Closure of Myelomeningocele Defects Using a Limberg Flap or Direct Repair
|
|
|
- Percival Watson
- 5 years ago
- Views:
Transcription
1 Closure of Myelomeningocele Defects Using a Limberg Flap or Direct Repair Original Article Jung-Hwan Shim 1, Na-Hyun Hwang 1, Eul-Sik Yoon 1, Eun-Sang Dhong 1, Deok-Woo Kim 1, Sang-Dae Kim 2 Departments of 1 Plastic and Reconstructive Surgery and 2 Neurosurgery, Korea University College of Medicine, Seoul, Korea Background The global prevalence of myelomeningocele has been reported to be per 1,000 live births. Early closure of the defect is considered to be the standard of care. Various surgical methods have been reported, such as primary skin closure, local skin flaps, musculocutaneous flaps, and skin grafts. The aim of this study was to describe the clinical characteristics of myelomeningocele defects and present the surgical outcomes of recent cases of mye lomeningocele at our institution. Methods Patients who underwent surgical closure of myelomeningocele at our institution from January 2004 to December 2013 were included in this study. A retrospective chart review of their medical records was performed, and comorbidities, defect size, location, surgical procedures, complications, and the final results were analyzed. Results A total of 14 patients underwent surgical closure for myelomeningocele defects. Twelve cases were closed with direct skin repair, while two cases required local skin flaps to cover the skin defects. Three cases of infection occurred, requiring incision and either drainage or removal of allogenic materials. One case of partial flap necrosis occurred, requiring secondary revision using a rotational flap and a full-thickness skin graft. Despite these complications, all wounds eventually healed completely. Conclusions Most myelomeningocele defects can be managed by direct skin repair alone. In cases of large defects, in which direct repair is not possible, local flaps may be used to cover the defect. Complications such as wound dehiscence and partial flap necrosis occurred in this study; however, all such complications were successfully managed with simple ancillary procedures. Correspondence: Deok-Woo Kim Department of Plastic and Reconstructive Surgery, Korea University College of Medicine, 123 Jeokgeum-ro, Danwon-gu, Ansan 15355, Korea Tel: Fax: deokwookim@gmail.com This article was presented at the Fourth Research and Reconstructive Forum on April 3 4, 2014 in Busan, Korea. Keywords Myelomeningocele / Surgical flap / Wound closure techniques No potential conflict of interest relevant to this article was reported. Received: 16 Mar 2015 Revised: 25 Jun 2015 Accepted: 6 Jul 2015 pissn: eissn: Arch Plast Surg 2016;43:26-31 INTRODUCTION Myelomeningocele is a form of spina bifida. At four weeks of gestation, the lateral edge of the neural plates elevate toward each other and fuse to form a tube known as the neural tube. Failure of this process results in a neural tube defect [1]. When the failure involves a posterior closure, it is called spina bifida [2]. While the etiology of neural tube defects remains poorly understood, recent studies have shown that genetics, geography, low socioeconomic status, and folic acid deficiency are factors associated with neural tube defects [3]. The global prevalence of myelomeningocele has been reported to be per 1,000 Copyright 2016 The Korean Society of Plastic and Reconstructive Surgeons This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. 26
2 Vol. 43 / No. 1 / January 2016 live births [4,5]. Closure of a large myelomeningocele defect is challenging for the reconstructive surgeon. The goals of closure are to preserve the function of the neural tissue and to prevent secondary infection [6]. If the myelomeningocele defect is small, direct repair can be performed; however, if the defect is large, various other reconstructive options are available [7]. In general, direct repair of myelomeningocele defects is performed in approximately 75% of cases, with the remaining 25% representing large myelomeningocele defects that require other methods of reconstruction [8]. Several reconstructive options exist for soft tissue closure, including local flaps, musculocutaneous flap variations, and skin grafting [9]. In this study, we report our ten-year experience with the treatment of myelomeningocele defects. We used direct repair or a Limberg flap to close the myelomeningocele defects, depending on the size of the defect. METHODS From January 2004 to December 2013, 14 patients with myelomeningocele defects underwent repair at our institution. Of these patients, eight (57%) were male and six (43%) were female, with a mean age of 67.4 days. Twelve patients (86%) underwent direct repair, and two patients (14%) underwent a Limberg flap procedure to cover the myelomeningocele defect. One patient required only one Limberg flap (Fig. 1), whereas the other patient required two Limberg flaps to cover the myelomeningocele defect (Fig. 2). In all patients, repair of the neural tube and dura mater was performed by a neurosurgeon. In six patients, a small myelomeningocele skin defect was closed by the same neurosurgeon, and the other eight cases were repaired by a plastic surgeon. Patient demographics are summarized in Table 1. Retrospective chart review of medical records was performed and comorbidities, defect size, location, surgical procedures, complications, and the final results were analyzed. Surgical technique: the Limberg flap The Limberg flap is an example of a transposition flap. Although angles may vary, the Limberg flap is basically a parallelogram with two 120 angles and two 60 angles (Fig. 3). It is versatile in that a random pattern flap can be raised from any or all corners of the rhomboid. In the cases included in this study, the neurosurgeon covered the dural defect during standard dural repair. Artificial dural tissue (Neuro-Patch, B. Braun Melsungen AG, Melsungen, Germany) was used to cover the dural defect in two cases. The margin of the defect was then trimmed into a parallelogram to act as the Limberg flap. A vertical line equal to the length of one side of the rhomboidal defect was determined, followed by a second line parallel to one side of the rhombus. A skin incision was made to the muscle fascia first, and then the Limberg flap was dissected above the muscle fascia. After the dissection, the Limberg flap was transpositioned to the myelomeningocele defect. Surgical technique: direct repair Small myelomeningocele defects were covered by direct repair. Fig. 1. Single Limberg flap (A) One Limberg flap was planned to be placed in a patient with a myelomeningocele defect. (B) Image taken five months postoperatively. A B 27
