Evaluation of Semi-Quantitative Scoring System for Metaiodobenzylguanidine (mibg) Scans in Patients With Relapsed Neuroblastoma
|
|
|
- Cordelia Lambert
- 5 years ago
- Views:
Transcription
1 Pediatr Blood Cancer 2006;47: Evaluation of Semi-Quantitative Scoring System for Metaiodobenzylguanidine (mibg) Scans in Patients With Relapsed Neuroblastoma Julia A. Messina, BS, 1 Su-Chun Cheng, ScD, 2 Benjamin L. Franc, MD, 3 Martin Charron, MD, 4 Barry Shulkin, MD, 6 Bao To, MD, 3 John M. Maris, MD, 5 Gregory Yanik, MD, 7 Randall A. Hawkins, MD, PhD, 3 and Katherine K. Matthay, MD 1 * Background. The purpose of this study was to determine the accuracy of two semi-quantitative scoring systems to assess response to 131 I-metaiodobenzylguanidine (mibg) therapy in recurrent neuroblastoma. Procedures. Diagnostic mibg scan pairs (n ¼ 57) were collected for patients who underwent 131 I-mIBG therapy for relapsed neuroblastoma. Two scoring systems were designated: Method 1, which divided the body into nine segments to view osteomedullary lesions with an additional tenth segment to assess soft tissue involvement; and Method 2, which divided the body into seven segments without a corresponding compartment for soft tissue involvement. Four nuclear medicine physicians independently assigned extension and intensity scores utilizing both methods, and separately recorded their impression of whether the post-therapy scan had improved, not changed, or worsened. Inter- and intraobserver concordance and correlation with overall response and progression-free survival (PFS) were performed. Results. Method 1 produced the highest inter-observer concordance and was used to calculate the relative extension scores (post-therapy score divided by pre-therapy score), which correlated significantly with overall response. Patients who achieved complete response (CR) or partial response (PR) (n ¼ 21) had lower relative extension scores, compared to those without response (P < 0.001). The readers overall impression associated highly (P < 0.001) with the relative extension scores though results were less quantitative. Concordance was higher if initial scores were >5. Relative extension score did not predict PFS. Conclusion. Semi-quantitative scoring of mibg scans provides a more reliable method of assessing response in patients with relapsed neuroblastoma than qualitative impression. The reproducibility and high inter-observer concordance makes mibg score an important component of overall response criteria in patients with recurrent neuroblastoma.pediatr Blood Cancer 2006;47: ß 2006 Wiley-Liss, Inc. Key words: 131 I-metaiodobenzylguanidine; international neuroblastoma response criteria; mibg score; neuroblastoma INTRODUCTION Neuroblastoma, the most common extra-cranial solid tumor in children, originates as a primary tumor of the sympathetic nervous system but metastasizes often to bone and bone marrow, resulting in a poor prognosis. Approximately 15% of patients who present with metastatic disease at diagnosis are refractory to induction chemotherapy while 40% will eventually relapse after having a complete response (CR) or partial response (PR) [1]. Intravenous administration of radiolabeled metaiodobenzylguanidine (mibg), a norepinephrine analog that specifically targets malignant cells of the sympathetic nervous system, is an effective therapy for patients with refractory disease, with response rates of 30 40% [2 8]. Many of the patients who undergo therapy with 131 I-mIBG or other treatments for relapsed neuroblastoma have sites of disease only apparent on mibg scans or in bone marrow biopsies and cannot be evaluated by standard response criteria for solid tumors, such as the RECIST criteria [9]. Therefore, a standardized scoring system to predict the clinical response and progression-free survival (PFS) with 131 I-mIBG treatment is needed to help quantitate therapeutic efficacy of agents used in treatment of refractory neuroblastoma. In recent analyses of high-risk, metastatic neuroblastoma, semi-quantitative scoring systems that divide the body into anatomical sections were developed to assign numeric scores to patients diagnostic 123 I and 131 I-mIBG scans [10 14]. Assessing extent of disease before, during, and after ß 2006 Wiley-Liss, Inc. DOI /pbc induction chemotherapy, three studies have shown a correlation between semi-quantitative scores either at diagnosis or during induction with response at the end of induction chemotherapy [10,12,13] while another showed good concordance among scan readers but poor correlation with response [14]. Although some of these studies showed a significant correlation between the change in semi-quantitative score 1 Department of Pediatrics, University of California, San Francisco, California; 2 Department of Epidemiology and Biostatistics, University of California, San Francisco, California; 3 Department of Nuclear Medicine, University of California, San Francisco, California; 4 Department of Nuclear Medicine, Hospital for Sick Children, University of Toronto, Toronto, Canada; 5 Department of Pediatrics, Children s Hospital of Philadelphia and the University of Pennsylvania, Philadelphia, Pennsylvania; 6 Department of Nuclear Medicine, St. Jude Children s Research Hospital, University of Michigan, Ann Arbor, Michigan; 7 Department of Pediatrics, University of Michigan, Ann Arbor, Michigan Grant sponsor: National Institute of Health; Grant numbers: PO1 CA81403, 2MO1 RR0127; Grant sponsor: Campini Foundation; Grant sponsor: Conner Research Fund; Grant sponsor: Katie Dougherty Foundation; Grant sponsor: Kasle and Tkalcevik Neuroblastoma Research Fund; Grant sponsor: Alex s Lemonade Stand and the Thrasher Foundation. *Correspondence to: Katherine K. Matthay, Department of Pediatrics, Box 0106, University of California, San Francisco, CA matthayk@peds.ucsf.edu Received 5 November 2005; Accepted 27 December 2005
2 866 Messina et al. and patient response to induction chemotherapy, each used slightly different methods to assign scores. In addition, these scoring systems have only been tested in newly diagnosed neuroblastoma patients. No investigation has been performed to correlate results from these scoring systems to response among neuroblastoma patients with refractory or relapsed disease later in the treatment course. In such patients, changes in score might be expected to be smaller, and the number of lesions at initiation of treatment would frequently be less than at the time of original diagnosis for stage 4 neuroblastoma. Based on an analysis of patients who have been treated with 131 I-mIBG in a Phase II study for refractory disease, the present study sought to determine whether or not methods from two semi-quantitative scoring systems correlated with response to therapy based on International Neuroblastoma Response Criteria (INRC) [15] and PFS in a relapse population. This study also evaluated inter- and intraobserver concordance among the four independent readers to determine the reliability of the two semi-quantitative scoring systems. METHODS Study Subjects This study included 49 patients with relapsed or refractory neuroblastoma who were treated at the University of California, San Francisco (n ¼ 36), the Children s Hospital of Philadelphia (n ¼ 7), and the University of Michigan (n ¼ 6) between February 20, 1998 and December 11, 2003 on the clinical trial, 131 I-Metaiodobenzyguanidine Therapy for Neuroblastoma: a Phase II study [7]. Patient characteristics are shown in Table I. Patients were treated with MBq/kg of 131 I-mIBG for one (n ¼ 42), two (n ¼ 6), or three (n ¼ 1) courses. Although some patients had only a few lesions, they all had relapsed metastatic disease, with high likelihood of other sub-clinical lesions, and therefore were candidates for the targeted radionuclide rather than local radiaotherapy. Patients were evaluated as described below for response approximately 2 weeks prior to each therapy and 8 weeks after each therapy. Appropriate informed consent was obtained for all patients with approval at each center by the institutional human research review board and radiation safety committee. mibg Scoring Method mibg scans were performed using a standard protocol, as described in [16]. Four nuclear medicine physicians (B.T., B.F., M.C., B.S.) assigned scores to 57 pre- and post-therapy mibg diagnostic scan pairs based upon two semi-quantitative scoring systems (Table II) [10,12]. Extension scores were assigned to each segment to quantify the extent of mibg-positive lesions within a given segment. Intensity scores were assigned to each segment to quantify the degree of mibg uptake within the lesions of a given segment. The present study differentiated between the two scoring systems as Method 1 and Method 2. For Method 1, the patient s skeleton was divided into nine segments to view osteomedullary lesions with an additional tenth segment to assess soft tissue involvement (Fig. 1A) [10,13]. For Method 2, the skeleton was divided into seven segments to view osteomedullary lesions without a corresponding compartment to assess soft tissue involvement (Fig. 1B) [12,14]. Absolute pre-therapy extension, post-therapy extension, pre-therapy intensity, and post-therapy intensity scores were calculated for Methods 1 and 2 by summing the segmental scores assigned by the readers. In each region, the lesions TABLE I. Patient Characteristics Characteristic Number of patients Gender Male 29 Female 20 MYCN gene amplification at diagnosis Amplified 12/34 tested (35.29%) Time from diagnosis to metaiodobenzylguanidine (mibg) treatment (years) Median [range] 2.6 [ ] Age at mibg treatment (years) Median [range] 8.2 [ ] Patients receiving multiple 7 treatments with mibg Sites of disease at time of mibg treatment Bone/bone marrow, soft tissue 26 Bone/bone marrow only 13 Soft tissue only 10 TABLE II. mibg Scan Characteristics Characteristic Number of mibg scans Number of scans reviewed a Paired pre- and post-therapy scans 57 Total number of individual scans 110 Type of scan 123 I I 6 Time interval between pre- and post-therapy scans (weeks) Median Range [3 22] Time interval between MIBG therapy and post-therapy scan (weeks) Median 7 Range [3 12] Scans with SPECT Views b 8 Scans with lateral views of skull 55 a In four cases, the post-therapy scan from the first MIBG treatment served as the pre-therapy scan for the second treatment. b Scores from the SPECT views were not used in the analysis.
