Target lobe volume reduction and COPD outcome measures after endobronchial valve therapy
|
|
|
- Chloe Franklin
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE COPD Target lobe volume reduction and COPD outcome measures after endobronchial valve therapy Arschang Valipour 1, Felix J.F. Herth 2, Otto C. Burghuber 1, Gerard Criner 3, Jean-Michel Vergnon 4, Jonathan Goldin 5, Frank Sciurba 6 and Armin Ernst 7 for the VENT study group Affiliations: 1 Dept of Respiratory and Critical Care Medicine, Ludwig-Boltzmann-Institute for COPD and Respiratory Epidemiology, Otto-Wagner-Hospital, Vienna, Austria. 2 Pneumology and Critical Care Medicine, Thoraxklinik Heidelberg, Germany. 3 Temple Lung Center, Pulmonary and Critical Care Medicine, Temple University, Philadelphia, PA, 5 Center for Computer Vision and Imaging Biomarkers, Dept of Radiological Sciences, David Geffen School of Medicine at UCLA, Los Angeles, CA, 6 University of Pittsburgh School of Medicine, Pittsburgh, PA, and 7 Interventional Pulmonology, St Elizabeth s Medical Center, Boston, MA, USA. 4 Pulmonary Medicine, Saint Étienne University Hospital, Saint Étienne, France. Correspondence: A. Valipour, Ludwig-Boltzmann-Institute for COPD, Dept of Respiratory and Critical Care Medicine, Otto-Wagner-Hospital, Vienna, Austria. arschang.valipour@wienkav.at ABSTRACT Endobronchial valve (EBV) therapy may be associated with improvements in chronic obstructive pulmonary disease-related outcomes and may therefore be linked to improvements in the body mass index, airflow obstruction, dyspnoea, exercise capacity (BODE) index. Data from 416 patients with advanced emphysema and hyperinflation across Europe and USA, who were randomised to EBV (n5284) or conservative therapy (n5132) were analysed. Quantitative image analysis was used to compare the volume of the targeted lobe at baseline and at 6 months to determine target lobe volume reduction (TLVR). 44% of patients receiving EBV therapy (versus 24.7% of controls) had clinically significant improvements in the BODE index (p,0.001). BODE index was significantly reduced by mean SD , and points in patients with TLVR.50%, 20% 50% and,20%, respectively (intergroup differences p,0.001), but increased by points in controls. Changes in BODE were predicted by baseline BODE and correlated significantly with lobar exclusion and lung volumes at 6 months. A greater proportion of patients in the treatment group than in the control group achieved a clinically meaningful improvement in BODE index; however, the likelihood of benefit was less than half in both groups. Patients in whom TLVR was obtained had greater improvements in clinical Patients treated with EBV were more likely to have a significantly reduced BODE score (44% treated versus 25% controls) This article has supplementary material available from Received: Aug Accepted after revision: May First published online: July Clinical trial: This study is registered at clinicaltrials.gov with identifier number NCT Conflict of interest: Disclosures can be found alongside the online version of this article at Copyright ßERS 2014 Eur Respir J 2014; 43: DOI: /
2 Introduction Endobronchial valve (EBV) therapy attempts to achieve the effects of surgical lung volume reduction [1, 2] by selectively occluding the airways supplying the most affected regions of the hyperinflated emphysematous lung, while permitting exhaled gas to escape. Reports of EBV therapy in selected patients with end-stage emphysema have shown significant improvements in lung function and exercise tolerance [3 6]. The most significant functional and subjective improvements are seen when atelectasis develops after the insertion of valves [7, 8]; however, EBV therapy may also be beneficial in the absence of atelectasis [9]. Given that lung volume reduction may be associated with improvements in airflow obstruction, exercise capacity and/or dyspnoea, we hypothesised that the information obtained by quantitative volumetric analysis prior to and after EBV therapy may be associated with changes in other important chronic obstructive pulmonary disease (COPD)-related outcome measures, such as the integrated body mass index, airflow obstruction, dyspnoea and exercise capacity (BODE) index. The BODE index is a multidimensional grading system, which has been shown to be better than forced expiratory volume in 1 s (FEV1) alone in predicting the risk of future COPD exacerbations, hospitalisations and/or death in patients with COPD [10 13]. The BODE index has been shown to be responsive to interventions such as pulmonary rehabilitation [14] and lung volume reduction surgery [15 17]. Furthermore, there is evidence that the BODE index has greater predictive value than individual outcome measures alone [18]. Thus, changes in BODE could serve as a measure of treatment success and should correlate with other important clinical outcomes in COPD patients undergoing EBV therapy. The Endobronchial Valve for Emphysema Palliation Trial (VENT) provides an ideal dataset to examine the relationship of changes in lung volume reduction to BODE index as it compared an active intervention with optimal medical therapy in a randomised trial. Individual data sets from USA [3] and European [19] VENT cohorts have already been published, and in these reports the analyses were confined to single outcome measures. In the analysis presented here, we have used the complete VENT dataset to examine the impact of EBV therapy upon the multidimensional BODE index and its relationship with target lobar volume reduction measured 6 months after the procedure. Methods The study group consisted of all patients with emphysema who participated in the USA and European VENT studies. The clinical protocols have identical inclusion/exclusion criteria, efficacy variables and adverse event collection. Details of the trial design and study eligibility criteria for VENT have been reported previously [18, 20]. Briefly, patients were randomly assigned in a ratio of 2:1 to receive EBV treatment along with optimised medical care or optimised medical care alone. All patients provided written informed consent as approved by the ethics committee overseeing each clinical site. Clinical effectiveness measures were obtained 6 months after the intervention. These included FEV1, the 6-min walk test, cycle ergometry workload and health-related quality of life (assessed using the St George s Respiratory Questionnaire (SGRQ)). Safety was evaluated by determining the rates of major complications (including death), a composite of pulmonary adverse events, cardiovascular events and implant-related adverse events (online supplementary table E1). 492 underwent random assignment 331 EBV group 161 control group 9 died 9 withdrawn 18 no visit 11 no follow-up CT scan 2 died 8 withdrawn 15 no visit 4 no follow-up CT scan 284 patients with TLVR measurements at 6 months 132 patients with TLVR measurements at 6 months FIGURE 1 Study flow chart. EBV: endobronchial valve; CT: computed tomography; TLVR: target lobe volume reduction. 388 DOI: /
3 TABLE 1 Characteristics of patients and controls at baseline Total sample Treatment group Control group Total treatment group Complete fissure Incomplete fissure p-value Subjects n Age years Male % BMI kg?m Smoking duration years FEV1 L FEV1 % pred FVC L FVC % pred FEV1/FVC Total lung capacity L Residual volume L IC/TLC min walk distance m BODE index mmrc dyspnoea scale SGRQ Cycle ergometry W Heterogeneity % Proportions of target lobes per lung % Left lung , Right lung , Patients with complete fissures % Data are presented as mean SD, unless otherwise stated. p-values were obtained by comparison of means by t-tests for independent samples, comparison of frequencies by crosstabs and Chi-squared tests. BMI: body mass index; FEV1: forced expiratory volume in 1 s; % pred: % predicted; FVC: forced vital capacity; IC: inspiratory capacity; TLC: total lung capacity; BODE: BMI, airflow obstruction, dyspnoea and exercise capacity; mmrc: modified Medical Research Council; SGRQ: St George s Respiratory Questionnaire. High-resolution computed tomography A computer-based quantitative analysis of standardised multirow detector computed tomography (CT) performed on the 10-mm reconstructed image set was analysed at a core laboratory to provide quantitative indices of lobar emphysema severity and lobar volumes and to identify the target lobe. The methods for evaluating the images have been reported previously [20]. When choosing the target lobe, both the degree of emphysema and heterogeneity were taken into account (a thorough description of the algorithm used has already been published [3]). In the case of the right lung, the middle lobe was ignored. Fissure integrity was analysed on the thin-section (,3 mm) reconstructed image dataset, and defined as the completeness of the fissure (.90% of the fissure present on thin-slice high-resolution CT) on at least one axis, as classified by the consensus of two independent blinded readers at the core laboratory. Quantitative image analysis by the core laboratory was used to measure and compare the volume of the targeted lobe at baseline and at 180 days in order to determine the target lobe volume reduction (TLVR). The CT scan obtained at 6 months was further used to determine lobar exclusion, i.e. correct placement of the valves in the targeted airways with the intention to isolate a lobe from ventilation. Procedure Bronchoscopy and periprocedural preparations were performed as previously described [20]. Valves were placed unilaterally in lobar, segmental or subsegmental bronchi based on individual anatomy with the intention of completely isolating the target lobe. The valve used in this study was a one-way silicone duckbill valve (Zephyr EBV; Pulmonx, Redwood City, CA, USA). The valve is available in two sizes, spanning airway diameters of mm and mm. DOI: /