3 Shim JH et al. Closure of myelomeningocele Fig. 2. Two Limberg flaps (A) Two Limberg flaps were planned to be placed in a patient with a myelomeningocele defect. (B) A magnetic resonance image showing kyphosis of the thoracic spine and myelomeningocele. Note that the defect is shaped like a hemisphere, with a bulging surface. (C) Appearance of the flap one month after surgery. The black arrows indicate skin necrosis and wound dehiscence. A rotational flap and a full-thickness skin graft were performed. (D) Appearance of the flap three months after surgery. A B C D Table 1. Patient demographics Patient no. Sex Age at operation Size of defects (cm 2 ) Procedure Complications Secondary procedures Final result 1 Male 10 mo 1 3 Direct repair 1. Infection 1. Incision and drainage Complete healing 2. Wound dehiscence 2. Local advancement flap 2 Female 3 day 2 2 Direct repair None None Complete healing 3 Male 3 day 11 1 Direct repair None None Complete healing 4 Male 55 day 5 1 Direct repair None None Complete healing 5 Male 19 day 3 1 Direct repair None None Complete healing 6 Male 31 day 8 2 Direct repair None None Complete healing 7 Male 3 day 4 2 Direct repair None None Complete healing 8 Female 1 day 5 1 Direct repair Infection Debridement and direct repair Complete healing 9 Female 2 day 8 8 Limberg flap 1. Infection 1. Debridement and artificial dura removal Complete healing 2. Dehiscence and infection 2. Debridement and direct repair 10 Male 2 day 9 2 Direct repair None None Complete healing 11 Female 12 day 10 1 Direct repair None None Complete healing 12 Female 14 mo 15 2 Direct repair None None Complete healing 13 Male 3 mo 15 1 Direct repair None None Complete healing 14 Female 2 day Limberg flaps Dehiscence and necrosis Rotational flap and FTSG Complete healing FTSG, full-thickness skin graft. After direct repair of the dural defect with non-absorbable sutures, an adjacent skin flap above the muscular layer was undermined to release tension, and the wound was closed directly. RESULTS A total of 14 patients underwent surgical closure of myelomeningocele defects. All patients except one had lumbosacral defects. One patient, in whom two Limberg flaps were used, developed a thoracic myelomeningocele defect. However, all defects were closed successfully. The mean follow-up period was 27 months (range, months). The mean defect size was 9.4 cm 2 in the direct repair cases and 64.0 cm 2 in the Limberg flap cases. The average operative time was minutes for direct repair and minutes for the Limberg flaps (Table 2). Both patients who underwent Limberg flap coverage developed hydrocephalus, and a ventriculoperitoneal shunt was required to decrease the pressure of the cerebrospinal fluid. Five of the 12 direct repair cases developed hydrocephalus, and two of these patients required a ventriculoperitoneal shunt. One 28
4 Vol. 43 / No. 1 / January 2016 Fig. 3. Schematic diagram of a Limberg flap The wound is basically rhomboid, with two 120 angles and two 60 angles. We made a vertical line equal to the length of one side of the rhomboidal defect. Subsequently, a second line was made parallel to one side of the rhombus. Table 3. Summary of complications Complication Group Direct repair (n= 12) Limberg flap (n=2) Infection 2 (16.7) 1 (50) Wound dehiscence 1 (8.3) 2 (100) Wound necrosis 0 1 (50) Values are presented as number (%). 60 Table 2. Summary of results Direct repair (n=12) 120 Group Limberg flap (n=2) Defect size (cm 2 ) 9.42± ±0 Operative time (min) 190.9± ±21.2 Complications, n (%) 2 (16.7) 2 (100) Limberg flap case and five direct repair cases underwent a twodimensional echocardiogram shortly after birth. All six patients were diagnosed with patent foramen ovale (PFO). However, further evaluation of the PFO was unnecessary, because the size of the foramen was insignificant. Two Limberg flap cases and five direct repair cases underwent abdominal ultrasonography, and none showed any abnormalities in the abdominal cavity. Complications developed after Limberg flap coverage in both patients (Table 3). One patient suffered from wound dehiscence with associated infection. The patient who underwent two Limberg flaps developed marginal flap necrosis and wound dehiscence at two different sites. Wound infection developed in two direct repair cases developed. Despite these complications, all wounds healed successfully after simple ancillary procedures. Both patients who underwent Limberg flap coverage developed paraplegia. Of the remaining 12 patients, one expired due to an underlying condition, three developed weakness of the lower extremities, and eight were able to walk independently. DISCUSSION Recently, fetal surgery for myelomeningocele repair has been introduced in some institutions and has been shown to result in improved neurological function and decreased morbidity [10]. However, fetal surgery is not preferred in many institutions due to the concerns of the parents or financial problems [7,11]. For these reasons, the postnatal closure of myelomeningocele is still considered the primary option for repairing myelomeningocele defects. In previous studies, approximately 75% of myelomeningocele defects were closed by direct repair, while the remaining 25% required other reconstructive options [8]. Musculocutaneous flaps are an option for the closure of extremely wide myelomeningocele defects [12]. In 1978, McCraw et al. [13] reported a bilateral latissimus dorsi musculocutaneous flap for the closure of myelomeningocele, and bilateral latissimus dorsi musculocutaneous flaps with extended gluteal fasciocutaneous flaps have also been used [14]. Limberg latissimus dorsi musculocutaneous flaps [15], distally based latissimus dorsi flaps [2], and reverse latissimus dorsi musculocutaneous flaps [16] have also been used to close myelomeningocele defects. For lower sacral defects, a combination of latissimus dorsi and gluteus maximus musculocutaneous flaps was described by Ramirez et al. [17]. More recently, in 2012, Patel et al. [18] described local turnover fascial flaps and midline linear skin closure for the treatment of myelomeningocele defects. The use of perforator flaps, including lumbar artery perforator flaps, superior gluteal artery perforator flaps, and dorsal intercostal artery perforator flaps, has also been previously described [19,20]. The use of local flaps for moderate to large lumbosacral myelomeningocele defects is considered a viable option. Many creative skin flaps have been described, such as bilobed flaps, double Z-rhomboid flaps, V-Y advancement flaps, rotation flaps, and Limberg flaps [5,21-23]. In 1979, Ohtsuka et al. [23] first described the use of the Limberg flap for closing myelomeningocele defects. Later, Cruz et al. [21] emphasized the utility of Limberg flaps for the closure of myelomeningocele. To our knowledge, this is the first report in Korea that provides support for 29