3 mibg Scoring in Relapsed Neuroblastoma 867 Fig. 1. A: Method 1, The patient s skeleton is divided into nine segments to view osteomedullary lesions [11] with an additional tenth segment to assess soft tissue osteomedullary lesions [11] with an additional tenth segment to assess soft tissue. B: Method 2, The patient s skeleton is divided into seven segments to view osteomedullary lesions [10]. were scored as follows for extension of metastases. The extension score for Method 1 was graded as: 0, no sites per segment; 1, one site per segment; 2, more than one site per segment; and 3, diffuse involvement (>50% of the segment). An example of the scoring by the four readers is shown in Figure 2A,B. The extension score for Method 2 was graded as: 0, no sites per segment; 1, one site per segment; 2, more than one site per segment. The intensity score for both methods was graded as: 0, for no uptake; 1, for doubtful uptake; 2, for obvious uptake; and 3, for strong uptake. Thus, the maximum extension and intensity score for Method 1 would be 30 and 30, and the maximum scores for Method 2 would be 14 and 21, respectively. The relative extension and intensity scores were calculated by dividing the absolute post-therapy score by the absolute pre-therapy score. The four readers scored the scan pairs independently from identical hard copies of the scans as digital copies were not available in many of the patients. Readers were blinded to both the clinical history of the patient s disease and to the patient s overall response to 131 I-mIBG therapy. To maintain consistency in the scoring process, general guidelines were established before the readers began scoring scans: (1) information as to whether or not a patient had a prior adrenalectomy or nephrectomy due to tumor involvement was provided, so that the readers could differentiate between physiologic uptake in an adrenal gland or kidney and active disease on the diagnostic mibg scan; (2) the pre-treatment scan was scored before the post-treatment scan using Method 1 followed by Method 2; (3) physiologic uptake of mibg in the liver was used as a point of reference to determine whether or not areas of abnormal uptake were of high or low intensity; and (4) when multiple sites of disease with varying intensities were present within a given segment, the intensity score for that segment was based upon the lesion with the greatest intensity. Finally, the readers also rated a patient s overall qualitative response to 131 I-mIBG based on their analysis of the diagnostic mibg scan pair. Disregarding numeric score, the readers recorded their impression of whether the post-therapy scan had improved, not changed, or worsened in comparison to the pre-therapy scan. To measure intra-observer consistency, three patients scan pairs were chosen to be scored on a second occasion in a blinded fashion by the four readers. These three patients scan pairs were selected based upon extent of disease to determine whether or not variations arose within a reader s results in scoring widespread versus localized disease. Response Evaluation Response to 131 I-mIBG therapy based upon INRC was rated as CR, very good partial response (VGPR), PR, mixed
4 868 Messina et al. post-mibg treatment and before a patient moved onto a new therapeutic regiment. One patient s scores were excluded from the INRC response and overall impression analyses after determining that the pre-therapy mibg scans were inadequate for response assessment. This patient still had scans included for the inter-observer concordance and was included in the overall PFS analysis. Fig. 2. A: Pre-therapy 123 I-metaiodobenzylguanidine (MIBG) scan and extension score by Method 1 by four readers. B: Post-therapy 123 I- MIBG scan and extension score by Method 1 by four readers. response (MR), no response (NR), or progressive disease (PD). Response was determined (prior to the current scoring study) by radiological review of post-therapy mibg, CT and MRI scans, morphologic analyses of bone marrow, and vanillylmandelic acid (VMA) and homovanillic acid (HVA) levels in urine [15]. Pre-therapy evaluation was done after a patient finished any prior therapeutic regimen and no earlier than 6 weeks before 131 I-mIBG treatment. Post-therapy response evaluation was required at 6 8 weeks Statistical Analysis To quantify the concordance in scoring among readers, the analysis used the generalized concordance correlation coefficient (CCC) [17,18]. The 95% confidence interval for CCC and the P-value for comparing concordance were calculated based on bootstrap bias-corrected confidence limits [19]. To assess the reader agreement on overall response impression, the analysis used the k-type statistics of O Connell and Dobson [20]. We assigned impression scales 1, 0, and 1 to categories improved, not changed, and worsened, respectively, and used two choices of disagreement function (o 1 and o 0 in O Connell and Dobson: with and without partial agreement). Given the definitions of the relative scores in the mibg Scoring Method section, a value of zero for the pre-therapy absolute score would result in an ill-defined relative score. When a reader assigned a pre-therapy absolute extension and intensity scores of 0 because he did not see any evidence of disease on the pre-therapy mibg scan, this reader s score was excluded from the analysis of relative scores. This was particularly a problem for Method 2, which excluded score assignment for soft tissue lesions. Correlation of scores with response was examined using logistic regression and generalized additive models [21]. The Wilcoxon rank sum test was used to compare continuous scores. Proportions of response were compared by the Fisher exact test and trend in proportions was assessed by the Cochran Armitage test. The accuracy of using the relative score or impression as a prognostic test for response was summarized in terms of false positive fractions, positive predictive values as well as positive and negative diagnostic likelihood ratios (DLR), and the accuracy of two tests was compared by their relative DLR [22]. PFS was defined as the amount of time in months between 131 I-mIBG therapy and disease progression or death. For patients who received multiple therapies, the date of their first therapy was used to determine the time between therapy and disease progression. Survival and PFS curves were estimated by the Kaplan Meier method and compared by the log-rank test [23]. In the PFS analysis, the time to disease progression was censored at the time a patient went on new therapy or at the time of the last follow-up visit. The proportion of patients changed to new therapy was estimated by its cumulative incidence rate with disease progression being a competing risk [24].
5 mibg Scoring in Relapsed Neuroblastoma 869 RESULTS Inter- and Intra-Observer Score Concordance Table III summarizes the pre- and post-therapy scores for all patients and gives the inter-observer concordance. In all cases, the inter-observer concordance for absolute scores was greater than or equal to Method 1 absolute extension scores produced the highest inter-observer concordance among the four raters. The absolute extension score concordance was marginally higher than the absolute intensity score concordance for both methods. The relative score concordance was lower for both methods in comparison to the absolute score concordance. To determine whether relative extension score concordance differed based upon extent of disease pre-therapy, the patient population was stratified into two groups based upon pre-therapy Method 1 absolute extension scores. Figure 3 shows the distribution of median (among four readers) pretherapy extension scores. There were 25 scans with the median score 3, 4 scans with the score >3 but 5, and 28 scans with the score >5. Thus, the stratification of five sites of disease pre-therapy was chosen as the cut-point for the analysis. The relative extension and intensity concordance for Method 1 scoring was significantly higher for the groups with more extensive disease, either scores >3 (P < 0.02) or >5 (P < 0.01) (Table IV). To evaluate the association of relative scores with the outcomes (INRC response and PFS), the median of the four readers Method 1 extension scores was used to compute the relative extension score for each scan. These scores were TABLE III. Scores and Inter-Observer Concordance on 57 Paired mibg Scans mibg Score Median Range Concordance (95%CI) Absolute extension scores Pre-therapy Method [0 30] 0.92 (0.86, 0.96) Post-therapy Method [0 30] 0.92 (0.82, 0.96) Pre-therapy Method [0 14] 0.91 (0.84, 0.94) Post-therapy Method [0 14] 0.89 (0.80, 0.94) Absolute intensity scores Pre-therapy Method [0 30] 0.91 (0.86, 0.94) Post-therapy Method [0 30] 0.88 (0.80, 0.93) Pre-therapy Method [0 21] 0.90 (0.85, 0.93) Post-therapy Method [0 21] 0.89 (0.82, 0.92) Relative extension scores a Method [ ] 0.47 (0.35, 0.61) Method [ ] 0.48 (0.31, 0.65) Relative intensity scores a Method [ ] 0.58 (0.43, 0.73) Method [ ] 0.51 (0.39, 0.69) a For Method 1, six pre-therapy scans received absolute scores of 0: two scans by two readers and four scans by one reader. For Method 2, which did not include scores for soft tissue lesions, 18 pre-therapy scans received absolute scores of 0: 2 scans by all four readers, 2 scans by three readers, 7 scans by two readers, and 7 scans by one reader. Fig. 3. Distribution of median pre-therapy extension scores. [Color figure can be viewed in the online issue, which is available at utilized because they produced very high inter-observer concordance, accounted for soft tissue lesions, and the median statistic is more robust than the mean. We also compared the median relative extension scores with the median relative intensity scores (correlation coefficient ¼ 0.88) and found no significant difference. In terms of high (>0.5) versus low (0.5) relative scores, the relative intensity and extension scores gave the same classifications except for one case (extension ¼ 0.42, intensity ¼ 0.71). For the intra-observer analysis of the four readers, three pairs of pre- and post-therapy scans were read on two separate blinded occasions. The scans had median pretherapy scores of 2, 14, and 19 in order to have a range of low (5) and high (>5) scores. Consistent with the results of the inter-observer concordance analysis, there was better agreement in scoring scans with high scores in comparison to low scores. Only 2 of these 12 pairs of relative scores resulted in a change in category between low (0.5) and high (>0.5) relative scores. Similarly, for the response by qualitative impression, 10/12 pairs were concordant and only 2 pairs of impression scores were discrepant for response. When assessing soft tissue lesions, certain inconsistencies arose in scoring for both methods. For Method 1, 13 patients received pre-therapy scores from multiple readers for the 10th compartment without any documented soft tissue involvement by other imaging modalities. In addition, 10 patients, who only had evidence of soft tissue disease pre-therapy, should have received soft tissue scores for the 10th compartment from all readers, but in 7 of the 10 cases, at least one reader gave a soft tissue score of 0. For Method 2, this same group of 10 patients should have received pre-therapy scores of 0 for all compartments due to lack of bone and bone marrow disease but 8 had scores mistakenly assigned as skeletal disease by at least one of the four readers.
