Prevalence and Impacts of Upper Limb Morbidity after Treatment for Breast Cancer: A Cross-Sectional Study of Lymphedema and Function
|
|
|
- Rosemary Simpson
- 6 years ago
- Views:
Transcription
1 Cancer and Oncology Research 1(2): 30-39, 2013 DOI: /cor Prevalence and Impacts of Upper Limb Morbidity after Treatment for Breast Cancer: A Cross-Sectional Study of Lymphedema and Function Catherine Bulley 1,*, Fiona Coutts 1, Christine Blyth 1, Wilma Jack 2, Mr Udi Chetty 2, Matthew Barber 2, Chee Wee Tan 1 1 School of Health Sciences, Queen Margaret University, Edinburgh, Queen Margaret University Drive, Musselburgh, East Lothian, EH21 6UU, United Kingdom 2 Western General Hospital, Breast Unit, Crewe Road South, Edinburgh, EH4 2XU, United Kingdom *Corresponding Author: cbulley@qmu.ac.uk Copyright 2013 Horizon Research Publishing All rights reserved. Abstract A cross-sectional study screened lymphedema, impaired upper limb function (ULF) and quality of life (QOL) in women post-breast cancer. Women attending review appointments who had completed surgery, chemotherapy and radiotherapy, were without recurrence, and could complete questionnaires in English were invited. Medical records were reviewed and questionnaires completed: the Morbidity Screening Tool (MST), Disability of the Arm, Shoulder and Hand questionnaire (DASH), and Functional Assessment of Cancer Therapy for breast cancer QOL questionnaire (FACTB+4). The vertical perometer (400T) measured percentage upper limb volume difference (%LVD), with 10% or greater difference diagnosed as lymphedema. Of 617 participants (mean age 62.3y, SD 10.0; mean time since treatment 63.0 months, SD 46.6), sufficient questionnaire data were available for 613 and perometry data for 417. Using the MST, 21.9% self-reported impaired ULF, 19.8% lymphedema, and 9.2% both. Based on %LVD, 26.5% had lymphedema. Histogram analysis for individuals in the first eight twelve-month intervals after treatment found impaired ULF prevalence peaked at three to five years and lymphedema at three years. Significantly worse function (DASH) and QOL (FACT B+4) resulted for those with morbidity (p<0.000). This provides evidence that impaired ULF and lymphedema negatively affect QOL years after treatment and are not necessarily linked. Keywords Lymphedema; Upper Limb Function; Prevalence; Quality of Life; Impacts 1. Introduction Increasing survival rates after breast cancer have led to greater focus on improving functional outcomes, reducing morbidity and improving quality of life. The necessary rigour of treatment can lead to long term morbidity, including impaired upper limb range of motion, strength and function, and swelling (lymphedema) that may develop immediately, or may emerge years later [1]. Lymphedema is an accumulation of interstitial fluid in the tissues due to interruption in the lymphatic system and can lead to skin fibrosis and cellulitis, as well as psychological sequelae. Prevalence estimates vary widely, from 2 to 86%, due to differences in study samples, measurement techniques, and diagnostic criteria [2]. Growing consensus indicates greater risk of lymphedema after axillary lymph node dissection (ALND), and radiotherapy to the axilla [3]. Previously, people have been recommended to avoid activity in the affected limb, with a link expected between treatment in the dominant limb and lymphedema, although this is unclear and requires further investigation [4].Several studies have compared breast cancer survivors with and without lymphedema, finding greater psychological morbidity and poorer function and quality of life in the former [5]. Reduced mobility of the shoulder, reduced grip strength, and pain can also develop, affecting work and activities of daily living [3,6]. A systematic review looking at prevalence of upper limb morbidity found wide variation, but concluded that impaired upper limb function is a long-term problem after breast cancer treatment, affecting quality of life [7]. However, several authors highlight the lack of understanding of relationships between late morbidity and activities of daily living, occupation, and quality of life [3,6,8]. Thomas-MacLean and colleagues advocate for research into inter-relationships between forms of arm morbidity, such as lymphedema and impaired upper limb function [8]. Lymphedema measurement often focuses on limb volume, using volumetry (water displacement), or calculations from circumferential measurement of segments of the limb. Perometry (opto-electronic scanning) and multifrequency
2 Cancer and Oncology Research 1(2): 30-39, bioelectrical impedance [1,9,10]. Lymphedema is frequently diagnosed through comparison of the affected and unaffected limbs, or within the same limb over time, most commonly specified as differences equal to or greater than 10%, 2cm, 5cm or 200ml in limb circumference or volume (as appropriate) [11]. A comparison study suggests that an increase in percentage limb volume of 10% or more is the most conservative classification, allowing for pre-existing bilateral limb volume differences [11]. Some evidence suggests that patient self-report provides an earlier and more sensitive diagnosis that does not rely on pre-operative limb volume measurements or expensive instrumentation and explores functional and psychosocial dimensions [1,4,11]. A combined approach is advocated by some [1]. Upper limb morbidity has been evaluated in various ways, including goniometry measurement of shoulder range of motion, dynamometry for grip strength, and self-report of pain and ability to perform activities of daily living [3]. Evidence suggests that when detected early, therapeutic intervention can lead to greater success in managing upper limb morbidity, with improved outcomes and quality of life [12], raising the importance of further investigation. A study was designed that screened for lymphedema and impaired arm function after breast cancer treatment, enabling investigation of the following research questions: 1. What are the prevalence rates of impaired upper limb function (ULF) and lymphedema in a cross-sectional sample of women who have completed treatment for breast cancer, and what is the relationship between the two? 2. How do the prevalence rates of impaired ULF and lymphedema differ between women who are at different time-points post-treatment in the sample? 3. To what extent do impaired ULF and lymphedema impact on quality of life, function and occupation of those within the sample, and do their impacts differ? 4. Does dominance of the treated limb affect prevalence of impaired ULF and lymphedema, and their impacts of morbidityon quality of life and function? A further research question, relating to relationships between morbidity and treatment characteristics, will be dealt with elsewhere. 2. Material and Methods 2.1. Study Design A cross-sectional study screened for impaired ULF and lymphedema in women who had completed treatment for breast cancer (surgery, chemotherapy and radiotherapy), between November 2009 and May The South East Scotland Research Ethics Committee classified this as service review and full ethical review was conducted within the Higher Education Institution Procedure and Measurement Women awaiting review appointments at the Breast Clinic, who did not have recurrence, and who could complete questionnaires in English were provided with information and a consent form. If willing, they completed a questionnaire booklet, and participated in objective tests in a private clinic room, and medical records were reviewed. The vertical perometer (400T) was used to objectively diagnose lymphedema where LVD was 10% or greater [11]. Evidence of validity and reliability exists in in women post-breast cancer, and with lymphedema [13,14]. A previously developed protocol was used to standardise the limb proportion being measured, position within the measurement frame, and rest period prior to testing Bulley et al., in press, European Journal of Physiotherapy Questionnaires included the DASH questionnaire [15]; the Functional Assessment of Cancer Therapy (FACTG) quality of life questionnaire with breast cancer sub-scale (FACTB) and additional questions relating to the upper limb (FACTB+4) [16]; anda Morbidity Screening Tool (MST) developed by the research group. The DASH Questionnaire focuses on day-to-day function of the upper limb and numerous studies support its psychometric properties in varied populations and translations [17].Previous research supports the reliability, validity and practicality of the FACT B and FACT B+4 [18]. The MST requests participant characteristics such as handedness and changes in occupation and then focuses on impaired ULFand lymphedema. It first establishes whether or not the person perceives that there is a problem, and then explores its impacts on activities and participation, as recommended by the World Health Organization [19]. Its validity was studied by investigating relationships with established objective (n=434) and subjective measures (n=613) Bulley et al., in press, Biomed Research International. These included Perometry limb volume measurement [9], upper limb combined range of motion (ROM) [20], the DASH and FACT B+4 questionnaires. Results supported use of the MST; for example, self-reported ULF impairment differentiated significantly as expected in relation to hand-behind-back range of motion (Mann Whitney U= ; p=0.001), DASH scores(u=7145.5; p<0.001), and FACT G scores(u= ; p<0.001). Self-reported lymphedema differentiated significantly as expected in relation to perometry percentage limb volume differences (%LVD) in those with unilateral treatment (U=112128; p<0.001), FACT G scores (u= ; p<0.001), and the FACT B+4 arm-specific subscale (u=9671.5; p<0.001) Analysis Non-normal distributions (Shapiro-Wilk test: p= ) led to selection of non-parametric analysis (significance set at p<0.05), using the Mann-Whitney U test (two groups) and Kruskal Wallis H test (multiple groups) for between-group differences; post-hoc analysis used the
3 32 Prevalence and Impacts of Upper Limb Morbidity After Treatment for Breast Cancer: A Cross-Sectional Study of Lymphedema and Function Mann-Whitney U test with Bonferroni corrections. Relationships were explored with the chi-square test for categorical variables. 3. Results Of 617 women who participated (approximately 46.6% recruitment rate) 613 had sufficient subjective data for analysis and 417 had subjective and objective data. A different response rate results for each analysis, due to variable questionnaire completion. Overall, participants were a mean age of 62.3 (complete data: n=595; SD 10.0; range years) and completed treatment (surgery and any chemotherapy or radiotherapy) 63.0 months (mean) previously (n=593; SD 46.6, range months). Of 596 with data, 7% (n=44) had bilateral breast cancer; of those with unilateral treatment, 25.5% received mastectomy and 73.6% wide local excision (WLE). Of 91.1% with unilateral axillary surgery 35.0% had full clearance, while 56.2% received either 4-node axillary sampling or sentinel lymph node biopsy (SLNB). Of 596 with data, 82.2% received breast radiotherapy, and 24.0% axillary. Out of 512, 40.2% received chemotherapy, and 75.2% received, or were still receiving, hormone therapy. 3.1 Prevalence of Impaired ULF, Lymphedema and Both As summarised in Table 1, approximately one fifth of participants self-reported impaired ULF, and one fifth lymphedema. Using perometry, 26.5% of 434 participants with unilateral treatment had lymphedema. Almost a tenth reported co-existence of impaired ULF and lymphedema. Table 1 provides participant characteristics for each of these categories and summarises inferential analysis: no significant differences in age were found between those self-reporting impaired upper limb function or not, lymphedema or not, and for those with both types of morbidity or not. from a median of 63.5 participants in each category, over the categories 21.6% impairment was reported (median no impairment = 49.5; impairment = 10.5). For lymphedema, there were 64.5 participants per category (median), with 22.8% impairment reported over the categories (median: no impairment = 51.5; impairment = 12.0). Figures 1 and 2 illustrate the differences in percentage impairment reported over each of the eight years; prevalence of impaired ULF in the sample peaked in the groups who were three to five years post-treatment, while prevalence of lymphedema was greatest year three, and then remained fairly static Impacts of Morbidity Comparison of DASH and FACT B subscale scores was undertaken for those responding they had impaired ULF, lymphedema, both, and neither (n=473), summarised in Table 2. The Kruskal Wallis H test found significant differences between the four groups. Post hoc analysis (Mann-Whitney U test; Bonferroni correction requiring p<0.008) found significant differences (p<0.007) in all groups for all variables, with the exceptions of comparisons between those with only impaired ULF and those with only lymphedema (DASH: U=1298.4, p=0.117; FACTB: U=1499.0, p=0.690; Breast cancer subscale: U=1205.0, p=0.035; Arm subscale: U=1248.5, p=0.061), and between those with neither type of morbidity and those with impaired ULF: for the Breast cancer subscale score only (U=7156.5, p=0.009). Lastly, relationships between morbidity and occupational status categories were explored (Table 3). Chi 2 results were statistically significant for both impaired ULF and lymphedema, supporting the negative impacts of morbidity. Descriptively, 14.4% of people with impaired ULF and 15.5% with lymphedema self-reported that they had stopped working since their breast cancer treatment, compared with 5.8% and 6.1% of those without impairment. Upper limb morbidity appears to be associated with negative changes in occupational status Differences in Morbidity Prevalence with Time since Treatment Table 1 summarises descriptive and inferential analysis comparing months since treatment according to morbidity category; no statistically significant differences were found for participants with self-reported impaired upper limb function and those without, for those with lymphedema and those without and for those with both types of morbidity and those with either type or neither.histogram analysis explored differences in prevalence of morbidity in participants who were in the first to eighth 12-month time interval categories post-treatment, where n>30 for each. For impaired ULF, 3.4. Relationships between Morbidity and Dominance of the Limb Treated Table 4 demonstrates that for those with self-reported impaired ULF and lymphedema, proportions of people treated on their dominant and non-dominant sides are approximately equal, with no significant difference in the impacts of treatment according to DASH and FACT B (and subscale) scores. The only borderline statistically significant result was that higher quality of life scores relating to breast cancer symptoms were found in those with impaired ULF who were not treated in their dominant limb.
