Lymphatic filariasis in children: Clinical features, infection burdens and future prospects for elimination
|
|
|
- Gordon McGee
- 5 years ago
- Views:
Transcription
1 Lymphatic filariasis in children: Clinical features, infection burdens and future prospects for elimination 1559 RANGANATHA KRISHNA SHENOY 1 and MOSES J. BOCKARIE 2 * 1 Filariasis Chemotherapy Unit, TD Medical College Hospital, Alappuzha , Kerala, India 2 Centre for Neglected Tropical Diseases, Liverpool School of Tropical Medicine, Pembroke Place, Liverpool, L3 5QA, UK (Received 13 December 2010; revised 24 February and 21 June 2011; accepted 21 June 2011; first published online 3 August 2011) SUMMARY Lymphatic filariasis (LF), a common parasitic infection in tropical countries, causes lymphoedema of limbs, hydrocele and acute attacks of dermato-lymphangio-adenitis. Recent advances in diagnosis have helped to recognize that LF infection is often acquired in childhood. Newly available diagnostic techniques like sensitive antigen and antibody assays, Doppler ultrasonography and lymphoscintigraphy have helped to understand the subclinical pathology caused by this infection, which was hitherto generally believed to be irreversible. Recent studies indicate that drugs used in the mass drug administration (MDA) programme under GPELF are capable of reversing the sub-clinical lymphatic damage in children and provide benefits other than interruption of transmission. Albendazole and ivermectin used in MDA are effective against soil-transmitted helminthic infections common in children in LF endemic areas. Thus MDA had other beyond LF benefits in treated children including increased appetite, weight gain, greater learning ability and concentration, better school attendance and prevention of anaemia. MDA should no longer be viewed as a measure for interrupting transmission alone. Recent findings of reversibility of early lymphatic pathology in treated children indicate that both MDA and foothygiene measures are effective strategies in preventing and managing morbidity. Programme managers should effectively utilize this information to strengthen their advocacy efforts to achieve high and sustainable coverage in MDA. Key words: Lymphatic filariasis, children, subclinical pathology, lymphangiectasia, reversal of lymphatic damage, prevention, mass drug administration, foot-care. INTRODUCTION Lymphatic filariasis (LF) is a mosquito-borne parasitic infection caused by filarial nematodes invading the human lymphatic tissue. It is an important public health problem endemic in 81 tropical countries. Globally, 1 3 billion people are at risk of this infection and about 120 million people are estimated to be affected by this disease (WHO, 2010a). Among the debilitating vector-borne tropical diseases, LF is ranked as the second most common cause of permanent physical disability worldwide (Taylor et al. 2010). The most common causative agent of the disease is Wuchereria bancrofti (90%) with, to a lesser extent, Brugia malayi (< 10%) and rarely Brugia timori. The various genera of mosquitoes transmitting these parasites in different geographical locations include Culex, Anopheles, Aedes or Mansonia (Bockarie et al. 2009). LF is still a major cause of disability and a significant impediment to socioeconomic development in large areas of Asia, Africa, Western Pacific and in certain regions of the Americas (WHO, 2010b). * Corresponding author: Centre for Neglected Tropical Diseases, Liverpool School of Tropical Medicine, Pembroke Place, Liverpool, L3 5QA, UK. Phone: + 44 (0) Fax: + 44(0) Mobile: moses.bockarie@liv.ac.uk The disease manifestations of LF include chronic lymphoedema and elephantiasis mainly involving the limbs or sometimes the genital region; also hydrocele and chyluria, along with acute attacks of recurrent dermato-lymphangio-adenitis (ADLA) due to bacterial infections. These acute attacks are responsible for the worsening of lymphoedema and progression to elephantiasis (Pani et al. 1995). These clinical manifestations affect 44 million people globally. Studies indicate that once established, the lymphatic pathology resulting in disease manifestations cannot be easily reversed by available treatment modalities (Freedman et al. 1994, 1995; Taylor et al. 2010). Thus LF is better prevented. The recent advances in the understanding of pathogenesis of LF, the biology of the parasite, and development of newer diagnostic tools and chemotherapeutic agents that are safe and effective have all contributed to new hope that this disease can be eradicated globally (Bockarie and Molyneux, 2009; Taylor et al. 2010). This Global Programme for Elimination of LF (GPELF) launched in 2000, is based on a dual approach consisting of (a) interruption of transmission of LF infection by treating the entire at risk population in endemic countries by annual single dose administration of a two-drug combination consisting of albendazole along with either diethyl carbamazine (DEC) or ivermectin for a period of 4 6 years and (b) alleviation Parasitology (2011), 138, Cambridge University Press 2011 doi: /s x
2 Ranganatha Krishna Shenoy and Moses J. Bockarie of the disability in those who already have the disease, by meticulous limb hygiene measures to prevent secondary bacterial and fungal infections that cause acute attacks of ADLA (Dreyer et al. 1999; Seim et al. 1999; Ottesen, 2000; Gyapong et al. 2005). GPELF is a rapidly expanding global health programme, probably the biggest in the history of public health (WHO, 2010c). Among the 81 countries considered endemic for LF, 53 have started implementing MDA to interrupt transmission. More than 2 8 billion treatments were delivered to a cumulative targeted population of 845 million people during 2000 to Of the 53 countries that have implemented MDA, 37 (70%) have completed the number of rounds of MDA thought to be adequate in most settings to interrupt transmission (55) in some of their implementation units. According to WHO estimates (WHO, 2010c), the overall economic benefit of the programme during is around US$24 billion. Many aspects of LF point to a baffling disease. In the initial stages of infection, when the live adult worms are present in the lymphatics and usually associated with microfilaraemia, the individual does not have any outward disease manifestation. There is a long interval between acquiring the infection and development of disease manifestations. This finding has important implications in the light of the recent observation that LF infection is acquired in childhood in many instances. These children develop clinical disease mostly in their later adult life (Witt and Ottesen, 2001; Shenoy, 2006). The knowledge that children are infected in early life is consequent to introduction of many newly available diagnostic techniques like sensitive antigen assays that provide diagnosis even in low density infections (Weil and Ramzy, 2007), demonstration of sub-clinical lymphatic pathology and detection of presence of live adult worms in lymphatics by Doppler ultrasonography (Dreyer et al. 1999; Shenoy et al. 2007b) and lymph vessel damage by lymphoscintigraphy (Shenoy et al. 2008). In the light of these findings it is quite relevant to discuss how LF affects the health prospects of children and the benefits they would accrue by elimination of this chronic, disabling and depressing illness from the community. This paper provides an up-to-date review of various aspects of LF in children including prevention of this infection. LYMPHATIC FILARIASIS IN CHILDREN Over 250 million children are exposed to LF worldwide. In some endemic communities, up to 10% of children under the age of 15 years are infected (Bockarie et al. 2002). More than 100 million children were treated in 2009 by mass drug administration to eliminate LF (WHO, 2010a). The outward disease manifestations of LF are seen mostly in adult life, 1560 even though there have been occasional reports from LF endemic areas of occurrence of lymphoedema and ADLA attacks in children including hydrocele in boys of pubertal age (Pani et al. 1991; Ramaiah et al. 1996; Witt and Ottesen, 2001; Weil and Ramzy, 2007). In the past there were several reasons why the incidence of LF in the paediatric population did not attract much attention. The foremost among them is the natural history of this disease, the early stages of which are remarkably silent and the progression to later stages of clinical disease is phenomenally slow. It is well known that the early stage of infection is characterized by asymptomatic microfilaraemia, which may continue so for varying periods. These subjects do not have any overt manifestation of the disease even though they have microfilariae (mf) in their blood, usually detected by blood examination at night. The routine stained, thick blood-smear examination was found to be not sensitive enough to detect all microfilaraemics when compared to the more recently available immunochromatography (ICT) card test for the detection of filarial antigen in bancroftian filariasis (Weil and Ramzy, 2007). This is specially so when the density of mf is low or when the infection is in an early stage where the adult worms have not started producing mf. Even during this early asymptomatic phase, children are shown to have dilatation of the lymphatics along with presence of live adult worms by ultrasonography (Dreyer et al. 1999; Shenoy et al. 2007a) and lymph vessel dilation by lymphoscintigraphy (Shenoy et al. 2008). This sub-clinical lymphatic pathology is difficult to diagnose by external examination. For these reasons, in the past many of these early infections in children were missed. Moreover, many earlier epidemiological studies did not include children less than 5 years. Certain epidemiological studies and case reports in the past and more so in recent times, tests for filarial antigenaemia and ultrasound examination of the lymphatics in children mentioned above have all indicated that LF may be more importantly a childhood infection (Witt and Ottesen, 2001). During the course of research activities in a Brugia malayi endemic area at the Filariasis Chemotherapy Unit in TD Medical College Hospital, Alappuzha, India it was observed that among the asymptomatic, mf-positive subjects screened *30% were aged 420 years, while 16 3% were <10 years. In a study on prevention of ADLA attacks in brugian filariasis, 32% of the adults who had lymphoedema of several years duration recalled during their interview, that their disease first manifested before they were 15 years of age (Suma et al. 2002). Factors influencing LF infection in children Many past studies have reported clustering of young individuals with mf in a given household. This has
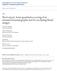
3 Lymphatic filariasis in children 1561 been attributed to several mechanisms such as environmental factors facilitating exposure to infective mosquito bites (Vanamail et al. 1989, 1992) intra-uterine sensitisation due to maternal infection, higher prevalence of mf in children born to microfilaraemic mothers (Lammie et al. 1991) and parental infection (maternal, paternal or both) predisposing to higher prevalence of mf in the offspring (Das et al. 1997). Exposure to infection within the household appeared to be the most important cause for acquiring LF infection in childhood, more than prenatal sensitisation or genetic factors (Das et al. 1997). Clinical features of LF disease in childhood One well known clinical presentation of LF disease in the paediatric group is non-specific lymph node enlargement or soft tissue swelling in the inguinal region, axilla or neck. Biopsy and histopathological examination of such swellings had confirmed presence of dead adult filarial worms or their remnants (Jungmann et al. 1991). Several studies from endemic areas for LF have recorded the presence of lymphoedema of limbs in children, the incidence being higher in older children (Fig. 1). Higher grades of oedema are not common since this depends upon the duration of the illness. Hydrocele of the scrotal sac is also described in boys of pubertal age or older. Acute attacks of ADLA were noted in children both with and without lymphoedema (Pani et al. 1991; Ramaiah et al. 1996; Foxet al. 2005). Episodes of ADLA are characterized by acute onset pain, fever, redness and tenderness of affected limb along with other constitutional symptoms like vomiting. The draining lymph nodes are usually painful and tender. The chronic manifestations are seen less often in children <10 years. In a recent study in a Brugia malayi endemic region, out of 7934 children screened for filarial infection and disease four girls between years old had grade II lymphoedema (Shenoy et al. 2007a). Occasionally they present with filarial lymphangitis caused by death of the adult worms in the lymphatics, either spontaneous or after treatment with the antifilarial drug DEC. In such situations dilated, inflamed and tender lymphatic channels stand out as cords ( string sign ) seen and palpated either by the side of the chest or inguinal region (Shenoy et al. 1998). Rarely chyluria and tropical pulmonary eosinophilia are also reported in children (Witt and Ottesen, 2001). Microfilaraemia in children Studies in different endemic populations on mf prevalence have shown a constant relationship between childhood and adult infections. The childhood mf prevalence rates were *30% of adult prevalence for <10 year olds and *69% for Fig. 1. Advanced lymphoedema in the left leg of a 14 year-old girl from an area endemic for lymphatic filariasis. years olds (Witt and Ottesen, 2001). The mf counts tended to be lower in young children and were higher in older children. Offspring of microfilaraemic mothers had a higher risk of microfilaraemia when compared to those born of uninfected mothers (Alexander et al. 1998). In a study of Brugia malayi filariasis, 32 children were detected to have microfilaraemia ranging from 28 to 1812/ml, three of them being just three years old (Shenoy et al. 2007a). Immuno-diagnosis of LF infection in childhood For bancroftian filariasis there are two sensitive tests presently available for detection of circulating filarial antigen, which can be carried out even during daytime in contrast to detection of mf by examination of blood at night. These are ICT card test and Og4C3 antibody based test in ELISA format (Weil and Ramzy, 2007). A positive test result indicates presence of live adult worms and thus active infection. The ICT card test is easier to perform than the ELISA test. Longitudinal studies conducted in children from endemic areas have demonstrated filarial antigenaemia in 6% of the two-year olds and the prevalence increased to 30% in four-year olds (Lammie et al. 1998). Test for the adult worm antigen is definitely a more sensitive method than blood mf counts to detect LF prevalence in children. If only the mf detection method by night blood examination is used for diagnosis, at least one-third of all infections would be missed (Witt and Ottesen, 2001). The filarial antigen prevalence (AGP) rates are always higher than the mf prevalence (MFP) in many field studies. One such study reported that AGP seen
