Tuberculosis Prophylaxis and Biologics Treatment for Rheumatoid Arthritis
|
|
|
- Hugo Hunt
- 5 years ago
- Views:
Transcription
1 NORTHERN (HIGH)LIGHTS Tuberculosis Prophylaxis and Biologics Treatment for Rheumatoid Arthritis By Nicholas M. Baniak, BSc; Vernon M. Hoeppner, MD, FRCPC; and Wojciech P. Olszynski, MD, PhD, FRCPC, CCD Tuberculosis (TB) infection is a prevalent, mostly latent, disease. Being treated with anti-tumor necrosis factor (TNF) inhibitors, a form of biologic therapy used for the treatment of rheumatoid arthritis (RA), is believed to increase the risk of reactivation. Accordingly, RA patients are recommended to go through screening for latent TB prior to initiating biologic therapy. If RA patients are found to have latent TB, it is recommended they initiate TB prophylaxis prior to beginning TNF inhibitor therapy. In the present study, a group of patients positive for latent TB were not provided prophylaxis before commencing TNF inhibitor therapy and were subsequently closely monitored for the development of overt TB symptoms. Of the 213 patients examined, 52% were male and 48% female, with 71% being over the age of 50. Furthermore, 95% of patients had been receiving treatment for longer than one year, with the longest being treated for 10 years. None of the patients showed evidence of active TB while on biologic therapy. Introduction A third of the world s population is infected with TB, 1,2 including 4% of the United States population. 3 In Canada, certain ethnicities possess higher levels of latent TB infection, such as foreign-born and First-Nations populations. There is an increased risk of TB associated with the use of TNF inhibitors, therapies commonly used for the management of autoimmune disorders, such as RA. 3 In a study of over 112,000 Canadian patients with RA, the rate of TB in patients not treated with TNF inhibitors was 2.2/1,000 patients, compared to 2.6/1,000 patients in those treated with TNF inhibitor therapy. 4,5 Mycobacteria are facultative intracellular pathogens. 1,6 When inhaled, TB bacilli are taken in by alveolar macrophages and encapsulating granulomas are subsequently developed in an attempt to limit the spread of the infectious bacteria. 1,6 Since the patient is not able to completely eliminate the pathogens, the resulting granulomas are the characteristic feature of latent pulmonary TB (LTBI). 7 Most immune-competent hosts have a sufficiently strong immune response to TB bacteria, limiting these pathogens to the lungs and associated lymph nodes. 7,8 The histiocytic transformation and formation of granulomas represents residual infection. 6 Disease reactivation occurs when latent bacteria from pre-existing granulomas are reactivated into an active, virulent state; reactivation is most common when the host immune response weakens or is suppressed. 7 Suppression of immune response is a well-known side effect of TNF inhibitor therapy. The interaction between activated macrophages and interferon-gamma (IFN-y)-secreting lymphocytes is vital to controlling the infection. TNFα, which is released by activated immune cells, also plays an important role in both granuloma formation and maintenance through its effects on expression of adhesion molecules and chemokines Therefore, TNF inhibitor treatment may cause the granuloma to fail, allowing TB release and reactivation. 11 In a TNFdeficient mouse model, rapid TB infection and subsequent death is observed. 7,15 TB screening is recommended for the identification of latent TB infection in patients considering initiating TNF inhibitor therapy for RA, 16 as surveys have shown that the incidence of TB is increased following the initiation of TNF inhibitor therapy. 11 Therefore, it is imperative that LTBI is identified and treated prior to initiating TNF inhibitor therapy to minimize the risk of reactivation. 17 The 2012 American College of Rheumatology (ACR) treatment recommendations for those with latent TB 6
2 (positive TST [tuberculin skin test] and negative chest X-ray [CXR]) are to take prophylactic medication before initiating any biologic medicine, such as a TNF inhibitor. 14 The treatment for LTBI is isoniazid (INH) 5 mg/kg (up to 300 mg) once daily or 15 mg/kg (up to 900 mg) twice weekly 18 for nine months. 1,19-21 However, as with any medication, the risk of side effects when taking the TB prophylaxis, especially hepatotoxicity, must be weighed against the benefit of preventing reactivation of TB In Saskatoon, Canada, RA patients with a positive TB skin test, but no other overt signs of TB, are initiated on TNF inhibitor therapy (after failing disease modifying antirheumatic drugs [DMARDs]) without prophylaxis and are monitored closely at the Saskatoon TB clinic. Patients with positive TSTs were compared to patients on TNF inhibitors with a negative TST to see if reactivation rates of TB differed between the two groups. The literature has shown no consistent pattern of serious TB infection risk associated with the use of TNF inhibitors. 25 In this study, it was hypothesized that the patients who were TST positive were not at any increased risk of TB reactivation by taking TNF inhibitors. The objective of this study was to determine if patients who test positive for TB have a significantly different risk of reactivation when not provided prophylaxis as compared to those who are prophylactically treated. Materials and Methods The cohort for this investigation consisted of all patients receiving biologic therapy at the office of a private urban rheumatology clinic and from the Royal University Hospital (RUH) in Saskatoon, Canada. Patient medical charts (n = 213) were reviewed from for the following variables: age, gender, type of biologic therapy, types of DMARDs (particularly prednisone), and signs of active TB. Patients were divided into two groups: those with either a positive TST (> 5 mm) or those with a negative TST ( 5 mm). Of the patients with a positive TST, 26 had RA, eight had ankylosing spondylitis (AS), and five had psoriatic arthritis (PsA). Of the patients with a negative TST, 127 had RA, 29 had AS, 16 had PsA, and two had inflammatory bowel disease (IBD) arthropathy. Total time that patients were receiving biologics was measured in months and patient years due to the unequal time in follow up in the different patients. There was no minimum amount of time that a patient had to be receiving biologics to be included, with the minimum time being three weeks for one patient. However, only two patients were receiving biologics for less than one year. No patient received TB prophylaxis. Results No evidence of TB reactivation occurred in either patient group. All of the patients included in this survey had moderate to severe RA as evidenced by having symptoms despite multiple types of DMARD treatments, and had thus been administered TNF inhibitor therapy. There were 39 patients with a positive TST currently receiving a TNF inhibitor and 174 patients with a negative TST receiving a TNF inhibitor. The majority of patients in both groups were over the age of 50 and were concurrently administered DMARDs (Table 1). Despite TNF inhibitor therapy, none of the patients showed evidence of active TB in follow up. All but two of the positive TST patients received TNF inhibitors for at least 12 months, with the two receiving therapy for 6.9 and 0.7 months (Table 2). At each time interval, the total number of patients that made that length of time was tabulated. The numbers steadily decreased; none of the patients were treated with biologics for more than 120 months (Figure 1). In total, the positive TST patients accumulated 146 patient years of TNF inhibitor therapy and the negative TST patients 746 patient years. Patients were treated with a range of TNF inhibitors; it was common for the patients to have been administered Table 1 TNF Inhibitor-treated RA Patient Characteristics for Those with a Positive TST versus Those with a Negative TST Characteristic Postive TST * Negative TST** Age over 50 years 76.9% 70.0% Male : female 22 male : 17 female 88 male : 86 female Patients on DMARDs 77.8% 74.7% Number of patients with TB 0% 0% * Based on 39 patients; ** Based on 174 patients. 7
3 NORTHERN (HIGH)LIGHTS more than one form of TNF inhibitor therapy over the course of their treatment (Table 3). A total of 74% of positive TST patients and 59% of negative TST patients were receiving infliximab at some point in time, which was the most commonly-used TNF inhibitor. Of the remaining agents, the most common to least commonly administered were adalimumab, abatacept, rituximab, tocilizumab, Table 2 Minimum Length of Time Patients with a Positive TST Have Received TNF Inhibitors* Time on TNF Inhibitor * Total patient-years was Number of Patients etanercept, and golimumab. None of the TST-positive patients had taken golimumab. Of the 39 patients with a positive TST, 17 (44%) had a history of prednisone use, while 59 of the 174 patients (34%) with a negative TST had a history of prednisone use. Discussion Despite using TNF inhibitors without TB prophylaxis in a population considered at risk for TB reactivation, that being patients with a positive TST, no cases of reactivation were observed. Investigations have reported that the majority of LTBI reactivations due to TNF inhibitor administration occur in the early phase of treatment, 4,11,26-28 with the median time of reactivation between weeks. 4,11 In this chart review, all but two of the patients received TNF inhibitors for more than 12 months. Furthermore, all of the patients were monitored closely at the Saskatoon TB clinic for two years after initiating TNF inhibitor therapy. If TB were to occur, the reactivations would have been most likely within that two-year window. 11,26 The level of increased risk of TB reactivation among the different biologics has been reported to differ. In one study, incident rates of TB reactivation were found to be highest with infliximab (1.5/1,000 patient-years), followed Figure 1. Patients with a Positive TST Receiving TNF Inhibitors: Minimum Length of Time Number of Patients Time (Months) Legend: At each time interval, the total number of patients that made that length of time was tabulated. Therefore, the numbers steadily decrease until none of the patients are on biologics for more than 120 months. 8
