Antidepressants for bipolar disorder:
|
|
|
- Edmund Thompson
- 6 years ago
- Views:
Transcription
1 NEURAL REGENERATION RESEARCH Volume 8, Issue 31, Jy doi: /j.issn [ Zhang YL, Yang H, Liang W, Dai P, Wang CH, Yang SC, Zhang YL. Antidepressants for bipolar disorder: a meta-analysis of randomized, double-blind, controlled trials. Neural Regen Res. 2013;8(31): Antidepressants for bipolar disorder: A meta-analysis of randomized, double-blind, controlled trials** Yingli Zhang 1, 2, Huan Yang 1, Shichang Yang 3, Wei Liang 4, Ping Dai 5, Changhong Wang 2, Yalin Zhang 1 1 Mental Health Institute, Second Xiangya Hospital, Central South University, Changsha , Hunan Province, China 2 Psychological Counseling Center, Second Affiliated Hospital of Xinxiang Medical University, Xinxiang , Henan Province, China 3 Department of Psychology, Xinxiang Medical University, Xinxiang , Henan Province, China 4 Department of Clinical Psychology, Second Affiliated Hospital of Xinxiang Medical University, Xinxiang , Henan Province, China 5 Sichuan University Library, Chengdu , Sichuan Province, China Research Highlights (1) The use of antidepressants in the treatment of bipolar disorder remains controversial. To the best of our knowledge, there have been no meta-analysis papers of randomized, double-blind, controlled trials and the therapeutic effects and safety of long-term antidepressants in the treatment of bipolar disorder were not evaluated. (2) The study involved new large-sample double-blind randomized controlled trials, excluded open-label design studies, and supplemented studies involving homogeneous patients. Strict inclusion criteria included limitation to double-blind randomized controlled studies and interventional treatment without use of antipsychotics to make the study results more objective and convincing. (3) The present results do not support that antidepressants are more effective in the treatment of bipolar disorder. Antidepressants are not superior to placebo and other medication in short-term, and long-term use of antidepressants cannot achieve higher response and remission rates of bipolar disorder. These findings guide future clinical studies and provide evidence for preparing treatment strategy for bipolar disorder. Abstract OBJECTIVE: To examine the efficacy and safety of short-term and long-term use of antidepressants in the treatment of bipolar disorder. DATA SOURCES: A literature search of randomized, double-blind, controlled trials published until December 2012 was performed using the PubMed, ISI Web of Science, Medline and Cochrane Central Register of Controlled Trials databases. The keywords bipolar disorder, bipolar I disorder, bipolar II disorder, bipolar mania, bipolar depression, cyclothymia, mixed mania and depression, rapid cycling and bipolar disorder, and antidepressant agent, antidepressive agents second- generation, antidepressive agents tricyclic, monoamine oxidase inhibitor, noradrenaline uptake inhibitor, serotonin uptake inhibitor, and tricyclic antidepressant agent were used. The studies that were listed in the reference list of the published papers but were not retrieved in the above-mentioned databases were supplemented. STUDY SELECTION: Studies selected were double-blind randomized controlled trials assessing the efficacy and safety of antidepressants in patients with bipolar disorder. All participants were aged 18 years or older, and were diagnosed as having primary bipolar disorder. Antidepressants or antidepressants combined with mood stabilizers were used in experimental interventions. Placebos, mood stabilizers, antipsychotics and other antide pressants were used in the control interventions. Studies that were quasi-randomized studies, or used antidepressants in combination with antipsychotics in the experimental group were excluded. All analyses were conducted using Review Manager 5.1 provided by the Cochrane Collaboration. MAIN OUTCOME MEASURES: The primary outcome was the response and switching to mania. The Yingli Zhang, Studying for doctorate, Chief physician. Corresponding author: Yalin Zhang, M.D., Professor, Mental Health Institute, Second Xiangya Hospital, Central South University, Changsha , Hunan Province, China, zhangyl69@vip.sina.com. Received: Accepted: (N ) Funding: This study was supported in part by the Key Projects of Science and Technology Research of the Department of Education in Henan Province, China, No.13A and a special fund from Henan Health Science and Technology Innovation Talent Project, No ( ). Author contributions: Zhang YL and Yang H designed this study, wrote the protocol and performed the statistical analysis. Liang W and Dai P designed the literature retrieval protocol and searched the database. Zhang YL managed the literature retrieval and analysis, and wrote the first draft of the manuscript. Yang SC and Wang CH advised and checked the manuscript. Zhang YL designed the study. All authors approved the final manuscript. Conflicts of interest: None declared. 1
2 secondary outcomes included remission, discontinuation rate, and suicidality. RESULTS: Among treatment studies published, 14 double-blind randomized controlled trials involving patients were included in the meta-analysis. Eleven short-term studies and three maintenance studies were included. Studies suggested that patients treated with antidepressants were not significantly more likely to achieve higher response and remission rates in the short-term or long-term treatment than patients treated with placebo and other medications. Antidepressants were not associated with an increased risk of discontinuation, relapse or suicidality. When one antidepressant was compared with another, no significant difference in efficacy and tolerability was found. CONCLUSION: Existing evidence of efficacy does not support the short-term or long-term application of antidepressant therapy in patients with bipolar disorder, although the tolerability and safety of antidepressants have been generally acknowledged. There is a need for large-sample, double-blind, randomized controlled trials to elucidate the role of antidepressants in patients with different subcategories of bipolar disorder. Key Words neural regeneration; evidence-based medicine; bipolar disorder; bipolar depression; antidepressant; response; switching to mania; suicidality; meta-analysis; grants-supported paper; neuroregeneration INTRODUCTION Bipolar disorder is a major psychotic disorder characterized by a chronic and highly recurrent course. Bipolar disorder is associated with a high rate of morbidity, disability [1], and comorbid anxiety and drug abuse [2], and has a major effect on social and occupational development [3-4]. The average onset age of bipolar disorder is between 20 and 40 years, while the lifetime prevalence ranges from 0.5% to 1.5%, with equal occurrence in women and men [5-6]. Because of its early onset and chronicity, bipolar disorder is one of the top thirty causes of worldwide disability [7-8]. Bipolar disorder is characterized by periods of mania, depression and mixed episodes. Most patients experience multiple episodes, with each lasting 3 6 months [9]. In the Diagnostic and Statistical Manual of Mental Disorders, fourth edition (DSM-IV) [10], bipolar disorder has been subcategorized into bipolar I and bipolar II disorders. Current data indicate that bipolar II disorder is more prevalent than bipolar I [11]. Despite mania being the hallmark of bipolar disorder, depression is the most important quantitative aspect of the illness and the one associated with higher levels of impaired social functioning and suicidality [3]. Over the last half-century, the management of bipolar disorder has been centered on manic phase treatment, and a great deal of research attention has been received regarding bipolar disorder treatment during this period [12-13]. While mood stabilizers, especially lithium, are the first the potential to increase the manic switch, while others recommend short-term antidepressant treatment and early discontinuation [18, 29].However, many of these are choice in the treatment of bipolar disorder, their efficacy in treating depression is suboptimal [14]. Studies have suggested that lithium reduces the rates of manic relapse and depressive relapse by about 40% and 25%, respectively [15]. Although there is some evidence that atypical antipsychotics are effective in the treatment of bipolar depression [16-17], the resulting adverse effects, such as weight gain, prolactin elevation, hyperglycemia, hyperlipidemia, and extrapyramidal symptoms, have become troublesome issues [18-19]. Meanwhile, little progress has been made on reducing the length of depressive episodes in bipolar disorder for the last 20 years [20]. It has been shown that pharmacological management of bipolar depression is an exceptionally difficult task [21]. Appropriate treatments for bipolar depression remain controversial. Avoiding antide pressant use has usually been proposed by clinical guide lines, considering the potential risk for switching to mania or rapid cycling during the treatment, while mood stabilizers (e.g., lithium, divalproex, and lamotrigine) as first line treatment drugs for bipolar disorder have been recommended [22-23]. However, recent reports have shown that short-term second-generation antidepressant treatment is effective for the treatment of bipolar disorder, and that second-generation antidepressant monotherapy might be associated with a relatively low manic switch rate [24-25]. Meanwhile, the use of mood stabilizers for acute episodes of depression, either alone or in combination with an antidepressant, has generally been recommended by treatment guidelines published over the past 5 to 10 years [26-28]. Some studies and treatment guidelines suggest that antidepressant treatment for bipolar disorder may have based on a single or several randomized controlled groups, rather than all high-quality randomized controlled trials presently. When most guidelines extrapolate from 2
3 studies of patients taking tricyclic antidepressants (TCAs) [30], the guidelines of bipolar depression with antidepressants are not informed by a rich evidence base and remain controversial. Meanwhile, little attention has been received for long-term antidepressant therapy of bipolar disorder. To the best of our knowledge, there are two review studies describing the efficacy and safety of antidepressants used in patients with bipolar disorder [31-32]. Unfortunately, their conclusions are inconsistent with each other. Specifically, the evidence for the effectiveness of antidepressants in the treatment of bipolar disorder is mostly based on an open-label trial, with potential high risk of bias, which is not powered or blinded to properly address clinical outcomes. Moreover, since that time, a number of double-blind, randomized controlled trials have been conducted. Given the high rates of suicidality and the negative effect on psychosocial function of bipolar disorder, the uncertain efficacy of antidepressants for the treatment of bipolar depression in the acute and maintenance phases, and controversies regarding benefits and potential risks, it is important to reevaluate and provide a quantitative review of antidepressant medication use in bipolar disorder. In this systematic review, double-blind randomized controlled trials were included to assess the efficacy and safety of short-term and long-term antidepressant use in the treatment of bipolar disorder and reduce the risks of study bias. MATERIALS AND METHODS Data retrieval Studies were found by performing literature retrieval in the PubMed, ISI Web of Science, Medline and Cochrane Central Register of Controlled Trials databases until December 2012, and by conducting a cross-reference search of the eligible articles to identify additional studies not found in the electronic search. The English terms used for retrieval of literature regarding diagnosis included bipolar disorder, bipolar I disorder, bipolar II disorder, bipolar III disorder, bipolar mania, bipolar depression, cyclothymia, manic depressive psychosis, mixed mania and depression, rapid cycling, manic depressive and bipolar affective disorder. The English terms used for literature regarding intervention and antidepressive agents were antidepressant agent, antidepressive agents, antidepressive agents secondgeneration, antidepressive agents tricyclic, monoamine oxidase inhibitor, noradrenaline uptake inhibitor, serotonin uptake inhibitor, tetracyclic antidepressant agent, and tricyclic antidepressant agent. Inclusion and exclusion criteria Inclusion criteria (1) Double-blind randomized controlled trials comparing antidepressants alone or in combination with mood stabilizers against placebos, mood stabilizers, antipsychotics or other antidepressants. (2) Participants aged 18 years or older, and with a primary diagnosis of bipolar disorder according to DSM third edition, revised (DSM-III-R) [33] or DSM-IV [10]. (3) Experimental interventions involving antidepressant mono-therapy or antidepressants in combination with mood stabilizers. No restrictions on category and dosages of antidepressant were applied. (4) Comparator intervention involving placebos, mood stabilizers, antipsychotics and other antidepressants. (5) Use of a valid and reliable scale [e.g., Hamilton Depression Rating Scale (HAMD) [34], Young Mania Rating Scale (YMRS) [35], Montgomery Asberg Depression Rating Scale (MADRS) [36] ] or a standardized psychiatric interview [e.g., Structured Diagnostic Interview for DSM-IV(SCID) [37] ] to assess changes in illness severity. Exclusion criteria (1) Studies that were quasi-randomized studies, such as those allocating use during alternate days of the week. (2) Repeatedly published literature. (3) Letters, reviews, editorials and other non-original research. (4) Treatments that included antidepressants in combination with antipsychotics. (5) Experimental treatments in which mood stabilizers, anxiolytics, alpha antagonists, inositol and N-acetylcysteine, scopolamine, and modafinil were used. (6) Studies without intact data or that did not provide data in adequate form. (7) Animal studies. Quality evaluation and data extraction Two independent reviewers extracted data and assessed the quality of methodological reports of selected studies using data extraction forms. The following data were recorded: authors and year of publication, sample size, gender, inpatient or outpatient status, dosage of the intervention agent, treatment duration, response, remission, switch mania, all cause discontinuation. The criteria for quality assessment were based on recommendations in the Cochrane Handbook for Systematic Reviews of Intervention [38]. For crossover studies, only data from the first crossover sequence were used. If multiple measures were used, HAMD and YMRS were used as first choice for data extraction. Disagreements were resolved through discussion. 3
