is helpful to try and increase your weight. If you smoke it is ideal to give up smoking as soon as you can before your operation, your GP can help with this. If you drink alcohol it is ideal to give up drinking for a month before your operation. It is also useful to increase you exercise, even a 30 minute walk every other day is a good start. Pre-assessment clinic You have attended your clinic appointment in the outpatients department where you received this booklet. During this appointment you were assessed for your operation. The Enhanced Recovery Programme was explained to you and this booklet should act as a reminder for you. Although you may not require a stoma to be formed, it is current practice for people undergoing certain operations to have the stoma specialist nurse mark the abdomen (site) before the operation. Preparing for your operation Please be aware that there may be a lot of waiting about if you are admitted the day before your operation, so bring a good book to read. There is a television on the ward. You may need to sit in the day room or dining room until your bed is ready. Do I need bowel preparation? Some patients will not require bowel preparation. You will be told by the nurse in the pre-assessment clinic whether you will need bowel preparation. If bowel preparation is required: The day before your operation, you may be asked to drink a laxative medicine to help clear the contents of your bowel at about 2:30pm and 5:30pm (or after your injection). If this is necessary you need to have a low fibre diet on the day before the bowel preparation. This day your diet should consist of some of the following foods - boiled or steamed white fish, chicken (no skins), egg, cheese, white bread, plain muffins, butter, margarine, white rice, white pasta, rich tea biscuits, potatoes (no skins), cauliflower, Tofu, natural yoghurts, plain cottage cheese, tinned peaches/pineapple, plain sponge cakes, clear soup (without bits in). DO NOT EAT foods such as red meat, pink fish, raw fruit or other vegetables, skins/pips, cereals, salad, mushrooms, nuts, seeds, sweetcorn, wholemeal bread etc. You also need to try and drink two litres of clear fluids (8-10 glasses). The bowel preparation gives you loose, watery stools. It is important that you drink plenty of clear fluids but not fizzy drinks to replace the fluid you are losing. Clear fluids include black tea or black coffee, water, squash but not juice. Clear soup and jelly is good to take. This should stop you from
3 feeling dizzy, sick or getting a headache. You should not eat any solids on the day you take the laxative drinks or until after the operation. Some people have a drip (intravenous fluids) and you will be told if this is needed. Some patients will be given an enema before the operation to clear the lower part of the bowel. Other preparations for your surgery If you are able to eat the day before surgery it is a very good idea to have a meal the evening before the operation. You will be given a small injection of dalteparin (fragmin) in the skin. This helps reduce the risk of blood clots (thrombosis) by thinning your blood. This will be given to you each day while you are in hospital. You will also be asked to wear elastic stockings while you are in hospital as these also help to prevent clots. People coming into hospital the day of their surgery will need to have this the day before their operation. You need this injection on the evening before surgery. Thus in preassessment it will be arranged how this will occur. Most people come to the theatre admissions unit the evening before the operation for the nurses there to give it. Please bring this leaflet into the hospital when you are admitted to remind yourself of what to expect. Day of your operation (Day 0) You will be admitted to hospital early in the morning (between 7.15 and 7.30am usually) on the day of your operation to the theatre admissions unit. Eating and drinking before your operation The pre-assessment nurse will give the instructions that are relevant to you. You can eat until six hours before your operation (provided that you are not having a laxative bowel preparation). From 6 hours until 2 hours (or 4 hours see below) before your operation you can drink water, black tea, black coffee or squash drinks. No milky drinks are allowed. We will give you two cartons of an energy drink (preop) to drink 3 hours before your operation. This improves your recovery. Stop drinking after you take these. You will be given these in the preassessment clinic. You must not have anything at all to drink for two hours before your operation. If you have a hiatus hernia or suffer from severe heartburn you should not have anything to drink for four hours before your operation. Bowel clearance You may be given an enema two hours before your operation to clear the lower end of your bowel. After your operation (Day 0) Mobilisation/getting out of bed Following your operation, when you wake up, it is important that you perform deep breathing exercises. Breathe in through your nose and relax the air out through your mouth, undertake this at least five times an hour. Do cough when you need to try holding your abdomen to reduce the pain.
