Rebound eosinophilia after treatment of hypereosinophilic syndrome and eosinophilic gastroenteritis with monoclonal anti IL-5 antibody SCH55700
|
|
|
- Mary Knight
- 6 years ago
- Views:
Transcription
1 Rebound eosinophilia after treatment of hypereosinophilic syndrome and eosinophilic gastroenteritis with monoclonal anti IL-5 antibody SCH55700 Yae-Jean Kim, MD, a Calman Prussin, MD, b Brian Martin, BS, a Melissa A. Law, RN, a Thomas P. Haverty, MD, c Thomas B. Nutman, MD, a and Amy D. Klion, MD a Bethesda, Md, and Kenilworth, NJ Background: Hypereosinophilic syndrome and eosinophilic gastroenteritis with peripheral eosinophilia are characterized by sustained eosinophilia and eosinophil-mediated tissue damage. Although treatment with the humanized monoclonal anti IL-5 antibody SCH55700 resulted in improvement of eosinophilia and clinical symptoms in 6 of 8 of patients with hypereosinophilic syndrome or eosinophilic gastroenteritis with peripheral eosinophilia for as long as 12 weeks, eosinophil counts subsequently rose above baseline levels, accompanied by an exacerbation of symptoms. Objective: To identify the mechanism underlying this rebound eosinophilia. Methods: Purified eosinophils from patients or normal donors were cultured with IL-5, patient serum, and/or anticytokine antibodies, and eosinophil survival was assessed by flow cytometry. Serum and intracellular cytokine levels were measured by multiplex sandwich ELISA and flow cytometry, respectively. Results: Before treatment with SCH55700, in vitro eosinophil survival in media and in response to recombinant IL-5 was similar in patients and normal donors. At 1 month posttreatment, the eosinophil survival curves were unchanged in 4 of 5 patients in media and in all 5 patients in response to recombinant IL-5. Normal eosinophil survival was prolonged in cultures containing posttreatment but not pretreatment sera (pretreatment vs posttreatment, 10.74% vs 73.02% live cells; P =.01). This posttreatment serum effect on eosinophil survival was reversed by the addition of the monoclonal anti IL-5 antibody TRFK5. Although increased levels of serum IL-5 were observed at 1 month compared with 2 to 3 days posttreatment in 5 of 6 patients (P =.04), intracellular cytokine analysis did not reveal increased production of IL-5 by peripheral blood mononuclear cells. Conclusions: The rebound eosinophilia after SCH55700 treatment is a result of a serum factor that enhances eosinophil From a the Laboratory of Parasitic Diseases and b the Laboratory of Allergic Diseases, National Institute of Allergy and Infectious Diseases, National Institutes of Health, Bethesda; Md, and c Schering-Plough Research Institute, Kenilworth, NJ. Received for publication March 2, 2004; revised August 8, 2004; accepted for publication August 10, Available online October 7, Reprint requests: Amy D. Klion, MD, Laboratory of Parasitic Diseases, National Institute of Allergy and Infectious Disease, National Institutes of Health, Bldg 4, Rm B1-05, 9000 Rockville Pike, Bethesda, MD aklion@niaid.nih.gov /$30.00 Ó 2004 American Academy of Allergy, Asthma and Immunology doi: /j.jaci survival. Reversal of this effect by the addition of antibody to IL-5 suggests that this factor may be IL-5 itself. (J Allergy Clin Immunol 2004;114: ) Key words: Anti IL-5, hypereosinophilic syndrome, eosinophilic gastroenteritis, monoclonal antibody, eosinophil Hypereosinophilic syndrome (HES) is a rare hematologic disorder characterized by sustained overproduction of eosinophils in the bone marrow, eosinophilia (>1500 eosinophils/mm 3 for at least 6 months) and tissue infiltration by eosinophils, resulting in end-organ damage. 1 Current therapies for HES, including corticosteroids, IFNa, hydroxyurea, 1-3 and imatinib mesylate, 4-8 are aimed at the reduction of end-organ damage by controlling peripheral blood eosinophil counts. Eosinophilic gastroenteritis (EG) is a disorder in which eosinophilic infiltration of the gastrointestinal wall results in a wide variety of gastrointestinal symptoms. 9,10 EG can lead to significant loss of function because of chronic abdominal pain, malabsorption, and weight loss. Marked peripheral blood eosinophilia is seen in association with EG in some patients and leads to overlap in the diagnosis with HES. EG is generally responsive to corticosteroids, although high doses may be necessary. A subset of patients with HES or EG become refractory to or develop significant side effects from conventional therapy, and it was for this group that novel therapeutic approaches were sought. SCH55700 is a humanized antihuman IL-5 mab that incorporates the antigen recognition sites from 39D10, a rat IgG2a antibody against human IL-5, and a consensus human IgG4 (k) constant region. 11 SCH55700 has been shown to bind human IL-5 with high affinity (Kd = 20 pmol/l) in vitro and to suppress tissue eosinophilia (lung and skin) in a variety of species in vivo. 11 In a pilot study of patients with persistent asthma, reduction of peripheral blood eosinophilia after SCH55700 administration was apparent within 48 hours and persisted for as long as 30 days in a dose-dependent manner (0.3 mg/kg vs 1 mg/kg) without any significant adverse effects. Although the FEV 1 of the patients with asthma improved at 24 hours after drug infusion, there were no significant changes in clinical indices of disease activity. 12 As part of a clinical study to assess the safety and efficacy of a single 1-mg/kg dose of SCH55700 in reducing peripheral blood eosinophilia in patients with 1449
2 1450 Kim et al J ALLERGY CLIN IMMUNOL DECEMBER 2004 Abbreviations used EG: Eosinophilic gastroenteritis EGE: Eosinophilic gastroenteritis with peripheral eosinophilia HES: Hypereosinophilic syndrome HES or EG with peripheral eosinophilia (EGE), eosinophil counts and symptoms were monitored in 8 patients for as long as 3 months after drug administration. Although peripheral eosinophilia resolved and clinical symptoms improved in 6 of the 8 patients within 48 hours of drug administration, eosinophil counts subsequently rose above baseline levels in all 6 SCH55700 responders. 13,14 The aim of the current study was to elucidate the mechanism of the rebound eosinophilia observed after anti IL-5 therapy. Our data suggest that anti IL-5 therapy induced significantly increased IL-5 levels by 1 month after therapy and that this increase in serum IL-5 was responsible for the rebound eosinophilia observed in patients with either HES or EGE. METHODS Participants Eight patients with HES (n = 4) or EGE (n = 4) refractory to or intolerant of conventional therapy were enrolled in a single-dose study of SCH55700 treatment. The demographic and clinical characteristics of these study participants are summarized in Table I. Peripheral blood samples were also obtained from 8 normal volunteers. All participants were seen as part of clinical protocols that were approved by the Institutional Review Board of the National Institute of Allergy and Infectious Diseases, and informed consent was obtained from all participants. Peripheral eosinophil counts were performed in the Clinical Pathology Department at the National Institutes of Health Clinical Center using an automated cell counter. Anti IL-5 treatment Patients received a single intravenous 1-mg/kg dose of the humanized monoclonal anti IL-5 antibody SCH55700 (provided by Schering-Plough Research Institute, Kenilworth, NJ) and were followed in an in-patient setting for a minimum of 72 hours to monitor adverse effects secondary to the infusion. Follow-up visits were performed at days 7, 14, and 28 in all patients and then monthly until the eosinophil count returned to baseline for 2 months. Therapies known to affect eosinophilia, including prednisone, hydroxyurea, and IFN-a, that were initiated before SCH55700 infusion were maintained at the same dose throughout the study period. Drug levels and pharmacokinetics of SCH55700 were comparable among the patients who were and were not taking other medications. Eosinophil purification Eosinophils were isolated from peripheral blood by immunomagnetic negative selection using a modification of the method of Hansel et al. 15 Briefly, EDTA venous blood diluted with PBS (ph 7.4) or granulocyte-enriched apheresis product were layered on Ficoll-Paque (Amersham Biosciences AB, Uppsala, Sweden) and centrifuged