Osteomyelitis is an uncommon but potentially. Success of Short-Course Parenteral AntibioticTherapy for Acute Osteomyelitis of Childhood
|
|
|
- Ashlyn Phelps
- 5 years ago
- Views:
Transcription
1 Success of Short-Course Parenteral AntibioticTherapy for Acute Osteomyelitis of Childhood Clinical Pediatrics Volume 46 Number 1 January Sage Publications / hosted at Richard Bachur, MD, Zrinka Pagon, MD The outcome of acute osteomyelitis treated with sequential therapy consisting of a short course of parenteral antibiotics, followed by oral antibiotics, was studied. To be considered acute osteomyelitis, related symptoms must have been present for less than 2 weeks before diagnosis. Short-course parenteral antibiotics (therapy for 7 days or less) and then oral antibiotics were used to treat 29 patients (median age, 6.3 years). Pathogens were identified from blood cultures and bone aspirates. Staphylococcus aureus was isolated in 59%. Median duration of parenteral antibiotics and oral antibiotics was 4 days (range, 0-7 days) and 28 days (range, days), respectively. Median duration of combined (parenteral and oral) therapy was 32 days (range, days). No failures or complications were noted at the 6-month follow-up, which was available for 27 patients. Shortcourse parenteral antibiotic therapy followed by oral therapy appears to be effective for treatment of acute, uncomplicated osteomyelitis. Keywords: osteomyelitis; parenteral antibiotic therapy; Staphylococcus aureus Introduction Osteomyelitis is an uncommon but potentially debilitating disease in children. The reported incidence is 0.02% in children younger than 13 years old. 1 The diagnosis of osteomyelitis involves a combination of clinical findings, laboratory data, bacteriologic tests, and radiologic studies. 2-4 The standard textbook recommendation for treatment of osteomyelitis consists of 3 to 6 weeks of antibiotic therapy, with varied recommendations for the duration of parenteral therapy. 5-8 The minimum duration of parenteral antibiotic treatment has been recently reconsidered The variation reported in treatment regimens is presumably based on historical treatment failures with shorter courses of therapy and the lack of distinguishing acute versus chronic osteomyelitis. We have summarized our experience with short-course parenteral antibiotic therapy for acute osteomyelitis to add insight into the efficacy and safety of such treatment. From the Division of Emergency Medicine, Children s Hospital, Boston, Massachusetts. Address correspondence to: Richard Bachur, MD, Division of Emergency Medicine, 300 Longwood Avenue, Children s Hospital, Boston, MA Methods We reviewed the medical records of all children with the discharged diagnosis of osteomyelitis for 5 consecutive years from 1995 to Charts were reviewed for the accuracy of diagnosis. Osteomyelitis was defined as a combination of (1) clinical suspicion based on fever, bone pain, or decreased usage of a limb, and (2) an abnormal bone scan or magnetic resonance image (MRI). We defined acute osteomyelitis as those patients with symptoms present for less than 14 days before diagnosis. Patients were excluded from the study for osteomyelitis symptoms exceeding 14 days (or recurrent), a chronic underlying medical condition, immunodeficiency, associated fracture, septic arthritis, chronic arthritis, multifocal osteomyelitis, or concomitant bone abscess (as defined by the need for surgical débridement or drainage). Parenteral antibiotic therapy for 7 days or less (intramuscular or intravenous administration) was considered short-course therapy. Patients with acute osteomyelitis who were treated with short-course antibiotic therapy constituted the study group. Followup was obtained from the hospital record or from the primary care office record. Cure was defined by the absence of symptoms for 1 year after discontinuing 30
2 Antibiotic Therapy for Acute Osteomyelitis / Bachur and Pagon 31 Long Bones antibiotics. Failures were defined by the need to switch from oral antibiotics back to parenteral antibiotics or restarting antibiotics after being discontinued. Statistical analyses were conducted using SPSS 12 (SPSS, Chicago, Ill). Medians and interquartile ranges (IQR, 25th-75th percentile) were provided for non-normal data. Confidence intervals for proportions were calculated using Stata 6 (StataCorp, College Station, Texas). The institutional review board of the hospital approved the study. Results Table 1. Study Group Our hospital discharged 138 patients with the principal diagnosis of osteomyelitis. A review of their records found that 100 (72%) fulfilled criteria for acute osteomyelitis. Sixty-one were excluded from the study because of chronic underlying disease (9), immunodeficiency (10), associated fracture (10), septic arthritis (5), multifocal osteomyelitis (14), and concomitant bone abscess (13). Of the remaining 39 patients, a short-course regimen of parenteral antibiotics was used to treat 29 (74%). Median age of the 29 study patients was 6.3 years (IQR, years), and 19 (70%) patients were boys. Distribution of the sites of osteomyelitis is shown in Table 1. Clinical Presentation Sites of Osteomyelitis Others Distal femur 7 Talus 2 Proximal femur 3 Pubis 2 Distal tibia 7 Ilium 1 Proximal tibia 2 Clavicle 1 Proximal fibula 1 Distal fibula 1 Distal humerus 1 Distal radius 1 Median duration of symptoms before admission was 4 days (range, 0-12 days). Decreased limb use (93%), pain (90%), and fever (83%) were the most common presenting symptoms. Point tenderness of the involved bone was the most common sign on physical examination, occurring in 72% of the patients. Other signs included decreased range of motion in the adjacent joint (52%), erythema (38%), and pain (31%). Laboratory Data All the patients had a complete blood count and erythrocyte sedimentation rate (ESR, Westergren) on admission. The median white blood cell count (WBC) was 11800/mm 3 (IQR, /mm 3 ), and median absolute neutrophil count was 7400/mm 3 (IQR, /mm 3 ). The median ESR was 42 mm/h (IQR, mm/h). Bacteriology Etiologic agents were identified in 20 (69%) of 29 patients. One or more blood cultures were obtained from all 29 patients. S aureus was the only pathogen identified in 10 (34%) of the blood cultures. Bone aspirate was performed in 14 (48%) patients, and 9 (64%) of these cultures were positive: S aureus was isolated in 6 patients and Streptococcus pyogenes in 3 patients. Two patients had both a positive blood culture and bone culture. In 1 patient, S aureus was isolated from soft tissue overlying the infected bone. None of the S aureus isolates were methicillin resistant. Radiology Plain radiographs were obtained in 28 patients (96%). Findings from radiographs at the time of admission were normal in 15 (54%), soft tissue changes were noted in 7 (25%), and 6 (21%) had decreased bone density and abnormality of the bone cortex or marrow. Technetium-labeled bone scans were performed in 24 (83%) of 29 patients, and all demonstrated focal, increased uptake. Nine patients (31%) had an MRI, including the 5 patients who did not have a bone scan; all had findings consistent with osteomyelitis. Management The median duration of parenteral antibiotic therapy was 4 days (range, 0-7 days). The median duration of subsequent oral antibiotic therapy was 28 days (range, days). The median duration of total combined antibiotic therapy was 32 days (range, 20-49). For patients with bacteremia, the median duration of parenteral therapy was 6 days (range, 4-7 days) (Figure 1). Cefazolin was the most frequently used parenteral antibiotic (93%), with a median daily dosage
3 32 Clinical Pediatrics / Vol. 46, No. 1, January Days of Antibiotic Therapy Parenteral Oral Figure 1. Parenteral and oral antibiotic therapy for each study patient. Patients with bacteremia are indicated by an arrow. of 150 mg/kg (IQR, mg/kg), and cephalexin was the most frequently used oral antibiotic (90%) with a median daily dosage of 100 mg/kg (IQR, mg/kg). Median duration of hospitalization was 4 days (range, 2-7 days). Follow-up for at least 6 months was available for 27 (93%) patients. Median duration of follow-up was 1.2 years (IQR, years). No failures and no other complications have been noted (95% CI, 0%-12%). Acute Uncomplicated Osteomyelitis Treated With Long-Course Therapy Ten patients with acute uncomplicated osteomyelitis were eligible for the short course of parenteral antibiotics but received longer courses of therapy. Their median age was 6.0 years (IQR, years), the median duration of parenteral therapy was 15 days (range, days), the median hospitalization was 10 days (range, 1-28 days), and the median total antibiotic therapy was 32 days (range days). No failures or complications were noted among this group of patients over a median follow-up of 1.5 years. Discussion Osteomyelitis is a relatively rare disease of childhood and is therefore difficult to study prospectively. Additionally, even among the rare cases of osteomyelitis, several patient subgroups must be considered and managed differently, including acute versus chronic osteomyelitis, transcutaneous inoculation versus hematogenous osteomyelitis, bony abscess versus uncomplicated osteomyelitis, and immunocompromised versus immunocompetent hosts. Most of the medical literature regarding treatment of osteomyelitis has been derived from historical reviews. During the last 2 decades, increasing evidence shows that acute hematogenous osteomyelitis can be treated with a short course of parenteral antibiotics and then a more prolonged course of oral antibiotics. We undertook this study to review our experience with such therapy for acute osteomyelitis. In defining our patients, we used a standard definition of acute, uncomplicated osteomyelitis as symptoms of less than 2 weeks and no associated open wounds, fractures, or joint infection. Accordingly, the presentation of patients with acute osteomyelitis in our study group was similar to previous reports. 12,13
