Consensus guidance for the use of debridement techniques in the UK
|
|
|
- Ami Clarke
- 5 years ago
- Views:
Transcription
1 Consensus guidance for the use of debridement techniques in the UK In Autumn 2010, a multidisciplinary group of clinicians met in Manchester to discuss the issue of debridement in wound management. There are various debridement techniques available in the UK, but facilities and skills vary. This paper, resulting from the meeting, briefly outlines the differing techniques used, the levels of skill required to use them and the wound types for which they are appropriate. It is important that clinicians practising debridement are aware of the variations in method, and the limitations of their own skills and competency so that, if appropriate, the patient can be referred to receive timely and appropriate intervention. David Gray*, Claire Acton, Paul Chadwick, Sian Fumarola, David Leaper, Clare Morris, Duncan Stang, Kathryn Vowden, Peter Vowden, Trudie Young KEY WORDS Wound debridement Skills Competency Referral The role of debridement within wound management is well recognised, but there is a lack of standardised guidance on debridement practice in the UK. There is a great disparity in the techniques used and the facilities available. An informal survey of tissue viability nurse specialists (TVNS) carried out by Fairbairn et al (2002) highlighted these issues in the area of sharp debridement. Although many of the TVNS questioned responded that they carried out sharp debridement regularly, their definitions of sharp debridement, the site and extent to which they debrided wounds, their experience and training all varied widely (Fairbairn et al, 2002). All authors were members of the consensus meeting panel; * Chair of the panel. Full author details in Box 1 Flanagan (1999) commented that there was little time for reflection on practice and many clinicians performed ritualistic practice. This is even more evident in today s pressurised work place. In terms of debridement, this can mean that practitioners may operate within their own range of competency (which for many will be autolytic debridement), but Agreement was reached at this meeting that more guidance in wound debridement was needed, and that a document outlining debridement strategies would assist practitioners to address clinical need. this may not be the most appropriate method for an individual patient or their wound. There is a skill in choosing the right debridement method at the right time. Upskilling practitioners in the most recent advances in debridement tools and techniques will help to ensure that the appropriate and optimum treatment options are implemented, thus improving patient care and clinical outcomes. A multidisciplinary group of clinicians (Box 1) held a consensus meeting in the autumn of this year to discuss the issues surrounding the use of wound debridement in the UK. Agreement was reached at this meeting that more guidance in wound debridement was needed, and that a document outlining debridement strategies would assist practitioners to address clinical need. It is important that practitioners are knowledgeable about the different types of debridement available and the level of skills and training required to use them in clinical practice. It was also agreed that clinicians should be able to recognise the indications and contraindications of the various methods, and the limitations of their own skills and competency, so that timely and appropriate referral can be made in order that the patient receives the most appropriate treatment for their wound and general health status. As with any area of practice, healthcare practitioners are responsible for ensuring that they are competent before undertaking a task such as sharp debridement. This document briefly outlines the differing techniques used in the UK, explains the level of skill required, and the patients and wound types on which they can be used. 77
2 Wound debridement The importance of debridement in wound management is well known, and its role in the preparation of the wound bed to promote healing is recognised (Falanga, 2001; Gray et al, 2006; Wolcott et al, 2009). Debridement occurs naturally in wounds and studies indicate that if the process is accelerated, healing will be achieved more quickly (Steed et al, 1996). Debridement is considered to be a beneficial component of wound management because: 8 The presence of devitalised tissue within the wound may mask or mimic signs of infection (O Brien, 2002) 8 Necrotic tissue may serve as a source of nutrients for bacteria, particularly anaerobes such as Bacteroides species and Clostridium perfringens (Leaper, 2002) 8 Devitalised tissue acts as a physical barrier to healing (Kubo et al, 2001) and could prevent the effectiveness of topical preparations such as antimicrobial agents, pain relief and steroids, and may impede normal matrix formation, angiogenesis, granulation tissue formation and epidermal resurfacing (Weir et al, 2007) 8 The presence of necrotic or devitalised tissue contributes to the stimulus to produce inflammatory cytokines which can promote a septic response (Leaper, 2002), and can also lead to the overproduction of matrix metalloproteases (MMPs) (Weir et al, 2007) 8 The presence of necrotic tissue within the wound which may impair healing and lead to an exaggerated inflammatory response, may prevent the clinician from gaining an accurate picture of the extent of tissue destruction, thus inhibiting the clinician s ability to assess the wound correctly (Vowden and Vowden, 1999a; Leaper, 2002; Weir et al, 2007). This may be of particular significance in pressure and diabetic foot ulcers, where the extent of the wound may be underestimated due to the presence of necrotic tissue. BOX 1 Members of the multidisciplinary group 8 Claire Acton, Tissue Viability Manager, Guy s and St Thomas NHS Foundation Trust, London 8 Paul Chadwick, Principal Podiatrist, Salford 8 Sian Fumarola, Clinical Nurse Specialist, University Hospital of North Staffordshire NHS Trust 8 David Gray, Clinical Nurse Specialist, NHS Grampian, Aberdeen 