4 TABLE 2 Clinical, functional and radiological outcomes presented as percentage of population in patients treated with endobronchial valve therapy and controls at 6 months according to fissure status Treatment group Control group Complete fissure Incomplete fissure p-value Subjects n Radiological outcomes TLVR.50% , TLVR 20 50% TLVR f20% Missing Clinical and functional outcomes (cut-off) FEV1 (12% pred) , min walk distance (26 m) SGRQ (4 points) mmrc (1 point) BODE index (1 point) Data are presented as %, unless otherwise stated. p-values were obtained by comparison of frequencies by crosstabs and Chi-squared tests. TLVR: target lobar volume reduction; FEV1: forced expiratory volume in 1 s; % pred: % predicted; SGRQ: St George s Respiratory Questionnaire; mmrc: modified Medical Research Council dyspnoea scale; BODE: body mass index, airflow obstruction, dyspnoea and exercise capacity scale. Statistical analysis Statistical analysis was performed using SPSS Statistics 17.0 (IBM, Armonk, NY, USA). Simple descriptive statistics were calculated for qualitative outcomes and standard measures were calculated for continuous variables. Unless otherwise indicated, data are presented as mean SD. Baseline characteristics for patients in the treatment group were analysed according to the presence or absence of complete interlobar fissures. Outcomes of interest were further presented according to TLVR cut-offs of,20%, 20 50% and.50%. These thresholds were chosen on the basis of cluster analysis and are consistent with recent reports [21]. Group differences according to continuous data were evaluated using two-sample t-tests for one variable, and the generalised linear model for multivariate analyses. Box s M test was applied to check equality of covariance matrices whenever required. For categorical data, crosstabs were generated and frequencies were analysed via the Pearson Chi-squared test or Fisher exact test. Minimal clinically important differences were defined according to recommended cut-offs for FEV1 [22], SGRQ [23], modified Medical Research Council dyspnoea scale [23] and 6-min walking test [24]. For the BODE index, a reduction of 1 point was considered clinically relevant [11]. Pearson s correlation coefficient was used for interval-scaled data as a measurement of the bivariate linear relationship. Multinomial logistic regression was applied to check the effects of a set of predictor variables (factors (scale) or covariates (ordinal)) on a dependent variable (ordinal variable with more than two categories). 40 EBV Control Proportion of total population % BODE score FIGURE 2 Distribution of body mass index, airflow obstruction, dyspnoea and exercise capacity (BODE) scores at 6 months in endobronchial valve (EBV)-treated patients and controls. 390 DOI: /
5 TABLE 3 Baseline predictors of change in body mass index, airflow obstruction, dyspnoea and exercise capacity (BODE) score at 6 months using stepwise linear regression analysis B SE p-value BODE index baseline ,0.001 Age Sex Residual volume Baseline destruction score Target lobe Ipsilateral lobe Target lobe heterogeneity Fissure status Results A total of 492 patients were enrolled across Europe (n5171) and the USA (n5321). For the purpose of this analysis, only patients with follow-up CT scans at 6 months were included. Thus, 416 patients were finally included in this study analysis (fig. 1). There were no significant differences in baseline characteristics between those included and excluded (data not shown). Of the 416 patients included, 284 received EBVs with optimised medical care (treatment group) and 132 received optimised medical care alone (controls). All patients were receiving bronchodilator therapy, 50% received inhaled corticosteroids and 61% received long-term oxygen treatment. There were no statistically significant differences in baseline characteristics between the treatment and control arms (table 1). Within the treatment group, significantly more patients with complete fissures on pretreatment CT scans were treated in the left lung than patients with incomplete fissures (p,0.001). TLVR and COPD-related outcomes at 6 months TLVR was significantly higher in the total group of patients receiving EBV therapy at 6 months than in controls ( ml versus ml, p,0.001). Of those randomised to the treatment group, 32% of patients with complete fissures showed a TLVR.50% at 6 months following intervention, 22% a TLVR between 20% and 50%, and 30% a TLVR f20% (table 2). In contrast, only 4% of patients with incomplete fissures had a TLVR.50% and the majority of patients (67%) had TLVR f20% (p,0.001 for intergroup differences). The distribution of BODE scores at 6 months in EBV-treated patients and controls is displayed in figure 2. 44% of patients randomised to EBV treatment compared to 24.7% of controls had improvement in BODE index at 6 months (p,0.001). In contrast, worsening of BODE was observed in 39% of controls compared with 25% of patients in the treatment arm (p,0.001). Patients with TLVR.50% at 6 months demonstrated greater improvements in lung function, exercise capacity, quality of life, dyspnoea and BODE index compared to the other groups (online supplementary table E2). Improvements in the BODE index of o1 point were observed in 67%, 37% and 41% of patients with TLVR.50%, TLVR 20 50% and TLVR,20%, respectively (p for intergroup differences). There were no statistically significant differences with respect to the percentage of patients with either improvement or worsening of BODE index between centres with fewer than five, between five and 10, and those with o10 EBV-treated patients in the study (online supplementary table E3). These findings did not change after correction for the prevalence of complete versus incomplete fissures. Predictors of a successful outcome We conducted linear regression analysis using a number of variables to determine baseline predictors of change in BODE index at 6 months, including age, sex, baseline BODE, fissure integrity, target lobe heterogeneity and baseline destruction scores of the treated and untreated ipsilateral lobe. Baseline BODE index score was the only independent predictor of changes in BODE index at 6 months (table 3). When removing baseline BODE from this analysis, baseline destruction score of the target lobe was revealed as the only independent predictor of change in BODE at 6 months (online supplemementary table E4). Correlates of a successful outcome At 6 months only 55.9% of the EBV-treated patients demonstrated CT evidence of lobar exclusion. A post hoc analysis was performed to investigate factors that were associated with changes in BODE index at DOI: /
6 TABLE 4 Correlates of change in body mass index, airflow obstruction, dyspnoea and exercise capacity (BODE) score at 6 months using stepwise linear regression analysis B SE p-value Lobar exclusion ,0.001 Change in residual volume ,0.001 Change in total lung capacity Age Sex Change in IC/TLC ratio Target lobar volume reduction Target lobe IC: inspiratory capacity; TLC: total lung capacity. 6 months using changes in lung volumes, target lobar volume reduction and lobar exclusion as potential correlates of a successful outcome (table 4). Changes in BODE index were associated with lobar exclusion, changes in residual volume and total lung capacity. Both patients with incomplete and those with complete fissures had significantly larger improvements in BODE index in the presence of lobar exclusion (fig. 3). TLVR and safety The relationship between treatment response and safety was assessed by analysing individual adverse events at 6 months. There were no significant differences in mortality between the intervention and control group (data not shown). The rate of pulmonary/thoracic adverse events, however, was higher in EBV-treated subjects compared with controls (table 5). This difference was mainly driven by the following subcategories of adverse events: haemoptysis (42% of EBV subjects compared with 2% of control subjects, p,0.0001) and noncardiac chest pain (16% of EBV subjects compared with 3% of control subjects, p ). There were no statistically significant differences in cumulative cardiovascular, pulmonary or implant-related adverse events groups between patients with complete and those with incomplete fissures. With respect to individual adverse events, however, there was a significantly higher pneumothorax rate (10.2%) in patients with TLVR.50% compared with the other groups (1.2% pneumothorax rate in the TLVR 20 50% group and 0.6% pneumothorax rate in TLVR,20% group) (online supplementary table E5). Of these, one patient with a prolonged pneumothorax underwent surgical oversew of the air leak. Removing these data from the analysis did not alter outcomes. Discussion One-way EBV therapy is intended to produce volume reduction, mimicking the health benefit effects of surgical lung volume reduction with overall lower morbidity and mortality [25]. Using data from two large randomised clinical trials of EBV therapy in patients with severe emphysema, the present analysis revealed a 4 p=0.029 p=0.001 Change in BODE score Lobar exclusion: No Yes Incomplete fissure Fissure status Complete fissure FIGURE 3 Boxplot of change in body mass index, airflow obstruction, dyspnoea and exercise capacity (BODE) score at 6monthsinpatientswithandwithout lobar exclusion according to fissure status. 392 DOI: /
7 TABLE 5 Most important adverse events (serious and non-serious) at 6 months according to fissure status Treatment group Control group Complete fissure Incomplete fissure p-value Subjects n Pulmonary/thoracic adverse events Pneumothorax Respiratory failure Implant-related adverse events NA Pneumonia distal to valve NA Cardiovascular adverse events Data are presented as %, unless otherwise stated. NA: not applicable. relationship between TLVR and clinically meaningful changes in relevant COPD outcome measures, such as the multidimensional BODE index. These changes were predominantly observed in the presence of complete fissures and lobar exclusion. The BODE index, evaluated at baseline in clinical trials, has been shown to exhibit greater predictive value than its individual components with respect to quality of life, exacerbation rates, morbidity and mortality in patients with COPD [10, 12, 13]. Furthermore, a recent study demonstrated that longitudinal changes in the BODE index, and not FEV1, were independently associated with an increased risk of dying [19]. Conversely, a few intervention studies have suggested that the BODE index changes after therapeutic intervention and that this change appears to be related to subsequent health outcomes. IMFELD et al. [15] found that improvement in the BODE index 3 months after surgical lung volume reduction was associated with lower subsequent mortality. Similar findings have been observed in a small cohort of patients who underwent EBV therapy for emphysema. DE OLIVEIRA et al. [26] demonstrated smaller improvements in BODE at 3 months following EBV implantation. However, these studies have been limited by small numbers and/or lack of controls. Improvements in BODE index in the present cohort were predicted by baseline BODE index, an observation that is consistent with recent findings from bronchoscopic lung volume reduction trials [27]. These findings