Nebulisers comparison with inhaled tobramycin in young children with cystic fibrosis
|
|
|
- Carmel Brooks
- 6 years ago
- Views:
Transcription
1 Journal of Cystic Fibrosis 6 (2007) Nebulisers comparison with inhaled tobramycin in young children with cystic fibrosis Aurélie Clavel a, Audrey Boulaméry b, Emmanuelle Bosdure a, Caroline Luc a, André Lanteaume c, Guillaume Gorincour d, Nathalie Stremler-Lebel e, Jacques Sarles e, Véronique Andrieu f, Jean-Christophe Dubus a,c,e, a Department of Pediatrics, Timone University Pediatric Hospital, Marseille, France b Department of Pharmacology, Timone University Hospital, Marseille, France c EA3287, IFR125, Faculty of Medicine, Marseille, Marseille, France d Department of Pediatric Radiology, Timone University Pediatric Hospital, Marseille, France e Pediatric Cystic Fibrosis Treatment Centre, Timone University Pediatric Hospital, Marseille, France f Department of Pharmacy, Faculty of Pharmacy, Marseille, France Received 4 October 2005; received in revised form 6 March 2006; accepted 11 June 2006 Available online 12 July 2006 Abstract Background: This randomised cross-over pilot study was undertaken in 10 cystic fibrosis children aged 10 to 63 months to describe lung absorption of tobramycin delivered by the PariLC+/PariTurboboyN (Pari GmbH) and the disposable NL9M/AtomisorBoxPlus (Diffusion Technique Française) nebulising systems. Methods: Each child inhaled 300 mg tobramycin delivered with one or the other apparatus via a facemask in two separate and standardised sessions. Urine was collected for 6 h. Tobramycin concentrations determined by immunoprecipitation were expressed in mg per g of creatinine and compared by a Wilcoxon test for matched pairs. The influences of age, weight and Brasfield score on this parameter were evaluated by correlation tests, and those of sex, previous nebulisation treatment, and crying or coughing were evaluated by Student's t-test. Results: The amount of tobramycin measured in urines was low and variable. Median values for urinary tobramycin concentration were 47.6 mg/g ( ) with the PariLC+ and 42.6 mg/g ( ) with the NL9M (p=0.6). PariLC+ delivered tobramycin in 22 min and NL9M in 12 min (p = 0.005). Crying or coughing dramatically reduced the amount of tobramycin collected. Conclusion: This pilot study shows that evaluation of nebulisers based on tobramycin renal excretion is feasible in young children with cystic fibrosis European Cystic Fibrosis Society. Published by Elsevier B.V. All rights reserved. Keywords: Child; Cystic fibrosis; Nebulisation; Pulmonary deposition; Tobramycin 1. Introduction This study was promoted by the Assistance Publique Hôpitaux de Marseille, without sponsorship by the pharmaceutical or medical industries. Corresponding author. Unité de Médecine Infantile, CHU Timone- Enfants, Marseille Cedex 5, France. Tel.: ; fax: address: jean-christophe.dubus@ap-hm.fr (J.-C. Dubus). Bronchial infection with Pseudomonas aeruginosa is always serious in children with cystic fibrosis. According to the Observatoire National de la Mucoviscidose, 45% of patients with cystic fibrosis are P. aeruginosa carriers in France, and almost 25% of patients aged 0 4 years have been infected at least once [1]. In patients diagnosed by neonatal screening, 43% of children aged less than 7 years in /$ - see front matter 2006 European Cystic Fibrosis Society. Published by Elsevier B.V. All rights reserved. doi: /j.jcf
2 138 A. Clavel et al. / Journal of Cystic Fibrosis 6 (2007) Australia [2] and up to 29% of those aged less than 6 months in the USA are affected by P. aeruginosa [3]. The risk factors for early infection with P. aeruginosa in these patients are female sex, homozygous ΔF508 genotype, and isolation of Staphylococcus aureus [4]. In one study [5], neonatal screening itself was more frequently associated with P. aeruginosa infection than in those who were not screened (80% vs 60%, p = 0.02), with lower ages at onset of infection (3.01 years vs 6.04 years, p=0.007), possibly because of earlier attendance at treatment centres. Antibiotic treatment must be aggressive in early infection with P. aeruginosa in order to have any possibility of eradication [3]. Several treatment regimens have been proposed, but most of them include the use of nebulised aminoglycosides, either in combination or alternating with other antibiotics [2,6 8]. Nebulisation is not easy in young children. The effectiveness depends on the pulmonary deposition achieved. In practice, deposition depends on the patient (e.g. age, respiratory function), on the drug nebulised and its physicochemical properties, on the apparatus used (which mainly determines the particle size), and on the inhalation technique [9]; the younger the child, the poorer the lung deposition. The few scintigraphic lung deposition studies undertaken in infants with cystic fibrosis show that only 1.3 to 2% of the nebulised drug reaches the lungs, that is about 10-fold lower than in adults [10,11]. Deposition can be further reduced by bronchial obstruction, inhalation without a facemask in young children (or mouthpiece in older children), crying and screaming. Tobi (Chiron Laboratories, Paris, France) is the only aminoglycoside officially registered for use by nebulisation. It is mainly used in cystic fibrosis for bronchial infection with P. aeruginosa, both during early infection and for chronic colonisation [12]. The usual long term dose is 300 mg morning and evening daily during alternate months. The apparatus dedicated for delivering Tobi is the PariLC+ jet nebuliser combined with various compressors as the PulmoAide (DeVilbiss, USA) or the new PariTurboBoyN (PariGmbH, Munchen, Germany), more potent than the PulmoAide and proposed by PariGmbH. Although administration of Tobi with this equipment is effective in children with cystic fibrosis under 6 years of age [8,13], the main disadvantage is the need for careful washing, disinfection and sterilization of the nebuliser after each use. In a recent study we have conducted in nebulisation in cystic fibrosis, 47% of families considered that treatment by nebulisation was difficult to administer on a daily basis and 84% considered that disposable apparatus would be very helpful [14]. The NL9M nebuliser (Diffusion Technique Française, Saint-Etienne, France) is a disposable jet nebuliser whose performance in vitro is comparable to that of the PariLC+ [15]. The aim of this study was to describe and explore the pulmonary deposition of 300 mg tobramycin by measuring renal excretion of this antibiotic delivered by these two nebulisers equipped with a facemask in children under 6 years of age with cystic fibrosis. 2. Materials and methods 2.1. Study subjects Inclusion criteria were: to have a cystic fibrosis (genetic mutations and 2 positive sweat tests), to be aged less than 6 years, to be regularly followed up in the Marseilles Cystic Fibrosis Treatment Centre, to have a clinically stable disease, to have a written consent for participation in the study from both parents. Exclusion criteria were inability to attend the Cystic Fibrosis Treatment Centre of the Timone University Pediatric Hospital twice in a month, patent bronchial infection at the time of inclusion, clinical bronchospasm, known hypersensitivity to aminoglycosides, and current treatment with Tobi. However, children who had received prior treatment with Tobi could be included if none had been received in the preceding week Study design This was a randomised cross-over pilot study, approved by the Ethics Committee of Aix-Marseille II, performed to describe and explore the pulmonary deposition by measuring renal excretion of tobramycin delivered by two different nebulising systems. Tobramycin delivery was done in children at two different sessions separated by at least a week and no longer than a month Methods Drugs and nebulisers The drug used was tobramycin (Tobi, 300 mg/5 ml solution for inhalation) because, like other aminoglycosides, tobramycin is considered to be a pharmacological tracer of pulmonary deposition [16,17]. In fact, tobramycin is only absorbed by the lungs, without any metabolisation. All the tobramycin found in the blood or urine thus directly reflects pulmonary absorption. Our primary end point was the urinary tobramycin concentration. The PariLC+/PariTurboBoyN combination (CE 0123) was compared with the NL9M/AtomisorBoxPlus combination (CE 0459), both with paediatric facemasks (Fig. 1). Both are breath-enhanced jet nebulisers. The facemask for the PariLC+ has to be held in place on the child's face during nebulisation, whereas that of the NL9M is kept in place by an elastic strap adjusted to the size of the child's head Experimental protocol After obtaining clinical history, all children were given a complete clinical examination, during which anthropometric measurements, pulmonary auscultation, pulsed oxygen saturation rate, and resting respiratory rate measured over 1 min were recorded. Brasfield radiological scoring [18] was