at 576g for 30 minutes. After removing the supernatant and PBMC layer, the granulocytes covering the red blood cell pellet were collected, and the red blood cells were lysed 2 times by hypotonic shock with sterile endotoxin-free ice-cold distilled water. To eliminate the neutrophils, granulocytes were incubated with micromagnetic beads coated with anti-cd16 (Miltenyi Biotech, Bergisch, Bladbach, Germany) for 40 minutes on ice before passage through the magnetic-activated separation column (Miltenyi Biotech). To remove further the minute numbers of contaminating T and B lymphocytes and monocytes, the CD16 2 cells were incubated with additional micromagnetic beads coated with anti-cd3, anti-cd14, and anti- CD19 (Miltenyi Biotech) for 20 minutes on ice before the second passage through the column (Miltenyi Biotech). Cytospin slides of purified eosinophils were stained with Diff-Quick fixative and solutions I and II (Dade Behring, Newark, Del), and 500 cells were counted to determine purity. The purity of eosinophils was consistently >99%. Eosinophil culture and survival assay Purified eosinophils from patients (pretreatment, n = 8; 1 month posttreatment, n = 5) and normal controls (n = 8) were cultured (10 5 cells/200 ml/well) in media containing RPMI-1640 (BioWhittaker, Walkersville, Md) supplemented with 10% heat-inactivated defined FCS (Hyclone, Logan, Utah), 20 mmol/l L-glutamine (BioWhittaker), 10 mmol/l HEPES (BioWhittaker), 50 mg/ml gentamicin (Mediatech, Herndon, Va), and 1 mmol/l pyruvate (Biofluids, Gaithersburg, Md) at 37 C in 96-well flat-bottom culture plates (Corning, Corning, NY). Various concentrations (50 fg/ml [~1.67 pmol/l] to 5 ng/ml [~ pmol/l]) of IL-5 (PharMingen, San Diego, Calif) were added to the culture media. All cultures were performed in triplicate. After 4 days of culture, cells were stained with annexin V and propidium iodide, and the percentage of live eosinophils (annexin V-negative and propidium iodide-negative cells) was determined by flow cytometry. In some cultures, purified eosinophils from a normal control donor were cultured with 1% heatinactivated sera from patients before and at 1 month after treatment with SCH In vitro blocking experiment To identify the nature of the serum factor responsible for the prolongation of eosinophil survival in vitro, blocking experiments were performed with anticytokine mabs. First, the minimum cytokine concentration required to produce >50% survival of normal donor eosinophils after 4 days in culture was determined for each cytokine (IL-5, IL-3, GM-CSF, and IFN-g). Next, normal donor eosinophils were cultured in the presence of this fixed cytokine concentration over a wide range of concentrations of the corresponding neutralizing antibody (10 ng/ml to 25 mg/ml). Purified eosinophils from a normal donor were then incubated with 1% posttreatment serum in the presence or absence of the same range of concentrations of neutralizing anticytokine antibodies (anti GM- CSF, anti IFN-g, anti IL-3; BD Pharmingen) or isotype control antibodies (rat IgG2a for anti GM-CSF; mouse IgG1 for anti IFN-g; rat IgG1 for anti IL-3 and anti IL-5; BD Pharmingen), and viability was assessed as described. Cytokine measurement and intracellular cytokine frequency assessment Serum levels of cytokines (IL-2, IL-3, IL-5, IL-8, IL-15, GM-CSF, IFN-g, and TNF-a) were determined using a multiplex sandwich ELISA (Pierce Biotechnology, Rockford, Ill). PBMC intracellular cytokine production was measured before and at 1 month posttreatment in 4 patients (2 patients with HES and 2 with EGE) by flow cytometry. Briefly, PBMCs were isolated by Ficoll diatrizoate gradient centrifugation lymphocyte separation medium; ICN Biomedicals, Aurora, Ohio). Erythrocytes were lysed using ACK lysis buffer (BioSource International, Camarillo, Calif). Cells
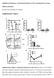
3 J ALLERGY CLIN IMMUNOL VOLUME 114, NUMBER 6 Kim et al 1451 TABLE I. Patient characteristics Patient number Diagnosis HES EGE Age (y) Sex M F M F F F M M Concomitant therapy* H P P, H, I H N N P N Baseline eosinophil count (per mm 3 ) Baseline serum IL-5 (pg/ml) < <1.95 < <1.95 Response to treatmentà R R NR NR R R R R *P, Prednisone; H, hydroxyurea; I, IFN-a; N, none. Serum IL-5 was measured by using a multiplex sandwich ELISA. àr, Responder; NR, nonresponder, as defined by a decrease in absolute eosinophil count of 30% in response to a single 1 mg/kg dose of SCH55700 and symptomatic improvement. FIG 1. Rebound eosinophilia after anti IL-5 treatment. Each line shows an individual patient s changes in eosinophil counts. The dates plotted on the x-axis are not linear to show better the changes in eosinophil count observed during the early time points after treatment. Open symbols, patients with HES; solid, patients with EGE. *,, 2 nonresponding patients, patients 3 and 4. were then washed and cultured at a concentration of /ml for 6 hours with or without phorbol 12-myristate 13-acetate (PMA; 50 ng/ ml)/ionomycin (1 mg/ml) in RPMI 1640 (BioWhittaker) supplemented with 10 mmol/l HEPES (BioWhittaker), 20 mmol/l glutamine (BioWhittaker), 10% heat-inactivated FCS (Harlan Bioproducts for Science, Madison, Wis), and 50 mg/ml gentamicin (Mediatech). Monensin (2 mmol/l) was added after the first hour of culture to block cytokine secretion. Cells were then fixed with 4% paraformaldehyde and frozen at 270 C until use. Fixed cells were thawed, permeabilized in PBS/0.1% saponin, and stained concurrently for surface and intracellular flow cytometry using the following antibodies from BD Pharmingen: fluorescein isothiocyanate labeled antihuman CD3 and CD14; peridinin chlorophyll-a protein (PerCP)- labeled antihuman CD4, CD8, and CD19; phycoerythrin-labeled GM-CSF and IL-3; and allophycocyanin-labeled IL-5 and IFN-g. Fluorescence was measured on a FACS Calibur (BD Biosciences, San José, Calif) using 50,000 gated lymphocytes, and frequencies of cells for each cytokine were analyzed. Because surface expression of CD4 is diminished in response to PMA, CD3 1 CD8 2 cells were used as a surrogate for CD3 1 CD4 1 cells in PMA-treated cultures. Statistical analysis Nonparametric comparisons of group means were made using the Mann-Whitney U test for unpaired data and the Wilcoxon signedrank test for paired comparisons. Data are presented as medians and interquartile ranges for medians. A P value <.05 was considered statistically significant for all tests. RESULTS Rebound eosinophilia Within 24 hours of SCH55700 administration, patient eosinophil counts decreased dramatically with concomitant symptomatic improvement. There was a sustained decrease in eosinophilia and symptoms in 6 patients; however, rebound eosinophilia (an increase in eosinophilia to levels greater than or equal to pretreatment levels) was observed in all 6 responders, with peak eosinophil counts occurring between 60 and 90 days posttreatment (Fig 1). Rebound eosinophilia was accompanied by a severe exacerbation of symptoms, including skin rash, mucosal ulceration, angioedema, fatigue, myalgias, and arthralgias. 13 With respect to the 2 nonresponders, there was no effect of SCH55700 on eosinophilia or symptoms in HES patient 3 (* in Fig 1) and a transient decrease in eosinophilia but no improvement in symptoms in HES patient 4 ( in Fig 1). Both patients (HES 3 and HES 4)
