Benign joint hypermobility syndrome (BJHS) is the occurrence
|
|
|
- Cory Greene
- 5 years ago
- Views:
Transcription
1 Benign Joint Hypermobility Syndrome: Evaluation, Diagnosis, and Management MAJ Michael R. Simpson, DO, MC, USA Benign joint hypermobility syndrome (BJHS) is a connective tissue disorder with hypermobility in which musculoskeletal symptoms occur in the absence of systemic rheumatologic disease. Although BJHS has been well recognized in the rheumatology and orthopedic literature, it has not been discussed in the family medicine literature. Because most patients with musculoskeletal complaints are first seen by family physicians, it behooves primary care physicians to be familiar with recognizing and diagnosing BJHS. When patients with this syndrome are first seen by a physician, their chief complaint is joint pain, so BJHS can be easily overlooked and not considered in the differential diagnosis. Use of the Brighton criteria facilitates the diagnosis of BJHS. Treatment modalities include patient education, activity modification, stretching and strengthening exercises for the affected joint, and osteopathic manipulative treatment. J Am Osteopath Assoc. 2006;106: Benign joint hypermobility syndrome (BJHS) is the occurrence of musculoskeletal symptoms in hypermobile individuals in the absence of systemic rheumatologic disease. This syndrome is thought to be an inherited connective tissue disorder. 1,2 The primary clinical manifestations of BJHS are hypermobility and pain in multiple joints. This syndrome is different from other disorders that cause local joint hypermobility and generalized joint laxity, such as Marfan syndrome and Ehlers Danlos syndrome (EDS). The Brighton criteria are used to diagnose BJHS, and laboratory tests are used to distinguish BJHS from other systemic diseases. 1,2 Other criteria have been proposed for diagnosis, From the US Army Health Clinic in Darmstadt, Germany. This paper has been reviewed by the US Army, and the content of the manuscript does not necessarily reflect the views of the US Army or the Department of Defense. Address correspondence to MAJ Michael R. Simpson, DO, MC, USA, USAHC DARMSTADT, CMR 431, APO AE michael.r.simpson@us.army.mil Submitted July 7, 2005; revision received November 28, 2005; accepted December 5, including Bulbena s criteria; however, the criteria defined by Brighton are the ones most frequently cited in the literature. 3 Generalized joint laxity is commonly seen in healthy individuals who do not have complaints. Hypermobility that is not associated with systemic disease occurs in 4% to 13% of the population. 4,5 Hypermobility diminishes as one ages, and it also appears to be related to sex and race. 5 In general, women have greater joint laxity than men, and up to 5% of healthy women have symptomatic joint hypermobility compared with 0.6% of men. 6 People of African, Asian, and Middle Eastern descent also have increased joint laxity Among studies examining the prevalence of generalized hypermobility in patients referred to rheumatologists, 5,9 11 one study found that hypermobility occurred in 66% of school children with arthralgia of unknown etiology. 10 Another study showed a similar prevalence of hypermobility in children; however, there was no association between hypermobility and the development of arthralgia. 11 These data suggest that generalized hypermobility exists without joint pain and it does not necessarily lead to arthralgia. Furthermore, patients with hypermobility often lead normal lives and do not have BJHS or another connective tissue disorder. Hypermobility may occur in several different connective tissue disorders including Marfan syndrome, EDS, and osteogenesis imperfecta. It may also be found in chromosomal and genetic disorders such as Down syndrome and in metabolic disorders such as homocystinuria and hyperlysinemia. Recurrent dislocation of the shoulder and patella as well as other orthopedic abnormalities are associated with joint laxity. Juvenile rheumatoid arthritis may also be associated with hypermobility, but many times, systemic symptoms are involved. 7 Patients with BJHS have generalized hypermobility as well as chronic joint pain and other neuromusculoskeletal signs related to a defect in collagen. 7 9 Benign joint hypermobility syndrome has a strong genetic component with an autosomal dominant pattern. First degree relatives with the disorder can be identified in as many as 50% of cases. The syndrome appears to be due to an abnormality in collagen or the ratio of collagen subtypes. Mutations in the fibrillin gene have also been identified in families with BJHS. 12 So, why do patients with BJHS present mainly with joint pain? It is thought that excessive joint laxity leads to wear and tear on joint surfaces and strains or fatigues the soft tissue JAOA Vol 106 No 9 September
2 Patient Interview Questions to Ask Can you now (or could you ever) place your hands flat on the floor without bending your knees? Can you now (or could you ever) bend your thumb to touch your forearm? As a child, did you amuse your friends by contorting your body into strange shapes or could you do the splits? As a child or teenager, did your shoulder or kneecap dislocate on more than one occasion? Do you consider yourself double-jointed? Figure 1. Questions physicians should ask patients to detect benign joint hypermobility syndrome. (Reproduced with permission from Hakim AJ, Cherkas LF, Grahame R, Spector TD, MacGregor AJ. The genetic epidemiology of joint hypermobility: A population study of female twins. Arthritis Rheum. 2004;50: ) surrounding these joints. Some studies also suggest that proprioception in the joints of patients with BJHS is impaired. This impairment can also lead to excessive joint trauma due to impaired sensory feedback from the joint affected. 1 4 Review of the Literature A search for the terms hypermobility, hypermobility syndrome, joint hypermobility, and benign joint hypermobility syndrome on MED- LINE and the MD Consult Core Collection covering 1966 through 2005 yielded 263 reports on BJHS looking at history, clinical presentation, diagnosis, treatment, and prognosis. Surveyed articles include review articles and case-control, retrospective, and observational studies, but no randomized controlled trials. In addition, the role of osteopathic manipulative treatment (OMT) of patients for hypermobility and chronic pain was researched by using the same databases with the key words manipulation and osteopathic manipulation used separately with hypermobility. Twenty articles were found on manipulation and hypermobility; however, none of these articles specifically address osteopathic manipulation. Clinical Presentation The signs and symptoms of BJHS are variable. Most commonly, the initial complaint in a hypermobile patient is joint pain, which may affect one or multiple joints and may be generalized or symmetric. Primary care physicians can use the five simple questions (Figure 1) to aid in recognizing hypermobility. 13 The onset of symptoms can occur at any age, and many patients have been referred to specialists in orthopedics, rheumatology, or physiatry. Typically, children have self-limited pain in multiple joints; however, pain can last for a prolonged time and may become constant in adulthood. Pain may involve any joint but most commonly involves the knee and ankle, presumably because they are weight bearing joints. Physical activity or repetitive use of the affected joint often exacerbates the pain. Consequently, pain usually occurs later in the day and morning stiffness is uncommon. Less common symptoms are joint stiffness, myalgia, muscle cramps, and nonarticular limb pain. Patients with BJHS often say that they are double-jointed or that they can contort their bodies into strange shapes (ie, volitionary subluxation) or do the splits. Such an admission, however, is not necessary for including BJHS in the differential diagnosis. Patients with BJHS may also have a history of shoulder or patellar dislocation. Patients with BJHS may have a family history of doublejointedness or recurrent dislocations. Other presentations include easy bruising, ligament or tendon rupture, congenital hip dysplasia, and temporomandibular joint dysfunction. 