8 Professor David Leaper, Visiting Professor, Department of Dermatology and Wound Healing, Cardiff University 8 Clare Morris, Tissue Viability Advisor, Betsi Cadwaladr University Health Board, North Wales 8 Duncan Stang, Highly Specialist Podiatrist, Hairmyres Hospital, NHS Lanarkshire 8 Kathryn Vowden, Nurse Consultant, Acute and Chronic Wounds, Bradford Teaching Hospitals NHS Foundation Trust and the University of Bradford 8 Peter Vowden, Professor of Wound Healing Research, Bradford Teaching Hospitals NHS Foundation Trust and the University of Bradford It is, therefore, important that necrotic tissue is removed as quickly and efficiently as possible to reduce bioburden and prevent infection (Ayello et al, 2004), promote wound closure and to assist with wound assessment (Reid and Morison, 1994). Wound debridement should be an integral element of good wound care, as outlined in the Best Practice Statement: Optimising Wound Care (2008). It is helpful to have a structured approach to the assessment, diagnosis and management of any type of wound. Figure 1 presents the key stages of assessing and managing a patient with a wound, placing the patient and their needs at the centre of all decisions. The circular nature of the diagram shows that the patient must remain in the centre of the pathway, undergoing continual review of their treatment and wound progress. On review, treatment objectives may change according to the findings and, if so, the patient will require reassessment and the setting of new objectives, etc, continuing around the pathway until the desired outcomes are achieved. The patient may leave and re-enter the pathway at any point, for example, the patient may need specialist referral and leave once a diagnosis has been established, re-entering the pathway at the implementation of treatment. Managers and service providers can also use the pathway, enabling their organisation to embrace workforce planning and allocate resources in a logical and structured way. By using this pathway, the delivery of routine or ritualistic debridement can be avoided and optimal debridement that is tailored to the individual and their wound can be delivered. As part of patient assessment, the practitioner should consider the risk that the devitalised tissue presents to the patient and if there is a need to ensure rapid debridement. Equally, attention should be paid to the patient s overall condition which may rule out surgical debridement but indicate one of the other rapid methods. In the case of a patient who is in the end stages of life and has a wound with devitalised tissue which is malodorous, there may be a strong argument to use a rapid 78
3 Patient assessment Establish a diagnosis and agree objectives Achieved agreed outcome Objective not achieved or new objective set The patient with a wound Establish and document treatment plan and timescale Ongoing review Implement treatment plan Figure 1. Pathway of care for a patient with a wound. method to improve the patient s quality of life. Moistening a wound and autolytic debridement may not always be in the interest of the patient. For example, in Figure 2, the best action would be to debride the slough at the line of demarcation but not to debride the eschar, and allow the digit to mummify and autoamputate (Vowden and Vowden, 1999b). The decision whether or not to debride should be based upon the steps in Figure 1. Methods of debridement should not be considered to be the realm of the specialist or the generalist, but for all clinicians providing that they have the knowledge base and appropriate clinical skills. It is important that the method of debridement selected is the most effective for the patient and not limited by the skills of the practitioner. If the practitioner lacks the required skills they should seek support from within their own team, or consider further training if the situation is likely to occur frequently. Before beginning debridement, the practitioner should consider: 1. What he/she hopes to achieve (prevention of infection, removal of non-viable tissue that will delay the healing process, symptom control). 2. How quickly he/she wishes to achieve this. This will be dependent on factors such as the amount of non-viable tissue to be removed, and its anatomical location. 3. How best to debride, and if he/she can perform the procedure or if referral is needed. Figure 2. Dry necrotic great toe which has mummified following the decision not to attempt autolytic debridement. 79
4 Description of wound Clinical PRACTICE DEVELOPMENT By asking these questions, the decision to debride or not, and the method to be used may become clearer. Access to and availability of skills, clinicians, appropriate products and resources, frequency of care needed and cost-effectiveness will all influence choice. Type of tissue dry necrotic This article will now focus upon the most commonly used methods of debridement in the UK, namely: 8 Autolytic 8 Larval 8 Mechanical 8 Hydrosurgical 8 Ultrasound 8 Sharp 8 Surgical. Autolytic debridement Autolytic debridement describes the use of the body s own enzymes and moisture to rehydrate, soften and liquefy hard eschar and slough. Autolysis of devitalised tissue usually requires a moist, vascular wound environment (Raymundo and Wells, 2000). The use of occlusive and semiocclusive dressings such as hydrogels, hydrocolloids and films help to keep wound fluid in contact with the necrotic tissue, thus maintaining a moist wound healing environment. During autolysis, phagocytic cells and proteolytic enzymes soften and liquefy necrotic tissue, so it can be digested by macrophages (Ayello et al, 2004). This is beneficial as the enzymes are selective to necrotic tissue (Dolynchuk, 2001). There is relatively little pain associated with this form of debridement and it is a versatile, easy technique requiring little or no technical skill (Dolynchuk, 2001). However, autolysis can be a slow process so it is contraindicated in the presence of infection, where rapid intervention is indicated. It can also be associated with an anaerobic odour (Dolynchuk, 2001) and may lead to maceration of the periwound skin if the moisture balance is not correct. wet necrotic dry slough Autolytic debridement is used in clinical practice to soften and rehydrate eschar before using other 80 Wounds Debridement paper C2-final.indd 4 uk, 2011, Vol 7, No 1 15/03/ :03