4 by adalimumab (0.9/1,000 patient-years), and then etanercept (0.5/1,000 patient-years). 17 Other reports also placed infliximab as the most at risk for causing TB reactivation, followed by adalumimab, then etanercept. 26 Some studies have found a three- to four-fold higher risk when on infliximab or adalimumab as compared to etanercept; while other investigations have claimed there to be no difference between infliximab, adalumimab, and etanercept with respect to TB reactivation. 25 There has been no consistent pattern of serious TB infection risk associated with the use of TNF inhibitors. 25 Adalimumab was launched after the risk of TB had emerged and screening initiated, which may account for some of the over-reported rates of TB in patients on adalimumab, as a consequence of increased vigilance. 25 The mechanism of action of rituximab is not a concern for TB reactivation as while receiving TNF inhibitors. 30 In fact, there are no reported cases to date with patients being treated with rituximab, 30 nor have increased rate of TB been shown with tocilizumab. 28 However, since none of the patients developed active TB in our study, there does not appear to be an increased risk with any of the medications used. As mentioned, the preferred regimen for treating LTBI is nine months of INH daily. 1,19,21,22 The efficacy of IHN has been reported as 60% for six months of daily INH (> 80% completion), 31,32 and 90% for nine months of daily INH. 33 The completion rate is, however, very low, with one study showing persistence as low as 39%, 34 and other reports claiming rates between 50% and 60%. 35,36 There are considerable risks associated with TB prophylaxis. The most serious side effect of INH is toxic Table 3 Breakdown of TNF-inhibitor Usage in the Two Patient Groups* TNF Inhibitor Infliximab Adalimumab Abatacept Rituximab Tocilizumab Etanercept Golimumab Positive TST** 74.1% 33.3% 29.6% 7.4% 11.1% 3.7% 0% Negative TST*** 58.6% 26.4% 17.8% 8.6% 9.8% 23.6% 6.9% *The percentages are based on patients receiving mediation for any period of time. ** Based on 39 patients. *** Based on 174 patients. hepatitis. 23 Hepatic adverse effects from INH range from a mild increases in aminotransferases (10%-20%) to overt hepatitis, which is rare. 24 Risk factors include age over 35 years, being female, baseline elevation of aspartate aminotransferase (AST), and the concurrent use of alcohol. 26,29,37 With over one million patients treated with INH since 1991, the incidence of INH-associated liver injury has been estimated at 1/1,000 patients, 19 hospitalization rates have been reported at 0.1 to 0.2/1,000, and mortality rates of 0.0 to 0.3/1,000. 6,20,37 In public health clinic studies, the incidence of INH hepatotoxicity has varied between 0.1% 24 and 4%. 38 The differences is perhaps due to age of the population or definition of hepatotoxicity in these studies. 39 Another study found a rate of 5.63 hepatotoxic events per 1,000 patients, with higher rates associated with patients over the age of It should be noted that in this database study, only 41% of patients were to found to have completed three months of INH therapy, and only 22% six months of therapy. 39 The toxicity may have been higher in some instances if the compliance had been higher. 39 In one trial, 53% of the 255 patients that completed the nine months of INH therapy reported some symptoms during the treatment. 2 In the same trial, hepatotoxicity accounted for 40% of those patients permanently discontinued from the treatment. 2 There are competing risks when considering treatment: TNF inhibitors and the reactivation of TB versus INH toxicity and compliance. If the annual risk of TB is greater than the risk of drug induced hepatitis, then prophylaxis should be received. 22 Conversely, if the risk of hepatitis is greater, then patients should not receive prophylaxis, but rather be monitored closely, having any symptoms that develop investigated quickly and diagnosed early. 22 When risk outweighs benefit, patients with an abnormal chest X-ray consistent with past TB (or prior extra pulmonary TB that has been adequately treated in the past) can begin TNF inhibitor treatment while being monitored clinically every three months. 22 If no adequate treatment was received, then the risk-benefit analysis favors chemotherapy. 22 To illustrate the point, consider treatment for an average RA patient in Saskatchewan. The incidence of TB in Canada is 5.1/100,000, while in Saskatchewan it is somewhat higher at 6.2 /100, Specific incidences of TB in Saskatchewan are less than 1/100,000 for Caucasians, 43/100,000 for status First Nations, 23/100,000 for Metis, and 17/100,000 for foreign-born Canadians. 31 The progression from latent infection to active TB has a 8a
5 NORTHERN (HIGH)LIGHTS universal estimate of a 10% incidence with a positive TST. 31 In Saskatchewan, the rates are 0.8% and 6.9% for White-European and Status First Nation individuals, respectively. 31 In order to make a risk calculation, the annual risk of TB should be multiplied by five (due to the increased risk caused by TNF inhibitor therapy) to account for TNF inhibitor medications, 22 which would be divided by the risk of INH hepatitis. 31 A ratio of less than one indicates observation is best, while a ratio of more than one would indicate that prophylaxis is preferred. 31 The incidence would be determined by reviewing local epidemiology for the patient group and the toxicity as 278/100,000 people. 31 For example, a Caucasian in Saskatchewan would have a risk of ([1/100,000]*5)/ ([278/100,000]), which would be 0.02, strongly favoring observation. 31 Even for a Status First Nation patient, the ratio would be 0.8 ([43 cases/100,000 people]*5)/ ([278 cases/100,000 people]). 30 In this study, 76.2% of the RA patients treated with TNF inhibitors with a positive TST were over the age of 50 years, they would have been at a higher risk of toxicity. The riskbenefit ratio was less than one for all of the patients as well. Therefore, all of the patients theoretically would be safer not receiving prophylaxis. In addition to being safer for the patient, not having to give prophylaxis would be beneficial for the health care system in terms of cost. In a study using financial information from Montreal, Canada, the estimated cost of treating one patient with nine months of INH was $1,073 if no symptoms developed, and $1,131 if symptoms developed but therapy was still completed. 2 Costs were attributable to routine visits, therapeutic agents, pharmacy charges, routine testing, and unscheduled visits. The costs of evaluation and management of specific adverse events varied from $668 to $1,249, depending on the severity of the adverse event. 2 Although medication is inexpensive for LTBI, the total costs are high because close monitoring is imperative due to the risk of drug-induced hepatitis. 2 The exact risk of morbidity of TB associated with corticosteroid therapy is unknown, but therapy with them is a well-known risk factor for TB. 40 Reactivation of TB after patients were administered corticosteroids has been documented Corticosteroids have an immunosuppressive effect, which can promote TB reactivation, therefore, careful observation of patients taking steroids is required. 42,44 However, there has also been no relationship found between total dose or duration and risk. 42 One of the limitations of this study was the small number of patients (39) with a positive TST, making it impossible to compare results with previous studies. With an expected risk of TB in TST-positive patients on TNF inhibitors of 2.6/1,000, the study would need about 400 patients to show one case of TB. There are not enough people in Saskatchewan to provide sufficient numbers. As far as we know, Saskatchewan is the only place providing biologics to TST-positive patients without receiving TB prophylaxis prior to therapy. Consequently, all the patients must come from Saskatchewan, making it very difficult to attain sufficient numbers of patients. Although the numbers of patients in this study are not sufficient to compare the levels of risks with other studies, it shows that none of the RA patients on TNF inhibitors had reactivation of their TB. Conclusion & Summary In this investigation we demonstrated that RA patients on TNF inhibitors who did not receive prophylaxis are not at risk for TB reactivation. Although we could not fully answer the objective question of whether patients are at increased risk by not being on prophylaxis, the study acts as a probing study into the possibility of treating RA with biologics in patients with latent TB without the need for TB prophylaxis. Between 400 and 5,000 patients would be needed to objectively determine that there is no increased risk, but it is at least suggested. More investigations are needed, along with more follow up to provide more data. We would like to acknowledge K. Shawn Davison for his contributions to editing. References 1. Winthrop KL. Update on tuberculosis and other opportunistic infections associated with drugs blocking tumour necrosis factor {alpha}. Ann Rheum Dis 2005; 64 Suppl 4:iv Aspler A, Long R, Trajman A, et al. Impact of treatment completion, intolerance and adverse events on health system costs in a randomised trial of 4 months rifampin or 9 months isoniazid for latent TB. Thorax 2010; 65(7): Bennett DE, Courval JM, Onorato I, et al. Prevalence of tuberculosis infection in the United States population: the national health and nutrition examination survey, Am J Respir Crit Care 2008; 177(3): Patkar NM, Teng GG, Curtis JR, et al. Association of infections and tuberculosis with antitumor necrosis factor alpha therapy. Curr Opin Rheumatol 2008; 20(3): Brassard P, Kezouh A, Suissa S. Antirheumatic drugs and the risk of tuberculosis. Clin Infect Dis 2006; 43(6): Villiger PM, Zellweger JP, Möller B. Novel screening tools for latent tuberculosis: time to leave an old friend? Curr Opin Rheumatol 2009; 21(3): Gupta A, Kaul A, Tsolaki AG, et al. Mycobacterium tuberculosis: immune evasion, latency and reactivation. Immunobiology 2012; 217(3): b