4 Antibiotic Therapy for Acute Osteomyelitis / Bachur and Pagon 33 Clinical features of our study group matched previous study patients with regard to sites of infection, results of the WBC count and ESR, frequency of bacteremia, 9,16,19 predominance of S aureus as the etiologic agent, 9,14,16 and the lack of plain radiographic changes at the time of diagnosis. 7,8 From a diagnostic standpoint, all patients had abnormal findings on the bone scan or MRI, and bone aspiration was superior to blood cultures for determining the pathogen, as previously noted. 13,15,20 Currently, most acute osteomyelitis is treated with sequential intravenous and then oral antibiotics. 5,9,17, This approach to treatment has become more common only in the last decade; before that time, therapy was entirely intravenous and lasted from 4 to 8 weeks. 13,25,26 Shorter intravenous antibiotic treatment and a greater reliance on oral antibiotic therapy has been supported in retrospective 10 and prospective studies, 24,27-29 but textbook recommendations and common practice continue to vary for duration of parenteral therapy and criteria for switching to oral antibiotic therapy. 6-8 The reasons for such variation between the medical literature and current practice are many. First, study populations reported in the osteomyelitis literature are often different because of variables of age, duration symptoms, pathogens, presence of joint involvement or bone abscess, and immune status; therefore, general recommendations for treating all cases will tend to suggest more conservative (longer) courses of parenteral antibiotics. Second, the size of the study groups has been limited, 24,27-29 and the duration of follow-up has been relatively short, 27, 29 which raises uncertainty about the long-term outcome for patients treated with short courses of parenteral antibiotics. For some, the prolonged use of oral antibiotics has raised concern about compliance. 22,23,30 Additionally, there is no consensus on a minimum duration of parenteral antibiotic treatment and no accepted recommendation on when to transition to oral therapy. Proposals for when to switch to oral therapy have included improved clinical condition (including the absence of fever) plus either falling ESR, 22 improved plain radiographs, 29 and more recently, a decreasing level of C-reactive protein. 31 The recent availability and confidence in home intravenous therapy with percutaneously placed central venous catheters has led to many patients getting prolonged parenteral therapy even beyond stages of clinical improvement, and the risk of these catheters must be weighed against the risk of treatment failure with oral therapy. 32 Finally, treatment failures using short-course parenteral therapy have been reported 27, 29, 33 ; however, the study groups in those studies include complex cases of osteomyelitis. In review of the prior related studies, two prospective studies by Cole et al, 34,35 were among the first studies to establish the efficacy of short-course parenteral therapy in acute osteomyelitis. The authors defined acute osteomyelitis based on history and symptoms of less than 14 days duration. Diagnosis was made on history and physical exam and not necessarily confirmed by radiograph. In the first study of 55 patients published in 1982, the authors reported their median parenteral therapy duration of 3 days (range, 2 to 5 days) and a total duration of antibiotic therapy of 6 weeks. Antibiotic levels were not monitored, follow-up was for 4 years after discharge from the hospital, and no failures were noted. In 1987, the same group reported excellent results with an additional 50 patients enrolled in a similar prospective study. The authors further shortened the duration of antibiotic therapy to a total of 3 weeks (with the same initial parenteral therapy as previously described) and showed similar outcomes. Most recently, Peltola et al 11,12 reported a prospective study of 50 pediatric cases of acute S aureus osteomyelitis. Their definition of acute osteomyelitis was identical to previous definition by Cole. Their patients received an average of 4 days of intravenous cephradine or clindamycin, followed by oral antibiotics for a total duration of treatment of 3 to 4 weeks. Peak antimicrobial serum inhibitory values or serum bactericidal levels were not monitored. The authors had excellent results with no complications or failures over an average follow-up of 27 months. They also concluded that the treatment of acute staphylococcal osteomyelitis could be simplified and made easier for patients. A corresponding editorial by Nelson 36 addressed the importance of monitoring of serum bactericidal activity of the oral antibiotics. Nelson agreed with the concept of an early switch to oral therapy, but he strongly argued that antibiotic levels need to be monitored for successful therapy. 36 This argument stemmed from his own studies conducted in 1978 and 1982, in which treatment failures were attributed to low serum bactericidal levels. 30, 37 The most recent retrospective analysis on acute osteomyelitis is one by Karwowska et al. 19 Their study presents the outcomes of 128 cases of acute
5 34 Clinical Pediatrics / Vol. 46, No. 1, January 2007 osteomyelitis treated between 1984 and Their median duration of intravenous therapy was 11 days, and the median duration of the total antibiotic course was 38 days. The median duration of followup was 1.2 months (range, months), and complications occurred in 6.6% of patients. Antibiotic levels were monitored in a few patients, and the only defined risk factor for complications was the higher incidence of polymicrobial infections, and not the duration of antibiotic therapy. Our study results agree with the prospective studies by Peltola et al 11 and Cole et al 34, 35 and retrospective studies from Nelson et al 30 and Karwowska et al. 19 Our median duration of parenteral therapy was only 4 days, and our median total antibiotic therapy was 32 days. Our median duration of hospital stay was 4 days, and our median duration of follow-up was 1 year. We did not identify any failures or complications within a limited follow-up. In our institution, general pediatricians alone care for some patients, and others are managed by the specialty services of infectious disease or orthopedic surgery; therefore, the decisions regarding antibiotic course, transition to oral therapy, and follow-up are not standardized. In general, the criteria for switching from intravenous to oral therapy often requires clinical improvement that includes a return to normal body temperature, improvement in local symptoms, and an ability to be compliant with an oral antibiotic comparable to the intravenous drug. In practice, patients often remain in the hospital pending results of cultures, antibiotic sensitivities of any isolates, and clearance of associated bacteremia. Furthermore, serum bactericidal levels (as an estimate of compliance and adequacy of oral therapy) have not been recommended routinely, but we use high doses of oral antibiotics and maintain close clinical follow-up. Although not an issue for our patients in this study, increasing rates of methicillin-resistant S aureus 38 may require prolonged courses of intravenous vancomycin in the future; this highlights the increasing importance for an accurate microbiologic diagnosis. Our data have several limitations. The confidence interval for our observed absence of complications or failures could still be as high as 12%. Although no complications of short-course parenteral therapy were noted, patients who were excluded for bony abscess may represent patients who were initially considered for short-course parenteral therapy before the need for surgical intervention was recognized. Additionally, with a relatively short duration of follow-up, long-term consequences of our management may not be appreciated. Finally, it is impossible to retrospectively determine why some patients who were eligible for short-course parenteral therapy received longer courses of antibiotic therapy. Conclusion Our results are adding to the accumulating data that short-course parenteral therapy for acute, uncomplicated osteomyelitis is safe and successful. As a corollary, failure to respond to initial parenteral antibiotic treatment should prompt further intravenous therapy and investigation for a bone sequestrum, subperiosteal abscess, or an atypical or resistant pathogen. Acknowledgment Zrinka Pagon, MD, was supported in part by the Zlatko and Joyce Balokovic Fellowship, Prof. Mary Ellen Avery Fellowship, and American Association for Infectious Diseases Fellowship. References 1. Bremmer A, Neligman G. Pyogenic osteitis. Recent Adv Pediatr. 1958: Demopulos GA, Bleck EE, McDougall IR. Role of radionuclide imaging in the diagnosis of acute osteomyelitis. J Pediatr Orthop. 1988;8: Gold R. Diagnosis of osteomyelitis. Pediatr Rev. 1991; 12: Roy DR. Osteomyelitis. Pediatr Rev. 1995;16: ; quiz Gutierrez K. Bone and joint infections in children. Pediatr Clin North Am. 2005;52: , vi. 6. Narasimban N, Marks M. Osteomyelitis and septic arthritis. In: Nelson W, ed. Nelson Textbook of Pediatrics. 15th ed. Philadelphia: W.B. Saunders Co; 1996: Krogstad P, Smith A. Osteomyelitis and septic arthritis. In: Feigin R, Cherry J, eds. Textbook of Pediatric Infectious Diseases. Vol 1. 4th ed. Philadelphia: W.B. Saunders Co; 1998: Mader J, Calhoun J. Osteomyelitis. In: Mandell G, ed. Principles and Practice of Infectious Diseases. Vol 1. 4th ed. New York: Churchill Livingston; 1995: Dunkle LM, Brock N. Long-term follow-up of ambulatory management of osteomyelitis. Clin Pediatr (Phila). 1982;21:
6 Antibiotic Therapy for Acute Osteomyelitis / Bachur and Pagon Syrogiannopoulos GA, Nelson JD. Duration of antimicrobial therapy for acute suppurative osteoarticular infections. Lancet. 1988;1: Peltola H, Unkila-Kallio L, Kallio MJ. Simplified treatment of acute staphylococcal osteomyelitis of childhood. The Finnish Study Group [see comments]. Pediatrics. 1997;99: Unkila-Kallio L, Kallio MJ, Peltola H. Acute haematogenous osteomyelitis in children in Finland. Finnish Study Group. Ann Med. 1993;25: Dich VQ, Nelson JD, Haltalin KC. Osteomyelitis in infants and children. A review of 163 cases. Am J Dis Child. 1975;129: Jackson MA, Nelson JD. Etiology and medical management of acute suppurative bone and joint infections in pediatric patients. J Pediatr Orthop. 1982;2: Mollan RA, Piggot J. Acute osteomyelitis in children. J Bone Joint Surg (Br). 1977;59: Scott RJ, Christofersen MR, Robertson WW Jr, Davidson RS, Rankin L, Drummond DS. Acute osteomyelitis in children: a review of 116 cases. J Pediatr Orthop. 1990;10: Prober CG. Oral antibiotic therapy for bone and joint infections. Pediatr Infect Dis. 1982;1: Unkila-Kallio L, Kallio MJ, Eskola J, Peltola H. Serum C-reactive protein, erythrocyte sedimentation rate, and white blood cell count in acute hematogenous osteomyelitis of children. Pediatrics. 1994;93: Karwowska A, Davies HD, Jadavji T. Epidemiology and outcome of osteomyelitis in the era of sequential intravenousoral therapy. Pediatr Infect Dis J. 1998;17: Faden H, Grossi M. Acute osteomyelitis in children. Reassessment of etiologic agents and their clinical characteristics. Am J Dis Child. 1991;145: Nelson JD. Acute osteomyelitis in children. Infect Dis Clin North Am. 1990;4: Dirschl DR. Acute pyogenic osteomyelitis in children. Orthop Rev. 1994;23: Dagan R. Management of acute hematogenous osteomyelitis and septic arthritis in the pediatric patient. Pediatr Infect Dis J. 1993;12: Kolyvas E, Ahronheim G, Marks MI, Gledhill R, Owen H, Rosenthall L. Oral antibiotic therapy of skeletal infections in children. Pediatrics. 1980;65: Mader JT, Landon GC, Calhoun J. Antimicrobial treatment of osteomyelitis. Clin Orthop. 1993: LaMont RL, Anderson PA, Dajani AS, Thirumoorthi MC. Acute hematogenous osteomyelitis in children. J Pediatr Orthop. 1987;7: Feigin RD, Pickering LK, Anderson D, Keeney RE, Shackleford PG. Clindamycin treatment of osteomyelitis and septic arthritis in children. Pediatrics. 1975; 55: Bryson YJ, Connor JD, LeClerc M, Giammona ST. Highdose oral dicloxacillin treatment of acute staphylococcal osteomyelitis in children. J Pediatr. 1979;94: Tetzlaff TR, McCracken GH, Jr., Nelson JD. Oral antibiotic therapy for skeletal infections of children. II. Therapy of osteomyelitis and suppurative arthritis. J Pediatr. 1978;92: Nelson JD, Bucholz RW, Kusmiesz H, Shelton S. Benefits and risks of sequential parenteral-oral cephalosporin therapy for suppurative bone and joint infections. J Pediatr Orthop. 1982;2: Roine I, Faingezicht I, Arguedas A, Herrera JF, Rodriguez F. Serial serum C-reactive protein to monitor recovery from acute hematogenous osteomyelitis in children. Pediatr Infect Dis J. 1995;14: Maraqa NF, Gomez MM, Rathore MH. Outpatient parenteral antimicrobial therapy in osteoarticular infections in children. J Pediatr Orthop. Jul-Aug 2002;22: Green JH. Cloxacillin in treatment of acute osteomyelitis. Br Med J. 1967;2: Cole WG, Dalziel RE, Leitl S. Treatment of acute osteomyelitis in childhood. J Bone Joint Surg [Br]. 1982;64: Cole WG. Treatment of early-acute osteomyelitis in childhood: brief report. J Bone Joint Surg [Br]. 1987;69: Nelson JD. Toward simple but safe management of osteomyelitis [comment]. Pediatrics. 1997;99: Nelson JD. Oral antibiotic therapy for serious infections in hospitalized patients [editorial]. J Pediatr. 1978;92: Martinez-Aguilar G, Avalos-Mishaan A, Hulten K, Hammerman W, Mason EO Jr, Kaplan SL. Communityacquired, methicillin-resistant and methicillin-susceptible Staphylococcus aureus musculoskeletal infections in children. Pediatr Infect Dis J. 2004;23:
Antibiotic Management of Pediatric Osteomyelitis
 Reprinted from www.antimicrobe.org Sandra Arnold, M.D. Antibiotic Management of Pediatric Osteomyelitis Several points uncertainty exist regarding the antimicrobial management of acute hematogenous osteomyelitis,
Reprinted from www.antimicrobe.org Sandra Arnold, M.D. Antibiotic Management of Pediatric Osteomyelitis Several points uncertainty exist regarding the antimicrobial management of acute hematogenous osteomyelitis,
A cute haematogenous osteomyelitis (AHOM) is a bacterial
 512 ORIGINAL ARTICLE Fosfomycin for the initial treatment of acute haematogenous osteomyelitis N Corti, F H Sennhauser, U G Stauffer, D Nadal... See end of article for authors affiliations... Correspondence
512 ORIGINAL ARTICLE Fosfomycin for the initial treatment of acute haematogenous osteomyelitis N Corti, F H Sennhauser, U G Stauffer, D Nadal... See end of article for authors affiliations... Correspondence
Although acute hematogenous osteomyelitis
 Group A -Hemolytic Streptococcal Osteomyelitis in Children Ekopimo O. Ibia, MD, MPH* ; Menfo Imoisili, MD, MPH* ; and Andreas Pikis, MD* ABSTRACT. Objective Little attention has been given to acute hematogenous
Group A -Hemolytic Streptococcal Osteomyelitis in Children Ekopimo O. Ibia, MD, MPH* ; Menfo Imoisili, MD, MPH* ; and Andreas Pikis, MD* ABSTRACT. Objective Little attention has been given to acute hematogenous
TREATMENT OF ACUTE OSTEOMYELITIS IN CHILDHOOD
 TREATMENT OF ACUTE OSTEOMYELITIS IN CHILDHOOD W. G. COLE, R. E. DALZIEL, S. LEITL From The Royal Children s Hospital, Melbourne A protocol of treatment for acute haematogenous osteomyelitis has been evaluated
TREATMENT OF ACUTE OSTEOMYELITIS IN CHILDHOOD W. G. COLE, R. E. DALZIEL, S. LEITL From The Royal Children s Hospital, Melbourne A protocol of treatment for acute haematogenous osteomyelitis has been evaluated
ESPID New Bone and Joint Infection Guidelines
 ESPID New Bone and Joint Infection Guidelines Theoklis Zaoutis, MD, MSCE Professor of Pediatrics and Epidemiology Perelman School of Medicine at the University of Pennsylvania Chief, Division of Infectious
ESPID New Bone and Joint Infection Guidelines Theoklis Zaoutis, MD, MSCE Professor of Pediatrics and Epidemiology Perelman School of Medicine at the University of Pennsylvania Chief, Division of Infectious
Osteomieliti STEOMIE
 OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
Osteomyelitis in infancy and childhood: A clinical and diagnostic overview M. Mearadji
 Osteomyelitis in infancy and childhood: A clinical and diagnostic overview M. Mearadji International Foundation for Pediatric Imaging Aid Introduction Osteomyelitis is a relative common disease in infancy
Osteomyelitis in infancy and childhood: A clinical and diagnostic overview M. Mearadji International Foundation for Pediatric Imaging Aid Introduction Osteomyelitis is a relative common disease in infancy
Prof Oluwadiya KS FMCS (Orthop) Consultant Orthopaedic Surgeon / Associate Professor Division of Orthopaedics and Traumatology Department of Surgery
 Prof Oluwadiya KS FMCS (Orthop) Consultant Orthopaedic Surgeon / Associate Professor Division of Orthopaedics and Traumatology Department of Surgery College of Health Sciences Ladoke Akintola University
Prof Oluwadiya KS FMCS (Orthop) Consultant Orthopaedic Surgeon / Associate Professor Division of Orthopaedics and Traumatology Department of Surgery College of Health Sciences Ladoke Akintola University
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
Acute Osteomyelitis: similar to septic arthritis but up to 40% may be afebrile swelling overlying the bone & tenderness
 Osteomyelitis / Bone and Joint Infections Bone infections in children are usually from haematogenous bacterial seeding to a single joint, usually the lower limbs, but may be multifocal. Approximately 10%
Osteomyelitis / Bone and Joint Infections Bone infections in children are usually from haematogenous bacterial seeding to a single joint, usually the lower limbs, but may be multifocal. Approximately 10%
P-1 (Former P-1) Are pediatric patients on oral or intravenous steroids at an increased risk of developing septic arthritis?