5 Clinical PRACTICE DEVELOPMENT methods of debridement (Vowden and Vowden, 1999a). Limitations of this method of debridement are that it is not always a safe method, e.g. the slowness of the process may raise the potential for infection, pain and maceration of the periwound skin. It should also not be used on ischaemic feet. Autolysis should be used for predebridement, e.g. before larval therapy, maintenance debridement, when there is a small volume of tissue and a manageable amount of slough, or if there is a risk of injury if other methods such as sharp debridement are used, e.g. not knowing when to stop sharp debridement. It would be suitable for a simple, uncomplicated wound or a traumatic wound with a scab. Autolytic debridement can be achieved using hydrogels, hydrofibre and hydrocolloids. They may be used in conjunction with antimicrobial agents if there is a risk of, or infection present. However, antimicrobial agents are not the answer to problems related to debridement. Further information on the use of antiseptic and antimicrobial agents can be found in documents by the European Wound Management Association (EWMA, 2006), the World Union of Wound Healing Societies (WUWHS, 2008) and the Best Practice Statement on the use of topical antiseptic/antimicrobial agents in wound management (2010). Key points for autolytic debridement include: 8 Most commonly used method of debridement in the UK 8 Can be used by both generalist and specialist practitioners 8 Use should be based on the patient s assessment, not the practitioner s level of skill 8 Appropriate dressings required because of the risk of maceration and/or infection 8 Longest treatment time of all methods of debridement 8 Softens devitalised tissue and encourages autolysis 8 Costs associated with dressings and repeat visits need to be considered. Type of tissue wet slough superficial wet slough haematoma Wounds Debridement paper C2-final.indd 5 uk, 2011, Vol 7, No /03/ :03
6 Wound Clinical care PRACTICE SCIENCE DEVELOPMENT Larval therapy Larval therapy is the use of larvae of the green bottle fly to remove necrotic and devitalised tissue from the wound. It is effective, rapid and highly selective and can therefore be regarded as micro-debridement (Vowden and Vowden, 1999a). There are three mechanisms of action by which maggots work: 8 Debridement 8 Antimicrobial 8 Facilitate healing. Maggots feed on necrotic tissue. They secrete enzymes which semiliquefy the tissue into a form that can be ingested (Sherman, 1998). Maggots have a pair of hooks which they use to attach to the tissue, which disrupt cell membranes to facilitate the penetration of their proteolytic enzymes. Medical maggots are born in sterile conditions and have traditionally been applied to the wound bed with a closed mesh dressing, to prevent the maggots from leaving the wound. However, nowadays, they are usually applied in closed foam bags. They are removed after hours of treatment. Larval therapy is not suitable for all patients. The condition of the wound must be correct to ensure survival of the maggots. For example, the maggots may be squashed by pressure, i.e. if they are used on the heel of an active patient. Larval therapy is quicker than autolytic debridement. Key points for larval therapy include: 8 Can be applied by competent practitioners with specialist training 8 Bagged method reduces the skill required to deliver larval therapy, and can be left in situ for 4 5 days 8 Larvae need to be ordered in advance but treatment time is short once in place 8 Most effective where the devitalised tissue is not dry; softens and liquefies devitalised tissue 8 Costs associated with treatment are higher than autolytic debridement, but treatment times are shorter. Mechanical (wet to dry) Mechanical debridement is used to describe the process of using dressings that adhere to wounds. These are usually wet-to-dry dressings such as gauze. The top layer of the wound bed dries and adheres to the dressing which is then removed. This is non-selective as, on removal, the dressing takes with it both healthy and unhealthy tissue. Being a non-selective method of debridement, it may traumatise healthy or healing tissue. It can be time-consuming, as it calls for frequent dressing changes and is also painful for the patient. Ultrasound There are two types of ultrasound device available in the UK: contact and non-contact. With contact devices the probe used to deliver ultrasound is kept in close contact with the wound bed (Sonoca-185, Söring) and has a built in lavage system which may aid in the reduction of cell debris and bacteria. The Sonoca device has sterile hand pieces. Using contact ultrasound can have good results; it is immediate, can be used for excisional debridement, is bactericidal at the surface of the wound, and can be used in a variety of settings by trained personnel. Limitations include lack of or cost of equipment, and trained personnel. Non-contact, non-thermal low frequency ultrasound (MIST Therapy System, Celleration) delivers ultrasound via an atomised saline solution to the wound bed, without direct contact of the device with the wound or the patient. Benefits are delivered by the effects of streaming and cavitation. It can be used to promote wound healing through cleansing and maintenance debridement through several sessions over time. Techniques are recommended by individual manufacturers of the device, but training must be undertaken. Aerosol contamination of the procedures means that clinicians and patients must wear appropriate infection control masks/gowns and the room be decontaminated according to local infection control policy. When the oscillating ultrasound waves are transmitted through the saline coupling fluid, thousands of micro-sized gas-filled bubbles or cavities are created, which