Hypersensitivity pneumonia, also known as extrinsic. Hypersensitivity Pneumonia. Role of Surgical Lung Biopsy
|
|
|
- Ashley Carmella Small
- 5 years ago
- Views:
Transcription
1 Lung biopsy often plays a key role in identifying patients with hypersensitivity pneumonia, especially in the absence of a typical history. A 69-year-old woman with a 2-year history of unexplained dyspnea on exertion underwent surgical lung biopsy for diagnosis of diffuse lung disease thought to represent idiopathic pulmonary fibrosis. Her biopsy showed honeycomb change and fibroblast foci suggestive of usual interstitial pneumonia, but also showed areas of cellular interstitial pneumonia with chronic bronchiolitis and a pattern of granulomatous inflammation typical of hypersensitivity pneumonia. The classic features of hypersensitivity pneumonia in surgical lung biopsy are emphasized, including a bronchiolocentric cellular interstitial pneumonia, chronic bronchiolitis, and poorly formed nonnecrotizing granulomas. As illustrated in our patient, sometimes subtle histologic clues are key in separating hypersensitivity pneumonia from usual interstitial pneumonia and other forms of idiopathic interstitial pneumonia. Making the distinction is important given differences in treatment strategies and natural history. (Arch Pathol Lab Med. 2012;136: ; doi: /arpa CR) Hypersensitivity pneumonia, also known as extrinsic allergic alveolitis, is a form of diffuse interstitial lung disease. The pathologic basis is an immune complex and cell-mediated immunologic response to a variety of inhaled organic antigens. 1 The most common antigens are molds, thermophilic bacteria, and animal proteins. The category of animal proteins is almost always avian (bird) antigens. Cats and dogs do not cause hypersensitivity pneumonia. The list of entities or unusual exposures that are reported to cause hypersensitivity pneumonia increases every year. 2 Exposure to certain inorganic compounds, mainly isocyanates, may also cause hypersensitivity pneumonia in a small percentage of exposed individuals. 3 Through the years specific names Accepted for publication March 13, From the Department of Pathology, University of Michigan, Ann Arbor. The authors have no relevant financial interest in the products or companies described in this article. Presented at the New Frontiers in Pathology: An Update for Practicing Pathologists meeting; October 14, 2011; Ann Arbor, Michigan. Reprints: Jonathon B. Herbst, MD, Department of Pathology, 2G332 UH, 1500 E Medical Center Dr, SPC 5054, Ann Arbor, MI ( jherbst@med.umich.edu). Hypersensitivity Pneumonia Role of Surgical Lung Biopsy Jonathon B. Herbst, MD; Jeffrey L. Myers, MD have been applied to patients with hypersensitivity pneumonia based on the unique circumstances of antigenic exposure, such as farmer s lung, bird fancier s lung, or pigeon breeder s lung. 4 Hargreave et al 5 first proposed the term bird breeder s (fancier s) lung to describe a syndrome analogous to farmer s lung following exposure to budgerigars. Chronic hypersensitivity pneumonia results from repeated exposures to antigens and can be lethal. We report a patient with hypersensitivity pneumonia who illustrates the sentinel features of hypersensitivity pneumonia and the key role that lung biopsy can play in making the diagnosis. CASE REPORT A 69-year-old woman had reported a nonproductive cough for 2 years with increased breathlessness with vigorous activity. She had a 6-year history of asthma. She had no pets or birds. She resided in a different US state, where her symptoms would improve, during the winter. Worsening of symptoms occurred during the summer months, when she returned to her primary residence. She attributed the fluctuation in her symptoms to improvement in her asthma when residing in a more arrid climate. A highresolution computed tomography (HRCT) scan of her chest demonstrated a combination of ground-glass opacities, traction bronchiectasis, and minimal subpleural honeycombing in the lower lobes. Video-assisted thoracoscopic surgery biopsy of the right middle and lower lobes was performed. Microscopic examination of the lower lobe biopsy at low power demonstrated areas of architectural distortion with honeycomb change (Figures 1 and 2). Scattered throughout were subepithelial interstitial foci comprising linearly oriented myofibroblasts within a pale staining matrix characteristic of fibroblast foci (Figure 3). This combination of features raised the possibility of usual interstitial pneumonia (UIP). However, in areas with less well-established fibrosis, a cellular interstitial pneumonia composed of mostly lymphocytes accompanied a chronic bronchiolitis (Figure 4). Within the interstitium were poorly formed granulomas, characterized by isolated giant cells containing various cytoplasmic inclusions including cholesterol-like clefts (Figure 5). The right middle lobe biopsy lacked the fibrosis and honeycomb change seen in the lower lobe biopsy and instead demonstrated an exquisitely airway-centered cellular interstitial pneumonia (Figure 6) with areas of peribronchiolar metaplasia (PBM) (Figure 7). Isolated giant cells were confined to peribronchiolar interstitium; many of the giant cells contained calcified cytoplasmic Schaumann bodies (Figures 8 and 9). The combination of a bronchiolocentric interstitial pneumonia with fibrosis, chronic bronchiolitis, and a characteristic pattern of nonnecrotizing granulomatous inflammation was diagnostic of chronic hypersensitivity pneumonia. COMMENT As demonstrated in our patient, surgical lung biopsy often plays a key role in establishing the diagnosis of hypersen- Arch Pathol Lab Med Vol 136, August 2012 Hypersensitivity Pneumonia: Role of Biopsy Herbst & Myers 889
2 Figure 1. Low-magnification photomicrograph of a surgical lung biopsy showing fibrosis and honeycomb change. Note the increased cellularity, represented by an increased blue quality. Usual interstitial pneumonia typically has a pink overall appearance at low power because of collagen fibrosis (hematoxylin-eosin, original magnification 320). Figure 2. Low-magnification photomicrograph of a surgical lung biopsy showing fibrosis and honeycomb change in a patient with chronic hypersensitivity pneumonia (hematoxylin-eosin, original magnification 340). Figure 3. High-magnification photomicrograph of a surgical lung biopsy showing a fibroblast focus. This is composed of linearly oriented myofibroblasts, mostly in a parallel orientation and a subepithelial location. Fibroblast foci, although characteristic of usual interstitial pneumonia, may be present in other conditions, including chronic hypersensitivity pneumonia (hematoxylin-eosin, original magnification 3200). 890 Arch Pathol Lab Med Vol 136, August 2012 Hypersensitivity Pneumonia: Role of Biopsy Herbst & Myers
3 sitivity pneumonia, especially in the absence of an incriminating exposure history. 6 Affected patients are often unaware of a specific environmental exposure. Episodic symptoms linked to a change in location can be helpful in narrowing the search for offending antigens. In our patient, for example, it is likely that an antigen in her primary residence was responsible, given her improvement while she was away in the winters. Radiologic studies, especially HRCT, may be helpful in suggesting the diagnosis in a subset of patients, but the findings are not specific and often overlap with other idiopathic diffuse lung diseases. Lung biopsy therefore often is essential to make the correct diagnosis, creating an opportunity for antigen avoidance and limiting progressive fibrosis and worsening of lung function. Conventionally, hypersensitivity pneumonia is classified as acute, subacute, or chronic. The nomenclature is only a general basis for the clinical distinction, as there can be significant overlap between these categories. 7 Acute hypersensitivity may include influenza-type symptoms, such as fever, chills, headache, and other symptoms that begin 2 to 9 hours after exposure and may last for days. 7 Dyspnea and cough are common complaints. The subacute form usually refers to patients with symptoms for less than 1 year. The symptoms may develop during a period of days to weeks. Severe dyspnea and hospitalization may occur. Chronic hypersensitivity usually refers to patients with complaints for longer than 1 year and is the form of the disease in which lung biopsy often is essential to diagnosis. Fibrosis is often already established in patients who present with the chronic form, hence the importance of early identification of this condition The onset of respiratory symptoms is often insidious, and a stepwise progression through the other forms need not have been previously identified. Clinical findings characterized by insidious onset include coughing, exertional dyspnea, anorexia, and weight loss. 11 Physical examination may identify crackles bilaterally, with clubbing seen in a minority of patients. Pulmonary function tests usually detect a restrictive defect. 