Since its introduction into anesthesia practice in
|
|
|
- William Barber
- 5 years ago
- Views:
Transcription
1 A Prospective, Randomized Comparison of Cobra Perilaryngeal Airway and Laryngeal Mask Airway Unique in Pediatric Patients Peter Szmuk, MD* Oscar Ghelber, MD Maria Matuszczak, MD Marry F. Rabb, MD Tiberiu Ezri, MD Daniel I. Sessler, MD BACKGROUND: The Cobra Perilaryngeal Airway (PLA) provides better sealing pressure than the Laryngeal Mask Airway Unique (LMAU) during positive-pressure ventilation in adults. We compared the performance of the CobraPLA and LMAU in infants and children. METHODS: Two-hundred pediatric patients were randomly assigned to a CobraPLA or an Laryngeal Mask Airway (LMA). We measured airway sealing at cuff inflation pressures of 40 and 60 cm H 2 O; ease and time of insertion; device stability; efficacy of ventilation; number of insertion attempts; incidence of postoperative sore throat, dysphonia, laryngospasm, bronchospasm, and gastric gas insufflation. Steady-state end-tidal CO2 was measured at the head of the CobraPLA and at the Y-piece piece of the anesthetic circuit. For the major outcomes, the airway groups were subdivided post hoc into small and large CobraPLA and small and large LMA subgroups. Results are presented as means sds; P 0.05 was considered statistically significant. RESULTS: Airway sealing pressure with the cuff inflated to 60 cm H 2 O in the large CobraPLA subgroup (22 7cmH 2 O) was significantly more than that of the small CobraPLA subgroup (18 5cmH 2 O) and large LMA subgroup (16 5cmH 2 O; P 0.001). The CobraPLA was more stable than the LMA (same anatomic fit score before and after surgery) and produced less gastric insufflation. Head CobraPLA end-tidal CO2 values were mm Hg more than those of the Y piece of the circle circuit. CONCLUSIONS: The CobraPLA airway performed as well as the LMAU during anesthesia in pediatric patients for a large range of outcomes and was superior for some. (Anesth Analg 2008;107: ) Since its introduction into anesthesia practice in 1988, the Laryngeal Mask Airway (LMA, The Laryngeal Mask Company Limited, Henley-on-Thames, From the *Department of Anesthesiology, University of Texas Southwestern Medical School and Children s Medical Center at Dallas, Texas; Department of Anesthesiology, University of Texas Medical School at Houston, Texas; Department of Anesthesia, Wolfson Medical Center, Holon, Affiliated to Tel Aviv University, Israel; and Department of Outcomes Research, The Cleveland Clinic, Ohio; Member Outcomes Research Consortium. Accepted for publication June 18, Supported by Engineered Medical Systems, Indianapolis, IN Grant HSC-MS Dr. Sessler s time was supported by the Joseph Drown Foundation (Los Angeles, CA). The sponsor was not involved in study design, data collection or analysis, nor manuscript preparation. Presented, in part, at the American Society of Anesthesiologists Meeting, Chicago, IL, October 14 18, 2006; American Society of Anesthesiologists Meeting, New Orleans, LA/Atlanta, GA, 2005; and IARS 79th Clinical and Scientific Congress, Honolulu, HI, March 11 15, Address correspondence and reprint requests to Peter Szmuk, MD, Department of Anesthesiology, University of Texas Southwestern Medical School and Children s Medical Center at Dallas, 1935, B3304, Motor St., Dallas, TX Address to peter.szmuk@utsouthwestern.edu. Copyright 2008 International Anesthesia Research Society DOI: /ane.0b013e UK) has been used in 150 million cases worldwide and has proved to be safe and effective in both adult and pediatric patients. 1 Nevertheless, more than one insertion attempt is required in 5% to 10% of all cases 2 ; furthermore, the LMA does not provide a reliable airtight seal around the larynx, and pressures of 15 to 20 cm H 2 O usually cause gas leakage. 3 Consequently, the device often functions poorly during positivepressure ventilation. Despite these minor problems, the LMA is currently used in many surgical patients, including those undergoing nonconventional surgeries (laparotomies or laparoscopies) 2,4 and is part of the ASA difficult airway algorithm. 5 The Cobra Perilaryngeal Airway (CobraPLA)(Engineered Medical Systems, Indianapolis, IN) was introduced into clinical practice in 2003 as a disposable extraglottic airway device. In adults, insertion time and performance characteristics were similar to the LMA, while airway-sealing pressures were greater: 23 6cmH 2 Ovs18 5cmH 2 O. 6 Several reports have shown the usefulness of the CobraPLA in pediatric patients 7 10 ; however, the device has yet to be fully evaluated in infants and Vol. 107, No. 5, November
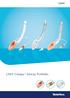
2 Figure 1. CobraPLA with end tidal CO 2 sampling site. CobraPLA features: 15 mm connector (1); CobraPLA head (2); Grill (3); Flexible tip (4); CobraPLA circular cuff (5). CobraPLA with CO 2 sampling prototype: end tidal CO 2 sampling tube (6) which opens at the head of the device (7). children. Our goal was thus to evaluate the use of CobraPLA in routine clinical practice in pediatric patients and compare its performance with the Laryngeal Mask Airway Unique (LMAU). Our primary outcome was the airway sealing pressure; secondary outcomes were ease and time for insertion, position and stability of the device, number of insertion attempts, incidence of gastric insufflation and of postoperative complications. Furthermore, in a subset of patients, we used a specially designed CobraPLA with a gas sampling site near the head of the device to test the hypothesis that the end-tidal CO 2 (ETco 2 ) and end-tidal sevoflurane (ET sevo ) concentrations measured at the head of the CobraPLA are greater (and presumably more accurate) than those measured at the Y- piece of the anesthetic circuit. METHODS With approval of the IRB at the University of Texas Medical School at Houston and written parental consent, 200 pediatric patients, ASA physical status I-II, 0 to 12-yr-old were enrolled in this prospective, randomized, single-blind study. The patients were scheduled for elective orthopedic and urological procedures with an estimated duration of anesthesia under 2 h. Patients with known gastrointestinal reflux, sore throat or upper respiratory airway infection, and with known or suspected difficult airways were excluded from the study. The CobraPLA comprises a breathing tube with a widened distal end. When the cuff of the CobraPLA is inflated it seals the distal end from the upper airway, thereby allowing positive-pressure ventilation. The distal Cobra head holds both soft tissues and the epiglottis away from the airway opening, thus allowing unimpeded ventilation. (Fig. 1) The CobraPLA is manufactured in eight sizes; four of them (0.5 2) are suitable for pediatric patients. Anesthetic Protocol All patients older than 10 mo were premedicated with oral midazolam, 0.5 mg/kg up to maximum of 15 mg. General anesthesia was induced with sevoflurane in a mixture of 30/70% O 2 /N 2 O through a facemask. An IV catheter was inserted and 1 mg/kg propofol and 1 g/kg fentanyl were administered. Both devices were lubricated with a water-based lubricant. Randomization to one of the airway devices (including anatomical fit and ET co2 subgroups) was based on computer-generated codes maintained in sequentially numbered opaque envelopes which were opened just before device insertion. Insertion of the device was attempted when the eyelash reflex had disappeared and the jaw was relaxed at least 60 sec after propofol administration. The LMAU was inserted with a partially inflated cuff. No muscle relaxants were administered before airway insertion. LMAU and CobraPLA sizes were selected based on manufacturer s recommendations, modified to avoid overlap of the weight groups. LMAU: Size 1 ( 5 kg), Size 1.5 (6 10 kg); Size 2 (11 20 kg), and Size 2.5 (21 30 kg). CobraPLA: Size 1/2 ( kg); Size 1 ( kg); Size 1.5 (16 30 kg); and Size 2 (31 60 kg). All the investigators had years of experience with use of the LMAU and at least 20 insertions with the CobraPLA. Failure to properly position an airway was defined by any one of the following: 1) inability to obtain an ET co2 waveform; 2) presence of an audible air leak at 10 cm H 2 O-peak inspiratory pressure; 3) an expired tidal volume 4 ml/kg; 4) signs of airway obstruction (peak airway pressure 25 cm H 2 O with low expired tidal volumes); or, 5) an Spo 2 93% with an Fio 2 of 100%. If insertion failed, the following algorithm was pursued: (a) two attempts with the randomly assigned airway, (b) insertion of a smaller size study device; (c) a single insertion attempt with the alternative airway device; (d) 0.6 mg/kg IV rocuronium and tracheal intubation. The attending anesthesiologists were free to intubate the patient s trachea at any time if clinically indicated. Anesthesia was maintained with 60/40% N 2 O/O 2, fentanyl ( 1 g kg 1 h 1 ), and sevoflurane was needed to maintain the mean arterial blood pressure within 20% of the preinduction value. In longer surgeries ( 45 min), the patients lungs were mechanically ventilated with a tidal volume of 8 ml/kg at a rate sufficient to maintain ET co2 near 40 mm Hg and then allowed to resume spontaneous ventilation towards the end of the procedure. If the delivered 8 ml/kg tidal volume produced airway pressure in excess of 20 cm H 2 O, tidal volume was reduced as necessary to maintain lower peak airway pressures. Fresh gas flow was maintained at a constant rate of 3 L/min. Airway device insertion depth was defined by the distance from the tip of the device to a mark made at the level of the incisors after insertion. After device insertion, the patient s head was maintained in neutral 1524 CobraPLA in Pediatric Patients ANESTHESIA & ANALGESIA