5 Shim JH et al. Closure of myelomeningocele Fig. 4. Schematic diagram of two Limberg flaps (A) The design of two Limberg flaps: one at the top and one at the bottom of the defect. (B) Two Limberg flaps were rotated to the center of the defect. Both ends of these flaps overlapped (gray shading) at the center of the defect, allowing three-dimensional resurfacing of the defect. A B the use of the Limberg flap in the closure of myelomeningocele defects. Since myelomeningocele is a disease with a very low incidence, it was difficult for us to compare different surgical techniques more thoroughly. However, this article may be used as a reference point for future studies. We chose the Limberg flap to cover lumbosacral myelomeningocele defects for several reasons. Some reports have suggested that it is advantageous to use a V-Y advancement flap, which leaves a vertical midline scar, for a secondary operation [18]. However, closure of the defect using a V-Y advancement flap did not seem possible in our patients due to a lack of sufficient skin on the lateral side. Additionally, the use of relaxing incisions is not feasible in cases of midline closure. In the Limberg flap, it is possible to use redundant skin from the scapular to upper thoracic area. Excess tension may arise due to insufficient circulation to the distal tip of the flap, but this problem resolves eventually, since the center of the defect is covered by the flap core, in which the circulation is stable. Marginal necrosis in the midline closure may pose a more serious problem. In our two cases requiring Limberg flaps, the defect was hemispherical, with a bulging surface area approximately 1.5 times larger than that of the corresponding plane surface, with mechanical pressure concentrated in the bulging surface (Fig. 2). This configuration may result in dehiscence of the midline closure. If two Limberg flaps are created, one at the top of the defect and one at the bottom of the defect, both ends of these flaps will overlap, allowing three-dimensional resurfacing at the center of the defect (Fig. 4). The Limberg flap has several additional advantages. In musculocutaneous or perforator flaps, the operating time is prolonged, thereby prolonging the anesthetic time, which may adversely affect the general condition of young patients. We found some perforators in our patients, but the size of the perforators was not reliable. The Limberg flap is also frequently performed to cover rectangular or round defects, because it has the advantage of preserving the back muscles, so that patients can maintain correct trunk posture as they grow up, and because the procedure can be performed with minimal blood loss [7]. Limberg flaps can fully cover large myelomeningocele defects (up to 8 8 cm 2 in our study). Theoretically, all sides of a rhomboid defect can be used as flaps, meaning that a total of four flaps can be elevated at once. Some complications occurred in our Limberg flaps. However, in one case, the complications were associated with an infection of the allogenic materials, not with the flap itself. One patient developed marginal necrosis, which was a flap-related complication; however, it was easily reversed, and complete healing was eventually achieved. In our opinion, simple closure should be the treatment of choice for small myelomeningocele defects. However, single or multiple rhomboid (Limberg) flaps can be applied very safely to treat larger defects (up to 64 cm 2 ). Extremely large defects may, however, require more complicated surgical procedures, involving musculocutaneous flaps. REFERENCES 1. Wallingford JB. Neural tube closure and neural tube defects: studies in animal models reveal known knowns and known unknowns. Am J Med Genet C Semin Med Genet 2005; 135C: Scheflan M, Mehrhof AI Jr, Ward JD. Meningomyelocele closure with distally based latissimus dorsi flap. Plast Reconstr Surg 1984;73: Botto LD, Moore CA, Khoury MJ, et al. Neural-tube defects. N Engl J Med 1999;341: Greenberg F, James LM, Oakley GP Jr. Estimates of birth prevalence rates of spina bifida in the United States from computer-generated maps. Am J Obstet Gynecol 1983;145: Lapid O, Rosenberg L, Cohen A. Meningomyelocele reconstruction with bilobed flaps. Br J Plast Surg 2001;54: El-khatib HA. Large thoracolumbar meningomyelocele de- 30
6 Vol. 43 / No. 1 / January 2016 fects: incidence and clinical experiences with different modalities of latissimus dorsi musculocutaneous flap. Br J Plast Surg 2004;57: Campobasso P, Pesce C, Costa L, et al. The use of the Limberg skin flap for closure of large lumbosacral myelomeningoceles. Pediatr Surg Int 2004;20: Patterson TJ. The use of rotation flaps following excision of lumbar myelo-meningoceles: an aid to the closure of large defects. Br J Surg 1959;46: Zide BM. Spina bifida. In: McCarthy JG, editor. Plastic surgery. Philadelphia: Saunders; p Adzick NS. Fetal surgery for spina bifida: past, present, future. Semin Pediatr Surg 2013;22: Muskett A, Barber WH, Parent AD, et al. Contemporary postnatal plastic surgical management of meningomyelocele. J Plast Reconstr Aesthet Surg 2012;65: Mustarde JC. Reconstruction of the spinal canal in severe spina bifida. Plast Reconstr Surg 1968;42: McCraw JB, Penix JO, Baker JW. Repair of major defects of the chest wall and spine with the latissimus dorsi myocutaneous flap. Plast Reconstr Surg 1978;62: McDevitt NB, Gillespie RP, Woosley RE, et al. Closure of thoracic and lumbar dysgraphic defects using bilateral latissimus dorsi myocutaneous flap transfer with extended gluteal fasciocutaneous flaps. Childs Brain 1982;9: Munro IR, Neu BR, Humphreys RP, et al. Limberg-latissimus dorsi myocutaneous flap for