11 Acute exacerbations may occur in chronic hypersensitivity pneumonia in a manner analogous to acute exacerbations in patients with UIP. 12,13 Miyazaki et al 14 described risk factors for exacerbations and concluded that low diffusing capacity of the lung for carbon dioxide, low mean total lung capacity, low lymphocyte levels in bronchoalveolar lavage fluid, and a UIP-like pattern on histology were risk factors for acute exacerbation. Specific immunoglobulin G precipitating antibodies have been used as an adjunct to diagnosis, but they are neither sensitive nor specific and are not by themselves diagnostic of hypersensitivity pneumonia. 15 The value of testing for precipitating antibodies depends to a large extent on pretest probabilities and is especially helpful in patients with exposure to a known antigen, exposure-related symptoms, crackles, and weight loss. 16 The test is performed by adding the patient s serum to wells that contain known antigens. Precipitation occurs when the serum contains antibody to the known antigens. Specific panels may be ordered depending on the occupational or environmental history. 1 False positives are common, as positive tests may be seen in those with exposure who lack evidence of lung disease. For example, a study using asymptomatic pigeon breeders as a control found they had positive antibodies at essentially the same rate as symptomatic patients thought to have hypersensitivity pneumonia. 17 Likewise, asymptomatic farmers may exhibit serum precipitins. 18 False negatives are common and can be due to underconcentrated serum, use of the wrong antigens, 19 poorly standardized reagents, or fluctuation in serum antibody levels. 20 Another laboratory test of potential value in patients for whom sarcoidosis is included in the differential diagnosis is serum levels of angiotensin-converting enzyme. Angiotensin-converting enzyme levels are not increased in hypersensitivity pneumonia, in contrast to the elevation usually seen in patients with sarcoidosis. 21,22 At some specialized centers, inhalational provocation testing may be performed by using a specific antigen to challenge patients with suspected hypersensitivity pneumonia. However, this requires first being able to identify an offending antigen. A study by Ohtani et al 23 demonstrated increased neutrophilia in bronchoalveolar lavage specimens after provocation testing in patients with chronic bird fancier s lung. Bronchoalveolar lavage with cell count and lymphocyte subset analysis may be helpful in evaluating patients with suspected hypersensitivity pneumonia. A lymphocytosis is typically seen and is characterized by a predominance of CD8 þ T lymphocytes. This technique has significant disadvantages, however, including variation in cellular profiles with disease state and elapsed time since antigen exposure. 24 A variety of radiologic abnormalities may be seen in patients with hypersensitivity pneumonia. HRCT scans are the most useful, showing a combination of mosaic attenuation with ground-glass opacification and centrilobular nodules that is useful in distinguishing patients with hypersensitivity pneumonia from those with idiopathic interstitial pneumonias (eg, UIP and nonspecific interstitial pneumonia [NSIP]) about half the time. 15,25 This characteristic combination of features is accompanied by radiologic evidence of fibrosis, including honeycombing, and/or emphysema in some patients. 15 The distribution of disease is important, as chronic hypersensitivity pneumonia may have a predilection for the mid to upper lungs, although lower lobe predominant disease also occurs. 26 Figure 4. Low-magnification photomicrograph of a surgical lung biopsy showing a cellular interstitial pneumonia along with a chronic bronchiolitis in a patient with chronic hypersensitivity pneumonia. Note the increased cellularity around bronchioles (hematoxylin-eosin, original magnification 340). Figure 5. High-magnification photomicrograph of a surgical lung biopsy demonstrating isolated giant cells (arrows) within the interstitium. Note the cholesterol cleft like material within the giant cells (hematoxylin-eosin, original magnification 3200). Figure 6. Low-magnification photomicrograph of a surgical lung biopsy showing a cellular interstitial pneumonia. There is expansion of the alveolar septa by a cellular process, mostly lymphocytes. Poorly formed granulomas can also be appreciated at this magnification (hematoxylin-eosin, original magnification 340). Arch Pathol Lab Med Vol 136, August 2012 Hypersensitivity Pneumonia: Role of Biopsy Herbst & Myers 891
4 The prognosis for hypersensitivity pneumonia is variable and in part depends on the degree of fibrosis. Retrospective observational case studies heavily weighted toward patients with farmer s lung demonstrate a collective mortality rate of 6.5%, ranging from 0% to 16.7% Most patients in these larger series either fully recovered (57.0%) or were alive with persistent disease (31.8%) Mortality rates may be higher in patients with chronic pigeon breeder s lung and were 29% at 5 years in a review of 78 patients from Mexico City. 32 Fibrosis may be a final common pathway in patients with progressive hypersensitivity pneumonia and when present in surgical lung biopsies is affiliated with shorter survival. 33 Retrospective studies published in the last decade and focusing on surgical lung biopsy findings show a collective mortality rate of 37%, which likely reflects a bias toward patients with fibrotic disease in whom the differential diagnosis is less easily resolved on the basis of clinical and radiologic findings alone. 8,34 37 Indeed, in some patients fibrotic lung disease may be indistinguishable from UIP and is associated with the same poor prognosis seen in patients with idiopathic pulmonary fibrosis. 34 Antigen avoidance is the mainstay of therapy and is thought to prevent disease progression, although recovery with continued antigen exposure is well documented in patients with either pigeon breeder s or farmer s lung. 28,38 Oral corticosteroids may be effective in acute or subacute forms of disease. 31,39 Lung function may improve during a period of months to years. Diffusing capacity of the lung for carbon dioxide is usually the slowest parameter to improve; defects in diffusing capacity of the lung for carbon dioxide may persist depending on stage of disease at diagnosis. 40,41 Smoking may also negatively influence outcome. 42 Vourlekis et al 33 also demonstrated that older age, smoking, and fibrosis all contribute to increased mortality compared with patients with nonhypersensitivity pneumonia. Acute hypersensitivity pneumonia rarely requires lung biopsy for diagnosis and therefore the histopathologic findings have been described in a limited number of patients. Hariri and colleagues 43 recently described a fibrinous air space exudate in 5 patients thought to have acute hypersensitivity pneumonia that resulted from exposure to mold in 4 of them. The fibrinous exudate included occasional eosinophils and was accompanied by interstitial neutrophils, a combination of findings that overlaps with so-called acute fibrinous and organizing pneumonia. 44 Importantly, all biopsies also showed a lymphocytic Figure 7. Intermediate-magnification photomicrograph demonstrating bronchiolitis with poorly formed nonnecrotizing granulomas more typical of subacute or chronic hypersensitivity pneumonia. The authors 43 also demonstrated a fibrinous air space exudate in 3 patients with established diagnoses of hypersensitivity pneumonia who experienced acute exacerbation of their symptoms. Autopsy of a patient who died during an episode of acute farmer s lung published more than 40 years earlier demonstrated similar alveolar exudates as well as a small-vessel vasculitis. 45 peribronchiolar metaplasia. Also note the rare poorly formed granuloma at the center of the field (hematoxylin-eosin, original magnification 3100). Chronic hypersensitivity pneumonia is usually characterized by a classic triad of pathologic features (Table). This triad includes a bronchiolocentric cellular chronic interstitial Figure 8. High-magnification photomicrograph demonstrating expansion of the interstitium by a cellular pneumonia, mostly lymphocytes with rare nonaggregated giant cells containing Schaumann bodies. Giant cells in other conditions, such as sarcoidosis, may also show Schaumann bodies, but the granulomas are characteristically well Figure 9. High-magnification photomicrograph showing an isolated formed in contrast to the poorly formed granulomas of hypersensitivity pneumonia (hematoxylin-eosin, original magnification 3200). giant cell with Schaumann bodies (hematoxylin-eosin, original magnification 3400). 892 Arch Pathol Lab Med Vol 136, August 2012 Hypersensitivity Pneumonia: Role of Biopsy Herbst & Myers