1,7,14 Findings of the physical examination vary based on the joint saffected. Pain in response to manipulation of the joint is common. Mild effusions are not common but may be present. Clinically significant tenderness along with redness, swelling, fever, or warmth suggests inflammation and is not present in patients with BJHS. 4,7 Signs of a typical connective tissue disorder may be present, including scoliosis, pes planus, genu valgum, lordosis, patellar subluxation or dislocation, marfanoid habitus, varicose veins, rectal or uterine prolapse, and thin skin (Figure 2). The association of BJHS with mitral valve prolapse (MVP) is a subject of controversy. Early studies showed an association between MVP and BJHS, 15 but later studies have questioned this association because of stricter echocardiographic criteria for MVP. 17 Primary care physicians should refer patients with hypermobility in whom cardiac findings suggest MVP to a cardiologist for further evaluation to rule out more serious cardiac abnormalities and connective tissue disorders. 7,15 17 Diagnosis Determining the Beighton score (Figure 3) is essential for making the diagnosis. The first step is to calculate the Beighton score, which is a measure of generalized joint laxity. 1 Physicians calculate this score by doing five simple maneuvers (Figure 4) that can be completed in 45 to 60 seconds. A Beighton score of 4 or more points is considered indicative of generalized joint laxity. Most patients with BJHS have symmetric joint laxity. The Brighton criteria were developed to establish diagnostic criteria for BJHS. Using these criteria helps physicians to distinguish BJHS from other connective tissue disorders. 1,4,14 Diagnosis of BJHS is one of exclusion. For patients with painful or swollen joints, it is important to rule out inflammatory, infectious, and autoimmune causes. Workup may 532 JAOA Vol 106 No 9 September 2006
3 Neuromusculoskeletal Signs Brighton Criteria Acute or Traumatic Sprains recurrent ankle sprains Meniscus tears Acute or recurrent dislocations or subluxations of the: shoulder patella metacarpophalangeal joint temporomandibular joint Traumatic arthritis Bruising Fractures Chronic or Nontraumatic Soft tissue rheumatism tendinitis epicondylitis rotator cuff syndrome synovitis juvenile episodic synovitis bursitis Chondromalacia Back pain Scoliosis Fibromyalgia Temporomandibular joint dysfunction Nerve compression disorders carpal tunnel syndrome tarsal tunnel syndrome acroparesthesia thoracic outlet syndrome Raynaud syndrome Flat feet and sequelae Unspecified arthralgia or effusion of affected joint(s) (foot, ankle, knee, hip, back, neck, shoulder, elbow, wrist, finger) Osteoarthritis Delayed motor development Congenital hip dislocation Major Criteria Beighton score of 4 Figure 4) Arthralgia for longer than 3 months in 4 or more joints Minor Criteria Beighton score of 1, 2, or 3 (Figure\!s>4) Arthralgia ( 3-month duration) in one to three joints or back pain ( 3-month duration)or spondylosis, spndylolysis/spondylolisthesis Dislocation or subluxation in more than one joint, or in one joint on more than one occasion Three or more soft tissue lesions (eg, epicondylitis, tenosynovitis, bursitis) Marfanoid habitus (tall, slim, span greater than height ( 1.03 ratio), upper segment less than lower segment (<0.89 ratio), arachnodactyly) Skin striae, hyperextensibility, thin skin, or abnormal scarring Ocular signs: drooping eyelids, myopia, antimongoloid slant Varicose veins, hernia, or uterine or rectal prolapse Mitral valve prolapse Requirement for Diagnosis Any one of the following: two major criteria one major plus two minor criteria four minor criteria two minor criteria and unequivocally affected firstdegree relative in family history Figure 3. Brighton criteria, based on determination of the Beighton score (Figure 4), is used to make the diagnosis of benign joint hypermobility syndrome. (Note: Readers should not be confused by the similarity of these two names. Beighton is the correct spelling of the name of the score, and Brighton, the correct spelling of the name of the criteria.) Figure 2. Neuromusculoskeletal signs and potential sequelae from benign joint hypermobility syndrome. include a complete blood cell count, erythrocyte sedimentation rate, rheumatoid factor, antinuclear antibody test, serum complement (C 3, C 4, CH 50 ) levels, and serum immunoglobulin (IgG, IgM, IgA) levels. Any of these test results that are not within the normal reference range suggest an alternate diagnosis. Sometimes, patients with BJHS have an effusion, but the joint aspirate shows a noninflammatory pattern from meniscal and cartilage irritation. Benign joint hypermobility syndrome needs to be distinguished from other disorders that share many common fea- tures, such as Marfan syndrome, EDS, and osteogenesis imperfecta. Generalized hypermobility is a common feature in all these hereditary connective tissue disorders and many features overlap, but often distinguishing features are present that enable differentiating these disorders. Ehlers Danlos Syndrome Ehlers Danlos syndrome comprises a group of connective tissue disorders that have gross joint laxity and may have purple papyraceous scars, skin hyperelasticity, and skin fragility that leads to easy bruising. Similarly to BJHS, EDS is inherited in an autosomal dominant fashion and is due to a defect in collagen. Of the many different types of EDS that exist, the most JAOA Vol 106 No 9 September
4 1 Point Each Side Apposition of the thumb to the flexor aspect of the forearm 1 Point Each Side Hyperextension of the knee beyond 90 degrees (neutral) 1 Point Each Side Hyperextension of the elbow beyond 90 degrees (neutral) 1 Point Each Side Passive dorsiflexion of the metacarpophalangeal joint to 90 degrees Figure 4. Maneuvers used to calculate the Beighton score. Four of the five maneuvers are each done on the right and left sides, and 1 point is awarded for each positive result. The photographs show how to perform each maneuver but do not necessarily represent a positive result. The highest possible score is 9. A score of 4 or higher meets the Brighton major criteria for hypermobility. (Note: Readers should not be confused by the similarity of these two names. Beighton is the correct spelling of the name of the score, and Brighton, the correct spelling of the name of the criteria.) 1 Point Forward flexion with the hands flat on floor and knees extended 534 JAOA Vol 106 No 9 September 2006