4 1452 Kim et al J ALLERGY CLIN IMMUNOL DECEMBER 2004 FIG 2. Normal control and patient pretreatment in vitro eosinophil survival. Eosinophil survival was assessed in media (A) or in the presence of IL-5 (B) for patients and controls. Results are expressed as the geometric mean values for triplicate cultures for each donor. Each symbol represents 1 individual. *Patients with the FIP1L1/ PDGFRA fusion. were treated with additional agents (imatinib mesylate and cyclosporine A, respectively) after the 1-month post- SCH55700 time point to control their eosinophilia and related symptoms. In vitro eosinophil survival To assess the effect of anti IL-5 therapy on eosinophil survival, purified eosinophils from normal donors and from patients before treatment with SCH55700 were cultured in the presence or absence of IL-5 and assessed for viability after 4 days of culture. The median percentages of live eosinophils from normal donors and patients did not differ either in media (controls vs patients, 2.97% [ ] vs 0.97% [ ]) or in response to IL-5 (controls vs patients, 83.2% [ ] vs 73.8% [ ]; Fig 2, A and B). Two patients with HES (patients 1 and 3) with the myeloproliferative variant of HES 4 showed decreased eosinophil survival in response to IL-5 (* in Fig 2, B). Eosinophil survival was compared between eosinophils obtained before and at 1 month post-sch55700 treatment from the 5 patients for whom eosinophils were available from both time points (Fig 3). Eosinophil survival was comparable at the 2 time points in media in 4 patients (patients 1, 2, 3, and 8) and in the presence of IL-5 in all 5 patients. Although the eosinophils from 1 patient with EGE (patient 6) did show increased survival in media (62.49%) at 1 month posttreatment, the response to IL-5 was unchanged (90.12% vs 87.68%). These results suggest that increased responsiveness of eosinophils to IL-5 is not observed after anti IL-5 administration. Posttreatment sera prolong survival of normal eosinophils When normal eosinophils were cultured in media containing 1% patient sera, eosinophil survival was prolonged at day 4 in cultures containing sera obtained 1 month posttreatment compared with those containing pretreatment sera in all 8 patients regardless of their clinical diagnosis (HES or EGE; pretreatment vs posttreatment, median, 10.74% [ ] vs 73.02% [ ] of live cells; P =.01, Wilcoxon signed rank test; Fig 4). Of interest, this posttreatment serum effect on prolonged eosinophil survival was reversed by the addition of the rat monoclonal anti IL-5 antibody TRFK5 in a concentration-dependent manner (Fig 5, B), similar to that observed in control experiments by using TRFK5 to block the effect of recombinant IL-5 on eosinophil survival (Fig 5, A) but not by anti GM-CSF, anti IFN-g, or anti IL-3 (data not shown). Serum cytokine measurements Among the serum cytokines measured (IL-2, IL-3, IL- 5, IL-8, IL-15, GM-CSF, IFN-g, and TNF-a), IL-5 was the only cytokine for which a significant change was observed after anti IL-5 therapy. Serum IL-5 levels were available for 6 patients at all 3 time points (pretreatment, 2-3 days posttreatment, and 1 month posttreatment). Before treatment, 1 patient with HES (patient 4) had markedly elevated serum IL-5 levels (223 pg/ml), and 2 patients with HES (patients 1 and 2) had low but detectable levels of serum IL-5 (2 pg/ml). Serum IL-5 levels fell by 2 to 3 days posttreatment in all 3 patients (patients 1, 2, and 4) with detectable pretreatment levels, although this was most dramatic in the patient with the highest levels at baseline (patient 4; Fig 6, A). When posttreatment serum IL-5 levels were compared, increased levels were observed at 1 month posttreatment compared with levels 2 to 3 days posttreatment in 5 of 6 patients tested (P =.04; Fig 6, B). Levels remained undetectable at all time points in HES patient 3 (Fig 6, A and B). There was no correlation between serum IL-5 levels and the eosinophil survival-enhancing activity of serum. Intracellular cytokine flow-cytometry analysis Frequencies of cytokine-producing PBMCs (T cells, B cells, and monocytes) were assessed by intracellular flow cytometry before and at 1 month posttreatment with SCH55700 in 4 patients (2 with HES and 2 with EGE). Frequencies of CD3 1 cells producing IL-5 spontaneously or in response to PMA/ionomycin were extremely low (<2.5%) in all patients before SCH55700 treatment. Furthermore, there was no significant change in the frequencies of IL-5 producing cells at 1 month posttreatment either unstimulated or PMA/ionomycin stimulated. Indeed, the median values for CD3 1 CD8 1 unstimulated cells were 0.00 vs 0.00 (pretreatment vs posttreatment) and for PMA/ionomycin stimulated cells, 0.03 vs 0.15 (P >.35 for both comparisons). Similarly, for the CD3 1 CD4 1 cells, the unstimulated median frequencies were 1.06 vs 0.00 (P =.89), and for the stimulated cells, 0.39 vs 0.60 (P =.77). No significant change in the frequencies of GM-CSF producing, IL-3 producing, and IFN-g producing T cells, B cells, or monocytes (both unstimulated and stimulated) was observed after SCH55700 treatment (P >.2 for all comparisons).
5 J ALLERGY CLIN IMMUNOL VOLUME 114, NUMBER 6 Kim et al 1453 FIG 3. In vitro eosinophil survival responses before and after treatment with anti IL-5. Eosinophil survival was assessed before and at 1 month posttreatment in media (A) and in the presence of IL-5 (B). Results are expressed as the geometric mean values for triplicate cultures for each donor. Pretreatment and posttreatment responses are indicated by gray and black bars, respectively. DISCUSSION Rebound eosinophilia was observed in all 6 subjects with HES and EGE who responded to SCH55700 with a sustained drop in eosinophil count and was accompanied by recurrence or exacerbation of symptoms in 75% (6/8) of subjects. This rebound appeared to be independent of the underlying cause of the eosinophilia, because it was seen in subjects with either FIP1L1/PDGFRA-positive or FIP1L1/PDGFRA-negative HES 13 and in subjects with EGE. 14 A similar rebound eosinophilia was observed in a pilot double-blind, randomized study of SCH55700 in human asthma after a single dose of 0.3 mg/kg, with a doubling of mean baseline eosinophil counts by day 90 posttreatment. 12 Rebound was not seen with higher-dose therapy (1 mg/kg), suggesting that the relationship between IL-5 and anti IL-5 levels may be crucial in determining when and whether rebound eosinophilia occurs. Although an increase in eosinophil count above baseline was not specifically described in a recent study of anti IL- 5 antibody (mepolizumab) treatment of 3 patients with HES and eosinophilic dermatitis, 16 additional antibody was given in 2 of the 3 patients for worsening eosinophil count and symptoms. However, differences in the antibodies (mepolizumab vs SCH55700), dosing (750 mg/dose of mepolizumab vs 1 mg/kg of SCH55700), patient populations, and study designs between the mepolizumab study and the current report make direct comparisons difficult. There are numerous potential explanations for the rebound eosinophilia observed in our study. SCH55700 could have led to an increase in eosinophil responsiveness to eosinophilopoietic cytokines through modulation of receptor expression. It has been shown previously that IL-5 induces downmodulation of IL-5Ra surface expression on eosinophils. 17 Because the addition of anti IL-5 in vitro can prevent this downregulation, 18 it is theoretically FIG 4. Prolongation of normal eosinophil survival by posttreatment patients sera. Normal eosinophils were incubated with 1% sera from patients with HES (open symbols) or EGE (solid symbols) before and at 1 month posttreatment, and survival was assessed by flow cytometry. The horizontal bars are the median values. P =.01, Wilcoxon signed-rank test. possible that the combination of increased IL-5Ra receptor expression and increased IL-5 levels could have led to a transient increase in eosinophilia. To address this possibility, we examined eosinophil survival in response to various concentrations of IL-5 before and after treatment with SCH Although less direct than quantification of surface expression levels of IL-5Ra by flow cytometry, this assay provides a more biologically relevant assessment of eosinophil responsiveness to IL-5. Eosinophil survival in response to IL-5 was not increased posttreatment (Fig 3, B), suggesting that increased or altered surface expression of IL-5Ra did not play a significant role in the rebound eosinophilia observed after treatment with SCH Potentiation of IL-5 signaling by mabs to IL-5 has been described in vitro 19 and could account for increased eosinophilia after the administration of SCH Although the timing of the observed rebound eosinophilia seemed inconsistent with this hypothesis, IL-5 mediated