6 870 Messina et al. TABLE IV. Concordance for Method 1 mibg Score After Stratification by Extent of Disease (mibg Score of 3 or 5) Pre-Therapy Extension concordance Intensity concordance Pre Post Relative P Pre Post Relative P Low (3) < <0.02 High (>3) Low (5) < <0.01 High (>5) Correlation of Score With Response There were 56 scan pairs associated with valid INRC response data, including 4 with CR, 17 with PR, 27 with NR (including 2 with MR), and 8 with PD. Figure 4A shows the relative extension score by Method 1 grouped by response. As shown by the outliers, seven therapies, that were scored as having a response with a relative score of 0.5, did not achieve CR or PR by other modalities, such as CT scan or bone marrow analysis (Table V). Conversely, six therapies failed to achieve response by relative score but still achieved response by INRC. Among these six therapies, five patients had low absolute pre-therapy extension scores (5) and also intermediate relative scores, and one therapy, with an absolute pre-therapy extension score of 7 and a median relative score of 1.04, resulted in NR by mibg scan but PR by CT. However, for this study, we used the median score, where the individual response by INRC was previously derived from an impression by a single nuclear medicine reader. The Method 1 relative extension score correlated with response to 131 I-mIBG therapy based on INRC, such that patients who achieved CR (n ¼ 4) or PR (n ¼ 17) had significantly lower relative extension scores (P < 0.001), with median score of 0.31 (CI 0.11, 0.51), compared to NR/ PD (n ¼ 35), with median of 0.98 (CI 0.90, 1.06) (Fig. 4A). Based on a linear logistic model, patients with low relative extension scores were significantly more likely to have a CR or PR to 131 I-mIBG therapy (P < 0.001) such that the odds of a CR or PR became about sixfold when relative extension scores drop by 0.5. Proportions of response (CR or PR) by INRC showed a significant decreasing trend (P < 0.001) among patients with low (0.5), intermediate (>0.5 but 1), and high (>1) relative extension scores. Of those who had a low relative score, 68% (15/22) had a response by INRC while only 20% (5/25) of those with an intermediate relative score and 11% (1/9) of those with a high relative score still achieved response. Compared to those with an intermediate score, patients with a low score were estimated to be 3.4 times (CI 1.5, 8.9) likely to achieve a response. The likelihood of response for patients with a high score was 0.56-fold (CI Fig. 4. A: Relationship between median relative score and tumor response to mibg therapy by International Neuroblastoma Response Criteria (INRC). X marks the mean; the bar marks the median; the lower and upper border mark the first (Q1) and the third (Q3) quartiles, respectively, complete response (CR)/partial response (PR) (n ¼ 21), no response (NR)/progressive disease (PD) (n ¼ 35); P < The five outliers with high relative score (iý1) in the CR/very good partial response (VGPR)/PR group had very low initial scores and poor agreement. B: Impression and relative extension score. Improved (n ¼ 29), not changed (n ¼ 20), worsened (n ¼ 7).
7 mibg Scoring in Relapsed Neuroblastoma 871 TABLE V. Patients With Relative Scores 0.5 but No Response (NR) by International Neuroblastoma Response Criteria (INRC) Patient # Median relative extension score Response by INRC Comments Progressive disease (PD) Previously negative bone marrow became positive for disease post-therapy 48 (Third therapy) 0.50 PD New nodule in breast positive for neuroblastoma by fine needle aspirate NR Bone marrow remained positive post-therapy NR Bone marrow remained positive post-therapy PD Increase in tumor size on CT PD Previously negative bone marrow became positive for disease post-therapy PD Previously negative bone marrow became positive for disease post-therapy 0.02, 4.02) compared to those with an intermediate score, although the difference was not significant. We also examined the correlation of response with relative score according to pre-therapy disease score using the stratification of 5 (low) and >5 (high). Proportions of response did not differ significantly (P > 0.9) between the two pre-therapy strata for patients with a low (0.5) relative score, and likewise (P > 0.4) for patients with a high (>1) relative score. However, for those with an intermediate relative score, 33% (5/15) achieved response (1 CR and 4 PR) in the low stratum compared to 0% (0/10) in the high stratum (P ¼ 0.06). Inter-Observer Overall Response Impression Agreement Impression of each scan was summarized as improved, not changed, or worsened for the INRC response and PFS analyses. Of the 57 scans, 23 (40%) scan pairs had a perfect agreement (all four raters agreed); 20 (35%) had a majority agreement (the same impression by three readers with the impression by the other reader differing by one category); 8 scans had a closely-split agreement (two readers agreed with each other, and the two readers differed by one category); the other 6 scan pairs had mixed impressions. Allowing for partial agreement, agreement is perfect (¼1.0) for 40%, excellent for 49%, and good (between 0.6 and 0.8) for 11% of the scans. Using the impression scales (described above), of the scans in perfect or majority agreement, 24, 14, and 4 scans (excluding 1 inevaluable for response) were classified as improved, not changed, and worsened, respectively. The readers overall impression of response associated well (P < with or without excluding the scans in mixed agreement) with the relative extension scores although these results were less quantitative (Fig. 4B). However, the use of the impression score was less accurate than the semi-quantitative scoring system for prediction of a good (positive) response. The relative accuracy of the relative score compared to the impression score was evaluated by comparing their DLRs to predict response. For the relative score, the positive DLR was 3.57 compared to 2.36 for the impression score, and the negative DLR was 0.36 compared to That is, the odds of response increased by 3.57-fold with knowledge of a low (0.5) relative score compared to only 2.36-fold by an improved impression. The relative positive DLR was 1.52, implying that a positive result on relative score is more indicative of response than impression. However, the relative negative DLR was 1.23, implying that a negative result on relative score is less convincing for nonresponse than a negative impression result. The lower accuracy of a negative result on relative score can be improved by taking the pre-therapy score into account for patients with a relative score between 0.5 and 1.0 as discussed in the previous section. Score and PFS Survival and PFS for all patients are shown in Figure 5A. The PFS curve is truncated as patients were censored when they went on to new therapy. PFS according to pre-therapy stratum of score 5or>5showed a trend for improved PFS with a lower pre-therapy score (P ¼ 0.20) (Fig. 5B). The relative extension score of 0.5 or >0.5 did not appear to affect PFS (Fig. 5C) and became even less significant when considering both disease progression and switching to new therapy as endpoint (P ¼ 0.73). The reversal of the expected order of the curves in Figure 4C is explained by the fact that patients with higher relative scores, and therefore poorer response to the mibg therapy, were about twice as likely to change to new therapy earlier, and therefore, be censored in the PFS analysis when compared to those with a lower relative score. In fact, by 4 months, 57% of patients with a high relative score >0.5 had changed to new therapy, and by 6 months post-mibg therapy, 70% had changed, whereas 28% and 39% of patients with a low relative score had changed to new therapy by 4 and 6 months, respectively. Ultimately, overall response by INRC to mibg therapy had no effect on PFS in this group of 49 refractory patients (data not shown). This finding was consistent with the lack of effect of relative score on PFS. DISCUSSION Several studies have shown that incorporation of mibg scan results into analysis of response is critical both for
8 872 Messina et al. Fig. 5. A: Overall survival (OS) (solid line) and progression-free survival (PFS) (dashed line) for all patients (n ¼ 49) from time of first mibg therapy. B: PFS by pre-therapy mibg extension score for low (5, solid line) or high score (>5, dashed line); P ¼ C: PFS by relative extension score post-therapy of 0.5 (solid line) or >0.5 (dashed line); P ¼ determining response and survival [11,25 28]. An objective and consistent method for interpretation of these scans is therefore critical for comparison of clinical outcomes. A prior study [10], using Method 1 to score patients at diagnosis, had a median pre-therapy extension score of 18, compared to the current study, with a median score of 4.5. The results of the current study show that semi-quantitative scoring of mibg scans is reliable in relapsed neuroblastoma despite the lower median score, with excellent inter- and intra-observer concordance, similar to results for newly diagnosed patients [10,13,14]. We have shown further that the calculation used in the relative score for response continues to be reliable though more error is introduced in patients with fewer than three to five lesions prior to therapy. Extension and intensity score concordances were very similar. Overall, the data showed no advantage in using both scores to assess response, and there was only one instance where the relative intensity score fell into a different category for response than the relative extension score. Method 1 relative extension scores can be used accurately for semi-quantitative analysis of response by mibg scan in refractory patients and correlate significantly with whether or not a patient had an overall response (CR, VGPR, or PR) or no response (NR, MR, or PD) by INRC to therapy. Based upon the results displayed in Figure 4A, the present study shows that a relative extension score of 0.5 indicates that a patient likely had a response to mibg therapy by INRC, and a relative extension score of >0.5 indicates that a patient likely had NR. Relative extension scores had the highest concordance among readers for patients with more than three to five sites of disease. For patients with fewer sites of disease, because the post-therapy score is divided by the pre-therapy score to calculate the relative score, a single digit difference assigned by the four raters in either of these scores will have a significant effect on this ratio. The data suggest that any decrease in absolute score is indicative of response in patients with scores below three to five at the commencement of therapy, but that the semi-quantitative scoring system is most useful in those with pre-treatment score 3. Method 2 (without assigning soft tissue scores) produced many pre-therapy absolute scores of 0, resulting in a