5 Prognosis The prognosis for patients with BJHS is generally good owing to the syndrome s nonprogressive nature and decreased joint laxity and symptoms that occur with age. However, patients need to be aware of the potential sequelae that have an increased frequency associated with BJHS. These sequelae include acute ligament and soft tissue injury, overuse injury, joint instability, possible increase in fractures and scoliosis, and increased frequency of uterine and rectal prolapse. In addition, these patients may be predisposed to osteoarthritis from years of excessive joint motion. 8 Also, an association between BJHS and panic disorder has been shown. 26 Despite these sequelae, patients should remain as active as possible. Altering their exercise regimen may avoid chronic joint pain. Good training strategies include slow, disciplined training, correct biomechanics, and effective proprioception. 20 Given the many sequelae that may develop and the potencommon are types I, II, and III. Benign joint hypermobility syndrome is thought to be a mild variation of EDS and most closely resembles EDS type III (hypermoblity type), which consists of joint pain, marked hypermobility, mild extra-articular involvement, and mild skin changes without scarring. 18,19 Researchers have suggested that BJHS lies on a continuum with EDS and may be its mildest form because of their overlapping features. 7,18 Marfan Syndrome Patients with Marfan syndrome often have a family history of the syndrome and tend to have cardiac and ocular features. Marfan syndrome is an autosomal dominant disorder in patients with a tall, thin body habitus (marfanoid habitus), generalized joint hypermobility, elongated fingers (arachnodactyly), myopia, and lens dislocation. Osteogenesis imperfecta is also characterized by a defect in collagen. Patients have excessive joint laxity, thin blue sclera, and bone fragility leading to multiple fractures and bony deformities. Juvenile Rheumatoid Arthritis Juvenile rheumatoid arthritis may be considered in children with hypermobility and joint pain, but its diagnosis requires the onset of arthritis before the age of 16 years, inflammation of one or more joints, and the exclusion of other rheumatic disorders. Management The first step in managing BJHS is to emphasize to patients that this syndrome is a nonprogressive, noninflammatory connective tissue disorder. 1,10,14 Effective treatment may be accomplished with lifestyle modification, altering the patient s exercise regimen, joint protection, and proper body mechanics. For acute symptoms, nonsteroidal anti-inflammatory drugs (NSAIDs) or acetaminophen have often been used for pain control. Joint complaints in these patients are not thought to be due to inflammation, so the use of NSAIDs for anything other than pain is disputed. 7,8,14 For moderate or severe pain, rest and abstaining from aggravating activities may improve symptoms. Physical therapy and joint protection may also help. 8,14 Long-term management of BJHS typically focuses on modification of activities, especially if they induce symptoms. Excessive joint movement is associated with the development of symptoms in patients with BJHS. Often, vigorous and repetitive activities have been targeted as aggravating factors. Overtraining, poor pacing, too many performances or athletic competitions, and focusing on joint flexibility rather than stability may all increase joint pain and the risk of injury. 20 If avoidance of these activities is not an acceptable option for patients, physicians may try other approaches. NSAIDs taken before competition often may reduce symptoms. Also, starting a strengthening program to provide muscular stability and sta- bilization to the joint may be beneficial. Stretching techniques that are targeted to isolate tight muscles without stressing the surrounding joints may reduce symptoms by improving balance and control. 14 Strength training should consist of a combination of both open kinetic (distal extremity moves freely) and closed kinetic chain (distal extremity meets resistance) exercises. Closed kinetic chain exercises often simulate functional demands of an extremity, while open kinetic chain activities are better for more targeted strength training. 14 Focusing on improving the proprioception of a joint may improve symptoms (eg, using a wobble board). 21,22 Sometimes, supportive splints along with appropriate footwear protect the joint, and supportive joint taping improves joint proprioception. 21 Focused exercises to improve muscle strength, balance, and coordination may help improve joint stability and proprioception. Improvement of proprioception may reduce strain to the ligaments surrounding the joint and avoid further injury. 21,22 Along with exercise therapy, OMT is a useful adjunctive treatment modality for BJHS. Thrust treatment techniques applying high velocity/low amplitude forces are the most widely used, but because of the increased tissue fragility seen in BJHS and weak supporting structures of the joint, gentler techniques like facilitated positional release and counterstrain are good alternatives. Osteopathic manipulative treatment helps induce articular release resulting in increased joint motion, and reduced pain as well as improved blood flow, lymphatic drainage, and proprioception. 15 It is thought that OMT can lead to hypermobility; however, not enough research has been conducted to confirm this hypothesis, and it is currently recommended that OMT be limited to no more than three times per week. 23 To help patients return to their activities while decreasing their symptoms and joint stress, osteopathic physicians should consider all these factors. 24,25 JAOA Vol 106 No 9 September
6 tial impact of BJHS on quality of life, some experts are questioning why BJHS is called a benign disorder; instead, they refer to the disorder as joint hypermobility syndrome. 18 However, most rheumatologists still refer to it as BJHS. In the future, more rheumatologists may use the changed name joint hypermobility syndrome because of the disorder s potential effects on quality of life. The potential complications of BJHS underscore the importance of making an early diagnosis and educating the patient. Comment Osteopathic physicians predominantly practice primary care medicine, and most patients with musculoskeletal complaints first see a primary care physician and are then referred to a rheumatologist. Hypermobility is a common cause of unexplained joint pain, yet it is often misdiagnosed in primary care. According to one source, primary care providers recognized generalized hypermobility in less than 10% of patients with generalized hypermobility who were referred to rheumatologists. 18 Therefore, physicians need to be aware of the clinical presentation of BJHS to enhance their diagnostic acumen. Benign joint hypermobility syndrome is the presence of musculoskeletal complaints in hypermobile individuals in the absence of systemic rheumatologic disease. It is a connective tissue disorder with a defect in collagen. The Brighton criteria are used to make the diagnosis. Education, activity modification, and exercise therapy to improve muscular stability and proprioception at specific joints are essential to symptom management. And, OMT is a useful adjunctive treatment modality to help reduce pain and improve proprioception. Finally, primary care physicians are the best resource to educate patients with BJHS about their illness, potential complications, and prognosis. Furthermore, a prompt diagnosis improves pain control and decreases disruptions in these patients physical activities, school, work, and quality of life. 18 Thus, by being the first medical contact for most of their patients with BJHS, physicians in primary care have the opportunity to diagnose and address BJHS and reduce the incidence of potential long-term sequelae, chronic pain, and traumatic injuries. References 1. Grahame R. The revised (Brighton 1998) criteria for the diagnosis of benign joint hypermobility syndrome (BJHS). J Rheumatol. 2000;27: Hakim AJ, Cherkas LF, Grahame R, Spector TD, MacGregor AJ. The genetic epidemiology of joint hypermobility: a population study of female twins. Arthritis Rheum. 2004;50: Available at: Accessed August 29, Bulbena A, Duro JC, Porta M, Faus S, Vallescar R, Martin Santos R. Clinical assessment of hypermobility of joints: assembling criteria. J Rheumatol. 1992;19: Biro F, Gewanter HL, Baum J. The hypermobility syndrome. Pediatrics. 1983;72: Seckin U, Sonel Tur B, Yilmaz O, Yagci I, Bodur H, Arasil T. The prevalence of joint hypermobility among high school students. Rheumatol Int. 2005;25: Engelbert R, Uiterwaal C, Van de Putte E, Helders P, Sakkers R, Van Tintelen P, et al. Pediatric generalized joint hypomobility and musculoskeletal complaints: a new entity? Clinical, biochemical, and osseal characteristics. Pediatrics. 