closure of myelomeningocele. Childs Brain 1983;10: VanderKolk CA, Adson MH, Stevenson TR. The reverse latissimus dorsi muscle flap for closure of meningomyelocele. Plast Reconstr Surg 1988;81: Ramirez OM, Ramasastry SS, Granick MS, et al. A new surgical approach to closure of large lumbosacral meningomyelocele defects. Plast Reconstr Surg 1987;80: Patel KB, Taghinia AH, Proctor MR, et al. Extradural myelomeningocele reconstruction using local turnover fascial flaps and midline linear skin closure. J Plast Reconstr Aesthet Surg 2012;65: El-Sabbagh AH, Zidan AS. Closure of large myelomeningocele by lumbar artery perforator flaps. J Reconstr Microsurg 2011;27: Duffy FJ Jr, Weprin BE, Swift DM. A new approach to closure of large lumbosacral myelomeningoceles: the superior gluteal artery perforator flap. Plast Reconstr Surg 2004;114: Cruz NI, Ariyan S, Duncan CC, et al. Repair of lumbosacral myelomeningoceles with double Z-rhomboid flaps. Technical note. J Neurosurg 1983;59: Habal MB, Vries JK. Tension free closure of large meningomyelocele defects. Surg Neurol 1977;8: Ohtsuka H, Shioya N, Yada K. Modified Limberg flap for lumbosacral meningomyelocele defects. Ann Plast Surg 1979; 3:
Using the sac membrane to close the flap donor site in large meningomyeloceles
 The British Association of Plastic Surgeons (2004) 57, 273 277 Using the sac membrane to close the flap donor site in large meningomyeloceles Cengiz Bozkurt a, Selçuk Akın a, *,Şeref Doğan b, Erkut Özdamar
The British Association of Plastic Surgeons (2004) 57, 273 277 Using the sac membrane to close the flap donor site in large meningomyeloceles Cengiz Bozkurt a, Selçuk Akın a, *,Şeref Doğan b, Erkut Özdamar
Large thoracolumbar meningomyelocele defects: incidence and clinical experiences with different modalities of latissimus dorsi musculocutaneus flap
 The British Association of Plastic Surgeons (2004) 57, 411 417 Large thoracolumbar meningomyelocele defects: incidence and clinical experiences with different modalities of latissimus dorsi musculocutaneus
The British Association of Plastic Surgeons (2004) 57, 411 417 Large thoracolumbar meningomyelocele defects: incidence and clinical experiences with different modalities of latissimus dorsi musculocutaneus
A decision-making guide for the closure of myelomeningocele skin defects with or without primary repair
 clinical article J Neurosurg Pediatr 18:187 191, 2016 A decision-making guide for the closure of myelomeningocele skin defects with or without primary repair Cemal Alper Kemaloğlu, MD, İrfan Özyazgan,
clinical article J Neurosurg Pediatr 18:187 191, 2016 A decision-making guide for the closure of myelomeningocele skin defects with or without primary repair Cemal Alper Kemaloğlu, MD, İrfan Özyazgan,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
The lumbar artery perforator based island flap: anatomical study and case reports
 British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Kuwabara, Kaoru; Nonaka, Takashi; H. Citation Journal of Clinical Urology, 7(5),
 NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
NAOSITE: Nagasaki University's Ac Title Author(s) Gluteal-fold adipofascial perforato fistula reconstruction Fujioka, Masaki; Hayashida, Kenji; Kuwabara, Kaoru; Nonaka, Takashi; H Citation Journal of Clinical
Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair
 Original Article Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair Yoon Seok Lee 1, Dong Hyeok Shin 1, Hyun Gon Choi 1, Jee Nam Kim 1, Myung Chul
Original Article Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair Yoon Seok Lee 1, Dong Hyeok Shin 1, Hyun Gon Choi 1, Jee Nam Kim 1, Myung Chul
A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers
 A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers Masaki Fujioka, MD, PhD; Kenji Hayashida, MD; Sin Morooka, MD; and Hiroto Saijo,
A Retrospective Comparison of Perforator and Rotation Flaps for the Closure of Extensive Stage IV Sacral Pressure Ulcers Masaki Fujioka, MD, PhD; Kenji Hayashida, MD; Sin Morooka, MD; and Hiroto Saijo,
Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear
 The British Association of Plastic Surgeons (2004) 57, 238 244 Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear Yong Oock Kim*, Beyoung Yun Park, Won Jae Lee Institute
The British Association of Plastic Surgeons (2004) 57, 238 244 Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear Yong Oock Kim*, Beyoung Yun Park, Won Jae Lee Institute
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
Plastic Surgery: An International Journal
 Plastic Surgery: An International Journal Vol. 2013 (2013), Article ID 874416, 29 minipages. DOI:10.5171/2013.874416 www.ibimapublishing.com Copyright 2013 Akira Saito, Noriko Saito, Emi Funayama and Hidehiko
Plastic Surgery: An International Journal Vol. 2013 (2013), Article ID 874416, 29 minipages. DOI:10.5171/2013.874416 www.ibimapublishing.com Copyright 2013 Akira Saito, Noriko Saito, Emi Funayama and Hidehiko
Formation of reconstruction protocol for sacral pressure sore defects
 International Journal of Medical and Health Research ISSN: 2454-9142 Impact Factor: RJIF 5.54 www.medicalsciencejournal.com Volume 4; Issue 8; August 2018; Page No. 18-24 Formation of reconstruction protocol
International Journal of Medical and Health Research ISSN: 2454-9142 Impact Factor: RJIF 5.54 www.medicalsciencejournal.com Volume 4; Issue 8; August 2018; Page No. 18-24 Formation of reconstruction protocol
Repair of Wide Myelomeningocele Defects with the Bilateral Fasciocutaneous Flap Method
 Repair of Wide Myelomeningocele Defects with the asciocutaneous lap Method Genifl Myelomeningosel Defektlerinin asiokutan lep Yöntemi ile Kapat lmas ABSTRACT OBJECTIVE: ive large defects repaired by bilateral
Repair of Wide Myelomeningocele Defects with the asciocutaneous lap Method Genifl Myelomeningosel Defektlerinin asiokutan lep Yöntemi ile Kapat lmas ABSTRACT OBJECTIVE: ive large defects repaired by bilateral
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2
 RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
Impact of Disturbed Wound Healing after Surgery on the Prognosis of Marjolin s Ulcer
 Impact of Disturbed Wound Healing after Surgery on the Prognosis of Marjolin s Ulcer Jae Yeon Choi, Yong Chan Bae, Su Bong Nam, Seong Hwan Bae Department of Plastic and Reconstructive Surgery, Pusan National