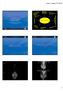
4 Cancer and Oncology Research 1(2): 30-39, Figure 1. Percentage prevalence of impaired upper limb function during the first eight years post-treatment Figure 2. Percentage prevalence of lymphedema during the first eight years post-treatment
5 34 Prevalence and Impacts of Upper Limb Morbidity After Treatment for Breast Cancer: A Cross-Sectional Study of Lymphedema and Function Table 1. Perceived morbidity prevalence according to the Morbidity Screening Tool and participant characteristics Perceived impaired upper limb function Perceived lymphedema Both impaired upper limb function and lymphedema Perceived morbidity - n (% 1): (response=580 2; 595 3; 575 4) Yes No Yes No Yes No (78.1%) (19.8%) (80.2%) (9.2%) 127 (21.9%) 522 (90.8%) Age (years): median (range) (response=580 2; 595 3; 575 4) ( ) ( ) ( ) ( ) ( ) ( ) Mann-Whitney U Test U=28093, Z=-0.401, p=.69 U= , Z=-1.18, p=.24 U= , Z=-0.28, p=.78 Monthssince treatment: median (range) (response=575 1; 590 2; 570 3) ( ) ( ) ( ) ( ) ( ) ( ) Mann-Whitney U Test U=27949, Z=-0.21, p=.84 U=27768, Z=-0.48, p=.96 U= , Z=-0.59, p =.55 Unilateral cancer - n (% 1): (response=558 2; 571 3; 555 4) 111 (91.74) 406 (92.91) 104 (91.23) 424 (92.78) 49 (92.45) 465 (92.63) Mastectomy - n (% 1): (response=555 2; 569 3; 550 4) 39 (32.23) 114 (26.27) 42 (36.21) 118 (26.05) 21 (40.38) 132 (26.51%) Wide Local Excision - n (% 1): (response=557 2; 571 3; 552 4) 83 (68.60) 326 (74.77) 75 (64.66) 341 (74.95) 31 (59.62) 373 (74.60) Axillary full node clearance - n (% 1): (response=556 2; 570 3; 551 4) 49 (40.50) 149 (34.25) 70 (59.83) 137 (30.24) 29 (55.77) 169 (33.87) Axillary sampling / SLNB 5 - n (% 1): (response=556 2; 570 3; 551 4) 66 (54.55) 259 (59.54) 47 (40.17) 282 (62.25) 23 (44.23) 298 (59.72) Radiotherapy to the breast - n (% 1): (response=561 2; 576 3; 556 4) 100 (81.97) 364 (82.92) 95 (80.51) 380 (82.97) 41 (77.36) 418 (83.10) Radiotherapy to the axilla - n (% 1): (response=560 2; 575 3; 555 4) 35 (28.69) 104 (23.74) 37 (31.36) 104 (22.76) 15 (28.30) 122 (24.30) Chemotherapy - n (% 1): (response=486 2; 496 3; 486 4) 44 (42.31) 151 (39.53) 53 (53.54) 147 (37.03) 17 (41.46) 177 (39.78) 1. % of respondents with relevant treatment who do / do not self-report morbidity 2. Perceived impaired upper limb function: response rate for item 3. Perceived lymphedema: response rate for item 4. Perceived impaired upper limb function and lymphedema: response rate for item 5. Four-node axillary sampling or sentinel lymph node biopsy
6 Cancer and Oncology Research 1(2): 30-39, Table 2. Comparison of DASH and FACT B scores for those with impaired upper limb function, with lymphedema, with both, and with neither: descriptive and inferential analysis People who perceive themselves (MST 1) to have: Neither impaired upper limb function / lymphoedema Impaired upper limb function only Lymphoedema only Both impaired upper limb function and lymphoedema N (%) 321 (67.9) 57 (12.1) 55 (11.6) 40 (8.5) Median (range) DASH 2 score 2.6 ( ) Kruskal Wallis H Test Chi 2 =125.0; p=0.000 Median (range) FACTB 3 score ( ) Kruskal Wallis H Test Chi 2 =59.0; p=0.000 Median (range) breast cancer subscale score 29.0 ( ) Kruskal Wallis H Test Chi 2 =65.7; p=0.000 Median (range) arm subscale score 20.0 ( ) Kruskal Wallis H Test Chi 2 =156.5; p= ( ) ( ) 27.0 ( ) 17.0 ( ) 1. MST: Morbidity Screening Tool; 2. DASH: Disability of the Arm, Shoulder and Hand questionnaire; 3. FACT-B: Functional Assessment of Cancer Therapy Breast Cancer specific quality of life questionnaire. 8.3 ( ) ( ) 25.0 ( ) 16.0 ( ) 25.0 ( ) 97.4 ( ) 22.0 ( ) 13.1 ( ) Table 3. Cross-tabulation of upper limb impairment and lymphedema with occupational status since breast cancer treatment (frequency) Upper limb impairment Lymphedema Self-report (MST 1) No Yes No Yes Employment ceased: n (%) 24 (57.1) 18 (42.9) 26 (60.5) 17 (39.5) Reduced hours of employment: n (%) 23 (85.2) 4 (14.8) 20 (74.1) 7 (25.9) No change in hours of employment: n (%) 199 (82.6) 42 (17.4) 198 (82.5) 42 (17.5) Increased hours of employment: n (%) 2 (50.0) 2 (50.0) 3 (75.0) 1 (25.0) Not applicable 2: n (%) 165 (73.7) 59 (26.3) 181 (80.8) 43 (19.2) Total: n Chi 2 with 4 degrees of freedom , p= , p= MST: Morbidity Screening Tool; 2. Not applicable, for example, retired from employment before treatment for breast cancer
7 36 Prevalence and Impacts of Upper Limb Morbidity After Treatment for Breast Cancer: A Cross-Sectional Study of Lymphedema and Function Table 4. Analysis of the differences in DASH and FACT B subscale scores according to treatment in the dominant or non-dominant limb for those with self-reported impaired upper limb function and lymphedema Those with impaired ULF (MST 1): treated in the dominant limb (n=97) Those with lymphedema (MST 1): treated in the dominant limb (n=94) Yes No Yes No N (%) 48 (49.5) 49 (50.5) 47 (50) 47 (50) Median (range) DASH 2 score 18.1 ( ) 17.5 ( ) 15.8 ( ) 15.2 ( ) Mann-Whitney U Test U=1163.5; p=0.928 U=1059.0; p=0.731 Median (range) FACT-B 3 subscale score ( ) ( ) ( ) ( ) Mann-Whitney U Test U=949.0; p=0.102 U=1068.0; p=0.783 Median (range) breast cancer subscale score 22.5 ( ) 26.0 ( ) 23.9 ( ) 24.0 ( ) Mann-Whitney U Test U=904.5; p=0.050 U=1055.0; p=0.708 Median (range) arm subscale score 16.0 ( ) 16.0 ( ) 16.0 ( ) Mann-Whitney U Test U=1157.0; p=0.890 U=1025.5; p= MST: Morbidity Screening Tool; 2. DASH: Disability of the Arm, Shoulder and Hand questionnaire; 3. FACT-B: Functional Assessment of Cancer Therapy Breast Cancer specific quality of life questionnaire ( ) 4. Discussion Some interesting insights into upper limb morbidity have been found and are discussed in turn. When comparing participant characteristics with one UK and one US study published in the previous six years [21,22], variations are not substantial considering such a heterogeneous population Prevalence of Impaired Upper Limb Function and Lymphedema and Relationships with Dominance of the Limb Treated The current study found similar proportions of about one fifth of participants self-reportingimpaired ULF and lymphedema, but under a tenth self-reported both, suggesting that they are not frequently linked. Fewer studies have looked at the prevalence of impaired ULF than lymphedema, but one recent systematic review included 32 longitudinal or cross-sectional studies and found decreased shoulder ROM varied from 1% to 67% prevalence (7 studies), and arm weakness, 9 to 28% (3 studies) [7]. Incidence rates were lowest when estimated by clinicians rather than from objective measurement or participant self-report; the latter was used by the current study, possibly explaining the prevalence estimate being at the mid-to-high end of the estimate range [7]. The current study s prevalence estimate for lymphedema is again at the higher end of the range found in the previously mentioned systematic review, 0-34% [7]. In the ALMANAC trial, at eighteen months from baseline, 8.4% of ALND patients and 3.8% with SLNB self-reported swollen or tender arms using the FACT B+4 arm subscale [21]. A recent study of incidence and course of lymphedema (circumferential measurement) six-to-twelve months post-surgery in 347 women found incidence rates of 9-16% depending on the criterion used, averaging 12% 8. Current findings are higher than both studies, possibly reflecting the high upper range of time since treatment, as evidence suggests incidence or prevalence estimates increase with
8 Cancer and Oncology Research 1(2): 30-39, longer follow-up [3]. The previously mentioned study [8] also investigated shoulder abduction and external rotation (10% difference indicated deficit); impairments were found in 41% and 28% respectively. Although both are greater than prevalence of impaired ULF in the current study a very similar result of under 10% of participants reporting both lymphedema and impaired ULF was found, supporting the finding that they are not related in the majority of participants. The current study found perometry measurement estimated lymphedema prevalence 7% higher than self-report; lower estimates from self-report were also found in a study of 211 women 2.5 years post-treatment: 41% compared with 45% (perometry: 10% change pre-to-post treatment) [22]. An earlier study of 176 women found the opposite, 27.8% from self-report and 11.9%, 0.6% and 11.4% found by objective criteria (summed arm circumferences: difference >5cm or >10%; multifrequency bioimpedance: 3+SD above reference score) [23]. Therefore, the relationship between subjective and objective prevalence estimation is unclear. The large number of participants in the current study enabled comparisons of prevalence in women at different time-points post-treatment, finding that impaired ULF was highest at three to five years post-treatment, while lymphedema peaked at 28% at three years. Prospective studies of lymphedema incidence have found similar results, for example, incidence increased from 20% at six months, to 32% with persistent swelling at three years (n=622) [24]. Although investigated less in relation to ULF, one study of impaired arm movement found some reduction over four years from 37 to 26% prevalence [25]. The persistence of arm problems over time in some women supports the current study findings. The current study found no evidence that prevalence and impacts of morbidity are greater when treated in the dominant limb. Evidence increasingly suggests that greater use of the dominant treated limb is beneficial; one study found 80% greater risk of lymphedema with treatment in the non-dominant limb [23] Impacts of Impaired Upper Limb Function and Lymphedema The current study found that for those self-reporting impaired ULF, and those with lymphedema, significantly poorer