2004;113: Available at: /content/full/113/4/714. Accessed August 29, Everman DB, Robin NH. Hypermobility syndrome. Pediatr Rev. 1998; 19: Finsterbush A, Pogrund H. The hypermobility syndrome. Clin Orthop Relat Res.May 1982: Larsson LG, Baum J, Mudholkar GS, Kollia GD. Benefits and disadvantages of joint hypermobility among musicians. N Engl J Med. 1993;329: Available at: /full/329/15/1079. Accessed August 29, Gedalia A, Brewer EJ. Joint hypermobility in pediatric practice a review. J Rheumatol. 1993;20: de Inocencio Arocena J, Ocaña Casas I, Benito Ortiz LB. Laxitud articular: prevalencia y relación con dolor musculosquelético. [Joint hypermobility: prevalence and relationship with musculoskeletal pain.] An Pediatr (Barc). 2004;61: Available at: /wdbcgi.exe/doyma/mrevista.pubmed_full?inctrl=05zi0103&rev=37&vol=61 &num=2&pag=162. Accessed August 29, Magnusson SP. Viscoelastic properties and flexibility of the human muscle tendon unit in benign joint hypermobility syndrome. J Rheumatol. 2001;28: Hakim AJ, Grahame R. A simple questionnaire to detect hypermobility: an adjunct to the assessment of patients with diffuse musculoskeletal pain. Int J Clin Pract. 2003;57: Russek LN. Examination and treatment of a patient with hypermobility syndrome. Phys Ther. 2000;80: Available at: Accessed August 29, Grahame R, Edwards JC, Pitcher D, Gabell A, Harvey W. A clinical and echocardiographic study of patients with the hypermobility syndrome. Ann Rheum Dis. 1981;40: Bird HA, Barton L. Joint hyperlaxity and its long-term effects on joints. J R Soc Health. 1993;113: Mishra MB, Ryan P, Atkinson P, Taylor H, Bell J, Calver D, et al. Extra-articular features of benign joint hypermobility syndrome. Br J Rheumatol. 1996;35: Adib N, Davies K, Grahame R, Woo P, Murray KJ. Joint hypermobility syndrome in childhood. A not so benign multisystem disorder? Rheumatology (Oxford). 2005;44: Skoumal M, Haberhauer G, Mayr H. Begleiterkrankungen bei primarer gelenkhypermobilitat. Med Klin. 2004;99: McCormack M, Briggs J, Hakim A, Grahame R. Joint laxity and the benign joint hypermobility syndrome in student and professional ballet dancers. J Rheumatol. 2004;31: Perlau R, Frank C, Fick G. The effect of elastic bandages on human knee proprioception in the uninjured population. Am J Sports Med. 1995;23: Hall MG, Ferrell WR, Sturrock RD, Hamblen DL, Baxendale RH. The effect of hypermobility syndrome on knee joint proprioception. Br J Rheumatol. 1995;34: Protapapas MG, Cymet TC. Joint cracking and popping: understanding noises that accompany articular release [published correction appears in J Am Osteopath Assoc. 2002;102:306]. J Am Osteopath Assoc. 2002;102: Available at: Accessed August 29, Fiechtner JJ, Brodeur RR. Manual and manipulation techniques for rheumatic disease. Med Clin North Am. 2002;86: Colloca CJ, Polkinghorn BS. Chiropractic management of Ehlers Danlos syndrome: a report of two cases. J Manipulative Physiol Ther. 2003;26: Martín-Santos R, Bulbena A, Porta M, Gago J, Molina L, Duró JC. Association between joint hypermobility syndrome and panic disorder. Am J Psychiatry. 1998;155: Available at: /content/full/155/11/1578. Accessed August 29, JAOA Vol 106 No 9 September 2006
HYPERLAXITY SYNDROME Symptoms Questions to the patient Signs Acute or Traumatic Chronic or Nontraumatic
 A 30 year old project manager, who is new to your general practice, presents with right anterior knee pain after slipping and landing on his knee three months ago. Imaging shows no abnormality, but he
A 30 year old project manager, who is new to your general practice, presents with right anterior knee pain after slipping and landing on his knee three months ago. Imaging shows no abnormality, but he
Biochemical marker changes benign hypermobility syndrome (BHMS)
 Original Research Article Biochemical marker changes benign hypermobility syndrome (BHMS) T. N. Tamilselvam 1*, Malarvizhi 2 1 Senior Assistant Professor, Institute of Rheumatology, Madras Medical College
Original Research Article Biochemical marker changes benign hypermobility syndrome (BHMS) T. N. Tamilselvam 1*, Malarvizhi 2 1 Senior Assistant Professor, Institute of Rheumatology, Madras Medical College
Dr. K. Brindha, M.D PG ESI PGIMSR, K.K Nagar, Chennai
 Dr. K. Brindha, M.D PG ESI PGIMSR, K.K Nagar, Chennai Case History 9 year old boy presented with a 3 week history of: Swelling of major lower limb joints Progression was additive (right ankle followed
Dr. K. Brindha, M.D PG ESI PGIMSR, K.K Nagar, Chennai Case History 9 year old boy presented with a 3 week history of: Swelling of major lower limb joints Progression was additive (right ankle followed
Joint hypermobility is a liability for the performing artist
 International Symposium on Performance Science ISBN 978-90-9022484-8 The Author 2007, Published by the AEC All rights reserved Joint hypermobility is a liability for the performing artist Rodney Grahame
International Symposium on Performance Science ISBN 978-90-9022484-8 The Author 2007, Published by the AEC All rights reserved Joint hypermobility is a liability for the performing artist Rodney Grahame
Currently at Cincinnati Children s Hospital As of 9/1/12, will be at Lutheran General Hospital in Chicago
 EDS and TOMORROW NO financial disclosures Currently at Cincinnati Children s Hospital As of 9/1/12, will be at Lutheran General Hospital in Chicago Also serve on the Board of Directors of the Ehlers-Danlos
EDS and TOMORROW NO financial disclosures Currently at Cincinnati Children s Hospital As of 9/1/12, will be at Lutheran General Hospital in Chicago Also serve on the Board of Directors of the Ehlers-Danlos
Forthomme B, Croisier JL, Crielaard JM. Departement of physical medicine and rehabilitation ULg.
 Contribution to an adapted physiotherapy in the hyperlaxity syndromes. Kaux JF, Foidart-Dessalle M, Toussaint G, Forthomme B, Croisier JL, Crielaard JM. Departement of physical medicine and rehabilitation
Contribution to an adapted physiotherapy in the hyperlaxity syndromes. Kaux JF, Foidart-Dessalle M, Toussaint G, Forthomme B, Croisier JL, Crielaard JM. Departement of physical medicine and rehabilitation
Alison Middleditch MCSP MMACP Director of Surrey Physiotherapy and is based in Coulsdon, Surrey
 Alison Middleditch MCSP MMACP Director of Surrey Physiotherapy and is based in Coulsdon, Surrey Alison qualified from Kings College Hospital and has worked in both the NHS and Private Practice. She held
Alison Middleditch MCSP MMACP Director of Surrey Physiotherapy and is based in Coulsdon, Surrey Alison qualified from Kings College Hospital and has worked in both the NHS and Private Practice. She held
EDNF Center for Clinical Care & Research at GBMC PHYSICIANS CONFERENCE September 15, 2014
 EDNF Center for Clinical Care & Research at GBMC 2014 PHYSICIANS CONFERENCE September 15, 2014 Pain in Ehlers-Danlos Syndrome Clair A. Francomano, M.D. Director, EDNF Center for Clinical Care and Research
EDNF Center for Clinical Care & Research at GBMC 2014 PHYSICIANS CONFERENCE September 15, 2014 Pain in Ehlers-Danlos Syndrome Clair A. Francomano, M.D. Director, EDNF Center for Clinical Care and Research
Instability due to disorders of collagen metabolism and inflammation
 Instability due to disorders of collagen metabolism and inflammation Chris Holroyd Consultant Rheumatologist University Hospital Southampton NHS Foundation Trust Outline Overview of hypermobility Genetic
Instability due to disorders of collagen metabolism and inflammation Chris Holroyd Consultant Rheumatologist University Hospital Southampton NHS Foundation Trust Outline Overview of hypermobility Genetic
Hypermobile Ehlers-Danlos syndrome (heds) vs. Hypermobility Spectrum Disorders (HSD): What s the Difference?