 Pediatrics Prevention P-1 (Former P-1) Are pediatric patients on oral or intravenous steroids at an increased risk of developing septic arthritis? RESEARCHED BY: Muhammad Amin Chinoy MD, Pakistan Literature:
Pediatrics Prevention P-1 (Former P-1) Are pediatric patients on oral or intravenous steroids at an increased risk of developing septic arthritis? RESEARCHED BY: Muhammad Amin Chinoy MD, Pakistan Literature:
Case Report Sequential MR Images and Radiographs of Epiphyseal Osteomyelitis in the Distal Femur of an Infant
 Case Reports in Radiology Volume 2013, Article ID 672815, 4 pages http://dx.doi.org/10.1155/2013/672815 Case Report Sequential MR Images and Radiographs of Epiphyseal Osteomyelitis in the Distal Femur
Case Reports in Radiology Volume 2013, Article ID 672815, 4 pages http://dx.doi.org/10.1155/2013/672815 Case Report Sequential MR Images and Radiographs of Epiphyseal Osteomyelitis in the Distal Femur
Research Article Septic Arthritis of the Pediatric Shoulder: From Infancy to Adolescence
 International Pediatrics Volume 2016, Article ID 3086019, 4 pages http://dx.doi.org/10.1155/2016/3086019 Research Article Septic Arthritis of the Pediatric Shoulder: From Infancy to Adolescence Justin
International Pediatrics Volume 2016, Article ID 3086019, 4 pages http://dx.doi.org/10.1155/2016/3086019 Research Article Septic Arthritis of the Pediatric Shoulder: From Infancy to Adolescence Justin
Osteomyelitis Samir S. Shah, MD, MSCE
 Osteomyelitis Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending Physician in Infectious Diseases
Osteomyelitis Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending Physician in Infectious Diseases
Utility of magnetic resonance imaging in the follow-up of children affected by acute osteomyelitis.
 Curr Pediatr Res 017; 1 (): 354-358 ISSN 0971-903 www.currentpediatrics.com Utility of magnetic resonance imaging in the follow-up of children affected by acute osteomyelitis. Valentina Fabiano 1, Giulia
Curr Pediatr Res 017; 1 (): 354-358 ISSN 0971-903 www.currentpediatrics.com Utility of magnetic resonance imaging in the follow-up of children affected by acute osteomyelitis. Valentina Fabiano 1, Giulia
Diagnosis of acute haematogenous. osteomyelitis (AHOM) and septic arthritis, 20 years experience at the University Children s Hospital Basel
 Original article Peer reviewed article SWISS MED WKLY 21;131:575 581 www.smw.ch 575 Diagnosis of acute haematogenous osteomyelitis and septic arthritis: 2 years experience at the University Children s
Original article Peer reviewed article SWISS MED WKLY 21;131:575 581 www.smw.ch 575 Diagnosis of acute haematogenous osteomyelitis and septic arthritis: 2 years experience at the University Children s
OSTEOMYELITIS AND SEPTIC ARTHRITIS IN CHILDREN: REVIEW
 OSTEOMYELITIS AND SEPTIC ARTHRITIS IN CHILDREN: REVIEW Dr. Roshan Sah* and Prof. Lui Ke bin Department of Orthopaedics, The First Affiliated Peoples Hospital of Yangtze University, Jingzhou, Hubei, PR.
OSTEOMYELITIS AND SEPTIC ARTHRITIS IN CHILDREN: REVIEW Dr. Roshan Sah* and Prof. Lui Ke bin Department of Orthopaedics, The First Affiliated Peoples Hospital of Yangtze University, Jingzhou, Hubei, PR.
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Case Report Acute Haematogenous Metacarpal Osteomyelitis in Children: A Case Report and Review of Literature
 Case Reports in Infectious Diseases Volume 2011, Article ID 674820, 4 pages doi:10.1155/2011/674820 Case Report Acute Haematogenous Metacarpal Osteomyelitis in Children: A Case Report and Review of Literature
Case Reports in Infectious Diseases Volume 2011, Article ID 674820, 4 pages doi:10.1155/2011/674820 Case Report Acute Haematogenous Metacarpal Osteomyelitis in Children: A Case Report and Review of Literature
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 2.417, ISSN: , Volume 3, Issue 11, December 2015
 MANAGEMENT OF PATHOLOGICAL FRACTURE SHAFT HUMERUS SECONDARY TO BACTERIAL OSTEOMYELITIS: A CASE REPORT DR. NARENDRA SINGH KUSHWAHA* DR.SHAH WALIULLAH** DR.VINEET KUMAR*** DR.VINEET SHARMA**** *Asst. Professor,
MANAGEMENT OF PATHOLOGICAL FRACTURE SHAFT HUMERUS SECONDARY TO BACTERIAL OSTEOMYELITIS: A CASE REPORT DR. NARENDRA SINGH KUSHWAHA* DR.SHAH WALIULLAH** DR.VINEET KUMAR*** DR.VINEET SHARMA**** *Asst. Professor,
Management of acute osteomyelitis: a ten-year experience
 Infectious Disease Reports 2016; volume 8:6350 Management of acute osteomyelitis: a ten-year experience Caitlin Helm, Emily Huschart, Rajat Kaul, Samina Bhumbra, R. Alexander Blackwood, Deepa Mukundan
Infectious Disease Reports 2016; volume 8:6350 Management of acute osteomyelitis: a ten-year experience Caitlin Helm, Emily Huschart, Rajat Kaul, Samina Bhumbra, R. Alexander Blackwood, Deepa Mukundan
Infections Amenable to OPAT. (Nabin Shrestha + Ajay Mathur)
 3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
(48.5%); aseptic necrosis of the femoral head, 75
 Annals of the Rheumatic Diseases, 1986; 45, 911-915 Acute osteomyelitis in Nigerians with sickle cell disease WALTON W EBONG From the University College Hospital, Ibadan, Nigeria SUMMARY Acute osteomyelitis
Annals of the Rheumatic Diseases, 1986; 45, 911-915 Acute osteomyelitis in Nigerians with sickle cell disease WALTON W EBONG From the University College Hospital, Ibadan, Nigeria SUMMARY Acute osteomyelitis
MRI Non-Joint Extremity Questionnaire
 MRI n-joint Extremity Questionnaire INSTRUCTIONS FOR COMPLETING QUESTIONNAIRE: Answer all of the initial questions (Pages 1 and 2) Select the reason for imaging by answering question #6. Based on your
MRI n-joint Extremity Questionnaire INSTRUCTIONS FOR COMPLETING QUESTIONNAIRE: Answer all of the initial questions (Pages 1 and 2) Select the reason for imaging by answering question #6. Based on your
Bacteriological Profile of Post Traumatic Osteomyelitis in a Tertiary Care Centre
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 367-372 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.044
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 367-372 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.044
Acute hematogenous osteomyelitis and septic arthritis in children
 Osteomyelitis J Microbiol Immunol and septic Infect arthritis 2003;36:260-265 Acute hematogenous osteomyelitis and septic arthritis in children Hui-Chin Kao 1, Yhu-Chering Huang 2, Cheng-Hsun Chiu 2, Luan-Yin
Osteomyelitis J Microbiol Immunol and septic Infect arthritis 2003;36:260-265 Acute hematogenous osteomyelitis and septic arthritis in children Hui-Chin Kao 1, Yhu-Chering Huang 2, Cheng-Hsun Chiu 2, Luan-Yin
ARTICLE. Differentiating Osteomyelitis From Vaso-occlusive Crisis. Elizabeth Berger, MD; Natasha Saunders, MD; Lisa Wang, MSc; Jeremy N.