suggest that improvements in ventilatory mechanics after EBV may have a higher impact in patients with more severe disease at baseline, a hypothesis that is further supported by post hoc evidence of an independent association between changes in lung volumes and BODE index at 6 months. However, clinically meaningful improvements in BODE in the present report were seen predominantly in the subgroup of patients who had lobar exclusion at 6 months and thus developed.50% lobar volume reduction. The majority of these patients (67%) had an improvement in BODE index of o1 point. Results from lung volume reduction surgery in the National Emphysema Treatment Trial [11] have shown that 32% of patients who underwent lung volume reduction surgery similarly had a 1-point improvement in BODE index at 6 months following randomisation. Importantly, this change in BODE was associated with a significant 43% decrease in subsequent mortality in that report. Thus, the magnitude of improvement in BODE index in patients with.50% lung volume reduction is in a range suggestive of potential benefits such as a reduction in mortality. This hypothesis is further supported by two recent studies that were able to demonstrate long-term survival benefits in the presence of significant lung volume reduction [7, 28]. It remains unclear whether EBV-treated patients may experience clinical benefits in the absence of atelectasis. HOPKINSON et al. [9] demonstrated improvements in lung function, dynamic hyperinflation, oesophageal pressure time product and a reduction in static compliance in a group of 19 patients who underwent valve treatment. Improvements in exercise capacity were independently associated with improvements in diffusing capacity and with reductions in static lung volumes, both in the presence and absence of atelectasis. This suggests that valve insertion may direct airflow into less affected areas of the lung, reducing dynamic hyperinflation during exercise [9]. This is of particular importance, as the daily physical activity of patients with COPD is mainly associated with dynamic hyperinflation, regardless of severity classification [29]. However, when the patients with atelectasis (defined as a change in the position of the interlobar fissure adjacent to the targeted area) in the report of HOPKINSON et al. [9] were excluded, the exercise improvement in the remaining group was no longer significant. DOI: /
8 It has to be acknowledged that the majority of patients in the present report did not have clinically relevant lobar volume reduction. A number of factors may have prevented benefits in a larger proportion of the treated patient population. Recent studies suggest that fissure status is an important predictor of treatment response [18]. Incomplete fissures suggest collateral ventilation across lobes, a phenomenon that is more common in emphysematous than in normal lungs [30]. There is evidence that the interlobar fissures are more often incomplete on the right than on the left side of the lung [31], thus left-side treated patients were more likely to develop greater TLVR. More recently, a catheter-based system (Chartis; Pulmonx) has been developed, which enables real-time assessment of collateral ventilation and, thus, can be used to predict lobar volume reduction in response to valve placement [32, 33]. However, the success of valve treatment may largely depend on lobar exclusion (i.e. all airways to the lobe are blocked by EBVs). A post hoc stepwise linear regression analysis identified lobar exclusion as the strongest independent correlate of changes in BODE index at 6 months. This observation is further supported by a recent report from NINANE et al. [34]. The authors intended to place valves bilaterally in the upper lobes. Per protocol, one segment of each upper lobe was not treated to achieve incomplete occlusion of the upper lobes. Using this approach, the authors reported a mean SD 7.3 9% TLVR at 3 months, with no clinically meaningful changes in lung function. Thus, one could argue that their entire study cohort matches the low-tlvr subgroup in our analysis. Moreover, a recent study by EBERHARDT et al. [35] confirms that a unilateral lobar approach with lobar exclusion is superior to a bilateral approach with incomplete lobar exclusion with respect to improvements in lung function and exercise capacity. A number of methodological issues need to be addressed. The present report is an intention-to-treat analysis. Thus, outcomes data presented at 6 months included patients with incomplete lobar exclusion due to bronchoscopic valve removal because of adverse events or migration of valves, coughing up valves, and/ or technical failure to place valves in the first place. Furthermore, lobar exclusion was assessed using CT analysis rather than bronchoscopic inspection at follow-up, and it yet remains to be established whether one is superior to the other. The absence of a sham procedure and the lack of longer follow-up are other potential limitations in the study design. Finally, with low overall mortality in the present report, we were unable to determine whether changes in the BODE index were in fact associated with actual long-term prognosis. Nevertheless, the consistent relationship between TLVR and clinical and functional parameters, and the magnitude of effects in patients with more than 50% TLVR, support a true intervention effect. As all patients and investigators were blinded to the magnitude of lobar volume collapse, one might speculate that results in lobar nonresponders (TLVR,20%), which are similar to controls in most outcome measures, may be comparable to those with sham procedures. Furthermore, we have to acknowledge that patients with.50% TLVR had a higher likelihood of developing a pneumothorax, a phenomenon which is most likely due to sheer stress on the ipsilateral adjacent untreated lobe. The majority of these events resolved with observation or chest tube placement, and only two patients reportedly underwent surgical air leak closure. As these patients experience substantial lobar volume reduction with large clinical benefits, the risk of developing a pneumothorax appears to be linked to the likelihood of a positive clinical response at 6 months [18]. In summary, the current study has shown that a minority subgroup of patients in the VENT trial experienced substantial TLVR with subsequent important health outcomes of patients with emphysema. Predictors of success identified in the present report need to be considered in the design of future valve treatment trials for emphysema. Acknowledgements We would like to thank the VENT study investigators and clinical sites for their diligent efforts in recruiting and following-up the patients participating in this study, and Andrea Schrott (StatistikAmbulanz KG, Leobendorf, Austria) for her contributions related to statistical evaluation of the data. Editing assistance was provided by Archimed Medical Communication (Zofingen, Switzerland). VENT Study Research Group members are as follows. Clinical centres: A. End, F. Schneider and W. Klepetko (Allgemeines Krankenhaus Wien, Vienna, Austria); F.Stanzel, N.Weber and K. Haeussinger (Asklepios Fachkliniken München-Gauting, Gauting, Germany); S. Gasparini and S. De Luca (Azienda Ospedaliera Umberto I, Ancona, Italy); E. Golden, M. Smith and G. Williams (Baptist Memorial Hospital, Memphis, TN, USA); A. Ernst, D. Feller-Kopman, R. Garland, S. Ashiku and M. DeCamp (Beth Israel Deaconess Medical Center, Boston, MA, USA); G. Ferguson and T. Murphy Thompson (Botsford Hospital, Livonia, MI, USA); R. McKenna Jr, C. Geaga and D. Kusuanco (Cedars-Sinai Medical Center, Los Angeles, CA, USA); CH. Pison, B. Wuyam, G. Ferretti, I. Vivodtzev and C. Righini (Centre Hospitalier Universitaire de Grenoble, Grenoble, Switzerland); F. Lebargy, G. Deslee and S. Dury (Centre Hospitalier Universitaire de Reims, Reims, France); C. Witt and B. Schmidt (Charité Campus Mitte, Berlin, Germany); J. Gonzalez-Bermejo, V. Trosini-Desert, T. Similowski, C. Beigelman and M.H. Becquemin (Groupe Hospitalier Pitié Salpétrière, Paris, France); M. Simoff and R. Almario (Henry Ford Hospital, Detroit, MI, USA); H. Mal, A. Marceau, M. Fournier, O. Brugière and G. Dauriat (Hôpital Beaujon, Paris, France); C. Marquette, S. Leroy, T. Perez and N. Bautin (Hôpital Calmette, Lille, France); G. Massard, R. Kessler, A. Charloux, M. Y. Jeung and A. Jory (Hôpital Civil, Strasbourg, France); J. F. Muir, 394 DOI: /
9 C. Viacroze, D. Benhamou, A. Cuvelier and L. Molano (Hôpital de Bois Guillaume, Rouen, France); B. Degano, C. Hermant, S. Pontier, J. Rami and V. Chabbert (Hôpital Larrey, Toulouse, France); J.M. Vergnon, C. Veyret, F. Costes aned L. De Matos (Hôpital Nord, Saint Étienne, France); M. Febvre, C. Chouaid and B. Lebeau (Hôpital Saint-Antoine, Paris, France); C. Pinet, H. Dutau, P. Thomas, M. Badier and J.Y. Gaubert (Hôpital Sainte Marguerite, Marseille, France); A. Xaubet, A. Torres, C. Agustí and J. Barberà (Hospital Clínic de Barcelona, Barcelona, Spain); A. Agustí, B. Togores, F. Renom, J. Sauleda and R. Ramos (Hospital Universitari Son Dureta, Palma Mallorca, Spain); S. Nathan, S. Ahmad, L. Collazo and E. Battle (Inova Fairfax Institute of Research, Falls Church, VA, USA); E. Hecker, J. Volmerig and T. Jahn (Klinikum Bremen-Ost, Bremen, Germany); J. Ficker, M. Wagner and T. Fink (Klinikum Nürnberg, Nuremberg, Germany); J. Egan and J. Coyle (Mater Misericordiae University Hospital, Dublin, Ireland); E. Edell, D. Midthun, J. Utz, B. Andrist and K. Meiras (Mayo Clinic, Rochester, MN, USA); C. Strange, G. Silvestri and E. Williams-Cummings (Medical University of South Carolina, Charleston, SC, USA); E. Freilich, D. Amin, J. Masson, D. Orlando and L. Morgan (Morton Plant, Clearwater, FL, USA); R. Bowler, C. Wheeler and K. Mitchell (National Jewish Medical and Research Center, Denver, CO, USA); R. Maxfield, M. Ginsburg, P. Jellen and F. Brogan (New York-Presbyterian Hospital, New York, NY, USA); A. Valipour, R. Kohansal and C. Burghuber (Otto-Wagner Spital, Vienna, Austria); D. Elton, A. Sy, E. McFarland, N. Haase and M. Stout (Palmetto Richland Memorial Hospital, Lexington, SC, USA); W. Tillis, P. Whitten, J. Crabb, K. Hartwig and A. Scott (Peoria Pulmonary Associates, Peoria, IL, USA); B. Levine, J. Ross, D. Baratz and L. Fu (Pulmonary Associates, Phoenix, AZ, USA); E. Cordasco, J. Adamo and J. Botte (Remington-Davis Clinical Research, Columbus, OH, USA); K. Voelker, T. Horiuchi, K. Hurwitz, G. Ferreira and K. Morgan (Sarasota Memorial Hospital, Sarasota, FL, USA); M. Jantz, A. Deem and