4 The staff will help you out of bed after your operation. You should try to spend up to two hours out of bed on the day of your operation. Eating and drinking after your operation After your operation it is important that you drink, unless you feel sick. Try to drink about five glasses or cups. You will be given energy drinks (Ensure Plus) after waking from your operation and should ask for them when you feel well enough. Pain control Good pain control improves your recovery as you can walk about, breathe deeply, eat and drink, feel relaxed and sleep well. You may have a tiny tube in your back (epidural) which provides a continuous supply of pain relieving medication. In addition you will be given other pain killers by mouth, which help in different ways. Alternatively you may have patient controlled analgesia (PCA). This has a button that you press to give yourself pain relief. There is a security device that prevents you taking too much. The anaesthetist will discuss these options with you before the operation Feeling sick After your operation you may feel sick or may vomit. This is usually caused by the anaesthetic or drugs used. You will be given medication during your operation to reduce this, but if you feel sick please speak to your nurse who will be able to give you something to help. Tubes and drips Whilst in theatre a tube (catheter) will be placed into your bladder so that your urine output can be measured. You will have a drip put into your arm and fluid will be given through this to ensure you do not become dehydrated. You will also have an oxygen mask or tubing on your face after the operation. Monitoring While you are in hospital we will check your blood pressure, pulse and temperature regularly. We will also check how much fluid you are taking in. Stoma If you have a stoma formed you may receive twice daily training to make sure that you can care for your stoma before you go home. The stoma specialist nurse will plan your care whilst you are in hospital and for your stoma care when at home. The day after your operation (Day 1) Mobilisation On each day after your surgery it is advised that, provided you feel well enough, you sit in the chair for a total of six hours, with intermittent rests on the bed as needed. You should aim to walk along the ward corridor and back four times (about 60 metres four times). By being out of bed in a more upright position and by walking regularly, your breathing is improved and there is less chance of you developing a chest infection or clots in your legs and your bowel function usually also recovers faster. Do cough when you need to try holding your abdomen to reduce the pain.
5 Eating and drinking It is important that you eat after your operation. You should try to drink about ten to twelve drinks (about 2000ml) per day unless you feel sick. Each cup is usually about ml. You can drink a variety of non-fizzy drinks whilst in hospital. High protein, high energy drinks are provided after your operation to help your body to heal, reduce the risk of infection and help your overall recovery. Try to take two or more each day. You will be encouraged to use the ward dining room for your meals. This also has an area for relaxation and reading. Please note that there is a fridge in the dining room that you can use to store food (that you have labelled with your name). We do not have facilities to heat food, but it can be useful to bring in snacks to have between meals. Meals times are approximately 8:30, 12:15 and 17:15 and we encourage all meals to be taken in the ward dining room, a bell will be rung 5 minutes before meals as a reminder to walk to the day room. You will have a laxative to encourage your bowels to work (but not if you have had your entire large bowel (colon) removed or if you have an ileostomy). Pain control You can continue to use your epidural or PCA. Regular pain killer tablets will be started on day 1. Some people find that walking can help with the pain. Feeling sick As before, tell the nurses if you feel sick. Tubes and drips If you are drinking well the drip will usually be removed in the morning. You will still keep your cannula (plastic tube in the vein). If you are mobilising the catheter in your bladder will usually be removed today, but after pelvic surgery we may leave the catheter until day 3. When the catheter is removed you will be asked to pass urine in a bottle or a bed pan so that we can measure your urine. Monitoring Your blood pressure, pulse, temperature, fluid balance and weight will be measured. You will be assessed regularly throughout the day. Washing and dressing After you have a wash today, you should put on your normal clothes, provided you feel well enough. This helps you feel positive about your recovery. The second day after your operation (Day 2) Mobilisation Continue to mobilise as before. Eating and drinking Continue to eat and drink, as you can tolerate. We advise ten to fifteen drinks each day. Pain control Your epidural or PCA will be removed today and you will continue on regular pain killer tablets. Monitoring Your blood pressure, pulse and temperature will be regularly monitored throughout the day.
6 The third day after your operation (Day 3) You need to continue to eat and drink, mobilise and get ready to go home. We will make arrangements for you to be seen in the outpatient clinic often two weeks after your operation. If your care needs to change from what is planned in this booklet we will tell you. The most likely problem that you may have is that your bowel stops working for a period of time after your operation (an ileus). This occurs in many patients undergoing bowel surgery, but in some people this can last a few days or longer. Having an ileus can make you feel sick or you might be sick. If this occurs tell your nurse. We may need to place a tube through your nostril to help with this. Discharge Criteria Before you are sent home we would ideally like you to: Be eating and drinking Be walking Have passed wind (flatus) Have your pain adequately controlled by pain killers Have no temperature We would ask you to leave your bed space by 10am and go to the day room, dining room or ideally the discharge lounge to wait for your discharge tablets and your lift home. What happens after discharge? It is well worthwhile planning in advance for your discharge. You may require someone to help with heavier jobs for a few weeks. This includes food shopping and heavy household jobs such as vacuuming and gardening. Although it is not necessary some people feel more confident