CASE REPORT. Abstract. Introduction
|
|
|
- Brooke Powell
- 5 years ago
- Views:
Transcription
1 CASE REPORT The Clinical Characteristics of Two Anti-OJ (Anti-IsoleucyltRNA Synthetase) Autoantibody-Positive Interstitial Lung Disease Patients with Polymyositis/Dermatomyositis Kei Kunimasa 1,8, Machiko Arita 1, Takashi Nakazawa 2, Maki Tanaka 1, Kazuya Tsubouchi 1,9, Satoshi Konishi 1,10, Yasushi Fukuda 1, Mika Saigusa 1,3, Hiroaki Nakagawa 1,4, Satoshi Ubukata 1,5, Yohei Korogi 1, Takao Fujii 6, Tsuneyo Mimori 7 and Tadashi Ishida 1 Abstract We herein report the clinical and laboratory characteristics of two anti-oj (anti-isoleucyl-trna synthetase) autoantibody-positive interstitial lung disease patients with polymyositis/dermatomyositis (PM/DM). We compared these characteristics with previously published findings. Previous reports and our present cases show that anti-oj autoantibody-positive interstitial lung disease (ILD) patients with PM/DM lack the manifestations of Raynaud s phenomenon and sclerodactyly and show good prognoses and responses to glucocorticoid therapy. These results indicate that the presence of anti-oj autoantibodies may be useful for predicting the prognosis of ILD and its clinical course in PM/DM patients. Key words: interstitial lung disease, polymyositis/dermatomyositis, anti-aminoacyl-trna antibodies (Intern Med 51: , 2012) () Introduction Anti-aminoacyl-tRNA synthetase (anti-ars) autoantibodies are generally found in patients with polymyositis (PM) and dermatomyositis (DM), particularly in those with associated interstitial lung disease (ILD) (1). Autoantibodies directed against aminoacyl-trna synthetases are found in approximately 25% to 35% of patients with PM and DM (2). ARS comprises a family of cytoplasmic enzymes that catalyze the formation of aminoacyl-trna from a specific amino acid and its cognate trna and play a crucial role in protein synthesis (3). Eight classes of autoantibodies that react with ARS have been recognized: anti-histidyl (anti-jo-1), anti-threonyl (anti-pl-7), anti-alanyl (anti-pl-12), antiglycyl (anti-ej), anti-isoleucyl (anti-oj), anti-asparaginyl (anti-ks), anti-phenylalanyl (anti-zo) and anti-tyrosyl-trna (anti-yrs) synthetases (4-6). Anti-Jo-1 antibodies were the first of these antibodies to be discovered and are detectable in approximately 20% to 30% of PM/DM patients (7). Anti- OJ antibodies appear to be associated with clinical manifestations that are generally similar to those of other antisynthetases, including myositis, ILD and Raynaud s phenomenon. In previous studies, anti-oj antibodies were found in fewer than 2% of all patients with PM/DM (8). Sato et al. (9) reported the clinical characteristics of seven Japanese patients with anti-oj autoantibodies. These patients lacked any manifestations of Raynaud s phenomenon or sclerodactyly and suffered from ILD associated with PM. This group showed that anti-oj antibodies are a clinically important Department of Respiratory Medicine, Kurashiki Central Hospital, Japan, Department of Endocrinology and Rheumatology, Kurashiki Central Hospital, Japan, Department of Palliative Medicine, Okayama Saiseikai General Hospital, Japan, Department of Respiratory Medicine, Shiga University of Medical Science, Japan, Department of Respiratory Diseases, Saka General Hospital, Japan, Department of the Control for Rheumatic Diseases, Graduate School of Medicine, Kyoto University, Japan, Department of Rheumatology and Clinical Immunology, Graduate School of Medicine, Kyoto University, Japan, Division of Genetics, Kobe University Graduate School of Medicine, Japan, Department of Respiratory Medicine, St. Mary s Hospital, Japan and Department of Respiratory Medicine, Graduate School of Medicine, Kyoto University, Japan Received for publication January 31, 2012; Accepted for publication September 10, 2012 Correspondence to Dr. Kei Kunimasa, keikunimasa@gmail.com 3405
2 Table 1. Laboratory and Radiological Data Patient number 1 2 CRP ( mg/dl) LDH ( IU/L) CK ( IU/L) ALD ( U/L) ANA cytoplasm pattern cytoplasm pattern Anti-SS-A Ab negative negative Anti-mitochondrial Ab negative negative Anti-OJ Ab positive positive KL-6 ( U/mL) 2, SP-D (<110.0 ng/ml) SP-A (<43.8 ng/ml) %VC %DLco electromyogram myogenic myogenic muscle biopsy not performed myositis BALF Recovery rate (%) Total cell coun Differential cell counts (%) Neutrophils 10 2 Lymphocytes Macrophages HRCT findings bilateral consolidation bilateral consolidation ground glass opacities ground glass opacities liner opacities traction bronchiectasis distribution lower lobe peribronchovascular lower lobe peribronchovascular and peripheral marker of a specific subset of anti-ars syndromes. However, there are still very few reports regarding the clinical characteristics of PM/DM patients with anti-oj autoantibodies; therefore, collecting cases to identify the clinical features is necessary. We herein present the clinical characteristics of two anti-oj autoantibody-positive ILD patients with PM/DM. Case 1 Case Reports Figure 1. Lower limb muscle MRI in three patients. Fatsuppressed T2-weighted imaging in Case 1 showing (A) diffuse, abnormally high signals in the bilateral quadriceps and in Case 2 showing (B) diffuse, abnormally high signals in the bilateral quadriceps. A 67-year-old woman was admitted to our hospital with a 2-month history of dry cough, slight fever and worsening dyspnea on exertion. She also complained of mild myalgia in both thighs. One month earlier, an abnormal chest roentgenogram was found, and she was referred to our hospital for extensive testing. She had a history of diabetes mellitus, which was treated with diet therapy, and carpal tunnel syndrome. She was on no medications. She had never smoked and had no history of alcohol use or pet ownership. She had a family history of diabetes mellitus and liver disease; however, she did not have a family history of connective tissue disease (CTD), rheumatic diseases, collagen vascular diseases or systemic autoimmune diseases. She lived with her husband in an old wooden house that had been standing for 40 years. A physical examination showed scaly erythema on the dorsum of the hands (Gottron s sign), mechanic s hand and spotty hemorrhages in some nail fold capillaries. Chest auscultation revealed fine crackles in the lower aspects of both lungs. On neurological examination, the patient s Manual Muscle Test (MMT) scores were 4 in the infraspinatus and iliopsoas muscles and 5 in the other muscles. The findings of other neurological assessments were normal, including those of the cranial nerves, sensory function and tendon reflexes. The laboratory findings and results of the pulmonary function tests are shown in Table 1. Magnetic resonance imaging (MRI) of the bilateral thighs showed diffuse, abnormally high T2-weighted imaging (T2WI) signals (Fig. 1A). Findings from needle electromyography of the right quadriceps indicated the presence of myogenic changes with concomitant active denervation. Chest X-ray and high-resolution computed tomography (HRCT) findings of the chest are shown in Figs. 2A, 3A, 3B. HRCT showed bilateral consolidation predominantly distributed along the bronchovascular bundles in both lower lobes and ground glass attenuation. Bronchoalveolar lavage (BAL) evaluation was performed (Table 1), which showed lymphocyte predominance. A Gram stain of the BAL fluid (BALF) was negative. It was difficult to perform a histopathological examination of the muscles or lungs due to deterioration of the patient s respiratory symptoms. These findings led us to diagnose the patient with interstitial pneumonia associated with DM. A fluorescent antinuclear antibody test was positive and showed a cytoplasmic pattern. An anti-jo-1 antibody test was negative; therefore, we assayed other anti-ars autoantibodies with an 3406
