Intra-vitreal injection of methotrexate in experimental endotoxin-induced uveitis in rabbit
|
|
|
- Bernadette Webb
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Veterinary Research Forum. 2018; 9 (4) doi: /vrf Journal Homepage: vrf.iranjournals.ir Veterinary Research Forum Intra-vitreal injection of methotrexate in experimental endotoxin-induced uveitis in rabbit Mohammad Abbaszadeh Hasiri 1, Effat Baghaei Moghaddam 1 *, Mohammad Reza Khalili 2, Amin Hossein Amini 1, Masoomeh Eghtedari 2, Mohammad Azizzadeh 3, Hooman Razmi 2 1 Department of Clinical Sciences, School of Veterinary Medicine, Shiraz University, Shiraz, Iran; 2 Poostchi Ophthalmology Research Center, Department of Ophthalmology, Shiraz University of Medical Sciences, Shiraz, Iran; 3 Department of Clinical Sciences, Faculty of Veterinary Medicine, Ferdowsi University of Mashhad, Mashhad, Iran. Article Info Article history: Received: 08 November 2017 Accepted: 09 January 2018 Available online: 15 December 2018 Key words: Inflammation Intra-vitreal injection Methotrexate Uveitis Abstract Uveitis is a major cause of vision loss. Methotrexate (MTX) has been widely used in uveitis due to its relatively safe profile. The purpose of this study was to evaluate the effects of two different dosages of MTX via intra-vitreal administration for treatment of endotoxin induced uveitis (EIU) in an experimental model. Thirty-five healthy rabbits were randomly divided into four groups and all animals were tolerated intra-vitreal injections. The first group received normal saline (NS), the second group received normal saline plus Salmonella typhimurium lipopolysaccharide endotoxin (LPS), (NS+LPS), the third group received 400 μg MTX plus LPS (LPS+MTX 400) and the fourth group received 800 μg MTX plus LPS (LPS+MTX 800). Intraocular inflammation was evaluated by clinical examination scoring during 7 post-injection days and histopathological examination at the end of study. Kruskal-Wallis and Mann-Whitney U tests were used to compare the histopathological and clinical scores. According to the clinical examinations, all groups demonstrated higher uveitis score than group 1 on first post-injection day. Also, groups 2 and 3 showed greater uveitis score than group 4. On the third, fifth and seventh post-injection days, clinical uveitis score in groups 2, 3 and 4 was significantly higher than group 1. The mean histopathological inflammation intensity scores in groups 2, 3 and 4 were significantly higher than group 1. Single intra-vitreal injection of 400 μg and 800 μg of MTX did not show significant anti-inflammatory effects on EIU in rabbits Urmia University. All rights reserved. چکیده تزریق داخل زجاجیهای متوترکسات در یووییت تجربی ناشی از اندوتوکسین در خرگوش یووییت عامل اصلی از بین رفتن بینایی است. متوترکسات به واسطه ماهیت نسبتا ایمن آن به طور گسترده در یووییت استفاده شده است. هدف این مطالعه بررسی آثار دو دوز مختلف متوترکسات از طریق تجویز داخل زجاجیهای برای درمان یووییت ناشی از اندوتوکسین در یک مدل تجربی بود. 53 خرگوش سالم به چهار گروه تقسیم شدند وتمام حیوانات تزریق داخل زجاجیهای را متحمل شدند. گروه اول سالین نرمال گروه دوم سالین نرمال به اضافه اندوتوکسین لیپوپلیساکارید سالمونال تایفیموریوم )لیپوپلیساکارید( گروه سوم 044 میکروگرم متوترکسات به اضافه لیپوپلیساکارید و گروه چهارم 044 میکروگرم متوترکسات به اضافه لیپوپلیساکارید دریافت کردند. التهاب داخل چشمی از طریق امتیاز بندی معاینه بالینی در طی هفت روز بعد از تزریق و بررسی هیستوپاتولوژیکی در انتهای مطالعه مورد ارزیابی قرار گرفت. آزمونهای آماری کروسکال والیس وU Mann-Whitney برای مقایسهی امتیازهای بالینی و هیستوپاتولوژیکی استفاده شد. بر اساس معاینات بالینی تمام گروهها امتیاز بالینی یووییت باالتری را 0 از گروه 1 در روز اول پس از تزریق نشان دادند. همچنین گروه 2 و 5 امتیاز یووییت بیشتری نسبت به گروه 0 نشان دادند. در روزهای سوم پنجم و هفتم پس از تزریق امتیاز بالینی یووییت در گروه 2 به طور معنی داری بیشتر از گروه 1 بود. میانگین امتیازهای شدت التهاب هیستوپاتولوژیکی در گروه های 2 و 5 و 5 میکروگرم متوترکسات آثار ضدالتهابی قابل توجهی بر روی یووییت ناشی از اندوتوکسین در خرگوشها نشان نداد. واژه های کلیدی: التهاب تزریق داخل زجاجیهای متوترکسات یووییت 0 به طور معنیداری بیشتر از گروه 1 بود. تک تزریق داخل زجاجیه ای دوزهای 044 و 044 *Correspondence: Effat Baghaei Moghaddam. DVM, DVSc Department of Clinical Sciences, School of Veterinary Medicine, Shiraz University, Shiraz, Iran effatbaghaii@shirazu.ac.ir This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License which allows users to read, copy, distribute and make derivative works for non-commercial purposes from the material, as long as the author of the original work is cited properly.
2 316 M. Abbaszadeh Hasiri et al. Veterinary Research Forum. 2018; 9 (4) Introduction Uveitis is a major cause of vision loss in adults. 1 It is the third leading cause of blindness that is potentially treatable. 2 Uveitis is inflammation of the vascular uveal tract of the eye including iris, ciliary body and choroid; however, surrounding structures such as retina, optic nerve, vitreous and sclera can also be affected. Clinically, uveitis is classified into four categories of anterior, intermediate, posterior and panuveitis depending on which anatomical structures of the eye are involved. 3 Uveitis comprises a heterogeneous group of diseases with complex pathogenesis. In general, uveitis can be divided into two major forms of origin including infectious and non-infectious uveitis. Non-infectious (or autoimmune) uveitis can be a part of systemic diseases such as juvenile inflammatory arthritis, spondyloarthritis and Behcet s disease. However, in many cases, no underlying cause can be found and uveitis is considered idiopathic. 4 In infectious uveitis, treating the underlying infection is a critical part of the ocular inflammation treatment. In non-infectious or immune-mediated cases of uveitis, the aim of treatment is to control the ocular inflammation. 5 Although the exact pathogenic mechanisms underlying uveitis are unknown, cytokines playing an important role as mediators of immunologic and inflammatory responses appear to be involved in this inflammatory disorder. Several cytokines including tumor necrosis factor-α (TNFα), interleukin-2 (IL-2), IL-6 and interferon-γ have been demonstrated in ocular tissues obtained from patients with uveitis. 6 Treatment of uveitis is important in order to avoid complications such as posterior synechiae, secondary glaucoma, cataract and macular edema. 4 The first treatment option for non-infectious uveitis is corticosteroids (CS). 7 Uveitis and its sight-threatening consequences such as cystoids macular edema (CME) may be treated with local (topical, periocular or intra-vitreal) or systemic (oral or intravenous) forms of CS or other immunosuppressive drugs. Local treatment is preferred where possible, especially for unilateral disease. However, this method for CS is associated with an increase in intra-ocular pressure in some patients. 8 Also, it can cause cataract, glaucoma and delay wound healing. 9 In some cases, corticosteroidsparing medications should be considered. Indications for the use of corticosteroid-sparing agents include the inability to control inflammation with high-dose CS, patients who require chronic oral corticosteroid therapy especially at doses greater than 10 mg per day and the occurrence of adverse effects that require tapering or discontinuation of CS. 7 In recent years, methotrexate (MTX) has been increasingly used in the treatment of ophthalmic diseases, both locally and systemically. 8 Several reports have shown that MTX is an effective therapy for ocular inflammatory diseases To our knowledge, the effects of intravitreal MTX on ocular inflammation in an experimental model of uveitis have not been assessed previously. All the previous works associated with MTX and ophthalmic inflammation have been based on oral medication and the reports of intra-vitreal usage of MTX for subsiding ophthalmic diseases are scarce. To the best of the authors knowledge, no previous study has investigated intra-vitreal administration of MTX in the management of experimental uveitis. The EIU is a widely accepted animal model for some types of human uveitis. The inflammatory reaction peaks 24 hr after endotoxin injection and subsides after five to seven days. Some species including New Zealand rabbits, rats and mice are usually used in EIU experiments. Salmonella typhimurium endotoxin, the lipopolysaccharide component of the Gram-negative bacterial cell wall, is commonly used for the uveitis induction. The endotoxin is usually injected into the footpad or vitreous body of the animal. 