Impact of Disturbed Wound Healing after Surgery on the Prognosis of Marjolin s Ulcer Jae Yeon Choi, Yong Chan Bae, Su Bong Nam, Seong Hwan Bae Department of Plastic and Reconstructive Surgery, Pusan National
Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
INTRODUCTION. Jong Gyu Kim, Soo Hyang Lee. Original Article
 Comparison of the Multidetector-row Computed Tomographic ngiography xial and Coronal Planes Usefulness for Detecting Thoracodorsal rtery Perforators Original rticle Jong Gyu Kim, Soo Hyang Lee Department
Comparison of the Multidetector-row Computed Tomographic ngiography xial and Coronal Planes Usefulness for Detecting Thoracodorsal rtery Perforators Original rticle Jong Gyu Kim, Soo Hyang Lee Department
Evaluation of the donor site after the median forehead flap
 Evaluation of the donor site after the median forehead flap June Seok Choi 1, Yong Chan Bae 1,2, Soo Bong Nam 1, Seong Hwan Bae 1, Geon Woo Kim 1 1 Department of Plastic and Reconstructive Surgery, Pusan
Evaluation of the donor site after the median forehead flap June Seok Choi 1, Yong Chan Bae 1,2, Soo Bong Nam 1, Seong Hwan Bae 1, Geon Woo Kim 1 1 Department of Plastic and Reconstructive Surgery, Pusan
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
A new classification system of nasal contractures
 Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Case Report The Reverse Latissimus Dorsi Flap for Large Lower Lumbar Defect
 Case Reports in Surgery Volume 2012, Article ID 964625, 5 pages doi:10.1155/2012/964625 Case Report The Reverse Latissimus Dorsi Flap for Large Lower Lumbar Defect Bouraoui Kotti, Olfa Jaidane, Jamel Ben
Case Reports in Surgery Volume 2012, Article ID 964625, 5 pages doi:10.1155/2012/964625 Case Report The Reverse Latissimus Dorsi Flap for Large Lower Lumbar Defect Bouraoui Kotti, Olfa Jaidane, Jamel Ben
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Clinical teaching/experi ence. Lectures/semina rs/conferences Self-directed. learning. Clinical teaching/experi ence
 Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Progressive Tension Sutures to Prevent Seroma Formation after Latissimus Dorsi Harvest
 Progressive Tension Sutures to Prevent Seroma Formation after Latissimus Dorsi Harvest Jose L. Rios, M.D., Todd Pollock, M.D., and William P. Adams, Jr., M.D. Dallas, Texas The latissimus dorsi muscle
Progressive Tension Sutures to Prevent Seroma Formation after Latissimus Dorsi Harvest Jose L. Rios, M.D., Todd Pollock, M.D., and William P. Adams, Jr., M.D. Dallas, Texas The latissimus dorsi muscle
Sliding Perforator Island Flap For Covering A Big Lumbosacral Defect
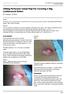 ISPUB.COM The Internet Journal of Plastic Surgery Volume 5 Number 2 Sliding Perforator Island Flap For Covering A Big Lumbosacral Defect R Hussein, S Anis Citation R Hussein, S Anis.. The Internet Journal
ISPUB.COM The Internet Journal of Plastic Surgery Volume 5 Number 2 Sliding Perforator Island Flap For Covering A Big Lumbosacral Defect R Hussein, S Anis Citation R Hussein, S Anis.. The Internet Journal
Guidelines in the management of neural tube defects and hydrocephalus
 Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
The gluteal perforator-based flap in repair of pressure sores
 The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
Effects of Bariatric Surgery on Facial Features
 Effects of Bariatric Surgery on Facial Features Vardan Papoian, Vartan Mardirossian 2, Donald Thomas Hess 2, Jeffrey H Spiegel 2 MedStar Washington Hospital Center, Washington, DC; 2 Department of Surgery,
Effects of Bariatric Surgery on Facial Features Vardan Papoian, Vartan Mardirossian 2, Donald Thomas Hess 2, Jeffrey H Spiegel 2 MedStar Washington Hospital Center, Washington, DC; 2 Department of Surgery,
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
Inferior Gluteus Maximus Island Flap for Reconstruction of Ischial Pressure Sores
 Original Article Inferior Gluteus Maximus Island Flap for Reconstruction of Ischial Pressure Sores Yawar Sajjad, 1 Beenish Rahat, 2 Salman Hameed 3 Abstract Surgical management of ischial pressure sores
Original Article Inferior Gluteus Maximus Island Flap for Reconstruction of Ischial Pressure Sores Yawar Sajjad, 1 Beenish Rahat, 2 Salman Hameed 3 Abstract Surgical management of ischial pressure sores
Interesting Case Series. Reconstruction of Dorsal Wrist Defects
 Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
Interesting Case Series. Fournier s Gangrene and the Reconstructive Challenges for the Plastic Surgeon
 Interesting Case Series Fournier s Gangrene and the Reconstructive Challenges for the Plastic Surgeon David Izadi, MB, BChir, MA(Oxon), MA(Cantab), MRCS, James Coelho, BMBS, MSc, MRCS, Sameer Gurjal, MBBCh,
Interesting Case Series Fournier s Gangrene and the Reconstructive Challenges for the Plastic Surgeon David Izadi, MB, BChir, MA(Oxon), MA(Cantab), MRCS, James Coelho, BMBS, MSc, MRCS, Sameer Gurjal, MBBCh,
The usefulness of pedicled perforator flap in partial breast reconstruction after breast conserving surgery in Korean women
 The usefulness of pedicled perforator flap in partial breast reconstruction after breast conserving surgery in Korean women Jae Bong Kim 1, Dong Kyu Kim 1, Jeong Woo Lee 1, Kang Young Choi 1, Ho Yun Chung
The usefulness of pedicled perforator flap in partial breast reconstruction after breast conserving surgery in Korean women Jae Bong Kim 1, Dong Kyu Kim 1, Jeong Woo Lee 1, Kang Young Choi 1, Ho Yun Chung
Reconstruction of the Chest Wall
 HOW TO DO IT Reconstruction of the Chest Wall Reed 0. Dingman, M.D., and Louis C. Argenta, M.D. ABSTRACT Reconstruction of the chest wall can now be accomplished reliably and expeditiously. Past experience
HOW TO DO IT Reconstruction of the Chest Wall Reed 0. Dingman, M.D., and Louis C. Argenta, M.D. ABSTRACT Reconstruction of the chest wall can now be accomplished reliably and expeditiously. Past experience
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function
 Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
J. Bryce Olenczak, MD, Matthew G. Stanwix, MD, and Gedge D. Rosson, MD
 CASE REPORT Complex Wound Closure of Partial Sacrectomy Defect With Human Acellular Dermal Matrix and Bilateral V to Y Gluteal Advancement Flaps in a Pediatric Patient J. Bryce Olenczak, MD, Matthew G.
CASE REPORT Complex Wound Closure of Partial Sacrectomy Defect With Human Acellular Dermal Matrix and Bilateral V to Y Gluteal Advancement Flaps in a Pediatric Patient J. Bryce Olenczak, MD, Matthew G.