6 1454 Kim et al J ALLERGY CLIN IMMUNOL DECEMBER 2004 FIG 5. Reversal of the prolongation of normal eosinophil survival by posttreatment serum by the rat monoclonal antihuman IL-5 antibody TRFK5. Eosinophil survival was assessed in the presence of 1% posttreatment serum from a patient with HES and increasing concentrations of TRFK5 or rat IgG1k isotype control antibody (B). Similar data are shown using a fixed concentration of recombinant IL-5 to prolong survival (A). FIG 6. Changes in serum IL-5 levels. Serum IL-5 levels are compared before and at 2 to 3 days posttreatment (A) and at 2 to 3 days and 1 month posttreatment (B) for 6 patients with HES (open) or EGE (solid). *,, 2 nonresponding patients. P =.04 for comparison between 2-day to 3-day posttreatment and 1-month posttreatment serum IL-5 levels. eosinophil survival was assessed in the presence of various concentrations of TRFK5, a murine antihuman IL-5 antibody that shares antibody specificity with SCH As expected, TRFK5 blocked (and did not potentiate) IL-5 induced eosinophil survival. The formation of neutralizing antibodies against SCH55700 could also lead to rapid clearance of the drug and subsequent rebound eosinophilia, although such antibodies were not detected in preclinical studies. Serum levels of SCH55700 remained detectable throughout the study period and rose with each additional dose in patients who later received multiple doses, inconsistent with this hypothesis. 13 Of note, this is consistent with the data from preclinical and human asthma studies in which neutralizing anti-sch55700 antibodies could not be demonstrated. 12 Finally, alterations in serum cytokine or chemokine levels after SCH55700 treatment might be responsible for the rebound eosinophilia. Of the serum cytokine levels examined, only IL-5 levels correlated with the observed rebound eosinophilia. This relationship was confirmed by eosinophil survival studies that demonstrated that the prolongation of eosinophil survival observed in the presence of posttreatment sera was reversed by adding
7 J ALLERGY CLIN IMMUNOL VOLUME 114, NUMBER 6 Kim et al 1455 anti IL-5 antibody in vitro. The presence of increased serum levels of IL-5 can be explained by at least 2 mechanisms: increased cellular production of IL5 and/or decreased clearance of biologically active cytokine/ antibody complexes. Several cells in the bone marrow and peripheral blood including eosinophils, mast cells, and CD4 1 T cells can produce significant amounts of IL Despite increased serum levels of IL-5 in 5 of 6 patients at 1 month after treatment with SCH55700, the numbers of IL-5 producing PBMCs detected by intracellular flow cytometry were very low and did not increase posttreatment. Increased IL-5 production by other cell types, including eosinophils and their progenitors, remains a possibility that could not be explored because of the lack of cells for study. Anti IL-5 antibody has been reported to have a preferential effect on later-stage eosinophil progenitors in the bone marrow, causing a transient maturational arrest in the bone marrow. 23 Although accumulation of eosinophil progenitors was not observed in our study, 13 the timing of the bone marrow examinations may not have been optimal to detect these changes. Prolongation of the in vivo effects of cytokines by soluble cytokine/anticytokine complexes has been described in vivo in a murine model and depends on the molar ratio of the cytokine to its antibody. 24 This effect is thought to result primarily from decreased clearance of biologically active cytokine/anticytokine complexes. Although we were unable to explore this phenomenon in vivo, addition of soluble cytokine/anticytokine complexes over a wide range of molar ratios to normal eosinophil cultures was unable to sustain eosinophil survival in vitro (data not shown). In conclusion, the rebound eosinophilia seen after SCH55700 treatment in patients with HES and EGE does not appear to be a result of a fundamental change in the eosinophils themselves but rather of a transient increase in serum IL-5 levels. The cellular source of this increased IL-5 and the mechanism by which it occurs need to be clarified to assess better the effect of rebound eosinophilia on the utility of anti IL-5 antibody treatment for eosinophil-mediated disorders. REFERENCES 1. Chusid MJ, Dale DC, West BC, Wolff SM. The hypereosinophilic syndrome: analysis of fourteen cases with review of the literature. Medicine (Baltimore) 1975;54: Butterfield JH, Gleich GJ. Response of six patients with idiopathic hypereosinophilic syndrome to interferon a. J Allergy Clin Immunol 1994;94: Parrillo JE, Fauci AS, Wolff SM. The hypereosinophilic syndrome: dramatic response to therapeutic intervention. Trans Assoc Am Physicians 1977;90: Klion AD, Noel P, Akin C, Law MA, Gilliland DG, Cools J, et al. Elevated serum tryptase levels identify a subset of patients with a myeloproliferative variant of idiopathic hypereosinophilic syndrome associated with tissue fibrosis, poor prognosis, and imatinib responsiveness. Blood 2003;101: Pardanani A, Reeder T, Porrata LF, Li CY, Tazelaar HD, Baxter EJ, et al. Imatinib therapy for hypereosinophilic syndrome and other eosinophilic disorders. Blood 2003;101: Ault P, Cortes J, Koller C, Kaled ES, Kantarjian H. Response of idiopathic hypereosinophilic syndrome to treatment with imatinib mesylate. Leuk Res 2002;26: Cortes J, Ault P, Koller C, Thomas D, Ferrajoli A, Wierda W, et al. Efficacy of imatinib mesylate in the treatment of idiopathic hypereosinophilic syndrome. Blood 2003;101: Cools J, DeAngelo DJ, Gotlib J, Stover EH, Legare RD, Cortes J, et al. A tyrosine kinase created by fusion of the PDGFRA and FIP1L1 genes as a therapeutic target of imatinib in idiopathic hypereosinophilic syndrome. N Engl J Med 2003;348: Lee M, Hodges WG, Huggins TL, Lee EL. Eosinophilic gastroenteritis. South Med J 1996;89: Kelly KJ. Eosinophilic gastroenteritis. J Pediatr Gastroenterol Nutr 2000; 30:S Egan RW, Athwal D, Bodmer MW, Carter JM, Chapman RW, Chou C, et al. Effect of Sch 55700, a humanized monoclonal antibody to human interleukin-5, on eosinophilic responses and bronchial hyperreactivity. Arzneimittelforschung 1999;49: Kips JC, O Connor BJ, Langley SJ, Woodcock A, Kerstjens HA, Postma DS, et al. Effect of SCH55700, a humanized anti-human interleukin-5 antibody, in severe persistent asthma: a pilot study. Am J Respir Crit Care Med 2003;167: Klion AD, Law MA, Noel P, Kim YJ, Haverty TP, Nutman TB. Safety and efficacy of the monoclonal anti-interleukin-5 antibody SCH55700 in the treatment of patients with hypereosinophilic syndrome. Blood 2004; 103: Prussin C, James SP, Huber MM, Klion AD, Metcalfe DD. Pilot study of anti-il-5 in eosinophilic gastroenteritis. J Allergy Clin Immunol 2003; 111:S Hansel TT, De Vries IJ, Iff T, Rihs S, Wandzilak M, Betz S, et al. An improved immunomagnetic procedure for the isolation of highly purified human blood eosinophils. J Immunol Methods 1991;145: Plotz SG, Simon HU, Darsow U, Simon D, Vassina E, Yousefi S, et al. Use of an anti-interleukin-5 antibody in the hypereosinophilic syndrome with eosinophilic dermatitis. N Engl J Med 2003;349: Liu LY, Sedgwick JB, Bates ME, Vrtis RF, Gern JE, Kita H, et al. Decreased expression of membrane IL-5 receptor a on human eosinophils, II: IL-5 down-modulates its receptor via a proteinase-mediated process. J Immunol 2002;169: Hellman C, Hallden G, Hylander B, Lundahl J. Regulation of the interleukin-5 receptor a-subunit on peripheral blood eosinophils from healthy subjects. Clin Exp Immunol 2003;131: Zabeau L, Van der Heyden J, Broekaert D, Verhee A, Vandekerckhove J, Wu SJ, et al. Neutralizing monoclonal antibodies can potentiate IL-5 signaling. Eur J Immunol 2001;31: Bradding P, Feather IH, Wilson S, Bardin PG, Heusser CH, Holgate ST, et al. Immunolocalization of cytokines in the nasal mucosa of normal and perennial rhinitic subjects: the mast cell as a source of IL-4, IL-5, and IL-6 in human allergic mucosal inflammation. J Immunol 1993;151: Enokihara H, Furusawa S, Nakakubo H, Kajitani H, Nagashima S, Saito K, et al. T cells from eosinophilic patients produce interleukin-5 with interleukin-2 stimulation. Blood 1989;73: Walker C, Virchow JC Jr, Bruijnzeel PL, Blaser K. T cell subsets and their soluble products regulate eosinophilia in allergic and nonallergic asthma. J Immunol 1991;146: Menzies-Gow A, Flood-Page P, Sehmi R, Burman J, Hamid Q, Robinson DS, et al. Anti-IL-5 (mepolizumab) therapy induces bone marrow eosinophil maturational arrest and decreases eosinophil progenitors in the bronchial mucosa of atopic asthmatics. J Allergy Clin Immunol 2003; 111: Finkelman FD, Morris SC. Development of an assay to measure in vivo cytokine production in the mouse. Int Immunol 1999;11:
National Horizon Scanning Centre. Mepolizumab (Bosatria) for hypereosinophilic syndrome first line in combination with corticosteroids.