A. Fox (Shands Hospital University of Florida, Gainesville, FL, USA); S. Campbell, T. Vincent and W. Shen (Southern Arizona VA Health Care System, Tucson, AZ, USA); S. Hazelrigg and T. Boley (Southern Illinois University, Springfield, IL, USA); W.M. Boomer, J. Goulet and C. Mullins (St Francis Hospital, Tulsa, OK, USA); J. Cicena and P. O Neill (St Vincent s Hospital Manhattan, New York, NY, USA); G. Criner, J. Travaline, W. Chatila, G. Jones (Temple University Hospital, Philadelphia, PA, USA); F. Herth and R. Eberhardt (Thoraxklinik Heidelberg, Heidelberg, Germany); W. Leeds, G. Fair, L. Ludlow, S. Nicklin and C. Davis (Veritas Clinical Specialties, Topeka, KS, USA); K. Kovitz and S. Ditta (Tulane University Hospital, New Orleans, LA, USA); A. Chan, R. Allen, T. Albertson, B. Morrissey and M. Juarez (UC Davis, Sacramento, CA, USA); P. Germonpre, A. Janssens and W. De Backer (University Hospital Antwerp, Edegem, Belgium); M. Noppen, J. De Mey and M. Meysman (University Hospital AZ-VUB, Brussels, Belgium); G. McLennan, J. Ferguson, A. Ross, K. Sprenger and J. Keating (University of Iowa Medical Center, Iowa City, IA, USA); M. Zgoda, R. Berger, J. McClung and R. Cortes (University of Kentucky, Lexington, KY, USA); M. Krasna, J. Britt, Z. Gamliel and I. Moskowitz (University of Maryland, Baltimore, MD, USA); S. Gay and J. Konkle (University of Michigan Medical Center, Ann Arbor, MI, USA); F. Sciurba, R. Landreneau, M. Crespo, L. Lane, W. Slivka, C. Fuhrman, P. Ferson and C. Witt (University of Pittsburgh Medical Center, Pittsburgh, PA, USA); S. Goodnight-White, S. Soubra, P. Smithwick and K. Velamuri (VA Medical Center, Houston, TX, USA). Other participants: clinical events committee: C. Cooper (University of California, Los Angeles, CA, USA), B. Badduke (Washington Township Medical Foundation, Fremont, CA, USA) and E. Hsiao (Santa Clara Valley Medical Center, San Jose, CA, USA); data safety monitoring board: R. Wise (Johns Hopkins University, Baltimore, MD, USA), B. Celli (Pulmonary Division, Brigham and Women s Hospital, Boston, MA, USA), A. Ciccone (University La Sapienza, Rome, Italy), R. Keenan (Division of Thoracic Surgery, Pittsburgh, PA, USA) and D. Gilman (ICRC, Inc., Reno, NV, USA); CT core laboratory: J. Goldin, M. Brown, M. McNitte-Gray, I. da Costa and J. Ho (University of California, Los Angeles, CA, USA); cost-effectiveness core laboratory: R. Kaplan and T. Ganiats; UCSD Health Outcomes Assessment Program: E. Groessl, J. Harvey and B. Mulligan (University of California, San Diego, CA, USA). References 1 Fishman A, Martinez F, Naunheim K, et al. A randomized trial comparing lung-volume-reduction surgery with medical therapy for severe emphysema. N Engl J Med 2003; 348: Sciurba FC, Rogers RM, Keenan RJ, et al. Improvement in pulmonary function and elastic recoil after lungreduction surgery for diffuse emphysema. N Engl J Med 1996; 334: Sciurba FC, Ernst A, Herth FJ, et al. A randomized study of endobronchial valves for advanced emphysema. N Engl J Med 2010; 363: Toma TP, Hopkinson NS, Hillier J, et al. Bronchoscopic volume reduction with valve implants in patients with severe emphysema. Lancet 2003; 361: Wan IY, Toma TP, Geddes DM, et al. Bronchoscopic lung volume reduction for end-stage emphysema: report on the first 98 patients. Chest 2006; 129: Wood DE, McKenna RJ Jr, Yusen RD, et al. A multicenter trial of an intrabronchial valve for treatment of severe emphysema. J Thorac Cardiovasc Surg 2007; 133: Hopkinson NS, Kemp SV, Toma TP, et al. Atelectasis and survival after bronchoscopic lung volume reduction for COPD. Eur Respir J 2011; 37: Springmeyer SC, Bolliger CT, Waddell TK, et al. Treatment of heterogeneous emphysema using the spiration IBV valves. Thorac Surg Clin 2009; 19: Hopkinson NS, Toma TP, Hansell DM, et al. Effects of bronchoscopic lung volume reduction on dynamic hyperinflation and exercise in emphysema. Am J Respir Crit Care Med 2005; 171: Celli BR, Cote CG, Marin JM, et al. The body-mass index, airflow obstruction, dyspnea, and exercise capacity index in chronic obstructive pulmonary disease. N Engl J Med 2004; 350: Martinez FJ, Han MK, Andrei AC, et al. Longitudinal change in the BODE index predicts mortality in severe emphysema. Am J Respir Crit Care Med 2008; 178: Ong KC, Earnest A, Lu SJ A multidimensional grading system (BODE index) as predictor of hospitalization for COPD, Chest 2005; 128: Marin JM, Carrizo SJ, Casanova C, et al. Prediction of risk of COPD exacerbations by the BODE index. Respir Med 2009; 103: Cote CG, Celli BR Pulmonary rehabilitation, the BODE index in COPD, Eur Respir J 2005; 26: Imfeld S, Bloch KE, Weder W, et al. The BODE index after lung volume reduction surgery correlates with survival. Chest 2006; 129: DOI: /
10 16 Lederer DJ, Thomashow BM, Ginsburg ME, et al. Lung-volume reduction surgery for pulmonary emphysema: improvement in body mass index, airflow obstruction, dyspnea, and exercise capacity index after 1 year. J Thorac Cardiovasc Surg 2007; 133: Martinez FJ, Foster G, Curtis JL, et al. Predictors of mortality in patients with emphysema and severe airflow obstruction. Am J Respir Crit Care Med 2006; 173: Casanova C, de Torres JP, Aguirre-Jaíme A, et al. The progression of chronic obstructive pulmonary disease is heterogeneous: the experience of the BODE cohort. Am J Respir Crit Care Med 2011; 184: Herth FJ, Noppen M, Valipour A, et al. Efficacy predictors of lung volume reduction with Zephyr valves in a European cohort. Eur Respir J 2012; 39: Strange C, Herth FJ, Kovitz KL, et al. Design of the Endobronchial Valve for Emphysema Palliation Trial (VENT): a non-surgical method of lung volume reduction. BMC Pulm Med 2007; 7: Brown MS, Kim HJ, Abtin FG, et al. Emphysema lung lobe volume reduction: effects on the ipsilateral and contralateral lobes. Eur Radiol 2012; 22: Pellegrino R, Viegi G, Brusasco V, et al. Interpretative strategies for lung function tests. Eur Respir J 2005; 26: Cazzola M, MacNee W, Martinez FJ, et al. Outcomes for COPD pharmacological trials: from lung function to biomarkers. Eur Respir J 2008; 31: Puhan MA, Chandra D, Mosenifar Z, et al. The minimal important difference of exercise tests in severe COPD. Eur Respir J 2011; 37: Ingenito EP, Wood DE, Utz JP. Bronchoscopic lung volume reduction in severe emphysema. Proc Am Thorac Soc 2008; 5: de Oliveira HG, Macedo-Neto AV, John AB, et al. Transbronchoscopic pulmonary emphysema treatment: 1-month to 24-month endoscopic follow-up. Chest 2006; 130: Herth FJ, Ernst A, Baker KM, et al. Characterization of outcomes 1 year after endoscopic thermal vapor ablation for patients with heterogeneous emphysema. Int J Chron Obstruct Pulmon Dis 2012; 7: Venuta F, Anile M, Diso D, et al. Long-term follow-up after bronchoscopic lung volume reduction in patients with emphysema. Eur Respir J 2012; 39: Garcia-Rio F, Lores V, Mediano O, et al. Daily physical activity in patients with chronic obstructive pulmonary disease is mainly associated with dynamic hyperinflation. Am J Respir Crit Care Med 2009; 180: Morrell NW, Wignall BK, Biggs T, et al. Collateral ventilation and gas exchange in emphysema. Am J Respir Crit Care Med 1994; 150: Aziz A, Ashizawa K, Nagaoki K, et al. High resolution CT anatomy of the pulmonary fissures. J Thorac Imaging 2004; 19: Gompelmann D, Eberhardt R, Michaud G, et al. Predicting atelectasis by assessment of collateral ventilation prior to endobronchial lung volume reduction: a feasibility study. Respiration 2010; 80: Herth FJ, Eberhardt R, Gompelmann D, et al. Radiological and clinical outcomes of using Chartis TM to plan endobronchial valve treatment. Eur Respir J 2013; 41: Ninane V, Geltner C, Bezzi M, et al. Multicentre European study for the treatment of advanced emphysema with bronchial valves. Eur Respir J 2012; 39: Eberhardt R, Gompelmann D, Schuhmann M, et al. Complete unilateral vs partial bilateral endoscopic lung volume reduction in patients with bilateral lung emphysema. Chest 2012; 142: DOI: /
Emphysema is a debilitating and progressive. Efficacy predictors of lung volume reduction with Zephyr valves in a European cohort
 Eur Respir J 2012; 39: 1334 1342 DOI: 10.1183/09031936.00161611 CopyrightßERS 2012 Efficacy predictors of lung volume reduction with Zephyr valves in a European cohort Felix J.F. Herth, Marc Noppen, Arschang
Eur Respir J 2012; 39: 1334 1342 DOI: 10.1183/09031936.00161611 CopyrightßERS 2012 Efficacy predictors of lung volume reduction with Zephyr valves in a European cohort Felix J.F. Herth, Marc Noppen, Arschang
Journal of the COPD Foundation. Journal Club - Endobronchial Valve Bronchoscopic Lung Volume Reduction Ron Balkissoon, MD, MSc, DIH, FRCPC 1
 118 Journal Club: Endobronchial Valve Lung Volume Reduction Chronic Obstructive Pulmonary Diseases: Journal of the COPD Foundation Journal Club Journal Club - Endobronchial Valve Bronchoscopic Lung Volume
118 Journal Club: Endobronchial Valve Lung Volume Reduction Chronic Obstructive Pulmonary Diseases: Journal of the COPD Foundation Journal Club Journal Club - Endobronchial Valve Bronchoscopic Lung Volume
Emphysema. Endoscopic lung volume reduction. PhD. Chief, department of chest diseases and thoracic oncology. JM VERGNON M.D, PhD.
 Emphysema Endoscopic lung volume reduction JM VERGNON M.D, PhD. PhD. Chief, department of chest diseases and thoracic oncology Genève 2010 INSERM IFR 143 Physiological concepts EMPHYSEMA Slide of Ch H
Emphysema Endoscopic lung volume reduction JM VERGNON M.D, PhD. PhD. Chief, department of chest diseases and thoracic oncology Genève 2010 INSERM IFR 143 Physiological concepts EMPHYSEMA Slide of Ch H
Bronchial Valves. Policy Number: Last Review: 4/2017 Origination: 4/2013 Next Review: 4/2018
 Bronchial Valves Policy Number: 7.01.128 Last Review: 4/2017 Origination: 4/2013 Next Review: 4/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for bronchial valves.
Bronchial Valves Policy Number: 7.01.128 Last Review: 4/2017 Origination: 4/2013 Next Review: 4/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for bronchial valves.
Efficacy Predictors of Lung Volume Reduction with Zephyr Valves in a European
 ERJ Express. Published on January 26, 2012 as doi: 10.1183/09031936.00161611 Efficacy Predictors of Lung Volume Reduction with Zephyr Valves in a European Cohort Felix JF Herth, MD 1 ; Marc Noppen, MD
ERJ Express. Published on January 26, 2012 as doi: 10.1183/09031936.00161611 Efficacy Predictors of Lung Volume Reduction with Zephyr Valves in a European Cohort Felix JF Herth, MD 1 ; Marc Noppen, MD
SPIRATION VALVE SYSTEM Patient Selection for the Treatment of Emphysema Based on Clinical Literature.