19 This study was designed to evaluate clinical and histopathological effects of intra-vitreal administration of MTX. The purpose of the present study was to evaluate the effects of two different dosages of intra-vitreal MTX for the treatment of endotoxin-induced uveitis (EIU) in an experimental model. Materials and Methods Animals. Thirty-five male New Zealand white rabbits weighing between 2.70 and 3.30 kg were used in this study. All rabbits were treated in accordance with the Association for Research in Vision and Ophthalmology Statement for the Use of Animals in Ophthalmic and Vision Research (NRC2011 and AAALAC s) 20 and our study was approved by the Institutional Review Board at the Shiraz University of Medical Sciences (IACUC No: 4687/63). Procedures. All procedures were carried out under general anesthesia with an intra-muscular injection of a mixture of 25 mg kg -1 ketamine hydrochloride 10.00% (Alfasan, Woerden, Netherlands) and 10 mg kg -1 xylazine hydrochloride 2.00% (Alfasan). Ophthalmic solution of tetracaine (0.50%; Sina Darou, Tehran, Iran) was administered for topical anesthesia. Only one eye of each animal (right eye) was used in this experiment. Rabbits were randomly divided into four groups. The first group (n = 5) received 0.10 ml normal saline (NS) intra-vitreally, the second group (n = 10) received 2.00 µg 0.05 ml -1 Salmonella typhimurium lipopolysaccharide endotoxin (LPS), (L6511; Sigma Chemical, St. Louis, USA) plus 0.05 ml NS (NS + LPS), the third group (n = 10) received 400 μg 0.05 ml -1 MTX without preservative (Mylan V.N, Saint-Priest, France) plus 2.00 μg 0.05 ml -1 LPS (LPS + MTX400) and the fourth group (n = 10) received 800 μg 0.05 ml -1 MTX plus 2 μg 0.05 ml -1 LPS (LPS + MTX800). The aseptic preparation
3 M. Abbaszadeh Hasiri et al. Veterinary Research Forum. 2018; 9 (4) was provided by 5.00% povidone iodine solution to the conjunctival sac before any manipulation. Injections were performed 2.50 mm posterior to the limbus into vitreaous cavity using a 30-gauge needle. Topical ciprofloxacine 0.30% (Sina Darou) and timolol 0.50% (Sina Darou) were applied before and after the injections and the eyes were monitored by indirect ophthalmoscopy for post-injection complications. All injections were done by a single investigator in a blind fashion. Clinical evaluations. All animals were examined for signs of clinical inflammation with slit lamp biomicroscopy (Sl 115; Carl Zeiss, Oberkochen, Germany). On days 1, 3, 5 and 7 after the intra-vitreal injection, the degree of the anterior uveitis intensity was clinically assessed in a masked manner by two ophthalmologists. All eyes were evaluated for inflammatory signs. The intensity of the signs of intra-ocular inflammation was graded by using the following clinical scoring system. 19 Iris hyperemia was scored for absence (0), mild (1), moderate (2) or severe (3), pupil was scored for miotic (1) or normal (0), anterior chamber exudate formation was scored for absence (0), mild (1) or severe (2) and hypopyon was scored for none (0) or positive (1). The maximum possible clinical uveitis score, the sum of four parameter scores, was 7. Histopathological evaluations. On the seventh post intra-vitreal injection day, the rabbits were euthanized by an intra-cardiac injected overdose of sodium pentobarbital. The eyes were enucleated immediately after euthanasia. The enucleated globes were fixed in 10% formaldehyde for three days and processed in the standard manner for light microscopy using hematoxylin and eosin staining. Pupillo-optic sections were cut. All infiltrating inflammatory cells in six random, noncontiguous fields at 200 magnification in both anterior (iris, anterior chamber and ciliary body) and posterior (vitreous and retina) segment parts were counted by a single masked ocular pathologist. Also, pathological uveitis score, the sum of five parameters of anterior chamber, iris, vitreous and retinal inflammation, was evaluated. A semilogarithmic grading scale using the following criteria, 21 was used to compare the median inflammatory cell infiltrate among the four groups; grade 0: no cells, grade 1: 1 to 10 cells, grade 2: 11 to 30 cells, grade 3: 31 to 100 cells and grade 4: 101 to 300 cells per field. Meanwhile, the ratio of polymorphonuclear cells (PMN) to mononuclear ones was estimated in each case and separately recorded as PMN dominant (PMNs > 80.00%) or mononuclear dominant (mononuclear cells > 50.00%). Statistical analyses. A Kruskal-Wallis test was used to compare the grading of histopathological and clinical scores and p value of less than 0.05 was considered significant. Mann-Whitney with Bonferroni correction was used to detect which pairs have significant difference and values of p < 0.01 were considered significant. The statistical analysis was performed using SPSS software (version 21.0; IBM Corp., Chicago, USA). Comparison of percentage of PMN dominancy between experimental groups was performed by Fisher Exact test. Results Clinical findings. Twenty-four hr after intra-vitreal injection, some degrees of ocular inflammation with regard to iris hyperemia, miosis and anterior chamber reaction (ACR) were seen in all eyes injected with LPS (groups 2, 3 and 4). Iris hyperemia, ACR, pupil condition and hyperemia were the parameters that were assessed clinically. Iris hyperemia in all experimental groups (2, 3 and 4) was significantly more severe than group 1 in day 1 (p < 0.01). Also, iris hyperemia in groups 2 and 3 was significantly more severe than group 4 in day 1. Iris hyperemia in groups 2, 3 and 4 was significantly more severe than group 1 in day 3 (p < 0.01). Iris hyperemia in groups 3 and 4 was significantly more severe than group 1 in day 5 (p < 0.01). The ACR in groups 2, 3 and 4 was significantly more severe than group 1 in days 1 and 3 (p < 0.01). Pupil miosis in group 4 was significantly more severe than group 1 in days three, five and seven. Also, pupil miosis in groups 2 and 3 was significantly more severe than group 1 in day 5. Hypopyon was not observed in any group. In subsequent examinations on the third, fifth and seventh post-injection days, rabbits in group 1 showed no clinical sign of ocular inflammation (clinical severity scores were 0), while in the other three groups, the degree of inflammation decreased gradually. Description of median clinical severity score according to the slit lamp examination grading in four groups and the details of comparing clinical uveitis score p value s between all groups are presented in Table 1. According to the clinical examination, all experimental groups demonstrated higher uveitis score than group 1 on first post-injection day (p < 0.01). Also, groups 2 and 3 showed greater uveitis score than group 4 (p < 0.01). On the third, fifth and seventh post-injection days, comparison of clinical uveitis score between groups 1 and 2, 1 and 3 and 1 and 4 showed a statistically significant difference (p < 0.01). In addition, there was no statistically significant difference with regard to clinical uveitis score between other groups on the third, fifth and seventh post-injection days. Histopathological findings. Anterior chamber inflammation was significantly higher in groups 2, 3 and 4 compared to group 1 (p < 0.01). Iris inflammation was also significantly higher in group 4 compared to group 1 (p = 0.008). Ciliary body inflammation and vitreous inflammation were significantly higher in groups 2, 3 and 4 compared to group 1 (p < 0.01). Retina inflammation was significantly higher in groups 2, 3 and 4 compared to group 1 (p < 0.01). The mean histopathological inflammation uveitis score (including anterior chamber, iris, ciliary body,
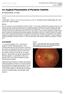