3 A. Clavel et al. / Journal of Cystic Fibrosis 6 (2007) A second nebulisation session took place under the same conditions between 1 week and 1 month after the first to test the second nebuliser. Fig. 1. PariLC+ nebuliser (top: Pari GmbH, Munchen, Germany) and NL9M nebuliser (bottom: Diffusion Technique Française, Saint-Etienne, France) with their respective facemasks. undertaken on the child's most recent chest X-ray performed within the preceding 3 months. The children were asked to pass urine before beginning the session, and Tobi inhalation was standardised as much as possible. The child was seated on the lap of his mother/ father with his head upright. One 300 mg ampoule of tobramycin was placed directly in the reservoir of the randomly selected nebuliser (PariLC+ or NL9M). Nebulisation was begun only when the facemask was in position, meanwhile monitoring oxygen saturation by pulsed oxymetry. Respiration was required to be as calm as possible. The nebuliser was maintained in an upright position, and nebulisation was continuously monitored by two or three of the investigators and was timed. Respiratory rate, chest auscultation, crying, screaming and coughing were noted at 0, 1, 2, 5, 10 and 15 min, as well as any other side-effect, and oxygen saturation. As recommended by Chiron Laboratories for the use of Tobi, nebulisation was stopped when the apparatus appeared to be no longer delivering the drug, as suspected by the absence of visible aerosol production and the noise's change. The apparatus was stripped down for cleaning according to current requirements at the end of nebulisation. The remaining solution in the reservoir was aspirated by a syringe and the residual volume was noted. Hydration was maintained by normal alimentation combined with administration of 100 ml water in a bottle or cup just after completing nebulisation. Urine was collected for 6 h. The children urinated directly into a receptacle or a pouch (e.g. Urinocol ) according to age. Urine was transferred to a sterile flask maintained at +4 C after each micturition. All micturitions obtained in 6 h were pooled and tobramycin concentration was then measured in fresh urines Measurement of urinary tobramycin concentrations Tobramycin concentrations are currently measured in our hospital using an immunoprecipitation method called PETINIA (particle enhanced turbidimetric inhibition immunoassay) using a RXL robot (Dade Behring, USA). As only the measurement of plasma levels of tobramycin has been validated by Dade Behring, the calibration curve for urinary measurements was calculated from the plasmatic curve. We validated urinary measurement by comparing several times the concentrations measured in 6 samples of known tobramycin concentrations (0.3, 1, 5, 10, 30, and 60 μg/ ml). The samples preparation was performed by adding tobramycin in fresh and tobramycin-free urine. The lower limit of quantification was 0.3 μg/ml. The accuracy (expressed as a coefficient of variation) was less than 15% at each of the 6 tobramycin concentrations and correlation coefficient was Reproducibility, also expressed as a coefficient of variation, was less than 5%. Measurements were performed on urinary samples stored at 4 C and bioassayed within 6 h after collection which is a situation daily observed for this analysis. Systematic measurement of urinary ph was also performed on all samples because the measurement method was valid only for ph between 5 and 8. Urinary creatinine was also measured Statistical analysis Because this study was a pilot study we have chosen arbitrary to enroll 10 children. Data are presented as median values with extremes. The amount of tobramycin collected was measured in urine collected over 6 h (mg/l) and then expressed as mg/g of urinary creatinine to limit intra-subject variations related to age or amount of urine collected. This ratio, reflecting in this study the lung absorption of tobramycin, was compared between nebulisers by Wilcoxon test for matched pairs. As no data were available on renal excretion of tobramycin in a young population of cystic fibrosis children, we had no definitive criteria to propose for proving similarity between both nebulisers. We postulated that more than a 15% difference in tobramycin/creatinine ratio between the two nebulisers would indicate non equivalence of the apparatuses. The influences of age, weight and Brasfield score on the tobramycin/creatinine ratio were evaluated by simple, non-parametric correlation tests. The influences of sex, previous use of a nebuliser and crying and/or coughing during the nebulisation session were evaluated by Student's t-test. A p value of less than 0.05 was considered to be statistically significant. 3. Results On the 16 eligible children of our Cystic Fibrosis Treatment Centre, 2 refused to participate to the study and
4 140 A. Clavel et al. / Journal of Cystic Fibrosis 6 (2007) Table 1 Clinical characteristics of the 10 children with cystic fibrosis Age (months) Sex Weight (kg) Height (cm) Shwachman Score Brasfield Score 10 F 9.3 (+1S.D.) 74 (+1S.D.) 95/100 2/25 Yes 16 M 13 (+2S.D.) 82 (+2S.D.) 95/100 0/25 Yes 17 M 10.1 ( 1S.D.) 75 ( 1S.D.) 95/100 0/25 No 23 M 11 ( 1S.D.) 83.5 ( 1S.D.) 90/100 4/25 Yes 33 M 10.8 ( 2S.D.) 87 ( 1S.D.) 90/100 1/25 No 39 F 12.5 ( 1S.D.) 88 ( 2S.D.) 95/100 1/25 Yes 46 M 12 ( 2S.D.) 93 ( 2S.D.) 80/100 6/25 No 49 M 13.2 ( 1S.D.) 94 ( 1S.D.) 90/100 1/25 No 57 F 15 ( 1S.D.) 100 ( 2S.D.) 80/100 5/25 Yes 63 F 16.5 ( 1S.D.) 111 normal 80/100 8/25 Yes M=male; F=female; S.D. =Standard deviation. Habituated to nebulisation 4 lived at more than 100 km distance from the hospital. The median age of the 10 remainder cystic fibrosis children (6 boys) was 35.3 months, range 10 to 63 months (Table 1). Median Shwachman score was 89/100 (80 95). All the children had experienced several bronchial infections since diagnosis, but the last sputum sample before initiating the study was sterile in 8 of the 10 children. Four children were currently being treated with nebulised tobramycin at home and 6 of 10 had already experienced nebulisation. The median Brasfield radiological score was 2.8/25 (0 8). Auscultation was normal for nine children, and the tenth had crackles during both nebulisation sessions. Measurement of respiratory rate revealed normal values for age, ranging from 40 per min in an infant of 23 months to 15 per min for a child of 57 months. Median pulsed oxymetry value before the nebulisation sessions began was 97% (94 100%). All the children completed the protocol. Two children had three nebulisation sessions instead of two, in one case because complete urine collections were impossible to collect, and in the other because the nebuliser was knocked over during the nebulisation process. No severe side-effect occurred. No hypoxaemia or wheezing episodes occurred during nebulisation. Monitoring respiratory rates did not reveal any variations during nebulisation, nor was there any difference between the two nebulisers. Median respiratory rate was 27.5 per min with the PariLC+ and 28.8 per min with the NL9M. Coughing or crying occurred during eight nebulisation sessions, four with each apparatus, and involved five children. Three had a slight cough (1 with the PariLC+, 1 with the NL9M and 1 with both), and two (the two youngest patients) cried throughout, in one case necessitating premature withdrawal from nebulisation with the PariLC+. Median duration of nebulisation was 22 min (13 28 min) for the PariLC+ and 12 min (10 19 min) for the NL9M (p=0.005). When the shortest period of 13 min in the case of the elective cessation of the session with the PariLC+ for continuous crying was not included, a 50% decrease was noted in duration with the NL9M. There was no significant difference between the PariLC+ and the NL9M in terms of median residual volume of tobramycin remaining in the nebulisation reservoir indicating that nearly the same volume of aerosol was available for inhalation with both nebulisers (0.83 ml, range 0.22 to 1.4, and 0.74 ml, range 0.42 to 1.7, respectively; p=0.87). Any relationship between residual volume and duration of nebulisation was observed in this study. Median diuresis over the 6 h was ml ( ml), and was similar for both nebulisers (124.9 ml for the PariLC+ and ml for the NL9M). The amount of tobramycin found in the urine was low, and varied considerably between children and even from one nebulisation session to another for the same child, from 0.13 to 7.70 mg/l (median of 2.6 mg for the PariLC+ and 2.2 mg for the NL9M; p=0.2). The same trend was found for the tobramycin/creatinine ratio (Fig. 2). As shown in Fig. 2, the inter-subjects variability was more important than the intrasubjects (or inter-nebulisers for a same child) variability. The ratio between subjects was highly variable from 6.3 mg/ g to mg/g, whereas in a same subject this ratio ranged from 1.2 to 41.4 mg/g. A 15% difference on this ratio between nebulisers was noted in 50% of the subjects. Median values for urinary tobramycin/creatinine concentration (Fig. 3) were Fig. 2. Individual ratio of tobramycin/creatinine obtained in 10 children with cystic fibrosis after inhaling 300 mg tobramycin with a PariLC+ and a NL9M nebuliser.