 Mepolizumab (Bosatria) for hypereosinophilic syndrome first line in combination with corticosteroids May 2008 This technology summary is based on information available at the time of research and a limited
Mepolizumab (Bosatria) for hypereosinophilic syndrome first line in combination with corticosteroids May 2008 This technology summary is based on information available at the time of research and a limited
Bead Based Assays for Cytokine Detection
 Bead Based Assays for Cytokine Detection September 27, 2014 6 th EFIS-EJI South East European Immunology School SEEIS 2014 Timisoara, Romania The Cells of the Immune System The Immune Reaction (Th2) (Th1)
Bead Based Assays for Cytokine Detection September 27, 2014 6 th EFIS-EJI South East European Immunology School SEEIS 2014 Timisoara, Romania The Cells of the Immune System The Immune Reaction (Th2) (Th1)
Recent Advances in the Diagnosis and Treatment of Hypereosinophilic Syndromes
 Recent Advances in the Diagnosis and Treatment of Hypereosinophilic Syndromes Amy D. Klion Hypereosinophilic syndromes (HES) are a heterogeneous group of disorders characterized by marked peripheral blood
Recent Advances in the Diagnosis and Treatment of Hypereosinophilic Syndromes Amy D. Klion Hypereosinophilic syndromes (HES) are a heterogeneous group of disorders characterized by marked peripheral blood
Technical Resources. BD Immunocytometry Systems. FastImmune Intracellular Cytokine Staining Procedures
 FastImmune Intracellular Cytokine Staining Procedures BD has developed protocols for the detection of intracellular cytokines in activated lymphocytes and in activated monocytes. The procedures have been
FastImmune Intracellular Cytokine Staining Procedures BD has developed protocols for the detection of intracellular cytokines in activated lymphocytes and in activated monocytes. The procedures have been
Use of an Anti Interleukin-5 Antibody in the Hypereosinophilic Syndrome with Eosinophilic Dermatitis
 The new england journal of medicine brief report Use of an Anti Interleukin-5 Antibody in the Hypereosinophilic Syndrome with Eosinophilic Dermatitis From the Division of Environmental Dermatology and
The new england journal of medicine brief report Use of an Anti Interleukin-5 Antibody in the Hypereosinophilic Syndrome with Eosinophilic Dermatitis From the Division of Environmental Dermatology and
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Organic dust-induced interleukin-12 production activates T- and natural killer cells
 Eur Respir J 22; 2: 686 69 DOI:.1183/931936.2.222 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Organic dust-induced interleukin-12 production
Eur Respir J 22; 2: 686 69 DOI:.1183/931936.2.222 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Organic dust-induced interleukin-12 production
Interferon γ regulates idiopathic pneumonia syndrome, a. Th17 + CD4 + T-cell-mediated GvH disease
 Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Detailed step-by-step operating procedures for NK cell and CTL degranulation assays
 Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
Primary Adult Naïve CD4+ CD45RA+ Cells. Prepared by: David Randolph at University of Alabama, Birmingham
 Primary Adult Naïve CD4+ CD45RA+ Cells Prepared by: David Randolph (drdrdr@uab.edu) at University of Alabama, Birmingham Goal: To obtain large numbers of highly pure primary CD4+ CD45RO- CD25- cells from
Primary Adult Naïve CD4+ CD45RA+ Cells Prepared by: David Randolph (drdrdr@uab.edu) at University of Alabama, Birmingham Goal: To obtain large numbers of highly pure primary CD4+ CD45RO- CD25- cells from
PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human
 Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Hypereosinophilic Syndrome. Fellow: Eunpi Cho Faculty Discussant: Michael Linenberger
 Hypereosinophilic Syndrome Fellow: Eunpi Cho Faculty Discussant: Michael Linenberger Case 19 yo M admitted to Evergreen Hospital after cardiac arrest. Troponin 8.41, BNP 12,087 Utox pos for amphetamines
Hypereosinophilic Syndrome Fellow: Eunpi Cho Faculty Discussant: Michael Linenberger Case 19 yo M admitted to Evergreen Hospital after cardiac arrest. Troponin 8.41, BNP 12,087 Utox pos for amphetamines
Hypereosinophilic syndromes: A multicenter, retrospective analysis of clinical characteristics and response to therapy
 Hypereosinophilic syndromes: A multicenter, retrospective analysis of clinical characteristics and response to therapy The Harvard community has made this article openly available. Please share how this
Hypereosinophilic syndromes: A multicenter, retrospective analysis of clinical characteristics and response to therapy The Harvard community has made this article openly available. Please share how this
SUPPLEMENTARY INFORMATION. Involvement of IL-21 in the epidermal hyperplasia of psoriasis
 SUPPLEMENTARY INFORMATION Involvement of IL-21 in the epidermal hyperplasia of psoriasis Roberta Caruso 1, Elisabetta Botti 2, Massimiliano Sarra 1, Maria Esposito 2, Carmine Stolfi 1, Laura Diluvio 2,
SUPPLEMENTARY INFORMATION Involvement of IL-21 in the epidermal hyperplasia of psoriasis Roberta Caruso 1, Elisabetta Botti 2, Massimiliano Sarra 1, Maria Esposito 2, Carmine Stolfi 1, Laura Diluvio 2,
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
Rapid antigen-specific T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
ILC1 and ILC3 isolation and culture Following cell sorting, we confirmed that the recovered cells belonged to the ILC1, ILC2 and
 Supplementary Methods and isolation and culture Following cell sorting, we confirmed that the recovered cells belonged to the, ILC2 and subsets. For this purpose we performed intracellular flow cytometry
Supplementary Methods and isolation and culture Following cell sorting, we confirmed that the recovered cells belonged to the, ILC2 and subsets. For this purpose we performed intracellular flow cytometry
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Supplemental Information. T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism
 Immunity, Volume 33 Supplemental Information T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism Franziska Petermann, Veit Rothhammer, Malte
Immunity, Volume 33 Supplemental Information T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism Franziska Petermann, Veit Rothhammer, Malte
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Supervisor: Prof. Dr. P Vandenberghe Dr. C Brusselmans
 Contribution of molecular diagnosis in eosinophilia/hypereosinophilia Eosinophilia Hypereosinophilia Hypereosinophilic syndrome Immune mediated hypereosinophilia Chronic eosinophilic leukemia (NOS)/ Idiopathic
Contribution of molecular diagnosis in eosinophilia/hypereosinophilia Eosinophilia Hypereosinophilia Hypereosinophilic syndrome Immune mediated hypereosinophilia Chronic eosinophilic leukemia (NOS)/ Idiopathic
staining and flow cytometry
 Detection of influenza virus-specific T cell responses by intracellular by cytokine intracellular staining cytokine staining and flow cytometry Detection of influenza virus-specific T cell responses and
Detection of influenza virus-specific T cell responses by intracellular by cytokine intracellular staining cytokine staining and flow cytometry Detection of influenza virus-specific T cell responses and
Effect of Interleukin 10 on the Hematopoietic Progenitor Cells from Patients with Aplastic Anemia
 Effect of Interleukin 10 on the Hematopoietic Progenitor Cells from Patients with Aplastic Anemia YOSHINOBU ASANO, SHOICHIRO SHIBATA, SHINJI KOBAYASHI, SEIICHI OKAMURA, YOSHIYUKI NIHO First Department
Effect of Interleukin 10 on the Hematopoietic Progenitor Cells from Patients with Aplastic Anemia YOSHINOBU ASANO, SHOICHIRO SHIBATA, SHINJI KOBAYASHI, SEIICHI OKAMURA, YOSHIYUKI NIHO First Department
METHODS Penh. Measurements and ribonuclease protection assay. Intracellular cytokine staining. ELISAs RT-PCR. Lung morphometry.
 METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
York criteria, 6 RA patients and 10 age- and gender-matched healthy controls (HCs).
 MATERIALS AND METHODS Study population Blood samples were obtained from 15 patients with AS fulfilling the modified New York criteria, 6 RA patients and 10 age- and gender-matched healthy controls (HCs).
MATERIALS AND METHODS Study population Blood samples were obtained from 15 patients with AS fulfilling the modified New York criteria, 6 RA patients and 10 age- and gender-matched healthy controls (HCs).
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Allergen-induced Increases in Sputum Levels of Group 2 Innate Lymphoid Cells. Guangzhou Medical University, Guangzhou, China.
 Online Supplemental Data Title: Allergen-induced Increases in Sputum Levels of Group 2 Innate Lymphoid Cells in Asthmatic Subjects Authors: Ruchong Chen 1,2, Steven G Smith 1, Brittany Salter 1, Amani
Online Supplemental Data Title: Allergen-induced Increases in Sputum Levels of Group 2 Innate Lymphoid Cells in Asthmatic Subjects Authors: Ruchong Chen 1,2, Steven G Smith 1, Brittany Salter 1, Amani
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
colorimetric sandwich ELISA kit datasheet
 colorimetric sandwich ELISA kit datasheet For the quantitative detection of human IL5 in serum, plasma, cell culture supernatants and urine. general information Catalogue Number Product Name Species cross-reactivity
colorimetric sandwich ELISA kit datasheet For the quantitative detection of human IL5 in serum, plasma, cell culture supernatants and urine. general information Catalogue Number Product Name Species cross-reactivity
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Human and mouse T cell regulation mediated by soluble CD52 interaction with Siglec-10. Esther Bandala-Sanchez, Yuxia Zhang, Simone Reinwald,
 Human and mouse T cell regulation mediated by soluble CD52 interaction with Siglec-1 Esther Bandala-Sanchez, Yuxia Zhang, Simone Reinwald, James A. Dromey, Bo Han Lee, Junyan Qian, Ralph M Böhmer and Leonard
Human and mouse T cell regulation mediated by soluble CD52 interaction with Siglec-1 Esther Bandala-Sanchez, Yuxia Zhang, Simone Reinwald, James A. Dromey, Bo Han Lee, Junyan Qian, Ralph M Böhmer and Leonard
Presentation by Dr. Robert Keller 1998 Conference on the Laboratory Science of HIV
 Presentation by Dr. Robert Keller 1998 Conference on the Laboratory Science of HIV ABSTRACT It has been previously demonstrated that HIV infection is associated with reduced levels of intracellular GSH.
