Management of Eating Disorders
|
|
|
- Sherilyn Roberts
- 6 years ago
- Views:
Transcription
1 Evidence Report/Technology Assessment Number 135 Management of Eating Disorders Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health and Human Services 540 Gaither Road Rockville, MD Contract No Prepared by: RTI-UNC Evidence-Based Practice Center, Research Triangle Park, NC Investigators Nancy D. Berkman, Ph.D. Cynthia M. Bulik, Ph.D. Kimberly A. Brownley, Ph.D. Kathleen N. Lohr, Ph.D. Jan A. Sedway, Ph.D. Adrienne Rooks, B.A. Gerald Gartlehner, M.D. AHRQ Publication No. 06-E010 April 2006
2 This report is based on research conducted by the RTI International University of North Carolina at Chapel Hill (RTI-UNC) Evidence-based Practice Center (EPC) under contract to the Agency for Healthcare Research and Quality (AHRQ), Rockville, MD (Contract No ). The findings and conclusions in this document are those of the author(s), who are responsible for its content, and do not necessarily represent the views of AHRQ. No statement in this report should be construed as an official position of AHRQ or of the U.S. Department of Health and Human Services. The information in this report is intended to help clinicians, employers, policymakers, and others make informed decisions about the provision of health care services. This report is intended as a reference and not as a substitute for clinical judgment. This report may be used, in whole or in part, as the basis for the development of clinical practice guidelines and other quality enhancement tools, or as a basis for reimbursement and coverage policies. AHRQ or U.S. Department of Health and Human Services endorsement of such derivative products may not be stated or implied.
3 This document is in the public domain and may be used and reprinted without permission except those copyrighted materials noted for which further reproduction is prohibited without the specific permission of copyright holders. Suggested Citation: Berkman ND, Bulik CM, Brownley KA, Lohr KN, Sedway JA, Rooks A, Gartlehner G. Management of Eating Disorders. Evidence Report/Technology Assessment No (Prepared by the RTI International-University of North Carolina Evidence-Based Practice Center under Contract No ) AHRQ Publication No. 06-E010. Rockville, MD: Agency for Healthcare Research and Quality. April ii
4 Preface The Agency for Healthcare Research and Quality (AHRQ), through its Evidence-Based Practice Centers (EPCs), sponsors the development of evidence reports and technology assessments to assist public- and private-sector organizations in their efforts to improve the quality of health care in the United States. The report topic was nominated by the American Psychiatric Association (APA) and the Laureate Psychiatric Clinic and Hospital. Funding for this report was provided by the Office of Research on Women s Health at the National Institutes of Health (NIH) and the Health Resources and Services Administration. The reports and assessments provide organizations with comprehensive, science-based information on common, costly medical conditions and new health care technologies. The EPCs systematically review the relevant scientific literature on topics assigned to them by AHRQ and conduct additional analyses when appropriate prior to developing their reports and assessments. To bring the broadest range of experts into the development of evidence reports and health technology assessments, AHRQ encourages the EPCs to form partnerships and enter into collaborations with other medical and research organizations. The EPCs work with these partner organizations to ensure that the evidence reports and technology assessments they produce will become building blocks for health care quality improvement projects throughout the Nation. The reports undergo peer review prior to their release. AHRQ expects that the EPC evidence reports and technology assessments will inform individual health plans, providers, and purchasers as well as the health care system as a whole by providing important information to help improve health care quality. We welcome comments on this evidence report. They may be sent by mail to the Task Order Officer named below at: Agency for Healthcare Research and Quality, 540 Gaither Road, Rockville, MD 20850, or by to epc@ahrq.gov. Carolyn M. Clancy, M.D. Director Agency for Healthcare Research and Quality Jean Slutsky, P.A., M.S.P.H. Director, Center for Outcomes and Evidence Agency for Healthcare Research and Quality Vivian W. Pinn, M.D. Director Office of Research on Women s Health National Institutes of Health Beth A. Collins Sharp, R.N., Ph.D. Acting Director, EPC Program Agency for Healthcare Research and Quality Sabrina A. Matoff-Stepp, M.A. Director Office of Women s Health Health Resources and Services Administration Marian James, Ph.D. EPC Program Task Order Officer Agency for Healthcare Research and Quality iii
5 Structured Abstract Objectives. The RTI International University of North Carolina at Chapel Hill Evidence-based Practice Center (RTI-UNC EPC) systematically reviewed evidence on efficacy of treatment for anorexia nervosa (AN), bulimia nervosa (BN), and binge eating disorder (BED), harms associated with treatments, factors associated with the treatment efficacy and with outcomes of these conditions, and whether treatment and outcomes for these conditions differ by sociodemographic characteristics. Data Sources. We searched MEDLINE, the Cumulative Index to Nursing and Applied Health (CINAHL), PSYCHINFO, the Educational Resources Information Center (ERIC), the National Agricultural Library (AGRICOLA), and Cochrane Collaboration libraries. Review Methods. We reviewed each study against a priori inclusion/exclusion criteria. For included articles, a primary reviewer abstracted data directly into evidence tables; a second senior reviewer confirmed accuracy. We included studies published from 1980 to September, 2005, in all languages. Studies had to involve populations diagnosed primarily with AN, BN, or BED and report on eating, psychiatric or psychological, or biomarker outcomes. Results. We report on 30 treatment studies for AN, 47 for BN, 25 for BED, and 34 outcome studies for AN, 13 for BN, 7 addressing both AN and BN, and 3 for BED. The AN literature on medications was sparse and inconclusive. Some forms of family therapy are efficacious in treating adolescents. Cognitive behavioral therapy (CBT) may reduce relapse risk for adults after weight restoration. For BN, fluoxetine (60 mg/day) reduces core bulimic symptoms (binge eating and purging) and associated psychological features in the short term. Individual or group CBT decreases core behavioral symptoms and psychological features in both the short and long term. How best to treat individuals who do not respond to CBT or fluoxetine remains unknown. In BED, individual or group CBT reduces binge eating and improves abstinence rates for up to 4 months after treatment; however, CBT is not associated with weight loss. Medications may play a role in treating BED patients. Further research addressing how best to achieve both abstinence from binge eating and weight loss in overweight patients is needed. Higher levels of depression and compulsivity were associated with poorer outcomes in AN; higher mortality was associated with concurrent alcohol and substance use disorders. Only depression was consistently associated with poorer outcomes in BN; BN was not associated with an increased risk of death. Because of sparse data, we could reach no conclusions concerning BED outcomes. No or only weak evidence addresses treatment or outcomes difference for these disorders. Conclusions. The literature regarding treatment efficacy and outcomes for AN, BN, and BED is of highly variable quality. In future studies, researchers must attend to issues of statistical power, research design, standardized outcome measures, and sophistication and appropriateness of statistical methodology. v
6 Contents Executive Summary...1 Evidence Report...9 Chapter 1. Introduction...9 Scope of the Problem...9 Anorexia Nervosa...9 Clinical Characteristics...9 Diagnostic Criteria...9 Epidemiology...9 Etiology...11 Course of Illness...12 Treatment...12 Bulimia Nervosa...13 Clinical Characteristics...13 Diagnostic Criteria...13 Epidemiology...15 Etiology...15 Course of Illness...16 Treatment...16 Eating Disorders Not Otherwise Specified (Binge Eating Disorder)...16 Clinical Characteristics...16 Diagnostic Criteria...17 Epidemiology...18 Etiology...18 Course of Illness...18 Treatment...18 Production of This Evidence Report...18 Organization...18 Technical Expert Panel...19 Uses of This Report...19 Chapter 2. Methods...21 Key Questions and Analytic Framework...21 Key Questions...21 Literature Review Methods...22 Inclusion and Exclusion Criteria...22 Literature Search and Retrieval Process...24 Literature Synthesis...26 Development of Evidence Tables and Data Abstraction Process...26 Quality and Strength of Evidence Evaluation...27 Peer Review Process...29 vii
7 Chapter 3. Results: Anorexia Nervosa...37 Overview of Included Studies...37 Participants...40 Key Question 1: Treatment Efficacy...42 Medication Trials...46 Behavioral Intervention Trials (for Anorexia Nervosa)...46 Key Question 2: Harms of Treatments for Anorexia Nervosa...52 Key Question 3: Factors Associated With Treatment Efficacy...53 Key Question 4: Treatment Efficacy by Subgroups...54 Chapter 4. Results: Bulimia Nervosa...57 Overview of Included Studies...57 Participants...59 Key Question 1: Treatment Efficacy...60 Medication-only trials...60 Medication Plus Behavioral Intervention Trials...70 Behavioral Intervention Trials (for Bulimia Nervosa)...74 Key Question 2: Harms of Treatment for Bulimia Nervosa...84 Key Question 3: Factors Associated With Treatment Efficacy...84 Medication Trials...84 Behavioral Intervention Trials...87 Self-help Trials...87 Other Interventions...87 Key Question 4: Treatment Efficacy by Subgroups...87 Chapter 5. Results: Binge Eating Disorder...89 Overview of Included Studies...89 Participants...91 Key Question 1: Treatment Efficacy...92 Medication-only trials...92 Medication Plus Behavioral Intervention Trials...98 Behavioral Interventions Trials Key Question 2: Harms of Treatment for Binge Eating Disorder Key Question 3: Factors Associated With Treatment Efficacy Key Question 4: Treatment Efficacy Subgroups Chapter 6. Outcomes of Eating Disorders Anorexia Nervosa Key Question 5: Factors associated with outcomes Key Question 6: Outcome Difference by Sex, Gender, Age, Race, Ethnicity, or Cultural Group Bulimia Nervosa Key Question 5: Factors Asociated with Outcomes Key Question 6: Outcome Difference by Sex, Gender, Age, Race, Ethnicity or Cultural Group viii
8 Binge Eating Disorder Key Question 5: Factors Associated with Outcomes Key Question 6: Outcome Difference by Sex, Gender, Age, Race, Ethnicity or Cultural Group Chapter 7. Discussion Critical Findings and Implications for Treatment of Eating Disorders Quality of Literature and Strength of Evidence Managing Patients with Medication Alone Managing Patients with Behavioral Interventions Alone Managing Patients with Combination Interventions Managing Patients with Novel Interventions Reducing Mortality Methods and Other Deficiencies in Reviewed Studies and Recommendations to Overcome Them Sample Sizes, Attrition, and Statistical Power Study Design and Statistical Analysis Issues Reporting Issues Future Research Needs Gaps in the Literature for Interventions Gaps in the Literature for Certain Types of Patients Gaps in the Overall Evidence Base Issues in Outcomes Research Conclusions References and Included Studies Figures Figure 1. Analytic framework...22 Figure 2. Eating disorders article disposition...25 Tables Table 1. Diagnostic criteria: anorexia nervosa...10 Table 2. Diagnostic criteria: bulimia nervosa...14 Table 3. Diagnostic criteria: binge eating disorders Table 4. Eating disorders literature searches: inclusion and exclusion criteria...23 Table 5. Diagnostic and outcome measures used in randomized controlled trials and outcome studies...30 Table 6. Reasons for poor quality ratings and number of trials with poor ratings: anorexia nervosa...38 Table 7. Dropout rates for randomized controlled trials: anorexia nervosa...41 Table 8. Results from medication trials: anorexia nervosa...43 Table 9. Results from behavioral intervention trials in adults: anorexia nervosa...47 ix