4 Outcome measurements The primary outcomes were the clinical response and the rate of switching to mania. Clinical response was defined by the study authors and included the proportion of participants experiencing a greater than 50% improvement on scale. The secondary outcomes included remission defined by the study authors, discontinuation for any reason, relapse, and suicidality (suicidal thinking or behavior). Statistical analysis All analyses were conducted using Review Manager 5.1 provided by the Cochrane Collaboration ( cochrane.org/revman/download). For binary outcomes, the relative risks were calculated using a Mantel-Haenszel fixed-effect model, and 95% confidence intervals (CI) were calculated. Analyses were performed using an intent-to-treat principle, with last observation carried- forward data used when provided. For efficacy and safety outcomes, the total number of patients was defined as those who received at least one post baseline follow-up assessment. Heterogeneity was assessed using χ 2 and I 2 tests by fixed-effect model (I 2 50% was initially identified as heterogeneity). The Z statistic was used to determine significance of pooled estimates, with a two- tailed P value of 0.05 considered statistically significant. Sensitivity analyses were performed to determine the effects of adjunctive mood stabilizer treatment and pharmaceutical funding of the trial on the estimated outcomes. RESULTS Data retrieval results Five thousand and one studies were initially identified through the electronic search. First pass screening eliminated studies, leaving 50 studies that were considered potentially relevant for further inspection. After screening the full text, 14 randomized controlled trials [39-52] (n = 1 244) were available for meta-analyses. Figure 1 shows the selection process for the articles. Baseline analysis and quality estimation Seven studies (n = 895) [39-41, 43, 45, 46, 48] compared one or more antidepressants with placebo, of which three studies (n = 433) [39, 41, 48] assessed long-term outcome. Four studies (n = 97) [42, 49-50, 52] compared an antidepressant with other [44, 47, 51] pharmacologic treatments. Three studies (n = 252) compared two different antidepressants. The majority of the studies included patients between the ages of 18 and 65 years. Potentially relevant publications identified by literature search (n = 5 001) Full length articles retrieved (n = 50) Rejected at first pass (n = 4 951) Rejected at second pass (n = 36): Duplicate publications (n = 6) Do not meet the inclusion criteria (n = 6) Not double-blind randomized controlled trials (n = 8) Inappropriate treatment (n = 3) Insufficient data (n = 5) Review (n = 1) Letters or case report (n = 4) Unobtainable for full text (n = 3) Randomized controlled trials included in analysis (n = 14) Figure 1 Progression of articles through each stage of systematic review. The duration of short-term treatments was 4 to 12 weeks, and that of long-term treatments was 26 to 50 weeks. Two studies were pharmaceutically funded. Seven trials contained a mix of bipolar I and II disorder patients. Two studies only included bipolar II patients, and five studies did not include bipolar II disorder as a separate disorder (Table 1 provides additional details for those studies). All included studies were reported as double-blind randomized controlled trials, but only two of them explicitly stated the method of random sequence generation. Poor study quality was associated with inadequate or unclear reporting of blinding, randomization protocols, selective reporting, incomplete outcome data, or grants from a pharmaceutical company (Figure 2). Meta-analysis results Antidepressant versus placebo Clinical response: In three studies [39, 41, 43], response was defined as at least a 50% reduction of HAMD score from baseline. In two studies [40, 45], response was defined as at least a 50% reduction of MADRS. In one study [48], response was defined as at least a 50% decrease on Subscales for Depression of Clinical Monitoring Form (SUM-D). Three short-term studies [43, 45-46] were included and found that the overall effect revealed a small, but not significant, benefit of antidepressant use over placebo [three randomized controlled trials, n = 445, RR = 1.23, 95%CI: 0.94,1.62, P = 0.14], but the I²value of 63% and the significant heterogeneity test indicated a substantial heterogeneity (P = 0.07). 4
5 Table 1 Characteristics of double-blind, randomized controlled trials included in the meta-analysis Study Sample size (n) Sex (F/M, n) Bipolar type (n) Treatment Duration (week) Concomitant medication Response Remission Switch mania Assessment scale Antidepressant vs. placebo Amsterdam and Shults, [39] 2005 Amsterdam and Shults, [40] 2005 Amsterdam and Shults, [41] 2010 Cohn et al, [43] 1989 McElroy et al, [45] 2010 Nemeroff et al, [46] 2001 Sachs et al, [48] /3 DSM-IV BD II and BD NOS MD Fluoxetine 20 mg/d vs. placebo 17 5/12 DSM-IV BD I, BD II depression Fluoxetine mg/d vs. olanzapine 5 20 mg/d vs. fluoxetine mg/d plus olanzapine 5 15 mg/d vs. placebo 55 28/27 DSM-IV BD II 89 51/38 BD depression /83 DSM-IV BP I, BD II /52 DSM-III-R BD depressive phase /157 DSM-IV BP I, BD II Antidepressant vs. other medication Bocchetta et al, [42] /10 DSM-III-R BD Schaffer and colleagues, [49] 2006 Shelton and Syahl, [50] 2004 Young et al, [52] /3 DSM-IV BD I, BD II, major depression 20 10/10 DSM-IV BD I, BD II 27 18/9 DSM-IV BD I, BD II DSM-III-R Antidepressant vs. antidepressant Himmelhoch 56 34/22 et al, 1991 [44] BD I, BD II Pilhatsch et al, 40 22/18 DSM-III-R 2010 [47] BD Fluoxetine mg/d vs. lithium mg/d vs. placebo Fluoxetine mg/d vs. imipramine, placebo Quetiapine 300 mg/d vs. quetiapine 600 mg/d vs. paroxetine 20 mg/d vs. placebo Paroxetine mg/d vs. imipramine mg/d vs. placebo Paroxetine vs. bupropion vs. mood stabilizer plus placebo Amitriptyline mg/d vs. L-sulpiride mg/d Citalopram mg/d vs. lamotrigine mg/d Risperidone 4 mg/d plus placebo vs. paroxetine 20 mg/d plus placebo Paroxetine 36 mg/d vs. mood stabilizer (lithium, divalproex) Imipramine mg/d vs. tranylcypromine mg/d Paroxetine mg/d vs. amitriptyline, mg/d Silverstone /91 DSM-III-R BD Moclobemide 450 ± 750 mg/d vs [51] imipramine 150 ± 250 mg/d 24 Olanzapine, lithium, valproate 8 Olanzapine, lithium, valproate 50 Short-term zolpidem ( 10 mg), lorazepam ( 2.0 mg), or trazodone ( 75 mg) 6 Lithium, chloral hydrate (0.5 to 1mg) for insomnia 8 Lorazepam (1 3 mg/d), zolpidem tartrate ( 10 mg/d), zaleplon ( 20 mg/d), zopiclone ( 7.5 mg/d), and chloral hydrate 50% reduction in baseline HAMD-17 score 50% reduction in baseline HAMD and MADRS score 50% reduction in baseline HAMD score 50% reduction in baseline HAMD score 50% decrease from baseline in MADRS total score HAM-D-17 9, or a final 17-item atypical symptom HAM-D 9 HAMD plus DSM-IV criteria, YMR scores 8 HAMD-17 9 or final DSM-IV, YMRS HAMD-17 9 scores 8 HAMD-17, YMRS HAMD-28, MADRS, YMRS DSM-IV: Diagnostic and Statistical Manual of Mental Disorders, fourth edition; DSM-III-R: Diagnostic and Statisti-cal Manual of Mental Disorders, third edition, revised; BD: bipolar disorder; BD I: bipolar I disorder, BD II: bipolar II disorder; NOS MD: Not otherwise specified, major depression; HAMD: Hamilton Depression Rating Scale; YMRS: Young Mania Rating Scale; MADRS: Montgomery-Asberg Depression Rating Scale; CGI: Clinical Global Impres-sions scale; SUM-D: Continuous symptom subscales for depression; SAS: Zung s Self-Rating Anxiety Scale; GAF: Global Assessment of Functioning scale. 5 HAM-D 8 10 Lithium Not defined HAMD-21 7 or CGI global improvement score 2 26 Mood Stabilizer 50% decrease from baseline in SUM-D 4 Lithium; lorazepam as a hypnotic at entry 50% reduction in HRSD-17 score 12 Mood stabilizer 50% decline in the MADRS 12 Mood stabilizer, lorazepam 3 mg/day 50% reduction in HAMD and CGI-S = 1 or 2 HAMD 14 plus DSM-IV criteria HAMD, YMRS Not defined Not defined HAMD, Raskin Depression Scale, CGI MADRS total score 12 Not defined MADRS, CGI, SDS at week 8 DSM IV, 50% improvement from baseline SUM-D score Not defined DSM IV HAMD-21, GCI MADRS, YMRS, SUM-D Not defined DSM-III-R HAMD, BDI, SAS, GAF MADRS score 8 Not defined HAMD, MADRS, YMRS, CGI HDRS score 7, DSM-IV YMRS 12; YMRS 8 also considered HAMD, BDI 6 Mood stabilizers Not defined Not defined Not defined HAMD-17, YMRS 6 Not reported 50% reduction in baseline HAMD score HAMD 7 and CGI 2 from baseline DSM-III-R HAMD-17, BDI, CGI 6 Lithium 50% reduction in HAMD-21 score HAMD21 score of 8 Not defined HAMD-21, CGI 8 Mood 50% decline in HAMD HAMD 10 YMRS 10 HAMD-17, MADRS, stabilizers CGI, YMRS
6 when compared with placebo in the short-term phase [two randomized controlled trials, n = 356, RR = 0.94, 95%CI: 0.71, 1.23, P = 0.64] [45-46] and in the long-term phase [one randomized controlled trial; n = 366, RR = 0.86, 95%CI: 0.60, 1.22, P = 0.40] [48] (Figure 3). [39-41, 48] Switching to mania: Four studies had defined switching to mania as DSM-III-R mania or hypomania, or a score 8 on YMRS, or HAMD 14. There was no significant difference in an increased risk of switching to mania [four randomized controlled trials, n = 462, RR = 1.06, 95%CI: 0.63, 1.78, P = 0.84] [40, 43, 45-46]. Long-term data also failed to show a significant difference [three randomized controlled trials, n = 433, RR = 0.81, 95%CI: 0.50, 1.32, P = 0.40] [39, 41, 48] (Figure 3). Figure 2 Risk of bias: low risk of bias (+), high risk of bias ( ), unclear risk of bias. Cohn et al [43] [n = 89, RR = 2.90, 95%CI: 1.26, 6.69] indicated a benefit for antidepressants, but McElroy et al [45] [n = 239, RR = 1.00; 95%CI: 0.70, 1.43] and Nemeroff et al [46] [n = 117, RR = 1.12, 95%CI: 0.68, 1.85] did not. The mean dose of antidepressant in the Cohn et al s study [43] (fluoxetine 62 mg/d) was higher than those in the McElroy et al [45] (paroxetine 20 mg/d) and Nemeroff et al s studies [46] (paroxetine 32 mg/d), which may contribute to the heterogeneity of the data. Excluding Cohn s study, the results were no longer heterogeneous, but the effect was equivocal [two randomized controlled trials, n = 356, RR = 1.04; 95%CI: 0.78, 1.39, P = 0.79]. Additionally, long-term data was equivocal between antidepressant and placebo [one randomized control trial, n = 366, RR= 0.85; 95%CI: 0.65, 1.13, P = 0.27] [48] (Figure 3). Clinical remission: In four studies [39-41, 46], remission was defined as the HAMD total score 7 or 9. One study [45] defined remission as the MADRS total score 12. One study [48] defined remission according to DSM-IV. Antidepressant medications did not offer statistical benefits Tolerability: Patients receiving short-term antidepressant treatment were slightly less likely to drop out compared with those receiving long-term treatment, but the effect did not show a significant difference [three randomized controlled trials, n = 445, RR = 0.78, 95%CI: 0.61,1.00, P = 0.05] [43, 45-46]. The discontinuation rate was 30.6% in the antidepressant group, and 40.4% in the placebo group. Long-term data did not show a significant difference [two randomized controlled trials, n = 421, RR = 1.41, 95%CI: 0.97, 2.05, P = 0.07] [41, 48]. There was no significant difference in an increased risk of relapse depression during long-term treatment between the antidepressant and placebo groups [two randomized controlled trials, n = 67, RR = 0.61, 95%CI: 0.37, 1.02, P = 0.06] [39, 41]. Suicidality: Suicidality occurred in two out of 118 patients who received short-term antidepressant treatment and in three out of 121 patients who received short-term other medications. There was no significant difference in suicidality between antideprassant group and placebo group [one randomized con-trolled trial, n = 239, RR = 0.68, CI: 0.12, 4.02, P = 0.67] [45]. Long-term data also failed to show a significant difference [one randomized controlled trial, n = 366, RR = 0.84, 95% CI: 0.23, 3.06, P = 0.79] [48], with suicidality occurring in four out of 179 patients who received antidepressant therapy and in five out of 187 patients who received placebo therapy. Antidepressant versus other medications There were no double-blind randomized controlled trials that provided data regarding long-term use of antidepressants versus other antipsychotics. Clinical response: In two trials [42, 50], response was defined as at least a 50% reduction in baseline HAMD. 6
