Northumbria Healthcare NHS Foundation Trust. Bronchiectasis. Issued by Respiratory Medicine
|
|
|
- Lindsey Golden
- 5 years ago
- Views:
Transcription
1 Northumbria Healthcare NHS Foundation Trust Bronchiectasis Issued by Respiratory Medicine
2 The aim of this booklet is to help you manage your bronchiectasis. It contains information which you should find helpful, but is not intended to be an exhaustive guide. Living with bronchiectasis can be difficult and there is a lot to think about and remember. This leaflet will also help you know what to do if you have a flare-up. A flare-up is called an exacerbation, and is a time when your symptoms get worse. Each exacerbation has an effect on your general health. What is bronchiectasis? Air is carried in and out of the lungs by a series of branching tubes called bronchi. These bronchi contain tiny glands which produce a small amount of mucus which keep the airways moist and healthy and trap dust and germs which are breathed in. The mucus is then swept away to the back of the throat by tiny hairs that line the airway called cilia. In bronchiectasis these hairs are damaged causing mucus and bacteria to build up. In bronchiectasis there is also a permanent widening of one or more of the airways. Extra mucus tends to form and pool in these areas which can be difficult to cough up. As a result people are more prone to infections which cause further inflammation and can lead to further damage. The extent of bronchiectasis can vary greatly. Some people may only have one area of the lung that is affected, others may have many. As the affected parts of the airway become damaged and inflamed, extra mucus is formed which is more difficult to clear. The airways also become more floppy and liable to collapse inward which may affect the airflow to the surrounding areas. The surrounding lung tissue may also be affected. 1
3 What causes bronchiectasis? The cause is not always clear and in about half of cases there is no obvious cause. Some conditions which affect the airways can cause bronchiectasis. These include: Severe lung infections such as tuberculosis, whooping cough, pneumonia and measles Some joint conditions such as rheumatoid arthritis Underlying genetic conditions such as cystic fibrosis, where the mucus in the airways is too thick. This is usually discovered in childhood Inhaling foreign bodies such as peanuts can damage the airways Regurgitated acid from the stomach which is then inhaled can also damage the airways, although this is rare A reduced immunity to infection by a lack of antibodies Some chronic lung conditions such as asthma 2
4 What are the symptoms of bronchiectasis? People with bronchiectasis often cough up a lot of sputum (phlegm) every day, which is usually yellow / green in colour, but some people only cough up sputum when unwell. Bad breath may also be a problem as the sputum can have an unpleasant smell. Sometime the sputum can be bloodstained due to tiny blood vessels breaking in the airways. You may also have problems with breathing and be quite wheezy. You may also feel tired and unwell and have a loss of appetite. Many people with bronchiectasis also have chronic infection of the nasal sinuses and a constant runny nose. Recurrent chest infections exacerbations or flare-ups are very common because an inflamed airway with extra mucus that is not cleared is ideal for bacteria to grow and multiply. Sputum turns more green/yellow when infected. If the amount of phlegm increases or the colour changes from your normal, this usually indicates an infection. The severity of symptoms from bronchiectasis varies greatly. Some people have only mild symptoms with a cough that comes and goes from time to time with the occasional chest infection. At the other extreme some people have severe symptoms with continuous symptoms of infection. Most people with bronchiectasis fall somewhere between these two extremes. 3
5 What tests may I have? A high resolution CT scan is used to diagnose bronchiectasis. This is a special X-ray which looks at the lungs in much more detail than a chest X-ray and can tell us how severe the bronchiectasis is. It is a painless test. Other tests include: Breathing ( lung function ) tests to help determine how well your lungs are working. Sputum analysis will tell us what bacteria are present and help guide antibiotic treatment. Blood tests will help try and find out what is causing the bronchiectasis, although in 50% of people we never find an actual cause. How is it treated? Although bronchiectasis cannot be cured, the majority of people have mild disease and there are a variety of treatment options available for all. These aim to try and break the cycle of repeated infections and lung damage. Your doctor will advise some of the following treatments for your bronchiectasis and potential side effects of the treatments will be discussed with you. Which treatments are given depends in part on how severe your condition is and your individual circumstances. One size does not fit all. 4
6 These are the main ways bronchiectasis is treated: Physiotherapy It is very important that you are able to clear your airways/lungs of phlegm on a daily basis to reduce your coughing, risk of infections and improve your everyday life. You will be referred to a physiotherapist to discuss the best way of doing this. The physiotherapist will ask you questions about your symptoms and your phlegm, and then discuss the options of different methods to help you remove the phlegm from your lungs. The physiotherapist will help you choose the airway clearance technique that is most suited to you and advise how often, how long, and in what position you should do the technique. Exercise (even going for a walk) is very beneficial for people with bronchiectasis. The physiotherapist will discuss exercise with you, and ways to help improve your ability to exercise. If you are breathless during daily activities then the physiotherapist can teach you ways to manage your breathlessness. Sometimes a specialised exercise programme (pulmonary rehabilitation) will be recommended to improve fitness with the aim of improving quality of life. Some people are also troubled by incontinence (leaking) of urine when coughing. This can be embarrassing or difficult to cope with in everyday life. The physiotherapist may be able to teach you some exercises to improve this. 5
7 Antibiotics Antibiotics are the main way of treating bacterial infections which people with bronchiectasis will have from time to time. A change in the colour of your sputum to green and feeling unwell usually indicates that you have a chest infection and you should put a sputum sample in to your doctor s surgery to help work out the best antibiotic for you to have. It is a good idea to have a spare sputum container at home so you can promptly provide a sputum for culture at the start of an infection. Your GP surgery will be able to provide one as can the hospital when you attend for your appointment. An antibiotic treatment regime can be created in order to limit the frequency and severity of exacerbations. Antibiotics can be taken in a number of different ways: orally (as a tablet that is swallowed) intravenously (a liquid injected into a vein) or inhaled with a nebuliser (a device that converts liquid into mist so that it can be breathed in). Chest infections may return quickly once you stop taking antibiotics. Some people may be advised to take antibiotics regularly to prevent infections from developing. And to reduce the amount of sputum coughed day to day. Occasionally it is recommended for people with more severe bronchiectasis to have regular antibiotics through a nebuliser. This is a way of giving high doses of antibiotics into the airways with only small amounts getting into the body. This reduces the problem of side-effects. This approach is most often used for people who grow a bacterium called Pseudomonas in their sputum. 6