3 Intern Med 51: , 2012 Figure 2. Chest radiographs. Case 1: (A) bilateral consolidation and ground glass attenuation with volume loss in both lower lobes; Case 2: (B) bilateral consolidation and ground glass attenuation with volume loss in both lower lobes. Figure 3. High-resolution chest CT scans. Case 1: (A, B) bilateral consolidation predominantly distributed along the bronchovascular bundles with volume loss in both lower lobes and areas of ground glass attenuation and liner opacities; Case 2: (C, D) bilateral consolidation predominantly distributed in peripheral areas with volume loss in both lower lobes and areas of ground glass attenuation, intralobular reticular opacities and traction bronchiectasis. RNA immunoprecipitation assay and found that the anti-oj antibody test was positive. The patient was treated with high-dose methylprednisolone (1 g/day intravenously for three days) followed by oral prednisolone (1 mg/kg/day) and cyclosporine (5 mg/kg/day). Her clinical condition and chest radiography findings showed remarkable improvements after 12 months of treatment. Case 2 A 74-year-old man was admitted to our hospital with a 1month history of fever, fatigue and worsening dyspnea on exertion. Two weeks prior to admission, he noticed a pro- 3407
4 Table 2. Clinical Characteristics Patient number 1 2 Gender female male Age Diagnosis DM PM initial symptoms cough + + dyspnea + + arthritis - - weight loss - - muscle weakness + - fever - + myositis + + Rash + - Raynaud's phenomenon - - abnormal capillaries of nail folds micro hemorrhage + + enlarged capillary - - sicca - - mechanic's hand + - Gottron sign (+) treatment PSL pulse 1.0mg/kg PSL 1.0mg/kg CyA effect Improved Improved ductive cough and was seen at the nearest clinic. He was diagnosed with bronchitis and treated with levofloxacin and a combination cold remedy. However, his clinical condition did not improve and instead gradually deteriorated. Therefore, he was referred to our hospital for extensive testing. He had a history of atrial fibrillation, mitral regurgitation, mitral stenosis and diabetes mellitus and had been hospitalized seven years earlier for approximately three months with infectious endocarditis caused by Group A Streptococcus. His medications included metildigoxin, fulosemide, warfarin, amlodipine, candesartan and glimepiride. He had never smoked and had no history of alcohol use or pet ownership. He had no family history of collagen or muscle disease. On physical examination, he was found to have cornification, but no erythema, spread in a symmetric fashion over the metacarpophalangeal joints along with spotty hemorrhages in some nail fold capillaries; however, no muscle weakness was observed. Cardiac auscultation revealed a systolic murmur (Levine III/VI), and chest auscultation showed fine crackles in the lower aspects of both lungs. On neurological examination, the MMT scores were full in all muscles. The findings of other neurological assessments were normal. The laboratory findings and results of the pulmonary function tests are shown in Table 1. Although the patient did not show any muscle symptoms, an MRI study of the bilateral thighs showed diffuse, abnormally high T2-WI signals (Fig. 1B). Findings from needle electromyography of the right quadriceps indicated the presence of myogenic changes with concomitant active denervation, and a muscle biopsy of the left quadriceps revealed myositis. The findings of chest X-ray and HRCT of the chest are shown in Figs. 2B, 3C, 3D. HRCT showed bilateral consolidation predominantly distributed along the bronchovascular bundles in both lower lobes and ground glass attenuation with traction bronchiectasis. A BAL analysis was performed (Table 1), which showed lymphocyte predominance. These findings led us to diagnose the patient with interstitial pneumonia associated with PM. Later, an anti-oj antibody test was shown to be positive. The patient was treated with oral prednisolone (1 mg/kg/day). His clinical condition and chest radiography findings showed remarkable improvements, and no deteriorations were observed over a 3-year treatment period. Discussion Previous studies have indicated that ILD is associated with high mortality in PM/DM patients. ILD occurs in as many as 53% of PM/DM patients (10) and may lead to life threatening complications, including ventilator failure and secondary pulmonary hypertension (11). Anti-ARS antibodies are directed against cytoplasmic enzymes that catalyze the formation of the aminoacyl-trna complex from an amino acid and its cognate trna (3). Marguerie et al. (12) described a series of 29 PM/DM patients with anti-ars antibodies who were more likely to have fevers, dyspnea, mechanic s hands, arthritis and ILD than those without such antibodies. Yoshifuji et al. (10) stratified 74 PM/DM patients into anti-ars-positive (including two anti-oj-positive patients) and -negative groups and found that ILD and mechanic s hand occurred significantly more frequently in the anti-ars-positive group. To date, eight antisynthetase antibodies have been identified, and anti-jo1, anti-pl7 and anti-pl12 antibodies are the strongest markers for ILD; anti-jo1 antibodies are the most common (13, 14). Anti-OJ autoantibodies are a type of anti- ARS antibodies originally identified after the original sera from patient OJ showed significant inhibition of isoleucyltrna synthetase activity (15). To the best of our knowledge, two reports have been published regarding the clinical significance of anti-oj autoantibodies in ILD patients with PM/DM (9, 16). Additionally, there are seven reports describing the clinical significance of anti-oj autoantibodies (9, 10, 16-20). Sato et al. (9) screened 1,135 Japanese patients who had or were suspected of having CTDs and detected seven patients positive for anti-oj autoantibodies (four with PM, three with IIPs), all of whom had ILD. These results suggested that the presence of anti-oj autoantibodies is more closely associated with ILD than myositis. Targoff et al. (16) reported the cases of six anti-oj autoantibody-positive PM/DM patients with ILD; however, he did not describe the details of these cases, including the symptoms observed on first visit and the responsiveness to the therapy. The characteristics of our present two patients are summarized in Table 2, and previous reports and our cases are summarized together in Table 3. Yoshifuji et al. (10) reported that, in anti-ars autoantibody-positive PM/DM patients, the development of ILD often precedes that of myopathy. Our patients experienced respiratory symptoms that preceded the development of other symp- 3408
