Parameters of Care: Clinical Practice Guidelines for Oral and Maxillofacial Surgery (AAOMS ParCare 2017) TEMPOROMANDIBULAR JOINT SURGERY
|
|
|
- Winifred Dorsey
- 6 years ago
- Views:
Transcription
1 Parameters of Care: Clinical Practice Guidelines for Oral and Maxillofacial Surgery () TEMPOROMANDIBULAR JOINT SURGERY Copyright 2017 by the American Association of Oral and Maxillofacial Surgeons. This document may not be copied or reproduced without the express written permission of the American Association of Oral and Maxillofacial Surgeons. All rights reserved. J Oral Maxillofac Surg THIS SECTION IS 1 OF 11 CLINICAL SECTIONS INCLUDED IN AAOMS PARCARE 2017, WHICH IS VIEWED AS A LIVING DOCUMENT APPLICABLE TO THE PRACTICE OF ORAL AND MAXILLOFACIAL SURGERY. IT WILL BE UPDATED AT DESIGNATED INTERVALS TO REFLECT NEW INFORMATION CONCERNING THE PRACTICE OF ORAL AND MAXILLOFACIAL SURGERY.
2 INTRODUCTION Temporomandibular joint (TMJ) surgery is indicated for the treatment of a wide range of pathologic conditions, including developmental and acquired deformities, internal derangements, arthritis, functional abnormalities, ankylosis, and infection. Parameters of care related to management of tumors of the TMJ are in the Diagnosis and Management of Pathological Conditions chapter, and those for fractures of the mandibular condyle are in the Trauma Surgery chapter. It is recognized that many patients undergoing TMJ surgeries have unique pain control requirements. As such, it may be appropriate to discuss a specific plan for postoperative pain control management. Such therapy might include the surgeon managing the patient s pain with narcotic prescriptions for a specified period, followed by referral to a pain control center. Some surgeons may wish to develop a contract with these patients that reviews the planning, timing and other specifics of such therapy. The parameters for TMJ surgery are based on the descriptions of pathologic entities and modalities for their treatment that have appeared in peer-reviewed medical literature. This field has undergone a considerable evolution during the past 15 to 20 years. Basic and clinical research is continuing to increase the potential for successful surgical results. GENERAL CRITERIA, PARAMETERS, AND CONSIDERATIONS FOR TEMPOROMANDIBULAR JOINT SURGERY INFORMED CONSENT: All surgery must be preceded by the patient's or legal guardian s consent, unless an emergent situation dictates otherwise. These circumstances should be documented in the patient s record. Informed consent is obtained after the patient or the legal guardian has been informed of the indications for the procedure(s), the goals of treatment, the known benefits and risks of the procedure(s), the factors that may affect the risk, the treatment options, and the favorable outcomes. PERIOPERATIVE ANTIBIOTIC THERAPY: In certain circumstances, the use of antimicrobial rinses and systemic antibiotics may be indicated to prevent infections related to surgery. The decision to employ prophylactic perioperative antibiotics is at the discretion of the treating surgeon and should be based on the patient s clinical condition as well as other comorbidities which may be present. DEALING WITH NEUROLOGIC DEFECITS: Injuries to the terminal branches of the trigeminal nerve (eg, lingual, inferior alveolar, long buccal nerves), as well as the facial nerve, are known risks of oral and maxillofacial surgery. It should be noted that the presence of a pathologic craniomaxillofacial condition, dentoskeletal or craniofacial abnormality, or traumatic craniomaxillofacial injury may result in nerve injury prior to surgical management. In addition, the use of local anesthesia (eg, mandibular block) may increase the risk of nerve injury. Most nerve injuries resolve spontaneously, but some do not, and these may require consideration for non-surgical and/or surgical intervention. Microneurosurgical repair should be considered when the disability is of concern to the patient, and there is clinical evidence of moderate, severe, or complete neurosensory impairment of various areas of the orofacial region (eg, lips, chin, tongue); paresis or paralysis of facial muscles; loss, decreased, or abnormal taste sensation; or neuropathic pain of peripheral origin. Surgical repair should incorporate specialized microsurgical techniques (eg, operating magnification, nerve grafting), when indicated. Also see the Reconstructive Surgery chapter. USE OF IMAGING MODALITIES: Imaging modalities may include panoramic radiograph, periapical and/or occlusal radiographs, maxillary and/or mandibular radiographs, computed tomography, cone beam computed tomography, positron emission tomography, positron emission tomography/computed tomography, radionucleotide imaging, and magnetic resonance imaging. In determining studies to be performed for imaging purposes, principles of ALARA (as low as reasonably achievable) should be followed.
3 USE OF ALLOPLASTIC MATERIALS: Partial or complete reconstruction of the temporomandibular joint may be accomplished using a wide variety of autogenous tissues, xenografts, or alloplastic implants. When alloplastic materials are used, they should be employed following the manufacturer s instructions and consistent with indications approved by the U.S. Food and Drug Administration (FDA). When a treating surgeon elects to use an alloplastic material outside these approved indications, he/she should base the decision on applicable scientific principles and available medical knowledge, and should document these considerations in the patient s record. Additionally, only the use of FDA approved devices is recommended. DOCUMENTATION: The includes documentation of objective findings, diagnoses, and patient management interventions. The ultimate judgment regarding the appropriateness of any specific procedure must be made by the individual surgeon in light of the circumstances presented by each patient. Understandably, there may be good clinical reasons to deviate from these parameters. When a surgeon chooses to deviate from an applicable parameter based on the circumstances of a particular patient, he/she is well advised to note in the patient's record the reason for the procedure followed. Moreover, it should be understood that adherence to the parameters does not guarantee a favorable outcome. GENERAL THERAPEUTIC GOALS FOR TEMPOROMANDIBULAR JOINT SURGERY: A. Improve function and form B. Limited period of disability C. Improved range of jaw motion and/or function D. Appropriate understanding by patient (family) of treatment options and acceptance of treatment plan E. Appropriate understanding and acceptance by patient (family) of favorable outcomes and known risks and complications F. Reduction in pain G. Improved Quality of Life GENERAL FACTORS AFFECTING RELATIVE RISK DURING TEMPOROMANDIBULAR JOINT SURGERY: A. Degree of patient and/or family understanding of the origin and natural course of the condition or disorder and therapeutic goals and acceptance of proposed treatment B. Presence of coexisting major systemic disease (eg, disease that increases a patient's American Society of Anesthesiologists classification to II, III, or IV as detailed in the Patient Assessment chapter) C. Age of patient D. Presence of concomitant facial pain (eg, dental pain, earache, headache) E. Presence of parafunctional habit F. Existing drug or alcohol dependence G. Issues of secondary gain (eg, pending litigation) H. Chronic pain disorders (eg, pain in excess of 3 months duration) I. Presence of malocclusion J. Presence of deformity or pathology of the TMJ K. Presence of concomitant skeletal deformity L. History of previous orthodontics, orthognathic surgery, or TMJ surgery M. History of sensory or motor nerve abnormality (eg, temporary or permanent) N. History of infection of surgical site O. Presence of local or systemic conditions that may interfere with the normal healing process and subsequent tissue homeostasis (eg, previously irradiated tissue, diabetes mellitus, chronic renal disease, liver disease, blood disorder, pregnancy, steroid therapy, contraceptive medication, immunosuppression, malnutrition, Ehlers-Danlos syndrome, fibromyalgia) P. Prolonged period of TMJ disuse (eg, ankylosis) Q. History of maxillofacial trauma GENERAL FAVORABLE THERAPEUTIC OUTCOMES FOR TEMPOROMANDIBULAR JOINT SURGERY:
4 A. Improved masticatory function and facial form B. A level of pain that is of little or no concern to the patient and preferably measured objectively (eg, visual analog scale) C. Improved mandibular function that is compatible with mastication, deglutition, speech, and oral hygiene D. A stable occlusion E. Limited period of disability F. Limit further morbidity G. Patient (family) acceptance of procedure and understanding of outcomes H. Improved quality of life GENERAL KNOWN RISKS AND COMPLICATIONS OF TEMPOROMANDIBULAR JOINT SURGERY: A. Unplanned admission to intensive care unit after elective surgery B. Unplanned intubation for longer than 12 hours after surgery C. Reintubation or tracheostomy after surgery D. Emergency tracheostomy (eg, ankylosis, trismus, unable to maintain airway) E. Use of parenteral drugs and/or fluids for longer than 72 hours after elective surgery F. Failure to ambulate within 48 hours of elective surgery G. Facial and/or trigeminal nerve dysfunction after surgery (eg, temporary or permanent facial muscle weakness resulting from surgery). The most common resulting problems are an inability to wrinkle the brow, raise the eyebrow, or gain tight closure of the eyelids and numbness (temporary or permanent) of certain areas of the skin in the region of the joint and sometimes in more remote areas of the face and scalp H. Facial fracture during or after surgery I. Unplanned exploratory procedures associated with surgery J. Dental injury during surgery K. Ocular injury during surgery and postoperative sequelae (eg, corneal abrasion, keratoconjunctivitis, blindness) L. Repeat oral and/or maxillofacial surgery M. Core temperature of greater than 101 F 72 hours after elective surgery N. Postsurgical radiograph indicating presence of foreign body O. Unplanned transfusion(s) of blood or blood components during or after surgery P. Readmission for complications or incomplete management of problems on previous hospitalization Q. Development of chronic pain disorder R. Increased and/or persistent pain S. Postoperative development of adhesions, heterotopic bone (reactive bone), or ankylosis within the joint space, which may cause continued jaw dysfunction, decreased range of jaw movement, difficulty chewing, and pain requiring further treatment T. Development of TMJ internal derangement U. New or worsened malocclusion V. Imaging evidence of further degenerative joint changes and development of adhesions (scar tissue), joint arthritis (contralateral joint in unilateral cases), or osteomyelitis of the jaw (bone infection) W. Significant joint noise with or without increased pain and/or dysfunction X. Ear pain and/or dysfunction Y. Development or worsening of a parafunctional habit Z. Abnormal mandibular growth (eg, excessive, restricted) AA. Prolonged period of disability BB. Infection CC. Development of complex regional pain syndrome DD. Foreign body reaction or allergic reaction and rejection of the implant, wear, displacement, breakage, or loosening of alloplastic device components EE. Ear problems, including inflammation of the canal, middle or inner ear infections, perforation of the ear drum, temporary or permanent hearing loss, ringing in the ears, or equilibrium problems FF. Postoperative and/or future treatments are not limited to but may include the following: physical therapy,