 Hypermobile Ehlers-Danlos syndrome (heds) vs. Hypermobility Spectrum Disorders (HSD): What s the Difference? There has been a major revision in the approach to joint hypermobility (JH) as a whole. To recognize
Hypermobile Ehlers-Danlos syndrome (heds) vs. Hypermobility Spectrum Disorders (HSD): What s the Difference? There has been a major revision in the approach to joint hypermobility (JH) as a whole. To recognize
DIAGNOSTIC ASSOCIATIONS WITH HYPERMOBUJTY IN RHEUMATOLOGY PATIENTS
 British Journal of Rheumatology 1995;34:1157-1161 DIAGNOSTIC ASSOCIATIONS WITH HYPERMOBUJTY IN RHEUMATOLOGY PATIENTS N. HUDSON, M. R. STARR, J. M. ESDAILE and M.-A. FTTZCHARLES Rheumatic Disease Unit,
British Journal of Rheumatology 1995;34:1157-1161 DIAGNOSTIC ASSOCIATIONS WITH HYPERMOBUJTY IN RHEUMATOLOGY PATIENTS N. HUDSON, M. R. STARR, J. M. ESDAILE and M.-A. FTTZCHARLES Rheumatic Disease Unit,
many patients seen on secondary referral as normal results in the presence of what had been considered
 Archives of Disease in Childhood, 1983, 58, 988-992 Articular hypermobility simulating chronic rheumatic disease R M LEWKONIA AND B M ANSELL Division of Rheumatology, Medical Research Council Clinical
Archives of Disease in Childhood, 1983, 58, 988-992 Articular hypermobility simulating chronic rheumatic disease R M LEWKONIA AND B M ANSELL Division of Rheumatology, Medical Research Council Clinical
IJPMR ORIGINAL ARTICLE ABSTRACT INTRODUCTION /jp-journals
 IJPMR ORIGINAL ARTICLE 10.5005/jp-journals-10066-0019 Benign Joint Hypermobility Syndrome Study of the Comparative Efficacy of Strengthening Exercise between Extensor Group of Muscles and Both Flexor and
IJPMR ORIGINAL ARTICLE 10.5005/jp-journals-10066-0019 Benign Joint Hypermobility Syndrome Study of the Comparative Efficacy of Strengthening Exercise between Extensor Group of Muscles and Both Flexor and
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM. What Are Musculoskeletal Disorders
 MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
Basics of Soft- Tissue Examination
 Basics of Soft- Tissue Examination Basics of Soft Tissue Exam For practitioners who primarily use their hands to treat the human structure: Examination must include functional tests to determine the type
Basics of Soft- Tissue Examination Basics of Soft Tissue Exam For practitioners who primarily use their hands to treat the human structure: Examination must include functional tests to determine the type
When a headache never goes away - Chronic daily headache in a teenager
 PBLD Table #6 When a headache never goes away - Chronic daily headache in a teenager Moderators: Taran Sangari M.D., Shailesh Shah M.D. Institution: Valley Children s Hospital, Madera, CA Objectives: Discuss
PBLD Table #6 When a headache never goes away - Chronic daily headache in a teenager Moderators: Taran Sangari M.D., Shailesh Shah M.D. Institution: Valley Children s Hospital, Madera, CA Objectives: Discuss
Non-inflammatory joint pain
 Non-inflammatory joint pain Lawrence Owino Okong o, Mmed (UoN); Mphil. (UCT). Lecturer, Department of Paediatrics and Child Health, University of Nairobi. Paediatrician/ Rheumatologist. INTRODUCTION Musculoskeletal
Non-inflammatory joint pain Lawrence Owino Okong o, Mmed (UoN); Mphil. (UCT). Lecturer, Department of Paediatrics and Child Health, University of Nairobi. Paediatrician/ Rheumatologist. INTRODUCTION Musculoskeletal
Inheritable Connective Tissue Diseases: Or It s Probably Not Marfan s. RJ Willes 4/23/2018
 Inheritable Connective Tissue Diseases: Or It s Probably Not Marfan s RJ Willes 4/23/2018 This pretty much sums it up. Inheritable Connective tissues diseases A homogenous collection of varied syndromes
Inheritable Connective Tissue Diseases: Or It s Probably Not Marfan s RJ Willes 4/23/2018 This pretty much sums it up. Inheritable Connective tissues diseases A homogenous collection of varied syndromes
Property of Latmedical, LLC.
 Dedicate to providing a strong product mix, Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine,
Dedicate to providing a strong product mix, Dr. Goed provides a complete and innovate product portfolio solution to the growing healthcare need within the field of non-invasive orthopedics, sports medicine,
NORTH BAY SYMPOSIUM SATURDAY JANUARY 20 TH 2018
 NORTH BAY SYMPOSIUM SATURDAY JANUARY 20 TH 2018 ROBERT HAIMSON, M.D. ORTHOPEDIC SURGEON SMGR FELLOW IN AAOS DIPLOMATE IN ABOS COMMON MUSCULOSKELETAL CONDITIONS COMMON MUSCULOSKELETAL CONDITIONS: WHAT
NORTH BAY SYMPOSIUM SATURDAY JANUARY 20 TH 2018 ROBERT HAIMSON, M.D. ORTHOPEDIC SURGEON SMGR FELLOW IN AAOS DIPLOMATE IN ABOS COMMON MUSCULOSKELETAL CONDITIONS COMMON MUSCULOSKELETAL CONDITIONS: WHAT
Soft Tissue Rheumatism. Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group
 Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
Soft Tissue Rheumatism Elinor Mody, MD Chief, Division of Rheumatology Reliant Medical Group Some problems are difficult, but diagnosing and treating most causes of joint pain are not! Common areas of
9/7/2017. Ehlers-Danlos Syndrome Hypermobility Type (heds) 5-Point Questionnaire for JHM. Joint Hypermobility Beighton Score
 http://medicalpicturesinfo.com/wp-content/uploads/2011/08/arachnodactyly-3.jpg 9/7/2017 Ehlers-Danlos Syndrome Hypermobility Type (heds) David Tilstra, MD MBA CentraCare Clinic No Disclosures Objectives:
http://medicalpicturesinfo.com/wp-content/uploads/2011/08/arachnodactyly-3.jpg 9/7/2017 Ehlers-Danlos Syndrome Hypermobility Type (heds) David Tilstra, MD MBA CentraCare Clinic No Disclosures Objectives:
WRIST SPRAIN. Description
 WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
Guide to Prevention of Sports Injuries
 Guide to Prevention of Sports Injuries Maintaining an active lifestyle offers a number of benefits for your physical and mental health. While exercise and sports-related activities often have a positive
Guide to Prevention of Sports Injuries Maintaining an active lifestyle offers a number of benefits for your physical and mental health. While exercise and sports-related activities often have a positive
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Contents. copyrighted material by PRO-ED, Inc. Chapter 1. Chapter 2. Chapter 3. Chapter 4. Chapter 5. Conditions in Athletic Injuries
 Acknowledgments xiii Introduction to the First Edition xv Introduction to the Second Edition xvii Chapter 1 Conditions in Athletic Injuries Anterior Cruciate Ligament (ACL) Tear 2 Biceps Tendon Strain
Acknowledgments xiii Introduction to the First Edition xv Introduction to the Second Edition xvii Chapter 1 Conditions in Athletic Injuries Anterior Cruciate Ligament (ACL) Tear 2 Biceps Tendon Strain
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS. Please check with the LCC bookstore for the required texts for this class.
 LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
Arm Injuries and Disorders
 Arm Injuries and Disorders Introduction Your arms are made up of muscles, joints, tendons and other connective tissue. There are many injuries and disorders that can affect the arm. Some arm injuries and
Arm Injuries and Disorders Introduction Your arms are made up of muscles, joints, tendons and other connective tissue. There are many injuries and disorders that can affect the arm. Some arm injuries and
Postural Tachycardia Syndrome and Hypermobility Syndrome
 Postural Tachycardia Syndrome and Hypermobility Syndrome Blair P. Grubb MD FACC Departments of Medicine and Pediatrics Health Science Campus University of Toledo Toledo, Ohio USA Over the years it became
Postural Tachycardia Syndrome and Hypermobility Syndrome Blair P. Grubb MD FACC Departments of Medicine and Pediatrics Health Science Campus University of Toledo Toledo, Ohio USA Over the years it became
The 2017 EDS/HSD Classification. May 3, 2017
 The 2017 Interntional Classification papers were published after peer review on March 17, 2017 in the American Journal of Human Genetics. They were written by the International Consortium on Ehlers-Danlos
The 2017 Interntional Classification papers were published after peer review on March 17, 2017 in the American Journal of Human Genetics. They were written by the International Consortium on Ehlers-Danlos
Joint Injuries and Disorders
 Joint Injuries and Disorders Introduction A joint is where two or more bones come together. Your joints include the knees, hips, elbows and shoulders. There are many types of joint disorders, including
Joint Injuries and Disorders Introduction A joint is where two or more bones come together. Your joints include the knees, hips, elbows and shoulders. There are many types of joint disorders, including
Page 1 of 6. Appendix 1
 Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
Case. 5 year old with 2 weeks leg pain and now refusing to walk + Fevers, lower leg swelling, warmth Denies and history of trauma or wounds
 Case 5 year old with 2 weeks leg pain and now refusing to walk + Fevers, lower leg swelling, warmth Denies and history of trauma or wounds Exam I: Swelling over entire tibia extending to foot P: Tenderness
Case 5 year old with 2 weeks leg pain and now refusing to walk + Fevers, lower leg swelling, warmth Denies and history of trauma or wounds Exam I: Swelling over entire tibia extending to foot P: Tenderness
Rheumatology & Immunology. Regional pain syndromes to be covered today. Some definitions. Tendinitis. Bursitis. History. History. Exam.
