Debridement masterclass <KOL>
|
|
|
- Lisa Stafford
- 5 years ago
- Views:
Transcription
1 Debridement masterclass <KOL> The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or reliability of the information contained in this presentation. Responsibility for obtaining permission to use images contained in this presentation is that of the presenter, not of Smith & Nephew.
2 Wound debridement Definitions Why debride? Types of debridement Your role in debridement
3 Access to debridement should be based on clinical need and not the skill of the clinician (sic) (Gray et al, 2011)
4 Definition debridement Taken from the French débridement, or débrider to remove adhesions. Collins, Hampton & White (2002) From the French desbrider, meaning to unbridle. Leaper (2002) Debridement is the removal of devitalised or infected tissue, fibrin, or foreign material from a wound. NICE (2001) Debridement is the removal of dead, non viable/devitalised tissue, infected or foreign material from the wound bed and surrounding skin. Wounds UK (2013)
5 Definition slough A mixture of dead white cells, dead bacteria, rehydrated necrotic tissue and fibrous tissue. Can be soft" slough and easily cleaned away, or fibrous slough which can resist even sharp debridement Collins, Hampton & White (2002)
6 Definition necrosis Death in a tissue or organ, which occurs in response to injury, disease or occlusion of blood flow. Continuity with neighbouring viable tissue is preserved. Can arise through infection, trauma such as pressure, and, localised ischaemia.the death of tissue, may appear blue black, grey, yellow and sloughy, often very painful, may have a halo of inflammation. Collins, Hampton & White (2002)
7 Why debride? Quicker healing Reduces risk of infection Dead tissue inhibits cell activity Dead tissue acts as physical barrier to epithelialisation Dead tissue can be malodorous Ongoing inflammation conversion of chronic into acute wound To aid full assessment Psychological stress Nutritional loss through exudate
8 Why don t we debride? Inability to access certain methods of debridement/services Inability to consult with the MDT Lack of knowledge around debridement Unclear referral pathways Funding issues/lack of access to services
9 Consider Type of wound to be debrided N.B. malignant wounds State of wound to be debrided Pain related to wound involved Past therapies/treatments Age of wound Exudate levels may increase in short term depending on technique used (e.g. larvae) Presence of infection in wound to be debrided and potential consequences Acceptability to patient of debridement method Combination of debridement methods?
10 Consider Define an aim E.g. does the wound need cleaning prior to grafting? Define a timescale How quickly does debridement need to happen? Define a method
11 Types of debridement Surgical Conservative sharp debridement Mechanical debridement Wet to dry dressings Monofilament soft pad High pressure fluid irrigation/hydrosurgical Enzymatic debridement Larval /biosurgical therapy Ultrasonic Autolytic debridement
12 How to choose method Wound characteristics Infection Pain Exudate Involved tissues Required rate of debridement The patient Available skills Available resources Products Costs
13 And assess/evaluate Amount of necrotic tissue should diminish/change if therapy appropriate Change in type of tissue in wound bed Dry, desiccated eschar soggy, so slough mucinous, easily dislodged tissue Brown/black yellow/tan Percentage of tissue types in wound bed Photography Linear measurement
14 Checklist for debridement decisions (adapted from Wounds UK, 2013) The aim/goal for the wound Is debridement appropriate for this wound? NO KEEP DRY Should I take a conservative approach (stabilise the wound)? YES AUTOLYTICALLY DEBRIDE Do I need to change method of debridement? YES CONSIDER OTHER METHODS Should I actively try to accelerate the wound healing process? YES ACCELERATE DEBRIDEMENT Is non viable tissue delaying healing? Does the wound edge/periwound skin or wound bed require accelerated debridement? Is acceleration of debridement going to help the management of infection in this wound? Is acceleration of debridement in the best interests of the patient at the