5 bite splint therapy, restorative or reconstructive dentistry, orthodontia, orthognathic surgery (jaw repositioning surgery), and further reconstructive TMJ surgery GG. Respiratory and/or cardiac arrest HH. Death SPECIAL CONSIDERATIONS FOR PEDIATRIC TEMPOROMANDIBULAR JOINT SURGERY Orofacial pains due to TMJ conditions are less common in young children compared with teenagers and adults. Internal derangements are uncommon. TMJ conditions other than congenital deformities (eg, hemifacial microsomia) or acquired anatomical abnormalities (eg, fractures, bony ankylosis, idiopathic condylar resorption) are very uncommon in children. When painful TMJ conditions do occur, underlying psychopathologic factors are more frequent. Informed consent issues specific to children as discussed in the Patient Assessment chapter are applicable for TMJ surgery. Imaging is frequently required to assess and treat pediatric patients. Every effort to minimize the frequency and complexity of imaging studies should be employed to reduce radiation exposure in this patient population. Whenever possible contrast should be avoided unless clinically indicated to further reduce the radiation dose and risks associated with the use of contrast. Masticatory muscle hyperactivity in children may present as nighttime grinding or bruxism, and this is common in the deciduous or mixed dentition stages of dental development. Children may complain of headaches, earaches, or jaw stiffness in the morning on awakening. Usually this can be managed with a night guard or biofeedback and appropriate medications, when indicated. Symptomatic clicking generally can be eliminated or diminished with midline hinge axis opening exercises to overcome an abnormal opening pattern. The origin of headache in the pediatric patient is primarily related to the sinus, eye, vascular system or cervicalgia. Any operative procedure on the TMJ of a growing child must consider the ultimate effect of the treatment on growth and development of the mandible and face. Management of ankylosis, juvenile idiopathic arthritis, degenerative joint disease (very rare in children), infectious arthritis, mandibular dislocation, and condylar resorption is similar in children and adults. Juvenile idiopathic arthritis involvement of the TMJs is not uncommon. These children require frequent monitoring and occasional imaging (MRI with gadolinium contrast) to manage their disease. Medical management can include systemics such as NSAIDs, disease-modifying antirheumatoid drugs (eg, methotrexate), and biologics (eg, adalimumab [Humira ]). Steroid injections may be required as a primary treatment, or for periodic management of exacerbations of disease activity to augment their medical management. Occasionally surgery is required to debride or reconstruct joints destroyed by this disease. The goal of reconstructing the TMJ and ramus-condyle unit in children includes the restoration of normal functioning anatomy. This is true regardless of the underlying condition (eg, tumor, traumatic defect, developmental defect). Therefore, autogenous donor sites with growth potential (eg, costochondral grafts) are recommended although alloplastic reconstruction may be considered in some children where the benefit of improving hypomobility outweighs the risk of asymmetric growth with the knowledge that additional surgical procedures may be necessary. MASTICATORY MUSCLE DISORDERS Masticatory muscle disorders can result in myofascial pain and/or muscle splinting. These disorders are the most common expression of temporomandibular disorders and may occur in combination with joint abnormalities or other pathologic conditions. Management of these disorders is nonsurgical, especially in children. When masticatory muscle disorders occur in combination with joint abnormalities or other pathologic conditions, the management of these disorders must be incorporated into the overall treatment plan. Pretreatment therapeutic goals are determined individually for each patient. I. Indications for Therapy for Masticatory Muscle Disorders
6 May include one or more of the following: A. Extra-articular pain related to muscles of the head and neck region B. Earaches, headaches, masticatory or facial myalgias C. Restricted masticatory function D. Restricted range of jaw motion E. Associated TMJ abnormalities or pathology F. Presence of sleep bruxism II. Specific Therapeutic Goals for Masticatory Muscle Disorders The goal of therapy is to restore form and/or function. However, risk factors and potential complications may preclude complete restoration of form and/or function. A. Presence of a general therapeutic goal, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Improved range of jaw motion and/or function C. Adequate control of pain in muscles of the head and neck region III. Specific Factors Affecting Risk for Masticatory Muscle Disorders Severity factors that increase risk and the potential for known complications: A. Presence of a general factor affecting risk, as listed in the section entitled General Criteria, Parameters, and Considerations for B. History of previous maxillofacial trauma IV. Indicated Therapeutic Parameters for Masticatory Muscle Disorders Some reduction in symptoms is expected within 3 months. If the symptoms persist or escalate during this period, further assessment of contributing etiologic and risk factors should be considered. A. The pretreatment assessment includes, at a minimum: 1. General history and physical examination, as detailed in the Patient Assessment chapter 2. A focused history and physical examination of the TMJ region to determine if pathology is present 3. An imaging examination, if indicated, based on the history and physical findings. The examination may include but is not limited to the following: screening panoramic radiography, cephalometric radiography, conventional tomography, computed tomography (CT), cone beam computed tomography, radionuclide scanning, and magnetic resonance imaging (MRI). The following procedures for the management of masticatory muscle disorders are not listed in order of preference: B. Nonsurgical Management 1. Patient education (eg, stress reduction, dietary recommendations, jaw rest, control of parafunctional jaw habits) 2. Medication (eg, nonsteroidal anti-inflammatory drugs [NSAIDs], analgesics, muscle relaxants, tricyclic antidepressants, anticonvulsants) 3. Physical medicine (eg, physical therapy, massage, heat, cold, ultrasonography, trigger point injections, neuromuscular blocking agents, dry needling, low level laser therapy) 4. Behavioral modification (eg, stress reduction, work modification, counseling, biofeedback, psychotherapy) 5. Orthopedic appliances (eg, splints) 6. Management of dental abnormalities 7. Surgery, other than manipulative treatment therapy, is not indicated for these disorders. 8. Instructions for posttreatment care and follow-up 9. Treatment of referred pain (eg cervical pain)
7 V. Outcome Assessment Indices for Masticatory Muscle Disorders Indices are used by the specialty to assess aggregate outcomes of care. Outcomes are assessed through clinical evaluation and may include an imaging evaluation. A. Favorable therapeutic outcomes General favorable therapeutic outcomes, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Known risks and complications associated with therapy Presence of a general known risk and/or complication, as listed in the section entitled General Criteria, Parameters, and Considerations for INTERNAL DERANGEMENT Surgical intervention for internal derangement is indicated only when nonsurgical therapy has been ineffective and pain and/or dysfunction are moderate to severe. Surgery is not indicated for asymptomatic or minimally symptomatic patients. Surgery also is not indicated for preventive reasons in patients without pain and with satisfactory function. Pretreatment therapeutic goals are determined individually for each patient. I. Indications for Therapy for Internal Derangement May include one or more of the following: A. Moderate-to-severe pain 1. Temporomandibular pain 2. Preauricular pain 3. Referred pain (eg, earaches) 4. Masticatory muscle pain (see Masticatory Muscle Disorders section) B. Dysfunction that is disabling and characterized by any of the following: 1. Restricted range of jaw motion (eg, locking of the joint: acute, chronic, intermittent, persistent) 2. Excessive range of jaw motion (eg, hypermobility; chronic dislocation: acute, chronic, intermittent, persistent) 3. Joint noises (eg, clicking, popping, crepitation) associated with pain 4. Abnormal masticatory function (eg, painful chewing) C. Imaging evidence of internal derangement D. Arthroscopic evidence of internal derangement E. Need for orthognathic surgery II. Specific Therapeutic Goals for Internal Derangement The goal of therapy is to restore form and/or function. However, risk factors and potential complications may preclude complete restoration of form and/or function. A. Presence of a general therapeutic goal, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Improved function C. Limited pain in the joint D. Elimination or reduction of noise in the joint III. Specific Factors Affecting Risk for Internal Derangement Severity factors that increase risk and the potential for known complications: A. Presence of a general factor affecting risk, as listed in the section entitled General Criteria, Parameters, and Considerations for