8 Inhalers Sometimes inhalers are prescribed for people with bronchiectasis to try and reduce swelling and narrowing of the airways and to help cough, phlegm and breathlessness. Your doctor or nurse will help you to find the right combination of medication that will help maximise your quality of life. Nasal sprays These can help if you have a sinus infection or runny nose. Steroid tablets Sometimes steroids tablets eg. Prednisolone are recommended for people with bronchiectasis. These are usually given for one to two weeks to treat an exacerbation. The aim of them is to reduce airway swelling and help breathlessness and wheeze. They are not suitable for everyone. 7
9 Treatment of any associated disease / the underlying cause Stopping smoking If you smoke this will make your symptoms and lungs worse, so we strongly encourage you to try and stop. We can help you with this as we know it is hard. Vaccinations As with anyone with chronic lung disease we would encourage you to have the pneumonia vaccine, which only needs to be given once, and a yearly flu vaccine. Your GP surgery will be able to organise the vaccines for you, and usually run vaccination programmes in the autumn. Surgery In the past, before we had the antibiotics we have now, surgery was a common treatment for bronchiectasis, although did not tend to cure it. Surgery is only now recommended in exceptional circumstances. How do I know when an exacerbation (flare-up) is on the way? Although the aims of managing bronchiectasis are to try and reduce the number of exacerbations and your day to day symptoms, you will get exacerbations from time to time. It is important to spot one early, and know what to do. If you have three or more of the following symptoms lasting more than 24 hours then this probably means you have an exacerbation or worsening of your bronchiectasis: 8
10 Increased cough for more than 24 hours Increased breathlessness and / or wheeze for more than 24 hours Increased sputum volume or change in colour to yellow or green Chest pain which increases with coughing or taking deep breath Coughing up blood What do I do when an exacerbation happens? In the event of an exacerbation: If you have a rescue pack of antibiotics at home please start taking them, after providing a sputum sample (which you should take to the GP surgery). If you do not have a rescue pack of antibiotics at home please make an appointment to see your GP straight away and take a sputum sample with you to the appointment if possible. If, despite taking your antibiotics you continue to feel worse, or you do not feel any better after the two week course please contact your GP or one of the Respiratory Nurse Specialists (contact numbers below). 9
11 What can go wrong? Complications which can happen are: Coughing blood (haemoptysis). Although coughing up blood is very common in people with bronchiectasis, and rarely requires specific treatment, there are other important causes. It would be advisable for you to seek medical help if you notice blood in your phlegm for the first time, or if it has been a problem before with infections, and does not settle with antibiotics. Infection being spread by the blood to other areas of the body and a lung abscess. Both of these are rare. Useful websites Contacts For further advice please ring the Respiratory Nurse specialists: Wansbeck General Hospital North Tyneside General Hospital Hexham General Hospital
12 PIN 597/V1 Review date: February 2016
Bronchiectasis. What is bronchiectasis? What causes bronchiectasis?
 This factsheet explains what bronchiectasis is, what causes it, and how it is diagnosed and managed. More detailed information is available on the Bronchiectasis Patient Priorities website: www.europeanlunginfo.org/bronchiectasis
This factsheet explains what bronchiectasis is, what causes it, and how it is diagnosed and managed. More detailed information is available on the Bronchiectasis Patient Priorities website: www.europeanlunginfo.org/bronchiectasis
Bronchiectasis. Information for patients Therapy Services - Surgical
 Bronchiectasis Information for patients Therapy Services - Surgical The aim of this booklet is to offer you practical suggestions for making the most of your lungs and coping with bronchiectasis. Contents
Bronchiectasis Information for patients Therapy Services - Surgical The aim of this booklet is to offer you practical suggestions for making the most of your lungs and coping with bronchiectasis. Contents
Chronic Obstructive Pulmonary Disease
 Page 1 of 5 Chronic Obstructive Pulmonary Disease Chronic Obstructive Pulmonary Disease (COPD) is an 'umbrella' term for people with chronic bronchitis, emphysema, or both. With COPD the airflow to the
Page 1 of 5 Chronic Obstructive Pulmonary Disease Chronic Obstructive Pulmonary Disease (COPD) is an 'umbrella' term for people with chronic bronchitis, emphysema, or both. With COPD the airflow to the
Bronchiectasis action plan
 University Teaching Trust Bronchiectasis action plan Turnberg Building Respiratory Medicine 0161 206 1604 All Rights Reserved 2016. Document for issue as handout. Name: Date of Birth: Hospital Number:
University Teaching Trust Bronchiectasis action plan Turnberg Building Respiratory Medicine 0161 206 1604 All Rights Reserved 2016. Document for issue as handout. Name: Date of Birth: Hospital Number:
Chronic Obstructive Pulmonary Disease (COPD) Self-management plan
 Chronic Obstructive Pulmonary Disease (COPD) Self-management plan Respiratory Respiratory Nurses Royal Lancaster Infirmary & Westmorland General Hospital 01524 583608 Furness General Hospital 01229 403584
Chronic Obstructive Pulmonary Disease (COPD) Self-management plan Respiratory Respiratory Nurses Royal Lancaster Infirmary & Westmorland General Hospital 01524 583608 Furness General Hospital 01229 403584
Your COPD action plan
 Your COPD action plan Patient name: Better Breathing 0161 206 3159 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: MED24(17). Review date: July 2019 Your COPD Action Plan This
Your COPD action plan Patient name: Better Breathing 0161 206 3159 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: MED24(17). Review date: July 2019 Your COPD Action Plan This
Self-management plan for COPD
 Sheffield Clinical Commissioning Group Sheffield Teaching Hospitals NHS Foundation Trust Self-management plan for COPD This is your personal management plan The aim of the plan is to help you have better
Sheffield Clinical Commissioning Group Sheffield Teaching Hospitals NHS Foundation Trust Self-management plan for COPD This is your personal management plan The aim of the plan is to help you have better
Chronic Obstructive Pulmonary Disease, shortened to COPD, is an umbrella term for a group of conditions which cause long-term damage to the airways.