5 Feature Cellular interstitial pneumonia Chronic bronchiolitis Poorly formed granulomas Classic Histologic Features of Hypersensitivity Pneumonia Histologic Appearance Expansion within the interstitium by a cellular process; should be mostly lymphocytes. Variable dense infiltrate of mononuclear cells that expands the peribronchiolar interstitium with or without fibrosis. Composed of predominately lymphocytes and often with granulomatous features. Located in the interstitium, not airways, except in hot tub lung. Isolated giant cells, loose congregation of histiocytes. Well-formed granulomas are not characteristic. May contain Schaumann bodies, cholesterol clefts, asteroid bodies, and calcium oxalate crystals. pneumonia, chronic bronchiolitis, and nonnecrotizing granulomatous inflammation largely confined to the peribronchiolar interstitium. 8,33,36,37,46,47 This classic combination of findings is often accompanied by other characteristic secondary features that may serve as supportive evidence in the proper setting. Chronic interstitial pneumonia is a nearly constant finding in surgical lung biopsies from patients with chronic hypersensitivity pneumonia (Figure 6) and is often described as NSIP-like. The interstitial pneumonia is always airway centered and includes a lymphocytic infiltrate that is most conspicuous around distal bronchioles. The inflammatory infiltrate consists of mostly lymphocytes; plasma cells, eosinophils, and neutrophils are often absent and if present should be infrequent (Figure 8). Expanded alveolar septa are lined by hyperplastic pneumocytes. Alveolar septal lymphocytic infiltrates may be accompanied by fibrosis; in some patients fibrosis may be a conspicuous feature. Biopsies showing extensive fibrosis often include areas of architectural distortion in the form of honeycomb change. Chronic bronchiolitis is the second key feature of hypersensitivity pneumonia and occurs as frequently as interstitial pneumonia (Figure 4). Bronchiolitis was the most common finding in surgical lung biopsies reported by Trahan et al 37 and was a useful feature for distinguishing chronic hypersensitivity pneumonia from UIP. Peribronchiolar interstitium is expanded by the same lymphocyte-rich infiltrate that characterizes the previously described interstitial pneumonia, accompanied by variable numbers of epithelioid histiocytes. Peribronchiolar lymphoid aggregates may be present and were seen in 79% of surgical lung biopsies reported by Trahan et al. 37 Fibrosis of peribronchiolar interstitium may accompany the lymphocytic infiltrate and include hyperplasia of bronchiolar-type epithelium, a combination of histologic findings for which the term PBM has been proposed. 48 Peribronchiolar metaplasia is not specific, however, and may be seen in other conditions including UIP, NSIP, desquamative interstitial pneumonia, and a unique form of diffuse fibrotic airway disease termed PBM interstitial lung disease or airway-centered interstitial fibrosis. 48,49 Peribronchiolar metaplasia is universal at autopsy in patients with chronic hypersensitivity pneumonia, but is also seen in nearly three-fourths of patients with UIP. 50 Other evidence of the bronchiolocentric nature of hypersensitivity pneumonia may include organizing pneumonia, referred to historically as bronchiolitis obliterans organizing pneumonia, which is present in as many as half of cases. Prominent foamy macrophage within peribronchiolar alveolar spaces (ie, microscopic obstructive pneumonia) is another finding that frequently attests to the presence of bronchiolitis and physiologic airflow obstruction in patients with hypersensitivity pneumonia. Granulomatous inflammation completes the classic histopathologic triad of hypersensitivity pneumonia, but it is the least constant of the characteristic features. Granulomas are present in about 80% of surgical lung biopsies from patients with hypersensitivity pneumonia and have distinct characteristics relating to their distribution and location as well as their composition. The granulomas characteristic of hypersensitivity pneumonia are centered upon the peribronchiolar interstitium rather than the lumens of airways and peribronchiolar air spaces (Figures 8 and 9). If the majority of granulomas are situated within airways or alveolar spaces, then one should consider an alternate possibility such as granulomatous infection or particulate aspiration. In addition, the granulomas of hypersensitivity pneumonia are poorly formed and therefore subtle. The granulomas may often be solitary giant cells, or a small cluster of loosely organized epithelioid histiocytes. The granulomas are often sufficiently subtle that they are easily missed unless the peribronchiolar infiltrates are scrutinized at higher magnification. Isolated giant cells may contain various cytoplasmic inclusions such as cholesterol clefts, Schaumann bodies, calcium oxalate crystals, or asteroid bodies that are not specific but may aid in their recognition (Figures 5 and 9). 46 Well-formed granulomas resembling those seen in sarcoidosis are uncommon in hypersensitivity pneumonia. A rare well-formed granuloma does not exclude the diagnosis, but should not be the dominant feature. The classic combination of bronchiolocentric interstitial pneumonia, bronchiolitis, and granulomatous inflammation accounted for less than one-half of 211 surgical lung biopsies reported in recent retrospective case-based series. 8,34 37 Together, UIP and NSIP comprised nearly as many cases, each accounting for just more than 20% of biopsies. These studies are biased in that they focused only on patients undergoing surgical lung biopsy, many of whom were suspected of having idiopathic interstitial pneumonia. The studies also vary in terms of criteria used to establish the diagnosis of hypersensitivity pneumonia. In addition, Ohtani and colleagues 36 assigned all 26 of their patients to histologically based categories using only the nomenclature more typically applied to the idiopathic interstitial pneumonias (ie, UIP, NSIP, and organizing pneumonia). Despite these shortcomings, taken together these observations highlight the importance of considering the possibility of hypersensitivity pneumonia when confronted with lung biopsies from patients otherwise suspected of having idiopathic diffuse lung disease. Chronic hypersensitivity pneumonia may develop a pattern of fibrosis and honeycomb change with fibroblast foci virtually indistinguishable from UIP. 8,34,36,37,50 Indeed, in some patients with late stage disease it may become nearly impossible to distinguish idiopathic pulmonary fibrosis from chronic hypersensitivity pneumonia, but at this stage the Arch Pathol Lab Med Vol 136, August 2012 Hypersensitivity Pneumonia: Role of Biopsy Herbst & Myers 893
6 distinction may have little impact on outcome as both have the same poor prognosis. 32,34 In other patients the distinction hinges on identifying areas away from the fibrosis that demonstrate the classic combination of a cellular, bronchiolocentric, lymphocyte-rich, interstitial infiltrate with the characteristic pattern of associated granulomatous inflammation. 6,37 Prominent PBM, although not specific, is more common and tends to be more extensive in chronic hypersensitivity pneumonia compared with UIP. 50 In an otherwise typical case of UIP, pronounced PBM should trigger a careful search for the findings more characteristic of classic chronic hypersensitivity pneumonia. Upper lobe predominance of honeycomb change, something likely to be more easily appreciated on HRCT than surgical lung biopsy, can serve as another clue to a diagnosis of chronic hypersensitivity pneumonia. An autopsy study comparing 16 patients with hypersensitivity pneumonia to 11 individuals with idiopathic pulmonary fibrosis/uip showed that lower and upper lobe honeycomb change occurred in both with the same frequency. 50 Lower lobe honeycomb change was seen in all patients, and upper lobe honeycomb change was seen in 91% of patients with UIP and 81% of patients with chronic hypersensitivity pneumonia. However, upper lobe dominant disease was seen only in patients with chronic hypersensitivity pneumonia, occurring in only 44% of patients. 