7 Figure 3 Clinical response, remission, and switching to mania in patients with bipolar disorder who received antidepressant versus placebo treatment. 7
8 Figure 4 Clinical response, remission, and switching to mania in patients with bipolar disorder who received antidepressant therapy versus other medications. In one study [49], it was defined as at least a 50% reduction in MADRS. There was no significant difference in effect size between short-term antidepressant treatment and other medication treatments [three randomized controlled trials, n = 70, RR = 0.95, 95%CI: 0.68, 1.34, P = 0.78] [42, 49-50] (Figure 4). Clinical remission: There was no significant difference in clinical remission between short-term antidepressant treatment and other medication treatments [two randomized controlled trials, n = 40, RR = 2.00, 95%CI: 0.75, 5.33, P = 0.17] [49-50] (Figure 4). Switching to mania: There was no significant difference in an increased risk of switching to a manic episode between short-term antidepressant treatment and other medication treatments [three randomized controlled trials, [42, 49-50] n = 70, RR = 1.40, 95%CI: 0.29, 6.65, P = 0.67] (Figure 4). Tolerability: The rate of discontinuation was 19.6% in the antidepressant group and 27.5% in the other medication group. The antidepressants did not cause significantly more discontinuation rates than other medications [four randomized controlled trials, n = 97, RR = 0.73, 95%CI: 0.35, 1.50, P = 0.39] [42, 49-50, 52]. The incidences of relapse were equal between short-term antidepressant treatment and other medications [one randomized controlled trial, n = 20, RR = 0.50, 95%CI: 0.12, 2.14, P = 0.35] [49], being 20.0% and 40.0%, respectively. Suicidality: There were no studies in which data on suicidal-ity were described between antidepressant treatment and other medications. 8
9 Figure 5 Clinical response and switching to mania in patients with bipolar disorder who received antidepressant treatment versus antidepressant treatment. Antidepressant versus antidepressant Clinical response: There was no difference in clinical response between TCAs and monoamine oxidase inhibitors (MAOIs) [two randomized controlled trials, n = 212, RR = 0.91, 95%CI: 0.70, 1.19, P = 0.50] [44, 51], with significant heterogeneity (P = 0.005, I 2 = 87%). A suitable interpretation had not been found for the cause of this heterogeneity. There was no significant difference in effect of response rate between SSRI and TCA groups [one randomized controlled trial, n = 40, RR = 1.07, 95%CI: 0.75, 1.53, P = 0.71] [47] (Figure 5). Clinical remission: There were no short-term or long-term studies in which data on clinical remission were described. Switching to mania: There was no evidence of an increased risk of switching to a manic episode between TCA and MAOI treatments [two randomized controlled trials, n = 212, RR = 1.57, 95%CI: 0.67, 3.68, P = 0.30] [44, 51], and the same effect was observed in SSRI and TCA treatments [one randomized controlled trial, n = 40, RR = 3.63, 95%CI: 0.16, 84.11, P = 0.42] [47].The risk of switching to a manic episode was 11.7% for TCA treatment, 7.3% for MAOI treatment, and 5.6% for SSRI treatment (Figure 5). Tolerability: There was no significant difference in the rate of discontinuation between the TCA group and the MAOI group (26.2% vs. 26.6%) [two randomized controlled trials, n = 212, RR = 1.00, 95%CI: 0.64, 1.55, P = 0.99] [44, 51]. Similarly, one randomized controlled trial found no significant difference in the rate of discontinuation between SSRI and TAC treatments [n = 40, RR = 9
10 2.44, 95%CI: 0.50, 11.86, P = 0.27] [47]. One randomized controlled trial [44] showed that the incidence of relapse was similar between the MAOI group and TCA group [n = 56, RR = 1.00, 95%CI: 0.07, 15.21]. Suicidality: There were no studies in which data on suicidality were described. Sensitivity analysis Sensitivity analyses were conducted to examine the influence of pharmaceutically funded or affiliated studies on the estimated treatment effects. Two of the 14 trials were industry funded. Sensitivity analysis on the effects of bipolar subtype, adjunct mood stabilizer was also conducted. When these factors were taken into account, there was no change in the overall profile of estimated treatment effects. DISCUSSION In this meta-analysis, we tried to elucidate whether there is evidence for or against the clinical efficacy of antidepressants for the treatment of bipolar disorder, using a meta-analysis approach for double-blind randomized controlled trials. Effectiveness criteria including response, remission, and switching to mania, and safety criteria including discontinuation of the study for any reason, relapse and suicidality, probably reflected the most valuable outcome parameters for clinical practice. Comparison with previous studies The data are based on 11 short-term and three long-term double-blind randomized controlled trials published up to December Our analysis excluded several trials that have been cited in recent reviews [31]. One [53] was the single-blind randomized control trial, two of them [54-55] were trials on anti-depressants in comparison with psychiatrics, and another trial [56] compared bupropion with alpha-2 antagonist idazoxan, which did not meet our included criterion. Three new double-blind randomized controlled trials [41, 45, 47] published from 2009 to 2012 were added. Antidepressant efficacy The current study showed that antidepressants were not associated with a significant increase in efficacy compared with placebo or other pharmacologic treatments in the acute and maintenance phase therapy of bipolar disorder. In the current analysis, when we controlled for study design factors known to influence therapy effect, the point estimates indicated a slight, but not significant, benefit of antidepressants over placebo in short-term use regarding response. The present analysis was in line with an earlier meta-analysis by Sidor et al [31] that focused on trials of short-term use of antidepressants. In addition, our study did not suggest that remission of long-term antidepressant treatment appeared to be better than long-term placebo or other medication treatments. Recent studies [19] indicated that second-generation antipsychotics significantly improved depressive symptoms in patients with bipolar disorder and second-generation antipsychotics, and combined with second-generation antideressants, had an even more robust antidepressant effect. To avoid the risks of intervention bias, we narrowed our study to antidepressant monotherapy or antidepressant combined with mood stabilizer. Two open-label design studies that were excluded from this analysis found that the effect was in favor of antidepressants. Amsterdam and Sbults [57] compared the effectiveness of venlafaxine with lithium monotherapy in 83 patients with bipolar II disorder and found that antidepressant monotherapy was superior to lithium with a similar hypomanic symptom. A large-scale study [58] used olanzapine combined with fluoxetine for the treatment of bipolar disorder and found that fluoxetine was more effective than placebo without an increased risk of switching to mania. Contrary to open-label trails, double-blind randomized controlled trials included in this study failed to confirm the efficacy of short-term and long-term antidepressant treatment for the treatment of bipolar disorder. This suggests that the open-label design introduced a study bias, and future study designs should take methodology bias into account. In the present analysis, we do not have enough evidence to support that antidepressant treatments yield significantly higher response rate and remission rate than placebo, mood stabilizer, or antipsychotic treatments. Switching to mania The classes of antidepressants studied here, mostly SSRIs and TCAs, did not increase the risk of switching. This finding is consistent with another previous study [31]. The rates of switching to mania did not support the belief that switching to mania is a common complication of treatment with antidepressants in bipolar disorder in the short-term spans of 4 to12 weeks or in long-term spans of 26 to 50 weeks. Bond et al [59] found that the switch rate for bipolar I disorder was 14% and 7% for bipolar II disorder during antidepressant treatment in the short-term. This result suggests that the reported switch rate can be influenced by the ratio of bipolar II to bipolar I disorder patients included in a study. While the current study failed to separate bipolar II disorder and bipolar I disorder, the interpretation of the findings that anti- 10
11 depressants did not increase the risk of switching to mania from the study should be care-fully considered. Tolerability There was no significant difference in the risk of discontinuation among patients who received antidepressants, other antipsychotic and placebo treatments in doubleblind randomized controlled trials. The rate of discontinuation was 32% for short-term placebo treatment, which was higher than that reported in open-label trials using active drugs (24%). This difference is possibly attributable to the physician s and patient s perception of treatment effectiveness with the active drugs. Our study indicated that compared with short-term placebo treatment, antidepressant treatment tended to yield a slightly, but not significantly, lower discontinuation rate. Double-blind randomized controlled trials included in this study suggest that the use of antidepressants in the treatment of bipolar disorder did not increase the rate of discontinuation for any reason. In addition, there was no significant difference in relapse rate for mania or depressive episode between patients who received short-term or long-term antidepressant, placebo, and other medication treatments. Suicidality Few data exist regarding the risk for suicidality in patients receiving antidepressant treatment. No excessive risks were found among short-term antidepressant treatments. Many studies have suggested that antidepressants could cause a generally increased risk for suicidality in teenagers [60], while a recent review indicated that SSRIs decreased the risk for attempted or completed suicidality among adults [61]. The current meta-analyses are consistent with a Food and Drug Administration (FDA) data analysis that the risk of suicide is not in-creased in adults [62]. Differences between antidepressants Data from this study are inadequate to definitively favor one antidepressant over another antidepressant, and these data also demonstrated that there was no effect on response and remission between SSRIs, TCAs and MAOIs either in short-term or long-term application. Data from this study showed that although SSRIs have been proposed as an antidepressant in the treatment of bipolar disorder because of their lower switching rate than TCAs or MAOIs, there was no significant difference in an increased risk of switching to a manic episode between SSRI and TCA treatments in patients with bipolar disorder. These findings are consistent with those from previous studies [31-32]. Advantage of this analysis The major advantage of our analysis is the inclusion of double-blind randomized controlled trials to reduce the risks of study bias and confounding factors that influence interpretation of outcome. The previous study [31-32] has been criticized for methodological shortcomings, because they included trials with a high risk for bias and open-label designs. For the current meta-analysis, we retained more rigid methods and excluded studies with a high risk for bias or open-label designs and limited mixed-treatment comparisons of antidepressants and mood stabilizers or other antipsychotics. Furthermore, whenever possible, we used meta-analyses of head-tohead studies to determine the efficacy. Limitations The present study suffers from several limitations. First, the limitations of this study relate largely to the quality of the studies. Many studies reported incomplete descriptions of methodology and few reported on, for example, method of randomization, method of concealment, success, or blinding. It is important to acknowledge that to date there have been relatively few high quality double-blind randomized con-trolled trials published and that methodological limitations often reduce the validity of the extant studies. Second, publication bias is a concern for all meta-analyses. Selective availability of studies with positive results can seriously bias conclusions, particularly when a pharmaceutical company compares two of its own drugs (as in the case of olanzapine and fluoxetine). Third, a small number of studies limit the validity of statistical methods to explore publication bias, such as funnel plots. Fourth, the antidepressants in the study differ to a large extent in the way they affect neurotransmitter physiology, and lumping those into one category can obscure the more favorable effectiveness of individual drugs. In light of currently available data, there is strong support for future large double-blind randomized controlled trials to elucidate the role of short- and long-term use of antidepressants for the treatment of bipolar I disorder and bipolar II disorder. The roles of second-generation antidepressants combined with second-generation antipsychotics, as well as other combinations of antidepressants with lithium, anticonvulsants, or atypical antipsychotics, especially in longer-term follow-up, should be further evaluated in double-blind randomized controlled trials. Conlusion There remains a lack of definitive evidence regarding the efficacy of short-term and long-term antidepressant therapy for the treatment of bipolar disorder. Existing evidence does not warrant choosing an antidepressant as therapy for acute phase or maintenance phase bipolar disorder, although better tolerability and safety of antidepressants have been generally acknowledged. 11