6 8. Gomez JE, McKinney JD, M. tuberculosis persistence, latency, and drug tolerance. Tuberculosis (Edinb) 2004; 84(1-2): Tufariello JM, Chan J, Flynn JL. Latent tuberculosis: mechanisms of host and bacillus that contribute to persistent infection. Lancet Infect Dis 2003; 3(9): Gardam MA, Keystone EC, Menzies R, et al. Anti-tumour necrosis factor agents and tuberculosis risk: mechanisms of action and clinical management. Lancet Infect Dis 2003; 3(3): Keane J, Gershon S, Wise RP, et al. Tuberculosis associated with infliximab, a tumor necrosis factor alpha-neutralizing agent. N Engl J Med 2001; 345(15): Settas LD, Tsimirikas G, Vosvotekas G, et al. Reactivation of pulmonary tuberculosis in a patient with rheumatoid arthritis during treatment with IL-1 receptor antagonists (anakinra). J Clin Rheumatol 2007; 13(4): Lin PL, Plessner HL, Voitenok NN,et al. Tumor necrosis factor and tuberculosis. J Investig Dermatol Symp Proc 2007; 12(1): Lin PL, Flynn JL. Understanding latent tuberculosis: a moving target. J Immunol 2010; 185(1): Botha T, Ryffel B. Reactivation of latent tuberculosis infection in TNF- deficient mice. J Immunol 2003; 171(6): Singh JA, Furst DE, Bharat A, et al update of the 2008 American College of Rheumatology recommendations for the use of disease-modifying antirheumatic drugs and biologic agents in the treatment of rheumatoid arthritis. Arthritis Care Res (Hoboken) 2012; 64(5): Dixon WG, Watson K, Lunt M, et al, on behalf of the British Society for Rheumatology Biologics Register. Rates of serious infection, including sitespecific and bacterial intracellular infection, in rheumatoid arthritis patients receiving anti tumor necrosis factor therapy: results from the British Society for Rheumatology Biologics Register. Arthritis Rheum 2006; 54(8): American Thoracic Society (ATS) and Centers for Disease Control Prevention (CDC). Targeted tuberculin testing and treatment of latent tuberculosis infection. Am J Respir Crit Care Med 2000; 161(4 Pt 2):S CDC. Targeted tuberculin testing and treatment of latent tuberculosis infection. MMWR Mortal Morb Wkly Rep 2000; 49(6): Targeted tuberculin testing and treatment of latent tuberculosis infection. This official statement of the American Thoracic Society was adopted by the ATS Board of Directors, July This is a joint statement of the American Thoracic Society (ATS) and the Centers for Disease Control and Prevention (CDC). This statement was endorsed by the Council of the Infectious Diseases Society of America (IDSA), September 1999, and the sections of this statement. Am J Respir Crit Care Med 2000; 161(4 pt 2):S Long R. Canadian tuberculosis standards. 6th ed. Ottawa, ON, Canada: Canadian Lung Association & Public Health Agency of Canada, British Thoracic Society Standards of Care Committee. BTS recommendations for assessing risk and for managing Mycobacterium tuberculosis infection and disease in patients due to start anti-tnf-alpha treatment. Thorax 2005; 60(10): da Rocha Castelar Pinheiro G. Rheumatoid arthritis and tuberculosis in the tumor necrosis factor inhibitors era: observations from Brazil. J Clin Rheumatol 2005; 11(6): Nolan CM, Goldberg SV, Buskin SE. Hepatotoxicity associated with isoniazid preventive therapy: a 7-year survey from a Public Health Tuberculosis Clinic. JAMA 1999; 281(11): Dixon WG, Watson K, Lunt M, et al. British Society for Rheumatology Biologics Register. Rates of serious infection, including site-specific and bacterial intracellular infection, in rheumatoid arthritis patients receiving antitumor necrosis factor therapy: results from the British Society for Rheumatology Biologics Register. Arthritis Rheum 2006; 54(8): Szeto T, Peterson J, Silva F. A case of tuberculous peritonitis in the United States in a patient with rheumatoid arthritis treated with adalimumab. J Clin Rheumatol 2010; 16(3): Tubach F, Salmon D, Ravaud P, et al. Risk of tuberculosis is higher with antitumor necrosis factor monoclonal antibody therapy than soluble tumor necrosis factor receptor therapy. Arthritis Rheum 2009; 60(7): Campbell L, Chen C, Bhagat SS, et al. Risk of adverse events including serious infections in rheumatoid arthritis patients treated with tocilizumab: a systematic literature review and meta-analysis of randomized controlled trials. Rheumatology (Oxford) 2011; 50(3): Jung N, Owczarczyk K, Hellmann M, et al. Efficacy and safety of rituximab in a patient with active rheumatoid arthritis and chronic disseminated pulmonary aspergillosis and history of tuberculosis. Rheumatology (Oxford) 2008; 47(6): Burr ML, Malaviya AP, Gaston JH, et al. Rituximab in rheumatoid arthritis following anti-tnf-associated tuberculosis. Rheumatology (Oxford) 2008; 47(5): Hoeppner V, Olszynski W. Prophylactic treatment of T infection: risks vs. benefits. Personal communications, Smieja MJ, Marchetti CA, Cook DJ, et al. Isoniazid for preventing tuberculosis in non-hiv infected persons (Cochrane Review). Cochrane Database Syst Rev 2000; (2):CD Comstock GW. How much isoniazid is needed for prevention of tuberculosis among immunocompetent adults? Int J Tuberc Lung Dis 1999; 3(10): Horsburgh CR Jr, Goldberg S, Bethel J, et al. Tuberculosis Epidemiologic Studies Consortium. Latent TB infection treatment acceptance and completion in the United States and Canada. Chest 2010; 137(2): Page KR, Sifakis F, Montes de OR, et al. Improved adherence and less toxicity with rifampin vs isoniazid for treatment of latent tuberculosis: a retrospective study. Arch Intern Med 2006; 166(17): Jasmer RM, Nahid P, Hopewell PC. Latent tuberculosis infection. N Engl J Med 2002; 347(23): Bruns H, Meinken C, Schauenberg P, et al. Anti-TNF immunotherapy reduces CD8+ T cell-mediated antimicrobial activity against Mycobacterium tuberculosis in humans. J Clin Invest 2009; 119(5): McNeill L, Allen M, Estrada C, Cook P. Pyrazinamide and rifampin vs isoniazid for the treatment of latent tuberculosis: improved completion rates but more hepatotoxicity. Chest 2003; 123(1): Fountain FF, Tolley E, Chrisman CR, et al. Isoniazid hepatotoxicity associated with treatment of latent tuberculosis infection: a 7-year evaluation from a public health tuberculosis clinic. Chest 2005; 128(1): Bass JB Jr, Farer LS, Hopewell PC, et al. Treatment of tuberculosis and tuberculosis infection in adults and children. American Thoracic Society and The Centers for Disease Control and Prevention. Am J Respir Crit Care Med 1994; 149(5): Haanaes OC, Bergmann A. Tuberculosis emerging in patients treated with corticosteroids. Eur J Respir Dis 1983; 64(4): Kobashi Y, Matsushima T. Clinical analysis of pulmonary tuberculosis in association with corticosteroid therapy. Intern Med 2002; 41(12): Sahn SA, Lakshminarayan S. Tuberculosis after corticosteroid therapy. Br J Dis Chest 1976; 70(3): Senderovitz T, Viskum K. Corticosteroids and tuberculosis. Respir Med 1994; 88(8): Nicholas M. Baniak, BSc College of Medicine, University of Saskatchewan Saskatoon, Saskatchewan Vernon M. Hoeppner, MD, FRCPC Professor and Head, Department of Medicine College of Medicine, University of Saskatchewan Saskatoon, Saskatchewan Wojciech P. Olszynski, MD, PhD, FRCPC, CCD Clinical Professor of Medicine Director, Saskatoon Osteoporosis and Arthritis Infusion Centre Honorary Consul of the Republic of Poland in Saskatoon Saskatoon, Saskatchewan 8c
Tuberculosis and Biologic Therapies: Risk and Prevention
 Tuberculosis and Biologic Therapies: Risk and Prevention Kevin L. Winthrop, MD, MPH Associate Professor, Divisions of Infectious Diseases, Public Health and Preventive Medicine Oregon Health & Science
Tuberculosis and Biologic Therapies: Risk and Prevention Kevin L. Winthrop, MD, MPH Associate Professor, Divisions of Infectious Diseases, Public Health and Preventive Medicine Oregon Health & Science
A Focus on Vaccinations & Infectious Diseases
 Spring 2014, Volume 24, Number 1 The Journal of the Canadian Rheumatology Association Under the Microscope: A Focus on Vaccinations & Infectious Diseases Editorial The Six Million Dollar Rheumatologist
Spring 2014, Volume 24, Number 1 The Journal of the Canadian Rheumatology Association Under the Microscope: A Focus on Vaccinations & Infectious Diseases Editorial The Six Million Dollar Rheumatologist
TUBERCULOSIS AND THE TNF-α INHIBITORS. Lloyd Friedman, M.D. Yale University Milford Hospital