moment? Am I certain what to do? NO CONSULT MULTIDISCIPLINARY TEAM, DO NOT DEBRIDE Accelerate healing through debridement Have I discussed the debridement options with the patient/family members? Do I have the skills to perform the chosen method of debridement myself? Am I confident in what I am doing? NO REFER Can I make things worse/do harm? YES REFER Is the current environment safe to undertake debridement? YES DEBRIDE Have I got the resources/equipment necessary? YES DEBRIDE NO REFER or PLAN RESOURCES Expected outcome of debridement Will the intervention remove non viable tissue in one go? Will it be a gradual/staged process? Will the debrided wound be ready for another therapy, e.g. negative pressure wound therapy, skin grafting? YES SET DATE FOR REVIEW Options at every stage Check clinical guidelines/policies Seek advice from a specialist or colleagues in the MDT (as simple as making a call) Refer to another practitioner for debridement Debride wound, selecting the most appropriate method based on wound and patient need, speed with which debridement is necessary and patient preference
15 Types of debridement Surgical Conservative sharp debridement Mechanical debridement Wet to dry dressings Monofilament soft pad High pressure fluid irrigation/hydrosurgical Enzymatic debridement Larval/biosurgical therapy Ultrasonic Autolytic debridement
16 Surgical debridement excision of necrotic material up to and including viable tissue margins Vowden & Vowden (1999)
17 Surgical debridement Often carried out under anaesthetic in theatre Fastest way of debridement especially for large areas Can be aggressive & extensive Not appropriate for all Resources
18 Conservative sharp debridement Carried out in stages removing layers of necrotic tissues Available equipment Patient environment surface, lighting BUT N.B. clotting disorders, malignant wounds, Achilles N.B. pain N.B training and level of competence
19 Competence A good knowledge of relevant anatomy Ability to identify viable tissue Access to adequate equipment, lighting, assistance Ability to explain procedure & obtain informed consent Ability to manage pain and discomfort before, during and after procedure Ability to deal with complications, such as bleeding Ability to recognise his/her skill limitations and those of techniques used Ability to plan secondary debridement techniques if necessary Ability to recognise when not to undertake a technique and when to refer patient to another member of MDT Refer to local guidance/policy/protocol/professional code
20 Mechanical debridement Wet to dry dressings Monofilament soft pad High pressure fluid irrigation/hydrosurgical Enzymatic debridement Larval/biosurgical therapy Ultrasonic
21 Mechanical debridement : wet to dry dressings Used in USA Saline soaked gauze Removed when dries Mechanical removal of slough/necrosis Painful!!! Often standard treatment in studies!!!!!
22 Mechanical debridement: Debrisoft Monofilament soft pad Soft polyester fibres Gentle removal of devitalised tissue, debris and hyperkeratosis
23 Mechanical debridement: Debrisoft The Debrisoft monofilament debridement pad for use in acute or chronic wounds Medical technologies guidance [MTG17] Published date: March 2014
24 Mechanical debridement: Debrisoft Advantages Selective, quick and easy Can remove hyperkeratosis Causes little pain Can be used before or after other methods Can be used in any care environment Patient can use product with education and instruction Disadvantages Cannot be used on hard, dry eschar Do not use on painful wounds
25 Mechanical debridement high pressure fluid irrigation Fast moving water in bath whirlpool VERSAJET TM Jet acts as scalpel Target precisely Vacuum created & sucks up debris Venturi effect Environment clinic v theatre