12 REFERENCES [1] Bruffaerts R, Vilagut G, Demyttenaere K, et al. Role of common mental and physical disorders in partial disability around the world. Br J Psychiatry. 2012;200(6): [2] Kenneson A, Funderburk JS, Maisto SA. Risk factors for secondary substance use disorders in people with childhood and adoles-cent-onset bipolar disorder: Opportunities for prevention. Compr Psychiatry. in press. [3] Undurraga J, Baldessarini RJ, Valenti M, et al. Suicidal risk factors in bipolar I and II disorder patients. J Clin Psychiatry. 2012;73(6): [4] Grande I, Goikolea JM, de Dios C, et al. Occupational disability in bipolar disorder: analysis of predictors of being on severe disablement benefit (PREBIS study data). Acta Psychiatr Scand. 2013;127(5): [5] Ebmeier KP. Managing bipolar disorder in primary care. Practitioner. 2010;254(1729): [6] Ketter TA. Diagnostic features, prevalence, and impact of bipolar disorder. J Clin Psychiatry. 2010;71(6):e14. [7] Ferrari AJ, Saha S, McGrath JJ, et al. Health states for schizophrenia and bipolar disorder within the Global Burden of Disease 2010 Study. Popul Health Metr. 2012; 10(1):16. [8] Magalhaes PV, Kapczinski F, Nierenberg AA, et al. Illness burden and medical comorbidity in the Systematic Treatment Enhancement Program for Bipolar Disorder. Acta Psychiatr Scand. 2012;125(4): [9] Angst J, Gamma A, Bowden CL, et al. Evidence-based definitions of bipolar-i and bipolar-ii disorders among 5,635 patients with major depressive episodes in the Bridge Study: validity and comorbidity. Eur Arch Psychiatry Clin Neurosci. in press. [10] American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4 th ed. Washington, DC: American Psychiatric Association [11] Baek JH, Park DY, Choi J, et al. Differences between bipolar I and bipolar II disorders in clinical features, comorbidity, and family history. J Affect Disord. 2011;131(1-3): [12] Yatham LN, Fountoulakis KN, Rahman Z, et al. Efficacy of aripiprazole versus placebo as adjuncts to lithium or valproate in relapse prevention of manic or mixed episodes in bipolar I patients stratified by index manic or mixed episode. J Affect Disord. 2013;147(1-3): [13] Kemp DE, Hert MD, Rahman Z, et al. Investigation into the long-term metabolic effects of aripiprazole adjunctive to lithium, valproate, or lamotrigine. J Affect Disord. 2013; 148(1): [14] Fornaro M, Martino M, De Pasquale C, et al. The argument of antidepressant drugs in the treatment of bipolar depression: mixed evidence or mixed states? Expert Opin Pharmacother. 2012;13(14): [15] Grof P, Duffy A, Alda M, et al. Lithium response across generations. Acta Psychiatr Scand. 2009;120(5): [16] Cipriani A, Rendell J, Geddes JR. Olanzapine in the long-term treatment of bipolar disorder: a systematic review and meta-analysis. J Psychopharmacol. 2010;24(12): [17] Sanford M, Keating GM. Quetiapine: a review of its use in the management of bipolar depression. CNS Drugs. 2012; 26(5): [18] Fountoulakis KN, Kasper S, Andreassen O, et al. Efficacy of pharmacotherapy in bipolar disorder: a report by the WPA section on pharmacopsychiatry. Eur Arch Psychiatry Clin Neurosci. 2012;262 Suppl 1:1-48. [19] Citrome L. Olanzapine-fluoxetine combination for the treatment of bipolar depression. Expert Opin Pharmacother. 2011;12(17): [20] Swartz HA, Thase ME. Pharmacotherapy for the treatment of acute bipolar II depression: current evidence. J Clin Psychiatry. 2011;72(3): [21] Frankle W, Perlis R, Deckersbach T, et al. Bipolar depression: relationship between episode length and antidepressant treatment. Psychol Med. 2002;32(8): [22] Malhi GS, Tanious M, Das P, et al. The science and practice of lithium therapy. Aust N Z J Psychiatry. 2012; 46(3): [23] Yatham LN, Kennedy SH, Schaffer A, et al. Canadian Network for Mood and Anxiety Treatments (CANMAT) and International Society for Bipolar Disorders (ISBD) collaborative update of CANMAT guidelines for the management of patients with bipolar disorder: update Bipolar Disord. 2009;11(3): [24] Amsterdam JD, Wang G, Shults J. Venlafaxine monotherapy in bipolar type II depressed patients unresponsive to prior lithium monotherapy. Acta Psychiatr Scand. 2010;121(3): [25] Amsterdam JD, Luo L, Shults J. Efficacy and mood conversion rate during long-term fluoxetine v. lithium monotherapy in rapid- and non-rapid-cycling bipolar II disorder. Br J Psychiatry. 2013;202(4): [26] Yatham LN, Kennedy SH, Parikh SV, et al. Canadian Network for Mood and Anxiety Treatments (CANMAT) and International Society for Bipolar Disorders (ISBD) collaborative update of CANMAT guidelines for the management of patients with bipolar disorder: update Bipolar Disord. 2013;15(1):1-44. [27] Nivoli AM, Colom F, Murru A, et al. New treatment guidelines for acute bipolar depression: a systematic review. J Affect Disord. 2011;129(1-3): [28] Musetti L, Del Grande C, Marazziti D, et al. Treatment of bipolar depression. CNS Spectr. 2013:1-11. [29] Podawiltz A. A review of current bipolar disorder treatment guidelines. J Clin Psychiatry. 2012;73(3):e12. [30] Walpoth-Niederwanger M, Kemmler G, Grunze H, et al. Treat-ment patterns in inpatients with bipolar disorder at a psychiatric uni-versity hospital over a 9-year period: focus on mood stabilizers. Int Clin Psychopharmacol. 2012; 27(5): [31] Sidor MM, Macqueen GM. Antidepressants for the acute treatment of bipolar depression: a systematic review and meta-analysis. J Clin Psychiatry. 2011;72(2):
13 [32] Gijsman HJ, Geddes JR, Rendell JM, et al. Antidepressants for bipolar depression: a systematic review of randomized, controlled trials. Am J Psychiatry. 2004;161(9): [33] Wilson M. DSM-III and the transformation of American psychiatry: a history. Am J Psychiatry. 1993;150(3): [34] Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23: [35] Young RC, Biggs JT, Ziegler VE, et al. A rating scale for mania: reliability, validity and sensitivity. Br J Psychiatry. 1978;133: [36] Kirschenfeld JJ. A community medical education program in Montgomery. J Med Assoc State Ala. 1979;48(9):7-8. [37] Steinberg M. Interviewers Guide to the Structured Clinical Interview for DSM-IV Dissociative Disorders (SCID-D). Washington, DC: American Psychiatric Press [38] Higgins JP, Green S. Cochrane Handbook for Systematic Reviews of Interventions Version 5.0.1[updated September 2008]. NewYork: John Wiley & Sons, Inc [39] Amsterdam JD, Shults J. Fluoxetine monotherapy of bipolar type II and bipolar NOS major depression: a double-blind, placebo-substitution, continuation study. Int Clin Psychopharmacol. 2005;20(5): [40] Amsterdam JD, Shults J. A-comparison of fluoxetine, olanzapine, and combined fluoxetine plus olanzapine initial therapy of bipolar type I and type II major depression--lack of manic induction. J Affect Disord. 2005;87(1): [41] Amsterdam JD, Shults J. Efficacy and safety of long-term fluoxetine versus lithium monotherapy of bipolar II disorder: a randomized, double-blind, placebo-substitution study. Am J Psychiatry. 2010;167(7): [42] Bocchetta A, Bernardi F, Burrai C, et al. A double-blind study of L-sulpiride versus amitriptyline in lithium-maintained bipolar depres-sives. Acta Psychiatr Scand. 1993;88(6): [43] Cohn JB, Collins G, Ashbrook E, et al. A comparison of fluoxetine imipramine and placebo in patients with bipolar depressive disorder. Int Clin Psychopharmacol.1989;4(4): [44] Himmelhoch JM, Thase ME, Mallinger AG, et al. Tranylcypromine versus imipramine in anergic bipolar depression. Am J Psychiatry. 1991;148(7): [45] McElroy SL, Weisler RH, Chang W, et al. A double-blind, placebo-controlled study of quetiapine and paroxetine as monotherapy in adults with bipolar depression (EM- BOLDEN II). J Clin Psychiatry. 2010;71(2): [46] Nemeroff CB, Evans DL, Gyulai L, et al. Double-blind, placebo-controlled comparison of imipramine and paroxetine in the treatment of bipolar depression. Am J Psychiatry. 2001;158(6): [47] Pilhatsch M, Wolf R, Winter C, et al. Comparison of paroxetine and amitriptyline as adjunct to lithium maintenance therapy in bipolar depression: a reanalysis of a randomized, double-blind study. J Affect Disord. 2010; 126(3): [48] Sachs GS, Nierenberg AA, Calabrese JR, et al. Effectiveness of adjunctive antidepressant treatment for bipolar depression. N Engl J Med. 2007;356(17): [49] Schaffer A, Zuker P, Levitt A. Randomized, double-blind pilot trial comparing lamotrigine versus citalopram for the treatment of bipolar depression. J Affect Disord. 2006; 96(1-2): [50] Shelton RC, Stahl SM. Risperidone and paroxetine given singly and in combination for bipolar depression. J Clin Psychiatry. 2004;65(12): [51] Silverstone T. Moclobemide vs. imipramine in bipolar depression: a multicentre double-blind clinical trial. Acta Psychiatr Scand. 2001;104(2): [52] Young LT, Joffe RT, Robb JC, et al. Double-blind comparison of addition of a second mood stabilizer versus an antidepressant to an initial mood stabilizer for treatment of patients with bipolar depres-sion. Am J Psychiatry. 2000;157(1): [53] Post RM, Altshuler LL, Leverich GS, et al. Mood switch in bipolar depression: comparison of adjunctive venlafaxine, bupropion and sertraline. Br J Psychiatry. 2006;189: [54] Brown EB, McElroy SL, Keck PE Jr, et al. A 7-week, randomized, double-blind trial of olanzapine/fluoxetine combination versus lamotrigine in the treatment of bipolar I depression. J Clin Psychiatry. 2006;67(7): [55] Tohen M, Vieta E, Calabrese J, et al. Efficacy of olanzapine and olanzapine-fluoxetine combination in the treatment of bipolar I de-pression. Arch Gen Psychiatry. 2003;60(11): [56] Grossman F, Potter WZ, Brown EA, et al. A double-blind study comparing idazoxan and bupropion in bipolar depressed patients. J Affect Disord. 1999;56(2-3): [57] Amsterdam JD, Shults J. Comparison of short-term venlafaxine versus lithium monotherapy for bipolar II major depressive episode: a randomized open-label study. J Clin Psychopharmacol. 2008;28(2): [58] Tamayo JM, Sutton VK, Mattei MA, et al. Effectiveness and safety of the combination of fluoxetine and olanzapine in outpatients with bipolar depression: an open-label, randomized, flexible-dose study in Puerto Rico. J Clin Psychopharmacol. 2009;29(4): [59] Bond DJ, Noronha MM, Kauer-Sant Anna M, et al. Antidepressant-associated mood elevations in bipolar II disorder compared with bipolar I disorder and major depressive disorder: a systematic review and meta-analysis. J Clin Psychiatry. 2008;69(10): [60] Wagner KD, Asarnow JR, Vitiello B, et al. Out of the black box: treatment of resistant depression in adolescents and the antidepressant controversy. J Child Adolesc Psychopharmacol. 2012;22(1):5-10. [61] Barbui C, Esposito E, Cipriani A. Selective serotonin reuptake inhibitors and risk of suicide: a systematic review of observational studies. CMAJ. 2009;180(3): [62] Valluri S, Zito JM, Safer DJ, et al. Impact of the 2004 Food and Drug Administration pediatric suicidality warning on antidepressant and psychotherapy treatment for newonset depression. Med Care. 2010;48(11): (Reviewed by Gautam B, Haase R, Wang GQ, Li NX) (Edited by Wang LM, Li CH, Song LP, Liu WJ, Zhao M) 13
The Pharmacological Management of Bipolar Disorder: An Update
 Psychobiology Research Group The Pharmacological Management of Bipolar Disorder: An Update R. Hamish McAllister-Williams, MD, PhD, FRCPsych Reader in Clinical Psychopharmacology Newcastle University Hon.