 TUBERCULOSIS AND THE TNF-α INHIBITORS Lloyd Friedman, M.D. Yale University Milford Hospital Outline TNF-α Anti-TNF-α medications Rates of tuberculosis Lower rates with etanercept Screening for latent tuberculosis
TUBERCULOSIS AND THE TNF-α INHIBITORS Lloyd Friedman, M.D. Yale University Milford Hospital Outline TNF-α Anti-TNF-α medications Rates of tuberculosis Lower rates with etanercept Screening for latent tuberculosis
Weekly. August 8, 2003 / 52(31);
 Weekly August 8, 2003 / 52(31);735-739 Update: Adverse Event Data and Revised American Thoracic Society/CDC Recommendations Against the Use of Rifampin and Pyrazinamide for Treatment of Latent Tuberculosis
Weekly August 8, 2003 / 52(31);735-739 Update: Adverse Event Data and Revised American Thoracic Society/CDC Recommendations Against the Use of Rifampin and Pyrazinamide for Treatment of Latent Tuberculosis
10/3/2017. Updates in Tuberculosis. Global Tuberculosis, WHO 2015 report. Objectives. Disclosures. I have nothing to disclose
 Disclosures Updates in Tuberculosis I have nothing to disclose Chris Keh, MD Assistant Clinical Professor, Division of Infectious Diseases, UCSF TB Controller, TB Prevention and Control Program, Population
Disclosures Updates in Tuberculosis I have nothing to disclose Chris Keh, MD Assistant Clinical Professor, Division of Infectious Diseases, UCSF TB Controller, TB Prevention and Control Program, Population
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: golimumab_simponi 8/2013 2/2018 2/2019 3/2018 Description of Procedure or Service Golimumab (Simponi and
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: golimumab_simponi 8/2013 2/2018 2/2019 3/2018 Description of Procedure or Service Golimumab (Simponi and
Jennifer Lam MPH candidate 2009 Johns Hopkins Bloomberg School of Public Health. Preceptors: Wendy Cronin, PhD MT(ASCP), Cathy Goldsborough, RN
 Jennifer Lam MPH candidate 2009 Johns Hopkins Bloomberg School of Public Health Preceptors: Wendy Cronin, PhD MT(ASCP), Cathy Goldsborough, RN Phase Symposium: May 6, 2009 Background & Rationale Maryland
Jennifer Lam MPH candidate 2009 Johns Hopkins Bloomberg School of Public Health Preceptors: Wendy Cronin, PhD MT(ASCP), Cathy Goldsborough, RN Phase Symposium: May 6, 2009 Background & Rationale Maryland
Tuberculosis Pathogenesis
 Tuberculosis Pathogenesis Renuka Khurana, MD, MPH May 12, 2015 TB for Community Providers May 12, 2015 Phoenix, Arizona EXCELLENCE EXPERTISE INNOVATION Renuka Khurana, MD, MPH has the following disclosures
Tuberculosis Pathogenesis Renuka Khurana, MD, MPH May 12, 2015 TB for Community Providers May 12, 2015 Phoenix, Arizona EXCELLENCE EXPERTISE INNOVATION Renuka Khurana, MD, MPH has the following disclosures
Tuberculosis Intensive
 Tuberculosis Intensive San Antonio, Texas April 3 6, 2012 Tuberculosis Pathogenesis Lynn Horvath, MD April 3, 2012 Lynn Horvath, MD has the following disclosures to make: No conflict of interests No relevant
Tuberculosis Intensive San Antonio, Texas April 3 6, 2012 Tuberculosis Pathogenesis Lynn Horvath, MD April 3, 2012 Lynn Horvath, MD has the following disclosures to make: No conflict of interests No relevant
Case reports. Patient 1
 REVIEW ARTICLE BJD British Journal of Dermatology Tuberculosis and tumour necrosis factor-a inhibitor therapy: a report of three cases in patients with psoriasis. Comprehensive screening and therapeutic
REVIEW ARTICLE BJD British Journal of Dermatology Tuberculosis and tumour necrosis factor-a inhibitor therapy: a report of three cases in patients with psoriasis. Comprehensive screening and therapeutic
Detecting latent tuberculosis infection during anti-tumour necrosis factor therapy
 Detecting latent tuberculosis infection during anti-tumour necrosis factor therapy J.S. Ringrose 1, S.E. Sanche 2, R.M. Taylor-Gjevre 3 1 Division of General Internal Medicine, Department of Medicine,
Detecting latent tuberculosis infection during anti-tumour necrosis factor therapy J.S. Ringrose 1, S.E. Sanche 2, R.M. Taylor-Gjevre 3 1 Division of General Internal Medicine, Department of Medicine,
CHAPTER 3: DEFINITION OF TERMS
 CHAPTER 3: DEFINITION OF TERMS NOTE: TB bacteria is used in place of Mycobacterium tuberculosis and Mycobacterium tuberculosis complex in most of the definitions presented here. 3.1 Acid-fast bacteria
CHAPTER 3: DEFINITION OF TERMS NOTE: TB bacteria is used in place of Mycobacterium tuberculosis and Mycobacterium tuberculosis complex in most of the definitions presented here. 3.1 Acid-fast bacteria
TB Intensive San Antonio, Texas December 1-3, 2010
 TB Intensive San Antonio, Texas December 1-3, 2010 TB Pathogenesis and Transmission Lynn Horvath, MD; TCID December 1, 2010 Tuberculosis Pathogenesis Lynn L. Horvath, MD, FACP, FIDSA Associate Professor
TB Intensive San Antonio, Texas December 1-3, 2010 TB Pathogenesis and Transmission Lynn Horvath, MD; TCID December 1, 2010 Tuberculosis Pathogenesis Lynn L. Horvath, MD, FACP, FIDSA Associate Professor
Let s Talk TB A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year
 A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Madhukar Pai, MD, PhD Author and Series Editor Camilla Rodrigues, MD co-author Abstract Most individuals who get exposed
A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Madhukar Pai, MD, PhD Author and Series Editor Camilla Rodrigues, MD co-author Abstract Most individuals who get exposed
Tuberculosis Tools: A Clinical Update
 Tuberculosis Tools: A Clinical Update CAPA Conference 2014 JoAnn Deasy, PA-C. MPH, DFAAPA jadeasy@sbcglobal.net Adjunct Faculty Touro PA Program Learning Objectives Outline the pathogenesis of active pulmonary
Tuberculosis Tools: A Clinical Update CAPA Conference 2014 JoAnn Deasy, PA-C. MPH, DFAAPA jadeasy@sbcglobal.net Adjunct Faculty Touro PA Program Learning Objectives Outline the pathogenesis of active pulmonary
Simponi / Simponi ARIA (golimumab)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 6 Last Review Date: September 15, 2016 Simponi / Simponi
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 6 Last Review Date: September 15, 2016 Simponi / Simponi
Actemra (tocilizumab) CG-DRUG-81
 Market DC Actemra (tocilizumab) CG-DRUG-81 Override(s) Prior Authorization Approval Duration 1 year Medications Line of Business Quantity Limit Actemra (tocilizumab) vials VA MCD and All L-AGP May be subject
Market DC Actemra (tocilizumab) CG-DRUG-81 Override(s) Prior Authorization Approval Duration 1 year Medications Line of Business Quantity Limit Actemra (tocilizumab) vials VA MCD and All L-AGP May be subject
*Bamrasnaradura Infectious Diseases Institute, Nonthaburi 11000, Bangkok Hospital, Bangkok, Thailand. ABSTRACT
 OriginalArticle Isoniazid Prophylaxis of Latent Tuberculous Infection among Healthcare Workers in Bamrasnaradura Infectious Diseases Institute Patama Suttha, M.D.*, Pranom Noppakun, M.NS.*, Patchara Tanthirapat,
OriginalArticle Isoniazid Prophylaxis of Latent Tuberculous Infection among Healthcare Workers in Bamrasnaradura Infectious Diseases Institute Patama Suttha, M.D.*, Pranom Noppakun, M.NS.*, Patchara Tanthirapat,
Cimzia. Cimzia (certolizumab pegol) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Cimzia Page: 1 of 5 Last Review Date: March 17, 2017 Cimzia Description Cimzia (certolizumab pegol)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Cimzia Page: 1 of 5 Last Review Date: March 17, 2017 Cimzia Description Cimzia (certolizumab pegol)
TB testing in children on biologics
 TB testing in children on biologics Version: 1 Approval Committee: Date of Approval: Ratification Group (eg Clinical network): Date of Ratification Signature of ratifying Group Chair Author(s) and title
TB testing in children on biologics Version: 1 Approval Committee: Date of Approval: Ratification Group (eg Clinical network): Date of Ratification Signature of ratifying Group Chair Author(s) and title
DENOMINATOR: All patients aged 18 and older with a diagnosis of inflammatory bowel disease
 Measure #274: Inflammatory Bowel Disease (IBD): Testing for Latent Tuberculosis (TB) Before Initiating Anti-TNF (Tumor Necrosis Factor) Therapy National Quality Strategy Domain: Effective Clinical Care
Measure #274: Inflammatory Bowel Disease (IBD): Testing for Latent Tuberculosis (TB) Before Initiating Anti-TNF (Tumor Necrosis Factor) Therapy National Quality Strategy Domain: Effective Clinical Care
Cimzia. Cimzia (certolizumab pegol) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Subject: Cimzia Page: 1 of 5 Last Review Date: December 8, 2017 Cimzia Description Cimzia (certolizumab
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Subject: Cimzia Page: 1 of 5 Last Review Date: December 8, 2017 Cimzia Description Cimzia (certolizumab
Regulatory Status FDA-approved indication: Orencia is a selective T cell costimulation modulator indicated for: (1)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.18 Subject: Orencia Page: 1 of 8 Last Review Date: March 16, 2018 Orencia Description Orencia (abatacept)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.18 Subject: Orencia Page: 1 of 8 Last Review Date: March 16, 2018 Orencia Description Orencia (abatacept)
Cimzia. Cimzia (certolizumab pegol) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Section: Prescription Drugs Effective Date: April 1, 2018 Subject: Cimzia Page: 1 of 5 Last Review
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.11 Section: Prescription Drugs Effective Date: April 1, 2018 Subject: Cimzia Page: 1 of 5 Last Review
TNF-alpha antagonist therapy modify the tuberculin skin test response