Presentation by Dr. Robert Keller 1998 Conference on the Laboratory Science of HIV ABSTRACT It has been previously demonstrated that HIV infection is associated with reduced levels of intracellular GSH.
Eosinophil Purification from Peripheral Blood
 Chapter 2 Eosinophil Purification from Peripheral Blood Praveen Akuthota, Kelsey Capron, and Peter F. Weller Abstract Eosinophils are granulocytes integral to allergic inflammation and parasitic responses
Chapter 2 Eosinophil Purification from Peripheral Blood Praveen Akuthota, Kelsey Capron, and Peter F. Weller Abstract Eosinophils are granulocytes integral to allergic inflammation and parasitic responses
Supplementary Materials for
 www.sciencesignaling.org/cgi/content/full/8/381/ra59/dc1 Supplementary Materials for Analysis of single-cell cytokine secretion reveals a role for paracrine signaling in coordinating macrophage responses
www.sciencesignaling.org/cgi/content/full/8/381/ra59/dc1 Supplementary Materials for Analysis of single-cell cytokine secretion reveals a role for paracrine signaling in coordinating macrophage responses
IgG3 regulates tissue-like memory B cells in HIV-infected individuals
 SUPPLEMENTARY INFORMATION Articles https://doi.org/10.1038/s41590-018-0180-5 In the format provided by the authors and unedited. IgG3 regulates tissue-like memory B cells in HIV-infected individuals Lela
SUPPLEMENTARY INFORMATION Articles https://doi.org/10.1038/s41590-018-0180-5 In the format provided by the authors and unedited. IgG3 regulates tissue-like memory B cells in HIV-infected individuals Lela
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
METHODS. participated in the study. Each subject had a normal physical examination, chest
 METHODS Subjects Thirty-four subjects (20 men and 14 women, mean age 28.5 ± 1.2 yr) participated in the study. Each subject had a normal physical examination, chest radiograph, electrocardiogram, and laboratory
METHODS Subjects Thirty-four subjects (20 men and 14 women, mean age 28.5 ± 1.2 yr) participated in the study. Each subject had a normal physical examination, chest radiograph, electrocardiogram, and laboratory
Policy Effective 4/1/2018
 Corporate Medical Policy Interleukin-5 Antagonists Notification File Name: Origination: Last CAP Review: Next CAP Review: Last Review: interleukin_5_antagonists 2/2016 11/2017 11/2018 2/2018 Policy Effective
Corporate Medical Policy Interleukin-5 Antagonists Notification File Name: Origination: Last CAP Review: Next CAP Review: Last Review: interleukin_5_antagonists 2/2016 11/2017 11/2018 2/2018 Policy Effective
NEW DEVELOPMENTS AND NOVEL THERAPIES FOR THE TREATMENT OF HES. Amy Klion, MD Laboratory of Parasitic Diseases, NIAID, NIH January 25, 2018
 NEW DEVELOPMENTS AND NOVEL THERAPIES FOR THE TREATMENT OF HES Amy Klion, MD Laboratory of Parasitic Diseases, NIAID, NIH January 25, 2018 Disclosures No financial relationships to disclose None of the
NEW DEVELOPMENTS AND NOVEL THERAPIES FOR THE TREATMENT OF HES Amy Klion, MD Laboratory of Parasitic Diseases, NIAID, NIH January 25, 2018 Disclosures No financial relationships to disclose None of the
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과
 감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
Nature Medicine: doi: /nm.2109
 HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
Gladstone Institutes, University of California (UCSF), San Francisco, USA
 Fluorescence-linked Antigen Quantification (FLAQ) Assay for Fast Quantification of HIV-1 p24 Gag Marianne Gesner, Mekhala Maiti, Robert Grant and Marielle Cavrois * Gladstone Institutes, University of
Fluorescence-linked Antigen Quantification (FLAQ) Assay for Fast Quantification of HIV-1 p24 Gag Marianne Gesner, Mekhala Maiti, Robert Grant and Marielle Cavrois * Gladstone Institutes, University of
Reversal of cardiac abnormalities in a young man with idiopathic hypereosinophilic syndrome using a tyrosine kinase inhibitor
 Eur J Echocardiography (2004) 5, 386e390 CASE REPORTS Reversal of cardiac abnormalities in a young man with idiopathic hypereosinophilic syndrome using a tyrosine kinase inhibitor Luigi Ascione a, ), Mario
Eur J Echocardiography (2004) 5, 386e390 CASE REPORTS Reversal of cardiac abnormalities in a young man with idiopathic hypereosinophilic syndrome using a tyrosine kinase inhibitor Luigi Ascione a, ), Mario
McAb and rhil-2 activated bone marrow on the killing and purging of leukemia cells
 Effects of McAb and rhil-2 activated bone marrow on the killing and purging of leukemia cells X.C. Wei, D.D. Yang, X.R. Han, Y.A. Zhao, Y.C. Li, L.J. Zhang and J.J. Wang Institute of hematological research,
Effects of McAb and rhil-2 activated bone marrow on the killing and purging of leukemia cells X.C. Wei, D.D. Yang, X.R. Han, Y.A. Zhao, Y.C. Li, L.J. Zhang and J.J. Wang Institute of hematological research,
In vitro human regulatory T cell expansion
 - 1 - Human CD4 + CD25 + regulatory T cell isolation, Workflow in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation of T
- 1 - Human CD4 + CD25 + regulatory T cell isolation, Workflow in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation of T
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
In vitro human regulatory T cell suppression assay
 Human CD4 + CD25 + regulatory T cell isolation, in vitro suppression assay and analysis In vitro human regulatory T cell suppression assay Introduction Regulatory T (Treg) cells are a subpopulation of
Human CD4 + CD25 + regulatory T cell isolation, in vitro suppression assay and analysis In vitro human regulatory T cell suppression assay Introduction Regulatory T (Treg) cells are a subpopulation of
In vitro human regulatory T cell expansion
 - 1 - Human CD4 + CD25 + CD127 dim/- regulatory T cell Workflow isolation, in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation
- 1 - Human CD4 + CD25 + CD127 dim/- regulatory T cell Workflow isolation, in vitro expansion and analysis In vitro human regulatory T cell expansion Introduction Regulatory T (Treg) cells are a subpopulation
Supporting Information
 Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4
 Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4 Ankita Garg, Rodney Trout and Stephen A. Spector,,* Department
Human Immunodeficiency Virus Type-1 Myeloid Derived Suppressor Cells Inhibit Cytomegalovirus Inflammation through Interleukin-27 and B7-H4 Ankita Garg, Rodney Trout and Stephen A. Spector,,* Department
Supplementary Figure 1. IL-12 serum levels and frequency of subsets in FL patients. (A) IL-12
 1 Supplementary Data Figure legends Supplementary Figure 1. IL-12 serum levels and frequency of subsets in FL patients. (A) IL-12 serum levels measured by multiplex ELISA (Luminex) in FL patients before
1 Supplementary Data Figure legends Supplementary Figure 1. IL-12 serum levels and frequency of subsets in FL patients. (A) IL-12 serum levels measured by multiplex ELISA (Luminex) in FL patients before
The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF
 CORRECTION NOTICE Nat.Immunol. 12, 568 575 (2011) The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF Mohamed El-Behi, Bogoljub Ciric, Hong
CORRECTION NOTICE Nat.Immunol. 12, 568 575 (2011) The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF Mohamed El-Behi, Bogoljub Ciric, Hong
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Anti-IgE: beyond asthma
 Anti-IgE: beyond asthma Yehia El-Gamal, MD, PhD, FAAAAI Professor of Pediatrics Pediatric Allergy and Immunology Unit Children s Hospital, Ain Shams University Member, WAO Board of Directors Disclosure
Anti-IgE: beyond asthma Yehia El-Gamal, MD, PhD, FAAAAI Professor of Pediatrics Pediatric Allergy and Immunology Unit Children s Hospital, Ain Shams University Member, WAO Board of Directors Disclosure
Supplementary Figure 1. Characterization of basophils after reconstitution of SCID mice
 Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Allergic rhinitis (Hay fever) Asthma Anaphylaxis Urticaria Atopic dermatitis
 Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Persistent food allergy might present a more challenging situation. Patients with the persistent form of food allergy are likely to have a less
 Iride Dello Iacono Food allergy is an increasingly prevalent problem in westernized countries, and there is an unmet medical need for an effective form of therapy. A number of therapeutic strategies are
Iride Dello Iacono Food allergy is an increasingly prevalent problem in westernized countries, and there is an unmet medical need for an effective form of therapy. A number of therapeutic strategies are
Optimizing Intracellular Flow Cytometry
 Optimizing Intracellular Flow Cytometry Detection of Cytokines, Transcription Factors, and Phosphoprotein by Flow Cytometry Presented by Erika O Donnell, PhD, BD Biosciences 23-14876-00 Outline Basic principles