9 Table 10. Results from behavioral intervention trials in adolescents only and adolescents and adults combined: anorexia nervosa...49 Table 11. Adverse events reported: anorexia nervosa...53 Table 12. Reasons for poor quality ratings and number of trials with poor ratings: bulimia nervosa trials...58 Table 13. Dropout rates for randomized controlled trials: bulimia nervosa...60 Table 14. Results from medication trials: bulimia nervosa Table 15. Results from medication plus behavioral intervention trials: bulimia nervosa...71 Table 16. Result from behavioral intervention trials: bulimia nervosa...75 Table 17. Results of self-help trials, no medication: bulimia nervosa Table 18. Results of other trials: bulimia nervosa...83 Table 19. Adverse events reported: bulimia nervosa trials...85 Table 20. Reasons for poor quality ratings and number of trials with poor ratings binge eating disorder...90 Table 21. Dropout rates for randomized controlled trials: binge eating disorder...93 Table 22. Results from medication trials: binge eating disorder...95 Table 23. Results from medication plus behavioral intervention trials: binge eating disorder...99 Table 24. Results from behavioral intervention trials, no medication: binge eating disorder Table 25. Results from self-help trials, no medication: binge eating disorder Table 26. Results from other trials: binge eating disorder Table 27. Adverse events reported: binge eating disorder Table 28. Outcome studies: reasons for poor quality ratings and number of poor ratings by disease type Table 29. Eating-related outcomes: anorexia nervosa Table 30. Psychological outcomes: anorexia nervosa Table 31. Biomarker outcomes: anorexia nervosa Table 32. Mortality outcomes: anorexia nervosa Table 33. Eating-related outcomes: bulimia nervosa Table 34. Psychological outcomes: bulimia nervosa Table 35. Biomarker outcomes: bulimia nervosa Table 36. Mortality outcomes: bulimia nervosa Table 37. Strength of evidence concerning four treatment key questions Table 38. Strength of evidence concerning two outcomes key questions Appendixes Appendix A: Exact Search Strings Appendix B: Sample Data Collection Forms Appendix C: Evidence Tables Appendix D: List of Excluded Articles Appendix E: Acknowledgments Appendixes and Evidence Tables for this report are provided electronically at x
10 xi
11 Executive Summary Introduction The RTI International University of North Carolina at Chapel Hill Evidence-based Practice Center (RTI-UNC EPC) conducted a systematic review of the literature on key questions concerning anorexia nervosa (AN), bulimia nervosa (BN), and eating disorders not otherwise specified (EDNOS) (focusing on binge eating disorder [BED]) to address questions posed by the American Psychiatric Association and Laureate Psychiatric Hospital through the Agency for Healthcare Research and Quality (AHRQ). Funding was provided by AHRQ, the Office of Research on Women s Health at the National Institutes of Health, and the Health Resources and Services Administration. We received guidance and input from a Technical Expert Panel (TEP). We systematically reviewed the evidence on two categories of issues treatment and outcomes for AN, BN, and BED in six key questions (KQs): (1) efficacy of treatment, (2) harms associated with treatment, (3) factors associated with the efficacy of treatment, (4) whether efficacy of treatment differs by sex, gender, age, race, ethnicity, or cultural group, (5) factors associated with outcomes, and (6) whether outcomes differ by sex, gender, age, race, ethnicity, or cultural group. AN is marked by low body weight, fear of weight gain, disturbance in the way in which one s body size is perceived, denial of illness, or undue influence of weight on self-evaluation. Although amenorrhea is a diagnostic criterion, it is of questionable relevance. BN is characterized by recurrent episodes of binge eating in combination with some form of compensatory behavior. Binge eating is the consumption of an uncharacteristically large amount of food by social comparison coupled with a feeling of being out of control. Compensatory behaviors include self-induced vomiting; misuse of laxatives, diuretics, or other agents; fasting; and excessive exercise. BED is marked by binge eating in the absence of compensatory behaviors, a series of associated features of binge eating, and marked distress regarding binge eating. Overweight and obesity are commonly seen in individuals with BED. Although rigorous epidemiologic data are lacking in the United States, the mean prevalence of AN is 0.3 percent, of subthreshold AN 0.37 percent to 1.3 percent, of BN 1.0 percent, and of BED 0.7 percent to 3.0 percent. Mortality from AN is about 5 percent per decade of followup. Treatment for severe AN can involve inpatient or partial hospitalization in costly specialized settings. Inadequate insurance coverage often truncates the recommended duration of treatment. Treatment costs for AN are higher than those for obsessive-compulsive disorder and comparable to those for schizophrenia. In contrast, treatment for BN in the United States is typically on an outpatient basis. Methods We searched MEDLINE, the Cumulative Index to Nursing and Applied Health (CINAHL), PSYCHINFO, the Educational Resources Information Center (ERIC), the National Agricultural Library (AGRICOLA), and Cochrane Collaboration libraries. Based on key questions and discussion with our TEP, we generated a list of article inclusion and exclusion criteria. We reviewed studies of humans, ages 10 years and older, of both sexes, published in all languages and from all nations, from 1980 to September Studies had to include populations diagnosed primarily with AN, BN, or BED and to report on at least one of our outcomes 1
12 categories of interest: eating-related behaviors, psychiatric and psychological outcomes, and biomarker measures. We reviewed each abstract and article systematically against a priori criteria to determine whether to include it in the review. One reviewer initially evaluated abstracts for inclusion or exclusion. If that reviewer concluded that the article should be included in the review, it was retained. Articles that the reviewer determined did not meet our criteria were re-reviewed by a senior reviewer who could include the article if she disagreed with the initial determination. We assigned each excluded article a reason for exclusion. The RTI-UNC EPC team abstracted data from included articles directly into evidence tables. For both the treatment and the outcomes literatures, a primary reviewer abstracted data directly into evidence tables; a second (senior) reviewer confirmed accuracy, completeness, and consistency. The two staff reconciled all disagreements about information in evidence tables. Each abstractor independently evaluated study quality. Because of differences in the treatment and outcomes literature, we evaluated the two bodies of literature using separate criteria. For the treatment literature, our evaluation used 25 items in 11 categories: (1) research aim/study question, (2) study population, (3) randomization, (4) blinding, (5) interventions, (6) outcomes, (7) statistical analysis, (8) results, (9) discussion, (10) external validity, and (11) funding/sponsorship. For the outcomes literature, we evaluated the evidence against 17 items in 8 categories: (1) research aim/study question, (2) study population, (3) eating disorder diagnosis method, (4) study design, (5) statistical analysis, (6) results/outcome measurement, (7) external validity, and (8) discussion. We focused our analysis on studies that received fair or good quality ratings. This included 19 studies discussed in 22 articles concerning treatment for AN: 38 studies discussed in 48 articles concerning treatment for BN: 20 studies discussed in 21 articles concerning treatment for BED: 26 studies discussed in 32 articles concerning outcomes for AN: 9 studies discussed in 13 articles concerning outcomes for BN: 7 studies discussed in 7 articles concerning outcomes for both AN and BN: and 3 studies discussed in 3 articles concerning outcomes for BED. Treatment Studies Results Anorexia Nervosa. We divided the treatment literature into medication-only (generally in the context of clinical management or hospitalization), medication plus behavioral intervention, and behavioral intervention only for either adults or adolescents. The literature regarding medication treatments for AN is sparse and inconclusive. The vast majority of studies had small sample sizes and rarely had adequate statistical power to allow for definitive conclusions. Although studies did include medication administered during or after inpatient intervention, no AN studies that systematically combined medication with behavioral interventions met our inclusion criteria, revealing a substantial gap in the literature. In the behavioral intervention literature, preliminary evidence suggests that cognitive behavioral therapy (CBT) may reduce relapse risk for adults with AN after weight restoration. Sufficient evidence does not exist to determine whether CBT has any effect during the acute phase of the illness, and one study, also requiring replication, showed that a manual-based treatment combining elements of sound clinical management and supportive psychotherapy by a specialist was more effective than CBT during the acute phase. Family therapy as currently conceptualized does not appear to be effective with adults with AN with longer duration of illness. Specific forms of family therapy initially focusing on parental control of renutrition is 2
13 efficacious in treating AN in adolescents and leads to clinically meaningful weight gain and psychological change. The lack of follow-up data compromises our ability to determine the extent to which treatment gains are maintained. Bulimia Nervosa. In medication trials, fluoxetine (60 mg/day) administered for 6 weeks to 18 weeks reduced the core bulimia symptoms of binge eating and purging and associated psychological features in the short term. The 60 mg dose performs better than lower doses and is associated with prevention of relapse at 1 year. Evidence for the long-term effectiveness of relatively brief medication treatment does not exist. The optimal duration of treatment and the optimal strategy for maintenance of treatment gains are unknown. Studies that combine drugs and behavioral interventions provide only preliminary evidence regarding the optimal combination of medication and psychotherapy or self-help. How best to treat individuals who do not respond to CBT or fluoxetine remains a major shortcoming of the literature. For behavioral interventions for BN, CBT administered individually or in group format is effective in reducing the core behavioral symptoms of binge eating and purging and psychological features in both the short and long term. Further evidence is required to establish the role for self-help in reducing bulimic behaviors. Binge Eating Disorder. For BED, we addressed two critical outcomes decrease in binge eating and decrease in weight in overweight individuals. Various medications were studied, including selective serotonin reuptake inhibitors (SSRIs); a combined serotonin, dopamine, and norepinephrine uptake inhibitor; tricyclic antidepressants; an anticonvulsant; and one appetite suppressant. In short-term trials, SSRIs led to greater rates of reduction in target eating, psychiatric and weight symptoms, and severity of illness than placebo controls. However, in the absence of clear endpoint data, and in the absence of data regarding abstinence from binge eating, we cannot judge the magnitude of the clinical impact of these interventions. Moreover, in the absence of follow-up data after drug discontinuation, we do not know whether observed changes in binge eating, depression, and weight persist. The combination of CBT plus medication may improve both binge eating and weight loss, although sufficient trials have not been done to determine definitively which medications are best at producing and maintaining weight loss. Moreover, the optimal duration of medication treatment for sustained weight loss has not yet been addressed empirically. Collectively, clinical trials incorporating CBT for BED indicated that CBT decreases either the number of binge days or the actual number of reported binge episodes. CBT leads to greater rates of abstinence than does a waiting list control approach when administered either individually or in group format, and this abstinence persists for up to 4 months posttreatment. CBT also improves the psychological aspects of BED, such as ratings of restraint, hunger, and disinhibition. Results are mixed as to whether CBT improves self-rated depression in this population. Finally, CBT does not appear to produce decreases in weight. Various forms of self-help were efficacious in decreasing binge days, binge eating episodes, and psychological features associated with BED. Self-help also led to greater abstinence from binge eating than waiting list; short-term abstinence rates approximate those seen in face-to-face psychotherapy trials. Strength of Evidence in Treatment Literature. We graded the strength of the body of evidence for each question separately. For efficacy of treatment (KQ 1), we graded evidence for AN treatment as weak, that for BN medication and behavioral interventions as strong, and that for BED therapies as moderate. For harms associated with treatment (KQ 2), we graded medication interventions for BN and BED as consistently strong; the literatures for all AN 3