 DOI 10.1007/s00296-010-1424-3 ORIGINAL ARTICLE TNF-alpha antagonist therapy modify the tuberculin skin test response Tulin Cagatay Zeki Kilicaslan Penbe Cagatay Munevver Mertsoylu Ziya Gulbaran Reyhan
DOI 10.1007/s00296-010-1424-3 ORIGINAL ARTICLE TNF-alpha antagonist therapy modify the tuberculin skin test response Tulin Cagatay Zeki Kilicaslan Penbe Cagatay Munevver Mertsoylu Ziya Gulbaran Reyhan
Amjevita (adalimumab-atto) CG-DRUG-64, CG-DRUG-65
 Market DC Amjevita (adalimumab-atto) CG-DRUG-64, CG-DRUG-65 Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2
Market DC Amjevita (adalimumab-atto) CG-DRUG-64, CG-DRUG-65 Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2
Regulatory Status FDA- approved indication: Simponi and Simponi ARIA are tumor necrosis factor (TNF) blockers indicated for the treatment of: (2-3)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 9 Last Review Date: March 16, 2018 Simponi / Simponi
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 9 Last Review Date: March 16, 2018 Simponi / Simponi
ESCMID Online Lecture Library. by author
 Tuberculosis prevention in immunodepressed patients M. Carmen Fariñas Álvarez Infectious Diseases.H.U.Marqués de Valdecilla University of Cantabria, Spain DISCLOSURES I have no potential conflicts with
Tuberculosis prevention in immunodepressed patients M. Carmen Fariñas Álvarez Infectious Diseases.H.U.Marqués de Valdecilla University of Cantabria, Spain DISCLOSURES I have no potential conflicts with
Tuberculosis in Non-HIV Infected Immunosuppresed Hosts. TNFα inhibitors and beyond
 Tuberculosis in Non-HIV Infected Immunosuppresed Hosts TNFα inhibitors and beyond David E. Griffith, MD Assistant Medical Director Heartland National TB Center Professor of Medicine University of Texas
Tuberculosis in Non-HIV Infected Immunosuppresed Hosts TNFα inhibitors and beyond David E. Griffith, MD Assistant Medical Director Heartland National TB Center Professor of Medicine University of Texas
Contact Investigation and Prevention in the USA
 Contact Investigation and Prevention in the USA George D. McSherry, MD Division of Infectious Disease Penn State Children s Hospital Pediatric Section TB Center of Excellence Rutgers Global Tuberculosis
Contact Investigation and Prevention in the USA George D. McSherry, MD Division of Infectious Disease Penn State Children s Hospital Pediatric Section TB Center of Excellence Rutgers Global Tuberculosis
Pathogenesis of Rheumatoid Arthritis. Smolen, J. S. et al. (2012) Nat. Rev. Rheumatol. doi: /nrrheum
 1 Pathogenesis of Rheumatoid Arthritis 2 Smolen, J. S. et al. (2012) Nat. Rev. Rheumatol. doi:10.1038/nrrheum 2012.23 Biologic therapies used in the treatment of rheumatoid arthritis 3 Etanercept Infliximab
1 Pathogenesis of Rheumatoid Arthritis 2 Smolen, J. S. et al. (2012) Nat. Rev. Rheumatol. doi:10.1038/nrrheum 2012.23 Biologic therapies used in the treatment of rheumatoid arthritis 3 Etanercept Infliximab
Tuberculosis Update. Topics to be Addressed
 Tuberculosis Update Robert M. Jasmer, M.D. University of California, San Francisco TB Control Section, San Francisco Department of Public Health Topics to be Addressed TB in the USA Screening recommendations
Tuberculosis Update Robert M. Jasmer, M.D. University of California, San Francisco TB Control Section, San Francisco Department of Public Health Topics to be Addressed TB in the USA Screening recommendations
Communicable Disease Control Manual Chapter 4: Tuberculosis
 Provincial TB Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 www.bccdc.ca Communicable Disease Control Manual Definitions Page 1 2.0 DEFINITIONS Many of the definitions that follow are taken from
Provincial TB Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 www.bccdc.ca Communicable Disease Control Manual Definitions Page 1 2.0 DEFINITIONS Many of the definitions that follow are taken from
PREVENTING TB IN PATIENTS WITH CROHN S DISEASE NEEDING INFLIXIMAB OR OTHER ANTI-TNF THERAPY
 Gut Online First, published on August 19, 2005 as 10.1136/gut.2005.076034 PREVENTING TB IN PATIENTS WITH CROHN S DISEASE NEEDING INFLIXIMAB OR OTHER ANTI-TNF THERAPY DS Rampton Centre for Gastroenterology,
Gut Online First, published on August 19, 2005 as 10.1136/gut.2005.076034 PREVENTING TB IN PATIENTS WITH CROHN S DISEASE NEEDING INFLIXIMAB OR OTHER ANTI-TNF THERAPY DS Rampton Centre for Gastroenterology,
LTBI Treatment and Anti TNF alpha
 LTBI Treatment and Anti TNF alpha Therapy Julie Higashi, MD PhD Director, TB Control Section San Francisco Department of Public Health TNF alpha is important for the immune response against TB Macrophages
LTBI Treatment and Anti TNF alpha Therapy Julie Higashi, MD PhD Director, TB Control Section San Francisco Department of Public Health TNF alpha is important for the immune response against TB Macrophages
A Clinician s Perspective: Improving Rheumatology Patient Care Using the T-SPOT.TB Test
 A Clinician s Perspective: Improving Rheumatology Patient Care Using the T-SPOT.TB Test Solomon Forouzesh, MD, FACD, FACR Medical Director Arthritis Care & Treatment Center Clinical Associate Professor
A Clinician s Perspective: Improving Rheumatology Patient Care Using the T-SPOT.TB Test Solomon Forouzesh, MD, FACD, FACR Medical Director Arthritis Care & Treatment Center Clinical Associate Professor
Dimitrios Vassilopoulos,* Stamatoula Tsikrika, Chrisoula Hatzara, Varvara Podia, Anna Kandili, Nikolaos Stamoulis, and Emilia Hadziyannis
 CLINICAL AND VACCINE IMMUNOLOGY, Dec. 2011, p. 2102 2108 Vol. 18, No. 12 1556-6811/11/$12.00 doi:10.1128/cvi.05299-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Comparison
CLINICAL AND VACCINE IMMUNOLOGY, Dec. 2011, p. 2102 2108 Vol. 18, No. 12 1556-6811/11/$12.00 doi:10.1128/cvi.05299-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Comparison
TUBERCULOSIS IN HEALTHCARE SETTINGS Diana M. Nilsen, MD, FCCP Director of Medical Affairs, Bureau of Tuberculosis Control New York City Department of
 TUBERCULOSIS IN HEALTHCARE SETTINGS Diana M. Nilsen, MD, FCCP Director of Medical Affairs, Bureau of Tuberculosis Control New York City Department of Health and Mental Hygiene TODAY S PRESENTATION Epidemiology
TUBERCULOSIS IN HEALTHCARE SETTINGS Diana M. Nilsen, MD, FCCP Director of Medical Affairs, Bureau of Tuberculosis Control New York City Department of Health and Mental Hygiene TODAY S PRESENTATION Epidemiology
Amjevita (adalimumab-atto)
 *- Florida Healthy Kids Amjevita (adalimumab-atto) Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2 #* ^ prefilled
*- Florida Healthy Kids Amjevita (adalimumab-atto) Override(s) Prior Authorization Quantity Limit Medications Amjevita 20 mg/0.4 ml prefilled syringe Amjevita (adalimumab-atto) 40 mg/0.8 ml 2 #* ^ prefilled
Sharing the Care: Working Together on LTBI Treatment and Management Webinar. September 24, Curry International Tuberculosis Center
 TB Infection Diagnostics and Treatment Neha Shah MD MPH Field Medical Officer Tuberculosis Control Branch California Department of Public Health Centers for Disease Control and Prevention 1 Curry International
TB Infection Diagnostics and Treatment Neha Shah MD MPH Field Medical Officer Tuberculosis Control Branch California Department of Public Health Centers for Disease Control and Prevention 1 Curry International
Isoniazid treatment for latent tuberculosis infection is tolerable for rheumatoid arthritis patients receiving tumor necrosis factor inhibitor therapy
 ORIGINAL ARTICLE 2017 Mar 13. [Epub ahead of print] Isoniazid treatment for latent tuberculosis infection is tolerable for rheumatoid arthritis patients receiving tumor necrosis factor inhibitor therapy
ORIGINAL ARTICLE 2017 Mar 13. [Epub ahead of print] Isoniazid treatment for latent tuberculosis infection is tolerable for rheumatoid arthritis patients receiving tumor necrosis factor inhibitor therapy
Latent Tuberculosis Infection Reporting Instructions for Civil Surgeons Using CalREDIE Provider Portal
 Latent Tuberculosis Infection Reporting Instructions for Civil Surgeons Using CalREDIE Provider Portal Civil surgeons are required to report tuberculosis (TB) screening outcomes that result in latent TB
Latent Tuberculosis Infection Reporting Instructions for Civil Surgeons Using CalREDIE Provider Portal Civil surgeons are required to report tuberculosis (TB) screening outcomes that result in latent TB
ESCMID Online Lecture Library. by author
 Therapies or diseases predisposing to infection Congenital immunodeficiences Acquired conditions Common variable immunedeficiency particular diseases (e.g. HIV, cancer,leukemia, lymphoma, diabetes, cystic
Therapies or diseases predisposing to infection Congenital immunodeficiences Acquired conditions Common variable immunedeficiency particular diseases (e.g. HIV, cancer,leukemia, lymphoma, diabetes, cystic
Cell-Mediated Immunity and T Lymphocytes
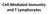 Cell-Mediated Immunity and T Lymphocytes T helper (Th) Cells Peripheral lymhoid tissue thymus Lymphoid stem cell CD8+ CD4+ CD4+ Treg CD8+ CTL + antigen Cytotoxic T lymphocyte CD4+ Th Helper T cell CD4+
Cell-Mediated Immunity and T Lymphocytes T helper (Th) Cells Peripheral lymhoid tissue thymus Lymphoid stem cell CD8+ CD4+ CD4+ Treg CD8+ CTL + antigen Cytotoxic T lymphocyte CD4+ Th Helper T cell CD4+
Clinical features of active tuberculosis that developed during anti-tumor necrosis factor therapy in patients with inflammatory bowel disease
 ORIGINAL ARTICLE pissn 1598-9100 eissn 2288-1956 http://dx.doi.org/10.5217/ir.2016.14.2.146 Intest Res 2016;14(2):146-151 Clinical features of active tuberculosis that developed during anti-tumor necrosis