5 A. Clavel et al. / Journal of Cystic Fibrosis 6 (2007) Fig. 3. Median values of the ratio tobramycin/creatinine obtained in 10 children with cystic fibrosis after inhaling 300 mg tobramycin with a PariLC+ and a NL9M nebuliser mg/g ( ) with the PariLC+ and 42.6 mg/g ( ) with the NL9M (p=0.6). No influence of age, weight, Brasfield score or familiarity with nebulisation was revealed by the parameter measured with either apparatus. On the other hand, crying and/or coughing significantly reduced the amount of urinary tobramycin collected over 6 h (1 vs 3.8 mg; p = 0.03), but did not affect the ratio tobramycin/creatinine for both nebulisers (41.3 vs 51.8 mg/g for the PariLC+, p=0.43; and 26.0 vs 63.7 mg/g for the NL9M, p=0.11). When the nebulisation sessions with crying and/or coughing were omitted from the results, the median age of the children was 47.5 months in both groups, and the median urinary tobramycin concentrations were not significantly different between nebulisers (49.3 mg/g ( ) for the PariLC+ and 59.0 mg/g ( ) for the NL9M; p=0.52). 4. Discussion This randomised cross-over pilot study demonstrates that measuring renal excretion of tobramycin for comparing the pulmonary deposition obtained with two different nebulisers in children with cystic fibrosis aged less than 6 years is possible, but that the ratio tobramycin/creatinine in this age range is low and highly variable. There are many methods of studying pulmonary deposition of inhaled drugs, mainly based on in vitro, scintigraphic, pharmacokinetic and pharmacodynamic techniques [19]. Pulmonary scintigraphy is one of the most valuable methods but such studies are rare in children, particularly in the youngest ones, because of practical difficulties in view of problems such as irradiation. Pharmacokinetics studies measure the drug which is absorbed by the lung surface. They are usually based on the determination of the drug concentration in the plasma or urine. Such studies are difficult to perform. The main stumbling block is to measure all the drug absorbed both by the lungs and by the upper respiratory and gastro-intestinal tracts [19]. This can partly be avoided through maximum standardisation of the inhalation technique, by monitoring variations in urinary excretion and by using only drugs that are exclusively absorbed by the lungs. Tobramycin was chosen to compare the ability of the NL9M and Pari LC+ nebulisers to deliver drugs because it is one of the few drugs which is administered via the airways and it is only absorbed by the lungs without any metabolisation. Urinary excretion is thus total [17]. We preferred to express the amount of tobramycin collected per g of creatinine to limit intra-subject variations, without limiting inter-subject variability. After 300 mg tobramycin inhalation, peak serum concentration occurs in 1 h and then decreases progressively over 2 h reaching negligible levels after 4 h, even in young children with cystic fibrosis [13,20]. However, a long and variable terminal half life has been described after 600 mg tobramycin nebulisation in adults (mean 9.47 ± 3.28 h) [21]. In another study [17], 2 subjects out of 6 have detectable urinary tobramycin concentrations at or just above the limit of detection for each of the four 12-h collection intervals. These subjects were female and had the same pharmacokinetic profile with the 3 tobramycin doses tested (80, 160, and 320 mg) [17]. In our study, urinary concentration of tobramycin over 6 h probably does not correspond to the total amount of tobramycin absorbed by the lungs, but it was likely sufficient to make a comparison in a same child between the two nebulisation apparatuses, particularly when, as in our study, urine collections over 6 h were complete for all children. Moreover, it was really difficult to keep quiet young children equipped with a urine pouch for a longer time (total duration of the study including clinical examination, nebulisation session and urine collection was about 8 h). Because of the extreme difficulty to obtain several urine samples at fixed periods in young children without invasive methods, particularly in a same child on 2 different study days, tobramycin elimination curve has not been characterized, and our study cannot be considered as a true pharmacokinetic study. Some bias must be considered in our study. Firstly, it is difficult to standardise nebulisation techniques in young children (2 of the 10 children had to return for a third session for technical reasons, 2 others cried continuously), and it is difficult to standardise urine collection, the volume of which is variable according to the session and age. The latter problem can be overcome by expressing urinary tobramycin concentration as mg/g creatinine. In addition, the small study group reduces the power of the study, particularly as there were considerable variations in measurements from child to child. The design of the study fails to prove equivalence of both nebulisers as we have defined it, but a similar profile of tobramycin renal excretion for both nebulisers, PariLC+ and NL9M, is found in children under 6 years of age with cystic fibrosis. A nebulisation time half as long and a disposable equipment are great advantages for the NL9M/AtomisorBoxPlus combination with facemask. Indeed, these two elements facilitate the use of this
6 142 A. Clavel et al. / Journal of Cystic Fibrosis 6 (2007) nebulisation equipment and may probably encourage treatment compliance. On the other hand, we have to limit our enthusiastic conclusions firstly because toxicity, which has to be evaluated on plasma levels of tobramycin, has not been determined in this study, and secondly because a population of 10 patients is not enough to prove a real equivalence between the studied nebulisers. We are unable to precisely quantify the pulmonary deposition, but it was not the aim of this pilot study. However, lung absorption of tobramycin appears to be very low, and highly variable between subjects. Conversely, inter-nebulisers variability is less important. In contrast to results published with other nebulised drugs, sex, age and weight were not found to have any influence on lung absorption [22]. We were also unable to demonstrate any relationship between parameters of pulmonary absorption of tobramycin and Brasfield score, but our patients fortunately had low levels of respiratory involvement. It was more surprising that there was no correlation between the tobramycin/creatinine ratio and previous use of nebulised treatment at home, which might have supposed a positive effect of prior learning. On the other hand, a three- or fourfold decrease in urinary tobramycin concentration was noted with both nebulisers when there was crying and/or coughing. This might be explained by changes in the site of deposition of the drug in the body, with increased nasopharyngeal and gastro-intestinal deposition rather than pulmonary deposition [23]. Therefore, this result was not confirmed when tobramycin was expressed in mg per g of creatinine, maybe because only 10 children were explored. Therefore in view of these findings, it would seem preferable to perform nebulisation in the youngest children with rapid delivery equipment in order to achieve optimal pulmonary deposition, possibly when they are calm such as during sleep. In conclusion, this pilot study describes and explores the pulmonary deposition by measuring renal excretion of tobramycin delivered by two different nebulisers equipped with a facemask in cystic fibrosis children under 6 years. The main factor which influences the amount of drug delivered to the lungs in this study is the occurrence of crying and/or coughing during the nebulisation session. This suggests that it would be preferable to use rapid nebulisers in periods when young children are calm. Other studies, conducted with an appropriate number of young cystic fibrosis patients and based on renal excretion of tobramycin, could be particularly interesting by comparing the fast and disposable NL9M nebuliser to the new nebulisers using a vibrating membrane which deliver 150 mg of tobramycin in vitro in 3 min [24], although they may be less easy to disinfect. Acknowledgements We thank the children and their families for participating in the study and our nurses, Mrs Jocelyne Liguori and Ingrid Pfau, for their help to this work. This study was not sponsored by the industry nor pharmaceutical laboratories. References [1] Vaincre la mucoviscidose. Résultats préliminaires du rapport sur la situation de la mucoviscidose en France en org/publications/resultats_preliminaires_onm2003.pdf. [2] Nixon GM, Armstrong DS, Carzino R, Carlin JB, Olinsky A, Robertson CF, et al. Clinical outcome after early Pseudomonas aeruginosa infection in cystic fibrosis. J Pediatr 2001;138: [3] Li Z, Kosorok MR, Farrell PM, Laxova A, West SE, Green CG, et al. Longitudinal development of mucoid Pseudomonas aeruginosa infection and lung disease progression in children with cystic fibrosis. JAMA 2005;293: [4] Maselli JH, Sontag MK, Norris JM, MacKenzie T, Wagener JS, Accurso FJ. Risk factors for initial acquisition of Pseudomonas aeruginosa in children with cystic fibrosis identified by newborn screening. Pediatr Pulmonol 2003;36: [5] Farrell PM, Li Z, Kosorok MR, Laxova A, Green CG, Collins J, et al. Bronchopulmonary disease in children with cystic fibrosis after early or delayed diagnosis. Am J Respir Crit Care Med 2003;168: [6] Wiesemann HG, Steinkamp G, Ratjen F, Bauernfeind A, Przyklenk B, Doring G, et al. Placebo-controlled, double-blind, randomized study of aerosolized tobramycin for early treatment of Pseudomonas aeruginosa colonization in cystic fibrosis. Pediatr Pulmonol 1998; 25: [7] Ratjen F, Doring G, Nikolaizik WH. Effects of inhaled tobramycin on early Pseudomonas aeruginosa colonisation in patients with cystic fibrosis. Lancet 2001;358: [8] Gibson RL, Emerson J, McNamara S, Burns JL, Rosenfeld M, Yunker A, et al. Cystic Fibrosis Therapeutics Development Network Study Group. Significant microbiological effect of inhaled tobramycin in young children with cystic fibrosis. Am J Respir Crit Care Med 2003;167: [9] De Benedictis FM, Selvaggio D. Use of inhaler devices in pediatric asthma. Paediatr Drugs 2003;5: [10] Chua HL, Collis GG, Newbury AM, Chan K, Bower GD, Sly PD, et al. The influence of age on aerosol deposition in children with cystic fibrosis. Eur J Respir 1994;7: [11] Maloll J, Rattray S, Walker G, Cook D, Robertson CF. Aerosol deposition in infants with cystic fibrosis. Pediatr Pulmonol 1996; 21: [12] Cheer SM, Waugh J, Noble S. Inhaled tobramycin (TOBI): a review of its use in the management of Pseudomonas aeruginosa infections in patients with cystic fibrosis. Drugs 2003;63: [13] Rosenfeld M, Gibson R. Serum and lower respiratory tract drug concentrations after tobramycin inhalation in young children with cystic fibrosis. J Pediatr 2001;139: [14] Dubus JC, Kammerl A, Stremler-Lebel N, Luc C, Mély L, Chazalette JP, et al. Nébulisation et mucoviscidose: la pratique. Arch Pediatr 2004;11:767 [abstract]. [15] Vecellio None L, Grimbert D, Bordenave J, Benoit G, Furet Y, Fauroux B, et al. Residual gravimetric method to nebulizer output. J Aerosol Med 2004;17: [16] Dequin PF, Faurisson F, Lemarié E, Delatour F, Marchand S, Valat C, et al. Urinary excretion reflects lung deposition of aminoglycoside aerosols in cystic fibrosis. Eur Respir J 2001;18: [17] Asmus MJ, Stewart BA, Milavetz G, Teresi ME, Han SH, Wang D, et al. Tobramycin as a pharmacologic tracer to compare airway deposition from nebulizers. Pharmacotherapy 2002;22: [18] Brasfield D, Hicks G. Evaluation of scoring system of the chest radiography in cystic fibrosis. AJR 1980;134: [19] Chrystyn H. Standards for bioequivalence of inhaled products. Clin Pharmacokinet 1994;26:1 6.
