A nonprofit independent licensee of the Blue Cross Blue Shield Association. Managing Your Asthma
|
|
|
- Madeleine Nelson
- 5 years ago
- Views:
Transcription
1 A nonprofit independent licensee of the Blue Cross Blue Shield Association Managing Your Asthma
2 Excellus Health Plan, Inc. 2010
3 Contents Introduction...1 Goals...1 What is Asthma...2 Asthma Signs and Symptoms...3 Asthma Triggers Asthma Treatment...5 Medications Inhaler/Nebulizer Peak Flow Meter...10 Asthma in School...10 Asthma In the Workplace...11 Traveling with Asthma...12 Croup...12 Asthma Diary...13
4
5 Introduction Working with your doctor Feeling comfortable talking with your doctor is an important step to managing your asthma. This will help you play an active role as a team member with your doctor. Good management of your asthma will allow you to take charge of your life. Here are some tips to help with asthma management: G Learn what asthma is and what your triggers are. G Take your medications as prescribed. G Learn to use the devices correctly. G Keep an asthma diary that includes symptoms, activities and peak flow readings (if you are measuring peak flow). G Obtain a yearly flu vaccine. If possible, have all family members get a flu vaccine. G Talk with your doctor regarding a pneumonia vaccine to see if you are a candidate. G Work with your doctor to see if an asthma action plan is needed. G Understand any changes in the asthma treatment and/or asthma action plan. G Make a list of questions or concerns prior to your doctor s appointment. G Schedule a doctor s visit just for asthma at least every six months. Tell your doctor G How often you are using your rescue inhaler. G What asthma symptoms you have. G How often nighttime symptoms occur. G If your asthma is limiting your ability to exercise, work, attend school or do other daily activities. Goals Goals of asthma care: G No asthma symptoms day or night. G No missed school/work/home activities. G Maintain normal or near-normal lung function. G Little or no use of rescue inhaler. G No adverse effects from medications. 1
6 What Is Asthma What is normal breathing? Normal breathing is when air (oxygen) comes in through your nose and mouth and goes through your airways to your lungs. The air ends up in small sacs called alveoli in your lungs. When you breathe out, you get rid of carbon dioxide from your body. What is asthma? Asthma is a chronic inflammatory disorder of the airways. Inflammation and tightening in the airways of your lungs make it hard for you to breathe. With asthma, inflammation is always present, but you may not notice it until you come in contact with a trigger. Here is what happens: Inflammation The cells of the inside walls of the airways become swollen and irritated. As these cells swell, they rupture and leak fluid into the airways. This produces a thick mucous, making the airways smaller and more difficult for the air to pass through into the lungs. Tightening (constriction) There are also muscle bands that surround the airways. They help to hold the airways open so air can pass through. When they cannot expand any further because of the swelling, they twitch (bronchospasm) and squeeze with each breath. The tightening causes the airways to become narrow so air cannot get through. This may cause you to feel tightness in your chest. Some of the airways are so tiny that there is not much room for swelling and mucous. The mucous then plugs the airways, which causes you to start coughing and makes it difficult for you to breathe. In some people, this inflammation causes recurrent episodes of coughing, wheezing, breathlessness and chest tightness. These are warning signs that something is wrong. You should learn what your particular symptoms are. Asthma flare-ups can be related to many different causes It is not known why some people have asthma and others do not. Heredity may be the reason for many people. For others, allergens or irritants in the air can trigger an allergic reaction, causing asthma to flare up. However, no matter what the cause is, we do know the basic problem is inflammation and constriction of the airways. *****Plants with pretty flowers are typically insect-pollinated. Very little of the pollen becomes airborne to cause allergy symptoms. Allergic Asthma: Triggered by inhaling or ingesting an allergen that causes an allergic reaction. Pollen from trees, weeds, grass Dust mites Mold spores Cockroaches Animal dander Food allergies Aspirin or other non-steroidal antiinflammatory medication Insect stings Non-A Non-Allergic Asthma: Trigger may be something irritating the airways rather than an allergen. Anxiety, stress, crying Exercise Cold air or dry air Hyperventilation Cigarette smoke or campfire smoke Viruses Chemical fumes Perfumes and scented candles Heartburn and GERD (gastroesophageal reflux disease) 2
7 Asthma Signs And Symptoms An asthma attack can happen suddenly or over a few days. These symptoms can occur anytime. It is important to know what triggers your asthma symptoms. Talk with your doctor if your asthma is not controlled. Asthma cannot be cured, but it can be controlled with medications and scheduled visits to your doctor. It is important to work with your doctor to develop an action plan. An action plan will include instructions of what to do when symptoms occur. Symptoms may include Breathing fast. Having less energy. Waking at night. Wheezing a whistling noise with breathing. Constant cough with or without mucous. Shortness of breath. Tightness in the chest. Allergy symptoms Sneezing. Runny nose. Stuffy nose. Coughing. Itchy, watery eyes; itchy nose and roof of mouth. Dark circles under eyes. Some asthmatics also have allergies to food, medicine, insect bites or latex. Your doctor may prescribe an Epipen for a severe allergy. This medication should be used at the earliest sign of severe allergy. You should always carry it with you. G When a severe asthma attack or allergy attack occurs, get help and call 911. A severe asthma attack can include: Difficulty talking. Blue-colored lips and/or grayishcolored skin. Using neck or chest muscles to breathe. Coughing that leads to vomiting. Signs of a severe allergy attack include: Itching or hives within minutes. Swelling of the lips, face and tongue. Difficulty swallowing or drooling. Dizziness or fainting. Vomiting. Trouble breathing. Asthma Triggers An asthma trigger sets off your asthma Here are some triggers and how to avoid or control them. Allergens Animal Dander - dried saliva on fur or feathers of pets can increase asthma symptoms. Dust Mites - tiny bugs found in mattresses and pillows, cloth furniture, carpeting. Many people with asthma react to dust mite droppings. Keep pets outdoors if possible; keep them out of the bedroom and away from carpeted surfaces. Keep bedroom doors closed. Keep pets away from cloth furniture and carpets. Bathe animals often. Consider shorthaired or non-shedding pets. Cover mattresses and pillows with allergy-proof covers. Wash sheets, pillowcases and blankets weekly in hot water that is at least 130ºF. Keep humidity in house low. Vacuum often with a HEPA (high efficiency particulate air) filter. Damp-mop non-carpeted floors frequently. Replace curtains or drapes with blinds, if possible. Keep stuffed toys to a minimum and wash frequently. 3
8 Cockroaches - some people with asthma react to cockroach droppings. Use closed containers for food not stored in the refrigerator. Keep garbage in closed container outside of house. Use pesticides cautiously and when asthma patient is out of house. Keep all poison bait away from children and pets. Pollen - budding trees, grass and weeds may affect asthma symptoms. Stay indoors when pollen count is high and during warmest part of the day. Use air conditioning for filtering these particles from household air. Shower and shampoo hair before going to bed. Avoid hanging laundry outside. Molds - damp or moist areas of your home promote mold growth. Use exhaust fan when showering. Check for and repair water leaks in basements, inside walls and under sinks. Use household cleaners that are safe for the environment. Outdoor mold grows on falling leaves. Avoid raking leaves or wear a mask while raking. Eliminate areas of standing water outside. This will decrease mold growth. Irritants Smoke - any form of smoke: tobacco, wood stove, campfire or barbecue can trigger asthma symptoms. If you smoke - quit. If a loved one smokes - encourage him or her to quit. Avoid secondhand smoke in automobiles, homes and other enclosed areas. Limit exposure to wood stoves and fireplaces. Make sure they are well vented. Do not store wood inside, which will also promote mold growth. Air irritants - small, invisible particles in the air may cause irritation in your airways. Stay indoors, close windows and use air conditioning during ozone alerts. Avoid using perfume, scented hair products, air fresheners and strongsmelling household cleaners. Avoid burning scented candles. Weather factors - weather extremes may affect your asthma. Wear a scarf over nose and mouth during cold, dry weather. Limit time outdoors during high humidity and ozone alerts. Exercise - exercise can help asthma and can cause flare-ups. Speak with your health care provider before starting an exercise program. Provider may recommend medication use prior to activity. Try warming up for exercise, such as slow walking. Avoid outdoor exercise during extreme weather (high humidity, high temperature, frigid air). Carry your rescue inhaler at all times. Cold and respiratory infections - can increase lung inflammation, making it difficult to breathe. Prevention is the key. Talk with your provider about getting an annual flu shot and a pneumonia shot every 10 years. Help prevent viral respiratory infection by: Frequent hand washing. Cover your mouth and nose when sneezing or coughing. Disinfecting doorknobs, railings and shared items, such as telephones, keyboards and computer equipment. Avoid sharing drinking and eating utensils. Other asthma triggers include Reflux - indigestion or heartburn. Emotions - laughing, crying, anger, anxiety or stress. Work place triggers - asthma triggers in the work place may be a result of fumes from chemicals, paint, cleaning products, exhaust, cooking and baking products. Also particles or smells from carpeting, furniture and newly painted or remodeled areas. Report increased asthma symptoms at work to your supervisor and health care provider. Wear a mask when chemicals are being used. 4