 10 Common QuESTIonS AbouT CoPD Chronic Obstructive Pulmonary Disease, shortened to COPD, is an umbrella term for a group of conditions which cause long-term damage to the airways. COPD includes: chronic
10 Common QuESTIonS AbouT CoPD Chronic Obstructive Pulmonary Disease, shortened to COPD, is an umbrella term for a group of conditions which cause long-term damage to the airways. COPD includes: chronic
Bronchitis. Anatomy of the Lungs The lungs allow us to fill our blood with oxygen. The oxygen we breathe is absorbed into our blood in the lungs.
 Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Sample blf.org.uk/copd
 Your COPD self-management plan blf.org.uk/copd Thank you to the people with lung conditions and leading health care professionals who helped to develop this plan. This resource has been developed in partnership
Your COPD self-management plan blf.org.uk/copd Thank you to the people with lung conditions and leading health care professionals who helped to develop this plan. This resource has been developed in partnership
Respiratory Patient Information Leaflet
 Bronchiectasis Self- Management Plan Respiratory Patient Information Leaflet Your Bronchiectasis Management Plan This plan is designed to help you manage your day to day symptoms and assist you in noticing
Bronchiectasis Self- Management Plan Respiratory Patient Information Leaflet Your Bronchiectasis Management Plan This plan is designed to help you manage your day to day symptoms and assist you in noticing
Signs and Symptoms of Chest Infections
 Signs and Symptoms of Chest Infections Chest infection If you have been diagnosed with a lung condition you can be at greater risk of contracting a chest infection. Chest infections can be caused by a
Signs and Symptoms of Chest Infections Chest infection If you have been diagnosed with a lung condition you can be at greater risk of contracting a chest infection. Chest infections can be caused by a
Living with bronchiectasis
 Living with bronchiectasis This information is about bronchiectasis in adults. It covers what bronchiectasis is, what the symptoms are, and how it is diagnosed and treated. Bronchiectasis is a long-term
Living with bronchiectasis This information is about bronchiectasis in adults. It covers what bronchiectasis is, what the symptoms are, and how it is diagnosed and treated. Bronchiectasis is a long-term
Chronic Obstructive Pulmonary Disease. Information about medication and an Action Plan to use if your condition gets worse due to an infection
 Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
Chronic Obstructive Pulmonary Disease (COPD)
 James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
information Chronic Obstructive Pulmonary Disease - COPD (1 of 5) What is COPD? What is going on in my lungs? What are the symptoms of COPD?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Patient Advice and Liaison Service (PALS) on 0800 374 208 email: pal.service@ salisbury.nhs.uk.
information If you need this information in another language or medium (audio, large print, etc) please contact the Patient Advice and Liaison Service (PALS) on 0800 374 208 email: pal.service@ salisbury.nhs.uk.
