Intrauterine devices (IUDs) are long-acting reversible
|
|
|
- Justin Reeves
- 5 years ago
- Views:
Transcription
1 Contraception: Original Research Paracervical Block for Intrauterine Device Placement Among Nulliparous Women A Randomized Controlled Trial Sheila K. Mody, MD, MPH, John Paul Farala, MD, Berenice Jimenez, MD, Moena Nishikawa, and Lynn L. Ngo, MD, MPH OBJECTIVE: To investigate whether a 20-mL buffered 1% lidocaine paracervical block decreases pain during intrauterine device (IUD) placement. METHODS: In a randomized, single-blind, placebo-controlled trial, women were assigned to receive either a 20-mL buffered 1% lidocaine paracervical block or no block before IUD placement. The primary outcome was pain with IUD placement measured on a 100-mm visual analog scale. Our sample size had 80% power (a50.05) to detect a 20-mm difference in visual analog scale scores with a SD of 28 mm. Secondary outcomes included pain with speculum placement, paracervical block administration, tenaculum placement, 5 minutes postprocedure, and overall pain perception. RESULTS: From October 7, 2014, through October 26, 2017, 64 women were enrolled and analyzed (33 in the paracervical block arm, 31 in the no-block arm). There were no differences in baseline demographics between the groups. Women who received the paracervical block From the Division of Family Planning, Department of Obstetrics, Gynecology, and Reproductive Sciences, University of California, and Southern California Permanente Medical Group, San Diego, California. Dr. Mody was partially funded by National Institutes of Health grant K12 HD The authors thank the clinic staff at University of California, San Diego and Planned Parenthood of the Pacific Southwest for collaborating on this study. Each author has indicated that he or she has met the journal s requirements for authorship. Received March 26, Received in revised form May 18, Accepted June 7, Corresponding author: Sheila K. Mody, MD, MPH, Division of Family Planning, Department of Obstetrics, Gynecology, and Reproductive Sciences, University of California, San Diego, 9300 Campus Point Drive, MC 743, La Jolla, CA 92037; smody@ucsd.edu. Financial Disclosure The authors did not report any potential conflicts of interest by the and Gynecologists. Published by Wolters Kluwer Health, Inc. All rights reserved. ISSN: /18 reported less pain with IUD placement compared with women who received no block (median visual analog scale score of 33 mm vs 54 mm, P5.002). Pain was significantly less in the intervention group for uterine sounding (30 mm vs 47 mm, P5.005), 5 minutes after placement (12 mm vs 27 mm, P5.005), and overall pain perception (30 mm vs 51 mm, P5.015). Participants who received the paracervical block experienced more pain with block administration compared with placebo (30 mm vs 8 mm, P5.003). There was no perceived pain difference for speculum insertion (10 mm vs 6 mm, P5.447) or tenaculum placement (15 mm vs 10 mm, P5.268). CONCLUSION: A 20-mL buffered 1% lidocaine paracervical block decreases pain with IUD placement (primary outcome), uterine sounding (secondary outcome), and 5 minutes after placement (secondary outcome). Although paracervical block administration can be painful, perception of pain for overall IUD placement procedure is lower compared with no block. CLINICAL TRIAL REGISTRATION: ClinicalTrials.gov, NCT (Obstet Gynecol 2018;132:575 82) DOI: /AOG Intrauterine devices (IUDs) are long-acting reversible contraceptives with a failure rate less than 1%. 1 Although IUD use is increasing, it is still less commonly used compared with less effective methods including pills and condoms. 2,3 Although IUD placement is an office procedure, fear of pain can be a barrier. This is especially a concern for nulliparous women, who experience more pain with placement compared with multiparous women. 4,5 Currently, there is no standard of care for pain management with IUD placement among adult nulliparous women. The majority of randomized controlled trials of oral and local anesthetics have not demonstrated a reduction in pain scores with IUD VOL. 132, NO. 3, SEPTEMBER 2018 OBSTETRICS & GYNECOLOGY 575
2 placement If effective, use of a local anesthetic during the IUD placement would be convenient because it would not interrupt clinic flow. Health care providers often suggest a paracervical block with IUD placement among nulliparous women. A previous trial evaluating a 10-mL 1% lidocaine block did not demonstrate a decrease in pain with IUD placement. 4 However, the 10-mL block may not have been a sufficient dose, because studies for other types of gynecologic procedures have shown efficacy of a 20- ml block. 16,17 A trial using a 10-mL 1% lidocaine block demonstrated a decrease in pain with IUD placement among nulliparous adolescents and young women (14 25 years old) receiving the levonorgestrel 13.5-mg IUD. 18 The levonorgestrel 52-mg and copper IUDs have slightly larger applicators, so it is difficult to extrapolate these results. This study evaluates whether a 20-mL buffered 1% lidocaine paracervical block will decrease pain with IUD placement. MATERIALS AND METHODS Approval was obtained from the institutional review board at University of California, San Diego. Nulliparous women years of age presenting for an IUD placement for contraception or treatment of abnormal uterine bleeding were approached to participate in this study. Exclusion criteria included pregnancy, any diagnosed chronic pain issues (fibromyalgia, endometriosis, dysmenorrhea, irritable bowel syndrome, interstitial cystitis), use of pain medication (eg, aspirin, nonsteroidal antiinflammatory drugs) within 6 hours of enrollment, misoprostol administration within 24 hours of enrollment, history of prior IUD placement, or known contraindications to IUD placement. Written informed consent was obtained. Each participant was randomly assigned to receive either a 20-mL buffered 1% lidocaine paracervical block or no paracervical block. We chose this buffered lidocaine because the sodium bicarbonate decreases the burning sensation associated with lidocaine administration. 19 We did not add vasopressin or epinephrine because IUD placements typically involve minimal risk for bleeding. Also, not including vasopressin or epinephrine makes the results more generalizable to clinics where these agents may not be available. Randomization was performed using a block size of four with group assignment through sequentially numbered, opaque, sealed envelopes. Given our smaller sample size, we chose a block size of four to ensure an equal distribution of participants who received the paracervical block and who did not receive the paracervical block. This study was singleblinded to the participants. After group allocation, the clinician was informed to administer either the paracervical block or no paracervical block (a capped needle). For the intervention group, we administered a 20- ml paracervical block that consisted of 18 ml of 1% lidocaine buffered with 2 ml 8.4% sodium bicarbonate. This block is most commonly reported in the literature After speculum insertion, 2 ml was injected at the tenaculum site superficially at 12 o clock on the anterior lip of the cervix. 23,24 The tenaculum was placed at 12 o clock. The remaining 18 ml was injected into the vaginal fornices equally at the 4 and 8 o clock positions. The injection was continuous from superficial to deep (3 cm) to superficial (injecting with insertion and withdrawal). 21,22,25,26 In the nonintervention group, the clinician performed a sham paracervical block as follows: 2 ml of buffered lidocaine was injected at the tenaculum site superficially at 12 o clock on the anterior lip of the cervix followed by tenaculum placement. Over 60 seconds, without moving the tenaculum, a capped needle gently touched the vaginal sidewall at the level of the external os at 4 and 8 o clock. All participants were counseled during the no block or paracervical block and tenaculum placement using standardized language, for example, You may or may not feel something to promote blinding. Placement of the IUD took place after application of the paracervical block or no block. The performing clinicians were obstetrics and gynecology attending physicians, resident physicians, and advance practice clinicians. We chose not to include a saline placebo block because the saline can distend the paracervical nerves and cause relief; therefore, it is not a true placebo. The capped needle approach is the same approach used by other paracervical studies. 