9 mibg Scoring in Relapsed Neuroblastoma 873 substantially decreased sample size since these scores were excluded from the analysis. Ideally, only 10 patients should have received pre-therapy scores of 0 by Method 2 because they were documented as having no evidence of soft tissue disease pre-therapy. However, only two patients received pre-therapy scores of 0 from all four readers. Even though these patients scans were dropped from the concordance analysis, failing to assess soft tissue lesions could result in an inaccurate response evaluation by semi-quantitative score. Discrepancies in assignment of score for soft tissue lesions might be eliminated by simply allowing readers to score any lesion within its appropriate anatomical segment instead of trying to differentiate between soft tissues or skeletal lesions. Although the impression of the reader as to whether a scan was improved, worsened, or stabilized showed reasonable concordance and correlated with the relative score and the response by INRC, the accuracy was lower than that of the semi-quantitative scoring system. For example, only 7/22 (these 7 patients are listed in Table V) patients with a low relative score of 0.5 had NR or PD, whereas 12/29 (6 of these 12 are in Table V) patients rated as improved on MIBG scan, fell into the NR or PD category by INRC. This corresponded to a positive predictive value of 68% for the relative score versus 59% for the impression. It also resulted in a false positive fraction of only 20% for the relative score compared to 34% for the impression. Despite a strong correlation with response by INRC, the relative extension scores carried no significance in predicting PFS. This may be a result of two factors. First, there was no difference in this group of 49 patients in PFS between those with response to therapy and those without response. Secondly, those that were left with residual disease were also often entered on a new therapy soon after the MIBG treatment. The semi-quantitative scoring system must be used in combination with other response criteria in refractory neuroblastoma as it only assesses disease visible on mibg scan and fails to include analysis of bone marrow and mibgnegative disease only evaluable on CT or MR. Current cooperative high-risk neuroblastoma protocols both in Europe and in North America are incorporating semiquantitative scoring by mibg scan into their central review of response, and a recent International Neuroblastoma Risk Group meeting of cooperative study groups from Asia, Europe, and North America in September, 2005 reached a consensus on incorporation of a common scoring system into their evaluation of response for a more objective measure and to facilitate comparison between studies. This new system will assign soft tissue lesions within their appropriate skeletal segment, and divide the body into seven segments: head, spine, ribs and chest, abdomen and pelvis, arms, legs. Semi-quantitative scoring of mibg scans provides a more reliable method of assessing response in mibg positive lesions in patients with relapsed neuroblastoma than a standard impression reading, especially in patients with initial scores >3. The scoring system is reproducible with good intra- and inter-observer concordance and will provide an important component of overall response criteria for this disease in patients with recurrent as well as newly diagnosed neuroblastoma. ACKNOWLEDGMENT We thank Sylvia Corpuz and John Huberty in the Department of Nuclear Medicine at UCSF for valuable technical assistance and Janet Veatch for coordination of the Phase II therapy study. We also acknowledge the financial support (in part) of the National Institute of Health grant PO1 CA81403, 2MO1 RR0127, as well as donations from the Campini Foundation, the Conner Research Fund, the Dougherty Foundation, Kasle and Tkalcevik Neuroblastoma Research Fund, Alex s Lemonade Stand, and the Thrasher Foundation. REFERENCES 1. Matthay KK, Villablanca JG, Seeger RC, et al. Treatment of highrisk neuroblastoma with intensive chemotherapy, radiotherapy, autologous bone marrow transplantation, and 13-cis- retinoic acid. Children s Cancer Group. N Engl J Med 1999;341: Garaventa A, Bellagamba O, Lo Piccolo MS, et al. 131Imetaiodobenzylguanidine ( 131 I-MIBG) therapy for residual neuroblastoma: A mono-institutional experience with 43 patients. Br J Cancer 1999;81: Kang TI, Brophy P, Hickeson M, et al. Targeted radiotherapy with submyeloablative doses of 131 I-MIBG is effective for disease palliation in highly refractory neuroblastoma. J Pediatr Hematol Oncol 2003;25: Troncone L, Riccardi R, Montemaggi P, et al. Treatment of neuroblastoma with 131 I-metaiodobenzylguanidine. Med Pediatr Oncol 1987;15: Hoefnagel CA, Voute PA, De Kraker J, et al. [131I]metaiodobenzylguanidine therapy after conventional therapy for neuroblastoma. J Nucl Biol Med 1991;35: Klingebiel T, Berthold F, Treuner J, et al. Metaiodobenzylguanidine (mibg) in treatment of 47 patients with neuroblastoma: Results of the German Neuroblastoma Trial. Med e palliation in highly refractory neuroblastoma. J Pediatr Hematol Oncol 2003; 25: Matthay KK, Panina C, Huberty J, et al. Correlation of tumor and whole-body dosimetry with tumor response and toxicity in refractory neuroblastoma treated with (131)I-MIBG. J Nucl Med 2001;42: Matthay KK, DeSantes K, Hasegawa B, et al. Phase I dose escalation of 131 I-metaiodobenzylguanidine with autologous bone marrow support in refractory neuroblastoma. J Clin Oncol 1998; 16: Therasse P, Arbuck SG, Eisenhauer EA, et al. New guidelines to evaluate the response to treatment in solid tumors. J Natl Cancer Inst 2000;92: Matthay KK, Edeline V, Lumbroso J, et al. Correlation of early metastatic response by 123 I-metaiodobenzylguanidine scintigraphy with overall response and event-free survival in stage IV neuroblastoma. J Clin Oncol 2003;21: Katzenstein HM, Cohn SL, Shore RM, et al. Scintigraphic response by 123 I-metaiodobenzylguanidine scan correlates with event-free
10 874 Messina et al. survival in high-risk neuroblastoma. J Clin Oncol 2004;22: Suc A, Lumbroso J, Rubie H, et al. Metastatic neuroblastoma in children older than one year: Prognostic significance of the initial metaiodobenzylguanidine scan and proposal for a scoring system. Cancer 1996;77: Ady N, Zucker JM, Asselain B, et al. A new 123 I-MIBG whole body scan scoring method Application to the prediction of the response of metastases to induction chemotherapy in stage IV neuroblastoma. Eur J Cancer 1995;31A: Frappaz D, Bonneu A, Chauvot P, et al. Metaiodobenzylguanidine assessment of metastatic neuroblastoma: Observer dependency and chemosensitivity evaluation. The SFOP Group. Med Pediatr Oncol 2000;34: Brodeur GM, Pritchard J, Berthold F, et al. Revisions of the international criteria for neuroblastoma diagnosis, staging, and response to treatment. J Clin Oncol 1993;11: (see comments). 16. Shulkin BL, Shapiro B. Current concepts on the diagnostic use of MIBG in children. J Nucl Med 1998;39: Lin LI. A concordance correlation coefficient to evaluate reproducibility. Biometrics 1989;45: Barnhart HX, Haber M, Song J. Overall concordance correlation coefficient for evaluating agreement among multiple observers. Biometrics 2002;58: Efron B, Tibshirani RJ. Better bootstrap confidence intervals. An introduction to the Bootstrap. New York: Chapman & Hall; pp O Connell DL, Dobson AJ. General observer-agrreement measures on individual subjects and groups of subjects. Biometrics 1984;40: Hastie T, Tibshirani R. Generalized additive models: Logistic regression. Generalized additive models. New York: Chapman and Hall; pp Pepe. Measures of accuracy for binary tests. New York: Oxford; pp Kaplan EL, Meier P. Nonparametric estimation from incomplete observations. J Am Stat Assoc 1958;53: Gray RJ. A class of K-sample tests for comparing the cumulative incidence of a competing risk. Ann Stat 1988;16: Kushner BH, Yeh SD, Kramer K, et al. Impact of metaiodobenzylguanidine scintigraphy on assessing response of high-risk neuroblastoma to dose-intensive induction chemotherapy. J Clin Oncol 2003;21: Ladenstein R, Philip T, Lasset C, et al. Multivariate analysis of risk factors in stage 4 neuroblastoma patients over the age of one year treated with megatherapy and stem-cell transplantation: A report from the European Bone Marrow Transplantation Solid Tumor Registry. J Clin Oncol 1998;16: Shah Syed GM, Naseer H, Usmani GN, et al. Role of iodine-131 MIBG scanning in the management of paediatric patients with neuroblastoma. Med Princ Pract 2004;13: Frappaz D, Combaret V, Desuzinges C, et al. Can MIBG scan replace the need for bone marrow assessment at diagnosis and reassessment in stage 4 neuroblastomas? Bull Cancer 2004;91: E253 E260.
NEUROBLASTOMA IS the most common extracranial
 Correlation of Early Metastatic Response by 123 I-Metaiodobenzylguanidine Scintigraphy With Overall Response and Event-Free Survival in Stage IV Neuroblastoma By Katherine K. Matthay, Veronique Edeline,
Correlation of Early Metastatic Response by 123 I-Metaiodobenzylguanidine Scintigraphy With Overall Response and Event-Free Survival in Stage IV Neuroblastoma By Katherine K. Matthay, Veronique Edeline,
J Clin Oncol 27: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 27 NUMBER 7 MARCH 1 2009 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T From the Departments of Pediatrics and Radiology, Nuclear Medicine Program, University of California San Francisco
VOLUME 27 NUMBER 7 MARCH 1 2009 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T From the Departments of Pediatrics and Radiology, Nuclear Medicine Program, University of California San Francisco
J Clin Oncol 27: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 27 NUMBER 32 NOVEMBER 10 2009 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Comparison of Iodine-123 Metaiodobenzylguanidine () Scan and [ 18 F]Fluorodeoxyglucose Positron Emission Tomography
VOLUME 27 NUMBER 32 NOVEMBER 10 2009 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Comparison of Iodine-123 Metaiodobenzylguanidine () Scan and [ 18 F]Fluorodeoxyglucose Positron Emission Tomography
Quantitative Nuclear Medicine Imaging in Oncology. Susan E. Sharp, MD
 Quantitative Nuclear Medicine Imaging in Oncology Susan E. Sharp, MD Disclosures None Objectives Describe scoring systems used in oncologic nuclear medicine imaging Deauville scoring in lymphoma Curie
Quantitative Nuclear Medicine Imaging in Oncology Susan E. Sharp, MD Disclosures None Objectives Describe scoring systems used in oncologic nuclear medicine imaging Deauville scoring in lymphoma Curie
Neuroblastoma. Elizabeth Roberts. Data Coordinator CIBMTR Data Managers Mentor. Tandem Meeting February 18
 Neuroblastoma Elizabeth Roberts Data Coordinator CIBMTR Data Managers Mentor Tandem Meeting February 18 Objectives Know what neuroblastoma is, how it is diagnosed, and how it is treated Complete form 2026:
Neuroblastoma Elizabeth Roberts Data Coordinator CIBMTR Data Managers Mentor Tandem Meeting February 18 Objectives Know what neuroblastoma is, how it is diagnosed, and how it is treated Complete form 2026:
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, :00 12:10 p.m.
 SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, 2018 10:00 12:10 p.m. Staging Susan E. Sharp, MD 1. In the International Neuroblastoma Risk Group Staging
SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, 2018 10:00 12:10 p.m. Staging Susan E. Sharp, MD 1. In the International Neuroblastoma Risk Group Staging
The use of both diagnostic and therapeutic MIBG in neuroblastoma patients Bleeker, G.
 UvA-DARE (Digital Academic Repository) The use of both diagnostic and therapeutic MIBG in neuroblastoma patients Bleeker, G. Link to publication Citation for published version (APA): Bleeker, G. (2014).
UvA-DARE (Digital Academic Repository) The use of both diagnostic and therapeutic MIBG in neuroblastoma patients Bleeker, G. Link to publication Citation for published version (APA): Bleeker, G. (2014).