COPD COPD. C - Chronic O - Obstructive P - Pulmonary D - Disease OBJECTIVES
 COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
Living well with COPD
 This factsheet aims to show people with chronic obstructive pulmonary disease (COPD) and their friends and family how they can live a full life with this disease. What is COPD? COPD is a condition that
This factsheet aims to show people with chronic obstructive pulmonary disease (COPD) and their friends and family how they can live a full life with this disease. What is COPD? COPD is a condition that
Leflunomide Treatment Rheumatology Patient Information Leaflet
 Leflunomide Treatment Rheumatology Patient Information Leaflet Originator: Dr K Douglas Date: September 2011 Version: 2 Date for Review: September 2014 DGOH Ref No: DGOH/PIL/00217 Contact numbers If your
Leflunomide Treatment Rheumatology Patient Information Leaflet Originator: Dr K Douglas Date: September 2011 Version: 2 Date for Review: September 2014 DGOH Ref No: DGOH/PIL/00217 Contact numbers If your
Pneumonia. Trachea , The Patient Education Institute, Inc. id Last reviewed: 11/11/2017 1
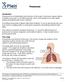 Pneumonia Introduction Pneumonia is an inflammation and infection of the lungs. Pneumonia causes millions of deaths every year. It can affect anybody, but is more dangerous to older adults, babies and
Pneumonia Introduction Pneumonia is an inflammation and infection of the lungs. Pneumonia causes millions of deaths every year. It can affect anybody, but is more dangerous to older adults, babies and
COPD and other lung conditions
 COPD and other lung conditions COPD COPD is an umbrella term used to describe a collection of lung diseases including emphysema and chronic bronchitis. C Chronic - long term condition O Obstructive - difficulty
COPD and other lung conditions COPD COPD is an umbrella term used to describe a collection of lung diseases including emphysema and chronic bronchitis. C Chronic - long term condition O Obstructive - difficulty
Looking after your lungs
 choking awareness! Looking after your lungs Useful information and top tips Colds and chest infections can be common, especially in the autumn and winter months. It is therefore very important that you
choking awareness! Looking after your lungs Useful information and top tips Colds and chest infections can be common, especially in the autumn and winter months. It is therefore very important that you
Asthma Action Plan and Education
 Acute Services Division Asthma Action Plan and Education Name: Date: Index What is Asthma? Page 4 Asthma Triggers Page 5 Peak Expiratory Flow Rate (Peak Flow) Page 6 Asthma Treatments Page 7 Asthma Action
Acute Services Division Asthma Action Plan and Education Name: Date: Index What is Asthma? Page 4 Asthma Triggers Page 5 Peak Expiratory Flow Rate (Peak Flow) Page 6 Asthma Treatments Page 7 Asthma Action
Northumbria Healthcare NHS Foundation Trust. Bronchoscopy and Endobronchial Ultrasound (EBUS) Issued by Respiratory Medicine
 Northumbria Healthcare NHS Foundation Trust Bronchoscopy and Endobronchial Ultrasound (EBUS) Issued by Respiratory Medicine Your appointment is on: Date Time Place 1 What is a bronchoscopy? A bronchoscopy
Northumbria Healthcare NHS Foundation Trust Bronchoscopy and Endobronchial Ultrasound (EBUS) Issued by Respiratory Medicine Your appointment is on: Date Time Place 1 What is a bronchoscopy? A bronchoscopy
Cough Assist. Information for patients, families and carers Therapy Services
 Cough Assist Information for patients, families and carers Therapy Services PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 16 Table of contents Why do I need a Cough
Cough Assist Information for patients, families and carers Therapy Services PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 16 Table of contents Why do I need a Cough
Cough Associated with Bronchitis
 Cough Associated with Bronchitis Bronchitis (bron-ki-tis) is a condition in which the bronchial tubes, the tubes that carry air to your lungs, become inflamed. People who have bronchitis often have a cough
Cough Associated with Bronchitis Bronchitis (bron-ki-tis) is a condition in which the bronchial tubes, the tubes that carry air to your lungs, become inflamed. People who have bronchitis often have a cough
Childhood Asthma / Wheeze
 Symptoms Asthma causes a range of breathing problems. These include wheezing, feeling of tightness in the lungs/chest and a cough (often in the night or early morning). The most serious of these is known
Symptoms Asthma causes a range of breathing problems. These include wheezing, feeling of tightness in the lungs/chest and a cough (often in the night or early morning). The most serious of these is known
NUCALA. mepolizumab. Patient Support
 NUCALA mepolizumab Patient Support This booklet has been developed by GSK UK/NLA/0007/15(1) Date of preparation: November 2016 INTRODUCTION This informative guide is for people who have been prescribed
NUCALA mepolizumab Patient Support This booklet has been developed by GSK UK/NLA/0007/15(1) Date of preparation: November 2016 INTRODUCTION This informative guide is for people who have been prescribed
Understanding Respiratory Illnesses
 Understanding Respiratory Illnesses Respiratory illnesses and the people you support Is a major cause of unplanned hospitalizations. Usually occur in fall and winter. It is important for you to Help people
Understanding Respiratory Illnesses Respiratory illnesses and the people you support Is a major cause of unplanned hospitalizations. Usually occur in fall and winter. It is important for you to Help people
Information Sheet. All Change
 All Change Dr Assad Hamid As most of our patients probably know by now Dr Assad Hamid will be leaving the practice at the end of December 2015. We are very pleased to say that Dr Hamid is not leaving Milton
All Change Dr Assad Hamid As most of our patients probably know by now Dr Assad Hamid will be leaving the practice at the end of December 2015. We are very pleased to say that Dr Hamid is not leaving Milton
Alpha-1-antitrypsin deficiency
 Alpha-1-antitrypsin deficiency This information is for people in the UK who have been diagnosed with alpha-1-antitrypsin deficiency, their families, friends and carers. It explains what alpha-1-antitrypsin
Alpha-1-antitrypsin deficiency This information is for people in the UK who have been diagnosed with alpha-1-antitrypsin deficiency, their families, friends and carers. It explains what alpha-1-antitrypsin
Bronchiectasis. Examples include: Viral infections (measles, adenovirus, influenza)
 Bronchiectasis What is Bronchiectasis? Bronchiectasis (pronounced bron-kee-ek'-tas-is) is a condition of the airways in the lungs. These airways (bronchial tubes) are tubelike structures that branch from
Bronchiectasis What is Bronchiectasis? Bronchiectasis (pronounced bron-kee-ek'-tas-is) is a condition of the airways in the lungs. These airways (bronchial tubes) are tubelike structures that branch from
Single Treatment of Radiotherapy to the Chest
 Patient Information Single Treatment of Radiotherapy to the Chest The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow G12 0YN This leaflet is for patients with lung cancer who will
Patient Information Single Treatment of Radiotherapy to the Chest The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow G12 0YN This leaflet is for patients with lung cancer who will
11.3 RESPIRATORY SYSTEM DISORDERS
 11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
Drug information. Baricitinib BARICITINIB. is used to treat rheumatoid arthritis. Helpline
 Drug information Baricitinib BARICITINIB is used to treat rheumatoid arthritis Helpline 0800 5200 520 1 Introduction Baricitinib is a drug that can help prevent your condition causing damage to your body.