Onlay Rib Bone Graft in Elevation of Reconstructed Auricle: 17 Years of Experience
 Onlay Rib one Graft in Elevation of Reconstructed uricle: 17 Years of Experience Taehoon Kim, Jihyeon Han, Yoonho Lee Department of Plastic and Reconstructive Surgery, Seoul National University College
Onlay Rib one Graft in Elevation of Reconstructed uricle: 17 Years of Experience Taehoon Kim, Jihyeon Han, Yoonho Lee Department of Plastic and Reconstructive Surgery, Seoul National University College
Usefulness of the orbicularis oculi myocutaneous flap in periorbital reconstruction
 Archives of Craniofacial Surgery Arch Craniofac Surg Vol.19 No.4, 254-259 Usefulness of the orbicularis oculi myocutaneous flap in periorbital reconstruction Original Article Geon Woo Kim 1, Yong Chan
Archives of Craniofacial Surgery Arch Craniofac Surg Vol.19 No.4, 254-259 Usefulness of the orbicularis oculi myocutaneous flap in periorbital reconstruction Original Article Geon Woo Kim 1, Yong Chan
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report
 Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
The distally-based island ulnar artery perforator flap for wrist defects
 Free full text on www.ijps.org Original Article The distally-based island ulnar artery perforator flap for wrist defects Durga Karki, A. K. Singh Post Graduate Department of Plastic and Reconstructive
Free full text on www.ijps.org Original Article The distally-based island ulnar artery perforator flap for wrist defects Durga Karki, A. K. Singh Post Graduate Department of Plastic and Reconstructive
Application of Local Axial Flaps to Scalp Reconstruction Original Article Yolanda Zayakova 1, Anton Stanev 1, Hristo Mihailov 2, Nicolai Pashaliev 1
 Application of Local Axial Flaps to Scalp Reconstruction Original Article Yolanda Zayakova 1, Anton Stanev 1, Hristo Mihailov 2, Nicolai Pashaliev 1 Departments of 1 Burns, Plastic and Aesthetic Surgery
Application of Local Axial Flaps to Scalp Reconstruction Original Article Yolanda Zayakova 1, Anton Stanev 1, Hristo Mihailov 2, Nicolai Pashaliev 1 Departments of 1 Burns, Plastic and Aesthetic Surgery
Original Article Modified O-T advancement flap for reconstruction of skin defects
 Int J Clin Exp Pathol 2017;10(9):9158-9163 www.ijcep.com /ISSN:1936-2625/IJCEP0057308 Original Article Modified O-T advancement flap for reconstruction of skin defects Zhuo-Ran Li 1, Yong Jiang 1, Jun-Yan
Int J Clin Exp Pathol 2017;10(9):9158-9163 www.ijcep.com /ISSN:1936-2625/IJCEP0057308 Original Article Modified O-T advancement flap for reconstruction of skin defects Zhuo-Ran Li 1, Yong Jiang 1, Jun-Yan
Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects
 Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects Osman Akdag, MD, a Mehtap Karamese, MD, a Muhammed NebilSelimoglu, MD, a Ahmet Akatekin, MD, a Malik Abacı,
Reverse Adipofascial Radial Forearm Flap Surgery for Soft-Tissue Reconstruction of Hand Defects Osman Akdag, MD, a Mehtap Karamese, MD, a Muhammed NebilSelimoglu, MD, a Ahmet Akatekin, MD, a Malik Abacı,
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
-primarily by apposition of the anterior rectus
 2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
Closure of Chronic Heel Ulcer by Simple V-Y Flap
 Egypt, J. Plast. Reconstr. Surg., Vol. 40, No. 1, January: 97-101, 2016 Closure of Chronic Heel Ulcer by Simple V-Y lap ESA TAAN,.D.; AYAN ARHAT,.D.; OUSTAA EKY,.D. and AHOUD NASI,.D. The Department of
Egypt, J. Plast. Reconstr. Surg., Vol. 40, No. 1, January: 97-101, 2016 Closure of Chronic Heel Ulcer by Simple V-Y lap ESA TAAN,.D.; AYAN ARHAT,.D.; OUSTAA EKY,.D. and AHOUD NASI,.D. The Department of
Large full-thickness nasal tip defects after Mohs
 RECONSTRUCTIVE CONUNDRUM Repair of a Large, Exposed-Cartilage Nasal Tip Defect Using Nasalis-Based Subcutaneous Pedicle Flaps and Full-Thickness Skin Grafting DIEGO E. MARRA, MD, EDGAR F. FINCHER, MD,
RECONSTRUCTIVE CONUNDRUM Repair of a Large, Exposed-Cartilage Nasal Tip Defect Using Nasalis-Based Subcutaneous Pedicle Flaps and Full-Thickness Skin Grafting DIEGO E. MARRA, MD, EDGAR F. FINCHER, MD,
Assessment of Breast Volume Change after Transverse Rectus Abdominis Myocutaneous Flap
 Assessment of Breast Volume Change after Transverse Rectus Abdominis Myocutaneous Flap Sang Uk Park, Jeong Su Shim Department of Plastic and Reconstructive Surgery, Catholic University of Daegu School
Assessment of Breast Volume Change after Transverse Rectus Abdominis Myocutaneous Flap Sang Uk Park, Jeong Su Shim Department of Plastic and Reconstructive Surgery, Catholic University of Daegu School
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications
 Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Distally Based Sural Artery Adipofascial Flap based on a Single Sural Nerve Branch: Anatomy and Clinical Applications Wan Loong James Mok 1, Yong Chen Por 1, Bien Keem Tan 2 1 Department of Plastic, Reconstructive
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
TRANSPOSITIONAL ADIPOFASCIAL FLAPS FOR COMPLICATED ACUTE FINGER INJURIES
 K.B. Poon, S.H. Chien, G.T. Lin, et al TRANSPSITINAL ADIPFASCIAL FLAPS FR CMPLICATED ACUTE FINGER INJURIES Kein Boon Poon, Song-Hsiung Chien, 1 Gau-Tyan Lin, 1 and Yin-Chih Fu 1 Department of rthopaedic
K.B. Poon, S.H. Chien, G.T. Lin, et al TRANSPSITINAL ADIPFASCIAL FLAPS FR CMPLICATED ACUTE FINGER INJURIES Kein Boon Poon, Song-Hsiung Chien, 1 Gau-Tyan Lin, 1 and Yin-Chih Fu 1 Department of rthopaedic