 SPIRATION VALVE SYSTEM Patient Selection for the Treatment of Emphysema Based on Clinical Literature. SPIRATION VALVE SYSTEM The Spiration Valve System is a device placed in the lung airway to treat severely
SPIRATION VALVE SYSTEM Patient Selection for the Treatment of Emphysema Based on Clinical Literature. SPIRATION VALVE SYSTEM The Spiration Valve System is a device placed in the lung airway to treat severely
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of endobronchial valves (with or without assessment for collateral
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of endobronchial valves (with or without assessment for collateral
Effectiveness and safety of unilateral endobronchial valve applying to severe emphysema: a meta-analysis
 Original Article Page 1 of 10 Effectiveness and safety of unilateral endobronchial valve applying to severe emphysema: a meta-analysis Wei-Song Chen, Dan Zhu, Hui Chen, Jian-Feng Luo Department of Respiratory,
Original Article Page 1 of 10 Effectiveness and safety of unilateral endobronchial valve applying to severe emphysema: a meta-analysis Wei-Song Chen, Dan Zhu, Hui Chen, Jian-Feng Luo Department of Respiratory,
2017 Blue Cross and Blue Shield of Louisiana
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Complications after bronchoscopic lung volume reduction
 Review Article Complications after bronchoscopic lung volume reduction Daniel Franzen 1, Gilles Straub 1, Lutz Freitag 2 1 Interventional Lung Center, Department of Pulmonology, University Hospital Zurich,
Review Article Complications after bronchoscopic lung volume reduction Daniel Franzen 1, Gilles Straub 1, Lutz Freitag 2 1 Interventional Lung Center, Department of Pulmonology, University Hospital Zurich,
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
COILS FOR THE TREATMENT OF ADVANCED EMPHYSEMA: A GROWING BODY OF EVIDENCE AND ROUTINE EXPERIENCE
 COILS FOR THE TREATMENT OF ADVANCED EMPHYSEMA: A GROWING BODY OF EVIDENCE AND ROUTINE EXPERIENCE *Jean-Marc Fellrath Internal Medicine Department/Service of Pneumology, Pourtalès Hospital, Neuchâtel, Switzerl
COILS FOR THE TREATMENT OF ADVANCED EMPHYSEMA: A GROWING BODY OF EVIDENCE AND ROUTINE EXPERIENCE *Jean-Marc Fellrath Internal Medicine Department/Service of Pneumology, Pourtalès Hospital, Neuchâtel, Switzerl
Service Evaluation: Bronchoscopic lung volume reduction using endobronchial valves for the symptomatic improvement of emphysema
 Service Evaluation: Bronchoscopic lung volume reduction using endobronchial valves for the symptomatic improvement of emphysema Saveria Di Gerlando, University of Bristol INTRODUCTION Chronic Obstructive
Service Evaluation: Bronchoscopic lung volume reduction using endobronchial valves for the symptomatic improvement of emphysema Saveria Di Gerlando, University of Bristol INTRODUCTION Chronic Obstructive
Bronchoscopic lung volume reduction using endobronchial valves for the symptomatic improvement of severe emphysema.
 WEMJ Volume 115 No 4 Article 5 December 2016 Bronchoscopic lung volume reduction using endobronchial valves for the symptomatic improvement of severe emphysema. Saveria Di Gerlando, Dr Bethannie McIntyre,
WEMJ Volume 115 No 4 Article 5 December 2016 Bronchoscopic lung volume reduction using endobronchial valves for the symptomatic improvement of severe emphysema. Saveria Di Gerlando, Dr Bethannie McIntyre,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of endobronchial nitinol coils to improve lung function in emphysema
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion of endobronchial nitinol coils to improve lung function in emphysema
Bronchoscopic lung volume reduction: recent updates
 Review Article of Interventional Pulmonology Corner Bronchoscopic lung volume reduction: recent updates Anuradha Ramaswamy, Jonathan Puchalski Section of Pulmonary, Critical Care and Sleep, Department
Review Article of Interventional Pulmonology Corner Bronchoscopic lung volume reduction: recent updates Anuradha Ramaswamy, Jonathan Puchalski Section of Pulmonary, Critical Care and Sleep, Department
Chronic obstructive pulmonary disease in over 16s: diagnosis and management
 National Institute for Health and Care Excellence Draft for consultation Chronic obstructive pulmonary disease in over 16s: diagnosis and management [G] Referral criteria for lung volume reduction procedures,
National Institute for Health and Care Excellence Draft for consultation Chronic obstructive pulmonary disease in over 16s: diagnosis and management [G] Referral criteria for lung volume reduction procedures,
PERSPECTIVES. Endoscopic Lung Volume Reduction A European Perspective. Abstract. Daniela Gompelmann 1, Ralf Eberhardt 1, and Felix J. F.
 Endoscopic Lung Volume Reduction A European Perspective Daniela Gompelmann 1, Ralf Eberhardt 1, and Felix J. F. Herth 1 1 Department of Pneumology and Respiratory Care Medicine, Thoraxklinik at University
Endoscopic Lung Volume Reduction A European Perspective Daniela Gompelmann 1, Ralf Eberhardt 1, and Felix J. F. Herth 1 1 Department of Pneumology and Respiratory Care Medicine, Thoraxklinik at University
LVRS and Endobronchial Therapy for Emphysema: Is it Still Viable?
 LVRS and Endobronchial Therapy for Emphysema: Is it Still Viable? Malcolm M. DeCamp, MD Fowler McCormick Professor of Surgery Feinberg School of Medicine Chief, Division of Thoracic Surgery Disclosures
LVRS and Endobronchial Therapy for Emphysema: Is it Still Viable? Malcolm M. DeCamp, MD Fowler McCormick Professor of Surgery Feinberg School of Medicine Chief, Division of Thoracic Surgery Disclosures
Supplementary Online Content
 Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Clinical management of lung volume reduction in end stage emphysema patients
 Review Article Clinical management of lung volume reduction in end stage emphysema patients Kaid Darwiche 1, Clemens Aigner 2 1 Department of Pneumology, Division of Interventional Bronchology, 2 Department
Review Article Clinical management of lung volume reduction in end stage emphysema patients Kaid Darwiche 1, Clemens Aigner 2 1 Department of Pneumology, Division of Interventional Bronchology, 2 Department
SPIRATION. VALVE SYSTEM For the Treatment of Emphysema or Air Leaks.
 SPIRATION VALVE SYSTEM For the Treatment of Emphysema or Air Leaks. 0000 ENGINEERED FOR AIRWAY MANAGEMENT Inspired by aerodynamics, the Spiration Valve redirects air away from diseased or damaged lung
SPIRATION VALVE SYSTEM For the Treatment of Emphysema or Air Leaks. 0000 ENGINEERED FOR AIRWAY MANAGEMENT Inspired by aerodynamics, the Spiration Valve redirects air away from diseased or damaged lung
A Randomized Study of Endobronchial Valves for Advanced Emphysema
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article A Randomized Study of Endobronchial Valves for Advanced Emphysema Frank C. Sciurba, M.D., Armin Ernst, M.D., Felix J.F. Herth, M.D.,
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article A Randomized Study of Endobronchial Valves for Advanced Emphysema Frank C. Sciurba, M.D., Armin Ernst, M.D., Felix J.F. Herth, M.D.,
The blocking therapy of BLVR for Emphysema Phenotype of COPD
 The blocking therapy of BLVR for Emphysema Phenotype of COPD Dr. Michela Bezzi Interventional Pulmonology University Hospital Brescia - Italy drmichela.bezzi@gmail.com Hyperinflation In Emphysema Hyperinflation
The blocking therapy of BLVR for Emphysema Phenotype of COPD Dr. Michela Bezzi Interventional Pulmonology University Hospital Brescia - Italy drmichela.bezzi@gmail.com Hyperinflation In Emphysema Hyperinflation
Five Consecutive Cases of Non-Pharmacologic Therapy for COPD
 Five Consecutive Cases of Non-Pharmacologic Therapy for COPD Michael Jantz, MD Director of Interventional Pulmonology University of Florida Michael.Jantz@medicine.ufl.edu Emphysema: Background Loss of
Five Consecutive Cases of Non-Pharmacologic Therapy for COPD Michael Jantz, MD Director of Interventional Pulmonology University of Florida Michael.Jantz@medicine.ufl.edu Emphysema: Background Loss of
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Chronic obstructive pulmonary disease. Lung volume reduction for severe emphysema: do we need a scalpel or a scope?
 Eur Respir Rev 2010; 19: 117, 242 247 DOI: 1183/09059180005810 CopyrightßERS 2010 REVIEW: ENDOSCOPY Lung volume reduction for severe emphysema: do we need a scalpel or a scope? D. Van Raemdonck* and V.
Eur Respir Rev 2010; 19: 117, 242 247 DOI: 1183/09059180005810 CopyrightßERS 2010 REVIEW: ENDOSCOPY Lung volume reduction for severe emphysema: do we need a scalpel or a scope? D. Van Raemdonck* and V.
Endobronchial coil therapy in severe emphysema: 6-month outcomes from a Swiss National Registry
 Original Article Endobronchial coil therapy in severe emphysema: 6-month outcomes from a Swiss National Registry Jean-Marc Fellrath 1, Thomas Scherer 2, Daniel P. Franzen 3, Alban Lovis 4, Christophe von
Original Article Endobronchial coil therapy in severe emphysema: 6-month outcomes from a Swiss National Registry Jean-Marc Fellrath 1, Thomas Scherer 2, Daniel P. Franzen 3, Alban Lovis 4, Christophe von
Attitudes and access to lung volume reduction surgery for COPD: a survey by the British Thoracic Society
 Chronic obstructive pulmonary disease Attitudes and access to lung volume reduction surgery for COPD: a survey by the British Thoracic Society William McNulty, Simon Jordan, Nicholas S Hopkinson on behalf
Chronic obstructive pulmonary disease Attitudes and access to lung volume reduction surgery for COPD: a survey by the British Thoracic Society William McNulty, Simon Jordan, Nicholas S Hopkinson on behalf
Complications related to endoscopic lung volume reduction for emphysema with endobronchial valves: results of a multicenter study
 Original Article Complications related to endoscopic lung volume reduction for emphysema with endobronchial valves: results of a multicenter study Alfonso Fiorelli 1#, Antonio D Andrilli 2#, Michela Bezzi
Original Article Complications related to endoscopic lung volume reduction for emphysema with endobronchial valves: results of a multicenter study Alfonso Fiorelli 1#, Antonio D Andrilli 2#, Michela Bezzi
Clinical and radiographic predictors of GOLD-Unclassified smokers in COPDGene
 Clinical and radiographic predictors of GOLD-Unclassified smokers in COPDGene Emily S. Wan, John E. Hokanson, James R. Murphy, Elizabeth A. Regan, Barry J. Make, David A. Lynch, James D. Crapo, Edwin K.