14 interventions and all other BN and BED interventions were graded as weak to nonexistent because many studies failed to address harms associated with treatment. For factors associated with efficacy of treatment (KQ 3), with the exception of behavioral interventions for BN, which we graded as moderate, we graded the literature uniformly as weak. No published literature provided evidence on whether the efficacy of treatment for these conditions differs by sociodemographic factors (KQ 4). Overall, the literature on the treatment of AN in particular was deficient. Outcomes Literature Outcomes of Eating Disorders. One prospective cohort study, conducted in Sweden, followed individuals with AN in the community. Over a 10-year period, approximately half of the group had fully recovered; a small percentage continued to suffer from AN, and the remainder still had other eating disorders. Members of the AN group no longer differed from those in the comparison group in terms of weight, but they continued to be more depressed and to suffer from a variety of personality disorders, obsessive-compulsive disorder, Asperger syndrome, and autism spectrum disorders. The remaining AN studies followed patient populations. Typically, at least one-half of the patients no longer suffered from AN at followup. However, many continued to have other eating disorders such as BN or EDNOS, and mortality was significantly higher than would be expected in the population matched by sex and age. Factors associated with recovery or good outcomes included lower levels of depression and compulsivity. Factors associated with increased mortality included concurrent alcohol and substance use disorders. All of the BN outcomes studies followed patient populations. This literature emphasizes comparisons of various definitions of disease outcomes and diagnostic subtypes. Generally, more than one-half of the patients followed no longer had a BN diagnosis at the end of the study. A substantial percentage continued to suffer from other eating disorders, but BN was not associated with an increased mortality risk. A limited number of analyses uncovered factors significantly associated with outcomes of this disease, but only depression was consistently associated with worse outcomes. Only sparse evidence addresses factors associated with BED outcomes. The three included studies have vastly different designs and research questions; more importantly, they do not converge on any systematic findings. Recalling that no studies of EDNOS outcomes exist, we conclude that the literature regarding outcomes of both EDNOS in general and BED in particular is seriously lacking; we believe that no conclusions can be drawn about factors influencing outcomes of these disorders. Age of AN disease onset was examined in several AN outcomes studies. However, the relation between this variable and outcomes was mixed. No additional differences by participant sex, gender, age, race, ethnicity, or cultural group emerged from the AN, BN, or BED outcomes literature. Strength of Evidence in Outcomes Literature. The strength of the evidence addressing factors associated with outcomes among individuals with AN and BN is moderate. In contrast, given the limited information about factors related to outcomes among individuals with BED (KQ 5), we rated BED evidence as weak. We used the body of literature concerning KQ 5 to examine differences in outcomes by sociodemographic factors (KQ 6). We graded the AN literature as weak and the BN and BED literature as nonexistent. 4
15 Discussion In conclusion, the literature regarding treatment efficacy and outcome for AN, BN, and BED is of highly variable quality. In the treatment literature, the largest deficiency rests with treatment efficacy for AN where the literature was weakest. Future studies require large numbers of participants, multiple sites, appropriate biomarker outcomes, and clear delineation of the age of participants. For BN, future studies should address novel treatments for the disorder, optimal duration of intervention, and optimal approaches for those who do not respond to medication or CBT. For BED, future studies should identify interventions that are effective for both elimination of binge eating and reduction of weight (in overweight individuals), optimal duration of intervention, and effective strategies for prevention of relapse. For all three disorders, exploration of additional treatment approaches is warranted. In addition, for all three disorders, greater attention must be paid to factors influencing outcomes, harms associated with treatment, and differential efficacy by sex, gender, age, race, ethnicity, or cultural group. For all three disorders, consensus definitions of remission, recovery, and relapse are essential. Greater attention to disease presentations currently grouped under the heading of EDNOS is required for both treatment and outcome literature. For outcome studies, especially for BN and BED, population-based cohort studies with comparison groups and adequate durations of followup are required. For both future treatment and outcome studies, researchers must carefully attend to issues of statistical power, research design including the use of similar outcome measures across studies, and sophistication and appropriateness of statistical analyses. 5
16 Evidence Report
17 Chapter 1. Introduction Scope of the Problem The eating disorders discussed in this report include anorexia nervosa (AN), bulimia nervosa (BN), and eating disorders not otherwise specified (EDNOS). Although rigorous epidemiologic data specific only to the United States are lacking, the mean prevalence of AN in young females in Western Europe and the United States is 0.3 percent and the mean prevalence of BN is 1.0 percent. Clinically concerning subthreshold conditions are more prevalent. 1 These eating disorders are associated with substantial morbidity and mortality. 2,3 The financial and social impact of these potentially fatal disorders on disability, productivity, and quality of life remains unknown. Clinical Characteristics Anorexia Nervosa AN is a serious psychiatric illness marked by an inability to maintain a normal healthy body weight, often dropping well below 85 percent of ideal body weight. Patients who are still growing fail to make expected increases in weight (and often height) and bone density. Despite increasing weight loss, individuals with AN continue to obsess about weight, remain dissatisfied with the perceived size of their bodies, and engage in an array of unhealthy behaviors to perpetuate weight loss (e.g., purging, dieting, excessive exercise, fasting). Individuals with AN place central importance on their shape and weight as a marker of self-worth and self-esteem. Although amenorrhea is a diagnostic criterion, it is of questionable relevance. There do not appear to be meaningful differences between individuals with AN who do and do not menstruate. 4,5 Typical personality features of individuals with AN include perfectionism, obsessionality, anxiety, harm avoidance, and low self-esteem. 6 The most common comorbid psychiatric conditions include major depression 7,8 and anxiety disorders. 9,10 Anxiety disorders often predate the onset of the eating disorder, 9,10 and depression often persists post-recovery. 11 Diagnostic Criteria Table 1 presents the diagnostic criteria that authors of articles reviewed in this report use. They include Russell criteria, 12 Feighner criteria, 13 Diagnostic and Statistical Manual for Mental Disorders III, III-R and IV (DSM III, III-R, and IV), and the International Classification of Diseases-Versions 9 and 10 (ICD-9 and ICD-10). 17 Epidemiology The mean prevalence of AN in young females in Western Europe and the United States is 0.3 percent. 1 The prevalence of subthreshold AN, defined as one criterion short of threshold, is greater ranging from 0.37 percent to 1.3 percent. 18,19 Although awareness of the disorder has increased, the data on changing incidence are conflicting. Some studies suggest that the incidence is increasing, and others report stable 9
18 Table 1. Diagnostic criteria: anorexia nervosa Diagnostic Criteria Russell s Criteria for Anorexia Nervosa Feighner s Criteria for Anorexia Nervosa DSM III Criteria for Anorexia Nervosa (307.10) DSM III-R Criteria for Anorexia Nervosa (307.10) DSM IV Criteria for Anorexia Nervosa (307.10) 1. Patient resorts to a variety of devices aimed at achieving weight loss (starvation, vomiting, laxatives, etc.) 2. Evidence of an endocrine disorder, amenorrhea in the female, and loss of sexual potency and interest in the male 3. Patient manifests the characteristic psychopathology of a morbid fear of becoming fat. This is accompanied by a distorted judgment by the patient of her body size 1. Onset prior to age Anorexia with accompanying weight loss of at least 25 percent of original body weight 3. A distorted implacable attitude toward eating food or weight that overrides hunger, admonitions, reassurances, and threats 4. No known medical illness accounts for the anorexia [nervosa] and weight loss 5. No other known psychiatric disorder, with particular reference to primary affective disorders, schizophrenia, obsessive, and compulsive and phobic neurosis 6. At least two of the following manifestations: amenorrhea, lanugo, bradycardia, periods of overactivity, episodes of bulimia, vomiting A. Intense fear of becoming obese, which does not diminish as weight loss progresses B. Disturbance of body image (e.g., claiming to "feel fat" even when emaciated) C. Weight loss of at least 25% of original body weight or, if under 18 years of age, weight loss from original body weight plus projected weight gain expected from growth charts may be combined to make the 25% D. Refusal to maintain body weight over a minimal normal weight for age and height E. No known physical illness that would account for the weight loss A. Refusal to maintain body weight over a minimal normal weight for age and height (e.g., weight loss leading to maintenance of body weight 15% below that expected or failure to make expected weight gain during period of growth, leading to body weight 15% below that expected) B. Intense fear of gaining weight or becoming fat, even though underweight C. Disturbance in the way in which one s body weight, size, or shape is experienced (e.g., the person claims to "feel fat" even when emaciated, believes that one area of the body is "too fat" even when obviously underweight) D. In females, absence of at least three consecutive menstrual cycles when otherwise expected to occur (primary and secondary amenorrhea). (A woman is considered to have amenorrhea if her periods occur only following hormone, e.g., estrogen, administration.) A. Refusal to maintain body weight at or above a minimally normal weight for age and height (e.g., weight loss leading to maintenance of body weight less than 85% of that expected or failure to make expected weight gain during period of growth, leading to body weight less than 85% of that expected). B. Intense fear of gaining weight or becoming fat, even though underweight. C. Disturbance in the way in which one's body weight or shape is experienced, undue influence of body weight or shape on self-evaluation, or denial of the seriousness of the current low body weight. D. In postmenarchal females, amenorrhea i.e., the absence of at least three consecutive cycles. (A woman is considered to have amenorrhea if her periods occur only following hormone, e.g., estrogen administration.) Specify type: Restricting Type: During the current episode of anorexia nervosa, the person has not regularly engaged in binge-eating or purging behavior (i.e., self-induced vomiting or the misuse of laxatives, diuretics, or enemas). Binge-Eating/Purging Type: During the current episode of anorexia nervosa, the person has regularly engaged in binge-eating or purging behavior (i.e., self-induced vomiting or the misuse of laxatives, diuretics, or enemas). DSM, Diagnostic and Statistical Manual; ICD, International Classification of Diseases. For citations, see text. 10