Optimizing Intracellular Flow Cytometry Detection of Cytokines, Transcription Factors, and Phosphoprotein by Flow Cytometry Presented by Erika O Donnell, PhD, BD Biosciences 23-14876-00 Outline Basic principles
Suppl Video: Tumor cells (green) and monocytes (white) are seeded on a confluent endothelial
 Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Difference in Cytokine Production and Cell Activation between Adenoidal Lymphocytes and Peripheral Blood Lymphocytes of Children with Otitis Media
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Sept. 2005, p. 1130 1134 Vol. 12, No. 9 1071-412X/05/$08.00 0 doi:10.1128/cdli.12.9.1130 1134.2005 Copyright 2005, American Society for Microbiology. All
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Sept. 2005, p. 1130 1134 Vol. 12, No. 9 1071-412X/05/$08.00 0 doi:10.1128/cdli.12.9.1130 1134.2005 Copyright 2005, American Society for Microbiology. All
GSI Canine IL-5 ELISA Kit-2 Plates DataSheet
 Interleukin5 (IL5) is a secreted glycoprotein that belongs to the α-helical group of cytokines (1, 2, 3). Unlike other family members, it is present as a covalently linked antiparallel dimer (4, 5). IL-5
Interleukin5 (IL5) is a secreted glycoprotein that belongs to the α-helical group of cytokines (1, 2, 3). Unlike other family members, it is present as a covalently linked antiparallel dimer (4, 5). IL-5
NK cell flow cytometric assay In vivo DC viability and migration assay
 NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
Supplementary Figures
 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
CD14 + S100A9 + Monocytic Myeloid-Derived Suppressor Cells and Their Clinical Relevance in Non-Small Cell Lung Cancer
 CD14 + S1A9 + Monocytic Myeloid-Derived Suppressor Cells and Their Clinical Relevance in Non-Small Cell Lung Cancer Po-Hao, Feng M.D., Kang-Yun, Lee, M.D. Ph.D., Ya-Ling Chang, Yao-Fei Chan, Lu- Wei, Kuo,Ting-Yu
CD14 + S1A9 + Monocytic Myeloid-Derived Suppressor Cells and Their Clinical Relevance in Non-Small Cell Lung Cancer Po-Hao, Feng M.D., Kang-Yun, Lee, M.D. Ph.D., Ya-Ling Chang, Yao-Fei Chan, Lu- Wei, Kuo,Ting-Yu
Spontaneous production of interleukin-5 and its heterogeneous effect on eosinophils in an adult T-cell leukemia patient
 Allergology International (2000) 49: 167 171 Case Report Spontaneous production of interleukin-5 and its heterogeneous effect on eosinophils in an adult T-cell leukemia patient Naoki Saita, Eisuke Goto,
Allergology International (2000) 49: 167 171 Case Report Spontaneous production of interleukin-5 and its heterogeneous effect on eosinophils in an adult T-cell leukemia patient Naoki Saita, Eisuke Goto,
Hypereosinophili c syndrome
 Hypereosinophili c syndrome Eosinophilia Eosinophilia is commonly defined as an elevated percentage of eosinophils, with an absolute eosinophil count > 500 cells per cubic millimeter Secondary Primary
Hypereosinophili c syndrome Eosinophilia Eosinophilia is commonly defined as an elevated percentage of eosinophils, with an absolute eosinophil count > 500 cells per cubic millimeter Secondary Primary
SUPPLEMENTARY INFORMATION
 doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/24366 holds various files of this Leiden University dissertation Author: Buddingh, Emilie Pauline Title: Innate immunity in osteosarcoma Issue Date: 2014-03-05
Cover Page The handle http://hdl.handle.net/1887/24366 holds various files of this Leiden University dissertation Author: Buddingh, Emilie Pauline Title: Innate immunity in osteosarcoma Issue Date: 2014-03-05
Figure S1. PMVs from THP-1 cells expose phosphatidylserine and carry actin. A) Flow
 SUPPLEMENTARY DATA Supplementary Figure Legends Figure S1. PMVs from THP-1 cells expose phosphatidylserine and carry actin. A) Flow cytometry analysis of PMVs labelled with annexin-v-pe (Guava technologies)
SUPPLEMENTARY DATA Supplementary Figure Legends Figure S1. PMVs from THP-1 cells expose phosphatidylserine and carry actin. A) Flow cytometry analysis of PMVs labelled with annexin-v-pe (Guava technologies)
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
Implications on therapy. Prof. of Medicine and Allergy Faculty of Medicine, Cairo University
 Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Therapeutic Immunization with Autologous DC Pulsed with Autologous Inactivated HIV-1 Infected Apoptotic Cells
 Therapeutic Immunization with Autologous DC Pulsed with Autologous Inactivated HIV-1 Infected Apoptotic Cells Sharon A. Riddler, MD, MPH University of Pittsburgh May 2008 Slide 1 HIV and DC Vaccines During
Therapeutic Immunization with Autologous DC Pulsed with Autologous Inactivated HIV-1 Infected Apoptotic Cells Sharon A. Riddler, MD, MPH University of Pittsburgh May 2008 Slide 1 HIV and DC Vaccines During
Supplemental Methods. CD107a assay
 Supplemental Methods CD107a assay For each T cell culture that was tested, two tubes were prepared. One tube contained BCMA-K562 cells, and the other tube contained NGFR-K562 cells. Both tubes contained
Supplemental Methods CD107a assay For each T cell culture that was tested, two tubes were prepared. One tube contained BCMA-K562 cells, and the other tube contained NGFR-K562 cells. Both tubes contained
CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads (Miltenyi Biotec) for depletion of CD25 +
 Supplements Supplemental Materials and Methods Depletion of CD25 + T-cells from PBMC. Fresh or HD precultured PBMC were stained with the conjugate CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads
Supplements Supplemental Materials and Methods Depletion of CD25 + T-cells from PBMC. Fresh or HD precultured PBMC were stained with the conjugate CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads
Supplementary Data Table of Contents:
 Supplementary Data Table of Contents: - Supplementary Methods - Supplementary Figures S1(A-B) - Supplementary Figures S2 (A-B) - Supplementary Figures S3 - Supplementary Figures S4(A-B) - Supplementary
Supplementary Data Table of Contents: - Supplementary Methods - Supplementary Figures S1(A-B) - Supplementary Figures S2 (A-B) - Supplementary Figures S3 - Supplementary Figures S4(A-B) - Supplementary
Mouse Cathepsin B ELISA Kit
 GenWay Biotech, Inc. 6777 Nancy Ridge Drive San Diego, CA 92121 Phone: 858.458.0866 Fax: 858.458.0833 Email: techline@genwaybio.com http://www.genwaybio.com Mouse Cathepsin B ELISA Kit Catalog No. GWB-ZZD154
GenWay Biotech, Inc. 6777 Nancy Ridge Drive San Diego, CA 92121 Phone: 858.458.0866 Fax: 858.458.0833 Email: techline@genwaybio.com http://www.genwaybio.com Mouse Cathepsin B ELISA Kit Catalog No. GWB-ZZD154
Effects of Gelsolin on Macrophage Inflammatory Responses to Implant Wear Debris
 Effects of Gelsolin on Macrophage Inflammatory Responses to Implant Wear Debris William Michael Mihalko, MD PhD, Lev Djenderedjian, Paramjeet S. Cheema, Richard A. Smith, PhD. University of Tennessee,
Effects of Gelsolin on Macrophage Inflammatory Responses to Implant Wear Debris William Michael Mihalko, MD PhD, Lev Djenderedjian, Paramjeet S. Cheema, Richard A. Smith, PhD. University of Tennessee,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Nair S, Branagan AR, Liu J, Boddupalli CS, Mistry PK, Dhodapkar
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Nair S, Branagan AR, Liu J, Boddupalli CS, Mistry PK, Dhodapkar
Crucial role for human Toll-like receptor 4 in the development of contact allergy to nickel
 Supplementary Figures 1-8 Crucial role for human Toll-like receptor 4 in the development of contact allergy to nickel Marc Schmidt 1,2, Badrinarayanan Raghavan 1,2, Verena Müller 1,2, Thomas Vogl 3, György
Supplementary Figures 1-8 Crucial role for human Toll-like receptor 4 in the development of contact allergy to nickel Marc Schmidt 1,2, Badrinarayanan Raghavan 1,2, Verena Müller 1,2, Thomas Vogl 3, György
Disclosures. Learning Objective. Biological therapies. Biologics with action against 11/30/2011. Biologic Asthma Therapies and Individualized Medicine
 Biologic Asthma Therapies and Individualized Medicine Mark S. Dykewicz, MD Director, Allergy & Immunology Fellowship Program Director Wake Forest University School of Medicine Winston-Salem, North Carolina
Biologic Asthma Therapies and Individualized Medicine Mark S. Dykewicz, MD Director, Allergy & Immunology Fellowship Program Director Wake Forest University School of Medicine Winston-Salem, North Carolina
Original Article CD4 + T cell proliferation and inhibition of activation-induced cell death (AICD) in childhood asthma
 Int J Clin Exp Med 2018;11(3):2319-2324 www.ijcem.com /ISSN:1940-5901/IJCEM0066213 Original Article CD4 + T cell proliferation and inhibition of activation-induced cell death (AICD) in childhood asthma
Int J Clin Exp Med 2018;11(3):2319-2324 www.ijcem.com /ISSN:1940-5901/IJCEM0066213 Original Article CD4 + T cell proliferation and inhibition of activation-induced cell death (AICD) in childhood asthma
BD Cytofix/Cytoperm Plus Fixation/Permeabilization Kit (with BD GolgiStop protein transport inhibitor containing monensin) (Cat. No.