function and quality of life resulted, and co-existence of both provided significantly worse scores than either. A review of the literature on health-related quality of life found poorer psychological well-being in those with lymphedema than the general population. Qualitative literature highlights contributions from fear, frustration, and poor body image [5] and significantly worse FACT B scores have been found in women with lymphedema than matched controls [24]. A change of at least five points in the FACT B has been stated to be clinically relevant [21]. Score differences in the current study were well above this threshold: between those with no impairment and those with impaired ULF (10 points), lymphedema (7 points), and both (28 points). The current study also provided evidence that UL morbidity can be associated with negative occupational changes. One recent study found between 11-44% of 3253 women, depending on treatment group, gave up activities after breast cancer treatment, and over a third of those working felt that this had been affected [2]. These data further support the increasing trend towards avoiding over-treatment of the axilla [3]. Although it is positive to note the increasing consensus regarding reduced risk of arm morbidity following SLNB, risk of morbidity remains, as the long-term effects are not yet known and a proportion of women will still require more extensive axillary surgery. There is evidence that earlier detection and management are most likely to be successful [12]. Therefore timely screening for morbidity should be part of follow-up care [8] and management of upper limb morbidity is important to improve function and quality of life after breast cancer treatment Study Considerations The current study is cross-sectional, and some women may have returned to clinic review sessions after longer periods post-treatment due to upper limb morbidity, rather than other concerns. Treatment protocols are likely to have developed over the time period, which could have increased morbidity prevalence in those with a longer time since treatment. However, the lack of significant differences in time since treatment among those who did or did not self-report impairment does not support these suggestions. 5. Conclusion To conclude, the current study findings found approximately a fifth of the study sample to have lymphedema, a fifth to have impaired upper limb function, and only 9% to have symptoms of both. Prevalence of impaired ULF appeared to be greatest among women who were three to five years post treatment, and prevalence of lymphedema peaked at three years, suggesting that upper limb morbidity is an ongoing problem after treatment for breast cancer. Statistically significant reductions in daily function and quality of life were evident in those with morbidity supported by negative impacts on occupational status. These insights into prevalence and impacts of upper limb morbidity expand our current understanding of the relationships between lymphedema and other forms of upper limb function, and their differential impacts on activities, participation in occupational roles and general quality of life, as well as providing further support for the chronicity of morbidity. The results support the need for timely screening as part of follow-up care and early management to improve function and quality of life after breast cancer treatment.
9 38 Prevalence and Impacts of Upper Limb Morbidity After Treatment for Breast Cancer: A Cross-Sectional Study of Lymphedema and Function Ongoing prospective investigation of these issues will be important as treatment protocols for breast cancer continue to develop, and further development and evaluation of screening and management strategies will be valuable. Acknowledgments We gratefully acknowledge the financial support of the Breast Cancer Institute in funding this study; they had no further involvement in data collection, analysis, interpretation or reporting, and encouraged submission for publication without any influence over the content. We also thank the Breast Unit staff, who provided great assistance in making this project possible. We would also like to thank all the participants in the study, and Miss Lindsay Dick and Miss Erin McGowan for carrying out data collection. REFERENCES [1] J. Armer, M. Radina, D. Porock, S. Culbertson. Predicting breast cancer-related lymphedema using self-reported symptoms. Nursing Research, Vol. 52, 370-9, [2] R. Gärtner, M.B. Jensen, L. Kronborg, M. Ewertz, H. Kehlet, N. Kroman. Self-reported arm-lymphedema and functional impairment after breast cancer treatment - A nationwide study of prevalence and associated factors. The Breast, Vol. 19, , [3] J.S. Rietman, P.U. Dijkstra, J.H.B. Geertzen, P. Baas, J. De Vries, W. Dolsma, J.W. Groothoff, W.H. Eisma, H.J. Hoekstra. Short-term morbidity of the upper limb after sentinel lymph node biopsy or axillary lymph node dissection for Stage I or II breast carcinoma. Cancer, Vol. 98, 690-6, [4] S.A. McLaughlin, M.J. Wright, K.T. Morris, M.R. Sampson, J.P. Brockway, K.E. Hurley, E.R. Riedel, K.J. Van Zee. Prevalence of lymphedema in women with breast cancer 5 years after Sentinel Lymph Node Biopsy or Axillary Dissection: patient perceptions and precautionary behaviors. Journal of Clinical Oncology, 26, , [5] P.A. Morgan, P.J. Franks, C.J. Moffatt. Health-related quality of life with lymphoedema: a review of the literature. International Wound Journal, Vol. 2, 47-62, [6] K. Johansson, C. Ingvar, M. Albertsson, C. Ekdahl. Arm lymphoedema, shoulder mobility and muscle strength after breast cancer treatment.a prospective 2 year study. Advances in Physiotherapy, Vol. 3, 55 66, [7] T.S. Lee, S.L. Kilbreath, K.M. Refshouge, R.D. Herbert, J.M. Beith. Prognosis of the upper limb following surgery and radiation for breast cancer. Breast Cancer Research and Treatment, Vol. 110, 19-37, [8] R.L. Thomas-MacLean, T. Hack, W. Kwan, A. Towers, B. Miedema, A. Tilley. Arm morbidity and disability after breast cancer: New directions for care. Oncology Nursing Forum, Vol. 35, 65-70, [9] A.W.B. Stanton, J.W. Northfield, B. Holroyd, P.S. Mortimer, J.R. Levick. Validation of an optelectronic limb volumeter (Perometer). Lymphology, Vol. 30, 77-97, [10] B.H. Cornish, B.E. Lingwood, L.C. Ward. Can bioimpedancespectroscopy (BIS) tell us about the form of lymphoedema? 13th International Conference on Electrical Bioimpedance and the 8th Conference on Electrical Impedance Tomography IFMBE Proceedings 2007, Vol. 17, 795-8, [11] J. Armer, B. StewartB. A comparison of four diagnostic criteria for lymphedema in a post-breast cancer population. Lymphatic Research and Biology, Vol. 3, , [12] J. Armer. The problem of post-breast cancer lymphedema: impact and measurement issues. Cancer Investigation, Vol. 1, 76-83, [13] T. Deltombe, J. Jamart, S. Recloux, C. Legrand, N. Vandenbroeck, S. Theys, P. Hanson. Reliability and limits of agreement of circumferential, water displacement, and optoelectronic volumetry in the measurement of upper limb lymphedema. Lymphology, Vol. 40, 26-34, [14] S.A. Czerniec, L.C. Ward, K.M. Refshauge, J. Beith, M.J. Lee, S. York, S.L. Kilbreath. Assessment of breast cancer-related arm lymphedema comparison of physical measurement methods and self-report. Cancer Investigation, Vol. 28, 54-62, [15] P. Hudak, P.C. Amadio, C. Bombardier, and the Upper Extremity Collaborative Group. Development of an upper extremity outcome measure: The DASH (Disabilities of the Arm, Shoulder, and Hand). American Journal of Industrial Medicine, Vol. 29, 602-8, [16] D. Cella, D. Tulsky, G. Gray, B. Sarafian, E. Linn, A. Bonomi, M. Silberman, S.B. Yellen, P. Winicour, J. Brannon. The Functional Assessment of Cancer Therapy scale: development and validation of the general measure. Journal of Clinical Oncology, Vol. 11, 570-9, [17] T. Westphal, S. Piatek, S. Schubert, T. Schuschke, S. Winckler. Reliability and validity of the upper limb DASH questionnaire in patients with distal radius fractures. Zeitschrift fur Orthopadie und IhreGrenzgebiete, Vol. 140, , [18] M.J. Brady, D.F. Cella, F. Mo, A.E. Bonomi, D.S. Tulsky, S.R. Lloyd, S. Deasy, M. Cobleigh, G. Shiomoto. Reliability and validity of the Functional Assessment of Cancer Therapy - Breast quality-of-life instrument. Journal of Clinical Oncology, Vol. 15, , [19] World Health Organisation. International Classification of Functioning, Disability and Health, WHO, Geneva, [20] American Academy of Orthopaedic Surgeons. Joint motion: method of measuring and recording, Churchill Livingstone, New York, [21] A. Fleissig, L.J. Fallowfield, C.I. Langridge, L. Johnson, R.G. Newcombe, J.M. Dixon, M. Kissin, R.E. Mansel. Post-operative arm morbidity and quality of life. Results of the ALMANAC randomized trial comparing sentinel node biopsy with standard axillary treatment in the management of patients with early breast cancer. Breast Cancer Research and Treatment, Vol. 95, , [22] J. Armer, B. Stewart, R. Shook. 30-month post-breast cancer
10 Cancer and Oncology Research 1(2): 30-39, treatment lymphoedema. Journal of Lymphoedema, Vol. 4, 14-8, [23] S. Hayes, B. Cornish, B. Newman. Comparison of methods to diagnose lymphoedema among breast cancer survivors: 6-month follow-up. Breast Cancer Research and Treatment, Vol. 89, 221-6, [24] E. D. Paskett, M.J. Naughton, T.P. McCoy, L.D. Case, J.M. Abbott. The epidemiology of arm and hand swelling in premenopausal breast cancer survivors. Cancer Epidemiology Biomarkers and Prevention, Vol.16, , [25] J. Engel, J. Kerr, Schlesinger-Raab, H. Sauer, D. Hölzel. Axilla surgery severely affects quality of life: results of a 5-year prospective study in breast cancer patients. Breast Cancer Research and Treatment, Vol. 79, 47-57, 2003.