4 318 M. Abbaszadeh Hasiri et al. Veterinary Research Forum. 2018; 9 (4) Table 1. Comparison of clinical uveitis scores according to slit lamp examination grading between four groups. All data are presented as median (inter quartile range). Groups Number Day 1 Day 3 Day 5 Day 7 NS* 5 1 (1 to 1) 0 (0 to 1) 0 (0 to 0) 0 (0 to 0) NS + LPS* 10 6 (5 to 6) 4 (3 to 5) 2 (1 to 3) 2 (1 to 3) LPS + MTX* (5 to 6) 4 (4 to 6) 3 (2 to 3) 1 (1 to 3) LPS + MTX (4 to 5) 4 (3 to 4) 3 (2 to 3) 2 (2 to 3) p value < Pair-wise comparison ǂ NS vs NS + LPS NS vs LPS + MTX NS vs LPS + MTX NS + LPS vs LPS + MTX NS + LPS vs LPS + MTX LPS + MTX 400 vs LPS + MTX *NS, normal saline; LPS, lipopolysaccharide, MTX; methotrexate; Calculated by the Kruskal-Wallis test (p < 0.05 considered as significant); ǂ Calculated by the Mann-Whitney U test (p < 0.01 considered as significant). vitreous and retina) in groups 2, 3 and 4 was significantly higher than group 1 (p < 0.01), (Fig. 1). Median histopathological uveitis score in groups 1, 2, 3 and 4 animals was 0.20 (range ), 1.60 (range ), 1.80 (range ) and 1.80 (range Fig. 1. Mean histopathological severity score of uveitis in groups 1 (NS), 2 (LPS + NS), 3 (LPS + MTX 400) and 4 (LPS + MTX 800) seven days after injection. The mean histopathological inflammation intensity score in groups 2, 3 and 4 was significantly higher than group 1. NS = normal saline; LPS = lipopolysaccharide, and MTX = methotraxte. 2.00), respectively. However, there were no significant differences between groups 2 and 3, groups 2 and 4 or groups 3 and 4. Histopathological examination (Figs. 2 and 3) revealed that MTX with either dose did not reduce inflammation after single intra-vitreal injection. Regarding type of inflammation, PMN dominated infiltration was seen in the majority of cases in groups 2, 3 and 4 except for three cases in group 2, one case in group 3 and three cases in group 4, in them, lymphocytes were predominant. However, the difference was not statistically significant (p > 0.05). Median histopathological uveitis score in groups 1, 2, 3 and 4 animals was 0.20 (range ), 1.60 (range ), 1.80 (range ) and 1.80 (range ), respectively. However, there were no significant differences between groups 2 and 3, groups 2 and 4 or groups 3 and 4. Histopathological examination (Figs. 2 and 3) revealed that MTX with either dose did not reduce inflammation after single intra-vitreal injection. Regarding type of inflammation, PMN dominated infiltration was seen in the majority of cases in groups 2, 3 and 4 except for three cases in group 2, one case in group 3 and three cases in group 4, in them, lymphocytes were predominant. However, the difference was not statistically significant (p > 0.05). Fig. 2. Photomicrographs of ciliary body of each group seven days after injection. A) In group 2 (LPS + NS), ciliary body shows considerable inflammatory cells infiltration in the anterior chamber and ciliary processes. B) In group 3 (LPS + MTX 400), eyes show less inflammation in the anterior chamber; however, C) increasing dose of the drug in group 4 (LPS + MTX 800) only increased the inflammatory reaction, (Hematoxylin and eosin, 1000 ).
5 M. Abbaszadeh Hasiri et al. Veterinary Research Forum. 2018; 9 (4) Fig. 3. Histopathological images of retina in different treatment groups. Note the presence of almost equal amounts of acute inflammatory cells and exudate in pre-retinal area and vitreous cavity in control (A) and group 3 (B: LPS + MTX 400) and group 4 (C: LPS + MTX 800), (Hematoxylin and eosin, 400 ). Discussion The MTX is an antimetabolite agent with antiinflammatory and immunosuppressive effects. The MTX was introduced in 1948 as an antineoplastic agent 22 and approved by the United States Food and Drug Administration as a treatment for rheumatoid arthritis in The anti-inflammatory effects of MTX are primarily mediated by the release of adenosine into the extracellular space. Adenosine is a potent inflammatory inhibitor and induces vasodilatation. 23 Adenosine also suppresses the pro-inflammatory mediators such as TNFα, IL-6, IL-8, macrophage inflammatory protein 1α, leukotriene B4 and nitric oxide while increasing the production of anti-inflammatory mediators IL-10 and IL-1 receptor antagonists. Finally, adenosine lessens the inflammation by decreasing macrophage activation and changing the T helper type 1 response to type 2 in body. 24 According to the results of clinical examination in present study, all experimental groups demonstrated higher uveitis score than control group and a high dose MTX was able to decrease uveitis score comparing to a low dose MTX on first post-injection day. Clinical uveitis scores between all treated groups were significantly different with control group, on the third, fifth and seventh post-injection days. The largest cohort of patients with ocular inflammatory disease on MTX treatment was described by Gangaputra et al. 12 This retrospective study comprised 384 uveitis patients on MTX therapy (including 126 patients with anterior uveitis). In patients with anterior uveitis, a complete remission was achieved in 55.60% of patients within 6 months and 67.20% of patients within 12 months. A retrospective study by Foeldvari and Wierk evaluated the effectiveness of MTX therapy in juvenile idiopathic arthritis associated with chronic uveitis. 11 The study group comprised 25 patients treated with MTX. Four of 25 patients did not show any significant improvement from MTX treatment and an additional immunosuppressive medication was needed. Shah et al. reported a good clinical response of different inflammatory ocular diseases to low doses of MTX. 15 Kaplan-Kaplan-Messas et al. retrospectively studied 39 consecutive patients with uveitis, who were treated with MTX following inadequate control with CS lasting five years. 13 Full or partial control of inflammation was achieved in 23 (79.00%) patients. All patients were still on corticosteroid therapy when MTX was started. The first use of intra-vitreal MTX in uveitis was reported in Hardwig et al. reported a retrospective study in patients with uveitis or advanced proliferative diabetic retinopathy, which 400 µg intra-vitreal MTX improved visual acuity (VA) in 75.00% of patients. 25 Taylor et al. reported a prospective case series of 15 patients with uveitis and uveitic CME in 2009, in which intra-vitreal MTX was found to be effective in intra-ocular inflammation control and VA improvement. 8 The authors reported a retrospective study in 2013 which showed intra-vitreal MTX was effective in controlling intra-ocular inflammation and improving vision in 30 of 38 eyes (79.00%). 26 Khalil et al. have reported 80.00% improvement in VA after intra-vitreal MTX in patients with Behcet s disease-associated ocular inflammation with posterior segment involvement. 24 A retrospective study by Samson et al. suggested that inflammation was controlled by MTX in a large series of patients (76.00%) with chronic uveitis. 14 Inflammation did not respond in 17.00% of the cases. Seventy-two patients (45.00%) had previously taken prednisone or were receiving systemic prednisone at the time of being offered MTX therapy, either pulse oral therapy (58.00%) or chronic daily oral therapy (42.00%). Bachta et al. evaluated prospectively the efficacy of MTX in the treatment of recurrent idiopathic acute anterior uveitis in 22 patients. 10 Remission was achieved in 84.00% of patients and reduced frequency of flares in 16.00% of patients. This study was the only one which focused on acute form of uveitis but shows systemic MTX therapy in doses considered optimal in rheumatic diseases controls inflammation in a one-month period. In contrast to this study, our results determined no clinical improvement after intra-vitreal injection of MTX in EIU, not even in 800 μg group. According to our results, there