3 position by rolls positioned bilaterally. All devices were examined upon removal for gross blood staining. Perioperative complications such as laryngospasm and bronchospasm were recorded both intra and postoperatively. Measurements Each device was evaluated by assessing the following variables: positioning, gas leak at 60 and 40 cm H 2 O cuff pressures, anatomical fit, gastric insufflation, and the degree of pharyngeal irritation. Standard anesthetic safety data were also recorded, including arterial blood pressure, heart rate, oxyhemoglobin saturation, peak airway pressure, and total amount of fentanyl administered. Time for successful airway insertion was measured by an independent observer beginning when the tip of the device was at the level of the incisors and ending after all the following were completed: the cuff was inflated, the breathing circuit was connected to the airway, an ETco 2 trace was detected, a tidal volume of more than 4 ml/kg body weight was measured, and no air leak was detected at a peak inspiratory positive airway pressure ventilation of 15 cm H 2 O. The number of attempts, the initial airway size and the size ultimately used were recorded. Once the device was optimally positioned, it was taped and its position was not altered unless clinically necessary. Ease of Insertion Ease of airway insertion was evaluated qualitatively, using the following scale: 1) smooth insertion without any need for adjustment; 2) need for at least one adjustment maneuver, and 3) more than one adjustment maneuver required to obtain adequate positioning. Airway sealing pressure was measured by closing the expiratory valve of the circle system at 3 L/min gas flow and recording the airway pressure at which the dial on the aneroid manometer reached equilibrium. 11 Assessment of airway sealing pressure was initially performed with the device s cuff inflated to 60 cm H 2 O followed immediately by measurement at 40 cm H 2 O. Subsequently, the cuff was fully deflated, an orogastric tube (OGT) was passed into the stomach to remove any air that entered during the assessment period. The OGT was then removed and the device s cuff reinflated, monitored with a manometer (Mallinckrodt) and maintained at 40 cm H 2 O throughout the procedure. In a random subgroup of patients from both groups, a flexible fiberoptic bronchoscope (Olympus BFP 30, O.D. 5.0 mm, Tokyo, Japan) was inserted through the device via a connector with a self-sealing diaphragm up to the mask aperture bars both before and at the end of the surgery. The airway position was scored as follows 12 :4 only vocal cords visible; 3 vocal cords plus posterior epiglottis visible; 2 vocal cords plus anterior epiglottis visible; 1 vocal cords not fiberoptically visible. At the end of surgery with the patient deeply anesthetized, the cuff of the device was deflated, an OGT was inserted under direct vision using a tong blade depressor and gas was aspirated from the stomach using a 60-mL syringe. 13 The amount of gas aspirated was recorded for each device. The position of the OGT was confirmed by the presence of gastric content at aspiration. If nothing was aspirated, 2 ml of air was injected while listening over the epigastrium to confirm the tube s position and clear any blockage. These 2 ml of air were then aspirated and omitted from calculations. Difficulties with the OGT insertion, if any, were noted. The oral cavity and part of the pharynx were inspected for blood or trauma before and after the placement of the OGT. One and 24 h postoperatively, the patient s parents (blinded to group assignment) were asked to rate the presence of dysphonia (Yes/No). Sore throat was assessed as present or absent (when age and willingness allowed the patients to respond) 1 h postoperatively. A specially designed CobraPLA prototype with an ETco 2 sampling site (Fig. 1) that opened at the head of the device was used in a subset of patients. Once steady-state was reached (10 15 min postinduction) both head and Y-piece ET co2 and ET sevo were recorded every 15 min. Statistical Analysis In adults, 6 the airway sealing pressures for CobraPLA and LMAU are reported to be 23 6 and 18 5cmH 2 O, respectively. In order to have 90% power to detect a difference in airway sealing pressures of 5 cm H 2 O between the two devices, we needed to study 25 patients per group for each of device size. Consequently, we recruited 200 patients (100 patients/ device with 25/size). Morphometric and anesthetic data were analyzed using Student s t-test. The numbers of failed device insertions were compared with a Fisher s exact test. For the major outcomes, the patients in the two groups were subdivided post hoc into four groups: small CobraPLA (CobraPLA sizes 0.5 and 1), small LMAU (LMAU sizes 1 and 1.5), large Cobra PLA (CobraPLA sizes 1.5 and 2), and large LMAU (LMAU sizes 2 and 2.5). Analysis of variance was used for continuous measurements and 2 tests for dichotomous values. Differences in anatomical fit between the CobraPLA group and LMAU group immediately after induction of anesthesia and before emergence were analyzed using Wilcoxon Signed Rank Test. The ET (co 2 and sevo) at head and Y-piece were compared with linear regression and Bland Altman statistics. Results are presented as means sds; P 0.05 was considered significant. Vol. 107, No. 5, November International Anesthesia Research Society 1525
4 Table 1. Morphometric and Anesthetic Data CobraPLA (n 100) LMA (n 100) P Age (mo) Weight (kg) Gender (female/male) 20/80 24/ Insertion time (sec) Upper incisor distance (cm) Overall average By device size 2.5 N/A N/A Duration of ventilation (min) Duration of anesthesia (min) Number of insertion attempts (1/2/3) 95/4/1 96/3/ Ease of insertion (1/2/3) a 92/6/2 86/10/ Number of failed devices (use of ETT) b Number of patients requiring rocuronium b Data presented as means SD s or numbers. a Ease of insertion graded as 1 smooth insertion without any need for adjustment; 2 need for at least one adjustment maneuver; 3 more than one adjustment maneuver required to obtain optimal positioning. b Fisher s Exact Test; ETT endotracheal tube. RESULTS There were no significant differences with regard to morphometric or anesthetic data (Table 1), except that the surgery and, hence anesthesia, lasted longer in the patients who received the CobraPLA: vs min, P First-attempt device insertion was successful in 95% of patients with a CobraPLA, and in 96% with an LMAU. However, the cumulative insertion success rate increased to 99% for both devices after the second attempt. Four patients in the CobraPLA group and three in the LMAU group required two attempts at insertion. One patient in each group required three attempts at insertion. Major Outcomes There were no significant differences between the CobraPLA and LMAU groups in the time and ease of insertion or the number of attempts required for successful insertion (Table 1). However, insertion times were significantly shorter with the smaller airway devices in both CobraPLA and LMAU (Table 2). Anatomical fit was assessed in 33 CobraPLA patients and 30 LMAU patients. The fiberoptic view was significantly better (scores 3 4) in the CobraPLA group than in the LMAU group both immediately after induction and before emergence (P 0.001). The overall fit was judged worse before emergence than after induction in the LMAU subgroups (scores 1 2) as compared with the CobraPLA subgroups in which there was no change (Table 2). This suggests that CobraPLA was more stable in the airway than the LMAU. The fiberoptic examination revealed no epiglottic down-folding or laryngeal view obstruction in the CobraPLA group, whereas in the LMAU group epiglottic down-folding and laryngeal view obstruction occurred in two patients after induction and in six patients before emergence. The airway sealing pressure at a cuff inflation pressure of 40 cm H 2 O in the large CobraPLA subgroup (18 6cmH 2 O) was more than that of the small PLA (15 4cmH 2 O) and the large LMAU subgroups (15 5cmH 2 O, P 0.003). The airway sealing at a cuff inflation pressure of 60 cm H 2 Ointhe large CobraPLA subgroup (22 7cmH 2 O) was also significantly more than that of the small PLA subgroup (18 5cmH 2 O) and the large LMAU subgroup (16 5cmH 2 O; P 0.001) (Fig. 2). In contrast, at inflation pressures of both 40 and 60 cm H 2 O, the airway sealing pressures were similar in the small and large LMAU groups. The peak airway pressure at 20 min was significantly smaller in the large LMAU subgroup than in any of the other three subgroups (Table 2). The incidences of complications (laryngospasm, bronchospasm, blood staining on the device, sore throat, and dysphagia) were similar in the four subgroups. The volume of stomach gas aspirated was significantly smaller (P 0.001) in patients having a CobraPLA (0.6 ml/kg) than in those given a LMAU (1.3 ml/kg). In addition, children in the large LMAU subgroup had a larger stomach gas volume than did children in the other subgroups (Table 2). There was neither difficulty nor apparent trauma with the OGT placement. In two patients in each device group (one each with the CobraPLA 1 and 1.5, LMAU 1 and 1.5) placement of the device failed due to either laryngospasm or bronchospasm. Three of the patients tracheas were intubated after the second attempt at placing the extraglottic device. In one case, the patient s trachea was intubated only after three failed insertion attempts with the assigned device (LMAU) and an additional failed attempt with a CobraPLA. None of these four patients had any additional complications CobraPLA in Pediatric Patients ANESTHESIA & ANALGESIA