9 Asthma Treatment It is recommended that a specialist (allergist or pulmonologist) be seen if: G Your asthma is not controlled. G Your asthma episodes result in emergency room visits or hospital admissions. G You need more education about asthma. G You need more testing. G You are not meeting your therapy goals in three to six months. G You have other medical conditions that affect your asthma. G An asthma specialist may try other treatment and testing options such as: Pulmonary functioning tests. Skin prick test for allergies. Blood test for allergies. Medications. Medications Medications: How do they work? Even though there is no cure for asthma, it can be controlled. The goal: G reduce the need to use your rescue inhaler. G prevent asthma attacks from occurring. Metered-dose inhaler devices, (MDIs) are made to release a premeasured amount of medication. MDIs deliver commonly used asthma medication to help open up the airways and make breathing easier. They are especially important for delivering quick relief medication in case of an asthma attack. MDIs are also used to deliver long-term control medications, anti-inflammatory medication and longacting bronchodilators. Two basic categories of medications: Category 1 Corticosteroid medication: Control medications. G They help to prevent and reduce the swelling in your air tubes and decrease the mucous. G You will not feel anything happening immediately after using your controller medication, but with continued use, you will notice fewer symptoms of asthma and less frequent need to use your quick reliever medication. G It is important that you take your controller medication everyday as prescribed for maximum benefit. G Never use your controller medications to relieve a sudden asthma attack. Side effects are uncommon: Oral thrush (yeast infection in the mouth). Hoarseness. Sore throat. Nervousness. Nausea. Having difficulty sleeping. Tell your doctor if you feel like this. He or she may want to change your dose or try a different medication. Be sure to rinse your mouth out after using your medication to prevent thrush and reduce hoarseness. Some people do not like it when they hear a medication has a steroid in it. Corticosteroids are not the steroids used by athletes. Those steroids are called anabolic steroids. Corticosteroids are safe to take for your asthma. Use of high-dose inhaled corticosteroids. Parents may worry about the effect on growth rate in their children if they are on these medications long term, but severe asthma that is uncontrolled can also reduce growth. Elderly patients who have been on high-dose inhaled corticosteroids may experience changes in their bone density and skin thickness. 5
10 These side effects are rare and less likely than those of oral steroids. Leukotriene antagonists: On occasion, people are put on these mildly anti-inflammatory medications. G Prevent airways from swelling when they come in contact with an asthma trigger. G These non-steroids can also help prevent asthma caused by exercise. Long-acting beta 2 agonists - Should not be used as a quick relief medication for an asthma attack. G Should not be taken without an inhaled corticosteroid. G Helps control daily symptoms of asthma, including nighttime asthma. G Can be used to prevent asthma induced by exercise. G There are commercially available inhalers that contain both an inhaled corticosteroid and a long-acting beta 2 agonist in one inhaler Oral corticosteroids (not anabolic steroids) - The hospital or your doctor may put you on this medication short-term to help get your asthma back under control quickly. Used as short-term treatment when you have a severe asthma attack. Quickly reduces inflammation. Category 2 Quick relief medications Short-acting bronchodilators - Rescue medication. G Help to stop an asthma attack after it has started. G Open airways by relaxing muscles that tighten the airways during an asthma attack. G Help prevent expected asthma attacks caused by exercise. Side Effects: Nervousness. Rapid heart rate. 6 Frequently Asked Questions About Controller Rescue Asthma Medications: Medication Medication Will I feel an immediate relief after using my inhaler? No Yes Is this medication used to stop an asthma attack? No Yes Can this medication cure my asthma? No No Can this medication be taken daily? Yes No Can I use this medication before I exercise? No Yes Will this medication help decrease swelling Yes No and mucous? Should I prime my inhaler first before using it? Yes Yes Dry-powdered inhaler: These inhalers release a fine dry powder with a quick and steady deep breath. There is no propellant to deliver the medication. These devices are dependent on the force of your inhalation to get the medication into your lungs. Side effects: Usually minor. Because it is a powder, much of the medication is left in the mouth and throat as you breathe it in, giving you a bad taste and even a little irritation to the tongue and throat. Rinsing your mouth out after every use will help eliminate this. You may also end up swallowing some of the medication that remains after rinsing, which can cause a minor upset stomach or heartburn. If this should occur, be sure to let your doctor know. Please note that many decongestants are not recommended for use in children. These medications should not be used in children under 2 years of age. Most products contain labels stating the medication should not be used for children under 4 or 6 years of age. A more common side effect is a yeast infection or oral thrush in the mouth and throat, which appears as a white coating of the mouth and throat. This is easily treated by your doctor. Allergy medication: Antihistamines: Relieve sneezing, itching and runny nose. They work best if taken routinely during the allergy season. They block the effect of histamine (a substance made by the body during an allergic reaction). Decongestants: Work by narrowing blood vessels and reducing fluid in the affected area, which helps clear congestion and improve breathing. Oral decongestants relieve stuffy nose and drainage. Please note that many decongestants are not recommended for use in children. These medications should not be used in children under 2 years of age. Most products contain labels stating the medication should not be used for children under 4 or 6 years of age. Leukotriene [loo-kuh-trahy-een] modifiers: Are not steroid medications but are long-term controller medications. They help reduce airway inflammation and swelling, decrease the amount of mucous and open the airways. The month before allergy season is the best time to start taking allergy medication. Your doctor may recommend an allergy medication to help control your symptoms, or he may recommend an over-the-counter allergy medication.
11 Inhaler/Nebulizer How to use an inhaler A metered dose inhaler, MDI, is a device to deliver asthma medication to your lungs. Prime If this is your first time using an inhaler, you will need to prime it. You should also prime an inhaler if it has been longer than two weeks since you last used it. 1. Take the cap off the mouthpiece. 2. Shake the inhaler for 5 seconds. 3. Press down on the canister, spaying the medication into the air two times (away from your face). Look to see if a fine mist has been released. Regular use 1. Remove cap and hold inhaler upright. 2. Shake inhaler five to 10 times to mix medicine. 3. Attach spacer if indicated by your doctor. 4. Take a deep breath, then exhale completely. 5. Place the mouthpiece in your mouth if using the closed-mouth method. 6. Close your lips around it tightly. 7. When using the open-mouth method, place inhaler 2 inches from open mouth. 8. Begin to breathe in slowly while you press down to release a puff of medication. 9. Hold your breath for five to ten seconds. This will allow medication to get deep into your lungs. 10. Breathe out slowly. 11. Repeat puffs as directed. Wait two to five minutes between puffs. How to use a spacer Your doctor may recommend using a spacer. It attaches to the inhaler. It holds the medication in a chamber. A spacer is recommended for use with all inhaled corticosteroids. It is also suggested for use with all MDI inhalers. Ask your doctor what is best for you. 1. Take deep breaths to inhale the dose of medication and hold your breath. 2. Repeat for second puff. Care of a metered dose inhaler It is important to keep your inhaler clean and ready for use. 1. Remove mouthpiece from canister. Rinse after each use. 2. If the mouthpiece or spacer becomes dirty, wash with mild soap and warm water. 3. Rinse well. 4. Always allow it to air dry completely. 5. Store inhaler in a cool dry place. Avoid placing it in sunlight. Do not store in car or near open flames. How to use dry powder diskus-type inhaler 1. The diskus inhaler is closed when you open original package. 2. An indicator may tell you how many doses are left. 3. Diskus inhalers may have an alert when doses are getting low. 4. Numbers will appear in red when you have about five doses left. Taking a dose Open 1. Hold inhaler in one hand. 2. Place thumb of the other hand on the thumb grip. 3. Push your thumb away from you until mouthpiece appears. 4. When you have pushed as far as you can, it will snap into place. Click 1. Hold inhaler level and flat. 2. Mouthpiece should be toward you. 3. Slide the lever away from you until it clicks. 4. Inhaler is now ready for use. Inhale 1. Take a deep, cleansing breath. Exhale fully. 2. Hold inhaler level. 3. Place mouthpiece to your lips. 4. Breathe in fast and deeply. 5. Take inhaler away from your mouth. 6. Hold your breath for as long as you can at least 10 seconds. 7. The medication from this inhaler is a dry powder. 8. You may be able to feel or taste it. 9. Rinse your mouth with warm water and spit it out. 7