6 320 M. Abbaszadeh Hasiri et al. Veterinary Research Forum. 2018; 9 (4) was no difference between test and control groups regarding clinical and histopathological findings after treatment of EIU with intra-vitreal injection of MTX. The severity of uveitis in NS + LPS group decreased gradually in one week spontaneously without any medication. This evidence indicates that if the study had been continued by repeated injections of Salmonella typhimurium lipopolysaccharide into the vitreous to extend acute phase of uveitis more than one week, the anti-inflammatory effects of MTX might have been manifested by decreasing clinical signs or histopathological findings of uveitis. Short duration of the research was the limitation of our study. Uveitis could be prolonged experimentally for a longer period in order to extend the maximum three to five days of disease process. 27 In the previous studies, patients were treated with different doses of MTX. More importantly, in almost all previous studies, some patients continued other systemic drugs such as cyclosporine or prednisolone or were treated with a combination of two immunosuppressive drugs while being treated with MTX. Thus, the observed beneficial effect might not be attributed completely to MTX therapy. Also, in previous studies, the patients included were suffering from different types of ocular inflammation and the dosages used differed significantly between the studies. Intra-vitreal injection of MTX has been used in human studies for treatment of noninfectious uveitis. Bae and Lee have demonstrated that intra-vitreal injection of 400 μg MTX in patients with refractory retinal vasculitis was effective in inflammation control and was associated with a significant reduction of intra-ocular levels of IL-6 and IL In another study by Taylor et al., it was suggested that effect of administration of 400 μg MTX could be comparable with intra-vitreal prednisolone administration. 26 This dose and route and even doubled dose had no efficacy in our study in an EIU in rabbit. The acute nature of inflammatory reaction induced in this study explains why mononuclear dominancy wasn t observed in histopathological examination. Longer follow up may be needed to see the effects of injection in chronic uveitis and can be a base for future studies. In conclusion, intra-vitreal injection of MTX did not show any beneficial effect in management of acute uveitis in an experimental model in rabbits. However, due to diversity in etiologies and types of uveitis, intravitreal MTX may be beneficial in certain cases. Clearly, there is a demand for future experimental and clinical studies in order to clarify the role of intra-vitreal MTX in uveitis management. Acknowledgments We are grateful to Mr. Omid Koohi for his assistance and cooperation in Laboratory Animal Center of Shiraz University of Medical Sciences, Shiraz, Iran during the present study. Conflict of interest The authors declare no conflict of interest. References 1. Durrani O, Tehrani N, Marr J, et al. Degree, duration, and causes of visual loss in uveitis. Br J Ophthalmol 2004; 88(9): Durrani O, Meads C, Murray P. Uveitis: A potentially blinding disease. Ophthalmologica 2004; 218(4): Jabs DA, Nussenblatt RB, Rosenbaum JT. Standardization of uveitis nomenclature for reporting clinical data. Results of the First International Workshop. Am J Ophthalmol 2005;140(3): Selmi C. Diagnosis and classification of autoimmune uveitis. Autoimmun Rev2014; 13(4-5): Leung TG, Thorne JE. Emerging drugs for the treatment of uveitis. Expert Opin Emerg Drugs 2013; 18(4): De Vos A, Hoekzema R, Kijlstra A. Cytokines and uveitis, a review. Curr Eye Res 1992; 11(6): Jabs DA, Rosenbaum JT, Foster CS, et al. Guidelines for the use of immunosuppressive drugs in patients with ocular inflammatory disorders: Recommendations of an expert panel. Am J Ophthalmol 2000; 130(4): Taylor SR, Habot-Wilner Z, Pacheco P, et al. Intraocular methotrexate in the treatment of uveitis and uveitic cystoid macular edema. Ophthalmology 2009; 116(4): Kulkarni P. Review: Uveitis and immunosuppressive drugs. J Ocul Pharmacol Ther 2001; 17(2): Bachta A, Kisiel B, Tłustochowicz M, et al. High efficacy of methotrexate in patients with recurrent idiopathic acute anterior uveitis: A prospective study. Arch Immunol Ther Exp (Warsz) 2017; 65(1): Foeldvari I, Wierk A. Methotrexate is an effective treatment for chronic uveitis associated with juvenile idiopathic arthritis. JRheumatol 2005; 32(2): Gangaputra S, Newcomb CW, Liesegang TL, et al. Methotrexate for ocular inflammatory diseases. Ophthalmology 2009; 116(11): e Kaplan-Messas A, Barkana Y, Avni I, et al. Methotrexate as a first-line corticosteroid-sparing therapy in a cohort of uveitis and scleritis. Ocul Immunol Inflamm 2003; 11(2): Samson CM, Waheed N, Baltatzis S, et al. Methotrexate therapy for chronic noninfectious uveitis: Analysis of a case series of 160 patients. Ophthalmology 2001; 108(6): Shah SS, Lowder CY, Schmitt MA, et al. Low-dose methotrexate therapy for ocular inflammatory disease. Ophthalmology 1992; 99(9):
7 M. Abbaszadeh Hasiri et al. Veterinary Research Forum. 2018; 9 (4) Bom S, Zamiri P, Lightman S. Use of methotrexate in the management of sight-threatening uveitis. Ocul Immunol Inflamm 2001; 9(1): Munoz-Fernandez S, Garcia-Aparicio AM, Hidalgo MV, et al. Methotrexate: An option for preventing the recurrence of acute anterior uveitis. Eye (Lond) 2009; 23(5): Weiss AH, Wallace CA, Sherry DD. Methotrexate for resistant chronic uveitis in children with juvenile rheumatoid arthritis. J Pediatr 1998; 133(2): Statement for the Use of Animals in Ophthalmic and Visual Research. Available at: onlinecoursematerials/phop6275/2015_materials/ph OP6275_Class3_3_Animals_in_Research_ARVO_Statem ent.pdf. Accessed Oct 15, Oztürk F, Kurt E, Emiroglu L, et al. Effect of propolis on endotoxin-induced uveitis in rabbits. Jpn J Ophthalmol 1999; 43(4): Verma MJ, Mukaida N, Vollmer Conna U, et al. Endotoxin-induced uveitis is partially inhibited by anti IL-8 antibody treatment. Invest Ophth Vis Sci 1999; 40(11): Farber S, Diamond LK, Mercer RD, et al. Temporary remissions in acute leukemia in children produced by folic acid antagonist, 4-aminopteroyl-glutamic acid. N Engl J Med 1948; 238(23): Cannella AC, O dell JR. Traditional DMARDs: Methotrexate, lefl unomide, sulfasalazine, hydroxylchloroquine, and combination therapies. In: Firestein G, Budd R, Gabriel SE, McInnes IB, O'Dell J (Eds.) Kelley s Textbook of Rheumatology. 8 th ed. Philadelphia, USA: Saunders Elsevier 2008; Khalil HEM, Raafat HA, Azab NA, et al. The role of intraocular methotrexate in the management of uveitis and posterior segment involvement in Behçet s disease patients. Egypt Rheumatol 2015; 37(3): Hardwig PW, Pulido JS, Erie JC, et al. Intraocular methotrexate in ocular diseases other than primary central nervous system lymphoma. Am J Ophthalmol 2006; 142(5): Taylor SR, Banker A, Schlaen A, et al. Intraocular methotrexate can induce extended remission in some patients in noninfectious uveitis. Retina 2013; 33(10): Eperon S, Balaskas K, Vaudaux J, et al. Experimental uveitis can be maintained in rabbits for a period of six weeks after a safe sensitization method. Curr Eye Res 2013; 38(3): Bae JH, Lee SC. Effect of intravitreal methotrexate and aqueous humor cytokine levels in refractory retinal vasculitis in Behcet disease. Retina 2012;32(7):
Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
Intravitreal Triamcinolone Acetonide for Macular Edema in HLA-B27 Negative Ankylosing Spondylitis
 105 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
105 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
UVEITIS. Dr. Yılmaz ÖZYAZGAN
 UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
Abbreviated Drug Evaluation: Fluocinolone acetonide intravitreal implant (Retisert )
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Uveitis unplugged: systemic therapy
 Uveitis unplugged: systemic therapy Hobart 2017 Peter McCluskey Save Sight Institute Sydney Eye Hospital Sydney Medical School University of Sydney Sydney Australia No financial or proprietary interest
Uveitis unplugged: systemic therapy Hobart 2017 Peter McCluskey Save Sight Institute Sydney Eye Hospital Sydney Medical School University of Sydney Sydney Australia No financial or proprietary interest
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Update on management of Anterior Uveitis
 Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
Nausheen Khuddus, MD Melissa Elder, MD, PhD
 Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Surgery in patients with uveitis. Lyndell Lim and Anthony Hall
 Surgery in patients with uveitis Lyndell Lim and Anthony Hall Disclosures Off label treatments Paid advisory board Bayer Paid research support Allergan (makers of Ozurdex) Paid research support B and L
Surgery in patients with uveitis Lyndell Lim and Anthony Hall Disclosures Off label treatments Paid advisory board Bayer Paid research support Allergan (makers of Ozurdex) Paid research support B and L
The effect of a single intravitreal implantation of dexamethasone on the fellow eye in bilateral non-infectious uveitis case report
 European Review for Medical and Pharmacological Sciences The effect of a single intravitreal implantation of dexamethasone on the fellow eye in bilateral non-infectious uveitis case report J. CISZEWSKA,
European Review for Medical and Pharmacological Sciences The effect of a single intravitreal implantation of dexamethasone on the fellow eye in bilateral non-infectious uveitis case report J. CISZEWSKA,
Management of uveitis
 Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Macular Hole Associated with Vogt-Koyanagi-Harada Disease at the Acute Uveitic Stage
 Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior Uveitis in a Korean Population
 J Korean Med Sci 2009; 24: 722-8 ISSN 1011-8934 DOI: 10.3346/jkms.2009.24.4.722 Copyright The Korean Academy of Medical Sciences Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior
J Korean Med Sci 2009; 24: 722-8 ISSN 1011-8934 DOI: 10.3346/jkms.2009.24.4.722 Copyright The Korean Academy of Medical Sciences Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior
Juvenile Idiopathic Arthritis with Associated Bilateral Anterior Uveitis in a Four Year- Old Girl
 Juvenile Idiopathic Arthritis with Associated Bilateral Anterior Uveitis in a Four Year- Old Girl Pavlina S. Kemp, MD, Susannah Q. Longmuir, MD August 14, 2012 Chief complaint: Central posterior synechiae
Juvenile Idiopathic Arthritis with Associated Bilateral Anterior Uveitis in a Four Year- Old Girl Pavlina S. Kemp, MD, Susannah Q. Longmuir, MD August 14, 2012 Chief complaint: Central posterior synechiae
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
New Drugs for Uveitis. Medical Eye Unit St Thomas Hospital
 New Drugs for Uveitis Miles Stanford Medical Eye Unit St Thomas Hospital x Epithelium x x Antigen Y Y Y Y IgG m cd4 IL-2 Y m + IL-12 Cytotoxic T B pmn Ig s PG s. LTB4 O - IL-6 TNFα IFNγγ IL-2 Th1 IL-10
New Drugs for Uveitis Miles Stanford Medical Eye Unit St Thomas Hospital x Epithelium x x Antigen Y Y Y Y IgG m cd4 IL-2 Y m + IL-12 Cytotoxic T B pmn Ig s PG s. LTB4 O - IL-6 TNFα IFNγγ IL-2 Th1 IL-10
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Uveitis of spondyloarthritis in Indian subcontinent: a cross sectional study
 International Journal of Advances in Medicine Ninan F et al. Int J Adv Med. 2017 Oct;4(5):1441-1446 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174300
International Journal of Advances in Medicine Ninan F et al. Int J Adv Med. 2017 Oct;4(5):1441-1446 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174300
Evolving therapies for posterior uveitis. Infliximab (Remicade) Infliximab: pharmacology. FDA-approved monoclonal antibody therapy Target
 Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
Interim Clinical Commissioning Policy Statement: Adalimumab for Severe Refractory Uveitis. Reference: NHS England: /PS
 Interim Clinical Commissioning Policy Statement: Adalimumab for Severe Refractory Uveitis Reference: NHS England: 170010/PS Publications Gateway Reference: Document Purpose Policy 05527s Document Name
Interim Clinical Commissioning Policy Statement: Adalimumab for Severe Refractory Uveitis Reference: NHS England: 170010/PS Publications Gateway Reference: Document Purpose Policy 05527s Document Name
Eye (2009) 23, & 2009 Macmillan Publishers Limited All rights reserved X/09 $32.00
 (2009) 23, 543 548 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Effects of the duration of initial oral corticosteroid treatment on the recurrence of inflammation
(2009) 23, 543 548 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Effects of the duration of initial oral corticosteroid treatment on the recurrence of inflammation
What you can expect with OZURDEX
 Important Information About Noninfectious Uveitis Affecting the Back Segment of the Eye and Treatment What you can expect with OZURDEX Approved Use OZURDEX (dexamethasone intravitreal implant) is a prescription
Important Information About Noninfectious Uveitis Affecting the Back Segment of the Eye and Treatment What you can expect with OZURDEX Approved Use OZURDEX (dexamethasone intravitreal implant) is a prescription
HLA-B27-related anterior Uveitis
 HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
A Clinical Study of Anterior Uveitis in a Rural Hospital
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
Optical coherence tomography findings in a child with posterior scleritis
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
Comparison of Intravitreal Injection of Bevacizumab and Triamcinolone Acetonide in the Treatment of Uveitic Macular Edema
 ISSN 1735-1383 Iran. J. Immunol. June 2012, 9 (2), 136-144 Mansour Rahimi, Seyed Sahabaldin Shahrzad, Mohammad Banifatemi Comparison of Intravitreal Injection of Bevacizumab and Triamcinolone Acetonide
ISSN 1735-1383 Iran. J. Immunol. June 2012, 9 (2), 136-144 Mansour Rahimi, Seyed Sahabaldin Shahrzad, Mohammad Banifatemi Comparison of Intravitreal Injection of Bevacizumab and Triamcinolone Acetonide
Adalimumab and dexamethasone for treating non-infectious uveitis [ID763]
![Adalimumab and dexamethasone for treating non-infectious uveitis [ID763] Adalimumab and dexamethasone for treating non-infectious uveitis [ID763]](/thumbs/82/86218480.jpg) Adalimumab and dexamethasone for treating non-infectious uveitis [ID763] Multiple Technology Appraisal 2 nd meeting: 12 th April 2017 Committee C Slides for Committee, projector and public [NoACIC] 1 The
Adalimumab and dexamethasone for treating non-infectious uveitis [ID763] Multiple Technology Appraisal 2 nd meeting: 12 th April 2017 Committee C Slides for Committee, projector and public [NoACIC] 1 The
Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization
 Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
You can C-ME after Uveitis
 You can C-ME after Uveitis Abstract: Approximately 50% of uveitis patients will present with vision loss secondary to cystoid macular edema[1]. Two patients with uveitis present with a constant decrease
You can C-ME after Uveitis Abstract: Approximately 50% of uveitis patients will present with vision loss secondary to cystoid macular edema[1]. Two patients with uveitis present with a constant decrease
Patterns of uveitis in a Philippine eye clinic
 VOL. NO. PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE - MARCH 5 Harvey S. Uy, MD Irene W. Tam, OD Asian Eye Institute Makati, Philippines Patterns of uveitis in a Philippine eye clinic
VOL. NO. PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE - MARCH 5 Harvey S. Uy, MD Irene W. Tam, OD Asian Eye Institute Makati, Philippines Patterns of uveitis in a Philippine eye clinic
UVEITIS A. D. RUEDEMANN, M.D.
 A. D. RUEDEMANN, M.D. The diagnosis of uveitis, especially of the low-grade recurring type, is one of the most exacting problems in medicine. Difficult to diagnose, difficult to treat, and offering a very
A. D. RUEDEMANN, M.D. The diagnosis of uveitis, especially of the low-grade recurring type, is one of the most exacting problems in medicine. Difficult to diagnose, difficult to treat, and offering a very
THE BURDEN OF NONINFECTIOUS UVEITIS OF THE POSTERIOR
 THE BURDEN OF NONINFECTIOUS UVEITIS OF THE POSTERIOR SEGMENT: A REVIEW New pharmacologic treatment options are urgently needed. BY STEVEN YEH, MD, and JESSICA G. SHANTHA, MD Noninfectious uveitis (NIU)
THE BURDEN OF NONINFECTIOUS UVEITIS OF THE POSTERIOR SEGMENT: A REVIEW New pharmacologic treatment options are urgently needed. BY STEVEN YEH, MD, and JESSICA G. SHANTHA, MD Noninfectious uveitis (NIU)
Uveitis. What is Uveitis?
 Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
Study Number CAIN457C2302 (core study) and CAIN457C2302E1 (extension study)
 Clinical Trial Results Database Page 1 Sponsor Novartis Generic Drug Name Secukinumab Therapeutic Area of Trial Uveitis Approved Indication Investigational Study Number CC2302 (core study) and CC2302E1
Clinical Trial Results Database Page 1 Sponsor Novartis Generic Drug Name Secukinumab Therapeutic Area of Trial Uveitis Approved Indication Investigational Study Number CC2302 (core study) and CC2302E1
Association of Cryptogenic Organizing Pneumonia in Bilateral Anterior Uveitis
 Published online: November 13, 2014 1663 2699/14/0053 0365$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: November 13, 2014 1663 2699/14/0053 0365$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY
 Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Uveitis literature 2014: the year in review. Russell N. Van Gelder, MD, PhD Department of Ophthalmology University of Washington Seattle, WA
 Uveitis literature 2014: the year in review Russell N. Van Gelder, MD, PhD Department of Ophthalmology University of Washington Seattle, WA Disclosures RVG serves as Associate Editor of IOVS Editorial
Uveitis literature 2014: the year in review Russell N. Van Gelder, MD, PhD Department of Ophthalmology University of Washington Seattle, WA Disclosures RVG serves as Associate Editor of IOVS Editorial
It has previously been shown that pine
 The effects of cortisone on pine pollen-induced uveitis in guinea pigs Stan L. Coleman and Samuel Canaan Injection of pine pollen into the vitreous of guinea pigs previously sensitized with Freund's adjuvant
The effects of cortisone on pine pollen-induced uveitis in guinea pigs Stan L. Coleman and Samuel Canaan Injection of pine pollen into the vitreous of guinea pigs previously sensitized with Freund's adjuvant
ISPUB.COM. An Atypical Presentation of Posterior Scleritis. A Ramanathan, A Gaur CASE REPORT
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema
 Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient
 CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
Clinical Outcomes of Cyclosporine Treatment for Noninfectious Uveitis
 pissn: 1011-8942 eissn: 2092-9382 Clinical Outcomes of Cyclosporine Treatment for Noninfectious Uveitis Korean J Ophthalmol 2012;26(1):21-25 http://dx.doi.org/10.3341/kjo.2012.26.1.21 Original Article
pissn: 1011-8942 eissn: 2092-9382 Clinical Outcomes of Cyclosporine Treatment for Noninfectious Uveitis Korean J Ophthalmol 2012;26(1):21-25 http://dx.doi.org/10.3341/kjo.2012.26.1.21 Original Article
Sclerokeratoplasty David S. Chu, M.D. Cases
 Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Technology appraisal guidance Published: 26 July 2017 nice.org.uk/guidance/ta460
 Adalimumab and dexamethasone for treating non-infectious uveitis Technology appraisal guidance Published: 26 July 2017 nice.org.uk/guidance/ta460 NICE 2017. All rights reserved. Subject to Notice of rights
Adalimumab and dexamethasone for treating non-infectious uveitis Technology appraisal guidance Published: 26 July 2017 nice.org.uk/guidance/ta460 NICE 2017. All rights reserved. Subject to Notice of rights
EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA
 Basrah Journal Of Surgery EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA Salah Zuhair Abed Al-Asadi MB,ChB, FICMS, Lecturer, Department of Surgery, College
Basrah Journal Of Surgery EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA Salah Zuhair Abed Al-Asadi MB,ChB, FICMS, Lecturer, Department of Surgery, College
o White dot syndromes pattern recognition o Activity and damage o Quality of life o Key points o Idiopathic o Sarcoidosis o Multiple sclerosis
 Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Immunohistochemical study of epiretinal membranes in patients with uveitis
 J Ophthal Inflamm Infect (2012) 2:243 248 DOI 10.1007/s12348-012-0074-x DISCUSSION BY CASE Immunohistochemical study of epiretinal membranes in patients with uveitis Arsham Sheybani & George J. Harocopos
J Ophthal Inflamm Infect (2012) 2:243 248 DOI 10.1007/s12348-012-0074-x DISCUSSION BY CASE Immunohistochemical study of epiretinal membranes in patients with uveitis Arsham Sheybani & George J. Harocopos
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Head prof. MUDr. E. Vlková, CSc.
 MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma
 Original Article Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma Irfan Qayyum Malik, M. Moin, A. Rehman, Mumtaz Hussain
Original Article Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma Irfan Qayyum Malik, M. Moin, A. Rehman, Mumtaz Hussain
iologic Agents in the Treatment of Non-Infectious Uveitis
 What is New B iologic Agents in the Treatment of Non-Infectious Uveitis Amala George DNB The treatment of non-infectious uveitis is a challenge to clinicians. The treatment involves suppressing the deleterious
What is New B iologic Agents in the Treatment of Non-Infectious Uveitis Amala George DNB The treatment of non-infectious uveitis is a challenge to clinicians. The treatment involves suppressing the deleterious
ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS
 ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
Relapse of Vogt-Koyanagi- Harada Disease during Interferon-α and Ribavirin Therapy in a Case of Chronic Viral Hepatitis C
 5 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
5 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Why Is Imaging Critical in My Uveitis Practice?
 Why Is Imaging Critical in My Uveitis Practice? Dilraj S. Grewal, MD Developed in collaboration Imaging Is the Backbone of Uveitis Workup and Monitoring Treatment Response FP FAF B- scan Multimodal Imaging
Why Is Imaging Critical in My Uveitis Practice? Dilraj S. Grewal, MD Developed in collaboration Imaging Is the Backbone of Uveitis Workup and Monitoring Treatment Response FP FAF B- scan Multimodal Imaging
Recurrent pseudohypopyon in association with primary vitreoretinal lymphoma: a case report
 Kitao et al. BMC Ophthalmology (2016) 16:103 DOI 10.1186/s12886-016-0279-0 CASE REPORT Open Access Recurrent pseudohypopyon in association with primary vitreoretinal lymphoma: a case report Masahiro Kitao,
Kitao et al. BMC Ophthalmology (2016) 16:103 DOI 10.1186/s12886-016-0279-0 CASE REPORT Open Access Recurrent pseudohypopyon in association with primary vitreoretinal lymphoma: a case report Masahiro Kitao,
Better ophthalmic surgery outcomes in recent years have created more Demanding Patients.