Clinical and radiographic predictors of GOLD-Unclassified smokers in COPDGene Emily S. Wan, John E. Hokanson, James R. Murphy, Elizabeth A. Regan, Barry J. Make, David A. Lynch, James D. Crapo, Edwin K.
Review Article Bronchoscopic Lung Volume Reduction
 Pulmonary Medicine Volume 2011, Article ID 610802, 6 pages doi:10.1155/2011/610802 Review Article Bronchoscopic Lung Volume Reduction Armin Ernst 1 and Devanand Anantham 2 1 Pulmonary, Critical Care and
Pulmonary Medicine Volume 2011, Article ID 610802, 6 pages doi:10.1155/2011/610802 Review Article Bronchoscopic Lung Volume Reduction Armin Ernst 1 and Devanand Anantham 2 1 Pulmonary, Critical Care and
EMPHYSEMA THERAPY. Information brochure for valve therapy in the treatment of emphysema.
 EMPHYSEMA THERAPY Information brochure for valve therapy in the treatment of emphysema. PATIENTS WITH EMPHYSEMA With every breath, lungs deliver oxygen to the rest of the body to perform essential life
EMPHYSEMA THERAPY Information brochure for valve therapy in the treatment of emphysema. PATIENTS WITH EMPHYSEMA With every breath, lungs deliver oxygen to the rest of the body to perform essential life
Keywords: bronchoscopy; emphysema; lung volume reduction
 Endoscopic Lung Volume Reduction An American Perspective Hans J. Lee 1 *, Samira Shojaee 2 *, and Daniel H. Sterman 3 1 Interventional Pulmonology, Pulmonary Disease, and Critical Care Medicine, The Johns
Endoscopic Lung Volume Reduction An American Perspective Hans J. Lee 1 *, Samira Shojaee 2 *, and Daniel H. Sterman 3 1 Interventional Pulmonology, Pulmonary Disease, and Critical Care Medicine, The Johns
Supplementary Online Content
 Supplementary Online Content Deslée G, Mal H, Dutau H, et al; REVOLENS Study Group. Lung volume reduction coil treatment vs usual care in patients with severe emphysema: the REVOLENS randomized clinical
Supplementary Online Content Deslée G, Mal H, Dutau H, et al; REVOLENS Study Group. Lung volume reduction coil treatment vs usual care in patients with severe emphysema: the REVOLENS randomized clinical
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lung_volume_reduction_surgery 4/1996 3/2018 3/2019 3/2018 Description of Procedure or Service Emphysema is
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lung_volume_reduction_surgery 4/1996 3/2018 3/2019 3/2018 Description of Procedure or Service Emphysema is
Lung volume reduction surgery in selected patients with severe emphysema: significant benefit with low peri-operative risk
 Mini-Review Page 1 of 6 Lung volume reduction surgery in selected patients with severe emphysema: significant benefit with low peri-operative risk Claudio Caviezel Department of Thoracic Surgery, University
Mini-Review Page 1 of 6 Lung volume reduction surgery in selected patients with severe emphysema: significant benefit with low peri-operative risk Claudio Caviezel Department of Thoracic Surgery, University
Introduction to Interventional Pulmonology
 Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Bronchoscopic interventions for severe COPD
 Review Article Bronchoscopic interventions for severe COPD Robert F. Browning 1, Scott Parrish 1, Saiyad Sarkar 2, William Krimsky 2, J. Francis Turner Jr. 3, Konstantinos Zarogoulidis 4, Ioanna Kougioumtzi
Review Article Bronchoscopic interventions for severe COPD Robert F. Browning 1, Scott Parrish 1, Saiyad Sarkar 2, William Krimsky 2, J. Francis Turner Jr. 3, Konstantinos Zarogoulidis 4, Ioanna Kougioumtzi
Reducing lung volume in emphysema Surgical Aspects
 Reducing lung volume in emphysema Surgical Aspects Simon Jordan Consultant Thoracic Surgeon Royal Brompton Hospital Thirteenth Cambridge Chest Meeting April 2015 Surgical aspects of LVR Why we should NOT
Reducing lung volume in emphysema Surgical Aspects Simon Jordan Consultant Thoracic Surgeon Royal Brompton Hospital Thirteenth Cambridge Chest Meeting April 2015 Surgical aspects of LVR Why we should NOT
Methodological Aspects of Bronchoscopic Lung Volume Reduction with a Proprietary System
 Technical Review Respiration 2003;70:658 664 DOI: 10.1159/000075217 Received: November 12, 2002 Accepted after revision: July 4, 2003 Methodological Aspects of Bronchoscopic Lung Volume Reduction with
Technical Review Respiration 2003;70:658 664 DOI: 10.1159/000075217 Received: November 12, 2002 Accepted after revision: July 4, 2003 Methodological Aspects of Bronchoscopic Lung Volume Reduction with
Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 4 Number 2 Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 4 Number 2 Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
Emphysema is a debilitating lung disease with a significant
 Bronchoscopic Lung-Volume Reduction With One-Way Valves in Patients With Heterogenous Emphysema Federico Venuta, MD, Tiziano de Giacomo, MD, Erino A. Rendina, MD, Anna Maria Ciccone, MD, Daniele Diso,
Bronchoscopic Lung-Volume Reduction With One-Way Valves in Patients With Heterogenous Emphysema Federico Venuta, MD, Tiziano de Giacomo, MD, Erino A. Rendina, MD, Anna Maria Ciccone, MD, Daniele Diso,
A method for the automatic quantification of the completeness of pulmonary fissures: evaluation in a database of subjects with severe emphysema
 Eur Radiol (2012) 22:302 309 DOI 10.1007/s00330-011-2278-0 CHEST A method for the automatic quantification of the completeness of pulmonary fissures: evaluation in a database of subjects with severe emphysema
Eur Radiol (2012) 22:302 309 DOI 10.1007/s00330-011-2278-0 CHEST A method for the automatic quantification of the completeness of pulmonary fissures: evaluation in a database of subjects with severe emphysema
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
LUNG VOLUME REDUCTION SURGERY IN PATIENTS WITH COPD
 LUNG VOLUME REDUCTION SURGERY IN PATIENTS WITH COPD Walter WEDER, Ilhan INCI, Michaela TUTIC Division of Thoracic Surgery University Hospital, Zurich, Switzerland e-mail: walter.weder@usz.ch INTRODUCTION
LUNG VOLUME REDUCTION SURGERY IN PATIENTS WITH COPD Walter WEDER, Ilhan INCI, Michaela TUTIC Division of Thoracic Surgery University Hospital, Zurich, Switzerland e-mail: walter.weder@usz.ch INTRODUCTION
ORIGINAL ARTICLE. Endobronchial Valve Therapy in Patients with Homogeneous Emphysema Results from the IMPACT Study. &get_box_var; Abstract
 &get_box_var; ORIGINAL ARTICLE Endobronchial Valve Therapy in Patients with Homogeneous Emphysema Results from the IMPACT Study Arschang Valipour 1, Dirk-Jan Slebos 2, Felix Herth 3, Kaid Darwiche 4, Manfred
&get_box_var; ORIGINAL ARTICLE Endobronchial Valve Therapy in Patients with Homogeneous Emphysema Results from the IMPACT Study Arschang Valipour 1, Dirk-Jan Slebos 2, Felix Herth 3, Kaid Darwiche 4, Manfred
Original Research. Mummadi, Srinivas; Pack, Sasheen; Hahn, Peter
 The Official Journal of the International Society of Pleural Diseases Original Research The Use of Bronchoscopic Oxygen Insufflation to Isolate Persistent Air Leaks in Secondary Pneumothorax Due to COPD
The Official Journal of the International Society of Pleural Diseases Original Research The Use of Bronchoscopic Oxygen Insufflation to Isolate Persistent Air Leaks in Secondary Pneumothorax Due to COPD
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
A randomised trial of lung sealant versus medical therapy for advanced emphysema
 ORIGINAL ARTICLE COPD A randomised trial of lung sealant versus medical therapy for advanced emphysema Carolyn E. Come, Mordechai R. Kramer, Mark T. Dransfield, Muhanned Abu-Hijleh, David Berkowitz, Michela
ORIGINAL ARTICLE COPD A randomised trial of lung sealant versus medical therapy for advanced emphysema Carolyn E. Come, Mordechai R. Kramer, Mark T. Dransfield, Muhanned Abu-Hijleh, David Berkowitz, Michela
Does the multidimensional grading system (BODE) correspond to differences in health status of patients with COPD?
 AUTHOR COPY ORIGINAL RESEARCH Does the multidimensional grading system (BODE) correspond to differences in health status of patients with COPD? Kian-Chung Ong 1 Suat-Jin Lu 1 Cindy Seok-Chin Soh 2 1 Department
AUTHOR COPY ORIGINAL RESEARCH Does the multidimensional grading system (BODE) correspond to differences in health status of patients with COPD? Kian-Chung Ong 1 Suat-Jin Lu 1 Cindy Seok-Chin Soh 2 1 Department
exacerbation has greater impact on functional status than frequency of exacerbation episodes.