19 Table 1. Diagnostic criteria: anorexia nervosa (continued) Diagnostic Criteria ICD-9 Criteria for Anorexia Nervosa (307.1) ICD-10 Criteria for Anorexia Nervosa (F50.0) ICD-10 Criteria for Atypical Anorexia Nervosa (F50.1) A disorder in which the main features are persistent active refusal to eat and marked loss of weight The level of activity and alertness is characteristically high in relation to the degree of emaciation Typically the disorder begins in teenage girls but it may sometimes begin before puberty and rarely occurs in males Amenorrhoea is usual and there may be a variety of other changes including slow pulse and respiration and low body temperature and dependent oedema Unusual eating habits and attitudes toward food are typical and sometimes starvation follows or alternates with periods of overeating The accompanying psychiatric symptoms are diverse A. There is weight loss or, in children, a lack of weight gain, leading to a body weight at least 15% below the normal or expected weight for age and height B. The weight loss is self-induced by avoidance of fattening foods C. There is self-perception of being too fat, with an intrusive dread of fatness, which leads to a self-imposed low weight threshold D. A widespread endocrine disorder involving the hypothalamic-pituitary-gonadal axis is manifested in women as amenorrhoea and in men as a loss of sexual interest and potency. (An apparent exception is the persistence of vaginal bleeds in anorexic women who are on replacement hormonal therapy, most commonly taken as a contraceptive pill) E. The disorder does not meet criteria A or B for bulimia nervosa Disorder that fulfills some of the features of anorexia nervosa but in which the overall clinical picture does not justify that diagnosis. For instance, one of the key symptoms, such as amenorrhoea or marked dread of being fat, may be absent in the presence of marked weight loss or weight-reducing behavior. This diagnosis should not be made in the presence of known physical disorders associated with weight loss rates Epidemiological studies indicate that the peak age of onset is between 15 and 19 years. 32 Anecdotal reports suggest increasing presentations in prepubertal children 33 and new onset cases in mid- and late-life. 34,35 The gender ratio for AN is approximately 9:1, women to men. 16 Etiology The etiology of AN remains incompletely understood. Although numerous psychological, social, and biological factors have been implicated as potentially causal, few specific risk factors have been consistently replicated in studies of the etiology of the disorder. 36,37 Although not disorder-specific, common risk factors across eating disorders include sex, race or ethnicity, childhood eating and gastrointestinal problems, elevated shape and weight concerns, negative self-evaluation, sexual abuse and other adverse events, and general psychiatric comorbidity. 36 In addition, prematurity, smallness for gestational age, and cephalohematoma have been identified as risk factors for AN. 38 The preponderance of reports from western cultures fueled early conceptualizations of AN as a culturally determined disorder, but the past decade of biological and genetic research has revealed that AN is familial 39 and that the observed familial aggregation is attributable primarily to genetic factors Moreover, molecular genetic studies have identified areas of the human 11
20 genome that may harbor susceptibility loci for AN 43,44 and specific genes that may influence risk. 45,46 In addition, an array of pharmacologic, genetic, and neuroimaging studies have identified fundamental disturbances in serotonergic function in individuals with AN even after recovery. 47 Although serotonin has received considerable research attention, given the interrelatedness of neurotransmitter function, other neurotransmitter systems, most notably dopamine, are also implicated in these disorders. 48 The ultimate understanding of AN etiology will likely include main effects of both biological and environmental factors as well as their interactions and correlations. Course of Illness AN has serious medical and psychological consequences that can persist even after recovery. Features associated with the eating disorder including depression, anxiety, social withdrawal, heightened self-consciousness, fatigue, and multiple medical complications. 7,49-51 The social toll of AN interferes with normal adolescent development. 52 Across psychiatric disorders, the highest risks of premature death, from both natural and unnatural causes, are from substance abuse and eating disorders. 53 A history of AN is associated with greater problems with reproduction, 54 osteoporosis, continued low body mass index (BMI, a commonly used measure of normal weight, overweight, or obesity calculated as weight in kilograms divided by height in meters squared [kg/m 2 ]), and major depression. 11 Chapter 6 reviews eating-related, psychological, and biomarker-measured outcomes of AN in detail. Treatment Given the high morbidity and mortality associated with AN, developing effective treatments for AN is critical. Because of the frequent medical complications and nutritional compromise, clinical practice typically includes a comprehensive medical evaluation and nutritional counseling. Typically, less medically compromised cases of AN are treated on an outpatient basis by psychiatrists, psychologists, and other therapists with primary care providers managing medical care. Professional organizations have developed several English-language treatment guidelines or position papers for the treatment of AN; these include the American Psychiatric Association, 58 the National Institute for Clinical Excellence, 59 the Society for Adolescent Medicine, 60 the American Academy of Pediatrics, 61 and the Royal Australian and New Zealand College of Psychiatrists. 62 Psychotherapeutic approaches include individual psychotherapy (cognitive-behavioral, interpersonal, behavioral, and psychodynamic), family therapy (especially for younger patients), and group therapy. The American Psychiatric Association Working Group on Eating Disorders concluded that hospitalization is appropriate for individuals below 75 percent of ideal body weight. 58 Weight is not the only parameter to be considered in level of care decisions. Other considerations include medical complications, suicide attempt or plan, failure of outpatient or partial hospitalization treatment, psychiatric comorbidity, role impairment, poor psychosocial support, compromised pregnancy, and lack of availability of less intensive treatment options. 58 Such treatment commonly involves highly specialized multidisciplinary teams including psychologists, psychiatrists, internists or pediatricians, nutritionists, social workers, and nurse specialists. 12
21 Striegel-Moore et al. reported the average length of stay to be 26 days using an insurance database of approximately 4 million individuals in the United States; 63 this is substantially shorter than the lengths of stay in other countries, including New Zealand (72 days) 64 and Europe, which ranges from 40.6 days (Finland) to days (Switzerland). 65 They found that, per patient, AN treatment costs in the United States were higher than those for obsessivecompulsive disorder and comparable to those for schizophrenia, both of which have prevalences similar to those of AN. 63 A workshop sponsored by the National Institute of Mental Health (NIMH) examined problems in conducting research on AN treatment. 66 It highlighted obstacles such as relatively low incidence and prevalence, lack of consensus on best treatments, variable presentation within the patient population based on age and illness factors, high costs of providing treatment, and the complex interaction of medical and psychiatric problems associated with the illness. This report also highlighted the importance of improving and expanding the workforce in the eating disorders research field. Clinical Characteristics Bulimia Nervosa BN is characterized by recurrent episodes of binge eating in combination with some form of inappropriate compensatory behavior. Binge eating is the consumption of an abnormally large amount of food coupled with a feeling of being out of control. Compensatory behaviors (aimed at preventing weight gain) include self-induced vomiting; the misuse of laxatives, diuretics, or other agents; fasting; and excessive exercise. The onset of BN usually occurs in adolescence or early adulthood and is most frequently seen in women who are of normal body weight. 16 Although the gender ratio is approximately 9:1, women to men, the diagnostic criteria themselves are gender-biased. In contrast to women, men tend to present with a greater reliance on nonpurging forms of compensatory behavior such as excessive exercise. 67,68 Considerations of differences in the clinical presentation of BN in men may lead to revised estimates. 67,69 Approximately 80 percent of patients with BN are diagnosed with another psychiatric disorder at some time in their life. 70 Commonly comorbid psychiatric conditions include anxiety disorders, major depression, dysthymia, substance use, and personality disorders. 9,71-77 Personality features of individuals with BN include some features shared with AN such as high harm avoidance, perfectionism, and low self-esteem. Features more specific to BN include higher novelty seeking, higher impulsivity, lower self-directedness, and lower cooperativeness Diagnostic Criteria Table 2 presents DSM III, III-R, and IV and ICD-10 diagnostic criteria for BN. According to DSM IV criteria, a diagnosis of BN requires a minimum of 3 months of binge eating and compensatory behavior occurring twice a week or more. Similar to AN, individuals have to report the undue influence of weight and shape on their self-esteem. In addition, BN is diagnosed 13
22 Table 2. Diagnostic criteria: bulimia nervosa Diagnostic Criteria DSM III Criteria for Bulimia Nervosa (307.51) DSM III-R Criteria for Bulimia Nervosa (307.51) DSM IV Criteria for Bulimia Nervosa (307.51) A. Recurrent episodes of binge eating (rapid consumption of a large amount of food in a discrete period of time, usually less than two hours) B. At least three of the following: (1) consumption of high-caloric, easily ingested food during a binge (2) inconspicuous eating during a binge (3) termination of such eating episodes by abdominal pain, sleep, social interruption, or self-induced vomiting (4) repeated attempts to lose weight by severely restrictive diets, self-induced vomiting, or use of cathartics or diuretics (5) frequent weight fluctuations greater than 10 pounds due to alternating binges and fasts C. Awareness that the eating pattern is abnormal and fear of not being able to stop eating voluntarily D. Depressed mood and self-deprecating thoughts following eating binges E. The bulimic episodes are not due to anorexia nervosa or any known physical disorder A. Recurrent episodes of binge eating (rapid consumption of a large amount of food in a discrete period of time) B. A feeling of lack of control over eating behavior during the eating binges C. The person regularly engages in either self-induced vomiting, use of laxatives or diuretics, strict dieting or fasting, or vigorous exercise in order to prevent weight gain D. A minimum average of two binge eating episodes a week for at least 3 months E. Persistent overconcern with body shape and weight A. Recurrent episodes of binge eating. An episode of binge eating is characterized by both of the following: (1) Eating, in a discrete period of time (e.g., within any 2-hour period), an amount of food that is definitely larger than most people would eat during a similar period of time and under similar circumstances (2) A sense of lack of control over eating during the episode (e.g., a feeling that one cannot stop eating or control what or how much one is eating) B. Recurrent inappropriate compensatory behavior in order to prevent weight gain, such as self-induced vomiting; misuse of laxatives, diuretics, enemas, or other medications; fasting or excessive exercise C. The binge eating and inappropriate compensatory behaviors both occur, on average, at least twice a week for 3 months D. Self-evaluation is unduly influenced by body shape and weight E. The disturbance does not occur exclusively during episodes of anorexia nervosa Specify type: Purging type: During the current episode of bulimia nervosa, the person has regularly engaged in self-induced vomiting or the misuse of laxatives, diuretics, or enemas Nonpurging type: During the current episode of bulimia nervosa, the person has used inappropriate compensatory behaviors, such as fasting or excessive exercise, but has not regularly engaged in self-induced vomiting or the misuse of laxatives, diuretics, or enemas DSM, Diagnostic and Statistical Manual; ICD, International Classification of Diseases. For citations, see text. 14
Healing The Hunger Recognition and Treatment of Eating Disorders
 Healing The Hunger Recognition and Treatment of Eating Disorders COPYRIGHT Copyright 2016 by Brian L. Bethel, PhD, LPCC-S, LCDC III, RPT-S Healing the Hunger, Recognition and Treatment of Eating Disorders.
Healing The Hunger Recognition and Treatment of Eating Disorders COPYRIGHT Copyright 2016 by Brian L. Bethel, PhD, LPCC-S, LCDC III, RPT-S Healing the Hunger, Recognition and Treatment of Eating Disorders.
Eating Disorders. Eating Disorders. Anorexia Nervosa. Chapter 11. The main symptoms of anorexia nervosa are:
 Eating Disorders Chapter 11 Slides & Handouts by Karen Clay Rhines, Ph.D. Northampton Community College Comer, Abnormal Psychology, 8e Eating Disorders It has not always done so, but Western society today
Eating Disorders Chapter 11 Slides & Handouts by Karen Clay Rhines, Ph.D. Northampton Community College Comer, Abnormal Psychology, 8e Eating Disorders It has not always done so, but Western society today
Hafizullah Azizi M.D.