Catherine Bulley, 1 Susanne Gaal, 1 Fiona Coutts, 1 Christine Blyth, 1 Wilma Jack, 2 Udi Chetty, 2 Matthew Barber, 2 and Chee-Wee Tan 1
 BioMed Research International Volume 2013, Article ID 807569, 8 pages http://dx.doi.org/10.1155/2013/807569 Research Article Comparison of Breast Cancer-Related Lymphedema (Upper Limb Swelling) Prevalence
BioMed Research International Volume 2013, Article ID 807569, 8 pages http://dx.doi.org/10.1155/2013/807569 Research Article Comparison of Breast Cancer-Related Lymphedema (Upper Limb Swelling) Prevalence
Improving best practices for diagnosing lymphedema
 Research Perspectives Improving best practices for diagnosing lymphedema A proposal to assess limbs according to segment Assessing limb segments can change the rate of diagnosis for lymphedema Introduction
Research Perspectives Improving best practices for diagnosing lymphedema A proposal to assess limbs according to segment Assessing limb segments can change the rate of diagnosis for lymphedema Introduction
EFFICACY OF DECONGESTIVE THERAPY AND INTERMITTENT PNEUMATIC COMPRESSION IN PATIENTS WITH LYMPHEDEMA OF THE ARM AFTER BREAST CANCER TREATMENT
 EFFICACY OF DECONGESTIVE THERAPY AND INTERMITTENT PNEUMATIC COMPRESSION IN PATIENTS WITH LYMPHEDEMA OF THE ARM AFTER BREAST CANCER TREATMENT Dragana Bojinović-Rodić MD, PhD Institute of Physical Medicine
EFFICACY OF DECONGESTIVE THERAPY AND INTERMITTENT PNEUMATIC COMPRESSION IN PATIENTS WITH LYMPHEDEMA OF THE ARM AFTER BREAST CANCER TREATMENT Dragana Bojinović-Rodić MD, PhD Institute of Physical Medicine
30-month post-breast cancer treatment lymphoedema. Jane M Armer, Bob R Stewart, Robin P Shook
 30-month post-breast cancer treatment lymphoedema Jane M Armer, Bob R Stewart, Robin P Shook Abstract Background: Quantification of lymphoedema (LE) has been problematic, and the reported incidence of
30-month post-breast cancer treatment lymphoedema Jane M Armer, Bob R Stewart, Robin P Shook Abstract Background: Quantification of lymphoedema (LE) has been problematic, and the reported incidence of
Bioimpedance Devices for Detection and Management of Lymphedema
 Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2017 Origination: 1/2011 Next Review: 5/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2017 Origination: 1/2011 Next Review: 5/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Bioimpedance Devices for Detection and Management of Lymphedema
 2.01.82 Bioimpedance Devices for Detection and Management of Lymphedema Section 2.0 Medicine Subsection Effective Date January 30, 2015 Original Policy Date July 2, 2010 Next Review Date January 2015 Medical
2.01.82 Bioimpedance Devices for Detection and Management of Lymphedema Section 2.0 Medicine Subsection Effective Date January 30, 2015 Original Policy Date July 2, 2010 Next Review Date January 2015 Medical
Section: Durable Medical Equipment Last Reviewed Date: June Policy No: 82 Effective Date: September 1, 2014
 Medical Policy Manual Topic: Bioimpedance Devices for Detection and Management of Lymphedema Date of Origin: April 2011 Section: Durable Medical Equipment Last Reviewed Date: June 2014 Policy No: 82 Effective
Medical Policy Manual Topic: Bioimpedance Devices for Detection and Management of Lymphedema Date of Origin: April 2011 Section: Durable Medical Equipment Last Reviewed Date: June 2014 Policy No: 82 Effective
Breast Imaging. Jamie L. Wagner, DO, FACOS. Digital vs Analog Mammography (2-D) Surgical Oncologist. Patient with Cancer. Radiology/ Interventional
 Breast Cancer Prevention, Treatment, and Survivorship Jamie L. Wagner, DO, FACOS Assistant Professor Chief, Division of Breast Surgery Department of Surgery Anesthesiology Surgical Oncologist Patient with
Breast Cancer Prevention, Treatment, and Survivorship Jamie L. Wagner, DO, FACOS Assistant Professor Chief, Division of Breast Surgery Department of Surgery Anesthesiology Surgical Oncologist Patient with
Measuring change in limb volume to evaluate lymphoedema treatment outcome
 adrid Spain EWMA n GNEAUPP 2014 Submitted to EWMA Journal, based on a presentation given at a free paper session (Free paper session: Quality of life) at the EWMA - GNEAUPP 2014, Madrid Measuring change
adrid Spain EWMA n GNEAUPP 2014 Submitted to EWMA Journal, based on a presentation given at a free paper session (Free paper session: Quality of life) at the EWMA - GNEAUPP 2014, Madrid Measuring change
Lymphoedema following treatment for breast cancer: a new approach to an old problem
 Lymphoedema following treatment for breast cancer: a new approach to an old problem Screening breast cancer patients for lymphoedema makes it possible to identify problems early and take action to halt
Lymphoedema following treatment for breast cancer: a new approach to an old problem Screening breast cancer patients for lymphoedema makes it possible to identify problems early and take action to halt
Debate Axillary dissection - con. Prof. Dr. Rodica Anghel Institute of Oncology Bucharest
 Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Early detection and prevention of lymphoedema
 Early detection and prevention of lymphoedema Katie Riches Senior Research Nurse Derby Hospitals NHSF Trust Background: Derby Lymphoedema Service Three lymphoedema services based in Acute Hospitals at
Early detection and prevention of lymphoedema Katie Riches Senior Research Nurse Derby Hospitals NHSF Trust Background: Derby Lymphoedema Service Three lymphoedema services based in Acute Hospitals at
Physiological effects of aquatic physiotherapy in women with lower limb lymphoedema compared to healthy women.
 Griffith Research Online https://research-repositorygriffitheduau Physiological effects of aquatic physiotherapy in women with lower limb lymphoedema compared to healthy women Author Reul-Hirche, Hildegard
Griffith Research Online https://research-repositorygriffitheduau Physiological effects of aquatic physiotherapy in women with lower limb lymphoedema compared to healthy women Author Reul-Hirche, Hildegard
Axillary Reverse Mapping to Reduce the Incidence of Lymphedema
 Axillary Reverse Mapping to Reduce the Incidence of Lymphedema Nathalie Johnson,MD,FACS Medical Director, Legacy Cancer Institute and Breast Health Centers Portland,Oregon Objectives for Learning Understand
Axillary Reverse Mapping to Reduce the Incidence of Lymphedema Nathalie Johnson,MD,FACS Medical Director, Legacy Cancer Institute and Breast Health Centers Portland,Oregon Objectives for Learning Understand
Submitted by: Date of request: 28 th October 2015
 Submitted by: Frank Vicini, MD, FACR Chief Medical Officer ImpediMed, Inc. 5900 Pasteur Court Suite 125 Carlsbad, CA 92008 Phone: 760 585 2100 Email: fvicini@impedimed.com Date of request: 28 th October
Submitted by: Frank Vicini, MD, FACR Chief Medical Officer ImpediMed, Inc. 5900 Pasteur Court Suite 125 Carlsbad, CA 92008 Phone: 760 585 2100 Email: fvicini@impedimed.com Date of request: 28 th October
Clinical Policy Title: Bioimpedance devices for detecting lymphedema
 Clinical Policy Title: Bioimpedance devices for detecting lymphedema Clinical Policy Number: 05.01.06 Effective Date: June 1, 2017 Initial Review Date: April 19, 2017 Most Recent Review Date: May 19, 2017
Clinical Policy Title: Bioimpedance devices for detecting lymphedema Clinical Policy Number: 05.01.06 Effective Date: June 1, 2017 Initial Review Date: April 19, 2017 Most Recent Review Date: May 19, 2017
Lymphedema. Kelly Reichart, DNP, RN. About 246,660 women
 ADVANCED PRACTICE ASSOCIATE EDITOR DEBORAH "HUTCH" ALLEN, PhD, RN, CNS, FNP-BC, AOCNP Downloaded on 11 28 2018. Single-user license only. Copyright 2018 by the Oncology Nursing Society. For permission
ADVANCED PRACTICE ASSOCIATE EDITOR DEBORAH "HUTCH" ALLEN, PhD, RN, CNS, FNP-BC, AOCNP Downloaded on 11 28 2018. Single-user license only. Copyright 2018 by the Oncology Nursing Society. For permission
Sentinel Lymph Node Biopsy for Breast Cancer
 Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
The impact of Lymphedema on occupational performance, an opportunity for Occupational Therapy. Byron Shier, MBA, B.Sc. OT, CLT-LANA, CHE.