to go home if a friend or family member can stay with them or put them up for a short period, if you live alone for example. Complications do not happen very often, but it is important that you know what to look out for. During the first two weeks after surgery, if you are worried about any of the following, please phone the ward (the number is at the end of this leaflet) to ask for advice. It may take a while for the telephone to be answered, keep trying. Abdominal pain It is not unusual to suffer gripping pains (colic) during the first week following removal of a portion of your bowel. The pain usually lasts for a few minutes and goes away between the spasms. If you have severe pain lasting more than one or two hours or have a fever and feel generally unwell within two weeks of your operation date, you should immediately contact the ward on the telephone numbers provided. Your wound It is not unusual for your wounds to be slightly red and uncomfortable during the first one or two weeks. Please telephone the ward if your wounds: - Become inflamed, painful or swollen - Start to discharge fluid Your bowels Your bowel habit may change after removal of part of the bowel and may become loose or constipated. Make sure you eat regular meals three or more times a day, drink adequate amounts, and take regular walks during the first two weeks after your operation. If constipation lasts for more
7 than three days then taking a laxative is advised. If you are passing loose stools more than three times per day for more than four days please call the ward and ask for advice. If you have a stoma, your stoma specialist nurse will explain about your stoma before you go home. Your stoma If you have a stoma and you have any problems with your stoma after you go home, please contact your stoma specialist nurse, you will be given contact details before you leave hospital. Passing urine Sometimes after bowel surgery you may experience a feeling that your bladder is not emptying fully. This usually improves with time. It is also worth keeping an eye on the colour of your urine. If you are well hydrated you should be passing straw colour urine. If you find that your urine is darker it may be a sign that you are dry and usually you should drink more. If you feel you are not emptying your bladder fully or if you have excessive stinging when passing urine, please ring the ward as you may have an infection. Diet A balanced, varied diet is recommended. Try eating three or more times a day. You may find that some foods upset you and cause loose bowel motions. If that is the case you should avoid those foods for the first few weeks following your surgery. If you are finding it difficult to eat it is still important to obtain an adequate amount of protein and calories to help your body heal. You may benefit from having three to four nourishing, high protein, high calorie drinks such as Build-up or Complan (available in supermarkets and chemists) to supplement your food. If you are suffering from diarrhoea then it is important to replace the fluid loss and to drink extra fluid and call Frederick Salmon for advice. If you are losing weight without trying to or are struggling to eat enough, you may benefit from a consultation with the dietitian; ask your GP to refer you. Exercise Walking is encouraged from the day following your operation. You should plan to undertake regular exercise several times a day and gradually increase this during the four weeks following your operation until you are back to your normal level of activity. The main restriction we would place on exercise is that you do not undertake heavy lifting and contact sports until six weeks following your surgery. In addition, if you are planning to restart a routine exercise such as jogging or swimming you should wait until at least two weeks after your operation and start gradually. Common sense will guide your exercise and rehabilitation. In general, if the wound is still uncomfortable, modify your exercise. Once the wounds are pain free you can normally undertake most activities. Work You should be able to return to work within two to four weeks after your operation. If your job is a heavy manual job then it is advised that heavy work should not be undertaken until six weeks after your operation. However you should check with your employer in case there are rules relevant to your return to work. Driving You should not drive until you are confident that you can drive safely. A good yardstick for this is when you have got back to most of your normal activities. Usually this will be within two to four weeks of surgery. It is important that any pain has resolved sufficiently to enable you to perform an emergency stop and turn the wheel quickly. Hobbies/Activities You should consider taking up your hobbies and activities as soon as possible again after surgery. It enables you to maintain your activity and will benefit your recovery. You should not need to restrict these unless they cause significant pain or involve heavy lifting, in which case avoid them for the first six weeks after your operation.
8 Tiredness You might find that you have low energy levels in the first few weeks that you are at home. It is important to mix activities with some rest as needed, but do get out of bed each day and get dressed if possible. Summary To enhance your recovery you will be expected to return to normal as quickly as possible. This means that you need to actively participate in your recovery by walking, eating and drinking. We will assist you by removing attachments such as the drip soon after the operation to make walking easier. Each day you should feel some improvement but do ask if you are worried about something. Frederick Salmon Ward visiting times 11:00-12:00 hours 13:00-17:00 hours 18:00-20:00 hours Contact details: For advice in the first few weeks after your discharge home, please call Frederick Salmon Ward: Ask to speak to Steve or Sarah (the peri-operative specialist practitioners) or the nurse in charge. North side South side If it is within 8am and 8pm Monday to Saturday you could contact Steve or Sarah on and ask for bleep 450. Admissions (for queries about your admission date before your operation). Jennie (enhanced recovery nurse) please note this number is not to be used for an emergency as the phone is not answered outside normal work hours or when on annual leave. For advice on any medicines you have received from the hospital, call Medicines Information on Opening hours are Monday Friday 9am 5pm. Alternatively you can via (patients and visitors/medicines advice for patients) St Mark s Hospital, Watford Road, Harrow, Middlesex, HA1 3UJ Authors: St Mark s Hospital multidisciplinary team Date: June 2013 Review date: January 2014