12 Close the inhaler when finished. 1. Place thumb on thumb grip. Slide it toward you all the way. 2. It will snap shut. 3. The inhaler is now ready for your next dose. Important points for dry powder inhaler DO Use inhaler in flat position. Rinse your mouth after use. Spit out rinse water. Store inhaler in a dry place. DON T Breathe into this inhaler. Take inhaler apart. Use with a spacer. Wash mouthpiece of inhaler. Take an extra dose if you do not taste or feel medication. How to use a twist-type inhaler Some twist-type inhalers need to be primed the first time they are used. Prime 1. Hold inhaler upright. 2. Grasp colored part (bottom) in one hand. 3. Grasp top of inhaler and lift off. 4. Grasp inhaler on bottom, colored part in one hand. 5. Grasp top of inhaler in the middle with the other hand. 6. Twist bottom as far as it will go to right and then to the left. 7. Then twist it in the other direction until it clicks. 8. Twist back and forth again. 9. Priming is complete. Remember when using dry powder or twist inhalers: DO Always hold inhaler level. Always hold inhaler upright when priming or loading. Always rinse mouth with warm water after use. This will help prevent fungal infections of the mouth. Wipe mouthpiece dry. Store in a dry place. Use 1. Hold inhaler in upright position. 2. Twist bottom of inhaler all the way to the right and back to the left. 3. Inhaler will click. 4. This loads a dose of medication. 5. Breathe out completely facing away from the inhaler. DON T Shake inhaler after loading dose. Exhale into inhaler. Swallow water you have rinsed your mouth with. Prime inhaler after the first use. Hold inhaler at the top of the mouthpiece. 6. Close lips around mouthpiece. 7. Inhale as deeply and forcefully as you can. 8. Remove from mouth and exhale. 9. Replace cover. 10. Rinse mouth with warm water and spit out. 8
13 How to use a nebulizer A nebulizer uses air to make a mist of your asthma medication. Breathe the mist into your lungs. 1. Your medicine may already be mixed. 2. Open it and place in the cup. 3. Attach the mouthpiece to the cup. 4. Attach these to the tubing of the machine. 5. Place mouthpiece in mouth. 6. If you use a mask, place it over your mouth and nose. 7. Turn on the machine. 8. Take deep, slow breaths through your mouth. 9. Try to hold each breath for two seconds. 10. Continue until medication is gone. This will be about 10 minutes. Care of a nebulizer Cleaning your nebulizer is very important. This helps prevent infections. Proper cleaning also makes the machine last longer. 1. Remove mouthpiece or mask from the cup. 2. Remove tubing. 3. Wash all parts, except tubing and machine. Use mild dish soap and warm water. 4. Rinse completely with warm water. 5. Shake off excess water. 6. Place on dry, clean cloth or paper towel. 7. Allow to air dry. 8. Attach parts and run machine 10 to 20 seconds. This will dry inside of machine. 9. Remove tubing. Store machine and parts in a plastic bag. 19. Twice a week, soak parts (not tubing or machine) in one part distilled white vinegar and two parts water. 11. Soak for 30 minutes. 12. Rinse parts for one minute. 13. Allow to air dry. 14. Put parts together. 15. Run machine 10 to 20 seconds. This will dry inside of machine. 9
14 Peak Flow Meter The peak flow meter is a monitoring device that helps measure how well air is coming out of your lungs. This measurement can be used to find out if you have reduced airflow hours or days before you have an asthma flare-up. This will allow you to use your rescue medication to stop the flare-up quickly. The meter is easy to use. Take a reading before you take your asthma medicine in the late afternoon or early evening. Asthma In School G Most common disease among children. G Leading cause of missed school days. It is very important to have a written asthma action plan from your doctor if your child has persistent asthma. If you use a rescue inhaler only for gym class or other sports, your doctor will write instructions. Always notify the school nurse of any illness.an asthma action plan should include: medications and dosages. asthma symptoms. peak flow readings if used. triggers. Inhaler required before gym or recess. Meet with the school staff yearly to talk about the following: How to use a peak flow meter 1. Hold the meter in your hand. 2. Move the pointer to zero. 3. Stand up. 4. Take a deep breath. 5. Place the meter in your mouth. Seal your lips around the mouthpiece. 6. Blow out as hard and fast as you can. 7. Write down the number at the pointer. 8. Repeat this two more times. 9. Record your best of three tries on your asthma diary. Asthma symptoms and triggers. Your child s ability to recognize symptoms. Emergency phone number for the parent or guardian and doctor. Discuss the school rules for medications. Who would be available to handle asthma symptoms for upcoming field trips? Changes in the classroom, such as new pets (gerbils, hamsters), construction, new cleaning products or classroom supplies (paints, glues, eraser dust). New York state has a law in place that allows children with severe asthma to carry their quick relief medication with them while in school. It is best to talk to your doctor regarding these rules and requirements. The highest reading you can record is called your personal best reading. Your doctor will use this reading for your asthma treatment. 10
15 Asthma In The Work Place Dust (dander) from animals and insects. Dust from wood, latex gloves, flour and poorly cleaned buildings. Mold in damp or water-damaged parts of buildings. Physical stimuli (cold/heat, humidity). Symptoms Refer to Asthma Signs and Symptoms You may be exposed to many different particles at work. Your employer should give you information of possible danger connected to your job. Your employer should keep a healthy work place. Special equipment may be needed to protect you. Report any unhealthy work conditions to your employer. Occupational asthma is worsening of symptoms in workers with a previous history of asthma. A worker with no previous history of asthma can also develop occupational asthma. Aggravated asthma is due to repeated contact to dust and fumes. Being in contact with these triggers is considered an irritation to the lungs. Early diagnosis and treatment may help end symptoms. Some common jobs with allergen or irritant exposure: Office workers. Construction workers, including welders. Janitors and cleaners. Farmers, bakers and grain handlers. Beauty salon workers. Teachers. Triggers: Each person has different triggers that start asthma attacks. Some triggers in the work place may include: Chemicals in paints, cleaning products and other things. Refer to work place triggers on page 4. Patterns of symptoms: Improvement of symptoms occurs during vacations or days off (may take a week or more). Symptoms may occur immediately (less than one hour), delayed (most commonly within two to eight hours after exposure), or at night. Initial symptoms may occur after high-level exposure (for example, chemical spills). Once sensitized, patients with occupational asthma may react to extremely low levels of airborne allergen. What can you do? Let your doctor know about your current job and other jobs you have had. Keep a daily record of your symptoms and asthma attacks. Let your doctor know when your asthma gets better or worse. Avoid triggers. Move to another work area. Wear proper equipment. You should work with your employer to remove yourself from triggers. 11
16 Traveling With Asthma Croup There are important things to do before going away when you have asthma. Your asthma should be controlled. Carry your inhalers and other asthma medications with you at all times. Bring a list of medications and dosages. Bring your doctor s and pharmacy name and phone numbers. Take a copy of your asthma action plan. Have enough medications to last the whole trip. Let family or friends know triggers ahead of time. Find out pollen counts and smog levels. While traveling, your living space should be: Smoke-free. Pet-free. Dusted. Vacuumed. Aired out. Remember that you may be in contact with triggers when using public transportation. Drink plenty of fluids when the air is dry to help prevent symptoms. Traveling by car Before traveling, run the air conditioner or heater for 10 minutes while the windows are open. This will help remove any odors or dust in the vents. Traveling by plane Check to see that it is a non-smoking flight (outside of the U.S.) Make sure that all medications have the original prescription label. What is it: G Inflammation in the upper airways voice box and windpipe. G Caused by a virus. G Most common in children (six months to three years). G Occurs in the fall/early winter. G Contagious through coughing, sneezing and close contact. Signs and symptoms: G Can start as a common cold, stuffy, runny nose and fever. G Child becomes hoarse with a loud, harsh barking cough like a barking seal. G Worse at night and when the child is upset or crying. G You may hear a high-pitched or squeaking noise as the child inhales (called stridor). G Breathing may be very fast and may have retractions. G Lasts two to five days. G Dehydration can occur. Resources - Centers for Disease Control and Prevention - New York State Department of Health - National Heart, Lung and Blood Institute - American Lung Association Treatment: G Try to stay calm and soothe your child. G Fill bathroom with steam and sit for 10 minutes, breathing in moist air. G Breathing cool, night air may help. G Humidifier in the child s room at night. G Do not smoke. G Keep child hydrated. G If symptoms do not improve in 30 minutes, call the doctor. 12
17 Asthma Diary This is a record of your peak flow readings, symptoms and medications. This log helps you and your doctor manage your asthma. Complete this form and take it to your next doctor s visit. Week of: My personal best is My green zone is liters per second (80% to 100% of my personal best*) My yellow zone is liters per second (50% to less than 88% of my personal best*) My red zone is less than liters per second (less than 50% of my personal best*) * To figure out 80% of personal best peak flow, multiply your personal best by To figure out 50% of personal best peak flow, multiply your personal best by My current long-term medications are: Date AM PM peak flow Trigger Symptoms Quick-relief medication Red zone visit and response to doctor Green Yellow Red or hospital? This information does not replace the advice of a doctor. 13
18
19
20 B-3165/ MCM excellusbcbs.com
Asthma Triggers. It is very important for you to find out what your child s asthma triggers are and learn ways to avoid them.