 ARTICLE Sickle Cell Disease in Children Differentiating Osteomyelitis From Vaso-occlusive Crisis Elizabeth Berger, MD; Natasha Saunders, MD; Lisa Wang, MSc; Jeremy N. Friedman, MD Objective: To identify
ARTICLE Sickle Cell Disease in Children Differentiating Osteomyelitis From Vaso-occlusive Crisis Elizabeth Berger, MD; Natasha Saunders, MD; Lisa Wang, MSc; Jeremy N. Friedman, MD Objective: To identify
Management of Acute Haematogenous Osteomyelitis. SAPOS ICL 2017 Anthony Robertson
 Management of Acute Haematogenous Osteomyelitis SAPOS ICL 2017 Anthony Robertson Diagnosis Diagnosis RED FLAGS: Nunn, Rollinson;; SAMJ 2007 Acute hip pain in a child Infant with loss of movement in a limb
Management of Acute Haematogenous Osteomyelitis SAPOS ICL 2017 Anthony Robertson Diagnosis Diagnosis RED FLAGS: Nunn, Rollinson;; SAMJ 2007 Acute hip pain in a child Infant with loss of movement in a limb
Maximal Daily. Dose. mg/kg/day %
 The new england journal of medicine Table 1. Antibiotic Treatment for Acute Osteomyelitis in Children.* Antibiotic Empirical treatment First-generation cephalosporin, if prevalence of MSSA in community
The new england journal of medicine Table 1. Antibiotic Treatment for Acute Osteomyelitis in Children.* Antibiotic Empirical treatment First-generation cephalosporin, if prevalence of MSSA in community
Case report. Open Access. Abstract
 Open Access Case report Primary sternal osteomyelitis in a 40 days old infant: a case report and review of the literature Nikolaos S Pettas 1 *, Alexandros P Apostolopoulos 2 *, Ioannis Flieger 3 and Omiros
Open Access Case report Primary sternal osteomyelitis in a 40 days old infant: a case report and review of the literature Nikolaos S Pettas 1 *, Alexandros P Apostolopoulos 2 *, Ioannis Flieger 3 and Omiros
MUSCULOSKELETAL INFECTIONS IN CHILDREN. Dr Caren Landes Alder Hey Children s NHS Foundation Trust Liverpool
 MUSCULOSKELETAL INFECTIONS IN CHILDREN Dr Caren Landes Alder Hey Children s NHS Foundation Trust Liverpool MUSCULOSKELETAL INFECTIONS Common and uncommon infections Common and uncommon presentations Imaging
MUSCULOSKELETAL INFECTIONS IN CHILDREN Dr Caren Landes Alder Hey Children s NHS Foundation Trust Liverpool MUSCULOSKELETAL INFECTIONS Common and uncommon infections Common and uncommon presentations Imaging
Khawaja Tahir Mahmood et al /J. Pharm. Sci. & Res. Vol.2 (11), 2010,
 RATIONAL USE OF ANTIBIOTICS IN OSTEOMYELITIS Khawaja Tahir Mahmood 1, Maryam Nadeem 2 Sundas Nadeem 2 and Fatima Amin 2 1 Drug Testing Lab, Lahore 2 Department of Pharmacy, Lahore College For Women University,
RATIONAL USE OF ANTIBIOTICS IN OSTEOMYELITIS Khawaja Tahir Mahmood 1, Maryam Nadeem 2 Sundas Nadeem 2 and Fatima Amin 2 1 Drug Testing Lab, Lahore 2 Department of Pharmacy, Lahore College For Women University,
ACUTE AND CHRONIC OSTEOMYELITIS
 ACUTE AND CHRONIC OSTEOMYELITIS DEFINITION Inflammation of the bone caused by an infecting organism HISTORY In the early 1900 s about 20% of patients with osteomyelitis died and patients who survived had
ACUTE AND CHRONIC OSTEOMYELITIS DEFINITION Inflammation of the bone caused by an infecting organism HISTORY In the early 1900 s about 20% of patients with osteomyelitis died and patients who survived had
Fever Interval before Diagnosis, Prior Antibiotic Treatment, and Clinical Outcome for Young Children with Bacterial Meningitis
 MAJOR ARTICLE Fever Interval before Diagnosis, Prior Antibiotic Treatment, and Clinical Outcome for Young Children with Bacterial Meningitis Bema K. Bonsu 1 and Marvin B. Harper 2 1 Department of Medicine,
MAJOR ARTICLE Fever Interval before Diagnosis, Prior Antibiotic Treatment, and Clinical Outcome for Young Children with Bacterial Meningitis Bema K. Bonsu 1 and Marvin B. Harper 2 1 Department of Medicine,
The use of CRP within a clinical prediction algorithm for the differentiation of septic arthritis and transient synovitis in children
 CHILDREN S ORTHOPAEDICS The use of CRP within a clinical prediction algorithm for the differentiation of septic arthritis and transient synovitis in children R. Singhal, D. C. Perry, F. N. Khan, D. Cohen,
CHILDREN S ORTHOPAEDICS The use of CRP within a clinical prediction algorithm for the differentiation of septic arthritis and transient synovitis in children R. Singhal, D. C. Perry, F. N. Khan, D. Cohen,
Acute Community-acquired Osteoarticular Infections in Children: High Incidence of Concomitant Bone and Joint Involvement
 Also available online http://www.e-jmii.com ISSN 1684-1182 Volume 43 Number 4 August 2010 Indexed in MEDLINE/Index Medicus, SCIE, BIOSIS, EMBASE, Aidsline, CancerLit, Chemical Abstracts, HealthSTAR The
Also available online http://www.e-jmii.com ISSN 1684-1182 Volume 43 Number 4 August 2010 Indexed in MEDLINE/Index Medicus, SCIE, BIOSIS, EMBASE, Aidsline, CancerLit, Chemical Abstracts, HealthSTAR The
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH)
 Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Treatment of infection
 Clinica Ortopedica e Traumatologica Università degli Studi di Pavia Fondazione IRCCS Policlinico San Matteo Chairman: Prof. F. Benazzo Goals: - Healing of infection - Healing of fracture - Try to keep
Clinica Ortopedica e Traumatologica Università degli Studi di Pavia Fondazione IRCCS Policlinico San Matteo Chairman: Prof. F. Benazzo Goals: - Healing of infection - Healing of fracture - Try to keep
THE USE OF THE PENICILLINASE-RESISTANT
 Therapeutic problems THE USE OF THE PENICILLINASE-RESISTANT PENICILLIN IN THE PNEUMONIAS OF CHILDREN MARTHA D. Yow, MARY A. SOUTH AND CHARLES G. HESS From the Department of Pediatrics, Baylor University
Therapeutic problems THE USE OF THE PENICILLINASE-RESISTANT PENICILLIN IN THE PNEUMONIAS OF CHILDREN MARTHA D. Yow, MARY A. SOUTH AND CHARLES G. HESS From the Department of Pediatrics, Baylor University
Osteomyelitis and Septic Joints; Practical Considerations. Coleen K. Cunningham
 Osteomyelitis and Septic Joints; Practical Considerations Coleen K. Cunningham Goals/objectives To improve understanding of the diagnosis, treatment, and follow-up of pediatric bone and joint infections
Osteomyelitis and Septic Joints; Practical Considerations Coleen K. Cunningham Goals/objectives To improve understanding of the diagnosis, treatment, and follow-up of pediatric bone and joint infections
MAJOR ARTICLE. (See the editorial commentary by Bradley, on pages )
 MAJOR ARTICLE Prospective, Randomized Trial of 10 Days versus 30 Days of Antimicrobial Treatment, Including a Short- Term Course of Parenteral Therapy, for Childhood Septic Arthritis Heikki Peltola, 1
MAJOR ARTICLE Prospective, Randomized Trial of 10 Days versus 30 Days of Antimicrobial Treatment, Including a Short- Term Course of Parenteral Therapy, for Childhood Septic Arthritis Heikki Peltola, 1
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia
 Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Morbidity & Mortality Conference Downstate Medical Center. Daniel Kaufman, MD
 Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery
 The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
The Spine Journal 6 (2006) 311 315 Serum C-reactive protein levels correlate with clinical response in patients treated with antibiotics for wound infections after spinal surgery Mustafa H. Khan, MD a,
Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry
 doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
Osteomyelitis and Complications in Pediatric Patients: Case and Literature Review
 Osteomyelitis and Complications in Pediatric Patients: Case and Literature Review Matthew Martin, D.O.; Matthew Carlson,D.O.; Michelle Mark, D.O.; Glenn Barnes, D.O.; Michelle Lin, D.O. Presented by: Michelle
Osteomyelitis and Complications in Pediatric Patients: Case and Literature Review Matthew Martin, D.O.; Matthew Carlson,D.O.; Michelle Mark, D.O.; Glenn Barnes, D.O.; Michelle Lin, D.O. Presented by: Michelle
1 Department of Pediatrics, Aarhus University Hospital, Aarhus, Denmark 2 Department of Clinical Microbiology, Aarhus University Hospital,
 Case Report Life-threatening MRSA sepsis with bilateral pneumonia, osteomyelitis, and septic arthritis of the knee in a previously healthy 13-year-old boy: a case report Acta Radiologica Open 5(10) 1 7!