Patient Information Leaflet
 Patient Information Leaflet The Enhanced Recovery Programme Explaining the Enhanced Recovery Programme This booklet is to help you understand the Rana Hospital Enhanced Recovery Programme and how you will
Patient Information Leaflet The Enhanced Recovery Programme Explaining the Enhanced Recovery Programme This booklet is to help you understand the Rana Hospital Enhanced Recovery Programme and how you will
Information for patients
 Introduction This booklet will help you understand the St Mark s Hospital Enhanced Recovery Programme and how you will play an active part in your recovery. Aspects of this care can vary from what you
Introduction This booklet will help you understand the St Mark s Hospital Enhanced Recovery Programme and how you will play an active part in your recovery. Aspects of this care can vary from what you
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Patient Information Leaflet. Treating Rectal Prolapse Delormes Operation
 Patient Information Leaflet Treating Rectal Prolapse Delormes Operation Treating Rectal Prolapse - Delormes operation What is a rectal prolapse? A rectal prolapse occurs when the normal supports of the
Patient Information Leaflet Treating Rectal Prolapse Delormes Operation Treating Rectal Prolapse - Delormes operation What is a rectal prolapse? A rectal prolapse occurs when the normal supports of the
Delormes Operation for Rectal Prolapse
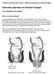 Delormes Operation for Rectal Prolapse Your Questions Answered What is a rectal prolapse? A rectal prolapse occurs when the normal supports of the rectum become weakened, allowing the muscle of the rectum
Delormes Operation for Rectal Prolapse Your Questions Answered What is a rectal prolapse? A rectal prolapse occurs when the normal supports of the rectum become weakened, allowing the muscle of the rectum
ABDOMINAL PERINEAL RESECTION
 ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Preparing for a Flexible Sigmoidoscopy
 The Ipswich Hospital NHS Trust Information for patients Preparing for a Flexible Sigmoidoscopy (an Examination of the Left Lower Part of Your Colon) Endoscopy Unit Tel: 01473 702352 DPS ref: 01086-18(RP)
The Ipswich Hospital NHS Trust Information for patients Preparing for a Flexible Sigmoidoscopy (an Examination of the Left Lower Part of Your Colon) Endoscopy Unit Tel: 01473 702352 DPS ref: 01086-18(RP)
Discharge Information following Bowel Surgery
 Discharge Information following Bowel Surgery Here is some information to help with your recovery at home and advice about returning to normal activities following bowel surgery. We hope this will be helpful
Discharge Information following Bowel Surgery Here is some information to help with your recovery at home and advice about returning to normal activities following bowel surgery. We hope this will be helpful
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients
 Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Diet advice for patients with a stoma
 Diet advice for patients with a stoma There are two different types of stoma; a colostomy or an ileostomy. A colostomy is a stoma that is formed from a part of the large bowel (colon). When undigested
Diet advice for patients with a stoma There are two different types of stoma; a colostomy or an ileostomy. A colostomy is a stoma that is formed from a part of the large bowel (colon). When undigested
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients
 Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
REVERSAL OF ILEOSTOMY. Patient information Leaflet
 REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
Delorme s Operation For Rectal Prolapse
 Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Delorme s Operation For Rectal Prolapse Patient Information Colorectal Surgery Author ID: NM Leaflet Number: Surg 045 Version: 3.1 Name of Leaflet: Delorme s Operation for Rectal Prolapse Date Produced:
Laparoscopic Cholecystectomy
 Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~
 Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter Bladder Urethra Small bowel An organ in the body that
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter Bladder Urethra Small bowel An organ in the body that
Adult barium enema. X-ray Department Ground Floor, St James Wing. What is a barium enema? Are there alternatives to Barium enema?
 Adult barium enema X-ray Department Ground Floor, St James Wing This information leaflet is for patients who are having a barium enema. It explains the procedure, how to prepare for it and what happens
Adult barium enema X-ray Department Ground Floor, St James Wing This information leaflet is for patients who are having a barium enema. It explains the procedure, how to prepare for it and what happens
Dietary advice for people with colostomies
 Dietary advice for people with colostomies Introduction During your surgery, you have had a colostomy formed. Colostomies are formed due to problems in the colon (large bowel). This leaflet is designed
Dietary advice for people with colostomies Introduction During your surgery, you have had a colostomy formed. Colostomies are formed due to problems in the colon (large bowel). This leaflet is designed
Laparoscopic Ventral Mesh Rectopexy
 Laparoscopic Ventral Mesh Rectopexy (LVMR) Information for patients General Surgery What is a LVMR? A laparoscopic ventral mesh rectopexy (LVMR) is an operation in which the rectum (last part of the bowel)
Laparoscopic Ventral Mesh Rectopexy (LVMR) Information for patients General Surgery What is a LVMR? A laparoscopic ventral mesh rectopexy (LVMR) is an operation in which the rectum (last part of the bowel)
Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients
 Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i The prostate The prostate is a small gland which is found only in men. It is situated at the base of the bladder
Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i The prostate The prostate is a small gland which is found only in men. It is situated at the base of the bladder
Subtotal and Total Gastrectomy
 DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
Reproduced with the kind permission of Health Press Ltd, Oxford
 Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
AN INFORMATION LEAFLET
 LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer.