 By Alaa EL Zawawi Prof. of Ophthalmology Alexandria - Egypt Launch Better ophthalmic surgery outcomes in recent years have created more Demanding Patients. 1 NSAIDs can play a pivotal role in facilitating
By Alaa EL Zawawi Prof. of Ophthalmology Alexandria - Egypt Launch Better ophthalmic surgery outcomes in recent years have created more Demanding Patients. 1 NSAIDs can play a pivotal role in facilitating
Screening for Uveitis in Children
 Information for patients and parents Manchester Royal Eye Hospital Paediatric Uveitis Service Screening for Uveitis in Children What is uveitis? Uveitis is inflammation of a layer of the eye, called the
Information for patients and parents Manchester Royal Eye Hospital Paediatric Uveitis Service Screening for Uveitis in Children What is uveitis? Uveitis is inflammation of a layer of the eye, called the
Regional vs. Systemic Therapy. Corticosteroids. Regional vs. Systemic Therapy for Uveitis. Considerations
 Regional vs. Systemic Therapy for Uveitis Nisha Acharya,, M.D., M.S. Director, Uveitis Service F.I. Proctor Foundation University of California, San Francisco December 4, 2010 No financial disclosures
Regional vs. Systemic Therapy for Uveitis Nisha Acharya,, M.D., M.S. Director, Uveitis Service F.I. Proctor Foundation University of California, San Francisco December 4, 2010 No financial disclosures
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
Original Effective Date: 12/13/2017. Subject: Intravitreal corticosteroid implants: Retisert (fluocinolone acetonide intravitreal implant)
 Subject: Intravitreal corticosteroid implants: Retisert (fluocinolone acetonide intravitreal implant) Policy Number: MCP-302 Original Effective Date: 12/13/2017 Revision Date(s): Review Date: DISCLAIMER
Subject: Intravitreal corticosteroid implants: Retisert (fluocinolone acetonide intravitreal implant) Policy Number: MCP-302 Original Effective Date: 12/13/2017 Revision Date(s): Review Date: DISCLAIMER
Adalimumab in Noninfectious Uveitis of Idiopathic Etiology Efficacy Across Different Anatomical Locations the VISUAL I and VISUAL II Trials
 9:00 AM Adalimumab in Noninfectious Uveitis of Idiopathic Etiology Efficacy Across Different Anatomical Locations the VISUAL I and VISUAL II Trials Pauline T. Merrill, MD Albert T. Vitale, MD Eric Fortin,
9:00 AM Adalimumab in Noninfectious Uveitis of Idiopathic Etiology Efficacy Across Different Anatomical Locations the VISUAL I and VISUAL II Trials Pauline T. Merrill, MD Albert T. Vitale, MD Eric Fortin,
SCHEDULING STATUS Schedule 4. PROPRIETARY NAME AND DOSAGE FORM OZURDEX intravitreal implant
 Page 1 of 10 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM intravitreal implant COMPOSITION One intravitreal implant contains: Dexamethasone 700 μg Excipients: Ester terminated 50:50 poly
Page 1 of 10 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM intravitreal implant COMPOSITION One intravitreal implant contains: Dexamethasone 700 μg Excipients: Ester terminated 50:50 poly
Review Article Gender and Spondyloarthropathy-Associated Uveitis
 Ophthalmology Volume 2013, Article ID 928264, 6 pages http://dx.doi.org/10.1155/2013/928264 Review Article Gender and Spondyloarthropathy-Associated Uveitis Wendy M. Smith MayoClinic,200FirstStreetSW,Rochester,MN55905,USA
Ophthalmology Volume 2013, Article ID 928264, 6 pages http://dx.doi.org/10.1155/2013/928264 Review Article Gender and Spondyloarthropathy-Associated Uveitis Wendy M. Smith MayoClinic,200FirstStreetSW,Rochester,MN55905,USA
Corporate Medical Policy
 Corporate Medical Policy Intravitreal Implant File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intravitreal_implant 11/2010 6/2017 6/2018 6/2017 Description of Procedure or Service
Corporate Medical Policy Intravitreal Implant File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intravitreal_implant 11/2010 6/2017 6/2018 6/2017 Description of Procedure or Service
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg
 An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
Case Rep Oncol 2012;5: DOI: /
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
A role for methotrexate in the management of non-infectious orbital inflammatory disease
 1220 Casey Eye Institute, Oregon Health Sciences University, Portland, Oregon, USA J R Smith J T Rosenbaum Correspondence to: Dr Justine R Smith, Casey Eye Institute, Oregon Health Sciences University,
1220 Casey Eye Institute, Oregon Health Sciences University, Portland, Oregon, USA J R Smith J T Rosenbaum Correspondence to: Dr Justine R Smith, Casey Eye Institute, Oregon Health Sciences University,
Assisting in Ophthalmology. Copyright 2011, 2007, 2003, 1999 by Saunders, an imprint of Elsevier Inc. All rights reserved.
 Assisting in Ophthalmology Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Apply critical thinking skills in performing patient assessment and care. Explain the differences
Assisting in Ophthalmology Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Apply critical thinking skills in performing patient assessment and care. Explain the differences
Combined Infliximab and Rituximab in Necrotising Scleritis
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
The Effect of Posterior versus Anterior Subtenon Injection of Triamcinolone on Intraocular Pressure in Eyes with Retinal Vein Occlusion
 The Effect of Posterior versus Anterior Subtenon Injection of Triamcinolone on Intraocular Pressure in Eyes with Retinal Vein Occlusion Hamid Fesharaki, MD 1 Farzan Kianersi, MD 1 Hamidreza Riazi, MD 2
The Effect of Posterior versus Anterior Subtenon Injection of Triamcinolone on Intraocular Pressure in Eyes with Retinal Vein Occlusion Hamid Fesharaki, MD 1 Farzan Kianersi, MD 1 Hamidreza Riazi, MD 2
Clinical Practice Guide for the Diagnosis, Treatment and Management of Anterior Eye Conditions. April 2018
 Clinical Practice Guide for the Diagnosis, Treatment and Management of Anterior Eye Conditions This Clinical Practice Guide provides evidence-based information about current best practice in the management
Clinical Practice Guide for the Diagnosis, Treatment and Management of Anterior Eye Conditions This Clinical Practice Guide provides evidence-based information about current best practice in the management
Cataract Surgery in Patients with Uveitis
 Cataract Surgery in Patients with Uveitis Chris Kalogeropoulos MD, PhD, FEBO Professor of Ophthalmology Faculty of Medicine, University of Ioannina President of Hellenic Society for the Study of Ocular
Cataract Surgery in Patients with Uveitis Chris Kalogeropoulos MD, PhD, FEBO Professor of Ophthalmology Faculty of Medicine, University of Ioannina President of Hellenic Society for the Study of Ocular
The Future Is Now: Biologics for Non-Infectious Pediatric Anterior Uveitis
 Pediatr Drugs (2015) 17:283 301 DOI 10.1007/s40272-015-0128-2 REVIEW ARTICLE The Future Is Now: Biologics for Non-Infectious Pediatric Anterior Uveitis Melissa A. Lerman 1 C. Egla Rabinovich 2 Published
Pediatr Drugs (2015) 17:283 301 DOI 10.1007/s40272-015-0128-2 REVIEW ARTICLE The Future Is Now: Biologics for Non-Infectious Pediatric Anterior Uveitis Melissa A. Lerman 1 C. Egla Rabinovich 2 Published
CLINICAL SCIENCES. Antineutrophil Cytoplasmic Antibody Associated Active Scleritis
 CLINICAL SCIENCES Antineutrophil Cytoplasmic Antibody Associated Active Scleritis Lani T. Hoang, MD; Lyndell L. Lim, MBBS, FRANZCO; Brian Vaillant, MD; Dongseok Choi, PhD; James T. Rosenbaum, MD Objective:
CLINICAL SCIENCES Antineutrophil Cytoplasmic Antibody Associated Active Scleritis Lani T. Hoang, MD; Lyndell L. Lim, MBBS, FRANZCO; Brian Vaillant, MD; Dongseok Choi, PhD; James T. Rosenbaum, MD Objective:
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Loss of efficacy during long-term infliximab therapy for sight-threatening childhood uveitis
 Rheumatology 08;47:10 14 Advance Access publication 1 August 08 doi:10.1093/rheumatology/ken298 Concise Report Loss of efficacy during long-term infliximab therapy for sight-threatening childhood uveitis
Rheumatology 08;47:10 14 Advance Access publication 1 August 08 doi:10.1093/rheumatology/ken298 Concise Report Loss of efficacy during long-term infliximab therapy for sight-threatening childhood uveitis
Medical Science. Research Paper. 2nd yr post graduate, Dept. Of Ophthalmology, SVS Medical College
 Dr. A.Narasimha Rao Dr. N.Deepika Dr. D.Chandrakanth Reddy Dr. M. Vijaya Ramaraju ABSTRACT KEYWORDS Research Paper Medical Science Comparative Evaluation of the Anti- Inflammatory Effect of Topical 1 %
Dr. A.Narasimha Rao Dr. N.Deepika Dr. D.Chandrakanth Reddy Dr. M. Vijaya Ramaraju ABSTRACT KEYWORDS Research Paper Medical Science Comparative Evaluation of the Anti- Inflammatory Effect of Topical 1 %
Optical Coherence Tomography (OCT) in Uveitis Piergiorgio Neri, BMedSc, MD, PhD Head Ocular Immunology Unit
 The Eye Clinic Polytechnic University of Marche Head: Prof Alfonso Giovannini November, 1991 Optical Coherence Tomography (OCT) in Uveitis Piergiorgio Neri, BMedSc, MD, PhD Head Ocular Immunology Unit
The Eye Clinic Polytechnic University of Marche Head: Prof Alfonso Giovannini November, 1991 Optical Coherence Tomography (OCT) in Uveitis Piergiorgio Neri, BMedSc, MD, PhD Head Ocular Immunology Unit
Ophthalmology. Juliette Stenz, MD
 Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 55/ July 09, 2015 Page 9665
 RARE PRESENTATION OF BILATERAL CHOROIDAL METASTASIS FROM PRIMARY MUCO-EPIDERMOID CARCINOMA OF THE PAROTID GLAND: A G. Premalatha 1, Ramya Seetamraju 2 HOW TO CITE THIS ARTICLE: G. Premalatha, Ramya Seetamraju.