ORIGINAL ARTICLE pissn 1598-9100 eissn 2288-1956 http://dx.doi.org/10.5217/ir.2016.14.2.146 Intest Res 2016;14(2):146-151 Clinical features of active tuberculosis that developed during anti-tumor necrosis
Treatment of TB Infection Lisa Y. Armitige, MD, PhD April 7, 2015
 Treatment of TB Infection Lisa Y. Armitige, MD, PhD April 7, 2015 Tuberculosis Infection Diagnosis and Treatment April 7, 2015 El Paso, TX EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has
Treatment of TB Infection Lisa Y. Armitige, MD, PhD April 7, 2015 Tuberculosis Infection Diagnosis and Treatment April 7, 2015 El Paso, TX EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has
A look at medical factors that increase the risk for TB disease
 A look at medical factors that increase the risk for TB disease Mark Lobato, MD New England TB Consultant Division of Tuberculosis Elimination CDC Overview The spectrum of M. tuberculosis infection Immune
A look at medical factors that increase the risk for TB disease Mark Lobato, MD New England TB Consultant Division of Tuberculosis Elimination CDC Overview The spectrum of M. tuberculosis infection Immune
TB Infection Who is Testing and Treating? TB Control and Elimination: Current Dilemma. Span of TB Control: 2010
 TB Infection Who is Testing and Treating? Jennifer Flood, M.D., M.P.H. California Department of Public Health Tuberculosis Control Branch Jennifer.Flood@cdph.ca.gov 1 TB Control and Elimination: Current
TB Infection Who is Testing and Treating? Jennifer Flood, M.D., M.P.H. California Department of Public Health Tuberculosis Control Branch Jennifer.Flood@cdph.ca.gov 1 TB Control and Elimination: Current
LATENT TUBERCULOSIS SCREENING AND TREATMENT:
 LATENT TUBERCULOSIS SCREENING AND TREATMENT: TB or not TB Christopher Kwong, MD and William Rifkin, MD Week 14 Educational Objectives: 1. Understand who should be screened for latent TB infection and why
LATENT TUBERCULOSIS SCREENING AND TREATMENT: TB or not TB Christopher Kwong, MD and William Rifkin, MD Week 14 Educational Objectives: 1. Understand who should be screened for latent TB infection and why
Center for Evidence-based Policy
 P&T Committee Brief Targeted Immune Modulators: Comparative Drug Class Review Alison Little, MD Center for Evidence-based Policy Oregon Health & Science University 3455 SW US Veterans Hospital Road, SN-4N
P&T Committee Brief Targeted Immune Modulators: Comparative Drug Class Review Alison Little, MD Center for Evidence-based Policy Oregon Health & Science University 3455 SW US Veterans Hospital Road, SN-4N
Inflammatory arthritis, such as rheumatoid arthritis (RA), is
 O r i g i n a l A r t i c l e Using Biologics in Inflammatory Arthritis: Assessing the Risks and Benefits Gina Rohekar MD FRCPC MSc (Clin Epi) About the Author Gina Rohekar is an assistant professor at
O r i g i n a l A r t i c l e Using Biologics in Inflammatory Arthritis: Assessing the Risks and Benefits Gina Rohekar MD FRCPC MSc (Clin Epi) About the Author Gina Rohekar is an assistant professor at
CHILDHOOD TUBERCULOSIS: NEW WRINKLES IN AN OLD DISEASE [FOR THE NON-TB EXPERT]
![CHILDHOOD TUBERCULOSIS: NEW WRINKLES IN AN OLD DISEASE [FOR THE NON-TB EXPERT] CHILDHOOD TUBERCULOSIS: NEW WRINKLES IN AN OLD DISEASE [FOR THE NON-TB EXPERT]](/thumbs/89/99628771.jpg) CHILDHOOD TUBERCULOSIS: NEW WRINKLES IN AN OLD DISEASE [FOR THE NON-TB EXPERT] QUESTION: : Which children in the United States should get a tuberculin skin test? Do questionnaires really work? Jeffrey
CHILDHOOD TUBERCULOSIS: NEW WRINKLES IN AN OLD DISEASE [FOR THE NON-TB EXPERT] QUESTION: : Which children in the United States should get a tuberculin skin test? Do questionnaires really work? Jeffrey
Regulatory Status FDA- approved indication: Simponi and Simponi ARIA are tumor necrosis factor (TNF) blockers indicated for the treatment of:
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 8 Last Review Date: March 17, 2017 Simponi / Simponi
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 8 Last Review Date: March 17, 2017 Simponi / Simponi
LATENT TUBERCULOSIS. Robert F. Tyree, MD
 LATENT TUBERCULOSIS Robert F. Tyree, MD 1 YK TB OFFICERS Ron Bowerman Elizabeth Roll Mien Chyi (Pediatrics) Cindi Mondesir (Pediatrics) The new guys: Philip Johnson Robert Tyree 2009 CDC TB CASE DEFINITION
LATENT TUBERCULOSIS Robert F. Tyree, MD 1 YK TB OFFICERS Ron Bowerman Elizabeth Roll Mien Chyi (Pediatrics) Cindi Mondesir (Pediatrics) The new guys: Philip Johnson Robert Tyree 2009 CDC TB CASE DEFINITION
Diagnosis & Management of Latent TB Infection
 Diagnosis & Management of Latent TB Infection Prof. Ashok Rattan, MD, MAMS, INSA DFG, WHO Lab Director Academics, Industry: Research, Diagnosis, Public Health, Academics Adviser: Laboratory Operations,
Diagnosis & Management of Latent TB Infection Prof. Ashok Rattan, MD, MAMS, INSA DFG, WHO Lab Director Academics, Industry: Research, Diagnosis, Public Health, Academics Adviser: Laboratory Operations,
Elevated risk of tuberculosis in patients with rheumatoid arthritis in Japan
 ARD Online First, published on July 12, 2006 as 10.1136/ard.2005.047274 Concise report Elevated risk of tuberculosis in patients with rheumatoid arthritis in Japan Toru Yamada, Ayako Nakajima, Eisuke Inoue,
ARD Online First, published on July 12, 2006 as 10.1136/ard.2005.047274 Concise report Elevated risk of tuberculosis in patients with rheumatoid arthritis in Japan Toru Yamada, Ayako Nakajima, Eisuke Inoue,
Experience with Pyrazinamide and Rifampin Regimens for Latent TB Infection
 Experience with Pyrazinamide and Rifampin Regimens for Latent TB Infection Krista Powell, MD, MPH Co-Project Officer, National Surveillance for Severe Adverse Events Associated with LTBI Treatment Lead,
Experience with Pyrazinamide and Rifampin Regimens for Latent TB Infection Krista Powell, MD, MPH Co-Project Officer, National Surveillance for Severe Adverse Events Associated with LTBI Treatment Lead,
London, 1 June 2006 Product name: REMICADE Procedure number: Remicade-H-240-II-73-AR SCIENTIFIC DISCUSSION 1/8
 London, 1 June 2006 Product name: REMICADE Procedure number: Remicade-H-240-II-73-AR SCIENTIFIC DISCUSSION 1/8 1. Introduction Infliximab is a chimeric human-murine IgG1κ monoclonal antibody, which binds
London, 1 June 2006 Product name: REMICADE Procedure number: Remicade-H-240-II-73-AR SCIENTIFIC DISCUSSION 1/8 1. Introduction Infliximab is a chimeric human-murine IgG1κ monoclonal antibody, which binds
Orencia (abatacept) DRUG.00040
 Market DC Orencia (abatacept) DRUG.00040 Override(s) Prior Authorization Quantity Limit Approval Duration 1 year Medications Comments Quantity Limit Orencia (abatacept) - AGP, VA MCD only 4 vials per 28
Market DC Orencia (abatacept) DRUG.00040 Override(s) Prior Authorization Quantity Limit Approval Duration 1 year Medications Comments Quantity Limit Orencia (abatacept) - AGP, VA MCD only 4 vials per 28
Tuberculosis and Diabetes Mellitus. Lana Kay Tyer, RN MSN WA State Department of Health TB Nurse Consultant
 Tuberculosis and Diabetes Mellitus Lana Kay Tyer, RN MSN WA State Department of Health TB Nurse Consultant Learning Objectives Understand the impact of uncontrolled diabetes mellitus (DM) on TB infection
Tuberculosis and Diabetes Mellitus Lana Kay Tyer, RN MSN WA State Department of Health TB Nurse Consultant Learning Objectives Understand the impact of uncontrolled diabetes mellitus (DM) on TB infection
RHEUMATOID ARTHRITIS DRUGS
 Rheumatology Biologics Criteria from the Exceptional Access Program RHEUMATOID ARTHRITIS DRUGS DRUG NAME BRS REIMBURSED DOSAGE FORM/ STRENGTH Adalimumab Humira 40 mg/0.8 syringe and 40mg/0.8 pen for Anakinra
Rheumatology Biologics Criteria from the Exceptional Access Program RHEUMATOID ARTHRITIS DRUGS DRUG NAME BRS REIMBURSED DOSAGE FORM/ STRENGTH Adalimumab Humira 40 mg/0.8 syringe and 40mg/0.8 pen for Anakinra
Diagnosis and Medical Management of Latent TB Infection
 Diagnosis and Medical Management of Latent TB Infection Marsha Majors, RN September 7, 2017 TB Contact Investigation 101 September 6 7, 2017 Little Rock, AR EXCELLENCE EXPERTISE INNOVATION Marsha Majors,
Diagnosis and Medical Management of Latent TB Infection Marsha Majors, RN September 7, 2017 TB Contact Investigation 101 September 6 7, 2017 Little Rock, AR EXCELLENCE EXPERTISE INNOVATION Marsha Majors,
Pre-Treatment Evaluation. Treatment of Latent TB Infection (LTBI) Initiating Treatment: Patient Education. Before initiating treatment for LTBI:
 Pre-Treatment Evaluation Before initiating treatment for LTBI: Treatment of Latent TB Infection (LTBI) Amee Patrawalla, MD Associate Professor, New Jersey Medical School Attending Physician, NJMS Global
Pre-Treatment Evaluation Before initiating treatment for LTBI: Treatment of Latent TB Infection (LTBI) Amee Patrawalla, MD Associate Professor, New Jersey Medical School Attending Physician, NJMS Global
Mycobacterial diseases developed during anti-tumour necrosis factor-a therapy
 ORIGINAL ARTICLE PULMONARY INFECTIONS Mycobacterial diseases developed during anti-tumour necrosis factor-a therapy Jung-Wan Yoo 1, Kyung-Wook Jo 1, Bo-Hyung Kang 1, Mi Young Kim 2, Bin Yoo 3, Chang-Keun
ORIGINAL ARTICLE PULMONARY INFECTIONS Mycobacterial diseases developed during anti-tumour necrosis factor-a therapy Jung-Wan Yoo 1, Kyung-Wook Jo 1, Bo-Hyung Kang 1, Mi Young Kim 2, Bin Yoo 3, Chang-Keun
Isoniazid Preventive Therapy (IPT)
 Isoniazid Preventive Therapy (IPT) Josefina Cadorna-Carlos, M.D. Professor of Pediatrics U E R M M M C Objectives 1. Define IPT. 2. Discuss the indications for IPT. 3. Present RCT s for IPT (6H vs 9H).