 Asthma s It is very important for you to find out what your child s asthma triggers are and learn ways to avoid them. With asthma, your child s airways are very sensitive. Things, called triggers, may
Asthma s It is very important for you to find out what your child s asthma triggers are and learn ways to avoid them. With asthma, your child s airways are very sensitive. Things, called triggers, may
CARE AT HOME: ASTHMA. A guide for parents. childrensmn.org
 CARE AT HOME: ASTHMA A guide for parents childrensmn.org Content Your child has asthma a chronic lung disease. To best control the symptoms of asthma, it is important that you learn all you can about asthma.
CARE AT HOME: ASTHMA A guide for parents childrensmn.org Content Your child has asthma a chronic lung disease. To best control the symptoms of asthma, it is important that you learn all you can about asthma.
ASTHMA CONTROL. Asthma is a chronic airway disease. You cannot cure asthma, but you can control it. Treatment can improve asthma symptoms.
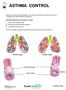 ASTHMA CONTROL Asthma is a chronic airway disease. You cannot cure asthma, but you can control it. Treatment can improve asthma symptoms. Asthma changes the lung airways in 3 ways: 1. Lining of the airways
ASTHMA CONTROL Asthma is a chronic airway disease. You cannot cure asthma, but you can control it. Treatment can improve asthma symptoms. Asthma changes the lung airways in 3 ways: 1. Lining of the airways
Breathe Easy. Tips for controlling your Asthma
 Breathe Easy Tips for controlling your Asthma Have you or a family member been told you have asthma? Are you or a family member coughing or wheezing? Do you or a family member have tightness in your chest?
Breathe Easy Tips for controlling your Asthma Have you or a family member been told you have asthma? Are you or a family member coughing or wheezing? Do you or a family member have tightness in your chest?
Kickin Asthma. Workbook for Children with Asthma. Name:
 Kickin Asthma Workbook for Children with Asthma Name: Why Have You Been Invited to Kickin Asthma? You have been invited to Kickin Asthma because you have asthma. Asthma is a disease of your air tubes that
Kickin Asthma Workbook for Children with Asthma Name: Why Have You Been Invited to Kickin Asthma? You have been invited to Kickin Asthma because you have asthma. Asthma is a disease of your air tubes that
In case of an urgent concern or emergency, call 911 or go to the nearest emergency department right away.
 Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Breathe Easy. Living with Asthma
 Breathe Easy Living with Asthma Got Asthma? You re Not Alone! More than 300 million people around the world have asthma. But having asthma doesn t have to limit what you can do. With education and treatment,
Breathe Easy Living with Asthma Got Asthma? You re Not Alone! More than 300 million people around the world have asthma. But having asthma doesn t have to limit what you can do. With education and treatment,
Glossary of Asthma Terms
 HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
Asthma. The prevalence of asthma has been increasing worldwide, but why this is happening is not known.
 Asthma What is asthma? Asthma is a chronic disorder of the airways of the lungs. The airways are reactive and may be inflamed even when symptoms are not present. The extent and severity of airway irritation
Asthma What is asthma? Asthma is a chronic disorder of the airways of the lungs. The airways are reactive and may be inflamed even when symptoms are not present. The extent and severity of airway irritation
Sources. Taking Charge of Your Asthma. Asthma Action Plan (to be completed with your doctor) UnitedHealthcare Insurance Company
 Asthma Action Plan (to be completed with your doctor) Green Zone: (80 to 00% of my personal best) Peak Flow between and (00% = personal best) You can do all the things you usually do. Your asthma medicine
Asthma Action Plan (to be completed with your doctor) Green Zone: (80 to 00% of my personal best) Peak Flow between and (00% = personal best) You can do all the things you usually do. Your asthma medicine
Welcome to our Asthma Program
 Welcome to our Asthma Program We re here to help you be your healthiest through information, education and support for your asthma. We ll work with you by: Partnering with your health care team to make
Welcome to our Asthma Program We re here to help you be your healthiest through information, education and support for your asthma. We ll work with you by: Partnering with your health care team to make
Breathe Easy ACTIVITIES. A Family Guide to Living with Asthma F O R T H E K ! I D S
 Breathe Easy A Family Guide to Living with Asthma ACTIVITIES FUN & EDUCATIONAL F O R T H E K! I D S What Is Asthma? Asthma is a disease of the lungs. It s a chronic (long-term) condition that affects the
Breathe Easy A Family Guide to Living with Asthma ACTIVITIES FUN & EDUCATIONAL F O R T H E K! I D S What Is Asthma? Asthma is a disease of the lungs. It s a chronic (long-term) condition that affects the
Living Well with Asthma
 Living Well with Asthma Understanding Asthma Monitoring Your Breathing Using an Inhaler Reducing Triggers Staying Active Living with Asthma If you have asthma, there s good news. Today, people with asthma
Living Well with Asthma Understanding Asthma Monitoring Your Breathing Using an Inhaler Reducing Triggers Staying Active Living with Asthma If you have asthma, there s good news. Today, people with asthma
Asthma. January 2011
 Asthma January 2011 What is Asthma? Asthma is a lung disease that affects the breathing tubes (airways) that allow air to go in and out of the lungs. Normal airways are wide open, so air can go in and
Asthma January 2011 What is Asthma? Asthma is a lung disease that affects the breathing tubes (airways) that allow air to go in and out of the lungs. Normal airways are wide open, so air can go in and
MANAGING ASTHMA. Nancy Davis, RRT, AE-C
 MANAGING ASTHMA Nancy Davis, RRT, AE-C What is asthma? Asthma is a chronic respiratory disease characterized by episodes or attacks of inflammation and narrowing of small airways in response to asthma
MANAGING ASTHMA Nancy Davis, RRT, AE-C What is asthma? Asthma is a chronic respiratory disease characterized by episodes or attacks of inflammation and narrowing of small airways in response to asthma
Learners Take Action to Reduce the Risk of Asthma
 Learners Take Action to Reduce the Risk of Asthma Lesson 2: What causes asthma? Identifying Asthma Triggers Teacher Instructions, Introduction, and Student Worksheets Objectives for Lesson 2: After completing
Learners Take Action to Reduce the Risk of Asthma Lesson 2: What causes asthma? Identifying Asthma Triggers Teacher Instructions, Introduction, and Student Worksheets Objectives for Lesson 2: After completing
Using an Inhaler and Nebulizer
 Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
How can I benefit most from my COPD medications?
 Fact Sheet: COPD Medications and Delivery Devices How can I benefit most from my COPD medications? COPD medications can improve your symptoms. By taking the right medication at the right time, you can
Fact Sheet: COPD Medications and Delivery Devices How can I benefit most from my COPD medications? COPD medications can improve your symptoms. By taking the right medication at the right time, you can
Teacher Training on Asthma
 Teacher Training on Asthma Understanding Asthma and How It Can Be Managed at School This presentation is made possible by a grant from: Training Objectives Describe the effects of asthma on students Discuss
Teacher Training on Asthma Understanding Asthma and How It Can Be Managed at School This presentation is made possible by a grant from: Training Objectives Describe the effects of asthma on students Discuss
Dealing with Asthma in Winter Weather
 Dealing with Asthma in Winter Weather Asthma is a chronic disease affecting more that twenty million children and adults in America. It is likely that some of the individuals you support may have asthma.
Dealing with Asthma in Winter Weather Asthma is a chronic disease affecting more that twenty million children and adults in America. It is likely that some of the individuals you support may have asthma.