4,16,17 The outcome of interest was the participant s pain on a visual analog scale (VAS) from 0 mm (no pain) to 100 mm (worst pain imaginable) at various steps during the IUD placement. Participants marked the VAS scale for anticipated and baseline pain, pain during speculum insertion, sham or paracervical block administration, tenaculum placement, uterine sounding, IUD placement, 5 minutes after placement, and overall pain. Visual analog scale scores for anticipated and baseline pain were obtained just before the start of the procedure. Visual analog scale scores for speculum insertion, sham or paracervical administration, tenaculum placement, sounding, and IUD placement were obtained immediately after that step of the procedure. Participation concluded with a survey that included questions asking overall satisfaction with IUD placement and whether they would recommend IUD placement to a friend using the same pain 576 Mody et al Paracervical Block for IUD Placement OBSTETRICS & GYNECOLOGY
3 control (Box 1). This survey was used in prior pain control for IUD placement studies. 4,14 Participants were offered acetaminophen or ibuprofen at 5 minutes after the procedure. Participants received a $10 gift card for participating. The calculation of the sample size was based on previous studies involving pain control for IUD placement using a 100-mm VAS. 4,5,15 The SD for pain with IUD placement was mm in previous studies in the United States. 4,12 Our sample size calculation used a SD of 28 mm. Prior studies have reported a range of 9 20 mm as clinically significant differences in VAS pain scores. We defined a 20-mm difference on the VAS as clinically significant. We chose the 20-mm difference to demonstrate a large enough difference to change clinical practice. Using these parameters, we calculated that 64 participants Box 1. Postintrauterine Device Insertion Patient Survey 1. Did you experience any of the following side effects from the paracervical block? (circle all that apply) a. Nausea b. Vomiting c. Dizziness d. Injection site pain? Please describe: 2. How would you describe the injection site pain? a. No injection pain b. Not as bad as the IUD placement c. Just as bad as the IUD placement d. Worse than the IUD placement e. Much worse than the IUD placement 3. How did the pain with IUD insertion compare with the expected pain? a. No pain with IUD insertion b. Not as bad as the expected pain c. Just as bad as the expected pain d. Worse than the expected pain e. Much worse than the expected pain 4. Are there are some things about the pain control you received that could be better? a. Yes b. No c. Not sure 5. Would you choose the same pain control method for a future IUD insertion? a. Yes b. No c. Not sure 6. Would you recommend this pain control method to a friend for IUD insertion? a. Yes b. No c. Not sure IUD, intrauterine device. would be required to achieve 80% power with a type I error (a) rate of 5% to detect this difference. 27 We planned recruitment of 67 participants to account for a 5% dropout rate. Data were analyzed with an intention-to-treat analysis. Visual analog scale pain scores were tested for normality using the Shapiro-Wilk test. The majority of VAS scores had a nonnormal distribution; therefore, median pain scores were compared using the Wilcoxon rank-sum test. For demographics and questionnaires, x 2 or Fisher exact tests were used to compare categorical variables and the t test or Wilcoxon rank-sum tests were used to compare continuous variables. Statistical analyses were completed using SAS 9.4. RESULTS Recruitment occurred from October 2014 to October 2017 at the University of California, San Diego and Planned Parenthood of the Pacific Southwest. A total of 67 women were enrolled and 64 of those women completed the study. Three participants dropped out of the study because they were unable to tolerate the pelvic examination and did not want to proceed with IUD placement (Fig. 1). There was no difference in baseline demographics including age, race or ethnicity, body mass index, or level of education between the two groups. There were six women in the paracervical block group and one in the no paracervical block group with prior abortions that were specified as terminations. None of the participants had more than one prior pregnancy. We do not have information on the type of termination (medical or surgical) or the trimester. No participants reported prior cervical procedures such as conization (Table 1). For the primary outcome of VAS score for IUD placement, the median pain score was less for the paracervical block group compared with the no paracervical block group (33 mm vs 54 mm, P5.002). Median pain scores were also less for the secondary outcomes of uterine sounding (30 mm vs 47 mm, P5.005), 5 minutes after IUD placement (12 mm vs 27 mm, P5.005), and overall pain perception for the procedure (30 mm vs 51 mm, P,.05). Pain with paracervical block administration was higher for the intervention group compared with the no paracervical block group (30 mm vs 8 mm, P5.003). There was no difference in baseline pain, anticipated pain, or pain with speculum or tenaculum placement (Table 2). There was no difference in patient-reported adverse effects. Participants in the no paracervical block group more often reported that IUD placement VOL. 132, NO. 3, SEPTEMBER 2018 Mody et al Paracervical Block for IUD Placement 577
4 Table 1. Demographics of Study Participants Demographic No Paracervical Block (n531) Paracervical Block (n533) P Age (y) * BMI (kg/m 2 ) * Ethnicity.556 Non-Hispanic 23 (74.2) 26 (81.3) Hispanic 8 (25.8) 6 (18.8) Race.289 Caucasian 20 (64.5) 21 (67.7) Black or African American 0 (0) 2 (6.5) Asian or Pacific Islander 5 (16.1) 6 (19.4) Native American or Alaska Native 0 (0) 0 (0) Other or multiracial 6 (19.4) 2 (6.5) Highest level of education completed.939 High school graduate 0 (0) 0 (0) Some college 7 (22.6) 7 (21.1) College degree 18 (58.1) 21 (63.6) Graduate degree 6 (19.4) 5 (15.2) Prior abortion History of LEEP or conization BMI, body mass index; LEEP, loop electrosurgical excision procedure. Data are mean6sd or n (%) unless otherwise specified. Percent totals may not add up to 100 because of rounding. * P value obtained from a t test. P value obtained from a Fisher exact test. pain was worse than expected pain (1.6% vs 14.1% for the paracervical vs no paracervical block group), whereas participants in the paracervical group more often reported no pain (10.9% vs 1.6%) or pain not as bad as expected (29.7% vs 18.8%) compared with the no paracervical block group (Table 3). There was no difference in the health care provider type, type of IUD inserted, purpose of IUD placement, uterine position, need for cervical dilation, or major complications reported by health care providers. There was also no difference in participants taking postprocedural ibuprofen or acetaminophen before leaving the office (Table 4). Of note, we were not powered to detect differences in these outcomes. Fig. 1. Patient flow chart. IUD, intrauterine device. Mody. Paracervical Block for IUD Placement. Obstet Gynecol Mody et al Paracervical Block for IUD Placement OBSTETRICS & GYNECOLOGY