Delayed Perforation Occurring after Endoscopic Submucosal Dissection for Early Gastric Cancer
 CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients
 JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
JFS (P) Kuldeep Singh et al ORIGINL RTICLE 10.5005/jp-journals-10040-1083 Heel Defect Reconstruction using Local Vascularized Flaps: Results and Clinical Outcomes in 16 Patients 1 Kuldeep Singh, 2 Zile
The Role of Negative-Pressure Wound Therapy in Latissimus Dorsi Flap Donor Site Seroma Prevention: A Cohort Study
 Original Article The Role of Negative-Pressure Wound Therapy in Latissimus Dorsi Flap Donor Site Seroma Prevention: A Cohort Study Apichai Angspatt, Thana Laopiyasakul, Pornthep Pungrasmi, Poonpissamai
Original Article The Role of Negative-Pressure Wound Therapy in Latissimus Dorsi Flap Donor Site Seroma Prevention: A Cohort Study Apichai Angspatt, Thana Laopiyasakul, Pornthep Pungrasmi, Poonpissamai
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
PECTORALIS MAJOR MYOCUTAJNEUUS FLAP FOR RECONSTRUCTION OF DEFECTS FOLLOWING RESECTIONS IN HEAD AND NECK AREA
 PECTORALIS MAJOR MYOCUTAJNEUUS FLAP FOR RECONSTRUCTION OF DEFECTS FOLLOWING RESECTIONS IN HEAD AND NECK AREA Pages with reference to book, From 72 To 76 Mohammad Arshad Cheema ( Department of Surgery,
PECTORALIS MAJOR MYOCUTAJNEUUS FLAP FOR RECONSTRUCTION OF DEFECTS FOLLOWING RESECTIONS IN HEAD AND NECK AREA Pages with reference to book, From 72 To 76 Mohammad Arshad Cheema ( Department of Surgery,
T. Rapis, S.N. Zanakis, I.F. Letsa, A.P. Karamanos CLINICAL CASE. Summary. Introduction
 Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts
 Breast Surgery Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts Scott L. Spear, MD; Samir S. Rao, MD; Ketan M. Patel, MD; and Maurice Y. Nahabedian, MD The combination of lumpectomy
Breast Surgery Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts Scott L. Spear, MD; Samir S. Rao, MD; Ketan M. Patel, MD; and Maurice Y. Nahabedian, MD The combination of lumpectomy
Partial Breast Reconstruction Using Various Oncoplastic Techniques for Centrally Located Breast Cancer
 Partial Breast Reconstruction Using Various Oncoplastic Techniques for Centrally Located Breast Cancer Original Article Hyo Chun Park 1, Hong Yeul Kim 1, Min Chul Kim 2, Jeong Woo Lee 2, Ho Yun Chung 2,
Partial Breast Reconstruction Using Various Oncoplastic Techniques for Centrally Located Breast Cancer Original Article Hyo Chun Park 1, Hong Yeul Kim 1, Min Chul Kim 2, Jeong Woo Lee 2, Ho Yun Chung 2,
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure sores
 ritish Journal of Plastic Surgery (1999), 52, 385 391 1999 The ritish ssociation of Plastic Surgeons The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure
ritish Journal of Plastic Surgery (1999), 52, 385 391 1999 The ritish ssociation of Plastic Surgeons The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure
4/30/2010. Options for abdominal wall reconstruction. Scott L. Hansen, MD
 Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
The limberg flap reconstruction - the optimal surgery for pilonidal sinus disease
 Original Article The limberg flap reconstruction - the optimal surgery for pilonidal sinus disease Ramu Shapur Srihari, Appaji Mandya Naveen, Harinatha Sreekar Department of General Surgery, Consultant,
Original Article The limberg flap reconstruction - the optimal surgery for pilonidal sinus disease Ramu Shapur Srihari, Appaji Mandya Naveen, Harinatha Sreekar Department of General Surgery, Consultant,
JMSCR Vol 05 Issue 09 Page September 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.93 Research Article Versatality of Limberg
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.93 Research Article Versatality of Limberg
Prognostic Factors of Orbital Fractures with Muscle Incarceration
 Prognostic Factors of Orbital Fractures with Muscle Incarceration Seung Chan Lee, Seung-Ha Park, Seung-Kyu Han, Eul-Sik Yoon, Eun-Sang Dhong, Sung-Ho Jung, Hi-Jin You, Deok-Woo Kim Department of Plastic
Prognostic Factors of Orbital Fractures with Muscle Incarceration Seung Chan Lee, Seung-Ha Park, Seung-Kyu Han, Eul-Sik Yoon, Eun-Sang Dhong, Sung-Ho Jung, Hi-Jin You, Deok-Woo Kim Department of Plastic
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
J Wound Management Res 2018 September;14(2):
 J Wound Management Res 2018 September;14(2):132-136 pissn 2586-0402 eissn 2586-0410 Journal of Wound Management and Research Functional and Aesthetic Reconstruction of Shoulder Using Pedicled LD Flap after
J Wound Management Res 2018 September;14(2):132-136 pissn 2586-0402 eissn 2586-0410 Journal of Wound Management and Research Functional and Aesthetic Reconstruction of Shoulder Using Pedicled LD Flap after
SCOPE OF PRACTICE PGY-6 PGY-7 PGY-8
 PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Other ways to use tissue expanded flaps
 The British Association of Plastic Surgeons (2004) 57, 336 341 CASE REPORTS Other ways to use tissue expanded flaps Donald A. Hudson* Department of Plastic and Reconstructive Surgery, University of Cape
The British Association of Plastic Surgeons (2004) 57, 336 341 CASE REPORTS Other ways to use tissue expanded flaps Donald A. Hudson* Department of Plastic and Reconstructive Surgery, University of Cape
Abdominal Wall Modification for the Difficult Ostomy
 Abdominal Wall Modification for the Difficult Ostomy David E. Beck, M.D. 1 ABSTRACT A select group of patients with major stomal problems may benefit from operative modification of the abdominal wall.