7 A. Clavel et al. / Journal of Cystic Fibrosis 6 (2007) [20] Geller DE, Rosenfeld M, Waltz DA. Efficiency of pulmonary administration of tobramycin solution for inhalation in cystic fibrosis using an improved drug delivery system. Chest 2003;123: [21] Le Brun PP, Vinks AA, Touw DJ, Hekelaar N, Mannes GP, Brimicombe RW, et al. Can tobramycin inhalation be improved with a jet nebuliser? Ther Drug Monit 1999;21: [22] Coates AL, Allen PD, MacNeish CF, Ho SL, Lands LC. Effect of size and disease on estimated deposition of drugs administered using jet nebulization in children with cystic fibrosis. Chest 2001;119: [23] Amirav I, Balanov I. Nebuliser hood compared to mask in wheezy infants: aerosol therapy without tears. Arch Dis Child 2003; 88: [24] Knoch M, Keller M. The customised electric nebuliser: a new category of liquid aerosol drug delivery systems. Expert Opin Drug Deliv 2005;2:
Eradication regimens for early or recurrent Pseudomonas aeruginosa infection
 Eradication regimens for early or recurrent Pseudomonas aeruginosa infection The Leeds Method of Management. April, 2008. Cystic fibrosis and eradication therapy for early or recurrent Pseudomonas aeruginosa
Eradication regimens for early or recurrent Pseudomonas aeruginosa infection The Leeds Method of Management. April, 2008. Cystic fibrosis and eradication therapy for early or recurrent Pseudomonas aeruginosa
Bronchial reactions to the inhalation of high-dose tobramycin in cystic fibrosis
 Eur Respir J 2002; 20: 122 126 DOI: 10.1183/09031936.02.00264002 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Bronchial reactions to the
Eur Respir J 2002; 20: 122 126 DOI: 10.1183/09031936.02.00264002 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Bronchial reactions to the
Journal Club The ELITE Trial. Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010
 Journal Club The ELITE Trial Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010 Overview Journal article Title, journal, authors, funding Abstract Introduction
Journal Club The ELITE Trial Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010 Overview Journal article Title, journal, authors, funding Abstract Introduction
This letter is to notify you of recent changes to the PULMOZYME product monograph. Please note, additions/changes have been highlighted in yellow.
 April 9, 2015 Subject: Revised Product Monograph - PULMOZYME (dornase alfa) Dear Drug Information / Poison Control Centres, This letter is to notify you of recent changes to the PULMOZYME product monograph.
April 9, 2015 Subject: Revised Product Monograph - PULMOZYME (dornase alfa) Dear Drug Information / Poison Control Centres, This letter is to notify you of recent changes to the PULMOZYME product monograph.
Early Pseudomonas Infection Control (EPIC) Clinical Study. Overview for Families
 Early Pseudomonas Infection Control (EPIC) Clinical Study Overview for Families What is the EPIC Clinical Study? The EPIC Clinical Study Compares different treatments for children with CF who have just
Early Pseudomonas Infection Control (EPIC) Clinical Study Overview for Families What is the EPIC Clinical Study? The EPIC Clinical Study Compares different treatments for children with CF who have just
Choice of Nebulizer for Inhaled Tobramycin Treatment in Cystic Fibrosis
 Respiratory Drug Delivery 2010 Müllinger et al. Choice of Nebulizer for Inhaled Tobramycin Treatment in Cystic Fibrosis Bernhard Müllinger, 1 Thomas C. Topini, 2 Anna L. Valeri, 2 Juliane Gleske, 1 Philipp
Respiratory Drug Delivery 2010 Müllinger et al. Choice of Nebulizer for Inhaled Tobramycin Treatment in Cystic Fibrosis Bernhard Müllinger, 1 Thomas C. Topini, 2 Anna L. Valeri, 2 Juliane Gleske, 1 Philipp
The role of serum Pseudomonas aeruginosa antibodies in the diagnosis and follow-up of cystic fibrosis
 The Turkish Journal of Pediatrics 2013; 55: 50-57 Original The role of serum Pseudomonas aeruginosa antibodies in the diagnosis and follow-up of cystic fibrosis Deniz Doğru 1, Sevgi Pekcan 1, Ebru Yalçın
The Turkish Journal of Pediatrics 2013; 55: 50-57 Original The role of serum Pseudomonas aeruginosa antibodies in the diagnosis and follow-up of cystic fibrosis Deniz Doğru 1, Sevgi Pekcan 1, Ebru Yalçın
N.U.A.G.E.S: A survey of nebulisation practice in France with regard to ERS guidelines
 Respiratory Medicine (2007) 101, 2561 2565 SHORT COMMUNICATION N.U.A.G.E.S: A survey of nebulisation practice in France with regard to ERS guidelines M. de Monte a, J. Scruignec a, J.C. Dubus b,c, J.P.
Respiratory Medicine (2007) 101, 2561 2565 SHORT COMMUNICATION N.U.A.G.E.S: A survey of nebulisation practice in France with regard to ERS guidelines M. de Monte a, J. Scruignec a, J.C. Dubus b,c, J.P.
Appendix D Clinical specialist statement template
 Appendix D Colistimethate sodium powder and tobramycin powder for inhalation for the treatment of pseudomonas lung infection in cystic fibrosis Thank you for agreeing to give us a statement on your organisation
Appendix D Colistimethate sodium powder and tobramycin powder for inhalation for the treatment of pseudomonas lung infection in cystic fibrosis Thank you for agreeing to give us a statement on your organisation
4.6 Small airways disease
 4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
Citation for published version (APA): Westerman, E. M. (2009). Studies on antibiotic aerosols for inhalation in cystic fibrosis s.n.
 University of Groningen Studies on antibiotic aerosols for inhalation in cystic fibrosis Westerman, Elisabeth Mechteld IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF)
University of Groningen Studies on antibiotic aerosols for inhalation in cystic fibrosis Westerman, Elisabeth Mechteld IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF)
Pseudomonas aeruginosa eradication guideline
 SCOTTISH PAEDIATRIC CYSTIC FIBROSIS MCN Pseudomonas aeruginosa eradication guideline Date Created: 27 th June 2013 Date Approved by Steering Group: 30 th May 2014 Date of Review: 31 st May 2016 Lead Author:
SCOTTISH PAEDIATRIC CYSTIC FIBROSIS MCN Pseudomonas aeruginosa eradication guideline Date Created: 27 th June 2013 Date Approved by Steering Group: 30 th May 2014 Date of Review: 31 st May 2016 Lead Author:
CYSTIC FIBROSIS INPATIENT PROTOCOL PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES DEFINITIONS EQUIPMENT
 PURPOSE Physiotherapy role for inpatients with cystic fibrosis. POLICY STATEMENTS On admission to hospital all patients will be assessed by the physiotherapist within 24 hours. Physiotherapists have standing
PURPOSE Physiotherapy role for inpatients with cystic fibrosis. POLICY STATEMENTS On admission to hospital all patients will be assessed by the physiotherapist within 24 hours. Physiotherapists have standing
Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review)
 Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review) Ryan G, Mukhopadhyay S, Singh M This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review) Ryan G, Mukhopadhyay S, Singh M This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
without the permission of the author Not to be copied and distributed to others
 Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions
 CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Performing a Methacholine Challenge Test
 powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
Hypertonic Saline (7%) Administration Guideline (adults)
 Hypertonic Saline (7%) Administration Guideline (adults) Full Title of Guideline: Author (include email and role): Hypertonic Saline (7%) Administration Guideline for Practice (Adults) Clair Martin, Senior
Hypertonic Saline (7%) Administration Guideline (adults) Full Title of Guideline: Author (include email and role): Hypertonic Saline (7%) Administration Guideline for Practice (Adults) Clair Martin, Senior
ADASUVE (LOXAPINE) INHALATION POWDER. EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS
 ADASUVE (LOXAPINE) INHALATION POWDER EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS August2017 December 2012 PMR-JUN-2017-0017 ADASUVE Risk Evaluation and Mitigation Strategy (REMS) Education Program Content
ADASUVE (LOXAPINE) INHALATION POWDER EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS August2017 December 2012 PMR-JUN-2017-0017 ADASUVE Risk Evaluation and Mitigation Strategy (REMS) Education Program Content
Shared Care Guideline
 Shared Care Guideline Gentamicin for Nebulisation For the long term prophylaxis of chronic lung infections in non CF bronchiectasis Executive Summary Indication Nebulised gentamicin is indicated in patients
Shared Care Guideline Gentamicin for Nebulisation For the long term prophylaxis of chronic lung infections in non CF bronchiectasis Executive Summary Indication Nebulised gentamicin is indicated in patients
Eradication of early Pseudomonas aeruginosa infection
 Journal of Cystic Fibrosis 4 (2005) 49 54 www.elsevier.com/locate/jcf Eradication of early Pseudomonas aeruginosa infection N. Høiby a, *, B. Frederiksen b, T. Pressler b a Department of Clinical Microbiology
Journal of Cystic Fibrosis 4 (2005) 49 54 www.elsevier.com/locate/jcf Eradication of early Pseudomonas aeruginosa infection N. Høiby a, *, B. Frederiksen b, T. Pressler b a Department of Clinical Microbiology
CYSTIC FIBROSIS OBJECTIVES NO CONFLICT OF INTEREST TO DISCLOSE
 CYSTIC FIBROSIS Madhu Pendurthi MD MPH Staff Physician, Mercy Hospital Springfield, MO NO CONFLICT OF INTEREST TO DISCLOSE OBJECTIVES Epidemiology of Cystic Fibrosis (CF) Genetic basis and pathophysiology
CYSTIC FIBROSIS Madhu Pendurthi MD MPH Staff Physician, Mercy Hospital Springfield, MO NO CONFLICT OF INTEREST TO DISCLOSE OBJECTIVES Epidemiology of Cystic Fibrosis (CF) Genetic basis and pathophysiology
Eradication therapy for Pseudomonas aeruginosa colonization episodes in cystic fibrosis patients not chronically colonized by P.