 The impact of Lymphedema on occupational performance, an opportunity for Occupational Therapy Byron Shier, MBA, B.Sc. OT, CLT-LANA, CHE. CLR Healthcare Inc. Presentation at 2013 Canadian Association of
The impact of Lymphedema on occupational performance, an opportunity for Occupational Therapy Byron Shier, MBA, B.Sc. OT, CLT-LANA, CHE. CLR Healthcare Inc. Presentation at 2013 Canadian Association of
RELIABILITY AND LIMITS OF AGREEMENT OF CIRCUMFERENTIAL, WATER DISPLACEMENT, AND OPTOELECTRONIC VOLUMETRY IN THE MEASUREMENT OF UPPER LIMB LYMPHEDEMA
 1 Lymphology 40(2007) 26-34 RELIABILITY AND LIMITS OF AGREEMENT OF CIRCUMFERENTIAL, WATER DISPLACEMENT, AND OPTOELECTRONIC VOLUMETRY IN THE MEASUREMENT OF UPPER LIMB LYMPHEDEMA T. Deltombe, J. Jamart,
1 Lymphology 40(2007) 26-34 RELIABILITY AND LIMITS OF AGREEMENT OF CIRCUMFERENTIAL, WATER DISPLACEMENT, AND OPTOELECTRONIC VOLUMETRY IN THE MEASUREMENT OF UPPER LIMB LYMPHEDEMA T. Deltombe, J. Jamart,
A NOVEL, VALIDATED METHOD TO QUANTIFY BREAST CANCER-RELATED LYMPHEDEMA (BCRL) FOLLOWING BILATERAL BREAST SURGERY
 64 Lymphology 46 (2013) 64-74 A NOVEL, VALIDATED METHOD TO QUANTIFY BREAST CANCER-RELATED LYMPHEDEMA (BCRL) FOLLOWING BILATERAL BREAST SURGERY C.L. Miller, M.C. Specht, N. Horick, M.N. Skolny, L.S. Jammallo,
64 Lymphology 46 (2013) 64-74 A NOVEL, VALIDATED METHOD TO QUANTIFY BREAST CANCER-RELATED LYMPHEDEMA (BCRL) FOLLOWING BILATERAL BREAST SURGERY C.L. Miller, M.C. Specht, N. Horick, M.N. Skolny, L.S. Jammallo,
Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer
 HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
Evaluation of shoulder girdle strength more than 12 month after modified radical mastectomy and axillary nodes dissection
 Original Article Evaluation of shoulder girdle strength more than 12 month after modified radical mastectomy and axillary nodes dissection Mahdieh Akoochakian, Heidar Ali Davari 1, Mohammad Hossein Alizadeh
Original Article Evaluation of shoulder girdle strength more than 12 month after modified radical mastectomy and axillary nodes dissection Mahdieh Akoochakian, Heidar Ali Davari 1, Mohammad Hossein Alizadeh
Bioimpedance Devices for Detection and Management of Lymphedema
 Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2018 Origination: 1/2011 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2018 Origination: 1/2011 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Audit. Public Health Monitoring Report on 2006 Data. National Breast & Ovarian Cancer Centre and Royal Australasian College of Surgeons.
 National Breast & Ovarian Cancer Centre and Royal Australasian College of Surgeons Audit Public Health Monitoring Report on 2006 Data November 2009 Prepared by: Australian Safety & Efficacy Register of
National Breast & Ovarian Cancer Centre and Royal Australasian College of Surgeons Audit Public Health Monitoring Report on 2006 Data November 2009 Prepared by: Australian Safety & Efficacy Register of
The Standard of Care for Lymphedema: Current Concepts and Physiological Considerations
 The Standard of Care for Lymphedema: Current Concepts and Physiological Considerations Harvey N. Mayrovitz PhD Professor of Physiology College of Medical Sciences Nova Southeastern University mayrovit@nova.edu
The Standard of Care for Lymphedema: Current Concepts and Physiological Considerations Harvey N. Mayrovitz PhD Professor of Physiology College of Medical Sciences Nova Southeastern University mayrovit@nova.edu
BREAST CANCER SITE STUDY REPORT By Robert O. Maganini, M.D., F.A.C.S. Breast Surgeon, Alexian Brothers Medical Group
 BREAST CANCER SITE STUDY REPORT By Robert O. Maganini, M.D., F.A.C.S. Breast Surgeon, Alexian Brothers Medical Group Breast cancer is the most common cancer diagnosed in women around the world. In the
BREAST CANCER SITE STUDY REPORT By Robert O. Maganini, M.D., F.A.C.S. Breast Surgeon, Alexian Brothers Medical Group Breast cancer is the most common cancer diagnosed in women around the world. In the
Incidence and risk of arm oedema following treatment for breast cancer: a three-year follow-up study
 Q J Med 2005; 98:343 348 Advance Access publication 8 April 2005 doi:10.1093/qjmed/hci053 Incidence and risk of arm oedema following treatment for breast cancer: a three-year follow-up study B. CLARK,
Q J Med 2005; 98:343 348 Advance Access publication 8 April 2005 doi:10.1093/qjmed/hci053 Incidence and risk of arm oedema following treatment for breast cancer: a three-year follow-up study B. CLARK,
Northumbria Healthcare NHS Foundation Trust. Breast Sentinel Lymph Node Biopsy. Issued by the Breast Team
 Northumbria Healthcare NHS Foundation Trust Breast Sentinel Lymph Node Biopsy Issued by the Breast Team Why do my Lymph Nodes require investigation? The lymphatic system is a pathway of lymph vessels and
Northumbria Healthcare NHS Foundation Trust Breast Sentinel Lymph Node Biopsy Issued by the Breast Team Why do my Lymph Nodes require investigation? The lymphatic system is a pathway of lymph vessels and
ORIGINAL ARTICLE BREAST ONCOLOGY. Ann Surg Oncol DOI /s z
 Ann Surg Oncol DOI 10.1245/s10434-016-5315-z ORIGINAL ARTICLE BREAST ONCOLOGY Implementing the Prospective Surveillance Model (PSM) of Rehabilitation for Breast Cancer Patients with 1-Year Postoperative
Ann Surg Oncol DOI 10.1245/s10434-016-5315-z ORIGINAL ARTICLE BREAST ONCOLOGY Implementing the Prospective Surveillance Model (PSM) of Rehabilitation for Breast Cancer Patients with 1-Year Postoperative
Arm Disability. after Breast Cancer. Exploring the impact of arm morbidity
 Arm Disability after Breast Cancer Research Team Roanne Thomas University of Ottawa Tom Hack University of Manitoba Winkle Kwan B.C. Cancer Agency Bo Miedema Dalhousie Family Medicine Teaching Unit Liz
Arm Disability after Breast Cancer Research Team Roanne Thomas University of Ottawa Tom Hack University of Manitoba Winkle Kwan B.C. Cancer Agency Bo Miedema Dalhousie Family Medicine Teaching Unit Liz
Appropriate Concept of Prevention of Lymphedema at the Initial Treatment
 Global Breast Cancer Conference 2018 Appropriate Concept of Prevention of Lymphedema at the Initial Treatment Zisun Kim Department of Surgery, Soonchunhyang University Bucheon Hospital, Soonchunhyang University
Global Breast Cancer Conference 2018 Appropriate Concept of Prevention of Lymphedema at the Initial Treatment Zisun Kim Department of Surgery, Soonchunhyang University Bucheon Hospital, Soonchunhyang University
Upper-Body Morbidity After Breast Cancer*
 Upper-Body Morbidity After Breast Cancer* Incidence and Evidence for Evaluation, Prevention, and Management Within a Prospective Surveillance Model of Care Sandra C. Hayes, PhD 1 ; Karin Johansson, PT,
Upper-Body Morbidity After Breast Cancer* Incidence and Evidence for Evaluation, Prevention, and Management Within a Prospective Surveillance Model of Care Sandra C. Hayes, PhD 1 ; Karin Johansson, PT,
Randomized Multicenter Trial of Sentinel Node Biopsy Versus Standard Axillary Treatment in Operable Breast Cancer: The ALMANAC Trial
 ARTICLES Randomized Multicenter Trial of Sentinel Node Biopsy Versus Standard Axillary Treatment in Operable Breast Cancer: The ALMANAC Trial Robert E. Mansel, Lesley Fallowfield, Mark Kissin, Amit Goyal,
ARTICLES Randomized Multicenter Trial of Sentinel Node Biopsy Versus Standard Axillary Treatment in Operable Breast Cancer: The ALMANAC Trial Robert E. Mansel, Lesley Fallowfield, Mark Kissin, Amit Goyal,
Soran, A., Ozmen, T. et al. Lymphat Res Biol 12(4):
 Early Detection and Treatment The importance of detection of subclinical lymphedema for the prevention of breast cancer-related clinical lymphedema after axillary lymph node dissection; a prospective observational
Early Detection and Treatment The importance of detection of subclinical lymphedema for the prevention of breast cancer-related clinical lymphedema after axillary lymph node dissection; a prospective observational
NCIN Breast Cancer Workshop 13 March 2014 Hilton Metropole, NEC, Birmingham. Kieran Horgan, Dick Rainsbury, Mark Sibbering, Gill lawrence
 NCIN Breast Cancer Workshop 13 March 2014 Hilton Metropole, NEC, Birmingham Kieran Horgan, Dick Rainsbury, Mark Sibbering, Gill lawrence 1 Interactive Workshop Session Professor Kieran Horgan Workshop
NCIN Breast Cancer Workshop 13 March 2014 Hilton Metropole, NEC, Birmingham Kieran Horgan, Dick Rainsbury, Mark Sibbering, Gill lawrence 1 Interactive Workshop Session Professor Kieran Horgan Workshop
Early arm swelling after breast surgery: changes on both sides
 Breast Cancer Res Treat (2007) 101:105 112 DOI 10.1007/s10549-006-9274-0 EPIDEMIOLOGY Early arm swelling after breast surgery: changes on both sides Terry P. Haines Æ Patricia Sinnamon Published online:
Breast Cancer Res Treat (2007) 101:105 112 DOI 10.1007/s10549-006-9274-0 EPIDEMIOLOGY Early arm swelling after breast surgery: changes on both sides Terry P. Haines Æ Patricia Sinnamon Published online:
CORRELATION AMONG BIOIMPEDANCE ANALYSIS, SONOGRAPHIC AND CIRCUMFERENTIAL MEASUREMENT IN ASSESSMENT OF BREAST CANCER-RELATED ARM LYMPHEDEMA
 123 Lymphology 47 (2014) 123-133 CORRELATION AMONG BIOIMPEDANCE ANALYSIS, SONOGRAPHIC AND CIRCUMFERENTIAL MEASUREMENT IN ASSESSMENT OF BREAST CANCER-RELATED ARM LYMPHEDEMA Y.-H. Choi, K.-S. Seo Department
123 Lymphology 47 (2014) 123-133 CORRELATION AMONG BIOIMPEDANCE ANALYSIS, SONOGRAPHIC AND CIRCUMFERENTIAL MEASUREMENT IN ASSESSMENT OF BREAST CANCER-RELATED ARM LYMPHEDEMA Y.-H. Choi, K.-S. Seo Department
Bioimpedance Devices for Detection and Management of Lymphedema
 Medical Policy Manual Durable Medical Equipment, Policy No. 82 Bioimpedance Devices for Detection and Management of Lymphedema Next Review: June 2018 Last Review: June 2017 Effective: August 1, 2017 IMPORTANT
Medical Policy Manual Durable Medical Equipment, Policy No. 82 Bioimpedance Devices for Detection and Management of Lymphedema Next Review: June 2018 Last Review: June 2017 Effective: August 1, 2017 IMPORTANT
Outcomes of patients with inflammatory breast cancer treated by breast-conserving surgery
 Breast Cancer Res Treat (2016) 160:387 391 DOI 10.1007/s10549-016-4017-3 EDITORIAL Outcomes of patients with inflammatory breast cancer treated by breast-conserving surgery Monika Brzezinska 1 Linda J.