Clear and Easy #12. Skypark Publishing. Molina Healthcare 24 Hour Nurse Advice Line
 Clear and Easy #12 Molina Healthcare 24 Hour Nurse Advice Line 1-888-275-8750 TTY: 1-866-735-2929 Molina Healthcare Línea de TeleSalud Disponible las 24 Horas 1-866-648-3537 TTY: 1-866-833-4703 Skypark
Clear and Easy #12 Molina Healthcare 24 Hour Nurse Advice Line 1-888-275-8750 TTY: 1-866-735-2929 Molina Healthcare Línea de TeleSalud Disponible las 24 Horas 1-866-648-3537 TTY: 1-866-833-4703 Skypark
Get Healthy Stay Healthy
 Asthma Management WHAT IS ASTHMA? Asthma causes swelling and inflammation in the breathing passages that lead to your lungs. When asthma flares up, the airways tighten and become narrower. This keeps the
Asthma Management WHAT IS ASTHMA? Asthma causes swelling and inflammation in the breathing passages that lead to your lungs. When asthma flares up, the airways tighten and become narrower. This keeps the
Nancy Davis, RRT, AE-C
 Nancy Davis, RRT, AE-C Asthma Statistics 25.6 million Americans diagnosed with asthma 6.8 million are children 10.5 million missed school days per year 14.2 lost work days for adults Approximately 10%
Nancy Davis, RRT, AE-C Asthma Statistics 25.6 million Americans diagnosed with asthma 6.8 million are children 10.5 million missed school days per year 14.2 lost work days for adults Approximately 10%
Home Management Plan. Cover Page
 Home Management Plan Cover Page What is Asthma? Asthma is a chronic disease of the lungs caused by swelling and irritation in the lining of airways Tightness of the airway muscles Excess mucus in the airways
Home Management Plan Cover Page What is Asthma? Asthma is a chronic disease of the lungs caused by swelling and irritation in the lining of airways Tightness of the airway muscles Excess mucus in the airways
Asthma Education. The Keys to Asthma Prevention and Control. what to do when one s asthma is flared! Lucile Packard Children s Hospital.
 Asthma Education Lucile Packa r d Children s H o spit al Created by Rachel Lawler RN, MSN, cpnp, AE-C, NPAT Pulmonary Pediatric Nurse Practitioner Lucile Packard Children s Hospital The Keys to Asthma
Asthma Education Lucile Packa r d Children s H o spit al Created by Rachel Lawler RN, MSN, cpnp, AE-C, NPAT Pulmonary Pediatric Nurse Practitioner Lucile Packard Children s Hospital The Keys to Asthma
Coach on Call. Thank you for your interest in Taking Care of Your Child s Asthma. I hope you find this tip sheet helpful.
 It was great to talk with you. Thank you for your interest in. I hope you find this tip sheet helpful. Please give me a call if you have more questions about this or other topics. As your UPMC Health Plan
It was great to talk with you. Thank you for your interest in. I hope you find this tip sheet helpful. Please give me a call if you have more questions about this or other topics. As your UPMC Health Plan
ASTHMA AND CHILDCARE PART 1. Presented by: Robin Costley, CRT, AE-C Marion County Public Health Department Manager, Asthma Alliance of Indianapolis
 ASTHMA AND CHILDCARE PART 1 Presented by: Robin Costley, CRT, AE-C Marion County Public Health Department Manager, Asthma Alliance of Indianapolis OBJECTIVES By the end of training, participants will:
ASTHMA AND CHILDCARE PART 1 Presented by: Robin Costley, CRT, AE-C Marion County Public Health Department Manager, Asthma Alliance of Indianapolis OBJECTIVES By the end of training, participants will:
MANAGEMENT OF ASTHMA SPRING Presented by:
 MEDS@Work MANAGEMENT OF ASTHMA SPRING 2013 Presented by: Lusia Fomuso PharmD candidate 2014 Olivia Sibailly PharmD candidate 2014 Kimberly Biedka PharmD candidate 2014 Dr. Donna Bartlett PharmD CGP RPh
MEDS@Work MANAGEMENT OF ASTHMA SPRING 2013 Presented by: Lusia Fomuso PharmD candidate 2014 Olivia Sibailly PharmD candidate 2014 Kimberly Biedka PharmD candidate 2014 Dr. Donna Bartlett PharmD CGP RPh
Your Guide to MANAGING ASTHMA
 Your Guide to MANAGING ASTHMA Asthma affects more than 24 MILLION AMERICANS. It is a chronic disease that causes your airways to become inflamed, making it hard to breathe. There is no cure for asthma.
Your Guide to MANAGING ASTHMA Asthma affects more than 24 MILLION AMERICANS. It is a chronic disease that causes your airways to become inflamed, making it hard to breathe. There is no cure for asthma.
Asthma and COPD Awareness
 Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Ohio Fall 2012 Importance of Controller Medicines Asthma is a disease that causes swelling
Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Ohio Fall 2012 Importance of Controller Medicines Asthma is a disease that causes swelling
Asthma and COPD Awareness
 Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Washington Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Washington Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
You Can Control Your Asthma
 asthma_brochureprint_v2.qxd 9/5/06 9:54 AM Page 2 For More Information on Controlling Asthma: Centers for Disease Control and Prevention National Center for Environmental Health, MS F52 4770 Buford Highway,
asthma_brochureprint_v2.qxd 9/5/06 9:54 AM Page 2 For More Information on Controlling Asthma: Centers for Disease Control and Prevention National Center for Environmental Health, MS F52 4770 Buford Highway,
Asthma. If an Ambulance is required - call immediately - do not delay. H & A Training PL RTO No:90871
 Asthma is a reversible breathing problem caused from sudden or progressive narrowing and spasming of the smaller airways and includes mucus production, which interferes with oxygen exchange. People who
Asthma is a reversible breathing problem caused from sudden or progressive narrowing and spasming of the smaller airways and includes mucus production, which interferes with oxygen exchange. People who
ASTHMA. Disclaimer. Multimedia Health Education
 ASTHMA Disclaimer This film is an educational resource, and should not be used for decisions about asthma treatment. All such decisions must be made in consultation with a physician or a healthcare provider.
ASTHMA Disclaimer This film is an educational resource, and should not be used for decisions about asthma treatment. All such decisions must be made in consultation with a physician or a healthcare provider.
Asthma (Short wind) in Children
 In partnership: Asthma (Short wind) in Children The lungs You have two lungs. They sit inside your chest, above your stomach and surround your heart. The lungs have a very important job inside your body.
In partnership: Asthma (Short wind) in Children The lungs You have two lungs. They sit inside your chest, above your stomach and surround your heart. The lungs have a very important job inside your body.
Breezhaler. Open to see clear capsule. How do I use my Breezhaler? Care of my Breezhaler
 Breezhaler 3 Pull cap off Press buttons once and release Breathe in rapidly and steadily. Hold. Open. Place capsule in chamber. Close (click). Breathe out 4 Open to see clear capsule. If not all clear
Breezhaler 3 Pull cap off Press buttons once and release Breathe in rapidly and steadily. Hold. Open. Place capsule in chamber. Close (click). Breathe out 4 Open to see clear capsule. If not all clear
Asthma symptoms are usually more active at night, when waking up in the early morning or after exercise. The asthma symptoms are:
 Health Bites - Asthma What Is Asthma? Asthma is a long-term disease that affects the air passages in the lungs. Air passages are tiny breathing tubes that carry air in and out of the lungs. People who
Health Bites - Asthma What Is Asthma? Asthma is a long-term disease that affects the air passages in the lungs. Air passages are tiny breathing tubes that carry air in and out of the lungs. People who
B.R.E.A.T.H.E. Bringing Reduction and Education of Asthma Triggers to the Home Environment
 B.R.E.A.T.H.E. Bringing Reduction and Education of Asthma Triggers to the Home Environment A collaborative project of HDHHS and the EPA Bureau of Community and Children s Environmental Health Acknowledgements
B.R.E.A.T.H.E. Bringing Reduction and Education of Asthma Triggers to the Home Environment A collaborative project of HDHHS and the EPA Bureau of Community and Children s Environmental Health Acknowledgements
Because the more you know, the better you ll feel.
 ABOUT ASTHMA Because the more you know, the better you ll feel. This booklet is designed to help you understand asthma and the things you can do every day to help control symptoms. As always, talk to your
ABOUT ASTHMA Because the more you know, the better you ll feel. This booklet is designed to help you understand asthma and the things you can do every day to help control symptoms. As always, talk to your
Asthma. Permafold Topics. What You Need To Know
 1. What Is Asthma? Asthma is a chronic disease that causes the airways to narrow. Airflow is limited due to inflammation in the airways. Asthma What You Need To Know Permafold Topics 1. What Is Asthma?
1. What Is Asthma? Asthma is a chronic disease that causes the airways to narrow. Airflow is limited due to inflammation in the airways. Asthma What You Need To Know Permafold Topics 1. What Is Asthma?