Surgical Outcomes of Patients with Neuroblastoma in a Tertiary Centre in Hong Kong: A 12-year Experience
 HK J Paediatr (new series) 2009;14:186-193 Surgical Outcomes of Patients with Neuroblastoma in a Tertiary Centre in Hong Kong: A 12-year Experience IHY CHAN, KKY WONG, GCF CHAN, PKH TAM Abstract Key words
HK J Paediatr (new series) 2009;14:186-193 Surgical Outcomes of Patients with Neuroblastoma in a Tertiary Centre in Hong Kong: A 12-year Experience IHY CHAN, KKY WONG, GCF CHAN, PKH TAM Abstract Key words
CCG-3891 LONG TERM OUTCOME FOR CHILDREN WITH HIGH RISK NEUROBLASTOMA Additional Information on Corrected Overall Survival Results April 10, 2014
 Group Chair Peter C. Adamson, M.D. adamson@email.chop.edu Group Vice Chair Susan Blaney, M.D. smblaney@txch.org Chief Operating Officer Elizabeth O Connor, M.P.H. econnor@childrensoncology group.org Chief
Group Chair Peter C. Adamson, M.D. adamson@email.chop.edu Group Vice Chair Susan Blaney, M.D. smblaney@txch.org Chief Operating Officer Elizabeth O Connor, M.P.H. econnor@childrensoncology group.org Chief
Neuroblastoma is the most common extracranial solid
 Journal of Nuclear Medicine, published on June 14, 2012 as doi:10.2967/jnumed.111.098624 Dose Escalation Study of No-Carrier-Added I-Metaiodobenzylguanidine for Relapsed or Refractory Neuroblastoma: New
Journal of Nuclear Medicine, published on June 14, 2012 as doi:10.2967/jnumed.111.098624 Dose Escalation Study of No-Carrier-Added I-Metaiodobenzylguanidine for Relapsed or Refractory Neuroblastoma: New
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES
 MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
J Clin Oncol 29: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 29 NUMBER 33 NOVEMBER 11 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Prognostic Value of the Stage 4S Metastatic Pattern and Tumor Biology in Patients With Metastatic Neuroblastoma
VOLUME 29 NUMBER 33 NOVEMBER 11 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Prognostic Value of the Stage 4S Metastatic Pattern and Tumor Biology in Patients With Metastatic Neuroblastoma
Institution INSTRUCTIONS (I6) 1. This form is to be completed by a DESIGNATED STUDY NUCLEAR MEDICINE SPECIALIST
 I6 ACRIN 6660 Whole Body MRI in the Evaluation of Pediatric Malignancies Conventional Scintigraphy Imaging Form If this is a revised or corrected form, indicate by checking box and fax to 215-717 - 0936.
I6 ACRIN 6660 Whole Body MRI in the Evaluation of Pediatric Malignancies Conventional Scintigraphy Imaging Form If this is a revised or corrected form, indicate by checking box and fax to 215-717 - 0936.
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD
 Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Chikako Suzuki M.D., Ph.D.
 Chikako Suzuki M.D., Ph.D. Main supervisor Lennart Blomqvist M.D. Ph.D Co supervisor Hans Jacobsson M.D. Ph.D., Hirofumi Fujii M.D Ph.D. Department of Molecular Medicine and Surgery, Karolinska Institutet
Chikako Suzuki M.D., Ph.D. Main supervisor Lennart Blomqvist M.D. Ph.D Co supervisor Hans Jacobsson M.D. Ph.D., Hirofumi Fujii M.D Ph.D. Department of Molecular Medicine and Surgery, Karolinska Institutet
Role of 131-I MIBG Therapy in the Treatment of Advanced Neuroblastoma
 Journal of the Egyptian Nat. Cancer Inst., Vol. 21,. 1, March: 51-58, 2009 Role of 131-I MIBG Therapy in the Treatment of Advanced Neuroblastoma RAEF RIAD, M.D.*; MAGDY KOTB, M.D.*; WALID OMAR, M.D.*;
Journal of the Egyptian Nat. Cancer Inst., Vol. 21,. 1, March: 51-58, 2009 Role of 131-I MIBG Therapy in the Treatment of Advanced Neuroblastoma RAEF RIAD, M.D.*; MAGDY KOTB, M.D.*; WALID OMAR, M.D.*;
Welcome to the RECIST 1.1 Quick Reference
 Welcome to the RECIST 1.1 Quick Reference *Eisenhauer, E. A., et al. New response evaluation criteria in solid tumours: Revised RECIST guideline (version 1.1). Eur J Cancer 2009;45:228-47. Subject Eligibility
Welcome to the RECIST 1.1 Quick Reference *Eisenhauer, E. A., et al. New response evaluation criteria in solid tumours: Revised RECIST guideline (version 1.1). Eur J Cancer 2009;45:228-47. Subject Eligibility
Wilms Tumor and Neuroblastoma
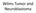 Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Published Ahead of Print on October 3, 2011 as /JCO J Clin Oncol by American Society of Clinical Oncology INTRODUCTION
 Published Ahead of Print on October 3, 11 as 10.10/JCO.11.35.9570 The latest version is at http://jco.ascopubs.org/cgi/doi/10.10/jco.11.35.9570 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T
Published Ahead of Print on October 3, 11 as 10.10/JCO.11.35.9570 The latest version is at http://jco.ascopubs.org/cgi/doi/10.10/jco.11.35.9570 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T
Guideline on the use of minimal residual disease as a clinical endpoint in multiple myeloma studies
 1 2 3 26 July 2018 EMA/CHMP/459559/2018 Committee for Medicinal Products for Human Use (CHMP) 4 5 6 Guideline on the use of minimal residual disease as a clinical endpoint in multiple Draft Draft agreed
1 2 3 26 July 2018 EMA/CHMP/459559/2018 Committee for Medicinal Products for Human Use (CHMP) 4 5 6 Guideline on the use of minimal residual disease as a clinical endpoint in multiple Draft Draft agreed
Doppler ultrasound of the abdomen and pelvis, and color Doppler
 - - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
- - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
PROCARBAZINE, lomustine, and vincristine (PCV) is
 RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
Radiologic assessment of response of tumors to treatment. Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1
 Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
Radiologic assessment of response of tumors to treatment Copyright 2008 TIMC, Matthew A. Barish M.D. All rights reserved. 1 Objective response assessment is important to describe the treatment effect of
Radiopharmaceutical Therapy with Radium-223 and 131 I-mIBG
 Radiopharmaceutical Therapy with Radium-223 and 131 I-mIBG Aaron C. Jessop, MD, MBA Associate Professor of Clinical Radiology Director of Nuclear Medicine and PET Vanderbilt University Medical Center Target
Radiopharmaceutical Therapy with Radium-223 and 131 I-mIBG Aaron C. Jessop, MD, MBA Associate Professor of Clinical Radiology Director of Nuclear Medicine and PET Vanderbilt University Medical Center Target
Neuroblastoma: experience from National University Health System, Singapore ( )
 Singapore Med J 2012; 53(1) : 19 Neuroblastoma: experience from National University Health System, Singapore (1987 2008) Tan C 1, BA, Sabai SM 2, MBBS, Tin AS 3, MBBS, MMed, Quah TC 4, MBBS, MMed, Aung
Singapore Med J 2012; 53(1) : 19 Neuroblastoma: experience from National University Health System, Singapore (1987 2008) Tan C 1, BA, Sabai SM 2, MBBS, Tin AS 3, MBBS, MMed, Quah TC 4, MBBS, MMed, Aung
Pros and Cons: Interim PET in DLBCL Ulrich Dührsen Department of Hematology University Hospital Essen
 3rd International Workshop on in Lymphoma Menton, September 26, 2011 Afternoon Controversies Pros and Cons: in DLBCL Ulrich Dührsen Department of Hematology University Hospital Essen Pros Is there any
3rd International Workshop on in Lymphoma Menton, September 26, 2011 Afternoon Controversies Pros and Cons: in DLBCL Ulrich Dührsen Department of Hematology University Hospital Essen Pros Is there any
Comparison of RECIST version 1.0 and 1.1 in assessment of tumor response by computed tomography in advanced gastric cancer
 Original Article Comparison of RECIST version 1.0 and 1.1 in assessment of tumor response by computed tomography in advanced gastric cancer Gil-Su Jang 1 *, Min-Jeong Kim 2 *, Hong-Il Ha 2, Jung Han Kim
Original Article Comparison of RECIST version 1.0 and 1.1 in assessment of tumor response by computed tomography in advanced gastric cancer Gil-Su Jang 1 *, Min-Jeong Kim 2 *, Hong-Il Ha 2, Jung Han Kim
Staging Colorectal Cancer
 Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Radiographic Assessment of Response An Overview of RECIST v1.1
 Radiographic Assessment of Response An Overview of RECIST v1.1 Stephen Liu, MD Georgetown University May 15 th, 2015 Presentation Objectives To understand the purpose of RECIST guidelines To describe the
Radiographic Assessment of Response An Overview of RECIST v1.1 Stephen Liu, MD Georgetown University May 15 th, 2015 Presentation Objectives To understand the purpose of RECIST guidelines To describe the
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Callegaro D, Miceli R, Bonvalot S, et al. Development
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Callegaro D, Miceli R, Bonvalot S, et al. Development
First Line Management of Classical Hodgkin Lymphoma
 First Line Management of Classical Hodgkin Lymphoma George Follows Cambridge University Hospitals NHS Foundation Trust george.follows@addenbrookes.nhs.uk The controversial areas Early stage non-bulky /
First Line Management of Classical Hodgkin Lymphoma George Follows Cambridge University Hospitals NHS Foundation Trust george.follows@addenbrookes.nhs.uk The controversial areas Early stage non-bulky /
Neuroblastoma, a childhood tumor derived from the
 Correlation of Tumor and Whole-Body Dosimetry with Tumor Response and Toxicity in Refractory Neuroblastoma Treated with 131 I-MIBG Katherine K. Matthay, Colleen Panina, John Huberty, David Price, David
Correlation of Tumor and Whole-Body Dosimetry with Tumor Response and Toxicity in Refractory Neuroblastoma Treated with 131 I-MIBG Katherine K. Matthay, Colleen Panina, John Huberty, David Price, David