Drug information Baricitinib BARICITINIB is used to treat rheumatoid arthritis Helpline 0800 5200 520 1 Introduction Baricitinib is a drug that can help prevent your condition causing damage to your body.
Guide to Cough Control. Physiotherapy Department Information for Patients
 Guide to Cough Control Physiotherapy Department Information for Patients i This leaflet is intended to provide information about: What happens when you cough Why cough control is important What is a good
Guide to Cough Control Physiotherapy Department Information for Patients i This leaflet is intended to provide information about: What happens when you cough Why cough control is important What is a good
COPD. The goals of COPD. about. you quit. If you. efforts to quit. Heart
 How Is COPD Treated? COPD has no cure yet. However, lifestyle changes and treatments can help you feel better, stay more active, and slow the progress of the disease. The goals of COPD treatment include:
How Is COPD Treated? COPD has no cure yet. However, lifestyle changes and treatments can help you feel better, stay more active, and slow the progress of the disease. The goals of COPD treatment include:
Dornase alfa (Pulmozyme ) for cystic fibrosis. Information for patients Pharmacy
 Dornase alfa (Pulmozyme ) for cystic fibrosis Information for patients Pharmacy page 2 of 8 This leaflet has been made to give you some more information to help you with your treatment. Please also read
Dornase alfa (Pulmozyme ) for cystic fibrosis Information for patients Pharmacy page 2 of 8 This leaflet has been made to give you some more information to help you with your treatment. Please also read
Understanding Respiratory Illnesses
 Understanding Respiratory Illnesses Respiratory illnesses can make you very sick. Some respiratory illnesses are not serious. A cold may make you feel sick for a few days, but you will get better. Other
Understanding Respiratory Illnesses Respiratory illnesses can make you very sick. Some respiratory illnesses are not serious. A cold may make you feel sick for a few days, but you will get better. Other
flu vaccination DRAFT The WINTER 2018/19 Who should have it and why Includes information for children and pregnant women mmunisation
 flu vaccination Who should have it and why The WINTER 2018/19 Includes information for children and pregnant women The flu vaccination 1 Winter 2018/19 Flu mmunisation Helping to protect everyone, every
flu vaccination Who should have it and why The WINTER 2018/19 Includes information for children and pregnant women The flu vaccination 1 Winter 2018/19 Flu mmunisation Helping to protect everyone, every
PATIENT INFORMATION Chronic Obstructive Pulmonary Disease (COPD) Fact Sheet
 PATIENT INFORMATION Chronic Obstructive Pulmonary Disease (COPD) Fact Sheet What is COPD? COPD is a general term, which includes the conditions chronic asthma, chronic bronchitis and emphysema. It is due
PATIENT INFORMATION Chronic Obstructive Pulmonary Disease (COPD) Fact Sheet What is COPD? COPD is a general term, which includes the conditions chronic asthma, chronic bronchitis and emphysema. It is due
Does this information apply to me? Information for the public Published: 1 June 2010 nice.org.uk
 Information for the public Published: 1 June 2010 nice.org.uk About this information NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Information for the public Published: 1 June 2010 nice.org.uk About this information NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Self-Management Plan for COPD
 Self-Management Plan for COPD This is your personal management plan. The aim of this plan is to help you have better control of your chronic obstructive pulmonary disease (COPD). It will enable you to
Self-Management Plan for COPD This is your personal management plan. The aim of this plan is to help you have better control of your chronic obstructive pulmonary disease (COPD). It will enable you to
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Methotrexate for inflammatory bowel disease: what you need to know
 Methotrexate for inflammatory bowel disease: what you need to know This leaflet aims to answer your questions about taking methotrexate for inflammatory bowel disease (IBD). If you have any questions or
Methotrexate for inflammatory bowel disease: what you need to know This leaflet aims to answer your questions about taking methotrexate for inflammatory bowel disease (IBD). If you have any questions or
Get Healthy Stay Healthy
 Asthma Management WHAT IS ASTHMA? Asthma causes swelling and inflammation in the breathing passages that lead to your lungs. When asthma flares up, the airways tighten and become narrower. This keeps the
Asthma Management WHAT IS ASTHMA? Asthma causes swelling and inflammation in the breathing passages that lead to your lungs. When asthma flares up, the airways tighten and become narrower. This keeps the
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Emphysema. Lungs The lungs help us breathe in oxygen and breathe out carbon dioxide. Everyone is born with 2 lungs: a right lung and a left lung.
 Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects millions of people worldwide. Emphysema involves damage to the air sacs in the lungs. This makes
Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects millions of people worldwide. Emphysema involves damage to the air sacs in the lungs. This makes
Ceritinib (Zykadia )
 (Ceritinib (Zykadia ) (Xalkori) Ceritinib (Zykadia ) This leaflet is offered as a guide to you and your family. Ceritinib (Zykadia ) is a type of anti-cancer treatment called a targeted therapy. The aim
(Ceritinib (Zykadia ) (Xalkori) Ceritinib (Zykadia ) This leaflet is offered as a guide to you and your family. Ceritinib (Zykadia ) is a type of anti-cancer treatment called a targeted therapy. The aim
Drug information. Tofacitinib TOFACITINIB. is used to treat rheumatoid arthritis and psoriatic arthritis. Helpline
 Drug information Tofacitinib TOFACITINIB is used to treat rheumatoid arthritis and psoriatic arthritis Helpline 0800 5200 520 1 Introduction Tofacitinib is a drug that can help prevent your condition causing
Drug information Tofacitinib TOFACITINIB is used to treat rheumatoid arthritis and psoriatic arthritis Helpline 0800 5200 520 1 Introduction Tofacitinib is a drug that can help prevent your condition causing
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Nebulised tobramycin for cystic fibrosis. Information for patients Pharmacy
 Nebulised tobramycin for cystic fibrosis Information for patients Pharmacy This leaflet has been made to give you some more information to help you with your treatment. Please also read the manufacturers
Nebulised tobramycin for cystic fibrosis Information for patients Pharmacy This leaflet has been made to give you some more information to help you with your treatment. Please also read the manufacturers
High dose (radical) radiotherapy to the lung or bronchus
 The Clatterbridge Cancer Centre NHS Foundation Trust High dose (radical) radiotherapy to the lung or bronchus Radiotherapy A guide for patients and carers Contents When radiotherapy is given... 1 Chemotherapy
The Clatterbridge Cancer Centre NHS Foundation Trust High dose (radical) radiotherapy to the lung or bronchus Radiotherapy A guide for patients and carers Contents When radiotherapy is given... 1 Chemotherapy
Drug information. Secukinumab SECUKINUMAB. is used to treat psoriatic arthritis and ankylosing spondylitis. Helpline
 Drug information Secukinumab SECUKINUMAB is used to treat psoriatic arthritis and ankylosing spondylitis Helpline 0800 5200 520 1 Introduction Secukinumab is a drug that can help prevent your condition
Drug information Secukinumab SECUKINUMAB is used to treat psoriatic arthritis and ankylosing spondylitis Helpline 0800 5200 520 1 Introduction Secukinumab is a drug that can help prevent your condition
Asthma Basic Facts. Staying safe and well with asthma. For people with asthma and their carers.
 Asthma Basic Facts Staying safe and well with asthma. For people with asthma and their carers. Asthma App Contact your local Asthma Foundation asthmaaustralia.org.au Breathing Breathing is how we get air
Asthma Basic Facts Staying safe and well with asthma. For people with asthma and their carers. Asthma App Contact your local Asthma Foundation asthmaaustralia.org.au Breathing Breathing is how we get air
Asthma 101. Introduction
 TRIGGERS Introduction Asthma is a chronic disease of the lungs that makes it difficult for people to breathe. Asthma is extremely common. About 20 million Americans have asthma. About 5,000 die each year
TRIGGERS Introduction Asthma is a chronic disease of the lungs that makes it difficult for people to breathe. Asthma is extremely common. About 20 million Americans have asthma. About 5,000 die each year
Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema.
 Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema. 2 LIVING WITH COPD You may have been told that you have COPD. It is a lung disease
Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema. 2 LIVING WITH COPD You may have been told that you have COPD. It is a lung disease
It is very common to get symptoms like cough, sore throat, runny nose and watery eyes. Usually when you
 A Publication of the National Center for Farmworker Health Let s Learn about Respiratory Infections It is very common to get symptoms like cough, sore throat, runny nose and watery eyes. Usually when you
A Publication of the National Center for Farmworker Health Let s Learn about Respiratory Infections It is very common to get symptoms like cough, sore throat, runny nose and watery eyes. Usually when you
Understanding Respiratory Illnesses
 Understanding Respiratory Illnesses Respiratory illnesses can make you very sick. Some respiratory illnesses are not serious. A cold may make you feel sick for a few days, but you will get better. Other
Understanding Respiratory Illnesses Respiratory illnesses can make you very sick. Some respiratory illnesses are not serious. A cold may make you feel sick for a few days, but you will get better. Other
A Patient s Guide to Chronic Obstructive Pulmonary Disease (COPD)
 A Patient s Guide to Chronic Obstructive Pulmonary Disease (COPD) Table of Contents What is COPD? 2 How the Lungs Work 2 Lungs with Chronic Bronchitis 3 Lungs with Emphysema 4 Causes of COPD 4 COPD Symptoms
A Patient s Guide to Chronic Obstructive Pulmonary Disease (COPD) Table of Contents What is COPD? 2 How the Lungs Work 2 Lungs with Chronic Bronchitis 3 Lungs with Emphysema 4 Causes of COPD 4 COPD Symptoms
Asthma in Children & Young People Advice for parents/carers
 Asthma in Children & Young People Advice for parents/carers Nursing & Patient Services Children s Services This leaflet has been designed to give you important information about your child s condition,
Asthma in Children & Young People Advice for parents/carers Nursing & Patient Services Children s Services This leaflet has been designed to give you important information about your child s condition,
Adult Asthma My Days of Living in Tension with Asthma are Over!
 Published on: 9 Jul 2014 Adult Asthma My Days of Living in Tension with Asthma are Over! Introduction This is a recent picture, taken when we went on a family picnic. We climbed up this big hill and I
Published on: 9 Jul 2014 Adult Asthma My Days of Living in Tension with Asthma are Over! Introduction This is a recent picture, taken when we went on a family picnic. We climbed up this big hill and I
A cough can be acute, subacute, or chronic, depending on how long it lasts.