 What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
After a kidney transplant
 The nursing staff will make sure that you are comfortable and will monitor the transplanted kidney to make sure it is working well. When you wake up you will notice that you will have a number of different
The nursing staff will make sure that you are comfortable and will monitor the transplanted kidney to make sure it is working well. When you wake up you will notice that you will have a number of different
Your anaesthetic for major surgery
 Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
ABDOMINAL PERINEAL RESECTION. Patient information Leaflet
 ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet
 Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
FACTSHEET F18 COPING WITH TIREDNESS
 COPING WITH TIREDNESS Many people with chest, heart and stroke conditions experience tiredness or fatigue. This factsheet explains some of the reasons why you might feel so tired. It also offers advice
COPING WITH TIREDNESS Many people with chest, heart and stroke conditions experience tiredness or fatigue. This factsheet explains some of the reasons why you might feel so tired. It also offers advice
Having an Anaesthetic Your Questions Answered
 PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
Enhanced Recovery After Surgery (ERAS) Diary
 Cardiac Surgery Enhanced Recovery After Surgery (ERAS) Diary Patient s Name: Options available If you d like a large print, audio, Braille or a translated version of this leaflet then please call: 01253
Cardiac Surgery Enhanced Recovery After Surgery (ERAS) Diary Patient s Name: Options available If you d like a large print, audio, Braille or a translated version of this leaflet then please call: 01253
Bowel Resection Surgery (Open Method)
 Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
ENHANCED RECOVERY CARE PROGRAMME FOR ABDOMINAL-BASED BREAST RECONSTRUCTIONS (MS-TRAM/DIEP)
 St Andrews Centre for Plastic Surgery ENHANCED RECOVERY CARE PROGRAMME FOR ABDOMINAL-BASED BREAST RECONSTRUCTIONS (MS-TRAM/DIEP) INTRODUCTION This leaflet aims to help you understand the Enhanced Recovery
St Andrews Centre for Plastic Surgery ENHANCED RECOVERY CARE PROGRAMME FOR ABDOMINAL-BASED BREAST RECONSTRUCTIONS (MS-TRAM/DIEP) INTRODUCTION This leaflet aims to help you understand the Enhanced Recovery
Pain relief after major surgery
 Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
CYSTOSCOPY PATIENT INFORMATION
 CYSTOSCOPY PATIENT INFORMATION ADHB Urology Department; Reviewed FEB 2005 Ubix code UPEB3 1 The information contained in this booklet is intended to assist you in understanding your proposed surgery; some
CYSTOSCOPY PATIENT INFORMATION ADHB Urology Department; Reviewed FEB 2005 Ubix code UPEB3 1 The information contained in this booklet is intended to assist you in understanding your proposed surgery; some
Transurethral Resection of Bladder Tumour (TURBT)
 Transurethral Resection of Bladder Tumour (TURBT) What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content
Transurethral Resection of Bladder Tumour (TURBT) What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content
Dietary. Ostomists. Advice. National: Scotland:
 Ostomists Dietary Advice www.fittleworth.com DTRY315-1 Opening Hours: 8 am to 8 pm Monday to Friday 9 am to 1 pm Saturday National: 0800 378 846 Scotland: 0800 783 7148 Dietary Advice for Ostomists Giving
Ostomists Dietary Advice www.fittleworth.com DTRY315-1 Opening Hours: 8 am to 8 pm Monday to Friday 9 am to 1 pm Saturday National: 0800 378 846 Scotland: 0800 783 7148 Dietary Advice for Ostomists Giving
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation
 Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Spinal Anaesthesia and Analgesia. Patient information Leaflet
 Spinal Anaesthesia and Analgesia Patient information Leaflet February 2018 Introduction For many operations, patients receive a general anaesthetic and remain asleep during the operation. A spinal anaesthetic
Spinal Anaesthesia and Analgesia Patient information Leaflet February 2018 Introduction For many operations, patients receive a general anaesthetic and remain asleep during the operation. A spinal anaesthetic
Department of Gynaecology Services Whiston Hospital, Warrington Road, Prescot L35 5DR Sacrocolpopexy
 Patient information leaflet Department of Gynaecology Services Whiston Hospital, Warrington Road, Prescot L35 5DR 0151 426 1600 Sacrocolpopexy What is a Sacrocolpopexy? A sacrocolpopexy is a procedure
Patient information leaflet Department of Gynaecology Services Whiston Hospital, Warrington Road, Prescot L35 5DR 0151 426 1600 Sacrocolpopexy What is a Sacrocolpopexy? A sacrocolpopexy is a procedure
Dietary advice when you have an Ileostomy
 Dietary advice when you have an Ileostomy Information for patients Name Your Dietitian Dietitian contact number: 0118 322 7116 What is an Ileostomy? An Ileostomy is a surgical procedure that brings out
Dietary advice when you have an Ileostomy Information for patients Name Your Dietitian Dietitian contact number: 0118 322 7116 What is an Ileostomy? An Ileostomy is a surgical procedure that brings out
Eating Well After Gastro-intestinal Surgery
 Lady Sobell Gastrointestinal Unit Wexham Park Hospital Introduction Eating Well After Gastro-intestinal Surgery This leaflet contains general information to help you with eating after surgery. If you need
Lady Sobell Gastrointestinal Unit Wexham Park Hospital Introduction Eating Well After Gastro-intestinal Surgery This leaflet contains general information to help you with eating after surgery. If you need
Your visit to theatre
 Your visit to theatre Information for you about your anaesthetic and your visit to the operating theatre This leaflet provides information about coming into hospital for your operation It explains anaesthetic
Your visit to theatre Information for you about your anaesthetic and your visit to the operating theatre This leaflet provides information about coming into hospital for your operation It explains anaesthetic