PATIENT INFORMATION FORM
 PATIENT INFORMATION FORM "I am going to ask you a number of questions about your asthma. The set of questions is somewhat long, but I will try to move through it fairly quickly so that we can complete
PATIENT INFORMATION FORM "I am going to ask you a number of questions about your asthma. The set of questions is somewhat long, but I will try to move through it fairly quickly so that we can complete
Asthma Friendly School Environments
 Asthma Friendly School Environments Our Mission Prevent lung disease and promote lung health in Mississippi through: Education Advocacy Research What is Asthma? Asthma: Is a life-long disease found in
Asthma Friendly School Environments Our Mission Prevent lung disease and promote lung health in Mississippi through: Education Advocacy Research What is Asthma? Asthma: Is a life-long disease found in
Clear and Easy. Skypark Publishing. Molina Healthcare 24 Hour Nurse Advice Line
 Clear and Easy #5 Molina Healthcare 24 Hour Nurse Advice Line 1-888-275-8750 TTY: 1-866-735-2929 Molina Healthcare Línea de TeleSalud Disponible las 24 Horas 1-866-648-3537 TTY: 1-866-833-4703 Skypark
Clear and Easy #5 Molina Healthcare 24 Hour Nurse Advice Line 1-888-275-8750 TTY: 1-866-735-2929 Molina Healthcare Línea de TeleSalud Disponible las 24 Horas 1-866-648-3537 TTY: 1-866-833-4703 Skypark
Safety Precaution Tips Against Seasonal Allergies (Hay Fever) By: Dr. Niru Prasad, M.D., F.A.A.P., F.A.C.E.P. WHAT IS HAY FEVER?
 Safety Precaution Tips Against Seasonal Allergies (Hay Fever) By: Dr. Niru Prasad, M.D., F.A.A.P., F.A.C.E.P. WHAT IS HAY FEVER? Hay Fever is the most common type of seasonal allergies experienced by the
Safety Precaution Tips Against Seasonal Allergies (Hay Fever) By: Dr. Niru Prasad, M.D., F.A.A.P., F.A.C.E.P. WHAT IS HAY FEVER? Hay Fever is the most common type of seasonal allergies experienced by the
Provided as an educational resource by Merck. A Guide to Living With Asthma
 Provided as an educational resource by Merck A Guide to Living With Asthma Table of Contents 1. Introduction...2 7 fast facts about asthma...2 2. Asthma Basics...3 6 What happens during an asthma attack?...3
Provided as an educational resource by Merck A Guide to Living With Asthma Table of Contents 1. Introduction...2 7 fast facts about asthma...2 2. Asthma Basics...3 6 What happens during an asthma attack?...3
LivingWith Asthma. A Guide to Understanding Asthma...
 A Guide to Understanding... LivingWith Understanding Diagnosing Treating Frequently Asked Questions [2] A Guide to Understanding... Understanding What Is? (AZ-muh) is a chronic disease that affects your
A Guide to Understanding... LivingWith Understanding Diagnosing Treating Frequently Asked Questions [2] A Guide to Understanding... Understanding What Is? (AZ-muh) is a chronic disease that affects your
CMS Asthma Education Program
 CMS Asthma Education Program ASTHMA IS Common Chronic Treatable Distressing Misunderstood Potentially Dangerous CMS Prevalence Number one chronic disease Leading cause of Absences 6481 CMS students (2003-04)
CMS Asthma Education Program ASTHMA IS Common Chronic Treatable Distressing Misunderstood Potentially Dangerous CMS Prevalence Number one chronic disease Leading cause of Absences 6481 CMS students (2003-04)
Because the more you know, the better you ll feel.
 ABOUT ASTHMA Because the more you know, the better you ll feel. What You ll Find Attitudes and Beliefs Asthma What Is It? Where You ll Find It Page 4-5 This booklet is designed to help you understand asthma
ABOUT ASTHMA Because the more you know, the better you ll feel. What You ll Find Attitudes and Beliefs Asthma What Is It? Where You ll Find It Page 4-5 This booklet is designed to help you understand asthma
Asthma 101. Introduction
 TRIGGERS Introduction Asthma is a chronic disease of the lungs that makes it difficult for people to breathe. Asthma is extremely common. About 20 million Americans have asthma. About 5,000 die each year
TRIGGERS Introduction Asthma is a chronic disease of the lungs that makes it difficult for people to breathe. Asthma is extremely common. About 20 million Americans have asthma. About 5,000 die each year
Welcome. We can control some of the things that cause problems in our homes.
 Welcome Lots of our children have asthma lots of us do, too. Luckily, we ve learned a great deal about how to avoid the things that trigger asthma attacks. We can control some of the things that cause
Welcome Lots of our children have asthma lots of us do, too. Luckily, we ve learned a great deal about how to avoid the things that trigger asthma attacks. We can control some of the things that cause
Asthma and COPD Awareness
 Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Texas Summer 2013 Asthma Triggers You may not always know when an asthma attack will
Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Texas Summer 2013 Asthma Triggers You may not always know when an asthma attack will
PATIENT INFORMATION. ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation
![PATIENT INFORMATION. ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation PATIENT INFORMATION. ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation](/thumbs/74/71128680.jpg) PATIENT INFORMATION ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation What is ADVAIR DISKUS? ADVAIR DISKUS combines the inhaled corticosteroid
PATIENT INFORMATION ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation What is ADVAIR DISKUS? ADVAIR DISKUS combines the inhaled corticosteroid
Asthma With a Slight Chance of Anaphylaxis
 Asthma With a Slight Chance of Anaphylaxis An Update for Alberta Oral Health Professionals Sept 25/13 Presented by Val Olson CRE Community Pediatric Asthma Service Air passes through the: Nose or mouth
Asthma With a Slight Chance of Anaphylaxis An Update for Alberta Oral Health Professionals Sept 25/13 Presented by Val Olson CRE Community Pediatric Asthma Service Air passes through the: Nose or mouth
Asthma Action Plan and Education
 Acute Services Division Asthma Action Plan and Education Name: Date: Index What is Asthma? Page 4 Asthma Triggers Page 5 Peak Expiratory Flow Rate (Peak Flow) Page 6 Asthma Treatments Page 7 Asthma Action
Acute Services Division Asthma Action Plan and Education Name: Date: Index What is Asthma? Page 4 Asthma Triggers Page 5 Peak Expiratory Flow Rate (Peak Flow) Page 6 Asthma Treatments Page 7 Asthma Action
Keys to Breathing Easy
 Keys to Breathing Easy Ways to Manage Your Asthma EHAP Environmental Health Action Project SUPPORTED IN PART BY: Project H17 MC 00170 from Healthy Tomorrows Partnership for Childrens Program, Maternal
Keys to Breathing Easy Ways to Manage Your Asthma EHAP Environmental Health Action Project SUPPORTED IN PART BY: Project H17 MC 00170 from Healthy Tomorrows Partnership for Childrens Program, Maternal
ESSENTIAL STANDARD. 6.PCH.1 Understand wellness, disease prevention, and recognition of symptoms.
 PRE-TEST 1.What are the basic functions of the respiratory system? 2.Describe five symptoms of asthma. 3.How can asthma be controlled? 4.What are some common asthma triggers? ESSENTIAL STANDARD 6.PCH.1
PRE-TEST 1.What are the basic functions of the respiratory system? 2.Describe five symptoms of asthma. 3.How can asthma be controlled? 4.What are some common asthma triggers? ESSENTIAL STANDARD 6.PCH.1
Helping Your Child Stay Healthy & Active
 Helping Your Child Stay Healthy & Active 11480 1401 Taking Control of Your Child s Asthma Learning that your child has asthma can be overwhelming. Asthma is a chronic (ongoing) disease of the airways in
Helping Your Child Stay Healthy & Active 11480 1401 Taking Control of Your Child s Asthma Learning that your child has asthma can be overwhelming. Asthma is a chronic (ongoing) disease of the airways in
My Asthma Log. Tommy Traffic Light. NHS Number: Name:
 My Asthma Log Tommy Traffic Light NHS Number: Name: My Asthma Log Book This book is designed to help you understand and learn about managing your asthma. You should take your book with you to all your
My Asthma Log Tommy Traffic Light NHS Number: Name: My Asthma Log Book This book is designed to help you understand and learn about managing your asthma. You should take your book with you to all your
How to Use Inhaled Medications for Asthma and COPD
 How to Use Inhaled Medications for Asthma and COPD This information is not intended to diagnose health problems or to take the place of medical advice or care you receive from your physician or other health
How to Use Inhaled Medications for Asthma and COPD This information is not intended to diagnose health problems or to take the place of medical advice or care you receive from your physician or other health
Asthma and COPD Awareness Molina Breathe with Ease and Chronic Obstructive Pulmonary Disease
 Asthma and COPD Awareness Molina Breathe with Ease and Chronic Obstructive Pulmonary Disease Molina Healthcare of Michigan - Spring 2014 Asthma and Your Home Asthma is one of our nation s most common chronic
Asthma and COPD Awareness Molina Breathe with Ease and Chronic Obstructive Pulmonary Disease Molina Healthcare of Michigan - Spring 2014 Asthma and Your Home Asthma is one of our nation s most common chronic
Asthma Basic Facts. Staying safe and well with asthma. For people with asthma and their carers.