Breast Cancer Res Treat (2016) 160:387 391 DOI 10.1007/s10549-016-4017-3 EDITORIAL Outcomes of patients with inflammatory breast cancer treated by breast-conserving surgery Monika Brzezinska 1 Linda J.
LYMPHOEDEMA Journal of Lymphoedema 2007, Vol 2, N 2,
 LYMPHOEDEMA Journal of Lymphoedema 2007, Vol 2, N 2, 30-36. COMPARISON OF THE EFFECTIVENESS OF MLD AND LPG TECHNIQUE. MOSELEY A.L. et al. www.lpgsystems.com www.cosire-lpg.com Contact : infomed@lpgsystems.com
LYMPHOEDEMA Journal of Lymphoedema 2007, Vol 2, N 2, 30-36. COMPARISON OF THE EFFECTIVENESS OF MLD AND LPG TECHNIQUE. MOSELEY A.L. et al. www.lpgsystems.com www.cosire-lpg.com Contact : infomed@lpgsystems.com
Implementing Breast Cancer Survivorship National Cancer Centre Singapore
 Team Members Implementing Breast Cancer Survivorship Programme @ National Cancer Centre Singapore Dr Ho Gay Hui & Ms Tan Beng Le Surgical Oncology & Nursing Ms Tan Beng Le Ms Mabel Tan May Leng Ms Clair
Team Members Implementing Breast Cancer Survivorship Programme @ National Cancer Centre Singapore Dr Ho Gay Hui & Ms Tan Beng Le Surgical Oncology & Nursing Ms Tan Beng Le Ms Mabel Tan May Leng Ms Clair
Impact of BIS Technology
 Skilled nursing leaders know that the number of women surviving breast cancer is rising. While this is good news, survivorship care has grown more complex and challenging for clinicians in skilled nursing
Skilled nursing leaders know that the number of women surviving breast cancer is rising. While this is good news, survivorship care has grown more complex and challenging for clinicians in skilled nursing
L.c. Ward, B.J. Thomas
 2 Lymphology 34 (2001) 2-11 EARLY DIAGNOSIS OF LYMPHEDEMA USING MULTIPLE FREQUENCY BIOIMPEDANCE B.H. Cornish, M. Chapman, C. Hirst, B. Mirolo, l.h. Bunce, L.c. Ward, B.J. Thomas Centre for Medical & Health
2 Lymphology 34 (2001) 2-11 EARLY DIAGNOSIS OF LYMPHEDEMA USING MULTIPLE FREQUENCY BIOIMPEDANCE B.H. Cornish, M. Chapman, C. Hirst, B. Mirolo, l.h. Bunce, L.c. Ward, B.J. Thomas Centre for Medical & Health
2017 San Antonio Breast Cancer Symposium: Local Therapy Highlights
 2017 San Antonio Breast Cancer Symposium: Local Therapy Highlights Mylin A. Torres, M.D. Director, Glenn Family Breast Center Associate Professor Department of Radiation Oncology Winship Cancer Institute
2017 San Antonio Breast Cancer Symposium: Local Therapy Highlights Mylin A. Torres, M.D. Director, Glenn Family Breast Center Associate Professor Department of Radiation Oncology Winship Cancer Institute
Reference Values for Assessing Localized Hand Lymphedema. using Inter-Hand Tissue Dielectric Constant (TDC) Ratios
 Reference Values for Assessing Localized Hand Lymphedema using Inter-Hand Tissue Dielectric Constant (TDC) Ratios Harvey N. Mayrovitz, PhD, College of Medical Sciences, Nova Southeastern University Evelina
Reference Values for Assessing Localized Hand Lymphedema using Inter-Hand Tissue Dielectric Constant (TDC) Ratios Harvey N. Mayrovitz, PhD, College of Medical Sciences, Nova Southeastern University Evelina
Changes Over Time in Occurrence, Severity, and Distress of Common Symptoms During and After Radiation Therapy for Breast Cancer
 98 Journal of Pain and Symptom Management Vol. 45 No. June Original Article Changes Over Time in Occurrence, Severity, and Distress of Common Symptoms During and After Radiation Therapy for Breast Cancer
98 Journal of Pain and Symptom Management Vol. 45 No. June Original Article Changes Over Time in Occurrence, Severity, and Distress of Common Symptoms During and After Radiation Therapy for Breast Cancer
BCRL questionnaires: climate and indigenous groups. Susan Gordon, Lorraine Sheppard, Anita Selby
 BCRL questionnaires: climate and indigenous groups Susan Gordon, Lorraine Sheppard, Anita Selby Valid and reliable subjective questionnaires are essential to enable research regarding the effect of breast
BCRL questionnaires: climate and indigenous groups Susan Gordon, Lorraine Sheppard, Anita Selby Valid and reliable subjective questionnaires are essential to enable research regarding the effect of breast
GUIDELINES FOR SELF MANAGEMENT OF LYMPHOEDEMA. Nicole L. Stout DPT, CLT-LANA,
 GUIDELINES FOR SELF MANAGEMENT OF LYMPHOEDEMA Nicole L. Stout DPT, CLT-LANA, FAPTA nicole.stout@nih.gov @nicolestoutpt Self Management in Lymphedema Prevention and Risk Reduction Secondary Lymphedema
GUIDELINES FOR SELF MANAGEMENT OF LYMPHOEDEMA Nicole L. Stout DPT, CLT-LANA, FAPTA nicole.stout@nih.gov @nicolestoutpt Self Management in Lymphedema Prevention and Risk Reduction Secondary Lymphedema
Systematic review of breast cancer related lymphoedema: making a balanced decision to perform an axillary clearance
 FVV in ObGyn, 2013, 5 (2): 106-115 Systematic review Systematic review of breast cancer related lymphoedema: making a balanced decision to perform an axillary clearance M. Göker 1, N. Devoogdt 2, G. Van
FVV in ObGyn, 2013, 5 (2): 106-115 Systematic review Systematic review of breast cancer related lymphoedema: making a balanced decision to perform an axillary clearance M. Göker 1, N. Devoogdt 2, G. Van
BreastScreen Aotearoa Annual Report 2015
 BreastScreen Aotearoa Annual Report 2015 EARLY AND LOCALLY ADVANCED BREAST CANCER PATIENTS DIAGNOSED IN NEW ZEALAND IN 2015 Prepared for Ministry of Health, New Zealand Version 1.0 Date November 2017 Prepared
BreastScreen Aotearoa Annual Report 2015 EARLY AND LOCALLY ADVANCED BREAST CANCER PATIENTS DIAGNOSED IN NEW ZEALAND IN 2015 Prepared for Ministry of Health, New Zealand Version 1.0 Date November 2017 Prepared
Prospective Lymphedema Surveillance in a Clinic Setting
 J. Pers. Med. 2015, 5, 311-325; doi:10.3390/jpm5030311 Article OPEN ACCESS Journal of Personalized Medicine ISSN 2075-4426 www.mdpi.com/journal/jpm/ Prospective Lymphedema Surveillance in a Clinic Setting
J. Pers. Med. 2015, 5, 311-325; doi:10.3390/jpm5030311 Article OPEN ACCESS Journal of Personalized Medicine ISSN 2075-4426 www.mdpi.com/journal/jpm/ Prospective Lymphedema Surveillance in a Clinic Setting
REVIEW. Arm Edema in Breast Cancer Patients. Virginia S. Erickson, Marjorie L. Pearson, Patricia A. Ganz, John Adams, Katherine L.