5 Table 3. Literature Review and Our Cases Sato et al. 9 Targoff et al. 16 Friedman et al. 20 other reports our cases Total No patients Age at onset, mean±s.d. years 53±18 52±13 36, 50 54±8 67, 74 53±11 No male/no. female 3/4 4/5 1/1 0/3 1/1 9/14 Dignosis PM/DM with ILD 3/7 6/9 0/2 0/3 2/2 11/23(47.8%) PM,RA with ILD 1/7 0/9 0/2 0/3 0/2 1/23(4.3%) IIPs 3/7 3/9 2/2 3/3 0/2 11/23(47.8%) fever 3/7 NA 0/2 0/3 1/2 4/14(2.9%) ILD 7/7 8/9 2/2 3/3 2/2 22/23(95.7%) arthritis 4/7 6/7* 1/2 2/3 0/2 13/21(61.9%) Raynaud's phenomenon 0/7 1/7* 0/2 1/3 0/2 2/21(9.5%) myositis 4/7 8/9 0/2 1/3 2/2 15/23(65.2%) PM: polymtositis, DM: dermatomyositis, RA: rheumatoid arthritis, IIPs: idiopathic intestitial pneumonias * a part of data were not available. NA, data not a vailable The diagnosis of IIPs (idiopathic interstitial pneumonias) was based on consensus classification of IIPs. 10 toms. On physical examination, neither sclerodactyly, Raynaud s phenomenon nor sicca were found in either patient. Although Raynaud s phenomenon is often associated with the presence of anti-jo-1 antibodies, it may not occur in patients with anti-oj antibodies (Table 3). The response of ILD to glucocorticoid therapy is significantly better in anti-ars positive PM/DM patients than in anti-ars negative patients. Three of the four anti-oj autoantibody-positive ILD patients with PM reported by Sato et al. also responded to glucocorticoid therapy. Both of our patients also showed good clinical responses following treatment with high-dose glucocorticoids without immunosuppressants. There may be a tendency for ILD patients with anti-oj autoantibodies to show good prognoses and good responses to glucocorticoid monotherapy. Although ILD has a tendency to recur in anti-ars autoantibodypositive patients (10), in both of the present cases, the ILD remained static since the first treatment. Performing a histopathological analysis of ILD is often difficult in patients with clinical symptoms due to the risk of deterioration. Although histopathological analyses could not be performed in the present cases, the CT findings suggested a diagnosis of ILD. To the best of our knowledge, there have been few detailed reports regarding the chest CT findings of ILD in PM/DM patients with anti-oj autoantibodies. Both of our cases showed similar findings on chest HRCT, including bilateral consolidation and ground glass attenuation with volume loss in the lower lobes and peribronchovascular predominance. Koreeda et al. (17) reported the chest HRCT findings of one anti-oj autoantibody-positive ILD patient without PM/DM, which included bilateral ground glass opacities, consolidations volume loss in the lung bases and peribronchovascular predominance. These reported findings are similar to the HRCT findings observed in our patients. Such findings may be associated with the presence of anti-oj autoantibodies. As described above, there are no reports regarding the detailed radiological and histopathological findings of ILD in PM/DM patients with anti-oj autoantibodies; however, some reports have described the details of radiological and histopathological analyses of idiopathic interstitial pneumonia (IIPs) patients with anti-oj autoantibodies. The results of a previous histopathological analysis of six IIP patients with anti-oj autoantibodies (9, 16-18) revealed an NSIP pattern in two of the six patients, a cryptogenic organizing pneumonia pattern in two patients, an UIP pattern in one patient and no diagnosis in one patient. Unfortunately, in our series, we could not perform video-assisted thoracoscopic surgery (VATS) due to a deterioration of respiratory symptoms. However, the chest HRCT findings were not typical of IPF/ UIP, as in previous reports. The histopathological analysis described above may indicate good responses to steroid therapy in ILD patients with anti-oj autoantibodies (21). Our results and those of previous reports suggest that anti-oj autoantibody-positive PM/DM patients with ILD exhibit distinct features compared to ILD patients with other anti-ars antibodies. The course of ILD in such patients may show a good response to glucocorticoid therapy and be associated with a good prognosis, as in other anti-ars antibody-positive patients (10). Lymphocyte-predominant BAL and HRCT findings of bilateral consolidation predominantly distributed along the bronchovascular bundles in both lower lobes and areas with ground glass attenuation and linear opacities may be clinical features of anti-oj autoantibody-positive PM/DM patients with ILD. In such patients, ILD has a tendency to follow a subacute pattern and not become a chronic disease. Although anti-oj autoantibody screening tests are not available, except in some research institutes, testing for anti-oj autoantibodies is very important clinically because it may distinguish subtypes of both PM/DM and anti-ars syndromes and predict a patient s prognosis. The clinical properties of ILD patients with PM/DM may be classified according to the presence or absence of anti-oj autoantibodies. Further accumulation and analysis should be conducted to clarify whether anti-ars autoantibodies truly affect the prognoses of ILD patients 3409