 Asthma Basic Facts Staying safe and well with asthma. For people with asthma and their carers. Asthma App Contact your local Asthma Foundation asthmaaustralia.org.au Breathing Breathing is how we get air
Asthma Basic Facts Staying safe and well with asthma. For people with asthma and their carers. Asthma App Contact your local Asthma Foundation asthmaaustralia.org.au Breathing Breathing is how we get air
LEARN ABOUT ANOTHER WAY TO TREAT YOUR ALLERGIES
 LEARN ABOUT ANOTHER WAY TO TREAT YOUR ALLERGIES WHAT ARE ALLERGIES? It s probably not something that you think about, but every time you open your mouth or inhale, tiny particles from the environment that
LEARN ABOUT ANOTHER WAY TO TREAT YOUR ALLERGIES WHAT ARE ALLERGIES? It s probably not something that you think about, but every time you open your mouth or inhale, tiny particles from the environment that
Asthma. What Is Asthma? Overview. Asthma
 Asthma What Is Asthma? Asthma is a chronic (long-term) lung disease that inflames and narrows the airways. Asthma causes recurring periods of wheezing (a whistling sound when you breathe), chest tightness,
Asthma What Is Asthma? Asthma is a chronic (long-term) lung disease that inflames and narrows the airways. Asthma causes recurring periods of wheezing (a whistling sound when you breathe), chest tightness,
Asthma. Guide to Good Health. Healthy Living Guide
 Asthma Guide to Good Health Healthy Living Guide Asthma Chronic Fatigue Syndrome (CFS) Chronic Obstructive Pulmonary Disease (COPD) Coronary Artery Disease (CAD) Depression Hyperlipidemia Hypertension
Asthma Guide to Good Health Healthy Living Guide Asthma Chronic Fatigue Syndrome (CFS) Chronic Obstructive Pulmonary Disease (COPD) Coronary Artery Disease (CAD) Depression Hyperlipidemia Hypertension
Asthma and COPD Awareness
 Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Texas Newsletter Spring 2011 Asthma Warning Signs In This Issue Asthma Warning Signs pg 1 Working with the Provider
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Texas Newsletter Spring 2011 Asthma Warning Signs In This Issue Asthma Warning Signs pg 1 Working with the Provider
Asthma and IAQ. Lani Wheeler, MD, Medical Officer Sarah Merkle, MPH, Program Analyst
 Asthma and IAQ Lani Wheeler, MD, Medical Officer Sarah Merkle, MPH, Program Analyst Division of Adolescent and School Health Centers for Disease Control and Prevention Asthma is a Major Public Health Problem
Asthma and IAQ Lani Wheeler, MD, Medical Officer Sarah Merkle, MPH, Program Analyst Division of Adolescent and School Health Centers for Disease Control and Prevention Asthma is a Major Public Health Problem
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
COPD Zone Tool & Action Plan
 COPD Zone Tool & Action Plan "I am doing well today!" reen Zone: ood Breathing Day Actions Additional Action Usual activity and exercise level Take daily medicines Plan Steps Made Usual amounts of cough
COPD Zone Tool & Action Plan "I am doing well today!" reen Zone: ood Breathing Day Actions Additional Action Usual activity and exercise level Take daily medicines Plan Steps Made Usual amounts of cough
9/30/2013. Asthma in the Classroom: What do teachers need to know? Asthma Impact. Asthma is Common
 Asthma in the Classroom: What do teachers need to know? Pulmonary Rehabilitation Asthma Impact Asthma affects over twenty five million people nationwide causes 10.5 million lost school days annually third-ranking
Asthma in the Classroom: What do teachers need to know? Pulmonary Rehabilitation Asthma Impact Asthma affects over twenty five million people nationwide causes 10.5 million lost school days annually third-ranking
Help Your Child Gain Control Over Asthma
 Help Your Child Gain Control Over Asthma United States Environmental Protection Agency Indoor Environments Division Office of Air and Radiation EPA 402-F-04-021 November 2004 It s hard to see your child
Help Your Child Gain Control Over Asthma United States Environmental Protection Agency Indoor Environments Division Office of Air and Radiation EPA 402-F-04-021 November 2004 It s hard to see your child
Asthma Medications: Information for Children and Families. What You Need to Know about Medicines for Asthma
 Page 1 of 8 PED-ALL-005-1992 Asthma Medications: Information for Children and Families What You Need to Know about Medicines for Asthma What Medicines Are used to Treat Asthma? There are two kinds of medicines:
Page 1 of 8 PED-ALL-005-1992 Asthma Medications: Information for Children and Families What You Need to Know about Medicines for Asthma What Medicines Are used to Treat Asthma? There are two kinds of medicines:
Date of Assessment: Assessed By: Questionnaire: Assessing Student Readiness to Self- Carry
 Student Name: Score: Date of Assessment: Assessed By: naire: Assessing Student Readiness to Self- Carry Having immediate access to quick- relief medicine is critical for people with asthma. The purpose
Student Name: Score: Date of Assessment: Assessed By: naire: Assessing Student Readiness to Self- Carry Having immediate access to quick- relief medicine is critical for people with asthma. The purpose
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease
 Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Michigan Newsletter Spring 2012 Getting Rid of Mold There are many types of molds. Molds will not grow without water
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Michigan Newsletter Spring 2012 Getting Rid of Mold There are many types of molds. Molds will not grow without water
Medications. prescribed. Use as. A s t h m a B a s i c s # 3
 Medications A s t h m a B a s i c s # 3 Use as prescribed The Asthma Basics Booklet Series was developed to provide Canadians with asthma, current and accurate information about asthma management. This
Medications A s t h m a B a s i c s # 3 Use as prescribed The Asthma Basics Booklet Series was developed to provide Canadians with asthma, current and accurate information about asthma management. This
PACKAGE LEAFLET: INFORMATION FOR THE USER Pulmicort Turbohaler budesonide. 1. What Pulmicort Turbohaler is and what it is used for
 PACKAGE LEAFLET: INFORMATION FOR THE USER Pulmicort Turbohaler budesonide Read all of this leaflet carefully before you start taking this medicine. Keep this leaflet. You may need to read it again. If
PACKAGE LEAFLET: INFORMATION FOR THE USER Pulmicort Turbohaler budesonide Read all of this leaflet carefully before you start taking this medicine. Keep this leaflet. You may need to read it again. If
Asthma By Mayo Clinic staff
 MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
al T ip Gu Seasonal Tip Guide Tips to help you stay healthy and safe throughout the year
 Seasonal Tip Guide al T ip Gu n o s ide a Se Tips to help you stay healthy and safe throughout the year HHC Health & Home Care Serving New Yorkers For Over 45 Years 1-866-NYC-HOME www.homecarenyc.org www.facebook.com/homecarenyc
Seasonal Tip Guide al T ip Gu n o s ide a Se Tips to help you stay healthy and safe throughout the year HHC Health & Home Care Serving New Yorkers For Over 45 Years 1-866-NYC-HOME www.homecarenyc.org www.facebook.com/homecarenyc
Flu: What You Can Do. Caring for People at Home
 Flu: What You Can Do Caring for People at Home Flu: What You Can Do Caring for People at Home For more information, please visit: www.mass.gov/dph/flu CONTENTS: What is the flu? 2 table of contents Flu
Flu: What You Can Do Caring for People at Home Flu: What You Can Do Caring for People at Home For more information, please visit: www.mass.gov/dph/flu CONTENTS: What is the flu? 2 table of contents Flu
Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema.
 Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema. 2 LIVING WITH COPD You may have been told that you have COPD. It is a lung disease
Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema. 2 LIVING WITH COPD You may have been told that you have COPD. It is a lung disease
About Asthma. Developed by the Asthma Education Service with assistance from the Department of Learning and Development.
 About Asthma Developed by the Asthma Education Service with assistance from the Department of Learning and Development. All rights reserved. No part of this book may be reproduced or transmitted in any
About Asthma Developed by the Asthma Education Service with assistance from the Department of Learning and Development. All rights reserved. No part of this book may be reproduced or transmitted in any
H1N1 (Swine) Influenza
 What is H1N1 influenza A? H1N1 (Swine) Influenza The new H1N1 influenza, also called swine flu, is a new influenza virus causing illness in people. This new virus was first detected in 2009. This virus
What is H1N1 influenza A? H1N1 (Swine) Influenza The new H1N1 influenza, also called swine flu, is a new influenza virus causing illness in people. This new virus was first detected in 2009. This virus
Year 2, 3 or 4 Asthma lesson presentation HARMFUL
 Year 2, 3 or 4 Asthma lesson presentation HARMFUL Asthma is a condition that affects the airways of the lungs. It can lead to the airways getting narrower; this makes it hard for the person to breathe.
Year 2, 3 or 4 Asthma lesson presentation HARMFUL Asthma is a condition that affects the airways of the lungs. It can lead to the airways getting narrower; this makes it hard for the person to breathe.
 $9.99 A B r i e f B i t o f I n f o r m a t i o n o n P a r t i c u l a t e s i n Y o u r H o m e This guide provides information and guidance for homeowners on a few indoor particulates to be aware of,
$9.99 A B r i e f B i t o f I n f o r m a t i o n o n P a r t i c u l a t e s i n Y o u r H o m e This guide provides information and guidance for homeowners on a few indoor particulates to be aware of,
Eczema: also called atopic dermatitis; a chronic, itchy, scaly rash not due to a particular substance exposure
 Allergy is a condition in which the immune system causes sneezing, itching, rashes, and wheezing, or sometimes even life-threatening allergic reactions. The more you know about allergies, the better prepared
Allergy is a condition in which the immune system causes sneezing, itching, rashes, and wheezing, or sometimes even life-threatening allergic reactions. The more you know about allergies, the better prepared
Aileen Gagney Environmental and Lung Health Program Manager American Lung Association of the Mountain Pacific
 Aileen Gagney Environmental and Lung Health Program Manager of the Mountain Pacific Course Objectives Learn the definition of asthma, alterations in the lung anatomy and the symptoms Learn to identify
Aileen Gagney Environmental and Lung Health Program Manager of the Mountain Pacific Course Objectives Learn the definition of asthma, alterations in the lung anatomy and the symptoms Learn to identify
Asthma and COPD Awareness
 Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Washington Newsletter Spring 2011 Asthma Warning Signs In This Issue Asthma Warning Signs pg 1 Working with the
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Washington Newsletter Spring 2011 Asthma Warning Signs In This Issue Asthma Warning Signs pg 1 Working with the
Asthma and Air Pollution
 Asthma and Air Pollution Health Effects Workshop Nov. 6, 2008 Joann Held with thanks to: Dave Brown Asthma and Airways Asthma Physiology A chronic disease that affects airways. The inside walls of airways
Asthma and Air Pollution Health Effects Workshop Nov. 6, 2008 Joann Held with thanks to: Dave Brown Asthma and Airways Asthma Physiology A chronic disease that affects airways. The inside walls of airways
Allergies and Asthma 5/21/2013. Objectives. Allergic Rhinitis (AR): Risk Factor for ASTHMA. Rhinitis and Asthma
 Allergies and Asthma Presented By: Dr. Fadwa Gillanders, Pharm.D Clinical Pharmacy Specialist May 2013 Objectives Understand the relationship between asthma and allergic rhinitis Understand what is going
Allergies and Asthma Presented By: Dr. Fadwa Gillanders, Pharm.D Clinical Pharmacy Specialist May 2013 Objectives Understand the relationship between asthma and allergic rhinitis Understand what is going
EARLY warning signs. Coughing (may be worse at night or with exercise) Wheezing
 Breathing Easier What is asthma? Asthma is a disease of the lungs that often leads to repeated episodes of wheezing, chest tightness, breathlessness, and early morning or nighttime coughing. Asthma currently
Breathing Easier What is asthma? Asthma is a disease of the lungs that often leads to repeated episodes of wheezing, chest tightness, breathlessness, and early morning or nighttime coughing. Asthma currently
Environmental Allergens. Allergies to Dust, Mold and Pollen. A Patient s Guide
 Environmental Allergens Allergies to Dust, Mold and Pollen A Patient s Guide Our environment, at home or outdoors, can be a potent source of allergens causing itchy, puffy and watery eyes, sneezing, a
Environmental Allergens Allergies to Dust, Mold and Pollen A Patient s Guide Our environment, at home or outdoors, can be a potent source of allergens causing itchy, puffy and watery eyes, sneezing, a
Complex Care Hub Manual Section: Asthma
 Complex Care Hub Manual Section: Asthma Table of Contents 1 What is Asthma?... 2 2 What causes asthma?... 2 2.1 Triggers... 2 3 Signs and Symptoms... 2 4 Treatment... 2 4.1 Relievers... 2 4.2 Preventers...
Complex Care Hub Manual Section: Asthma Table of Contents 1 What is Asthma?... 2 2 What causes asthma?... 2 2.1 Triggers... 2 3 Signs and Symptoms... 2 4 Treatment... 2 4.1 Relievers... 2 4.2 Preventers...
MANAGING COPD AT HOME. Karla Schlichtmann, RRT
 MANAGING COPD AT HOME Karla Schlichtmann, RRT Chronic Obstructive Pulmonary Disease (COPD) is a progressive lung disease. WHAT IS COPD? The airways in your lungs become inflamed and thickens. This results
MANAGING COPD AT HOME Karla Schlichtmann, RRT Chronic Obstructive Pulmonary Disease (COPD) is a progressive lung disease. WHAT IS COPD? The airways in your lungs become inflamed and thickens. This results
Learners Take Action to Reduce the Risk of Asthma
 Learners Take Action to Reduce the Risk of Asthma Lesson 3: What can you do about asthma? Taking action Teacher Instructions, Introduction, and Student Worksheets Objectives for Lesson 3: After completing
Learners Take Action to Reduce the Risk of Asthma Lesson 3: What can you do about asthma? Taking action Teacher Instructions, Introduction, and Student Worksheets Objectives for Lesson 3: After completing
My Asthma Guide. This is my guide. Patient s Name
 My Asthma Guide This is my guide Patient s Name Table of Contents Section 1 What is Asthma? What is Asthma? 3 Asthma Symptoms 3 Asthma Can be Controlled 3 Airways When You Don t Have Asthma 4 Airways When
My Asthma Guide This is my guide Patient s Name Table of Contents Section 1 What is Asthma? What is Asthma? 3 Asthma Symptoms 3 Asthma Can be Controlled 3 Airways When You Don t Have Asthma 4 Airways When
New Patient Questionnaire
 - - Toda y 's Date: Primary Care Provider's Name: Was a consultation recommended? Primary Clinic: Referring provider's name (if different): Please answer the following questions to facilitate the diagnosis
- - Toda y 's Date: Primary Care Provider's Name: Was a consultation recommended? Primary Clinic: Referring provider's name (if different): Please answer the following questions to facilitate the diagnosis
Appendix E: Device Technique
 Adult Asthma Care Guidelines for Nurses: Promoting Control of Asthma Appendix E: Device Technique Medications: Inhalation Devices Adapted with permission from The Lung Association: www.lung.ca/asthma/manage/devices.html
Adult Asthma Care Guidelines for Nurses: Promoting Control of Asthma Appendix E: Device Technique Medications: Inhalation Devices Adapted with permission from The Lung Association: www.lung.ca/asthma/manage/devices.html
INFLUENZA (FLU) Cleaning to Prevent the Flu
 INFLUENZA (FLU) Cleaning to Prevent the Flu Cleaning to Prevent the Flu 24 hours How long can the flu virus live on objects, such as doorknobs and tables? The flu virus can live on some surfaces for up
INFLUENZA (FLU) Cleaning to Prevent the Flu Cleaning to Prevent the Flu 24 hours How long can the flu virus live on objects, such as doorknobs and tables? The flu virus can live on some surfaces for up
MEDICATION GUIDE. ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol
![MEDICATION GUIDE. ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol MEDICATION GUIDE. ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol](/thumbs/78/76835983.jpg) MEDICATION GUIDE ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol ADVAIR HFA 115/21 (fluticasone propionate 115 mcg and salmeterol 21 mcg) Inhalation
MEDICATION GUIDE ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol ADVAIR HFA 115/21 (fluticasone propionate 115 mcg and salmeterol 21 mcg) Inhalation