8 B. Presence of alloplast or autograft C. History of previous temporomandibular operative procedures D. History of previous maxillofacial trauma E. History of orthognathic surgery IV. Indicated Therapeutic Parameters for Internal Derangement A. The pretreatment assessment includes, at a minimum: 1. General history and physical examination, as detailed in the Patient Assessment chapter 2. A focused history and physical examination of the TMJ region to determine the presence of indications for care for internal derangement and to identify factors affecting risks 3. An imaging examination, if indicated, based on the history and physical findings. The examination may include but is not limited to the following: panoramic radiography, cephalometric radiography, conventional tomography, arthrography, CT, cone beam computed tomography, radionuclide scanning, and/or MRI. The following procedures for the management of internal derangement are not listed in order of preference: B. Nonsurgical management 1. Patient education (eg, stress reduction, dietary recommendations, jaw rest) 2. Medication (eg, NSAIDs, analgesics, muscle relaxants) 3. Physical medicine (eg, physical therapy, massage, heat, cold, ultrasonography, trigger point injections) 4. Intracapsular diagnostic and therapeutic injections 5. Behavioral modification (eg, stress reduction, work modification, counseling, biofeedback, psychotherapy) 6. Orthopedic appliances (eg, splints) 7. Management of dental abnormalities 8. Diagnostic records to determine progression of the disease (eg, serial bite registration and models, imaging studies in selected cases) C. Surgical management 1. Examination and observation under anesthesia 2. Manipulation 3. Arthrocentesis 4. Arthroscopic surgery 5. Arthrotomy or arthroplasty a. Disk repair procedures b. Diskectomy without replacement c. Diskectomy with replacement d. Articular surface recontouring (condyle/eminence) 6. Mandibular condylotomy may be considered in some situations such as chronic closed lock with or without pain and intra-articular pain secondary to internal derangement 7. Orthognathic surgery as an adjunct to the management of temporomandibular joint disorders 8. Correction of skeletal jaw deformities may be indicated before or after definitive joint treatment D. Posttreatment management 1. Wound care 2. Physical therapy 3. Pain management 4. Diet and oral hygiene management 5. Orthotic appliance 6. Patient reassessment 7. Instructions for posttreatment care and follow-up V. Outcome Assessment Indices for Internal Derangement Indices are used by the specialty to assess aggregate outcomes of care. Outcomes are assessed through clinical evaluation and may include an imaging evaluation.
9 A. Favorable therapeutic outcomes 1. General favorable therapeutic outcomes, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Improved mandibular function 3. Acceptable clinical appearance (eg, absence of motor deficits, absence of hypertrophic scar formation, absence of facial asymmetry or deformity) B. Known risks and complications associated with therapy 1. Presence of a general known risk and/or complication, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Removal of autograft or alloplast 3. Ankylosis 4. Need for additional surgical intervention DEGENERATIVE JOINT DISEASE Surgical intervention is indicated only when nonsurgical therapy has been ineffective and pain and/or dysfunction are moderate to severe. Surgery is not indicated for asymptomatic or minimally symptomatic patients. Surgery also is not indicated for preventive reasons in patients without pain and with satisfactory function. Pretreatment therapeutic goals are determined individually for each patient. I. Indications for Therapy for Degenerative Joint Disease May include one or more of the following: A. Moderate-to-severe pain 1. Temporomandibular pain 2. Preauricular pain 3. Referred pain (eg, earaches) 4. Masticatory muscle pain (see Masticatory Muscle Disorders section) B. Dysfunction that is disabling and characterized by any of the following: 1. Restricted range of jaw motion (eg, locking of the joint: acute, chronic, intermittent, persistent) 2. Excessive range of jaw motion (eg, hypermobility; chronic dislocation: acute, chronic, intermittent, and persistent) 3. Joint noises (eg, clicking, popping, crepitation) 4. Abnormal masticatory function (eg, painful chewing) C. Imaging evidence of arthritic condition D. Arthroscopic evidence of arthritic condition E. Failed alloplastic implants F. Failed prior TMJ surgery G. Need for orthognathic surgery II. Specific Therapeutic Goals for Degenerative Joint Disease The goal of therapy is to restore form and/or function. However, risk factors and potential complications may preclude complete restoration of form and/or function. A. Presence of a general therapeutic goal, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Improved function C. Improved pain in the joint D. Improved maxillomandibular relationship E. Limited progression of the disease III. Specific Factors Affecting Risk for Degenerative Joint Disease
10 Severity factors that increase risk and the potential for known complications: A. Presence of a general factor affecting risk, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Presence of an alloplast or autograft C. History of previous maxillofacial trauma D. Degenerative disease affecting other joints E. Prior temporomandibular joint surgery F. History of prior orthognathic surgery (PCR) IV. Indicated Therapeutic Parameters for Degenerative Joint Disease A. The pretreatment assessment includes, at a minimum: 1. General history and physical examination, as detailed in the Patient Assessment chapter 2. Focused history and physical examination of the TMJ region to determine the presence of indications for care for degenerative joint disease and to identify factors affecting risks 3. An imaging examination, if indicated, based on the history and physical findings. The examination may include but is not limited to the following: panoramic radiography, cephalometric radiography, conventional tomography, arthrography, CT, cone beam computed tomography, radionuclide scanning, and/or MRI. The following procedures for the management of degenerative joint disease are not listed in order of preference: B. Nonsurgical management 1. Patient education (eg, stress reduction, dietary recommendations, jaw rest) 2. Medication (eg, NSAIDs, analgesics, muscle relaxants, antiarthritics, steroids) 3. Physical medicine (eg, physical therapy, massage, heat, cold, ultrasonography, trigger point injections) 4. Intracapsular diagnostic and therapeutic injections 5. Behavioral modification (eg, stress reduction, work modification, counseling, biofeedback, psychotherapy) 6. Orthopedic appliances (eg, splints) 7. Management of dental abnormalities 8. Appropriate diagnostic records to determine progression of the disease (eg, serial bite registration and models, imaging studies in selected cases) C. Surgical management 1. Manipulation 2. Arthrocentesis 3. Arthroscopic surgery 4. Arthrotomy or arthroplasty a. Disk repair procedures b. Diskectomy without replacement c. Diskectomy with replacement d. Arthroplasty e. Removal of failed alloplastic implant 5. Condylectomy (partial or total, with or without replacement) 6. Orthognathic surgery (the correction of skeletal jaw deformities may be indicated before or after definitive joint treatment as an adjunct to the management of temporomandibular disorders) 7. Total alloplastic or autogenous joint replacement D. Posttreatment management 1. Wound care 2. Pain management 3. Diet and oral hygiene management 4. Physical therapy
11 Occlusal management 6. Patient reassessment 7. Instructions for posttreatment care and follow-up V. Outcome Assessment Indices for Degenerative Joint Disease Indices are used by the specialty to assess aggregate outcomes of care. Outcomes are assessed through clinical evaluation and may include an imaging evaluation. A. Favorable therapeutic outcomes 1. General favorable therapeutic outcomes, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Acceptable clinical appearance (eg, absence of motor deficits, absence of hypertrophic scar formation, absence of facial asymmetry or deformity) 3. Improved mandibular function (eg, maximum incisal opening, lateral and protrusive excursions) B. Known risks and complications associated with therapy 1. Presence of a general know risk and/or complication, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Removal of autograft or alloplast 3. Ankylosis RHEUMATOID ARTHRITIS Rheumatoid arthritis is one of a constellation of systemic autoimmune diseases that may affect the TMJ. In many cases, these conditions should be managed with the close cooperation of the patient s physician and/or rheumatologist. It is important to distinguish whether the condylar resorption is active (progressive) or stable (nonprogressive). In its most severe form, rheumatoid arthritis may result in ankylosis and/or condylar destruction with resultant mandibular retrognathism, anterior skeletal open bite, and painful limitation of function. Surgical intervention for arthritic conditions is indicated only when nonsurgical therapy has been ineffective and pain and/or dysfunction are moderate to severe. Surgery is not indicated for asymptomatic or minimally symptomatic patients. Surgery also is not indicated for preventive reasons in patients without pain and with satisfactory function. Pretreatment therapeutic goals are determined individually for each patient. I. Indications for Therapy for Rheumatoid Arthritis May include one or more of the following: A. Moderate-to-severe pain 1. Temporomandibular pain 2. Preauricular pain 3. Referred pain (eg, earaches) 4. Masticatory muscle pain (see Masticatory Muscle Disorders section) B. Dysfunction that is disabling and characterized by any of the following: 1. Restricted range of jaw motion (eg, locking of the joint: acute, chronic, intermittent, persistent) 2. Excessive range of jaw motion (eg, hypermobility, chronic dislocation: acute, chronic, intermittent, persistent) 3. Joint noises (eg, clicking, popping, crepitation) 4. Abnormal masticatory function (eg, painful chewing, malocclusion) 5. Joint swelling and/or effusion C. Imaging evidence of arthritic process D. Maxillofacial deformity