 What Is? A cough is a natural reflex that protects your lungs. ing helps clear your airways of lung irritants, such as smoke and mucus (a slimy substance). This helps prevent infections. A cough also can
What Is? A cough is a natural reflex that protects your lungs. ing helps clear your airways of lung irritants, such as smoke and mucus (a slimy substance). This helps prevent infections. A cough also can
Self-Management Plan for COPD
 Self-Management Plan for COPD This is your personal management plan. The aim of this plan is to help you have better control of your chronic obstructive pulmonary disease (COPD). It will enable you to
Self-Management Plan for COPD This is your personal management plan. The aim of this plan is to help you have better control of your chronic obstructive pulmonary disease (COPD). It will enable you to
flu vaccination The Who should have it and why WINTER 2017/18 Includes information for children and pregnant women mmunisation in England in 2017/18
 flu WINTER 2017/18 The vaccination Who should have it and why Includes information for children and pregnant women Flu mmunisation in England in 2017/18 The flu vaccination 1 Winter 2017/18 Helping to
flu WINTER 2017/18 The vaccination Who should have it and why Includes information for children and pregnant women Flu mmunisation in England in 2017/18 The flu vaccination 1 Winter 2017/18 Helping to
UNDERSTANDING & MANAGING
 UNDERSTANDING & MANAGING YOUR CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)* *Includes chronic bronchitis, emphysema, or both Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any
UNDERSTANDING & MANAGING YOUR CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)* *Includes chronic bronchitis, emphysema, or both Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any
Non-invasive ventilation (also called bi-level or BIPAP)
 Patient information service Bristol Royal Infirmary Non-invasive ventilation (also called bi-level or BIPAP) Respecting everyone Embracing change Recognising success Working together Our hospitals. 2 Why
Patient information service Bristol Royal Infirmary Non-invasive ventilation (also called bi-level or BIPAP) Respecting everyone Embracing change Recognising success Working together Our hospitals. 2 Why
Glossary of Asthma Terms
 HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
A patient educational resource provided by Boehringer Ingelheim Pharmaceuticals, Inc.
 Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets its disease management products and services. A patient educational resource provided
Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets its disease management products and services. A patient educational resource provided
Bevacizumab (Avastin ) treatment for Neurofibromatosis Type 2 (NF2) Information for patients
 Bevacizumab (Avastin ) treatment for Neurofibromatosis Type 2 (NF2) Information for patients This booklet has been written to give you more information about bevacizumab (commonly known as Avastin). This
Bevacizumab (Avastin ) treatment for Neurofibromatosis Type 2 (NF2) Information for patients This booklet has been written to give you more information about bevacizumab (commonly known as Avastin). This
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
Flu. is a killer. If you are at risk you should have your free flu vaccination every year.
 Flu is a killer. If you are at risk you should have your free flu vaccination every year. What is flu? Flu spreads easily and can cause serious illnesses which need to be treated in hospital. It is not
Flu is a killer. If you are at risk you should have your free flu vaccination every year. What is flu? Flu spreads easily and can cause serious illnesses which need to be treated in hospital. It is not
We ALL appreciate your PATIENCE in waiting.
 Maureen Goulden Health Care Assistant and Gina Donnelly Receptionist. As you may know Maureen has been a member of the surgery for 23 years and Gina for 11 years. Both have been loyal, hardworking members
Maureen Goulden Health Care Assistant and Gina Donnelly Receptionist. As you may know Maureen has been a member of the surgery for 23 years and Gina for 11 years. Both have been loyal, hardworking members
Protecting your child against flu
 Protecting your child against flu Information for parents Flu immunisation in England Flu mmunisation Helping to protect everyone, every winter Flu vaccine is offered free each year to most: children aged
Protecting your child against flu Information for parents Flu immunisation in England Flu mmunisation Helping to protect everyone, every winter Flu vaccine is offered free each year to most: children aged
Because we care about your health
 Contact us For information on Trust services see www.awp.nhs.uk PALS To make a comment, raise a concern or make a complaint, please contact the Trust s Patient Advice and Liaison Service (PALS). Smoking
Contact us For information on Trust services see www.awp.nhs.uk PALS To make a comment, raise a concern or make a complaint, please contact the Trust s Patient Advice and Liaison Service (PALS). Smoking
Gemcitabine and carboplatin (Lung)
 Gemcitabine and carboplatin (Lung) Gemcitabine and carboplatin (Lung) This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy may
Gemcitabine and carboplatin (Lung) Gemcitabine and carboplatin (Lung) This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy may
Pulmonary Rehabilitation Information Leaflet
 Community Respiratory Services Luton Treatment Centre Vestry Close Luton LU1 1AR Tel: 0333 405 3159 Notes Pulmonary Rehabilitation Information Leaflet We hope you have enjoyed the pulmonary rehabilitation
Community Respiratory Services Luton Treatment Centre Vestry Close Luton LU1 1AR Tel: 0333 405 3159 Notes Pulmonary Rehabilitation Information Leaflet We hope you have enjoyed the pulmonary rehabilitation
Infliximab infusion for patients with Crohn s disease. GI Unit Patient Information Leaflet
 Infliximab infusion for patients with Crohn s disease GI Unit Patient Information Leaflet What is Infliximab? Infliximab (Remicade) is a medication that is used for patients with Crohn s disease whose
Infliximab infusion for patients with Crohn s disease GI Unit Patient Information Leaflet What is Infliximab? Infliximab (Remicade) is a medication that is used for patients with Crohn s disease whose
Living with COPD. Chronic bronchitis. Emphysema
 Living with COPD This information is for people with chronic obstructive pulmonary disease (COPD), their families, friends and carers. It provides advice and information about COPD, including what the
Living with COPD This information is for people with chronic obstructive pulmonary disease (COPD), their families, friends and carers. It provides advice and information about COPD, including what the