4 Ranganatha Krishna Shenoy and Moses J. Bockarie on ICT test was higher than MFP varying between 11 3 to 12% (Sunish et al. 2002). In another study, while 62% children had microfilaraemia, 81% had antigenaemia on Og4C3 testing (Fox et al. 2005). Such antigen detection tests as described above are not available so far for a specific diagnosis of Brugia malayi infection. But a filaria-specific IgG4 antibody test using a recombinant antigen (BmR1) has been developed, which has 95 97% sensitivity, 99% specificity, 97% positive predictive value and 99% negative predictive value (Rahmah et al. 2001, 2003). This test is available in an ELISA format, as a dipstick test termed Brugia Rapid (BR) and also in cassette form. The BR test was used in a study of LF infection in children in a Brugia-endemic area, where 7934 children were screened in villages for filarial infection and disease. In this population, it was found on screening that, while the prevalence of microfilaraemia by blood-smear examination was only 0 38%, the BR test was positive in 10 97%. Similar to what is seen by ICT card testing in bancroftian filariasis, the BR test thus identified nearly 27 times more infected individuals in Brugia malayi infection than the conventional mf detection by blood smear examination (Shenoy et al. 2007a, 2009). From the above group, 100 children were enrolled for the chemotherapy studies, out of which 77 tested positive for filaria-specific IgG4 antibody. This IgG4 positive group had more individuals who had other unmistakable evidence of filarial infection or subclinical lymphatic pathology. Thus it was seen that 94% of the microfilaraemics, 86% of the children with live adult worm nests detected on Doppler ultrasonography and 78% of the children who had abnormal lymphatics on lymphoscintigraphy (LSG) were IgG4 positive. Based on these observations it was concluded that a positive BR test is a reliable marker of B. malayi infection (Shenoy et al. 2009) amicrofilaraemic child (Dreyer et al. 1999). USG is not as sensitive as mf detection on night blood examination or tests for antigenaemia. Thus one study of W. bancrofti (WB) LF in 5 13 year old children found that while microfilaraemia was present in 62% and antigenaemia in 81%, FDS was seen only in 15% (Fox et al. 2005). In Brugia malayi infection where there is no genital involvement, one study using ultrasonography with a 7 5 MHz probe failed to locate any adult worm nests in the scrotal lymphatics in adults. It was concluded that this failure to demonstrate B. malayi (BM) parasites was due to either technological inadequacies (resolution of the probe, lack of Doppler techniques) or possibly due to intrinsic biological characteristics of the worm such as their smaller size, ability to locate to deeper tissues or inability to populate classical bancroftian locations such as the scrotal lymphatics (Shenoy et al. 2000). Thus in the recent study of BM infection in children, Colour Power Doppler (CPD) and Pulse Wave Doppler (PWD) examination were employed to locate adult worm nests, if any were present. This additional facility is essential to locate with confidence the small adult worm nests in BM infection and differentiate them from the echoes from blood vessels (Mand et al. 2006). By this method 18 nests with FDS were identified in 14 children comprising 11 boys and 3 girls. Four subjects had two nests each. The youngest two children who showed FDS were only 3 years old. FDS was seen in the axilla in 12 children, in the thigh in two and in the epitrochlear and popliteal area in one child each (Fig. 2A and 2B). The worm nests were distinctly smaller and the wriggling movements were less rapid and less conspicuous than those of bancroftian filariasis. Lymph vessel dilations were observed on DSG in 38 out of the 100 enrolled children (Shenoy et al. 2007a). Doppler and ultrasonography in LF infection in children One of the important recent tools in the diagnosis of LF infection is ultrasonography (USG) and Doppler sonography (DSG) (Shenoy et al. 2007a). Live adult worm nests, hydrocele, chylocele and lymph vessel dilatation (lymphangiectasia) can be detected by this procedure. As with adult males, older children with asymptomatic bancroftian microfilaraemia were shown to harbour live adult worms in the scrotal lymphatics. Ultrasound examination using a 7 5 MHz probe in eight boys aged years revealed the existence of adult filarial worms indicated by the filaria dance sign (FDS) in the nests along with diffuse dilatation of the lymphatic vessels. FDS was also present in crural lymphatics and axillary lymph node in two girls aged 9 and 7 years respectively. FDS was detected even in one Lymphoscintigraphy in LF infection in children Lymphoscintigraphy has been carried out earlier in subjects with established lymphoedema of the limbs to delineate the underlying pathology of the lymph vessels and lymph nodes such as delayed or absent transport of the radiotracer, tortuous and bizarre deep lymphatics, dermal diffusion, retrograde tracer flow and faint or absent regional nodal visualization (Witte et al. 1993). More recently, lymphoscintigraphic studies have documented abnormal lymphatics even in asymptomatic individuals who had only circulating microfilaraemia due to W. bancrofti infection suggesting that lymphatic damage preceded onset of clinical disease (Freedman et al. 1994). In a B. malayi-endemic area LSG was carried out in 100 children, 3 15 year-olds, who had either asymptomatic microfilaraemia, history or evidence of filarial disease or were positive for filariasis-specific
5 Lymphatic filariasis in children 1563 A B Fig. 2. (A). Ultrasound examination (B mode) of the right axilla of a 9 year-old male with asymptomatic microfilaremia showing the site of a dilated lymph vessel (arrow) with the filaria dance sign (FDS), indicating presence of adult parasite nest. (B). Colour Power Doppler (CPD) examination of the site of FDS above. Arrow points to the area of FDS, which shows irregular mosaic signals on CPD that are different from the characteristic signals produced from blood vessels. IgG4 antibody. This was done by intradermally injecting 0 5 ml of a solution containing 2 μci of Tc 99m -tagged sulphur colloid into the first web spaces of both feet and hands and the lymphatics were imaged using gamma camera (Shenoy et al. 2007b). Dilated lymphatic channels were seen in 80 of the 100 children. This included 81% of the microfilaraemics (Fig. 3A and 3B), 79% children with filarial disease and 79% of those who were only IgG4 positive. Five children who had lymph vessel dilation were only three years old. Dilated lymph vessels (LV), with tortuosity in some subjects, were commonly seen in the lower limbs. Upper limb involvement was less common. Both in the upper and lower limbs the entire length of the affected lymphatics appeared dilated. Inguinal, axillary and less commonly popliteal or epitrochlear lymph nodes were visualized on lymphoscintigraphy in all the 100 children examined. This study demonstrated that LF infection in children is associated with subclinical pathology even in the pre symptomatic phase of the infection when they had only microfilaraemia or were only IgG4 positive (Shenoy et al. 2008). Histopathology of LF infection in children A not uncommon clinical manifestation of bancroftian filariasis in children in endemic areas is presentation with enlarged lymph nodes or soft tissue swellings in the axilla, groin or neck. Biopsy and histopathological studies of these lymph nodes and tissues demonstrated the presence of adult filarial parasites and mf associated with marked dilation of lymph vessels in these children who did not have any other evidence of filarial disease (Figueredo-Silva et al. 1994; Dreyer et al. 2001). The fact that lymphangiectasia is not restricted to the exact segment where the adult worms are located indicates that it may be the result of the action of soluble parasite-specific factors or excretory products on responsive lymphatic endothelial cells. Live parasites were not associated with any inflammatory reaction in the lymph vessels, while dead worms induced granulomatous inflammatory reaction with variable numbers of eosinophils, lymphocytes, plasma cells and large macrophages. There may be large numbers of eosinophils, especially in cases treated with DEC (Figueredo-Silva et al. 2002). Another important aspect of the pathology of LF has been the finding that the bacterial endosymbionts Wolbachia, present in the filarial parasites, may be responsible for the inflammatory process associated with the progression of this disease. Exposure to Wolbachia lipoproteins could be responsible for promoting lymphangiogenesis, lymphatic endothelial proliferation and dilation of lymph vessels, which are known to result in chronic manifestations of LF disease (Taylor et al. 2010). Studies are needed on this aspect of LF in children. Social and psychological impact of LF in the young LF disease poses several important problems in childhood and adolescence. The social and
6 Ranganatha Krishna Shenoy and Moses J. Bockarie 1564 A B Fig. 3. (A). Lymphoscintigraph of a 9 year-old boy with asymptomatic microfilaraemia showing lymph vessel dilation in both legs (left panel). (B). Note absence of lymph vessel dilation in the legs on 30 months follow up, after administration of five doses of DEC and albendazole once every six months. psychological impact of this malady in this age group had been addressed in some studies in the affected communities. The clinical manifestations of LF in the younger age group were associated with social stigma and psychological problems that interfered with their education and self-confidence. In a study conducted in two villages in South India, 28 subjects aged <20 years had clinical manifestations that included lymphoedema and ADLA attacks. Hydrocele was present in boys aged years. Their social problems included feeling of shame, embarrassment and ridicule especially due to hydrocele. The presence of hydrocele and lymphoedema even interfered with their conventional school dress. Frequent absence from school due to the acute attacks and sometimes discontinuation of studies in this population would have socio-economic implications for their future (Ramaiah and Vijay Kumar, 2000). This chronic disease may thus interfere with the quality of life of these children as they develop. Diagnosis of LF infection and disease in children Children living in LF-endemic communities have a higher risk of developing the infection, which is first acquired by many in their early childhood itself. The dilatation of the lymphatics, which is the early and basic sub-clinical pathology induced by the adult worms, once established is reported to be irreversible even with treatment (Freedman et al. 1995). In the affected limbs this persistent lymphatic damage predisposes to later development of lymph stasis, secondary bacterial infections precipitating ADLA attacks, consequent development of lymphoedema and its progression (Shenoy et al. 1999). Therefore detection of LF infection in the early asymptomatic stage itself and prompt treatment are important in preventing future chronic disability. The investigations that are useful for diagnosis in the early stages are examination of thick blood-smears obtained at night for presence of mf; Nuclepore membrane filtration to quantify the parasitaemia, ICT card test or Og4C3 test for filarial antigenaemia in WB infection and filariasis-specific IgG4 antibody test in BM infection. USG and DSG may be employed in doubtful situations to detect any FDS, though this is not as specific as the other two methods. LSG being a costly investigation is rarely employed for routine diagnosis of LF infection. There is scope for future development of diagnostics in LF infection in children such as refinement in the use of PCR technique and detection of filariasis-specific antigen/ antibodies. Once the subject presents with swelling of the limbs or with an ADLA attack, a clinical diagnosis of LF is suspected under certain circumstances such as the subject residing in a region endemic for LF, familial clustering of such cases, swelling more often unilateral involving the lower limbs or rarely upper limbs of long duration except during initial stages and asymmetry of the swelling when bilateral. The oedema is pitting in early stages, though non-pitting due to thickening of skin in the later stages. This stage