are visible as a mist. As the tip is gently and continuously moved over the wound surface, the bubbles oscillate to create a shearing force against the tissue as the bubbles implode on contact (Tan, 2007). The gas bubbles test the strength of each cell, and because necrotic tissue has less tensile strength than healthy tissue, the cavitations separate the nonviable proteinaceous material from the wound base (Torke, 2004). In this way, low-frequency ultrasound distinguishes between necrotic and healthy tissue. Key points for ultrasound therapy include: 8 Becoming established in the UK, usually delivered by a competent practitioner with specialist training 8 Requires sterilised hand pieces and technology 8 Short treatment time, capable of removing most if not all devitalised tissue from the wound 8 Appears effective in all tissue types except dry eschar but most suited to superficial slough 8 Can be used in all clinical settings but manufacturers guidelines and infection control policies should be followed (aerosol contamination should be considered) 8 Costs associated with sterilising hand pieces and technology required should be considered. Hydrosurgical debridement This describes the removal of dead tissue using a high energy water beam. The device used to deliver hydrosurgery delivers a stream of saline via a handpiece at high energy, 82
7 turning the saline beam into a cutting implement. If the saline is held parallel to the wound, the cutting mechanism provides a highly controlled tangential excision, whereas if it is held in an oblique position, irrigation and tissue removal is accomplished. The pressure and velocity of the jet can be adapted to regulate debridement; the faster the water, the more effective the cutting technique (Weir et al, 2007). It is recommended that dry eschar is removed from wounds by sharp debridement before this method is used to remove remaining necrotic debris (Weir et al, 2007). Key points for hydrosurgical debridement include: 8 Established in the UK and usually delivered by a competent practitioner with relevant training 8 Can be used in all clinical settings but manufacturers guidelines and infection control policies should be followed (aerosol contamination should be considered) 8 Short treatment time, capable of removing most if not all devitalised tissue from the wound 8 Appears effective in all tissue types except dry eschar 8 Costs associated with disposable hand pieces and technology required should be considered. Sharp debridement Sharp debridement, also known as conservative sharp debridement, refers to the removal of dead or devitalised tissue from healthy tissue using a scalpel, scissors and forceps. It is selective, but does not result in total debridement. While surgeons may debride until the wound bed is bleeding, sharp debridement has a more conservative approach, removing dead tissue to just above the viable tissue level (Fairbairn et al, 2002). This conservative approach is quick and effective, minimises the risk of complications and is considered safe for a wider range of practitioners to undertake in a variety of settings, following training (Preece, 2003). However, some practitioners such as podiatrists may debride to a bleeding wound bed. More than one session may be required. Clinicians must be able to distinguish tissue types and understand the anatomy of the area being debrided (Ayello et al, 2004), since the procedure carries the risk of blood vessels, nerves and tendons being hidden by slough (Tong, 1999). Wound debridement can play a key role in the promotion of healing, reducing the risk of infection and/or improving patient quality of life. Sharp debridement is usually undertaken by a doctor with surgical skills, a podiatrist or a competent practitioner with specialist training (Raymundo and Wells, 2000) and can be carried out at the bedside or in a procedure room (Leaper, 2002). It should be performed in an environment that is equipped to deal with any complications that may arise and by a practitioner who is able to deal with them. It is a quick method of debridement which offers instant results. Limitations include access to a competent clinician, e.g. if the patient is cared for in a nursing home. It is also not appropriate for certain patient types. Initial debridement may need followup treatments, or may be used in conjunction with other debridement techniques such as autolysis (Edwards, 2000). Repeated minor tissue sparing debridement may be required (Leaper, 2002). There are variations in technique depending on the site and presentation of non-viable tissue, e.g. in a deep cavity wound. Sharp debridement in a patient with diabetic foot ulcers is a complex but essential undertaking and should involve a multidisciplinary team approach. Diabetes is associated with small and large blood vessel disease and increased risk of infection and poor healing. There may be underlying neuropathy. Patients therefore need careful assessment and control of their diabetes and infection (Leaper, 2002). Key points for sharp debridement include: 8 Requires a competent practitioner with specialist training 8 Requires effective instruments 8 May require eschar to be softened beforehand 8 Short treatment time, as can be performed in the patient s home, clinic or at the bedside 8 Can debulk devitalised tissue in a wound and has a faster treatment time than autolytic debridement 8 Costs associated with instruments and staff time need to be considered. Surgical debridement Surgical debridement describes the excision or wider resection of necrotic tissue, including the removal of healthy tissue from the wound margins (Fairbairn et al, 2002). It is an effective method, as it quickly cuts away debris in a selective manner, enabling the clinician performing the procedure to have complete control over which tissue is removed and which is left behind (Preece, 2003). It is best used on large areas, or in cases of contaminated tissue or sepsis where rapid removal is required. It needs to be undertaken by surgeons or practitioners with surgical training and requires theatre space thus incurring associated costs. Being an invasive procedure, anaesthesia is usually needed which may be contraindicated in some patients, and also brings with it associated risks. It can be a painful and extensive procedure. Key points for surgical debridement include: 8 Performed by a surgeon or competent practitioner with surgical training 8 Requires surgical environment 8 Quick treatment time 8 Technique involves removing nonviable tissue down to and including viable tissue 8 Costs associated with theatre time, 83