6 with PM/DM and distinguish between the differences observed among types of anti-ars autoantibody-positive ILD. Author s disclosure of potential Conflicts of Interest (COI). Ishida T: Honoraria, Abott, Taisyo-Toyama and Daiichi-Sankyo. References 1. Targoff IN. Immune manifestations of inflammatory muscle disease. Rheum Dis Clin North Am 20: , Hirakata M, Nagai S. Interstitial lung disease in polymyositis and dermatomyositis. Curr Opin Rheumatol 12: , Mathews M, Berstein R. Myositis auto-antibodies inhibits histidyltrna synthetase: a model for auto-immunity. Nature 83: , Hirakata M, Suwa A, Nagai S, et al. Anti-KS: identification of autoantibodies to asparaginyl-transfer RNA synthetase associated with interstitial lung disease. J Immunol 162: , Betteridge Z, Gunawardena H, North J, Slinn J, McHugh N. Antisynthetase syndrome: a new autoantibody to phenylalanyl transfer RNA synthetase (anti-zo) associated with polymyositis and interstitial pneumonia. Rheumatology 46: , Katzap E, Barilla-LaBarca ML, Marder G. Antisynthetase syndrome. Curr Rheumatol Rep 13: , Love LA, Leff RL, Fraser DD, et al. A new approach to the classification of idiopathic inflammatory myopathy: myositis-specific autoantibodies define useful homogeneous patient groups. Medicine 70: , Suwa A, Hirakata M, Satoh S, Ezaki T, Mimori T, Inada S. A case of polymyositis with anti-oj (isoleucyl-transfer RNA synthetase) antibodies. Clin Exp Rheumatol 17: , Sato S, Kuwana M, Hirakata M. Clinical characteristics of Japanese patients with anti-oj (anti-isoleucyl-trna synthetase) autoantibodies. Rheumatology 46: , Yoshifuji H, Fujii T, Kobayashi S, et al. Anti-aminoacyl-tRNA synthetase antibodies in clinical course prediction of interstitial lung disease complicated with idiopathic inflammatory myopathies. Autoimmunity 39: , Marie I, Hatron PY, Dominique S, et al. Short-term and long-term outcomes of interstitial lung disease in polymyositis and dermatomyositis: a series of 107 patients. Arthritis Rheum 63: , Marguerie C, Bunn CC, Beynon HL, et al. Polymyositis, pulmonary fibrosis and autoantibodies to aminoacyl-trna synthetase enzymes. Q J Med 77: , Kang EH, Lee EB, Shin KC, et al. Interstitial lung disease in patients with polymyositis, dermatomyositis and amyopathic dermatomyositis. Rheumatology 44: , Connors GR, Christopher-Stine L, Oddis CV, Danoff SK. Interstitial lung disease associated with the idiopathic inflammatory myopathies: what progress has been made in the past 35 years? Chest 138: , Targoff IN. Autoantibodies to aminoacyl-tranfer RNA synthetases for isoleucine and glycine. Two additional synthetases are antigenic in myositis. J Immunol 144: , Targoff IN, Trieu EP, Miller FW. Reaction of anti-oj autoantibodies with components of the multi-enzyme complex of aminoacyltrna synthetases in addition to isoleucyl-trna synthetase. J Clin Invest 91: , Koreeda Y, Higashimoto I, Yamamoto M, et al. Clinical and pathological findings of interstitial lung disease patients with antiaminoacyl-trna synthetase autoantibodies. Intern Med 49: , Shimizu K, Tai H, Kuwano K. A case of cellular NSIP with anti- OJ (anti-isoleucyl trna synthetase) antibodies. Nihon Kokyuki Gakkai Zasshi 48: 45-48, Gelpí C, Kanterewicz E, Gratacos J, Targoff IN, Rodríguez- Sánchez JL. Coexistence of two antisynthetases in a patient with the antisynthetase syndrome. Arthritis Rheum 39: , Friedman AW, Targoff IN, Arnett FC. Interstitial lung disease with autoantibodies against aminoacyl-trna synthetases in the absence of clinically apparent myositis. Semin Arthritis Rheum 26: , Flaherty KR, Toews GB, Travis WD, et al. Clinical significance of histological classification of idiopathic interstitial pneumonia. Eur Respir J 19: , The Japanese Society of Internal Medicine
Clinical and Pathological Findings of Interstitial Lung Disease Patients with Anti-Aminoacyl-tRNA Synthetase Autoantibodies
 ORIGINAL ARTICLE Clinical and Pathological Findings of Interstitial Lung Disease Patients with Anti-Aminoacyl-tRNA Synthetase Autoantibodies Yoshimizu Koreeda 1, Ikkou Higashimoto 1, Masuki Yamamoto 1,
ORIGINAL ARTICLE Clinical and Pathological Findings of Interstitial Lung Disease Patients with Anti-Aminoacyl-tRNA Synthetase Autoantibodies Yoshimizu Koreeda 1, Ikkou Higashimoto 1, Masuki Yamamoto 1,
Citation Clinical rheumatology (2011), 30(3)
 A case of antisynthetase syndrome i Titlepatient with anti-pl-12 antibody fo etanercept. Ishikawa, Yuki; Yukawa, Naoichiro; Author(s) Ohmura, Koichiro; Fujii, Takao; Usu Tsuneyo Citation Clinical rheumatology
A case of antisynthetase syndrome i Titlepatient with anti-pl-12 antibody fo etanercept. Ishikawa, Yuki; Yukawa, Naoichiro; Author(s) Ohmura, Koichiro; Fujii, Takao; Usu Tsuneyo Citation Clinical rheumatology
PL-7 and Anti-Jo-1 Antibodies. publication is available at link.sp
 NAOSITE: Nagasaki University's Ac Title Author(s) Comparison of Pulmonary Involvement PL-7 and Anti-Jo-1 Antibodies Tomonaga, Masaomi; Sakamoto, Noriho Tomoyuki; Harada, Tatsuhiko; Nakash Shintaro; Horai,
NAOSITE: Nagasaki University's Ac Title Author(s) Comparison of Pulmonary Involvement PL-7 and Anti-Jo-1 Antibodies Tomonaga, Masaomi; Sakamoto, Noriho Tomoyuki; Harada, Tatsuhiko; Nakash Shintaro; Horai,
CASE REPORT. Introduction. Case Report
 doi: 10.2169/internalmedicine.9553-17 http://internmed.jp CASE REPORT Successful Treatment of Rapidly Progressive Unclassifiable Idiopathic Interstitial Pneumonia with Anti-melanoma Differentiation-associated
doi: 10.2169/internalmedicine.9553-17 http://internmed.jp CASE REPORT Successful Treatment of Rapidly Progressive Unclassifiable Idiopathic Interstitial Pneumonia with Anti-melanoma Differentiation-associated
The Onset of Eosinophilic Pneumonia Preceding Anti-synthetase Syndrome
 doi: 10.2169/internalmedicine.8955-17 http://internmed.jp CASE REPORT The Onset of Eosinophilic Pneumonia Preceding Anti-synthetase Syndrome Yoshimasa Hachisu 1, Yasuhiko Koga 1, Noriaki Sunaga 1,2, Chiharu
doi: 10.2169/internalmedicine.8955-17 http://internmed.jp CASE REPORT The Onset of Eosinophilic Pneumonia Preceding Anti-synthetase Syndrome Yoshimasa Hachisu 1, Yasuhiko Koga 1, Noriaki Sunaga 1,2, Chiharu
Overview of Diagnostic Autoantibodies in Inflammatory Myopathy
 Overview of Diagnostic Autoantibodies in Inflammatory Myopathy Minoru Satoh, M.D., Ph.D. Research Associate Professor of Medicine Division of Rheumatology and Clinical Immunology University of Florida
Overview of Diagnostic Autoantibodies in Inflammatory Myopathy Minoru Satoh, M.D., Ph.D. Research Associate Professor of Medicine Division of Rheumatology and Clinical Immunology University of Florida
CTD-related Lung Disease
 13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
Clinical features of seven Japanese patients with anti-pl- antibody frequent positivity for anti-cyclic citrullinated peptide antibody
 Cace report Clinical features of seven Japanese patients with anti-pl- antibody frequent positivity for anti-cyclic citrullinated peptide antibody Yoichiro Akiyama 1, Takao Nagashima 1, Masahiro Iwamoto
Cace report Clinical features of seven Japanese patients with anti-pl- antibody frequent positivity for anti-cyclic citrullinated peptide antibody Yoichiro Akiyama 1, Takao Nagashima 1, Masahiro Iwamoto
Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan
 CASE REPORT Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan Kenichiro Tokunaga 1 and Noboru Hagino 2 Abstract We performed a retrospective
CASE REPORT Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan Kenichiro Tokunaga 1 and Noboru Hagino 2 Abstract We performed a retrospective
Clinical characteristics of Japanese patients with anti-pl-7 (anti-threonyl-trna synthetase) autoantibodies
 Clinical characteristics of Japanese patients with anti-pl-7 (anti-threonyl-trna synthetase) autoantibodies S. Sato 1, M. Hirakata 1, M. Kuwana 2, K. Nakamura 1, A. Suwa 1, S. Inada 3, T. Mimori 4, Y.