26 Mechanical debridement high pressure fluid irrigation Advantages Selectively removes necrotic/devitalised tissue, while sparing healthy tissue (Matsumura et al) Shown to reduce debridement time by about 50% when compared to conventional sharp debridement (McAleer et al) VERSAJET TM can reduce the average time to achieve complete chronic ulcer debridement (Mosti et al) Has demonstrated a reduction in bacterial load in the wound following debridement (Mosti et al) Disadvantages Requires specialist training Not widely available Initial cost Matsumura, H. et al. The Estimation of Tissue Loss During Tangential Hydrosurgical Debridement. Ann. Plast. Surg. 69, (2012). McAleer, JP et al. A Prospective Randomized Study Evaluating the Time Efficiency of the VERSAJET Hydrosurgery System and Traditional Wound Debridement, 2005, Presented at ACFAS Conference. Data on File. Mosti G et al. The Debridement of Chronic Leg Ulcers by Means of a New, Fluidjet Based Device. Wounds, 2006, 18,
27 Mechanical debridement enzymatic debridement Varidase Topical Papain papaya Collagenase Antarctic krill Burning sensation Skin erythema Use at least once daily Labour intensive/resource heavy Reaction with thrombolytic agents (Varidase) All Trademarks acknowledged
28 Mechanical debridement larval/biosurgical therapy Larvae of Lucilia sericata common greenbottle Loose or bagged dressing Feed on necrotic tissue Role in removing bacteria Acute & chronic wounds Patient acceptance? Peri wound prep Cost versus speed
29 Mechanical debridement larval/biosurgical therapy Advantages Selective Quick debridement Can be used on infected wounds Minimal training required Cost effective compared with standard treatment Disadvantages Will not remove callus (NB neuropathic diabetic foot ulcers) Patient acceptance Plan in advance Not suitable for dry eschar Use with caution in highly exuding wounds, wounds requiring occlusion, patients with clotting issues, malignancies, close to large vessels
30 Ultrasonic debridement Ultrasound delivered direct to wound bed or via atomised solution Low frequency ultrasound provides a gentle maintenance debridement
31 Ultrasonic debridement MIST Therapy The MIST Therapy system for the promotion of wound healing Medical technologies guidance [MTG5] Published date: July 2011
32 Ultrasonic debridement Advantages Selective and immediate Can be used for excisional debridement Can be used for maintenance debridement Has some antimicrobial activity Does not require specialist training if low frequency Disadvantages High cost Set up time consuming as well as decontamination following procedure High frequency ultrasound requires specialist training Contraindicated in vascular abnormalities, haemorrhagic conditions, malignancies, tissue previously treated with radiation, deep x ray or irradiation
33 Autolytic debridement Wound macrophages produce collagenase & proteases Split & breakdown proteins which hold eschar on the wound When proteins broken down, become detached and debridement occurs Process also stimulates neutrophils which increase debridement process Called autolytic debridement Is a natural process relies on warm, moist environment Dressings key role in creating & sustaining environment Stimulation enzymatic activity has potential to affect all tissue important to protect peri wound skin from moisture
34 Autolytic debridement Advantages Can be used before or between other methods of debridement Can be used on painful wounds Can be used in any care environment No special skills required Disadvantages Slow method of debridement Can cause peri wound maceration Can increase risk of infection May require frequent dressing changes
35 Autolytic debridement dressings Promote wound moisture: Hydrogels Films Hydrocolloids Maintain moist wound bed/absorption: Foam Alginate Hydrofiber Rehydrate necrotic tissue Use on wet, sloughy tissue Cadexomer iodine dressings
36 Autolytic/chemical debridement honey Autolytic effect Honey facilitates proteases proteases in extra fluid honey draws from wound tissue (osmotic effect) Proteases break down slough/necrosis Protease activity enhanced as hydrogen peroxide inactivates inhibitors of proteases
37
38 When not to debride Dry necrosis or gangrene without infection in the ischaemic diabetic foot Inadequate blood supply Terminally ill N.B. In some cases debridement may be appropriate but location of wound requires specialist input
39 Think about referring on No wound improvement over several weeks Dry gangrene/dry ischaemia Evidence of cellulitis or gross infection/purulence Impending exposed tendon or bone Evidence of abscess or undermined areas What if wound resloughs?