5 Table 2. Median Pain Scores for All Time Points All Participants No Paracervical Block (mm) (n531) Paracervical Block (mm) (n533) Difference in Pain Scores P* Anticipated pain 51 (30 70) 58 (48 68) Baseline pain 0 (0 2) 0 (0 2) Speculum insertion 6 (2 20) 10 (4 14) Capped needle or PCB 8 (2 20) 30 (17 47) +22,.001 Tenaculum placement 10 (4 19) 15 (6 24) Uterine sounding 47 (24 65) 30 (8 43) IUD placement 54 (33 75) 33 (10 56) min after IUD 27 (15 50) 12 (6 27) placement Overall pain 51 (21 65) 30 (16 48) PCB, paracervical block; IUD, intrauterine device. Data are median (interquartile range [25 75%]). Pain scores reported in millimeters on a mm visual analog scale. * P value obtained from a Wilcoxon rank-sum test. Primary outcome; all others are secondary outcomes. DISCUSSION This study demonstrates that lidocaine administered locally through a paracervical block decreases pain with placement of the most commonly used IUDs, levonorgestrel 52 mg (Mirena) and CuT380A. The study by Akers et al 18 showed a decrease in pain with a 10 ml 1% lidocaine block, but had used the smaller levonorgestrel 13.5-mg IUD with adolescent and young adult Table 3. Results of the Participant Survey Completed 5 Minutes After Intrauterine Device Placement No Paracervical Block (n531) Paracervical Block (n533) P* Side effects Nausea 4 (6.3) 3 (4.7).625 Vomiting 0 (0) 0 (0) Dizziness 8 (12.5) 10 (15.6).689 Injection site pain 11 (17.2) 19 (29.7).077 Injection site pain.128 None 10 (32.3) 9 (27.3) Not as bad as the IUD placement 16 (51.6) 12 (36.4) Just as bad as the IUD placement 4 (12.9) 3 (9.1) Worse than the IUD placement 1 (3.2) 8 (24.2) Much worse than the IUD placement 0 (0) 1 (3.0) Pain with IUD placement vs expected pain.002 No pain with IUD placement 1 (3.2) 7 (21.2) Not as bad as expected pain 12 (38.7) 19 (57.6) Just as bad as expected pain 5 (16.1) 6 (18.2) Worse than expected pain 9 (29.0) 1 (3.0) Much worse than expected pain 4 (12.9) 0 (0) Choose the same pain control method for.479 a future IUD Yes 15 (48.4) 20 (60.6) No 7 (22.6) 4 (12.1) Not sure 9 (29.0) 9 (27.3) Recommend this pain control method to.078 a friend for IUD placement Yes 16 (51.6) 25 (78.1) No 6 (19.4) 2 (6.3) Not sure 9 (29.0) 5 (15.6) IUD, intrauterine device. Data are n (%) unless otherwise specified. Percent totals may not add up to 100 because of rounding. * P values are derived from the x 2 test. VOL. 132, NO. 3, SEPTEMBER 2018 Mody et al Paracervical Block for IUD Placement 579
6 Table 4. Results of the Health Care Provider Survey Completed After Completion of Intrauterine Device Placement No Paracervical Block (n531) Paracervical Block (n533) P* Clinician type.557 Resident 2 (6.5) 3 (9.1) Attending at UCSD 21 (67.7) 18 (54.6) Nurse practitioner at PPPSW 8 (25.8) 12 (36.4) IUD type.447 LNG 52 mg (Mirena) 24 (77.4) 21 (63.6) CuT380A (Paragard) 6 (19.4) 11 (33.3) LNG 13.5 mg (Skyla) 1 (3.2) 1 (3.0) Purpose of IUD Contraception 31 (100) 33 (100) Abnormal uterine bleeding 0 (0) 0 (0) Position of the uterus.205 Anteverted 24 (77.4) 20 (60.6) Retroverted 2 (6.5) 7 (21.2) Midpositioned 5 (16.1) 6 (18.2) Need for cervical dilation.108 No 25 (80.7) 31 (93.9) Yes 6 (19.4) 2 (6.1) Unable to complete IUD placement No 31 (100) 33 (100) Yes 0 (0) 0 (0) Significant bleeding (greater than 5 min).329 No 31 (100) 32 (96.7) Yes 0 (0) 1 (3.0) Major complications No 31 (100) 33 (100) Yes 0 (0) 0 (0) Ibuprofen or acetaminophen before leaving the office.068 No 19 (61.3) 27 (81.8) Yes 12 (38.7) 6 (18.2) UCSD, University of California, San Diego; PPPSW, Planned Parenthood of the Pacific Southwest; IUD, intrauterine device; LNG, levonorgestrel. Data are n (%) unless otherwise specified. Percent totals may not add up to 100 because of rounding. * P values were derived from the x 2 test. participants who were years old. A phase II trial of lower-dose levonorgestrel IUDs demonstrated less pain associated with insertion of these smaller framed IUDs compared with the levonorgestrel 52-mg IUD. 28 Our study includes nulliparous women years old receiving mostly the larger framed levonorgestrel 52-mg and CuT380A IUDs, which are the most commonly used IUDs in the United States. Most of the IUDs included in our study provide the longer duration of use compared with the smaller, lower dose IUDs. In addition, the levonorgestrel 52-mg IUD provides the highest likelihood of amenorrhea compared with the lower dose levonorgestrel IUDs. Our sample size is powered to detect a 20-mm difference in VAS pain scores, which is consistent in being a clinically significant difference. This study provides more information for counseling about using a lidocaine paracervical block and counseling nulliparous patients about pain and IUD placement. For example, the patient may be informed during counseling that the paracervical block typically does cause some pain (30 mm on a 100-mm scale), but that the paracervical block reduces pain with IUD placement, pain 5 minutes after the procedure, and perceived pain for the overall procedure. Limitations of this study include the lack of diversity in age, race, and education level. The study had an underrepresentation of African American participants compared with the national population, although representative of local demographics. Participants also tended to have higher education levels and were younger compared with the population of nationwide IUD recipients. These factors may limit the generalizability of the results. We also acknowledge that adding sodium bicarbonate may add a level of complexity to incorporating the results of this study into 580 Mody et al Paracervical Block for IUD Placement OBSTETRICS & GYNECOLOGY
7 clinics that do not typically buffer the lidocaine. Another weakness of the study is that it did not include the newer levonorgestrel 52-mg IUD (Liletta) that is now widely used. Although the levonorgestrel 52-mg IUD was introduced nationally during the study period, it was not routinely offered at the study institutions during the recruitment period. Recruitment for this study took 3 years. A major challenge in recruitment was the exclusion criteria of ibuprofen and other pain medication use before IUD placement. Although the literature does not support ibuprofen as effective analgesia for IUD placement, this study excluded women who used ibuprofen within 6 hours of study enrollment to eliminate any possible confounding effect of pain medications. However, because women are often told to take ibuprofen by nurses or friends, this screened out many potential participants from the study. Major strengths of this study include that it is a randomized controlled trial, use of the VAS, and use of a paracervical block technique comparable with other IUD placement pain studies. This allows better comparison with other studies evaluating pain studies with IUD placement. We included both an academic site and the Planned Parenthood site to increase diversity of the participants. We also included a variety of clinician types including advance practice clinicians, residents, and obstetrics and gynecology attendings. This is one of the few studies to demonstrate an intervention that helps decrease pain with IUD placement and which could be offered to nulliparous women presenting for IUD placement. REFERENCES 1. Trussell J. Contraceptive efficacy. In: Hatcher RA, Trussell J, Nelson AL, Cate W, Kowal D, Policar M, editors. Contraceptive technology. 20th revised ed. New York (NY): Ardent Media; Kavanaugh ML, Jerman J, Finer LB. Changes in use of longacting reversible contraceptive methods among United States women, Obstet Gynecol 2015;126: Guttmacher Institute. September 2016 fact sheet: contraceptive use in the United States. Available at: Retrieved March 5, Mody SK, Kiley J, Rademaker A, Gawron L, Stika C, Hammond C. Pain control for intrauterine device insertion: a randomized trial of 1% lidocaine paracervical block. Contraception 2012;86: Ngo LL, Ward KK, Mody SK. Ketorolac for pain control with intrauterine device placement: a randomized controlled trial. Obstet Gynecol 2015;126: Nelson AL, Fong JK. Intrauterine infusion of lidocaine does not reduce pain scores during IUD insertion. Contraception 2013; 88: Lopez LM, Bernholc A, Zeng Y, Allen RH, Bartz D, O Brien PA, et al. Interventions for pain with intrauterine device insertion. The Cochrane Database of Systematic Reviews 2015, Issue 7. Art. No.: CD DOI: / CD pub3. 