Isoniazid Preventive Therapy (IPT) Josefina Cadorna-Carlos, M.D. Professor of Pediatrics U E R M M M C Objectives 1. Define IPT. 2. Discuss the indications for IPT. 3. Present RCT s for IPT (6H vs 9H).
Tuberculosis and TNF Inhibitors
 Tuberculosis and TNF Inhibitors Sundari Mase MD, MPH Medical Team Lead CDC/DTBE/FSEB January 18, 2011 Objectives Discuss the association between and epidemiology of TNF inhibitors and TB Discuss the challenges
Tuberculosis and TNF Inhibitors Sundari Mase MD, MPH Medical Team Lead CDC/DTBE/FSEB January 18, 2011 Objectives Discuss the association between and epidemiology of TNF inhibitors and TB Discuss the challenges
Delayed response to anti-tuberculosis treatment in a patient on infliximab
 Respiratory Medicine (2005) 99, 648 652 CASE REPORT Delayed response to anti-tuberculosis treatment in a patient on infliximab Elina Vlachaki a, Kostas Psathakis a,, Kostas Tsintiris a, Alexios Iliopoulos
Respiratory Medicine (2005) 99, 648 652 CASE REPORT Delayed response to anti-tuberculosis treatment in a patient on infliximab Elina Vlachaki a, Kostas Psathakis a,, Kostas Tsintiris a, Alexios Iliopoulos
6 ADRs, 2 LOE. 2 ADRs, 4 LOE. Ineffectiveness 24 ADRs 7, 1 pt for convenience. 48% had antibodies against Infliximab at baseline
 Summary of Published Switch data Table 1. Information Patients Switch from (n) Reason for switch Switch to: (n) Results Numbers Presse Med. 2002 (1) 14 Infliximab (8) (6) 6 ADRs, 2 LOE 2 ADRs, 4 LOE (8)
Summary of Published Switch data Table 1. Information Patients Switch from (n) Reason for switch Switch to: (n) Results Numbers Presse Med. 2002 (1) 14 Infliximab (8) (6) 6 ADRs, 2 LOE 2 ADRs, 4 LOE (8)
Pediatric Tuberculosis Lisa Y. Armitige, MD, PhD September 14, 2017
 Pediatric Tuberculosis Lisa Y. Armitige, MD, PhD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following disclosures
Pediatric Tuberculosis Lisa Y. Armitige, MD, PhD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following disclosures
(2) 83.3% b/w TST and T-SPOT, (2) 77.4% b/w TST and T-SPOT. 77.7% b/w TST and QFT-GIT. QFT-GIT, 22.2% in T-SPOT. TSPOT vs. TST (> 5 mm) vs.
 Supplementary Table 1. Study characteristics of the included literature Low to moderate TB endemic region Shovman et al. (2009) [21] Minguez et al. (2012) [16], type 35 RA 35 RA 53 Patients with s (RA
Supplementary Table 1. Study characteristics of the included literature Low to moderate TB endemic region Shovman et al. (2009) [21] Minguez et al. (2012) [16], type 35 RA 35 RA 53 Patients with s (RA
Targeted Tuberculin Testing and Treatment of Latent Tuberculosis Infection (LTBI) Lloyd Friedman, M.D. Milford Hospital Yale University
 Targeted Tuberculin Testing and Treatment of Latent Tuberculosis Infection (LTBI) Lloyd Friedman, M.D. Milford Hospital Yale University Tuberculosis Estimates USA World Infection 15,000,000 2,000,000,000
Targeted Tuberculin Testing and Treatment of Latent Tuberculosis Infection (LTBI) Lloyd Friedman, M.D. Milford Hospital Yale University Tuberculosis Estimates USA World Infection 15,000,000 2,000,000,000
Remicade. Remicade (infliximab), Inflectra (infliximab-dyyb) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.02 Subsection: Gastrointestinal nts Original Policy Date: May 20, 2011 Subject: Remicade Page: 1 of
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.50.02 Subsection: Gastrointestinal nts Original Policy Date: May 20, 2011 Subject: Remicade Page: 1 of