CHL 5225 H Advanced Statistical Methods for Clinical Trials. CHL 5225 H The Language of Clinical Trials
 CHL 5225 H Advanced Statistical Methods for Clinical Trials Two sources for course material 1. Electronic blackboard required readings 2. www.andywillan.com/chl5225h code of conduct course outline schedule
CHL 5225 H Advanced Statistical Methods for Clinical Trials Two sources for course material 1. Electronic blackboard required readings 2. www.andywillan.com/chl5225h code of conduct course outline schedule
Response Assessment Classification in Patients with Advanced Renal Cell Carcinoma Treated on Clinical Trials
 1611 Response Assessment Classification in Patients with Advanced Renal Cell Carcinoma Treated on Clinical Trials Effect of Measurement Criteria and Other Parameters Lawrence H. Schwartz, M.D. 1,2 Madhu
1611 Response Assessment Classification in Patients with Advanced Renal Cell Carcinoma Treated on Clinical Trials Effect of Measurement Criteria and Other Parameters Lawrence H. Schwartz, M.D. 1,2 Madhu
Bone Metastases in Muscle-Invasive Bladder Cancer
 Journal of the Egyptian Nat. Cancer Inst., Vol. 18, No. 3, September: 03-08, 006 AZZA N. TAHER, M.D.* and MAGDY H. KOTB, M.D.** The Departments of Radiation Oncology* and Nuclear Medicine**, National Cancer
Journal of the Egyptian Nat. Cancer Inst., Vol. 18, No. 3, September: 03-08, 006 AZZA N. TAHER, M.D.* and MAGDY H. KOTB, M.D.** The Departments of Radiation Oncology* and Nuclear Medicine**, National Cancer
Histopathology Defines Prognostic Subsets of Ganglioneuroblastoma, Nodular
 1150 Histopathology Defines Prognostic Subsets of Ganglioneuroblastoma, Nodular A Report from the Children s Cancer Group Shunsuke Umehara, M.D. 1 Atsuko Nakagawa, M.D. 1 Katherine K. Matthay, M.D. 2 John
1150 Histopathology Defines Prognostic Subsets of Ganglioneuroblastoma, Nodular A Report from the Children s Cancer Group Shunsuke Umehara, M.D. 1 Atsuko Nakagawa, M.D. 1 Katherine K. Matthay, M.D. 2 John
COG-ANBL1232: Utilizing Response- and Biology-Based Risk Factors to Guide Therapy in Patients with Non-High-Risk Neuroblastoma
 Page 1 of 10 COG-ANBL1232: Utilizing Response- and Biology-Based Risk Factors to Guide Therapy in Patients with Non-High-Risk Neuroblastoma FAST FACTS Eligibility Reviewed and Verified By MD/DO Date RN
Page 1 of 10 COG-ANBL1232: Utilizing Response- and Biology-Based Risk Factors to Guide Therapy in Patients with Non-High-Risk Neuroblastoma FAST FACTS Eligibility Reviewed and Verified By MD/DO Date RN
PET/CT for Therapy Assessment in Oncology
 PET/CT for Therapy Assessment in Oncology Rodolfo Núñez Miller, M.D. Nuclear Medicine Section Division of Human Health International Atomic Energy Agency Vienna, Austria Clinical Applications of PET/CT
PET/CT for Therapy Assessment in Oncology Rodolfo Núñez Miller, M.D. Nuclear Medicine Section Division of Human Health International Atomic Energy Agency Vienna, Austria Clinical Applications of PET/CT
Utility of 18 F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer
 Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Effective local and systemic therapy is necessary for the cure of Ewing tumor Most chemotherapy regimens are a combination of cyclophosphamide,
 Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Evaluation of Lung Cancer Response: Current Practice and Advances
 Evaluation of Lung Cancer Response: Current Practice and Advances Jeremy J. Erasmus I have no financial relationships, arrangements or affiliations and this presentation will not include discussion of
Evaluation of Lung Cancer Response: Current Practice and Advances Jeremy J. Erasmus I have no financial relationships, arrangements or affiliations and this presentation will not include discussion of
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995
 Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Supplementary Appendix to manuscript submitted by Trappe, R.U. et al:
 Supplementary Appendix to manuscript submitted by Trappe, R.U. et al: Response to rituximab induction is a predictive marker in B-cell post-transplant lymphoproliferative disorder and allows successful
Supplementary Appendix to manuscript submitted by Trappe, R.U. et al: Response to rituximab induction is a predictive marker in B-cell post-transplant lymphoproliferative disorder and allows successful
NEUROBLASTOMA IS the most common extracranial
 Pilot Study of Iodine-131 Metaiodobenzylguanidine in Combination With Myeloablative Chemotherapy and Autologous Stem-Cell Support for the Treatment of Neuroblastoma By Gregory A. Yanik, John E. Levine,
Pilot Study of Iodine-131 Metaiodobenzylguanidine in Combination With Myeloablative Chemotherapy and Autologous Stem-Cell Support for the Treatment of Neuroblastoma By Gregory A. Yanik, John E. Levine,
I-MIBG in the diagnosis of primary and metastatic neuroblastoma
 I-MIBG in the diagnosis of primary and metastatic neuroblastoma T. El- Maghraby Nuclear Medicine Section- Radiology Department, Saad Specialist Hospital, Al-Khobar, Saudi Arabia. Abstract Objective Neuroblastoma
I-MIBG in the diagnosis of primary and metastatic neuroblastoma T. El- Maghraby Nuclear Medicine Section- Radiology Department, Saad Specialist Hospital, Al-Khobar, Saudi Arabia. Abstract Objective Neuroblastoma
FDG PET/CT Versus I-131 MIBG Scan in Diagnosis of Neuroblastoma Osseous Infiltrates; Comparative Study
 Egyptian J. Nucl. Med., Vol. 10, No. 2, Dec 2014 85 Original article, Oncology FDG PET/CT Versus I-131 MIBG Scan in Diagnosis of Neuroblastoma Osseous Infiltrates; Comparative Study Amr, M 1. Kotb, M 1,
Egyptian J. Nucl. Med., Vol. 10, No. 2, Dec 2014 85 Original article, Oncology FDG PET/CT Versus I-131 MIBG Scan in Diagnosis of Neuroblastoma Osseous Infiltrates; Comparative Study Amr, M 1. Kotb, M 1,
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
Bendamustine is Effective Therapy in Patients with Rituximab-Refractory, Indolent B-Cell Non-Hodgkin Lymphoma
 Bendamustine is Effective Therapy in Patients with Rituximab-Refractory, Indolent B-Cell Non-Hodgkin Lymphoma Kahl BS et al. Cancer 2010;116(1):106-14. Introduction > Bendamustine is a novel alkylating
Bendamustine is Effective Therapy in Patients with Rituximab-Refractory, Indolent B-Cell Non-Hodgkin Lymphoma Kahl BS et al. Cancer 2010;116(1):106-14. Introduction > Bendamustine is a novel alkylating
8/10/2016. PET/CT Radiomics for Tumor. Anatomic Tumor Response Assessment in CT or MRI. Metabolic Tumor Response Assessment in FDG-PET
 PET/CT Radiomics for Tumor Response Evaluation August 1, 2016 Wei Lu, PhD Department of Medical Physics www.mskcc.org Department of Radiation Oncology www.umaryland.edu Anatomic Tumor Response Assessment
PET/CT Radiomics for Tumor Response Evaluation August 1, 2016 Wei Lu, PhD Department of Medical Physics www.mskcc.org Department of Radiation Oncology www.umaryland.edu Anatomic Tumor Response Assessment
Chapter 10. Summary, conclusions and future perspectives
 Chapter 10 Summary, conclusions and future perspectives 10.1 SUMMARY In this thesis, a new tumor imaging tracer in nuclear medicine is studied. This 123 tracer, L-3-[ I]Iodo-alpha-methyl-tyrosine (IMT),
Chapter 10 Summary, conclusions and future perspectives 10.1 SUMMARY In this thesis, a new tumor imaging tracer in nuclear medicine is studied. This 123 tracer, L-3-[ I]Iodo-alpha-methyl-tyrosine (IMT),
BIOSTATISTICAL METHODS AND RESEARCH DESIGNS. Xihong Lin Department of Biostatistics, University of Michigan, Ann Arbor, MI, USA
 BIOSTATISTICAL METHODS AND RESEARCH DESIGNS Xihong Lin Department of Biostatistics, University of Michigan, Ann Arbor, MI, USA Keywords: Case-control study, Cohort study, Cross-Sectional Study, Generalized
BIOSTATISTICAL METHODS AND RESEARCH DESIGNS Xihong Lin Department of Biostatistics, University of Michigan, Ann Arbor, MI, USA Keywords: Case-control study, Cohort study, Cross-Sectional Study, Generalized
Navigating Treatment Pathways in Relapsed/Refractory Hodgkin Lymphoma
 Welcome to Managing Hodgkin Lymphoma. I am Dr. John Sweetenham from Huntsman Cancer Institute at the University of Utah. In today s presentation, I will be discussing navigating treatment pathways in relapsed
Welcome to Managing Hodgkin Lymphoma. I am Dr. John Sweetenham from Huntsman Cancer Institute at the University of Utah. In today s presentation, I will be discussing navigating treatment pathways in relapsed
PDF created with pdffactory Pro trial version
 Neuroblastoma Tumor derived from neural crest cell that form the sympathetic ganglia&adrenal medulla. Causes *unknown. *familial neuroblastoma has been reported but is rare. * The incidence is 1:100,000
Neuroblastoma Tumor derived from neural crest cell that form the sympathetic ganglia&adrenal medulla. Causes *unknown. *familial neuroblastoma has been reported but is rare. * The incidence is 1:100,000
Lugano classification: Role of PET-CT in lymphoma follow-up
 CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
microrna PCR System (Exiqon), following the manufacturer s instructions. In brief, 10ng of
 SUPPLEMENTAL MATERIALS AND METHODS Quantitative RT-PCR Quantitative RT-PCR analysis was performed using the Universal mircury LNA TM microrna PCR System (Exiqon), following the manufacturer s instructions.
SUPPLEMENTAL MATERIALS AND METHODS Quantitative RT-PCR Quantitative RT-PCR analysis was performed using the Universal mircury LNA TM microrna PCR System (Exiqon), following the manufacturer s instructions.