In-patient brachytherapy for gynaecological cancer. Cancer Services Information for patients
 In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
Having an operation on the pancreas
 Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Having a ureteric stent inserted
 Having a ureteric stent inserted This leaflet explains more about having a ureteric stent inserted. It describes the benefits, risks, alternatives and what you can expect when you come to hospital. If
Having a ureteric stent inserted This leaflet explains more about having a ureteric stent inserted. It describes the benefits, risks, alternatives and what you can expect when you come to hospital. If
Preparing for your colonscopy or sigmoidoscopy (afternoon appointment)
 These are instructions telling you how to take Klean Prep. What is Klean Prep? Klean Prep is a strong laxative that you need to take before your colonoscopy or sigmoidoscopy. Klean Prep will give you diarrhoea
These are instructions telling you how to take Klean Prep. What is Klean Prep? Klean Prep is a strong laxative that you need to take before your colonoscopy or sigmoidoscopy. Klean Prep will give you diarrhoea
Dietary advice when you have a colostomy
 Dietary advice when you have a colostomy Information for patients Name Your Dietitian Dietitian contact number: 0118 322 7116 What is a colostomy? A colostomy is a surgical procedure that brings out the
Dietary advice when you have a colostomy Information for patients Name Your Dietitian Dietitian contact number: 0118 322 7116 What is a colostomy? A colostomy is a surgical procedure that brings out the
Laser Trans Urethral Resection of Prostate (TURP)
 Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Maternity Information Leaflet
 Maternity Information Leaflet Recovery following your Caesarean Section This leaflet provides information to help you recover following a Caesarean Section (CS) birth. Recovery after a CS may take a little
Maternity Information Leaflet Recovery following your Caesarean Section This leaflet provides information to help you recover following a Caesarean Section (CS) birth. Recovery after a CS may take a little
LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION
 LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION WHAT IS LUMBAR DECOMPRESSION / DISCECTOMY SURGERY? During lumbar decompression/ discectomy back surgery, a small portion of the bone over the nerve
LUMBAR DECOMPRESSION / DISCECTOMY SURGERY INFORMATION WHAT IS LUMBAR DECOMPRESSION / DISCECTOMY SURGERY? During lumbar decompression/ discectomy back surgery, a small portion of the bone over the nerve
TURP - TransUrethral Resection of the Prostate
 TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
Patient Information. A guide to your anaesthetic
 Patient Information A guide to your anaesthetic This booklet has been produced to answer your questions and to help ease your mind about the anaesthetic you are to have. Contents Page 1. What is anaesthesia?
Patient Information A guide to your anaesthetic This booklet has been produced to answer your questions and to help ease your mind about the anaesthetic you are to have. Contents Page 1. What is anaesthesia?
Abdomino Perineal Excision of Rectum (APER)
 PATIENT INFORMATION Abdomino Perineal Excision of Rectum (APER) Introduction/Procedure This leaflet tells you about the procedure known as abdomino perineal excision/resection (APER) of the rectum. What
PATIENT INFORMATION Abdomino Perineal Excision of Rectum (APER) Introduction/Procedure This leaflet tells you about the procedure known as abdomino perineal excision/resection (APER) of the rectum. What
This leaflet provides information for patients due to have an operation or procedure with general anaesthetic and/or sedation.
 Page 1 of 5 Your anaesthetic Introduction This leaflet provides information for patients due to have an operation or procedure with general anaesthetic and/or sedation. Who is an anaesthetist? Anaesthetists
Page 1 of 5 Your anaesthetic Introduction This leaflet provides information for patients due to have an operation or procedure with general anaesthetic and/or sedation. Who is an anaesthetist? Anaesthetists
UROLOGY SYDNEY Level 1, St George Medical Centre 1 South Street Kogarah NSW 2217 Ph: Fax:
 Pre Operative care: Preop investigations: Radical Prostatectomy Pre and Post Operative Care Once your surgery date has been decided you will be sent for routine blood and urine tests, an ECG will also
Pre Operative care: Preop investigations: Radical Prostatectomy Pre and Post Operative Care Once your surgery date has been decided you will be sent for routine blood and urine tests, an ECG will also
Managing your pain at home after surgery. Information for patients
 Managing your pain at home after surgery Information for patients Managing your pain at home after surgery This leaflet has been written in order to give you some advice regarding your pain management
Managing your pain at home after surgery Information for patients Managing your pain at home after surgery This leaflet has been written in order to give you some advice regarding your pain management
Esophagectomy Surgery
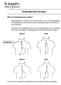 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Trans urethral resection of prostate (TURP)
 Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
Trans urethral resection of prostate (TURP) Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST What is the prostate? Only men have a prostate
Preparing For Colonoscopy
 Preparing For Colonoscopy COLONOSCOPY OVERVIEW A colonoscopy is an exam of the lower part of the gastrointestinal tract, which is called the colon or large intestine (bowel). Colonoscopy is a safe procedure
Preparing For Colonoscopy COLONOSCOPY OVERVIEW A colonoscopy is an exam of the lower part of the gastrointestinal tract, which is called the colon or large intestine (bowel). Colonoscopy is a safe procedure
16 Colostomy. The function of the large bowel (colon) is to absorb water and salts from our food during the process of digestion.