12 II. Specific Therapeutic Goals for Rheumatoid Arthritis The goal of therapy is to restore form and/or function. However, risk factors and potential complications may preclude complete restoration of form and/or function. A. Presence of a general therapeutic goal, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Limited pain in the joint C. Improved maxillomandibular function D. Corrected or improved associated maxillofacial relationship E. Limited progression of the disease III. Specific Factors Affecting Risk for Rheumatoid Arthritis Severity factors that increase risk and the potential for known complications: A. Presence of a general factor affecting risk, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Active process of resorption C. Ankylosis D. Presence of alloplast or autograft E. Rheumatoid disease affecting other joints IV. Indicated Therapeutic Parameters for Rheumatoid Arthritis A. The pretreatment assessment includes, at a minimum: 1. General history and physical examination, as detailed in the Patient Assessment chapter 2. Focused history and physical examination of the TMJ region to determine the presence of indications for care for rheumatoid arthritis and to identify factors affecting risks 3. Appropriate laboratory studies to confirm the diagnosis of rheumatoid arthritis (eg, antinuclear antibody, sedimentation rate, rheumatoid factor) 4. An imaging examination, if indicated, based on the history and physical findings. The examination may include but is not limited to the following: panoramic radiography, cephalometric radiography, conventional tomography, arthrography, CT, cone beam computed tomography, radionuclide scanning, and/or MRI 5. Appropriate diagnostic records to determine progression of the disease (eg, serial bite registration and models, imaging studies, laboratory studies) The following procedures for the management of rheumatoid arthritis are not listed in order of preference: B. Nonsurgical management 1. Patient education (eg, stress reduction, dietary recommendations, jaw rest) 2. Medication (eg, NSAIDs, analgesics, muscle relaxants, antiarthritics, steroids) 3. Physical medicine (eg, physical therapy, massage, heat, cold, ultrasonography, trigger point injections) 4. Intracapsular diagnostic and therapeutic injections 5. Behavioral modification (eg, stress reduction, work modification, counseling, biofeedback, psychotherapy) 6. Orthopedic appliances (eg, splints) 7. Management of dental abnormalities 8. Appropriate diagnostic records to determine progression of the disease (eg, serial bite registration and models, imaging studies in selected cases) C. Surgical management The activity of the systemic disease must be considered prior to surgical management of the TMJ. 1. Active (progressive) TMJ disease
13 a. Arthrocentesis b. Arthroscopic surgery c. Biopsy d. Arthroplasty e. Total alloplastic or autogenous graft joint replacement 2. Stable (nonprogressive) TMJ disease a. Arthrocentesis b. Arthroscopic surgery c. Biopsy d. Arthroplasty e. Orthognathic surgery f. Total alloplastic or autogenous graft joint replacement D. Posttreatment management 1. Wound care 2. Pain management 3. Diet and oral hygiene management 4. Physical therapy 5. Ongoing rheumatologic management 6. Occlusal management 7. Patient reassessment 8. Instructions for posttreatment care and follow-up V. Outcome Assessment Indices for Rheumatoid Arthritis Indices are used by the specialty to assess aggregate outcomes of care. Outcomes are assessed through clinical evaluation and may include an imaging evaluation. A. Favorable therapeutic outcomes 1. General favorable therapeutic outcomes, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Acceptable clinical appearance (eg, absence of motor deficits, absence of hypertrophic scar formation, absence of facial asymmetry or deformity) 3. Improved mandibular function (eg, maximum incisal opening, lateral and protrusive excursions) B. Known risks and complications associated with therapy 1. Presence of a general known risk and/or complication, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Removal of autograft or alloplast 3. Ankylosis INFECTIOUS ARTHRITIS The management of infectious arthritis depends on whether the condition is acute or chronic and primary or secondary. Treatment objectives are directed toward the elimination of causes. Surgical intervention for infectious arthritis is indicated only when nonsurgical therapy has been ineffective and pain and/or dysfunction are moderate to severe. Pretreatment therapeutic goals are determined individually for each patient. I. Indications for Therapy for Infectious Arthritis May include one or more of the following: A. Evidence of localized or systemic infection B. Moderate-to-severe pain
14 Temporomandibular pain 2. Preauricular pain 3. Referred pain (eg, earaches) 4. Masticatory muscle pain (see Masticatory Muscle Disorders section) C. Dysfunction that is disabling and characterized by any of the following: 1. Restricted range of jaw motion (eg, hypomobility: acute, chronic, intermittent, persistent) 2. Joint noises (eg, crepitation) 3. Abnormal masticatory function (eg, painful chewing, malocclusion) 4. Swelling, erythema, suppuration, and/or joint effusion D. Imaging evidence of infectious process, failed prosthesis, or foreign body E. Maxillofacial deformity II. Specific Therapeutic Goals for Infectious Arthritis The goal of therapy is to restore form and/or function. However, risk factors and potential complications may preclude complete restoration of form and/or function. A. Presence of a general therapeutic goal, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Elimination of infection C. Removal of any foreign body D. Alleviation or reduction in pain in the joint E. Elimination or reduction in noise in the joint F. Limited progression of disease G. Corrected malocclusion H. Corrected or improved associated maxillofacial deformity III. Specific Factors Affecting Risk for Infectious Arthritis Severity factors that increase risk and the potential for known complications: A. Presence of a general factor affecting risk, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Virulence of microorganisms C. Compromised host defenses D. Presence of alloplast or autograft E. Extent of infection IV. Indicated Therapeutic Parameters for Infectious Arthritis The source of the infection (eg, extension of an otologic infection), systemic manifestations of the infection (eg, septicemia), presence of systemic disease (eg, diabetes mellitus), and host response (eg, human immunodeficiency virus infection, immunosuppression) all must be considered before surgical management of the infected TMJ. A. The pretreatment assessment includes, at a minimum: 1. General history and physical examination, as detailed in the Patient Assessment chapter 2. Focused history and physical examination of the TMJ region to determine the presence of indications for care for infectious arthritis and to identify factors affecting risks 3. Appropriate laboratory studies to confirm the diagnosis of infectious arthritis (eg, white blood cell count by serum or aspiration, Gram stain, bacterial culture, and sensitivity) 4. An imaging examination, if indicated, based on the history and physical findings. The examination may include but is not limited to the following: panoramic radiography, cephalometric radiography, conventional tomography, arthrography, CT, cone beam computed tomography, radionuclide scanning, and/or MRI The following procedures for the management of infectious arthritis are not listed in order of preference:
15 B. Nonsurgical management 1. Patient education (eg, dietary recommendations, jaw rest) 2. Antibiotic therapy 3. Pain management 4. Physical therapy 5. Supportive therapy (eg, hydration, antipyretics) C. Surgical management 1. Acute infection a. Aspiration and/or arthrocentesis b. Incision and drainage with culture and sensitivity studies c. Identification and elimination of etiology d. Arthroscopic surgery e. Removal of implant or foreign body 2. Chronic infection a. Aspiration and/or arthrocentesis b. Incision and drainage with culture and sensitivity studies c. Identification and elimination of etiology d. Arthroscopic surgery e. Biopsy f. Arthroplasty g. Alloplastic joint replacement D. Posttreatment management 1. Ongoing medical management of infection 2. Wound care 3. Pain management 4. Diet and oral hygiene management 5. Physical therapy 6. Reassessment of infectious process 7. Instructions for posttreatment care and follow-up 8. Management of residual deformity after elimination of infectious process (eg, orthognathic surgery, joint reconstruction) V. Outcome Assessment Indices for Infectious Arthritis Indices are used by the specialty to assess aggregate outcomes of care. Outcomes are assessed through clinical evaluation and may include an imaging evaluation. A. Favorable therapeutic outcomes 1. General favorable therapeutic outcomes, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Elimination of infection 3. Limited period of disability 4. Acceptable clinical appearance (eg, absence of motor deficits, absence of hypertrophic scar formation, absence of facial asymmetry or deformity) 5. Improved mandibular function (eg, maximum incisal opening, lateral and protrusive excursions) B. Known risks and complications associated with surgery 1. Presence of a general known risk and/or complication, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Need to remove an autograft or alloplast 3. Ankylosis 4. Progression of infection (eg, osteomyelitis, sepsis, deep space infection) 5. Adherent unacceptable scar formation MANDIBULAR DISLOCATION: RECURRENT OR PERSISTENT