5 Table 2. Major Outcomes CobraPLA subgroups LMA subgroups Small 0.5 and 1 (n 50) Large 1.5 and 2 (n 50) Small 1 and 1.5 (n 50) Large 2 and 2.5 (n 50) P Insertion of device Insertion time (sec) 16 6 a 20 7 b 15 4 a 19 6 b Ease of insertion (1/2/3) d 48/2/0 47/2/1 47/2/1 49/1/ Attempts (1/2/3) 48/2/0 49/1/0 47/2/1 49/1/ Anatomical fit after 0/1/13/3 a 1/1/6/9 a 6/7/5/0 b 2/5/6/0 b induction (1/2/3/4) e Anatomical fit before 0/2/11/4 a 1/1/6/9 a 8/9/0/1 b 6/6/0/1 b emergence (1/2/3/4) e Maintenance of anesthesia Airway sealing pressure 15 4 a 18 6 b 16 5 ab 15 5 a at 40 cm H 2 0 Airway sealing pressure 18 5 a 22 7 b 18 5 a 16 5 a at 60 cm H 2 0 Peak airway pressure at 17 5 a 17 5 a 16 3 ab 14 4 b min (cm H 2 0) Removal of airway device and complications Laryngospasm (no/yes) 48/2 49/0 48/2 46/ Bronchospasm (no/yes) 49/0 49/0 48/1 47/ Blood staining (no/yes) 47/3 44/6 42/8 39/ Sore throat (no/yes) 47/3 a 38/12 b 47/3 a 40/10 b Dysphonia (no/yes) 42/8 44/6 41/9 41/ Gastric gas volume (ml) 8 5 a ab 15 9 b c Data presented as means SD s or counts. For post hoc tests, the letters a, b, and c are used to designate which groups are similar and which are different. Groups that share the same letter are considered to NOT be statistically different from each other. d Ease of insertion graded as 1 smooth insertion without any need for adjustment; 2 need for at least one adjustment maneuver; 3 more than one adjustment maneuver required to obtain optimal positioning. e For the anatomical fit 30 LMA and 33 CobraPLA patients were assessed. Scoring: 1 vocal cords not fiberoptically visible; 2 vocal cords plus anterior epiglottis visible; 3 vocal cords plus posterior epiglottis visible; 4 only vocal cords visible. Figure 2. Airway sealing pressures for CobraPLA and LMA Unique subgroups at two cuff inflation pressures. The airway sealing pressure in the large CobraPLA subgroup (Sizes 1.5 and 2) was significantly greater than that in the small CobraPLA subgroup (Sizes 0.5 and 1) and large LMA Unique subgroup (Sizes 2 and 2.5) at inflation pressures of 40 and 60 cm H 2 O. *P Figure 3. Regression line of ETco 2 at the CobraPLA head versus standard Y-piece sampling sites in mm Hg. Ypiece value 0.83 ( Head value) 2.6, r Ventilation Data for ET co2 and ET sevo were collected from 44 patients with all sizes of the CobraPLA used in the study (size 0.5 n 10; size 1 n 11; size 1.5 n 13; size 2 n 10). Measurements in an additional six patients were abandoned due to sample line obstruction. The mean ( sd) measurement times were 48 17, 45 12, 38 14, and min for CobraPLA sizes 0.5, 1, 1.5, and 2, respectively. Linear regression and the Bland Altman plot for ETco 2 are presented in Figures 3 and 4. Linear regression between the measurement sites for ET co2 indicated that the values at the Y-piece site were more than that at the head site (Proximal measurement Vol. 107, No. 5, November International Anesthesia Research Society 1527
6 Figure 4. The difference between ET co2 at the CobraPLA head and measurements at the Y-piece of the circle system (bias) versus the average measurement in mm Hg. Figure 5. Bland Altman plot for ET CO2 differences as a function of patient s weight. 0.8 [head measurement] 3, r 0.75). The head values were 6.4 6cmH 2 O more than those of the Y-piece site. Linear regression between weight and the ET CO2 differences at the CobraPLA head and the Y-piece peace are presented in Figure 5. We found that substantial differences between ET CO2 concentrations at the Cobra PLA s head and the circuit Y-piece occurred in children up to at least 30 kg. Linear regression indicated that the sevoflurane concentrations at the Y-piece and head measurement sites were essentially equal (Y-piece measurement 0.9 [head measurement] 0.2, r 0.88). The mean bias was DISCUSSION Our results show that the CobraPLA airway performs as well as the LMAU Classic during anesthesia in pediatric patients for a large range of outcomes and out-performed the LMAU for others. We could only partially confirm previous reports in adults that the CobraPLA provides superior sealing pressures to LMAU during controlled ventilation. 6,14 Overall, there were no significant differences between the sealing pressures in the two airway groups at 40 or 60 cm H 2 O; however, subgroup analysis revealed that the sealing pressures in the large CobraPLA subgroups (1.5 and 2) were more than those of the small CobraPLA subgroup (0.5 and 1) and the large LMAU subgroup (2 and 2.5) at both inflation pressures. The lack of an increased sealing pressure in pediatric patients receiving the small CobraPLA sizes might have been the result of a difference in the anatomical shape of the pharynx in infants versus older children and adults. In fact, Arens et al. 15 assessed the airway dimensions of children aged 1 to 11 yr by magnetic resonance imaging and found a linear increase in the upper airway dimensions with age. They concluded that soft tissues surrounding the upper airway, including tonsils and adenoids, grow proportionally to the skeletal structures. Sealing pressures were measured at two different cuff inflation pressures: 40 and 60 cm H 2 O. In adults 70 cm H 2 O (range, 51 92) intracuff pressure in a cuffed oropharyngeal airway generated a mucosal pressure of 56 cm H 2 O (range, 22 87). With increased intracuff pressure, mucosal blood flow decreases progressively until it is abolished at mucosal pressures more than 80 cm H 2 O. 16 The 60 cm H 2 O inflation pressure is, however, higher than the mean arterial blood pressure of children and infants, and thus we selected a second lower cuff inflation pressure below this range (40 cm H 2 O). No data are available on the optimal cuff pressure to preserve pharyngeal mucosal blood flow in infants and children. We assumed that if sealing were effective at 40 cm H 2 O the side effects of higher inflation pressures (e.g., sore throat) would be minimized. The sealing pressures at 40 and 60 cm H 2 O cuff inflation were similar. Age is often reported as a risk factor for complications during pediatric anesthesia. 17 In a survey of 9289 anesthetics in patients younger than 62 mo, the incidence of airway complications were related to age. 18 Our study was not powered to confirm these results, especially as complications other than sore throat and dysphonia were uncommon. LMAU use in infants has been limited due to the relatively frequent incidence of airway complications associated with the size 1 LMAU One study found a 22% incidence of airway complications when the LMAU 1 was used. 20 Bagshaw 22 reported a complication rate of 42% with the use of a size 1.5 LMAU with complications more common in younger patients. Positioning the size 1 LMAU was also found to be difficult and resulted in respiratory complications in 30% of the patients. 17 In 6% of patients, the device functioned inadequately with insertion followed by delayed airway obstruction in 24% of children. 16 Others report similar difficulties with small sizes of LMAUs. 23 These problems resulted from distortion of the airway with epiglottic down-folding that might have contributed to the partial upper airway obstruction. 17 Once in place, accidental dislodgement of the LMAU can occur, but this is considered a minor complication if the patient s airway is accessible. 23 Distortion of the LMAU by epiglottic down-folding occurs in as many as 90% of children after the insertion of sizes 2 and 2.5 LMAUs; this might contribute to 1528 CobraPLA in Pediatric Patients ANESTHESIA & ANALGESIA
7 partial upper airway obstruction. 17,24 Usually, this does not affect the device s functionality with spontaneous breathing but it can cause difficulties with positive pressure ventilation and it may hamper intubation through an LMAU. Epiglottic folding causing partial or complete obstruction was also found in 77% of patients 10 kg and undermanaged with CobraPLA. 25 In marked contrast, we did not observe laryngeal view obstruction by the epiglottis in the CobraPLA group. In the LMAU group, however, there were two cases with epiglottis down-folding after induction and six before emergence, which indicated the tendency for the position of LMAU to shift during anesthesia. As in other studies this shift in LMAU position did not seriously affect ventilation. 17 The success rate at first and second attempts was more than 95% and 99% respectively with both airways. This contrasts with earlier reports of a 90% 26 and 86% 24 success rate for LMAU placement at first attempt with only a 97% success rate by the third attempt. The fit and sealing characteristics of CobraPLA (1.5 and 2) in mechanically ventilated children were found adequate in 90% of cases at the first attempt and 97.5% at the second attempt. 27 We found the CobraPLA to be more stable than the LMAU. The apparent stability of the CobraPLA can be attributed to its wide, flat distal head, which is rigid enough to prevent rotation of the device. The better anatomical fit of the CobraPLA becomes especially important if fiberoptic intubation through the device is needed. 8,10 Distension of the stomach can lead to pulmonary embarrassment by splinting the diaphragm and could predispose reflux and pulmonary aspiration of gastric contents. The incidence of gastroesophageal insufflation during use of the LMAU, assessed qualitatively, depends on airway pressure and is reported to range from 0% 28 to 35%. 29 In a previous study, LMAU malposition increased the chance of gastric insufflation from 3% to 19%. 30 Our CobraPLA patients had less gastric volume than those in the LMAU group which may have related to a better anatomical fit with the CobraPLA. Nitrous oxide was administered at the same concentration in all patients, and its influence on cuff pressure was limited by monitoring and maintaining cuff pressure at 40 mm Hg. Nonetheless, patients in the CobraPLA group had a slightly longer anesthesia time and less gastric distention than the LMAU group. A limitation is that we measured gastric volume by OGT aspiration. Although gastric volume has been measured this way in previous studies, 23,31 the method can be inaccurate. Gastric volume can be qualitatively assessed by epigastric auscultation, since as little as 5 ml of gas entering the stomach can be detected by this method. 