RARE PRESENTATION OF BILATERAL CHOROIDAL METASTASIS FROM PRIMARY MUCO-EPIDERMOID CARCINOMA OF THE PAROTID GLAND: A G. Premalatha 1, Ramya Seetamraju 2 HOW TO CITE THIS ARTICLE: G. Premalatha, Ramya Seetamraju.
Focus on Ophthalmology Inside the Eye of the Horse
 www.ivis.org Proceedings of the American Association of Equine Practitioners - Focus Meeting Focus on Ophthalmology Inside the Eye of the Horse Raleigh, NC, USA 2012 Next Focus Meetings: August 4-6, 2013
www.ivis.org Proceedings of the American Association of Equine Practitioners - Focus Meeting Focus on Ophthalmology Inside the Eye of the Horse Raleigh, NC, USA 2012 Next Focus Meetings: August 4-6, 2013
PRODUCTION ANIMAL AND EQUINE OPHTHALMOLOGY
 REF. NO. TITLE: C-VO.2 PRODUCTION ANIMAL AND EQUINE OPHTHALMOLOGY VALUE: 10 CREDITS NOTIONAL STUDY HOURS: 100 This module is intended to cover the theoretical knowledge of both Production Animal and Equine
REF. NO. TITLE: C-VO.2 PRODUCTION ANIMAL AND EQUINE OPHTHALMOLOGY VALUE: 10 CREDITS NOTIONAL STUDY HOURS: 100 This module is intended to cover the theoretical knowledge of both Production Animal and Equine
The Inflammatory Role of Endotoxin in Rabbit Gram-Negative Bacterial Endophthalmitis
 The Inflammatory Role of Endotoxin in Rabbit Gram-Negative Bacterial Endophthalmitis Dean R. Jacobs and Howard B. Cohen The authors used the limulus lysate assays to measure the amount of gram-negative
The Inflammatory Role of Endotoxin in Rabbit Gram-Negative Bacterial Endophthalmitis Dean R. Jacobs and Howard B. Cohen The authors used the limulus lysate assays to measure the amount of gram-negative
Uveitis in childhood is a potentially blinding condition with
 Immunology and Microbiology Infiltration of Plasma Cells in the Iris of Children With ANA-Positive Anterior Uveitis Viera Kalinina Ayuso, 1 Marijke R. van Dijk, 2 and Joke H. de Boer 1 1 Department of
Immunology and Microbiology Infiltration of Plasma Cells in the Iris of Children With ANA-Positive Anterior Uveitis Viera Kalinina Ayuso, 1 Marijke R. van Dijk, 2 and Joke H. de Boer 1 1 Department of
Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO
 Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO brujic@prodigy.net Summary As optometry s role in health care increases, so does our responsibility to appropriately diagnose and appropriately
Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO brujic@prodigy.net Summary As optometry s role in health care increases, so does our responsibility to appropriately diagnose and appropriately
Posner-Schlossman syndrome: a 10-year review of clinical experience
 Original Article Page 1 of 7 Posner-Schlossman syndrome: a 10-year review of clinical experience Ling Wang 1, Gang Yin 2, Dabo Wang 1, Zhiying Yu 1 1 Department of Ophthalmology, Affiliated Hospital of
Original Article Page 1 of 7 Posner-Schlossman syndrome: a 10-year review of clinical experience Ling Wang 1, Gang Yin 2, Dabo Wang 1, Zhiying Yu 1 1 Department of Ophthalmology, Affiliated Hospital of
Course, complications, and outcome of juvenile arthritis related uveitis
 Major Articles Course, complications, and outcome of juvenile arthritis related uveitis Kourosh Sabri, MB, ChB, FRCOphth, a Rotraud K. Saurenmann, MD, b,a Earl D. Silverman, MD, FRCPC, b,c and Alex V.
Major Articles Course, complications, and outcome of juvenile arthritis related uveitis Kourosh Sabri, MB, ChB, FRCOphth, a Rotraud K. Saurenmann, MD, b,a Earl D. Silverman, MD, FRCPC, b,c and Alex V.
Ophthalmology Subcommittee of PTAC Meeting held 30 October (minutes for web publishing)
 Ophthalmology Subcommittee of PTAC Meeting held 30 October 2014 (minutes for web publishing) Ophthalmology Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology
Ophthalmology Subcommittee of PTAC Meeting held 30 October 2014 (minutes for web publishing) Ophthalmology Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology
Eye (2013) 27, & 2013 Macmillan Publishers Limited All rights reserved X/13 S Basu, S Nayak, TR Padhi and T Das
 (2013) 27, 657 662 & 2013 Macmillan Publishers Limited All rights reserved 0950-222X/13 www.nature.com/eye Progressive ocular inflammation following antitubercular therapy for presumed ocular tuberculosis
(2013) 27, 657 662 & 2013 Macmillan Publishers Limited All rights reserved 0950-222X/13 www.nature.com/eye Progressive ocular inflammation following antitubercular therapy for presumed ocular tuberculosis
High-speed optical coherence tomography as a reliable adjuvant tool to grade ocular anterior chamber inflammation.
 Thomas Jefferson University Jefferson Digital Commons Wills Eye Institute Papers Wills Eye Institute 3-2014 High-speed optical coherence tomography as a reliable adjuvant tool to grade ocular anterior
Thomas Jefferson University Jefferson Digital Commons Wills Eye Institute Papers Wills Eye Institute 3-2014 High-speed optical coherence tomography as a reliable adjuvant tool to grade ocular anterior
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 19 September 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 19 September 2012 OZURDEX 700 micrograms, intravitreal implant in applicator Box of 1 sachet with applicator (CIP:
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 19 September 2012 OZURDEX 700 micrograms, intravitreal implant in applicator Box of 1 sachet with applicator (CIP:
Efficacy of latanoprost in management of chronic angle closure glaucoma. Kumar S 1, Malik A 2 Singh M 3, Sood S 4. Abstract
 Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Indian Journal of Basic & Applied Medical Research; June 2013: Issue-7, Vol.-2, P
 Original article Clinial Study of different types of Uveitis in Western Maharashtra *Yellambkar ST, *Chavan WM,**Tayade MC *Dept. of Ophthalmology & **Department of Physiology, Rural Medical College, Pravara
Original article Clinial Study of different types of Uveitis in Western Maharashtra *Yellambkar ST, *Chavan WM,**Tayade MC *Dept. of Ophthalmology & **Department of Physiology, Rural Medical College, Pravara
INVELTYS (loteprednol etabonate ophthalmic suspension) 1%, for topical ophthalmic use Initial U.S. Approval: 1998
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use INVELTYS safely and effectively. See full prescribing information for INVELTYS. INVELTYS (loteprednol
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use INVELTYS safely and effectively. See full prescribing information for INVELTYS. INVELTYS (loteprednol
Complete Visual Rehabilitation in a Patient with No Light Perception after Surgical Management of a Penetrating Open-Globe Injury: A Case Report
 Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