Abatacept (Orencia) for active rheumatoid arthritis. August 2009
 Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
C. Assess clinical response after the first three months of treatment.
 Government Health Plan (GHP) of Puerto Rico Authorization Criteria Tumor Necrosis Factor Alpha (TNFα) Adalimumab (Humira ) Managed by MCO Section I. Prior Authorization Criteria A. Physician must submit
Government Health Plan (GHP) of Puerto Rico Authorization Criteria Tumor Necrosis Factor Alpha (TNFα) Adalimumab (Humira ) Managed by MCO Section I. Prior Authorization Criteria A. Physician must submit
Latent tuberculosis (TB) infection (LTBI), a
 COMMENTARY Time for a change? Updated guidelines using interferon gamma release assays for detection of latent tuberculosis infection in the office setting Marisa Kardos, BS, and Alexa Boer Kimball, MD,
COMMENTARY Time for a change? Updated guidelines using interferon gamma release assays for detection of latent tuberculosis infection in the office setting Marisa Kardos, BS, and Alexa Boer Kimball, MD,
Diagnosis and Treatment of Tuberculosis, 2011
 Diagnosis of TB Diagnosis and Treatment of Tuberculosis, 2011 Alfred Lardizabal, MD NJMS Global Tuberculosis Institute Diagnosis of TB, 2011 Diagnosis follows Suspicion When should we Think TB? Who is
Diagnosis of TB Diagnosis and Treatment of Tuberculosis, 2011 Alfred Lardizabal, MD NJMS Global Tuberculosis Institute Diagnosis of TB, 2011 Diagnosis follows Suspicion When should we Think TB? Who is
has the following disclosures to make:
 CLINICAL DIAGNOSIS AND MANAGEMENT OF TB DISEASE Annie Kizilbash MD, MPH September 22, 2015 TB Nurse Case Management September 22 24, 2015 San Antonio. TX EXCELLENCE EXPERTISE INNOVATION Annie Kizilbash
CLINICAL DIAGNOSIS AND MANAGEMENT OF TB DISEASE Annie Kizilbash MD, MPH September 22, 2015 TB Nurse Case Management September 22 24, 2015 San Antonio. TX EXCELLENCE EXPERTISE INNOVATION Annie Kizilbash
Remicade (infliximab) DRUG.00002
 Applicability/Effective Date *- Florida Healthy Kids Remicade (infliximab) DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Approval Duration 1 year Comment Intravenous
Applicability/Effective Date *- Florida Healthy Kids Remicade (infliximab) DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Approval Duration 1 year Comment Intravenous
Latent TB Infection (LTBI)
 Latent TB Infection (LTBI) Diagnosis & Treatment of Latent TB Infection (LTBI) Amee Patrawalla MD MPH Assistant Professor UMDNJ-New Jersey Medical School Infection with Mycobacterium tuberculosis without
Latent TB Infection (LTBI) Diagnosis & Treatment of Latent TB Infection (LTBI) Amee Patrawalla MD MPH Assistant Professor UMDNJ-New Jersey Medical School Infection with Mycobacterium tuberculosis without
Infliximab/Infliximab-dyyb DRUG.00002
 Infliximab/Infliximab-dyyb DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Inflectra (inflectra-dyyb) Approval Duration 1 year Comment Intravenous administration
Infliximab/Infliximab-dyyb DRUG.00002 Override(s) Prior Authorization Step Therapy Medications Remicade (infliximab) Inflectra (inflectra-dyyb) Approval Duration 1 year Comment Intravenous administration
Remicade. Remicade (infliximab), Inflectra (infliximab-dyyb) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Remicade Page: 1 of 9 Last Review Date: June 22, 2017 Remicade Description Remicade (infliximab),
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Remicade Page: 1 of 9 Last Review Date: June 22, 2017 Remicade Description Remicade (infliximab),
Infections and Biologics
 Overview Infections and Biologics James Galloway What is the risk of infection with biologics? Are some patients at greater risk? Are some drugs safer? Case scenario You recently commenced Judith, a 54
Overview Infections and Biologics James Galloway What is the risk of infection with biologics? Are some patients at greater risk? Are some drugs safer? Case scenario You recently commenced Judith, a 54
8/11/2015. Febrile neutropenia Bone marrow transplant Immunosuppressant medications
 Dean Van Loo Pharm.D. Febrile neutropenia Bone marrow transplant Immunosuppressant medications Steroids Biologics Antineoplastic Most data from cancer chemotherapy Bone marrow suppression Fever is the
Dean Van Loo Pharm.D. Febrile neutropenia Bone marrow transplant Immunosuppressant medications Steroids Biologics Antineoplastic Most data from cancer chemotherapy Bone marrow suppression Fever is the
Evaluation and Management of the Patient with Latent Tuberculosis Infection (LTBI)
 Evaluation and Management of the Patient with Latent Tuberculosis Infection (LTBI) CURTIS FOWLER MPT,PA C ASSISTANT CLINICAL PROFESSOR UNIVERSITY OF THE PACIFIC Learning objectives Recognize the appropriate
Evaluation and Management of the Patient with Latent Tuberculosis Infection (LTBI) CURTIS FOWLER MPT,PA C ASSISTANT CLINICAL PROFESSOR UNIVERSITY OF THE PACIFIC Learning objectives Recognize the appropriate
Treatment of Tuberculosis
 TB Intensive Tyler, Texas June 1-3, 2009 Treatment of Tuberculosis Barbara Seaworth, MD June 3, 2009 Treatment of Tuberculosis Barbara J Seaworth MD Medical Director Heartland National TB Center 1 Purpose
TB Intensive Tyler, Texas June 1-3, 2009 Treatment of Tuberculosis Barbara Seaworth, MD June 3, 2009 Treatment of Tuberculosis Barbara J Seaworth MD Medical Director Heartland National TB Center 1 Purpose
Synoviocytes. Macrophage. B cell C H R O N I C. Neutrophil. Mast cell I N F L A M M A T I O N. Tissue cell. Endothelial cell. Th1/Th17 IL17 IL22
 DC IL12, IL23 chemokines, ECM, Co-stimulation IL17, IL22 IFNγ ± Macrophage peptidoglycan lipopolysaccharide heat shock proteins Th1/Th17 IL17 IL22 Cell contact, co-stimulation immune complexes acute phase
DC IL12, IL23 chemokines, ECM, Co-stimulation IL17, IL22 IFNγ ± Macrophage peptidoglycan lipopolysaccharide heat shock proteins Th1/Th17 IL17 IL22 Cell contact, co-stimulation immune complexes acute phase
Regulatory Status FDA-approved indication: Orencia is a selective T cell co-stimulation modulator indicated for: (1)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Orencia Page: 1 of 9 Last Review Date: September 20, 2018 Orencia Description Orencia (abatacept)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Orencia Page: 1 of 9 Last Review Date: September 20, 2018 Orencia Description Orencia (abatacept)
Sarcoidosis Case. Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA. WASOG: educational material
 Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Disclosures. TB and CoMorbidities Challenges and Opportunities. Burden of TB. Outline of the lecture. Target testing for TB Infection TB HIV 3/25/2012
 Disclosures TB and CoMorbidities Challenges and Opportunities E. Jane Carter, M.D. Associate Professor of Medicine Alpert School of Medicine, Brown University Providence, Rhode Island No financial disclosures
Disclosures TB and CoMorbidities Challenges and Opportunities E. Jane Carter, M.D. Associate Professor of Medicine Alpert School of Medicine, Brown University Providence, Rhode Island No financial disclosures
Communicable Disease Control Manual Chapter 4: Tuberculosis. Assessment and Follow-Up of TB Contacts
 Provincial TB Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 www.bccdc.ca Communicable Disease Control Manual Assessment and Follow-Up of TB July, 2018 Page 1 TABLE OF CONTENTS 8.0 ASSESSMENT AND
Provincial TB Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 www.bccdc.ca Communicable Disease Control Manual Assessment and Follow-Up of TB July, 2018 Page 1 TABLE OF CONTENTS 8.0 ASSESSMENT AND
Detection and Treatment of Tuberculosis in Correctional Facilities: Opportunities and Challenges
 Detection and Treatment of Tuberculosis in Correctional Facilities: Opportunities and Challenges David Karol, MD, MA Bureau of Prisons, FMC Butner Duke University Medical Center June 26, 2013 No Disclosures
Detection and Treatment of Tuberculosis in Correctional Facilities: Opportunities and Challenges David Karol, MD, MA Bureau of Prisons, FMC Butner Duke University Medical Center June 26, 2013 No Disclosures
Welcome to Rheumatology Highlights Report; I m Dr. Len Calabrese from the R.J. Fasenmyer Center for Clinical Immunology. And, in the next 15 minutes
 Welcome to Rheumatology Highlights Report; I m Dr. Len Calabrese from the R.J. Fasenmyer Center for Clinical Immunology. And, in the next 15 minutes I m going to update you on the safety of biologics.
Welcome to Rheumatology Highlights Report; I m Dr. Len Calabrese from the R.J. Fasenmyer Center for Clinical Immunology. And, in the next 15 minutes I m going to update you on the safety of biologics.
The Tip of the Iceberg: Addressing Latent Tuberculosis Infection to Accelerate Tuberculosis Elimination
 Four Corners TB and HIV Conference November 3, 2015 Durango, CO The Tip of the Iceberg: Addressing Latent Tuberculosis Infection to Accelerate Tuberculosis Elimination Philip LoBue, MD National Center
Four Corners TB and HIV Conference November 3, 2015 Durango, CO The Tip of the Iceberg: Addressing Latent Tuberculosis Infection to Accelerate Tuberculosis Elimination Philip LoBue, MD National Center
Management of Pediatric Tuberculosis in New Jersey
 Management of Pediatric Tuberculosis in New Jersey Helen Aguila, MD NJMS Global TB Institute December 15, 2011 This presentation is in part adapted from Pediatric Tuberculosis by Ann Loeffler, MD : Francis
Management of Pediatric Tuberculosis in New Jersey Helen Aguila, MD NJMS Global TB Institute December 15, 2011 This presentation is in part adapted from Pediatric Tuberculosis by Ann Loeffler, MD : Francis
Drug Therapy Guidelines
 Simponi, Simponi Aria Applicable Medical Benefit x Effective: 2/13/18 Pharmacy- Formulary 1 x Next Review: 12/18 Pharmacy- Formulary 2 x Date of Origin: 7/2010 Pharmacy- Formulary 3/Exclusive x Review
Simponi, Simponi Aria Applicable Medical Benefit x Effective: 2/13/18 Pharmacy- Formulary 1 x Next Review: 12/18 Pharmacy- Formulary 2 x Date of Origin: 7/2010 Pharmacy- Formulary 3/Exclusive x Review
Fundamentals of Tuberculosis (TB)
 TB in the United States Fundamentals of Tuberculosis (TB) From 1953 to 1984, reported cases decreased by approximately 5.6% each year From 1985 to 1992, reported cases increased by 20% 25,313 cases reported
TB in the United States Fundamentals of Tuberculosis (TB) From 1953 to 1984, reported cases decreased by approximately 5.6% each year From 1985 to 1992, reported cases increased by 20% 25,313 cases reported
TUBERCULOSIS. Pathogenesis and Transmission
 TUBERCULOSIS Pathogenesis and Transmission TUBERCULOSIS Pathogenesis and Transmission Infection to Disease Diagnostic & Isolation Updates Treatment Updates Pathogenesis Droplet nuclei of 5µm or less are
TUBERCULOSIS Pathogenesis and Transmission TUBERCULOSIS Pathogenesis and Transmission Infection to Disease Diagnostic & Isolation Updates Treatment Updates Pathogenesis Droplet nuclei of 5µm or less are
Background. The global burden of latent M. tuberculosis. More than 2 billion people infected
 What s New in Treatment tof LTBI Alfred Lardizabal, MD November 17, 2011 Washington, D.C. Background The global burden of latent M. tuberculosis infection is enormous More than 2 billion people infected
What s New in Treatment tof LTBI Alfred Lardizabal, MD November 17, 2011 Washington, D.C. Background The global burden of latent M. tuberculosis infection is enormous More than 2 billion people infected