 Hafizullah Azizi M.D. Eating disorders Feeding and Eating Disorders of Infancy and Early Childhood and Obesity Anorexia Nervosa Bulimia Nervosa EDNOS Binge Eating Disorder Purging Disorder Night Eating
Hafizullah Azizi M.D. Eating disorders Feeding and Eating Disorders of Infancy and Early Childhood and Obesity Anorexia Nervosa Bulimia Nervosa EDNOS Binge Eating Disorder Purging Disorder Night Eating
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI
 Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia Nervosa A. A refusal to maintain body weight
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia Nervosa A. A refusal to maintain body weight
Eating Disorders. Abnormal Psychology PSYCH Eating Disorders: An Overview. DSM-IV: Anorexia Nervosa
 Abnormal Psychology PSYCH 40111 Eating Disorders Eating Disorders: An Overview Two Major Types of DSM-IV Eating Disorders Anorexia nervosa and bulimia nervosa Severe disruptions in eating behavior Extreme
Abnormal Psychology PSYCH 40111 Eating Disorders Eating Disorders: An Overview Two Major Types of DSM-IV Eating Disorders Anorexia nervosa and bulimia nervosa Severe disruptions in eating behavior Extreme
Eating Disorders in Youth
 Eating Disorders in Youth Evaluating and Treating in the Medical Home February 27, 2017 Rebecca Marshall, MD, MPH Outline Anorexia Nervosa Bulimia Nervosa Binge Eating Disorder Avoidant Restrictive Food
Eating Disorders in Youth Evaluating and Treating in the Medical Home February 27, 2017 Rebecca Marshall, MD, MPH Outline Anorexia Nervosa Bulimia Nervosa Binge Eating Disorder Avoidant Restrictive Food
Module B7: Eating Disorders
 Module B7: Eating Disorders Entry scenario: The entry scenario addresses a variety of issues and problems associated with the module topic. It may be used in class to identify the needs and interests of
Module B7: Eating Disorders Entry scenario: The entry scenario addresses a variety of issues and problems associated with the module topic. It may be used in class to identify the needs and interests of
EATING DISORDERS By Briana Vittorini
 EATING DISORDERS By Briana Vittorini OVERVIEW What is an eating disorder? Important facts The SHOCKING truth The most common forms Beliefs about eating disorders Prevalence vs. Funding OVERVIEW Specific
EATING DISORDERS By Briana Vittorini OVERVIEW What is an eating disorder? Important facts The SHOCKING truth The most common forms Beliefs about eating disorders Prevalence vs. Funding OVERVIEW Specific
EATING DISORDERS AND SUBSTANCE ABUSE. Margot L. Waitz, DO October 7, 2017 AOAAM - OMED
 EATING DISORDERS AND SUBSTANCE ABUSE Margot L. Waitz, DO October 7, 2017 AOAAM - OMED OBJECTIVES Review criteria for diagnosis of several eating disorders Discuss co-morbidity of substance abuse in patients
EATING DISORDERS AND SUBSTANCE ABUSE Margot L. Waitz, DO October 7, 2017 AOAAM - OMED OBJECTIVES Review criteria for diagnosis of several eating disorders Discuss co-morbidity of substance abuse in patients
Eating Disorders Diploma Course Sample Pages Page 1
 Appallingly, a girl named Sarah Jacob died in 1967 following fasting supervised by a team of nurses who would allow her neither food nor water. The autopsy revealed that she died of dehydration and renal
Appallingly, a girl named Sarah Jacob died in 1967 following fasting supervised by a team of nurses who would allow her neither food nor water. The autopsy revealed that she died of dehydration and renal
Disordered Eating. Chapter Summary. Learning Objectives
 IN DEPTH CHAPTER 13.5 Disordered Eating Chapter Summary Eating behaviors occur along a continuum from normal, to somewhat abnormal, to disordered. An eating disorder is a psychiatric condition that involves
IN DEPTH CHAPTER 13.5 Disordered Eating Chapter Summary Eating behaviors occur along a continuum from normal, to somewhat abnormal, to disordered. An eating disorder is a psychiatric condition that involves
Eating Disorders. Anorexia Nervosa. DSM 5:Eating Disorders. DSM 5: Feeding and Eating Disorders 9/24/2015
 DSM 5: Feeding and Eating Disorders Eating Disorders Marsha D. Marcus, PhD The North American Menopause Society October 3, 2015 Feeding and Eating Disorders are characterized by a persistent disturbance
DSM 5: Feeding and Eating Disorders Eating Disorders Marsha D. Marcus, PhD The North American Menopause Society October 3, 2015 Feeding and Eating Disorders are characterized by a persistent disturbance
Disorders and Symptoms
 Eating Disorders Eating disorders is the term used to describe a category of mental illnesses involving disordered eating and weight problems. This category can then generally be separated into four main
Eating Disorders Eating disorders is the term used to describe a category of mental illnesses involving disordered eating and weight problems. This category can then generally be separated into four main
HealthPartners Care Coordination Clinical Care Planning and Resource Guide EATING DISORDER
 The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Mental Health) and the National Eating Disorders Association
The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Mental Health) and the National Eating Disorders Association
Contextualizing eating disorders. Eating Disorders. Contextualizing eating disorders. Contextualizing eating disorders
 Eating Disorders Contextualizing eating disorders Culture and gender are going to affect these in very large ways Are there different cultures with with more emphasis on physicality? Are there subcultures
Eating Disorders Contextualizing eating disorders Culture and gender are going to affect these in very large ways Are there different cultures with with more emphasis on physicality? Are there subcultures
Eating Disorders. About more than Food Teena
 Eating Disorders About more than Food Teena Eating Disorders: About More than Food What are eating disorders? The eating disorders anorexia nervosa, bulimia nervosa, and binge-eating disorder, and their
Eating Disorders About more than Food Teena Eating Disorders: About More than Food What are eating disorders? The eating disorders anorexia nervosa, bulimia nervosa, and binge-eating disorder, and their
Counseling College Women Experiencing Eating Disorder Not Otherwise Specified: A Cognitive Behavior Therapy Model
 Counseling College Women Experiencing Eating Disorder Not Otherwise Specified: A Cognitive Behavior Therapy Model Sarina: 1. Although the Counseling College Women article suggests utilizing CBT to treat
Counseling College Women Experiencing Eating Disorder Not Otherwise Specified: A Cognitive Behavior Therapy Model Sarina: 1. Although the Counseling College Women article suggests utilizing CBT to treat
Early-onset eating disorders
 Early-onset eating disorders Principal investigators Debra K. Katzman, MD, FRCPC, Division of Adolescent Medicine, Department of Paediatrics* Anne Morris, MB, BS, MPH, FRACP, Division of Adolescent Medicine,
Early-onset eating disorders Principal investigators Debra K. Katzman, MD, FRCPC, Division of Adolescent Medicine, Department of Paediatrics* Anne Morris, MB, BS, MPH, FRACP, Division of Adolescent Medicine,
Contents. Eating Disorders: Introduction. Who Gets Eating Disorders? What is Anorexia Nervosa?
 Contents Eating Disorders: Introduction Who Gets Eating Disorders? What is Anorexia Nervosa? Physical and Psychological Effects What is Bulimia Nervosa? Physical Effects What is Eating Disorders Not Otherwise
Contents Eating Disorders: Introduction Who Gets Eating Disorders? What is Anorexia Nervosa? Physical and Psychological Effects What is Bulimia Nervosa? Physical Effects What is Eating Disorders Not Otherwise
Today s Discussion Anorexia Nervosa Bulimia Nervosa Binge Eating Disorder Other eating disorders
 Kari Anderson DBH, LPC Today s Discussion Anorexia Nervosa Bulimia Nervosa Binge Eating Disorder Other eating disorders Defining an Eating Disorder An eating disorder is a complex illness that develops
Kari Anderson DBH, LPC Today s Discussion Anorexia Nervosa Bulimia Nervosa Binge Eating Disorder Other eating disorders Defining an Eating Disorder An eating disorder is a complex illness that develops
Brief Notes on the Mental Health of Children and Adolescents
 Brief Notes on the Mental Health of Children and Adolescents The future of our country depends on the mental health and strength of our young people. However, many children have mental health problems
Brief Notes on the Mental Health of Children and Adolescents The future of our country depends on the mental health and strength of our young people. However, many children have mental health problems
Eating Disorders Detection and Treatment. Scott Crow, M.D. Professor of Psychiatry University of Minnesota Chief Research Officer The Emily Program
 Eating Disorders Detection and Treatment Scott Crow, M.D. Professor of Psychiatry University of Minnesota Chief Research Officer The Emily Program Obesity Trends* Among U.S. Adults BRFSS, 1990, 1995, 2005
Eating Disorders Detection and Treatment Scott Crow, M.D. Professor of Psychiatry University of Minnesota Chief Research Officer The Emily Program Obesity Trends* Among U.S. Adults BRFSS, 1990, 1995, 2005
Disappearing Act: Interventions for Students Who Are Dying to be Thin
 Disappearing Act: Interventions for Students Who Are Dying to be Thin Judy Ordogne, MA, LPC Stacy Hall, MEd, LPC-I 4840 W Panther Creek Dr., Suite 212 The Woodlands, Texas 77381 281-465-9229 Prevalence
Disappearing Act: Interventions for Students Who Are Dying to be Thin Judy Ordogne, MA, LPC Stacy Hall, MEd, LPC-I 4840 W Panther Creek Dr., Suite 212 The Woodlands, Texas 77381 281-465-9229 Prevalence
Feeding and Eating Disorders
 The Time is Here: Differential Diagnosis and Coding Using the DSM 5 and ICD 10 Diane Snow, PhD, RN, PMHNP-BC, FAANP, FIAAN University of Texas at Arlington College of Nursing and Health Innovation IntNSA
The Time is Here: Differential Diagnosis and Coding Using the DSM 5 and ICD 10 Diane Snow, PhD, RN, PMHNP-BC, FAANP, FIAAN University of Texas at Arlington College of Nursing and Health Innovation IntNSA
+ Eating. Disorders. By: Rachel Jones & Anahi Rangel
 Eating Disorders By: Rachel Jones & Anahi Rangel Quick Facts n In the United States, 20 million women and 10 million men suffer from a clinically significant eating disorder at some time in their life
Eating Disorders By: Rachel Jones & Anahi Rangel Quick Facts n In the United States, 20 million women and 10 million men suffer from a clinically significant eating disorder at some time in their life
Outcomes of Eating Disorders: A Systematic Review of the Literature
 SPECIAL SECTION ARTICLE Outcomes of Eating Disorders: A Systematic Review of the Literature Nancy D. Berkman, PhD 1 Kathleen N. Lohr, PhD 1 Cynthia M. Bulik, PhD 2,3 * ABSTRACT Objective: The RTI International-University
SPECIAL SECTION ARTICLE Outcomes of Eating Disorders: A Systematic Review of the Literature Nancy D. Berkman, PhD 1 Kathleen N. Lohr, PhD 1 Cynthia M. Bulik, PhD 2,3 * ABSTRACT Objective: The RTI International-University
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI
 Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia A. A refusal to maintain body weight at or
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia A. A refusal to maintain body weight at or
USING DIALECTICAL BEHAVIOR THERAPY TO TREAT A VARIETY
 USING DIALECTICAL BEHAVIOR THERAPY TO TREAT A VARIETY OF DISORDERS DeLinda Spain, LCSW, CGP, CEDS Austin, Texas LEARNING OBJECTIVES Diagnostic criteria for Eating Disorders Diagnosis History of Dialectical
USING DIALECTICAL BEHAVIOR THERAPY TO TREAT A VARIETY OF DISORDERS DeLinda Spain, LCSW, CGP, CEDS Austin, Texas LEARNING OBJECTIVES Diagnostic criteria for Eating Disorders Diagnosis History of Dialectical
Diagnosing adult patients with feeding and eating disorders - challenges and pitfalls
 Diagnosing adult patients with feeding and eating disorders - challenges and pitfalls Professor Øyvind Rø, MD Psychologist Kristin Stedal, PhD Oslo Universitetssykehus oyvind.ro@ous-hf.no After 20 years
Diagnosing adult patients with feeding and eating disorders - challenges and pitfalls Professor Øyvind Rø, MD Psychologist Kristin Stedal, PhD Oslo Universitetssykehus oyvind.ro@ous-hf.no After 20 years