A new score predicting the survival of patients with spinal cord compression from myeloma
 Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
How to evaluate tumor response? Yonsei University College of Medicine Kim, Beom Kyung
 How to evaluate tumor response? Yonsei University College of Medicine Kim, Beom Kyung End points in research for solid cancers Overall survival (OS) The most ideal one, but requires long follow-up duration
How to evaluate tumor response? Yonsei University College of Medicine Kim, Beom Kyung End points in research for solid cancers Overall survival (OS) The most ideal one, but requires long follow-up duration
THE IMPORTANCE OF COMORBIDITY TO CANCER CARE AND STATISTICS AMERICAN CANCER SOCIETY PRESENTATION COPYRIGHT NOTICE
 THE IMPORTANCE OF COMORBIDITY TO CANCER CARE AND STATISTICS AMERICAN CANCER SOCIETY PRESENTATION COPYRIGHT NOTICE Washington University grants permission to use and reproduce the The Importance of Comorbidity
THE IMPORTANCE OF COMORBIDITY TO CANCER CARE AND STATISTICS AMERICAN CANCER SOCIETY PRESENTATION COPYRIGHT NOTICE Washington University grants permission to use and reproduce the The Importance of Comorbidity
J 13 (10) : , 1995 STUDY DESIGN AND CONDUCT
 High-Dose Chemotherapy With Hematopoietic Rescue as Primary Treatment for Metastatic Breast Cancer: A Randomized Trial. Bezwoda WR, Seymour L and Dansey RD. J Clin Oncology, 13 (10) : 2483-2489, Oct 1995
High-Dose Chemotherapy With Hematopoietic Rescue as Primary Treatment for Metastatic Breast Cancer: A Randomized Trial. Bezwoda WR, Seymour L and Dansey RD. J Clin Oncology, 13 (10) : 2483-2489, Oct 1995
Smoldering Myeloma: Leave them alone!
 Smoldering Myeloma: Leave them alone! David H. Vesole, MD, PhD Co-Director, Myeloma Division Director, Myeloma Research John Theurer Cancer Center Hackensack University Medical Center Prevalence 1960 2002
Smoldering Myeloma: Leave them alone! David H. Vesole, MD, PhD Co-Director, Myeloma Division Director, Myeloma Research John Theurer Cancer Center Hackensack University Medical Center Prevalence 1960 2002
Systemic Management of Malignant Pleural Mesothelioma
 ESO-ESMO EASTERN EUROPE AND BALKAN REGION MASTERCLASS IN MEDICAL ONCOLOGY 15.June-19.June 2018 Belgrade, Serbia Systemic Management of Malignant Pleural Mesothelioma Dragana Jovanovic University Hospital
ESO-ESMO EASTERN EUROPE AND BALKAN REGION MASTERCLASS IN MEDICAL ONCOLOGY 15.June-19.June 2018 Belgrade, Serbia Systemic Management of Malignant Pleural Mesothelioma Dragana Jovanovic University Hospital
The prognostic value of fast molecular response of marrow disease in patients aged over 1 year with stage 4 neuroblastoma
 E U R O P E A N J O U R N A L O F CA N C E R47 (211) 1193 122 available at www.sciencedirect.com journal homepage: www.ejconline.com The prognostic value of fast molecular response of marrow disease in
E U R O P E A N J O U R N A L O F CA N C E R47 (211) 1193 122 available at www.sciencedirect.com journal homepage: www.ejconline.com The prognostic value of fast molecular response of marrow disease in
Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C.
 Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
1 st Appraisal Committee meeting Background & Clinical Effectiveness Gillian Ells & Malcolm Oswald 24/11/2016
 Lead team presentation Nivolumab for treating recurrent or metastatic squamous-cell carcinoma of the head and neck after platinum-based chemotherapy [ID971] 1 st Appraisal Committee meeting Background
Lead team presentation Nivolumab for treating recurrent or metastatic squamous-cell carcinoma of the head and neck after platinum-based chemotherapy [ID971] 1 st Appraisal Committee meeting Background
Cancer Prevention & Control in Adolescent & Young Adult Survivors
 + Cancer Prevention & Control in Adolescent & Young Adult Survivors NCPF Workshop July 15-16, 2013 Patricia A. Ganz, MD UCLA Schools of Medicine & Public Health Jonsson Comprehensive Cancer Center + Overview
+ Cancer Prevention & Control in Adolescent & Young Adult Survivors NCPF Workshop July 15-16, 2013 Patricia A. Ganz, MD UCLA Schools of Medicine & Public Health Jonsson Comprehensive Cancer Center + Overview
PET-imaging: when can it be used to direct lymphoma treatment?
 PET-imaging: when can it be used to direct lymphoma treatment? Luca Ceriani Nuclear Medicine and PET-CT centre Oncology Institute of Southern Switzerland Bellinzona Disclosure slide I declare no conflict
PET-imaging: when can it be used to direct lymphoma treatment? Luca Ceriani Nuclear Medicine and PET-CT centre Oncology Institute of Southern Switzerland Bellinzona Disclosure slide I declare no conflict
Whole Body MRI. Dr. Nina Tunariu. Prostate Cancer recurrence, progression and restaging
 Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
Blinded, independent, central image review in oncology trials: how the study endpoint impacts the adjudication rate
 Blinded, independent, central image review in oncology trials: how the study endpoint impacts the adjudication rate Poster No.: C-0200 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit
Blinded, independent, central image review in oncology trials: how the study endpoint impacts the adjudication rate Poster No.: C-0200 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit
UK Musculoskeletal Oncology: Something for All Ages. Lars Wagner, MD Pediatric Hematology/Oncology University of Kentucky
 UK Musculoskeletal Oncology: Something for All Ages Lars Wagner, MD Pediatric Hematology/Oncology University of Kentucky Pediatric-Type Sarcomas of Bone and Soft Tissue The incidence of sarcoma continues
UK Musculoskeletal Oncology: Something for All Ages Lars Wagner, MD Pediatric Hematology/Oncology University of Kentucky Pediatric-Type Sarcomas of Bone and Soft Tissue The incidence of sarcoma continues
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
CA 125 definitions agreed by GCIG November 2005
 CA 125 definitions agreed by GCIG November 2005 The GCIG has agreed criteria for defining response and progression of ovarian carcinoma which use the serum marker CA 125, and the situations where these
CA 125 definitions agreed by GCIG November 2005 The GCIG has agreed criteria for defining response and progression of ovarian carcinoma which use the serum marker CA 125, and the situations where these
Gene expression profiling predicts clinical outcome of prostate cancer. Gennadi V. Glinsky, Anna B. Glinskii, Andrew J. Stephenson, Robert M.
 SUPPLEMENTARY DATA Gene expression profiling predicts clinical outcome of prostate cancer Gennadi V. Glinsky, Anna B. Glinskii, Andrew J. Stephenson, Robert M. Hoffman, William L. Gerald Table of Contents
SUPPLEMENTARY DATA Gene expression profiling predicts clinical outcome of prostate cancer Gennadi V. Glinsky, Anna B. Glinskii, Andrew J. Stephenson, Robert M. Hoffman, William L. Gerald Table of Contents
DISCLOSURE SLIDE. ARGOS: research funding, scientific advisory board
 INTERIM ANALYSIS OF THE PHASE 3 ADAPT TRIAL EVALUATING ROCAPULDENCEL-T (AGS-003), AN INDIVIDUALIZED IMMUNOTHERAPY FOR THE TREATMENT OF NEWLY-DIAGNOSED PATIENTS WITH METASTATIC RENAL CELL CARCINOMA (MRCC)
INTERIM ANALYSIS OF THE PHASE 3 ADAPT TRIAL EVALUATING ROCAPULDENCEL-T (AGS-003), AN INDIVIDUALIZED IMMUNOTHERAPY FOR THE TREATMENT OF NEWLY-DIAGNOSED PATIENTS WITH METASTATIC RENAL CELL CARCINOMA (MRCC)
Tumor Growth Rate (TGR) A New Indicator of Antitumor Activity in NETS? IPSEN NET Masterclass Athens, 12 th November 2016
 1 Tumor Growth Rate (TGR) A New Indicator of Antitumor Activity in NETS? IPSEN NET Masterclass Athens, 12 th November 2016 Philippe RUSZNIEWSKI ENETS Centre of Excellence, Beaujon Hospital, Clichy, France
1 Tumor Growth Rate (TGR) A New Indicator of Antitumor Activity in NETS? IPSEN NET Masterclass Athens, 12 th November 2016 Philippe RUSZNIEWSKI ENETS Centre of Excellence, Beaujon Hospital, Clichy, France
SYNOPSIS PROTOCOL N UC-0107/1602
 SYNOPSIS PROTOCOL N UC-0107/1602 A) TRIAL IDENTIFICATION SPONSOR PROTOCOL CODE NUMBER: UC-0107/1602 VERSION (NR & DATE): 0.1, MARCH 2016 TRIAL TITLE: Extracranial Stereotactic Body Radiation Therapy (SBRT)
SYNOPSIS PROTOCOL N UC-0107/1602 A) TRIAL IDENTIFICATION SPONSOR PROTOCOL CODE NUMBER: UC-0107/1602 VERSION (NR & DATE): 0.1, MARCH 2016 TRIAL TITLE: Extracranial Stereotactic Body Radiation Therapy (SBRT)
Designing Studies of Diagnostic Imaging
 Designing Studies of Diagnostic Imaging Chaya S. Moskowitz, PhD With thanks to Nancy Obuchowski Outline What is study design? Building blocks of imaging studies Strategies to improve study efficiency What
Designing Studies of Diagnostic Imaging Chaya S. Moskowitz, PhD With thanks to Nancy Obuchowski Outline What is study design? Building blocks of imaging studies Strategies to improve study efficiency What
THORACIC MALIGNANCIES
 THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
Best Papers. F. Fusco
 Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
FOLLICULAR LYMPHOMA: US vs. Europe: different approach on first relapse setting?