Clinical characteristics of Japanese patients with anti-pl-7 (anti-threonyl-trna synthetase) autoantibodies S. Sato 1, M. Hirakata 1, M. Kuwana 2, K. Nakamura 1, A. Suwa 1, S. Inada 3, T. Mimori 4, Y.
Acute Respiratory Distress Syndrome as the Initial Clinical Manifestation of an Antisynthetase Syndrome
 CASE REPORT http://dx.doi.org/10.4046/trd.2016.79.3.188 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:188-192 Acute Respiratory Distress Syndrome as the Initial Clinical Manifestation
CASE REPORT http://dx.doi.org/10.4046/trd.2016.79.3.188 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:188-192 Acute Respiratory Distress Syndrome as the Initial Clinical Manifestation
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Autoantibodies in the Idiopathic Inflammatory Myopathies
 Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Autoantibodies andprognosis. Jiří Vencovský Institute of Rheumatology, Prague, Czech Republic
 Autoantibodies andprognosis Jiří Vencovský Institute of Rheumatology, Prague, Czech Republic HeterogeneityofIIMs Diagnosis Polymyositis Dermatomyositis IBM Necrotising myopathy Paraneoplastic Amyopathic
Autoantibodies andprognosis Jiří Vencovský Institute of Rheumatology, Prague, Czech Republic HeterogeneityofIIMs Diagnosis Polymyositis Dermatomyositis IBM Necrotising myopathy Paraneoplastic Amyopathic
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Autoantibodies to a 140-kd Polypeptide, CADM-140, in Japanese Patients With Clinically Amyopathic Dermatomyositis
 ARTHRITIS & RHEUMATISM Vol. 52, No. 5, May 2005, pp 1571 1576 DOI 10.1002/art.21023 2005, American College of Rheumatology Autoantibodies to a 140-kd Polypeptide, CADM-140, in Japanese Patients With Clinically
ARTHRITIS & RHEUMATISM Vol. 52, No. 5, May 2005, pp 1571 1576 DOI 10.1002/art.21023 2005, American College of Rheumatology Autoantibodies to a 140-kd Polypeptide, CADM-140, in Japanese Patients With Clinically
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
Significance of antibody testing in idiopathic inflammatory myopathies
 2/0/20 Significance of antibody testing in idiopathic inflammatory myopathies Jiří Vencovský Institute of Rheumatology, Prague Diagnosis Polymyositis Juvenile DM (JPM) Paraneoplastic Myositis in overlap
2/0/20 Significance of antibody testing in idiopathic inflammatory myopathies Jiří Vencovský Institute of Rheumatology, Prague Diagnosis Polymyositis Juvenile DM (JPM) Paraneoplastic Myositis in overlap
Disclosures. Clinical Approach: Evaluating CTD-ILD for the pulmonologist. ILD in CTD. connective tissue disease or collagen vascular disease
 Disclosures Clinical Approach: Evaluating CTD-ILD for the pulmonologist Industry relationships: Actelion, atyr Pharma, Boehringer-Ingelheim, Genentech- Roche, Gilead Aryeh Fischer, MD Associate Professor
Disclosures Clinical Approach: Evaluating CTD-ILD for the pulmonologist Industry relationships: Actelion, atyr Pharma, Boehringer-Ingelheim, Genentech- Roche, Gilead Aryeh Fischer, MD Associate Professor
myopathy and interstitial lung dise
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case of primary Sjögren's syndrom myopathy and interstitial lung dise Koga, Tomohiro; Kouhisa, Yukiko; Na Akinari; Motomura, Masakatsu; Kawak
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case of primary Sjögren's syndrom myopathy and interstitial lung dise Koga, Tomohiro; Kouhisa, Yukiko; Na Akinari; Motomura, Masakatsu; Kawak
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
A Review of Interstitial Lung Diseases. Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco
 A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION!
 UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION! STÉPHANE JOUNEAU 11 JULY 2014 Respiratory Medicine Department, Pontchaillou Hospital, Rennes, France CASE OVERVIEW This case highlights how a usual
UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION! STÉPHANE JOUNEAU 11 JULY 2014 Respiratory Medicine Department, Pontchaillou Hospital, Rennes, France CASE OVERVIEW This case highlights how a usual
Clinical significance of serum surfactant protein D (SP-D) in patients with polymyositisudermatomyositis: correlation with interstitial lung disease
 Rheumatology 2002;41:1268 1272 Clinical significance of serum surfactant protein D (SP-D) in patients with polymyositisudermatomyositis: correlation with interstitial lung disease H. Ihn, Y. Asano, M.
Rheumatology 2002;41:1268 1272 Clinical significance of serum surfactant protein D (SP-D) in patients with polymyositisudermatomyositis: correlation with interstitial lung disease H. Ihn, Y. Asano, M.