 Kit Manual BD Cytofix/Cytoperm Fixation/Permeabilization Kit (Cat. No. 554714) BD Cytofix/Cytoperm Plus Fixation/Permeabilization Kit (with BD GolgiStop protein transport inhibitor containing monensin)
Kit Manual BD Cytofix/Cytoperm Fixation/Permeabilization Kit (Cat. No. 554714) BD Cytofix/Cytoperm Plus Fixation/Permeabilization Kit (with BD GolgiStop protein transport inhibitor containing monensin)
Human Cathepsin D ELISA Kit
 GenWay Biotech, Inc. 6777 Nancy Ridge Drive San Diego, CA 92121 Phone: 858.458.0866 Fax: 858.458.0833 Email: techline@genwaybio.com http://www.genwaybio.com Human Cathepsin D ELISA Kit Catalog No. GWB-J4JVV9
GenWay Biotech, Inc. 6777 Nancy Ridge Drive San Diego, CA 92121 Phone: 858.458.0866 Fax: 858.458.0833 Email: techline@genwaybio.com http://www.genwaybio.com Human Cathepsin D ELISA Kit Catalog No. GWB-J4JVV9
Supplementary Information. A vital role for IL-2 trans-presentation in DC-mediated T cell activation in humans as revealed by daclizumab therapy
 Supplementary Information A vital role for IL-2 trans-presentation in DC-mediated T cell activation in humans as revealed by daclizumab therapy Simone C. Wuest 1, Jehad Edwan 1, Jayne F. Martin 1, Sungpil
Supplementary Information A vital role for IL-2 trans-presentation in DC-mediated T cell activation in humans as revealed by daclizumab therapy Simone C. Wuest 1, Jehad Edwan 1, Jayne F. Martin 1, Sungpil
Peptide stimulation and Intracellular Cytokine Staining
 v Peptide stimulation and Intracellular Cytokine Staining Authors A. Cosma, S. Allgayer MATERIALS Date 01-02-2007 REAGENTS: Version 1.0 - PBMCs - Culture medium - Costimulating antibodies - Peptide pools
v Peptide stimulation and Intracellular Cytokine Staining Authors A. Cosma, S. Allgayer MATERIALS Date 01-02-2007 REAGENTS: Version 1.0 - PBMCs - Culture medium - Costimulating antibodies - Peptide pools
Biologic Therapy in the Management of Asthma. Nabeel Farooqui, MD
 Biologic Therapy in the Management of Asthma Nabeel Farooqui, MD None Disclosures Objectives Define severe asthma phenotypes and endotypes Describe the role of biologics in asthma management Review pivotal
Biologic Therapy in the Management of Asthma Nabeel Farooqui, MD None Disclosures Objectives Define severe asthma phenotypes and endotypes Describe the role of biologics in asthma management Review pivotal
Expression of Fc Gamma Receptors on Peripheral Blood Monocytes and Evaluation of their Role in Phagocytosis Using a Novel Method.
 Expression of Fc Gamma Receptors on Peripheral Blood Monocytes and Evaluation of their Role in Phagocytosis Using a Novel Method. Camilla Holt Degree project in biology, 2006 Examensarbete i biologi 20p,
Expression of Fc Gamma Receptors on Peripheral Blood Monocytes and Evaluation of their Role in Phagocytosis Using a Novel Method. Camilla Holt Degree project in biology, 2006 Examensarbete i biologi 20p,
In vitro bactericidal assay Fig. S8 Gentamicin protection assay Phagocytosis assay
 In vitro bactericidal assay Mouse bone marrow was isolated from the femur and the tibia. Cells were suspended in phosphate buffered saline containing.5% BSA and 2 mm EDTA and filtered through a cell strainer.
In vitro bactericidal assay Mouse bone marrow was isolated from the femur and the tibia. Cells were suspended in phosphate buffered saline containing.5% BSA and 2 mm EDTA and filtered through a cell strainer.
Advances in diagnosis and treatment of eosinophilia
 Advances in diagnosis and treatment of eosinophilia The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version
Advances in diagnosis and treatment of eosinophilia The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version
SUPPLEMENTARY INFORMATION
 Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Supplementalgfigureg1gSchematicgdiagramgofgtumor1modellingg
 SChinjectionh F:LuchLCLsh IVhinjectionh T:cellsh Monitorhforhtumorh growthhandhxeno: reactivehgvhd GVLgexperimentg kcbgvsgpbgt1cellse Xeno1reactiveg experimentg kcbgvsgpbgt1cellse IVhinjectionh 5xh,N^6
SChinjectionh F:LuchLCLsh IVhinjectionh T:cellsh Monitorhforhtumorh growthhandhxeno: reactivehgvhd GVLgexperimentg kcbgvsgpbgt1cellse Xeno1reactiveg experimentg kcbgvsgpbgt1cellse IVhinjectionh 5xh,N^6
Supplementary Figure 1. Efficient DC depletion in CD11c.DOG transgenic mice
 Supplementary Figure 1. Efficient DC depletion in CD11c.DOG transgenic mice (a) CD11c.DOG transgenic mice (tg) were treated with 8 ng/g body weight (b.w.) diphtheria toxin (DT) i.p. on day -1 and every
Supplementary Figure 1. Efficient DC depletion in CD11c.DOG transgenic mice (a) CD11c.DOG transgenic mice (tg) were treated with 8 ng/g body weight (b.w.) diphtheria toxin (DT) i.p. on day -1 and every
Supporting Information
 Supporting Information Bellora et al. 10.1073/pnas.1007654108 SI Materials and Methods Cells. NK cells purified from peripheral blood mononuclear cells (PBMC) of healthy donors (Human NK Cell Isolation
Supporting Information Bellora et al. 10.1073/pnas.1007654108 SI Materials and Methods Cells. NK cells purified from peripheral blood mononuclear cells (PBMC) of healthy donors (Human NK Cell Isolation
Validation of the Efficacy of a Practical Method for Neutrophils Isolation from Peripheral Blood
 Validation of the Efficacy of a Practical Method for Neutrophils Isolation from Peripheral Blood JONATHAN DEGEL, MASIH SHOKRANI OBJECTIVE: The objectives of this study were to validate the Polymorphprep
Validation of the Efficacy of a Practical Method for Neutrophils Isolation from Peripheral Blood JONATHAN DEGEL, MASIH SHOKRANI OBJECTIVE: The objectives of this study were to validate the Polymorphprep
Nature Medicine doi: /nm.3957
 Supplementary Fig. 1. p38 alternative activation, IL-21 expression, and T helper cell transcription factors in PDAC tissue. (a) Tissue microarrays of pancreatic tissue from 192 patients with pancreatic
Supplementary Fig. 1. p38 alternative activation, IL-21 expression, and T helper cell transcription factors in PDAC tissue. (a) Tissue microarrays of pancreatic tissue from 192 patients with pancreatic