8 instruments and staff need to be considered. Discussion Wound debridement can play a key role in the promotion of healing, reducing the risk of infection and/or improving patient quality of life. Given its potentially important role in wound management, it is vital that each and every patient has access to the most appropriate method. There may be a need to use more than one method at different stages in the wound management process. This paper has considered a number of different debridement methods available in the UK. While there is a lack of empirical evidence to support the efficacy of these methods, as with many aspects of wound management, that should not detract from their potential to improve the lives of patients with wounds. The link between the presence of devitalised tissue in the wound bed and the risk of infection is clear (Ayello et al, 2004). In the majority of cases, the removal of devitalised tissue will increase the chances of healing and reduce the risk of wound infection. However, it is important that each patient is considered and assessed individually, and that the method(s) of debridement selected are chosen on the basis of patient need, not practitioner skill. Conclusion The decision of whether or not to debride a wound should be based upon thorough patient assessment and formulation of a relevant treatment plan. Given the potential benefits of debridement for faster healing and reduced infection rates, both the generalist and specialist alike have a responsibility to ensure that the most effective method of debridement is made available to the patient. This may require referral to a colleague, or continued professional development (CPD) to acquire the necessary skills and competencies for the client base concerned. Wuk References Ayello AE, Baranoski S, Kerstein MD, Cuddington I (2004) Wound debridement. In: Wound Care Essentials: Practice Principals. Lippincott, Williams and Wilkins, Springhouse, Pennsylvania Best Practice Statement: Optimising wound care. Wounds UK, Aberdeen. Available online at: id=141&articleid=8950&page=1 Best Practice Statement: The use of topical antiseptic/antimicrobial agents in wound management. Wounds UK, Aberdeen. Available online at: article.php?contentid=141&articleid=9627 &page=1 Dolynchuk K (2001) Debridement. In: Chronic Wound Care: A Clinical Source Book for Healthcare professionals. 3rd edn. HMP Communications, Philadelphia Edwards J (2000) Sharp debridement of wounds. J Comm Nurs 14: 1 European Wound Management Association (2006) Position Document: Identifying criteria for wound infection. MEP, London Fairbairn K, Grier J, Hunter C, Preece J (2002) A sharp debridement procedure devised by specialist nurses. J Wound Care 11(10): Falanga V (2001) Introducing the concept of wound bed preparation. Int Forum Wound Care 16(1): 1 4 Flanagan M (1999) Editorial. Reviewing the case for debridement. J Wound Care 8(6): 267 Gray D, White R, Cooper P, Kingsley A (2006) Applied wound management. In: Essential wound management: an introduction for undergraduates. Wounds UK, Aberdeen: Kubo M, Van der Water L, Plantefaber LC, et al (2001) Fibrinogen and fibrin are antiadhesive for keratinocytes: a mechanism for fibrin eschar and slough during wound repair. J Invest Dermatol 117(6): Leaper D (2002) Surgical debridement. Worldwidewounds.com. Available online at: december/leaper/sharp-debridement.html Nursing and Midwifery Council (2008) Professional Code of Conduct. NMC, London O Brien M (2002) Exploring methods of wound debridement. Br J Comm Nurs 10(12): 14 Preece J (2003) Sharp debridement: the need for training and education. Nurs Standard 99(25): 54 Raymundo J, Wells J (2000) Wound debridement. In: Bryant RA (ed) Acute and chronic wounds: nursing management. Mosby, St Louis Reid J, Morison M (1994) Towards a consensus: classification of pressure sores. J Wound Care 3: Key points 8 Wound debridement can lead to faster healing, reduced risk of infection and improved quality of life. 8 The decision of whether or not to debride should be based on thorough assessment. 8 Patients should receive the debridement method which meets their clinical needs. Sherman RA (1998) Maggot debridement in modern medicine. Infect Med 15(9): Steed DL, Donohoe D, Webster MW, Lindsley L (1996) Effect of extensive debridement and treatment on the healing of diabetic foot ulcers. Diabetic Ulcer Study Group. J Am Coll Surg 183(1): 61 4 Tan J, Abisis S, Smith A, Burnand KG (2007) A painless method of ultrasonically assisted debridement of chronic leg ulcers: a pilot study. Eur J Vasc Endovasc Surg 33: Tong A (1999) The identification and treatment of slough. J Wound Care 8(7): Torke K (2004) Healing wounds through ultrasound. Podiatry Management Nov/Dec: Vowden K, Vowden P (1999a) Wound debridement Part 1: non-sharp techniques. J Wound Care 8(5): Vowden K, Vowden P (1999b) Wound debridement part 2: sharp techniques. J Wound Care 8(6): Weir D, Scarborough P, Niezgoda JA (2007) Wound debridement. In: Krasner DL, Rodeheaver GT, Sibbald RG, eds. Chronic Wound Care: A Clinical Source Book for Healthcare professionals. 4th edn. HMP Communications, Malvern: Wolcott RD, Kennedy JP, Dowd SE (2009) Regular debridement is the main tool for maintaining a healthy wound bed in most chronic wounds. J Wound Care 18(2): 54 6 World Union of Wound Healing Societies (2008) Principles of best practice: Wound infection in clinical practice. An international consensus. MEP, London 84
The word debridement derives from the
 Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Debridement: treatment, options and selection.