8. Maguire K, Davis A, Rosario Tejeda L, Westhoff C. Intracervical lidocaine gel for IUD insertion: a randomized control trial. Contraception 2012;86: Chor J, Bregand-White J, Golobof A, Harwood B, Cowett A. Ibuprofen prophylaxis for levonorgestrel-releasing intrauterine device system insertion: a randomized controlled trial. Contraception 2012;85: Hubacher D, Reyes V, Lillo S, Zepeda A, Chen PL, Croxatto H. Pain from copper intrauterine device insertion: randomized trial of prophylactic ibuprofen. Am J Obstet Gynecol 2006;195: Jensen HH, Blaabjerg J, Lundrup J. Prophylactic use of prostaglandin synthesis inhibitors in connection with IUD insertion [in Danish]. Ugeskr Laeger 1998;160: Bednark PH, Crenin MD, Reeves MF, Espey E, Jensen JT; Post- Aspiration IUD Randomization (PAIR) Study Trial Group. Prophylactic ibuprofen does not improve pain with IUD insertion: a randomized trial. Contraception 2015;91: Edelman AB, Schaefer E, Olson A, Van Houten L, Bednarek P, Leclair C, et al. Effects of prophylactic misoprostol administration prior to intrauterine device insertion in nulliparous women. Contraception 2011;84: Sääv I, Aronsson A, Marions L, Stephansson O, Gemzell-Danielsson K. Cervical priming with sublingual misoprostol prior to insertion of an intrauterine device in nulliparous women: a randomized controlled trial. Hum Reprod 2007;22: Ngo LL, Braaten KP, Eichen E, Fortin J, Maurer R, Goldberg AB. Naproxen sodium for pain control with intrauterine device insertion: a randomized controlled trial. Obstet Gynecol 2016; 128: Renner RM, Nichols MD, Jensen JT, Li H, Edelman AB. Paracervical block for pain control in first-trimester surgical abortion: a randomized controlled trial. Obstet Gynecol 2012;119: Soon R, Tschann M, Salcedo J, Stevens K, Ahn HJ, Kaneshiro B. Paracervical block for laminaria insertion before secondtrimester abortion: a randomized controlled trial. Obstet Gynecol 2017;130: Akers AY, Steinway C, Sonalkar S, Perriera LK, Schreiber C, Harding J, et al. Reducing pain during intrauterine device insertion: a randomized controlled trial in adolescents and young women. Obstet Gynecol 2017;130: McGee DL. Local and topical anesthesia. In: Roberts JR, Hedges JR, editors. Clinical procedures in emergency medicine. 5th ed. Philadelphia (PA): Saunders; O Connell K, Jones HE, Simon M, Saporta V, Paul M, Lichtenberg ES; National Abortion Federation Members. First-trimester surgical abortion practices: a survey of National Abortion Federation members. Contraception 2009;79: Renner RM, Jensen JT, Nichols MD, Edelman A. Pain control in first trimester surgical abortion. The Cochrane Database of Systematic Reviews 2009, Issue 2. Art. No.: CD DOI: / CD pub Wiebe ER. Comparison of the efficacy of different local anesthetics and techniques of local anesthesia in therapeutic abortions. Am J Obstet Gynecol 1992;167: Rabin JM, Spitzer M, Dwyer AT, Kaiser IH. Topical anesthesia for gynecologic procedures. Obstet Gynecol 1989;73: Zullo F, Pellicano M, Stigliano CM, Di Carlo C, Fabrizio A, Nappi C. Topical anesthesia for office hysteroscopy. A prospective, randomized study comparing two modalities. J Reprod Med 1999;44: VOL. 132, NO. 3, SEPTEMBER 2018 Mody et al Paracervical Block for IUD Placement 581
8 25. Cetin A, Cetin M. Effect of deep injections of local anesthetics and basal dilatation of cervix in management of pain during legal abortions. A randomized, controlled study. Contraception 1997;56: Phair N, Jensen JT, Nichols MD. Paracervical block and elective abortion: the effect on pain of waiting between injection and procedure. Am J Obstet Gynecol 2002;186: Todd KH, Funk KG, Funk JP, Bonacci R. Clinical significance of reported changes in pain severity. Ann Emerg Med 1996;27: Gemzell-Danielsson K, Schellschmidt I, Apter D. A randomized, phase II study describing the efficacy, bleeding profile, and safety of two low-dose levonorgestrel-releasing intrauterine contraceptive systems and Mirena. Fertil Steril 2012;97: e Mody et al Paracervical Block for IUD Placement OBSTETRICS & GYNECOLOGY
LOCAL ANAESTHESIA IN FIRST TRIMESTER SURGICAL ABORTION. Regina-Maria Renner MD MPH
 LOCAL ANAESTHESIA IN FIRST TRIMESTER SURGICAL ABORTION Regina-Maria Renner MD MPH FIAPAC October 20, 2012 Disclosures none Objectives Provide an introduction to pain pathways Provide background regarding
LOCAL ANAESTHESIA IN FIRST TRIMESTER SURGICAL ABORTION Regina-Maria Renner MD MPH FIAPAC October 20, 2012 Disclosures none Objectives Provide an introduction to pain pathways Provide background regarding
SALSA: Self-Administered Lidocaine Gel for Pain Management with First Trimester Surgical Abortion A Randomized Trial. Paul D Blumenthal, MD, MPH
 SALSA: Self-Administered Lidocaine Gel for Pain Management with First Trimester Surgical Abortion A Randomized Trial Paul D Blumenthal, MD, MPH Background Pain is a limiting factor in where and how abortion
SALSA: Self-Administered Lidocaine Gel for Pain Management with First Trimester Surgical Abortion A Randomized Trial Paul D Blumenthal, MD, MPH Background Pain is a limiting factor in where and how abortion
Interventions for pain with intrauterine device insertion (Review)
 Interventions for pain with intrauterine device insertion (Review) Allen RH, Bartz D, Grimes DA, Hubacher D, O Brien P This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Interventions for pain with intrauterine device insertion (Review) Allen RH, Bartz D, Grimes DA, Hubacher D, O Brien P This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
BRIEF REPORTS. Providing Long-Acting Reversible Contraception in an Academic Family Medicine Center Jennifer Amico, MD, MPH; Justine Wu, MD, MPH
 Providing Long-Acting Reversible Contraception in an Academic Family Medicine Center Jennifer Amico, MD, MPH; Justine Wu, MD, MPH BACKGROUND AND OBJECTIVES: Providing long-acting reversible contraception
Providing Long-Acting Reversible Contraception in an Academic Family Medicine Center Jennifer Amico, MD, MPH; Justine Wu, MD, MPH BACKGROUND AND OBJECTIVES: Providing long-acting reversible contraception
The use of long-acting reversible contraceptive
 Overcoming LARC complications: 7 case challenges The strings to your patient s intrauterine device (IUD) are missing. Clinical experience and ACOG direction guide the management plans for this and more
Overcoming LARC complications: 7 case challenges The strings to your patient s intrauterine device (IUD) are missing. Clinical experience and ACOG direction guide the management plans for this and more
Lindsey Tingen, MD Department of Obstetrics and Gynecology, Greenville Health System Greenville, SC
 Postpartum IUD Insertion: Continued Usage at Six Months Based on Expulsion and Removal Rates at Greenville Memorial Hospital in the First Year After Adoption of the Practice Lindsey Tingen, MD Department
Postpartum IUD Insertion: Continued Usage at Six Months Based on Expulsion and Removal Rates at Greenville Memorial Hospital in the First Year After Adoption of the Practice Lindsey Tingen, MD Department
Simplifying Vide Contraception. University of Utah Department of Ob/Gyn Post Grad Course February 13, 2017 David Turok
 Simplifying Vide Contraception University of Utah Department of Ob/Gyn Post Grad Course February 13, 2017 David Turok Background Objectives At the conclusion of this presentation participants will be able
Simplifying Vide Contraception University of Utah Department of Ob/Gyn Post Grad Course February 13, 2017 David Turok Background Objectives At the conclusion of this presentation participants will be able
LEARNING OBJECTIVES. Beyond the Pill: Long Acting Contraception. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy is Common
 4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
Unintended Pregnancy is Common LEARNING OBJECTIVES. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy And Contraceptive Use
 3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
LARC: Disclosures. Long Acting Reversible Contraception. Objectives 10/23/2013. I have no relevant financial disclosures
 LARC: Long Acting Reversible Contraception Disclosures I have no relevant financial disclosures Jennifer Kerns, MD, MPH Assistant Professor, UCSF Obstetrics, Gynecology and Reproductive Sciences San Francisco
LARC: Long Acting Reversible Contraception Disclosures I have no relevant financial disclosures Jennifer Kerns, MD, MPH Assistant Professor, UCSF Obstetrics, Gynecology and Reproductive Sciences San Francisco
Dr. Russo reports no financial relationships relevant to this article. Dr Creinin is a senior clinical advisor for Medicines360.