 REVIEW Arm Edema in Breast Cancer Patients Virginia S. Erickson, Marjorie L. Pearson, Patricia A. Ganz, John Adams, Katherine L. Kahn The improvement in the life expectancy of women with breast cancer
REVIEW Arm Edema in Breast Cancer Patients Virginia S. Erickson, Marjorie L. Pearson, Patricia A. Ganz, John Adams, Katherine L. Kahn The improvement in the life expectancy of women with breast cancer
Utilization of bioimpedance spectroscopy in the prevention of chronic breast cancer-related lymphedema
 Breast Cancer Res Treat (2017) 166:809 815 DOI 10.1007/s10549-017-4451-x CLINICAL TRIAL Utilization of bioimpedance spectroscopy in the prevention of chronic breast cancer-related lymphedema David I. Kaufman
Breast Cancer Res Treat (2017) 166:809 815 DOI 10.1007/s10549-017-4451-x CLINICAL TRIAL Utilization of bioimpedance spectroscopy in the prevention of chronic breast cancer-related lymphedema David I. Kaufman
Results, morbidity, and quality of life of melanoma patients undergoing sentinel lymph node staging Vries, Mattijs de
 University of Groningen Results, morbidity, and quality of life of melanoma patients undergoing sentinel lymph node staging Vries, Mattijs de IMPORTANT NOTE: You are advised to consult the publisher's
University of Groningen Results, morbidity, and quality of life of melanoma patients undergoing sentinel lymph node staging Vries, Mattijs de IMPORTANT NOTE: You are advised to consult the publisher's
Physiotherapy in Breast Cancer: developing clinical practice
 Physiotherapy in Breast Cancer: developing clinical practice Dr Karen Robb Macmillan Cancer Rehabilitation Strategy Development Manager Consultant Physiotherapist Member of Macmillan Consequences of Cancer
Physiotherapy in Breast Cancer: developing clinical practice Dr Karen Robb Macmillan Cancer Rehabilitation Strategy Development Manager Consultant Physiotherapist Member of Macmillan Consequences of Cancer
Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy
 Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy Mitsui Memorial Hospital Department of Breast and Endocine surgery Daisuke Ota No financial support
Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy Mitsui Memorial Hospital Department of Breast and Endocine surgery Daisuke Ota No financial support
Impact of adjuvant taxane-based chemotherapy on development of breast cancer-related lymphedema: results from a large prospective cohort
 Breast Cancer Res Treat (2015) 151:393 403 DOI 10.1007/s10549-015-3408-1 CLINICAL TRIAL Impact of adjuvant taxane-based chemotherapy on development of breast cancer-related lymphedema: results from a large
Breast Cancer Res Treat (2015) 151:393 403 DOI 10.1007/s10549-015-3408-1 CLINICAL TRIAL Impact of adjuvant taxane-based chemotherapy on development of breast cancer-related lymphedema: results from a large
Evaluation of the Axilla Post Z-0011 Trial New Paradigm
 Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
Quantifying Lymphedema with Noninvasive Methodology
 Quantifying Lymphedema with Noninvasive Methodology Physical Principles Practical Aspects Potential Limitations NLN2014 Washington D.C. 9/5/2014 Harvey N. Mayrovitz PhD Professor of Physiology College
Quantifying Lymphedema with Noninvasive Methodology Physical Principles Practical Aspects Potential Limitations NLN2014 Washington D.C. 9/5/2014 Harvey N. Mayrovitz PhD Professor of Physiology College
J Clin Oncol 30: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 30 NUMBER 30 OCTOBER 20 2012 JOURNAL OF CLINICAL ONCOLOGY R E V I E W A R T I C L E Cancer-Related Lymphedema Risk Factors, Diagnosis, Treatment, and Impact: A Review Electra D. Paskett, Julie A.
VOLUME 30 NUMBER 30 OCTOBER 20 2012 JOURNAL OF CLINICAL ONCOLOGY R E V I E W A R T I C L E Cancer-Related Lymphedema Risk Factors, Diagnosis, Treatment, and Impact: A Review Electra D. Paskett, Julie A.
Is Complete Axillary Dissection Needed Following Mastectomy and Sentinel Node Biopsy for N1 disease?
 Is Complete Axillary Dissection Needed Following Mastectomy and Sentinel Node Biopsy for N1 disease? Mylin A. Torres, MD Director, Glenn Family Breast Center Louis and Rand Glenn Family Chair in Breast
Is Complete Axillary Dissection Needed Following Mastectomy and Sentinel Node Biopsy for N1 disease? Mylin A. Torres, MD Director, Glenn Family Breast Center Louis and Rand Glenn Family Chair in Breast
Clinical Practice Guideline
 Clinical Practice Guideline Diagnosis of Upper Quadrant Lymphedema Secondary to Cancer: Clinical Practice Guideline From the Oncology Section of the American Physical Therapy Association Kimberly Levenhagen,
Clinical Practice Guideline Diagnosis of Upper Quadrant Lymphedema Secondary to Cancer: Clinical Practice Guideline From the Oncology Section of the American Physical Therapy Association Kimberly Levenhagen,
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection
 The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
BREAST CANCER CARE IN RESOURCE CONSTRAINED REGIONS BBCC 2017 DHAKA. M.J.PAUL MS,DNB, FRCS (Glasg) Professor, Endocrine Surgery CMC Vellore, India
 BREAST CANCER CARE IN RESOURCE CONSTRAINED REGIONS BBCC 2017 DHAKA M.J.PAUL MS,DNB, FRCS (Glasg) Professor, Endocrine Surgery CMC Vellore, India BREAST CANCER THE COMING WAVE THE DEMOGRAPHIC CHANGE Increase
BREAST CANCER CARE IN RESOURCE CONSTRAINED REGIONS BBCC 2017 DHAKA M.J.PAUL MS,DNB, FRCS (Glasg) Professor, Endocrine Surgery CMC Vellore, India BREAST CANCER THE COMING WAVE THE DEMOGRAPHIC CHANGE Increase
ORIGINAL ARTICLE. Lymphedema and Quality of Life in Survivors of Early-Stage Breast Cancer
 ORIGINAL ARTICLE and Quality of Life in Survivors of Early-Stage Breast Cancer Sarah M. Beaulac, MPH; Lindsay A. McNair, MD, MPH; Thayer E. Scott, MPH; Wayne W. LaMorte, MD, PhD, MPH; Maureen T. Kavanah,
ORIGINAL ARTICLE and Quality of Life in Survivors of Early-Stage Breast Cancer Sarah M. Beaulac, MPH; Lindsay A. McNair, MD, MPH; Thayer E. Scott, MPH; Wayne W. LaMorte, MD, PhD, MPH; Maureen T. Kavanah,
Prevention and Treatment of Upper Extremity Dysfunction in Tissue Expander Patients
 Prevention and Treatment of Upper Extremity Dysfunction in Tissue Expander Patients Kristen McNiff, BSN, RN, CPSN Trish Coyle, MSN, RN, CPSN Plastic and Reconstructive Surgery Objectives Discuss common
Prevention and Treatment of Upper Extremity Dysfunction in Tissue Expander Patients Kristen McNiff, BSN, RN, CPSN Trish Coyle, MSN, RN, CPSN Plastic and Reconstructive Surgery Objectives Discuss common
BREAST CANCER 2010 COMPARATIVE AUDIT REPORT
 SOUTH EAST SCOTLAND CANCER PROSPECTIVE CANCER AUDIT BREAST CANCER 2010 COMPARATIVE AUDIT REPORT Dr Jeremy Thomas, NHS Lothian Chair, Breast Group Miss Fawzia Ashkanani, NHS Dumfries and Galloway Mr Matthew
SOUTH EAST SCOTLAND CANCER PROSPECTIVE CANCER AUDIT BREAST CANCER 2010 COMPARATIVE AUDIT REPORT Dr Jeremy Thomas, NHS Lothian Chair, Breast Group Miss Fawzia Ashkanani, NHS Dumfries and Galloway Mr Matthew
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Certified Breast Care Nurse (CBCN ) Test Content Outline (Effective 2018)
 Certified Breast Care Nurse (CBCN ) Test Content Outline (Effective 2018) I. Coordination of Care - 26% A. Breast health, screening, early detection, risk assessment and reduction 1. Issues related to
Certified Breast Care Nurse (CBCN ) Test Content Outline (Effective 2018) I. Coordination of Care - 26% A. Breast health, screening, early detection, risk assessment and reduction 1. Issues related to
Welcome to Allied Health Telehealth
 Welcome to Allied Health Telehealth Paediatric lymphoedema A challenge for clinicians and families To receive an attendance certificate please complete your online evaluation at: https://www.surveymonkey.com/s/paedlymphoedema
Welcome to Allied Health Telehealth Paediatric lymphoedema A challenge for clinicians and families To receive an attendance certificate please complete your online evaluation at: https://www.surveymonkey.com/s/paedlymphoedema
Moving from the Means to the Standard Deviations in Symptom Management Research
 Moving from the Means to the Standard Deviations in Symptom Management Research Christine Miaskowski, RN, PhD, FAAN Professor American Cancer Society Clinical Research Professor Sharon A. Lamb Endowed
Moving from the Means to the Standard Deviations in Symptom Management Research Christine Miaskowski, RN, PhD, FAAN Professor American Cancer Society Clinical Research Professor Sharon A. Lamb Endowed
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Bioelectrical impedance for monitoring the efficacy of lymphoedema treatment programmes
 Breast Cancer Research and Treatment 38: 169-176, 1996. @ 1996 Kluwer Academic Publishers. Printed in the Netherlands. Report Bioelectrical impedance for monitoring the efficacy of lymphoedema treatment
Breast Cancer Research and Treatment 38: 169-176, 1996. @ 1996 Kluwer Academic Publishers. Printed in the Netherlands. Report Bioelectrical impedance for monitoring the efficacy of lymphoedema treatment
Sentinel lymph node biopsy at the time of mastectomy does not increase the risk of lymphedema: implications for prophylactic surgery
 Sentinel lymph node biopsy at the time of mastectomy does not increase the risk of lymphedema: implications for prophylactic surgery The Harvard community has made this article openly available. Please
Sentinel lymph node biopsy at the time of mastectomy does not increase the risk of lymphedema: implications for prophylactic surgery The Harvard community has made this article openly available. Please
Economic Benefits of BIS-Aided Assessment of Post-BC Lymphedema in the United States