Psychobiology Research Group The Pharmacological Management of Bipolar Disorder: An Update R. Hamish McAllister-Williams, MD, PhD, FRCPsych Reader in Clinical Psychopharmacology Newcastle University Hon.
Treatment of Bipolar disorder
 8/6/215 Treatment of Bipolar disorder Pichai Ittasakul, M.D. Department of Psychiatry, Ramathibodi Hospital, Mahidol University Bipolar disorder Manic-depressive Illness. is characterized by the occurrence
8/6/215 Treatment of Bipolar disorder Pichai Ittasakul, M.D. Department of Psychiatry, Ramathibodi Hospital, Mahidol University Bipolar disorder Manic-depressive Illness. is characterized by the occurrence
Your footnote
 MANIA Your footnote Your footnote Cipriani A, Barbui C, Salanti G et al. Comparative efficacy and acceptability of antimanic drugs in acute mania: a multiple-treatments meta-analysis. The Lancet 2011;
MANIA Your footnote Your footnote Cipriani A, Barbui C, Salanti G et al. Comparative efficacy and acceptability of antimanic drugs in acute mania: a multiple-treatments meta-analysis. The Lancet 2011;
Challenges in identifying and treating bipolar depression: a guide
 Challenges in identifying and treating bipolar depression: a guide Dr. Paul Stokes Clinical Senior Lecturer, Centre for Affective Disorders, Department of Psychological Medicine Overview Challenges in
Challenges in identifying and treating bipolar depression: a guide Dr. Paul Stokes Clinical Senior Lecturer, Centre for Affective Disorders, Department of Psychological Medicine Overview Challenges in
A systematic review of the evidence on the treatment of rapid cycling bipolar disorder
 Bipolar Disorders 2013: 15: 115 137 Review Article Ó 2013 John Wiley and Sons A/S Published by Blackwell Publishing Ltd. BIPOLAR DISORDERS A systematic review of the evidence on the treatment of rapid
Bipolar Disorders 2013: 15: 115 137 Review Article Ó 2013 John Wiley and Sons A/S Published by Blackwell Publishing Ltd. BIPOLAR DISORDERS A systematic review of the evidence on the treatment of rapid
Clinical Guideline for the Management of Bipolar Disorder in Adults
 Clinical Guideline for the Management of Bipolar Disorder in Adults Goal: To improve the quality of life of adults with bipolar disorder Identification and Treatment of Bipolar Disorder Criteria for Diagnosis:
Clinical Guideline for the Management of Bipolar Disorder in Adults Goal: To improve the quality of life of adults with bipolar disorder Identification and Treatment of Bipolar Disorder Criteria for Diagnosis:
Bipolar Disorder in Youth
 Bipolar Disorder in Youth Janet Wozniak, M.D. Associate Professor of Psychiatry Director, Pediatric Bipolar Disorder Research Program Harvard Medical School Massachusetts General Hospital Pediatric-Onset
Bipolar Disorder in Youth Janet Wozniak, M.D. Associate Professor of Psychiatry Director, Pediatric Bipolar Disorder Research Program Harvard Medical School Massachusetts General Hospital Pediatric-Onset
Florida Best Practice Medication Guidelines Principles of Practice for Adults
 http://flmedicaidbh.fmhi.usf.edu Florida Best Practice Medication Guidelines Principles of Practice for Adults 1. Goal of the Guidelines Persistent gaps exist in the quality of mental health care delivered
http://flmedicaidbh.fmhi.usf.edu Florida Best Practice Medication Guidelines Principles of Practice for Adults 1. Goal of the Guidelines Persistent gaps exist in the quality of mental health care delivered
3. Depressione unipolare
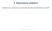 3. Depressione unipolare Depressione unipolare con mancata risposta al trattamento con SSRI Question: Should switching from SSRIs to another antidepressant class vs switching within class (SSRIs) be used
3. Depressione unipolare Depressione unipolare con mancata risposta al trattamento con SSRI Question: Should switching from SSRIs to another antidepressant class vs switching within class (SSRIs) be used
Bipolar Disorder A Focus on Depression
 clinical practice Bipolar Disorder A Focus on Depression Mark A. Frye, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies
clinical practice Bipolar Disorder A Focus on Depression Mark A. Frye, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies
Treatment Options for Bipolar Disorder Contents
 Keeping Your Balance Treatment Options for Bipolar Disorder Contents Medication Treatment for Bipolar Disorder 2 Page Medication Record 5 Psychosocial Treatments for Bipolar Disorder 6 Module Summary 8
Keeping Your Balance Treatment Options for Bipolar Disorder Contents Medication Treatment for Bipolar Disorder 2 Page Medication Record 5 Psychosocial Treatments for Bipolar Disorder 6 Module Summary 8
Management of Bipolar Depression
 Management of Bipolar Depression Haresh M. Tharwani, M.D. Associate Clinical Professor Medical Director-DRH & Duke Psychiatry Specialty Clinic of Cary, N.C. Bipolar Disorders (Manic-Depressive illness)
Management of Bipolar Depression Haresh M. Tharwani, M.D. Associate Clinical Professor Medical Director-DRH & Duke Psychiatry Specialty Clinic of Cary, N.C. Bipolar Disorders (Manic-Depressive illness)
Practical Guide to Long-Term Pharmacotherapy in Bipolar Disorder: An Updated Synthesis of Current Clinical Guidelines
 SECOND-GENERATION ANTIPSYCHOTICS IN BIPOLAR DISORDER Practical Guide to Long-Term Pharmacotherapy in Bipolar Disorder: An Updated Synthesis of Current s Flavio Guzman, MD Editor Psychopharmacology Institute
SECOND-GENERATION ANTIPSYCHOTICS IN BIPOLAR DISORDER Practical Guide to Long-Term Pharmacotherapy in Bipolar Disorder: An Updated Synthesis of Current s Flavio Guzman, MD Editor Psychopharmacology Institute
Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A
 Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A Faculty/Presenter Disclosures Faculty: Mike Allan Salary: College
Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A Faculty/Presenter Disclosures Faculty: Mike Allan Salary: College
September 26 28, 2013 Westin Tampa Harbour Island. Co-sponsored by
 September 26 28, 2013 Westin Tampa Harbour Island Co-sponsored by Best Practices in the Management of Bipolar Disorder Robert M. A. Hirschfeld, MD University of Texas Medical Branch Galveston, TX Peter
September 26 28, 2013 Westin Tampa Harbour Island Co-sponsored by Best Practices in the Management of Bipolar Disorder Robert M. A. Hirschfeld, MD University of Texas Medical Branch Galveston, TX Peter
CHAIR SUMMIT 7TH ANNUAL #CHAIR2014. Master Class for Neuroscience Professional Development. September 11 13, Westin Tampa Harbour Island
 #CHAIR2014 7TH ANNUAL CHAIR SUMMIT Master Class for Neuroscience Professional Development September 11 13, 2014 Westin Tampa Harbour Island Sponsored by #CHAIR2014 Bipolar Depression: Putting the End Goal
#CHAIR2014 7TH ANNUAL CHAIR SUMMIT Master Class for Neuroscience Professional Development September 11 13, 2014 Westin Tampa Harbour Island Sponsored by #CHAIR2014 Bipolar Depression: Putting the End Goal
Multistate Outcome Analysis of Treatment MOAT
 Multistate Outcome Analysis of Treatment MOAT Charles L. Bowden, M.D. Presented with Fond Memories of an Outstanding Statistician and Investigative Scientist Andy Leon Design contributors to low generalizability
Multistate Outcome Analysis of Treatment MOAT Charles L. Bowden, M.D. Presented with Fond Memories of an Outstanding Statistician and Investigative Scientist Andy Leon Design contributors to low generalizability
Comparative efficacy and acceptability of drug treatments for bipolar depression: a multiple-treatments meta-analysis
 Acta Psychiatr Scand 2014: 130: 452 469 All rights reserved DOI: 10.1111/acps.12343 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd ACTA PSYCHIATRICA SCANDINAVICA Meta-analysis Comparative
Acta Psychiatr Scand 2014: 130: 452 469 All rights reserved DOI: 10.1111/acps.12343 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd ACTA PSYCHIATRICA SCANDINAVICA Meta-analysis Comparative
Bipolar Depression: Engaging the Patient. Mark Frye, MD Mayo Clinic Rochester, MN
 Bipolar Depression: Engaging the Patient Mark Frye, MD Mayo Clinic Rochester, MN Mark Frye, MD Disclosures Research/Grants: AssureRX Health Inc.; Janssen Research & Development, LLC; Mayo Foundation for
Bipolar Depression: Engaging the Patient Mark Frye, MD Mayo Clinic Rochester, MN Mark Frye, MD Disclosures Research/Grants: AssureRX Health Inc.; Janssen Research & Development, LLC; Mayo Foundation for
Class Update: Oral Antipsychotics
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
1 1 Evidence-based pharmacotherapy of major depressive disorder. Michael J. Ostacher, Jeffrey Huffman, Roy Perlis, and Andrew A.
 1 1 Evidence-based pharmacotherapy of major depressive disorder Michael J. Ostacher, Jeffrey Huffman, Roy Perlis, and Andrew A. Nierenberg Massachusetts General Hospital and Harvard University, Boston,
1 1 Evidence-based pharmacotherapy of major depressive disorder Michael J. Ostacher, Jeffrey Huffman, Roy Perlis, and Andrew A. Nierenberg Massachusetts General Hospital and Harvard University, Boston,
The Challenge of Treatment in Bipolar Depression: Evidence from Clinical Guidelines, Treatment Recommendations and Complex Treatment Situations
 53 The Challenge of Treatment in Bipolar Depression: Evidence from Clinical Guidelines, Treatment Recommendations and Complex Treatment Situations Authors S. Köhler 1, S. Gaus 1, T. Bschor 2, 3 Affiliations
53 The Challenge of Treatment in Bipolar Depression: Evidence from Clinical Guidelines, Treatment Recommendations and Complex Treatment Situations Authors S. Köhler 1, S. Gaus 1, T. Bschor 2, 3 Affiliations
35-year-old woman with Hx of BPII Dx; currently separated from husband; has 1 child
 Stephen M. Strakowski, MD Chart Review: Bipolar Disorder PATIENT INFO 35 Age: Female Sex: 35-year-old woman with Hx of BPII Dx; currently separated from husband; has 1 child Background: SI and hospitalization
Stephen M. Strakowski, MD Chart Review: Bipolar Disorder PATIENT INFO 35 Age: Female Sex: 35-year-old woman with Hx of BPII Dx; currently separated from husband; has 1 child Background: SI and hospitalization
Antipsychotics in Bipolar
 Use of Second-Generation Antipsychotics in Bipolar Disorder: A Practical Guide Flavio Guzman, MD Editor Psychopharmacology Institute This practical guide is an update on the use of second-generation antipsychotics
Use of Second-Generation Antipsychotics in Bipolar Disorder: A Practical Guide Flavio Guzman, MD Editor Psychopharmacology Institute This practical guide is an update on the use of second-generation antipsychotics
Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A
 Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A Faculty/Presenter Disclosures Faculty: Mike Allan Salary: College
Is Depression management getting you down? G. Michael Allan Director Programs and Practice Support, CFPC Professor, Family Med, U of A Faculty/Presenter Disclosures Faculty: Mike Allan Salary: College
University of Groningen. Lamotrigine in bipolar depression Loos, Marcus Lambertus Maria van der
 University of Groningen Lamotrigine in bipolar depression Loos, Marcus Lambertus Maria van der IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Lamotrigine in bipolar depression Loos, Marcus Lambertus Maria van der IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Resubmission. Scottish Medicines Consortium
 Scottish Medicines Consortium Resubmission aripiprazole 5mg, 10mg, 15mg, 0mg tablets; 10mg, 15mg orodispersible tablets; 1mg/mL oral solution (Abilify ) No. (498/08) Bristol-Myers Squibb Pharmaceuticals
Scottish Medicines Consortium Resubmission aripiprazole 5mg, 10mg, 15mg, 0mg tablets; 10mg, 15mg orodispersible tablets; 1mg/mL oral solution (Abilify ) No. (498/08) Bristol-Myers Squibb Pharmaceuticals
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 18 February 2009
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 February 2009 ABILIFY 5 mg tablets, pack of 28 (CIP: 364 069-7) ABILIFY 10 mg tablets, pack of 28 (CIP: 364 073-4)
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 February 2009 ABILIFY 5 mg tablets, pack of 28 (CIP: 364 069-7) ABILIFY 10 mg tablets, pack of 28 (CIP: 364 073-4)
Improving the Recognition and Treatment of Bipolar Depression
 Handout for the Neuroscience Education Institute (NEI) online activity: Improving the Recognition and Treatment of Bipolar Depression Learning Objectives Apply evidence-based tools that aid in differentiating
Handout for the Neuroscience Education Institute (NEI) online activity: Improving the Recognition and Treatment of Bipolar Depression Learning Objectives Apply evidence-based tools that aid in differentiating
Effectiveness of psychotropic medications in the maintenance phase of bipolar disorder: a meta-analysis of randomized controlled trials
 International Journal of Neuropsychopharmacology (2011), 14, 1029 1049. f CINP 2011 doi:10.1017/s1461145711000885 Effectiveness of psychotropic medications in the maintenance phase of bipolar disorder:
International Journal of Neuropsychopharmacology (2011), 14, 1029 1049. f CINP 2011 doi:10.1017/s1461145711000885 Effectiveness of psychotropic medications in the maintenance phase of bipolar disorder:
Where to from Here? Evidence-Based Strategies for Treatment of Refractory Depression
 Where to from Here? Evidence-Based Strategies for Treatment of Refractory Depression Michael D. Jibson, MD, PhD Professor of Psychiatry University of Michigan Major Depression #1 WHO cause of disability
Where to from Here? Evidence-Based Strategies for Treatment of Refractory Depression Michael D. Jibson, MD, PhD Professor of Psychiatry University of Michigan Major Depression #1 WHO cause of disability
What s new in the treatment of bipolar disorder?