16 Mandibular dislocation can be acute, recurrent, or persistent. All of these refer to the dislocation of the intact nonfractured condyle. Acute dislocation describes blockage of the condyle by the eminence that prevents its return to the glenoid fossa, thus causing inability to close the mouth. Recurrent dislocation describes multiple episodes of dislocation during a specific period. Persistent dislocation describes a long-term blockage of the condyle by the eminence and may be associated with irreversible intracapsular pathology. This section addresses the therapy for recurrent or persistent dislocation. Acute dislocation is addressed in the Trauma Surgery chapter. I. Indications for Therapy for Mandibular Dislocation: Recurrent or Persistent May include one or more of the following: A. Moderate-to-severe pain 1. Temporomandibular pain 2. Preauricular pain 3. Masticatory muscle pain (see Masticatory Muscle Disorders section) B. Dysfunction that is disabling and characterized by any of the following: 1. Frequent, recurrent and/or persistent mandibular dislocation 2. Restricted range of jaw motion 3. Excessive range of jaw motion in patients who relocate after the dislocation 4. Joint noises (eg, clicking, popping, crepitation) 5. Abnormal masticatory function (eg, painful chewing, malocclusion) 6. Displaced autograft or alloplastic implant C. Imaging evidence of dislocation and/or displaced autograft or alloplastic implant II. Specific Therapeutic Goals for Mandibular Dislocation: Recurrent or Persistent The goal of therapy is to restore form and/or function. However, risk factors and potential complications may preclude complete restoration of form and/or function. A. Presence of a general therapeutic goal, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Correction and prevention of dislocation C. Limited pain in the joint D. Elimination or reduction of noise in the joint III. Specific Factors Affecting Risk for Mandibular Dislocation: Recurrent or Persistent Severity factors that increase risk and the potential for known complications: A. Presence of a general factor affecting risk, as listed in the section entitled General Criteria, Parameters, and Considerations for B. Status and/or degree of abnormal condylar and/or articular eminence growth and development C. Presence of autograft and/or alloplastic implant D. Presence of oromandibular dystonia or other jaw dyskinesia E. Therapeutic use of medications causing extrapyramidal reactions IV. Indicated Therapeutic Parameters for Mandibular Dislocation: Recurrent or Persistent A. The pretreatment assessment includes, at a minimum: 1. General history and physical examination, as detailed in the Patient Assessment chapter 2. Focused history and physical examination of the TMJ region to determine the presence of indications for care of mandibular dislocation and to identify factors affecting risks 3. An imaging examination, based on the history and physical findings, may include but is not limited to the following: panoramic radiography, cephalometric radiography, conventional tomography, arthrography, CT, cone beam computed tomography, radionuclide scanning, and/or MRI The following procedures for the management of mandibular dislocation are not listed in order of preference:
17 B. Nonsurgical management 1. Patient education (eg, dietary recommendations, jaw rest, decreased range of motion) 2. Discontinuation of use of medications causing extrapyramidal reactions 3. Medication (eg, drugs used to manage tremors, NSAIDs, analgesics, muscle relaxants, steroids) 4. Physical medicine (eg, physical therapy, massage, heat, cold, ultrasonography) 5. Intracapsular diagnostic and therapeutic injections 6. Behavioral modification (eg, counseling, biofeedback, psychotherapy) C. Surgical management 1. Manipulation and relocation of the condyle 2. Application of maxillomandibular fixation 3. Arthroscopic surgery 4. Arthrotomy or arthroplasty a. Disk repair procedures b. Diskectomy without replacement c. Diskectomy with replacement d. Articular surface recontouring (condyle/eminence) e. Removal of displaced autograft or alloplastic implant 5. Autogenous graft to limit condylar movement 6. Temporalis muscle scarification 7. Inferomedial fracture of zygomatic arch 8. Orthognathic surgery 9. Autogenous or alloplastic joint replacement 10. Neuromuscular blocking agents D. Posttreatment management 1. Wound care 2. Pain management 3. Diet and oral hygiene management 4. Physical therapy 5. Occlusal management 6. Patient reassessment 7. Instructions for posttreatment care and follow-up V. Outcome Assessment Indices for Mandibular Dislocation: Recurrent or Persistent Indices are used by the specialty to assess aggregate outcomes of care. Outcomes are assessed through clinical evaluation and may include an imaging evaluation. A. Favorable therapeutic outcomes 1. General favorable therapeutic outcomes, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Absence of recurrent or persistent mandibular dislocation B. Known risks and complications associated with therapy 1. Presence of a general known risk and/or complication, as listed in the section entitled General Criteria, Parameters, and Considerations for 2. Need to remove an autograft or alloplast 3. Continued dislocation ANKYLOSIS AND RESTRICTED JAW MOTION Intra-articular and extra-articular processes may restrict jaw motion severely. Ankylosis of the TMJ is an intraarticular process characterized by fibrous, fibro-osseous, or osseous obliteration of the joint space. Extracapsular causes of restricted jaw motion (pseudoankylosis) include but are not limited to coronoidzygomatic fusion, coronoid hypertrophy, and muscular fibrosis.
TEMPORO-MANDIBULAR JOINT DISORDERS
 Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Initial Doctor Questionnaire
 Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Up Date on TMD WHAT IS TMD? Temporomandibular Disorders (TMD)*: Donald Nixdorf DDS, MS
 Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
TMJ Parametro Classico
 TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
TMJ Joint Replacement System
 TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
Corporate Medical Policy
 Corporate Medical Policy Temporomandibular Joint Dysfunction (TMJD) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: temporomandibular_joint_dysfunction_(tmjd) 1/1996 10/2017 10/2018
Corporate Medical Policy Temporomandibular Joint Dysfunction (TMJD) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: temporomandibular_joint_dysfunction_(tmjd) 1/1996 10/2017 10/2018
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health
 T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
Chapter 79: Temporomandibular Joint Disorders. Daniel M. Laskin
 Chapter 79: Temporomandibular Joint Disorders Daniel M. Laskin It has been estimated that as many as 10 million people in the USA suffer from disorders of the temporomandibular joint and such disorders
Chapter 79: Temporomandibular Joint Disorders Daniel M. Laskin It has been estimated that as many as 10 million people in the USA suffer from disorders of the temporomandibular joint and such disorders
CHAPTER 8 SECTION 1.4 ORAL SURGERY TRICARE/CHAMPUS POLICY MANUAL M DEC 1998 SPECIAL BENEFIT INFORMATION
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
TMJ UNDERSTANDING SYNDROME SPECIAL REPORT By Paul R. White, D.D.S. Special Report: Understanding TMJ Syndrome
 SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
Parameters of Care: Clinical Practice Guidelines for Oral and Maxillofacial Surgery (AAOMS ParCare 2017) TRAUMA SURGERY
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 Parameters of Care: Clinical Practice Guidelines
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 Parameters of Care: Clinical Practice Guidelines
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ)
 Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries
 JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
Parameters of Care: Clinical Practice Guidelines for Oral and Maxillofacial Surgery (AAOMS ParCare 2017)
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 Parameters of Care: Clinical Practice Guidelines for
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 Parameters of Care: Clinical Practice Guidelines for
Index. Dent Clin N Am 51 (2007) Note: Page numbers of article titles are in boldface type.
 Dent Clin N Am 51 (2007) 275 279 Index Note: Page numbers of article titles are in boldface type. A Acupuncture, in persistent facial pain, 269 270 Analgesic systems, sex differences in, 6 8 Anticholinergic
Dent Clin N Am 51 (2007) 275 279 Index Note: Page numbers of article titles are in boldface type. A Acupuncture, in persistent facial pain, 269 270 Analgesic systems, sex differences in, 6 8 Anticholinergic
Preface Introduction Initial Evaluation Patient Interview Review of the "Initial Patient Questionnaire" Clinical Examination Range of Motion TMJ
 Preface Introduction Initial Evaluation Patient Interview Review of the "Initial Patient Questionnaire" Clinical Examination Range of Motion TMJ Noise TMD Palpations Intraoral Examination Occlusal Changes
Preface Introduction Initial Evaluation Patient Interview Review of the "Initial Patient Questionnaire" Clinical Examination Range of Motion TMJ Noise TMD Palpations Intraoral Examination Occlusal Changes
Oral and Maxillofacial Surgery Privileges REAPPOINTMENT Effective from July 1, 2015 to June 30, 2016
 Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants must meet the following requirements as approved by the Health Authority or Hospital, effective: 11/Dec/2014.
Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants must meet the following requirements as approved by the Health Authority or Hospital, effective: 11/Dec/2014.
Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani. Background & Etiology
 Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani Background & Etiology TMD affects approximately 10-15% of the population, but only 5% seek treatment. Incidence peaks from
Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani Background & Etiology TMD affects approximately 10-15% of the population, but only 5% seek treatment. Incidence peaks from
INFORMED CONSENT. For the Orthodontic Patient. Risks and Limitations of Orthodontic Treatment
 INFORMED CONSENT For the Orthodontic Patient Risks and Limitations of Orthodontic Treatment Successful orthodontic treatment is a partnership between the orthodontist, or pediatric dentist, and the patient.
INFORMED CONSENT For the Orthodontic Patient Risks and Limitations of Orthodontic Treatment Successful orthodontic treatment is a partnership between the orthodontist, or pediatric dentist, and the patient.
PhD in Oral Surgery (50 Credit Hours)
 PhD in Oral Surgery (50 Credit Hours) First Semester (9 Credit Hours) OSRG 701 Oral Surgery I 1 OSRG 791 Oral Surgery Clinics I 2 OSRG 706 Applied Surgical Anatomy 1 OSRG 707 Pain and Anxiety Control 1
PhD in Oral Surgery (50 Credit Hours) First Semester (9 Credit Hours) OSRG 701 Oral Surgery I 1 OSRG 791 Oral Surgery Clinics I 2 OSRG 706 Applied Surgical Anatomy 1 OSRG 707 Pain and Anxiety Control 1
DOD MPL, GENERAL DENTISTRY, GENERATED FROM CCQAS FOR AFMS USE, June
 LIST OF CLINICAL PRIVILEGES GENERAL DENTISTRY AUTHORITY: Title 10, U.S.C. Chapter 55, Sections 1094 and 1102. PRINCIPAL PURPOSE: To define the scope and limits of practice for individual providers. Privileges
LIST OF CLINICAL PRIVILEGES GENERAL DENTISTRY AUTHORITY: Title 10, U.S.C. Chapter 55, Sections 1094 and 1102. PRINCIPAL PURPOSE: To define the scope and limits of practice for individual providers. Privileges
Informed Consent. for the orthodontic Patient. risks and Limitations of orthodontic treatment
 Informed Consent for the orthodontic Patient risks and Limitations of orthodontic treatment Successful orthodontic treatment is a partnership between the orthodontist and the patient. The doctor and staff
Informed Consent for the orthodontic Patient risks and Limitations of orthodontic treatment Successful orthodontic treatment is a partnership between the orthodontist and the patient. The doctor and staff
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines TEMPOROMANDIBULAR JOINT (TMJ) MRI Original Date: May 23, 2003 Page 1 of 5 CPT Code: 70336 Last Review Date: May 2016 NCD 220.2 MRI Last Effective Date:
National Imaging Associates, Inc. Clinical guidelines TEMPOROMANDIBULAR JOINT (TMJ) MRI Original Date: May 23, 2003 Page 1 of 5 CPT Code: 70336 Last Review Date: May 2016 NCD 220.2 MRI Last Effective Date:
CBCT Specific Guidelines for South African Practice as Indicated by Current Literature:
 CBCT Specific Guidelines for South African Practice as Indicated by Current Literature: CF Hoogendijk Maxillo- facial and Oral surgery: Trauma: 1. Facial trauma for the confirmation or exclusion of fractures
CBCT Specific Guidelines for South African Practice as Indicated by Current Literature: CF Hoogendijk Maxillo- facial and Oral surgery: Trauma: 1. Facial trauma for the confirmation or exclusion of fractures
Temporomandibular Joint (TMJ) Disorder Surgery
 Medical Coverage Policy Effective Date...01/15/2018 Next Review Date...01/15/2019 Coverage Policy Number... 0156 Temporomandibular Joint (TMJ) Disorder Surgery Table of Contents Related Coverage Resources
Medical Coverage Policy Effective Date...01/15/2018 Next Review Date...01/15/2019 Coverage Policy Number... 0156 Temporomandibular Joint (TMJ) Disorder Surgery Table of Contents Related Coverage Resources
Prosthetic Management of TMJ Disorders
 Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Arthrogenous disorders of the TMJ
 Arthrogenous disorders of the TMJ Seena Patel DMD, MPH Assistant Professor, Associate Director of Oral Medicine Arizona School of Dentistry & Oral Health, A.T. Still University, Mesa, AZ Southwest Orofacial
Arthrogenous disorders of the TMJ Seena Patel DMD, MPH Assistant Professor, Associate Director of Oral Medicine Arizona School of Dentistry & Oral Health, A.T. Still University, Mesa, AZ Southwest Orofacial
The America Association of Oral and Maxillofacial Surgeons classify occlusion/malocclusion in to the following three categories:
 Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Subject: Orthognathic Surgery Policy Effective Date: 04/2016 Revision Date: 07/2018 DESCRIPTION Orthognathic surgery is an open surgical procedure that corrects anomalies or malformations of the lower
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alveolar osteitis (dry socket), periodontal pain due to, 436 Aphthous stomatitis, recurrent, mucosal pain due to, 439 440 Arthrocentesis/arthroscopy,
Index Note: Page numbers of article titles are in boldface type. A Alveolar osteitis (dry socket), periodontal pain due to, 436 Aphthous stomatitis, recurrent, mucosal pain due to, 439 440 Arthrocentesis/arthroscopy,
Principle of Occlusion
 Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
STERILE IMPLANT PRODUCT INSERT PATIENT-FITTED TEMPOROMANDIBULAR JOINT RECONSTRUCTION PROSTHESIS SYSTEM
 STERILE IMPLANT PRODUCT INSERT PATIENT-FITTED TEMPOROMANDIBULAR JOINT RECONSTRUCTION PROSTHESIS SYSTEM CAUTION United States Federal Law restricts this device to sale by or on the order of a physician.
STERILE IMPLANT PRODUCT INSERT PATIENT-FITTED TEMPOROMANDIBULAR JOINT RECONSTRUCTION PROSTHESIS SYSTEM CAUTION United States Federal Law restricts this device to sale by or on the order of a physician.
Screening orthodontic patients for temporomandibular disorders
 Clin Dent Rev (2017) 1:8 https://doi.org/10.1007/s41894-017-0007-z DIAGNOSIS Screening orthodontic patients for temporomandibular disorders Gary Klasser 1 Charles Greene 2 Received: 5 April 2017 / Accepted:
Clin Dent Rev (2017) 1:8 https://doi.org/10.1007/s41894-017-0007-z DIAGNOSIS Screening orthodontic patients for temporomandibular disorders Gary Klasser 1 Charles Greene 2 Received: 5 April 2017 / Accepted:
Toma este vals con la boca cerrada. Frederico Garcia Lorca: Pequeño vals vienés
 Toma este vals con la boca cerrada. Frederico Garcia Lorca: Pequeño vals vienés Toma este vals con la boca cerrada. Ay, Ay, Ay, Ay Take this waltz, take this waltz Take this waltz with the clamp on its
Toma este vals con la boca cerrada. Frederico Garcia Lorca: Pequeño vals vienés Toma este vals con la boca cerrada. Ay, Ay, Ay, Ay Take this waltz, take this waltz Take this waltz with the clamp on its
Establish a Healthy TMJ
 TW TMJ Establish a Healthy TMJ Prior to Restorative, Orthodontic or Prosthetic Treatment Dr. Brock Rondeau, D.D.S., I.B.O., D.A.B.C.P. Author: Dr. Brock Rondeau is one of North America s most sought after
TW TMJ Establish a Healthy TMJ Prior to Restorative, Orthodontic or Prosthetic Treatment Dr. Brock Rondeau, D.D.S., I.B.O., D.A.B.C.P. Author: Dr. Brock Rondeau is one of North America s most sought after
Temporomandibular joint reconstruction with alloplastic prosthesis: the outcomes of four cases
 Park et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:6 DOI 10.1186/s40902-017-0103-7 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Temporomandibular joint reconstruction
Park et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:6 DOI 10.1186/s40902-017-0103-7 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Temporomandibular joint reconstruction
Intraoral mandibular distraction osteogenesis in facial asymmetry patients with unilateral temporomandibular joint bony ankylosis
 Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Temporomandibular Joint : Is a synovial joint located between the condyle (head of the mandible) and the glenoid fossa (inferior surface of the squamous part of Temporal
Temporomandibular Joint Disorders Temporomandibular Joint : Is a synovial joint located between the condyle (head of the mandible) and the glenoid fossa (inferior surface of the squamous part of Temporal
Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle
 Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Classification of Tempromandibular Disorders
 Classification of Tempromandibular Disorders Defined as any disorder that affects or that is affected by deformity, disease, misalignment, or dysfunction of the tempromandibular articulation. This includes
Classification of Tempromandibular Disorders Defined as any disorder that affects or that is affected by deformity, disease, misalignment, or dysfunction of the tempromandibular articulation. This includes