 n clinical n Economic Benefits of BIS-Aided Assessment of Post-BC Lymphedema in the United States Sara P. Bilir, MS; Mitchell P. DeKoven, MHSA; and Juliet Munakata, MS Objectives: To estimate the economic
n clinical n Economic Benefits of BIS-Aided Assessment of Post-BC Lymphedema in the United States Sara P. Bilir, MS; Mitchell P. DeKoven, MHSA; and Juliet Munakata, MS Objectives: To estimate the economic
Breast Cancer Treatment and Lymphedema
 Breast Cancer Treatment and Lymphedema Over the last decade, major advances have been made in the prevention and treatment of breast cancer in the United States, but minimal attention has been given to
Breast Cancer Treatment and Lymphedema Over the last decade, major advances have been made in the prevention and treatment of breast cancer in the United States, but minimal attention has been given to
Muscle strength in patients with chronic pain
 Clinical Rehabilitation 2003; 17: 885 889 Muscle strength in patients with chronic pain CP van Wilgen Painexpertise Centre, Department of Rehabilitation, Department of Oral and Maxillofacial Surgery University
Clinical Rehabilitation 2003; 17: 885 889 Muscle strength in patients with chronic pain CP van Wilgen Painexpertise Centre, Department of Rehabilitation, Department of Oral and Maxillofacial Surgery University
Table of contents. Page 2 of 40
 Page 1 of 40 Table of contents Introduction... 4 1. Background Information... 6 1a: Referral source for the New Zealand episodes... 6 1b. Invasive and DCIS episodes by referral source... 7 1d. Age of the
Page 1 of 40 Table of contents Introduction... 4 1. Background Information... 6 1a: Referral source for the New Zealand episodes... 6 1b. Invasive and DCIS episodes by referral source... 7 1d. Age of the
Research Report. Measurement Decisions for Clinical Assessment of Limb Volume Changes in Patients With Bilateral and Unilateral Limb Edema
 Research Report Measurement Decisions for Clinical Assessment of Limb Volume Changes in Patients With Bilateral and Unilateral Limb Edema Harvey N Mayrovitz, John Macdonald, Suzanne Davey, Kelly Olson,
Research Report Measurement Decisions for Clinical Assessment of Limb Volume Changes in Patients With Bilateral and Unilateral Limb Edema Harvey N Mayrovitz, John Macdonald, Suzanne Davey, Kelly Olson,
Measure #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care
 Measure #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: The percentage
Measure #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: The percentage
Liposuction for chronic lymphoedema
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Liposuction for chronic lymphoedema Chronic lymphoedema is the swelling and build-up of body fluid and fat,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Liposuction for chronic lymphoedema Chronic lymphoedema is the swelling and build-up of body fluid and fat,
Axillary treatment for patients with early breast cancer and lymph node metastasis: systematic review protocol
 Goyal et al. World Journal of Surgical Oncology 2013, 11:6 WORLD JOURNAL OF SURGICAL ONCOLOGY REVIEW Open Access Axillary treatment for patients with early breast cancer and lymph node metastasis: systematic
Goyal et al. World Journal of Surgical Oncology 2013, 11:6 WORLD JOURNAL OF SURGICAL ONCOLOGY REVIEW Open Access Axillary treatment for patients with early breast cancer and lymph node metastasis: systematic
Breast cancer: an update
 Breast cancer: an update Dr. Sanjeewa Seneviratne M.D, MRCS, Ph.D. Senior Lecturer and Honorary Consultant Surgeon Department of Surgery Faculty of Medicine, Colombo Plan The problem Screening & early
Breast cancer: an update Dr. Sanjeewa Seneviratne M.D, MRCS, Ph.D. Senior Lecturer and Honorary Consultant Surgeon Department of Surgery Faculty of Medicine, Colombo Plan The problem Screening & early
Midwest Metastatic Breast Cancer Conference. Renata Beaman, PT, MS, MA, OCS, CLT Exercise & Cancer
 Midwest Metastatic Breast Cancer Conference Renata Beaman, PT, MS, MA, OCS, CLT Exercise & Cancer Presented By: Title Sponsor: Renata Beaman, PT, MS, MA, OCS, CLT OrthoRehab Specialists, Inc. Edina, MN
Midwest Metastatic Breast Cancer Conference Renata Beaman, PT, MS, MA, OCS, CLT Exercise & Cancer Presented By: Title Sponsor: Renata Beaman, PT, MS, MA, OCS, CLT OrthoRehab Specialists, Inc. Edina, MN
Results of the ACOSOG Z0011 Trial
 DCIS and Early Breast Cancer Symposium JUNE 15-17 2012 CAPPADOCIA Results of the ACOSOG Z0011 Trial Kelly K. Hunt, M.D. Professor of Surgery Axillary Node Dissection Staging, Regional control, Survival
DCIS and Early Breast Cancer Symposium JUNE 15-17 2012 CAPPADOCIA Results of the ACOSOG Z0011 Trial Kelly K. Hunt, M.D. Professor of Surgery Axillary Node Dissection Staging, Regional control, Survival
Conservative Surgery and Radiation Stage I and II Breast Cancer
 Conservative Surgery and Radiation Stage I and II Breast Cancer Variant 1: Premenopausal 41-year-old woman, 1.1-cm GII IDC, upper outer quadrant (UOQ), ER/PR ( ), HER2 ( ), primary excised with lumpectomy,
Conservative Surgery and Radiation Stage I and II Breast Cancer Variant 1: Premenopausal 41-year-old woman, 1.1-cm GII IDC, upper outer quadrant (UOQ), ER/PR ( ), HER2 ( ), primary excised with lumpectomy,
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Physiotherapy Management of Post-Operative Breast Cancer Patients: A Qualitative Study
 A Peer Reviewed Publication of the College of Health Care Sciences at Nova Southeastern University Dedicated to allied health professional practice and education http://ijahsp.nova.edu Vol. 12 No. 4 ISSN
A Peer Reviewed Publication of the College of Health Care Sciences at Nova Southeastern University Dedicated to allied health professional practice and education http://ijahsp.nova.edu Vol. 12 No. 4 ISSN
Occurrence of Lymphedema Following Sentinel Node Biopsy (SNB) for Lower Extremity Melanoma
 Original Article Elmer Press Occurrence of Lymphedema Following Sentinel Node Biopsy (SNB) for Lower Extremity Melanoma Patrick D. Magoon a, Roger A. Graham b, d, Janice G. Rothschild b, Yoojin Lee c Abstract
Original Article Elmer Press Occurrence of Lymphedema Following Sentinel Node Biopsy (SNB) for Lower Extremity Melanoma Patrick D. Magoon a, Roger A. Graham b, d, Janice G. Rothschild b, Yoojin Lee c Abstract
Removal of sentinel lymph node(s)
 Removal of sentinel lymph node(s) Exceptional healthcare, personally delivered What is a sentinel lymph node? The sentinel lymph nodes (glands) are the first lymph nodes in your armpit to which breast
Removal of sentinel lymph node(s) Exceptional healthcare, personally delivered What is a sentinel lymph node? The sentinel lymph nodes (glands) are the first lymph nodes in your armpit to which breast
Breast Cancer MultiDisciplinary Approach
 Breast Cancer MultiDisciplinary Approach October 30, 2012 Kristi Dolcetti RN, CON, CBPNC-IC OTN Bookings Regional Cancer Care is booking indirect Patient visits for our Multidisciplinary Cancer Conferences
Breast Cancer MultiDisciplinary Approach October 30, 2012 Kristi Dolcetti RN, CON, CBPNC-IC OTN Bookings Regional Cancer Care is booking indirect Patient visits for our Multidisciplinary Cancer Conferences
EFFECTS OF RESISTANCE EXERCISES AND COMPLEX DECONGESTIVE THERAPY ON ARM FUNCTION AND MUSCULAR STRENGTH IN BREAST CANCER RELATED LYMPHEDEMA
 184 Lymphology 48 (2015) 184-196 EFFECTS OF RESISTANCE EXERCISES AND COMPLEX DECONGESTIVE THERAPY ON ARM FUNCTION AND MUSCULAR STRENGTH IN BREAST CANCER RELATED LYMPHEDEMA J.H. Do, W. Kim, Y.K. Cho, J.
184 Lymphology 48 (2015) 184-196 EFFECTS OF RESISTANCE EXERCISES AND COMPLEX DECONGESTIVE THERAPY ON ARM FUNCTION AND MUSCULAR STRENGTH IN BREAST CANCER RELATED LYMPHEDEMA J.H. Do, W. Kim, Y.K. Cho, J.
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Defining the Role of Rehabilitation in Breast Cancer Care
 Defining the Role of Rehabilitation in Breast Cancer Care Ashley Dew, PT, DPT Ochsner Therapy and Wellness Manager of Program Development Physical Therapist at the Tansey Breast Center I have no relevant
Defining the Role of Rehabilitation in Breast Cancer Care Ashley Dew, PT, DPT Ochsner Therapy and Wellness Manager of Program Development Physical Therapist at the Tansey Breast Center I have no relevant
VENIPUNCTURE AND LYMPHEDEMA
 VENIPUNCTURE AND LYMPHEDEMA AUTHOR: LYNN HADAWAY, M.ED., RN, BC, CRNI THE CLINICAL QUESTION Is it acceptable to perform venipuncture or VAD insertion on the ipsilateral arm after any type of breast cancer
VENIPUNCTURE AND LYMPHEDEMA AUTHOR: LYNN HADAWAY, M.ED., RN, BC, CRNI THE CLINICAL QUESTION Is it acceptable to perform venipuncture or VAD insertion on the ipsilateral arm after any type of breast cancer
Axillary treatment for operable primary breast cancer(review)
 Cochrane Database of Systematic Reviews Axillary treatment for operable primary breast cancer (Review) Bromham N, Schmidt-Hansen M, Astin M, Hasler E, Reed MW Bromham N, Schmidt-Hansen M, Astin M, Hasler
Cochrane Database of Systematic Reviews Axillary treatment for operable primary breast cancer (Review) Bromham N, Schmidt-Hansen M, Astin M, Hasler E, Reed MW Bromham N, Schmidt-Hansen M, Astin M, Hasler
Abstract of dissertation entitled. A clinical guideline for management of lymphoedema using nurse-led. manual lymphatic drainage therapy.
 Abstract of dissertation entitled A clinical guideline for management of lymphoedema using nurse-led manual lymphatic drainage therapy Submitted by Tang Kit Sum For the degree of Master of Nursing at the
Abstract of dissertation entitled A clinical guideline for management of lymphoedema using nurse-led manual lymphatic drainage therapy Submitted by Tang Kit Sum For the degree of Master of Nursing at the