50 Vourlekis et al 33,47 described NSIP as the only histologic finding in 6 patients, representing 7.1% of patients with hypersensitivity pneumonia who underwent surgical lung biopsy in the course of their evaluation. The biopsies included 2 purely cellular lesions ( cellular NSIP ) and 4 with concomitant fibrosis ( fibrotic NSIP ). There were no granulomas in any of their patients. One patient died 6.8 years after lung biopsy; all others were alive after an average follow-up of 5.5 years. Since then a number of authors have confirmed the presence of what might otherwise be taken as idiopathic NSIP in patients thought to have hypersensitivity pneumonia. 8,34 37 As with UIP, important clues that should raise the possibility of hypersensitivity pneumonia include a bronchiolocentric distribution of the inflammation and/or fibrosis, PBM, and other evidence of small-airway injury such as organizing pneumonia and foamy alveolar macrophages in peribronchiolar air spaces. 8,37,48 Thus it is important to remain vigilant of the possibility even if all the classic findings are not seen. Sampling bias may be a factor in separating chronic hypersensitivity pneumonia from idiopathic interstitial pneumonias, as illustrated in our patient. Trahan and colleagues 37 reported 15 patients with a clinical diagnosis of chronic hypersensitivity pneumonia who underwent lung biopsy of 1 to 3 lobes. Two patients had discordant findings in that they had classic features of hypersensitivity pneumonia in 1 specimen and UIP or nonspecific changes in others. Biopsies from 2 showed only UIP, and 1 showed NSIP. The authors concluded that sampling more than one lobe may be useful in distinguishing hypersensitivity pneumonia from idiopathic interstitial pneumonias. Occasionally the differential diagnosis includes granulomatous infection, especially a hypersensitivity pneumonia like syndrome resulting from exposure to contaminated hot tubs (hot tub lung). Hot tub lung is caused by Mycobacterium avium-intracellulare complex, which thrives in the warm environment of hot tubs. Affected patients develop a syndrome with hypersensitivity-like features following exposure to indoor hot tubs. Hot tub lung has important clinical and histopathologic distinctions from classic hypersensitivity pneumonia, suggesting that the pathogenesis may combine elements of infection and hypersensitivity. 51,52 Key to the distinction in surgical lung biopsies is the location and morphology of the granulomas, which are distributed within the lumens of distal airways in hot tub lung, rather than the interstitial location more typical of hypersensitivity pneumonia. 51,52 In addition the granulomas tend to be well formed and may show small foci of central necrosis. 52 In these cases, culture results and acid-fast bacilli/gomori methenamine silver staining may play an important role in delineation between hypersensitivity and this condition. Transbronchial biopsy may be useful in recognizing hypersensitivity pneumonia in selected patients but is relatively insensitive compared with surgical lung biopsy. A study by Morell et al 17 evaluating retrospective data from 86 patients with bird fancier s lung demonstrated the characteristic triad of histopathologic findings in only 9% of 33 patients undergoing transbronchial biopsy. They also pointed out, however, that at least 1 of the characteristic histologic findings was present in just less than half of patients, including poorly formed granulomas in 7 (21%). 17 This suggests that transbronchial biopsy may be most useful in patients for whom there is a strong clinical suspicion and supportive radiologic findings on HRCT. In summary, the diagnosis of hypersensitivity pneumonia is one in which the pathologist often plays an important role. Consider the diagnosis any time a biopsy shows a combination of bronchiolocentric interstitial pneumonia, chronic bronchiolitis, and poorly formed, nonnecrotizing, granulomatous inflammation confined to peribronchiolar interstitium, even in the absence of an exposure history. The possibility of chronic hypersensitivity pneumonia should also be investigated in any patient whose surgical lung biopsy shows features resembling UIP or NSIP by looking for this same combination of findings away from the areas of most pronounced fibrosis and honeycomb change. Making this distinction creates an opportunity for discovering an offending antigen with important implications for treatment and prognosis. References 1. Mohr LC. Hypersensitivity pneumonitis. Curr Opin Pulm Med. 2004;10(5): Girard M, Cormier Y. Hypersensitivity pneumonitis. Curr Opin Allergy Clin Immunol. 2010;10(2): Baur X. Hypersensitivity pneumonitis (extrinsic allergic alveolitis) induced by isocyanates. J Allergy Clin Immunol. 1995;95(5, pt 1): Allen JT, Spiteri MA. Pigeon breeder s disease. J Lab Clin Med. 1996;127(1): Hargreave FE, Pepys J, Longbottom JL, Wraith DG. Bird breeder s (fancier s) lung. Lancet. 1966;1(7435): Myers JL. Hypersensitivity pneumonia: the role of lung biopsy in diagnosis and management. Mod Pathol. 2012;25(suppl 1):S58 S Girard M, Lacasse Y, Cormier Y. Hypersensitivity pneumonitis. Allergy. 2009;64(3): Churg A, Sin DD, Everett D, Brown K, Cool C. Pathologic patterns and survival in chronic hypersensitivity pneumonitis. Am J Surg Pathol. 2009;33(12): Hanak V, Golbin JM, Hartman TE, Ryu JH. High-resolution CT findings of parenchymal fibrosis correlate with prognosis in hypersensitivity pneumonitis. Chest. 2008;134(1): Sahin H, Brown KK, Curran-Everett D, et al. Chronic hypersensitivity pneumonitis: CT features comparison with pathologic evidence of fibrosis and survival. Radiology. 2007;244(2): Hirschmann JV, Pipavath SN, Godwin JD. Hypersensitivity pneumonitis: a historical, clinical, and radiologic review. Radiographics. 2009;29(7): Collard HR, Moore BB, Flaherty KR, et al. Acute exacerbations of idiopathic pulmonary fibrosis. Am J Respir Crit Care Med. 2007;176(7): Arch Pathol Lab Med Vol 136, August 2012 Hypersensitivity Pneumonia: Role of Biopsy Herbst & Myers
7 13. Olson AL, Huie TJ, Groshong SD, et al. Acute exacerbations of fibrotic hypersensitivity pneumonitis: a case series. Chest. 2008;134(4): Miyazaki Y, Tateishi T, Akashi T, Ohtani Y, Inase N, Yoshizawa Y. Clinical predictors and histologic appearance of acute exacerbations in chronic hypersensitivity pneumonitis. Chest. 2008;134(6): Glazer CS, Rose CS, Lynch DA. Clinical and radiologic manifestations of hypersensitivity pneumonitis. J Thorac Imaging. 2002;17(4): Lacasse Y, Selman M, Costabel U, et al. Clinical diagnosis of hypersensitivity pneumonitis. Am J Respir Crit Care Med. 2003;168(8): Morell F, Roger A, Reyes L, Cruz MJ, Murio C, Munoz X. Bird fancier s lung: a series of 86 patients. Medicine (Baltimore). Mar 2008;87(2): Cormier Y, Belanger J, Beaudoin J, Laviolette M, Beaudoin R, Hebert J. Abnormal bronchoalveolar lavage in asymptomatic dairy farmers: study of lymphocytes. Am Rev Respir Dis. 1984;130(6): Krasnick J, Meuwissen HJ, Nakao MA, Yeldandi A, Patterson R. Hypersensitivity pneumonitis: problems in diagnosis. J Allergy Clin Immunol. 1996;97(4): Cormier Y, Belanger J. The fluctuant nature of precipitating antibodies in dairy farmers. Thorax. 1989;44(6): McCormick JR, Thrall RS, Ward PA, Moore VL, Fink JN. Serum angiotensinconverting enzyme levels in patients with pigeon-breeder s disease. Chest. 1981;80(4): Tewksbury DA, Marx JJ Jr, Roberts RC, Emanuel DA. Angiotensinconverting enzyme in farmer s lung. Chest. 1981;79(1): Ohtani Y, Kojima K, Sumi Y, et al. Inhalation provocation tests in chronic bird fancier s lung. Chest. 2000;118(5): Fink JN, Ortega HG, Reynolds HY, et al. Needs and opportunities for research in hypersensitivity pneumonitis. Am J Respir Crit Care Med. 2005;171(7): Silva CI, Churg A, Muller NL. Hypersensitivity pneumonitis: spectrum of high-resolution CT and pathologic findings. AJR Am J Roentgenol. 2007;188(2): Hartman TE. The HRCT features of extrinsic allergic alveolitis. Semin Respir Crit Care Med. 2003;24(4): Barbee RA, Callies Q, Dickie HA, Rankin J. The long-term prognosis in farmer s lung. Am Rev Respir Dis. 1968;97(2): Emanuel DA, Wenzel FJ, Bowerman CI, Lawton BR. Farmer s lung: clinical, pathologic and immunologic study of twenty-four patients. Am J Med. 1964;37: Braun SR, dopico GA, Tsiatis A, Horvath E, Dickie HA, Rankin J. Farmer s lung disease: long-term clinical and physiologic outcome. Am Rev Respir Dis. 1979;119(2): Hanak V, Golbin JM, Ryu JH. Causes and presenting features in 85 consecutive patients with hypersensitivity pneumonitis. Mayo Clin Proc. 2007;82(7): Monkare S, Haahtela T. Farmer s lung a 5-year follow-up of eighty-six patients. Clin Allergy. 1987;17(2): Perez-Padilla R, Salas J, Chapela R, et al. Mortality in Mexican patients with chronic pigeon breeder s lung compared with those with usual interstitial pneumonia. Am Rev Respir Dis. 1993;148(1): Vourlekis JS, Schwarz MI, Cherniack RM, et al. The effect of pulmonary fibrosis on survival in patients with hypersensitivity pneumonitis. Am J Med. 2004;116(10): Gaxiola M, Buendia-Roldan I, Mejia M, et al. Morphologic diversity of chronic pigeon breeder s disease: clinical features and survival. Respir Med. 2011;105(4): Hayakawa H, Shirai M, Sato A, et al. Clinicopathological features of chronic hypersensitivity pneumonitis. Respirology. 