Case Report Life-threatening MRSA sepsis with bilateral pneumonia, osteomyelitis, and septic arthritis of the knee in a previously healthy 13-year-old boy: a case report Acta Radiologica Open 5(10) 1 7!
Interesting Case Series. Pyogenic (Suppurative) Flexor Tenosynovitis: Assessment and Management
 Interesting Case Series Pyogenic (Suppurative) Flexor Tenosynovitis: Assessment and Management Renee L. Barry, BS a,nicholass.adams,md a,b, and Matthew D. Martin, MD a,b,c a Michigan State University College
Interesting Case Series Pyogenic (Suppurative) Flexor Tenosynovitis: Assessment and Management Renee L. Barry, BS a,nicholass.adams,md a,b, and Matthew D. Martin, MD a,b,c a Michigan State University College
PSOAS ABSCESS. Dr Noman Ullah Wazir
 PSOAS ABSCESS Dr Noman Ullah Wazir Psoas Major muscle The psoas major is a long fusiform muscle located on the side of the lumbar region of the vertebral column and brim of the lesser pelvis. Psoas Major
PSOAS ABSCESS Dr Noman Ullah Wazir Psoas Major muscle The psoas major is a long fusiform muscle located on the side of the lumbar region of the vertebral column and brim of the lesser pelvis. Psoas Major
EPIDEMIOLOGICAL, CLINICAL AND LABORATORY ASPECTS OF INFECTIOUS CELLULITIS
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 1-2012 EPIDEMIOLOGICAL, CLINICAL AND LABORATORY ASPECTS OF INFECTIOUS CELLULITIS C. COSTACHE 1 D. COSTACHE
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 1-2012 EPIDEMIOLOGICAL, CLINICAL AND LABORATORY ASPECTS OF INFECTIOUS CELLULITIS C. COSTACHE 1 D. COSTACHE
Foot infections in persons with diabetes are
 DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
Methicillin-Resistant Staphylococcus aureus (MRSA) S urveillance Report 2008 Background Methods
 Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Medical Center, Jerusalem, affiliated with the Faculty of Health Sciences, Ben-Gurion University of the Negev, Beer Sheva, Israel
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2005.01200.x Non-Typhi Salmonella gastroenteritis in children presenting to the emergency department: characteristics of patients with associated bacteraemia M. Bar-Meir
ORIGINAL ARTICLE 10.1111/j.1469-0691.2005.01200.x Non-Typhi Salmonella gastroenteritis in children presenting to the emergency department: characteristics of patients with associated bacteraemia M. Bar-Meir
Acute Hematogenous Osteomyelitis in Children Recognition and Management
 Pediatr Drugs 2004; 6 (6): 333-346 THERAPY IN PRACTICE 1174-5878/04/0006-0333/$31.00/0 2004 Adis Data Information BV. All rights reserved. Acute Hematogenous Osteomyelitis in Children Recognition and Management
Pediatr Drugs 2004; 6 (6): 333-346 THERAPY IN PRACTICE 1174-5878/04/0006-0333/$31.00/0 2004 Adis Data Information BV. All rights reserved. Acute Hematogenous Osteomyelitis in Children Recognition and Management
a Total Hip Prosthesis by Clostridum perfringens. A Case Report
 Haematogenous Infection of a Total Hip Prosthesis by Clostridum perfringens. A Case Report CHAPTER 5 CHAPTER 5 5.1. Introduction In orthopaedic surgery, an infection of a prosthesis is a very serious,
Haematogenous Infection of a Total Hip Prosthesis by Clostridum perfringens. A Case Report CHAPTER 5 CHAPTER 5 5.1. Introduction In orthopaedic surgery, an infection of a prosthesis is a very serious,
Pyogenic spondylitis as a complication of ear piercing : Differentiating between spondylitis and discitis
 Acta Orthop. Belg., 2007, 73, 128-132 CASE REPORT Pyogenic spondylitis as a complication of ear piercing : Differentiating between spondylitis and discitis Miguel SEWNATH, Tina FABER, Rene CASTELEIN From
Acta Orthop. Belg., 2007, 73, 128-132 CASE REPORT Pyogenic spondylitis as a complication of ear piercing : Differentiating between spondylitis and discitis Miguel SEWNATH, Tina FABER, Rene CASTELEIN From
with chronic disease, orthopedic hardware, puncture wounds, or an infected contiguous focus were excluded.
 Role of Operative or Interventional Radiology-Guided Cultures for Osteomyelitis J. Chase McNeil, MD, Andrea R. Forbes, RN, Jesus G. Vallejo, MD, Anthony R. Flores, MD, MPH, PhD, Kristina G. Hultén, PhD,
Role of Operative or Interventional Radiology-Guided Cultures for Osteomyelitis J. Chase McNeil, MD, Andrea R. Forbes, RN, Jesus G. Vallejo, MD, Anthony R. Flores, MD, MPH, PhD, Kristina G. Hultén, PhD,
ORIGINAL ARTICLES. Haematogenous pyogenic bone and joint sepsis reducing avoidable morbidity. Methods. T Nunn, P Rollinson
 Haematogenous pyogenic bone and joint sepsis reducing avoidable morbidity T Nunn, P Rollinson Background and objectives. Delayed presentation of haematogenous bone and joint sepsis is common in our childhood
Haematogenous pyogenic bone and joint sepsis reducing avoidable morbidity T Nunn, P Rollinson Background and objectives. Delayed presentation of haematogenous bone and joint sepsis is common in our childhood
Nuclear medicine and Prosthetic Joint Infections
 Nuclear medicine and Prosthetic Joint Infections Christophe Van de Wiele, M.D., Ph.D. Department of Nuclear Medicine, University Hospital Ghent, Belgium Orthopedic prostheses: world market 1996 Prosthetic
Nuclear medicine and Prosthetic Joint Infections Christophe Van de Wiele, M.D., Ph.D. Department of Nuclear Medicine, University Hospital Ghent, Belgium Orthopedic prostheses: world market 1996 Prosthetic
Prolonged infection at the tibial bone tunnel after anterior cruciate ligament reconstruction
 Fukushima J. Med. Sci., Vol. 63, No. 2, 2017 [Case Report] Prolonged infection after ACL Reconstruction 121 Prolonged infection at the tibial bone tunnel after anterior cruciate ligament reconstruction
Fukushima J. Med. Sci., Vol. 63, No. 2, 2017 [Case Report] Prolonged infection after ACL Reconstruction 121 Prolonged infection at the tibial bone tunnel after anterior cruciate ligament reconstruction
Chronic recurrent multifocal osteomyelitis (CRMO) advancing the diagnosis
 Roderick et al. Pediatric Rheumatology (2016) 14:47 DOI 10.1186/s12969-016-0109-1 SHORT REPORT Chronic recurrent multifocal osteomyelitis (CRMO) advancing the diagnosis M. R. Roderick 1,2*, R. Shah 2,
Roderick et al. Pediatric Rheumatology (2016) 14:47 DOI 10.1186/s12969-016-0109-1 SHORT REPORT Chronic recurrent multifocal osteomyelitis (CRMO) advancing the diagnosis M. R. Roderick 1,2*, R. Shah 2,
Bacteria may reach bone through direct inoculation from traumatic
 The new england journal of medicine review article Edward W. Campion, M.D., Editor Acute Osteomyelitis in Children Heikki Peltola, M.D., and Markus Pääkkönen, M.D. From Children s Hospital, University
The new england journal of medicine review article Edward W. Campion, M.D., Editor Acute Osteomyelitis in Children Heikki Peltola, M.D., and Markus Pääkkönen, M.D. From Children s Hospital, University
ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST
 www.manchesterchildrensent.com ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST A CHILD WITH EARACHE UNCOMPLICATED AOM ACUTE OTITIS MEDIA Acute otitis media
www.manchesterchildrensent.com ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST A CHILD WITH EARACHE UNCOMPLICATED AOM ACUTE OTITIS MEDIA Acute otitis media
Updates in Osteomyelitis Management
 Updates in Osteomyelitis Management Russell McCulloh, MD Assistant Professor, Pediatrics and Internal Medicine Divisions of Hospital Medicine and Infectious Diseases Children s Mercy Hospital Disclosure
Updates in Osteomyelitis Management Russell McCulloh, MD Assistant Professor, Pediatrics and Internal Medicine Divisions of Hospital Medicine and Infectious Diseases Children s Mercy Hospital Disclosure
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Factors predictive of relapse in adult bacterial osteomyelitis of long bones.