 Journal of Cystic Fibrosis 12 (2013) 1 8 www.elsevier.com/locate/jcf Review Eradication therapy for Pseudomonas aeruginosa colonization episodes in cystic fibrosis patients not chronically colonized by
Journal of Cystic Fibrosis 12 (2013) 1 8 www.elsevier.com/locate/jcf Review Eradication therapy for Pseudomonas aeruginosa colonization episodes in cystic fibrosis patients not chronically colonized by
Chronic Stenotrophomonas maltophilia infection and mortality or lung transplantation in cystic fibrosis patients
 Journal of Cystic Fibrosis 12 (2013) 482 486 www.elsevier.com/locate/jcf Original Article Chronic Stenotrophomonas maltophilia infection and mortality or lung transplantation in cystic fibrosis patients
Journal of Cystic Fibrosis 12 (2013) 482 486 www.elsevier.com/locate/jcf Original Article Chronic Stenotrophomonas maltophilia infection and mortality or lung transplantation in cystic fibrosis patients
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1
 PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis
 Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
Nebulised tobramycin for cystic fibrosis. Information for patients Pharmacy
 Nebulised tobramycin for cystic fibrosis Information for patients Pharmacy This leaflet has been made to give you some more information to help you with your treatment. Please also read the manufacturers
Nebulised tobramycin for cystic fibrosis Information for patients Pharmacy This leaflet has been made to give you some more information to help you with your treatment. Please also read the manufacturers
Pulmonary exacerbations and clinical outcomes in a longitudinal cohort of infants and preschool children with cystic fibrosis
 Hoppe et al. BMC Pulmonary Medicine (2017) 17:188 DOI 10.1186/s12890-017-0546-8 RESEARCH ARTICLE Open Access Pulmonary exacerbations and clinical outcomes in a longitudinal cohort of infants and preschool
Hoppe et al. BMC Pulmonary Medicine (2017) 17:188 DOI 10.1186/s12890-017-0546-8 RESEARCH ARTICLE Open Access Pulmonary exacerbations and clinical outcomes in a longitudinal cohort of infants and preschool
TRANSPARENCY COMMITTEE OPINION. 15 October Date of Marketing Authorisation (national procedure): 16 April 1997, variation of 18 February 2008
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 October 2008 MERONEM 1 g, powder for solution for IV Injection Box of 10 vials (CIP: 387 830-6) Applicant: ASTRAZENECA
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 October 2008 MERONEM 1 g, powder for solution for IV Injection Box of 10 vials (CIP: 387 830-6) Applicant: ASTRAZENECA
Experience the Powder of Non-nebulized Pa Treatment
 For people 6 years and older with cystic fibrosis (CF), Pseudomonas aeruginosa (Pa), and FEV 1 25% to 80% predicted and who do not have Burkholderia cepacia. Experience the Powder of Non-nebulized Pa Treatment
For people 6 years and older with cystic fibrosis (CF), Pseudomonas aeruginosa (Pa), and FEV 1 25% to 80% predicted and who do not have Burkholderia cepacia. Experience the Powder of Non-nebulized Pa Treatment
TIP NO AEROSOLIZED DRUGS TECHNICAL INFORMATION PAPER NO PURPOSE.
 AEROSOLIZED DRUGS TECHNICAL INFORMATION PAPER NO. 56-088-0618 PURPOSE. Healthcare workers risk exposure to exhaled aerosolized drugs along with infectious airborne pathogens during administration and routine
AEROSOLIZED DRUGS TECHNICAL INFORMATION PAPER NO. 56-088-0618 PURPOSE. Healthcare workers risk exposure to exhaled aerosolized drugs along with infectious airborne pathogens during administration and routine
Air or oxygen as driving gas for nebulised salbutamol
 Archives of Disease in Childhood, 1988, 63, 9-94 Air or oxygen as driving gas for nebulised salbutamol J G A GLEESON, S GREEN, AND J F PRICE Paediatric Respiratory Laboratory, Department of Thoracic Medicine,
Archives of Disease in Childhood, 1988, 63, 9-94 Air or oxygen as driving gas for nebulised salbutamol J G A GLEESON, S GREEN, AND J F PRICE Paediatric Respiratory Laboratory, Department of Thoracic Medicine,
Latex Free. An affordable, easy to use, high density, small volume nebulizer with a breath enhanced design! Breath Enhanced High Density Jet Nebulizer
 Latex Free Breath Enhanced High Density Jet Nebulizer The NebuTech HDN nebulizer, a breath enhanced design, by Salter Labs is quickly becoming the product of choice for caregivers and patients alike. This
Latex Free Breath Enhanced High Density Jet Nebulizer The NebuTech HDN nebulizer, a breath enhanced design, by Salter Labs is quickly becoming the product of choice for caregivers and patients alike. This
Changes in the management of children with Cystic Fibrosis. Caroline Murphy & Deirdre O Donovan CF Nurses
 Changes in the management of children with Cystic Fibrosis Caroline Murphy & Deirdre O Donovan CF Nurses What Is Cystic Fibrosis? Cystic fibrosis (CF) is an inherited chronic disease that primarily affects
Changes in the management of children with Cystic Fibrosis Caroline Murphy & Deirdre O Donovan CF Nurses What Is Cystic Fibrosis? Cystic fibrosis (CF) is an inherited chronic disease that primarily affects
NIV and Aerosoltherapy
 NIV and Aerosoltherapy Workshop Jean-Bernard Michotte (Lausanne-CH) Simone Gambazza (Milano-IT) Jean-Bernard Michotte Haute Ecole de Santé Vaud, 1011 Lausanne - Suisse Cliniques Universitaires Saint-Luc,
NIV and Aerosoltherapy Workshop Jean-Bernard Michotte (Lausanne-CH) Simone Gambazza (Milano-IT) Jean-Bernard Michotte Haute Ecole de Santé Vaud, 1011 Lausanne - Suisse Cliniques Universitaires Saint-Luc,
A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS
 THE DOSING INSTITUTE CLINICAL REVIEW SERIES: TOBRAMYCIN IN CYSTIC FIBROSIS MAY 2017 A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS THE DOSING INSTITUTE The Dosing Institute
THE DOSING INSTITUTE CLINICAL REVIEW SERIES: TOBRAMYCIN IN CYSTIC FIBROSIS MAY 2017 A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS THE DOSING INSTITUTE The Dosing Institute
Towards zero prevalence of chronic Pseudomonas aeruginosa infection in children with cystic fibrosis B
 Journal of Cystic Fibrosis 5 (2006) 237 244 www.elsevier.com/locate/jcf Towards zero prevalence of chronic Pseudomonas aeruginosa infection in children with cystic fibrosis B Patrick Lebecque a, *, Teresinha
Journal of Cystic Fibrosis 5 (2006) 237 244 www.elsevier.com/locate/jcf Towards zero prevalence of chronic Pseudomonas aeruginosa infection in children with cystic fibrosis B Patrick Lebecque a, *, Teresinha
Effective Date: August 31, 2006 SUBJECT: CARE AND USE OF NEBULIZER AND INTERMITTENT POSITIVE PRESSURE BREATHING DEVICE
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 421 Effective Date: August 31, 2006 SUBJECT: CARE AND USE OF NEBULIZER AND INTERMITTENT POSITIVE PRESSURE
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 421 Effective Date: August 31, 2006 SUBJECT: CARE AND USE OF NEBULIZER AND INTERMITTENT POSITIVE PRESSURE
Improving rate of decline of FEV1 in young adults with cystic
 Thorax Online First, published on December 29, 2005 as 10.1136/thx.2005.043372 Improving rate of decline of FEV1 in young adults with cystic fibrosis Chengli Que, Paul Cullinan, Duncan Geddes Department
Thorax Online First, published on December 29, 2005 as 10.1136/thx.2005.043372 Improving rate of decline of FEV1 in young adults with cystic fibrosis Chengli Que, Paul Cullinan, Duncan Geddes Department
National Horizon Scanning Centre. Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis. April 2008
 Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
BIOPHARMACEUTICS and CLINICAL PHARMACY
 11 years papers covered BIOPHARMACEUTICS and CLINICAL PHARMACY IV B.Pharm II Semester, Andhra University Topics: Absorption Distribution Protein binding Metabolism Excretion Bioavailability Drug Interactions
11 years papers covered BIOPHARMACEUTICS and CLINICAL PHARMACY IV B.Pharm II Semester, Andhra University Topics: Absorption Distribution Protein binding Metabolism Excretion Bioavailability Drug Interactions