2002;7(4): Ohtani Y, Saiki S, Kitaichi M, et al. Chronic bird fancier s lung: histopathological and clinical correlation: an application of the 2002 ATS/ERS consensus classification of the idiopathic interstitial pneumonias. Thorax. 2005;60(8): Trahan S, Hanak V, Ryu JH, Myers JL. Role of surgical lung biopsy in separating chronic hypersensitivity pneumonia from usual interstitial pneumonia/ idiopathic pulmonary fibrosis: analysis of 31 biopsies from 15 patients. Chest. 2008;134(1): Bourke SJ, Banham SW, Carter R, Lynch P, Boyd G. Longitudinal course of extrinsic allergic alveolitis in pigeon breeders. Thorax. 1989;44(5): Cormier Y, Israel-Assayag E, Desmeules M, Lesur O. Effect of contact avoidance or treatment with oral prednisolone on bronchoalveolar lavage surfactant protein A levels in subjects with farmer s lung. Thorax. 1996;51(12): Erkinjuntti-Pekkanen R, Kokkarinen JI, Tukiainen HO, Pekkanen J, Husman K, Terho EO. Long-term outcome of pulmonary function in farmer s lung: a 14 year follow-up with matched controls. Eur Respir J. 1997;10(9): Kokkarinen JI, Tukiainen HO, Terho EO. Recovery of pulmonary function in farmer s lung: a five-year follow-up study. Am Rev Respir Dis. 1993;147(4): Ohtsuka Y, Munakata M, Tanimura K, et al. Smoking promotes insidious and chronic farmer s lung disease, and deteriorates the clinical outcome. Intern Med. 1995;34(10): Hariri LP, Mino-Kenudson M, Shea B, et al. Distinct histopathology of acute onset or abrupt exacerbation of hypersensitivity pneumonitis [published online ahead of print August 18, 2011]. Hum Pathol. 2012;43(5): Beasley MB, Franks TJ, Galvin JR, Gochuico B, Travis WD. Acute fibrinous and organizing pneumonia: a histological pattern of lung injury and possible variant of diffuse alveolar damage. Arch Pathol Lab Med. 2002;126(9): Barrowcliff DF, Arblaster PG. Farmer s lung: a study of an early acute fatal case. Thorax. 1968;23(5): Coleman A, Colby TV. Histologic diagnosis of extrinsic allergic alveolitis. Am J Surg Pathol. 1988;12(7): Vourlekis JS, Schwarz MI, Cool CD, Tuder RM, King TE, Brown KK. Nonspecific interstitial pneumonitis as the sole histologic expression of hypersensitivity pneumonitis. Am J Med. 2002;112(6): Fukuoka J, Franks TJ, Colby TV, et al. Peribronchiolar metaplasia: a common histologic lesion in diffuse lung disease and a rare cause of interstitial lung disease: clinicopathologic features of 15 cases. Am J Surg Pathol. 2005;29(7): Churg A, Myers J, Suarez T, et al. Airway-centered interstitial fibrosis: a distinct form of aggressive diffuse lung disease. Am J Surg Pathol. 2004;28(1): Akashi T, Takemura T, Ando N, et al. Histopathologic analysis of sixteen autopsy cases of chronic hypersensitivity pneumonitis and comparison with idiopathic pulmonary fibrosis/usual interstitial pneumonia. Am J Clin Pathol. 2009;131(3): Hanak V, Kalra S, Aksamit TR, Hartman TE, Tazelaar HD, Ryu JH. Hot tub lung: presenting features and clinical course of 21 patients. Respir Med. 2006;100(4): Khoor A, Leslie KO, Tazelaar HD, Helmers RA, Colby TV. Diffuse pulmonary disease caused by nontuberculous mycobacteria in immunocompetent people (hot tub lung). Am J Clin Pathol. 2001;115(5): Arch Pathol Lab Med Vol 136, August 2012 Hypersensitivity Pneumonia: Role of Biopsy Herbst & Myers 895
Hypersensitivity Pneumonitis: Spectrum of High-Resolution CT and Pathologic Findings
 CT of Hypersensitivity Pneumonitis Chest Imaging Pictorial Essay C. Isabela S. Silva 1 ndrew Churg 2 Nestor L. Müller 1 Silva CIS, Churg, Müller NL Keywords: high-resolution CT, hypersensitivity pneumonitis,
CT of Hypersensitivity Pneumonitis Chest Imaging Pictorial Essay C. Isabela S. Silva 1 ndrew Churg 2 Nestor L. Müller 1 Silva CIS, Churg, Müller NL Keywords: high-resolution CT, hypersensitivity pneumonitis,
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
Hypersensitivity Pneumonitis: Epidemiology and Classification
 Hypersensitivity Pneumonitis: Epidemiology and Classification Ulrich Costabel, MD University of Duisburg-Essen, Ruhrlandklinik Department of Pneumology/Allergy Objectives Definitions, Etiology Epidemiology
Hypersensitivity Pneumonitis: Epidemiology and Classification Ulrich Costabel, MD University of Duisburg-Essen, Ruhrlandklinik Department of Pneumology/Allergy Objectives Definitions, Etiology Epidemiology
H ypersensitivity pneumonitis (HP) comprises a group of
 665 INTERSTITIAL LUNG DISEASE Chronic bird fancier s lung: histopathological and clinical correlation. An application of the 2002 ATS/ERS consensus classification of the idiopathic interstitial pneumonias
665 INTERSTITIAL LUNG DISEASE Chronic bird fancier s lung: histopathological and clinical correlation. An application of the 2002 ATS/ERS consensus classification of the idiopathic interstitial pneumonias
NONE OVERVIEW FINANCIAL DISCLOSURES UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF (UIP) FOR PATHOLOGISTS. IPF = Idiopathic UIP Radiologic UIP Path UIP
 UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Hypersensitivity Pneumonitis Common Diagnostic and Treatment Dilemmas
 Hypersensitivity Pneumonitis Common Diagnostic and Treatment Dilemmas Rishi Raj MD Director, Interstitial Lung Diseases Program Clinical Professor of Pulmonary and Critical Care Medicine Stanford University
Hypersensitivity Pneumonitis Common Diagnostic and Treatment Dilemmas Rishi Raj MD Director, Interstitial Lung Diseases Program Clinical Professor of Pulmonary and Critical Care Medicine Stanford University
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review.
 Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
Liebow and Carrington's original classification of IIP
 Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Pathology of Chronic Hypersensitivity Pneumonitis. What Is It? What Are the Diagnostic Criteria? Why Do We Care?
 Pathology of Chronic Hypersensitivity Pneumonitis What Is It? What Are the Diagnostic Criteria? Why Do We Care? Andrew Churg, MD; AnaMaria Bilawich, MD; Joanne L. Wright, MD Context. Chronic hypersensitivity
Pathology of Chronic Hypersensitivity Pneumonitis What Is It? What Are the Diagnostic Criteria? Why Do We Care? Andrew Churg, MD; AnaMaria Bilawich, MD; Joanne L. Wright, MD Context. Chronic hypersensitivity
Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School, University of Crete Prague, June 2014
 Hypersensitivity pneumonitis: Causes, clinical course, diagnosis and differential diagnosis, treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
Hypersensitivity pneumonitis: Causes, clinical course, diagnosis and differential diagnosis, treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
Outline Definition of Terms: Lexicon. Traction Bronchiectasis
 HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Non-neoplastic Lung Disease II
 Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
International consensus statement on idiopathic pulmonary fibrosis
 Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
I don t need you. Disclosure Statement. Pathology Approach to ILD 11/5/2016. Kirk D. Jones, MD UCSF Dept of Pathology
 Pathology Approach to ILD Disclosure Statement Relevant financial relationships with a commercial interest: Boeringer Ingleheim, speaker Kirk D. Jones, MD UCSF Dept of Pathology kirk.jones@ucsf.edu I don
Pathology Approach to ILD Disclosure Statement Relevant financial relationships with a commercial interest: Boeringer Ingleheim, speaker Kirk D. Jones, MD UCSF Dept of Pathology kirk.jones@ucsf.edu I don
CTD-related Lung Disease
 13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Hypersensitivity pneumonitis is a diffuse,
 HYPERSENSITIVITY PNEUMONITIS: ESSENTIAL RADIOLOGIC AND PATHOLOGIC FINDINGS Teri J. Franks, MD a, *, Jeffrey R. Galvin, MD b,c KEYWORDS Hypersensitivity pneumonitis Hypersensitivity pneumonia Extrinsic
HYPERSENSITIVITY PNEUMONITIS: ESSENTIAL RADIOLOGIC AND PATHOLOGIC FINDINGS Teri J. Franks, MD a, *, Jeffrey R. Galvin, MD b,c KEYWORDS Hypersensitivity pneumonitis Hypersensitivity pneumonia Extrinsic
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia. Nitra and the Gangs.
 Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Diffuse Interstitial Lung Diseases: Is There Really Anything New?
 : Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
: Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
Leslie Case 4. Prac%cal Approach to Granulomatous Lung Disease. PRE-TEST Which of these images is more likely to have organisms on special stains?