7 Lymphatic filariasis in children is uncommon in children since the thickening of skin depends on longer duration of disease. Presentation with lymphoedema or hydrocele are seen mostly in children >10 years of age. In special situations, investigations like CT, MRI and MR angiography are sometimes employed in children to differentiate filarial swelling from other causes of lymphoedema like malformations of lymph vessels seen in association with certain congenital diseases (Stanton et al. 2000). Management of LF infection and disease in children Treatment of LF infection. DEC is the drug of choice when there is active infection from W. bancrofti, B. malayi or B. timori. Though it is very effective as a microfilaricidal agent, DEC kills only around 50% of adult worms. Even though the standard dose of DEC recommended in LF over the years was 6 mg/kg daily for 12 days, recent studies have shown that a single dose of 6 mg/kg is as effective as the 12-day course both against the mf and adult worms (Gyapong et al. 2005). In early stages of lymphoedema, DEC may be helpful if there is active filarial infection and its use might prevent further lymphatic damage through its macrofilaricidal action. The other antifilarial drugs, ivermectin and albendazole, even though important in the sustained reduction of blood mf levels and arresting LF transmission, have no role in the management of lymphoedema or acute attacks. Treatment of ADLA. These attacks can easily be treated and further episodes prevented. Bed rest, elevation of the affected limb and symptomatic treatment with simple drugs like paracetamol are sufficient in mild cases. Any local precipitating entry lesions like injury and bacterial or fungal infection should be treated with local antibiotic or antifungal ointments or with systemic antibiotics where needed. Proper and regular practice of local hygiene measures of the affected limbs are effective in preventing ADLA attacks (Shenoy et al. 1998). This is aimed at prevention of fungal and bacterial infections and has become the mainstay for disability alleviation in GPELF (Ottesen, 2000). Treatment of lymphoedema. In early lymphoedema, occasionally seen in older children, applying elastocrepe bandage to the affected limb while ambulant and keeping the limb elevated at night are effective to obtain relief. Anti-Wolbachia therapy in LF. Studies in adults with LF infection have documented the encouraging results of treatment with doxycycline at 200 mg daily given for varying periods from 3 to 8 weeks. This has resulted in long-term sterility and eventual death of 1565 the adult worms (Taylor et al. 2010). There are presently no reports of such a protracted course of doxycycline treatment in children with LF. Due to the adverse effects that doxycycline is known to cause, this drug is generally not used in pregnant women and children (Taylor et al. 2010). It may be recalled here that in a recent study on BM infection in children the presently available anti-filarial drugs are generally well tolerated and effective in clearing microfilaraemia and the FDS indicating presence of live adult worms and also in reversing the early subclinical lymphatic pathology (Shenoy et al. 2009). Prevention of LF infection and disease in children Prevention of filarial infection in children can be achieved either through arresting the parasite transmission by reducing the mf load in the community employing mass drug administration (MDA), by thorough vector control or by preventing man-vector contact. Of these, MDA initiated by GPELF is now the most effective method since Presently 53 out of the initially identified 81 LF-endemic countries are under MDA (WHO, 2010c). In countries endemic for bancroftian infection, 4 6 annual rounds of MDA have been found to be effective in lowering the mf levels in the community, in reducing the filarial antigen levels in the population including children and thus preventing parasite transmission in the treated communities (Ramaiah et al. 2002, 2007). In children from a WBendemic area treated with DEC and albendazole, FDS indicating adult worm nests disappeared after treatment (Fox et al. 2005). In assessing the impact of GPELF after 8 years of its institution, it is reported that this has prevented LF disease in 6 6 million newborns who would otherwise have acquired LF, thus averting in their lifetimes nearly 1 4 million cases of hydrocele, 800,000 cases of lymphoedema and 4 4 million cases of subclinical disease (Ottesen et al. 2008). In a recently published study in children with Brugia malayi infection in India, it was demonstrated for the first time that anti-filarial drugs in doses employed in MDA by the GPELF, reversed the subclinical lymphatic pathology. In this study, tests for antifilarial IgG4, Doppler ultrasonography and lymphoscintigraphy were employed to identify the sub-clinical pathology in 100 children. They were either asymptomatic microfilaraemic, amicrofilaraemic but had past or present filarial disease or were asymptomatic amicrofilaraemic but positive only for IgG4. They were treated every six months with single combined doses of DEC (6 mg/kg) and albendazole (400 mg) and followed up for three years. At the end of three years all children were amicrofilaraemic, FDS was abolished in the 14 children who were initially positive and the lymphoedema (grade II) had
8 Ranganatha Krishna Shenoy and Moses J. Bockarie disappeared in all the four girls who had it initially. Lymphoscintigraphy at the last follow-up revealed that the lymph node and vessel damage observed during enrollment had reversed in 89 6% children. They included 96% of the mf positives, 85% of those with filarial disease and 87 5% of those who were only positive for IgG4 (Shenoy et al. 2009). These results suggest that MDA is effective in reversing the subclinical pathology induced by the adult worms in children, if they are treated early in LF infection. This is in contrast to the findings reported in adults that the sub-clinical pathology once established is irreversible even with treatment (Freedman et al. 1995). In the context of GPELF, the present guidelines for interruption of LF transmission require that after achieving a microfilaraemia prevalence status of <1%, a sample of 3000 children in the age group of 6 10 years should be tested for filarial antigenaemia with the ICT card test. If one or more children are positive, MDA has to be continued and also that such children are investigated and treated (WHO, 2000). This indicates the importance of parasitaemia in children in the transmission of LF. In the present scenario of integrated vector management, the use of mosquito repellant-impregnated bed nets will be helpful in preventing LF infection in children in communities where there is co-endemicity of malaria, filariasis and other vectorborne parasitic infections. DISCUSSION It is being increasingly appreciated that, in endemic countries, filarial parasites infect children early in life. Though asymptomatic at this stage, recently available diagnostic techniques have made it possible to recognize LF infection and sub-clinical lymphatic damage in children. Apart from microfilaraemia, circulating filarial antigen in WB infection, filariasisspecific IgG4 antibody in BM infection, nests of live adult parasites in the lymphatics and the subclinical changes in the lymph vessels can all now be detected. The sub-clinical pathology caused by the adult worms in infected children is extensive in the affected lymph vessels, though these subjects do not have disease manifestations until later in their adult life (Figueredo-Silva et al. 2002; Shenoy et al. 2008). The gravity of this public health issue in LF-endemic countries can be understood when it is known that LF infection occurs in 10% of the at-risk population; 66 7% of such infections have sub-clinical damage, 20 8% result in hydrocele and 12 5% result in lymphoedema (Ottesen et al. 2008). The MDA under GPELF being carried out among the at-risk population in endemic countries for the last nine years has prevented disease in many children born after MDA commenced (Ottesen et al. 2008). In this programme children aged 2 years and above are 1566 included. The drug albendazole, with either DEC or ivermectin, used in mass drug treatment is mainly aimed at preventing parasite transmission and ultimately eliminating LF infection in treated communities. The intention is thus primary prevention of the disease. In the last eight years, MDA is estimated to have prevented LF disease in 6 6 million future newborns and averted in their lifetimes nearly 1 4 million cases of hydrocele, 800,000 cases of lymphoedema and 4 4 million cases of subclinical disease which they would otherwise are expected to develop (Ottesen et al. 2008). There have been many earlier reports indicating the beneficial effects of drugs used in MDA especially DEC, such as improvement or reduction in the incidence of lymphoedema, hydrocele and ADLA in treated communities (March et al. 1960; Meyrowitsch and Simonsen, 1998; Bockarie et al. 2002; Meyrowitsch et al. 2004). Hitherto the assumption has been that the underlying lymphangiectasia could not be reversed even after treatment. Now it has been shown that, at least in B. malayi infection in children, the sub-clinical pathology can be reversed by the drugs DEC and albendazole in doses used in MDA (Shenoy et al. 2007a). This indicates that MDA is also capable of secondary prevention of LF. This finding has tremendous impact in the present LF elimination campaign. The foot care or limb hygiene programme recommended under disability management of GPELF is very effective in preventing the occurrence of acute ADLA attacks in LF. These episodes are responsible for worsening the lymphatic damage and future development of swelling in the limbs (Shenoy et al. 1999). In children having asymptomatic LF infection, the underlying sub-clinical lymphatic damage predisposes them to acute attacks following minor injuries or bacterial skin infections. They are thus prone to develop lymphoedema which, when established, is difficult to reverse. So to prevent this disability, regular foot-care must be instituted in at-risk children in endemic communities from an early age. Innovative approaches, such as introduction of this foot-care programme in the school curriculum in endemic areas, would be a progressive step in this direction (Shenoy, 2006). Apart from elimination of LF infection, mass treatment of children in endemic countries with albendazole and ivermectin has been shown to have other beyond-lf benefits. Both these drugs are also effective against intestinal, soil-transmitted helminthiases (STH), namely hookworm, roundworm and whipworm infection, which are very common in children. In addition, ivermectin is efficacious against Strongyloides stercoralis. Recent studies indicate that combining ivermectin and albendazole result in high cure rates in Trichuris trichura infection also (Knopp et al. 2010). STH infections are prevalent throughout the pan-tropical belt where LF is endemic (de Silva
9 Lymphatic filariasis in children et al. 2003). Mass treatment with these drugs has beneficial effects in treated children including increased appetite and weight gain, greater learning ability and concentration, better school attendance and prevention of anaemia (Stephenson et al. 1993; Adams et al. 1994). The above findings support the need for strengthening efforts to ensure high treatment coverage among eligible children at-risk since the benefits extend well beyond clearance of LF infections. Programme managers and pediatricians in endemic countries recognizing the invisible disability imposed by filarial infection should institute simple measures of hygiene to alleviate morbidity in these children. MDA should no longer be viewed as a measure for interrupting transmission alone. Recent findings of reversibility of early lymphatic pathology in treated children provide ample proof that both the MDA strategy and foot-hygiene measures can be viewed as an effective measure in preventing and managing morbidity. Programme managers should effectively utilize this information to strengthen their advocacy efforts to achieve high and sustainable coverage in MDA (Shenoy et al. 2009). ACKNOWLEDGEMENTS We thank Rinki Deb for her assistance with the manuscript. The Centre for Neglected Tropical Diseases, Liverpool School of Tropical Medicine is funded by the UK Department for International Development (DFID). The British Society for Parasitology covered the local travel and accommodation expenses for Moses Bockarie. REFERENCES Adams, E. J., Stephenson, L. S., Latham, M. C. and Kinoti, S. N. (1994). Physical activity and growth of Kenyan school children with hookworm, Trichuris trichiura and Ascaris lumbricoides infections are improved after treatment with albendazole. Journal of Nutrition 124, Alexander, N. D., Kazura, J. W., Bockarie, M. J., Perry, R. T., Dimber, Z. B., Grenfell, B. T. and Alpers, M. P. (1998). Parental infection confounded with local infection intensity as risk factors for childhood microfilaraemia in bancroftian filariasis. Transactions of the Royal Society of Tropical Medicine and Hygiene 92, Bockarie, M. J. and Molyneux, D. H. (2009). The end of lymphatic filariasis? British Medical Journal 338, b1686. Bockarie, M. J., Pedersen, E. M., White, G. B. and Michael, E. (2009). Role of vector control in the global program to eliminate lymphatic filariasis. Annual Review of Entomology 54, doi: /annurev. ento Bockarie, M. J., Tisch, D. J., Kastens, W., Alexander, N. D., Dimber, Z., Bockarie, F., Ibam, E., Alpers, M. P. and Kazura, J. W. (2002). Mass treatment to eliminate filariasis in Papua New Guinea. New England Journal of Medicine 347, doi: /NEJMoa /23/1841 [pii]. Das, P. K., Sirvidya, A., Vanamail, P., Ramaiah, K. D., Pani, S. P., Michael, E. and Bundy, D. A. (1997). Wuchereria bancrofti microfilaraemia in children in relation to parental infection status. Transactions of Royal Society of Tropical Medicine and Hygiene 91, de Silva, N. R., Brooker, S., Hotez, P. J., Montresor, A., Engels, D. and Savioli, L. (2003). Soil-transmitted helminth infections: updating the global picture. Trends in Parasitology 19, doi: S [pii]. Dreyer, G., Figueredo-Silva, J., Carvalho, K., Amaral, F. and Ottesen, E. A. (2001). Lymphatic filariasis in children: adenopathy and 1567 its evolution in two young girls. American Journal of Tropical Medicine and Hygiene 65, Dreyer, G., Noroes, J., Addiss, D., Santos, A., Medeiros, Z. and Figueredo-Silva, J. (1999). Bancroftian filariasis in a paediatric population: an ultrasonographic study. Transactions of Royal Society of Tropical Medicine and Hygiene 93, Figueredo-Silva, J., Dreyer, G., Guimaraes, K., Brandt, C. and Medeiros, Z. (1994). Bancroftian lymphadenopathy: absence of eosinophils in tissues despite peripheral blood hypereosinophilia. Journal of Tropical Medicine and Hygiene 97, Figueredo-Silva, J., Noroes, J., Cedenho, A. and Dreyer, G. (2002). The histopathology of bancroftian filariasis revisited: the role of the adult worm in the lymphatic-vessel disease. Annals of Tropical Medicine & Parasitology 96, doi: / Fox, L. M., Furness, B. W., Haser, J. K., Brissau, J. M., Louis- Charles, J., Wilson, S. F., Addiss, D. G., Lammie, P. J. and Beach, M. J. (2005). Ultrasonographic examination of Haitian children with lymphatic filariasis: a longitudinal assessment in the context of antifilarial drug treatment. American Journal of Tropical Medicine and Hygiene 72, doi: 72/5/642 [pii]. Freedman, D. O., Bui, T., De Almeida Filho, P. J., Braga, C., Maia e Silva, M. C., Maciel, A. and Furtado, A. F. (1995). Lymphoscintigraphic assessment of the effect of diethylcarbamazine treatment on lymphatic damage in human bancroftian filariasis. American Journal of Tropical Medicine and Hygiene 52, Freedman, D. O., de Almeida Filho, P. J., Besh, S., Maia e Silva, M. C., Braga, C. and Maciel, A. (1994). Lymphoscintigraphic analysis of lymphatic abnormalities in symptomatic and asymptomatic human filariasis. Journal of Infectious Diseases 170, Gyapong, J. O., Kumaraswami, V., Biswas, G. and Ottesen, E. A. (2005). Treatment strategies underpinning the global programme to eliminate lymphatic filariasis. Expert Opinion Pharmacotherapy 6, doi: EOP [pii] / Jungmann, P., Figueredo-Silva, J. and Dreyer, G. (1991). Bancroftian lymphadenopathy: a histopathologic study of fifty-eight cases from northeastern Brazil. American Journal of Tropical Medicine and Hygiene 45, Knopp, S., Mohammed, K. A., Speich, B., Hattendorf, J., Khamis, I. S., Stothard, J. R., Rollinson, D., Marti, H. and Utzinger, J. (2010). Albendazole and mebendazole administered alone or in combination with ivermectin against Trichuris trichiura: a randomized controlled trial. Clinical Infectious Diseases 51, Lammie, P. J., Hitch, W. L., Walker Allen, E. M., Hightower, W. and Eberhard, M. L. (1991). Maternal filarial infection as risk factor for infection in children. Lancet 337, Lammie, P. J., Reiss, M. D., Dimock, K. A., Streit, T. G., Roberts, J. M. and Eberhard, M. L. (1998). Longitudinal analysis of the development of filarial infection and antifilarial immunity in a cohort of Haitian children. American Journal of Tropical Medicine and Hygiene 59, Mand, S., Supali, T., Djuardi, J., Kar, S., Ravindran, B. and Hoerauf, A. (2006). Detection of adult Brugia malayi filariae by ultrasonography in humans in India and Indonesia. Tropical Medicine and International Health 11, doi: TMI1693 [pii] /j x. March, H. N., Laigret, J., Kessel, J. F. and Bambridge, B. (1960). Reduction in the prevalence of clinical filariasis in Tahiti following adoption of a control program. American Journal of Tropical Medicine and Hygiene 9, Meyrowitsch, D. W. and Simonsen, P. E. (1998). Long-term effect of mass diethylcarbamazine chemotherapy on bancroftian filariasis, results at four years after start of treatment. Transactions of the Royal Society of Tropical Medicine and Hygiene 92, Meyrowitsch, D. W., Simonsen, P. E. and Magesa, S. M. (2004). Longterm effect of three different strategies for mass diethylcarbamazine administration in bancroftian filariasis: follow-up at 10 years after treatment. Transactions of the Royal Society of Tropical Medicine and Hygiene 98, doi: /j.trstmh S [pii]. Ottesen, E. A. (2000). The global programme to eliminate lymphatic filariasis. Tropical Medicine and International Health 5, doi: tmi620 [pii]. Ottesen, E. A., Hooper, P. J., Bradley, M. and Biswas, G. (2008). The global programme to eliminate lymphatic filariasis: health impact after 8 years. PLOS Neglected Tropical Diseases 2, e317. doi: /journal. pntd Pani, S. P., Balakrishnan, N., Srividya, A., Bundy, D. A. and Grenfell, B. T. (1991). Clinical epidemiology of bancroftian filariasis: effect of age and gender. Transactions of Royal Society of Tropical Medicine and Hygiene 85,
10 Ranganatha Krishna Shenoy and Moses J. Bockarie Pani, S. P., Yuvaraj, J., Vanamail, P., Dhanda, V., Michael, E., Grenfell, B. T. and Bundy, D. A. (1995). Episodic adenolymphangitis and lymphoedema in patients with bancroftian filariasis. Transactions of Royal Society of Tropical Medicine and Hygiene 89, Ramaiah, K. D., Ramu, K., Kumar, K. N. and Guyatt, H. (1996). Epidemiology of acute filarial episodes caused by Wuchereria bancrofti infection in two rural villages in Tamil, Nadu, south India. Transactions of Royal Society of Tropical Medicine and Hygiene 90, Ramaiah, K. D., Vanamail, P. and Das, P. K. (2007). Changes in Wuchereria bancrofti infection in a highly endemic community following 10 rounds of mass administration of diethylcarbamazine. Transactions of Royal Society of Tropical Medicine and Hygiene 101, doi: S (06) [pii] /j.trstmh Ramaiah, K. D., Vanamail, P., Pani, S. P., Yuvaraj, J. and Das, P. K. (2002). The effect of six rounds of single dose mass treatment with diethylcarbamazine or ivermectin on Wuchereria bancrofti infection and its implications for lymphatic filariasis elimination. Tropical Medicine and International Health 7, doi: 935 [pii]. Ramaiah, K. D. and Vijay Kumar, K. N. (2000). Effect of lymphatic filariasis on school children. Acta Tropica 76, doi: S X(00) [pii]. Rahmah, N., Shenoy, R. K., Nutman, T. B., Weiss, N., Gilmour, K., Maizels, R. M., Yazdanbakhsh, M. and Sartono, E. (2003). Multicentre laboratory evaluation of Brugia Rapid dipstick test for detection of brugian filariasis. Tropical Medicine and International Health 8, doi: 1102 [pii]. Rahmah, N., Taniawati, S., Shenoy, R. K., Lim, B. H., Kumaraswami, V., Anuar, A. K., Hakim, S. L., Hayati, M. I., Chan, B. T., Suharni, M. and Ramachandran, C. P. (2001). Specificity and sensitivity of a rapid dipstick test (Brugia Rapid) in the detection of Brugia malayi infection. Transactions of Royal Society of Tropical Medicine and Hygiene 95, Seim, A. R., Dreyer, G. and Addiss, D. G. (1999). Controlling morbidity and interrupting transmission: twin pillars of lymphatic filariasis elimination. Revista da Sociedade Brasileria de Medicina Tropical 32, Shenoy, R. K. (2006). Lymphatic filariasis in children. Journal of Communicable Diseases 38, Shenoy, R. K., John, A., Hameed, S., Suma, T. K. and Kumaraswami, V. (2000). Apparent failure of ultrasonography to detect adult worms of Brugia malayi. Annals of Tropical Medicine and Parasitology 94, Shenoy, R. K., Kumaraswami, V., Suma, T. K., Rajan, K. and Radhakuttyamma, G. (1999). A double-blind, placebo-controlled study of the efficacy of oral penicillin, diethylcarbamazine or local treatment of the affected limb in preventing acute adenolymphangitis in lymphoedema caused by brugian filariasis. Annals of Tropical Medicine and Parasitology 93, Shenoy, R. K., Suma, T. K., Kumaraswami, V., Padma, S., Rahmah, N., Abhilash, G. and Ramesh, C. (2007a). Doppler ultrasonography reveals adult-worm nests in the lymph vessels of children with brugian filariasis. Annals of Tropical Medicine and Parasitology 101, doi: / X Shenoy, R. K., Suma, T. K., Kumaraswami, V., Rahmah, N., Dhananjayan, G., Padma, S., Abhilash, G. and Ramesh, C. (2007b). Preliminary findings from a cross-sectional study on lymphatic filariasis in children, in an area of India endemic for Brugia malayi infection. Annals of Tropical Medicine and Parasitology 101, doi: / X Shenoy, R. K., Suma, T. K., Rajan, K. and Kumaraswami, V. (1998). Prevention of acute adenolymphangitis in brugian filariasis: comparison of the efficacy of ivermectin and diethylcarbamazine, each combined with local 1568 treatment of the affected limb. Annals of Tropical Medicine and Parasitology 92, Shenoy, R. K., Suma, T. K., Kumaraswami, V., Dhananjayan, G., Rahmah, N., Abhilash, G. and Ramesh, C. (2008). Lymphoscintigraphic evidence of lymph vessel dilation in the limbs of children with Brugia malayi infection. Journal of Communicable Diseases 40, Shenoy, R. K., Suma, T. K., Kumaraswami, V., Rahmah, N., Dhananjayan, G. and Padma, S. (2009). Antifilarial drugs, in the doses employed in mass drug administrations by the Global Programme to Eliminate Lymphatic Filariasis, reverse lymphatic pathology in children with Brugia malayi infection. Annals of Tropical Medicine and Parasitology 103, doi: / X Stanton, A. W., Badger, C. and Sitzia, J. (2000). Non-invasive assessment of the lymphedematous limb. Lymphology 33, Stephenson, L. S., Latham, M. C., Adams, E. J., Kinoti, S. N. and Pertet, A. (1993). Physical fitness, growth and appetite of Kenyan school boys with hookworm, Trichuris trichiura and Ascaris lumbricoides infections are improved four months after a single dose of albendazole. Journal of Nutrition 123, Suma, T. K., Shenoy, R. K. and Kumaraswami, V. (2002). Efficacy and sustainability of a footcare programme in preventing acute attacks of adenolymphangitis in Brugian filariasis. Tropical Medicine and International health 7, doi: 914 [pii]. Sunish, I. P., Rajendran, R., Mani, T. R., Munirathinam, A., Tewari, S. C., Hiriyan, J., Gajanana, A. and Satyanarayana, K. (2002). Resurgence in filarial transmission after withdrawal of mass drug administration and the relationship between antigenaemia and microfilaraemia a longitudinal study. Tropical Medicine and International Health 7, doi: _828 [pii]. Taylor, M. J., Hoerauf, A. and Bockarie, M. (2010). Lymphatic filariasis and onchocerciasis. Lancet 376, doi: S (10) [pii] /S (10) Vanamail, P., Ramaiah, K. D., Krishnamoorthy, K., Pani, S. P. and Das, P. K. (1992). Distribution oif microfilaria carriers and clinical cases of bancroftian filariasis in relation to family size in an urban situation. Tropical Biomedicine 9, Vanamail, P., Subramanian, S., Das, P. K., Pani, S. P. and Bundy, D. A. P. (1989). Familial clusttering in Wuchereria bancrofti infection. Tropical Biomedicine 6, Weil, G. J. and Ramzy, R. M. (2007). Diagnostic tools for filariasis elimination programs. Trends in Parasitology 23, doi: S (06) [pii] /j.pt World Health Organization (2000). Preparing and implementing a national plan to eliminate lymphatic filariasis. WHO/CDS/CPE/CEE/ , 29 pp. World Health Organization (2010a). Global programme to eliminate lymphatic filariasis. Weekly Epidemiological Record 85, World Health Organization (2010b). Working to overcome the global impact of neglected tropical diseases. First WHO Report on Neglected Tropical Diseases, WHO/HTM/NTD/2010.1, 172 pp. World Health Organization (2010c). World Health Organization Global Programme to Eliminate Lymphatic Filariasis: Progress report and strategic plan of the global programme to eliminate lymphatic filariasis: halfway towards eliminating lymphatic filariasis. WHO/HTM/NTD/PCT/2010.6, 79 pp. Witt, C. and Ottesen, E. A. (2001). Lymphatic filariasis: an infection of childhood. Tropical Medicine and International Health 6, doi: tmi765 [pii]. Witte, M. H., Jamal, S., Williams, W. H., Witte, C. L., Kumaraswami, V., McNeill, G. C., Case, T. C. and Panicker, T. M. (1993). Lymphatic abnormalities in human filariasis as depicted by lymphangioscintigraphy. Archives of Internal Medicine 153,
Clinical and Pathological Aspects of Filarial Lymphedema and Its Management
 MINI-REVIEW Korean J Parasitol. Vol. 46, No. 3: 119-125, September 2008 DOI: 10.3347/kjp.2008.46.3.119 Clinical and Pathological Aspects of Filarial Lymphedema and Its Management R. K. Shenoy Filariasis
MINI-REVIEW Korean J Parasitol. Vol. 46, No. 3: 119-125, September 2008 DOI: 10.3347/kjp.2008.46.3.119 Clinical and Pathological Aspects of Filarial Lymphedema and Its Management R. K. Shenoy Filariasis
Evaluation of the ICT whole blood antigen card test to detect infection due to nocturnally periodic Wuchereria bancrofti in South India
 TMIH559 Tropical Medicine and International Health volume 5 no 5 pp 359 363 may 2000 Evaluation of the ICT whole blood antigen card test to detect infection due to nocturnally periodic Wuchereria bancrofti
TMIH559 Tropical Medicine and International Health volume 5 no 5 pp 359 363 may 2000 Evaluation of the ICT whole blood antigen card test to detect infection due to nocturnally periodic Wuchereria bancrofti
PARASITOLOGY CASE HISTORY #13 (BLOOD PARASITES) (Lynne S. Garcia)
 PARASITOLOGY CASE HISTORY #13 (BLOOD PARASITES) (Lynne S. Garcia) An epidemiologic survey was undertaken in a small town in Myanmar (Burma) endemic for lymphatic filariasis. Blood specimens were collected
PARASITOLOGY CASE HISTORY #13 (BLOOD PARASITES) (Lynne S. Garcia) An epidemiologic survey was undertaken in a small town in Myanmar (Burma) endemic for lymphatic filariasis. Blood specimens were collected
A survey on foot care practices among filarial lymphoedema patients in Orissa, India
 Tropical Biomedicine 24(2): 7 14 (2007) A survey on foot care practices among filarial lymphoedema patients in Orissa, India Bontha V. Babu, Abhay N. Nayak and Anna S. Kerketta Division of Epidemiology,
Tropical Biomedicine 24(2): 7 14 (2007) A survey on foot care practices among filarial lymphoedema patients in Orissa, India Bontha V. Babu, Abhay N. Nayak and Anna S. Kerketta Division of Epidemiology,
SEA-CD-275. Frequently asked questions
 SEA-CD-275 Frequently asked questions on LYMPHATIC FILARIASIS (ELEPHANTIASIS) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate
SEA-CD-275 Frequently asked questions on LYMPHATIC FILARIASIS (ELEPHANTIASIS) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate
44th Myanmar Health Research Congress
 44th Myanmar Health Research Congress Early Detection of Lymphatic Disturbance in Adolescent Infected with Lymphatic Filariasis Jan Douglass 1, Susan Gordon 1, Patricia Graves 1, Ben Dickson 1, Dr Ni Ni
44th Myanmar Health Research Congress Early Detection of Lymphatic Disturbance in Adolescent Infected with Lymphatic Filariasis Jan Douglass 1, Susan Gordon 1, Patricia Graves 1, Ben Dickson 1, Dr Ni Ni
Regional Medical Research Centre (ICMR), Field Practice Unit, Car Nicobar Andaman & Nicobar Islands & *
 Indian J Med Res 141, March 2015, pp 330-339 Impact on prevalence of intestinal helminth infection in school children administered with seven annual rounds of diethyl carbamazine (DEC) with albendazole
Indian J Med Res 141, March 2015, pp 330-339 Impact on prevalence of intestinal helminth infection in school children administered with seven annual rounds of diethyl carbamazine (DEC) with albendazole
An Operational Research on Annual Mass Drug Administration (MDA) For Elimination of Lymphatic Filariasis in Medak District, Telangana
 Original Research Article An Operational Research on Annual Mass Drug Administration (MDA) For Elimination of Lymphatic Filariasis in Medak District, Telangana P. Samuel Rajkumar 1*, Tukaram Kishanrao
Original Research Article An Operational Research on Annual Mass Drug Administration (MDA) For Elimination of Lymphatic Filariasis in Medak District, Telangana P. Samuel Rajkumar 1*, Tukaram Kishanrao
INTRODUCTION MATERIALS AND METHODS
 Am. J. Trop. Med. Hyg., 70(2), 2004, pp. 191 196 Copyright 2004 by The American Society of Tropical Medicine and Hygiene A RANDOMIZED CLINICAL TRIAL COMPARING SINGLE- AND MULTI-DOSE COMBINATION THERAPY
Am. J. Trop. Med. Hyg., 70(2), 2004, pp. 191 196 Copyright 2004 by The American Society of Tropical Medicine and Hygiene A RANDOMIZED CLINICAL TRIAL COMPARING SINGLE- AND MULTI-DOSE COMBINATION THERAPY
Module 2. NTD Strategies
 Overview LF and Trachoma MMDP Spectrum of morbidity associated with LF and its impact Cause and management of lymphoedema caused by LF Cause and management of hydrocele caused by LF How LF morbidity management
Overview LF and Trachoma MMDP Spectrum of morbidity associated with LF and its impact Cause and management of lymphoedema caused by LF Cause and management of hydrocele caused by LF How LF morbidity management
Multicentre laboratory evaluation of Brugia Rapid dipstick test for detection of brugian filariasis
 Tropical Medicine and International Health volume 8 no 10 pp 895 900 october 2003 Multicentre laboratory evaluation of Brugia Rapid dipstick test for detection of brugian filariasis N. Rahmah 1, R. K.