 16 Colostomy Eating and drinking with a colostomy The function of the large bowel (colon) is to absorb water and salts from our food during the process of digestion. If you have an end colostomy then the
16 Colostomy Eating and drinking with a colostomy The function of the large bowel (colon) is to absorb water and salts from our food during the process of digestion. If you have an end colostomy then the
How to Prepare for your. Colonoscopy using. Bowel Preparation. Type 2 Oral Medication. Diabetes Management YOUR QUESTIONS ANSWERED
 How to Prepare for your Colonoscopy using Bowel Preparation Type 2 Oral Medication Diabetes Management YOUR QUESTIONS ANSWERED Page 1 of 12 Page 2 of 12 Contents Introduction Page 4 What is the bowel preparation?
How to Prepare for your Colonoscopy using Bowel Preparation Type 2 Oral Medication Diabetes Management YOUR QUESTIONS ANSWERED Page 1 of 12 Page 2 of 12 Contents Introduction Page 4 What is the bowel preparation?
Leg artery bypass (fem-pop bypass)
 Leg artery bypass (fem-pop bypass) The femoral artery runs down from the groin and into the thigh. This artery delivers blood to your legs. When the femoral artery reaches the back of the knee it becomes
Leg artery bypass (fem-pop bypass) The femoral artery runs down from the groin and into the thigh. This artery delivers blood to your legs. When the femoral artery reaches the back of the knee it becomes
HARTMANNS PROCEDURE. Patient information Leaflet
 HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
Laparotomy for large retroperitoneal mass:
 Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
This operation is necessary to remove the area of bowel that is diseased.
 PATIENT INFORMATION Sigmoid Colectomy Introduction / Procedure This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of the common complications
PATIENT INFORMATION Sigmoid Colectomy Introduction / Procedure This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of the common complications
Managing Pain and Sickness after Surgery
 Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
Laparoscopic Ventral Mesh Rectopexy
 Patient Information Laparoscopic Ventral Mesh Rectopexy Introduction We expect you to make a rapid recovery after your operation and to experience no serious problems. However, it is important that you
Patient Information Laparoscopic Ventral Mesh Rectopexy Introduction We expect you to make a rapid recovery after your operation and to experience no serious problems. However, it is important that you
Afternoon Appointment - GASTROSCOPY AND COLONOSCOPY
 Endoscopy Unit MOVIPREP Afternoon Appointment - GASTROSCOPY AND COLONOSCOPY Information for patients Please follow these instructions and NOT the instructions in the box of bowel prep medication that you
Endoscopy Unit MOVIPREP Afternoon Appointment - GASTROSCOPY AND COLONOSCOPY Information for patients Please follow these instructions and NOT the instructions in the box of bowel prep medication that you
Wound care Keep your wound clean and dry. You do not need to have a dressing over it unless you are told otherwise by your hospital staff.
 After thoracic or lumbar spinal surgery We ve given you this factsheet because you have recently had thoracic or lumbar spinal surgery at Wessex Spinal Unit. It contains useful information and advice that
After thoracic or lumbar spinal surgery We ve given you this factsheet because you have recently had thoracic or lumbar spinal surgery at Wessex Spinal Unit. It contains useful information and advice that
Recovery at home following open abdominal aortic aneurysm repair Vascular Surgery Patient Information Leaflet
 Recovery at home following open abdominal aortic aneurysm repair Vascular Surgery Patient Information Leaflet Surgeons, anaesthetists, radiologists and nurses from Russells Hall Hospital in Dudley, New
Recovery at home following open abdominal aortic aneurysm repair Vascular Surgery Patient Information Leaflet Surgeons, anaesthetists, radiologists and nurses from Russells Hall Hospital in Dudley, New
Recovery from open surgery for abdominal aortic aneurysm repair
 Recovery from open surgery for abdominal aortic aneurysm repair Information for patients and carers from the East Kent Vascular Unit After open surgery to repair your abdominal aortic aneurysm (AAA) it
Recovery from open surgery for abdominal aortic aneurysm repair Information for patients and carers from the East Kent Vascular Unit After open surgery to repair your abdominal aortic aneurysm (AAA) it
Mr Sanjeev Sarin MS FRCS. Aortic Aneurysms Patient Information Sheet
 Aortic Aneurysms Patient Information Sheet The aim of this information sheet is to ensure that you understand the nature of the treatment you wish to undertake. Please read it carefully and discuss any
Aortic Aneurysms Patient Information Sheet The aim of this information sheet is to ensure that you understand the nature of the treatment you wish to undertake. Please read it carefully and discuss any
Bladder neck incision
 Bladder neck incision What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content may apply to you. Feel free
Bladder neck incision What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content may apply to you. Feel free
Royal College of Obstetricians and Gynaecologists. Information for you after a laparoscopy