Tacjana Pressler *, Birgitte Frederiksen, Marianne Skov, Peter Garred, Christian Koch, Niels Høiby
 Journal of Cystic Fibrosis 5 (2006) 9 15 www.elsevier.com/locate/jcf Early rise of anti-pseudomonas antibodies and a mucoid phenotype of Pseudomonas aeruginosa are risk factors for development of chronic
Journal of Cystic Fibrosis 5 (2006) 9 15 www.elsevier.com/locate/jcf Early rise of anti-pseudomonas antibodies and a mucoid phenotype of Pseudomonas aeruginosa are risk factors for development of chronic
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING
 TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health POLICY: Nebulizer Therapy DATE: 5-10-93 PROCEDURE: a) Nebulizer Therapy With Non-oxygenated
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health POLICY: Nebulizer Therapy DATE: 5-10-93 PROCEDURE: a) Nebulizer Therapy With Non-oxygenated
Treatment of early Pseudomonas aeruginosa infection in patients with cystic fibrosis: the ELITE trial
 < Supplementary figures are published online only at http:// thorax.bmj.com/content/vol65/ issue4 1 Hospital for Sick Children, Toronto, Canada 2 Hospital Robert Debre, AP-HP Paris, France 3 Novartis Horsham
< Supplementary figures are published online only at http:// thorax.bmj.com/content/vol65/ issue4 1 Hospital for Sick Children, Toronto, Canada 2 Hospital Robert Debre, AP-HP Paris, France 3 Novartis Horsham
NEBULIZERS, METERED DOSE INHALERS, AND DRY POWDER INHALERS
 NEBULIZERS, METERED DOSE INHALERS, AND DRY POWDER INHALERS Douglas S. Gardenhire, Ed.D, RRT-NPS MODULE 1 Manipulate Small Volume Nebulizers by Order or Protocol 1 Objectives for Module 1 At the end of
NEBULIZERS, METERED DOSE INHALERS, AND DRY POWDER INHALERS Douglas S. Gardenhire, Ed.D, RRT-NPS MODULE 1 Manipulate Small Volume Nebulizers by Order or Protocol 1 Objectives for Module 1 At the end of
INFECTION PREVENTION AND CONTROL POLICY AND PROCEDURES Sussex Partnership NHS Foundation Trust (The Trust)
 A member of: Association of UK University Hospitals INFECTION PREVENTION AND CONTROL POLICY AND PROCEDURES Sussex Partnership NHS Foundation Trust (The Trust) IPC17 SINGLE USE AND SINGLE PATIENT USE MEDICAL
A member of: Association of UK University Hospitals INFECTION PREVENTION AND CONTROL POLICY AND PROCEDURES Sussex Partnership NHS Foundation Trust (The Trust) IPC17 SINGLE USE AND SINGLE PATIENT USE MEDICAL
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012
 Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Antibiotic strategies for eradicating Pseudomonas aeruginosa in people with cystic fibrosis (Review)
 Antibiotic strategies for eradicating Pseudomonas aeruginosa in people with cystic fibrosis (Review) Langton Hewer SC, Smyth AR This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
Antibiotic strategies for eradicating Pseudomonas aeruginosa in people with cystic fibrosis (Review) Langton Hewer SC, Smyth AR This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
Pediatrics in mechanical ventilation
 Pediatrics Optimization Intitulé du cours of aerosol therapy in mechanical ventilation Thèmes donnés Ermindo Di Paolo, PhD Departments of Pharmacy and Pediatrics Lausanne University Hospital Switzerland
Pediatrics Optimization Intitulé du cours of aerosol therapy in mechanical ventilation Thèmes donnés Ermindo Di Paolo, PhD Departments of Pharmacy and Pediatrics Lausanne University Hospital Switzerland
Cystic fibrosis (CF) patients suffer from chronic
 Pharmacokinetics and Bioavailability of Aerosolized Tobramycin in Cystic Fibrosis* David E. Geller, MD; William H. Pitlick, PhD; Pasqua A. Nardella, BS; William G. Tracewell, PhD; and Bonnie W. Ramsey,
Pharmacokinetics and Bioavailability of Aerosolized Tobramycin in Cystic Fibrosis* David E. Geller, MD; William H. Pitlick, PhD; Pasqua A. Nardella, BS; William G. Tracewell, PhD; and Bonnie W. Ramsey,
Cystic Fibrosis. Cystic Fibrosis. Cystic Fibrosis 5/01/2011 CYSTIC FIBROSIS OF THE PANCREAS AND ITS RELATION TO CELIAC DISEASE. D ANDERSEN.
 1938 OF THE PANCREAS AND ITS RELATION TO CELIAC DISEASE. D ANDERSEN. American Journal Diseases Children. : The beginning May 1938: 49 cases 25 20 15 Nos of cases 10 5 0 0.5 1 1.5 2 2.5 3 3.5 4 4.5 5 Age
1938 OF THE PANCREAS AND ITS RELATION TO CELIAC DISEASE. D ANDERSEN. American Journal Diseases Children. : The beginning May 1938: 49 cases 25 20 15 Nos of cases 10 5 0 0.5 1 1.5 2 2.5 3 3.5 4 4.5 5 Age
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis
 Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
Saline (0.9%) Nebuliser Guideline
 Saline (0.9%) Nebuliser Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Saline (0.9%) Nebuliser Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Budesonide treatment of moderate and severe asthma in children: A doseresponse
 Budesonide treatment of moderate and severe asthma in children: A doseresponse study Soren Pedersen, MD, PhD, and Ove Ramsgaard Hansen, MD Kolding, Denmark Objective: The purpose of the study was to evaluate
Budesonide treatment of moderate and severe asthma in children: A doseresponse study Soren Pedersen, MD, PhD, and Ove Ramsgaard Hansen, MD Kolding, Denmark Objective: The purpose of the study was to evaluate
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Moss RB, Flume PA, Elborn JS, et al, on behalf
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Moss RB, Flume PA, Elborn JS, et al, on behalf
Patient. Device Clinician. Safety & efficacy
 Patient Device Clinician Formulation Safety & efficacy 1. Modified from Daley-Yates et al., Expert Opin. Drug Deliv. 2011: 8(10):1297-1308 2. Modified from Laube et al., Eur Respir J 2011; 37: 1308 1331
Patient Device Clinician Formulation Safety & efficacy 1. Modified from Daley-Yates et al., Expert Opin. Drug Deliv. 2011: 8(10):1297-1308 2. Modified from Laube et al., Eur Respir J 2011; 37: 1308 1331
Fungal (Aspergillus and Candida) infections in Cystic fibrosis
 Fungal (Aspergillus and Candida) infections in Cystic fibrosis Malena Cohen-Cymberknoh, MD CF Center Hadassah-Hebrew University Medical Center Jerusalem, Israel Israeli Annual CF Conference, Herzlyia,
Fungal (Aspergillus and Candida) infections in Cystic fibrosis Malena Cohen-Cymberknoh, MD CF Center Hadassah-Hebrew University Medical Center Jerusalem, Israel Israeli Annual CF Conference, Herzlyia,
Metered Dose Inhalers with Valved Holding Chamber: A Pediatric Hospital Experience
 Metered Dose Inhalers with Valved Holding Chamber: A Pediatric Hospital Experience 8th Annual North Regional Respiratory Care Conference Minnesota & Wisconsin Societies for Respiratory Care Mayo Civic
Metered Dose Inhalers with Valved Holding Chamber: A Pediatric Hospital Experience 8th Annual North Regional Respiratory Care Conference Minnesota & Wisconsin Societies for Respiratory Care Mayo Civic
European Medicines Agency decision
 EMA/357972/2017 European Medicines Agency decision P/0173/2017 of 3 July 2017 on the acceptance of a modification of an agreed paediatric investigation plan for colistimethate sodium (Colobreathe), (EMEA-000176-PIP01-07-M05)
EMA/357972/2017 European Medicines Agency decision P/0173/2017 of 3 July 2017 on the acceptance of a modification of an agreed paediatric investigation plan for colistimethate sodium (Colobreathe), (EMEA-000176-PIP01-07-M05)
GlaxoSmithKline. Renal impairment. Hepatic impairment
 RELENZA GlaxoSmithKline Zanamivir QUALITATIVE AND QUANTITATIVE COMPOSITION Each RELENZA ROTADISK consists of four regularly spaced double foil blisters each containing a white to off-white micronised powder
RELENZA GlaxoSmithKline Zanamivir QUALITATIVE AND QUANTITATIVE COMPOSITION Each RELENZA ROTADISK consists of four regularly spaced double foil blisters each containing a white to off-white micronised powder
There has been a renewed interest in the use of
 consensus conference Use of Aerosolized Antibiotics in Patients With Cystic Fibrosis Chairpersons: Preston W. Campbell III, MD, and Lisa Saiman, MD* (CHEST 1999; 116:775 788) Abbreviations: CF cystic fibrosis;