 Original Article Singapore Med J 2011, 52(12) 894 Changes in the BODE index, exacerbation duration and hospitalisation in a cohort of COPD patients Bu X N, Yang T, Thompson M A, Hutchinson A F, Irving
Original Article Singapore Med J 2011, 52(12) 894 Changes in the BODE index, exacerbation duration and hospitalisation in a cohort of COPD patients Bu X N, Yang T, Thompson M A, Hutchinson A F, Irving
629s Abstract printing supported by. Visit Chiesi at Stand D.30
 390. Treatment beyond inhalers: endoscopic lung volume reduction P3526 Late-breaking abstract: Prevalence of emphysema heterogeneity measured with thoracic computed tomography soft in combination with
390. Treatment beyond inhalers: endoscopic lung volume reduction P3526 Late-breaking abstract: Prevalence of emphysema heterogeneity measured with thoracic computed tomography soft in combination with
BREATHING INNOVATION INTO LIFE
 BREATHING INNOVATION INTO LIFE About Emphysema A Clinical Research Study for people with severe emphysema. Find out if this study may be Emphysema is a form of chronic obstructive pulmonary disease (COPD)
BREATHING INNOVATION INTO LIFE About Emphysema A Clinical Research Study for people with severe emphysema. Find out if this study may be Emphysema is a form of chronic obstructive pulmonary disease (COPD)
BioScience Trends. 2018; 12(4):
 395 Original Article DOI: 10.5582/bst.2018.01134 Importance of bronchoscopic lung volume reduction coil therapy in potential candidates for lung transplantation Askin Gulsen 1,2, * 1 Department of Pneumology,
395 Original Article DOI: 10.5582/bst.2018.01134 Importance of bronchoscopic lung volume reduction coil therapy in potential candidates for lung transplantation Askin Gulsen 1,2, * 1 Department of Pneumology,
Description. Section: Medicine Effective Date: October 15, 2014 Subsection: Medicine Original Policy Date: December 7, 2011 Subject:
 Page: 1 of 9 Last Review Status/Date: September 2014 Description Lung volume reduction surgery (LVRS) is proposed as a treatment option for patients with severe emphysema who have failed optimal medical
Page: 1 of 9 Last Review Status/Date: September 2014 Description Lung volume reduction surgery (LVRS) is proposed as a treatment option for patients with severe emphysema who have failed optimal medical
Endobronchial Valves for Emphysema without Interlobar Collateral Ventilation
 The new england journal of medicine Original Article Endobronchial Valves for Emphysema without Interlobar Collateral Ventilation Karin Klooster, Nick H.T. ten Hacken, M.D., Ph.D., Jorine E. Hartman, Ph.D.,
The new england journal of medicine Original Article Endobronchial Valves for Emphysema without Interlobar Collateral Ventilation Karin Klooster, Nick H.T. ten Hacken, M.D., Ph.D., Jorine E. Hartman, Ph.D.,
WHAT ARE THE PHYSIOLOGICAL DETERMINANTS OF EXPIRATORY FLOW?
 Lung Volume the physiology of breathing: OBSTRUCTIVE LUNG DISORDERS Dr. Andrew Fon MBBS FRACP Respiratory and Sleep Medicine Physician PhD Research Fellow Dept. of Thoracic Medicine, ROYAL ADELAIDE HOSPITAL
Lung Volume the physiology of breathing: OBSTRUCTIVE LUNG DISORDERS Dr. Andrew Fon MBBS FRACP Respiratory and Sleep Medicine Physician PhD Research Fellow Dept. of Thoracic Medicine, ROYAL ADELAIDE HOSPITAL
Increased difference between slow and forced vital capacity is associated with reduced exercise tolerance in COPD patients
 Yuan et al. BMC Pulmonary Medicine 2014, 14:16 RESEARCH ARTICLE Open Access Increased difference between slow and forced vital capacity is associated with reduced exercise tolerance in COPD patients Wei
Yuan et al. BMC Pulmonary Medicine 2014, 14:16 RESEARCH ARTICLE Open Access Increased difference between slow and forced vital capacity is associated with reduced exercise tolerance in COPD patients Wei
Long-term follow-up after bronchoscopic lung volume reduction in patients with emphysema
 Eur Respir J 2012; 39: 1084 1089 DOI: 10.1183/09031936.00071311 CopyrightßERS 2012 Long-term follow-up after bronchoscopic lung volume reduction in patients with emphysema Federico Venuta, Marco Anile,
Eur Respir J 2012; 39: 1084 1089 DOI: 10.1183/09031936.00071311 CopyrightßERS 2012 Long-term follow-up after bronchoscopic lung volume reduction in patients with emphysema Federico Venuta, Marco Anile,
Incomplete fissures are associated with increased alveolar ventilation via spiracles in severe emphysema
 Interactive CardioVascular and Thoracic Surgery 25 (2017) 851 855 doi:10.1093/icvts/ivx220 Advance Access publication 6 July 2017 THORACIC Cite this article as: Khauli S, Abston E, Sajjad H, Bolukbas S,
Interactive CardioVascular and Thoracic Surgery 25 (2017) 851 855 doi:10.1093/icvts/ivx220 Advance Access publication 6 July 2017 THORACIC Cite this article as: Khauli S, Abston E, Sajjad H, Bolukbas S,
Yuriy Feschenko, Liudmyla Iashyna, Ksenia Nazarenko and Svitlana Opimakh
 2018; 7(1): 74-78 ISSN (E): 2277-7695 ISSN (P): 2349-8242 NAAS Rating: 5.03 TPI 2018; 7(1): 74-78 2018 TPI www.thepharmajournal.com Received: 11-11-2017 Accepted: 12-12-2017 Yuriy Feschenko Liudmyla Iashyna
2018; 7(1): 74-78 ISSN (E): 2277-7695 ISSN (P): 2349-8242 NAAS Rating: 5.03 TPI 2018; 7(1): 74-78 2018 TPI www.thepharmajournal.com Received: 11-11-2017 Accepted: 12-12-2017 Yuriy Feschenko Liudmyla Iashyna
DOES SMOKING MARIJUANA INCREASE THE RISK OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE?
 DOES SMOKING MARIJUANA INCREASE THE RISK OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE Pubdate: Tue, 14 Apr 2009 Source: Canadian Medical Association Journal (Canada) Copyright: 2009 Canadian Medical Association
DOES SMOKING MARIJUANA INCREASE THE RISK OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE Pubdate: Tue, 14 Apr 2009 Source: Canadian Medical Association Journal (Canada) Copyright: 2009 Canadian Medical Association
TORCH: Salmeterol and Fluticasone Propionate and Survival in COPD
 TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
KD : A Phase 2 Trial of KD025 to Assess Safety, Efficacy and Tolerability in Patients with Idiopathic Pulmonary Fibrosis (IPF)
 -207: A Phase 2 Trial of to Assess Safety, Efficacy and Tolerability in Patients with Idiopathic Pulmonary Fibrosis (IPF) K. F. Gibson 1, F. Averill 2, T.E. Albertson 3, D. M. Baratz 4, S. Chaudhary 5,
-207: A Phase 2 Trial of to Assess Safety, Efficacy and Tolerability in Patients with Idiopathic Pulmonary Fibrosis (IPF) K. F. Gibson 1, F. Averill 2, T.E. Albertson 3, D. M. Baratz 4, S. Chaudhary 5,
Survival impact of lung transplantation for COPD
 Eur Respir J 2010; 36: 74 80 DOI: 10.1183/09031936.00087809 CopyrightßERS 2010 Survival impact of lung transplantation for COPD S. Lahzami*, P.O. Bridevaux #, P.M. Soccal #,", J. Wellinger +, J.H. Robert
Eur Respir J 2010; 36: 74 80 DOI: 10.1183/09031936.00087809 CopyrightßERS 2010 Survival impact of lung transplantation for COPD S. Lahzami*, P.O. Bridevaux #, P.M. Soccal #,", J. Wellinger +, J.H. Robert
The History and Future Treatment of Emphysema Emphysema Valves, Emphysema Coils and Volume Reduction Surgery
 The History and Future Treatment of Emphysema Emphysema Valves, Emphysema Coils and Volume Reduction Surgery Dr Nabil Jarad PhD FRCP Consultant Respiratory Physician Bristol Royal Infirmary Bristol BS2
The History and Future Treatment of Emphysema Emphysema Valves, Emphysema Coils and Volume Reduction Surgery Dr Nabil Jarad PhD FRCP Consultant Respiratory Physician Bristol Royal Infirmary Bristol BS2
Protocol. Lung Volume Reduction Surgery for Severe Emphysema
 Protocol Lung Volume Reduction Surgery for Severe Emphysema (70171) Medical Benefit Effective Date: 01/01/12 Next Review Date: 09/14 Preauthorization Yes Review Dates: 02/07, 01/08, 11/08, 09/09, 09/10,
Protocol Lung Volume Reduction Surgery for Severe Emphysema (70171) Medical Benefit Effective Date: 01/01/12 Next Review Date: 09/14 Preauthorization Yes Review Dates: 02/07, 01/08, 11/08, 09/09, 09/10,
The distribution of COPD in UK general practice using the new GOLD classification
 ORIGINAL ARTICLE COPD The distribution of COPD in UK general practice using the new GOLD classification John Haughney 1, Kevin Gruffydd-Jones 2, June Roberts 3, Amanda J. Lee 4, Alison Hardwell 5 and Lorcan
ORIGINAL ARTICLE COPD The distribution of COPD in UK general practice using the new GOLD classification John Haughney 1, Kevin Gruffydd-Jones 2, June Roberts 3, Amanda J. Lee 4, Alison Hardwell 5 and Lorcan
Bode index as a predictor of severity in patients with chronic obstructive pulmonary disease.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VII (May. 2016), PP 93-100 www.iosrjournals.org Bode index as a predictor of severity
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VII (May. 2016), PP 93-100 www.iosrjournals.org Bode index as a predictor of severity
The History and Future Treatment of Emphysema Emphysema Valves, Emphysema Coils and Volume Reduction Surgery
 The History and Future Treatment of Emphysema Emphysema Valves, Emphysema Coils and Volume Reduction Surgery Dr Nabil Jarad PhD FRCP Consultant Respiratory Physician Bristol Royal Infirmary Bristol BS2
The History and Future Treatment of Emphysema Emphysema Valves, Emphysema Coils and Volume Reduction Surgery Dr Nabil Jarad PhD FRCP Consultant Respiratory Physician Bristol Royal Infirmary Bristol BS2
University of Groningen
 Endobronchial Valves for Endoscopic Lung Volume Reduction Slebos, Dirk; Shah, Pallav L.; Herth, Felix J. F.; Valipour, Arschang Published in: Respiration DOI: 10.1159/000453588 IMPORTANT NOTE: You are
Endobronchial Valves for Endoscopic Lung Volume Reduction Slebos, Dirk; Shah, Pallav L.; Herth, Felix J. F.; Valipour, Arschang Published in: Respiration DOI: 10.1159/000453588 IMPORTANT NOTE: You are
Predictive Models of Emphysema Progression in HIV
 Predictive Models of Emphysema Progression in HIV Janice Leung, MD FRCPC A. Malagoli, A. Santoro, G. Besutti, G. Ligabue, D. Dai, J. Mayo, S. Lam, D. Sin, S. Man, G. Guaraldi COPD: An Emerging Comorbidity
Predictive Models of Emphysema Progression in HIV Janice Leung, MD FRCPC A. Malagoli, A. Santoro, G. Besutti, G. Ligabue, D. Dai, J. Mayo, S. Lam, D. Sin, S. Man, G. Guaraldi COPD: An Emerging Comorbidity
A perspective on lung volume reduction surgery for pulmonary emphysema
 Perspective Page 1 of 9 A perspective on lung volume reduction surgery for pulmonary emphysema Mariano Di Martino, Prity Gupta, David A. Waller Barts Thorax Centre, Barts Health NHS Trust, London, UK Correspondence
Perspective Page 1 of 9 A perspective on lung volume reduction surgery for pulmonary emphysema Mariano Di Martino, Prity Gupta, David A. Waller Barts Thorax Centre, Barts Health NHS Trust, London, UK Correspondence
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: bronchial_thermoplasty 10/2010 3/2018 3/2019 3/2018 Description of Procedure or Service Bronchial thermoplasty
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: bronchial_thermoplasty 10/2010 3/2018 3/2019 3/2018 Description of Procedure or Service Bronchial thermoplasty
The role of a multidisciplinary severe chronic obstructive pulmonary disease hyperinflation service in patient selection for lung volume reduction
 Review Article The role of a multidisciplinary severe chronic obstructive pulmonary disease hyperinflation service in patient selection for lung volume reduction Joyce Chew, Ravi Mahadeva Cambridge COPD
Review Article The role of a multidisciplinary severe chronic obstructive pulmonary disease hyperinflation service in patient selection for lung volume reduction Joyce Chew, Ravi Mahadeva Cambridge COPD
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Double Y-stenting for tracheobronchial stenosis
 ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
Prognostic evaluation of COPD patients: GOLD 2011 versus BODE and the COPD comorbidity index COTE
 For numbered affiliations see end of article. Correspondence to Dr Juan P de Torres, Pulmonary Department, Clínica Universidad de Navarra, Avda Pio XII, 36, Pamplona 31200, Spain; jpdetorres@unav.es Received
For numbered affiliations see end of article. Correspondence to Dr Juan P de Torres, Pulmonary Department, Clínica Universidad de Navarra, Avda Pio XII, 36, Pamplona 31200, Spain; jpdetorres@unav.es Received
Title: Real-life use of inhaled corticosteroids in COPD patients vs. GOLD proposals: a paradigm shift in GOLD 2011?