 What s new in the treatment of bipolar disorder? Dr. David Cousins MRC Clinician Scientist Institute of Neuroscience Newcastle University NCMD 2017 What s new in the treatment of bipolar disorder? Dr.
What s new in the treatment of bipolar disorder? Dr. David Cousins MRC Clinician Scientist Institute of Neuroscience Newcastle University NCMD 2017 What s new in the treatment of bipolar disorder? Dr.
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
PDF created with pdffactory Pro trial version
 با ی د ر ا ر وه روا ز ش ی دا ه ع وم ش ی ا ان Treatment Challenges in BD Major depressive episode Mixed states= 20% Rapid cycling= 18% (annually), 31.5% (lifetime) Psychiatric Comorbidity (substance abuse,
با ی د ر ا ر وه روا ز ش ی دا ه ع وم ش ی ا ان Treatment Challenges in BD Major depressive episode Mixed states= 20% Rapid cycling= 18% (annually), 31.5% (lifetime) Psychiatric Comorbidity (substance abuse,
resources/guidelines-policies/locg.html
 BIPOLAR AND RELATED DISORDERS Optum Coverage Determination Guideline Policy Number: BH803BPD0518 Effective Date: May 9, 2018 Table of Contents Page BENEFIT CONSIDERATIONS...1 COVERAGE RATIONALE...1 EVIDENCE-BASED
BIPOLAR AND RELATED DISORDERS Optum Coverage Determination Guideline Policy Number: BH803BPD0518 Effective Date: May 9, 2018 Table of Contents Page BENEFIT CONSIDERATIONS...1 COVERAGE RATIONALE...1 EVIDENCE-BASED
Objectives. DSM-V Changes: Elimination of Multiaxial Diagnostic System
 Conflicts of Interest I have no conflicts to disclose. 2014 Updates to the Updates in Pharmacotherapy Webinar Psychiatry Updates for Pharmacotherapy Specialists Jacintha S. Cauffield, Pharm.D., BCPS Associate
Conflicts of Interest I have no conflicts to disclose. 2014 Updates to the Updates in Pharmacotherapy Webinar Psychiatry Updates for Pharmacotherapy Specialists Jacintha S. Cauffield, Pharm.D., BCPS Associate
Suitable dose and duration of fluvoxamine administration to treat depression
 PCN Psychiatric and Clinical Neurosciences 1323-13162003 Blackwell Science Pty Ltd 572April 2003 1098 Dose and duration of fluvoxamine S. Morishita and S. Arita 10.1046/j.1323-1316.2002.01098.x Original
PCN Psychiatric and Clinical Neurosciences 1323-13162003 Blackwell Science Pty Ltd 572April 2003 1098 Dose and duration of fluvoxamine S. Morishita and S. Arita 10.1046/j.1323-1316.2002.01098.x Original
Medication for Anxiety and Depression. PJ Cowen Department of Psychiatry, University of Oxford
 Medication for Anxiety and Depression PJ Cowen Department of Psychiatry, University of Oxford Topics Medication for anxiety disorders Medication for first line depression treatment Medication for resistant
Medication for Anxiety and Depression PJ Cowen Department of Psychiatry, University of Oxford Topics Medication for anxiety disorders Medication for first line depression treatment Medication for resistant
Guilt Suicidality. Depression Co-Occurs with Medical Illness The rate of major depression among those with medical illness is significant.
 1-800-PSYCH If you are obsessive-compulsive, dial 1 repeatedly If you are paranoid-delusional, dial 2 and wait, your call is being traced If you are schizophrenic, a little voice will tell you what number
1-800-PSYCH If you are obsessive-compulsive, dial 1 repeatedly If you are paranoid-delusional, dial 2 and wait, your call is being traced If you are schizophrenic, a little voice will tell you what number
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Šagud M., Pivac N., Mustapić M., Nedić G., Mihaljević Peleš A., Kramarić M., Jakovljević M., Muck-Šeler D. (2008) The effect of lamotrigine on platelet serotonin concentration
Središnja medicinska knjižnica Šagud M., Pivac N., Mustapić M., Nedić G., Mihaljević Peleš A., Kramarić M., Jakovljević M., Muck-Šeler D. (2008) The effect of lamotrigine on platelet serotonin concentration
Clinical Perspective on Conducting TRD Studies. Hans Eriksson, M.D., Ph.D., M.B.A. Chief Medical Specialist, H. Lundbeck A/S Valby, Denmark
 Clinical Perspective on Conducting TRD Studies Hans Eriksson, M.D., Ph.D., M.B.A. Chief Medical Specialist, H. Lundbeck A/S Valby, Denmark Overview of Presentation Treatment-Resistant Depression (TRD)
Clinical Perspective on Conducting TRD Studies Hans Eriksson, M.D., Ph.D., M.B.A. Chief Medical Specialist, H. Lundbeck A/S Valby, Denmark Overview of Presentation Treatment-Resistant Depression (TRD)
The Comparison of the Effectiveness of Thiothixene and Risperidone as a Combination with Lithium for the Treatment of Patients with Bipolar Disorder
 Zahedan Journal of Research in Medical Sciences Journal homepage: www.zjrms.ir The Comparison of the Effectiveness of Thiothixene and Risperidone as a Combination with Lithium for the Treatment of Patients
Zahedan Journal of Research in Medical Sciences Journal homepage: www.zjrms.ir The Comparison of the Effectiveness of Thiothixene and Risperidone as a Combination with Lithium for the Treatment of Patients
Comprehensive Pharmacologic Management of Bipolar Depression Alexander McGirr, MD, MSc 1 David J. Bond, MD, PhD 2,*
 Current Treatment Options in Psychiatry (2014) 1:263 277 DOI 10.1007/s40501-014-0017-2 Mood Disorders (AH Young, Section Editor) Comprehensive Pharmacologic Management of Bipolar Depression Alexander McGirr,
Current Treatment Options in Psychiatry (2014) 1:263 277 DOI 10.1007/s40501-014-0017-2 Mood Disorders (AH Young, Section Editor) Comprehensive Pharmacologic Management of Bipolar Depression Alexander McGirr,
Treating treatment resistant depression
 Treating treatment resistant depression These slides are the intellectual property of Ian Anderson and must not be reproduced Ian Anderson Neuroscience and Psychiatry Unit University of Manchester and
Treating treatment resistant depression These slides are the intellectual property of Ian Anderson and must not be reproduced Ian Anderson Neuroscience and Psychiatry Unit University of Manchester and
Agomelatine versus placebo: A meta-analysis of published and unpublished trials
 Agomelatine versus placebo: A meta-analysis of published and unpublished trials (Protocol for a systematic review, Ulm, January 17, 2011) Markus Kösters, Andrea Cipriani, Giuseppe Guaiana, Thomas Becker
Agomelatine versus placebo: A meta-analysis of published and unpublished trials (Protocol for a systematic review, Ulm, January 17, 2011) Markus Kösters, Andrea Cipriani, Giuseppe Guaiana, Thomas Becker
The armamentarium of treatments for bipolar disorder: a review of the literature
 International Journal of Neuropsychopharmacology (2007), 10, 411 431. Copyright f 2006 CINP doi:10.1017/s1461145706007413 The armamentarium of treatments for bipolar disorder: a review of the literature
International Journal of Neuropsychopharmacology (2007), 10, 411 431. Copyright f 2006 CINP doi:10.1017/s1461145706007413 The armamentarium of treatments for bipolar disorder: a review of the literature
Pharmacological Treatment of Bipolar Depression: Qualitative Systematic Review of Double-Blind Randomized Clinical Trials
 Psychiatr Q (2012) 83:161 175 DOI 10.1007/s11126-011-9191-1 ORIGINAL PAPER Pharmacological Treatment of Bipolar Depression: Qualitative Systematic Review of Double-Blind Randomized Clinical Trials Lucas
Psychiatr Q (2012) 83:161 175 DOI 10.1007/s11126-011-9191-1 ORIGINAL PAPER Pharmacological Treatment of Bipolar Depression: Qualitative Systematic Review of Double-Blind Randomized Clinical Trials Lucas
Efficacy of modern antipsychotics in placebo-controlled trials in bipolar depression: a meta-analysis
 International Journal of Neuropsychopharmacology (2010), 13, 5 14. Copyright f CINP 2009 doi:10.1017/s1461145709990344 Efficacy of modern antipsychotics in placebo-controlled trials in bipolar depression:
International Journal of Neuropsychopharmacology (2010), 13, 5 14. Copyright f CINP 2009 doi:10.1017/s1461145709990344 Efficacy of modern antipsychotics in placebo-controlled trials in bipolar depression:
Department of Psychiatry & Behavioral Sciences. University of Texas Medical Branch
 Depression in Childhood: Advances and Controversies in Treatment Karen Dineen Wagner, MD, PhD Marie B. Gale Centennial Professor & Vice Chair Department of Psychiatry & Behavioral Sciences Director, Division
Depression in Childhood: Advances and Controversies in Treatment Karen Dineen Wagner, MD, PhD Marie B. Gale Centennial Professor & Vice Chair Department of Psychiatry & Behavioral Sciences Director, Division
Augmentation and Combination Strategies in Antidepressants treatment of Depression
 Augmentation and Combination Strategies in Antidepressants treatment of Depression Byung-Joo Ham, M.D. Department of Psychiatry Korea University College of Medicine Background The response rates reported
Augmentation and Combination Strategies in Antidepressants treatment of Depression Byung-Joo Ham, M.D. Department of Psychiatry Korea University College of Medicine Background The response rates reported
Mood Disorders.
 Mood Disorders Shamim Nejad, MD Medical Director, Psycho-Oncology Services Swedish Cancer Institute Swedish Medical Center Seattle, Washington Shamim.Nejad@swedish.org Disclosures Neither I nor my spouse/partner
Mood Disorders Shamim Nejad, MD Medical Director, Psycho-Oncology Services Swedish Cancer Institute Swedish Medical Center Seattle, Washington Shamim.Nejad@swedish.org Disclosures Neither I nor my spouse/partner
HHS Public Access Author manuscript Bipolar Disord. Author manuscript; available in PMC 2016 June 01.