Abdominal Wall Modification for the Difficult Ostomy David E. Beck, M.D. 1 ABSTRACT A select group of patients with major stomal problems may benefit from operative modification of the abdominal wall.
Feasibility and Aesthetic Results of Small Bilateral V-Y Advancement Flaps in the Extremities and Back
 ORIGINAL ARTICLE https://doi.org/10.14730/.2017.23.3.127 Arch Aesthetic Plast Surg 2017;23(3):127-134 pissn: 2234-0831 eissn: 2288-9337 Archives of Feasibility and Aesthetic Results of Small Bilateral
ORIGINAL ARTICLE https://doi.org/10.14730/.2017.23.3.127 Arch Aesthetic Plast Surg 2017;23(3):127-134 pissn: 2234-0831 eissn: 2288-9337 Archives of Feasibility and Aesthetic Results of Small Bilateral
ASJ. A Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia. Asian Spine Journal. Introduction
 sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
Correction of Long Standing Proximal Interphalangeal Flexion Contractures with Cross Finger Flaps and Vigorous Postoperative Exercises
 Original Article DOI 10.3349/ymj.2010.51.4.574 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(4):574-578, 2010 Correction of Long Standing Proximal Interphalangeal Flexion Contractures with Cross Finger
Original Article DOI 10.3349/ymj.2010.51.4.574 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(4):574-578, 2010 Correction of Long Standing Proximal Interphalangeal Flexion Contractures with Cross Finger
1 62, M Biopsy Paget s disease 8/5/92 Perianal skin, None, NED anal canal,
 British Journal of Plastic Surgery (1999), 52, 471 475 1999 The British Association of Plastic Surgeons Reconstruction of perianal skin defect using a V Y advancement of bilateral gluteus maximus musculocutaneous
British Journal of Plastic Surgery (1999), 52, 471 475 1999 The British Association of Plastic Surgeons Reconstruction of perianal skin defect using a V Y advancement of bilateral gluteus maximus musculocutaneous
Anatomical relationship between arteries and veins in the paraumbilical region q
 The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
THE USE OF DEEPITHELIALIZATION
 THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
THE USE OF DEEPITHELIALIZATION IN URETHROPLASTY - Deepithelialization Stratum corneum - Epidermis Papillary dermis Reticular dermis Skin Healing in any reconstructive surgery depends on not only the intact
Risk Factors for Hinge Fracture Associated with Surgery Following Cervical Open-Door Laminoplasty
 CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
Interesting Case Series. Creating Accurate Flap Designs Using a Hydrocolloid Dressing as a Template
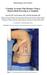 Interesting Case Series Creating Accurate Flap Designs Using a Hydrocolloid Dressing as a Template Amra Kuc, BS a, Jared Gopman, MD b, and Deniz Dayicioglu, MD c a Morsani College of Medicine, University
Interesting Case Series Creating Accurate Flap Designs Using a Hydrocolloid Dressing as a Template Amra Kuc, BS a, Jared Gopman, MD b, and Deniz Dayicioglu, MD c a Morsani College of Medicine, University
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
The Reverse Galeal Hinge Flap: Another Valuable Technique in the Repair of Scalp
 TITLE PAGE TITLE: The Reverse Galeal Hinge Flap: Another Valuable Technique in the Repair of Scalp Defects Extending to the Calvarium AUTHORS: Lam, Thomas, BA; Indiana University School of Medicine Miletta,
TITLE PAGE TITLE: The Reverse Galeal Hinge Flap: Another Valuable Technique in the Repair of Scalp Defects Extending to the Calvarium AUTHORS: Lam, Thomas, BA; Indiana University School of Medicine Miletta,
Interesting Case Series. Omental Flap for Thoracic Aortic Graft Infection
 Interesting Case Series Omental Flap for Thoracic Aortic Graft Infection Andrew A. Marano, BA, Adam M. Feintisch, MD, and Mark S. Granick, MD Division of Plastic Surgery, Department of Surgery, Rutgers
Interesting Case Series Omental Flap for Thoracic Aortic Graft Infection Andrew A. Marano, BA, Adam M. Feintisch, MD, and Mark S. Granick, MD Division of Plastic Surgery, Department of Surgery, Rutgers
Traumatic Hemi Facial Soft Tissue Amputation. Immediate Surgical Flap Reconstruction
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 3 Number 1 Traumatic Hemi Facial Soft Tissue Amputation. Immediate Surgical Flap Reconstruction J Mohammad Citation J Mohammad. Traumatic Hemi Facial
ISPUB.COM The Internet Journal of Plastic Surgery Volume 3 Number 1 Traumatic Hemi Facial Soft Tissue Amputation. Immediate Surgical Flap Reconstruction J Mohammad Citation J Mohammad. Traumatic Hemi Facial
Sure closure skin stretching system, our clinical experience
 Free full text on www.ijps.org Original Article Sure closure skin stretching system, our clinical experience K. I. Subramania, S. Mohit, P. R. Sasidharan, M. K. Abraham, P. Arun, V. Kekatpure Department
Free full text on www.ijps.org Original Article Sure closure skin stretching system, our clinical experience K. I. Subramania, S. Mohit, P. R. Sasidharan, M. K. Abraham, P. Arun, V. Kekatpure Department
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Reconstruction of large oroantral defects using a pedicled buccal fat pad
 Yang et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:7 https://doi.org/10.1186/s40902-018-0144-6 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Reconstruction
Yang et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:7 https://doi.org/10.1186/s40902-018-0144-6 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Reconstruction
The Practical Use of LIGASANO white in Plastic Surgery
 Practical experience 3 The Practical Use of LIGASANO white in Plastic Surgery Emergency Hospital of Mureş County, Romania Reports of practical experience from the burn center and plastic surgery department
Practical experience 3 The Practical Use of LIGASANO white in Plastic Surgery Emergency Hospital of Mureş County, Romania Reports of practical experience from the burn center and plastic surgery department
An alternative approach for correction of constricted ears of moderate severity
 British Journal of Plastic Surgery (2005) 58, 389 393 An alternative approach for correction of constricted ears of moderate severity M.M. Al-Qattan* Division of Plastic Surgery, King Saud University,
British Journal of Plastic Surgery (2005) 58, 389 393 An alternative approach for correction of constricted ears of moderate severity M.M. Al-Qattan* Division of Plastic Surgery, King Saud University,