1 What is an Eating Disorder?
 3259-Gilbert-01.qxd 4/5/2005 5:53 PM Page 1 1 What is an Eating Disorder? Interest in eating disorders has mushroomed in the past twenty years. Until the early 1980s, most people knew about the existence
3259-Gilbert-01.qxd 4/5/2005 5:53 PM Page 1 1 What is an Eating Disorder? Interest in eating disorders has mushroomed in the past twenty years. Until the early 1980s, most people knew about the existence
IMPLICATIONS OF THE DSM-5 REVISIONS ON THE DIAGNOSIS AND TREATMENT OF EATING DISORDERS
 IMPLICATIONS OF THE DSM-5 REVISIONS ON THE DIAGNOSIS AND TREATMENT OF EATING DISORDERS PRESENTED BY KARYN L. SCHER, PH.D. 6/18/14 PENNSYLVANIA PSYCHOLOGICAL ASSOCIATION ANNUAL CONVENTION ABSTRACT Eating
IMPLICATIONS OF THE DSM-5 REVISIONS ON THE DIAGNOSIS AND TREATMENT OF EATING DISORDERS PRESENTED BY KARYN L. SCHER, PH.D. 6/18/14 PENNSYLVANIA PSYCHOLOGICAL ASSOCIATION ANNUAL CONVENTION ABSTRACT Eating
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE. Personality Disorder: the clinical management of borderline personality disorder
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality Disorder: the clinical management of borderline personality disorder 1.1 Short title Borderline personality disorder
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality Disorder: the clinical management of borderline personality disorder 1.1 Short title Borderline personality disorder
The diagnosis and classification of feeding and eating disorders in children and young people
 The diagnosis and classification of feeding and eating disorders in children and young people Joy Olver Medical doctor Consultant child and adolescent psychiatrist NHS Tayside since 2004 Lead for Eating
The diagnosis and classification of feeding and eating disorders in children and young people Joy Olver Medical doctor Consultant child and adolescent psychiatrist NHS Tayside since 2004 Lead for Eating
Contemporary Psychiatric-Mental Health Nursing. Effect of Culture. Biologic Theory. Chapter 21 Eating Disorders
 Contemporary Psychiatric-Mental Health Nursing Chapter 21 Eating Disorders Effect of Culture Cultural stereotypes Preoccupation with the body Cultural ideal of thinness Identity and self-esteem are dependent
Contemporary Psychiatric-Mental Health Nursing Chapter 21 Eating Disorders Effect of Culture Cultural stereotypes Preoccupation with the body Cultural ideal of thinness Identity and self-esteem are dependent
SECTION 1. Children and Adolescents with Depressive Disorder: Summary of Findings. from the Literature and Clinical Consultation in Ontario
 SECTION 1 Children and Adolescents with Depressive Disorder: Summary of Findings from the Literature and Clinical Consultation in Ontario Children's Mental Health Ontario Children and Adolescents with
SECTION 1 Children and Adolescents with Depressive Disorder: Summary of Findings from the Literature and Clinical Consultation in Ontario Children's Mental Health Ontario Children and Adolescents with
Nonpharmacologic Interventions for Treatment-Resistant Depression in Adults
 Comparative Effectiveness Review Number XX Nonpharmacologic Interventions for Treatment-Resistant Depression in Adults Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health
Comparative Effectiveness Review Number XX Nonpharmacologic Interventions for Treatment-Resistant Depression in Adults Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health
BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES
 BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES Craig Johnson, PhD, FAED, CEDS, Chief Science Officer Emmett R. Bishop Jr., MD, FAED,
BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES Craig Johnson, PhD, FAED, CEDS, Chief Science Officer Emmett R. Bishop Jr., MD, FAED,
The Carter-Jenkins Center presents
 The Carter-Jenkins Center presents Michael Poff, MSW, MA Anorexia in Childhood: A Case Presentation Michael Poff, MSW, MA The Carter-Jenkins Center Diagnosis, Epidemiology and Related Findings Eating disturbances
The Carter-Jenkins Center presents Michael Poff, MSW, MA Anorexia in Childhood: A Case Presentation Michael Poff, MSW, MA The Carter-Jenkins Center Diagnosis, Epidemiology and Related Findings Eating disturbances
MEDICAL POLICY No R8 EATING DISORDERS POLICY/CRITERIA
 EATING DISORDERS MEDICAL POLICY Effective Date: June 27, 2016 Review Dates: 1/93, 8/96, 4/99, 12/01, 12/02, 11/03, 11/04, 10/05, 10/06, 10/07, 8/08, 8/09, 8/10, 8/11, 8/12, 8/13, 5/14, 5/15, 5/16 Date
EATING DISORDERS MEDICAL POLICY Effective Date: June 27, 2016 Review Dates: 1/93, 8/96, 4/99, 12/01, 12/02, 11/03, 11/04, 10/05, 10/06, 10/07, 8/08, 8/09, 8/10, 8/11, 8/12, 8/13, 5/14, 5/15, 5/16 Date
Eating Disorders in Athletes: Women and Men
 Eating Disorders in : Women and Men Barbara J Long MD MPH Associate Clinical Professor Division of Adolescent Medicine University of California, San Francisco Why discuss eating disorders and the athlete?
Eating Disorders in : Women and Men Barbara J Long MD MPH Associate Clinical Professor Division of Adolescent Medicine University of California, San Francisco Why discuss eating disorders and the athlete?
Eating Disorders. Anorexia Nervosa Bulimia Nervosa
 Eating Disorders Anorexia Nervosa Bulimia Nervosa DSM-IV-TR Anorexia Nervosa: nervous loss of appetite Anorexia: loss of appetite Anorexia Nervosa Characterized by: Intense fear of becoming fat or
Eating Disorders Anorexia Nervosa Bulimia Nervosa DSM-IV-TR Anorexia Nervosa: nervous loss of appetite Anorexia: loss of appetite Anorexia Nervosa Characterized by: Intense fear of becoming fat or
Cognition and Psychopathology
 Cognition and Psychopathology Lecture 6: Eating Disorders Eating Disorders Eating disorders are characterized by severe disturbances in eating behaviour, coupled with distorted cognitions involving body
Cognition and Psychopathology Lecture 6: Eating Disorders Eating Disorders Eating disorders are characterized by severe disturbances in eating behaviour, coupled with distorted cognitions involving body
The Interesting Relationship Between ADHD, Eating Disorders and Body Image
 The Interesting Relationship Between ADHD, Eating Disorders and Body Image Roberto Olivardia, Ph.D. Harvard Medical School Roberto_Olivardia@hms.harvard.edu Binge Eating Disorder Recurrent episodes of
The Interesting Relationship Between ADHD, Eating Disorders and Body Image Roberto Olivardia, Ph.D. Harvard Medical School Roberto_Olivardia@hms.harvard.edu Binge Eating Disorder Recurrent episodes of
Anorexia nervosa ---concept / etiology
 Eating Disorders Epidemiology; 4% of adolescent and young adults students Anorexia nervosa has\been reported more frequently over the past several decades with increasing reports of the disorder in the
Eating Disorders Epidemiology; 4% of adolescent and young adults students Anorexia nervosa has\been reported more frequently over the past several decades with increasing reports of the disorder in the
Psychology Session 11 Psychological Disorders
 Psychology Session 11 Psychological Disorders Date: November 18th, 2016 Course instructor: Cherry Chan Mothercraft College Agenda 1. Normal vs. Abnormal 2. Communication disorders 3. Anxiety disorders
Psychology Session 11 Psychological Disorders Date: November 18th, 2016 Course instructor: Cherry Chan Mothercraft College Agenda 1. Normal vs. Abnormal 2. Communication disorders 3. Anxiety disorders
INTRODUCTION S. Who are Therapy Partners? Who am I and what do I do?
 INTRODUCTION S Who are Therapy Partners? Who am I and what do I do? Therapy Partners are a Team of Specialists that work together with one goal in mind, to help support young People that have developed
INTRODUCTION S Who are Therapy Partners? Who am I and what do I do? Therapy Partners are a Team of Specialists that work together with one goal in mind, to help support young People that have developed
Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care
 Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care CLINICAL ASSESSMENT AND DIAGNOSIS (ADULTS) Obsessive-Compulsive Disorder (OCD) is categorized by recurrent obsessions,
Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care CLINICAL ASSESSMENT AND DIAGNOSIS (ADULTS) Obsessive-Compulsive Disorder (OCD) is categorized by recurrent obsessions,
Declaration. Overview Eating Disorders in Children and Adolescents
 Eating Disorders in Children and Adolescents Dr Pei-Yoong Lam FRACP Assistant Clinical Professor, Division of Adolescent Health and Medicine Declaration I have no commercial affiliations or conflicts of
Eating Disorders in Children and Adolescents Dr Pei-Yoong Lam FRACP Assistant Clinical Professor, Division of Adolescent Health and Medicine Declaration I have no commercial affiliations or conflicts of
Methods Research Report Comparative Effectiveness Review Methods: Clinical Heterogeneity
 Methods Research Report Comparative Effectiveness Review Methods: Clinical Heterogeneity Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health and Human Services 540 Gaither
Methods Research Report Comparative Effectiveness Review Methods: Clinical Heterogeneity Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health and Human Services 540 Gaither
THE EATING DISORDERS ASSOCIATION OF QLD. 12 Chatsworth Road Greenslopes STUDENT PACK. On eating disorders
 THE EATING DISORDERS ASSOCIATION OF QLD 12 Chatsworth Road Greenslopes 4120 07 3394 3661 www.eda.org.au STUDENT PACK On eating disorders Eating Disorders: An Information Pack Eating Disorders - Overview
THE EATING DISORDERS ASSOCIATION OF QLD 12 Chatsworth Road Greenslopes 4120 07 3394 3661 www.eda.org.au STUDENT PACK On eating disorders Eating Disorders: An Information Pack Eating Disorders - Overview
Self Evaluation. Bulimia Nervosa Diagnostic Criteria 30/08/2012. Client's Current Self-Evaluation Pie Chart Relationship
 Rachel Lawson Acting Clinical Head Project Leader Eating Disorders The Werry Centre ED and SUDS in Adolescence Background Research is limited Prevalence about a third Vast majority of those will have Bulimia
Rachel Lawson Acting Clinical Head Project Leader Eating Disorders The Werry Centre ED and SUDS in Adolescence Background Research is limited Prevalence about a third Vast majority of those will have Bulimia
Developing a new treatment approach to binge eating and weight management. Clinical Psychology Forum, Number 244, April 2013.
 Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
Eating Disorders: Clinical Features, Comorbidity, and Treatment
 Eating Disorders: Clinical Features, Comorbidity, and Treatment Carol B. Peterson, PhD Associate Professor Eating Disorders Research Program Department of Psychiatry University of Minnesota peter161@umn.edu
Eating Disorders: Clinical Features, Comorbidity, and Treatment Carol B. Peterson, PhD Associate Professor Eating Disorders Research Program Department of Psychiatry University of Minnesota peter161@umn.edu
b) Not being bothered about weight gain c) Regularly engaging in purging activities to help control weight gain (A) d) Eating only certain food types
 Chapter 9 Teachers 1. According to DSM-IV-TR which of the following is a diagnostic criterion for anorexia nervosa? a. A refusal to maintain a minimal body weight b. A pathological fear of gaining weight
Chapter 9 Teachers 1. According to DSM-IV-TR which of the following is a diagnostic criterion for anorexia nervosa? a. A refusal to maintain a minimal body weight b. A pathological fear of gaining weight
Eating Disorders in Adolescents
 Eating Disorders in Adolescents Rose Calderon, Ph.D. Associate Professor University of Washington Clinical Director Eating Disorders Program Children s Hospital and Regional Medical Center Objectives Gain
Eating Disorders in Adolescents Rose Calderon, Ph.D. Associate Professor University of Washington Clinical Director Eating Disorders Program Children s Hospital and Regional Medical Center Objectives Gain
Chapter 33. The Child with an Emotional or Behavioral Condition
 Chapter 33 The Child with an Emotional or Behavioral Condition Objectives Differentiate among the following terms: psychiatrist, psychoanalyst, clinical psychologist, and counselor. Discuss the impact
Chapter 33 The Child with an Emotional or Behavioral Condition Objectives Differentiate among the following terms: psychiatrist, psychoanalyst, clinical psychologist, and counselor. Discuss the impact
Paper s Information. Eating Disorder Diagnoses. Paper Type: Essay. Word Count: 1700 words. Referencing Style: APA Style
 1 Paper s Information Topic: Eating Disorder Diagnoses Paper Type: Essay Word Count: 1700 words Pages: 7pages Referencing Style: APA Style Education Level: Under Graduate 2 Running Head: EATING DISORDER
1 Paper s Information Topic: Eating Disorder Diagnoses Paper Type: Essay Word Count: 1700 words Pages: 7pages Referencing Style: APA Style Education Level: Under Graduate 2 Running Head: EATING DISORDER
U.S. Preventive Services Task Force Methods and Processes. Alex R. Kemper, MD, MPH, MS June 16, 2014
 1 U.S. Preventive Services Task Force Methods and Processes Alex R. Kemper, MD, MPH, MS June 16, 2014 2 Goals Improve understanding of the U.S. Preventive Services Task Force (USPSTF or Task Force) Explain
1 U.S. Preventive Services Task Force Methods and Processes Alex R. Kemper, MD, MPH, MS June 16, 2014 2 Goals Improve understanding of the U.S. Preventive Services Task Force (USPSTF or Task Force) Explain
Eating Disorders. Sristi Nath, D.O. Early Identification and Proactive Treatment November 12, Disclosures
 Eating Disorders Sristi Nath, D.O. Early Identification and Proactive Treatment November 12, 2016 1 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation.
Eating Disorders Sristi Nath, D.O. Early Identification and Proactive Treatment November 12, 2016 1 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation.
Core interventions in the treatment and management of anorexia nervosa, bulimia nervosa and related eating disorders
 Issue date: January 2004 Quick reference guide Eating disorders ore interventions in the treatment and management of anorexia nervosa, bulimia nervosa and related eating disorders linical Guideline 9 Developed
Issue date: January 2004 Quick reference guide Eating disorders ore interventions in the treatment and management of anorexia nervosa, bulimia nervosa and related eating disorders linical Guideline 9 Developed
Pediatric Psychopharmacology
 Pediatric Psychopharmacology General issues to consider. Pharmacokinetic differences Availability of Clinical Data Psychiatric Disorders can be common in childhood. Early intervention may prevent disorders
Pediatric Psychopharmacology General issues to consider. Pharmacokinetic differences Availability of Clinical Data Psychiatric Disorders can be common in childhood. Early intervention may prevent disorders
Avoidant Restrictive Food Intake Disorder (ARFID)
 Avoidant Restrictive Food Intake Disorder (ARFID) TABLE OF CONTENTS Introduction................................................3 What Is ARFID?............................................. 4 How Is ARFID
Avoidant Restrictive Food Intake Disorder (ARFID) TABLE OF CONTENTS Introduction................................................3 What Is ARFID?............................................. 4 How Is ARFID
CARE BUNDLE Robyn Girling-Butcher
 CARE BUNDLE Robyn Girling-Butcher Senior Clinical Psychologist Child, Adolescent & Family Service Mental Health MidCentral DHB Principles of Care AN has highest death rate of any mental health disorder
CARE BUNDLE Robyn Girling-Butcher Senior Clinical Psychologist Child, Adolescent & Family Service Mental Health MidCentral DHB Principles of Care AN has highest death rate of any mental health disorder
Review Article. Eating Disorders in Children and Adolescents Fayyaz Khan and Uttom Chowdhury. BJMP 2011;4(1):a405
 BJMP 2011;4(1):a405 Review Article Eating Disorders in Children and Adolescents Fayyaz Khan and Uttom Chowdhury Eating disorders are defined as those disorders in which there is excessive concern with
BJMP 2011;4(1):a405 Review Article Eating Disorders in Children and Adolescents Fayyaz Khan and Uttom Chowdhury Eating disorders are defined as those disorders in which there is excessive concern with
DIETARY AND EXERCISE PATTERNS
 DIETARY AND EXERCISE PATTERNS Establishing healthy eating and physical exercise habits at an early age is important Both dietary and exercise patterns formed during childhood can carry into adulthood producing
DIETARY AND EXERCISE PATTERNS Establishing healthy eating and physical exercise habits at an early age is important Both dietary and exercise patterns formed during childhood can carry into adulthood producing
Eating Disorders A Hidden Killer
 Eating Disorders A Hidden Killer Scott K. Bullock M.S.W., LISW-S, CEDS Clinical Director/Family Therapist Child and Adolescent Services Harold C. Schott Eating Disorder Foundation Founder/Director PROXIMI
Eating Disorders A Hidden Killer Scott K. Bullock M.S.W., LISW-S, CEDS Clinical Director/Family Therapist Child and Adolescent Services Harold C. Schott Eating Disorder Foundation Founder/Director PROXIMI
Eating disorders and hyperactivity. By: Cristina González, Luis Mayo and Mariña Prego
 Eating disorders and hyperactivity By: Cristina González, Luis Mayo and Mariña Prego 1.- Eating disorders: 1.1.- What is it about? 1.2.- Origin and factors 1.3.- Treatment 1.4.- Examples and cases Index
Eating disorders and hyperactivity By: Cristina González, Luis Mayo and Mariña Prego 1.- Eating disorders: 1.1.- What is it about? 1.2.- Origin and factors 1.3.- Treatment 1.4.- Examples and cases Index
Challenges of Adolescence. Chapter 11 - Adolescence
 Challenges of Adolescence Chapter 11 - Adolescence Eating Disorders Anorexia Nervosa Bulimia Magazines Diet Articles in 1920 s- 0 Diet Articles 1930 s and 1940 sone diet article for every ten issues. Diet
Challenges of Adolescence Chapter 11 - Adolescence Eating Disorders Anorexia Nervosa Bulimia Magazines Diet Articles in 1920 s- 0 Diet Articles 1930 s and 1940 sone diet article for every ten issues. Diet
Eating disorders. Introduction SUMMARY
 8 Eating disorders SUMMARY The eating disorders included in this chapter are relatively uncommon and in many cases are not treated. The numbers of people with these eating disorders is likely to increase
8 Eating disorders SUMMARY The eating disorders included in this chapter are relatively uncommon and in many cases are not treated. The numbers of people with these eating disorders is likely to increase
Psychological Definition of a Mental Disorder
 Mental Illness Disclaimer Please do not start diagnosing yourself, friends, family, or school mates. This section will provide common traits of certain Mental Illnesses, it will not enable you to make
Mental Illness Disclaimer Please do not start diagnosing yourself, friends, family, or school mates. This section will provide common traits of certain Mental Illnesses, it will not enable you to make
Eating Disorders in Old Age
 Eating Disorders in Old Age Dr. William Rhys Jones Consultant Psychiatrist & Clinical Lead CONNECT: The West Yorkshire and Harrogate Adult Eating Disorders Service r.jones9@nhs.net 0113 855 6400 Eating
Eating Disorders in Old Age Dr. William Rhys Jones Consultant Psychiatrist & Clinical Lead CONNECT: The West Yorkshire and Harrogate Adult Eating Disorders Service r.jones9@nhs.net 0113 855 6400 Eating
Test Your Knowledge! True or False? CLASS OBJECTIVES: Mirror, mirror on the wall, who's the fattest one of all?"
 Mirror, mirror on the wall, who's the fattest one of all?" CLASS OBJECTIVES: What are eating disorders? What is the difference between Bulimia Nervosa and Anorexia Nervosa? What are the diagnostic characteristics
Mirror, mirror on the wall, who's the fattest one of all?" CLASS OBJECTIVES: What are eating disorders? What is the difference between Bulimia Nervosa and Anorexia Nervosa? What are the diagnostic characteristics
Pharmacotherapy for Alcohol Dependence
 Evidence Report/Technology Assessment: Number 3 Pharmacotherapy for Alcohol Dependence Summary Under its Evidence-Based Practice Program, the Agency for Health Care Policy and Research (AHCPR) is developing
Evidence Report/Technology Assessment: Number 3 Pharmacotherapy for Alcohol Dependence Summary Under its Evidence-Based Practice Program, the Agency for Health Care Policy and Research (AHCPR) is developing
Avoidant/restrictive food intake disorder: Introducing a new DSM-5 eating disorder
 Avoidant/restrictive food intake disorder: Introducing a new DSM-5 eating disorder Debra Katzman, MD FRCPC, The Hospital for Sick Children and University of Toronto Karizma Mawjee, BA MA, The Hospital
Avoidant/restrictive food intake disorder: Introducing a new DSM-5 eating disorder Debra Katzman, MD FRCPC, The Hospital for Sick Children and University of Toronto Karizma Mawjee, BA MA, The Hospital
HERTFORDSHIRE PARTNERSHIP UNIVERSITY NHS FOUNDATION TRUST. Referral Criteria for Specialist Tier 3 CAMHS
 Referral Criteria for Specialist Tier 3 CAMHS Specialist CAMHS provides mental health support, advice and guidance and treatment for Children and Young People with moderate or severe mental health difficulties,
Referral Criteria for Specialist Tier 3 CAMHS Specialist CAMHS provides mental health support, advice and guidance and treatment for Children and Young People with moderate or severe mental health difficulties,
6/22/2012. Co-morbidity - when two or more conditions occur together. The two conditions may or may not be causally related.