 Leslie Case 4 Prac%cal pproach to Granulomatous Lung Disease Kevin O. Leslie, MD Professor and Consultant Mayo Clinic rizona PRE-TEST have organisms on special stains? PRE-TEST represent infection? PRE-TEST
Leslie Case 4 Prac%cal pproach to Granulomatous Lung Disease Kevin O. Leslie, MD Professor and Consultant Mayo Clinic rizona PRE-TEST have organisms on special stains? PRE-TEST represent infection? PRE-TEST
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Challenges in the Diagnosis of Interstitial Lung Disease
 Challenges in the Diagnosis of Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept. of Pathology kirk.jones@ucsf.edu Overview New Classification of IIP Prior classification Modifications for new classification
Challenges in the Diagnosis of Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept. of Pathology kirk.jones@ucsf.edu Overview New Classification of IIP Prior classification Modifications for new classification
Pathologic Assessment of Interstitial Lung Disease
 Pathologic Assessment of Interstitial Lung Disease Dry and itchy? It could be eczema or fungal infection. We don t need to worry, the drugs aren t that dangerous. Kirk D. Jones, MD UCSF Dept. of Pathology
Pathologic Assessment of Interstitial Lung Disease Dry and itchy? It could be eczema or fungal infection. We don t need to worry, the drugs aren t that dangerous. Kirk D. Jones, MD UCSF Dept. of Pathology
Case 4 History. 58 yo man presented with prox IP joint swelling 2 months later pain and swelling in multiple joints Chest radiograph: bi-basilar
 Case 4 History 58 yo man presented with prox IP joint swelling 2 months later pain and swelling in multiple joints Chest radiograph: bi-basilar basilar infiltrates suggestive of pulmonary fibrosis Open
Case 4 History 58 yo man presented with prox IP joint swelling 2 months later pain and swelling in multiple joints Chest radiograph: bi-basilar basilar infiltrates suggestive of pulmonary fibrosis Open
Replacement of air with fluid, inflammatory. cells or cellular debris. Parenchymal, Interstitial (Restrictive) and Vascular Diseases.
 Parenchymal, Interstitial (Restrictive) and Vascular Diseases Alain C. Borczuk, M.D. Dept of Pathology Replacement of air with fluid, inflammatory cells Pulmonary Edema Pneumonia Hemorrhage Diffuse alveolar
Parenchymal, Interstitial (Restrictive) and Vascular Diseases Alain C. Borczuk, M.D. Dept of Pathology Replacement of air with fluid, inflammatory cells Pulmonary Edema Pneumonia Hemorrhage Diffuse alveolar
Hypersensitivity pneumonia: the role of lung biopsy in diagnosis and management
 S58 & 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 Hypersensitivity pneumonia: the role of lung biopsy in diagnosis and management Jeffrey L Myers Department of Pathology, University of Michigan,
S58 & 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 Hypersensitivity pneumonia: the role of lung biopsy in diagnosis and management Jeffrey L Myers Department of Pathology, University of Michigan,
Histopathologic Approach to Interstitial Lung Disease
 Histopathologic Approach to Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept of Pathology kirk.jones@ucsf.edu Disclosures I have nothing to disclose 1 Why? Much of interstitial lung disease biopsies
Histopathologic Approach to Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept of Pathology kirk.jones@ucsf.edu Disclosures I have nothing to disclose 1 Why? Much of interstitial lung disease biopsies
CASE REPORT. Introduction. Case Report
 doi: 10.2169/internalmedicine.1142-18 http://internmed.jp CASE REPORT The Analysis of Surgical Lung Biopsy and Explanted Lung Specimens Sheds Light on the Pathological Progression of Chronic Bird-related
doi: 10.2169/internalmedicine.1142-18 http://internmed.jp CASE REPORT The Analysis of Surgical Lung Biopsy and Explanted Lung Specimens Sheds Light on the Pathological Progression of Chronic Bird-related
Challenges in the Diagnosis of Interstitial Lung Disease
 Challenges in the Diagnosis of Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept. of Pathology kirk.jones@ucsf.edu Overview New Classification of IIP Prior classification Modifications for new classification
Challenges in the Diagnosis of Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept. of Pathology kirk.jones@ucsf.edu Overview New Classification of IIP Prior classification Modifications for new classification
Bronkhorst colloquium Interstitiële longziekten. Katrien Grünberg, klinisch patholoog
 Bronkhorst colloquium 2013-2014 Interstitiële longziekten De pathologie achter de CT Katrien Grünberg, klinisch patholoog K.grunberg@vumc.nl Preparing: introduction and 3 cases The introduction on microscopic
Bronkhorst colloquium 2013-2014 Interstitiële longziekten De pathologie achter de CT Katrien Grünberg, klinisch patholoog K.grunberg@vumc.nl Preparing: introduction and 3 cases The introduction on microscopic
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
Progress in Idiopathic Pulmonary Fibrosis
 Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
A Review of Interstitial Lung Diseases. Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco
 A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
Restrictive lung diseases
 Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
Restrictive lung diseases Restrictive lung diseases are diseases that affect the interstitium of the lung. Interstitium of the lung is the very thin walls surrounding the alveoli, it s formed of epithelium
A Review of Interstitial Lung Diseases
 Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases
 CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
Bronchoalveolar Lavage and Histopathologic Diagnosis Based on Biopsy
 Idiopathic Pulmonary Fibrosis Bronchoalveolar Lavage and Histopathologic Diagnosis Based on Biopsy JMAJ 46(11): 469 474, 2003 Yukihiko SUGIYAMA Professor, Division of Pulmonary Medicine, Department of
Idiopathic Pulmonary Fibrosis Bronchoalveolar Lavage and Histopathologic Diagnosis Based on Biopsy JMAJ 46(11): 469 474, 2003 Yukihiko SUGIYAMA Professor, Division of Pulmonary Medicine, Department of
Acute and Chronic Lung Disease
 KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
Radiologic Approach to Smoking Related Interstitial Lung Disease
 Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
Smoking-related lung pathology represents a histologically
 A Review of Smoking-Related Interstitial Fibrosis, Respiratory Bronchiolitis, and Desquamative Interstitial Pneumonia Overlapping Histology and Confusing Terminology Smoking-related lung diseases traverse
A Review of Smoking-Related Interstitial Fibrosis, Respiratory Bronchiolitis, and Desquamative Interstitial Pneumonia Overlapping Histology and Confusing Terminology Smoking-related lung diseases traverse
October 2012 Imaging Case of the Month. Michael B. Gotway, MD Associate Editor Imaging. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
T he diagnostic evaluation of a patient with
 546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis
 Original Article Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis Xia Li 1, Chang Chen 2, Jinfu Xu 1, Jinming Liu 1, Xianghua
Original Article Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis Xia Li 1, Chang Chen 2, Jinfu Xu 1, Jinming Liu 1, Xianghua
Abstract. American Society for Clinical Pathology. Am J Clin Pathol 2009;131: DOI: /AJCPNWX4SLZRP9SW 405
 Anatomic Pathology / Chronic Hypersensitivity Pneumonitis Histopathologic Analysis of Sixteen Autopsy Cases of Chronic Hypersensitivity Pneumonitis and Comparison With Idiopathic Pulmonary Fibrosis/Usual
Anatomic Pathology / Chronic Hypersensitivity Pneumonitis Histopathologic Analysis of Sixteen Autopsy Cases of Chronic Hypersensitivity Pneumonitis and Comparison With Idiopathic Pulmonary Fibrosis/Usual
Beyond a consensus classification for idiopathic interstitial pneumonias: progress and controversies
 Histopathology 2009, 54, 90 103. DOI: 10.1111/j.1365-2559.2008.03173.x REVIEW Beyond a consensus classification for idiopathic interstitial pneumonias: progress and controversies Jeffrey L Myers & Anna-Luise
Histopathology 2009, 54, 90 103. DOI: 10.1111/j.1365-2559.2008.03173.x REVIEW Beyond a consensus classification for idiopathic interstitial pneumonias: progress and controversies Jeffrey L Myers & Anna-Luise
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines
 Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT
 Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Diagnostic challenges in IPF
 Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Parenchymal, Interstitial i (Restrictive) i and Vascular Diseases
 Pulmonary Diseases: Structure-Function Correlation II Parenchymal, Interstitial i (Restrictive) i and Vascular Diseases Alain C. Borczuk, M.D. Dept of Pathology Pulmonary Diseases: Structure-Function Correlation
Pulmonary Diseases: Structure-Function Correlation II Parenchymal, Interstitial i (Restrictive) i and Vascular Diseases Alain C. Borczuk, M.D. Dept of Pathology Pulmonary Diseases: Structure-Function Correlation
The crazy-paving pattern: A radiological-pathological correlated and illustrated overview
 The crazy-paving pattern: A radiological-pathological correlated and illustrated overview Poster No.: C-0827 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: W. F. M. De Wever, J. Coolen,
The crazy-paving pattern: A radiological-pathological correlated and illustrated overview Poster No.: C-0827 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: W. F. M. De Wever, J. Coolen,
Overview of Idiopathic Pulmonary Fibrosis: Diagnosis and Therapy
 Overview of Idiopathic Pulmonary Fibrosis: Diagnosis and Therapy Jeff Swigris, DO, MS Director, ILD Program National Jewish Health Disclosures Speaker - Boehringer Ingelheim and Genentech Objectives Describe
Overview of Idiopathic Pulmonary Fibrosis: Diagnosis and Therapy Jeff Swigris, DO, MS Director, ILD Program National Jewish Health Disclosures Speaker - Boehringer Ingelheim and Genentech Objectives Describe
Imaging: how to recognise idiopathic pulmonary fibrosis
 REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
Chronic hypersensitivity pneumonitis in Japan: A nationwide epidemiologic survey
 Environmental and occupational disorders Chronic hypersensitivity pneumonitis in Japan: A nationwide epidemiologic survey Yasuyuki Yoshizawa, MD, a Yoshio Ohtani, MD, a Hiroshi Hayakawa, MD, b Atsuhiko
Environmental and occupational disorders Chronic hypersensitivity pneumonitis in Japan: A nationwide epidemiologic survey Yasuyuki Yoshizawa, MD, a Yoshio Ohtani, MD, a Hiroshi Hayakawa, MD, b Atsuhiko
Diffuse interstitial lung diseases (DILDs) are a heterogeneous group of non-neoplastic, noninfectious
 Focused Issue of This Month Diagnostic Approaches to Diffuse Interstitial Lung Diseases Dong Soon Kim, MD Department of Pulmonary and Critical Care Medicine, University of Ulsan College of Medicine E -
Focused Issue of This Month Diagnostic Approaches to Diffuse Interstitial Lung Diseases Dong Soon Kim, MD Department of Pulmonary and Critical Care Medicine, University of Ulsan College of Medicine E -
Unpaid scientific collaborator & advisor with Veracyte, Inc.