40 Access to debridement should be based on clinical need and not the skill of the clinician (sic) (Gray et al, 2011)
41
42 Any questions?
43 References Anderson, I. (2006) Debridement methods in wound care. Nursing Standard 20, Collons,F, Hampton, S. & White, R. (2002) A Z Dictionary of Wound Care. Quay Books, London Gray, D., Acton, D, Chadwick, P. et al (2011) Consensus guidance for the use of debridement techniques in the UK. Wounds UK 10, Houghton, D. (2015) Using newly acquired skills to debride a heel ulcer: a reflective account. Wounds Essentials 10, Leaper, D. (2002) Sharp technique for wound debridement. Available at: Debridement.html Lloyd Jones, M. (2015) Should necrotic wounds always be debrided? Wounds Essentials 10, National Institute for Health and Clinical Excellence (2014) The Debrisoft monofilament debridement pad for use in acute or chronic wounds. NICE, London Price, B. & Young, T. (2013) Debridement consensus: recommendations for practice. Wounds Essentials 8, Stephen Haynes, J. & Callaghan, R. (2012) A new debridement technique tested on pressure ulcers. Wounds UK 8,3 S6 S12 Young, T. (2012) Safe debridement in the community setting. Wounds Essentials Vol Wounds UK (2013) Effective debridement in a changing NHS: a UK consensus. London, Wounds UK ( uk.com) Wounds UK (2014) Quick Guide Debridement. London, Wounds UK TM Trademark of Smith & Nephew All Trademarks acknowledged June 2017 Fiona Kelly 09197
44 Smith & Nephew Croxley Park Building 5, Lakeside Hatters Lane, Watford Hertfordshire WD18 8YE T +44 (0) F +44 (0) nephew.com/uk Trademark of Smith & Nephew All Trademarks acknowledged June 2017 Smith & Nephew Supporting healthcare professionals for over 150 years
45 Questions
46 According to its most recent definition, debridement is 0 1 The removal of dead, non viable/devitalised tissue, infected or foreign material from the wound bed and surrounding skin 2 The removal of devitalised or infected tissue, fibrin, or foreign material from a wound 3 The medical removal of dead, damaged, or infected tissue to improve the healing potential of the remaining healthy tissue
47 According to its most recent definition, debridement is 1 The removal of dead, nonviable/devitalised tissue, infected or foreign material from the wound bed and surrounding skin 2 The removal of devitalised or infected tissue, fibrin, or foreign material from a wound 3 The medical removal of dead, damaged, or infected tissue to improve the healing potential of the remaining healthy tissue 0% 0% 0%
48 How would you describe slough? 0 1 A creamy, shiny, yellow/greyish substance containing bacteria 2 A mixture of dead white cells, dead bacteria, rehydrated necrotic tissue and fibrous tissue 3 A yellow, fibrinous tissue that consists of fibrin, pus, and proteinaceous material
49 How would you describe slough? 1 A creamy, shiny, yellow/greyish substance containing bacteria 0% 2 A mixture of dead white cells, dead bacteria, rehydrated necrotic tissue and fibrous tissue 0% 3 A yellow, fibrinous tissue that consists of fibrin, pus, and proteinaceous material 0%
50 What do you need to consider before debriding? 0 1 Define an aim, timescale and method 2 Establish a plan, assign roles and pick a debriding method 3 Assess the wound, define a method and select the correct dressing
51 What do you need to consider before debriding? 1 Define an aim, timescale and method 0% 2 Establish a plan, assign roles and pick a debriding method 0% 3 Assess the wound, define a method and select the correct dressing 0%
52 Which of the following methods of debridement are mistakenly thought to be the same? 0 1 Surgical and mechanical debridement 2 Mechanical and autolytic debridement 3 Sharp and surgical debridement
53 Which of the following methods of debridement are mistakenly thought to be the same? 1 Surgical and mechanical debridement 0% 2 Mechanical and autolytic debridement 0% 3 Sharp and surgical debridement 0%
54 In most cases, when should you avoid debriding? 0 1 When there is necrosis or gangrene 2 When there is an inadequate blood supply 3 When the patient cannot stand the pain
55 In most cases, when should you avoid debriding? 1 When there is necrosis or gangrene 0% 2 When there is an inadequate blood supply 0% 3 When the patient cannot stand the pain 0%
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Debridement: treatment, options and selection.