 Rheumatology & Immunology Some problems are difficult, but diagnosing and treating soft tissue syndromes are not! Soft tissue syndromes one of the most common reasons patients present to their doctor.
Rheumatology & Immunology Some problems are difficult, but diagnosing and treating soft tissue syndromes are not! Soft tissue syndromes one of the most common reasons patients present to their doctor.
Kineto. Orthopaedics & Rehabilitation Products
 Member of Vincent Medical Holdings Limited Kineto Orthopaedics & Rehabilitation Products Our orthopaedic and rehabilitation products comprise of a variety of adjustable rehabilitation braces for support,
Member of Vincent Medical Holdings Limited Kineto Orthopaedics & Rehabilitation Products Our orthopaedic and rehabilitation products comprise of a variety of adjustable rehabilitation braces for support,
UNIT 2.- SPORT INJURIES: SYMPTOMS AND TREATMENT
 UNIT 2.- SPORT INJURIES: SYMPTOMS AND TREATMENT Every year, millions of teenagers participate in high school sports. An injury to a high school athlete can be a significant disappointment for the teen,
UNIT 2.- SPORT INJURIES: SYMPTOMS AND TREATMENT Every year, millions of teenagers participate in high school sports. An injury to a high school athlete can be a significant disappointment for the teen,
Hypermobility Syndromes. Middlesbrough Masterclass Nov 2013
 Hypermobility Syndromes Middlesbrough Masterclass Nov 2013 Speakers Dr Alan Hakim - Physician & Rheumatologist Dr Jane Simmonds- Physiotherapist They work at a specialist HM Unit for the diagnosis & management
Hypermobility Syndromes Middlesbrough Masterclass Nov 2013 Speakers Dr Alan Hakim - Physician & Rheumatologist Dr Jane Simmonds- Physiotherapist They work at a specialist HM Unit for the diagnosis & management
Inter-examiner reproducibility of tests and criteria for generalized joint hypermobility and benign joint hypermobility syndrome
 Rheumatology 2007;46:1835 1841 doi:10.1093/rheumatology/kem290 Inter-examiner reproducibility of tests and criteria for generalized joint hypermobility and benign joint hypermobility syndrome B. Juul-Kristensen
Rheumatology 2007;46:1835 1841 doi:10.1093/rheumatology/kem290 Inter-examiner reproducibility of tests and criteria for generalized joint hypermobility and benign joint hypermobility syndrome B. Juul-Kristensen
Joint Disorders. Musculoskeletal Disorders (Part B-2) Module 7 -Chapter 10. Overview Disorders of the Muscular System Disorders of the Skeletal System
 Musculoskeletal Disorders (Part B-2) Module 7 -Chapter 10 Overview Disorders of the Muscular System Disorders of the Skeletal System Susie Turner, MD 1/9/13 Joint Disorders Arthritis Inflammation of Joint
Musculoskeletal Disorders (Part B-2) Module 7 -Chapter 10 Overview Disorders of the Muscular System Disorders of the Skeletal System Susie Turner, MD 1/9/13 Joint Disorders Arthritis Inflammation of Joint
Anterior Knee Pain in Children. Joseph Chorley, MD Associate Professor, Pediatrics Baylor College of Medicine
 Anterior Knee Pain in Children Joseph Chorley, MD Associate Professor, Pediatrics Baylor College of Medicine Goals and Objectives To learn how to care for patients with chronic knee pain To be able to
Anterior Knee Pain in Children Joseph Chorley, MD Associate Professor, Pediatrics Baylor College of Medicine Goals and Objectives To learn how to care for patients with chronic knee pain To be able to
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Definitions of joint hypermobility: o Joint hypermobility (JH): Capability for a joint to move beyond normal physiological limits.
 Definitions of joint hypermobility: o Joint hypermobility (JH): Capability for a joint to move beyond normal physiological limits. Descriptor, not diagnosis Also known as joint laxity, double-jointedness,
Definitions of joint hypermobility: o Joint hypermobility (JH): Capability for a joint to move beyond normal physiological limits. Descriptor, not diagnosis Also known as joint laxity, double-jointedness,
Ehlers-Danlos Syndromes Overview for primary care providers
 Ehlers-Danlos Syndromes Overview for primary care providers Roberto Mendoza-Londono MD, MSc, FCCMG, FRCPC Medical Director-EDS service, Hospital for Sick Children/UHN Interim Division Head, Genetics, HSC
Ehlers-Danlos Syndromes Overview for primary care providers Roberto Mendoza-Londono MD, MSc, FCCMG, FRCPC Medical Director-EDS service, Hospital for Sick Children/UHN Interim Division Head, Genetics, HSC
Understanding Rheumatoid Arthritis
 Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Prevalence of generalised joint hypermobility in school-aged children from east-central European region
 O R I G I N A L A R T I C L E Folia Morphol. Vol. 75, No. 1, pp. 48 52 DOI: 10.5603/FM.a2015.0065 Copyright 2016 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Prevalence of generalised joint hypermobility
O R I G I N A L A R T I C L E Folia Morphol. Vol. 75, No. 1, pp. 48 52 DOI: 10.5603/FM.a2015.0065 Copyright 2016 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Prevalence of generalised joint hypermobility
Arthritis and Rheumatology Clinics of Kansas Patient Education
 Arthritis and Rheumatology Clinics of Kansas Patient Education Regional Pain Syndromes Introduction: At some time in the course of life, virtually everyone will experience pain in a tendon, muscle, or
Arthritis and Rheumatology Clinics of Kansas Patient Education Regional Pain Syndromes Introduction: At some time in the course of life, virtually everyone will experience pain in a tendon, muscle, or
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross All rights reserved.
 Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity
 Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
SPORTS INJURIES IN CYCLING. dr. Luthfi Hidayat, Sp. OT (K)
 SPORTS INJURIES IN CYCLING dr. Luthfi Hidayat, Sp. OT (K) But, injury can happen Acute traumatic injuries due to fall Overuse injuries develop gradually overtime (due to repeated movement patterns or
SPORTS INJURIES IN CYCLING dr. Luthfi Hidayat, Sp. OT (K) But, injury can happen Acute traumatic injuries due to fall Overuse injuries develop gradually overtime (due to repeated movement patterns or
Common Elbow Problems
 Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Welcome! Capital Area Ehlers-Danlos Syndrome Support Group
 Welcome! Capital Area Ehlers-Danlos Syndrome Support Group Ehlers-Danlos Syndrome A N O V E R V I E W G A Y L E Y A N K E E, M S N, N P ( R E T. ) J U N E 1 4, 2 0 1 8 What is Ehlers-Danlos Syndrome (EDS)?
Welcome! Capital Area Ehlers-Danlos Syndrome Support Group Ehlers-Danlos Syndrome A N O V E R V I E W G A Y L E Y A N K E E, M S N, N P ( R E T. ) J U N E 1 4, 2 0 1 8 What is Ehlers-Danlos Syndrome (EDS)?
Ergonomics Glossary. Force The amount of physical effort a person uses to do a task.