Tropical Medicine and International Health volume 8 no 10 pp 895 900 october 2003 Multicentre laboratory evaluation of Brugia Rapid dipstick test for detection of brugian filariasis N. Rahmah 1, R. K.
Effect of aggressive prolonged diethylcarbamazine therapy on circulating antigen levels in bancroftian lariasis
 Tropical Medicine and International Health volume 6 no 1 pp 37±41 january 2001 Effect of aggressive prolonged diethylcarbamazine therapy on circulating antigen levels in bancroftian lariasis David O. Freedman
Tropical Medicine and International Health volume 6 no 1 pp 37±41 january 2001 Effect of aggressive prolonged diethylcarbamazine therapy on circulating antigen levels in bancroftian lariasis David O. Freedman
The Filarial Dance Sign in Scrotal Filarial Infection
 The Filarial Dance Sign in Scrotal Filarial Infection Poster No.: C-0232 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit P. P. Suthar 1, N. Patel 2 ; 1 Vadodara, Gu/IN, 2 Vadodara,
The Filarial Dance Sign in Scrotal Filarial Infection Poster No.: C-0232 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit P. P. Suthar 1, N. Patel 2 ; 1 Vadodara, Gu/IN, 2 Vadodara,
Epidemiology and immunopathology of bancroftian filariasis
 Microbes and Infection, 1, 1999, 1015 1022 1999 Éditions scientifiques et médicales Elsevier SAS. All rights reserved Review Epidemiology and immunopathology of bancroftian filariasis Adriana B. de Almeida*,
Microbes and Infection, 1, 1999, 1015 1022 1999 Éditions scientifiques et médicales Elsevier SAS. All rights reserved Review Epidemiology and immunopathology of bancroftian filariasis Adriana B. de Almeida*,
Downloaded from:
 O Hara, GA; Elliott, AM (2016) HIV and Helminths - Not All Worms Created Equal? Trends in parasitology. ISSN 1471-4922 DOI: https://doi.org/10.1016/j.pt.2016 Downloaded from: http://researchonline.lshtm.ac.uk/3327115/
O Hara, GA; Elliott, AM (2016) HIV and Helminths - Not All Worms Created Equal? Trends in parasitology. ISSN 1471-4922 DOI: https://doi.org/10.1016/j.pt.2016 Downloaded from: http://researchonline.lshtm.ac.uk/3327115/
IN THIS ISSUE: LYMPHATIC FILARIASIS: ELIMINATING ONE OF HUMANITY S MOST DEVASTATING DISEASES
 ACTION AGAINST WORMS JULY 2010 ISSUE 14 Lymphatic filariasis patient, Debaraj Behera, in Dhalapathar, Orissa, India, 2009. IN THIS ISSUE: Lymphatic filariasis: eliminating one of humanity s most devastating
ACTION AGAINST WORMS JULY 2010 ISSUE 14 Lymphatic filariasis patient, Debaraj Behera, in Dhalapathar, Orissa, India, 2009. IN THIS ISSUE: Lymphatic filariasis: eliminating one of humanity s most devastating
MASS TREATMENT FOR LYMPHATIC FILARIASIS MASS TREATMENT TO ELIMINATE FILARIASIS IN PAPUA NEW GUINEA
 MASS TREATMENT FOR LYMPHATIC FILARIASIS MASS TREATMENT TO ELIMINATE FILARIASIS IN PAPUA NEW GUINEA MOSES J. BOCKARIE, PH.D., DANIEL J. TISCH, M.P.H., WILL KASTENS, B.SC., NEAL D.E. ALEXANDER, PH.D., ZACHARY
MASS TREATMENT FOR LYMPHATIC FILARIASIS MASS TREATMENT TO ELIMINATE FILARIASIS IN PAPUA NEW GUINEA MOSES J. BOCKARIE, PH.D., DANIEL J. TISCH, M.P.H., WILL KASTENS, B.SC., NEAL D.E. ALEXANDER, PH.D., ZACHARY
Sensitivity and Specificity of ELISA in Detection of Microfilariae
 ORIGINAL ARTICLE Sensitivity and Specificity of in Detection of Microfilariae Lakshmi Jyothi 1, MVR Reddy 2 1. Associate Professor of Microbiology, Medicity Institute of Medical Sciences, Hyderabad. 2.
ORIGINAL ARTICLE Sensitivity and Specificity of in Detection of Microfilariae Lakshmi Jyothi 1, MVR Reddy 2 1. Associate Professor of Microbiology, Medicity Institute of Medical Sciences, Hyderabad. 2.
Subramanian Swaminathan
 Modelling Lymphatic Filariasis Transmission and Control Subramanian Swaminathan This thesis was realized with support from a WHO/TDR Research training grant, and with financial support from the Stichting
Modelling Lymphatic Filariasis Transmission and Control Subramanian Swaminathan This thesis was realized with support from a WHO/TDR Research training grant, and with financial support from the Stichting
Eliminating Lymphatic Filariasis. Success in science, intervention and beyond..
 Eliminating Lymphatic Filariasis Success in science, intervention and beyond.. Eric A. Ottesen, M.D. 30 January 2007 LF Disease LF Disease Adult parasites (W. bancrofti) in scrotal lymphatic Dreyer & Noroes
Eliminating Lymphatic Filariasis Success in science, intervention and beyond.. Eric A. Ottesen, M.D. 30 January 2007 LF Disease LF Disease Adult parasites (W. bancrofti) in scrotal lymphatic Dreyer & Noroes
Histopathologic Improvement with Lymphedema Management, Léogâne, Haiti
 Histopathologic Improvement with Lymphedema Management, Léogâne, Haiti Susan F. Wilson,* Jeannette Guarner,* Alix L. Valme, Jacky Louis-Charles, Tara L. Jones,* and David G. Addiss* In countries where
Histopathologic Improvement with Lymphedema Management, Léogâne, Haiti Susan F. Wilson,* Jeannette Guarner,* Alix L. Valme, Jacky Louis-Charles, Tara L. Jones,* and David G. Addiss* In countries where
A survey of treatment practices and burden of lymphoedema in Togo
 Transactions of the Royal Society of Tropical Medicine and Hygiene (2007) 101, 391 397 available at www.sciencedirect.com journal homepage: www.elsevierhealth.com/journals/trst A survey of treatment practices
Transactions of the Royal Society of Tropical Medicine and Hygiene (2007) 101, 391 397 available at www.sciencedirect.com journal homepage: www.elsevierhealth.com/journals/trst A survey of treatment practices
Coverage and compliance of mass drug administration for elimination of lymphatic filariasis in Khammam district
 International Journal of Community Medicine and Public Health Alwala RR et al. Int J Community Med Public Health. 2018 Dec;5(12):5121-5125 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original
International Journal of Community Medicine and Public Health Alwala RR et al. Int J Community Med Public Health. 2018 Dec;5(12):5121-5125 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original
IMMUNO-EPIDEMIOLOGY OF BANCROFTIAN FILARIASIS : A 14-YEAR FOLLOW-UP STUDY IN ODISHA, INDIA
 IMMUNO-EPIDEMIOLOGY OF BANCROFTIAN FILARIASIS : A 14-YEAR FOLLOW-UP STUDY IN ODISHA, INDIA NN Mandal, KG Achary, SK Kar and MS Bal Division of Immunology, Regional Medical Research Centre, Indian Council
IMMUNO-EPIDEMIOLOGY OF BANCROFTIAN FILARIASIS : A 14-YEAR FOLLOW-UP STUDY IN ODISHA, INDIA NN Mandal, KG Achary, SK Kar and MS Bal Division of Immunology, Regional Medical Research Centre, Indian Council
Wuchereria Morphology 10 cm 250 : m
 Wucheria bancrofti Brugia malayi Lymphatic filariasis Lymphatic Filariasis 119 million infected Elephantiasis Manifestation of lymphatic filariasis Morphology I Adult: White and thread-like. Two rings
Wucheria bancrofti Brugia malayi Lymphatic filariasis Lymphatic Filariasis 119 million infected Elephantiasis Manifestation of lymphatic filariasis Morphology I Adult: White and thread-like. Two rings
Acta Tropica 120S (2011) S55 S61. Contents lists available at ScienceDirect. Acta Tropica. journa l h o me pa g e:
 Acta Tropica 120S (2011) S55 S61 Contents lists available at ScienceDirect Acta Tropica journa l h o me pa g e: www.elsevier.com/locate/actatropica Efficacy of home-based lymphoedema management in reducing
Acta Tropica 120S (2011) S55 S61 Contents lists available at ScienceDirect Acta Tropica journa l h o me pa g e: www.elsevier.com/locate/actatropica Efficacy of home-based lymphoedema management in reducing
Filaria Journal. Open Access. Abstract
 Filaria Journal BioMed Central Review Advances and challenges in predicting the impact of lymphatic filariasis elimination programmes by mathematical modelling Wilma A Stolk*, Sake J de Vlas and J Dik
Filaria Journal BioMed Central Review Advances and challenges in predicting the impact of lymphatic filariasis elimination programmes by mathematical modelling Wilma A Stolk*, Sake J de Vlas and J Dik
BANCROFTIAN FILARIASIS IN KWALE DISTRICT, KENYA. S.M. NJENGA, M. MUITA, G. KIRIGI, J. MBUGUA, Y. MITSUI, Y. FUJIMAKI and Y.
 May 2000 EAST AFRICAN MEDICAL JOURNAL 245 East African Medical Journal Vol. 77 No. 5 May 2000 BANCROFTIAN FILARIASIS IN KWALE DISTRICT, KENYA S.M. Njenga, MSc, M. Muita, MPH, G. Kirigi, Dip. (Clin. Med.)