 Royal College of Obstetricians and Gynaecologists Information for you after a laparoscopy Who is this information for? This information is for you if you are about to have, or you are recovering from,
Royal College of Obstetricians and Gynaecologists Information for you after a laparoscopy Who is this information for? This information is for you if you are about to have, or you are recovering from,
Nephrectomy. What you need to know
 Nephrectomy What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to you. Feel free to discuss
Nephrectomy What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to you. Feel free to discuss
Anaesthesia and pain (Daycase Patient) Patient information Leaflet
 Anaesthesia and pain (Daycase Patient) Patient information Leaflet February 2018 INTRODUCTION Welcome to Tameside Hospital, this leaflet gives basic information to help you prepare for your anaesthetic,
Anaesthesia and pain (Daycase Patient) Patient information Leaflet February 2018 INTRODUCTION Welcome to Tameside Hospital, this leaflet gives basic information to help you prepare for your anaesthetic,
Enhanced Recovery Patient Diary
 Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
Summary of Important Points Please note that the time given to you is your arrival time and not the time of your procedure. The time taken to perform
 Summary of Important Points Please note that the time given to you is your arrival time and not the time of your procedure. The time taken to perform endoscopy procedures vary and emergency patients sometimes
Summary of Important Points Please note that the time given to you is your arrival time and not the time of your procedure. The time taken to perform endoscopy procedures vary and emergency patients sometimes
Burch Colposuspension
 Burch Colposuspension Department of Gynaecology Patient Information What is is botulinum Burch colposuspension? toxin A? The operation is intended to support the bladder neck, which is the area between
Burch Colposuspension Department of Gynaecology Patient Information What is is botulinum Burch colposuspension? toxin A? The operation is intended to support the bladder neck, which is the area between
Patient information. Information for Patients Undergoing Lumbar Disc Surgery. Trauma and Orthopaedic Directorate PIF 1359/V3
 Patient information Information for Patients Undergoing Lumbar Disc Surgery Trauma and Orthopaedic Directorate PIF 1359/V3 Your Consultant / Doctor has advised you to have a Lumbar Microdiscectomy. What
Patient information Information for Patients Undergoing Lumbar Disc Surgery Trauma and Orthopaedic Directorate PIF 1359/V3 Your Consultant / Doctor has advised you to have a Lumbar Microdiscectomy. What
Lumbar Decompression GUIDELINES FOR PATIENTS HAVING A. Lumbar Decompression
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
What Should I Eat to Help my Pressure Sore or Wound Heal?
 What Should I Eat to Help my Pressure Sore or Wound Heal? Information for Patients i UHL Nutrition and Dietetic Service UHL Tissue Viability Team Introduction If you have a pressure sore or a large wound
What Should I Eat to Help my Pressure Sore or Wound Heal? Information for Patients i UHL Nutrition and Dietetic Service UHL Tissue Viability Team Introduction If you have a pressure sore or a large wound
Keck School of Medicine of USC
 To: Patients undergoing colorectal surgery From: Kyle Cologne, MD Welcome to USC! I m glad you have chosen us here at USC for your surgical care. I understand this can be a very difficult time filled with
To: Patients undergoing colorectal surgery From: Kyle Cologne, MD Welcome to USC! I m glad you have chosen us here at USC for your surgical care. I understand this can be a very difficult time filled with
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
Urology Department Percutaneous Nephrolithotomy (PCNL)
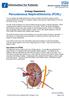 Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
Preparing For Colonoscopy
 Preparing For Colonoscopy COLONOSCOPY OVERVIEW A colonoscopy is an exam of the lower part of the gastrointestinal tract, which is called the colon or large intestine (bowel). Colonoscopy is a safe procedure
Preparing For Colonoscopy COLONOSCOPY OVERVIEW A colonoscopy is an exam of the lower part of the gastrointestinal tract, which is called the colon or large intestine (bowel). Colonoscopy is a safe procedure
Hydrocele repair. Information for parents and carers
 Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
Colposuspension operation
 Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Colposuspension operation This information explains: Overview... 1 Your admission date... 1 The operation... 2 The anaesthetic... 2 After the operation... 3 Problems... 3 Going home... 4 Getting back to
Antigrade Colonic Enema (ACE) Information for patients Spinal Injuries
 Antigrade Colonic Enema (ACE) Information for patients Spinal Injuries page 2 of 8 This leaflet has been produced in support of the explanation and counselling provided by your urologist and nurse specialist.
Antigrade Colonic Enema (ACE) Information for patients Spinal Injuries page 2 of 8 This leaflet has been produced in support of the explanation and counselling provided by your urologist and nurse specialist.
Femoropopliteal/distal. bypass grafts. Vascular Surgery Patient Information Leaflet
 Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients
 Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