 Ergonomics Glossary Administrative controls Procedures used to reduce the duration, frequency, or severity of exposure to a hazard. They may include training, job rotation, and gradual introduction to
Ergonomics Glossary Administrative controls Procedures used to reduce the duration, frequency, or severity of exposure to a hazard. They may include training, job rotation, and gradual introduction to
Ergonomics Keeping the Worker on the Job
 Ergonomics Keeping the Worker on the Job Job Site Analysis WorkRisk Analysis WorkTask Analysis WorkStation Analysis David Raptosh, MA, OTR/L Regional Director of WorkStrategies Job Site Analysis - Identify
Ergonomics Keeping the Worker on the Job Job Site Analysis WorkRisk Analysis WorkTask Analysis WorkStation Analysis David Raptosh, MA, OTR/L Regional Director of WorkStrategies Job Site Analysis - Identify
Pain or stiffness in joints after periods of inactivity or excessive use
 Arthritis Awareness* Some older adults call it Arthur ; others refer to it as their constant compassion, but most describe it as extremely painful Arthritis is a chronic joint disease It is commonly believed
Arthritis Awareness* Some older adults call it Arthur ; others refer to it as their constant compassion, but most describe it as extremely painful Arthritis is a chronic joint disease It is commonly believed
Chiropractic Healthcare
 ebook 2 Chiropractic Healthcare Four symptoms explained Introduction 3 Chapter 1 Carpal Tunnel Syndrome 4 Chapter 2 Common Shoulder Pain Issues 8 Chapter 3 Headaches and Chiropractic Care 14 Chapter 4
ebook 2 Chiropractic Healthcare Four symptoms explained Introduction 3 Chapter 1 Carpal Tunnel Syndrome 4 Chapter 2 Common Shoulder Pain Issues 8 Chapter 3 Headaches and Chiropractic Care 14 Chapter 4
Recognizing common injuries to the lower extremity
 Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Lower Extremity Sports Injuries
 Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Lower Extremity Sports Injuries AAP Musculoskeletal Boot Camp Sigrid F. Wolf, MD Pediatric Sports Medicine Fellow Northwestern University Lurie Children s Hospital Disclosure I have no relevant financial
Joint involment in orthopedic diseases
 Joint involment in orthopedic diseases PReS Latin America Basic Pediatric Rheumatology Course 2015 Aguas de São Pedro, São Paulo, Brazil Carmen L. De Cunto carmen.decunto@hospitalitaliano.org.ar Sección
Joint involment in orthopedic diseases PReS Latin America Basic Pediatric Rheumatology Course 2015 Aguas de São Pedro, São Paulo, Brazil Carmen L. De Cunto carmen.decunto@hospitalitaliano.org.ar Sección
MORE FOR BACKS PROGRAM. User guide for osteopaths and osteopathy code list (ICD-10-AM codes)
 MORE FOR BACKS PROGRAM User guide for osteopaths and osteopathy code list (ICD-10-AM codes) APRIL 2017 WELCOME TO THE MORE FOR BACKS PROGRAM This program reimburses 100% of the agreed charge for an initial
MORE FOR BACKS PROGRAM User guide for osteopaths and osteopathy code list (ICD-10-AM codes) APRIL 2017 WELCOME TO THE MORE FOR BACKS PROGRAM This program reimburses 100% of the agreed charge for an initial
Unit 1 The Human Body in Motion AREA OF STUDY 1 - HOW DOES THE MUSCULOSKELETAL SYSTEM WORK TO PRODUCE MOVEMENT?
 Unit 1 The Human Body in Motion AREA OF STUDY 1 - HOW DOES THE MUSCULOSKELETAL SYSTEM WORK TO PRODUCE MOVEMENT? Acute and Chronic Injuries of the Musculoskeletal System AREA OF STUDY 1 - HOW DOES THE MUSCULOSKELETAL
Unit 1 The Human Body in Motion AREA OF STUDY 1 - HOW DOES THE MUSCULOSKELETAL SYSTEM WORK TO PRODUCE MOVEMENT? Acute and Chronic Injuries of the Musculoskeletal System AREA OF STUDY 1 - HOW DOES THE MUSCULOSKELETAL
Unit 6 Orthopedic Physiotherapy
 Unit 6 Orthopedic Physiotherapy Task 1 Human Body Look at the diagram and study the main muscles of the body. Define which muscles have the following functions: Pectoral muscle lowers the arm. Intercostals
Unit 6 Orthopedic Physiotherapy Task 1 Human Body Look at the diagram and study the main muscles of the body. Define which muscles have the following functions: Pectoral muscle lowers the arm. Intercostals
EHLERS DANLOS SYNDROME. Fransiska Malfait, MD PhD Centre for Medical Genetics Ghent University Hospital Ghent, Belgium
 EHLERS DANLOS SYNDROME Fransiska Malfait, MD PhD Centre for Medical Genetics Ghent University Hospital Ghent, Belgium EDS is a heritable collagen disorder Heterogeneous group of diseases with: - Multi-systemic
EHLERS DANLOS SYNDROME Fransiska Malfait, MD PhD Centre for Medical Genetics Ghent University Hospital Ghent, Belgium EDS is a heritable collagen disorder Heterogeneous group of diseases with: - Multi-systemic
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
History: Pain Traumatic vs. atraumatic? Acute vs Chronic Previous procedures done on the knee? Swelling, catching, instability General Setup Examine standing, sitting and supine Evaluate gait Examine hip
COURSE OUTLINE-IB 128: SPORTS MEDICINE INTRODUCTION
 COURSE OUTLINE-IB 128: SPORTS MEDICINE INTRODUCTION Definition of sports medicine Pre-participation physical exam Epidemiology of sports injuries injury rates for various sports sports risks relative to
COURSE OUTLINE-IB 128: SPORTS MEDICINE INTRODUCTION Definition of sports medicine Pre-participation physical exam Epidemiology of sports injuries injury rates for various sports sports risks relative to
Patella Instability in Children and Adolescents
 Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Evaluation of the Knee and Shoulder
 Evaluation of the Knee and Shoulder Karen J. Boselli, MD Northeast Regional Nurse Practitioner Conference May 2018 Knee Overview History Examination Top 5 diagnoses When to image When to refer Pain most
Evaluation of the Knee and Shoulder Karen J. Boselli, MD Northeast Regional Nurse Practitioner Conference May 2018 Knee Overview History Examination Top 5 diagnoses When to image When to refer Pain most
Osteoarthritis. RA Hughes
 Osteoarthritis RA Hughes Osteoarthritis (OA) OA is the most common form of arthritis and the most common joint disease Most of the people who have OA are older than age 45, and women are more commonly
Osteoarthritis RA Hughes Osteoarthritis (OA) OA is the most common form of arthritis and the most common joint disease Most of the people who have OA are older than age 45, and women are more commonly
Information on hypermobility (Ehlers-Danlos) and Dysautonomia, for parents and professors.
 Information on hypermobility (Ehlers-Danlos) and Dysautonomia, for parents and professors. The Ehlers-Danlos Syndrome (EDS) is a disease and not only a condition, that affects 40% of the population. These
Information on hypermobility (Ehlers-Danlos) and Dysautonomia, for parents and professors. The Ehlers-Danlos Syndrome (EDS) is a disease and not only a condition, that affects 40% of the population. These
General appearance examination
 Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
For more information call , or visit
 Target Coding ICD-10 List for Chiropractic HEADACHE G43: Migraine G43.0: Migraine without aura (common migraine) G43.009: Migraine without aura, not intractable, without status migrainosus (migraine without
Target Coding ICD-10 List for Chiropractic HEADACHE G43: Migraine G43.0: Migraine without aura (common migraine) G43.009: Migraine without aura, not intractable, without status migrainosus (migraine without
Physical Examination of the Knee
 History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
History: Pain Traumatic vs. atraumatic Acute vs Chronic Mechanism of injury Swelling, catching, instability Previous evaluation and treatment General Setup Examine standing, sitting and supine Evaluate
I have no relevant relationships/affiliations with any proprietary entity producing health care goods or services.