35 In one study, for children managed with a LMAU, the stomach gas volume measured by auscultation was reportedly lower ( ml/kg) 26 than in our patients (1.3 ml/kg). This difference may have been that we aspirated the stomach after we performed the airway sealing measurements and then removed the OGT; at the end of anesthesia we reinserted the OGT. Our measured gas volume thus reflected the gas volume leaked into the stomach during surgery. In contrast, an OGT left in situ, as in previous studies, may allow some air to escape around it. Previous work suggests that the small tidal volumes in infants make ETco 2 measurements at the Y-piece piece of the circle system inaccurate compared with measurements at the end of an endotracheal tube. 36 Our results support this assertion, as values were greater (and presumably more accurate) at the head of the CobraPLA. The difference was 6.4 6mm Hg which could be clinically important. The substantial differences found between ET CO2 concentrations at the Cobra PLA s head and the circuit Y-piece in children up to 30 kg suggest that CobraPLA head gas sampling is potentially beneficial in most pediatric patients, not just infants. It remains unclear whether this difference results only from increased dead-space or if a leak around the CobraPLA may have also contributed. In summary, the CobraPLA performed as well as the LMAU Classic during anesthesia in infants and children but proved superior with regards to the anatomical fit and stability within the airway. The CobraPLA also produced less gastric insufflation. In infants, the distal site sampling of ET co2 with the CobraPLA may be more accurate than the standard measurement site at the Y-piece piece of the anesthesia circuit. ACKNOWLEDGMENTS The authors thank Gil Haugh, MS, from the University of Louisville, KY, for his assistance with the statistical analysis. REFERENCES 1. Pennant JH, White PF. The laryngeal mask airway. Its uses in anesthesiology. Anesthesiology 1993;79: Brimacombe J. Analysis of 1500 laryngeal mask uses by one anaesthetist in adults undergoing routine anaesthesia. Anaesthesia 1996;51: Maltby JR, Loken RG, Watson NC. The laryngeal mask airway: clinical appraisal in 250 patients. Can J Anaesth 1990;37: Verghese C, Brimacombe JR. Survey of laryngeal mask airway usage in 11,910 patients: safety and efficacy for conventional and nonconventional usage. Anesth Analg 1996;82: Practice guidelines for management of the difficult airway: an updated report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology 2003;98: Akça O, Wadhwa A, Sengupta P, Durrani J, Hanni K, Wenke M, Yücel Y, Lenhardt R, Doufas AG, Sessler DI. The new perilaryngeal airway (CobraPLA ) is as efficient as the laryngeal mask airway (LMAU ), but provides better airway sealing pressures. Anesth Analg 2004;99: Szmuk P, Ezri T, Akca O, Alfery DD. Use of a new supraglottic airway device the cobrapla in a difficult to intubate/difficult to ventilate scenario. Acta Anaesthesiol Scand 2005;49: Szmuk P, Ezri T, Narwani A, Alfery DD. Use of cobrapla as a conduit for fiberoptic intubation in a child with neck instability. Paediatr Anaesth 2006;16:217 8 Vol. 107, No. 5, November International Anesthesia Research Society 1529
8 9. Szmuk P, Ghelber O, Akca O, Ezri T. CobraPLA as a conduit for flexible bronchoscopy in a child under general anaesthesia. Br J Anaesth 2005;94: Szmuk P, Matuszczeak M, Carlson RF, Warters RD, Rabb MF, Ezri T. Use of cobrapla for airway management in a neonate with desbuquois syndrome. Case report and anesthetic implications. Paediatr Anaesth 2005;15: Keller C, Brimacombe JR, Keller K, Morris R. Comparison of four methods for assessing airway sealing pressure with the laryngeal mask airway in adult patients. Br J Anaesth 1999;82: Brimacombe J, Berry A. A proposed fiber-optic scoring system to standardize the assessment of laryngeal mask airway position. Anesth Analg 1993;76: Graziotti PJ. Intermittent positive pressure ventilation through a laryngeal mask airway. Is a nasogastric tube useful? Anaesthesia 1992;47: Galvin EM, van Doorn M, Blazquez J, Ubben JF, Zijlstra FJ, Klein J, Verbrugge SJ. A randomized prospective study comparing the cobra perilaryngeal airway and laryngeal mask airway-classic during controlled ventilation for gynecological laparoscopy. Anesth Analg 2007;104: Arens R, McDonough JM, Corbin AM, Hernandez ME, Maislin G, Schwab RJ, Pack AI. Linear dimensions of the upper airway structure during development: assessment by magnetic resonance imaging. Am J Respir Crit Care Med 2002;165: Brimacombe J, Keller C, Puhringer F. Pharyngeal mucosal pressure and perfusion: a fiberoptic evaluation of the posterior pharynx in anesthetized adult patients with a modified cuffed oropharyngeal airway. Anesthesiology 1999;91: Bordet F, Allaouchiche B, Lansiaux S, Combet S, Pouyau A, Taylor P, Bonnard C, Chassard D. Risk factors for airway complications during general anaesthesia in paediatric patients. Paediatr Anaesth 2002;12: Bonoli P, Grillone G, Fossa S, Franceschelli N, Lari S, Leykin Y, Nastasi M, Zanoni A. [Complications of pediatric anesthesia. Survey carried out by the study group SIAARTI for anesthesia and intensive therapy in children]. Minerva Anestesiol 1995;61: Harnett M, Kinirons B, Heffernan A, Motherway C, Casey W. Airway complications in infants: comparison of laryngeal mask airway and the facemask-oral airway. Can J Anaesth 2000;47: Lopez-Gil M, Brimacombe J, Cebrian J, Arranz J. Laryngeal mask airway in pediatric practice: a prospective study of skill acquisition by anesthesia residents. Anesthesiology 1996; 84: Mizushima A, Wardall GJ, Simpson DL. The laryngeal mask airway in infants. Anaesthesia 1992;47: Bagshaw O. The size 1.5 laryngeal mask airway (LMAU) in paediatric anaesthetic practice. Paediatr Anaesth 2002;12: Dubreuil M, Laffon M, Plaud B, Penon C, Ecoffey C. Complications and fiberoptic assessment of size 1 laryngeal mask airway. Anesth Analg 1993;76: McGinn G, Haynes SR, Morton NS. An evaluation of the laryngeal mask airway during routine paediatric anaesthesia. Paediatr Anaesth 1993;3: Polaner DM, Ahuja D, Zuk J, Pan Z. Video assessment of supraglottic airway orientation through the perilaryngeal airway in pediatric patients. Anesth Analg 2006;102: Mason DG, Bingham RM. The laryngeal mask airway in children. Anaesthesia 1990;45: Passariello M, Almenrader N, Coccetti B, Haiberger R, Pietropaoli P. Insertion characteristics, sealing pressure and fiberoptic positioning of cobrapla in children. Paediatr Anaesth 2007;17: Epstein RH, Ferouz F, Jenkins MA. Airway sealing pressures of the laryngeal mask airway in pediatric patients. J Clin Anesth 1996;8: Devitt JH, Wenstone R, Noel AG, O Donnell MP. The laryngeal mask airway and positive-pressure ventilation. Anesthesiology 1994;80: Latorre F, Eberle B, Weiler N, Mienert R, Stanek A, Goedecke R, Heinrichs W. Laryngeal mask airway position and the risk of gastric insufflation. Anesth Analg 1998;86: Selby IR, Morris P. Intermittent positive ventilation through a laryngeal mask in children: does it cause gastric dilatation? Paediatr Anaesth 1997;7: Asai T, Kawashima A, Hidaka I, Kawachi S. The laryngeal tube compared with the laryngeal mask: insertion, gas leak pressure and gastric insufflation. Br J Anaesth 2002;89: Ho-Tai LM, Devitt JH, Noel AG, O Donnell MP. Gas leak and gastric insufflation during controlled ventilation: face mask versus laryngeal mask airway. Can J Anaesth 1998;45: Wahlen BM, Heinrichs W, Latorre F. Gastric insufflation pressure, air leakage and respiratory mechanics in the use of the laryngeal mask airway (LMAU) in children. Paediatr Anaesth 2004;14: Brimacomb J, Keller C, Kurian S, Myles J. Reliability of epigastric auscultation to detect gastric insufflation. Br J Anaesth 2002;88: Badgwell JM, McLeod ME, Lerman J, Creighton RE. End-tidal PCO2 measurements sampled at the distal and proximal ends of the endotracheal tube in infants and children. Anesth Analg 1987;66: CobraPLA in Pediatric Patients ANESTHESIA & ANALGESIA
A randomised comparison between Cobra PLA and classic laryngeal mask airway and laryngeal tube during mechanical ventilation for general anaesthesia
 ORIGINAL AND CLINICAL PAPERS Anaesthesiology Intensive Therapy 2013, vol. 45, no 1, 20 24 ISSN 1642 5758 DOI: 10.5603/AIT.2013.0004 www.ait.viamedica.pl A randomised comparison between Cobra PLA and classic
ORIGINAL AND CLINICAL PAPERS Anaesthesiology Intensive Therapy 2013, vol. 45, no 1, 20 24 ISSN 1642 5758 DOI: 10.5603/AIT.2013.0004 www.ait.viamedica.pl A randomised comparison between Cobra PLA and classic
Use of the Intubating Laryngeal Mask Airway
 340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
Comparison of Three Disposable Extraglottic Airway Devices in Spontaneously Breathing Adults
 Anesthesiology 2006; 104:1165 9 2006 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Comparison of Three Disposable Extraglottic Airway Devices in Spontaneously Breathing
Anesthesiology 2006; 104:1165 9 2006 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Comparison of Three Disposable Extraglottic Airway Devices in Spontaneously Breathing
The Laryngeal Mask and Other Supraglottic Airways: Application to Clinical Airway Management
 The Laryngeal Mask and Other Supraglottic Airways: Application to Clinical Airway Management D. John Doyle MD PhD FRCPC Department of General Anesthesiology Cleveland Clinic Foundation 9500 Euclid Avenue
The Laryngeal Mask and Other Supraglottic Airways: Application to Clinical Airway Management D. John Doyle MD PhD FRCPC Department of General Anesthesiology Cleveland Clinic Foundation 9500 Euclid Avenue
Citation British journal of anaesthesia, 104. pp ; 2010 is available onlin
 NAOSITE: Nagasaki University's Ac Title Laryngeal mask airway Supreme for a Author(s) Murata, Hiroaki; Nagaishi, Chikako; Citation British journal of anaesthesia, 104 Issue Date 2010-03 URL Right http://hdl.handle.net/10069/24856
NAOSITE: Nagasaki University's Ac Title Laryngeal mask airway Supreme for a Author(s) Murata, Hiroaki; Nagaishi, Chikako; Citation British journal of anaesthesia, 104 Issue Date 2010-03 URL Right http://hdl.handle.net/10069/24856
Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients.
 Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
Positive pressure ventilation with the laryngeal mask airway in non-paralysed patients: comparison of sevoflurane and propofol maintenance techniques
 British Journal of Anaesthesia 1998; 80: 33 336 Positive pressure ventilation with the laryngeal mask airway in non-paralysed patients: comparison of sevoflurane and propofol maintenance techniques C.
British Journal of Anaesthesia 1998; 80: 33 336 Positive pressure ventilation with the laryngeal mask airway in non-paralysed patients: comparison of sevoflurane and propofol maintenance techniques C.
Dr. Ranjeet Rana De 1, Dr. Saurav Shekhar 2, Dr. D G Pathak 3, Dr. Harshwardhan 4, Dr. Shashank Dhiraj 5 1,2,4,5
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. X (April. 2017), PP 26-31 www.iosrjournals.org A Comparative Study of Classic Laryngeal
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. X (April. 2017), PP 26-31 www.iosrjournals.org A Comparative Study of Classic Laryngeal
Comparison of clinical performance of i-gel with laryngeal mask airway pro-seal in elective surgery in adults
 Curpod et al. Sri Lankan Journal of Anaesthesiology: 5():5-3(7) DOI:.438 /slja.v5i.895 Comparison of clinical performance of i-gel with laryngeal mask airway pro-seal in elective surgery in adults SG Curpod
Curpod et al. Sri Lankan Journal of Anaesthesiology: 5():5-3(7) DOI:.438 /slja.v5i.895 Comparison of clinical performance of i-gel with laryngeal mask airway pro-seal in elective surgery in adults SG Curpod
I-gel vs cuffed tracheal tube during volume controlled ventilation in elective laparoscopic cholecystectomy
 Egyptian Journal of Anaesthesia (2011) 27, 7 11 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article I-gel vs cuffed
Egyptian Journal of Anaesthesia (2011) 27, 7 11 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article I-gel vs cuffed
Original Contributions
 Standard Laryngeal Mask Airway and LMA-ProSeal during Laparoscopic Surgery Giuseppe Natalini, MD,* Gabriella Lanza, MD,* Antonio Rosano, MD,* Piera Dell Agnolo, MD,* Achille Bernardini, MD Department of
Standard Laryngeal Mask Airway and LMA-ProSeal during Laparoscopic Surgery Giuseppe Natalini, MD,* Gabriella Lanza, MD,* Antonio Rosano, MD,* Piera Dell Agnolo, MD,* Achille Bernardini, MD Department of
LMA Supreme Second Seal. Maintain the airway. Manage gastric contents. Meet NAP4 recommendations.
 LMA Supreme Second Seal Maintain the airway. Manage gastric contents. Meet NAP4 recommendations. A proven double seal The importance of the Second Seal (oesophageal seal) is significant: it can minimise
LMA Supreme Second Seal Maintain the airway. Manage gastric contents. Meet NAP4 recommendations. A proven double seal The importance of the Second Seal (oesophageal seal) is significant: it can minimise
British Journal of Anaesthesia 82 (5): (1999)
 British Journal of Anaesthesia 82 (5): 703 7 (1999) Laryngeal mask airway size selection in males and females: ease of insertion, oropharyngeal leak pressure, pharyngeal mucosal pressures and anatomical
British Journal of Anaesthesia 82 (5): 703 7 (1999) Laryngeal mask airway size selection in males and females: ease of insertion, oropharyngeal leak pressure, pharyngeal mucosal pressures and anatomical
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Cricoid pressure: useful or dangerous?
 Cricoid pressure: useful or dangerous? Francis VEYCKEMANS Cliniques Universitaires Saint Luc Bruxelles (2009) Controversial issue - Can J Anaesth 1997 JR Brimacombe - Pediatr Anesth 2002 JG Brock-Utne
Cricoid pressure: useful or dangerous? Francis VEYCKEMANS Cliniques Universitaires Saint Luc Bruxelles (2009) Controversial issue - Can J Anaesth 1997 JR Brimacombe - Pediatr Anesth 2002 JG Brock-Utne
Randomized Comparison of Actual and Ideal Body Weight for Size Selection of the Laryngeal Mask Airway Classic in Overweight Patients
 ORIGINAL ARTICLE Anesthesiology & Pain http://dx.doi.org/10.3346/jkms.2015.30.8.1197 J Korean Med Sci 2015; 30: 1197-1202 Randomized Comparison of Actual and Ideal Body Weight for Size Selection of the
ORIGINAL ARTICLE Anesthesiology & Pain http://dx.doi.org/10.3346/jkms.2015.30.8.1197 J Korean Med Sci 2015; 30: 1197-1202 Randomized Comparison of Actual and Ideal Body Weight for Size Selection of the
The Laryngeal Tube. An Evaluation of the Laryngeal Tube During General Anesthesia Using Mechanical Ventilation
 An Evaluation of the Laryngeal Tube During General Anesthesia Using Mechanical Ventilation Luis A. Gaitini, MD*, Sonia J. Vaida, MD*, Mostafa Somri, MD*, Victor Kaplan, MD*, Boris Yanovski, MD*, Robert
An Evaluation of the Laryngeal Tube During General Anesthesia Using Mechanical Ventilation Luis A. Gaitini, MD*, Sonia J. Vaida, MD*, Mostafa Somri, MD*, Victor Kaplan, MD*, Boris Yanovski, MD*, Robert
Recent Advances in Airway Management HA Convention 2014
 Recent Advances in Airway Management HA Convention 2014 Dr. HK Cheng Chief of Service (Dept. of Anaesthesia & OT) Service Director (Ambulatory Surgery Centre) Tseung Kwan O Hospital Recent Advances in
Recent Advances in Airway Management HA Convention 2014 Dr. HK Cheng Chief of Service (Dept. of Anaesthesia & OT) Service Director (Ambulatory Surgery Centre) Tseung Kwan O Hospital Recent Advances in
A Comparative Study of Classic LMA and Proseal LMA in Paralyzed Anaesthetized Patients
 Original article: A Comparative Study of Classic LMA and Proseal LMA in Paralyzed Anaesthetized Patients Dr. Gurdeep Singh Jheetay Associate Professor, Department of Anaesthesia, Shri Guru Ram Rai Institute
Original article: A Comparative Study of Classic LMA and Proseal LMA in Paralyzed Anaesthetized Patients Dr. Gurdeep Singh Jheetay Associate Professor, Department of Anaesthesia, Shri Guru Ram Rai Institute
DIFFICULT AIRWAY MANAGMENT. Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr)
 DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
The effect of head rotation on efficiency of ventilation and cuff pressure using the PLMA in pediatric patients
 Clinical Research Article Korean J Anesthesiol 2011 September 61(3): 220-224 http://dx.doi.org/10.4097/kjae.2011.61.3.220 The effect of head rotation on efficiency of ventilation and cuff pressure using
Clinical Research Article Korean J Anesthesiol 2011 September 61(3): 220-224 http://dx.doi.org/10.4097/kjae.2011.61.3.220 The effect of head rotation on efficiency of ventilation and cuff pressure using
I - Gel Versus Cuffed Tracheal Tube in Elective Laparoscopic Cholecystectomy A Clinical Comparative Study
 Original Research I - Gel Versus Cuffed Tracheal Tube in Elective Laparoscopic Cholecystectomy A Clinical Comparative Study Siddharam Jamagond 1, Anuradha H 2, Ramesh.K 3 1 Senior resident, Department
Original Research I - Gel Versus Cuffed Tracheal Tube in Elective Laparoscopic Cholecystectomy A Clinical Comparative Study Siddharam Jamagond 1, Anuradha H 2, Ramesh.K 3 1 Senior resident, Department
The LMA CTrach TM, a new laryngeal mask airway for endotracheal intubation under vision: evaluation in 100 patients
 British Journal of Anaesthesia 96 (3): 396 400 (2006) doi:10.1093/bja/ael001 Advance Access publication January 16, 2006 The LMA CTrach TM, a new laryngeal mask airway for endotracheal intubation under
British Journal of Anaesthesia 96 (3): 396 400 (2006) doi:10.1093/bja/ael001 Advance Access publication January 16, 2006 The LMA CTrach TM, a new laryngeal mask airway for endotracheal intubation under
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Tibe ProSeal Laryngeal Mask Airway
 104 Anesthesioloby 2ooO; 93: 104-9 0 ZOO0 American Society of Anesthesiologists, Inc Lippincoa Williams & wilkins, Inc. Tibe ProSeal Laryngeal Mask Airway A Randomized, Crossover Study with the Standard
104 Anesthesioloby 2ooO; 93: 104-9 0 ZOO0 American Society of Anesthesiologists, Inc Lippincoa Williams & wilkins, Inc. Tibe ProSeal Laryngeal Mask Airway A Randomized, Crossover Study with the Standard
Introducing the Fastrach-LMA. Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council
 Introducing the Fastrach-LMA Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council Objectives Review Anatomy of the Upper Airway Review LFEMSC LMA Protocol Discuss Indications
Introducing the Fastrach-LMA Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council Objectives Review Anatomy of the Upper Airway Review LFEMSC LMA Protocol Discuss Indications
ISPUB.COM. The Use of LMA in Newborn Resuscitation. R Vadhera INTRODUCTION VENTILATION
 ISPUB.COM The Internet Journal of Anesthesiology Volume 1 Number 4 The Use of LMA in Newborn Resuscitation R Vadhera Citation R Vadhera. The Use of LMA in Newborn Resuscitation. The Internet Journal of