consensus conference Use of Aerosolized Antibiotics in Patients With Cystic Fibrosis Chairpersons: Preston W. Campbell III, MD, and Lisa Saiman, MD* (CHEST 1999; 116:775 788) Abbreviations: CF cystic fibrosis;
A Quick Guide to the. I507del. Mutation CFTR SCIENCE
 A Quick Guide to the I507del Mutation CFTR SCIENCE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of CFTR activity is the underlying cause of cystic fibrosis (CF) 1 Spectrum
A Quick Guide to the I507del Mutation CFTR SCIENCE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of CFTR activity is the underlying cause of cystic fibrosis (CF) 1 Spectrum
Characterizing aggressiveness and predicting future progression of CF lung disease
 Journal of Cystic Fibrosis Volume 8 Suppl 1 (2009) S15 S19 www.elsevier.com/locate/jcf Characterizing aggressiveness and predicting future progression of CF lung disease Michael W. Konstan a, *, Jeffrey
Journal of Cystic Fibrosis Volume 8 Suppl 1 (2009) S15 S19 www.elsevier.com/locate/jcf Characterizing aggressiveness and predicting future progression of CF lung disease Michael W. Konstan a, *, Jeffrey
The FDA Critical Path Initiative
 The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
OPTIMISING ANALYTICAL STRATEGIES FOR THE DEMONSTRATION OF BIOEQUIVALENCE IN A GENERIC NEBULISER
 OPTIMISING ANALYTICAL STRATEGIES FOR THE DEMONSTRATION OF BIOEQUIVALENCE IN A GENERIC NEBULISER US FDA guidance for the in vitro demonstration of bioequivalence in a generic nebuliser directly references
OPTIMISING ANALYTICAL STRATEGIES FOR THE DEMONSTRATION OF BIOEQUIVALENCE IN A GENERIC NEBULISER US FDA guidance for the in vitro demonstration of bioequivalence in a generic nebuliser directly references
Spirometry and Flow Volume Measurements
 Spirometry and Flow Volume Measurements Standards & Guidelines December 1998 To serve the public and guide the medical profession Revision Dates: December 1998 Approval Date: June 1998 Originating Committee:
Spirometry and Flow Volume Measurements Standards & Guidelines December 1998 To serve the public and guide the medical profession Revision Dates: December 1998 Approval Date: June 1998 Originating Committee:
Controlled trial of cycled antibiotic prophylaxis to prevent initial Pseudomonas aeruginosa infection in children with cystic fibrosis
 1 Department of Paediatric Respiratory Medicine, Cystic Fibrosis Center, Wilhelmina Children s Hospital, University Medical Center Utrecht, The Netherlands 2 Department of Pediatric Infectious Diseases,
1 Department of Paediatric Respiratory Medicine, Cystic Fibrosis Center, Wilhelmina Children s Hospital, University Medical Center Utrecht, The Netherlands 2 Department of Pediatric Infectious Diseases,
VENTOLIN RESPIRATOR SOLUTION
 VENTOLIN RESPIRATOR SOLUTION Salbutamol QUALITATIVE AND QUANTITATIVE COMPOSITION VENTOLIN Respirator Solution contains 5mg salbutamol, as sulphate, per ml of solution and is supplied in 10 ml bottles.
VENTOLIN RESPIRATOR SOLUTION Salbutamol QUALITATIVE AND QUANTITATIVE COMPOSITION VENTOLIN Respirator Solution contains 5mg salbutamol, as sulphate, per ml of solution and is supplied in 10 ml bottles.
Annex II. Scientific conclusions
 Annex II Scientific conclusions 5 Scientific conclusions Beclometasone dipropionate (BDP) is a glucocorticoid and a prodrug of the active metabolite, beclometasone-17-monopropionate. Beclometasone dipropionate
Annex II Scientific conclusions 5 Scientific conclusions Beclometasone dipropionate (BDP) is a glucocorticoid and a prodrug of the active metabolite, beclometasone-17-monopropionate. Beclometasone dipropionate
Cystic fibrosis: From childhood to adulthood. Eitan Kerem Department of Pediatrics and CF Center Hadassah University Hospital Jerusalem Israel
 Cystic fibrosis: From childhood to adulthood Eitan Kerem Department of Pediatrics and CF Center Hadassah University Hospital Jerusalem Israel Vas deference H 2 O Cl - Na + H 2 O Na + Cl - Cl - Cl -
Cystic fibrosis: From childhood to adulthood Eitan Kerem Department of Pediatrics and CF Center Hadassah University Hospital Jerusalem Israel Vas deference H 2 O Cl - Na + H 2 O Na + Cl - Cl - Cl -
Pulmonary Exacerbations:
 Pulmonary Exacerbations: Better Understanding Needed Michael Tracy, MD Clinical Assistant Professor Pediatric Pulmonary CF Pulmonary Exacerbations Definition Importance Causes Treatment Research opportunities
Pulmonary Exacerbations: Better Understanding Needed Michael Tracy, MD Clinical Assistant Professor Pediatric Pulmonary CF Pulmonary Exacerbations Definition Importance Causes Treatment Research opportunities
Treating Cystic Fibrosis in Resource Poor Environment
 Treating Cystic Fibrosis in Resource Poor Environment SK Kabra, M Kabra, R Lodha, S Shastri Department of Pediatrics All India Institute of Medical Sciences New Delhi India Corresponding author: S K Kabra,
Treating Cystic Fibrosis in Resource Poor Environment SK Kabra, M Kabra, R Lodha, S Shastri Department of Pediatrics All India Institute of Medical Sciences New Delhi India Corresponding author: S K Kabra,
. Type of solution/medication. Amount/dose to be delivered. Frequency/duration. Mode of administration.
 Page 1 of 9 (Large, Medium Volume, and Aerogen Continuous Nebulizer) Purpose Scope Physician's Order To standardize the use of continuous aerosol therapy as a modality used for the rescue of patients with
Page 1 of 9 (Large, Medium Volume, and Aerogen Continuous Nebulizer) Purpose Scope Physician's Order To standardize the use of continuous aerosol therapy as a modality used for the rescue of patients with
Is There a Treatment for BPD?
 Is There a Treatment for BPD? Amir Kugelman, Pediatric Pulmonary Unit and Department of Neonatology Bnai Zion Medical Center, Rappaport Faculty of Medicine Haifa, Israel Conflict of Interest Our study
Is There a Treatment for BPD? Amir Kugelman, Pediatric Pulmonary Unit and Department of Neonatology Bnai Zion Medical Center, Rappaport Faculty of Medicine Haifa, Israel Conflict of Interest Our study
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: exhaled_nitric_oxide_measurement 2/2009 3/2018 3/2019 3/2018 Description of Procedure or Service Asthma is
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: exhaled_nitric_oxide_measurement 2/2009 3/2018 3/2019 3/2018 Description of Procedure or Service Asthma is
Problem Based Learning Session. Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days.
 Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
MONITORING NEBULISER USAGE & LUNG FUNCTION IN CLINICAL TRIALS
 MONITORING NEBULISER USAGE & LUNG FUNCTION IN CLINICAL TRIALS Adherence levels to inhalation treatments are known to be generally low. This issue is particularly important when testing nebulised drugs
MONITORING NEBULISER USAGE & LUNG FUNCTION IN CLINICAL TRIALS Adherence levels to inhalation treatments are known to be generally low. This issue is particularly important when testing nebulised drugs
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
St. Dominic Jackson Memorial Hospital. Pulmonary Services. Therapist Driven Protocol. Assess and Treat Aerosol Therapy
 St. Dominic Jackson Memorial Hospital Pulmonary Services Therapist Driven Protocol Assess and Treat Aerosol Therapy Purpose The purpose of the Therapist Driven Protocol (TDP) aerosol therapy is to create
St. Dominic Jackson Memorial Hospital Pulmonary Services Therapist Driven Protocol Assess and Treat Aerosol Therapy Purpose The purpose of the Therapist Driven Protocol (TDP) aerosol therapy is to create
UNDERSTANDING CYSTIC FIBROSIS
 UNDERSTANDING CYSTIC FIBROSIS INTRODUCTION Cystic fibrosis is a chronic disease that affects the respiratory and gastrointestinal systems. People with cystic fibrosis have a genetic defect of the lungs
UNDERSTANDING CYSTIC FIBROSIS INTRODUCTION Cystic fibrosis is a chronic disease that affects the respiratory and gastrointestinal systems. People with cystic fibrosis have a genetic defect of the lungs
Correspondence: Dr Sushil K. Kabra, Professor, Department of Pediatrics, AIIMS, New Delhi , India.
 JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 5, 2012 Comparison of Effects of 3 and 7% Hypertonic Saline Nebulization on Lung Function in Children with Cystic Fibrosis: A Double-Blind Randomized, Controlled
JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 5, 2012 Comparison of Effects of 3 and 7% Hypertonic Saline Nebulization on Lung Function in Children with Cystic Fibrosis: A Double-Blind Randomized, Controlled
Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages)
 Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages) NHS England Reference: 1732P NHS England INFORMATION READER BOX Directorate
Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages) NHS England Reference: 1732P NHS England INFORMATION READER BOX Directorate
Office Asthma Care: Practical Elements of Asthma Management. Learning Objectives. Diagnosis
 Office Asthma Care: Practical Elements of Asthma Management Pri-Med West Annual Conference March 29, 2014 Anaheim, CA Sande Okelo, MD, PhD, University of California Los Angeles sokelo@mednet.ucla.edu www.uclahealth.org/pedspulmonology
Office Asthma Care: Practical Elements of Asthma Management Pri-Med West Annual Conference March 29, 2014 Anaheim, CA Sande Okelo, MD, PhD, University of California Los Angeles sokelo@mednet.ucla.edu www.uclahealth.org/pedspulmonology
פורמט עלון זה נקבע ע"י משרד הבריאות ותוכנו נבדק ואושר על-ידו בדצמבר Recombinant Human Deoxyribonuclease (Dornase alfa)
 פורמט עלון זה נקבע ע"י משרד הבריאות ותוכנו נבדק ואושר על-ידו בדצמבר 2015 r Pulmozyme Recombinant Human Deoxyribonuclease (Dornase alfa) Solution for inhalation 2.5 mg/ 2.5 ml 1 NAME OF THE MEDICINAL PRODUCT
פורמט עלון זה נקבע ע"י משרד הבריאות ותוכנו נבדק ואושר על-ידו בדצמבר 2015 r Pulmozyme Recombinant Human Deoxyribonuclease (Dornase alfa) Solution for inhalation 2.5 mg/ 2.5 ml 1 NAME OF THE MEDICINAL PRODUCT
Cystic Fibrosis. Jennifer McDaniel, BS, RRT-NPS
 Cystic Fibrosis Jennifer McDaniel, BS, RRT-NPS Overview Cystic fibrosis is the most common fatal, inherited disease in the U. S. CF results from a defective autosomal recessive gene One copy of gene =
Cystic Fibrosis Jennifer McDaniel, BS, RRT-NPS Overview Cystic fibrosis is the most common fatal, inherited disease in the U. S. CF results from a defective autosomal recessive gene One copy of gene =
Dolci U 1, Sidler-Moix AL 1, Di Paolo ER 1,Berger- Gryllaki 1 M, Pannatier A 1, Cotting J 2
 SALBUTAMOL DELIVERY IN AN IN VITRO PAEDIATRIC VENTILATOR-LUNG MODEL: COMPARISON OF JET, ULTRASONIC AND MESH NEBULISERS Dolci U 1, Sidler-Moix AL 1, Di Paolo ER 1,Berger- Gryllaki 1 M, Pannatier A 1, Cotting
SALBUTAMOL DELIVERY IN AN IN VITRO PAEDIATRIC VENTILATOR-LUNG MODEL: COMPARISON OF JET, ULTRASONIC AND MESH NEBULISERS Dolci U 1, Sidler-Moix AL 1, Di Paolo ER 1,Berger- Gryllaki 1 M, Pannatier A 1, Cotting
AEROSOL THERAPY: THE PRACTICALITIES
 AEROSOL THERAPY: THE PRACTICALITIES Lester I. Harrison, PhD Section Head, Clinical Pharmacokinetics, 3M Pharmaceuticals, 3M Center 270-3S-05, St. Paul, MN, USA 55144 liharrison@mmm.com Introduction: Horses,
AEROSOL THERAPY: THE PRACTICALITIES Lester I. Harrison, PhD Section Head, Clinical Pharmacokinetics, 3M Pharmaceuticals, 3M Center 270-3S-05, St. Paul, MN, USA 55144 liharrison@mmm.com Introduction: Horses,
Antibiotic strategies for eradicating Pseudomonas aeruginosa in people with cystic fibrosis(review)
 Cochrane Database of Systematic Reviews Antibiotic strategies for eradicating Pseudomonas aeruginosa in people with cystic fibrosis(review) Langton Hewer SC, Smyth AR Langton Hewer SC, Smyth AR. Antibiotic
Cochrane Database of Systematic Reviews Antibiotic strategies for eradicating Pseudomonas aeruginosa in people with cystic fibrosis(review) Langton Hewer SC, Smyth AR Langton Hewer SC, Smyth AR. Antibiotic
THE NEW ZEALAND MEDICAL JOURNAL
 THE NEW ZEALAND MEDICAL JOURNAL Vol 120 No 1267 ISSN 1175 8716 Is Salamol less effective than Ventolin? A randomised, blinded, crossover study in New Zealand Catherina L Chang, Manisha Cooray, Graham Mills,
THE NEW ZEALAND MEDICAL JOURNAL Vol 120 No 1267 ISSN 1175 8716 Is Salamol less effective than Ventolin? A randomised, blinded, crossover study in New Zealand Catherina L Chang, Manisha Cooray, Graham Mills,
Core Safety Profile. Pharmaceutical form(s)/strength: Dry Powder Inhaler, Nebuliser Suspension, pressurised Metered Dose Inhaler (pmdi)
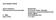 Core Safety Profile Active substance: Budesonide Pharmaceutical form(s)/strength: Dry Powder Inhaler, Nebuliser Suspension, pressurised Metered Dose Inhaler (pmdi) P - RMS: DK/H/PSUR/0041/001 Date of FAR:
Core Safety Profile Active substance: Budesonide Pharmaceutical form(s)/strength: Dry Powder Inhaler, Nebuliser Suspension, pressurised Metered Dose Inhaler (pmdi) P - RMS: DK/H/PSUR/0041/001 Date of FAR:
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION
 SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
A NEBULISERS AND NEBULISED MEDICATION. Generic Guide for the use of nebulisers and nebulised medication
 A NEBULISERS AND NEBULISED MEDICATION Generic Guide for the use of nebulisers and nebulised medication Aim The aim of this guide is to provide a template for those who wish to develop their own nebuliser
A NEBULISERS AND NEBULISED MEDICATION Generic Guide for the use of nebulisers and nebulised medication Aim The aim of this guide is to provide a template for those who wish to develop their own nebuliser
Lung deposition of inhaled tobramycin with eflow rapid/lc Plus jet nebuliser in healthy and cystic fibrosis subjects
 Journal of Cystic Fibrosis 10 (2011) 9 14 www.elsevier.com/locate/jcf Original Article Lung deposition of inhaled tobramycin with eflow rapid/lc Plus jet nebuliser in healthy and cystic fibrosis subjects
Journal of Cystic Fibrosis 10 (2011) 9 14 www.elsevier.com/locate/jcf Original Article Lung deposition of inhaled tobramycin with eflow rapid/lc Plus jet nebuliser in healthy and cystic fibrosis subjects
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Inhalational antibacterial regimens in non-cystic fibrosis patients. Jeff Alder Bayer HealthCare
 Inhalational antibacterial regimens in non-cystic fibrosis patients Jeff Alder Bayer HealthCare Alder - Inhaled therapy for non-cf - EMA 25-26 Oct 2012 1 Inhalational antibacterials: two approaches 1.
Inhalational antibacterial regimens in non-cystic fibrosis patients Jeff Alder Bayer HealthCare Alder - Inhaled therapy for non-cf - EMA 25-26 Oct 2012 1 Inhalational antibacterials: two approaches 1.
IPAC-RS/UF Orlando Inhalation Conference March 20, S.T. Horhota 1, C.B. Verkleij 2, P.J.G. Cornelissen 2, L. Bour 3, A. Sharma 3, M.
 IPAC-RS/UF Orlando Inhalation Conference March 20, 2014 Case Study: Pharmacokinetics and Pharmacodynamics of Tiotropium and Salmeterol Following Parallel Administration in COPD Patients Using Different
IPAC-RS/UF Orlando Inhalation Conference March 20, 2014 Case Study: Pharmacokinetics and Pharmacodynamics of Tiotropium and Salmeterol Following Parallel Administration in COPD Patients Using Different
NG80. Asthma: diagnosis, monitoring and chronic asthma management (NG80)
 Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Contents. Who should read / have access to this document? What is new in this version?
 1 Nebulised Colistin Colistimethate sodium (Colomycin ) for the treatment of Pseudomonas Aeruginosa colonisation and infection in adult patients with non-cystic Fibrosis bronchiectasis or bronchial sepsis
1 Nebulised Colistin Colistimethate sodium (Colomycin ) for the treatment of Pseudomonas Aeruginosa colonisation and infection in adult patients with non-cystic Fibrosis bronchiectasis or bronchial sepsis