2018 Dental Code Set For dates of service from 1/1/ /31/2018
 D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
2018 Dental Code Set
 D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
ORTHOGNATHIC SURGERY
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-16 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Arthritis of the Shoulder
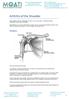 Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
Review Article A 5 Year Retrospective Study on the Clinical Outcomes of Performing Arthrocentesis in Basildon Hospital
 Cronicon OPEN ACCESS Nikhil Gogna* and Jamal Siddiqi Department of Oral & Maxillofacial Surgery, Basildon Hospital, United Kingdom Received: July 17, 2015; Published: July 23, 2015. DENTAL SCIENCE Review
Cronicon OPEN ACCESS Nikhil Gogna* and Jamal Siddiqi Department of Oral & Maxillofacial Surgery, Basildon Hospital, United Kingdom Received: July 17, 2015; Published: July 23, 2015. DENTAL SCIENCE Review
Oral and Maxillofacial Surgery Privileges
 Name: Effective from / / to / / Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants should meet the following requirements as approved by the governing body,
Name: Effective from / / to / / Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants should meet the following requirements as approved by the governing body,
Outcomes of surgical versus nonsurgical treatment of mandibular condyle fractures
 International Surgery Journal Ragupathy K. Int Surg J. 2016 Feb;3(1):47-51 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151508
International Surgery Journal Ragupathy K. Int Surg J. 2016 Feb;3(1):47-51 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151508
RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY
 RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY INFORMATION AND CONSENT FOR IMPLANT SURGERY PURPOSE OF THIS FORM: State law requires
RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY INFORMATION AND CONSENT FOR IMPLANT SURGERY PURPOSE OF THIS FORM: State law requires
Osteochondroma of the mandibular condyle cured by conservative resection
 Journal of Dental Sciences (2014) 9, 91e95 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Osteochondroma of the mandibular condyle cured by conservative resection
Journal of Dental Sciences (2014) 9, 91e95 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Osteochondroma of the mandibular condyle cured by conservative resection
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL
 What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY
 MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
Medicare C/D Medical Coverage Policy
 Orthognathic Surgery Origination: June 1998 Review Date: February 15, 2017 Next Review: February 2019 Medicare C/D Medical Coverage Policy DESCRIPTION OF PROCEDURE SERVICE Orthognathic surgery is a class
Orthognathic Surgery Origination: June 1998 Review Date: February 15, 2017 Next Review: February 2019 Medicare C/D Medical Coverage Policy DESCRIPTION OF PROCEDURE SERVICE Orthognathic surgery is a class
Prof. Zvan Bojana, M.D., Ph.D., senior consultant, FESO University Medical Centre Ljubljana, Slovenia Clinical Department of Vascular Neurology
 TEPOROMANDIBULAR PAIN Prof. Zvan Bojana, M.D., Ph.D., senior consultant, FESO University Medical Centre Ljubljana, Slovenia Clinical Department of Vascular Neurology Facial pain TMJ pathology Other ethiology
TEPOROMANDIBULAR PAIN Prof. Zvan Bojana, M.D., Ph.D., senior consultant, FESO University Medical Centre Ljubljana, Slovenia Clinical Department of Vascular Neurology Facial pain TMJ pathology Other ethiology
A Look at Two Syndromes: TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT. John Mitakides D.D.S., FAACP
 TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty
 Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Q2Q3 Reza Movahed, DMD a, *, Larry Wolford, DMD b,c. oralmaxsurgery.theclinics.com KEYWORDS KEY POINTS
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 Protocol for Concomitant Temporomandibular
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 Protocol for Concomitant Temporomandibular
Department of Oral & Maxillofacial Surgery. Referral Guidelines
 Department of Oral & Maxillofacial Surgery Referral Guidelines 2015 To all General Dental Practitioners and General Medical Practitioners The Department of Oral & Maxillofacial Surgery has outpatient clinics
Department of Oral & Maxillofacial Surgery Referral Guidelines 2015 To all General Dental Practitioners and General Medical Practitioners The Department of Oral & Maxillofacial Surgery has outpatient clinics
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: orthodontics_for_pediatric_patients 2/2014 10/2017 10/2018 10/2017 Description of Procedure or Service Children
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: orthodontics_for_pediatric_patients 2/2014 10/2017 10/2018 10/2017 Description of Procedure or Service Children
The Melbourne Temporomandibular Total Joint Replacement System
 The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
Blue Edge Dental SCHEDULE OF BENEFITS, EXCLUSIONS AND LIMITATIONS - HIGH A. BENEFITS
 Blue Edge Dental SCHEDULE OF BENEFITS, EXCLUSIONS AND LIMITATIONS - HIGH A. BENEFITS Annual Deductible Per Insured Person Annual Deductible Per Insured Family $100 Per Calendar Year $300 Per Calendar Year
Blue Edge Dental SCHEDULE OF BENEFITS, EXCLUSIONS AND LIMITATIONS - HIGH A. BENEFITS Annual Deductible Per Insured Person Annual Deductible Per Insured Family $100 Per Calendar Year $300 Per Calendar Year
Frequent discussions and formal reviews with individual residents and residents as a group. Discussions with attendings responsible for the
 NewYork-Presbyterian Hospital Weill Cornell Medicine Division of Oral and Maxillofacial Surgery & Dentistry Advanced Education Program in Oral and Maxillofacial Surgery Goals and Objectives The goal of
NewYork-Presbyterian Hospital Weill Cornell Medicine Division of Oral and Maxillofacial Surgery & Dentistry Advanced Education Program in Oral and Maxillofacial Surgery Goals and Objectives The goal of
Diagnosis and Management of Temporomandibular Disorders
 Chapter 32 Diagnosis and Management of Temporomandibular Disorders Fina Navi, Mohammad Hosein Kalantar Motamedi, Koroush Taheri Talesh, Esshagh Lasemi and Zahra Nematollahi Additional information is available
Chapter 32 Diagnosis and Management of Temporomandibular Disorders Fina Navi, Mohammad Hosein Kalantar Motamedi, Koroush Taheri Talesh, Esshagh Lasemi and Zahra Nematollahi Additional information is available
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Blue Edge Dental SCHEDULE OF BENEFITS, EXCLUSIONS AND LIMITATIONS - HIGH
 Blue Edge Dental A. BENEFITS SCHEDULE OF BENEFITS, EXCLUSIONS AND LIMITATIONS - HIGH Annual Deductible Per Insured Person $50 Per Calendar Year Annual Maximum Per Insured Person $1,000 Covered Services:
Blue Edge Dental A. BENEFITS SCHEDULE OF BENEFITS, EXCLUSIONS AND LIMITATIONS - HIGH Annual Deductible Per Insured Person $50 Per Calendar Year Annual Maximum Per Insured Person $1,000 Covered Services:
General Dental Treatment Consent Form
 General Dental Treatment Consent Form I authorize dental treatment including necessary or advisable examination, radiographs (x-rays), diagnostic aids or local anesthesia. In general terms, dental treatment
General Dental Treatment Consent Form I authorize dental treatment including necessary or advisable examination, radiographs (x-rays), diagnostic aids or local anesthesia. In general terms, dental treatment
Patient information booklet Orthognathic Surgery
 Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Dr. James B. Lowe Plastic Surgery ORAL SOFT TISSUE SURGERY INFORMATION SHEET AND INFORMED CONSENT
 Dr. James B. Lowe Plastic Surgery ORAL SOFT TISSUE SURGERY INFORMATION SHEET AND INFORMED CONSENT Instructions This is an informed consent document that has been prepared to assist your plastic surgeon
Dr. James B. Lowe Plastic Surgery ORAL SOFT TISSUE SURGERY INFORMATION SHEET AND INFORMED CONSENT Instructions This is an informed consent document that has been prepared to assist your plastic surgeon
DR. PETER DAWSON S PHILOSOPHY OF FUNCTIONAL OCCLUSION
 DR. PETER DAWSON S PHILOSOPHY OF FUNCTIONAL OCCLUSION WHO IS PETER DAWSON? WHO IS PETER DAWSON? Peter Dawson is a dentist that specializes in the treatment of the exposed exterior surfaces of the teeth.
DR. PETER DAWSON S PHILOSOPHY OF FUNCTIONAL OCCLUSION WHO IS PETER DAWSON? WHO IS PETER DAWSON? Peter Dawson is a dentist that specializes in the treatment of the exposed exterior surfaces of the teeth.