 CONTRACEPTION Demand for long-acting reversible contraception is growing, including in adolescents and nulliparas. We need to challenge our historical reservations about the IUD and heed the call. Jennefer
CONTRACEPTION Demand for long-acting reversible contraception is growing, including in adolescents and nulliparas. We need to challenge our historical reservations about the IUD and heed the call. Jennefer
Lidocaine-Prilocaine Cream as Analgesia for IUD Insertion: A Prospective, Randomized, Controlled, Triple Blinded Study
 Global Journal of Health Science; Vol. 7, No. 4; 2015 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Lidocaine-Prilocaine Cream as Analgesia for IUD Insertion: A
Global Journal of Health Science; Vol. 7, No. 4; 2015 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Lidocaine-Prilocaine Cream as Analgesia for IUD Insertion: A
Contraception for Obese Women RENEE E. MESTAD, MD, MSCI ACOG DISTRICT II UPSTATE MEETING APRIL 29, 2016
 Contraception for Obese Women RENEE E. MESTAD, MD, MSCI ACOG DISTRICT II UPSTATE MEETING APRIL 29, 2016 Disclosure I am a Nexplanon trainer for Merck. Objectives Understand how obesity may affect pharmacokinetics
Contraception for Obese Women RENEE E. MESTAD, MD, MSCI ACOG DISTRICT II UPSTATE MEETING APRIL 29, 2016 Disclosure I am a Nexplanon trainer for Merck. Objectives Understand how obesity may affect pharmacokinetics
The most commonly chosen methods of contraception
 Original Research Effects of Age, Parity, and Device Type on Complications and Discontinuation of Intrauterine Devices Joelle Aoun, MD, Virginia A. Dines, BS, Dale W. Stovall, MD, Mihriye Mete, PhD, Casey
Original Research Effects of Age, Parity, and Device Type on Complications and Discontinuation of Intrauterine Devices Joelle Aoun, MD, Virginia A. Dines, BS, Dale W. Stovall, MD, Mihriye Mete, PhD, Casey
LONG-ACTING REVERSIBLE CONTRACEPTION. Summary Tables
 LONG-ACTING REVERSIBLE CONTRACEPTION Summary Tables Bridging the Divide: A Project of the Jacobs Institute of Women s Health June 2016 Table 1. Summary of LARC Methods Available Years Since Effective Copper
LONG-ACTING REVERSIBLE CONTRACEPTION Summary Tables Bridging the Divide: A Project of the Jacobs Institute of Women s Health June 2016 Table 1. Summary of LARC Methods Available Years Since Effective Copper
An evaluation of hydrocodone/actaminophen for pain control in first trimester surgical abortion
 Oregon Health & Science University OHSU Digital Commons Scholar Archive May 2012 An evaluation of hydrocodone/actaminophen for pain control in first trimester surgical abortion Elizabeth A. Micks Follow
Oregon Health & Science University OHSU Digital Commons Scholar Archive May 2012 An evaluation of hydrocodone/actaminophen for pain control in first trimester surgical abortion Elizabeth A. Micks Follow
Teen Sexual Health Survey
 Instructions Teen Sexual Health Survey Thank you for taking part in our survey. DO NOT write your name on this survey. The answers you give will be kept private. No one will know what you write. Answer
Instructions Teen Sexual Health Survey Thank you for taking part in our survey. DO NOT write your name on this survey. The answers you give will be kept private. No one will know what you write. Answer
Long Acting Reversible Contraception: First Line Care for Adolescents. David A. Levine, MD, FAAP Melissa Kottke, MD, MPH, FACOG
 Long Acting Reversible Contraception: First Line Care for Adolescents David A. Levine, MD, FAAP Melissa Kottke, MD, MPH, FACOG Disclosures Melissa Kottke is a Nexplanon trainer for Merck Objectives Describe
Long Acting Reversible Contraception: First Line Care for Adolescents David A. Levine, MD, FAAP Melissa Kottke, MD, MPH, FACOG Disclosures Melissa Kottke is a Nexplanon trainer for Merck Objectives Describe
VCHIP LARC Needs Assessment Survey
 VCHIP LARC Needs Assessment Survey Demographics 1. How many have you been in practice (post-training)? Choose one of the following answers 0-5 6-10 11-15 16-20 21 or more 2. What are your professional
VCHIP LARC Needs Assessment Survey Demographics 1. How many have you been in practice (post-training)? Choose one of the following answers 0-5 6-10 11-15 16-20 21 or more 2. What are your professional
Instruction for the patient
 WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
Long-Acting Reversible Contraception: The Contraceptive CHOICE Project
 Long-Acting Reversible Contraception: The Contraceptive CHOICE Project Jeffrey F. Peipert, M.D., Ph.D. Vice Chair of Clinical Research Robert J. Terry Professor Department of Obstetrics & Gynecology Washington
Long-Acting Reversible Contraception: The Contraceptive CHOICE Project Jeffrey F. Peipert, M.D., Ph.D. Vice Chair of Clinical Research Robert J. Terry Professor Department of Obstetrics & Gynecology Washington
A Study of Physician Recommendations for Reversible Contraceptive Methods Using Standardized Patients
 A Study of Physician Recommendations for Reversible Contraceptive Methods Using Standardized Patients By Christine Dehlendorf, Kevin Grumbach, Eric Vittinghoff, Rachel Ruskin and Jody Steinauer Christine
A Study of Physician Recommendations for Reversible Contraceptive Methods Using Standardized Patients By Christine Dehlendorf, Kevin Grumbach, Eric Vittinghoff, Rachel Ruskin and Jody Steinauer Christine
Intrauterine Devices (IUDs): Access for Women in the U.S.
 November 2016 Fact Sheet Intrauterine Devices (IUDs): Access for Women in the U.S. Intrauterine devices (IUDs) are one of the most effective forms of reversible contraception. IUDs, along with implants,
November 2016 Fact Sheet Intrauterine Devices (IUDs): Access for Women in the U.S. Intrauterine devices (IUDs) are one of the most effective forms of reversible contraception. IUDs, along with implants,
Characteristics of users of intrauterine devices and other reversible contraceptive methods in the United States
 CONTRACEPTION Characteristics of users of intrauterine devices and other reversible contraceptive methods in the United States Xin Xu, Ph.D., a Maurizio Macaluso, M.D., Dr.P.H., a Jennifer Frost, Ph.D.,
CONTRACEPTION Characteristics of users of intrauterine devices and other reversible contraceptive methods in the United States Xin Xu, Ph.D., a Maurizio Macaluso, M.D., Dr.P.H., a Jennifer Frost, Ph.D.,
Disclosures. Learning Objectives 4/18/2017 ADOLESCENT CONTRACEPTION UPDATE APRIL 28, Nexplanon trainer for Merck
 ADOLESCENT CONTRACEPTION UPDATE APRIL 28, 2017 Brandy Mitchell, MN, RN, ANP BC, WHNP BC University of Iowa Hospitals and Clinics Obstetrics and Gynecology Iowa Association of Nurse Practitioners Spring
ADOLESCENT CONTRACEPTION UPDATE APRIL 28, 2017 Brandy Mitchell, MN, RN, ANP BC, WHNP BC University of Iowa Hospitals and Clinics Obstetrics and Gynecology Iowa Association of Nurse Practitioners Spring
The modern intrauterine device (IUD) is highly reliable and
 Intrauterine Device Knowledge and Practices: A National Survey of Obstetrics and Gynecology Residents Jennifer Tang, MD, MSCR, Rie Maurer, MA, and Deborah Bartz, MD, MPH Objectives: The primary objective
Intrauterine Device Knowledge and Practices: A National Survey of Obstetrics and Gynecology Residents Jennifer Tang, MD, MSCR, Rie Maurer, MA, and Deborah Bartz, MD, MPH Objectives: The primary objective
WHAT ARE CONTRACEPTIVES?
 CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
Disturbance of uterine bleeding patterns, often anecdotally
 Management of Initial Bleeding or Spotting After Levonorgestrel-Releasing Intrauterine System Placement A Randomized Controlled Trial Terje Sørdal, MD, Pirjo Inki, MD, PhD, John Draeby, MD, Mary O Flynn,
Management of Initial Bleeding or Spotting After Levonorgestrel-Releasing Intrauterine System Placement A Randomized Controlled Trial Terje Sørdal, MD, Pirjo Inki, MD, PhD, John Draeby, MD, Mary O Flynn,
Chapter 7 Infertility, Contraception, and Abortion
 Chapter 7 Infertility, Contraception, and Abortion Infertility Incidence Affects about 10% to 15% of reproductive-age population Subfertility: prolonged time to conceive Sterility: inability to conceive
Chapter 7 Infertility, Contraception, and Abortion Infertility Incidence Affects about 10% to 15% of reproductive-age population Subfertility: prolonged time to conceive Sterility: inability to conceive
Emergency Contraception THE FACTS
 Emergency Contraception Quick Facts What is it? Emergency contraception is birth control that you use after you have had unprotected sex--if you didn t use birth control or your regular birth control failed.
Emergency Contraception Quick Facts What is it? Emergency contraception is birth control that you use after you have had unprotected sex--if you didn t use birth control or your regular birth control failed.
Examining Long-Acting Reversible Contraceptive Methods
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/examining-long-acting-reversible-contraceptivemethods/7078/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/examining-long-acting-reversible-contraceptivemethods/7078/
What s New in Adolescent Contraception?
 What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
2
 1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
Support for Acetaminophen 1000 mg Over-the-Counter Dose:
 Support for Acetaminophen 1000 mg Over-the-Counter Dose: The Dental Impaction Pain Model and Efficacy and Safety Results from McNeil Randomized, Double-Blind, Single-Dose Study of Acetaminophen 1000 mg,
Support for Acetaminophen 1000 mg Over-the-Counter Dose: The Dental Impaction Pain Model and Efficacy and Safety Results from McNeil Randomized, Double-Blind, Single-Dose Study of Acetaminophen 1000 mg,
Differences in Women Who Choose Subdermal Implants Versus Intrauterine Devices
 The Journal of Reproductive Medicine Differences in Women Who Choose Subdermal Implants Versus Intrauterine Devices Vien C. Lam, M.D., Emily E. Hadley, M.D., Abbey B. Berenson, M.D., Ph.D., Jacqueline
The Journal of Reproductive Medicine Differences in Women Who Choose Subdermal Implants Versus Intrauterine Devices Vien C. Lam, M.D., Emily E. Hadley, M.D., Abbey B. Berenson, M.D., Ph.D., Jacqueline
Postpartum intrauterine device placement: a patient-friendly option
 Cwiak and Cordes Contraception and Reproductive Medicine (2018) 3:3 https://doi.org/10.1186/s40834-018-0057-x Contraception and Reproductive Medicine REVIEW Postpartum intrauterine device placement: a
Cwiak and Cordes Contraception and Reproductive Medicine (2018) 3:3 https://doi.org/10.1186/s40834-018-0057-x Contraception and Reproductive Medicine REVIEW Postpartum intrauterine device placement: a
International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage:
 Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
1. Ortiz, M. E et al. Mechanisms of action of intrauterine devices. Obstet & Gynl Survey 1996; 51(12), 42S-51S.
 1 2 1. Ortiz, M. E et al. Mechanisms of action of intrauterine devices. Obstet & Gynl Survey 1996; 51(12), 42S-51S. The contraceptive action of all IUDs is mainly in the uterine cavity. The major effect
1 2 1. Ortiz, M. E et al. Mechanisms of action of intrauterine devices. Obstet & Gynl Survey 1996; 51(12), 42S-51S. The contraceptive action of all IUDs is mainly in the uterine cavity. The major effect
Example CLINICAL GUIDELINES for Postpartum IUD insertion
 Example CLINICAL GUIDELINES for Postpartum IUD insertion Postpartum Intrauterine Device Insertion 1.0 Indications: 1.1 Insertion of an intrauterine device (IUD) for long-acting reversible contraception
Example CLINICAL GUIDELINES for Postpartum IUD insertion Postpartum Intrauterine Device Insertion 1.0 Indications: 1.1 Insertion of an intrauterine device (IUD) for long-acting reversible contraception
Primary dysmenorrhea, defined as painful menstruation
 Oral Contraceptives for Dysmenorrhea in Adolescent Girls A Randomized Trial Anne Rachel Davis, MD, Carolyn Westhoff, MD, Katharine O Connell, MD, and Nancy Gallagher, RN Objective: To assess whether a
Oral Contraceptives for Dysmenorrhea in Adolescent Girls A Randomized Trial Anne Rachel Davis, MD, Carolyn Westhoff, MD, Katharine O Connell, MD, and Nancy Gallagher, RN Objective: To assess whether a
Can an iud cause back pain
 Can an iud cause back pain 3-11-2016 It can cause your periods to. Some women may also feel lightheaded from the pain. You can have most IUDs placed at any. "Intrauterine Device ( IUD )." Do not use this
Can an iud cause back pain 3-11-2016 It can cause your periods to. Some women may also feel lightheaded from the pain. You can have most IUDs placed at any. "Intrauterine Device ( IUD )." Do not use this
Patient or Clinician: Duration of Use of Intrauterine Devices Based on Who Initiated Discussion of Placement
 ORIGINAL RESEARCH Patient or Clinician: Duration of Use of Intrauterine Devices Based on Who Initiated Discussion of Placement Tammy Chang, MD, MPH, MS, Michelle H. Moniz, MD, MSc, Melissa A. Plegue, MA,
ORIGINAL RESEARCH Patient or Clinician: Duration of Use of Intrauterine Devices Based on Who Initiated Discussion of Placement Tammy Chang, MD, MPH, MS, Michelle H. Moniz, MD, MSc, Melissa A. Plegue, MA,
Transcervical Sterilization
 Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
Same-Day Access to Highly Effective Reversible Contraception: Moving from Plan B to Happily Ever After
 Same-Day Access to Highly Effective Reversible Contraception: Moving from Plan B to Happily Ever After Eleanor Bimla Schwarz, MD, MS Director, Women s Health Services Research Unit Center for Research
Same-Day Access to Highly Effective Reversible Contraception: Moving from Plan B to Happily Ever After Eleanor Bimla Schwarz, MD, MS Director, Women s Health Services Research Unit Center for Research
levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer
 levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer 6 March 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer 6 March 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
Maximizing LARC Availability: Bringing the Lessons of the CHOICE Project to Your Community
 Maximizing LARC Availability: Bringing the Lessons of the CHOICE Project to Your Community Reproductive Health 2012 September 21, 2012 David Turok, MD/MPH Objectives Communicate to colleagues the reduction
Maximizing LARC Availability: Bringing the Lessons of the CHOICE Project to Your Community Reproductive Health 2012 September 21, 2012 David Turok, MD/MPH Objectives Communicate to colleagues the reduction
Product Information. Confidence that lasts
 Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert.
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. PROPRIETARY DRUG NAME / GENERIC DRUG NAME: Advil / Ibuprofen
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. PROPRIETARY DRUG NAME / GENERIC DRUG NAME: Advil / Ibuprofen
Intrauterine contraception
 For reprint orders, please contact: reprints@futuremedicine.com Intrauterine devices (IUDs) are effective, reversible forms of contraception with high patient satisfaction and continuation. IUDs can be
For reprint orders, please contact: reprints@futuremedicine.com Intrauterine devices (IUDs) are effective, reversible forms of contraception with high patient satisfaction and continuation. IUDs can be
An Overview of Long Acting Reversible Contraception Methods
 An Overview of Long Acting Reversible Contraception Methods Unintended Pregnancy All pregnancies should be intended; that is, they should be consciously and clearly desired at the time of conception. -
An Overview of Long Acting Reversible Contraception Methods Unintended Pregnancy All pregnancies should be intended; that is, they should be consciously and clearly desired at the time of conception. -
Patient Awareness and Understanding of Intrauterine Devices
 University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2016 Patient Awareness and Understanding of Intrauterine Devices Lindsey Marie Eastman University
University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2016 Patient Awareness and Understanding of Intrauterine Devices Lindsey Marie Eastman University
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea
 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Policy Number: 4.01.17 Last Review: 11/2013 Origination: 11/2007 Next Review: 11/2014 Policy Blue Cross and Blue Shield
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Policy Number: 4.01.17 Last Review: 11/2013 Origination: 11/2007 Next Review: 11/2014 Policy Blue Cross and Blue Shield
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea
 Page: 1 of 7 Last Review Status/Date: June 2015 for Primary and Secondary Dysmenorrhea Description Two laparoscopic surgical approaches are proposed as adjuncts to conservative surgical therapy for the
Page: 1 of 7 Last Review Status/Date: June 2015 for Primary and Secondary Dysmenorrhea Description Two laparoscopic surgical approaches are proposed as adjuncts to conservative surgical therapy for the
Disclosures. Contraceptive Method Use, U.S. Best Practices in Contraception: Advances, Tips, and Tricks
 Best Practices in Contraception: Advances, Tips, and Tricks Disclosures I have no disclosures I may discuss off-label use of some contraceptives Biftu Mengesha MD MAS Department of Obstetrics, Gynecology
Best Practices in Contraception: Advances, Tips, and Tricks Disclosures I have no disclosures I may discuss off-label use of some contraceptives Biftu Mengesha MD MAS Department of Obstetrics, Gynecology
Is Outpatient Hysteroscopy the New Gold Standard?
 Is Outpatient Hysteroscopy the New Gold Standard? McIlwaine K, Readman E, Ma T, Manwaring J, Ellett L, Hicks L, Porter J, Cameron M, Maher P. Mercy Hospital for Women, Melbourne, Australia Background Abnormal
Is Outpatient Hysteroscopy the New Gold Standard? McIlwaine K, Readman E, Ma T, Manwaring J, Ellett L, Hicks L, Porter J, Cameron M, Maher P. Mercy Hospital for Women, Melbourne, Australia Background Abnormal
Pain Management for Offi ce Hysteroscopy -
 International Journal of Reproductive Medicine & Gynecology Review Article Pain Management for Offi ce Hysteroscopy - Carugno Jose* and Andrade Fausto Obstetrics and Gynecology Department, Minimally Invasive
International Journal of Reproductive Medicine & Gynecology Review Article Pain Management for Offi ce Hysteroscopy - Carugno Jose* and Andrade Fausto Obstetrics and Gynecology Department, Minimally Invasive
The number of women using long-acting reversible
 Long-acting reversible contraception: Who, what, when, and how This review provides practical tips and dispels some common misconceptions about these devices, which have higher rates of patient satisfaction
Long-acting reversible contraception: Who, what, when, and how This review provides practical tips and dispels some common misconceptions about these devices, which have higher rates of patient satisfaction
Women spend about 5 years of their
 CONTRACEPTION Why we have not yet reduced the unintended pregnancy rate Melody Y. Hou, MD, MPH Dr. Hou is Assistant Professor of Obstetrics and Gynecology at the University of California, Davis, in Sacramento.
CONTRACEPTION Why we have not yet reduced the unintended pregnancy rate Melody Y. Hou, MD, MPH Dr. Hou is Assistant Professor of Obstetrics and Gynecology at the University of California, Davis, in Sacramento.