ISPUB.COM The Internet Journal of Anesthesiology Volume 1 Number 4 The Use of LMA in Newborn Resuscitation R Vadhera Citation R Vadhera. The Use of LMA in Newborn Resuscitation. The Internet Journal of
Observation of ventilation effects of I-gel TM, Supreme TM and Ambu AuraOnce TM with respiratory dynamics monitoring in small children
 J Clin Monit Comput (2017) 31:1035 1041 DOI 10.1007/s10877-016-9917-6 ORIGINAL RESEARCH Observation of ventilation effects of I-gel TM, Supreme TM and Ambu AuraOnce TM with respiratory dynamics monitoring
J Clin Monit Comput (2017) 31:1035 1041 DOI 10.1007/s10877-016-9917-6 ORIGINAL RESEARCH Observation of ventilation effects of I-gel TM, Supreme TM and Ambu AuraOnce TM with respiratory dynamics monitoring
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
ISSN X (Print) Research Article. *Corresponding author Dr. Souvik Saha
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(6B):2238-2243 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(6B):2238-2243 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Comparison of Ease of Insertion and Hemodynamic Response to Lma with Propofol and Thiopentone.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 22-30 www.iosrjournals.org Comparison of Ease of Insertion and Hemodynamic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 22-30 www.iosrjournals.org Comparison of Ease of Insertion and Hemodynamic
Comparison of efficacy of the Laryngeal tube with the Laryngeal mask airway in securing the upper airway
 Original Research Article Comparison of efficacy of the Laryngeal tube with the Laryngeal mask airway in securing the upper airway Khaja Ali Hassan 1,*, Ahsan Mustafa 2 1,2 Assistant Professor, Department
Original Research Article Comparison of efficacy of the Laryngeal tube with the Laryngeal mask airway in securing the upper airway Khaja Ali Hassan 1,*, Ahsan Mustafa 2 1,2 Assistant Professor, Department
Randomised comparison of the LMA Supreme with the I-Gel in spontaneously breathing anaesthetised adult patients
 Anaesth Intensive Care 2010; 38: Randomised comparison of the LMA Supreme with the I-Gel in spontaneously breathing anaesthetised adult patients E. F. F. CHEW*, N. HANEEM, C. Y. WANG Department of Anaesthesia,
Anaesth Intensive Care 2010; 38: Randomised comparison of the LMA Supreme with the I-Gel in spontaneously breathing anaesthetised adult patients E. F. F. CHEW*, N. HANEEM, C. Y. WANG Department of Anaesthesia,
ORIGINAL ARTICLE. Shashank Chitmulwar, MD, Charulata Deshpande, MD, DA ABSTRACT. ANAESTHESIA, PAIN & INTENSIVE CARE
 ORIGINAL ARTICLE ANAESTHESIA, PAIN & INTENSIVE CARE www.apicareonline.com Comparison of insertion characteristics between LMA- Supreme and Laryngeal tube with suction in patients undergoing short duration
ORIGINAL ARTICLE ANAESTHESIA, PAIN & INTENSIVE CARE www.apicareonline.com Comparison of insertion characteristics between LMA- Supreme and Laryngeal tube with suction in patients undergoing short duration
AIRWAY MANAGEMENT AND VENTILATION
 AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Evaluation of Postoperative Sore Throat and Hoarseness of Voice with Three Variants of Laryngeal
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Evaluation of Postoperative Sore Throat and Hoarseness of Voice with Three Variants of Laryngeal
Use of the Aintree Intubation Catheter with the Laryngeal Mask Airway and a Fiberoptic Bronchoscope in a Patient with an Unexpected Difficult Airway
 Case Report Use of the Aintree Intubation Catheter with the Laryngeal Mask Airway and a Fiberoptic Bronchoscope in a Patient with an Unexpected Difficult Airway Andrew Zura MD, D. John Doyle MD PhD FRCPC,
Case Report Use of the Aintree Intubation Catheter with the Laryngeal Mask Airway and a Fiberoptic Bronchoscope in a Patient with an Unexpected Difficult Airway Andrew Zura MD, D. John Doyle MD PhD FRCPC,
A Comparative Study of Two Disposable Supraglottic Devices in Diagnostic Laparoscopy in Gynecology
 10.5005/jp-journals-10006-1243 Suman ORIGINAL Chattopadhyay, ARTICLESebanti Goswami A Comparative Study of Two Disposable Supraglottic Devices in Diagnostic Laparoscopy in Gynecology Suman Chattopadhyay,
10.5005/jp-journals-10006-1243 Suman ORIGINAL Chattopadhyay, ARTICLESebanti Goswami A Comparative Study of Two Disposable Supraglottic Devices in Diagnostic Laparoscopy in Gynecology Suman Chattopadhyay,
Use of laryngeal mask airway compared to endotracheal tube with positive-pressure ventilation in anesthetized swine
 Veterinary Anaesthesia and Analgesia, 2007, 34, 284 288 doi:10.1111/j.1467-2995.2006.00329.x RESEARCH PAPER Use of laryngeal mask airway compared to endotracheal tube with positive-pressure ventilation
Veterinary Anaesthesia and Analgesia, 2007, 34, 284 288 doi:10.1111/j.1467-2995.2006.00329.x RESEARCH PAPER Use of laryngeal mask airway compared to endotracheal tube with positive-pressure ventilation
Pharyngolaryngeal Morbidity with the Laryngeal Mask Airway in Spontaneously Breathing Patients
 Anesthesiology 2001; 94:760 6 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Pharyngolaryngeal Morbidity with the Laryngeal Mask Airway in Spontaneously Breathing
Anesthesiology 2001; 94:760 6 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Pharyngolaryngeal Morbidity with the Laryngeal Mask Airway in Spontaneously Breathing
Deposited on: 11 February 2010
 Uppal, V. and Gangaiah, S. and Fletcher, G. and Kinsella, J. (2009) Randomized crossover comparison between the i-gel and the LMA- Unique in anaesthetized, paralysed adults. British Journal of Anaesthesia,
Uppal, V. and Gangaiah, S. and Fletcher, G. and Kinsella, J. (2009) Randomized crossover comparison between the i-gel and the LMA- Unique in anaesthetized, paralysed adults. British Journal of Anaesthesia,
Gastroesophageal regurgitation during anesthesia and controlled ventilation with six airway devices
 Journal of Clinical Anesthesia (2008) 20, 508 513 Original contribution Gastroesophageal regurgitation during anesthesia and controlled ventilation with six airway devices Vadim Khazin MD (Deputy Head,
Journal of Clinical Anesthesia (2008) 20, 508 513 Original contribution Gastroesophageal regurgitation during anesthesia and controlled ventilation with six airway devices Vadim Khazin MD (Deputy Head,
Cuffed or uncuffed ETT in pediatric anesthesia? Dr. Renata Haghedooren Dr. Sophie Chullikal Dr. Julie Lauweryns
 Cuffed or uncuffed ETT in pediatric anesthesia? Dr. Renata Haghedooren Dr. Sophie Chullikal Dr. Julie Lauweryns Overview History Survey Tradition Pro-Con Debate Conclusions History of intubation 1878:
Cuffed or uncuffed ETT in pediatric anesthesia? Dr. Renata Haghedooren Dr. Sophie Chullikal Dr. Julie Lauweryns Overview History Survey Tradition Pro-Con Debate Conclusions History of intubation 1878:
A Clinical Evaluation of the Intubating Laryngeal Airway as a Conduit for Tracheal Intubation in Children
 Society for Pediatric Anesthesia Section Editor: Peter J. Davis A Clinical Evaluation of the Intubating Laryngeal Airway as a Conduit for Tracheal Intubation in Children Narasimhan Jagannathan, MD, Ryan
Society for Pediatric Anesthesia Section Editor: Peter J. Davis A Clinical Evaluation of the Intubating Laryngeal Airway as a Conduit for Tracheal Intubation in Children Narasimhan Jagannathan, MD, Ryan
Optimal Size AMBU Laryngeal Mask Airway Among Asian Adult Population
 ORIGINAL ARTICLE Optimal Size AMBU Laryngeal Mask Airway Among Asian Adult Population Mee Yee Tang, FANZCA*; Ing Ping Tang, MS (ORL-HNS)*; Chew Yin Wang, FRCA** *Department of Surgery, Faculty of Medicine
ORIGINAL ARTICLE Optimal Size AMBU Laryngeal Mask Airway Among Asian Adult Population Mee Yee Tang, FANZCA*; Ing Ping Tang, MS (ORL-HNS)*; Chew Yin Wang, FRCA** *Department of Surgery, Faculty of Medicine
REVERSE LMA INSERTION IN A NEONATE WITH KLIPPEL-FEIL SYNDROME
 REVERSE LMA INSERTION IN A NEONATE WITH KLIPPEL-FEIL SYNDROME - Case report - TARIQ AL ZAHRANI * Klippel-Feil syndrome (KFS) was first described by Maurice Klippel and Andre Feil in 1912 in a patient with
REVERSE LMA INSERTION IN A NEONATE WITH KLIPPEL-FEIL SYNDROME - Case report - TARIQ AL ZAHRANI * Klippel-Feil syndrome (KFS) was first described by Maurice Klippel and Andre Feil in 1912 in a patient with
RESPIRATION AND THE AIRWAY Comparison of the i-gel with the cuffed tracheal tube during pressure-controlled ventilation
 RESPIRATION AND THE AIRWAY Comparison of the i-gel with the cuffed tracheal tube during pressure-controlled ventilation V. Uppal 1, G. Fletcher 2 and J. Kinsella 1 1 Section of Anaesthesia, Pain and Critical