May 2000 EAST AFRICAN MEDICAL JOURNAL 245 East African Medical Journal Vol. 77 No. 5 May 2000 BANCROFTIAN FILARIASIS IN KWALE DISTRICT, KENYA S.M. Njenga, MSc, M. Muita, MPH, G. Kirigi, Dip. (Clin. Med.)
Acute adenolymphangitis due to bancroftian filariasis in Rufiji district, south east Tanzania
 ecommons@aku Pathology, East Africa Medical College, East Africa January 2000 Acute adenolymphangitis due to bancroftian filariasis in Rufiji district, south east Tanzania D.B. Gasarasi Muhimbili University
ecommons@aku Pathology, East Africa Medical College, East Africa January 2000 Acute adenolymphangitis due to bancroftian filariasis in Rufiji district, south east Tanzania D.B. Gasarasi Muhimbili University
INTRODUCTION. Tropical Biomedicine 23(2): (2006)
 Tropical Biomedicine 23(2): 156 162 (2006) Knowledge and perceptions about lymphatic filariasis: a study during the programme to eliminate lymphatic filariasis in an urban community of Orissa, India Rath,
Tropical Biomedicine 23(2): 156 162 (2006) Knowledge and perceptions about lymphatic filariasis: a study during the programme to eliminate lymphatic filariasis in an urban community of Orissa, India Rath,
Measuring impact on filarial infection status in a community study: Role of coverage of mass drug administration (MDA)
 Tropical Biomedicine 31(2): 225 229 (2014) Measuring impact on filarial infection status in a community study: Role of coverage of mass drug administration (MDA) Anil Kumar 1* and Pawan Sachan 2 National
Tropical Biomedicine 31(2): 225 229 (2014) Measuring impact on filarial infection status in a community study: Role of coverage of mass drug administration (MDA) Anil Kumar 1* and Pawan Sachan 2 National
Departments of Pathology and *Parasitology, Faculty of Medicine, University of Malaya
 Malaysian J Pathol 2004; 26(2) : 119 123 MICROFILARIA IN HYDROCELE FLUID CYTOLOGY CASE REPORT Microfilaria in hydrocele fluid cytology Patricia Ann CHANDRAN MD, Gita JAYARAM MIAC, FRCPath, *Rohela MAHMUD
Malaysian J Pathol 2004; 26(2) : 119 123 MICROFILARIA IN HYDROCELE FLUID CYTOLOGY CASE REPORT Microfilaria in hydrocele fluid cytology Patricia Ann CHANDRAN MD, Gita JAYARAM MIAC, FRCPath, *Rohela MAHMUD
Purushothaman Jambulingam 1, Swaminathan Subramanian 1*, S. J. de Vlas 2, Chellasamy Vinubala 1 and W. A. Stolk 2
 Jambulingam et al. Parasites & Vectors (2016) 9:501 DOI 10.1186/s13071-016-1768-y RESEARCH Mathematical modelling of lymphatic filariasis elimination programmes in India: required duration of mass drug
Jambulingam et al. Parasites & Vectors (2016) 9:501 DOI 10.1186/s13071-016-1768-y RESEARCH Mathematical modelling of lymphatic filariasis elimination programmes in India: required duration of mass drug
DIAGNOSTIC SLIDE SESSION CASE 10
 DIAGNOSTIC SLIDE SESSION CASE 10 B.K. Kleinschmidt-DeMasters, MD Disclosures: I am not a trainee Caterina made me do this CASE 2016-10: : The patient is a 5-year-old girl with Down syndrome, obstructive
DIAGNOSTIC SLIDE SESSION CASE 10 B.K. Kleinschmidt-DeMasters, MD Disclosures: I am not a trainee Caterina made me do this CASE 2016-10: : The patient is a 5-year-old girl with Down syndrome, obstructive
Influence of Maternal Filariasis on Childhood Infection and Immunity to Wuchereria bancrofti in Kenya
 INFECTION AND IMMUNITY, Sept. 2003, p. 5231 5237 Vol. 71, No. 9 0019-9567/03/$08.00 0 DOI: 10.1128/IAI.71.9.5231 5237.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Influence
INFECTION AND IMMUNITY, Sept. 2003, p. 5231 5237 Vol. 71, No. 9 0019-9567/03/$08.00 0 DOI: 10.1128/IAI.71.9.5231 5237.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Influence
Lymphatic Filariasis: A Method to Identify Subclinical Lower Limb Change in PNG Adolescents
 Lymphatic Filariasis: A Method to Identify Subclinical Lower Limb Change in PNG Adolescents Susan Gordon 1 *, Wayne Melrose 1, Jeffrey Warner 2, Petra Buttner 1, Leigh Ward 3 1 School of Public Health,
Lymphatic Filariasis: A Method to Identify Subclinical Lower Limb Change in PNG Adolescents Susan Gordon 1 *, Wayne Melrose 1, Jeffrey Warner 2, Petra Buttner 1, Leigh Ward 3 1 School of Public Health,
Unusual presentation of Filariasis in a tertiary care hospital in Western Rajasthan: A case report
 ISSN: 2319-7706 Volume 4 Number 1 (2015) pp. 685-689 http://www.ijcmas.com Original Research Article Unusual presentation of Filariasis in a tertiary care hospital in Western Rajasthan: A case report Swati
ISSN: 2319-7706 Volume 4 Number 1 (2015) pp. 685-689 http://www.ijcmas.com Original Research Article Unusual presentation of Filariasis in a tertiary care hospital in Western Rajasthan: A case report Swati
Transactions of the Royal Society of Tropical Medicine and Hygiene
 Transactions of the Royal Society of Tropical Medicine and Hygiene 105 (2011) 109 114 Contents lists available at ScienceDirect Transactions of the Royal Society of Tropical Medicine and Hygiene journal
Transactions of the Royal Society of Tropical Medicine and Hygiene 105 (2011) 109 114 Contents lists available at ScienceDirect Transactions of the Royal Society of Tropical Medicine and Hygiene journal
Helminths in tropical regions
 Helminths in tropical regions Schistosoma spp. Blood flukes Schistosomiasis is one of the most widespread parasitic infections in humans Humans are the principal hosts for: Schistosoma mansoni, Schistosoma
Helminths in tropical regions Schistosoma spp. Blood flukes Schistosomiasis is one of the most widespread parasitic infections in humans Humans are the principal hosts for: Schistosoma mansoni, Schistosoma
HIGH PREVALENCE OF BRUGIA TIMORI INFECTION IN THE HIGHLAND OF ALOR ISLAND, INDONESIA
 Am. J. Trop. Med. Hyg., 66(5), 2002, pp. 560 565 Copyright 2002 by The American Society of Tropical Medicine and Hygiene HIGH PREVALENCE OF BRUGIA TIMORI INFECTION IN THE HIGHLAND OF ALOR ISLAND, INDONESIA
Am. J. Trop. Med. Hyg., 66(5), 2002, pp. 560 565 Copyright 2002 by The American Society of Tropical Medicine and Hygiene HIGH PREVALENCE OF BRUGIA TIMORI INFECTION IN THE HIGHLAND OF ALOR ISLAND, INDONESIA
The Regional Strategic Plan for Elimination of Lymphatic Filariasis
 Lymphatic filariasis is the second leading cause of disability worldwide. The WHO South-East Asia Region accounts for about 65% of the global population at risk. Strategic plans for 2007 2010 for lymphatic
Lymphatic filariasis is the second leading cause of disability worldwide. The WHO South-East Asia Region accounts for about 65% of the global population at risk. Strategic plans for 2007 2010 for lymphatic
Impact of a Community-Based Lymphedema Management Program on Episodes of Adenolymphangitis (ADLA) and Lymphedema Progression - Odisha State, India
 Impact of a Community-Based Lymphedema Management Program on Episodes of Adenolymphangitis (ADLA) and Lymphedema Progression - Odisha State, India Katherine E. Mues, Emory University Michael Deming, Emory
Impact of a Community-Based Lymphedema Management Program on Episodes of Adenolymphangitis (ADLA) and Lymphedema Progression - Odisha State, India Katherine E. Mues, Emory University Michael Deming, Emory
Economic Costs and Benefits of a Community- Based Lymphedema Management Program for Lymphatic Filariasis in Odisha State, India
 Economics Faculty Publications Economics 8-29-2016 Economic Costs and Benefits of a Community- Based Lymphedema Management Program for Lymphatic Filariasis in Odisha State, India Eileen Stillwaggon Gettysburg
Economics Faculty Publications Economics 8-29-2016 Economic Costs and Benefits of a Community- Based Lymphedema Management Program for Lymphatic Filariasis in Odisha State, India Eileen Stillwaggon Gettysburg
LYMPHATIC FILARIASIS STRENGTHENING THE ASSESSMENT OF LYMPHATIC FILARIASIS TRANSMISSION AND DOCUMENTING THE ACHIEVEMENT OF ELIMINATION
 STRENGTHENING THE ASSESSMENT OF LYMPHATIC FILARIASIS TRANSMISSION AND DOCUMENTING THE ACHIEVEMENT OF ELIMINATION MEETING OF THE NEGLECTED TROPICAL DISEASES STRATEGIC AND TECHNICAL ADVISORY GROUP S MONITORING
STRENGTHENING THE ASSESSMENT OF LYMPHATIC FILARIASIS TRANSMISSION AND DOCUMENTING THE ACHIEVEMENT OF ELIMINATION MEETING OF THE NEGLECTED TROPICAL DISEASES STRATEGIC AND TECHNICAL ADVISORY GROUP S MONITORING
USER-FRIENDLY DATABASE for INTEGRATED CONTROL of BANCROFTIAN FILARIASIS in EAST and WEST GODAVARI DISTRICTS of ANDHRA PRADESH, INDIA
 379 USER-FRIENDLY DATABASE for INTEGRATED CONTROL of BANCROFTIAN FILARIASIS in EAST and WEST GODAVARI DISTRICTS of ANDHRA PRADESH, INDIA U. Suryanarayana Murty 1, D.V.R. Satya Kumar 1, K. Siram 1, K. Madhusudhan
379 USER-FRIENDLY DATABASE for INTEGRATED CONTROL of BANCROFTIAN FILARIASIS in EAST and WEST GODAVARI DISTRICTS of ANDHRA PRADESH, INDIA U. Suryanarayana Murty 1, D.V.R. Satya Kumar 1, K. Siram 1, K. Madhusudhan
EDO UNIVERSITY IYAMHO
 EDO UNIVERSITY IYAMHO FACULTY OF SCIENCE SEMINAR SERIES INTESTINAL HELMINTHIASIS: SOIL TRANSMITTED INFECTIONS. PRESENTED BY Mrs. Habibat Joy, Ozemoka 3rd August, 2018 INTRODUCTION Intestinal helminthiasis
EDO UNIVERSITY IYAMHO FACULTY OF SCIENCE SEMINAR SERIES INTESTINAL HELMINTHIASIS: SOIL TRANSMITTED INFECTIONS. PRESENTED BY Mrs. Habibat Joy, Ozemoka 3rd August, 2018 INTRODUCTION Intestinal helminthiasis
Microfilaria persistent foci during post MDA and the risk assessment of resurgence in India
 Mehta et al. Tropical Medicine and Health (2018) 46:25 https://doi.org/10.1186/s41182-018-0107-8 Tropical Medicine and Health RESEARCH Microfilaria persistent foci during post MDA and the risk assessment
Mehta et al. Tropical Medicine and Health (2018) 46:25 https://doi.org/10.1186/s41182-018-0107-8 Tropical Medicine and Health RESEARCH Microfilaria persistent foci during post MDA and the risk assessment
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO MD (MEDICAL PARASITOLOGY) EXAMINATION JANUARY, 2001 PAPER 1
 JANUARY, 2001 Date: 15 th January 2001 Time: 2.00 p.m. -500 p.m. PAPER 1 Answer all five (5) questions Answer each question in a separate book 1. Discuss the underlying principles relating to the use of
JANUARY, 2001 Date: 15 th January 2001 Time: 2.00 p.m. -500 p.m. PAPER 1 Answer all five (5) questions Answer each question in a separate book 1. Discuss the underlying principles relating to the use of
District NTD Training module
 Revision Date: 13 May 2015 District NTD Training module Learner s Guide Module 6: Morbidity Management and Disability Prevention (MMDP) Part I: Introduction Session purpose: Session 3: Hydrocele Surgery
Revision Date: 13 May 2015 District NTD Training module Learner s Guide Module 6: Morbidity Management and Disability Prevention (MMDP) Part I: Introduction Session purpose: Session 3: Hydrocele Surgery
Policy and technical topics: Selected neglected tropical diseases targeted for elimination: kala-azar, leprosy, yaws, filariasis and schistosomiasis
 REGIONAL COMMITTEE Provisional Agenda item 8.3 Sixty-eighth Session SEA/RC68/12 Dili, Timor-Leste 7 11 September 2015 21 July 2015 Policy and technical topics: Selected neglected tropical diseases targeted
REGIONAL COMMITTEE Provisional Agenda item 8.3 Sixty-eighth Session SEA/RC68/12 Dili, Timor-Leste 7 11 September 2015 21 July 2015 Policy and technical topics: Selected neglected tropical diseases targeted
Short report: Semi-quantitative scoring of an immunochromatographic test for circulating filarial antigen
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2013 Short report: Semi-quantitative scoring of an immunochromatographic test for circulating filarial antigen Cedric
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2013 Short report: Semi-quantitative scoring of an immunochromatographic test for circulating filarial antigen Cedric
I. Wuchereria bancrofti
 Parasites that affect the Musculoskeletal system (continued) Filarial Worms - Nematodes. - Tissue parasites. - Require an intermediate host, which is usually an insect. - Do not lay eggs like other worms,
Parasites that affect the Musculoskeletal system (continued) Filarial Worms - Nematodes. - Tissue parasites. - Require an intermediate host, which is usually an insect. - Do not lay eggs like other worms,
Summary of the Twelfth Meeting of the ITFDE (II) May 6, 2008
 Summary of the Twelfth Meeting of the ITFDE (II) May 6, 2008 The Twelfth Meeting of the International Task Force for Disease Eradication (ITFDE) was convened at The Carter Center from 8:30am to 4:00pm
Summary of the Twelfth Meeting of the ITFDE (II) May 6, 2008 The Twelfth Meeting of the International Task Force for Disease Eradication (ITFDE) was convened at The Carter Center from 8:30am to 4:00pm
Monitoring and epidemiological assessment of the programme to eliminate lymphatic filariasis at implementation unit level WHO/CDS/CPE/CEE/2005.