Anti-synthetase syndrome
 Anti-synthetase syndrome Floranne C. Ernste, M.D. The Myositis Association Annual Conference Louisville, KY September 7, 2018 2017 MFMER slide-1 Disclosures Octapharma: clinical trial support Genentech:
Anti-synthetase syndrome Floranne C. Ernste, M.D. The Myositis Association Annual Conference Louisville, KY September 7, 2018 2017 MFMER slide-1 Disclosures Octapharma: clinical trial support Genentech:
Outline Definition of Terms: Lexicon. Traction Bronchiectasis
 HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
A Review of Interstitial Lung Diseases
 Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates
 Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
IPF: Epidemiologia e stato dell arte
 IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
Clinical Features of Anti-MDA5 Antibody-positive Rapidly Progressive Interstitial Lung Disease without Signs of Dermatomyositis
 doi: 10.2169/internalmedicine.1516-18 http://internmed.jp CASE REPORT Clinical Features of Anti-MDA5 Antibody-positive Rapidly Progressive Interstitial Lung Disease without Signs of Dermatomyositis Noriho
doi: 10.2169/internalmedicine.1516-18 http://internmed.jp CASE REPORT Clinical Features of Anti-MDA5 Antibody-positive Rapidly Progressive Interstitial Lung Disease without Signs of Dermatomyositis Noriho
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Autoantibodies in Idiopathic Inflammatory Myopathies. Vidya Limaye Rheumatology Department Royal Adelaide Hospital
 Autoantibodies in Idiopathic Inflammatory Myopathies Vidya Limaye Rheumatology Department Royal Adelaide Hospital Idiopathic Inflammatory Myopathies (IIM) Heterogeneous group of systemic autoimmune syndromes
Autoantibodies in Idiopathic Inflammatory Myopathies Vidya Limaye Rheumatology Department Royal Adelaide Hospital Idiopathic Inflammatory Myopathies (IIM) Heterogeneous group of systemic autoimmune syndromes
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Interstitial lung diseases associated with amyopathic dermatomyositis
 Eur Respir J 2006; 28: 1005 1012 DOI: 10.1183/09031936.06.00038806 CopyrightßERS Journals Ltd 2006 Interstitial lung diseases associated with amyopathic dermatomyositis T. Suda*, T. Fujisawa*, N. Enomoto*,
Eur Respir J 2006; 28: 1005 1012 DOI: 10.1183/09031936.06.00038806 CopyrightßERS Journals Ltd 2006 Interstitial lung diseases associated with amyopathic dermatomyositis T. Suda*, T. Fujisawa*, N. Enomoto*,
Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18
![Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18 Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18](/thumbs/95/125595183.jpg) Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Rheumatoid Factor
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Rheumatoid Factor
Overview of Idiopathic Pulmonary Fibrosis: Diagnosis and Therapy
 Overview of Idiopathic Pulmonary Fibrosis: Diagnosis and Therapy Jeff Swigris, DO, MS Director, ILD Program National Jewish Health Disclosures Speaker - Boehringer Ingelheim and Genentech Objectives Describe
Overview of Idiopathic Pulmonary Fibrosis: Diagnosis and Therapy Jeff Swigris, DO, MS Director, ILD Program National Jewish Health Disclosures Speaker - Boehringer Ingelheim and Genentech Objectives Describe
Clinical Study A Clinical Analysis of Risk Factors for Interstitial Lung Disease in Patients with Idiopathic Inflammatory Myopathy
 Clinical and Developmental Immunology Volume 2013, Article ID 648570, 4 pages http://dx.doi.org/10.1155/2013/648570 Clinical Study A Clinical Analysis of Risk Factors for Interstitial Lung Disease in Patients
Clinical and Developmental Immunology Volume 2013, Article ID 648570, 4 pages http://dx.doi.org/10.1155/2013/648570 Clinical Study A Clinical Analysis of Risk Factors for Interstitial Lung Disease in Patients
Progress in Idiopathic Pulmonary Fibrosis
 Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
dermatomyositis: report of a case.
 Living-donor lobar lung transplanta Titleinterstitial pneumonia associated w dermatomyositis: report of a case., Tsuyoshi; Bando, Toru; Fujin Author(s) Fengshi; Sasano, Hajime; Yukawa, Na Tsuneyo; Date,
Living-donor lobar lung transplanta Titleinterstitial pneumonia associated w dermatomyositis: report of a case., Tsuyoshi; Bando, Toru; Fujin Author(s) Fengshi; Sasano, Hajime; Yukawa, Na Tsuneyo; Date,
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Key words: CT scanners; interstitial lung diseases; polymyositis-dermatomyositis; x-ray
 Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment
 Prague, June 2014 Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
Prague, June 2014 Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases
 CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
Atlas of Antinuclear Antibodies
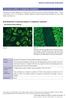 Fluorescence patterns of cytoplasmic autoantigens There are many important organelles in the cytoplasm which fulfill various functions of the cell as described in section 1. Various autoantibodies, known
Fluorescence patterns of cytoplasmic autoantigens There are many important organelles in the cytoplasm which fulfill various functions of the cell as described in section 1. Various autoantibodies, known
Liebow and Carrington's original classification of IIP
 Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Rapidly Progressive Pulmonary Fibrosis Following the Onset of Diffuse Alveolar Hemorrhage in Sjögren s Syndrome: An Autopsy Case Report
 CASE REPORT Rapidly Progressive Pulmonary Fibrosis Following the Onset of Diffuse Alveolar Hemorrhage in Sjögren s Syndrome: An Autopsy Case Report Yusuke Tomita 1,2, Shunsuke Mori 3, Nobuyuki Arima 4,
CASE REPORT Rapidly Progressive Pulmonary Fibrosis Following the Onset of Diffuse Alveolar Hemorrhage in Sjögren s Syndrome: An Autopsy Case Report Yusuke Tomita 1,2, Shunsuke Mori 3, Nobuyuki Arima 4,
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
Comparison of clinical course of polymyositis and dermatomyositis :a follow-up study in Tokushima University
 9 ORIGINAL Comparison of clinical course of polymyositis and dermatomyositis :a follow-up study in Tokushima University Hospital Kenji Tani, Reiko Tomioka,KeikoSato, Chiyuki Furukawa, Takeshi Nakajima,
9 ORIGINAL Comparison of clinical course of polymyositis and dermatomyositis :a follow-up study in Tokushima University Hospital Kenji Tani, Reiko Tomioka,KeikoSato, Chiyuki Furukawa, Takeshi Nakajima,
What your autoantibodies tell us about your disease. Mark Gourley, MD
 What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
CASE REPORT JOURNAL OF MEDICAL. Ellen De Langhe 1*, Jan Lenaerts 1, Xavier Bossuyt 2, Rene Westhovens 1 and Wim A Wuyts 3
 De Langhe et al. Journal of Medical Case Reports (2015) 9:82 DOI 10.1186/s13256-015-0571-2 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Mechanic s hands in a woman with undifferentiated connective
De Langhe et al. Journal of Medical Case Reports (2015) 9:82 DOI 10.1186/s13256-015-0571-2 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Mechanic s hands in a woman with undifferentiated connective
The many faces of myositis. Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands
 The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
Clinical and pathophysiological significance of myositis-specific and myositis-associated autoantibodies
 CME Review Clinical and pathophysiological significance of myositis-specific and myositis-associated autoantibodies Autoantibodies to various cellular constituents are detected in the sera of patients
CME Review Clinical and pathophysiological significance of myositis-specific and myositis-associated autoantibodies Autoantibodies to various cellular constituents are detected in the sera of patients
Test Name Results Units Bio. Ref. Interval
 LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines
 Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
IPF - Inquadramento clinico
 IPF - Inquadramento clinico Sergio Harari Unità Operativa di Pneumologia UTIR Servizio di Fisiopat. Resp. e Emodinamica Polmonare Ospedale S. Giuseppe, Milano Clinical Classification Diffuse parenchimal
IPF - Inquadramento clinico Sergio Harari Unità Operativa di Pneumologia UTIR Servizio di Fisiopat. Resp. e Emodinamica Polmonare Ospedale S. Giuseppe, Milano Clinical Classification Diffuse parenchimal
Faculty of Medicine, Titu Maiorescu University, Bucharest, Romania b. Dr. Ion Stoia Clinical Center for Rheumatic Diseases, Bucharest, Romania c
 Mædica - a Journal of Clinical Medicine MAEDICA a Journal of Clinical Medicine 2016; 11(6): 130-135 STATE OF THE ART New Insights into Antisynthetase Syndrome Manole COJOCARU a,b ; Inimioara Mihaela COJOCARU
Mædica - a Journal of Clinical Medicine MAEDICA a Journal of Clinical Medicine 2016; 11(6): 130-135 STATE OF THE ART New Insights into Antisynthetase Syndrome Manole COJOCARU a,b ; Inimioara Mihaela COJOCARU
Clinical Laboratory. [None
 Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
Idiopathic inflammatory myopathies
 Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia. Nitra and the Gangs.
 Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation
 Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
Test Name Results Units Bio. Ref. Interval
 135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
Utility of dermatomyositis-specific autoantibodies for diagnosis and clinical subsetting
 International Journal of Clinical Rheumatology Review ositis Utility of dermatomyositis-specific autoantibodies for diagnosis and clinical subsetting Autoantibodies directed against nuclear or cellular
International Journal of Clinical Rheumatology Review ositis Utility of dermatomyositis-specific autoantibodies for diagnosis and clinical subsetting Autoantibodies directed against nuclear or cellular
Diagnostic challenges in IPF
 Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Idiopathic non-specific interstitial pneumonia: as an autoimmune interstitial pneumonia
 Respiratory Medicine (2005) 99, 234 240 Idiopathic non-specific interstitial pneumonia: as an autoimmune interstitial pneumonia Jiro Fujita a,, Yuji Ohtsuki b, Takeo Yoshinouchi c, Ichiro Yamadori d, Shuji
Respiratory Medicine (2005) 99, 234 240 Idiopathic non-specific interstitial pneumonia: as an autoimmune interstitial pneumonia Jiro Fujita a,, Yuji Ohtsuki b, Takeo Yoshinouchi c, Ichiro Yamadori d, Shuji
A case of a patient with IPF treated with nintedanib. Prof. Kreuter and Prof. Heussel
 A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
Myositis 101. Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic, Rochester, MN
 Myositis 101 Steven R. Ytterberg, M.D. Rheumatology Mayo Clinic, Rochester, MN Myositis Association Annual Conference Louisville, KY Sept. 6 & 7, 2018 Disclosures Consulting: Dynavax Pfizer Off-label use:
Myositis 101 Steven R. Ytterberg, M.D. Rheumatology Mayo Clinic, Rochester, MN Myositis Association Annual Conference Louisville, KY Sept. 6 & 7, 2018 Disclosures Consulting: Dynavax Pfizer Off-label use:
Lung Allograft Dysfunction
 Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Discovery, Understanding, and Progress in Myositis
 Discovery, Understanding, and Progress in Myositis Steven Ytterberg, M.D. TMA Annual Patient Conference New Orleans, LA Sept. 2, 2016 Disclosures Financial: Dynavax Corp. Pfizer Mallinckrodt American Board
Discovery, Understanding, and Progress in Myositis Steven Ytterberg, M.D. TMA Annual Patient Conference New Orleans, LA Sept. 2, 2016 Disclosures Financial: Dynavax Corp. Pfizer Mallinckrodt American Board
Diffuse Interstitial Lung Diseases: Is There Really Anything New?
 : Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
: Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
INTERSTITIAL LUNG DISEASE Dr. Zulqarnain Ashraf
 Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
DIAGNOSTIC NOTE TEMPLATE
 DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
Annual Rheumatology & Therapeutics Review for Organizations & Societies
 Annual Rheumatology & Therapeutics Review for Organizations & Societies A Rheumatologist s Approach to Interstitial Lung Disease Outline ILD classification and patterns in CTD The clinical landscape and
Annual Rheumatology & Therapeutics Review for Organizations & Societies A Rheumatologist s Approach to Interstitial Lung Disease Outline ILD classification and patterns in CTD The clinical landscape and
International consensus statement on idiopathic pulmonary fibrosis
 Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Inflammatory Myopathies 4 th year MBBS. Marwan Adwan MBChB, MSc, MRCPI, MRCP(rheum) Consultant Rheumatologist
 Inflammatory Myopathies 4 th year MBBS Marwan Adwan MBChB, MSc, MRCPI, MRCP(rheum) Consultant Rheumatologist Case A 64 woman presents with erythematous itchy rash over back of hands & forehead. For 1 month
Inflammatory Myopathies 4 th year MBBS Marwan Adwan MBChB, MSc, MRCPI, MRCP(rheum) Consultant Rheumatologist Case A 64 woman presents with erythematous itchy rash over back of hands & forehead. For 1 month
Case 4 History. 58 yo man presented with prox IP joint swelling 2 months later pain and swelling in multiple joints Chest radiograph: bi-basilar
 Case 4 History 58 yo man presented with prox IP joint swelling 2 months later pain and swelling in multiple joints Chest radiograph: bi-basilar basilar infiltrates suggestive of pulmonary fibrosis Open
Case 4 History 58 yo man presented with prox IP joint swelling 2 months later pain and swelling in multiple joints Chest radiograph: bi-basilar basilar infiltrates suggestive of pulmonary fibrosis Open
Interstitial Pneumonia Associated with the Influenza Vaccine: A Report of Two Cases
 CASE REPORT Interstitial Pneumonia Associated with the Influenza Vaccine: A Report of Two Cases Makoto Hibino and Tetsuri Kondo Abstract Although the influenza vaccine is relatively safe and effective,
CASE REPORT Interstitial Pneumonia Associated with the Influenza Vaccine: A Report of Two Cases Makoto Hibino and Tetsuri Kondo Abstract Although the influenza vaccine is relatively safe and effective,
NIH Public Access Author Manuscript J Bras Pneumol. Author manuscript; available in PMC 2013 June 09.