 This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
EFFECTIVE DEBRIDEMENT IN A CHANGING NHS A UK consensus
 GUIDELINES FOR PRACTICE EFFECTIVE DEBRIDEMENT IN A CHANGING NHS A UK consensus Wounds UK EDITOR: Rita Som PUBLISHER: Kathy Day PUBLISHED BY: Wounds UK Enterprise House 1 2 Hatfields London SE1 9PG, UK
GUIDELINES FOR PRACTICE EFFECTIVE DEBRIDEMENT IN A CHANGING NHS A UK consensus Wounds UK EDITOR: Rita Som PUBLISHER: Kathy Day PUBLISHED BY: Wounds UK Enterprise House 1 2 Hatfields London SE1 9PG, UK
Wound debridement: guidelines and practice to remove barriers to healing
 Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Debridement Another Tool for Your Box! Foot Health Day 2 Kettering Wednesday 11 th June 2014
 Debridement Another Tool for Your Box! Foot Health Day 2 Kettering Wednesday 11 th June 2014 Sue Simm Regional Woundcare Specialist Activa Healthcare Best practice Debridement Debridement is a natural
Debridement Another Tool for Your Box! Foot Health Day 2 Kettering Wednesday 11 th June 2014 Sue Simm Regional Woundcare Specialist Activa Healthcare Best practice Debridement Debridement is a natural
Appropriate targeted foot care of
 Understanding the role of a monofilament fibre debridement pad in the management of diabetic foot ulcers Paul Chadwick, Andrew Findlow A diabetic foot ulcer (DFU) is a pivotal event for a person with diabetes,
Understanding the role of a monofilament fibre debridement pad in the management of diabetic foot ulcers Paul Chadwick, Andrew Findlow A diabetic foot ulcer (DFU) is a pivotal event for a person with diabetes,
CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS)
 CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS) Introduction The use of maggots for wound debridement has a long history and the introduction of sterile maggots specifically bred for wound management
CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS) Introduction The use of maggots for wound debridement has a long history and the introduction of sterile maggots specifically bred for wound management
Disclosures for Tarik Alam. Wound Bed Preparation. Wound Prognosis. Session Objectives. Debridement 4/26/2015
 Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Topical antimicrobials (antiseptics) Iodine, Silver, Honey
 Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Understanding Debridement
 Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Haycocks and Chadwick (2012)
 SAFE DEBRIDEMENT IN THE COMMUNITY SETTING It is widely accepted that wound debridement is necessary for optimal wound healing Debridement has become an accepted part of wound bed preparation with the ultimate
SAFE DEBRIDEMENT IN THE COMMUNITY SETTING It is widely accepted that wound debridement is necessary for optimal wound healing Debridement has become an accepted part of wound bed preparation with the ultimate
Debridement masterclass <KOL>
 Debridement masterclass The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee
Debridement masterclass The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee
DRESSING SELECTION SIMPLIFIED
 10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Fundamentals Of Wound Management. Julie Hewish Senior Tissue Viability Nurse
 Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Understanding Debridement of Sores
 Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement of Sores
 Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
I ve a drawer full of dressings i don t know how to use!
 I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
The Triangle of Wound Assessment
 The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
DEBRIDEMENT. In This Chapter. Chapter 8. Necrotic Tissue Eschar Slough Types of Debridement When Not to Debride...
 Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
This article is based on a symposium held
 Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
Pressure Ulcer Prevention Guidelines
 EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Wound Healing Community Outreach Service
 Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Larval debridement therapy (LDT)
 Meeting report Appropriate use of larval debridement therapy in diabetic foot management: consensus recommendations Paul Chadwick, Joanne McCardle, Elaine Ricci, Duncan Stang, Stella Vig Recent evidence
Meeting report Appropriate use of larval debridement therapy in diabetic foot management: consensus recommendations Paul Chadwick, Joanne McCardle, Elaine Ricci, Duncan Stang, Stella Vig Recent evidence
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
DEBRIDEMENT. Four Methods of Debridement
 Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
Many patients with chronic wounds. Case reports. The use of Prontosan in combination with Askina Calgitrol : an independent case series
 Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Medical technology guidance
 NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
Wound bed preparation: TIME in practice
 Wound bed preparation: TIME in practice Wound bed preparation is now a well established concept and the TIME framework has been developed as a practical tool to assist practitioners when assessing and
Wound bed preparation: TIME in practice Wound bed preparation is now a well established concept and the TIME framework has been developed as a practical tool to assist practitioners when assessing and
Exudate in the early stages of wound healing
 Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
The VERSAJET II Hydrosurgery System
 Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Prontosan. Clean. Easy Wound Healing. Wound Cleansing
 Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude
 Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Thorough and selective. Ultrasonic-Assisted Wound Debridement (UAW).