 A single infusion of ketamine improves depression scores in patients with anxious bipolar depression Dawn F Ionescu a,b, David A Luckenbaugh c, Mark J Niciu c, Erica M Richards c, and Carlos A Zarate Jr
A single infusion of ketamine improves depression scores in patients with anxious bipolar depression Dawn F Ionescu a,b, David A Luckenbaugh c, Mark J Niciu c, Erica M Richards c, and Carlos A Zarate Jr
SOMEWHERE OVER THE RAINBOW: RECOMMENDATIONS FOR THE DIAGNOSIS AND TREATMENT OF DEPRESSIVE MIXED STATES
 SOMEWHERE OVER THE RAINBOW: RECOMMENDATIONS FOR THE DIAGNOSIS AND TREATMENT OF DEPRESSIVE MIXED STATES Learning Objectives Impart the importance of screening for the presence of mixed features and family
SOMEWHERE OVER THE RAINBOW: RECOMMENDATIONS FOR THE DIAGNOSIS AND TREATMENT OF DEPRESSIVE MIXED STATES Learning Objectives Impart the importance of screening for the presence of mixed features and family
Manual of Clinical Psychopharmacology
 Manual of Clinical Psychopharmacology Fourth Edition Alan F. Schatzberg, M.D. Kenneth T. Norris, Jr., Professor and Chairman, Department of Psychiatry and Behavioral Sciences, Stanford University School
Manual of Clinical Psychopharmacology Fourth Edition Alan F. Schatzberg, M.D. Kenneth T. Norris, Jr., Professor and Chairman, Department of Psychiatry and Behavioral Sciences, Stanford University School
Lithium in bipolar disorders.
 Lithium in bipolar disorders. S. Mehdi Samimi Ardestani M.D. Department of Psychiatry, Shahid Beheshti University of Medical Science, Behavioral science research center Iranian psychiatric association,
Lithium in bipolar disorders. S. Mehdi Samimi Ardestani M.D. Department of Psychiatry, Shahid Beheshti University of Medical Science, Behavioral science research center Iranian psychiatric association,
Clinical Significance of Anxiety in Depressed Patients Selecting an Antidepressant
 The Clinical Significance of Anxiety Disorders and the DSM-5 Anxious Distress Specifier in Depressed Patients Clinical Significance of Anxiety in Depressed Patients Selecting an Antidepressant Rhode Island
The Clinical Significance of Anxiety Disorders and the DSM-5 Anxious Distress Specifier in Depressed Patients Clinical Significance of Anxiety in Depressed Patients Selecting an Antidepressant Rhode Island
Switch Phenomenon in Bipolar Disorders: What is it?
 Review Article Anand Bhogaraju Professor, Dept. of Psychiatry, MRIMS, Hyderabad, Telangana Email: anand6121957@gmail.com Abstract The phenomenon of Affective switch process is not well understood. It is
Review Article Anand Bhogaraju Professor, Dept. of Psychiatry, MRIMS, Hyderabad, Telangana Email: anand6121957@gmail.com Abstract The phenomenon of Affective switch process is not well understood. It is
BIPOLAR DISORDERS DIAGNOSTIC AND TREATMENT ISSUES RICHARD RIES MD
 Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences BIPOLAR DISORDERS DIAGNOSTIC AND TREATMENT ISSUES RICHARD RIES MD PROFESSOR DEPARTMENT OF PSYCHIATRY UNIVERSITY
Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences BIPOLAR DISORDERS DIAGNOSTIC AND TREATMENT ISSUES RICHARD RIES MD PROFESSOR DEPARTMENT OF PSYCHIATRY UNIVERSITY
Psychopharmacology. Psychopharmacology. Hamish McAllister-Williams Reader in Clinical. Department of Psychiatry, RVI
 Regional Affective Disorders Service Psychopharmacology Northumberland, Tyne and Wear NHS Trust Hamish McAllister-Williams Reader in Clinical Psychopharmacology Department of Psychiatry, RVI Intro NOT
Regional Affective Disorders Service Psychopharmacology Northumberland, Tyne and Wear NHS Trust Hamish McAllister-Williams Reader in Clinical Psychopharmacology Department of Psychiatry, RVI Intro NOT
Drug Surveillance 1.
 22 * * 3 1 2 3. 4 Drug Surveillance 1. 6-9 2 3 DSM-IV Anxious depression 4 Drug Surveillance GPRD A. (TCA) (SSRI) (SNRI) 20-77 - SSRI 1999 SNRI 2000 5 56 80 SSRI 1 1999 2005 2 2005 92.4, 2010 1999 3 1
22 * * 3 1 2 3. 4 Drug Surveillance 1. 6-9 2 3 DSM-IV Anxious depression 4 Drug Surveillance GPRD A. (TCA) (SSRI) (SNRI) 20-77 - SSRI 1999 SNRI 2000 5 56 80 SSRI 1 1999 2005 2 2005 92.4, 2010 1999 3 1
Depression. University of Illinois at Chicago College of Nursing
 Depression University of Illinois at Chicago College of Nursing 1 Learning Objectives Upon completion of this session, participants will be better able to: 1. Recognize depression, its symptoms and behaviors
Depression University of Illinois at Chicago College of Nursing 1 Learning Objectives Upon completion of this session, participants will be better able to: 1. Recognize depression, its symptoms and behaviors
REVIEW ARTICLE MANAGEMENT OF PATIENTS WITH MOOD DISORDERS AND COMORBID SUDS
 MANAGEMENT OF PATIENTS WITH MOOD DISORDERS AND COMORBID SUDS ANNALS OF CLINICAL PSYCHIATRY 2012;24(1):38-55 REVIEW ARTICLE The Canadian Network for Mood and Anxiety Treatments (CANMAT) task force recommendations
MANAGEMENT OF PATIENTS WITH MOOD DISORDERS AND COMORBID SUDS ANNALS OF CLINICAL PSYCHIATRY 2012;24(1):38-55 REVIEW ARTICLE The Canadian Network for Mood and Anxiety Treatments (CANMAT) task force recommendations
Therapeutic drug monitoring in neuropsychopharmacology: does it hold its promises?
 Therapeutic drug monitoring in neuropsychopharmacology: does it hold its promises? Prof. Dr. Christoph Hiemke Psychiatrische Klinik und Poliklinik Universität Mainz Psychopharmacotherapy Psychiatric Patient
Therapeutic drug monitoring in neuropsychopharmacology: does it hold its promises? Prof. Dr. Christoph Hiemke Psychiatrische Klinik und Poliklinik Universität Mainz Psychopharmacotherapy Psychiatric Patient
Adverse events of common psychiatric medications: an umbrella review
 Adverse events of common psychiatric medications: an umbrella review Katrina Bartellas, 1 Thomas Bajorek 1 Sarah Stockton, 1 Stefan Leucht, 2 Andrea Cipriani, 1 Seena Fazel 1 1 Department of Psychiatry,
Adverse events of common psychiatric medications: an umbrella review Katrina Bartellas, 1 Thomas Bajorek 1 Sarah Stockton, 1 Stefan Leucht, 2 Andrea Cipriani, 1 Seena Fazel 1 1 Department of Psychiatry,
Psychiatry Clinical Reviews Treating Bipolar Depression
 Mayo School of Continuous Professional Development Psychiatry Clinical Reviews Treating Bipolar Depression Mark A. Frye, MD October 6-8, 2016 Intercontinental Chicago Magnificent Mile Chicago, IL 2015
Mayo School of Continuous Professional Development Psychiatry Clinical Reviews Treating Bipolar Depression Mark A. Frye, MD October 6-8, 2016 Intercontinental Chicago Magnificent Mile Chicago, IL 2015
Summary ID#7029. Clinical Study Summary: Study F1D-MC-HGKQ
 CT Registry ID# 7029 Page 1 Summary ID#7029 Clinical Study Summary: Study F1D-MC-HGKQ Clinical Study Report: Versus Divalproex and Placebo in the Treatment of Mild to Moderate Mania Associated with Bipolar
CT Registry ID# 7029 Page 1 Summary ID#7029 Clinical Study Summary: Study F1D-MC-HGKQ Clinical Study Report: Versus Divalproex and Placebo in the Treatment of Mild to Moderate Mania Associated with Bipolar
It's Cycling, Not Polarity Understanding and Diagnosing the Bipolar Spectrum
 It's Cycling, Not Polarity Understanding and Diagnosing the Bipolar Spectrum Session 4022: American Psychiatric Nurses Association National Conference, Louisville, KY Andrew Penn, RN, MS, NP, CNS Psychiatric
It's Cycling, Not Polarity Understanding and Diagnosing the Bipolar Spectrum Session 4022: American Psychiatric Nurses Association National Conference, Louisville, KY Andrew Penn, RN, MS, NP, CNS Psychiatric
Long term use of lurasidone in patients with bipolar disorder: safety and effectiveness over 2 years of treatment
 DOI 10.1186/s40345-017-0075-7 RESEARCH Open Access Long term use of lurasidone in patients with bipolar disorder: safety and effectiveness over 2 years of treatment Andrei Pikalov *, Joyce Tsai, Yongcai
DOI 10.1186/s40345-017-0075-7 RESEARCH Open Access Long term use of lurasidone in patients with bipolar disorder: safety and effectiveness over 2 years of treatment Andrei Pikalov *, Joyce Tsai, Yongcai
The best drug treatment for psychotic depression: antidepressants, antipsychotics or both combined?
 BJPsych Advances (2017), vol. 23, 3 8 doi: 10.1192/apt.23.1.3 The best drug treatment for psychotic depression: antidepressants, antipsychotics or both combined? COMMENTARY ON COCHRANE CORNER Katharine
BJPsych Advances (2017), vol. 23, 3 8 doi: 10.1192/apt.23.1.3 The best drug treatment for psychotic depression: antidepressants, antipsychotics or both combined? COMMENTARY ON COCHRANE CORNER Katharine
APPENDIX 33: HEALTH ECONOMICS ECONOMIC EVIDENCE PROFILES
 APPENDIX 33: HEALTH ECONOMICS ECONOMIC EVIDENCE PROFILES 1.1 Case identification assessment of adults with bipolar disorder... 2 1.1.1 Clinical/economic question: Mood Disorder Questionnaire (MDQ) versus
APPENDIX 33: HEALTH ECONOMICS ECONOMIC EVIDENCE PROFILES 1.1 Case identification assessment of adults with bipolar disorder... 2 1.1.1 Clinical/economic question: Mood Disorder Questionnaire (MDQ) versus
DISEASES AND DISORDERS
 DISEASES AND DISORDERS 13. The mood (affective) disorders 99 14. The psychotic disorders: schizophrenia 105 15. The anxiety and somatoform disorders 111 16. Dementia and delirium 117 17. Alcohol and substance-related
DISEASES AND DISORDERS 13. The mood (affective) disorders 99 14. The psychotic disorders: schizophrenia 105 15. The anxiety and somatoform disorders 111 16. Dementia and delirium 117 17. Alcohol and substance-related
Comparison of the Usefulness of Lithium and Valproate
 Review Article CNPT4(2013) 1-5 Comparison of the Usefulness of Lithium and Valproate, M.D., Ph.D. Department of Neuropsychiatry, Oita University Faculty of Medicine ABSTRACT This review shows that lithium
Review Article CNPT4(2013) 1-5 Comparison of the Usefulness of Lithium and Valproate, M.D., Ph.D. Department of Neuropsychiatry, Oita University Faculty of Medicine ABSTRACT This review shows that lithium
Antidepressants (Tricyclic Antidepressants, Selective Serotonin Reuptake Inhibitors) in children 6-12 years of age with depressive episode/disorder
 updated 2012 Antidepressants (Tricyclic Antidepressants, Selective Serotonin Reuptake Inhibitors) in children 6-12 years of age with depressive episode/disorder Q10: Are antidepressants (Tricyclic antidepressants
updated 2012 Antidepressants (Tricyclic Antidepressants, Selective Serotonin Reuptake Inhibitors) in children 6-12 years of age with depressive episode/disorder Q10: Are antidepressants (Tricyclic antidepressants
Objectives. Objectives. A practice review. 02-Nov-16 MAJOR DEPRESSIVE DISORDER: NEW DEVELOPMENTS AND PRACTICAL IMPLICATIONS
 MAJOR DEPRESSIVE DISORDER: NEW DEVELOPMENTS AND PRACTICAL IMPLICATIONS Jon-Paul Khoo What is treatment resistance really? Database review 328 consecutive non-remitted MDD patients referred for private
MAJOR DEPRESSIVE DISORDER: NEW DEVELOPMENTS AND PRACTICAL IMPLICATIONS Jon-Paul Khoo What is treatment resistance really? Database review 328 consecutive non-remitted MDD patients referred for private
Treatment strategies in major depression What to use when?