RESPIRATION AND THE AIRWAY Comparison of the i-gel with the cuffed tracheal tube during pressure-controlled ventilation V. Uppal 1, G. Fletcher 2 and J. Kinsella 1 1 Section of Anaesthesia, Pain and Critical
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Success of Tracheal Intubation with Intubating Laryngeal Mask Airways
 Anesthesiology 2008; 108:621 6 Copyright 2008, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Success of Tracheal Intubation with Intubating Laryngeal Mask Airways
Anesthesiology 2008; 108:621 6 Copyright 2008, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Success of Tracheal Intubation with Intubating Laryngeal Mask Airways
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Materials and Methods
 Anesthesiology 2004; 101:316 20 2004 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. A Randomized Controlled Trial Comparing the ProSeal Laryngeal Mask Airway with the Laryngeal
Anesthesiology 2004; 101:316 20 2004 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. A Randomized Controlled Trial Comparing the ProSeal Laryngeal Mask Airway with the Laryngeal
Comparison of the Hemodynamic Responses with. with LMA vs Endotracheal Intubation
 Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Nicolette Mosinski MPAS, PA-C
 Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital
 AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 64/Nov24, 2014 Page 13923
 SUCCESS RATE OF INTUBATING LARYNGEAL MASK AIRWAY FOR BLIND ORAL INTUBATION IN PATIENTS UNDERGOING SURGERY UNDER GENERAL ANESTHESIA Lokesh Kumar K. S 1, Rajalakshmi J 2, Santosh Kumar 3 HOW TO CITE THIS
SUCCESS RATE OF INTUBATING LARYNGEAL MASK AIRWAY FOR BLIND ORAL INTUBATION IN PATIENTS UNDERGOING SURGERY UNDER GENERAL ANESTHESIA Lokesh Kumar K. S 1, Rajalakshmi J 2, Santosh Kumar 3 HOW TO CITE THIS
Deposited on: 24 February 2009
 Uppal, V. and Fletcher, G. and Kinsella, J. (2009) Comparison of the i- gel with the cuffed tracheal tube during pressure-controlled ventilation. British Journal of Anaesthesia, 102 (2). 264-268. ISSN
Uppal, V. and Fletcher, G. and Kinsella, J. (2009) Comparison of the i- gel with the cuffed tracheal tube during pressure-controlled ventilation. British Journal of Anaesthesia, 102 (2). 264-268. ISSN
J. Brimacombe, 1 L. Holyoake, 2 C. Keller, 3 J. Barry, 4 D. Mecklem, 4 A. Blinco 5 and K. Weidmann 5
 Emergence characteristics and postoperative laryngopharyngeal morbidity with the laryngeal mask airway: a comparison of high versus low initial cuff volume J. Brimacombe, 1 L. Holyoake, 2 C. Keller, 3
Emergence characteristics and postoperative laryngopharyngeal morbidity with the laryngeal mask airway: a comparison of high versus low initial cuff volume J. Brimacombe, 1 L. Holyoake, 2 C. Keller, 3
Asai and Shingu Table 1 Size selection and recommended cuff volumes Size Patients Body size Recommended cuff volumes (ml) Connector colour 0 Newborn <
 British Journal of Anaesthesia 95 (6): 729 36 (2005) doi:10.1093/bja/aei269 REVIEW ARTICLE The laryngeal tube T. Asai* y and K. Shingu Department of Anaesthesiology, Kansai Medical University, 10 15 Fumizono-cho,
British Journal of Anaesthesia 95 (6): 729 36 (2005) doi:10.1093/bja/aei269 REVIEW ARTICLE The laryngeal tube T. Asai* y and K. Shingu Department of Anaesthesiology, Kansai Medical University, 10 15 Fumizono-cho,
LMA Unique Airway Portfolio
 LMA Unique Airway Portfolio LMA Unique (Silicone Cuff) Airway with Cuff Pilot Technology The Single-Use LMA Airway Designed for Patient Comfort The LMA Unique (Silicone Cuff) Airway from Teleflex is a
LMA Unique Airway Portfolio LMA Unique (Silicone Cuff) Airway with Cuff Pilot Technology The Single-Use LMA Airway Designed for Patient Comfort The LMA Unique (Silicone Cuff) Airway from Teleflex is a
Received 1 November 2009 Revised 8 December 2009 Accepted 10 December 2009
 ORIGINAL ARTICLE Safety and efficacy of laryngeal mask airway Supreme versus laryngeal mask airway ProSeal: a randomized controlled trial Edwin Seet, Subramanyam Rajeev, Tamal Firoz, Farhanah Yousaf, Jean
ORIGINAL ARTICLE Safety and efficacy of laryngeal mask airway Supreme versus laryngeal mask airway ProSeal: a randomized controlled trial Edwin Seet, Subramanyam Rajeev, Tamal Firoz, Farhanah Yousaf, Jean
Difficult Airway. Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital
 Difficult Airway Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital Difficult Airway Definition Predicting a difficult airway Preparing for a difficult airway Extubation
Difficult Airway Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital Difficult Airway Definition Predicting a difficult airway Preparing for a difficult airway Extubation
The flexible laryngeal mask airway (FLMA) was
 GENERAL ARTICLES The Influence of the Tonsillar Gag on Efficacy of Seal, Anatomic Position, Airway Patency, and Airway Protection with the Flexible Laryngeal Mask Airway: A Randomized, Cross-Over Study
GENERAL ARTICLES The Influence of the Tonsillar Gag on Efficacy of Seal, Anatomic Position, Airway Patency, and Airway Protection with the Flexible Laryngeal Mask Airway: A Randomized, Cross-Over Study
Clinical Study Randomised Comparison of the AMBU AuraOnce Laryngeal Mask and the LMA Unique Laryngeal Mask Airway in Spontaneously Breathing Adults
 Hindawi Publishing Corporation Anesthesiology Research and Practice Volume 2012, Article ID 405812, 5 pages doi:10.1155/2012/405812 Clinical Study Randomised Comparison of the AMBU AuraOnce Laryngeal Mask
Hindawi Publishing Corporation Anesthesiology Research and Practice Volume 2012, Article ID 405812, 5 pages doi:10.1155/2012/405812 Clinical Study Randomised Comparison of the AMBU AuraOnce Laryngeal Mask
Blind Insertion Airway Devices (BIAD)
 P03 Procedures 2017-05-12 All ages Office of the Medical Director Blind Insertion Airway Devices (BIAD) Primary Intermediate Advanced Critical From AIRWAY & BREATHING MANAGEMENT or AIRWAY OBSTRUCTION Yes
P03 Procedures 2017-05-12 All ages Office of the Medical Director Blind Insertion Airway Devices (BIAD) Primary Intermediate Advanced Critical From AIRWAY & BREATHING MANAGEMENT or AIRWAY OBSTRUCTION Yes
Proper insertion depth of endotracheal tubes in adults by topographic landmarks measurements
 Journal of Clinical Anesthesia (2007) 19, 15 19 Original contribution Proper insertion depth of endotracheal tubes in adults by topographic landmarks measurements Shmuel Evron MD a,c, Marian Weisenberg
Journal of Clinical Anesthesia (2007) 19, 15 19 Original contribution Proper insertion depth of endotracheal tubes in adults by topographic landmarks measurements Shmuel Evron MD a,c, Marian Weisenberg
L.J. Hoeve and R.H.M. van Poppelen * (Received 12 July 1989) (Accepted 10 August 1989)
 International Journal of Pediatric Otorhinolaryngolo~. 18 (1990) 241-245 Elsevier 241 PEDOT 00617 Fiberoptic laryngoscopy under in neonates general anesthesia L.J. Hoeve and R.H.M. van Poppelen * Lkpar?ments
International Journal of Pediatric Otorhinolaryngolo~. 18 (1990) 241-245 Elsevier 241 PEDOT 00617 Fiberoptic laryngoscopy under in neonates general anesthesia L.J. Hoeve and R.H.M. van Poppelen * Lkpar?ments
Comparative evaluation of Ambu AuraGain with ProSeal laryngeal mask airway in patients undergoing laparoscopic cholecystectomy
 Original Article Comparative evaluation of Ambu AuraGain with ProSeal laryngeal mask airway in patients undergoing laparoscopic cholecystectomy Address for correspondence: Dr. Kriti Singh, Department of
Original Article Comparative evaluation of Ambu AuraGain with ProSeal laryngeal mask airway in patients undergoing laparoscopic cholecystectomy Address for correspondence: Dr. Kriti Singh, Department of
Advanced Airway Management
 CHAPTER 37 Advanced Airway Management Airway Anatomy and Physiology Review Respiratory System: The Airway Respiratory System (Supine) Physiology: Factors of Adequate Breathing Functioning brainstem Open
CHAPTER 37 Advanced Airway Management Airway Anatomy and Physiology Review Respiratory System: The Airway Respiratory System (Supine) Physiology: Factors of Adequate Breathing Functioning brainstem Open
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
University of Groningen
 University of Groningen A comparison of the clinical use of the Laryngeal Tube S (TM) and the ProSeal (R) Laryngeal Mask Airway by first-month anaesthesia residents in anaesthetised patients Klaver, N.
University of Groningen A comparison of the clinical use of the Laryngeal Tube S (TM) and the ProSeal (R) Laryngeal Mask Airway by first-month anaesthesia residents in anaesthetised patients Klaver, N.