 Diagnosis and Classification of Idiopathic Interstitial Pneumonias: Role of Histopathology in the Golden Age of Consensus Jeffrey L. Myers, M.D. A. James French Professor of Diagnostic Pathology Vice Chair
Diagnosis and Classification of Idiopathic Interstitial Pneumonias: Role of Histopathology in the Golden Age of Consensus Jeffrey L. Myers, M.D. A. James French Professor of Diagnostic Pathology Vice Chair
Atopic Pulmonary Disease: Findings on Thoracic Imaging
 July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
How to identify interstitial pneumonias.
 How to identify interstitial pneumonias. Poster No.: C-0804 Congress: ECR 2014 Type: Educational Exhibit Authors: S. claret loaiza, M. C. Cañete Moslero, R. Carreño Gonzalez, C. de la Torre; Malaga/ES
How to identify interstitial pneumonias. Poster No.: C-0804 Congress: ECR 2014 Type: Educational Exhibit Authors: S. claret loaiza, M. C. Cañete Moslero, R. Carreño Gonzalez, C. de la Torre; Malaga/ES
INVITED REVIEW SERIES: PULMONARY FIBROSIS SERIES EDITORS: MARTIN KOLB AND GERARD COX
 INVITED REVIEW SERIES: PULMONARY FIBROSIS SERIES EDITORS: MARTIN KOLB AND GERARD COX Diagnosing fibrotic lung disease: When is high-resolution computed tomography sufficient to make a diagnosis of idiopathic
INVITED REVIEW SERIES: PULMONARY FIBROSIS SERIES EDITORS: MARTIN KOLB AND GERARD COX Diagnosing fibrotic lung disease: When is high-resolution computed tomography sufficient to make a diagnosis of idiopathic
Key words: CT scanners; interstitial lung diseases; polymyositis-dermatomyositis; x-ray
 Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
INTERSTITIAL LUNG DISEASE Dr. Zulqarnain Ashraf
 Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Manish Powari Regional Training Day 10/12/2014
 Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Lung Allograft Dysfunction
 Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Dr.kassim.m.sultan F.R.C.P
 Dr.kassim.m.sultan F.R.C.P inflammatory disorder of the lung, involving alveolar walls and terminal airways, that is induced, in a susceptible host, by repeated inhalation of a variety of organic agents.
Dr.kassim.m.sultan F.R.C.P inflammatory disorder of the lung, involving alveolar walls and terminal airways, that is induced, in a susceptible host, by repeated inhalation of a variety of organic agents.
The radiological differential diagnosis of the UIP pattern
 5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
ARTICLE IN PRESS. Ahuva Grubstein a, Daniele Bendayan b, Ithak Schactman c, Maya Cohen a, David Shitrit b, Mordechai R. Kramer b,
 Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
IPF: Epidemiologia e stato dell arte
 IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
Hypersensitivity pneumonitis (HP) is an immunologically. Inhalation Provocation Tests in Chronic Bird Fancier s Lung*
 Inhalation Provocation Tests in Chronic Bird Fancier s Lung* Yoshio Ohtani, MD; Kaoru Kojima, MD; Yuki Sumi, MD; Megumi Sawada, MD; Naohiko Inase, MD; Shuji Miyake, MD; Yasuyuki Yoshizawa, MD, PhD, FCCP
Inhalation Provocation Tests in Chronic Bird Fancier s Lung* Yoshio Ohtani, MD; Kaoru Kojima, MD; Yuki Sumi, MD; Megumi Sawada, MD; Naohiko Inase, MD; Shuji Miyake, MD; Yasuyuki Yoshizawa, MD, PhD, FCCP
Idiopathic interstitial pneumonias (IIPs) are a group of
 SYMPOSIA C. Isabela S. Silva, MD, PhD and Nestor L. Müller, MD, PhD Abstract: The idiopathic interstitial pneumonias (IIPs) are a group of diffuse parenchymal lung diseases of unknown etiology characterized
SYMPOSIA C. Isabela S. Silva, MD, PhD and Nestor L. Müller, MD, PhD Abstract: The idiopathic interstitial pneumonias (IIPs) are a group of diffuse parenchymal lung diseases of unknown etiology characterized
Imaging Small Airways Diseases: Not Just Air trapping. Eric J. Stern MD University of Washington
 Imaging Small Airways Diseases: Not Just Air trapping Eric J. Stern MD University of Washington What we are discussing SAD classification SAD imaging with MDCT emphasis What is a small airway? Airway with
Imaging Small Airways Diseases: Not Just Air trapping Eric J. Stern MD University of Washington What we are discussing SAD classification SAD imaging with MDCT emphasis What is a small airway? Airway with
Idiopathic Pulmonary Fibrosis: The Importance of Qualitative and Quantitative Phenotyping
 Idiopathic Pulmonary Fibrosis: The Importance of Qualitative and Quantitative Phenotyping K. R. Flaherty Division of Pulmonary and Critical Care Medicine, University of Michigan Health System, Ann Arbor,
Idiopathic Pulmonary Fibrosis: The Importance of Qualitative and Quantitative Phenotyping K. R. Flaherty Division of Pulmonary and Critical Care Medicine, University of Michigan Health System, Ann Arbor,
Careful histopathological evaluation has shown the traditionally clinical diagnosis of
 Demystifying Idiopathic Interstitial Pneumonia Harold R. Collard, MD; Talmadge E. King, Jr, MD REVIEW ARTICLE Careful histopathological evaluation has shown the traditionally clinical diagnosis of idiopathic
Demystifying Idiopathic Interstitial Pneumonia Harold R. Collard, MD; Talmadge E. King, Jr, MD REVIEW ARTICLE Careful histopathological evaluation has shown the traditionally clinical diagnosis of idiopathic
Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings
 Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings Poster No.: C-2358 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Cuartero Revilla, M. Nogueras Carrasco, P. Olmedilla
Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings Poster No.: C-2358 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Cuartero Revilla, M. Nogueras Carrasco, P. Olmedilla
Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients
 Respiratory Medicine (2008) 102, 307 312 Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients Michelle R. Aerni a, Robert Vassallo a,, Jeffrey L. Myers b, Rebecca M.
Respiratory Medicine (2008) 102, 307 312 Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients Michelle R. Aerni a, Robert Vassallo a,, Jeffrey L. Myers b, Rebecca M.