 NIH Public Access Author Manuscript Published in final edited form as: J Bras Pneumol. 2011 February ; 37(1): 100 109. Myositis-related interstitial lung disease and antisynthetase syndrome*,,** Joshua
NIH Public Access Author Manuscript Published in final edited form as: J Bras Pneumol. 2011 February ; 37(1): 100 109. Myositis-related interstitial lung disease and antisynthetase syndrome*,,** Joshua
Clinical Laboratory. 14:41:00 Complement Component 3 50 mg/dl Oct-18
 Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Thyroid Peroxidase (TPO) Antibody 5.0 IU/mL [0.0-9.0] 18-289-900139 16-Oct-18 Complement Component 3 50 mg/dl 18-289-900139
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Thyroid Peroxidase (TPO) Antibody 5.0 IU/mL [0.0-9.0] 18-289-900139 16-Oct-18 Complement Component 3 50 mg/dl 18-289-900139
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW
 SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Clinical Differences Between Interstitial Lung Disease Associated With Clinically Amyopathic Dermatomyositis and Classic Dermatomyositis
 CHEST Clinical Differences Between Interstitial Lung Disease Associated With Clinically Amyopathic Dermatomyositis and Classic Dermatomyositis Hiroshi Mukae, MD, PhD; Hiroshi Ishimoto, MD; Noriho Sakamoto,
CHEST Clinical Differences Between Interstitial Lung Disease Associated With Clinically Amyopathic Dermatomyositis and Classic Dermatomyositis Hiroshi Mukae, MD, PhD; Hiroshi Ishimoto, MD; Noriho Sakamoto,
P olymyositis (PM) and dermatomyositis (DM) are systemic
 297 EXTENDED REPORT Interstitial lung disease, a common manifestation of newly diagnosed polymyositis and dermatomyositis M Fathi, M Dastmalchi, E Rasmussen, I E Lundberg, G Tornling... See end of article
297 EXTENDED REPORT Interstitial lung disease, a common manifestation of newly diagnosed polymyositis and dermatomyositis M Fathi, M Dastmalchi, E Rasmussen, I E Lundberg, G Tornling... See end of article
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Influence of Smoking in Interstitial Pneumonia Presenting with a Non-Specific Interstitial Pneumonia Pattern
 ORIGINAL ARTICLE Influence of Smoking in Interstitial Pneumonia Presenting with a Non-Specific Interstitial Pneumonia Pattern Tetsuro Sawata, Masashi Bando, Masayuki Nakayama, Naoko Mato, Hideaki Yamasawa
ORIGINAL ARTICLE Influence of Smoking in Interstitial Pneumonia Presenting with a Non-Specific Interstitial Pneumonia Pattern Tetsuro Sawata, Masashi Bando, Masayuki Nakayama, Naoko Mato, Hideaki Yamasawa
Accumulation of periostin in acute exacerbation of familial idiopathic pulmonary fibrosis
 Case Report Accumulation of periostin in acute exacerbation of familial idiopathic pulmonary fibrosis Keisuke Murata 1, Yasuhiko Koga 1, Norimitsu Kasahara 1, Yoshimasa Hachisu 1, Satoshi Nunomura 2, Nozomi
Case Report Accumulation of periostin in acute exacerbation of familial idiopathic pulmonary fibrosis Keisuke Murata 1, Yasuhiko Koga 1, Norimitsu Kasahara 1, Yoshimasa Hachisu 1, Satoshi Nunomura 2, Nozomi
Idiopathic inflammatory myopathies and the lung
 EUROPEAN RESPIRATORY UPDATE IDIOPATHIC INFLAMMATORY MYOPATHIES Idiopathic inflammatory myopathies and the lung Jean-Christophe Lega 1,2, Quitterie Reynaud 1, Alexandre Belot 3, Nicole Fabien 4, Isabelle
EUROPEAN RESPIRATORY UPDATE IDIOPATHIC INFLAMMATORY MYOPATHIES Idiopathic inflammatory myopathies and the lung Jean-Christophe Lega 1,2, Quitterie Reynaud 1, Alexandre Belot 3, Nicole Fabien 4, Isabelle
Rapidly Progressive Interstitial Lung Disease in a
 CASE REPORT Rapidly Progressive Interstitial Lung Disease in a Dermatomyositis Patient with High Levels of Creatine Phosphokinase, Severe Muscle Symptomsand Positive Anti-Jo-1 Antibody Kosuke Kashiwabara
CASE REPORT Rapidly Progressive Interstitial Lung Disease in a Dermatomyositis Patient with High Levels of Creatine Phosphokinase, Severe Muscle Symptomsand Positive Anti-Jo-1 Antibody Kosuke Kashiwabara
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT
 Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
HUNGARIAN MYOSITIS COHORT
 CLINICAL ADVANCES OF ANTI- TIF1Γ AUTOANTIBODY IN A HUNGARIAN MYOSITIS COHORT Melinda Nagy-Vincze 1, Zoltán Griger 1, Levente Bodoki 1, Zsuzsa Szankai 1, Zoe E. Betteridge 2, Katalin Dankó 1 1 University
CLINICAL ADVANCES OF ANTI- TIF1Γ AUTOANTIBODY IN A HUNGARIAN MYOSITIS COHORT Melinda Nagy-Vincze 1, Zoltán Griger 1, Levente Bodoki 1, Zsuzsa Szankai 1, Zoe E. Betteridge 2, Katalin Dankó 1 1 University
Interstitial lung disease in patients with polymyositis, dermatomyositis and amyopathic dermatomyositis
 Rheumatology Advance Access published June 21, 2005 Rheumatology 2005; 1 of 5 doi:10.1093/rheumatology/keh723 Concise Report Interstitial lung disease in patients with polymyositis, dermatomyositis and
Rheumatology Advance Access published June 21, 2005 Rheumatology 2005; 1 of 5 doi:10.1093/rheumatology/keh723 Concise Report Interstitial lung disease in patients with polymyositis, dermatomyositis and
Radiation Pneumonitis with Eosinophilic Alveolitis in a Lung Cancer Patient
 doi: 10.2169/internalmedicine.9338-17 Intern Med 57: 1281-1285, 2018 http://internmed.jp CASE REPORT Radiation Pneumonitis with Eosinophilic Alveolitis in a Lung Cancer Patient Yuki Hosono, Nobuhiko Sawa,
doi: 10.2169/internalmedicine.9338-17 Intern Med 57: 1281-1285, 2018 http://internmed.jp CASE REPORT Radiation Pneumonitis with Eosinophilic Alveolitis in a Lung Cancer Patient Yuki Hosono, Nobuhiko Sawa,
*Pari Basharat ABSTRACT OVERVIEW OF IDIOPATHIC INFLAMMATORY MYOPATHIES
 IDIOPATHIC INFLAMMATORY MYOPATHIES: ASSOCIATION WITH OVERLAP MYOSITIS AND SYNDROMES: CLASSIFICATION, CLINICAL CHARACTERISTICS, AND ASSOCIATED AUTOANTIBODIES *Pari Basharat University of Western Ontario,
IDIOPATHIC INFLAMMATORY MYOPATHIES: ASSOCIATION WITH OVERLAP MYOSITIS AND SYNDROMES: CLASSIFICATION, CLINICAL CHARACTERISTICS, AND ASSOCIATED AUTOANTIBODIES *Pari Basharat University of Western Ontario,
Naomi Yoshida, Shinjiro Kaieda, Kumi Tomozoe, Morihiro Tajiri, Daisuke Wakasugi, Masaki Okamoto, Masaki Tominaga, Hiroaki Ida and Tomoaki Hoshino
 CASE REPORT An Autopsy Case of Anti-melanoma Differentiation-associated Gene-5 Antibody-positive Clinical Amyopathic Dermatomyositis Complicated by Rapidly Progressive Interstitial Lung Disease Naomi Yoshida,
CASE REPORT An Autopsy Case of Anti-melanoma Differentiation-associated Gene-5 Antibody-positive Clinical Amyopathic Dermatomyositis Complicated by Rapidly Progressive Interstitial Lung Disease Naomi Yoshida,
ENFERMEDADES AUTOINMUNES SISTÉMICAS. Dr. J. María Pego Reigosa
 ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