COMPARATIVE CLINICAL EVALUATION OF PROSEAL LMA WITH I - GEL AIRWAY IN PATIENTS UNDERGOING ELECTIVE SURGICAL PROCEDURES UNDER GENERAL ANAESTHESIA
 COMPARATIVE CLINICAL EVALUATION OF PROSEAL LMA WITH I - GEL AIRWAY IN PATIENTS UNDERGOING ELECTIVE SURGICAL PROCEDURES UNDER GENERAL ANAESTHESIA Sugata Dasgupta 1, *Dipasri Bhattacharya 1 and Saswati Paul
COMPARATIVE CLINICAL EVALUATION OF PROSEAL LMA WITH I - GEL AIRWAY IN PATIENTS UNDERGOING ELECTIVE SURGICAL PROCEDURES UNDER GENERAL ANAESTHESIA Sugata Dasgupta 1, *Dipasri Bhattacharya 1 and Saswati Paul
Complications following the use of the Combitube, tracheal tube and laryngeal mask airway
 Complications following the use of the Combitube, tracheal tube and laryngeal mask airway W. Oczenski, 1 H. Krenn, 1 A. A. Dahaba, 2 M. Binder, 1 I. El-Schahawi-Kienzl, 3 S. Kohout, 4 S. Schwarz 5 and
Complications following the use of the Combitube, tracheal tube and laryngeal mask airway W. Oczenski, 1 H. Krenn, 1 A. A. Dahaba, 2 M. Binder, 1 I. El-Schahawi-Kienzl, 3 S. Kohout, 4 S. Schwarz 5 and
Anesthetic challenges when elective case becomes emergent
 Anesthetic challenges when elective case becomes emergent Shridevi Pandya Shah MD Asst Professor Dept of Anesthesiology Rutgers-NJMS Rutgers, The State University of New Jersey Conflicts of interest: none
Anesthetic challenges when elective case becomes emergent Shridevi Pandya Shah MD Asst Professor Dept of Anesthesiology Rutgers-NJMS Rutgers, The State University of New Jersey Conflicts of interest: none
CONTINUING EDUCATION IN HONOR OF NORMAN TRIEGER, DMD, MD
 CONTINUING EDUCATION IN HONOR OF NORMAN TRIEGER, DMD, MD Essentials of Airway Management, Oxygenation, and Ventilation: Part 2: Advanced Airway Devices: Supraglottic Airways M. B. Rosenberg, DMD,* J. C.
CONTINUING EDUCATION IN HONOR OF NORMAN TRIEGER, DMD, MD Essentials of Airway Management, Oxygenation, and Ventilation: Part 2: Advanced Airway Devices: Supraglottic Airways M. B. Rosenberg, DMD,* J. C.
REVISTA BRASILEIRA DE ANESTESIOLOGIA
 Rev Bras Anestesiol. 2013;63(6):445 9 2013;63(6):445 449 REVISTA BRASILEIRA DE ANESTESIOLOGIA Official Publication of the Brazilian Society of Anesthesiology www.sba.com.br SCIENTIFIC ARTICLE Comparison
Rev Bras Anestesiol. 2013;63(6):445 9 2013;63(6):445 449 REVISTA BRASILEIRA DE ANESTESIOLOGIA Official Publication of the Brazilian Society of Anesthesiology www.sba.com.br SCIENTIFIC ARTICLE Comparison
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
General OR Rotations GOALS & OBJECTIVES
 General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
Journal of Anesthesia & Clinical
 Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
EUROANESTHESIA 2007 Munich, Germany, 9-12 June 2007
 AIRWAY MANAGEMENT AND VENTILATION IN DAY SURGERY EUROANESTHESIA 2007 Munich, Germany, 9-12 June 2007 2RC1 IAN SMITH Senior Lecturer in Anaesthesia University Hospital of North Staffordshire Stoke-on-Trent,
AIRWAY MANAGEMENT AND VENTILATION IN DAY SURGERY EUROANESTHESIA 2007 Munich, Germany, 9-12 June 2007 2RC1 IAN SMITH Senior Lecturer in Anaesthesia University Hospital of North Staffordshire Stoke-on-Trent,
Airway Management. Teeradej Kuptanon, MD
 Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Overview. Chapter 37. Advanced Airway Techniques. Sellick Maneuver 9/11/2012
 Chapter 37 Advanced Airway Techniques Slide 1 Sellick Maneuver Purpose Anatomic Location Technique Special Considerations Overview Advanced Airway Management of Adults Esophageal Tracheal Combitubes Tracheal
Chapter 37 Advanced Airway Techniques Slide 1 Sellick Maneuver Purpose Anatomic Location Technique Special Considerations Overview Advanced Airway Management of Adults Esophageal Tracheal Combitubes Tracheal
1. Influence of isoflurane exposure in pregnant rats on the learning and memory of offspring
 1. Influence of isoflurane exposure in pregnant rats on the learning and memory of offspring Huang W, Dong Y, Zhao G, et al. BMC Anesthesiology 2018 18:5 Concerns remain about possible effects of general
1. Influence of isoflurane exposure in pregnant rats on the learning and memory of offspring Huang W, Dong Y, Zhao G, et al. BMC Anesthesiology 2018 18:5 Concerns remain about possible effects of general
Disclosures. Learning Objectives. Coeditor/author. Associate Science Editor, American Heart Association
 Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Supra-glottic Airway Devices
 Supra-glottic Airway Devices Dr.K.Sudarshan Consultant Anaesthesiologist Coimbatore The ability to maintain an airway is one of the core skills and defining role of an anaesthetist. It is needless to say
Supra-glottic Airway Devices Dr.K.Sudarshan Consultant Anaesthesiologist Coimbatore The ability to maintain an airway is one of the core skills and defining role of an anaesthetist. It is needless to say
Original Research Article. Amol P. Singam 1, Arpita A. Jaiswal 2 *, Ashok R. Chaudhari 1
 International Journal of Research in Medical Sciences Singam AP et al. Int J Res Med Sci. 2018 Jan;6(1):129-134 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20175538
International Journal of Research in Medical Sciences Singam AP et al. Int J Res Med Sci. 2018 Jan;6(1):129-134 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20175538
Cuffed Tracheal Tubes in Children - Myths and Facts. PD Dr. Markus Weiss Department of Anaesthesia University Children s Hospital Zurich Switzerland
 Cuffed Tracheal Tubes in Children - Myths and Department of Anaesthesia University Children s Hospital Zurich Switzerland PRO Reduced gas leak, low fresh gas flow Decreased atmospheric pollution Constant
Cuffed Tracheal Tubes in Children - Myths and Department of Anaesthesia University Children s Hospital Zurich Switzerland PRO Reduced gas leak, low fresh gas flow Decreased atmospheric pollution Constant
Comparison of I-gel with Baska Mask Airway for Controlled Ventilation in Obese Patients Undergoing Ambulatory Surgery: A Prospective Randomized Trial
 Journal of Anesthesiology 2017; 5(4): 29-35 http://www.sciencepublishinggroup.com/j/ja doi: 10.11648/j.ja.20170504.12 ISSN: 2376-7766(Print); ISSN: 2376-7774(Online) Comparison of I-gel with Baska Mask
Journal of Anesthesiology 2017; 5(4): 29-35 http://www.sciencepublishinggroup.com/j/ja doi: 10.11648/j.ja.20170504.12 ISSN: 2376-7766(Print); ISSN: 2376-7774(Online) Comparison of I-gel with Baska Mask
Role of laryngeal mask airway in emergency department and pre-hospital environment
 Hong Kong Journal of Emergency Medicine Role of laryngeal mask airway in emergency department and pre-hospital environment FKC Chu LMA and Intubating LMA (LMA-Fastrach) have been widely used by anesthesiologists
Hong Kong Journal of Emergency Medicine Role of laryngeal mask airway in emergency department and pre-hospital environment FKC Chu LMA and Intubating LMA (LMA-Fastrach) have been widely used by anesthesiologists
The laryngeal mask airway in infants and children
 CARDIOTHORACIC ANESTHESIA, RESPIRATIONANDAIRWAY 413 Chongdoo Park MD,* Jae-Hyon Bahk MD, Won-Sik Ahn MD, Sang-Hwan Do MD, Kook-Hyun Lee MD The laryngeal mask airway in infants and children Purpose: To
CARDIOTHORACIC ANESTHESIA, RESPIRATIONANDAIRWAY 413 Chongdoo Park MD,* Jae-Hyon Bahk MD, Won-Sik Ahn MD, Sang-Hwan Do MD, Kook-Hyun Lee MD The laryngeal mask airway in infants and children Purpose: To
If you suspect airway problems, get a second opinion before you anaesthetise, not after!
 Assessing the airway It is more important to be aware of the various methods of dealing with difficult laryngoscopy than to expect to be able to accurately identify the rare difficult patients without
Assessing the airway It is more important to be aware of the various methods of dealing with difficult laryngoscopy than to expect to be able to accurately identify the rare difficult patients without
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
Unanticipated difficult tracheal intubation - during routine induction of anaesthesia in an adult patient
 Unanticipated difficult tracheal intubation - during routine induction of anaesthesia in an adult patient Direct laryngoscopy Any problems Call for help Plan A: Initial tracheal intubation plan Direct
Unanticipated difficult tracheal intubation - during routine induction of anaesthesia in an adult patient Direct laryngoscopy Any problems Call for help Plan A: Initial tracheal intubation plan Direct
Evaluation of Baska Mask Performance in Laparoscopic Cholecystectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 4 Ver. 12 (April. 2018), PP 74-78 www.iosrjournals.org Evaluation of Baska Mask Performance
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 4 Ver. 12 (April. 2018), PP 74-78 www.iosrjournals.org Evaluation of Baska Mask Performance
Ventilating the paediatric patient. Lizzie Barrett Nurse Educator November 2016
 Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
ISPUB.COM. M Roberts, M Mani, A Wilkes, E Flavell, N Goodwin INTRODUCTION
 ISPUB.COM The Internet Journal of Anesthesiology Volume 30 Number 2 A Randomised Crossover Study Comparing The Disposable Laryngeal Mask Airway Supreme With The Laryngeal Mask Airway Proseal In Unparalysed
ISPUB.COM The Internet Journal of Anesthesiology Volume 30 Number 2 A Randomised Crossover Study Comparing The Disposable Laryngeal Mask Airway Supreme With The Laryngeal Mask Airway Proseal In Unparalysed
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
Difficult Airway. Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.)
 Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
INDEPENDENT LUNG VENTILATION
 INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
The use of AIR-Q as conduit for fiberoptic endotracheal intubation in adult paralyzed patients
 Egyptian Journal of Anaesthesia (2012) 28, 249 255 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article The use of AIR-Q
Egyptian Journal of Anaesthesia (2012) 28, 249 255 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article The use of AIR-Q