 AT LIMINATE MPLEMENTATION LEVEL UNIT OF THE PROGRAMME LYMPHATIC FILARIASIS OF THE TO ASSESSMENT TO ELIMINATE AT IMPLEMENTATION ROGRAMME EPIDEMIOLOGICAL AND MONITORING MONITORING AND EPIDEMIOLOGICAL ASSESSMENT
AT LIMINATE MPLEMENTATION LEVEL UNIT OF THE PROGRAMME LYMPHATIC FILARIASIS OF THE TO ASSESSMENT TO ELIMINATE AT IMPLEMENTATION ROGRAMME EPIDEMIOLOGICAL AND MONITORING MONITORING AND EPIDEMIOLOGICAL ASSESSMENT
District NTD Training module
 Revision Date: 13 May 2015 Part I: Introduction Session Purpose: District NTD Training module Learner s Guide Module 6: Morbidity Management and Disability Prevention (MMDP) Session 2: Lymphoedema Management
Revision Date: 13 May 2015 Part I: Introduction Session Purpose: District NTD Training module Learner s Guide Module 6: Morbidity Management and Disability Prevention (MMDP) Session 2: Lymphoedema Management
Yellow fever. Key facts
 From: http://www.who.int/en/news-room/fact-sheets/detail/yellow-fever WHO/E. Soteras Jalil Yellow fever 14 March 2018 Key facts Yellow fever is an acute viral haemorrhagic disease transmitted by infected
From: http://www.who.int/en/news-room/fact-sheets/detail/yellow-fever WHO/E. Soteras Jalil Yellow fever 14 March 2018 Key facts Yellow fever is an acute viral haemorrhagic disease transmitted by infected
District NTD Training module 9 Learners Guide
 District NTD Training module 9 Learners Guide Session 3: Diagnostic and laboratory tools for filarial worms, Soil- Transmitted Helminths and Schistosomiasis Key message addressed to communities: Community
District NTD Training module 9 Learners Guide Session 3: Diagnostic and laboratory tools for filarial worms, Soil- Transmitted Helminths and Schistosomiasis Key message addressed to communities: Community
Real-time PCR detection of the HhaI tandem DNA repeat in pre- and post-patent Brugia malayi infections: a study in Indonesian transmigrants
 Albers et al. Parasites & Vectors 2014, 7:146 RESEARCH Open Access Real-time PCR detection of the HhaI tandem DNA repeat in pre- and post-patent Brugia malayi infections: a study in Indonesian transmigrants
Albers et al. Parasites & Vectors 2014, 7:146 RESEARCH Open Access Real-time PCR detection of the HhaI tandem DNA repeat in pre- and post-patent Brugia malayi infections: a study in Indonesian transmigrants
Department of Parasitology, Faculty of Public Health, Mahidol University, Bangkok; 2
 RELATIONSHIP BETWEEN MALE HYDROCELE AND INFECTION PREVALENCES IN CLUSTERED COMMUNITIES WITH UNCERTAIN TRANSMISSION OF WUCHERERIA BANCROFTI ON THE THAILAND-MYANMAR BORDER Adisak Bhumiratana 1, Boontuan
RELATIONSHIP BETWEEN MALE HYDROCELE AND INFECTION PREVALENCES IN CLUSTERED COMMUNITIES WITH UNCERTAIN TRANSMISSION OF WUCHERERIA BANCROFTI ON THE THAILAND-MYANMAR BORDER Adisak Bhumiratana 1, Boontuan
Mass Drug Administration against Filariasis - A study on coverage and compliance, in a coastal district of Odisha
 Research Article Mass Drug Administration against Filariasis - A study on coverage and compliance, in a coastal district of Odisha Introduction Alpana Mishra *, Krishna Kar **, Durgamadhab Satapathy ***
Research Article Mass Drug Administration against Filariasis - A study on coverage and compliance, in a coastal district of Odisha Introduction Alpana Mishra *, Krishna Kar **, Durgamadhab Satapathy ***
Lymphatic Filariasis
 REFERENCES CONTENT ALERTS Characterization of Antibody Responses to Wolbachia Surface Protein in Humans with Lymphatic Filariasis George A. Punkosdy, David G. Addiss and Patrick J. Lammie Infect. Immun.
REFERENCES CONTENT ALERTS Characterization of Antibody Responses to Wolbachia Surface Protein in Humans with Lymphatic Filariasis George A. Punkosdy, David G. Addiss and Patrick J. Lammie Infect. Immun.
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Health Related Quality of Life (HRQoL) Among Patients with Lymphatic Filariasis K.T.Harichandrakumar
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Health Related Quality of Life (HRQoL) Among Patients with Lymphatic Filariasis K.T.Harichandrakumar
Impact of Mass Drug Administration on Elimination of Lymphatic Filariasis in Surat city, India
 J. Commun. Dis. 44(4) 2012 : 251-259 Impact of Mass Drug Administration on Elimination of Lymphatic Filariasis in Surat city, India Vaishnav KG*, Desai HS*, Srivastava PK**, Joshi PT***, Kurian G***, Thakor
J. Commun. Dis. 44(4) 2012 : 251-259 Impact of Mass Drug Administration on Elimination of Lymphatic Filariasis in Surat city, India Vaishnav KG*, Desai HS*, Srivastava PK**, Joshi PT***, Kurian G***, Thakor
INTRODUCTION. Lymphatic filariasis (LF), a deforming and debilitating disease transmitted by
 INTRODUCTION Lymphatic filariasis (LF), a deforming and debilitating disease transmitted by '. mosquitoes, causes elephantiasis and male genital damage and is a major social and economic scourge in the
INTRODUCTION Lymphatic filariasis (LF), a deforming and debilitating disease transmitted by '. mosquitoes, causes elephantiasis and male genital damage and is a major social and economic scourge in the
The Neglected Tropical Diseases of Guinea, Liberia, Sierra Leone
 The Neglected Tropical Diseases of Guinea, Liberia, Sierra Leone Peter Hotez MD PhD @PeterHotez The Millennium Development Goals 1. Eradicate extreme poverty and hunger. 2. Achieve universal primary education.
The Neglected Tropical Diseases of Guinea, Liberia, Sierra Leone Peter Hotez MD PhD @PeterHotez The Millennium Development Goals 1. Eradicate extreme poverty and hunger. 2. Achieve universal primary education.
Lecture 5: Dr. Jabar Etaby
 Lecture 5: Dr. Jabar Etaby 1 2 Onchocerca volvulus (Blinding filariasis; river blindness) Microfilaria of Onchocerca volvulus, from skin snip from a patient seen in Guatemala. Wet preparation 3 Some important
Lecture 5: Dr. Jabar Etaby 1 2 Onchocerca volvulus (Blinding filariasis; river blindness) Microfilaria of Onchocerca volvulus, from skin snip from a patient seen in Guatemala. Wet preparation 3 Some important
Insecticidal Bed Nets and Filariasis Transmission in Papua New Guinea
 original article Insecticidal and Filariasis Transmission in Papua New Guinea Lisa J. Reimer, Ph.D., Edward K. Thomsen, M.Sc., Daniel J. Tisch, Ph.D., Cara N. Henry-Halldin, Ph.D., Peter A. Zimmerman,
original article Insecticidal and Filariasis Transmission in Papua New Guinea Lisa J. Reimer, Ph.D., Edward K. Thomsen, M.Sc., Daniel J. Tisch, Ph.D., Cara N. Henry-Halldin, Ph.D., Peter A. Zimmerman,
1.1.2 Discovery of Microfilariae (1863 and 1866)
 CHAPTER-2 1 REVIEW OF LITERATURE Lymphatic filariasis is vector borne parasitic disease caused by three lymphatic dwelling nematode worms living in the lymphatic system, namely Wuchereria bancrofti, Brugia
CHAPTER-2 1 REVIEW OF LITERATURE Lymphatic filariasis is vector borne parasitic disease caused by three lymphatic dwelling nematode worms living in the lymphatic system, namely Wuchereria bancrofti, Brugia
Clinical manifestations of Bancroftian filariasis in relation to microfilaraemia and diethylcarbamazine therapy
 PANI ellll. : BANCROFflAN FILARIASIS IN RELATION TO MICROfiLARAEMIA AND DEC THERAPY 9 1 Dalla DV. Bhagwat AG. Idiopathic portal hypertension-a review. Bull PGIMER 1981;15:173--9. Foster JH. Conkle OM.
PANI ellll. : BANCROFflAN FILARIASIS IN RELATION TO MICROfiLARAEMIA AND DEC THERAPY 9 1 Dalla DV. Bhagwat AG. Idiopathic portal hypertension-a review. Bull PGIMER 1981;15:173--9. Foster JH. Conkle OM.
SUMMARY OF THE THIRD MEETING OF THE ITFDE(II) October 18, 2002
 SUMMARY OF THE THIRD MEETING OF THE ITFDE(II) October 18, 2002 This meeting of the International Task Force for Disease Eradication (ITFDE) was convened at The Carter Center from 9:00am to 4:00pm on October
SUMMARY OF THE THIRD MEETING OF THE ITFDE(II) October 18, 2002 This meeting of the International Task Force for Disease Eradication (ITFDE) was convened at The Carter Center from 9:00am to 4:00pm on October
Elimination of lymphatic filariasis as a public health problem from the Cook Islands
 Ave et al. Tropical Medicine and Health (2018) 46:12 https://doi.org/10.1186/s41182-018-0094-9 Tropical Medicine and Health RESEARCH Open Access Elimination of lymphatic filariasis as a public health problem
Ave et al. Tropical Medicine and Health (2018) 46:12 https://doi.org/10.1186/s41182-018-0094-9 Tropical Medicine and Health RESEARCH Open Access Elimination of lymphatic filariasis as a public health problem
Abraham Rocha 1 / +, Cynthia Braga 1, Marcela Belém 1, Arturo Carrera 1, Ana Aguiar-Santos 1, Paula Oliveira 1, Maria José Texeira 1, André Furtado 2
 Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 104(4): 621-625, July 2009 621 Comparison of tests for the detection of circulating filarial antigen (Og4C3-ELISA and AD12-ICT) and ultrasound in diagnosis of
Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 104(4): 621-625, July 2009 621 Comparison of tests for the detection of circulating filarial antigen (Og4C3-ELISA and AD12-ICT) and ultrasound in diagnosis of
The impact of 34 years of massive DEC chemotherapy on Wuchereria bancrofti infection and transmission: the Maupiti cohort
 Tropical Medicine and International Health volume 6 no 3 pp 190±195 march 2001 The impact of 34 years of massive DEC chemotherapy on Wuchereria bancrofti infection and transmission: the Maupiti cohort
Tropical Medicine and International Health volume 6 no 3 pp 190±195 march 2001 The impact of 34 years of massive DEC chemotherapy on Wuchereria bancrofti infection and transmission: the Maupiti cohort
Model development, quantification and application
 4 Model development, quantification and application 4.1 The LYMFASIM simulation program for modelling lymphatic filariasis and its control A.P. Plaisier, S. Subramanian, P.K. Das, W. Souza, T. Lapa, A.F.
4 Model development, quantification and application 4.1 The LYMFASIM simulation program for modelling lymphatic filariasis and its control A.P. Plaisier, S. Subramanian, P.K. Das, W. Souza, T. Lapa, A.F.