Subject: Removal of Teeth Guideline #: Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018
 DDental Policy Dental Subject: Removal of Teeth Guideline #: 07-101 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses the removal of teeth, erupted
DDental Policy Dental Subject: Removal of Teeth Guideline #: 07-101 Publish Date: 03/15/2018 Status: Revised Last Review Date: 02/06/2018 Description This document addresses the removal of teeth, erupted
ORTHOGNATHIC SURGERY
 ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
ORTHOGNATHIC SURGERY MEDICAL POLICY Effective Date: February 1, 2017 Review Dates: 1/93, 7/95, 10/97, 4/99, 10/00, 8/01, 12/01, 4/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11,
INFORMED-CONSENT-SKIN GRAFT SURGERY
 INFORMED-CONSENT-SKIN GRAFT SURGERY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and
INFORMED-CONSENT-SKIN GRAFT SURGERY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and
MAHP Orthognathic Surgery Guidelines. Medical Policy Statement. Criteria
 Introduction The word orthognathic comes from the Greek words for straighten and jaw. Orthognathic surgery is the surgical correction of abnormalities of the mandible and/or maxilla. 1 It involves the
Introduction The word orthognathic comes from the Greek words for straighten and jaw. Orthognathic surgery is the surgical correction of abnormalities of the mandible and/or maxilla. 1 It involves the
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
THIS PLAN DOES NOT MEET THE MINIMUM ESSENTIAL HEALTH BENEFIT REQUIREMENTS FOR
 SCHEDULE OF EXCLUSIONS AND LIMITATIONS THIS PLAN DOES NOT MEET THE MINIMUM ESSENTIAL HEALTH BENEFIT REQUIREMENTS FOR PEDIATRIC ORAL HEALTH AS REQUIRED UNDER THE FEDERAL AFFORDABLE CARE ACT. Exclusions
SCHEDULE OF EXCLUSIONS AND LIMITATIONS THIS PLAN DOES NOT MEET THE MINIMUM ESSENTIAL HEALTH BENEFIT REQUIREMENTS FOR PEDIATRIC ORAL HEALTH AS REQUIRED UNDER THE FEDERAL AFFORDABLE CARE ACT. Exclusions
PRE-OP and POST-OP SURGICAL CONSIDERATIONS
 PRE-OP and POST-OP SURGICAL CONSIDERATIONS Darlene Sorrell, DMD, is not an oral surgeon. AIDC is an out-patient facility. 29 years of experience in IHS. Advanced General Practice Residency. No access
PRE-OP and POST-OP SURGICAL CONSIDERATIONS Darlene Sorrell, DMD, is not an oral surgeon. AIDC is an out-patient facility. 29 years of experience in IHS. Advanced General Practice Residency. No access
Concepts of occlusion Balanced occlusion. Monoplane occlusion. Lingualized occlusion. Figure (10-1)
 Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Ankle Replacement Surgery
 Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
2016 Dental Code Set For dates of service from 1/1/16-12/31/16
 HCPCS DESCRIPTIONS D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0260 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0470 D0502 D1110 D1206 D1208 D1352 D2140 D2150 D2160 D2161
HCPCS DESCRIPTIONS D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0260 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0470 D0502 D1110 D1206 D1208 D1352 D2140 D2150 D2160 D2161
Medical Review Criteria Dental and Oral Surgery Services
 Medical Review Criteria Dental and Oral Surgery Services Subject: Dental and Oral Surgery Services Effective Date: 11/2001 Policy: HPHC covers medically necessary dental/oral surgery services included
Medical Review Criteria Dental and Oral Surgery Services Subject: Dental and Oral Surgery Services Effective Date: 11/2001 Policy: HPHC covers medically necessary dental/oral surgery services included
A Rare Case of Cheerleader Syndrome, Case Report
 47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
LOCAL ANESTHESIA IN PEDIATRIC DENTISTRY
 Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of local anesthesia in pediatric dentistry must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of local anesthesia in pediatric dentistry must be made in conjunction
OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC
 Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
INTRODUCTION TO GUARDIAN CLINICAL POLICY
 DENTAL INSURANCE INTRODUCTION TO GUARDIAN CLINICAL POLICY April 26, 2018 Introduction and General Clinical Guidelines Prosthodontics Periodontics Oral Surgery General Anesthesia/IV Sedation Page 1 of 6
DENTAL INSURANCE INTRODUCTION TO GUARDIAN CLINICAL POLICY April 26, 2018 Introduction and General Clinical Guidelines Prosthodontics Periodontics Oral Surgery General Anesthesia/IV Sedation Page 1 of 6
Non Surgical Treatment of TMJ Dislocation
 Cronicon OPEN ACCESS DENTAL SCIENCE Mini Review Non Surgical Treatment of TMJ Dislocation Essam Soussa 1 * and Magued Fahmy 2 1 Department of Oral Biology, Dental College, Mansoura University, Egypt 2
Cronicon OPEN ACCESS DENTAL SCIENCE Mini Review Non Surgical Treatment of TMJ Dislocation Essam Soussa 1 * and Magued Fahmy 2 1 Department of Oral Biology, Dental College, Mansoura University, Egypt 2
Original Research Article
 KNOWLEDGE ON TEMPOROMANDIBULAR JOINT DISORDERS AMONG DENTISTS IN CHENNAI, TAMILNADU K. Niraimathi 1, K. Ranjith 2, Vidya Albert Yen 3, Edward Nijesh 4, Shalini P 5, Preetha E. Chaly 6, Satheesh 7, Sathyanarayanan
KNOWLEDGE ON TEMPOROMANDIBULAR JOINT DISORDERS AMONG DENTISTS IN CHENNAI, TAMILNADU K. Niraimathi 1, K. Ranjith 2, Vidya Albert Yen 3, Edward Nijesh 4, Shalini P 5, Preetha E. Chaly 6, Satheesh 7, Sathyanarayanan
Appropriate Management of Temporomandibular Disorders in the Elderly
 Arthritis Appropriate Management of in the Elderly Benjamin R. Davis, BSc, DDS, FRCD(C), Department of Oral and Maxillofacial Surgery, Queen Elizabeth II Health Sciences Centre, Halifax, NS. Temporomandibular
Arthritis Appropriate Management of in the Elderly Benjamin R. Davis, BSc, DDS, FRCD(C), Department of Oral and Maxillofacial Surgery, Queen Elizabeth II Health Sciences Centre, Halifax, NS. Temporomandibular
Concomitant Temporomandibular Joint and Orthognathic Surgery
 CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 61:1198-1204, 2003 Concomitant Temporomandibular Joint and Orthognathic Surgery Larry M. Wolford, DMD* *Clinical
CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 61:1198-1204, 2003 Concomitant Temporomandibular Joint and Orthognathic Surgery Larry M. Wolford, DMD* *Clinical
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
I have been encouraged to seek a second opinion if I so desire before consenting to this surgery.
 Dr has examined my mouth and made treatment recommendations to restore my teeth. The risks and benefits of the recommended treatment have been explained to me. Alternative forms of treatment including
Dr has examined my mouth and made treatment recommendations to restore my teeth. The risks and benefits of the recommended treatment have been explained to me. Alternative forms of treatment including
Case Presentation #1 for the American Board of Craniofacial Pain July 2013
 Case Presentation #1 for the American Board of Craniofacial Pain July 2013 Case I Summary Presentation Pain in right temporomandibular joint with opening of mouth( 7 out of 10 ). Acute right non-reducing
Case Presentation #1 for the American Board of Craniofacial Pain July 2013 Case I Summary Presentation Pain in right temporomandibular joint with opening of mouth( 7 out of 10 ). Acute right non-reducing
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report
 Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
A Resource Guide for Temporomandibular Disorders
 A Resource Guide for Temporomandibular Disorders The TMJ Association, Ltd. Welcome The TMJ Association presents this information as a guide to patients to help them with their health care decisions. The
A Resource Guide for Temporomandibular Disorders The TMJ Association, Ltd. Welcome The TMJ Association presents this information as a guide to patients to help them with their health care decisions. The
Volume 22 No. 14 September Dentists, Federally Qualified Health Centers and Health Maintenance Organizations For Action
 State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 22 No. 14 September 2012 TO: Dentists, Federally Qualified Health Centers and Health Maintenance
State of New Jersey Department of Human Services Division of Medical Assistance & Health Services Volume 22 No. 14 September 2012 TO: Dentists, Federally Qualified Health Centers and Health Maintenance
06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.]
![06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.] 06/12/18. [Note: When orthognathic surgery is not a covered benefit, it is non-covered for any diagnosis, including sleep apnea.]](/thumbs/84/91182117.jpg) Reference #: MC/B002 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS)
Reference #: MC/B002 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Community Health Plan (PCHP) PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS)
Arthritis of the Shoulder
 Page 1 of 7 Arthritis of the Shoulder This article is also available in Spanish: Artritis del hombro (Arthritis of the Shoulder) (topic.cfm?topic=a00723). In 2011, more than 50 million people in the United
Page 1 of 7 Arthritis of the Shoulder This article is also available in Spanish: Artritis del hombro (Arthritis of the Shoulder) (topic.cfm?topic=a00723). In 2011, more than 50 million people in the United
Purpose: To review the evolution of Temporomandibular joint TMJ surgery together with the biological evidence for surgical disease
 Stiesch-Scholz M, Kempert J, Wolter S, et al. Comparative prospective study on splint therapy of anterior disc displacement without reduction. J Oral Rehabilitation 2005; 32:474-479. (29 refs.) Purpose:
Stiesch-Scholz M, Kempert J, Wolter S, et al. Comparative prospective study on splint therapy of anterior disc displacement without reduction. J Oral Rehabilitation 2005; 32:474-479. (29 refs.) Purpose:
