ORIGINAL ARTICLE. Absence of Nasal Mucosal Atrophy With Fluticasone Aqueous Nasal Spray
|
|
|
- Tyrone Preston
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Absence of Nasal Mucosal Atrophy With Fluticasone Aqueous Nasal Spray Fuad M. Baroody, MD; Cheng-Chou Cheng, MD; Birgitta Moylan, BSc; Marcy detineo, RN; Lauran Haney, BS; Kenneth D. Reed, BS; Cindy K. Cook, MS; Ronald E. Westlund, MS; Elizabeth Sengupta, MD; Jacquelynne P. Corey, MD; Alkis Togias, MD; Robert M. Naclerio, MD Objective: To evaluate whether 1 year of continuous treatment with intranasal fluticasone propionate would lead to atrophy in the nasal mucosa compared with an active control, oral terfenadine. Design: Prospective, randomized, multicenter, openlabel, parallel-group study. Setting: Two tertiary care academic institutions. Patients: Seventy-five subjects older than 18 years with perennial allergic rhinitis. Interventions: Patients received either fluticasone propionate aqueous nasal spray, 200 µg once daily, or terfenadine, 60 mg twice daily, for 1 year. Nasal biopsy specimens were obtained before and after 1 year of treatment and were evaluated for evidence of atrophy. Main Outcome Measures: Epithelial and collagen layer thickness of the nasal mucosa as assessed by light microscopy and the presence and degree of edema, and regularity of collagen fibrils as assessed by electron microscopy. Analyses were performed without knowledge of subject identity or treatment assignment. Results: Neither fluticasone nor terfenadine treatment led to atrophy in the nasal mucosa by clinical or histologic observation. No significant changes from baseline were observed for any assessment of atrophy. In contrast to what would have been expected if atrophy were to occur, mean epithelial layer thickness in the fluticasone group significantly increased compared with terfenadine treatment (P=.03). Conclusions: Treatment with intranasal fluticasone for 1 year increases the thickness of the nasal epithelium as compared with a year s treatment with terfenadine and does not lead to atrophy in the nasal mucosa. The increased thickness in the fluticasone treatment may represent repair from epithelial damage caused by chronic allergic inflammation. Arch Otolaryngol Head Neck Surg. 2001;127: From the Section of Otolaryngology Head and Neck Surgery (Drs Baroody, Cheng, Corey, and Naclerio and Mss detineo and Haney) and the Department of Pathology (Dr Sengupta), Pritzker School of Medicine, University of Chicago, Chicago, Ill; Department of Medicine (Division of Clinical Immunology), The Johns Hopkins University School of Medicine, Baltimore, Md (Ms Moylan and Dr Togias); and Glaxo Wellcome Inc, Research Triangle Park, NC (Messrs Reed and Westlund and Ms Cook). ALLERGIC RHINITIS affects more than 40 million Americans and costs society more than $3 billion each year. 1 A major characteristic of allergic rhinitis is inflammation. 2 The inflammatory process stimulates the glands, blood vessels, and nerves of the nasal mucosa, creating the symptoms of the disease. Whether this inflammation causes changes to matrix structures, such as the epithelium, the basement membrane, and the collagen matrix, is not known. Intranasal corticosteroids are among the most commonly prescribed and effective medications used to treat this disease. 3,4 The safety and efficacy of intranasal corticosteroids have been well established in multiple clinical trials. Furthermore, the widespread clinical use of these compounds during the past 25 years has not been associated with substantial untoward adverse events. 3 Intranasal corticosteroids exert a potent topical anti-inflammatory effect. 3,5 They inhibit the recruitment of inflammatory cells and prevent the release of inflammatory mediators, resulting in a decrease in symptoms and the blocking of both the earlyand late-phase allergic reactions. 3-6 Appropriate treatment options must be evaluated over the long term for potential adverse sequelae. This is particularly true for patients with perennial allergic rhinitis who may require longterm treatment over several years to control their disease. Long-term use of oral corticosteroids and topical dermatologic corticosteroids (ie, creams and ointments) have been observed to lead to atrophic changes in the skin Although there is no clinical or histologic evidence that intranasal corticosteroid treatment leads 193
2 SUBJECTS AND METHODS SUBJECTS Men and nonpregnant, nonlactating women 18 years of age or older were recruited from The Johns Hopkins University Hospital, Baltimore, Md, and the University of Chicago Hospitals, Chicago, Ill, to participate in this study. All subjects had to have a diagnosis of perennial allergic rhinitis and a skin test positive for dust mites. Eligible subjects also had to have nasal symptoms for more than 1 hour per day on most days for which they used at least 1 antirhinitis medication during the 12 months before the study. Subjects with a marked ( 50%) physical obstruction in the nose, previous nasal septal surgery or perforation, or viral or bacterial infection within 30 days of screening were excluded. Medications that could affect rhinitis symptoms or allergic inflammation, such as topical and systemic glucocorticoid therapy, intranasal cromolyn sodium, and antihistamines, were not permitted for at least 1 month before or during the study. None of the subjects was taking immunotherapy during the study, and those who had received previous immunotherapy had to have stopped taking it at least 2 years before participation. Before initiation of the study, the protocol and informed consent document were reviewed and approved by the institutional review board governing research at each site. All subjects provided written informed consent before participation. DESIGN This was a randomized, open-label, parallel-group study in 75 subjects with perennial allergic rhinitis that compared the effects on the nasal mucosa of 1 year of treatment with fluticasone propionate aqueous nasal spray, 200 µg once daily, vs an active control, oral terfenadine, 60-mg tablet twice daily. At the time this study was conducted in the mid-1990s, terfenadine was a commonly prescribed medication for the treatment of allergic rhinitis and was considered a suitable therapeutic alternative to intranasal corticosteroid therapy. The study consisted of a 21-day screening phase and a 12-month randomized, open-label treatment phase. During the screening phase, eligibility for the study was confirmed and baseline rhinoscopy and nasal biopsy were performed. After healing of the nasal biopsy site (approximately 1 week later), subjects were randomly assigned to receive 1 of the following study treatments for 1 year: intranasal fluticasone propionate once daily (2 sprays of 50 µg per spray in each nostril in the morning) or terfenadine, 60-mg tablet orally twice daily. Subjects were allowed to take only pseudoephedrine as needed for the relief of breakthrough symptoms during the study and were allowed to take other medications that did not interfere with allergic inflammation, such as analgesics. Subjects returned to the clinic at monthly intervals to reinforce medication adherence, receive additional medication, and assess their clinical status. After 12 months of treatment, another nasal biopsy specimen was obtained from the opposite nostril to avoid the confounding effects of scar formation at the site of the first biopsy specimen. NASAL BIOPSY After local anesthesia was induced with 1% lidocaine hydrochloride with epinephrine 1:100000, biopsy samples were obtained with punch forceps from the anterior tip of the inferior turbinate by standard methods. 12 This biopsy site was selected because it is the expected site of drug impact with aqueous nasal spray medications and a major site for allergen deposition. Each biopsy specimen was divided into sections to enable light and electron microscopic evaluation of atrophy and labeled such that subject to atrophy of the nasal mucosa, we undertook this comparative nasal biopsy study to investigate the effects of 2 treatment options for allergic rhinitis. We compared the structural characteristics of nasal mucosal biopsy specimens from subjects allergic to dust mites who were treated with either fluticasone propionate aqueous nasal spray or oral terfenadine, the active control. Nasal mucosal atrophy was assessed qualitatively and quantitatively by means of light and electron microscopy. Thus, this study was designed to examine whether 1 year of treatment with a topical corticosteroid (fluticasone) causes atrophic nasal mucosal changes when compared with an oral antihistamine (terfenadine). RESULTS SUBJECT DISPOSITION AND DEMOGRAPHICS Seventy-five subjects (38 in the fluticasone group and 37 in the terfenadine group) were enrolled in the study (Table 2). The treatment groups were similar with respect to age, sex distribution, ethnic origin, and number of subjects withdrawn early. The most common reason for attrition during the 12-month study period was that subjects failed to return to the clinic. Four subjects were withdrawn from the study because of nonserious adverse events: 3 in the fluticasone group (epistaxis, nasal dryness, and exacerbation of asthma) and 1 in the terfenadine group (exacerbation of uveitis). The adverse event profile was similar to that observed in previous studies. There were no serious or unusual events. BIOPSY RESULTS All evaluable nasal biopsy specimens from subjects with both baseline and study end biopsy samples were included in the analyses of atrophy (n=52). This included samples from the 51 subjects who completed the study and 1 subject who was discontinued from the study after 8 months of treatment because of relocation. As would be expected because of the location of the biopsy (anterior tip of the inferior turbinate), all specimens but 1 had nonciliated squamous epithelium present at baseline. In 2 specimens, both respiratory and squamous epithelium were seen, and in 1 specimen, only respiratory epithelium was seen in the areas examined. 194
3 identity, treatment, and date of biopsy were not apparent to those evaluating the specimens. Biopsy samples were prepared as follows: 1. Section 1 of the biopsy specimen was fixed in formalin, embedded in paraffin, sectioned into 5-µm sections, and stained with hematoxylin-eosin. These samples were evaluated by means of light microscopy. 2. Section 2 of the biopsy specimen was fixed in 2.5% glutaraldehyde in Millonig buffer (1.7% monobasic sodium phosphate + 0.3% sodium hydroxide in distilled water with ph ) at 4 C for 24 hours, then transferred and stored in Millonig buffer at 4 C until postfixing in 1% osmium tetroxide, dehydrating, infiltrating, and embedding in epoxy resin. The epoxy resin embedded tissue was then sectioned into 50- to 70-nm sections, placed on copper grids, and contrast stained with 1.5% uranyl acetate aqueous solution and Reynold lead citrate solution and examined by transmission electron microscopy (Philips CM- 10; Philips Inc, Mahway, NJ). ASSESSMENT OF ATROPHY Atrophy was assessed by means of 4 objective and quantitative measures based on light and transmission electron microscopy (Table 1). In addition, qualitative evaluations including the presence of squamous and respiratory epithelium, elastin, basal lamina duplication, and collagen type were performed with electron microscopy. Specimens were visualized at 1000 to examine the epithelium and underlying stroma (Figure 1), 8000 to evaluate the superficial vessels, for high-power views of the basal lamina and the epithelium, and for evaluation of collagen. Prints at each of these magnifications were unidentified as to subject name and treatment received and were examined by 2 investigators (C.C.C. and E.S.). The thickness of the collagen and epithelium was measured in the hematoxylin-eosin stained sections under 400 magnification with a microscope with a computercontrolled stage (Axioplan; Zeiss Inc, Thornwood, NY) coupled to an image analysis program (Neurolucida; Microbrightfield Inc, Colchester, Vt). The thickness of the collagen layer was measured in micrometers at 5 points along the specimen and that of the epithelium at 3 points along the specimen. The average value of these respective measurements was used for analysis. The presence of edema (presence of lucent spaces) and regularity of collagen fibrils were graded on the scoring system described in Table 1. Micrographs representative of the low and high ends of these scales are provided in Figure 2 and Figure 3, respectively. Figure 2 shows the electronlucent spaces between the collagen fibrils. Figure 2A ( 15500) demonstrates the lack of lucent spaces (0 or none) between the collagen fibrils, and Figure 2B ( 14500) demonstrates a large number of electron-lucent spaces (3 or severe). Figures 3A and 3B show low (+1, least regular) and high (+3, most regular) regularity, respectively, of collagen fibrils observed at magnification. STATISTICAL ANALYSES Atrophy of the nasal mucosa was assessed by the evaluation of epithelial and collagen layer thickness, presence of edema (lucent spaces), and the regularity of collagen fibrils. Treatment groups were compared in data sets that included all subjects who had both baseline and end-oftreatment biopsy data available. Small sample size and distributional properties required that nonparametric statistical tests be used for within- and between-treatment comparisons for both light and electron microscopy data. Two analyses were conducted: a main-effects analysis using a Wilcoxon rank sum test and a rank analysis of covariance. Within treatment group, changes from baseline to study end were also analyzed with a Wilcoxon signed rank test. The nasal biopsy specimens taken at the end of the study similarly included squamous epithelium, although 2 specimens contained both respiratory and squamous epithelial cells. At both baseline and study end, the collagen was type I, basal lamina duplication was rare, and no elastin fibers were seen, providing reassurance that severely damaged nasal mucosa had not been observed. Biopsy results for epithelial layer thickness, collagen layer thickness, lucent spaces score, and regularity of collagen score are summarized in Table 3. At baseline, the mean epithelial layer thicknesses in the fluticasone group (27.77 µm) and the terfenadine group (28.55 µm) were not significantly different. After 1 year of treatment, the mean epithelial layer thickness had increased to µm (+7.40 µm) in the fluticasone group whereas it had decreased to µm ( 7.64 µm) in the terfenadine group. These changes did not represent a significant change from baseline for either group as tested by the Wilcoxon signed rank test (for fluticasone, P=.37; for terfenadine, P=.23). However, when the treatment groups were compared at study end, significant differences were observed for both the main-effects analysis based on the Wilcoxon rank sum test (P=.05) and when baseline effects were included as a covariate in the model (P=.03, rank analysis of covariance). This was a significantly higher epithelial thickness at the end of treatment in the fluticasone group (35.17 µm) compared with the terfenadine group (20.91 µm). Mean collagen layer thickness was not significantly different before or after 1 year s treatment with either fluticasone (P=.68) or terfenadine (P=.47). At baseline, the mean collagen layer thickness was µm in the fluticasone group and µm in the terfenadine group. At study end, mean collagen layer thickness values remained essentially unchanged (11.97 µm in the fluticasone group and µm in the terfenadine group). A lucent spaces score, graded on a 4-point scale of 0 (none), 1 (mild), 2 (moderate), and 3 (severe), was created to quantify the degree of tissue edema observed. The mean scores at baseline were similar: 1.19 for the fluticasone group and 1.09 for the terfenadine group, indicating mild edema. No significant within or between treatment group differences were observed after 1 year of treatment. The mean score at study end was essentially unchanged for both treatment groups (1.05 for the fluticasone group and 1.14 for the terfenadine group). 195
4 Table 1. Assessment of Atrophy Measure of Atrophy Epithelium layer thickness (light microscopy) Collagen layer thickness (light microscopy) Presence of edema (electron microscopy) Regularity of collagen fibrils (electron microscopy) Expected Changes From Baseline if Atrophy Occurred* How Measured Interpretation Thickness measured in micrometers at 3 points along specimen; mean value analyzed Thickness measured in micrometers at 5 points along specimen; mean value analyzed 4-Point scale for lucent spaces: 0 (none), 1 (mild), 2 (moderate), 3 (severe) 3-Point scale: +1 (least regular) to +3 (most regular) Decrease in thickness suggestive of tissue atrophy Decrease in thickness suggestive of tissue atrophy The higher the score, the more edema; suggestive of tissue damage Highest degree of regularity (+3) indicated tissue damage *Downward arrow indicates decreased; upward arrow, increased. Figure 1. Low-power transmission electron micrograph of the nasal mucosa demonstrating, from top to bottom, the epithelium, collagen layer, lamina propria, and the glandular layer (original magnification 1200). The regularity of collagen was graded on a 3-point scale of +1 (least regular) to +3 (most regular). The mean scores at baseline were not significantly different: 1.83 for the fluticasone group and 1.75 for the terfenadine group, indicating a midrange level of regularity. After 1 year of treatment, the regularity scores increased slightly in both groups (2.05 in the fluticasone group and 1.85 in the terfenadine group). No significant within treatment group changes were observed, and no significant differences were observed when the treatment groups were compared. COMMENT The primary objective of this study was to evaluate the effect of fluticasone on the nasal mucosa and determine whether atrophy would be observed after continuous treatment for 1 year. The presence of atrophy was primarily based on 4 objective evaluations, including epithelial and basement membrane (collagen layer) thicknesses, the degree of edema (lucent spaces), and the regularity of the collagen fibrils, as well as clinical observation of the nasal mucosa during the monthly visits. Our results showed that there was no evidence that treatment with fluticasone propionate aqueous nasal spray, 200 µg once daily, caused nasal mucosal atrophy as compared with oral terfenadine, the active control. None of the expected quantitative changes that could have indicated atrophy were observed, and qualitative assessments confirmed that elastin was not present, type I collagen was not replaced, and basal lamina duplication did not increase. Furthermore, clinical observations during the monthly visits showed no abnormalities on rhinoscopy. When the treatment groups were compared, no significant differences between treatment groups were observed with the exception of epithelial layer thickness, which showed a significant difference between treatments. The fluticasone group experienced a mean increase in the epithelial layer thickness at study end, while the terfenadine group experienced a mean decrease. This result, coupled with the qualitative assessments based on visualization of nasal mucosal tissue, suggests that the integrity of the nasal mucosa was not affected adversely during treatment with fluticasone in subjects with perennial allergic rhinitis. Furthermore, the increase in epithelial thickness after fluticasone treatment may represent repair of epithelial damage associated with the chronic inflammation that is characteristic of perennial allergic disease. Our findings are consistent with the existing literature and confirm what has been the clinical experience for decades, ie, that long-term use of intranasal corticosteroid therapy does not lead to atrophy or other severe adverse sequelae in the nasal mucosa. Moreover, our study is the first, to our knowledge, to use objective and quantitative assessment of the nasal mucosa by transmission electron microscopy and in which lack of change in these objective criteria were used to conclude that fluticasone treatment did not have deleterious effects on the nasal mucosa. Several other intranasal biopsy studies have similarly failed to find an atrophic effect of other intranasal corticosteroids or fluticasone
5 A B Figure 2. Transmission electron micrographs of the collagen layer showing the presence of electron-lucent spaces between the collagen fibrils. A, Lack of lucent spaces between the collagen fibrils, scored 0 (original magnification 15500). B, Large number of electron-lucent spaces between the collagen fibrils, scored 3. The epithelium is seen above the collagen layer (original magnification 14500). A B Figure 3. Transmission electron micrographs of the collagen layer (immediately beneath the epithelium) showing regularity of the collagen fibrils (original magnification 11500). A, Low regularity, scored +1. B, High regularity, scored +3. Among the findings of interest, Sørensen et al 13 in 1976 performed biopsies of polyps after treatment with beclomethasone dipropionate aerosol for 1 year and observed decreased interstitial fluid within the tissue by light microscopy. Furthermore, there were no consistent changes of the surface epithelium by transmission electron microscopy. Quantitative data or controls were not presented. In 1977, Poytner 14 observed that no mucosal atrophy occurred in patients treated with beclomethasone for 2.5 to 3.5 years. In 1978, Mygind et al 15 re- 197
6 Table 2. Subject Demographics and Disposition Table 3. Light and Electron Microscopic Evaluations of Atrophy Measure No. of Patients Fluticasone Propionate, 200 µg/d Fluticasone Propionate, 200 µg/d (n = 38) Mean (SE) No. of Patients Terfenadine, 60 mg Twice Daily Mean (SE) Epithelium layer thickness, µm Baseline (4.97) (4.27) Study end (5.14)* (2.50) Collagen layer thickness, µm Baseline (0.58) (0.82) Study end (0.84) (0.87) Lucent spaces score Baseline (0.15) (0.13) Study end (0.18) (0.17) Regularity of collagen fibrils score Baseline (0.16) (0.14) Study end (0.14) (0.11) *Significant difference vs terfenadine ( P.05). Terfenadine, 60 mg Twice Daily (n = 37) Mean age (range), y 28.8 (20-58) 30.4 (19-61) Sex, No. (%) M 22 (58) 25 (68) F 16 (42) 12 (32) Ethnic origin, No. (%) White 31 (82) 32 (86) Black 4 (11) 1 (3) Other 3 (7) 4 (11) Completed study, No. (%) 25 (66) 26 (70) Withdrawn from study, No. (%) 13 (34) 11 (30) Adverse event 3 (8) 1 (3) Failed to return 6 (16) 5 (14) Lack of efficacy 0 2 (5) Other 4 (11) 3 (8) ported that biopsy specimens of nasal polyps in patients receiving beclomethasone treatment for 3 years showed no changes in epithelial metaplasia or ciliary structure. In 1982, Holopainen and colleagues 16 performed biopsies in 6 patients after 6 years of treatment with beclomethasone and observed no evidence of atrophy. No quantitative data were presented. In 1983, Knight and Kolin 17 performed biopsies in 9 patients with perennial rhinitis with or without allergy after the patients had received beclomethasone for 48 weeks in an open, noncomparative study. They reported no evidence of atrophy or scarring as assessed by light microscopy, but few details were presented. In 1988, Pipkorn et al 18 reported on a multicenter, open longitudinal study of 24 patients receiving budesonide. Biopsy specimens obtained at entry and after 1 year (5 patients) and between 2.5 and 5.5 years (5 patients) of use showed no significant change. In a more recent study, Minshall and colleagues 20 evaluated nasal biopsy specimens from an open study of 52 subjects with perennial rhinitis before and after 1 year of treatment with mometasone furoate by light microscopy and compared the results with those from 24 healthy subjects who underwent biopsy at baseline and after 1 year without treatment. They found no change in epithelial thickness, no signs of atrophy, and a decrease in focal metaplasia. In 1991, Orgel and colleagues 19 evaluated 41 paired nasal biopsy specimens from an open-label study of fluocortin butyl. They reported no evidence of basement membrane thinning and, similar to our findings, observed a tendency for improvement of the epithelium toward columnar. The authors concluded that intranasal corticosteroids improve epithelial injury secondary to chronic inflammation. Holm and colleagues 21 performed a double-blind, placebo-controlled biopsy study with fluticasone with the use of light microscopy in patients with perennial allergic rhinitis. Twenty-eight sets of paired biopsy data were able to be evaluated before and after 1 year of treatment. No differences between the groups were observed before or after treatment. The biopsy site in the Holm et al study (inferior edge of the inferior turbinate) differed from that in ours (anterior tip of the inferior turbinate) but demonstrated that a year s treatment with fluticasone did not alter the mucosa in the ciliated epithelium. Skin atrophy from topically applied corticosteroids can be detected within time frames varying from 1 to 4 months of administration Why the nasal mucosa acts differently from the skin is not known. There are several possible explanations. One explanation is that, while the nose contains only type I collagen, the skin contains elastin and type IV collagen. The latter elements may be more glucocorticoid sensitive. Another explanation may relate to residence time of drug at the application site. With dermatologic preparations, the creams or ointments are applied to a specific site and left in situ, sometimes under occluded conditions, for up to 24 hours. With an intranasal spray, drug is removed within a few hours from the airways by mucociliary transport. An open-label study, although not generally optimal, was specifically selected as the design for this study. Any attempt to double-blind this study, given the differences in the formulations of the test medications (intranasal spray vs oral tablets), would have required a doubledummy design that would have necessitated that all subjects take both oral medication and intranasal spray. Although not expected to have detrimental effects on the nasal mucosa, a placebo spray or the insertion of the device into the nostrils to deliver the nasal spray could potentially have confounded the biopsy data. To obviate this problem, all biopsy evaluations were performed by clinicians who were otherwise uninvolved in the care of subjects and who were blinded to the subject s treatment and identity. This eliminated potential bias and ensured the validity of the nasal mucosa assessments, which were the primary safety assessments in this study. This study was not designed to compare the efficacy of these compounds in the treatment of allergic rhinitis. Fluticasone and terfenadine have been compared in well-controlled clinical trials by others However, 198
7 subjects were examined in this study on a monthly basis to demonstrate that therapeutic doses of both treatment regimens were being taken by the subjects and to reinforce medication adherence. During the study, the treatment groups experienced reductions from baseline in their rhinitis symptom scores as assessed by both clinicians and subjects. Thus, it appeared from these assessments that study medication adherence was sufficient to derive therapeutic benefit. Study treatments were well tolerated during this yearlong study. The adverse event profile was similar between treatments and to that observed in numerous other studies. No serious or unusual events were observed. Only 1 subject withdrew from the fluticasone group because of localized bleeding. Whether this patient would have shown changes on a nasal biopsy specimen consistent with mucosal damage is unknown. Our findings, however, support the clinical impression that, if patients are tolerating intranasal corticosteroids, they can safely continue them. It is therefore prudent to reinforce the clinical practice of examining patients within 2 to 4 weeks of initiation of intranasal corticosteroid treatment with careful attention to the nasal mucosa. If bothersome bleeding is reported by the subject and the nasal mucosa shows evidence of injury, it is prudent to decrease the dose of administered corticosteroids or even discontinue them. The results of this study show that the use of intranasal fluticasone propionate aqueous nasal spray, 200 µg once daily for 1 year, does not lead to atrophy in the nasal mucosa. Conversely, this study shows that treatment with fluticasone leads to a significant increase in epithelial thickness compared with the posttreatment epithelial thickness in the terfenadine-treated group. This suggests a positive effect of intranasal fluticasone on the nasal epithelium. Our study has extended the previous work of others with nasal biopsy by using quantitative objective measures of atrophy from light and electron microscopy in a larger number of subjects and comparing the results with those of biopsy specimens from subjects using a suitable therapeutic alternative. In compilation, these studies all speak to the lack of histologic damage induced by intranasal corticosteroids. In summary, our study should make clinicians feel more secure in their use of intranasal corticosteroids to treat allergic rhinitis. Using light and electron microscopy, we performed a detailed and controlled investigation of the nasal mucosa and found no evidence of structural damage after 1 year of use. Combining these observations with the established efficacy of intranasal corticosteroids in treating nasal symptoms argues that they should be a first-line treatment in patients with perennial allergic rhinitis. Accepted for publication July 31, This study was supported in part by grants AI45583 and DC02714 from the National Institutes of Health, Bethesda, Md, and a grant-in-aid from Glaxo Wellcome Inc, Research Triangle Park, NC. Corresponding author and reprints: Fuad M. Baroody, MD, Section of Otolaryngology Head and Neck Surgery, University of Chicago, 5841 S Maryland Ave, MC1035, Chicago, IL ( fbaroody@surgery.bsd.uchicago.edu). REFERENCES 1. Storms W, Meltzer EO, Nathan RA, Selner JC. The economic impact of allergic rhinitis. J Allergy Clin Immunol. 1997;99(suppl):S820-S Naclerio RM. Allergic rhinitis. N Engl J Med. 1991;325: Mygind N. Glucocorticosteroids and rhinitis. Allergy. 1993;48: Siegel SC. Topical intranasal therapy in rhinitis. J Allergy Clin Immunol. 1988; 81: LaForce C. Use of nasal steroids in managing allergic rhinitis. J Allergy Clin Immunol. 1999;103(suppl 3, pt 2):S388-S Pipkorn U, Proud D, Lichtenstein LM, Kagey-Sobotka A, Norman PS, Naclerio RM. Inhibition of mediator release in allergic rhinitis by pretreatment with topical glucocorticosteroids. N Engl J Med. 1987;316: Jablonska S, Groniowska M, Dabrowski J. Comparative evaluation of skin atrophy in man induced by topical corticoids. Br J Dermatol. 1979;100: Wilson Jones E. Steroid atrophy a histological appraisal. Dermatologica. 1976; 152(suppl 1): Groniowska M, Dabrowski J, Maciejewski W, Walski M. Electron-microscopic evaluation of collagen fibrils after topical corticosteroid therapy. Dermatologica. 1976;152(suppl): Lehmann P, Zheng P, Lavker RM, Kligman AM. Corticosteroid atrophy in human skin: a study by light, scanning and transmission electron microscopy. J Invest Dermatol. 1983;81: Stevanovic DV. Corticosteroid-induced atrophy of the skin with telangiectasia. Br J Dermatol. 1972;87: Lee BJ, Naclerio RM, Bochner BS, Taylor RM, Lim MC, Baroody FM. Nasal challenge with allergen upregulates the local expression of vascular endothelial adhesion molecules. J Allergy Clin Immunol. 1994;94: Sørensen H, Mygind N, Pedersen CB, Prytz S. Long-term treatment of nasal polyps with beclomethasone dipropionate aerosol, III: morphological studies and conclusions. Acta Otolaryngol. 1976;82: Poynter D. Beclomethasone dipropionate aerosol and nasal mucosa. Br J Clin Pharmacol. 1977;4(suppl 3):295S-301S. 15. Mygind N, Sorensen H, Pedersen CB. The nasal mucosa during long-term treatment with beclomethasone dipropionate aerosol: a light- and scanning electron microscopic study of nasal polyps. Acta Otolaryngol. 1978;85: Holopainen E, Malmberg H, Binder E. Long-term follow-up of intranasal beclomethasone treatment: a clinical and histologic study. Acta Otolaryngol Suppl. 1982;386: Knight A, Kolin A. Long term efficacy and safety of beclomethasone dipropionate aerosol in perennial rhinitis. Ann Allergy. 1983;50: Pipkorn U, Pukander J, Suonpää J, Mäkinen J, Lindqvist N. Long-term safety of budesonide nasal aerosol: a 5.5-year follow-up study. Clin Allergy. 1988;18: Orgel HA, Meltzer EO, Beirman CW, et al. Intranasal fluocortin butyl in patients with perennial rhinitis: a 12-month efficacy and safety study including nasal biopsy. J Allergy Clin Immunol. 1991;88: Minshall E, Ghaffar O, Cameron L, et al. Assessment by nasal biopsy of longterm use of mometasone furoate aqueous nasal spray (Nasonex) in the treatment of perennial rhinitis. Otolaryngol Head Neck Surg. 1998;118: Holm AF, Fokkens WJ, Godthelp T, Mulder PG, Vroom TM, Rijntjes E. A 1-year placebo-controlled study of intranasal fluticasone propionate aqueous nasal spray in patients with perennial allergic rhinitis: a safety and biopsy study. Clin Otolaryngol. 1998;23: Bronsky EA, Dockhorn RJ, Meltzer EO, et al. Fluticasone propionate aqueous nasal spray compared with terfenadine tablets in the treatment of seasonal allergic rhinitis. J Allergy Clin Immunol. 1996;97: van Bavel J, Findlay SR, Hampel FC Jr, Martin BG, Ratner P, Field E. Intranasal fluticasone propionate is more effective than terfenadine tablets for seasonal allergic rhinitis [published correction appears in Arch Intern Med. 1995;155:276]. Arch Intern Med. 1994;154: Darnell R, Pecoud A, Richards DH. A double-blind comparison of fluticasone propionate aqueous nasal spray, terfenadine tablets and placebo in the treatment of patients with seasonal allergic rhinitis to grass pollen. Clin Exp Allergy. 1994; 24:
As-needed use of fluticasone propionate nasal spray reduces symptoms of seasonal allergic rhinitis
 As-needed use of fluticasone propionate nasal spray reduces symptoms of seasonal allergic rhinitis Albert Jen, MD, Fuad Baroody, MD, Marcy detineo, BSN, Lauran Haney, BSc, Christopher Blair, BSc, and Robert
As-needed use of fluticasone propionate nasal spray reduces symptoms of seasonal allergic rhinitis Albert Jen, MD, Fuad Baroody, MD, Marcy detineo, BSN, Lauran Haney, BSc, Christopher Blair, BSc, and Robert
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION Superiority of an Intranasal Corticosteroid Compared With an Oral Antihistamine in the As-Needed Treatment of Seasonal Allergic Rhinitis Scott M. Kaszuba, MD; Fuad M. Baroody, MD;
ORIGINAL INVESTIGATION Superiority of an Intranasal Corticosteroid Compared With an Oral Antihistamine in the As-Needed Treatment of Seasonal Allergic Rhinitis Scott M. Kaszuba, MD; Fuad M. Baroody, MD;
Safety and efficacy of mometasone furoate aqueous nasal spray in children with allergic rhinitis: Results of recent clinical trials
 Safety and efficacy of mometasone furoate aqueous nasal spray in children with allergic rhinitis: Results of recent clinical trials Javier Dibildox, MD San Luis Potosí, Mexico Intranasal mometasone furoate
Safety and efficacy of mometasone furoate aqueous nasal spray in children with allergic rhinitis: Results of recent clinical trials Javier Dibildox, MD San Luis Potosí, Mexico Intranasal mometasone furoate
Intranasal steroids and the myth of mucosal atrophy: A systematic review of original histological assessments METHODS
 Intranasal steroids and the myth of mucosal atrophy: A systematic review of original histological assessments Misha M. Verkerk, M.B.B.S., 1 Daman Bhatia, M.B.B.S., 2 Janet Rimmer, F.R.A.C.P., 3 Peter Earls,
Intranasal steroids and the myth of mucosal atrophy: A systematic review of original histological assessments Misha M. Verkerk, M.B.B.S., 1 Daman Bhatia, M.B.B.S., 2 Janet Rimmer, F.R.A.C.P., 3 Peter Earls,
Scottish Medicines Consortium
 Scottish Medicines Consortium fluticasone furoate, 27.5 micrograms /actuation nasal (Avamys ) No. (544/09) GlaxoSmithKline 06 March 2009 The Scottish Medicines Consortium (SMC) has completed its assessment
Scottish Medicines Consortium fluticasone furoate, 27.5 micrograms /actuation nasal (Avamys ) No. (544/09) GlaxoSmithKline 06 March 2009 The Scottish Medicines Consortium (SMC) has completed its assessment
BECLOMETHASONE DIPROPIONATE AEROSOL AND NASAL MUCOSA
 Br. J. clin. Pharmac. (1977), 4, 295S-31S BECLOMETHASONE DIPROPIONATE AEROSOL AND NASAL MUCOSA Medical Division, Allen & Hanburys Research Limited,Ware, Hertfordshire, UK I Biopsies taken from the inferior
Br. J. clin. Pharmac. (1977), 4, 295S-31S BECLOMETHASONE DIPROPIONATE AEROSOL AND NASAL MUCOSA Medical Division, Allen & Hanburys Research Limited,Ware, Hertfordshire, UK I Biopsies taken from the inferior
Phototherapy in Allergic Rhinitis
 Phototherapy in Allergic Rhinitis Rhinology Chair KSU KAUH Ibrahim AlAwadh 18\1\2017 MBBS, SB & KSUF Resident, ORL-H&N Background: Endonasal phototherapy can relieve the symptoms of allergic rhinitis
Phototherapy in Allergic Rhinitis Rhinology Chair KSU KAUH Ibrahim AlAwadh 18\1\2017 MBBS, SB & KSUF Resident, ORL-H&N Background: Endonasal phototherapy can relieve the symptoms of allergic rhinitis
The role of histamine in allergic rhinitis
 The role of histamine in allergic rhinitis Robert M. Naclerio, MD Baltimore, Maryland Studies using nasal provocation followed by nasal lavage have demonstrated that histamine plays a n important role
The role of histamine in allergic rhinitis Robert M. Naclerio, MD Baltimore, Maryland Studies using nasal provocation followed by nasal lavage have demonstrated that histamine plays a n important role
The Medical Letter. on Drugs and Therapeutics. Drug Some Formulations OTC/Rx Usual Dosage Comments Class Comments Cost 1
 The Medical Letter publications are protected by US and international copyright laws. Forwarding, copying or any other distribution of this material is strictly prohibited. For further information call:
The Medical Letter publications are protected by US and international copyright laws. Forwarding, copying or any other distribution of this material is strictly prohibited. For further information call:
A clinical trial of ipratropium bromide nasal spray in patients with perennial nonallergic rhinitis
 A clinical trial of ipratropium bromide nasal spray in patients with perennial nonallergic rhinitis Edwin A. Bronsky, MD, Howard Druce, MD, Steven R. Findlay, MD, Frank C. Hampel, MD, Harold Kaiser, MD,
A clinical trial of ipratropium bromide nasal spray in patients with perennial nonallergic rhinitis Edwin A. Bronsky, MD, Howard Druce, MD, Steven R. Findlay, MD, Frank C. Hampel, MD, Harold Kaiser, MD,
ORIGINAL ARTICLE. Increased Nasal Airflow With Budesonide Compared With Desloratadine During the Allergy Season
 ORIGINAL ARTICLE Increased Nasal Airflow With Budesonide Compared With Desloratadine During the Allergy Season Sandeep Bhatia, BS; Fuad M. Baroody, MD; Marcy detineo, BSN; Robert M. Naclerio, MD Objective:
ORIGINAL ARTICLE Increased Nasal Airflow With Budesonide Compared With Desloratadine During the Allergy Season Sandeep Bhatia, BS; Fuad M. Baroody, MD; Marcy detineo, BSN; Robert M. Naclerio, MD Objective:
Repeated antigen challenge in patients with perennial allergic rhinitis to house dust mites
 Allergology International (2003) 52: 207 212 Original Article Repeated antigen challenge in patients with perennial allergic rhinitis to house dust mites Minoru Gotoh, Kimihiro Okubo and Minoru Okuda Department
Allergology International (2003) 52: 207 212 Original Article Repeated antigen challenge in patients with perennial allergic rhinitis to house dust mites Minoru Gotoh, Kimihiro Okubo and Minoru Okuda Department
EFFICACY AND SAFETY OF OLOPATADINE/MOMETASONE COMBINATION NASAL SPRAY FOR THE TREATMENT OF SEASONAL ALLERGIC RHINITIS
 EFFICACY AND SAFETY OF OLOPATADINE/MOMETASONE COMBINATION NASAL SPRAY FOR THE TREATMENT OF SEASONAL ALLERGIC RHINITIS PAUL H. RATNER 1 ; FRANK HAMPEL 2 ; AURORA BREAZNA 3 ; CYNTHIA F. CARACTA 3 ; SUDEESH
EFFICACY AND SAFETY OF OLOPATADINE/MOMETASONE COMBINATION NASAL SPRAY FOR THE TREATMENT OF SEASONAL ALLERGIC RHINITIS PAUL H. RATNER 1 ; FRANK HAMPEL 2 ; AURORA BREAZNA 3 ; CYNTHIA F. CARACTA 3 ; SUDEESH
ALLERGIC RHINITIS Eve Kerr, M.D., M.P.H.
 - 63-3. ALLERGIC RHINITIS Eve Kerr, M.D., M.P.H. We conducted a MEDLINE search of review articles on rhinitis between the years of 1990-1995 and selected articles pertaining to allergic rhinitis. We also
- 63-3. ALLERGIC RHINITIS Eve Kerr, M.D., M.P.H. We conducted a MEDLINE search of review articles on rhinitis between the years of 1990-1995 and selected articles pertaining to allergic rhinitis. We also
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
CENTENE PHARMACY AND THERAPEUTICS DRUG REVIEW 1Q18 January February
 BRAND NAME Xhance GENERIC NAME Fluticasone propionate MANUFACTURER Optinose DATE OF APPROVAL September 18 th, 2017 PRODUCT LAUNCH DATE 1 Second quarter of 2018 REVIEW TYPE Review type 1 (RT1): New Drug
BRAND NAME Xhance GENERIC NAME Fluticasone propionate MANUFACTURER Optinose DATE OF APPROVAL September 18 th, 2017 PRODUCT LAUNCH DATE 1 Second quarter of 2018 REVIEW TYPE Review type 1 (RT1): New Drug
Patients with chronic fatigue syndrome (CFS) have severe,
 Effect of Topical Nasal Corticosteroids on Patients With Chronic Fatigue Syndrome and Rhinitis Sujani S. Kakumanu, MD; Cathy N. Mende, RNP; Erik B. Lehman, MA; Kathleen Hughes, MD; Timothy J. Craig, DO
Effect of Topical Nasal Corticosteroids on Patients With Chronic Fatigue Syndrome and Rhinitis Sujani S. Kakumanu, MD; Cathy N. Mende, RNP; Erik B. Lehman, MA; Kathleen Hughes, MD; Timothy J. Craig, DO
Allergic Rhinitis 6/10/2016. Clinical and Economic Impact. Clinical and Economic Impact. Symptoms. Genetic/Environmental factors
 I have no disclosures to make other than I too suffer from allergic rhinitis Allergic Rhinitis Betsy Close, MD Assistant Professor UT College of Medicine, Department of Family Medicine Clinical and Economic
I have no disclosures to make other than I too suffer from allergic rhinitis Allergic Rhinitis Betsy Close, MD Assistant Professor UT College of Medicine, Department of Family Medicine Clinical and Economic
Clinical and antiinflammatory effects of intranasal budesonide aqueous pump spray in the treatment of perennial allergic rhinitis Eli O Meltzer, MD
 Clinical and antiinflammatory effects of intranasal budesonide aqueous pump spray in the treatment of perennial allergic rhinitis Eli O Meltzer, MD Background: Intranasal corticosteroids are among the
Clinical and antiinflammatory effects of intranasal budesonide aqueous pump spray in the treatment of perennial allergic rhinitis Eli O Meltzer, MD Background: Intranasal corticosteroids are among the
Allergic Rhinitis. Abstract Allergic rhinitis is defined as an immunologic response moderated by IgE and is. Continuing Education Column
 Allergic Rhinitis Hun Jong Dhong, M.D. Department of Otorhinolaryngology Head and Neck Surgery Sungkyunkwan University School of Medicine, Samsung Medical Center E mail : hjdhong@smc.samsung.co.kr Abstract
Allergic Rhinitis Hun Jong Dhong, M.D. Department of Otorhinolaryngology Head and Neck Surgery Sungkyunkwan University School of Medicine, Samsung Medical Center E mail : hjdhong@smc.samsung.co.kr Abstract
Meda Pharmaceuticals
 MP03-33 Nasal Spray Page 1 of 9 Meda Pharmaceuticals Active-Controlled Trial of the Safety and Tolerability of MP03-33 in Patients with Chronic Allergic or Nonallergic Rhinitis (MP432) FINAL CLINICAL STUDY
MP03-33 Nasal Spray Page 1 of 9 Meda Pharmaceuticals Active-Controlled Trial of the Safety and Tolerability of MP03-33 in Patients with Chronic Allergic or Nonallergic Rhinitis (MP432) FINAL CLINICAL STUDY
Azelastine And Xylometazoline-induced Microscopic Changes In The Nasal Mucosa And Olfactory Bulb
 Azelastine And Xylometazoline-induced Microscopic Changes In The Nasal Mucosa And Olfactory Bulb M. Azim Khan, Aijaz A. Khan and Nafis A. Faruqi JNMC, AMU, Aligarh Abstract: Topical nasal decongestants
Azelastine And Xylometazoline-induced Microscopic Changes In The Nasal Mucosa And Olfactory Bulb M. Azim Khan, Aijaz A. Khan and Nafis A. Faruqi JNMC, AMU, Aligarh Abstract: Topical nasal decongestants
Middleton Chapter 42b (pages ): Allergic and Nonallergic Rhinitis Prepared by: Tammy Peng, MD
 FIT Board Review Corner November 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
FIT Board Review Corner November 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
Case Study. Allergic Rhinitis 5/18/2015
 John A. Fling, M.D. Professor Allergy/Immunology University of North Texas Health Science Center, Fort Worth, Texas Case Study 38 year old male with a history of nasal congestion, clear nasal discharge
John A. Fling, M.D. Professor Allergy/Immunology University of North Texas Health Science Center, Fort Worth, Texas Case Study 38 year old male with a history of nasal congestion, clear nasal discharge
A double-blind, controlled trial to assess the safety and efficacy of azelastine nasal spray in seasonal allergic rhinitis
 A double-blind, controlled trial to assess the safety and efficacy of azelastine nasal spray in seasonal allergic rhinitis Paul H. Ratner, MDfl Steven R. Findlay, MD, b Frank Hampel, Jr., MD, Julius van
A double-blind, controlled trial to assess the safety and efficacy of azelastine nasal spray in seasonal allergic rhinitis Paul H. Ratner, MDfl Steven R. Findlay, MD, b Frank Hampel, Jr., MD, Julius van
Cost-effectiveness analysis of budesonide aqueous nasal spray and fluticasone propionate nasal spray in the treatment of perennial allergic rhinitis
 Cost-effectiveness analysis of budesonide aqueous nasal spray and fluticasone propionate nasal spray in the treatment of perennial allergic rhinitis Stahl E, van Rompay W, Wang E C, Thomson D M Record
Cost-effectiveness analysis of budesonide aqueous nasal spray and fluticasone propionate nasal spray in the treatment of perennial allergic rhinitis Stahl E, van Rompay W, Wang E C, Thomson D M Record
Randy Russell Assistant Director, Regulatory Affairs Alcon Research, Ltd South Freeway, R3-54 Fort Worth, TX
 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Silver Spring, MD 20993 Randy Russell Assistant Director, Regulatory Affairs 6201 South Freeway, R3-54 Fort Worth,
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Silver Spring, MD 20993 Randy Russell Assistant Director, Regulatory Affairs 6201 South Freeway, R3-54 Fort Worth,
Seasonal Allergic Rhinoconjunctivitis
 Seasonal Allergic Rhinoconjunctivitis Allergic rhinoconjunctivitis is a common condition. Most patients can achieve good symptom control through allergen avoidance and pharmacotherapy with non-sedating
Seasonal Allergic Rhinoconjunctivitis Allergic rhinoconjunctivitis is a common condition. Most patients can achieve good symptom control through allergen avoidance and pharmacotherapy with non-sedating
EFFICACY AND SAFETY OF OLOPATADINE/MOMETASONE COMBINATION NASAL SPRAY FOR THE TREATMENT OF SEASONAL ALLERGIC RHINITIS
 EFFICACY AND SAFETY OF OLOPATADINE/MOMETASONE COMBINATION NASAL SPRAY FOR THE TREATMENT OF SEASONAL ALLERGIC RHINITIS GARY GROSS 1 ; FRANK HAMPEL 2 ; AURORA BREAZNA 3 ; CYNTHIA F. CARACTA 3 ; SUDEESH K.
EFFICACY AND SAFETY OF OLOPATADINE/MOMETASONE COMBINATION NASAL SPRAY FOR THE TREATMENT OF SEASONAL ALLERGIC RHINITIS GARY GROSS 1 ; FRANK HAMPEL 2 ; AURORA BREAZNA 3 ; CYNTHIA F. CARACTA 3 ; SUDEESH K.
ON THE PRESENCE OF A CILIATED COLUMNAR EPITHELIAL CELL TYPE WITHIN THE BOVINE CERVICAL MUCOSA 1
 ON THE PRESENCE OF A CILIATED COLUMNAR EPITHELIAL CELL TYPE WITHIN THE BOVINE CERVICAL MUCOSA 1 R. I. Wordinger, 2 J. B. Ramsey, I. F. Dickey and I. R. Hill, Jr. Clemson University, Clemson, South Carolina
ON THE PRESENCE OF A CILIATED COLUMNAR EPITHELIAL CELL TYPE WITHIN THE BOVINE CERVICAL MUCOSA 1 R. I. Wordinger, 2 J. B. Ramsey, I. F. Dickey and I. R. Hill, Jr. Clemson University, Clemson, South Carolina
Allergic Rhinitis and Its Impact on Ast. Rhinitis: A Risk Factor for Asthma? Ronald Dahl, Aarhus University Hospital, Denmark
 Allergic Rhinitis and Its Impact on Ast Rhinitis: A Risk Factor for Asthma? Ronald Dahl, Aarhus University Hospital, Denmark Rhinitis and asthma SIT-SLIT Evidence A SIT-SLIT Evidence A? SIT Evidence? Rhinitis
Allergic Rhinitis and Its Impact on Ast Rhinitis: A Risk Factor for Asthma? Ronald Dahl, Aarhus University Hospital, Denmark Rhinitis and asthma SIT-SLIT Evidence A SIT-SLIT Evidence A? SIT Evidence? Rhinitis
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of intranasal phototherapy for allergic rhinitis Allergic rhinitis is inflammation
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of intranasal phototherapy for allergic rhinitis Allergic rhinitis is inflammation
Dual-Controller Asthma Therapy: Rationale and Clinical Benefits
 B/1 Dual-Controller Asthma Therapy: Rationale and Clinical Benefits MODULE B The 1997 National Heart, Lung, and Blood Institute (NHLBI) Expert Panel guidelines on asthma management recommend a 4-step approach
B/1 Dual-Controller Asthma Therapy: Rationale and Clinical Benefits MODULE B The 1997 National Heart, Lung, and Blood Institute (NHLBI) Expert Panel guidelines on asthma management recommend a 4-step approach
Corporate Medical Policy Septoplasty
 Corporate Medical Policy Septoplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: septoplasty 4/1999 8/2018 8/2019 8/2018 Description of Procedure or Service There are many potential
Corporate Medical Policy Septoplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: septoplasty 4/1999 8/2018 8/2019 8/2018 Description of Procedure or Service There are many potential
Matt Stumpe, MD Otolaryngologist Mid Kansas Ear, Nose, & Throat
 Matt Stumpe, MD Otolaryngologist Mid Kansas Ear, Nose, & Throat Inflammation of the nasal mucosa secondary to an inappropriate hypersensitivity reaction to an allergen IgE mediated immune response with
Matt Stumpe, MD Otolaryngologist Mid Kansas Ear, Nose, & Throat Inflammation of the nasal mucosa secondary to an inappropriate hypersensitivity reaction to an allergen IgE mediated immune response with
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS
 MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
Allergic rhinitis affects up to 400 million people worldwide
 ORIGINAL ARTICLE A pilot study of the effects of intranasal budesonide delivered by NasoNeb R on patients with perennial allergic rhinitis Kristal Brown, MD, James Lane, BSc, Marianella Paz Silva, MD,
ORIGINAL ARTICLE A pilot study of the effects of intranasal budesonide delivered by NasoNeb R on patients with perennial allergic rhinitis Kristal Brown, MD, James Lane, BSc, Marianella Paz Silva, MD,
Allergic rhinitis (AR) is a highly prevalent disease, affecting
 Cost Efficiency of Intranasal Corticosteroid Prescribing Patterns in the Management of Allergic Rhinitis DEBI REISSMAN, PharmD; TOM PRICE, BA; and CHRISTOPHER W. LEIBMAN, PharmD, MS ABSTRACT BACKGROUND:
Cost Efficiency of Intranasal Corticosteroid Prescribing Patterns in the Management of Allergic Rhinitis DEBI REISSMAN, PharmD; TOM PRICE, BA; and CHRISTOPHER W. LEIBMAN, PharmD, MS ABSTRACT BACKGROUND:
SYNOPSIS. A Multi-center, Double-blind, Randomized, Placebo-controlled, Parallel Group, Phase II Study to Assess the Efficacy and Safety of RHINOCORT
 Drug product: RHINOCORT AQUA Drug substance(s): Budesonide Edition No.: Final Study code: D5360C00703 Date: 8 November 2005 SYNOPSIS A Multi-center, Double-blind, Randomized, Placebo-controlled, Parallel
Drug product: RHINOCORT AQUA Drug substance(s): Budesonide Edition No.: Final Study code: D5360C00703 Date: 8 November 2005 SYNOPSIS A Multi-center, Double-blind, Randomized, Placebo-controlled, Parallel
Fluticasone furoate (Avamys): new intranasal steroid spray Steve Chaplin MSc, MRPharmS
 Fluticasone furoate (Avamys): new intranasal steroid spray Steve Chaplin MSc, MRPharmS KEY POINTS Avamys is a metered-dose nasal spray containing 27.5µg fluticasone furoate per dose indicated for the treatment
Fluticasone furoate (Avamys): new intranasal steroid spray Steve Chaplin MSc, MRPharmS KEY POINTS Avamys is a metered-dose nasal spray containing 27.5µg fluticasone furoate per dose indicated for the treatment
Clinical Study Long-Term Histologic Changes in Nasal Mucosa after Total Laryngectomy
 International Otolaryngology Volume 2010, Article ID 137128, 4 pages doi:10.1155/2010/137128 Clinical Study Long-Term Histologic Changes in asal Mucosa after Total Laryngectomy Çiğdem Tepe Karaca, 1 Erdoğan
International Otolaryngology Volume 2010, Article ID 137128, 4 pages doi:10.1155/2010/137128 Clinical Study Long-Term Histologic Changes in asal Mucosa after Total Laryngectomy Çiğdem Tepe Karaca, 1 Erdoğan
9/18/2018. Disclosures. Objectives
 Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Scottish Medicines Consortium
 Scottish Medicines Consortium Standardised allergen extract of grass pollen from Timothy (Phleum pratense) 75,000 SQ-T per oral lyophilisate (Grazax ) No. (367/07) ALK-Abellό Ltd 6 April 2007 The Scottish
Scottish Medicines Consortium Standardised allergen extract of grass pollen from Timothy (Phleum pratense) 75,000 SQ-T per oral lyophilisate (Grazax ) No. (367/07) ALK-Abellό Ltd 6 April 2007 The Scottish
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Latest advances in the management of childhood allergic rhinitis
 Latest advances in the management of childhood allergic rhinitis Jason Y K Chan Assistant Professor Department of Otorhinolaryngology, Head & Neck Surgery The Chinese University of Hong Kong Disclosures
Latest advances in the management of childhood allergic rhinitis Jason Y K Chan Assistant Professor Department of Otorhinolaryngology, Head & Neck Surgery The Chinese University of Hong Kong Disclosures
Overview of inhaled and nasal corticosteroids and haematoma
 Overview of inhaled and nasal corticosteroids and haematoma Introduction Inhaled glucocorticoids (ICS) are widely used to treat asthma and chronic obstructive pulmonary disease (COPD). Nasal glucocorticoids
Overview of inhaled and nasal corticosteroids and haematoma Introduction Inhaled glucocorticoids (ICS) are widely used to treat asthma and chronic obstructive pulmonary disease (COPD). Nasal glucocorticoids
Introduction. Allergic Rhinitis. Seventh Pediatric Asthma Education Conference 5/9/2018
 It Is All One Airway Or How Allergic Rhinitis and Its Management can Affect Asthmatic Patients Stacy Dorris, MD Allergy/Immunology Vanderbilt Medical Center May 9, 2018 Introduction Allergic Rhinitis Allergic
It Is All One Airway Or How Allergic Rhinitis and Its Management can Affect Asthmatic Patients Stacy Dorris, MD Allergy/Immunology Vanderbilt Medical Center May 9, 2018 Introduction Allergic Rhinitis Allergic
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: House dust mite allergen extract (Odactra) Reference Number: CP.PMN.111 Effective Date: 08.01.17 Last Review Date: 08.18 Line of Business: Commercial, Medicaid Revision Log See Important
Clinical Policy: House dust mite allergen extract (Odactra) Reference Number: CP.PMN.111 Effective Date: 08.01.17 Last Review Date: 08.18 Line of Business: Commercial, Medicaid Revision Log See Important
Azelastine nasal spray: the treatment of choice for allergic rhinitis
 PRESS RELEASE Azelastine nasal spray: the treatment of choice for allergic rhinitis An astonishing one quarter of the planet s population suffers from allergic rhinitis, living with the aggravating symptoms
PRESS RELEASE Azelastine nasal spray: the treatment of choice for allergic rhinitis An astonishing one quarter of the planet s population suffers from allergic rhinitis, living with the aggravating symptoms
Derriford Hospital. Peninsula Medical School
 Asthma and Allergic Rhinitis iti What is the Connection? Hisham Khalil Consultant ENT Surgeon Clinical Senior Lecturer, PMS Clinical Sub-Dean GP Evening 25 June 2008 Plymouth Derriford Hospital Peninsula
Asthma and Allergic Rhinitis iti What is the Connection? Hisham Khalil Consultant ENT Surgeon Clinical Senior Lecturer, PMS Clinical Sub-Dean GP Evening 25 June 2008 Plymouth Derriford Hospital Peninsula
Raising awareness of upper airway diseases: Overview of management and prevention strategies WANG De-yun *
 Med J Chin PLA, Vol. 42, No. 10, October 1, 2017 843 ( ) 2017 10 11 (ARIA2001 2008) (GA2LEN) - (EP3OS 2007 2012) (2016) Allergy Therapeutics and Clinical Risk Management Military Medical Research 20-230
Med J Chin PLA, Vol. 42, No. 10, October 1, 2017 843 ( ) 2017 10 11 (ARIA2001 2008) (GA2LEN) - (EP3OS 2007 2012) (2016) Allergy Therapeutics and Clinical Risk Management Military Medical Research 20-230
The effectiveness of oxymetazoline plus intranasal steroid in the treatment of chronic rhinitis: A randomised controlled trial
 Original article The effectiveness of oxymetazoline plus intranasal steroid in the treatment of chronic rhinitis: A randomised controlled trial Torpong Thongngarm, 1 Paraya Assanasen, 2 Panitan Pradubpongsa
Original article The effectiveness of oxymetazoline plus intranasal steroid in the treatment of chronic rhinitis: A randomised controlled trial Torpong Thongngarm, 1 Paraya Assanasen, 2 Panitan Pradubpongsa
Secondary Outcome/Efficacy Variable(s):
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Aerospan (flunisolide)
 STRENGTH DOSAGE FORM ROUTE GPID 80mcg/actuation HFA aerosol inhaler w/ Inhaled 35718 8.9 g/canister adapter MANUFACTURER Meda Pharmaceuticals INDICATION Aerospan Inhalation Aerosol is indicated for the
STRENGTH DOSAGE FORM ROUTE GPID 80mcg/actuation HFA aerosol inhaler w/ Inhaled 35718 8.9 g/canister adapter MANUFACTURER Meda Pharmaceuticals INDICATION Aerospan Inhalation Aerosol is indicated for the
International Journal of Research and Review E-ISSN: ; P-ISSN:
 International Journal of Research and Review www.ijrrjournal.com E-ISSN: 2349-9788; P-ISSN: 2454-2237 Original Research Article Quantitative Nasal Eosinophilia: An Objective Tool to Optimize Intranasal
International Journal of Research and Review www.ijrrjournal.com E-ISSN: 2349-9788; P-ISSN: 2454-2237 Original Research Article Quantitative Nasal Eosinophilia: An Objective Tool to Optimize Intranasal
Medicine Review. Medicine / Trade name Azelastine and fluticasone / Dymista Manufacturer
 East & South East England Specialist Pharmacy Services East of England, London, South Central & South East Coast East Anglia Medicines Information Service Medicine Review Medicine / Trade name Azelastine
East & South East England Specialist Pharmacy Services East of England, London, South Central & South East Coast East Anglia Medicines Information Service Medicine Review Medicine / Trade name Azelastine
Changes in Nasal Reactivity in Patients with Rhinitis medicamentosa after Treatment with Fluticasone Propionate and Placebo Nasal Spray
 Original Paper ORL 1998;60:334 338 Received: November 24, 1997 Accepted after revision: May 19, 1998 Peter M. Graf Hans Hallén Department of Otorhinolaryngology, Huddinge University Hospital, Stockholm,
Original Paper ORL 1998;60:334 338 Received: November 24, 1997 Accepted after revision: May 19, 1998 Peter M. Graf Hans Hallén Department of Otorhinolaryngology, Huddinge University Hospital, Stockholm,
Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino Jul-Aug; 21(4):423-7
 AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
Yara Saddam. Amr Alkhatib. Ihsan
 1 Yara Saddam Amr Alkhatib Ihsan NOTE: Yellow highlighting=correction/addition to the previous version of the sheet. Histology (micro anatomy) :- the study of tissues and how they are arranged into organs.
1 Yara Saddam Amr Alkhatib Ihsan NOTE: Yellow highlighting=correction/addition to the previous version of the sheet. Histology (micro anatomy) :- the study of tissues and how they are arranged into organs.
INVESTIGATIONS & PROCEDURES IN PULMONOLOGY. Immunotherapy in Asthma Dr. Zia Hashim
 INVESTIGATIONS & PROCEDURES IN PULMONOLOGY Immunotherapy in Asthma Dr. Zia Hashim Definition Involves Administration of gradually increasing quantities of specific allergens to patients with IgE-mediated
INVESTIGATIONS & PROCEDURES IN PULMONOLOGY Immunotherapy in Asthma Dr. Zia Hashim Definition Involves Administration of gradually increasing quantities of specific allergens to patients with IgE-mediated
Inferior turbinate hypertrophy is a common cause of nasal. Prediction of outcome of radiofrequency ablation of the inferior turbinates
 ORIGINAL ARTICLE Prediction of outcome of radiofrequency ablation of the inferior turbinates Asli Sahin-Yilmaz, MD 1,Çağatay Oysu, MD 1, Ibrahim Devecioglu, MD 1, Kadri Demir, MD 1 and Jacquelynne P. Corey,
ORIGINAL ARTICLE Prediction of outcome of radiofrequency ablation of the inferior turbinates Asli Sahin-Yilmaz, MD 1,Çağatay Oysu, MD 1, Ibrahim Devecioglu, MD 1, Kadri Demir, MD 1 and Jacquelynne P. Corey,
ARIA. At-A-Glance Pocket Reference 2007
 ARIA_Glance_2007_8pg:ARIA_Glance_English 9/14/07 3:10 PM Page 1 ARIA At-A-Glance Pocket Reference 2007 1 st Edition NEW ARIA UPDATE BASED ON THE ALLERGIC RHINITIS AND ITS IMPACT ON ASTHMA WORKSHOP REPORT
ARIA_Glance_2007_8pg:ARIA_Glance_English 9/14/07 3:10 PM Page 1 ARIA At-A-Glance Pocket Reference 2007 1 st Edition NEW ARIA UPDATE BASED ON THE ALLERGIC RHINITIS AND ITS IMPACT ON ASTHMA WORKSHOP REPORT
Intranasal corticosteroids versus oral H 1
 Intranasal corticosteroids versus oral H 1 antagonists in allergic rhinitis: systematic review of randomised controlled trials John M Weiner, Michael J Abramson, Robert M Puy Department of Medicine, Monash
Intranasal corticosteroids versus oral H 1 antagonists in allergic rhinitis: systematic review of randomised controlled trials John M Weiner, Michael J Abramson, Robert M Puy Department of Medicine, Monash
PRODUCT INFORMATION FLIXONASE ALLERGY & HAYFEVER 24 HOUR
 PRODUCT INFORMATION FLIXONASE ALLERGY & HAYFEVER 24 HOUR NAME Fluticasone propionate DESCRIPTION FLIXONASE ALLERGY & HAYFEVER 24 HOUR Fluticasone Aqueous Nasal Spray (0.05 w/w) is an aqueous suspension
PRODUCT INFORMATION FLIXONASE ALLERGY & HAYFEVER 24 HOUR NAME Fluticasone propionate DESCRIPTION FLIXONASE ALLERGY & HAYFEVER 24 HOUR Fluticasone Aqueous Nasal Spray (0.05 w/w) is an aqueous suspension
ALLERGIC RHINITIS AND ASTHMA :
 ALLERGIC RHINITIS AND ASTHMA : from the Link to Emerging Therapies Allergic rhinitis and asthma are both chronic heterogeneous disorders, with an overlapping epidemiology of prevalence, health care costs
ALLERGIC RHINITIS AND ASTHMA : from the Link to Emerging Therapies Allergic rhinitis and asthma are both chronic heterogeneous disorders, with an overlapping epidemiology of prevalence, health care costs
This report will provide a review on the comparative clinical effectiveness and safety between intranasal triamcinolone and beclomethasone.
 TITLE: Intranasal Triamcinolone versus Intranasal Beclomethasone for Acute and Chronic Sinus Inflammation: A Review of Comparative Clinical Effectiveness and Safety DATE: 29 January 2013 CONTEXT AND POLICY
TITLE: Intranasal Triamcinolone versus Intranasal Beclomethasone for Acute and Chronic Sinus Inflammation: A Review of Comparative Clinical Effectiveness and Safety DATE: 29 January 2013 CONTEXT AND POLICY
Distribution The in vitro protein binding for Mometasone furoate was reported to be 98% to 99% in concentra on range of 5 to 500 ng/ml.
 NOSATREX Composition Mometasone Furoate 0.05% w/w Spray Action Mechanism of Action Mometasone Nasal Spray 50 mcg is a cor costeroid demonstra ng potent an -inflammatory properties. The precise mechanism
NOSATREX Composition Mometasone Furoate 0.05% w/w Spray Action Mechanism of Action Mometasone Nasal Spray 50 mcg is a cor costeroid demonstra ng potent an -inflammatory properties. The precise mechanism
Managing and Treating Allergic Rhinitis in the Primary Care Setting
 University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2014 Managing and Treating Allergic Rhinitis in the Primary Care Setting Leah Novinger University
University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2014 Managing and Treating Allergic Rhinitis in the Primary Care Setting Leah Novinger University
Clinical & Experimental Allergy
 ORIGINAL ARTICLE Clinical & Experimental Allergy, 1 7 doi: 10.1111/j.1365-2222.2010.03660.x c 2010 Blackwell Publishing Ltd Effects of mometasone furoate on the quality of life: a randomized placebo-controlled
ORIGINAL ARTICLE Clinical & Experimental Allergy, 1 7 doi: 10.1111/j.1365-2222.2010.03660.x c 2010 Blackwell Publishing Ltd Effects of mometasone furoate on the quality of life: a randomized placebo-controlled
Omalizumab (Xolair ) ( Genentech, Inc., Novartis Pharmaceuticals Corp.) September Indication
 ( Genentech, Inc., Novartis Pharmaceuticals Corp.) September 2003 Indication The FDA recently approved Omalizumab on June 20, 2003 for adults and adolescents (12 years of age and above) with moderate to
( Genentech, Inc., Novartis Pharmaceuticals Corp.) September 2003 Indication The FDA recently approved Omalizumab on June 20, 2003 for adults and adolescents (12 years of age and above) with moderate to
Scottish Medicines Consortium
 Scottish Medicines Consortium montelukast 10mg tablets (Singulair ) No. (185/05) Merck, Sharp & Dohme Ltd (MSD) New indication: for asthmatic patients in whom montelukast is indicated in asthma, montelukast
Scottish Medicines Consortium montelukast 10mg tablets (Singulair ) No. (185/05) Merck, Sharp & Dohme Ltd (MSD) New indication: for asthmatic patients in whom montelukast is indicated in asthma, montelukast
ORIGINAL ARTICLE. Epithelial Shedding of the Inferior Turbinate in Perennial Allergic and Nonallergic Rhinitis
 ORIGINAL ARTICLE Epithelial Shedding of the Inferior Turbinate in Perennial Allergic and Nonallergic Rhinitis A Riddle to Solve Gilead Berger, MD; Joelle Bernheim, MD; Dov Ophir, MD Objective: To examine
ORIGINAL ARTICLE Epithelial Shedding of the Inferior Turbinate in Perennial Allergic and Nonallergic Rhinitis A Riddle to Solve Gilead Berger, MD; Joelle Bernheim, MD; Dov Ophir, MD Objective: To examine
PRINCIPAL MEDICATION OPTIONS FOR RHINITIS
 SEE INDICATED SUMMARY STATEMENT (SS#) DISCUSSION FOR SUPPORTING DATA ALLERGIC RHINITIS (AR): SEASONAL (SAR) AND PERENNIAL (PAR) MONOTHERAPY ORAL Antihistamines, oral (H1 receptor antagonists) (SS# 61-64)
SEE INDICATED SUMMARY STATEMENT (SS#) DISCUSSION FOR SUPPORTING DATA ALLERGIC RHINITIS (AR): SEASONAL (SAR) AND PERENNIAL (PAR) MONOTHERAPY ORAL Antihistamines, oral (H1 receptor antagonists) (SS# 61-64)
Observational study of tympanic membrane changes in allergic rhinitis
 International Journal of Research in Medical Sciences Katiyar VMH et al. Int J Res Med Sci. 2016 Sep;4(9):3977-3981 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162918
International Journal of Research in Medical Sciences Katiyar VMH et al. Int J Res Med Sci. 2016 Sep;4(9):3977-3981 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162918
Allergic rhinitis is defined as a symptomatic disorder
 Efficacy of mometasone furoate and fluticasone furoate on persistent allergic rhinoconjunctivitis W. Hamizan Aneeza, M.S., Salina Husain, M.S., Roslenda Abdul Rahman, M.S., Dexter Van Dort, M.B.B.S., Asma
Efficacy of mometasone furoate and fluticasone furoate on persistent allergic rhinoconjunctivitis W. Hamizan Aneeza, M.S., Salina Husain, M.S., Roslenda Abdul Rahman, M.S., Dexter Van Dort, M.B.B.S., Asma
New Medicine Report (Adopted by the CCG until review and further
 New Medicine Report (Adopted by the CCG until review and further GRASS ALLERGEN TREATMENT notice) Document Status Decision following Suffolk D&TC meeting Traffic Light Decision Red for 2007 with review
New Medicine Report (Adopted by the CCG until review and further GRASS ALLERGEN TREATMENT notice) Document Status Decision following Suffolk D&TC meeting Traffic Light Decision Red for 2007 with review
An Innovative Treatment Option for Patients with Recurrent Nasal Polyps
 An Innovative Treatment Option for Patients with Recurrent Nasal Polyps Burden of illness and management of Chronic Sinusitis with Nasal Polyps Continuum of care and polyp recurrence Clinical and health
An Innovative Treatment Option for Patients with Recurrent Nasal Polyps Burden of illness and management of Chronic Sinusitis with Nasal Polyps Continuum of care and polyp recurrence Clinical and health
Annex II. Scientific conclusions
 Annex II Scientific conclusions 5 Scientific conclusions Beclometasone dipropionate (BDP) is a glucocorticoid and a prodrug of the active metabolite, beclometasone-17-monopropionate. Beclometasone dipropionate
Annex II Scientific conclusions 5 Scientific conclusions Beclometasone dipropionate (BDP) is a glucocorticoid and a prodrug of the active metabolite, beclometasone-17-monopropionate. Beclometasone dipropionate
Drug Use Criteria: Leukotriene Receptor Antagonists
 Texas Vendor Drug Program Drug Use Criteria: Leukotriene Receptor Antagonists Publication History Developed February 2007. Revised March 2016; June 2014; October 2012; November 2010; October 2010; September
Texas Vendor Drug Program Drug Use Criteria: Leukotriene Receptor Antagonists Publication History Developed February 2007. Revised March 2016; June 2014; October 2012; November 2010; October 2010; September
Allergic Disorders. Allergic Disorders. IgE-dependent Release of Inflammatory Mediators. TH1/TH2 Paradigm
 Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Allergic Disorders. Allergic Disorders. IgE-dependent Release of Inflammatory Mediators. TH1/TH2 Paradigm
 Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Light and electron microscopical studies of focal glomerular sclerosis
 J. clin. Path., 1971, 24, 846-850 Light and electron microscopical studies of focal glomerular sclerosis A. H. NAGI, F. ALEXANDER, AND R. LANNIGAN From the Department of Pathology, Queen's University of
J. clin. Path., 1971, 24, 846-850 Light and electron microscopical studies of focal glomerular sclerosis A. H. NAGI, F. ALEXANDER, AND R. LANNIGAN From the Department of Pathology, Queen's University of
Efficacy of Levocetirizine Compared with Montelukast for the Treatment of Allergic Rhinitis
 Human Journals Research Article July 2018 Vol.:10, Issue:1 All rights are reserved by Manju K Mathew et al. Efficacy of Levocetirizine Compared with Montelukast for the Treatment of Allergic Rhinitis Keywords:
Human Journals Research Article July 2018 Vol.:10, Issue:1 All rights are reserved by Manju K Mathew et al. Efficacy of Levocetirizine Compared with Montelukast for the Treatment of Allergic Rhinitis Keywords:
NASONEX Aqueous Nasal Spray Mometasone Furoate. Schering-Plough
 NASONEX Aqueous Nasal Spray Mometasone Furoate Schering-Plough COMPOSITION NASONEX Aqueous Nasal Spray is a metered-dose, manual pump spray unit containing a suspension of mometasone furoate. Each metered-dose
NASONEX Aqueous Nasal Spray Mometasone Furoate Schering-Plough COMPOSITION NASONEX Aqueous Nasal Spray is a metered-dose, manual pump spray unit containing a suspension of mometasone furoate. Each metered-dose
Pharmacologic Treatment of Atopic Dermatitis
 J KMA Pharmacotherapeutics Pharmacologic Treatment of Atopic Dermatitis Chun Wook Park, MD Department of Dermatology, Hallym University College of Medicine E mail : dermap@paran.com J Korean Med Assoc
J KMA Pharmacotherapeutics Pharmacologic Treatment of Atopic Dermatitis Chun Wook Park, MD Department of Dermatology, Hallym University College of Medicine E mail : dermap@paran.com J Korean Med Assoc
Study No.: SAM40012 Title: A multicentre, randomised, double-blind, double-dummy, parallel group comparison of three treatments : 1)
 Study No.: SAM40012 Title: A multicentre, randomised, double-blind, double-dummy, parallel group comparison of three treatments : 1) salmeterol/fluticasone propionate () (mcg strength) bd via DISKUS/ACCUHALER
Study No.: SAM40012 Title: A multicentre, randomised, double-blind, double-dummy, parallel group comparison of three treatments : 1) salmeterol/fluticasone propionate () (mcg strength) bd via DISKUS/ACCUHALER
How immunology informs the design of immunotherapeutics.
 How immunology informs the design of immunotherapeutics. Stephen R Durham Allergy and Clinical Immunology, Royal Brompton Hospital and Imperial College London WAO Cancun Mon Dec 5 th 2011 How immunology
How immunology informs the design of immunotherapeutics. Stephen R Durham Allergy and Clinical Immunology, Royal Brompton Hospital and Imperial College London WAO Cancun Mon Dec 5 th 2011 How immunology
Dr. Heba Kalbouneh. Dr. Heba Kalbouneh. Dr. Heba Kalbouneh
 Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Basement membrane: What is the basement membrane? - It is a layer of ECM separating the epithelial cells from the underlying connective tissue Basement
Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Basement membrane: What is the basement membrane? - It is a layer of ECM separating the epithelial cells from the underlying connective tissue Basement
Allergies and Asthma 5/21/2013. Objectives. Allergic Rhinitis (AR): Risk Factor for ASTHMA. Rhinitis and Asthma
 Allergies and Asthma Presented By: Dr. Fadwa Gillanders, Pharm.D Clinical Pharmacy Specialist May 2013 Objectives Understand the relationship between asthma and allergic rhinitis Understand what is going
Allergies and Asthma Presented By: Dr. Fadwa Gillanders, Pharm.D Clinical Pharmacy Specialist May 2013 Objectives Understand the relationship between asthma and allergic rhinitis Understand what is going
Coverage Criteria: Express Scripts, Inc. monograph dated 03/03/2010
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Xolair (omalizumab) Commercial HMO/PPO/CDHP HMO/PPO/CDHP: Rx
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Xolair (omalizumab) Commercial HMO/PPO/CDHP HMO/PPO/CDHP: Rx
Allergic Rhinitis: When to Refer to an Allergist
 Allergic Rhinitis: When to Refer to an Allergist Kirsten Kloepfer, MD, MS Assistant Professor of Pediatrics Section of Pulmonary, Allergy and Sleep Medicine Disclosures NIH K23 American Academy of Allergy,
Allergic Rhinitis: When to Refer to an Allergist Kirsten Kloepfer, MD, MS Assistant Professor of Pediatrics Section of Pulmonary, Allergy and Sleep Medicine Disclosures NIH K23 American Academy of Allergy,
The Effect of Beclomethasone Nasal Spray on the Size of Adenoid and its Related Obstructive Symptoms in Children with Adenoid Hypertrophy.
 In the name of God Shiraz E-Medical Journal Vol. 10, No. 1, January 2009 http://semj.sums.ac.ir/vol10/jan2009/86051.htm The Effect of Beclomethasone Nasal Spray on the Size of Adenoid and its Related Obstructive
In the name of God Shiraz E-Medical Journal Vol. 10, No. 1, January 2009 http://semj.sums.ac.ir/vol10/jan2009/86051.htm The Effect of Beclomethasone Nasal Spray on the Size of Adenoid and its Related Obstructive
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Grastek) Reference Number: CP.PMN.84 Effective Date: 11.16.16 Last Review Date: 08.18 Line of Business: Commercial, HIM, Medicaid Revision Log See Important Reminder at the end of this
Clinical Policy: (Grastek) Reference Number: CP.PMN.84 Effective Date: 11.16.16 Last Review Date: 08.18 Line of Business: Commercial, HIM, Medicaid Revision Log See Important Reminder at the end of this
Systemic availability of budesonide after nasal administration of three different formulations: pressurized aerosol, aqueous pump spray, and powder
 Systemic availability of budesonide after nasal administration of three different formulations: pressurized aerosol, aqueous pump spray, and powder L. Thorsson, 1,2 O. Borgå 2 & S. Edsbäcker 1,2 1 Department
Systemic availability of budesonide after nasal administration of three different formulations: pressurized aerosol, aqueous pump spray, and powder L. Thorsson, 1,2 O. Borgå 2 & S. Edsbäcker 1,2 1 Department
Teet Pullerits, MD, PhD, a Lea Praks, MD, PhD, b Vahur Ristioja, MD, c and Jan Lötvall, MD, PhD a Gothenburg, Sweden, and Tartu, Estonia
 Comparison of a nasal glucocorticoid, antileukotriene, and a combination of antileukotriene and antihistamine in the treatment of seasonal allergic rhinitis Teet Pullerits, MD, PhD, a Lea Praks, MD, PhD,
Comparison of a nasal glucocorticoid, antileukotriene, and a combination of antileukotriene and antihistamine in the treatment of seasonal allergic rhinitis Teet Pullerits, MD, PhD, a Lea Praks, MD, PhD,
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
While allergic rhinitis is merely a nuisance to
 APPLIED EVIDENCE Evaluation and treatment of the patient with allergic rhinitis STEPHEN J. CONNER, MD Ft. Gordon, Georgia KEY POINTS FOR CLINICIANS Physical clues to allergic rhinitis include boggy, pale,
APPLIED EVIDENCE Evaluation and treatment of the patient with allergic rhinitis STEPHEN J. CONNER, MD Ft. Gordon, Georgia KEY POINTS FOR CLINICIANS Physical clues to allergic rhinitis include boggy, pale,
How Effective is Acupuncture in Treating Persistent Allergic Rhinitis in Children and Adults?
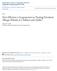 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 How Effective is Acupuncture in Treating
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 How Effective is Acupuncture in Treating
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Sweet Vernal, Orchard, Perennial Rye, Timothy, and Kentucky (Oralair) Reference Number: CP.PMN.85 Effective Date: 11.16.16 Last Review Date: 08.18 Line of Business: Commercial, Medicaid
Clinical Policy: Sweet Vernal, Orchard, Perennial Rye, Timothy, and Kentucky (Oralair) Reference Number: CP.PMN.85 Effective Date: 11.16.16 Last Review Date: 08.18 Line of Business: Commercial, Medicaid
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