 Treatment strategies in major depression What to use when? Michael Bauer, MD, PhD Professor and Chair of Psychiatry University Hospital Carl Gustav Carus Technische Universität Dresden Germany First-line
Treatment strategies in major depression What to use when? Michael Bauer, MD, PhD Professor and Chair of Psychiatry University Hospital Carl Gustav Carus Technische Universität Dresden Germany First-line
35-year-old woman with Hx of BPII Dx; currently separated from husband; has 1 child
 Stephen M. Strakowski, MD Chart Review: Bipolar Disorder PATIENT INFO 35 Age: Female Sex: 35-year-old woman with Hx of BPII Dx; currently separated from husband; has 1 child Background: SI and hospitalization
Stephen M. Strakowski, MD Chart Review: Bipolar Disorder PATIENT INFO 35 Age: Female Sex: 35-year-old woman with Hx of BPII Dx; currently separated from husband; has 1 child Background: SI and hospitalization
Introduction to Drug Treatment
 Introduction to Drug Treatment LPT Gondar Mental Health Group www.le.ac.uk Introduction to Psychiatric Drugs Drugs and Neurotransmitters 5 Classes of Psychotropic medications Mechanism of action Clinical
Introduction to Drug Treatment LPT Gondar Mental Health Group www.le.ac.uk Introduction to Psychiatric Drugs Drugs and Neurotransmitters 5 Classes of Psychotropic medications Mechanism of action Clinical
Mixing and Matching: Layering Medications as Family Physicians
 Mixing and Matching: Layering Medications as Family Physicians Family Medicine Forum Vancouver, B.C. November 9-12, 2016. Jon Davine, CCFP, FRCP(C) McMaster University Objectives Discuss different examples
Mixing and Matching: Layering Medications as Family Physicians Family Medicine Forum Vancouver, B.C. November 9-12, 2016. Jon Davine, CCFP, FRCP(C) McMaster University Objectives Discuss different examples
Evidence-Based, Pharmacological Treatment Guideline for Depression in Korea, Revised Edition
 SPECIAL ARTICLE Psychiatry & Psychology http://dx.doi.org/10.3346/jkms.2014.29.4.468 J Korean Med Sci 2014; 29: 468-484 -Based, Pharmacological Treatment Guideline for Depression in Korea, Revised Edition
SPECIAL ARTICLE Psychiatry & Psychology http://dx.doi.org/10.3346/jkms.2014.29.4.468 J Korean Med Sci 2014; 29: 468-484 -Based, Pharmacological Treatment Guideline for Depression in Korea, Revised Edition
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Single Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Single Technology Appraisal Aripiprazole for the treatment and prevention of acute manic and mixed episodes in bipolar disorder in children and adolescents
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Single Technology Appraisal Aripiprazole for the treatment and prevention of acute manic and mixed episodes in bipolar disorder in children and adolescents
Practice Parameter for the Assessment and Treatment of Children and Adolescents with Bipolar Disorder,
 Practice Parameter for the Assessment and Treatment of Children and Adolescents with Bipolar Disorder, Journal of the Academy of Child and Adolescent Psychiatry, 1997 Primary Authors: Jon McClellan MD
Practice Parameter for the Assessment and Treatment of Children and Adolescents with Bipolar Disorder, Journal of the Academy of Child and Adolescent Psychiatry, 1997 Primary Authors: Jon McClellan MD
Interventions for acute depression study characteristics. Abbreviations Australia bipolar I disorder. Great Britain
 APPENDIX 16: INTERVENTIONS FOR ACUTE DEPRESSION STUDY CHARACTERISTICS 1.1 Pharmacological interventions... 2 1.2 Nutritional interventions... 7 1.3 Physical interventions... 7 Abbreviations BPI CHN Dur
APPENDIX 16: INTERVENTIONS FOR ACUTE DEPRESSION STUDY CHARACTERISTICS 1.1 Pharmacological interventions... 2 1.2 Nutritional interventions... 7 1.3 Physical interventions... 7 Abbreviations BPI CHN Dur
48 th Annual Meeting. Clinical Pearls: Depression, Insomnia and Bipolar Disorder DSM-5. Disclosure. Depression. Patient Case. Objectives 7/19/2014
 48 th Annual Meeting Clinical Pearls: Depression, Insomnia and Bipolar Disorder DSM-5 Diagnostic and Statistical Manual of Mental Disorders (DSM-5) Published in 2013 Most published treatment guidelines
48 th Annual Meeting Clinical Pearls: Depression, Insomnia and Bipolar Disorder DSM-5 Diagnostic and Statistical Manual of Mental Disorders (DSM-5) Published in 2013 Most published treatment guidelines
Pharmacological management of bipolar disorder:a review
 Review Pharmacological management of bipolar disorder:a review Mahesh Rajasuriya, Varuni de Silva and Raveen Hanwella Background Bipolar disorder is a chronic recurrent neuropsychiatric disorder. The management
Review Pharmacological management of bipolar disorder:a review Mahesh Rajasuriya, Varuni de Silva and Raveen Hanwella Background Bipolar disorder is a chronic recurrent neuropsychiatric disorder. The management
Patients in the MIDAS Project. Exclusion Due to Bipolarity or Psychosis. Results
 Things You Think You Know Things You Think You Know, That May Not Be True in the Diagnosis and Treatment of Depression Mark Zimmerman, MD Director of Outpatient Psychiatry Director of the Partial Hospital
Things You Think You Know Things You Think You Know, That May Not Be True in the Diagnosis and Treatment of Depression Mark Zimmerman, MD Director of Outpatient Psychiatry Director of the Partial Hospital
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 05 May 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 05 May 2010 LAMICTAL 2 mg, dispersible / chewable tablet B/30 (CIP: 354 581-7) LAMICTAL 5 mg, dispersible / chewable
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 05 May 2010 LAMICTAL 2 mg, dispersible / chewable tablet B/30 (CIP: 354 581-7) LAMICTAL 5 mg, dispersible / chewable
Index. Note: Page numbers of article titles are in boldface type. A ADHD. See Attention-deficit/hyperactivity disorder (ADHD) b-adrenergic blockers
 Note: Page numbers of article titles are in boldface type. A ADHD. See Attention-deficit/hyperactivity disorder (ADHD) a-adrenergic blockers for PTSD, 798 b-adrenergic blockers for PTSD, 798 Adrenergic
Note: Page numbers of article titles are in boldface type. A ADHD. See Attention-deficit/hyperactivity disorder (ADHD) a-adrenergic blockers for PTSD, 798 b-adrenergic blockers for PTSD, 798 Adrenergic
Suicide Risk and Melancholic Features of Major Depressive Disorder: A Diagnostic Imperative
 Suicide Risk and Melancholic Features of Major Depressive Disorder: A Diagnostic Imperative Robert I. Simon, M.D.* Suicide risk is increased in patients with Major Depressive Disorder with Melancholic
Suicide Risk and Melancholic Features of Major Depressive Disorder: A Diagnostic Imperative Robert I. Simon, M.D.* Suicide risk is increased in patients with Major Depressive Disorder with Melancholic
Bipolar Disorder Clinical Practice Guideline Summary for Primary Care
 Bipolar Disorder Clinical Practice Guideline Summary for Primary Care DIAGNOSIS AND CLINICAL ASSESSMENT Bipolar Disorder is categorized by extreme mood cycling; manifested by periods of euphoria, grandiosity,
Bipolar Disorder Clinical Practice Guideline Summary for Primary Care DIAGNOSIS AND CLINICAL ASSESSMENT Bipolar Disorder is categorized by extreme mood cycling; manifested by periods of euphoria, grandiosity,
Major Depressive Disorder (MDD) in Children under Age 6
 in Children under Age 6 Level 0 Comprehensive assessment. Refer to Principles of Practice on page 6. Level 1 Psychotherapeutic intervention (e.g., dyadic therapy) for 6 to 9 months; assessment of parent/guardian
in Children under Age 6 Level 0 Comprehensive assessment. Refer to Principles of Practice on page 6. Level 1 Psychotherapeutic intervention (e.g., dyadic therapy) for 6 to 9 months; assessment of parent/guardian
Bipolar disorders: treatment options and patient satisfaction
 REVIEW Bipolar disorders: treatment options and patient satisfaction Charles Bowden Vivek Singh Department of Psychiatry, The University of Texas Health Science Center at San Antonio, San Antonio, TX,
REVIEW Bipolar disorders: treatment options and patient satisfaction Charles Bowden Vivek Singh Department of Psychiatry, The University of Texas Health Science Center at San Antonio, San Antonio, TX,
Supplementary Online Content
 Supplementary Online Content Weitz ES, Hollon SD, Twisk J, et al. Baseline depression severity as moderator of depression outcomes between cognitive behavioral therapy vs pharmacotherapy: an individual
Supplementary Online Content Weitz ES, Hollon SD, Twisk J, et al. Baseline depression severity as moderator of depression outcomes between cognitive behavioral therapy vs pharmacotherapy: an individual
Psychiatry in Primary Care: What is the Role of Pharmacist?
 Psychiatry in Primary Care: What is the Role of Pharmacist? Benjamin Chavez, PharmD, BCPP, BCACP Clinical Associate Professor Director of Behavioral Health Pharmacy Services January 12, 2019 Disclosure
Psychiatry in Primary Care: What is the Role of Pharmacist? Benjamin Chavez, PharmD, BCPP, BCACP Clinical Associate Professor Director of Behavioral Health Pharmacy Services January 12, 2019 Disclosure
Medications for Anxiety & Behavior in Williams Syndrome. Disclosure of Potential Conflicts. None 9/22/2016. Evaluation
 Medications for Anxiety & Behavior in Williams Syndrome Christopher J. McDougle, M.D. Director, Lurie Center for Autism Professor of Psychiatry and Pediatrics Massachusetts General Hospital and MassGeneral
Medications for Anxiety & Behavior in Williams Syndrome Christopher J. McDougle, M.D. Director, Lurie Center for Autism Professor of Psychiatry and Pediatrics Massachusetts General Hospital and MassGeneral
Surveillance report Published: 26 October 2017 nice.org.uk
 Surveillance report 2017 Bipolar disorder: assessment and management (2014) NICE guideline Surveillance report Published: 26 October 2017 nice.org.uk NICE 2017. All rights reserved. Subject to Notice of
Surveillance report 2017 Bipolar disorder: assessment and management (2014) NICE guideline Surveillance report Published: 26 October 2017 nice.org.uk NICE 2017. All rights reserved. Subject to Notice of
Major Depressive Disorder (MDD) in Children under Age 6
 in Children under Age 6 Level 0 Comprehensive assessment. Refer to Principles of Practice on page 5. Level 1 Psychotherapeutic intervention (e.g., dyadic therapy) for 6 to 9 months; assessment of parent/guardian
in Children under Age 6 Level 0 Comprehensive assessment. Refer to Principles of Practice on page 5. Level 1 Psychotherapeutic intervention (e.g., dyadic therapy) for 6 to 9 months; assessment of parent/guardian
RESEARCH INTRODUCTION
 Reboxetine for acute treatment of major depression: systematic review and meta-analysis of published and unpublished placebo and selective serotonin reuptake inhibitor controlled trials Dirk Eyding, project
Reboxetine for acute treatment of major depression: systematic review and meta-analysis of published and unpublished placebo and selective serotonin reuptake inhibitor controlled trials Dirk Eyding, project
Drugs, Society and Behavior
 SOCI 270 Drugs, Society and Behavior Spring 2016 Professor Kurt Reymers, Ph.D. Chapter 8 Medication for Mental Disorders 1. Mental Disorders: a. The Medical Model Model: symptoms diagnosis determination
SOCI 270 Drugs, Society and Behavior Spring 2016 Professor Kurt Reymers, Ph.D. Chapter 8 Medication for Mental Disorders 1. Mental Disorders: a. The Medical Model Model: symptoms diagnosis determination
Bipolar treatment update
 Bipolar treatment update Evidence is driving change Texas Medication Algorithm Project will weigh data on atypical antipsychotics in mania and on continuing antidepressants after bipolar depression remits.
Bipolar treatment update Evidence is driving change Texas Medication Algorithm Project will weigh data on atypical antipsychotics in mania and on continuing antidepressants after bipolar depression remits.
Clozapine as Add-On Medication in the Maintenance Treatment of Bipolar and Schizoaffective Disorders
 Neuropsychobiology 2002;45(suppl 1):37 42 Clozapine as Add-On Medication in the Maintenance Treatment of Bipolar and Schizoaffective Disorders A Case Series B. Hummel S. Dittmann A. Forsthoff N. Matzner
Neuropsychobiology 2002;45(suppl 1):37 42 Clozapine as Add-On Medication in the Maintenance Treatment of Bipolar and Schizoaffective Disorders A Case Series B. Hummel S. Dittmann A. Forsthoff N. Matzner