 I have no relevant relationships/affiliations with any proprietary entity producing health care goods or services. OCSA 2017 OMT For Extremity Disorders and Torticollis in Children Ava C. Stanczak, D.O.,
I have no relevant relationships/affiliations with any proprietary entity producing health care goods or services. OCSA 2017 OMT For Extremity Disorders and Torticollis in Children Ava C. Stanczak, D.O.,
THE SUPPORT YOU NEED.
 PROFESSIONAL ORTHOPAEDIC RANGE THE SUPPORT YOU NEED. Introductory Offer ends 30 JUNE 2018 BACK Introductory Special Offer 20% OFF. VLK-2262 Sacro Belt Provides support and compression to the sacroiliac
PROFESSIONAL ORTHOPAEDIC RANGE THE SUPPORT YOU NEED. Introductory Offer ends 30 JUNE 2018 BACK Introductory Special Offer 20% OFF. VLK-2262 Sacro Belt Provides support and compression to the sacroiliac
Trauma & Orthopaedic Undergraduate Syllabus
 Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
Pediatric Orthopedic Pathology Pathology 2 Dr. Gary Mumaugh
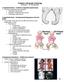 Pediatric Orthopedic Pathology Pathology 2 Dr. Gary Mumaugh Congenital Defects - Clubfoot (congenital equinovarus) Forefoot is adducted and supinated o Positional equinovarus o Idiopathic congenital equinovarus
Pediatric Orthopedic Pathology Pathology 2 Dr. Gary Mumaugh Congenital Defects - Clubfoot (congenital equinovarus) Forefoot is adducted and supinated o Positional equinovarus o Idiopathic congenital equinovarus
Sports Medicine Unit 16 Elbow
 Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Disclosures Head to Toe: Common Sports Injuries in Kids
 Disclosures Head to Toe: Common Sports Injuries in Kids None R. Jay Lee MD Director Pediatric Orthopaedic Fellowship Assistant Professor Pediatric Orthopaedics Johns Hopkins / Bloomberg Children s Objectives
Disclosures Head to Toe: Common Sports Injuries in Kids None R. Jay Lee MD Director Pediatric Orthopaedic Fellowship Assistant Professor Pediatric Orthopaedics Johns Hopkins / Bloomberg Children s Objectives
Functional Well-Being. Neck, Shoulders and Wrist
 Functional Well-Being Neck, Shoulders and Wrist 1 Neck Definition and Structure Your neck (cervical spine) is made up of 7 vertebrae that extend from the skull to the upper torso. 2 Causes of Neck Pain
Functional Well-Being Neck, Shoulders and Wrist 1 Neck Definition and Structure Your neck (cervical spine) is made up of 7 vertebrae that extend from the skull to the upper torso. 2 Causes of Neck Pain
Ehlers-Danlos syndrome hypermobility type is associated with rheumatic diseases
 Supplementary Information Scientific Reports Ehlers-Danlos syndrome hypermobility type is associated with rheumatic diseases Kyla R Rodgers, BS 1, Jiang Gui, PhD 2,3,6, Mary Beth P. Dinulos, MD 4,5,7,
Supplementary Information Scientific Reports Ehlers-Danlos syndrome hypermobility type is associated with rheumatic diseases Kyla R Rodgers, BS 1, Jiang Gui, PhD 2,3,6, Mary Beth P. Dinulos, MD 4,5,7,
Chapter 30 - Musculoskeletal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
MORE FOR BACKS PROGRAM. User guide for chiropractors and chiropractic code list (ICD-10-AM codes)
 MORE FOR BACKS PROGRAM User guide for chiropractors and chiropractic code list (ICD-10-AM codes) APRIL 2017 WELCOME TO THE MORE FOR BACKS PROGRAM This program reimburses 100% of the agreed charge for an
MORE FOR BACKS PROGRAM User guide for chiropractors and chiropractic code list (ICD-10-AM codes) APRIL 2017 WELCOME TO THE MORE FOR BACKS PROGRAM This program reimburses 100% of the agreed charge for an
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MUSCULOSKELETAL INJURIES
 WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy
 Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy Prevalence of Overuse Injuries 30 to 50% of all sport injuries are from overuse In some sports
Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy Prevalence of Overuse Injuries 30 to 50% of all sport injuries are from overuse In some sports
SMF PCP Treatment & Referral Guideline Orthopedics Developed February 1, 2003 Revised: October, 2011
 SUTTER MEDICAL FOUNDATION (SMF) 2800 L Street, 7 th Floor Sacramento, CA 95816 SMF PCP Treatment & Referral Guideline Orthopedics Developed February 1, 2003 Revised: October, 2011 I. Shoulder Pain...Page
SUTTER MEDICAL FOUNDATION (SMF) 2800 L Street, 7 th Floor Sacramento, CA 95816 SMF PCP Treatment & Referral Guideline Orthopedics Developed February 1, 2003 Revised: October, 2011 I. Shoulder Pain...Page
The role of orthopedic surgery in the Ehlers-Danlos syndromes
 The Ehlers-Danlos Society P.O. Box 87463 Montgomery Village, MD 20886 USA Phone: +1 410-670-7577 The Ehlers-Danlos Society - Europe Office 7 35-37 Ludgate Hill London EC4M 7JN UK Phone: +44 203 887 6132
The Ehlers-Danlos Society P.O. Box 87463 Montgomery Village, MD 20886 USA Phone: +1 410-670-7577 The Ehlers-Danlos Society - Europe Office 7 35-37 Ludgate Hill London EC4M 7JN UK Phone: +44 203 887 6132
DISCOID MENISCUS. Description
 DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
What Are Shoulder Problems?
 What Are the Parts of the Shoulder? The shoulder joint is made up of bones held in place by muscles, tendons, and ligaments. Tendons are tough cords of tissue that hold the shoulder muscles to bones. They
What Are the Parts of the Shoulder? The shoulder joint is made up of bones held in place by muscles, tendons, and ligaments. Tendons are tough cords of tissue that hold the shoulder muscles to bones. They
erhem Thoracal spine section Elastic shoulder brace with support bracing Application:
 ERH 53/1 Elastic shoulder brace with support bracing Augmentation of proper upright posture Stable fractures of the clavicle Scheuermann s kyphosis Funnel chest Osteoporotic lesions The shoulder brace
ERH 53/1 Elastic shoulder brace with support bracing Augmentation of proper upright posture Stable fractures of the clavicle Scheuermann s kyphosis Funnel chest Osteoporotic lesions The shoulder brace
DISCOID MENISCUS. Description
 Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
MORE FOR BACKS PROGRAM. User guide for chiropractors and chiropractic code list (ICD-10-AM codes)
 MORE FOR BACKS PROGRAM User guide for chiropractors and chiropractic code list (ICD-10-AM codes) MAY 2018 WELCOME TO THE MORE FOR BACKS PROGRAM This program reimburses 100% of the agreed charge for an
MORE FOR BACKS PROGRAM User guide for chiropractors and chiropractic code list (ICD-10-AM codes) MAY 2018 WELCOME TO THE MORE FOR BACKS PROGRAM This program reimburses 100% of the agreed charge for an
Types of osteoarthritis
 ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
13/02/2011. Ergonomics
 13/02/2011 Ergonomics Workplace Safety Electrical Safety Medical & First Aid Lockout/Tag-out Confined Space Asbestos Control Fire Prevention Personal Protective Equipment Hazard Communication Chemical
13/02/2011 Ergonomics Workplace Safety Electrical Safety Medical & First Aid Lockout/Tag-out Confined Space Asbestos Control Fire Prevention Personal Protective Equipment Hazard Communication Chemical
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