The Intrauterine Device in Women of Childbearing Age Has A Greater Long-Term Cost-Benefit than Oral Contraception Pills
 Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects Summer 8-13-2016 The Intrauterine Device in Women of Childbearing Age Has A Greater
Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects Summer 8-13-2016 The Intrauterine Device in Women of Childbearing Age Has A Greater
Pain from copper intrauterine device insertion: Randomized trial of prophylactic ibuprofen
 American Journal of Obstetrics and Gynecology (2006) 195, 1272 7 www.ajog.org Pain from copper intrauterine device insertion: Randomized trial of prophylactic ibuprofen David Hubacher, PhD, a Veronica
American Journal of Obstetrics and Gynecology (2006) 195, 1272 7 www.ajog.org Pain from copper intrauterine device insertion: Randomized trial of prophylactic ibuprofen David Hubacher, PhD, a Veronica
The Doctor Is In. Brent N Davidson MD Vice Chair Women s Health Henry Ford Health System Medical Director Family Planning MDCH
 The Doctor Is In Brent N Davidson MD Vice Chair Women s Health Henry Ford Health System Medical Director Family Planning MDCH Contraception Resources from the CDC: 2016 U.S. Medical Eligibility Criteria
The Doctor Is In Brent N Davidson MD Vice Chair Women s Health Henry Ford Health System Medical Director Family Planning MDCH Contraception Resources from the CDC: 2016 U.S. Medical Eligibility Criteria
38 OBG Management August 2012 Vol. 24 No. 8 obgmanagement.com
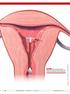 FIGURE 1 Copper intrauterine device displaced in the lower uterine segment with the left arm embedded in the myometrium. illustrations: craig zuckerman for obg management 38 OBG Management August 2012
FIGURE 1 Copper intrauterine device displaced in the lower uterine segment with the left arm embedded in the myometrium. illustrations: craig zuckerman for obg management 38 OBG Management August 2012
UCSF UC San Francisco Previously Published Works
 UCSF UC San Francisco Previously Published Works Title California Family Planning Health Care Providers' Challenges to Same-Day Long- Acting Reversible Contraception Provision Permalink https://escholarship.org/uc/item/55r8x2nr
UCSF UC San Francisco Previously Published Works Title California Family Planning Health Care Providers' Challenges to Same-Day Long- Acting Reversible Contraception Provision Permalink https://escholarship.org/uc/item/55r8x2nr
Intrauterine contraceptive devices (IUDs) are becoming
 Malpositioned Intrauterine Contraceptive Devices Risk Factors, Outcomes, and Future Pregnancies Kari P. Braaten, MD, MPH, Carol B. Benson, MD, Rie Maurer, MA, and Alisa B. Goldberg, MD, MPH OBJECTIVE:
Malpositioned Intrauterine Contraceptive Devices Risk Factors, Outcomes, and Future Pregnancies Kari P. Braaten, MD, MPH, Carol B. Benson, MD, Rie Maurer, MA, and Alisa B. Goldberg, MD, MPH OBJECTIVE:
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics THE ROLE OF POST- ABORTION CONTRACEPTION IN PREVENTION OF UNSAFE ABORTION THE ROLE OF POST- ABORTION CONTRACEPTION IN PREVENTION OF UNSAFE ABORTION
International Federation of Gynecology and Obstetrics THE ROLE OF POST- ABORTION CONTRACEPTION IN PREVENTION OF UNSAFE ABORTION THE ROLE OF POST- ABORTION CONTRACEPTION IN PREVENTION OF UNSAFE ABORTION
Contraception. Yolanda Evans MD MPH Assistant Professor of Pediatrics Division of Adolescent Medicine
 Contraception Yolanda Evans MD MPH Assistant Professor of Pediatrics Division of Adolescent Medicine Disclosures No financial relationships to disclose I have no commercial, financial, research ties to
Contraception Yolanda Evans MD MPH Assistant Professor of Pediatrics Division of Adolescent Medicine Disclosures No financial relationships to disclose I have no commercial, financial, research ties to
Coding for the Contraceptive Implant and IUDs
 LARC Quick Coding Guide 2018 UPDATE Coding for the Contraceptive Implant and IUDs CORRECT CODING can result in more appropriate compensation for services and devices. To help practices receive appropriate
LARC Quick Coding Guide 2018 UPDATE Coding for the Contraceptive Implant and IUDs CORRECT CODING can result in more appropriate compensation for services and devices. To help practices receive appropriate
Immediate versus Delayed IUD Insertion after Uterine Aspiration
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Immediate versus Delayed IUD Insertion after Uterine Aspiration Paula H. Bednarek, M.D., M.P.H., Mitchell D. Creinin, M.D., Matthew
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Immediate versus Delayed IUD Insertion after Uterine Aspiration Paula H. Bednarek, M.D., M.P.H., Mitchell D. Creinin, M.D., Matthew
Contraception: The Pill Needs to Share (or Move Over) Frankly Speaking EP 17
 Contraception: The Pill Needs to Share (or Move Over) Frankly Speaking EP 17 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional
Contraception: The Pill Needs to Share (or Move Over) Frankly Speaking EP 17 Transcript Details This is a transcript of an episode from the podcast series Frankly Speaking accessible at Pri- Med.com. Additional
Office hysteroscopy offers many benefits
 MINIMALLY INVASIVE GYNECOLOGY How to reduce patient anxiety and pain during in-office hysteroscopy Amy L. Garcia, MD Dr. Garcia is Director, Center for Women s Surgery and Garcia Institute for Hysteroscopic
MINIMALLY INVASIVE GYNECOLOGY How to reduce patient anxiety and pain during in-office hysteroscopy Amy L. Garcia, MD Dr. Garcia is Director, Center for Women s Surgery and Garcia Institute for Hysteroscopic
Extended use of intrauterine devices: How long can we go?
 Extended use of intrauterine devices: How long can we go? Justine P. Wu, MD, MPH Sarah Pickle, MD Rutgers Robert Wood Johnson Medical School Department of Family Medicine & Community Health Disclosures
Extended use of intrauterine devices: How long can we go? Justine P. Wu, MD, MPH Sarah Pickle, MD Rutgers Robert Wood Johnson Medical School Department of Family Medicine & Community Health Disclosures
Levonorgestrel Intrauterine Device
 CHAPTER 11 Levonorgestrel Intrauterine Device Key Points for Providers and Clients y Long-term pregnancy protection. Very effective for 5 years, immediately reversible. yinserted into the uterus by a specifically
CHAPTER 11 Levonorgestrel Intrauterine Device Key Points for Providers and Clients y Long-term pregnancy protection. Very effective for 5 years, immediately reversible. yinserted into the uterus by a specifically
Power Point Use in EBPs. CAPP & PREP Learning Community May 15, 2018
 Power Point Use in EBPs CAPP & PREP Learning Community May 15, 2018 Objectives Best practices for power point use Why use power point for EBP delivery Examples: the Good, the Bad and the Ugly Recommendations
Power Point Use in EBPs CAPP & PREP Learning Community May 15, 2018 Objectives Best practices for power point use Why use power point for EBP delivery Examples: the Good, the Bad and the Ugly Recommendations
Adolescent pregnancies have declined
 Gut tmacher Policy Review GPR Fall 2013 Volume 16 Number 4 Leveling the Playing Field: The Promise of Long-Acting Reversible Contraceptives for Adolescents By Heather D. Boonstra Rate per 1,000 women aged
Gut tmacher Policy Review GPR Fall 2013 Volume 16 Number 4 Leveling the Playing Field: The Promise of Long-Acting Reversible Contraceptives for Adolescents By Heather D. Boonstra Rate per 1,000 women aged
Pain with Office Gyn Procedures: Tips, Tricks and Evidence
 Pain with Office Gyn Procedures: Tips, Tricks and Evidence Disclosures Dr. Meckstroth receives an honorarium from Danco, Inc. to serve as an expert for an FDAmandated hotline for clinicians with questions
Pain with Office Gyn Procedures: Tips, Tricks and Evidence Disclosures Dr. Meckstroth receives an honorarium from Danco, Inc. to serve as an expert for an FDAmandated hotline for clinicians with questions
Contraception and gynecological pathologies
 1 Contraception and gynecological pathologies 18 years old, 2 CMI normal First menstruation at 14 years old Irregular (every 2/3 months), painful + She does not need contraception She is worried about
1 Contraception and gynecological pathologies 18 years old, 2 CMI normal First menstruation at 14 years old Irregular (every 2/3 months), painful + She does not need contraception She is worried about
Page 1 of 6. Icahn School of Medicine at Mount Sinai Fellowship in Family Planning Program Overview
 Icahn School of Medicine at Mount Sinai Fellowship in Family Planning 2016 Program Overview The Icahn School of Medicine at Mount Sinai Fellowship in Family Planning is proud to be the 28th fellowship
Icahn School of Medicine at Mount Sinai Fellowship in Family Planning 2016 Program Overview The Icahn School of Medicine at Mount Sinai Fellowship in Family Planning is proud to be the 28th fellowship
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea. Original Policy Date
 MP 4.01.10 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 4.01.10 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
A Comparative Study between the Side Effects of Copper Intrauterine Device in Women with Non-scarred and Scarred Uterus
 Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 161-659 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ A Comparative Study between the Side Effects of Copper Intrauterine
Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 161-659 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ A Comparative Study between the Side Effects of Copper Intrauterine
FACT SHEET: Copper IUD
 FACT SHEET: Copper IUD How does the copper IUD help me? The copper IUD is a hormone-free option. If you don t like the copper IUD or you decide to get pregnant, your health care provider can remove the
FACT SHEET: Copper IUD How does the copper IUD help me? The copper IUD is a hormone-free option. If you don t like the copper IUD or you decide to get pregnant, your health care provider can remove the
Counseling About IUDs: A Mixed-Methods Analysis
 Counseling About IUDs: A Mixed-Methods Analysis CONTEXT: IUDs are infrequently used in the United States. Assessing how counseling about this method is delivered can help identify barriers to IUD use that
Counseling About IUDs: A Mixed-Methods Analysis CONTEXT: IUDs are infrequently used in the United States. Assessing how counseling about this method is delivered can help identify barriers to IUD use that
Improving IUD Usage Among Adolescents Through Provider Education
 Improving IUD Usage Among Adolescents Through Provider Education Item Type text; Electronic Thesis Authors Griswold, Sophie Emmaline Publisher The University of Arizona. Rights Copyright is held by the
Improving IUD Usage Among Adolescents Through Provider Education Item Type text; Electronic Thesis Authors Griswold, Sophie Emmaline Publisher The University of Arizona. Rights Copyright is held by the
Protocol. This trial protocol has been provided by the authors to give readers additional information about their work.
 Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Bednarek PH, Creinin MD, Reeves MF, et al. Immediate versus delayed
Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Bednarek PH, Creinin MD, Reeves MF, et al. Immediate versus delayed
NAVY AND MARINE CORPS PUBLIC HEALTH CENTER HEALTH ANALYSIS DEPARTMENT
 NAVY AND MARINE CORPS PUBLIC HEALTH CENTER HEALTH ANALYSIS DEPARTMENT 620 John Paul Jones Circle, Portsmouth, VA 23708 Phone: 757.953.0700 E-mail: health-analysis@nehc.mar.med.navy.mil Analysis of Long-Acting
NAVY AND MARINE CORPS PUBLIC HEALTH CENTER HEALTH ANALYSIS DEPARTMENT 620 John Paul Jones Circle, Portsmouth, VA 23708 Phone: 757.953.0700 E-mail: health-analysis@nehc.mar.med.navy.mil Analysis of Long-Acting
Adolescent Hot Topics: Contraception
 Adolescent Hot Topics: Contraception Dr. Stephanie Addison Holt Adolescent Medicine Objectives Discuss way to counsel the sexually active adolescent Explore the latest recommendations and updates regarding
Adolescent Hot Topics: Contraception Dr. Stephanie Addison Holt Adolescent Medicine Objectives Discuss way to counsel the sexually active adolescent Explore the latest recommendations and updates regarding
Information for Informed Consent for Insertion of a Mirena IUD
 Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
INTRAUTERINE DEVICES AND INFECTIONS. Tips for Evaluation and Management
 INTRAUTERINE DEVICES AND INFECTIONS Tips for Evaluation and Management Objectives At the end of this presentation, the participant should be able to: 1. Diagnose infection after IUD placement 2. Provide
INTRAUTERINE DEVICES AND INFECTIONS Tips for Evaluation and Management Objectives At the end of this presentation, the participant should be able to: 1. Diagnose infection after IUD placement 2. Provide
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
ClincialTrials.gov Identifier: sanofi-aventis. Sponsor/company:
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClincialTrials.gov
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClincialTrials.gov
Global Contraception
 Video Companion Guide Global Contraception Learning Objectives: By the end of the session, learners will be able to: Describe of all contraceptive methods. Develop a basic understanding of patient-centered
Video Companion Guide Global Contraception Learning Objectives: By the end of the session, learners will be able to: Describe of all contraceptive methods. Develop a basic understanding of patient-centered
Non-steroidal anti-inflammatory drugs for heavy bleeding or pain associated with intrauterine-device use(review)
 Cochrane Database of Systematic Reviews Non-steroidal anti-inflammatory drugs for heavy bleeding or pain associated with intrauterine-device use(review) GrimesDA,HubacherD,LopezLM,SchulzKF Grimes DA, Hubacher
Cochrane Database of Systematic Reviews Non-steroidal anti-inflammatory drugs for heavy bleeding or pain associated with intrauterine-device use(review) GrimesDA,HubacherD,LopezLM,SchulzKF Grimes DA, Hubacher
Labeling for Permanent Hysteroscopically-Placed Tubal Implants Intended for Sterilization
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 Labeling for Permanent Hysteroscopically-Placed Tubal Implants Intended for Sterilization Draft Guidance for Industry and Food and Drug
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 Labeling for Permanent Hysteroscopically-Placed Tubal Implants Intended for Sterilization Draft Guidance for Industry and Food and Drug
Research. Reported weight gain is one of the
 Research www.ajog.org GENERAL GYNECOLOGY Validity of perceived weight gain in women using long-acting reversible contraception and depot medroxyprogesterone acetate Ashley M. Nault, BS; Jeffrey F. Peipert,
Research www.ajog.org GENERAL GYNECOLOGY Validity of perceived weight gain in women using long-acting reversible contraception and depot medroxyprogesterone acetate Ashley M. Nault, BS; Jeffrey F. Peipert,
VASECTOMY INFORMATION AND CONSENT
 VASECTOMY INFORMATION AND CONSENT This information will help you understand more about the vasectomy: the indications for this procedure, the success and failure rates, the alternative forms of contraception,
VASECTOMY INFORMATION AND CONSENT This information will help you understand more about the vasectomy: the indications for this procedure, the success and failure rates, the alternative forms of contraception,
Example Clinical Guideline for Immediate Postpartum LARC Insertion
 Example Clinical Guideline for Immediate Postpartum LARC Insertion RATIONALE Delay in contraceptive provision until the six week postpartum appointment can leave some women at risk for rapid repeat pregnancy.
Example Clinical Guideline for Immediate Postpartum LARC Insertion RATIONALE Delay in contraceptive provision until the six week postpartum appointment can leave some women at risk for rapid repeat pregnancy.
Contraception Choices: An Evidence Based Approach Case Study Approach. Susan Hellier PhD, DNP, FNP-BC, CNE
 Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
Postpartum LARC. (Long Acting Reversible Contraception) NURSING EDUCATION
 Postpartum LARC (Long Acting Reversible Contraception) NURSING EDUCATION What is LARC Long-acting reversible contraception (LARC) methods include the intrauterine device (IUD) and the birth control implant.
Postpartum LARC (Long Acting Reversible Contraception) NURSING EDUCATION What is LARC Long-acting reversible contraception (LARC) methods include the intrauterine device (IUD) and the birth control implant.
According to data from the 2006 to 2008 National Survey
 ORIGINAL RESEARCH Modeled Cost Differences Associated With Use of Levonorgestrel Intrauterine Devices Amy Law, PharmD; Mark McCoy, PharmD, MBA; Melissa Lingohr-Smith, PhD; Jay Lin, PhD, MBA; and Richard
ORIGINAL RESEARCH Modeled Cost Differences Associated With Use of Levonorgestrel Intrauterine Devices Amy Law, PharmD; Mark McCoy, PharmD, MBA; Melissa Lingohr-Smith, PhD; Jay Lin, PhD, MBA; and Richard
Aim For the Bullseye: Presented on 2/10/2016 for the NC Child Fatality Task Force. LARC and Pregnancy Prevention in NC
 Aim For the Bullseye: Presented on for the NC Child Fatality Task Force LARC and Pregnancy Prevention in NC 2 What is LARC? 3 L=Long A=Acting R=Reversible C=Contraception 4 Learning Objectives Describe
Aim For the Bullseye: Presented on for the NC Child Fatality Task Force LARC and Pregnancy Prevention in NC 2 What is LARC? 3 L=Long A=Acting R=Reversible C=Contraception 4 Learning Objectives Describe