 This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
Wound debridement: guidelines and practice to remove barriers to healing
 Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Debridement Another Tool for Your Box! Foot Health Day 2 Kettering Wednesday 11 th June 2014
 Debridement Another Tool for Your Box! Foot Health Day 2 Kettering Wednesday 11 th June 2014 Sue Simm Regional Woundcare Specialist Activa Healthcare Best practice Debridement Debridement is a natural
Debridement Another Tool for Your Box! Foot Health Day 2 Kettering Wednesday 11 th June 2014 Sue Simm Regional Woundcare Specialist Activa Healthcare Best practice Debridement Debridement is a natural
The Triangle of Wound Assessment
 The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
Understanding Debridement
 Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
Medical technology guidance
 NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
I ve a drawer full of dressings i don t know how to use!
 I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
The word debridement derives from the
 Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Appropriate targeted foot care of
 Understanding the role of a monofilament fibre debridement pad in the management of diabetic foot ulcers Paul Chadwick, Andrew Findlow A diabetic foot ulcer (DFU) is a pivotal event for a person with diabetes,
Understanding the role of a monofilament fibre debridement pad in the management of diabetic foot ulcers Paul Chadwick, Andrew Findlow A diabetic foot ulcer (DFU) is a pivotal event for a person with diabetes,
DRESSING SELECTION SIMPLIFIED
 10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
Disclosures for Tarik Alam. Wound Bed Preparation. Wound Prognosis. Session Objectives. Debridement 4/26/2015
 Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
EFFECTIVE DEBRIDEMENT IN A CHANGING NHS A UK consensus
 GUIDELINES FOR PRACTICE EFFECTIVE DEBRIDEMENT IN A CHANGING NHS A UK consensus Wounds UK EDITOR: Rita Som PUBLISHER: Kathy Day PUBLISHED BY: Wounds UK Enterprise House 1 2 Hatfields London SE1 9PG, UK
GUIDELINES FOR PRACTICE EFFECTIVE DEBRIDEMENT IN A CHANGING NHS A UK consensus Wounds UK EDITOR: Rita Som PUBLISHER: Kathy Day PUBLISHED BY: Wounds UK Enterprise House 1 2 Hatfields London SE1 9PG, UK
WHY WOUNDS FAIL TO HEAL SIMPLIFIED
 WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
Fundamentals Of Wound Management. Julie Hewish Senior Tissue Viability Nurse
 Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
Understanding Debridement of Sores
 Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Topical antimicrobials (antiseptics) Iodine, Silver, Honey
 Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Understanding Debridement of Sores
 Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Understanding Debridement of Sores Introduction Some sores have trouble healing on their own. Sores that will not heal are also known as wounds or chronic wounds. A chronic wound is a sore that is having
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL. of the infection risk in chronic wound
 Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Assessing and managing pain <KOL>
 Assessing and managing pain The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee
Assessing and managing pain The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee
The VERSAJET II Hydrosurgery System
 Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
Managing Wounds. Esther White Tissue Viability Nurse
 Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
DEBRIDEMENT. Four Methods of Debridement
 Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
DEBRIDEMENT. In This Chapter. Chapter 8. Necrotic Tissue Eschar Slough Types of Debridement When Not to Debride...
 Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Use of an outside force to remove nonviable. Wound Debridement Guide South West Regional Wound Care Program Last Updated March 12,
 Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Consensus guidance for the use of debridement techniques in the UK
 Consensus guidance for the use of debridement techniques in the UK In Autumn 2010, a multidisciplinary group of clinicians met in Manchester to discuss the issue of debridement in wound management. There
Consensus guidance for the use of debridement techniques in the UK In Autumn 2010, a multidisciplinary group of clinicians met in Manchester to discuss the issue of debridement in wound management. There
Tissue Viability Service Wound Management Primary Care Formulary 2017
 Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
TIME CONCEPT AND LOCAL WOUND MANAGEMENT
 TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
PRESSURE ULCERS SIMPLIFIED
 10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
Haycocks and Chadwick (2012)
 SAFE DEBRIDEMENT IN THE COMMUNITY SETTING It is widely accepted that wound debridement is necessary for optimal wound healing Debridement has become an accepted part of wound bed preparation with the ultimate
SAFE DEBRIDEMENT IN THE COMMUNITY SETTING It is widely accepted that wound debridement is necessary for optimal wound healing Debridement has become an accepted part of wound bed preparation with the ultimate
RN Cathy Hammond. Specialist Wound Management Service at Nurse Maude Christchurch
 RN Cathy Hammond Specialist Wound Management Service at Nurse Maude Christchurch 14:00-14:55 WS #141: Wound Infection - What You Need to Know 15:05-16:00 WS #153: Wound Infection - What You Need to Know
RN Cathy Hammond Specialist Wound Management Service at Nurse Maude Christchurch 14:00-14:55 WS #141: Wound Infection - What You Need to Know 15:05-16:00 WS #153: Wound Infection - What You Need to Know
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Multiple Interventions for Diabetic Foot Ulcer Treatment Trial (MIDFUT)
 Multiple Interventions for Diabetic Foot Ulcer Treatment Trial (MIDFUT) Nikki Dewhirst MIDFUT Clinical Co-ordinator, Clinical Trials Research Unit, University of Leeds Senior Vascular Research Nurse, Leeds
Multiple Interventions for Diabetic Foot Ulcer Treatment Trial (MIDFUT) Nikki Dewhirst MIDFUT Clinical Co-ordinator, Clinical Trials Research Unit, University of Leeds Senior Vascular Research Nurse, Leeds
Workshop on Debridement
 MEDICINSK TEKNIK I SÅRDIAGNOSTIK OCH SÅRBEHANDLING Monday, 20 th of april 2015 Stockholm Sweden Workshop on Debridement Sources for best practice Reference documents available in several languages : WHY
MEDICINSK TEKNIK I SÅRDIAGNOSTIK OCH SÅRBEHANDLING Monday, 20 th of april 2015 Stockholm Sweden Workshop on Debridement Sources for best practice Reference documents available in several languages : WHY
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
o Venous edema o Stasis ulcers o Varicose veins (not including spider veins) o Lipodermatosclerosis
 Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Ray Norris, Rachel Henchy
 Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Tissue Viability Service Wound Management Primary Care Formulary 2017
 Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Precise excision. Preserve viable tissue and reduce time to closure (1,2)
 Precise excision Preserve viable tissue and reduce time to closure (1,2) Precision to preserve Conventional surgical excision Non-viable tissue VERSAJET II excision More precise tissue removal Non-viable
Precise excision Preserve viable tissue and reduce time to closure (1,2) Precision to preserve Conventional surgical excision Non-viable tissue VERSAJET II excision More precise tissue removal Non-viable
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
SDMA Categorisation of Wound Care and Associated Products
 Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell
 Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS)
 CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS) Introduction The use of maggots for wound debridement has a long history and the introduction of sterile maggots specifically bred for wound management
CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS) Introduction The use of maggots for wound debridement has a long history and the introduction of sterile maggots specifically bred for wound management
Resources to Guide the Management of Suspected Infection in Chronic Wounds
 Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Wound bed preparation: TIME in practice
 Wound bed preparation: TIME in practice Wound bed preparation is now a well established concept and the TIME framework has been developed as a practical tool to assist practitioners when assessing and
Wound bed preparation: TIME in practice Wound bed preparation is now a well established concept and the TIME framework has been developed as a practical tool to assist practitioners when assessing and
Mean percent reduction in ulcer area from baseline at six weeks 62 % SANTYL Ointment + supportive care* + sharp debridement 1 (P<0.
 Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
AWMA MODULE ACCREDITATION. Module Seven: Conservative Sharp Wound Debridement
 AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advancing the science of wound bed preparation
 Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Diabetic Foot Ulcers. A guide to help minimise pain, trauma and stress
 Diabetic Foot Ulcers A guide to help minimise pain, trauma and stress From day one, Safetac was about less pain to patients. It s an easy story it does not stick to the wound, so it does not damage or
Diabetic Foot Ulcers A guide to help minimise pain, trauma and stress From day one, Safetac was about less pain to patients. It s an easy story it does not stick to the wound, so it does not damage or
Welcome to NuMed! Our Commitment: Quality Products, Cost Savings, Exceptional Service
 It s a New Day in Wound Care Welcome to NuMed! Our Commitment: Quality Products, Cost Savings, Exceptional Service NuMed Industries is a manufacturing company that specializes in Advanced Wound Care products.
It s a New Day in Wound Care Welcome to NuMed! Our Commitment: Quality Products, Cost Savings, Exceptional Service NuMed Industries is a manufacturing company that specializes in Advanced Wound Care products.
TRUST-WIDE CLINICAL POLICY DOCUMENT WOUND DEBRIDEMENT. Policy Number: 122
 TRUST-WIDE CLINICAL POLICY DOCUMENT WOUND DEBRIDEMENT Policy Number: 122 Scope of this Document: Recommending Committee: Approving Committee: To be applied by all Healthcare professionals within Mersey
TRUST-WIDE CLINICAL POLICY DOCUMENT WOUND DEBRIDEMENT Policy Number: 122 Scope of this Document: Recommending Committee: Approving Committee: To be applied by all Healthcare professionals within Mersey
Wound Assessment & Treatment
 Wound Assessment & Treatment Cathy Lyle Advanced Practice Nurse Providence Care, SMOL site LTC Physicians CME June 2011 Outline l Is it healing? l Will it heal? l What colour is it? l How wet is it? l
Wound Assessment & Treatment Cathy Lyle Advanced Practice Nurse Providence Care, SMOL site LTC Physicians CME June 2011 Outline l Is it healing? l Will it heal? l What colour is it? l How wet is it? l
Clinical Policy Title: Debridement of diabetic foot ulcers
 Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
ACOFP 55th Annual Convention & Scientific Seminars. New Physicians and Residents: Introduction to Wound Care. Katherine Lincoln, DO, FAAFP
 8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
Slough is a complex, generally fibrinous,
 Article Management of slough in diabetic foot wounds Steve Young A common presentation of diabetic foot wounds is a chronic ulcer with a yellowcoloured, viscous adherent layer of debris. This yellow wound
Article Management of slough in diabetic foot wounds Steve Young A common presentation of diabetic foot wounds is a chronic ulcer with a yellowcoloured, viscous adherent layer of debris. This yellow wound
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Wound assessment is a
 Wound assessment part 2: exudate Wound exudate provides the moist environment required for cell regeneration. However, in chronic wounds exudate can become excessive and prevent healing. Changes in the
Wound assessment part 2: exudate Wound exudate provides the moist environment required for cell regeneration. However, in chronic wounds exudate can become excessive and prevent healing. Changes in the
Palliative Care. EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for. Treatment. Improving Quality of Care Based on CMS Guidelines 39
 Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers
 A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Healing: General Principles. Mansour Dib MD
 Wound Healing: General Principles Mansour Dib MD Normal Wound Healing Chronic Wounds: Stuck Where does it get stuck? Mostly Proliferation Sometimes Remodeling Why? Systemic factors Local factors How do
Wound Healing: General Principles Mansour Dib MD Normal Wound Healing Chronic Wounds: Stuck Where does it get stuck? Mostly Proliferation Sometimes Remodeling Why? Systemic factors Local factors How do
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Larval Debridement Therapy Making healing possible
 Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE
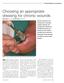 Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
Partnering the burn community
 * At smith&nephew we seek imaginative solutions that improve wound outcomes for patients and at the same time conserve resources for healthcare systems. Partnering the burn community Dedicated to the management
* At smith&nephew we seek imaginative solutions that improve wound outcomes for patients and at the same time conserve resources for healthcare systems. Partnering the burn community Dedicated to the management
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
NPUAP Mission. Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries. npuap.org
 Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries Margaret Goldberg, MSN, RN, CWOCN June 29, 2016 NPUAP Mission The National Pressure Ulcer Advisory Panel (NPUAP) serves
Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries Margaret Goldberg, MSN, RN, CWOCN June 29, 2016 NPUAP Mission The National Pressure Ulcer Advisory Panel (NPUAP) serves
January Adult Burn Injured patients
 Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition
Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition
Categorisation of Wound Care and Associated Products
 Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Northern Ireland Wound Care Formulary
 Northern Ireland Wound Care Formulary 2nd Edition April 2011 Wound Care Formulary 2 Wounds cause pain and discomfort to many people in Northern Ireland. Management of wounds requires considerable resources
Northern Ireland Wound Care Formulary 2nd Edition April 2011 Wound Care Formulary 2 Wounds cause pain and discomfort to many people in Northern Ireland. Management of wounds requires considerable resources
Basic Dressing Categories
 Category of Dressing Examples Advantages/Indications Disadvantages/Contraindications Hydrofiber Aquacel AG - ConvaTec Aquacel - Convatec Excellent for absorbing excess exudate These dressings form a gel
Category of Dressing Examples Advantages/Indications Disadvantages/Contraindications Hydrofiber Aquacel AG - ConvaTec Aquacel - Convatec Excellent for absorbing excess exudate These dressings form a gel
Wound Care Program for Nursing Assistants-
 Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Medical technologies guidance Published: 25 March 2014 nice.org.uk/guidance/mtg17
 The Debrisoft monofilament debridement pad for use in acute or chronic wounds Medical technologies guidance Published: 25 March 2014 nice.org.uk/guidance/mtg17 NICE 2018. All rights reserved. Subject to
The Debrisoft monofilament debridement pad for use in acute or chronic wounds Medical technologies guidance Published: 25 March 2014 nice.org.uk/guidance/mtg17 NICE 2018. All rights reserved. Subject to
Education Module. Use of Conservative Sharp Wound Debridement to Debride Necrotic Tissue in Wounds
 British Columbia Provincial Nurses Skin and Wound Committee Education Module: Conservative Sharp Wound Debridement. Developed by the BC Provincial Nursing Skin and Wound Committee in collaboration with
British Columbia Provincial Nurses Skin and Wound Committee Education Module: Conservative Sharp Wound Debridement. Developed by the BC Provincial Nursing Skin and Wound Committee in collaboration with
This article is based on a symposium held
 Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management
 An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine
 Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
Vacuumed Assisted Closure
 Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
THERAPIES. HAND IN HAND. Need safe and efficient infection prevention and management? 1 The Cutimed. Closing wounds. Together.
 Closing wounds. Together. Need safe and efficient infection prevention and management? 1 The Cutimed Sorbact range. A responsible choice. THERAPIES. HAND IN HAND. www.bsnmedical.co.uk TOGETHER WE CAN MAKE
Closing wounds. Together. Need safe and efficient infection prevention and management? 1 The Cutimed Sorbact range. A responsible choice. THERAPIES. HAND IN HAND. www.bsnmedical.co.uk TOGETHER WE CAN MAKE
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology
 The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