ETHIOPIA SCHISTOSOMIASIS AND SOIL-TRANSMITTED HELMINTHES CONTROL PROGRAMME: PROGRESS AND PROSPECTS ABSTRACT INTRODUCTION
 Nebiyu Negussu, Birhan Mengistu, Biruck Kebede, Kebede Deribe, Ephrem Ejigu, Gemechu Tadesse, Kalkidan Mekete, Mesfin Sileshi, Ethiop Med J, 2017, Vol. 55, Supp. 1 ETHIOPIA SCHISTOSOMIASIS AND SOIL-TRANSMITTED
Nebiyu Negussu, Birhan Mengistu, Biruck Kebede, Kebede Deribe, Ephrem Ejigu, Gemechu Tadesse, Kalkidan Mekete, Mesfin Sileshi, Ethiop Med J, 2017, Vol. 55, Supp. 1 ETHIOPIA SCHISTOSOMIASIS AND SOIL-TRANSMITTED
General Introduction 1. FILARIA AND HUMAN HEALTH
 1. FILARIA AND HUMAN HEALTH Human lymphatic filariasis (LF) is an infectious disease caused by lymphdwelling nematode parasites and transmitted by mosquitoes. It is one of the oldest and most debilitating
1. FILARIA AND HUMAN HEALTH Human lymphatic filariasis (LF) is an infectious disease caused by lymphdwelling nematode parasites and transmitted by mosquitoes. It is one of the oldest and most debilitating
OBSERVATIONS ON THE SIX YEAR RESULTS OF THE PILOT PROJECT FOR THE CONTROL OF MALAYAN FILARIASIS IN THAILAND!"
 OBSERVATIONS ON THE SIX YEAR RESULTS OF THE PILOT PROJECT FOR THE CONTROL OF MALAYAN FILARIASIS IN THAILAND!" CHAMLONG HARINASUTA, PRICHA CHAROENLARP, PENSRI GUPTAVANIJ, SUPAT SUCHARIT, THONGCHAI DEESIN,
OBSERVATIONS ON THE SIX YEAR RESULTS OF THE PILOT PROJECT FOR THE CONTROL OF MALAYAN FILARIASIS IN THAILAND!" CHAMLONG HARINASUTA, PRICHA CHAROENLARP, PENSRI GUPTAVANIJ, SUPAT SUCHARIT, THONGCHAI DEESIN,
The impact of density-dependent processes on the eradicability of parasitic diseases
 The impact of density-dependent processes on the eradicability of parasitic diseases Hans Peter Duerr Martin Eichner Klaus Dietz Department of Medical Biometry University of Tübingen Oberwolfach 2004 1/12
The impact of density-dependent processes on the eradicability of parasitic diseases Hans Peter Duerr Martin Eichner Klaus Dietz Department of Medical Biometry University of Tübingen Oberwolfach 2004 1/12
Part I. Health-related Millennium Development Goals
 11 1111111111111111111111111 111111111111111111111111111111 1111111111111111111111111 1111111111111111111111111111111 111111111111111111111111111111 1111111111111111111111111111111 213 Part I Health-related
11 1111111111111111111111111 111111111111111111111111111111 1111111111111111111111111 1111111111111111111111111111111 111111111111111111111111111111 1111111111111111111111111111111 213 Part I Health-related
Invest in the future, defeat malaria
 Invest in the future, defeat malaria Malaria is caused by parasites from the genus Plasmodium, which are spread to people by infected mosquitoes. There are five species of Plasmodium that can infect humans.
Invest in the future, defeat malaria Malaria is caused by parasites from the genus Plasmodium, which are spread to people by infected mosquitoes. There are five species of Plasmodium that can infect humans.
Killing filarial nematode parasites: role of treatment options and host immune response
 Kwarteng et al. Infectious Diseases of Poverty (2016) 5:86 DOI 10.1186/s40249-016-0183-0 SCOPING REVIEW Killing filarial nematode parasites: role of treatment options and host immune response Alexander
Kwarteng et al. Infectious Diseases of Poverty (2016) 5:86 DOI 10.1186/s40249-016-0183-0 SCOPING REVIEW Killing filarial nematode parasites: role of treatment options and host immune response Alexander
Regulation of the immune response in lymphatic filariasis: perspectives on acute and chronic infection with Wuchereria bancrofti in South India
 Parasite Immunology, 2001: 23: 389±399 Regulation of the immune response in lymphatic filariasis: perspectives on acute and chronic infection with Wuchereria bancrofti in South India THOMAS B.NUTMAN 1
Parasite Immunology, 2001: 23: 389±399 Regulation of the immune response in lymphatic filariasis: perspectives on acute and chronic infection with Wuchereria bancrofti in South India THOMAS B.NUTMAN 1
This file is part of the following reference:
 This file is part of the following reference: Reeve, David Mark (2010) Comparative accuracy and 'field friendly' effectiveness of diagnostic tools for lymphatic filariasis and neurocyticercosis in Papua
This file is part of the following reference: Reeve, David Mark (2010) Comparative accuracy and 'field friendly' effectiveness of diagnostic tools for lymphatic filariasis and neurocyticercosis in Papua
Western Pacific Region Neglected Tropical Diseases News
 Western Pacific Region Neglected Tropical Diseases News 2015 Issue 1 Welcome to Western Pacific NTD News! This newsletter, to be published quarterly by the WHO Regional Office for the Western Pacific,
Western Pacific Region Neglected Tropical Diseases News 2015 Issue 1 Welcome to Western Pacific NTD News! This newsletter, to be published quarterly by the WHO Regional Office for the Western Pacific,
CHAPTER 1 INTRODUCTION
 1 CHAPTER 1 INTRODUCTION 1.1 BACKGROUND Lymphatic filariasis is a mosquito- borne parasitic disease caused by thread like, filaroid nematode worms that include Wucheraria bancrofti, Brugia malayi, and
1 CHAPTER 1 INTRODUCTION 1.1 BACKGROUND Lymphatic filariasis is a mosquito- borne parasitic disease caused by thread like, filaroid nematode worms that include Wucheraria bancrofti, Brugia malayi, and
A critical appraisal of molecular xenomonitoring as a tool for assessing progress toward elimination of lymphatic filariasis
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2007 A critical appraisal of molecular xenomonitoring as a tool for assessing progress toward elimination of lymphatic
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2007 A critical appraisal of molecular xenomonitoring as a tool for assessing progress toward elimination of lymphatic
A simple and quick method for enhanced detection of specific IgE in serum from lymphatic filariasis patients
 Acta Tropica 80 (2001) 51 57 www.parasitology-online.com A simple and quick method for enhanced detection of specific IgE in serum from lymphatic filariasis patients Walter G. Jaoko a, Mette Lund b, Edwin
Acta Tropica 80 (2001) 51 57 www.parasitology-online.com A simple and quick method for enhanced detection of specific IgE in serum from lymphatic filariasis patients Walter G. Jaoko a, Mette Lund b, Edwin
Eosinophilic lung diseases
 Eosinophilic lung diseases Chai Gin Tsen Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital The eyes do not see what the mind does not know Not very common A high index of suspicion
Eosinophilic lung diseases Chai Gin Tsen Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital The eyes do not see what the mind does not know Not very common A high index of suspicion
Lymphatic filariasis: new insights and prospects for control Thomas B. Nutman
 Lymphatic filariasis: new insights and prospects for control Thomas B Nutman Although lymphatic filariasis remains among the major causes of disability among the tropical infectious diseases, dramatic
Lymphatic filariasis: new insights and prospects for control Thomas B Nutman Although lymphatic filariasis remains among the major causes of disability among the tropical infectious diseases, dramatic
A practical strategy for responding to a case of lymphatic filariasis post-elimination in Pacific Islands
 Harrington et al. Parasites & Vectors 2013, 6:218 RESEARCH Open Access A practical strategy for responding to a case of lymphatic filariasis post-elimination in Pacific Islands Humpress Harrington 1, James
Harrington et al. Parasites & Vectors 2013, 6:218 RESEARCH Open Access A practical strategy for responding to a case of lymphatic filariasis post-elimination in Pacific Islands Humpress Harrington 1, James
Against intervention No recommendation Strong Conditional Conditional Strong. For intervention. High Moderate Low Very low
 Draft recommendation: Consider using MDA as an additional tool for the elimination of malaria in low prevalence island or nonisland settings where the risk of imported malaria is low Balance of desirable
Draft recommendation: Consider using MDA as an additional tool for the elimination of malaria in low prevalence island or nonisland settings where the risk of imported malaria is low Balance of desirable
Rheumatic heart disease
 EXECUTIVE BOARD EB141/4 141st session 1 May 2017 Provisional agenda item 6.2 Rheumatic heart disease Report by the Secretariat 1. Rheumatic heart disease is a preventable yet serious public health problem
EXECUTIVE BOARD EB141/4 141st session 1 May 2017 Provisional agenda item 6.2 Rheumatic heart disease Report by the Secretariat 1. Rheumatic heart disease is a preventable yet serious public health problem
A review of lymphoscintigraphy - what constitutes a positive result and how this affects the patients management.
 A review of lymphoscintigraphy - what constitutes a positive result and how this affects the patients management. Poster No.: C-1030 Congress: ECR 2014 Type: Educational Exhibit Authors: N. J. Ley, E.
A review of lymphoscintigraphy - what constitutes a positive result and how this affects the patients management. Poster No.: C-1030 Congress: ECR 2014 Type: Educational Exhibit Authors: N. J. Ley, E.
Changes in Cytokine, Filarial Antigen, and DNA Levels Associated With Adverse Events Following Treatment of Lymphatic Filariasis
 The Journal of Infectious Diseases MAJOR ARTICLE Changes in Cytokine, Filarial Antigen, and DNA Levels Associated With Adverse Events Following Treatment of Lymphatic Filariasis Britt J. Andersen, 1 Jessica
The Journal of Infectious Diseases MAJOR ARTICLE Changes in Cytokine, Filarial Antigen, and DNA Levels Associated With Adverse Events Following Treatment of Lymphatic Filariasis Britt J. Andersen, 1 Jessica
Eliminating Lymphatic Filariasis
 Eliminating Lymphatic Filariasis A View from the Field THOMAS STREIT a AND JACK GUY LAFONTANT a,b,c a Center for Global Health and Infectious Diseases, Department of Biological Sciences, University of
Eliminating Lymphatic Filariasis A View from the Field THOMAS STREIT a AND JACK GUY LAFONTANT a,b,c a Center for Global Health and Infectious Diseases, Department of Biological Sciences, University of
The Lymphatic System. Oedema (Edema) Lymphoedema (Lymphedema)
 The Lymphatic System The lymphatic system is similar to the blood system and has just as many vessels - but they contain lymph, which is clear and so cannot be seen (unless a suitable dye is injected).
The Lymphatic System The lymphatic system is similar to the blood system and has just as many vessels - but they contain lymph, which is clear and so cannot be seen (unless a suitable dye is injected).
This summary outlines the burden of targeted diseases and program implementation outcomes in Guinea-Bissau. AFRICAN REGION LIC
 -Bissau The control of neglected tropical diseases represents a major challenge to those providing healthcare services in the endemic countries. The purpose of this country profile is to provide public
-Bissau The control of neglected tropical diseases represents a major challenge to those providing healthcare services in the endemic countries. The purpose of this country profile is to provide public
Clinicopathological Spectrum of Chronic Filarial Epididymo- Orchitis: Experience from a Tertiary Care Institute
 Original Article DOI: 10.21276/APALM.1958 Clinicopathological Spectrum of Chronic Filarial Epididymo- Orchitis: Experience from a Tertiary Care Institute Preethi Anni Mercy Paul 1 *, Kanwardeep Singh Kwatra
Original Article DOI: 10.21276/APALM.1958 Clinicopathological Spectrum of Chronic Filarial Epididymo- Orchitis: Experience from a Tertiary Care Institute Preethi Anni Mercy Paul 1 *, Kanwardeep Singh Kwatra
MESA research grants 2014
 MESA research grants 2014 MESA operational research grant Principal investigator Mopping up and getting to zero: mapping residual malaria transmission for targeted response in urban Lusaka, Zambia. Daniel
MESA research grants 2014 MESA operational research grant Principal investigator Mopping up and getting to zero: mapping residual malaria transmission for targeted response in urban Lusaka, Zambia. Daniel
Filarial hydrocele: a neglected condition of a neglected tropical disease
 Review Filarial hydrocele: a neglected condition of a neglected tropical disease Kenneth Bentum Otabil 1,2, Seth Boateng Tenkorang 2 ¹ Department of community Medicine and Health, Anglican University College
Review Filarial hydrocele: a neglected condition of a neglected tropical disease Kenneth Bentum Otabil 1,2, Seth Boateng Tenkorang 2 ¹ Department of community Medicine and Health, Anglican University College