224a Pulmonary Pathology: New and Evolving Concepts, Diagnostic Dilemmas and Controversies (Part 1- Cases) Donald Guinee Jr, MD William Travis MD
 224a Pulmonary Pathology: New and Evolving Concepts, Diagnostic Dilemmas and Controversies (Part 1- Cases) Donald Guinee Jr, MD William Travis MD 2011 Annual Meeting Las Vegas, NV AMERICAN SOCIETY FOR
224a Pulmonary Pathology: New and Evolving Concepts, Diagnostic Dilemmas and Controversies (Part 1- Cases) Donald Guinee Jr, MD William Travis MD 2011 Annual Meeting Las Vegas, NV AMERICAN SOCIETY FOR
Epidemiology and classification of smoking related interstitial lung diseases
 Epidemiology and classification of smoking related interstitial lung diseases Šterclová M. Department of Respiratory Diseases, Thomayer Hospital, Prague, Czech Republic Supported by an IGA Grant No G 1207
Epidemiology and classification of smoking related interstitial lung diseases Šterclová M. Department of Respiratory Diseases, Thomayer Hospital, Prague, Czech Republic Supported by an IGA Grant No G 1207
Asbestosis: diagnosis and attribution criteria. Eduardo Algranti Serviço de Medicina FUNDACENTRO
 Asbestosis: diagnosis and attribution criteria Eduardo Algranti Serviço de Medicina FUNDACENTRO Asbestosis A declining disease in developed countries Most cases of asbestosis are due to occupational exposure
Asbestosis: diagnosis and attribution criteria Eduardo Algranti Serviço de Medicina FUNDACENTRO Asbestosis A declining disease in developed countries Most cases of asbestosis are due to occupational exposure
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
Chronic Interstitial (Restrictive) Lung Disease
 Chronic Interstitial (Restrictive) Lung Disease Fibrosing Usual interstitial pneumonia (idiopathic pulmonary fibrosis) IPF/UIP Nonspecific interstitial pneumonia(nsip) Cryptogenic organizing pneumonia(cop)
Chronic Interstitial (Restrictive) Lung Disease Fibrosing Usual interstitial pneumonia (idiopathic pulmonary fibrosis) IPF/UIP Nonspecific interstitial pneumonia(nsip) Cryptogenic organizing pneumonia(cop)
DIAGNOSTIC NOTE TEMPLATE
 DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
* * APPROACH TO NON- NEOPLASTIC LUNG DISEASE IN TRANSBRONCHIAL AND SURGICAL BIOPSIES. Financial Disclosures: NONE. BIOPSY TECHNIQUES Bronchoscopic
 APPROACH TO NON- NEOPLASTIC LUNG DISEASE IN TRANSBRONCHIAL AND SURGICAL BIOPSIES Thomas V. Colby, M.D. Mayo Clinic Arizona Geraldine C. Zeiler Professor of Cytopathology Mayo Clinic Arizona Financial Disclosures:
APPROACH TO NON- NEOPLASTIC LUNG DISEASE IN TRANSBRONCHIAL AND SURGICAL BIOPSIES Thomas V. Colby, M.D. Mayo Clinic Arizona Geraldine C. Zeiler Professor of Cytopathology Mayo Clinic Arizona Financial Disclosures:
The concept of respiratory bronchiolitis/interstitial lung
 Respiratory Bronchiolitis/Interstitial Lung Disease Fibrosis, Pulmonary Function, and Evolving Concepts Andrew Churg, MD; Nestor L. Müller, MD, PhD; Joanne L. Wright, MD Context. The concept of respiratory
Respiratory Bronchiolitis/Interstitial Lung Disease Fibrosis, Pulmonary Function, and Evolving Concepts Andrew Churg, MD; Nestor L. Müller, MD, PhD; Joanne L. Wright, MD Context. The concept of respiratory
Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis
 Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis JULIE A. BJORAKER, JAY H. RYU, MARK K. EDWIN, JEFFREY L. MYERS, HENRY D. TAZELAAR, DARRELL R. SCHROEDER, and KENNETH
Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis JULIE A. BJORAKER, JAY H. RYU, MARK K. EDWIN, JEFFREY L. MYERS, HENRY D. TAZELAAR, DARRELL R. SCHROEDER, and KENNETH
HRCT in Diffuse Interstitial Lung Disease Steps in High Resolution CT Diagnosis. Where are the lymphatics? Anatomic distribution
 Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Idiopathic Pulmonary of Care
 Chapter 6.1 Living Medical etextbook A Digital Tool at the Point of Care From Projects In Knowledge Pulmonology Idiopathic Pulmonary Fibrosis @Point of Care IPF Case Study: Typical Presentation, Role of
Chapter 6.1 Living Medical etextbook A Digital Tool at the Point of Care From Projects In Knowledge Pulmonology Idiopathic Pulmonary Fibrosis @Point of Care IPF Case Study: Typical Presentation, Role of
CLEARING THE AIR ON DIFFUSE PARENCHYMAL (INTERSTITIAL) LUNG DISEASE (ILD)
 CLEARING THE AIR ON DIFFUSE PARENCHYMAL (INTERSTITIAL) LUNG DISEASE (ILD) David Northrop MBA, RRT Assistant Director of Respiratory Therapy Services The University of Kansas Health System Clinical Assistant
CLEARING THE AIR ON DIFFUSE PARENCHYMAL (INTERSTITIAL) LUNG DISEASE (ILD) David Northrop MBA, RRT Assistant Director of Respiratory Therapy Services The University of Kansas Health System Clinical Assistant
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
Chronic Cough Due to Chronic Interstitial Pulmonary Diseases. ACCP Evidence-Based Clinical Practice Guidelines
 Chronic Cough Due to Chronic Interstitial Pulmonary Diseases ACCP Evidence-Based Clinical Practice Guidelines Kevin K. Brown, MD, FCCP Objectives: To review the role of chronic interstitial pulmonary disease
Chronic Cough Due to Chronic Interstitial Pulmonary Diseases ACCP Evidence-Based Clinical Practice Guidelines Kevin K. Brown, MD, FCCP Objectives: To review the role of chronic interstitial pulmonary disease
In medicine, the term overlap is very common, to the extent that there is even a
 Case Report Payam Mehrian (MD) 1 Ali Cheraghvandi (MD) 2 Atousa Droudnia (PhD) 3 Firouzeh Talischi (MD) 4 Saeid Fallah Tafti (MD) *5 Shahram Kahkouee (MD) 6 Hamidreza Jamaati (MD) 7 1. Pediatric Respiratory
Case Report Payam Mehrian (MD) 1 Ali Cheraghvandi (MD) 2 Atousa Droudnia (PhD) 3 Firouzeh Talischi (MD) 4 Saeid Fallah Tafti (MD) *5 Shahram Kahkouee (MD) 6 Hamidreza Jamaati (MD) 7 1. Pediatric Respiratory
Lung CT: Part 2, The Interstitial Pneumonias Clinical, Histologic, and CT Manifestations
 Integrative Imaging Review Ferguson and Berkowitz CT of Interstitial Pneumonia Integrative Imaging Review CME SAM Lung CT FOCUS ON: Emma C. Ferguson 1 Eugene A. Berkowitz 2 Ferguson EC, Berkowitz EA Keywords:
Integrative Imaging Review Ferguson and Berkowitz CT of Interstitial Pneumonia Integrative Imaging Review CME SAM Lung CT FOCUS ON: Emma C. Ferguson 1 Eugene A. Berkowitz 2 Ferguson EC, Berkowitz EA Keywords:
Diagnostic Approach to Advanced Fibrotic Interstitial Lung Disease. Bringing Together Clinical, Radiologic, and Histologic Clues
 Diagnostic Approach to Advanced Fibrotic Interstitial Lung Disease Bringing Together Clinical, Radiologic, and Histologic Clues Brandon T. Larsen, MD, PhD; Maxwell L. Smith, MD; Brett M. Elicker, MD; Jessica
Diagnostic Approach to Advanced Fibrotic Interstitial Lung Disease Bringing Together Clinical, Radiologic, and Histologic Clues Brandon T. Larsen, MD, PhD; Maxwell L. Smith, MD; Brett M. Elicker, MD; Jessica
pulmonary and critical care pearls
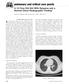 pulmonary and critical care pearls A 12-Year-Old Girl With Dyspnea and a Normal Chest Radiographic Finding* Kristin B. Highland, MD; and Patrick A. Flume, MD, FCCP (CHEST 2001; 120:1372 1376) A 12-year-old
pulmonary and critical care pearls A 12-Year-Old Girl With Dyspnea and a Normal Chest Radiographic Finding* Kristin B. Highland, MD; and Patrick A. Flume, MD, FCCP (CHEST 2001; 120:1372 1376) A 12-year-old
Radiologic pathologic discordance in biopsy-proven usual interstitial pneumonia
 ERJ Express. Published on February 25, 2016 as doi: 10.1183/13993003.01680-2015 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Radiologic pathologic discordance in biopsy-proven usual interstitial pneumonia
ERJ Express. Published on February 25, 2016 as doi: 10.1183/13993003.01680-2015 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Radiologic pathologic discordance in biopsy-proven usual interstitial pneumonia
Nontuberculous Mycobacterial Lung Disease
 Non-TB Mycobacterial Disease Jeffrey P. Kanne, MD Nontuberculous Mycobacterial Lung Disease Jeffrey P. Kanne, M.D. Consultant Disclosures Perceptive Informatics Royalties (book author) Amirsys, Inc. Wolters
Non-TB Mycobacterial Disease Jeffrey P. Kanne, MD Nontuberculous Mycobacterial Lung Disease Jeffrey P. Kanne, M.D. Consultant Disclosures Perceptive Informatics Royalties (book author) Amirsys, Inc. Wolters