 Autism Spectrum Disorders and Co-existing Mental Health Issues By Dr. Karen Berkman Objective To present an overview of common psychiatric conditions that occur in persons with autism spectrum disorders
Autism Spectrum Disorders and Co-existing Mental Health Issues By Dr. Karen Berkman Objective To present an overview of common psychiatric conditions that occur in persons with autism spectrum disorders
UC Merced UC Merced Undergraduate Research Journal
 UC Merced UC Merced Undergraduate Research Journal Title Efficacy of Cognitive Behavioral Therapy in Treating Anorexia Nervosa: A Review of Literature Permalink https://escholarship.org/uc/item/2c06j71p
UC Merced UC Merced Undergraduate Research Journal Title Efficacy of Cognitive Behavioral Therapy in Treating Anorexia Nervosa: A Review of Literature Permalink https://escholarship.org/uc/item/2c06j71p
New Directions, a psycho-educational program for adolescents with eating disorders: Stage two in a multi-step program evaluation
 New Directions, a psycho-educational program for adolescents with eating disorders: Stage two in a multi-step program evaluation Authors: Mary Kaye Lucier MSW, RSW, Executive Director, Bulimia Anorexia
New Directions, a psycho-educational program for adolescents with eating disorders: Stage two in a multi-step program evaluation Authors: Mary Kaye Lucier MSW, RSW, Executive Director, Bulimia Anorexia
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency London, 15 November 2007 Doc. Ref. EMEA/CHMP/EWP/517497/2007 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON CLINICAL EVALUATION OF MEDICINAL PRODUCTS USED
European Medicines Agency London, 15 November 2007 Doc. Ref. EMEA/CHMP/EWP/517497/2007 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON CLINICAL EVALUATION OF MEDICINAL PRODUCTS USED
Linkoping University/ Sweden An-Najah National University Nursing College College of Higher Educaion. Dr Aidah Abu Elsoud Alkaissi
 Dr. Aidah Abu Elsoud Alkaissi Linkoping University/ Sweden An-Najah National University Nursing College College of Higher Educaion 1 Are predominantly diseases of females, who comprise between 90% and
Dr. Aidah Abu Elsoud Alkaissi Linkoping University/ Sweden An-Najah National University Nursing College College of Higher Educaion 1 Are predominantly diseases of females, who comprise between 90% and
Inpatient Mental Health
 Inpatient Mental Health BEACON HEALTH STRATEGIES, LLC ORIGINAL EFFECTIVE DATE HAWAII LEVEL OF CARE CRITERIA 2013 CURRENT EFFECTIVE DATE 2016 I. Description Acute Inpatient Psychiatric Services are the
Inpatient Mental Health BEACON HEALTH STRATEGIES, LLC ORIGINAL EFFECTIVE DATE HAWAII LEVEL OF CARE CRITERIA 2013 CURRENT EFFECTIVE DATE 2016 I. Description Acute Inpatient Psychiatric Services are the
To increase understanding and awareness of eating disorders. To provide support to staff dealing with pupils suffering from eating disorders
 Policy on Eating Disorders The care of those who are sick in the community is an absolute priority which must rank before every other requirement so that there may be no doubt that it is Christ who is
Policy on Eating Disorders The care of those who are sick in the community is an absolute priority which must rank before every other requirement so that there may be no doubt that it is Christ who is
EATING DISORDER? COULD IT BE THAT YOU SUFFER FROM AN. ebook
 COULD IT BE THAT YOU SUFFER FROM AN EATING DISORDER? ebook 1. Introduction 2. Types of eating disorders 2.1 Anorexia Nervosa 2.2 Bulimia Nervosa 2.3 Eating Disorder Not Otherwise Specified (EDNOS) 2.3.1
COULD IT BE THAT YOU SUFFER FROM AN EATING DISORDER? ebook 1. Introduction 2. Types of eating disorders 2.1 Anorexia Nervosa 2.2 Bulimia Nervosa 2.3 Eating Disorder Not Otherwise Specified (EDNOS) 2.3.1
Department of Psychiatry, Hokkaido University Graduate School of Medicine North 15, West 7, Sapporo , JAPAN
 Title Clinical Study of Early-Onset Eating Disorders Authors Kenzo Denda, M.D., Ph.D. 1 Yuki Kako, M.D. 1 Nobuki Kitagawa, M.D. 1 Tsukasa Koyama, M.D., Ph.D. 1 Affiliation 1 Department of Psychiatry, Hokkaido
Title Clinical Study of Early-Onset Eating Disorders Authors Kenzo Denda, M.D., Ph.D. 1 Yuki Kako, M.D. 1 Nobuki Kitagawa, M.D. 1 Tsukasa Koyama, M.D., Ph.D. 1 Affiliation 1 Department of Psychiatry, Hokkaido
Condensed Clinical Practice Guideline Treatment Of Patients With Schizophrenia
 Condensed Clinical Practice Guideline Treatment Of Patients With Schizophrenia I. Key Points a. Schizophrenia is a chronic illness affecting all aspects of person s life i. Treatment Planning Goals 1.
Condensed Clinical Practice Guideline Treatment Of Patients With Schizophrenia I. Key Points a. Schizophrenia is a chronic illness affecting all aspects of person s life i. Treatment Planning Goals 1.
Summary of guideline for the. treatment of depression RANZCP CLINICAL PRACTICE GUIDELINES ASSESSMENT
 RANZCP CLINICAL PRACTICE GUIDELINES Summary of guideline for the RANZCP CLINICAL PRACTICE GUIDELINES treatment of depression Pete M. Ellis, Ian B. Hickie and Don A. R. Smith for the RANZCP Clinical Practice
RANZCP CLINICAL PRACTICE GUIDELINES Summary of guideline for the RANZCP CLINICAL PRACTICE GUIDELINES treatment of depression Pete M. Ellis, Ian B. Hickie and Don A. R. Smith for the RANZCP Clinical Practice
MEDICAL POLICY EFFECTIVE DATE: 04/28/11 REVISED DATE: 04/26/12, 04/25/13, 04/24/14, 06/25/15, 06/22/16, 06/22/17
 MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
Eating Disorders 2.0 Contact Hours Presented by: CEU Professor
 Eating Disorders 2.0 Contact Hours Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2007 The Magellan Group, LLC All Rights Reserved. Reproduction and distribution of these materials
Eating Disorders 2.0 Contact Hours Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2007 The Magellan Group, LLC All Rights Reserved. Reproduction and distribution of these materials
Psychological Disorders. Schizophrenia Spectrum & Other Psychotic Disorders. Schizophrenia. Neurodevelopmental Disorders 4/12/2018
 Psychological s Schizophrenia Spectrum & Other Psychotic s Schizophrenia Spectrum & Other Psychotic s 0Presence of delusions, hallucinations, disorganized thinking/speech, disorganized or abnormal motor
Psychological s Schizophrenia Spectrum & Other Psychotic s Schizophrenia Spectrum & Other Psychotic s 0Presence of delusions, hallucinations, disorganized thinking/speech, disorganized or abnormal motor
Eating disorders and disordered eating in sport
 member of the ioc medical research network 2015-18 Eating disorders and disordered eating in sport An introduction for coaches and sports professionals National Centre for Sport and Exercise Medicine East
member of the ioc medical research network 2015-18 Eating disorders and disordered eating in sport An introduction for coaches and sports professionals National Centre for Sport and Exercise Medicine East
Washington County. Mental Health Practice Guidelines 2007
 Washington County Mental Health Practice Guidelines 2007 Washington County Mental Health Practice Guidelines 2007 Please direct any comments, revisions or requests for updated versions to: Jill Archer,
Washington County Mental Health Practice Guidelines 2007 Washington County Mental Health Practice Guidelines 2007 Please direct any comments, revisions or requests for updated versions to: Jill Archer,
NUTRITIONAL COUNSELING Corporate Medical Policy
 NUTRITIONAL COUNSELING Corporate Medical Policy File Name: Nutritional Counseling File Code: RB.NC.01 Origination: 04/2002 Last Review: 07/2018 Next Review: 07/2019 Effective Date: 11/01/2018 Description/Summary
NUTRITIONAL COUNSELING Corporate Medical Policy File Name: Nutritional Counseling File Code: RB.NC.01 Origination: 04/2002 Last Review: 07/2018 Next Review: 07/2019 Effective Date: 11/01/2018 Description/Summary
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality disorder: the management and prevention of antisocial (dissocial) personality disorder 1.1 Short title Antisocial
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality disorder: the management and prevention of antisocial (dissocial) personality disorder 1.1 Short title Antisocial
Washington County. Mental Health Practice Guidelines 2013
 Washington County Mental Health Practice Guidelines 2013 Washington County Mental Health Practice Guidelines 2013 Please direct any comments, revisions or requests for updated versions to: Nicholas Ocon,
Washington County Mental Health Practice Guidelines 2013 Washington County Mental Health Practice Guidelines 2013 Please direct any comments, revisions or requests for updated versions to: Nicholas Ocon,
Treatment and Outreach Program for Eating Disorders (TOP-ED)
 Treatment and Outreach Program for Eating Disorders (TOP-ED) www.aubmc.org Copyright 2017 American University of Beirut. All rights reserved. 1 What Are Eating Disorders? Eating disorders are disturbances
Treatment and Outreach Program for Eating Disorders (TOP-ED) www.aubmc.org Copyright 2017 American University of Beirut. All rights reserved. 1 What Are Eating Disorders? Eating disorders are disturbances
Follow this and additional works at: Part of the Medicine and Health Sciences Commons
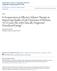 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Acupuncture an Effective Adjunct Therapy
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Acupuncture an Effective Adjunct Therapy
Obesity Management of patients with mental illness
 Obesity Management of patients with mental illness Prof. Dr. Mohamed Aboulghate Faculty of Medicine, Cairo University Secretary General, EMASO Points to be discussed Is obesity a psychiatric disorder(addiction,
Obesity Management of patients with mental illness Prof. Dr. Mohamed Aboulghate Faculty of Medicine, Cairo University Secretary General, EMASO Points to be discussed Is obesity a psychiatric disorder(addiction,
TREATMENT OUTCOMES REPORT
 TREATMENT OUTCOMES REPORT 2016 EDITION Helping patients, families and professionals understand treatment results Eating Recovery Center Treatment Outcomes Report, 2016 Edition Helping patients, families
TREATMENT OUTCOMES REPORT 2016 EDITION Helping patients, families and professionals understand treatment results Eating Recovery Center Treatment Outcomes Report, 2016 Edition Helping patients, families
EATING DISORDER ESSENTIALS. Jess Willard, LCSW-C Professional Relations Representative The Renfrew Center
 EATING DISORDER ESSENTIALS Jess Willard, LCSW-C Professional Relations Representative The Renfrew Center EATING DISORDERS ARE illnesses not choices THE DANGEROUS REALITY There is a lingering perception
EATING DISORDER ESSENTIALS Jess Willard, LCSW-C Professional Relations Representative The Renfrew Center EATING DISORDERS ARE illnesses not choices THE DANGEROUS REALITY There is a lingering perception