 Wound Thorough and selective. Ultrasonic-Assisted Wound Debridement (UAW). www.soering.com For chronic and acute wounds: disrupting of biofilms and effective removal of non-viable tissue UAW is a recognized
Wound Thorough and selective. Ultrasonic-Assisted Wound Debridement (UAW). www.soering.com For chronic and acute wounds: disrupting of biofilms and effective removal of non-viable tissue UAW is a recognized
Emil Schmidt Wound Care specialist SDHB - Otago
 Prospective randomised trial of low frequency ultrasound debridement (LFUD) in management of lower limb wounds Krysa J, Schmidt E, Thomson I, van Rij A Emil Schmidt Wound Care specialist SDHB - Otago Background
Prospective randomised trial of low frequency ultrasound debridement (LFUD) in management of lower limb wounds Krysa J, Schmidt E, Thomson I, van Rij A Emil Schmidt Wound Care specialist SDHB - Otago Background
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
TRUST-WIDE CLINICAL POLICY DOCUMENT WOUND DEBRIDEMENT. Policy Number: 122
 TRUST-WIDE CLINICAL POLICY DOCUMENT WOUND DEBRIDEMENT Policy Number: 122 Scope of this Document: Recommending Committee: Approving Committee: To be applied by all Healthcare professionals within Mersey
TRUST-WIDE CLINICAL POLICY DOCUMENT WOUND DEBRIDEMENT Policy Number: 122 Scope of this Document: Recommending Committee: Approving Committee: To be applied by all Healthcare professionals within Mersey
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
TIME CONCEPT AND LOCAL WOUND MANAGEMENT
 TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
Galen ( A.D) Advanced Wound Dressing
 Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
WHY WOUNDS FAIL TO HEAL SIMPLIFIED
 WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
Clinical Policy Title: Debridement of diabetic foot ulcers
 Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
Haemoglobin. Granulox: TOPICAL HAEMOGLOBIN
 QUICK GUIDE Haemoglobin Granulox: TOPICAL HAEMOGLOBIN OXYGEN AND WOUND HEALING 1 Oxygen is needed at all phases of wound healing Insufficient wound tissue oxygenation is a major risk factor for delayed
QUICK GUIDE Haemoglobin Granulox: TOPICAL HAEMOGLOBIN OXYGEN AND WOUND HEALING 1 Oxygen is needed at all phases of wound healing Insufficient wound tissue oxygenation is a major risk factor for delayed
Protocol for the Use of Sterile Larvae in Wound Management
 Protocol for the Use of Sterile Larvae in Wound Management Approved by: CHS Clinical Policy Group and Clinical Quality and Governance Committee On: 10 August 2009 Review Date: 31 July 2011 Directorate
Protocol for the Use of Sterile Larvae in Wound Management Approved by: CHS Clinical Policy Group and Clinical Quality and Governance Committee On: 10 August 2009 Review Date: 31 July 2011 Directorate
Essity Internal. Taking the fear out of wound infection: conquering everyday issues
 Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
The Proven Multifunctional Dressing
 The Proven Multifunctional Dressing belongs to an innovative class of multifunctional wound care dressings. dressings effectively cleanse, fill, absorb and moisten wounds throughout the healing continuum.
The Proven Multifunctional Dressing belongs to an innovative class of multifunctional wound care dressings. dressings effectively cleanse, fill, absorb and moisten wounds throughout the healing continuum.
AWMA MODULE ACCREDITATION. Module Seven: Conservative Sharp Wound Debridement
 AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
In line with the professional requirements of the Nursing and Midwifery Council
 STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
Wound culture. (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center
 Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management
 An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE
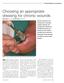 Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
PRESSURE ULCERS SIMPLIFIED
 10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Use of an outside force to remove nonviable. Wound Debridement Guide South West Regional Wound Care Program Last Updated March 12,
 Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
ACOFP 55th Annual Convention & Scientific Seminars. New Physicians and Residents: Introduction to Wound Care. Katherine Lincoln, DO, FAAFP
 8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
Ray Norris, Rachel Henchy
 Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Resources to Guide the Management of Suspected Infection in Chronic Wounds
 Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
easy made Triangle of Wound Assessment
 Triangle of Wound made easy Wounds Asia May 2015 www.woundsasia.com Introduction Wound assessment is essential in informing the selection of appropriate therapeutic strategies to achieve clinical goals,
Triangle of Wound made easy Wounds Asia May 2015 www.woundsasia.com Introduction Wound assessment is essential in informing the selection of appropriate therapeutic strategies to achieve clinical goals,
Managing Wounds. Esther White Tissue Viability Nurse
 Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
INVESTIGATING: WOUND INFECTION
 INVESTIGATING: WOUND INFECTION Diagnosing infection in surgical and other wounds involves nurses being able to observe the clinical signs in a wound rather than simply obtaining positive microbiology results
INVESTIGATING: WOUND INFECTION Diagnosing infection in surgical and other wounds involves nurses being able to observe the clinical signs in a wound rather than simply obtaining positive microbiology results
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Vacuumed Assisted Closure
 Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
Wound assessment is a
 Wound assessment part 2: exudate Wound exudate provides the moist environment required for cell regeneration. However, in chronic wounds exudate can become excessive and prevent healing. Changes in the
Wound assessment part 2: exudate Wound exudate provides the moist environment required for cell regeneration. However, in chronic wounds exudate can become excessive and prevent healing. Changes in the
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
John Timmons, David Gray, Fiona Russell
 Silflex soft silicone wound contact dressing It is hard to believe that it has taken so long for the message to get through, that dressings and dressing removal should not cause additional pain or trauma
Silflex soft silicone wound contact dressing It is hard to believe that it has taken so long for the message to get through, that dressings and dressing removal should not cause additional pain or trauma
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine
 Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
CASE 1: TYPE-II DIABETIC FOOT ULCER
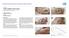 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009)
 Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009) This guidance should be read in conjunction with your local dressing formulary and anti-biotic prescribing guidelines.
Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009) This guidance should be read in conjunction with your local dressing formulary and anti-biotic prescribing guidelines.
Multiple Interventions for Diabetic Foot Ulcer Treatment Trial (MIDFUT)
 Multiple Interventions for Diabetic Foot Ulcer Treatment Trial (MIDFUT) Nikki Dewhirst MIDFUT Clinical Co-ordinator, Clinical Trials Research Unit, University of Leeds Senior Vascular Research Nurse, Leeds
Multiple Interventions for Diabetic Foot Ulcer Treatment Trial (MIDFUT) Nikki Dewhirst MIDFUT Clinical Co-ordinator, Clinical Trials Research Unit, University of Leeds Senior Vascular Research Nurse, Leeds
EWMA Educational Development Programme. Curriculum Development Project. Education Module. Wound Infection
 EWMA Educational Development Programme Curriculum Development Project Education Module Wound Infection Latest revision: February 2014 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME The Programme is designed
EWMA Educational Development Programme Curriculum Development Project Education Module Wound Infection Latest revision: February 2014 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME The Programme is designed
Larval Debridement Therapy Making healing possible
 Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Palliative Care. EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for. Treatment. Improving Quality of Care Based on CMS Guidelines 39
 Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
The challenge for nurses lies in. Controlling exudate and promoting healing of a chronic wound
 Product FOCUS KEY WORDS Diabetic feet Type 2 diabetes Chronic wounds Dressing selection Benbow M (2011) Dressing awkward wounds. J Comm Nurs 25(6) Clayton W, Elasy TA (2009) A review of the pathophysiology,
Product FOCUS KEY WORDS Diabetic feet Type 2 diabetes Chronic wounds Dressing selection Benbow M (2011) Dressing awkward wounds. J Comm Nurs 25(6) Clayton W, Elasy TA (2009) A review of the pathophysiology,
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4
 A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4 Gill Wicks, Nurse Consultant, Tissue Viability for Wiltshire Primary Care Trust and Lecturer at University of West England Pressure ulcers
A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4 Gill Wicks, Nurse Consultant, Tissue Viability for Wiltshire Primary Care Trust and Lecturer at University of West England Pressure ulcers
Currently, the NHS is facing the challenge of
 Evaluation of a superabsorbent dressing in a primary care organization Jackie Stephen-Haynes and Claire Stephens Jackie Stephen-Haynes is Professor and Nurse Consultant, Practice Development Unit, Birmingham
Evaluation of a superabsorbent dressing in a primary care organization Jackie Stephen-Haynes and Claire Stephens Jackie Stephen-Haynes is Professor and Nurse Consultant, Practice Development Unit, Birmingham
Oxygen is required for normal cellular
 Article The role of topical oxygen therapy in the management of diabetic foot ulcer s in Scotland: round table recommendations Citation: Stang D, Young M, Wilson D et al (18) The role of topical oxygen
Article The role of topical oxygen therapy in the management of diabetic foot ulcer s in Scotland: round table recommendations Citation: Stang D, Young M, Wilson D et al (18) The role of topical oxygen
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell
 Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Healthcare Improvement Scotland
 Article Relevance of a Health Technology Assessment report: antimicrobial wound dressings for diabetic foot chronic wounds with local infection Lynne Watret, Alison Rodgers, Karen Macpherson, Susan Myles,
Article Relevance of a Health Technology Assessment report: antimicrobial wound dressings for diabetic foot chronic wounds with local infection Lynne Watret, Alison Rodgers, Karen Macpherson, Susan Myles,
Understanding the importance of holistic wound assessment
 Understanding the importance of holistic wound assessment It is important to undertake a holistic assessment of the patient who presents with a wound. Karen Ousey and Leanne Cook give an overview of the
Understanding the importance of holistic wound assessment It is important to undertake a holistic assessment of the patient who presents with a wound. Karen Ousey and Leanne Cook give an overview of the
The concept of self-care is becoming more. Topical oxygen-haemoglobin use on sloughy wounds: positive patient outcomes and the promotion of self-care
 Topical oxygen-haemoglobin use on sloughy wounds: positive patient outcomes and the promotion of self-care KEY WORDS Haemoglobin spray Healing, slow healing and non-healing wounds Self-care Slough Topical
Topical oxygen-haemoglobin use on sloughy wounds: positive patient outcomes and the promotion of self-care KEY WORDS Haemoglobin spray Healing, slow healing and non-healing wounds Self-care Slough Topical
Tissue Viability. Autolysis: mechanisms of action in the removal of devitalised tissue. November In association with
 November 2016 In association with Tissue Viability Autolysis: mechanisms of action in the removal of devitalised tissue Leanne Atkin, Vascular Nurse Specialist/Lecturer Practitioner, Mid Yorks NHS Trust/University
November 2016 In association with Tissue Viability Autolysis: mechanisms of action in the removal of devitalised tissue Leanne Atkin, Vascular Nurse Specialist/Lecturer Practitioner, Mid Yorks NHS Trust/University
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