 Garcia del Pozo et al. BMC Infectious Diseases (2018) 18:635 https://doi.org/10.1186/s12879-018-3550-6 RESEARCH ARTICLE Open Access Factors predictive of relapse in adult bacterial osteomyelitis of long
Garcia del Pozo et al. BMC Infectious Diseases (2018) 18:635 https://doi.org/10.1186/s12879-018-3550-6 RESEARCH ARTICLE Open Access Factors predictive of relapse in adult bacterial osteomyelitis of long
Bone and prosthetic joint infections: what the ID specialist needs?
 Bone and prosthetic joint infections: what the ID specialist needs? Andrej Trampuz Charité University Medicine Berlin Center for Septic Surgery Hip and knee replacements in Europe Germany Austria Belgium
Bone and prosthetic joint infections: what the ID specialist needs? Andrej Trampuz Charité University Medicine Berlin Center for Septic Surgery Hip and knee replacements in Europe Germany Austria Belgium
Title: Childhood osteomyelitis-incidence and differentiation from other acute onset musculoskeletal features in a population-based study
 Author's response to reviews Title: Childhood osteomyelitis-incidence and differentiation from other acute onset musculoskeletal features in a population-based study Authors: Øystein Riise (oystein.riise@rikshospitalet.no)
Author's response to reviews Title: Childhood osteomyelitis-incidence and differentiation from other acute onset musculoskeletal features in a population-based study Authors: Øystein Riise (oystein.riise@rikshospitalet.no)
Setting The setting of the study was tertiary care (teaching hospitals). The study was conducted in Hong Kong.
 Sequential intravenous/oral antibiotic vs. continuous intravenous antibiotic in the treatment of pyogenic liver abscess Ng F H, Wong W M, Wong B C, Kng C, Wong S Y, Lai K C, Cheng C S, Yuen W C, Lam S
Sequential intravenous/oral antibiotic vs. continuous intravenous antibiotic in the treatment of pyogenic liver abscess Ng F H, Wong W M, Wong B C, Kng C, Wong S Y, Lai K C, Cheng C S, Yuen W C, Lam S
Musculoskeletal infection (MSKI) is a common cause
 ORIGINAL ARTICLE A Novel Classification System Based on Dissemination of Musculoskeletal Infection is Predictive of Hospital Outcomes Megan E. Mignemi, MD,* Michael A. Benvenuti, BS,w Thomas J. An, BA,w
ORIGINAL ARTICLE A Novel Classification System Based on Dissemination of Musculoskeletal Infection is Predictive of Hospital Outcomes Megan E. Mignemi, MD,* Michael A. Benvenuti, BS,w Thomas J. An, BA,w
Osteomyelitis and septic arthritis in children: current concepts
 REVIEW C URRENT OPINION Osteomyelitis and septic arthritis in children: current concepts Emily R. Dodwell Purpose of review The cause, epidemiology, diagnosis, and treatment of osteoarticular infections
REVIEW C URRENT OPINION Osteomyelitis and septic arthritis in children: current concepts Emily R. Dodwell Purpose of review The cause, epidemiology, diagnosis, and treatment of osteoarticular infections
Infection. Arthrocentesis: Cell count Differential Culture. Infection and associated microorganism(s) confirmed
 Painful joint History and examination Radiograph of affected joint Erythrocyte sedimentation rate C-reactive protein Infection No infection suspected Arthrocentesis: Cell count Differential Culture Stop
Painful joint History and examination Radiograph of affected joint Erythrocyte sedimentation rate C-reactive protein Infection No infection suspected Arthrocentesis: Cell count Differential Culture Stop
Critical Review Form Diagnostic Test
 Critical Review Form Diagnostic Test The clinical presentation and impact of diagnostic delays on emergency department patients with spinal epidural abscess, J Emerg Med 2004; 26:285-291 Objectives: To
Critical Review Form Diagnostic Test The clinical presentation and impact of diagnostic delays on emergency department patients with spinal epidural abscess, J Emerg Med 2004; 26:285-291 Objectives: To
Tuberculosis Of The Talus: Report Of A Child Case
 ISPUB.COM The Internet Journal of Rheumatology Volume 1 Number 1 Tuberculosis Of The Talus: Report Of A Child Case Y Teklali, Z El Alami, T El Madhi, H Gourinda, A Miri Citation Y Teklali, Z El Alami,
ISPUB.COM The Internet Journal of Rheumatology Volume 1 Number 1 Tuberculosis Of The Talus: Report Of A Child Case Y Teklali, Z El Alami, T El Madhi, H Gourinda, A Miri Citation Y Teklali, Z El Alami,
SEPTIC ARTHRITIS. Dr Ahmed Husam Al Ahmed Rheumatologist SYRIA. University of Science and technology Hospital Sanaa Yemen 18/Dec/2014
 SEPTIC ARTHRITIS Dr Ahmed Husam Al Ahmed Rheumatologist SYRIA University of Science and technology Hospital Sanaa Yemen 18/Dec/2014 Objectives be able to define Septic Arthritis know what factors predispose
SEPTIC ARTHRITIS Dr Ahmed Husam Al Ahmed Rheumatologist SYRIA University of Science and technology Hospital Sanaa Yemen 18/Dec/2014 Objectives be able to define Septic Arthritis know what factors predispose
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Device-associated Events Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of
Device-associated Events Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
BONE AND JOINT INFECTION. Dr.Jónás Zoltán Dept.of Orthopaedics
 BONE AND JOINT INFECTION Dr.Jónás Zoltán Dept.of Orthopaedics www.ortopedia.dote.hu Order of verbal exams: The students are able to register for the exam on the Neptun system. The students pick two titles,
BONE AND JOINT INFECTION Dr.Jónás Zoltán Dept.of Orthopaedics www.ortopedia.dote.hu Order of verbal exams: The students are able to register for the exam on the Neptun system. The students pick two titles,
Clinical and Microbiological Evaluation of Osteomyelitis
 Bahrain Medical Bulletin, Vol.23, No.2, June 2001 Clinical and Microbiological Evaluation of Osteomyelitis Haider Abdul-Lateef Mousa, MBChB, MSc* Thamer A Hamdan, MBChB, FRCS** Sundus S Bakr, BSc, PhD***
Bahrain Medical Bulletin, Vol.23, No.2, June 2001 Clinical and Microbiological Evaluation of Osteomyelitis Haider Abdul-Lateef Mousa, MBChB, MSc* Thamer A Hamdan, MBChB, FRCS** Sundus S Bakr, BSc, PhD***
Title: Successful treatment of Candida Discitis with 5-Flucytosine and Fluconazole.