 ERJ Express. Published on October 31, 2013 as doi: 10.1183/09031936.00162313 Letter to the Editor Title: Real-life use of inhaled corticosteroids in COPD patients vs. GOLD proposals: a paradigm shift in
ERJ Express. Published on October 31, 2013 as doi: 10.1183/09031936.00162313 Letter to the Editor Title: Real-life use of inhaled corticosteroids in COPD patients vs. GOLD proposals: a paradigm shift in
Health-related quality of life is associated with COPD severity: a comparison between the GOLD staging and the BODE index
 Chronic Respiratory Disease 2009; 6: 75 80 http://crd.sagepub.com ORIGINAL PAPER Health-related quality of life is associated with COPD severity: a comparison between the GOLD staging and the BODE index
Chronic Respiratory Disease 2009; 6: 75 80 http://crd.sagepub.com ORIGINAL PAPER Health-related quality of life is associated with COPD severity: a comparison between the GOLD staging and the BODE index
APSR RESPIRATORY UPDATES
 APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
Pulmonary Fissure Integrity and Collateral Ventilation in COPD Patients
 and Collateral Ventilation in COPD Patients Jiantao Pu 1,2,3 *, Zhimin Wang 1, Suicheng Gu 1, Carl Fuhrman 1, Joseph K. Leader 1, Xin Meng 1, John Tedrow 4, Frank C. Sciurba 4 1 Imaging Research Center,
and Collateral Ventilation in COPD Patients Jiantao Pu 1,2,3 *, Zhimin Wang 1, Suicheng Gu 1, Carl Fuhrman 1, Joseph K. Leader 1, Xin Meng 1, John Tedrow 4, Frank C. Sciurba 4 1 Imaging Research Center,
Bronchial valve treatment for pulmonary air leak after anatomic lung resection for cancer.
 ERJ Express. Published on November 14, 2013 as doi: 10.1183/09031936.00117613 Bronchial valve treatment for air leak. Bronchial valve treatment for pulmonary air leak after anatomic lung resection for
ERJ Express. Published on November 14, 2013 as doi: 10.1183/09031936.00117613 Bronchial valve treatment for air leak. Bronchial valve treatment for pulmonary air leak after anatomic lung resection for
Imaging biomarkers for patient selection and treatment planning in emphysema
 Review Imaging biomarkers for patient selection and treatment planning in emphysema Emphysema is a disease that causes destruction of lung tissue and an overall reduction in lung compliance as air becomes
Review Imaging biomarkers for patient selection and treatment planning in emphysema Emphysema is a disease that causes destruction of lung tissue and an overall reduction in lung compliance as air becomes
Parametric response mapping
 Parametric response mapping Utility of a novel imaging biomarker in pulmonary disease Dharshan Vummidi MD, Lama VN MD, Yanik G MD, Kazerooni EA MD, Meilan Han MD, Galban C PhD Radiology, Pulmonary & Critical
Parametric response mapping Utility of a novel imaging biomarker in pulmonary disease Dharshan Vummidi MD, Lama VN MD, Yanik G MD, Kazerooni EA MD, Meilan Han MD, Galban C PhD Radiology, Pulmonary & Critical
C hronic obstructive pulmonary disease (COPD) is a
 288 CHRONIC OBSTRUCTIVE PULMONARY DISEASE Altered thoracic gas compression contributes to improvement in spirometry with lung volume reduction surgery A Sharafkhaneh, S Goodnight-White, T M Officer, J
288 CHRONIC OBSTRUCTIVE PULMONARY DISEASE Altered thoracic gas compression contributes to improvement in spirometry with lung volume reduction surgery A Sharafkhaneh, S Goodnight-White, T M Officer, J
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Coexistence of confirmed obstruction in spirometry and restriction in body plethysmography, e.g.: COPD + pulmonary fibrosis
 Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Bronchodilator responsiveness in patients with COPD
 Eur Respir J 28; 31: 742 75 DOI: 1.1183/931936.12967 CopyrightßERS Journals Ltd 28 Bronchodilator responsiveness in patients with COPD D.P. Tashkin*, B. Celli #, M. Decramer ", D. Liu +, D. Burkhart +,
Eur Respir J 28; 31: 742 75 DOI: 1.1183/931936.12967 CopyrightßERS Journals Ltd 28 Bronchodilator responsiveness in patients with COPD D.P. Tashkin*, B. Celli #, M. Decramer ", D. Liu +, D. Burkhart +,
CT Assessment of Lobar Heterogenity and Fissure Integrity in Pulmonary Emphysema for Bronchoscopic Lung Volume Reduction with Valve
 CT image analysis of emphysema. 77 Original Article J. St. Marianna Univ. Vol. 5, pp. 77 83, 2014 CT Assessment of Lobar Heterogenity and Fissure Integrity in Pulmonary Emphysema for Bronchoscopic Lung
CT image analysis of emphysema. 77 Original Article J. St. Marianna Univ. Vol. 5, pp. 77 83, 2014 CT Assessment of Lobar Heterogenity and Fissure Integrity in Pulmonary Emphysema for Bronchoscopic Lung
Lung Volume Reduction Surgery for Severe Emphysema. Original Policy Date
 MP 7.01.55 Lung Volume Reduction Surgery for Severe Emphysema Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
MP 7.01.55 Lung Volume Reduction Surgery for Severe Emphysema Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
POLICIES AND PROCEDURE MANUAL
 POLICIES AND PROCEDURE MANUAL Policy: MP060 Section: Medical Benefit Policy Subject: Lung Volume Reduction Surgery I. Policy: Lung Volume Reduction Surgery II. Purpose/Objective: To provide a policy of
POLICIES AND PROCEDURE MANUAL Policy: MP060 Section: Medical Benefit Policy Subject: Lung Volume Reduction Surgery I. Policy: Lung Volume Reduction Surgery II. Purpose/Objective: To provide a policy of
Chronic obstructive pulmonary disease in over 16s: diagnosis and management
 National Institute for Health and Care Excellence Final Chronic obstructive pulmonary disease in over 16s: diagnosis and management [D] Diagnosing COPD and predicting outcomes NICE guideline NG115 Evidence
National Institute for Health and Care Excellence Final Chronic obstructive pulmonary disease in over 16s: diagnosis and management [D] Diagnosing COPD and predicting outcomes NICE guideline NG115 Evidence
TITLE: VALIDATION OF THE CONCEPT OF CONTROL OF COPD IN CLINICAL PRACTICE
 RESPIRATORY EFFECTIVENESS GROUP (REG) RESEARCH PROPOSAL TITLE: VALIDATION OF THE CONCEPT OF CONTROL OF COPD IN CLINICAL PRACTICE PREPARED BY: Marc Miravitlles (on behalf of REG) PREPARED FOR: Novartis
RESPIRATORY EFFECTIVENESS GROUP (REG) RESEARCH PROPOSAL TITLE: VALIDATION OF THE CONCEPT OF CONTROL OF COPD IN CLINICAL PRACTICE PREPARED BY: Marc Miravitlles (on behalf of REG) PREPARED FOR: Novartis
Supplementary Appendix
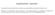 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Woodruff PG, Barr RG, Bleecker E, et al. Clinical significance
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Woodruff PG, Barr RG, Bleecker E, et al. Clinical significance
ERS Annual Congress Milan September 2017 Skills workshop SW 8, 10, 12 Endoscopy
 ERS Annual Congress Milan 09 13 September 2017 Skills workshop SW 8, 10, 12 Endoscopy Monday, 11 September 2017 08:00 10:20 10:40 13:00 14:30 16:50 Green 1 (North) MICO You can access an electronic copy
ERS Annual Congress Milan 09 13 September 2017 Skills workshop SW 8, 10, 12 Endoscopy Monday, 11 September 2017 08:00 10:20 10:40 13:00 14:30 16:50 Green 1 (North) MICO You can access an electronic copy
Referring for specialist respiratory input. Dr Melissa Heightman Consultant respiratory physician, UCLH,WH, CNWL
 Referring for specialist respiratory input Dr Melissa Heightman Consultant respiratory physician, UCLH,WH, CNWL Respiratory Specialist- who? GPSI Community Team Secondary Care Respiratory physician and
Referring for specialist respiratory input Dr Melissa Heightman Consultant respiratory physician, UCLH,WH, CNWL Respiratory Specialist- who? GPSI Community Team Secondary Care Respiratory physician and