Asthma. & Older Adults. A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS
 Asthma & Older Adults A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS what is Asthma? Asthma is a disease of the airways, the small tubes which carry air in and out
Asthma & Older Adults A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS what is Asthma? Asthma is a disease of the airways, the small tubes which carry air in and out
CHILDREN S SERVICES. Patient information Leaflet BRONCHIOLITIS
 CHILDREN S SERVICES Patient information Leaflet BRONCHIOLITIS Sept 2014 INTRODUCTION This leaflet aims to help you understand bronchiolitis, how to make your child comfortable and when to contact for emergency
CHILDREN S SERVICES Patient information Leaflet BRONCHIOLITIS Sept 2014 INTRODUCTION This leaflet aims to help you understand bronchiolitis, how to make your child comfortable and when to contact for emergency
Patient information from BMJ
 Patient information from BMJ Last published: Dec 02, 2016 Lung cancer (non-small-cell) It can be devastating to find out that you or someone close to you has lung cancer. You will have to make some important
Patient information from BMJ Last published: Dec 02, 2016 Lung cancer (non-small-cell) It can be devastating to find out that you or someone close to you has lung cancer. You will have to make some important
Your Chemotherapy. The Common side effects are:
 1 10 This information leaflet is designed to help you understand more about the treatment you have opted to undertake. You will be receiving both chemotherapy and radiotherapy that work together to treat
1 10 This information leaflet is designed to help you understand more about the treatment you have opted to undertake. You will be receiving both chemotherapy and radiotherapy that work together to treat
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
Rheumatology Department Patient Information Leaflet
 Methotrexate Rheumatology Department Patient Information Leaflet Please keep this information in a safe place Introduction This leaflet provides information about methotrexate which will be discussed with
Methotrexate Rheumatology Department Patient Information Leaflet Please keep this information in a safe place Introduction This leaflet provides information about methotrexate which will be discussed with
Physiotherapy and cystic fibrosis
 Physiotherapy and cystic fibrosis A guide to transition to adult services Information for patients Therapy Services - Surgical Sheffield Adult Cystic Fibrosis Centre The aim of this booklet is to offer
Physiotherapy and cystic fibrosis A guide to transition to adult services Information for patients Therapy Services - Surgical Sheffield Adult Cystic Fibrosis Centre The aim of this booklet is to offer
Gemcitabine and carboplatin (Breast)
 Gemcitabine and carboplatin (Breast) Gemcitabine and carboplatin (Breast) This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy
Gemcitabine and carboplatin (Breast) Gemcitabine and carboplatin (Breast) This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy
Methotrexate in Inflammatory Bowel Disease. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Methotrexate in Inflammatory Bowel Disease An information guide Methotrexate in Inflammatory Bowel Disease Your doctor is planning to start
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Methotrexate in Inflammatory Bowel Disease An information guide Methotrexate in Inflammatory Bowel Disease Your doctor is planning to start
Northumbria Healthcare NHS Foundation Trust. Your guide to discharge from the breast clinic. Issued by the Breast Team
 Northumbria Healthcare NHS Foundation Trust Your guide to discharge from the breast clinic Issued by the Breast Team This leaflet gives you information about your discharge from the Breast Clinic. Why
Northumbria Healthcare NHS Foundation Trust Your guide to discharge from the breast clinic Issued by the Breast Team This leaflet gives you information about your discharge from the Breast Clinic. Why
PNEUMONIA. Your Treatment and Recovery
 PNEUMONIA Your Treatment and Recovery Understanding Pneumonia Symptoms of Pneumonia Do you feel feverish and tired, with a cough that won t go away? If so, you may have pneumonia. This is a lung infection
PNEUMONIA Your Treatment and Recovery Understanding Pneumonia Symptoms of Pneumonia Do you feel feverish and tired, with a cough that won t go away? If so, you may have pneumonia. This is a lung infection
What Is This Module About? What Will You Learn From This Module?
 What Is This Module About? Breathing is very important and natural to man. Every breath means life. Do you know what system of the human body helps us breathe? What elements in air does man need to live?
What Is This Module About? Breathing is very important and natural to man. Every breath means life. Do you know what system of the human body helps us breathe? What elements in air does man need to live?
PIDS AND RESPIRATORY DISORDERS
 PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
Bronchiectasis in Adults - Suspected
 Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Gemcitabine and Cisplatin (urology)
 Gemcitabine and Cisplatin Gemcitabine and Cisplatin (urology) This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy may reduce
Gemcitabine and Cisplatin Gemcitabine and Cisplatin (urology) This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy may reduce
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
Influenza. What Is Influenza?
 Flu is usually a mild, but uncomfortable disease. You can treat it yourself by staying home and drinking plenty of fluids. What Is?, often just called the flu, is the most common disease in the world,
Flu is usually a mild, but uncomfortable disease. You can treat it yourself by staying home and drinking plenty of fluids. What Is?, often just called the flu, is the most common disease in the world,
INFORMATION FOR PATIENTS AND FAMILIES. CT guided lung biopsy (under local anaesthetic)
 INFORMATION FOR PATIENTS AND FAMILIES CT guided lung biopsy (under local anaesthetic) This leaflet provides information about the test you are due to have. It should replace the discussions you have with
INFORMATION FOR PATIENTS AND FAMILIES CT guided lung biopsy (under local anaesthetic) This leaflet provides information about the test you are due to have. It should replace the discussions you have with
Living with COPD: 5 steps to better lung health
 Living with COPD: 5 steps to better lung health Breathe better Feel good Do more Name: Date: COPD or chronic obstructive pulmonary disease mainly affects your lungs and how well you can breathe, but it
Living with COPD: 5 steps to better lung health Breathe better Feel good Do more Name: Date: COPD or chronic obstructive pulmonary disease mainly affects your lungs and how well you can breathe, but it