 Title: Successful treatment of Candida Discitis with 5-Flucytosine and Fluconazole. Authors: S.M. Rachapalli, R Malaiya, TAMT Mohd, RA Hughes Institution: Department of Rheumatology, St Peter s Hospital,
Title: Successful treatment of Candida Discitis with 5-Flucytosine and Fluconazole. Authors: S.M. Rachapalli, R Malaiya, TAMT Mohd, RA Hughes Institution: Department of Rheumatology, St Peter s Hospital,
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
EAST PRACTICE MANAGEMENT GUIDELINES WORK GROUP: UPDATE TO PRACTICE MANAGEMENT GUIDELINES FOR PROPHYLACTIC ANTIBIOTIC USE IN OPEN FRACTURES
 EAST PRACTICE MANAGEMENT GUIDELINES WORK GROUP: UPDATE TO PRACTICE MANAGEMENT GUIDELINES FOR PROPHYLACTIC ANTIBIOTIC USE IN OPEN FRACTURES William S. Hoff, MD, FACS 1, John A. Bonadies, MD, FACS 2, Riad
EAST PRACTICE MANAGEMENT GUIDELINES WORK GROUP: UPDATE TO PRACTICE MANAGEMENT GUIDELINES FOR PROPHYLACTIC ANTIBIOTIC USE IN OPEN FRACTURES William S. Hoff, MD, FACS 1, John A. Bonadies, MD, FACS 2, Riad
Pyomyositis is a primary bacterial infection of
 Case Report & Literature Review Tropical Myositis (Pyomyositis) in Children in Temperate Climates: A Report of 3 Cases on Long Island, New York, and a Review of the Literature Jacob Weinberg, MD, Samara
Case Report & Literature Review Tropical Myositis (Pyomyositis) in Children in Temperate Climates: A Report of 3 Cases on Long Island, New York, and a Review of the Literature Jacob Weinberg, MD, Samara
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29
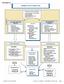 PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
Acute Diverticulitis. Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh
 Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
EXTREMITY injury is a common cause for visits
 ACADEMIC EMERGENCY MEDICINE October 1999, Volume 6, Number 10 1005 Validation of the Ankle Rules in Children with Ankle Injuries AMY C. PLINT, MD, BLAKE BULLOCH, MD, MARTIN H. OSMOND, MD, IAN STIELL, MD,
ACADEMIC EMERGENCY MEDICINE October 1999, Volume 6, Number 10 1005 Validation of the Ankle Rules in Children with Ankle Injuries AMY C. PLINT, MD, BLAKE BULLOCH, MD, MARTIN H. OSMOND, MD, IAN STIELL, MD,
The Challenge of Managing Staphylococcus aureus Bacteremia
 The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
Of 142 cases where sex was known, 56 percent were male; of 127cases where race was known, 90 percent were white, 4 percent were
 Group B Streptococcus Surveillance Report 2014 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: November 2015 Background The Active Bacterial Core surveillance
Group B Streptococcus Surveillance Report 2014 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: November 2015 Background The Active Bacterial Core surveillance
Cierny-Mader classification of chronic osteomyelitis: Preoperative evaluation with cross-sectional imaging
 Cierny-Mader classification of chronic osteomyelitis: Preoperative evaluation with cross-sectional imaging Poster No.: C-590 Congress: ECR 2009 Type: Topic: Educational Exhibit Musculoskeletal Authors:
Cierny-Mader classification of chronic osteomyelitis: Preoperative evaluation with cross-sectional imaging Poster No.: C-590 Congress: ECR 2009 Type: Topic: Educational Exhibit Musculoskeletal Authors:
Case Report: Arthroscopic Treatment of Psoas Abscess Concurrent with Septic Arthritis of the Hip Joint
 Case Report: Arthroscopic Treatment of Psoas Abscess Concurrent with Septic Arthritis of the Hip Joint Pil Whan Yoon, MD*, Jeong Joon Yoo, MD, Hee Joong Kim, MD, and Kang Sup Yoon, MD* Department of Orthopedic
Case Report: Arthroscopic Treatment of Psoas Abscess Concurrent with Septic Arthritis of the Hip Joint Pil Whan Yoon, MD*, Jeong Joon Yoo, MD, Hee Joong Kim, MD, and Kang Sup Yoon, MD* Department of Orthopedic
BCG OSTEITIS. B. Varbanova 1, V. Vasileva 1, P. Minchev 2, R. Nedeva 1 and E. Dyankov 1 BCG. . Bacille-Calmette Guerin (BCG) BCG.
 68 BCG. 1,. 1,. 2,. 1. 1 1 2, BCG OSTEITIS B. Varbanova 1, V. Vasileva 1, P. Minchev 2, R. Nedeva 1 and E. Dyankov 1 1 University Hospital Sv. Marina Varna 2 University Children s Clinic of Pulmonary Diseases,
68 BCG. 1,. 1,. 2,. 1. 1 1 2, BCG OSTEITIS B. Varbanova 1, V. Vasileva 1, P. Minchev 2, R. Nedeva 1 and E. Dyankov 1 1 University Hospital Sv. Marina Varna 2 University Children s Clinic of Pulmonary Diseases,
Evaluation of Vancomycin Continuous Infusion in Trauma Patients
 OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
Case Report Arthroscopic Treatment of Septic Arthritis of the Elbow in a 4-Year-Old Girl
 Case Reports in Orthopedics Volume 2015, Article ID 853974, 4 pages http://dx.doi.org/10.1155/2015/853974 Case Report Arthroscopic Treatment of Septic Arthritis of the Elbow in a 4-Year-Old Girl Masashi
Case Reports in Orthopedics Volume 2015, Article ID 853974, 4 pages http://dx.doi.org/10.1155/2015/853974 Case Report Arthroscopic Treatment of Septic Arthritis of the Elbow in a 4-Year-Old Girl Masashi
TUBERCULOUS OSTEOMYELITIS OF PATELLA: A CASE REPORT Babu B. Hundekar 1
 TUBERCULOUS OSTEOMYELITIS OF PATELLA: A Babu B. Hundekar 1 HOW TO CITE THIS ARTICLE: Babu B. Hundekar. Tuberculous Osteomyelitis of Patella: A Case Report. Journal of Evolution of Medical and Dental Sciences
TUBERCULOUS OSTEOMYELITIS OF PATELLA: A Babu B. Hundekar 1 HOW TO CITE THIS ARTICLE: Babu B. Hundekar. Tuberculous Osteomyelitis of Patella: A Case Report. Journal of Evolution of Medical and Dental Sciences
RESTORING PATENCY TO CENTRAL VENOUS ACCESS DEVICES
 RESTORING PATENCY TO CENTRAL VENOUS ACCESS DEVICES Indications Venous access is poor Intravenous therapy involves venous sclerosants Ambulatory chemotherapy given as an outpatient Repeated sampling, or
RESTORING PATENCY TO CENTRAL VENOUS ACCESS DEVICES Indications Venous access is poor Intravenous therapy involves venous sclerosants Ambulatory chemotherapy given as an outpatient Repeated sampling, or
6/18/2014. John K. Midturi, DO, MPH June 5 th, 2014
 John K. Midturi, DO, MPH June 5 th, 2014 Heterogeneous disease Disease of antiquity Evolved from disease of high mortality disease with high morbidity One of the most difficult infections to treat Thomas
John K. Midturi, DO, MPH June 5 th, 2014 Heterogeneous disease Disease of antiquity Evolved from disease of high mortality disease with high morbidity One of the most difficult infections to treat Thomas
Case report Central Eur J Paed 2017;13(2): DOI /p
 Case report Central Eur J Paed 2017;13(2):166-170 DOI 10.5457/p2005-114.185 SEPARATION OF THE DISTAL HUMERAL EPIPHYSIS IN A NEWBORN: A CASE AND LITERATURE REVIEW Mojca VIDRIH 1, Damjana KLJUČEVŠEK 2, Tomo
Case report Central Eur J Paed 2017;13(2):166-170 DOI 10.5457/p2005-114.185 SEPARATION OF THE DISTAL HUMERAL EPIPHYSIS IN A NEWBORN: A CASE AND LITERATURE REVIEW Mojca VIDRIH 1, Damjana KLJUČEVŠEK 2, Tomo
Effects of renal function on the intraosseous. concentrations and inhibitory effects on. prophylactic cefazolin in knee arthroplasty
 European Review for Medical and Pharmacological Sciences 2016; 20: 5216-5222 Effects of renal function on the intraosseous concentration and inhibitory effect of prophylactic cefazolin in knee arthroplasty
European Review for Medical and Pharmacological Sciences 2016; 20: 5216-5222 Effects of renal function on the intraosseous concentration and inhibitory effect of prophylactic cefazolin in knee arthroplasty
Effect of Antibiotic Pretreatment on Cerebrospinal Fluid Profiles of Children with Acute Bacterial Meningitis
 Effect of Antibiotic Pretreatment on Cerebrospinal Fluid Profiles of Children with Acute Bacterial Meningitis Adhikari S, 1* Gauchan E, 1 BK G, 1 Rao KS 1 1 Department of Paediatrics, Manipal College of
Effect of Antibiotic Pretreatment on Cerebrospinal Fluid Profiles of Children with Acute Bacterial Meningitis Adhikari S, 1* Gauchan E, 1 BK G, 1 Rao KS 1 1 Department of Paediatrics, Manipal College of