 Indolent Lymphoma Workshop Bologna, Royal Hotel Carlton May 2017 FOLLICULAR LYMPHOMA: US vs. Europe: different approach on first relapse setting? Armando López-Guillermo Department of Hematology, Hospital
Indolent Lymphoma Workshop Bologna, Royal Hotel Carlton May 2017 FOLLICULAR LYMPHOMA: US vs. Europe: different approach on first relapse setting? Armando López-Guillermo Department of Hematology, Hospital
Targeting and Treating Cancer
 Targeting and Treating Cancer Mark R. Baker, Chief Executive Officer Jefferies Healthcare Conference June 2015 Disclosure Notice This presentation may contain projections and other forward-looking statements
Targeting and Treating Cancer Mark R. Baker, Chief Executive Officer Jefferies Healthcare Conference June 2015 Disclosure Notice This presentation may contain projections and other forward-looking statements
Framework for Defining Evidentiary Standards for Biomarker Qualification: Minimal Residual Disease (MRD) in Multiple Myeloma (MM)
 Framework for Defining Evidentiary Standards for Biomarker Qualification: Minimal Residual Disease (MRD) in Multiple Myeloma (MM) MRD in Multiple Myeloma Team Biomarker Qualification Workshop Framework
Framework for Defining Evidentiary Standards for Biomarker Qualification: Minimal Residual Disease (MRD) in Multiple Myeloma (MM) MRD in Multiple Myeloma Team Biomarker Qualification Workshop Framework
Neuroblastoma. mibg in its Diagnosis and Management. Judy Moyes' V. Ralph McCready Ann Fullbrook
 Judy Moyes' V. Ralph McCready Ann Fullbrook Neuroblastoma mibg in its Diagnosis and Management With 241 Figures Springer-Verlag London Berlin Heidelberg New York Paris Tokyo Judy S.E. Moyes. MA (Cantab).
Judy Moyes' V. Ralph McCready Ann Fullbrook Neuroblastoma mibg in its Diagnosis and Management With 241 Figures Springer-Verlag London Berlin Heidelberg New York Paris Tokyo Judy S.E. Moyes. MA (Cantab).
Integrating FDG PET data for lymphoma management. Michel Meignan, France
 Integrating FDG PET data for lymphoma management Michel Meignan, France Combining metabolic data from baseline, interim or post treatment PET PET Data can be combined: 1. Together 2. With baseline clinical
Integrating FDG PET data for lymphoma management Michel Meignan, France Combining metabolic data from baseline, interim or post treatment PET PET Data can be combined: 1. Together 2. With baseline clinical
Chromosome 1p and 11q Deletions and Outcome in Neuroblastoma
 original article Chromosome 1p and 11q Deletions and Outcome in Neuroblastoma Edward F. Attiyeh, M.D., Wendy B. London, Ph.D., Yael P. Mossé, M.D., Qun Wang, M.D., Ph.D., Cynthia Winter, B.A., Deepa Khazi,
original article Chromosome 1p and 11q Deletions and Outcome in Neuroblastoma Edward F. Attiyeh, M.D., Wendy B. London, Ph.D., Yael P. Mossé, M.D., Qun Wang, M.D., Ph.D., Cynthia Winter, B.A., Deepa Khazi,
18F-FDG PET/CT Versus I-131 MIBG Scan in Diagnosis of Neuroblastoma Osseous Infiltrates; Comparative Study
 Egyptian J. Nucl. Med., Vol. 11, No. 1, Dec 2015 28 Original article, Oncology 18F-FDG PET/CT Versus I-131 MIBG Scan in Diagnosis of Neuroblastoma Osseous Infiltrates; Comparative Study Amr, M 1. Kotb,
Egyptian J. Nucl. Med., Vol. 11, No. 1, Dec 2015 28 Original article, Oncology 18F-FDG PET/CT Versus I-131 MIBG Scan in Diagnosis of Neuroblastoma Osseous Infiltrates; Comparative Study Amr, M 1. Kotb,
NOTE: This policy is not effective until March 1, To view the current policy, click here.
 Medical Policy Manual Topic: Hematopoietic Stem-Cell Transplantation for Solid Tumors of Childhood Date of Origin: May 2010 Section: Transplant Last Reviewed Date: August 2012 Policy No: 45.37 Effective
Medical Policy Manual Topic: Hematopoietic Stem-Cell Transplantation for Solid Tumors of Childhood Date of Origin: May 2010 Section: Transplant Last Reviewed Date: August 2012 Policy No: 45.37 Effective
Teaching A Way of Implementing Statistical Methods for Ordinal Data to Researchers
 Journal of Mathematics and System Science (01) 8-1 D DAVID PUBLISHING Teaching A Way of Implementing Statistical Methods for Ordinal Data to Researchers Elisabeth Svensson Department of Statistics, Örebro
Journal of Mathematics and System Science (01) 8-1 D DAVID PUBLISHING Teaching A Way of Implementing Statistical Methods for Ordinal Data to Researchers Elisabeth Svensson Department of Statistics, Örebro
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010
 Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
STUDY ON CHANGES OF PLASMA CELL-FREE DNA OF EPSTEIN-BARR VIRUS DURING CHEMORADIOTHERAPY OF NASOPHARYNGEAL CARCINOMA PATIENTS
 Journal of military pharmacomedicine n o 12019 STUDY ON CHANGES OF PLASMA CELLFREE DNA OF EPSTEINBARR VIRUS DURING CHEMORADIOTHERAPY OF NASOPHARYNGEAL CARCINOMA PATIENTS Pham Quynh Huong 1 ; Vu Nguyen
Journal of military pharmacomedicine n o 12019 STUDY ON CHANGES OF PLASMA CELLFREE DNA OF EPSTEINBARR VIRUS DURING CHEMORADIOTHERAPY OF NASOPHARYNGEAL CARCINOMA PATIENTS Pham Quynh Huong 1 ; Vu Nguyen
Ependymoma Programme Synopsis
 Ependymoma Programme Synopsis TITLE SPONSOR PROTOCOL NUMBER EUDRACT NUMBER NATIONAL INVESTIGATOR- COORDINATOR SIOP Ependymoma program II: An International Clinical Program for the diagnosis and treatment
Ependymoma Programme Synopsis TITLE SPONSOR PROTOCOL NUMBER EUDRACT NUMBER NATIONAL INVESTIGATOR- COORDINATOR SIOP Ependymoma program II: An International Clinical Program for the diagnosis and treatment
BEST PRACTICES FOR IMPLEMENTATION AND ANALYSIS OF PAIN SCALE PATIENT REPORTED OUTCOMES IN CLINICAL TRIALS
 BEST PRACTICES FOR IMPLEMENTATION AND ANALYSIS OF PAIN SCALE PATIENT REPORTED OUTCOMES IN CLINICAL TRIALS Nan Shao, Ph.D. Director, Biostatistics Premier Research Group, Limited and Mark Jaros, Ph.D. Senior
BEST PRACTICES FOR IMPLEMENTATION AND ANALYSIS OF PAIN SCALE PATIENT REPORTED OUTCOMES IN CLINICAL TRIALS Nan Shao, Ph.D. Director, Biostatistics Premier Research Group, Limited and Mark Jaros, Ph.D. Senior
Radiotherapy symptoms control in bone mets. Francesco Cellini GemelliART. Ernesto Maranzano,MD. Session 5: Symptoms management
 Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
The case for maintenance rituximab in FL
 New-York, October 23 rd 2015 The case for maintenance rituximab in FL Pr. Gilles SALLES For FL patients, progression-free survival still needs to be improved Median R-CHVP-I 66 months P
New-York, October 23 rd 2015 The case for maintenance rituximab in FL Pr. Gilles SALLES For FL patients, progression-free survival still needs to be improved Median R-CHVP-I 66 months P
Evidence tables from the systematic literature search for premature ovarian insufficiency surveillance in female CAYA cancer survivors.
 Evidence tables from the systematic literature search for premature ovarian insufficiency surveillance in female CAYA cancer survivors. Who needs surveillance? Chiarelli et al. Early menopause and Infertility
Evidence tables from the systematic literature search for premature ovarian insufficiency surveillance in female CAYA cancer survivors. Who needs surveillance? Chiarelli et al. Early menopause and Infertility
Evaluation of SIRFLOX Study Results. Prof. V. Heinemann CCC LMU, Klinikum Grosshadern Ludwig-Maximilian-University of Munich, Germany
 Evaluation of SIRLX Study Results Prof. V. Heinemann CCC LMU, Klinikum Grosshadern Ludwig-Maximilian-University of Munich, Germany ESM Guideline: Response is a Goal of Treatment Performance Status of the
Evaluation of SIRLX Study Results Prof. V. Heinemann CCC LMU, Klinikum Grosshadern Ludwig-Maximilian-University of Munich, Germany ESM Guideline: Response is a Goal of Treatment Performance Status of the
Key Statistical Concepts in Cancer Research
 Key Statistical Concepts in Cancer Research Qian Shi, PhD, and Daniel J. Sargent, PhD The authors are affiliated with the Department of Health Science Research at the Mayo Clinic in Rochester, Minnesota.
Key Statistical Concepts in Cancer Research Qian Shi, PhD, and Daniel J. Sargent, PhD The authors are affiliated with the Department of Health Science Research at the Mayo Clinic in Rochester, Minnesota.
FAST FACTS Eligibility Reviewed and Verified By MD/DO/RN/LPN/CRA Date MD/DO/RN/LPN/CRA Date Consent Version Dated
 Page 1 of 5 COG-ANBL1531: A Phase 3 Study of 131I-Metaiodobenzylguanidine (131I-MIBG) or Crizotinib Added to Intensive Therapy for Children with Newly Diagnosed High-Risk (NBL) (IND# 134379) FAST FACTS
Page 1 of 5 COG-ANBL1531: A Phase 3 Study of 131I-Metaiodobenzylguanidine (131I-MIBG) or Crizotinib Added to Intensive Therapy for Children with Newly Diagnosed High-Risk (NBL) (IND# 134379) FAST FACTS
CON: Removal of the Breast Primary in Patients with Metastatic Breast Cancer
 CON: Removal of the Breast Primary in Patients with Metastatic Breast Cancer Amelia B. Zelnak, M.D., M.Sc. Assistant Professor of Hematology and Medical Oncology Winship Cancer Institute Emory University
CON: Removal of the Breast Primary in Patients with Metastatic Breast Cancer Amelia B. Zelnak, M.D., M.Sc. Assistant Professor of Hematology and Medical Oncology Winship Cancer Institute Emory University
